Demand for Health Insurance
|
|
|
- Shawn Horn
- 10 years ago
- Views:
Transcription
1 Demand for Health Insurance Demand for Health Insurance is principally derived from the uncertainty or randomness with which illnesses befall individuals. Consequently, the derived demand for health insurance is to protect the individual from the financial risk created due to the illness and the consequent cost of care needed to return to health if possible. With a health insurance market, individual s best bet would be to self-insure through saving, or through a network of family and friends that would assist in times of need. Further, the latter includes a network that is capable of monitoring deviant behavior which the group may choose not to insure against. Further, the highly informal nature ensures that nothing is verifiable to the courts. 1. Why do we dislike Risky Events? In general, economic agents are typically risk averse, in the sense that if given a chance, they would rather do without a risky venture. This explains why agents often pay insurance companies more than their average loss they may confront to secure certainty. We know that the marginal utility from consumption of private goods, and medical goods, which gives rise to health, is positive. This in turn means that the marginal utility from income is also increasing, but increasing at a decreasing rate due to the fact of diminishing marginal utility. This means that if we were to plot the relationship with respect to income, we would get a increasing but concave curve. Another way of thinking about this is that given two income levels, the lower with certainty, and the higher without, the individual would pick the lower income with certainty. 2. Risk Aversion Utility E(C) A C C C B C is the average outcome derived from having B occur with some probability (1-a), and A with probability a. Risk Premium Income The above diagram describes why the idea of diminishing marginal utility is synonymous with risk aversion. Consider a gamble where on the low side, you d
2 get an income level of A, and a high winning the same as from B. The expected winning is what is typically termed a convex combination or weighted average of A and B, which I have arbitrarily denoted at point C. Note that although this level of expected income yields a higher income with uncertainty, it has the same level of utility as a situation where a lower level of income occurs with uncertainty. Comparing to another situation where the individual could get the same level of income with certainty at the same average income level, the individual would obviously prefer the certainty situation. The horizontal distance between C and C is the risk premium, or the premium that an individual is willing to pay to avoid risky outcomes. (Note that we obtain this outcome without developing any new microeconomic theory.) The greater the risk aversion is, the greater the risk premium. Choice of Insurance Policy Let C be the coinsurance rate of an insurance policy, than (1 - C)% of a patient s medical bills is paid for by the insurance company. Although an insurance policy is far more complicated, this simplification would still allow us to glean some important insights. As noted, the insurance contract obliges the insurer to pay ( ) p m 1 C m, for the m units of medical care that the patient obtains. However, as we have realized, with insurance coverage, the effective price of health care reduces, and consequently you have the problem of moral hazard. That is as C increases, m increases as well. However, this behavior is not necessarily a deviant behavior, but a rational response to a reduction in price. In order to understand the mechanics of deciding on the optimal level of coinsurance, we must understand what happens with its changes. Some of the key issues are the following; 1. The effects of insurance coverage on demand for health care feedbacks onto demand for insurance since as demand for health care increases, the marginal value falls. 2. The increased consumption leads to the patients consuming more health care (that gives a lower marginal value, than it costs to provide it. This means then that there is a fall in welfare for society as a whole. The problem is that health insurance breaks the link for the patients between the price of health care, and the costs of provision. 3. At the same time, necessarily, the provision of health insurance raises the welfare of the patients eliminating the financial risks. Then in deciding the optimal level of coinsurance, we have to balance the welfare gain versus the welfare loss in 2.
