Is pleurectomy and decortication superior to palliative care in the treatment of malignant pleural mesothelioma?
|
|
|
- Wilfrid Newman
- 8 years ago
- Views:
Transcription
1 doi: /icvts Interactive CardioVascular and Thoracic Surgery 12 (2011) Best evidence topic - Thoracic oncologic Is pleurectomy and decortication superior to palliative care in the treatment of malignant pleural mesothelioma? a a b b, Imran Zahid, Sumera Sharif, Tom Routledge, Marco Scarci * a Imperial College London, South Kensington Campus, London SW7 2AZ, UK b Department of Thoracic Surgery, Guy s Hospital, Great Maze Pond, London SE1 9RT, UK Received 18 September 2010; received in revised form 25 January 2011; accepted 27 January 2011 Summary A best evidence topic in thoracic surgery was written according to a structured protocol. The question addressed was whether pleurectomyy decortication (PyD) is superior to palliative care in the treatment of patients with malignant pleural mesothelioma (MPM). Overall 80 papers were found using the reported search, of which 11 represented the best evidence to answer the clinical question. The authors, journal, date and country of publication, patient group studied, study type, relevant outcomes and results are tabulated. We conclude that PyD may lead to superior survival rates but at the expense of higher morbidity rates to palliative treatment. Six studies reported patient outcomes after use of radical PyD to treat patients with MPM. Radical PyD leads to a higher median survival than supportive care (14.5 vs. 4.5 months) and non-radical decortication (15.3 vs. 7.1 months, P-0.000). However, radical PyD had a complication rate of 30%, hospital stay of 12 days with an operative mortality rate of 9.1%. One-year survival rate was 65% but this fell to 0 24% at three years. Three studies highlighted the use of palliative chemotherapy to manage patients with MPM. Median survival (14 vs. 10 months) was higher in patients who received chemotherapy early compared to those on a delayed protocol. Early chemotherapy had a longer time to disease progression (25 vs. 11 weeks, Ps0.1) and greater one-year survival (66% vs. 36%) than the delayed group. Active symptom control (ASC) alone had lower symptom control rates than the combination of ASC plus MVP (mitomycinqvinblastineqcisplatin) (7% vs. 11%, Ps0.0017) and ASC plus vinorelbine (4% vs. 7%, Ps0.047). Three studies reported results of palliative surgery in patients with known MPM. Median survival period was 213 days with a 30-day mortality rate of 7.8%. Survival rates reduced from 70.6% at three months to 25.5% at one-year post-surgery. Prolonged air-leak and postoperative empyema complicated 9.8% and 4% of patients, respectively. PyD is a morbid operation that is associated with significant perioperative mortality and complication rates. Although a number of retrospective studies have shown a small benefit in survival with PyD, the heavily documented similarity in patient outcomes between PyD and extrapleural pneumonectomy along with the results of the Mesothelioma and Radical Surgery trial, should induce the surgical community to consider the use of PyD only in patients with malignant mesothelioma enrolled in prospective trials Published by European Association for Cardio-Thoracic Surgery. All rights reserved. Keywords: Pleurectomyydecortication; Malignant mesothelioma; Supportive care 1. Introduction A best evidence topic was constructed according to a structured protocol. This is fully described in the ICVTS w1x. 2. Three-part question In wpatients with malignant pleural mesotheliomax is wpleurectomyydecortication (PyD)x superior to wpalliative carex in terms of wmorbidity, symptom control and survivalx. 3. Clinical scenario You review a 63-year-old retired miner, with a known diagnosis of malignant pleural mesothelioma (MPM), complaining of chest pain and worsening cough. CT chest and abdomen evaluated the tumour to be International Meso- *Corresponding author. Tel.: q ; fax: q address: marco.scarci@mac.com (M. Scarci) Published by European Association for Cardio-Thoracic Surgery thelioma Interest Group (IMIG) stage III disease with no chest wall involvement. You are unsure as to whether undergoing radical pleurectomyydecortication (P/D) would be superior to palliative care. You resolve to check the literature. 4. Search strategy Medline search 1950 to August 2010 was performed using the OVID interface wpleurectomyydecortication.mp OR PyD.mpx OR wexp Mesotheliomayor mesothelioma.mp.x 5. Search outcome Eighty papers were found using the reported search. From these, 11 papers were identified that provided the best evidence to answer the question. These are presented in Table 1. In addition, the reference list of each paper was searched.