3 p Welfare loss from insurance. Price without insurance. Excess consumption due to insurance Demand Price with insurance. m * Read the specific example on page of your text for a more detailed expression of these welfare ideas. Further, the expected moral hazard loss is in turn dependent on the elasticity of demand. Intuitively, if the elasticity of demand were small, then the change in pricing resulting from insurance purchased would mean that the welfare loss (due to moral hazard) would be small, as compared to the situation when the elasticity of demand is large. This then mean that the more price elastic is demand for medical services, the less desirable it is to insure against the risk due to the welfare loss involved. This leads to two testable predictions 1. The greater the variance or financial risk involved the greater the demand for insurance. 2. The greater the elasticity of demand, the lower the demand for insurance. It turns out that all of them hold empirical true, for example, most individuals tended to purchase insurance against hospitalization which is the type of care that creates the greatest financial risk. On the other hand, dental care has the lowest incidence of health insurance on account of the high degree of price elasticity. It should be noted that the price of insurance as we had noted before is not the premium paid by the consumers, but it s the markup above the expected benefit. To use the notation we had above, the insurance premium is R = ( 1+ L)( 1 C) p m m where L is the loading fee which insurance firms charges above the expected benefits so as to cover the cost of risk bearing, and administration fees. Then the larger the loading fees, the larger the coinsurance rates, C, that the consumer would select. If the insurers were to include deductibles into the insurance contracts, then the larger the loading fees,
4 the larger would the consumer pick for the deductible so as to reduce the cost of insurance. This then reveals that the relationship between the demand for insurance in the form of coinsurance, and deductibles is just as a typical demand, i.e. is negative with respect to the loading fee/price of insurance. The Supply of Insurance The insurance firm performs essentially two tasks: 1. The processing of claims on insurance contracts. In that sense, the output of a insurance firm are these payments, and the equipment it needs to perform these duties such as Actuaries, Insurance Agents, Clerical Staff, etc (And including equipment such as computers, and office space). The administrative costs that are to be covered by the loading fees are meant to cover these costs at the least. Just as there are several types of Hospitals, there are several types of insurance firms, a. For Profit (Prudential, Manulife etc) and Not-for-Profit (Blue Cross and Blue Shield). The key difference between the two are that; a. Not-for-Profit (Blue Plan) firms are exempt from taxation. b. Exemption from many State regulations such as minimum cash reserves regulations. The principal reason why the Not-for-Profit Insurance firms has not flourished principally is because, c. Organized on a State or Sub-State level that prevents them from enjoying or reaping economies of scale (especially where risks within a state are rather correlated). d. They also tended to insure only against low risk events. The above two features then prevent the Blue Plan firms from capturing the market. 2. Bearing and spreading of risk. This is reliant on the idea that if risks borne individually are uncorrelated (risk of earthquakes along the inhabitants of the San Andreas Fault is a correlated risk. One gets it, all gets it.) It should be noted that although with insurance, average risks falls with pooling done by Insurance firms, as a society, the transfer of individual risk to an insurance firm does not reduce the risk in/to our society. Is the Insurance Market Stable? : The Question of Self-Selection The basic problem remains in insurance; that causes us to wonder about the stability of the market. That is the inherent problem that the consumer know more about their own risk of illness than do the insurance firms; i.e. the problem of asymmetric information. We have already argued that this may lead to from of adverse selection where individuals with poor risk end up signing up for the policies. A Simple Model A way to force individuals to identify their true tendency towards usage is to offer set plans. Then their selection of the plans would indicate their type to the insurance firm. If such plans could be found, insurance firms would be able to avoid the problem of
5 adverse selection. However, on the down side, the insurance firm in doing so denies the healthy individuals from buying an insurance plan they would prefer. We can think of the budget constraint for an individual choosing between the optimal level of private consumption good and health insurance as a negatively sloped concave shaped curve since it is more costly in terms of consumption good lost as an individual increase his purchase of health insurance. X 1-C Then equilibrium occurs at the point where the individual s utility is tangent to her budget constraint. In a perfect world where the insurance company is aware of everyone s proclivities, they would know that the budget constraint of a healthy individual has a larger budget set than that of an individual with ill health since in such a perfect world, the insurer knows that the probability of ill health is lower for the healthy individual, and consequently the price charged is lower.
6 X Utility of Unhealthy Individual Utility of Healthy Individual 1-C This then implies that in equilibrium, the consumption of the healthy individual would also be higher in all respects. However, reality does not commiserate with that analogy, but rather is parallel to one of asymmetric information. If both the above insurance schemes were offered to everyone under that scenario, if would only be rational that the ill health individual try to pass off as someone healthy, and consume more of insurance and consumption goods. This then leads to a higher expected payout for the insurance firm. To force the high risk individuals to reveal themselves then the insurance firm deny the portion of the insurance that would make the healthy individuals better off to everyone, thereby forcing the high risk individuals to reveal themselves. X Utility of Unhealthy Individual Utility of Healthy Individual Budget constraint of someone unhealthy Budget Constraint of someone healthy 1-C
7 This is reflected in the above diagram as the bold line. In that scenario, the high risk individual is ambivalent between the policy offered to herself, and that offer to someone healthier. This however reduces the set of insurance that a healthy individual could purchase, and make her worse off. This is known as a Separating Equilibrium. Other Possible Pareto Improvement Schemes An alternative solution to the problem of asymmetric information is to force insurance companies to offer the same rates to everyone in the community, called community rating. Such a scheme causes everyone s budget constraint to be the same, and creates a budget constraint that is between the two above. The exact location of which is dependent on whether it is individuals with ill health, or healthy individuals that dominate. The greater the proportion of healthy individuals, the greater the proximity of the community rated budget constraint is to the healthy individual s. This is a pareto improving scheme since everyone is made better off compared to the separating equilibrium, but it also means that the healthy are paying for the purchase of insurance for the unhealthy. Yet another possibility is through insurance firms selling insurance policies directly to employers since the reason for an individual joining a particular firm are for purposes (such as high pay, matching of skills desired, etc.) other than to purchase insurance, thereby averting the consideration of self-selection/adverse selection. Virtually, all employers have a community rating scheme within a firm. However, if within a society, the problem rests in coverage of long term care, such insurance plans would fail to solve the problem for individuals dominant in that sub-market, the elderly. In summary, group insurance 1. provides for economies of scale (since it eliminates the sale of insurance individually, negates the collection of individual health histories, etc.), and 2. avoids adverse selection. Empirical Estimates of Demand for Insurance The estimation of demand for insurance has two approaches: 1. By examining choices made by individuals and groups, since the differences in income allow estimation of how demand varies across income groups. 2. By examining aggregated data over time, and estimating how total insurance premiums respond to changes in income, loading fees, etc. The summary of these finding are as follows: 1. Income elasticities has been found to be positive, and generally small (less than 1) when using individual level data. Using aggregate data, the findings however yield measures between 1 and 2 (closer to 2). 2. Price elasticities found using both types of data has yielded values between -1 to - 2. However, studies using differences in the marginal tax across households to determine the effect of price on insurance has yielded much smaller estimates of
8 General Considerations for a National Health Policy 1. Should such a system have universal coverage, and if so, how should it be achieved? 2. How would such a coverage policy be financed? 3. What should be the scope and cost sharing scheme in such a policy? 4. How would expenditure be controlled? 5. How would new technologies be introduced? 6. How would quality of care be maintained? Issues regarding Universal Coverage Why should we have universal coverage? 1. Medical Care is a merit good, whose consumption by fellow citizens yield increases in ones utility. If true, this would make the societal demand far larger than individual private demand for medical good and service. 2. Individuals without insurance free ride of individuals who do have through their inability to acquire it. It is claimed that eliminating private insurance and instituting universal insurance eliminates this problem. Do you think universal insurance really eliminates free riding? Consider universal unemployment insurance; does it eliminate free riding? 3. Market failures due to asymmetry in information. Universal insurance such as community rating eliminates this problem by providing a solution that is pareto welfare enhancing. How can we really think about or measure the loss of wealth for individuals of good health really? How can Universal Insurance be achieved? 1. Government provision of Health Insurance (Canada), or Health Care provision (United Kingdom). 2. Legislate mandatory purchase of health insurance, and subsidizing needy individuals and households in this endeavor (Germany and Japan) 3. Legislate mandatory purchase of group health insurance by employers (as proposed in the United States). How to Finance Universal Health Insurance? 1. Taxation 2. Subsidies However these financing schemes necessarily have a redistributive effect dependent on who bears the greatest burden in the tax increase (read of your text). Further, insofar as the taxes are on either individuals and/or firms, this means that there will be distortions created in individual choices. Consider an increase in taxes to finance universal insurance. We know that labor supply would fall if the income effect dominates the substitution effect, thereby reducing an economies production, and hampering the society s ability to sustain the provision.