2 I. Zahid et al. / Interactive CardioVascular and Thoracic Surgery 12 (2011) Table 1. Best evidence papers Author, date and country, Patient group Outcomes Key results Comments Study type (level of evidence) Schipper et al., (2008), Single centre experience Median survival Total PyD: 17.2 Total PyD leads to superior Ann Thorac Surg, UK, over 18 years (ns285) (months) Subtotal PyD: 8.1 patient outcomes than w2x Exploration without subtotal PyD and Total PyD (ns10) resection: 6.8 exploration without Retrospective Subtotal PyD (ns34) resection cohort study Exploration without Survival )31 days Total PyD: 0.74 resection (ns22) postoperative Subtotal PyD: 1.62 (Hazard ratio) Exploration without resection: 1.97 Hospital stay (days) Total PyD: 6.5 Subtotal PyD: 6.5 Exploration without resection: 6 Complications Total PyD: 20% Luckraz et al., (2010), Single centre experience Thirty-day mortality 1.1% Multimodality therapy Eur J Cardiothorac Surg, over 30 years ns85 provides leads to lower UK, w3x Complications (%) PyD: 18 complication and higher PyD (ns34) PyDqCTqRT: 13 survival rates Retrospective cohort PyDqCTqRT (ns24) (P-0.02) (90% 95% tumour excision) Median survival PyD: 8.3 (months) PyDqCTqRT: 26 (P-0.001) Flores et al., (2008), Retrospective Operative mortality 4% PyD can manage malignant J Thorac Cardiovasc Surg, multicentre experience mesothelioma but leads to USA, w4x over 16 years Respiratory 6.4% high respiratory complications complications Retrospective PyD (ns278) cohort study Survival (months) 16 Okada et al., (2008), Single centre experience Median survival PyD: 17 months Pleurectomyydecortication Interact CardioVasc over 20 years EPP: 13 months results in equivalent Thorac Surg, Japan, survival rates to EPP w5x PyD (ns34) Three-year survival PyD: 24% EPP (ns31) rate EPP: 33% Retrospective cohort study Operative mortality PyD: 0 Major complication PyD: 15% rate postoperative Nakas et al., (2008), Single centre study Mortality: There was a significantly Eur J Cardiothorac Surg, over 10 years ns days 5.9 vs. 9.8% (Ps0.36) higher 90-day mortality in UK, w6x 90 days 9.8 vs. 29.4% (Ps0.012) patients with radical Group R: surgery Cohort study Radical PyD (ns51) Morbidity 55 vs. 28% (Ps0.023) Major complications Group NR: Hospital stay 12 vs. 10 (Ps0.99) included chylothorax, Non-radical (days) oesophageal rupture, decortication (ns51) bleeding and diaphragmatic Median survival 15.3 vs. 7.1 (P-0.000) patch disruption (months) When patients were split into subgroups according to cell type, radical surgery had longer survival only for epithelioid cell type Best Evidence Topic Maziak et al., (2005), Thirty-two studies were Median survival PyD: 14.5 Three out of eight Lung Cancer, Canada, identified involving (months) Supportive: 4.5 prospective studies w7x 3152 patients reported increased survival Operative mortality 9.1% for PyD compared to Systematic review All patients had a supportive care (level 2a) known diagnosis of MPM Complications 30% (Continued on next page)
3 814 I. Zahid et al. / Interactive CardioVascular and Thoracic Surgery 12 (2011) Table 1. (Continued) Author, date and country, Patient group Outcomes Key results Comments Study type (level of evidence) PyD leads to very high complication rates O Brien et al., (2006), Multicentre Time to commence Early: 0 weeks Early introduction of Ann Oncol, UK, w8x randomised control trial chemotherapy Delayed: 17 weeks chemotherapy produces over four years (range 3 96) greater symptom Randomised control trial improvement and survival (level 1b) Early chemotherapy Median time to Early: 25 weeks rates in patients with (ns21) symptom progression Delayed: 11 weeks malignant mesothelioma (Ps0.1) Delayed chemotherapy (ns17) Patients requiring Early: ns4 second line Delayed: ns0 All patients had WHO chemotherapy performance score F2, GFR G35 mlyh, no Median survival Early: 14 months rapid change on CXR Delayed: 10 months over four weeks preoperative One-year survival Early: 66% rate Delayed: 36% Mean change in quality of life scores at follow-up Physical functioning: Early: (Ps0.6) Delayed: (Ps0.008) Dyspnoea: Early: (Ps0.7) Delayed: (Ps0.025) Muers et al., (2008), Multicentre Completion of ASCqMVP: 64% Addition of chemotherapy Lancet, UK, w9x randomised control trial treatment schedule ASCqV: 50% to ASC leads to greater involving 409 patients tumour response rate and Randomised control trial over five years Tumour response rate Formally assessed: symptomatic improvement (level 1b) ASCqMVP: 10% in patients with MPM Active symptom ASCqV: 16% control (ASC) alone (ns136) Clinician opinion at 15 weeks: ASC: 14% ASCqMVP ASCqMVP: 29% chemotherapy (ns137) ASCqV: 31% ASCqvinorelbine Symptom Chest pain: chemotherapy (ns136) improvement ASC: 7% ASCqMVP: 11% (Ps0.0017) Median time from ASCqV: 10% (Ps0.051) diagnosis to randomisations60 days Lethargy: Patients were mainly ASC: 4% IMIG disease stage III ASCqMVP: 9% (Ps0.54) (31%) or IV (45%) ASCqV: 7% (Ps0.047) Sweating: ASC: 5% ASCqMVP: 9% (Ps0.012) ASCqV: 6% (Ps0.48) Side effect profile Haematological: ASC: 0% ASCqMVP: 13.3% ASCqV: 36% Quality of life Physical functioning: EORTC questionnaire ASC: 66 score at three months ASCqMVP: 70 ASCqV: 70 Global quality of life: ASC: 56 (Continued on next page)
4 I. Zahid et al. / Interactive CardioVascular and Thoracic Surgery 12 (2011) Table 1. (Continued) Author, date and country, Patient group Outcomes Key results Comments Study type (level of evidence) ASCqMVP: 56 ASCqV: 57 Survival Hazard ratio ASC: 1 ASCqMVP: 0.99 (Ps0.95) ASCqV: 0.77 (Ps0.04) ASCqchemotherapy: 0.89 (Ps0.29) % Alive at one year: ASC: 29 ASCqchemotherapy: 32 Median survival (months): ASC: 7.6 ASCqV: 9.5 ASCqchemotherapy: 8.5 Merritt et al., (2001), Single centre Treatment types Talc pleurodesis: ns70 Palliative treatment for J Surg Oncol, retrospective study Radiotherapy: ns30 MPM leads to a short Canada, w10x over 12 years Chemotherapy: ns9 overall survival period which was not affected by Retrospective Palliative treatment Median survival 213 days (95% CI: the type of palliative cohort study (ns101) ) treatment option (Ps0.59) MPM was confirmed Mortality at 89.1% using surgical follow-up biopsy and immunohistochemistry Aziz et al., (2002), Single centre experience Median survival PyD: 14 PyD leads to equivalent Eur J Cardiothorac Surg, over nine years (months) Supportive care: 7 survival rates to EPP UK, w11x (range 1 19) PyD (ns47) EPP: 13 Retrospective EPP (ns64) cohort study Thirty-day operative PyD: 0 mortality Major complication rate PyD: 4% incl. bleeding Survival rate for PyD One year: 65% Three years: 0% Martin-Ucar et al., (2001), Single centre Treatment types VATS pleurectomy: ns17 Surgical debulking with Eur J Cardiothorac Surg prospective study over VATS decortication: ns3 palliative intent produces UK, w12x four years Open decortication: ns31 poor survival rates Prospective cohort study Palliative surgical Median hospital stay Seven days (range 2 17) It leads to high morbidity debulking (ns51) postoperative rates and low symptom improvement rates in MPM was confirmed Thirty-day mortality 7.8% patients with MPM using surgical biopsy and Morbidity Prolonged air-leak (9.8%) immunohistochemistry Postoperative empyema (4%) Best Evidence Topic Median survival 215 days (95% CI: ) Survival rate Three months: 70.6% Six months: 47.1% One-year: 25.5% Symptom Three months: 78.4% improvement Six months: 41.2% One-year: 25.5% EPP, extrapleural pneumonectomy; MPM, malignant pleural mesothelioma; RT, radiotherapy; GFR, glomerular filtration rate; CXR, chest X-ray; VATS, videoassisted thoracoscopic surgery.