9 Features of the Canadian Health Care System and its Consequences Some Stylized Facts 1. Prior to 1971, Canada spent 7.4% if its GNP on healthcare compared with 7.6 in the United States. 2. Prior to 1971, the most common found of insurance in Canada are group insurance provided for by employers, with some government coverage. Doctors and Hospitals operated as private entities then, and where Doctor s fees are determined by the market, while that of the hospital was through controls and bargaining with the government. 3. In 1971 Canada instituted a universal Medicare System, which then caused a deviation between the two countries. Due to a strong and comprehensive control on spending growth, and its share of GNP dedicated to healthcare, Canada today only dedicates 10% of its GNP on healthcare, compared to 15% in the United States. 4. Financed by Value-Added-Tax (VAT) (neutral in redistributive effect) and Income taxes (progressive in redistributive effect). 5. Scope of benefits includes almost all standard services and charges for care are small. 6. Hospitals are paid negotiated budgets, and doctors are paid on the basis of fees negotiated between the government and medical societies. 7. Capacity controls exists that constrains the provision of care, limits cost increases through time, and also provides for filters on the introduction of new technologies. How does it work? 1. Insurance is Universal in Canada today, and the plan is organized around its provinces (i.e. provided for by the Provincial governments), where each province has its own Medicare system. Although there are idiosyncrasies across provinces, common ground is imposed by the federal government on the provinces. With this private insurance has disappeared. 2. Hospitals came under the authority of the provincial government, with a budget cap established by the government for all hospitals. Within that cap, every provincial hospital receives a direct budget. 3. Physicians receive a fee according to a negotiated schedule within the province, but continue to function as independent firms. What is it like today? 1. Health care cost growth in Canada is this an entirely political decision, with no role for the markets to set prices. Since 1971 when US saw an increase of proportion of GNP received by physicians by 40%, Canada saw only 10%. 2. Hospital spending has also increased at a lower rate than in the US. 3. Admission rates in Canada and US has been the same, which means that the cost cuts does not seem to have dampened quantity. 4. US length of stay in hospital is lower than that of Canada s. 5. Doctor office visits have remained the same in both countries.
10 6. Because funding comes from the Government, the rate at which the Canadian system has adopted technology has been notably slower than in the US. This hence explains a part of the cost differential between the two countries. 7. A substantial proportion of consumers in Canada also seek health treatments across the border to bypass the waiting period associated with the Canadian system. This is evident from the thriving health markets catering to Canadian demand in cities that are close to the Canada-US border.
Social Insurance (Chapter-12) Part-1
 (Chapter-12) Part-1 Background Dramatic change in the composition of government spending in the U.S. over time Background Social insurance programs: Government interventions in the provision of insurance
(Chapter-12) Part-1 Background Dramatic change in the composition of government spending in the U.S. over time Background Social insurance programs: Government interventions in the provision of insurance
Demand and supply of health insurance. Folland et al Chapter 8
 Demand and supply of health Folland et al Chapter 8 Chris Auld Economics 317 February 9, 2011 What is insurance? From an individual s perspective, insurance transfers wealth from good states of the world
Demand and supply of health Folland et al Chapter 8 Chris Auld Economics 317 February 9, 2011 What is insurance? From an individual s perspective, insurance transfers wealth from good states of the world
Second Hour Exam Public Finance - 180.365 Fall, 2007. Answers
 Second Hour Exam Public Finance - 180.365 Fall, 2007 Answers HourExam2-Fall07, November 20, 2007 1 Multiple Choice (4 pts each) Correct answer indicated by 1. The portion of income received by the middle
Second Hour Exam Public Finance - 180.365 Fall, 2007 Answers HourExam2-Fall07, November 20, 2007 1 Multiple Choice (4 pts each) Correct answer indicated by 1. The portion of income received by the middle
Health Economics. University of Linz & Demand and supply of health insurance. Gerald J. Pruckner. Lecture Notes, Summer Term 2010
 Health Economics Demand and supply of health insurance University of Linz & Gerald J. Pruckner Lecture Notes, Summer Term 2010 Gerald J. Pruckner Health insurance 1 / 25 Introduction Insurance plays a
Health Economics Demand and supply of health insurance University of Linz & Gerald J. Pruckner Lecture Notes, Summer Term 2010 Gerald J. Pruckner Health insurance 1 / 25 Introduction Insurance plays a
Applied Economics For Managers Recitation 5 Tuesday July 6th 2004
 Applied Economics For Managers Recitation 5 Tuesday July 6th 2004 Outline 1 Uncertainty and asset prices 2 Informational efficiency - rational expectations, random walks 3 Asymmetric information - lemons,
Applied Economics For Managers Recitation 5 Tuesday July 6th 2004 Outline 1 Uncertainty and asset prices 2 Informational efficiency - rational expectations, random walks 3 Asymmetric information - lemons,
Why is Insurance Good? An Example Jon Bakija, Williams College (Revised October 2013)
 Why is Insurance Good? An Example Jon Bakija, Williams College (Revised October 2013) Introduction The United States government is, to a rough approximation, an insurance company with an army. 1 That is
Why is Insurance Good? An Example Jon Bakija, Williams College (Revised October 2013) Introduction The United States government is, to a rough approximation, an insurance company with an army. 1 That is
Advanced Health Economics Econ555/HPA543. Week 4: Health Insurance
 Advanced Health Economics Econ555/HPA543 Week 4: Health Insurance Types of Insurance Coverage Fee-for-Service: Coinsurance Deductibles Catastrophic Maximum Indemnity Capitation Mixed Coinsurance - Patient
Advanced Health Economics Econ555/HPA543 Week 4: Health Insurance Types of Insurance Coverage Fee-for-Service: Coinsurance Deductibles Catastrophic Maximum Indemnity Capitation Mixed Coinsurance - Patient
Moral Hazard and Adverse Selection. Topic 6
 Moral Hazard and Adverse Selection Topic 6 Outline 1. Government as a Provider of Insurance. 2. Adverse Selection and the Supply of Insurance. 3. Moral Hazard. 4. Moral Hazard and Incentives in Organizations.
Moral Hazard and Adverse Selection Topic 6 Outline 1. Government as a Provider of Insurance. 2. Adverse Selection and the Supply of Insurance. 3. Moral Hazard. 4. Moral Hazard and Incentives in Organizations.
Unraveling versus Unraveling: A Memo on Competitive Equilibriums and Trade in Insurance Markets
 Unraveling versus Unraveling: A Memo on Competitive Equilibriums and Trade in Insurance Markets Nathaniel Hendren January, 2014 Abstract Both Akerlof (1970) and Rothschild and Stiglitz (1976) show that
Unraveling versus Unraveling: A Memo on Competitive Equilibriums and Trade in Insurance Markets Nathaniel Hendren January, 2014 Abstract Both Akerlof (1970) and Rothschild and Stiglitz (1976) show that
Moral Hazard. Itay Goldstein. Wharton School, University of Pennsylvania
 Moral Hazard Itay Goldstein Wharton School, University of Pennsylvania 1 Principal-Agent Problem Basic problem in corporate finance: separation of ownership and control: o The owners of the firm are typically
Moral Hazard Itay Goldstein Wharton School, University of Pennsylvania 1 Principal-Agent Problem Basic problem in corporate finance: separation of ownership and control: o The owners of the firm are typically
Notes - Gruber, Public Finance Section 12.1 Social Insurance What is insurance? Individuals pay money to an insurer (private firm or gov).
 Notes - Gruber, Public Finance Section 12.1 Social Insurance What is insurance? Individuals pay money to an insurer (private firm or gov). These payments are called premiums. Insurer promises to make a
Notes - Gruber, Public Finance Section 12.1 Social Insurance What is insurance? Individuals pay money to an insurer (private firm or gov). These payments are called premiums. Insurer promises to make a
What we ll be discussing
 Teaching programme: Course: Main text: Master of Public Health, University of Tromsø, Norway Health economics and policy (HEL3007) JA Olsen (2009): Principles in Health Economics and Policy, Oxford University
Teaching programme: Course: Main text: Master of Public Health, University of Tromsø, Norway Health economics and policy (HEL3007) JA Olsen (2009): Principles in Health Economics and Policy, Oxford University
1 Uncertainty and Preferences
 In this chapter, we present the theory of consumer preferences on risky outcomes. The theory is then applied to study the demand for insurance. Consider the following story. John wants to mail a package
In this chapter, we present the theory of consumer preferences on risky outcomes. The theory is then applied to study the demand for insurance. Consider the following story. John wants to mail a package
Health Economics. University of Linz & Information, health insurance and compulsory coverage. Gerald J. Pruckner. Lecture Notes, Summer Term 2010
 Health Economics Information, health insurance and compulsory coverage University of Linz & Gerald J. Pruckner Lecture Notes, Summer Term 2010 Gerald J. Pruckner Information 1 / 19 Asymmetric information
Health Economics Information, health insurance and compulsory coverage University of Linz & Gerald J. Pruckner Lecture Notes, Summer Term 2010 Gerald J. Pruckner Information 1 / 19 Asymmetric information
What we ll be discussing
 Teaching programmes: Master of Public Health, University of Tromsø, Norway HEL-3007 Health Economics and Policy Master of Public Health, Monash University, Australia ECC-5979 Health Economics Master of
Teaching programmes: Master of Public Health, University of Tromsø, Norway HEL-3007 Health Economics and Policy Master of Public Health, Monash University, Australia ECC-5979 Health Economics Master of
Lecture notes for Choice Under Uncertainty
 Lecture notes for Choice Under Uncertainty 1. Introduction In this lecture we examine the theory of decision-making under uncertainty and its application to the demand for insurance. The undergraduate