5 816 I. Zahid et al. / Interactive CardioVascular and Thoracic Surgery 12 (2011) Results Palliative management of MPM includes the use of chemotherapy or surgery to reduce patient symptoms or prolong survival without the prospect of a cure. We define the operative technique of radicalytotal PyD as complete parietal, visceral and mediastinal pleurectomy, with or without removal of the pericardium or ipsilateral hemi-diaphragm with curative intent. Any study that deviates from this definition of PyD is highlighted. Diagnosis of MPM was confirmed by histopathology in all studies unless stated otherwise. Six studies reported patient outcomes after use of PyD to treat patients with MPM. Schipper et al. w2x managed MPM using total PyD (ns10), subtotal PyD (ns34) or exploration without resection (ns22). Subtotal PyD is a non-radical decortication that involves removal of up to 70% of the parietal pleura. Total PyD had greater median survival period (17.2 vs. 8.1 vs. 6.8 months) than subtotal PyD and exploration without resection, respectively. Luckraz et al. w3x reported patient outcomes after PyD with chemoradiotherapy (ns24) and PyD alone (ns34). Multimodality therapy produced higher median survival rates (26 vs. 8.3 months, P-0.001) and lower complication rates (13% vs. 18%, P-0.02) than PyD alone. Flores et al. w4x reported longer median survival (16 vs. 12 months, P-0.001) with PyD compared to extrapleural pneumonectomy (EPP). Patients with epithelial MPM or American Joint Committee on Cancer (AJCC) stage I disease had greater survival than non-epithelial or higher stage disease (P-0.001). In contrast, Okada et al. w5x reported equivalent median (17 vs. 13 months, Ps0.922) and three-year survival rates (24% vs. 33%, Ps0.922) with PyD compared to EPP. However, they also found greater survival with epithelial MPM (Ps0.0048) and stage I disease (Ps0.8927) compared to non-epithelial and stage II disease, respectively. Pivotally, Treasure w13x is aiming to follow-up his Mesothelioma and Radical Surgery (MARS) trial, with a multicentre randomised control trial, provisionally called MARS-2, to determine whether radical PyD is superior to best continued care. Interestingly, initial results of the MARS trial wtreasure T, Waller D, Tan C, Entwisle J, O Brien M, O Bryne K, Thomas G, Snee M, Spicer J, Landau D, Lang-Lazdunski L, Bliss J, Peckitt C, Rogers S, Marriage E, Coombes G, Webster-smith M and Peto J. Principal results of the feasibility phase of the Mesothelioma and Radical Surgery trial (MARS-feasibility) 2010 Available from have demonstrated a clear disadvantage of conducting radical EPP surgery (ns24) compared to no-epp (ns26) with lower 12- month survival rates (52.2% vs. 73.1%) with a hazard ratio of 2.75 (95% CI: , Ps0.02) in favour of no EPP. Although the MARS trial analysed patient outcomes after EPP, radical PyD is a morbid operation that leads to similar survival rates as EPP. Nakas et al. w6x compared outcomes of radical PyD (ns51) to palliative non-radical decortication (ns51), which spared the diaphragm and pericardium. Although a pathological diagnosis of MPM was established in only 65% of patients, the remainder were treated on the basis of highly suspicious pleural biopsies. Radical PyD led to higher morbidity rates (55% vs. 28%, Ps0.023) and equivalent hospital stay (12 vs. 10 days, Ps0.99) compared to non-radical decortication. Maziak et al. w7x systematically reviewed 32 studies and found PyD had a longer median survival (14.5 vs. 4.5 months) than supportive care but led to an operative mortality rate of 9.1% with a complication rate of 30%. Two studies highlighted patient outcomes after palliative use of chemotherapy to manage unresectable MPM. O Brien et al. w8x randomised patients to receive chemotherapy either early (ns21) or after a delay (ns17) of 17 weeks. Early chemotherapy produced a longer median survival period (14 vs. 10 months) and greater one-year survival rates (66% vs. 36%) than delayed chemotherapy. Muers et al. w9x reported significant improvements in chest pain (11% vs. 7%, Ps0.0017) and sweating (9% vs. 5%, Ps0.012) in patients with adjunctive chemotherapy to active symptom control (ASC) alone. Adjunctive chemotherapy conferred a marginal survival advantage (8.5 vs. 7.6 months) compared to ASC alone. Three studies reported results of palliative surgery in patients with known MPM. Merritt et al. w10x carried out talc pleurodesis (ns70), chemotherapy (ns30) and radiotherapy (ns9) with palliative intent. Median survival was 213 days with a high mortality rate of 89.1% at four-year follow-up. Aziz et al. w11x found that palliative PyD had a longer median survival period (14 vs. 7 vs. 13 months) than supportive care but equivalent to EPP, respectively. PyD led to major complications in 4% of cases with no mortalities at 30 days postoperative. Survival rates were 65% at one-year but fell to 0% by three years postoperative. Martin-Ucar et al. w12x performed thoracoscopic (ns3) and open (ns31) decortications and