Lecture notes for Choice Under Uncertainty 1. Introduction In this lecture we examine the theory of decision-making under uncertainty and its application to the demand for insurance. The undergraduate
How to Study for Chapter 12 The Economics of Health Care
 1 How to Study for Chapter 12 The Economics of Health Care Chapter 12 introduces some new concepts to allow analysis of the health care industry and the problems for the United States that exist in health
1 How to Study for Chapter 12 The Economics of Health Care Chapter 12 introduces some new concepts to allow analysis of the health care industry and the problems for the United States that exist in health
Mandatory Private Health Insurance as Supplementary Financing
 Chapter 12 SUPPLEMENTARY FINANCING OPTION (5) MANDATORY PRIVATE HEALTH INSURANCE Mandatory Private Health Insurance as Supplementary Financing 12.1 Mandatory private health insurance is where private health
Chapter 12 SUPPLEMENTARY FINANCING OPTION (5) MANDATORY PRIVATE HEALTH INSURANCE Mandatory Private Health Insurance as Supplementary Financing 12.1 Mandatory private health insurance is where private health
Midterm exam, Health economics, Spring 2007 Answer key
 Midterm exam, Health economics, Spring 2007 Answer key Instructions: All points on true/false and multiple choice questions will be given for the explanation. Note that you can choose which questions to
Midterm exam, Health economics, Spring 2007 Answer key Instructions: All points on true/false and multiple choice questions will be given for the explanation. Note that you can choose which questions to
Chapter 11 SUPPLEMENTARY FINANCING OPTION (4) VOLUNTARY PRIVATE HEALTH INSURANCE. Voluntary Private Health Insurance as Supplementary Financing
 Chapter 11 SUPPLEMENTARY FINANCING OPTION (4) VOLUNTARY PRIVATE HEALTH INSURANCE Voluntary Private Health Insurance as Supplementary Financing 11.1 Voluntary private health insurance includes both employer
Chapter 11 SUPPLEMENTARY FINANCING OPTION (4) VOLUNTARY PRIVATE HEALTH INSURANCE Voluntary Private Health Insurance as Supplementary Financing 11.1 Voluntary private health insurance includes both employer
Econ 149: Health Economics Problem Set IV (Extra credit) Answer Key
 Econ 149: Health Economics Problem Set IV (Extra credit) Answer Key 1. Your utility function is given by U = ln(4c), where C is consumption. You make $30,000 per year and enjoy jumping out of perfectly
Econ 149: Health Economics Problem Set IV (Extra credit) Answer Key 1. Your utility function is given by U = ln(4c), where C is consumption. You make $30,000 per year and enjoy jumping out of perfectly
Equilibrium in Competitive Insurance Markets: An Essay on the Economic of Imperfect Information
 Equilibrium in Competitive Insurance Markets: An Essay on the Economic of Imperfect Information By: Michael Rothschild and Joseph Stiglitz Presented by Benjamin S. Barber IV, Xiaoshu Bei, Zhi Chen, Shaiobi
Equilibrium in Competitive Insurance Markets: An Essay on the Economic of Imperfect Information By: Michael Rothschild and Joseph Stiglitz Presented by Benjamin S. Barber IV, Xiaoshu Bei, Zhi Chen, Shaiobi
Notes on indifference curve analysis of the choice between leisure and labor, and the deadweight loss of taxation. Jon Bakija
 Notes on indifference curve analysis of the choice between leisure and labor, and the deadweight loss of taxation Jon Bakija This example shows how to use a budget constraint and indifference curve diagram
Notes on indifference curve analysis of the choice between leisure and labor, and the deadweight loss of taxation Jon Bakija This example shows how to use a budget constraint and indifference curve diagram
Investing on hope? Small Cap and Growth Investing!