thoracoscopic pleurectomies (ns17), to debulk disease with palliative intent. The median survival period was 215 days. Survival rates fell from 70.6% at three months to 25.5% at one-year postoperative. The optimal approach for decortication is currently debated. Srivastava et al. w14x reported effective symptoms palliation using VATS decortication in patients with MPM. 7. Clinical bottom line PyD is a morbid operation that is associated with significant perioperative mortality and complication rates. Although a number of retrospective studies have shown a small benefit in survival with PyD, the heavily documented similarity in patient outcomes between PyD and EPP along with the results of the MARS trial, should induce the surgical community to consider the use of PyD only in patients with malignant mesothelioma enrolled in prospective trials. References w1x Dunning J, Prendergast B, Mackway-Jones K. Towards evidence-based medicine in cardiothoracic surgery: best BETS. Interact CardioVasc Thorac Surg 2003;2: w2x Schipper PH, Nichols FC, Thomse KM, Deschamps C, Cassivi SD, Allen MS, Pairolero PC. Malignant pleural mesothelioma: surgical management in 285 patients. Ann Thorac Surg 2008;85: ; discussion 264. w3x Luckraz H, Rahman M, Patel N, Szafranek A, Gibbs AR, Butchart EG. Three decades of experience in the surgical multi-modality management of pleural mesothelioma. Eur J Cardiothorac Surg 2010;37:
6 I. Zahid et al. / Interactive CardioVascular and Thoracic Surgery 12 (2011) w4x Flores RM, Pass HI, Seshan VE, Dycoco J, Zakowski M, Carbone M, Bains MS, Rusch VW. Extrapleural pneumonectomy versus pleurectomyydecortication in the surgical management of malignant pleural mesothelioma: results in 663 patients. J Thorac Cardiovasc Surg 2008;135: , 626.e1 626.e3. w5x Okada M, Mimura T, Ohbayashi C, Sakuma T, Soejima T, Tsubota N. Radical surgery for malignant pleural mesothelioma: results and prognosis. Interact CardioVasc Thorac Surg 2008;7: w6x Nakas A, Trousse DS, Martin-Ucar AE, Waller DA. Open lung-sparing surgery for malignant pleural mesothelioma: the benefits of a radical approach within multimodality therapy. Eur J Cardiothorac Surg 2008; 34: w7x Maziak DE, Gagliardi A, Haynes AE, Mackay JA, Evans WK, Cancer Care Ontario Program in Evidence-based Care Lung Cancer Disease Site Group. Surgical management of malignant pleural mesothelioma: a systematic review and evidence summary. Lung Cancer 2005;48: w8x O Brien ME, Watkins D, Ryan C, Priest K, Corbishley C, Norton A, Ashley S, Rowell N, Sayer R. A randomised trial in malignant mesothelioma (M) of early (E) versus delayed (D) chemotherapy in symptomatically stable patients: the MED trial. Ann Oncol 2006;17: w9x Muers MF, Stephens RJ, Fisher P, Darlison L, Higgs CM, Lowry E, Nicholson AG, O Brien M, Peake M, Rudd R, Snee M, Steele J, Girling DJ, Nankivell M, Pugh C, Parmar MK, MS01 Trial Management Group. Active symptom control with or without chemotherapy in the treatment of patients with malignant pleural mesothelioma (MS01): a multicentre randomised trial. Lancet 2008;371: w10x Merritt N, Blewett CJ, Miller JD, Bennett WF, Young JEM, Urschel JD. Survival after conservative (palliative) management of pleural malignant mesothelioma. J Surg Oncol 2001;78: w11x Aziz T, Jilaihawi A, Prakash D. The management of malignant pleural mesothelioma; single centre experience in 10 years. Eur J Cardiothorac Surg 2002;22: w12x Martin-Ucar AE, Edwards JG, Rengajaran A, Muller S, Waller DA. Palliative surgical debulking in malignant mesothelioma. Predictors of survival and symptom control. Eur J Cardiothorac Surg 2001;20: w13x Treasure T. Surgery for mesothelioma: MARS landing and future missions. Eur J Cardiothorac Surg 2010;3: w14x Srivastava V, Dunning J, Au J. Does video-assisted thoracoscopic decortication in advanced malignant mesothelioma improve prognosis? Interact CardioVasc Thorac Surg 2009;8: Work in Editorial New Ideas Progress Report Protocol Institutional Report ESCVS Article Proposal for Bailout Procedure Negative Results Follow-up Paper State-of-the-art Best Evidence Topic Nomenclature Historical Pages Brief Case Report Communication
Surgical therapy of. who should be operated
 SAMO Interdisciplinary Workshop on Chest Tumors Lucerne, 13th and 14th January 2012 Surgical therapy of mesothelioma, who should be operated Walter Weder MD Professor of Surgery University Hospital Zurich
SAMO Interdisciplinary Workshop on Chest Tumors Lucerne, 13th and 14th January 2012 Surgical therapy of mesothelioma, who should be operated Walter Weder MD Professor of Surgery University Hospital Zurich
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
How To Treat Mesothelioma
 Mesothelioma in the UK Liz Darlison Mesothelioma UK The National Macmillan Mesothelioma Resource Centre June 2010 Mesothelioma Applied Research Foundation - 2010 www.curemeso.org Contents Size of Mesothelioma
Mesothelioma in the UK Liz Darlison Mesothelioma UK The National Macmillan Mesothelioma Resource Centre June 2010 Mesothelioma Applied Research Foundation - 2010 www.curemeso.org Contents Size of Mesothelioma
Malignant pleural mesothelioma P/D vs. EPP
 3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
Malignant pleural mesothelioma: outcome of limited surgical management
 Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Correspondence should be addressed to Sayonara Papaspyros; sayonarafo@yahoo.com.br
 ISRN Surgery, Article ID 817203, 13 pages http://dx.doi.org/10.1155/2014/817203 Review Article Surgical Management of Malignant Pleural Mesothelioma: Impact of Surgery on Survival and Quality of Life Relation
ISRN Surgery, Article ID 817203, 13 pages http://dx.doi.org/10.1155/2014/817203 Review Article Surgical Management of Malignant Pleural Mesothelioma: Impact of Surgery on Survival and Quality of Life Relation
A systematic review of lungsparing extirpative surgery for pleural mesothelioma
 RESEARCH A systematic review of lungsparing extirpative surgery for pleural mesothelioma Elaine Teh 1 + Francesca Fiorentino 2 + Carol Tan 3 + Tom Treasure 2 1 The Rayne Institute (King s College London),
RESEARCH A systematic review of lungsparing extirpative surgery for pleural mesothelioma Elaine Teh 1 + Francesca Fiorentino 2 + Carol Tan 3 + Tom Treasure 2 1 The Rayne Institute (King s College London),
How To Treat A Cancer With A Radical
 Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
MESOTHELIOMA. Not Just a Late Night Commercial. Graciela Hoal, RN, MSN, ACNP-BC
 MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Malignant Mesothelioma
 Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Mesothelioma
 Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Radical surgery for malignant pleural mesothelioma: results and prognosis
 doi:10.1510/icvts.2007.166322 Interactive CardioVascular and Thoracic Surgery 7 (2008) 102 106 www.icvts.org Institutional report - Thoracic general Radical surgery for malignant pleural mesothelioma:
doi:10.1510/icvts.2007.166322 Interactive CardioVascular and Thoracic Surgery 7 (2008) 102 106 www.icvts.org Institutional report - Thoracic general Radical surgery for malignant pleural mesothelioma:
What is the best way to diagnose and stage malignant pleural mesothelioma?
 doi:10.1510/icvts.2010.255893 Interactive CardioVascular and Thoracic Surgery 12 (2011) 254 259 Best evidence topic - Thoracic oncologic What is the best way to diagnose and stage malignant pleural mesothelioma?
doi:10.1510/icvts.2010.255893 Interactive CardioVascular and Thoracic Surgery 12 (2011) 254 259 Best evidence topic - Thoracic oncologic What is the best way to diagnose and stage malignant pleural mesothelioma?
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Multimodal therapy of malignant pleural mesothelioma: is the replacement of radical surgery imminent?
 Interactive CardioVascular and Thoracic Surgery Advance Access published November 21, 2012 Interactive CardioVascular and Thoracic Surgery (2012) 1 7 doi:10.1093/icvts/ivs465 ORIGINAL ARTICLE Multimodal
Interactive CardioVascular and Thoracic Surgery Advance Access published November 21, 2012 Interactive CardioVascular and Thoracic Surgery (2012) 1 7 doi:10.1093/icvts/ivs465 ORIGINAL ARTICLE Multimodal
Malignant Pleural Mesothelioma in Singapore
 RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
Malignant Mesothelioma Current Approaches to a Difficult Problem. Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline
 Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Treatment of mesothelioma in Bloemfontein, South Africa
 European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database
 Featured Article Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database Valerie W. Rusch 1, Dorothy Giroux 2 1 Memorial Sloan-Kettering Cancer Center, New
Featured Article Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database Valerie W. Rusch 1, Dorothy Giroux 2 1 Memorial Sloan-Kettering Cancer Center, New
Articles. Funding Cancer Research UK (CRUK/04/003), the June Hancock Mesothelioma Research Fund, and Guy s and St Thomas NHS Foundation Trust.
 Extra-pleural pneumonectomy versus no extra-pleural pneumonectomy for patients with malignant pleural mesothelioma: clinical outcomes of the Mesothelioma and Radical Surgery (MARS) randomised feasibility
Extra-pleural pneumonectomy versus no extra-pleural pneumonectomy for patients with malignant pleural mesothelioma: clinical outcomes of the Mesothelioma and Radical Surgery (MARS) randomised feasibility
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines
 Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
Surgeons Role in Symptom Management. A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND
 Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
MesoPDT. Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI. Image Assisted Laser Therapy for Oncology
 MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
Surgical treatment for malignant pleural mesothelioma: extrapleural pneumonectomy, pleurectomy/decortication or extended pleurectomy?