 Investing on hope? Small Cap and Growth Investing! Aswath Damodaran Aswath Damodaran! 1! Who is a growth investor?! The Conventional definition: An investor who buys high price earnings ratio stocks or
Investing on hope? Small Cap and Growth Investing! Aswath Damodaran Aswath Damodaran! 1! Who is a growth investor?! The Conventional definition: An investor who buys high price earnings ratio stocks or
HANDOUTS Property Taxation Review Committee
 HANDOUTS Property Taxation Review Committee Legislative Services Agency September 1, 2004 Criteria For Good Proposals for Property Tax Reform Dr. Thomas Pogue, University of Iowa DISCLAIMER The Iowa General
HANDOUTS Property Taxation Review Committee Legislative Services Agency September 1, 2004 Criteria For Good Proposals for Property Tax Reform Dr. Thomas Pogue, University of Iowa DISCLAIMER The Iowa General
Inflation. Chapter 8. 8.1 Money Supply and Demand
 Chapter 8 Inflation This chapter examines the causes and consequences of inflation. Sections 8.1 and 8.2 relate inflation to money supply and demand. Although the presentation differs somewhat from that
Chapter 8 Inflation This chapter examines the causes and consequences of inflation. Sections 8.1 and 8.2 relate inflation to money supply and demand. Although the presentation differs somewhat from that
MARKET FAILURE AND GOVERNMENT INTERVENTION
 MARKET FAILURE AND GOVERNMENT INTERVENTION ECONOMY AND MARKET Objective of an economy is to generate wealth and welfare for the society, using the available resources. These resources are scarce and there
MARKET FAILURE AND GOVERNMENT INTERVENTION ECONOMY AND MARKET Objective of an economy is to generate wealth and welfare for the society, using the available resources. These resources are scarce and there
Notes - Gruber, Public Finance Chapter 20.3 A calculation that finds the optimal income tax in a simple model: Gruber and Saez (2002).
 Notes - Gruber, Public Finance Chapter 20.3 A calculation that finds the optimal income tax in a simple model: Gruber and Saez (2002). Description of the model. This is a special case of a Mirrlees model.
Notes - Gruber, Public Finance Chapter 20.3 A calculation that finds the optimal income tax in a simple model: Gruber and Saez (2002). Description of the model. This is a special case of a Mirrlees model.
Insurance and Public Pensions : (b) Adverse Selection
 Insurance and Public Pensions : (b) Adverse Selection Adverse selection is said to occur if potential buyers of insurance know their own probabilities of loss better than do insurance companies. So suppose
Insurance and Public Pensions : (b) Adverse Selection Adverse selection is said to occur if potential buyers of insurance know their own probabilities of loss better than do insurance companies. So suppose
2. Information Economics
 2. Information Economics In General Equilibrium Theory all agents had full information regarding any variable of interest (prices, commodities, state of nature, cost function, preferences, etc.) In many
2. Information Economics In General Equilibrium Theory all agents had full information regarding any variable of interest (prices, commodities, state of nature, cost function, preferences, etc.) In many
Uncertainty, Asymmetric Information, and Market Failure
 2-1 INTERNET CHAPTER TWO Uncertainty, Asymmetric Information, and Market Failure The failure of the market to insure against uncertainties has created many social institutions in which the usual assumptions
2-1 INTERNET CHAPTER TWO Uncertainty, Asymmetric Information, and Market Failure The failure of the market to insure against uncertainties has created many social institutions in which the usual assumptions
QE1: Economics Notes 1
 QE1: Economics Notes 1 Box 1: The Household and Consumer Welfare The final basket of goods that is chosen are determined by three factors: a. Income b. Price c. Preferences Substitution Effect: change
QE1: Economics Notes 1 Box 1: The Household and Consumer Welfare The final basket of goods that is chosen are determined by three factors: a. Income b. Price c. Preferences Substitution Effect: change
Lecture Note 16 Adverse Selection, Risk Aversion and Insurance Markets.