 JBUON 2015; 20(2): 376-380 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com REVIEW ARTICLE Surgical treatment for malignant pleural mesothelioma: extrapleural pneumonectomy,
JBUON 2015; 20(2): 376-380 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com REVIEW ARTICLE Surgical treatment for malignant pleural mesothelioma: extrapleural pneumonectomy,
Malignant Mesothelioma: an Update
 Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
Post-operative intrapleural chemotherapy for mesothelioma
 Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Characteristics of Malignant Pleural Mesothelioma in Women
 Characteristics of Malignant Pleural Mesothelioma in Women Andrea S. Wolf, MD, MPH, William G. Richards, PhD, Tamara R. Tilleman, MD, PhD, Lucian Chirieac, MD, Shelley Hurwitz, PhD, Raphael Bueno, MD,
Characteristics of Malignant Pleural Mesothelioma in Women Andrea S. Wolf, MD, MPH, William G. Richards, PhD, Tamara R. Tilleman, MD, PhD, Lucian Chirieac, MD, Shelley Hurwitz, PhD, Raphael Bueno, MD,
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Trimodality therapy for malignant pleural mesothelioma: results from an EORTC phase II multicentre trial
 Eur Respir J 2010; 36: 1362 1369 DOI: 10.1183/09031936.00039510 CopyrightßERS 2010 Trimodality therapy for malignant pleural mesothelioma: results from an EORTC phase II multicentre trial P.E. Van Schil*,
Eur Respir J 2010; 36: 1362 1369 DOI: 10.1183/09031936.00039510 CopyrightßERS 2010 Trimodality therapy for malignant pleural mesothelioma: results from an EORTC phase II multicentre trial P.E. Van Schil*,
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
prognostic scoring systems. We
 Thorax 2000;55:731 735 731 Original articles Prognostic factors for malignant mesothelioma in 142 patients: validation of CALGB and EORTC prognostic scoring systems J G Edwards, K R Abrams, J N Leverment,
Thorax 2000;55:731 735 731 Original articles Prognostic factors for malignant mesothelioma in 142 patients: validation of CALGB and EORTC prognostic scoring systems J G Edwards, K R Abrams, J N Leverment,
Columbia University Mesothelioma Applied Research Foundation - 2009 - www.curemeso.org. Mesothelioma Center www.mesocenter.org
 Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
Does positron emission tomography offer prognostic information in malignant pleural mesothelioma?
 doi:10.1510/icvts.2010.255901 Interactive CardioVascular and Thoracic Surgery 12 (2011) 806 811 www.icvts.org Best evidence topic - Thoracic oncologic Does positron emission tomography offer prognostic
doi:10.1510/icvts.2010.255901 Interactive CardioVascular and Thoracic Surgery 12 (2011) 806 811 www.icvts.org Best evidence topic - Thoracic oncologic Does positron emission tomography offer prognostic
International Journal of Case Reports in Medicine
 International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
the standard of care 2009 5/1/2009 Mesothelioma: The standard of care take home messages PILC 2006 Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009
 Mesothelioma: The standard of care Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009 take home messages PILC 2006 All patients should receive adequate palliation of dyspnea and pain before starting chemotherapy
Mesothelioma: The standard of care Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009 take home messages PILC 2006 All patients should receive adequate palliation of dyspnea and pain before starting chemotherapy
Multimodal management of malignant pleural mesothelioma: where are we today?
 SERIES THORACIC ONCOLOGY Multimodal management of malignant pleural mesothelioma: where are we today? Paul E. Van Schil 1, Isabelle Opitz 2, Walter Weder 2, Christophe De Laet 1, Andreas Domen 1, Patrick
SERIES THORACIC ONCOLOGY Multimodal management of malignant pleural mesothelioma: where are we today? Paul E. Van Schil 1, Isabelle Opitz 2, Walter Weder 2, Christophe De Laet 1, Andreas Domen 1, Patrick
The epidemiology and treatment of mesothelioma in South East England 1985 2002
 The epidemiology and treatment of mesothelioma in South East England 1985 2002 V Mak, E Davies, V Putcha, B Choodari-Oskooei, H Møller King s College London, Thames Cancer Registry, London, UK Correspondence
The epidemiology and treatment of mesothelioma in South East England 1985 2002 V Mak, E Davies, V Putcha, B Choodari-Oskooei, H Møller King s College London, Thames Cancer Registry, London, UK Correspondence
Malignant Pleural Mesothelioma: Clinicopathologic and Survival Characteristic in a Consecutive Series of 40 Patients *
 Ann Thorac Cardiovasc Surg 2011; 17: 130 136 Original Article Complete translation of the original article Malignant Pleural Mesothelioma: Clinicopathologic and Survival Characteristic in a Consecutive
Ann Thorac Cardiovasc Surg 2011; 17: 130 136 Original Article Complete translation of the original article Malignant Pleural Mesothelioma: Clinicopathologic and Survival Characteristic in a Consecutive
B10/S/a Cancer: Malignant Mesothelioma (Adult)
 B10/S/a 2013/14 NHS STANDARD CONTRACT FOR CANCER: MALIGNANT MESOTHELIOMA (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date
B10/S/a 2013/14 NHS STANDARD CONTRACT FOR CANCER: MALIGNANT MESOTHELIOMA (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date
Research Article Frequency of Surgery in Black Patients with Malignant Pleural Mesothelioma
 Disease Markers Volume 2015, Article ID 282145, 5 pages http://dx.doi.org/10.1155/2015/282145 Research Article Frequency of Surgery in Black Patients with Malignant Pleural Mesothelioma Emanuela Taioli,
Disease Markers Volume 2015, Article ID 282145, 5 pages http://dx.doi.org/10.1155/2015/282145 Research Article Frequency of Surgery in Black Patients with Malignant Pleural Mesothelioma Emanuela Taioli,
Sternotomy and removal of the tumor
 Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma
 Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka
 Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project
 INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
Survey on the treatment of non-small cell lung cancer (NSCLC) in England and Wales
 Eur Respir J 1997; 10: 1552 1558 DOI: 10.1183/09031936.97.10071552 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Survey on the treatment
Eur Respir J 1997; 10: 1552 1558 DOI: 10.1183/09031936.97.10071552 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Survey on the treatment
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE MESOTHELIOMA Lung Site Group Mesothelioma Date Guideline Created: April 2013 Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE MESOTHELIOMA Lung Site Group Mesothelioma Date Guideline Created: April 2013 Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1.
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Research Article Malignant Pleural Mesothelioma Outcomes in the Era of Combined Platinum and Folate Antimetabolite Chemotherapy
 Lung Cancer International Volume 2015, Article ID 590148, 7 pages http://dx.doi.org/10.1155/2015/590148 Research Article Malignant Pleural Mesothelioma Outcomes in the Era of Combined Platinum and Folate
Lung Cancer International Volume 2015, Article ID 590148, 7 pages http://dx.doi.org/10.1155/2015/590148 Research Article Malignant Pleural Mesothelioma Outcomes in the Era of Combined Platinum and Folate
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
ASBESTOS MANAGEMENT REVIEW A CRITICAL REVIEW OF MEDICAL MANAGEMENT IN MALIGNANT PLEURAL MESOTHELIOMA - AUSTRALIA, 2011
 ASBESTOS MANAGEMENT REVIEW A CRITICAL REVIEW OF MEDICAL MANAGEMENT IN MALIGNANT PLEURAL MESOTHELIOMA - AUSTRALIA, 2011 Dr Malcolm Feigen Senior Radiation Oncologist Radiation Oncology Centre Austin Health
ASBESTOS MANAGEMENT REVIEW A CRITICAL REVIEW OF MEDICAL MANAGEMENT IN MALIGNANT PLEURAL MESOTHELIOMA - AUSTRALIA, 2011 Dr Malcolm Feigen Senior Radiation Oncologist Radiation Oncology Centre Austin Health
Treatment and recovery: Malignant pleural mesothelioma. Jocelyn Mclean Case Manager for Thoracic Surgery RPAH
 Treatment and recovery: Malignant pleural mesothelioma Jocelyn Mclean Case Manager for Thoracic Surgery RPAH This presenta?on Treatment - management op?ons Recovery well living programme Caring for pa?ents,
Treatment and recovery: Malignant pleural mesothelioma Jocelyn Mclean Case Manager for Thoracic Surgery RPAH This presenta?on Treatment - management op?ons Recovery well living programme Caring for pa?ents,
Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases
 Original Article Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases William G. Richards, PhD 1,2 ; John J. Godleski, MD 2,3 ; Beow Y.
Original Article Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases William G. Richards, PhD 1,2 ; John J. Godleski, MD 2,3 ; Beow Y.
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
Evaluation of asbestos-exposure, clinical diagnosis and treatment of MPM
 Evaluation of asbestos-exposure, clinical diagnosis and treatment of MPM Aija Knuuttila, MD, PhD Dept. of Pulmonary Medicine Helsinki University Central Hospital, Finland 15.11.2007 Malignant pleural mesothelioma
Evaluation of asbestos-exposure, clinical diagnosis and treatment of MPM Aija Knuuttila, MD, PhD Dept. of Pulmonary Medicine Helsinki University Central Hospital, Finland 15.11.2007 Malignant pleural mesothelioma
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Therapy of pleural effusions Modern techniques
 Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Principal Investigator: Valerie W. Rusch, MD, FACS, Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Adjuvant Therapy Non Small Cell Lung Cancer. Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015
 Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Recommendations for the Reporting of Pleural Mesothelioma
 Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
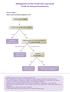 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Pre-workshop exercise
 Setting research priorities for mesothelioma workshop 10 th November 2014 Pre-workshop exercise Your individual ranking of unanswered questions about the diagnosis, treatment and care of mesothelioma Please
Setting research priorities for mesothelioma workshop 10 th November 2014 Pre-workshop exercise Your individual ranking of unanswered questions about the diagnosis, treatment and care of mesothelioma Please
Screening, early referral and treatment for asbestos related cancer
 Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline
 Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Scottish Medicines Consortium
 Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
Post-recurrence survival in completely resected stage I non-small cell lung cancer with local recurrence
 Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Management of Chest Tubes and Air Leaks after Lung Resection
 Management of Chest Tubes and Air Leaks after Lung Resection Emily Kluck PA-C The Johns Hopkins Hospital Baltimore, MD AATS 2014, Toronto, CAN April 2014 Management of Chest Tubes 1 Overview Review the
Management of Chest Tubes and Air Leaks after Lung Resection Emily Kluck PA-C The Johns Hopkins Hospital Baltimore, MD AATS 2014, Toronto, CAN April 2014 Management of Chest Tubes 1 Overview Review the
Clinical characteristics, treatment and survival outcomes in malignant pleural mesothelioma: An institutional experience in Turkey
 JBUON 2014; 19(1): 164-170 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Clinical characteristics, treatment and survival outcomes in malignant
JBUON 2014; 19(1): 164-170 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Clinical characteristics, treatment and survival outcomes in malignant
Photodynamic Therapy for Malignant Pleural Mesothelioma
 S-75 Photodynamic Therapy for Malignant Pleural Mesothelioma Presented by Joseph S. Friedberg, MD, University of Pennsylvania Health System, Philadelphia, Pennsylvania Abstract Surgery is the treatment
S-75 Photodynamic Therapy for Malignant Pleural Mesothelioma Presented by Joseph S. Friedberg, MD, University of Pennsylvania Health System, Philadelphia, Pennsylvania Abstract Surgery is the treatment
British Thoracic Society Standards of Care Committee
 250 Thorax 2001;56:250 265 BTS statement Statement on malignant mesothelioma in the United Kingdom British Thoracic Society Standards of Care Committee Correspondence to: Dr J Wiggins, Wexham Park Hospital,
250 Thorax 2001;56:250 265 BTS statement Statement on malignant mesothelioma in the United Kingdom British Thoracic Society Standards of Care Committee Correspondence to: Dr J Wiggins, Wexham Park Hospital,
COMMISSIONING. for ULTRA-RADICAL SURGERY ADVANCED OVARIAN CANCER
 COMMISSIONING for ULTRA-RADICAL SURGERY in ADVANCED OVARIAN CANCER WHY THIS MUST HAPPEN PERSPECTIVE COMMISSIONING FOR WHO, FOR WHAT? Biological Basis Surgical Basis International and national standards
COMMISSIONING for ULTRA-RADICAL SURGERY in ADVANCED OVARIAN CANCER WHY THIS MUST HAPPEN PERSPECTIVE COMMISSIONING FOR WHO, FOR WHAT? Biological Basis Surgical Basis International and national standards
Lung cancer case study
 Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Please see the LUCADA data manual v3.1.3, available in the downloads section
 National Lung Cancer Audit Frequently Asked Questions What dataset should be used? Please see the LUCADA data manual v3.1.3, available in the downloads section What does LUCADA stand for? LUCADA stands
National Lung Cancer Audit Frequently Asked Questions What dataset should be used? Please see the LUCADA data manual v3.1.3, available in the downloads section What does LUCADA stand for? LUCADA stands
Population-based survival for malignant mesothelioma after introduction of novel chemotherapy
 Eur Respir J 2012; 40: 185 189 DOI: 10.1183/09031936.00153611 CopyrightßERS 2012 Population-based survival for malignant mesothelioma after introduction of novel chemotherapy Ronald A.M. Damhuis*, Caroline
Eur Respir J 2012; 40: 185 189 DOI: 10.1183/09031936.00153611 CopyrightßERS 2012 Population-based survival for malignant mesothelioma after introduction of novel chemotherapy Ronald A.M. Damhuis*, Caroline
Surgery. Wedge resection only part of the lung, not. not a lobe, is removed. Cancer Council NSW
 The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3
 ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
Cancer research in the Midland Region the prostate and bowel cancer projects
 Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy and Photodynamic Therapy
 CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.1.36 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:36-40 A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy
CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.1.36 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:36-40 A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
treated and 64 untreated patients
 Thorax 1984;39:255-259 Malignant mesothelioma of the pleura: a study of 52 treated and 64 untreated patients MR LAW, ANNA GREGOR, MARGARET E HODSON, HJG BLOOM, M TURNER-WARWICK From the Cardiothoracic
Thorax 1984;39:255-259 Malignant mesothelioma of the pleura: a study of 52 treated and 64 untreated patients MR LAW, ANNA GREGOR, MARGARET E HODSON, HJG BLOOM, M TURNER-WARWICK From the Cardiothoracic
CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015. 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV
 CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV Meta-analisis LACE: adyuvancia vs no adyuvancia Pignon JP, et al.
CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV Meta-analisis LACE: adyuvancia vs no adyuvancia Pignon JP, et al.
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
GIVING INFORMATION TO LUNG CANCER PATIENTS
 GIVING INFORMATION TO LUNG CANCER PATIENTS Guidance For Healthcare Professionals Discussing Options For Patients On The Lung Cancer Pathway British Thoracic Society Lung Cancer and Mesothelioma Specialist
GIVING INFORMATION TO LUNG CANCER PATIENTS Guidance For Healthcare Professionals Discussing Options For Patients On The Lung Cancer Pathway British Thoracic Society Lung Cancer and Mesothelioma Specialist
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality. Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006
 The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
Surgical Management of Malignant Pleural Mesothelioma
 Evidence-based Series 7-14-2 Version 2 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Surgical Management of Malignant Pleural Mesothelioma Members of the
Evidence-based Series 7-14-2 Version 2 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Surgical Management of Malignant Pleural Mesothelioma Members of the
Good symptom relief with palliative MVP (mitomycin-c, vinblastine and cisplatin) chemotherapy in malignant mesothelioma
 Annals of Oncology 9: 9-7, 998. 998 Khmer Academic Publishers. Printed in the Netherlands Original article Good symptom relief with palliative MVP (mitomycin-c, vinblastine and cisplatin) chemotherapy
Annals of Oncology 9: 9-7, 998. 998 Khmer Academic Publishers. Printed in the Netherlands Original article Good symptom relief with palliative MVP (mitomycin-c, vinblastine and cisplatin) chemotherapy
Case Report Pleural Mesothelioma Presenting as Periumbilical Metastasis: The First Clinical Documentation
 Volume 2013, Article ID 198729, 4 pages http://dx.doi.org/10.1155/2013/198729 Case Report Pleural Mesothelioma Presenting as Periumbilical Metastasis: The First Clinical Documentation R. F. Falkenstern-Ge,
Volume 2013, Article ID 198729, 4 pages http://dx.doi.org/10.1155/2013/198729 Case Report Pleural Mesothelioma Presenting as Periumbilical Metastasis: The First Clinical Documentation R. F. Falkenstern-Ge,
available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/lungcan
 Lung Cancer (2007) 57, 89 95 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/lungcan Induction chemotherapy, extrapleural pneumonectomy (EPP) and adjuvant hemi-thoracic radiation
Lung Cancer (2007) 57, 89 95 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/lungcan Induction chemotherapy, extrapleural pneumonectomy (EPP) and adjuvant hemi-thoracic radiation
1 page Overview. CONCURRENT 1D, 1E, 1F Biology & Pathogenesis Multi-Modality Immunology 1
 1 page Overview 21 Oct Tuesday 1500 on REGISTRATION 1800 Welcome Reception & Cocktails at the Cape Town International Conference Centre (CTICC) 22 Oct Wednesday 0730 REGISTRATION 0830 OPENING 0900 PLENARY
1 page Overview 21 Oct Tuesday 1500 on REGISTRATION 1800 Welcome Reception & Cocktails at the Cape Town International Conference Centre (CTICC) 22 Oct Wednesday 0730 REGISTRATION 0830 OPENING 0900 PLENARY