 Lecture Note 16 Adverse Selection, Risk Aversion and Insurance Markets. 14.03/14003 Applied Microeconomic Theory and Public Policy, Fall 2010 David Autor, Massachusetts Institute of Technology November
Lecture Note 16 Adverse Selection, Risk Aversion and Insurance Markets. 14.03/14003 Applied Microeconomic Theory and Public Policy, Fall 2010 David Autor, Massachusetts Institute of Technology November
Insurance. Michael Peters. December 27, 2013
 Insurance Michael Peters December 27, 2013 1 Introduction In this chapter, we study a very simple model of insurance using the ideas and concepts developed in the chapter on risk aversion. You may recall
Insurance Michael Peters December 27, 2013 1 Introduction In this chapter, we study a very simple model of insurance using the ideas and concepts developed in the chapter on risk aversion. You may recall
The Reasonable Person Negligence Standard and Liability Insurance. Vickie Bajtelsmit * Colorado State University
 \ins\liab\dlirpr.v3a 06-06-07 The Reasonable Person Negligence Standard and Liability Insurance Vickie Bajtelsmit * Colorado State University Paul Thistle University of Nevada Las Vegas Thistle s research
\ins\liab\dlirpr.v3a 06-06-07 The Reasonable Person Negligence Standard and Liability Insurance Vickie Bajtelsmit * Colorado State University Paul Thistle University of Nevada Las Vegas Thistle s research
Problem Set 1 Solutions
 Health Economics Economics 156 Prof. Jay Bhattacharya Problem Set 1 Solutions A. Risk Aversion Consider a risk averse consumer with probability p of becoming sick. Let I s be the consumer s income if he
Health Economics Economics 156 Prof. Jay Bhattacharya Problem Set 1 Solutions A. Risk Aversion Consider a risk averse consumer with probability p of becoming sick. Let I s be the consumer s income if he
Chapter 23: Asymmetric Information
 Chapter 23: Asymmetric Information Asymmetric Information Adverse Selection Moral Hazard Lemons Market Second-Best Mechanism Designs Principal Agent Market Failure Signaling Screening Insurance Employer/
Chapter 23: Asymmetric Information Asymmetric Information Adverse Selection Moral Hazard Lemons Market Second-Best Mechanism Designs Principal Agent Market Failure Signaling Screening Insurance Employer/
4/17/2015. Health Insurance. The Framework. The importance of health care. the role of government, and reasons for the costs increase
 Health Insurance PhD. Anto Bajo Faculty of Economics and Business, University of Zagreb The Framework The importance of healthcare, the role of government, and reasons for the costs increase Financing
Health Insurance PhD. Anto Bajo Faculty of Economics and Business, University of Zagreb The Framework The importance of healthcare, the role of government, and reasons for the costs increase Financing
Rafal Borkowski, Hipoteczna 18/22 m. 8, 91-337 Lodz, POLAND, E-mail: [email protected]
 Rafal Borkowski, Hipoteczna 18/22 m. 8, 91-337 Lodz, POLAND, E-mail: [email protected] Krzysztof M. Ostaszewski, Actuarial Program Director, Illinois State University, Normal, IL 61790-4520, U.S.A., e-mail:
Rafal Borkowski, Hipoteczna 18/22 m. 8, 91-337 Lodz, POLAND, E-mail: [email protected] Krzysztof M. Ostaszewski, Actuarial Program Director, Illinois State University, Normal, IL 61790-4520, U.S.A., e-mail:
The Supply of Medical Care, The Market for Health Insurance and Market Competition. Lecture 25. Economics 157 Health Economics Summer 2003
 The Supply of Medical Care, The Market for Health Insurance and Market Competition Lecture 25 Economics 157 Health Economics Summer 2003 Lectures 25; Graphic 25 No. 1 Announcements (1) Tuesday 080503:
The Supply of Medical Care, The Market for Health Insurance and Market Competition Lecture 25 Economics 157 Health Economics Summer 2003 Lectures 25; Graphic 25 No. 1 Announcements (1) Tuesday 080503:
. In this case the leakage effect of tax increases is mitigated because some of the reduction in disposable income would have otherwise been saved.
 Chapter 4 Review Questions. Explain how an increase in government spending and an equal increase in lump sum taxes can generate an increase in equilibrium output. Under what conditions will a balanced
Chapter 4 Review Questions. Explain how an increase in government spending and an equal increase in lump sum taxes can generate an increase in equilibrium output. Under what conditions will a balanced
Chapter 5 Departments of Health and Justice and Consumer Affairs Health Levy
 Departments of Health and Justice and Consumer Affairs Contents Background................................................. 159 Scope..................................................... 160 Overall conclusion.............................................
Departments of Health and Justice and Consumer Affairs Contents Background................................................. 159 Scope..................................................... 160 Overall conclusion.............................................
Universal Health Coverage: An Economist s Perspective
 INFORMATION BRIEF Research Department Minnesota House of Representatives 600 State Office Building St. Paul, MN 55155 Donald Hirasuna, Legislative Analyst 651-296-8038 September 2007 Universal Health Coverage:
INFORMATION BRIEF Research Department Minnesota House of Representatives 600 State Office Building St. Paul, MN 55155 Donald Hirasuna, Legislative Analyst 651-296-8038 September 2007 Universal Health Coverage:
Chapter 4 Specific Factors and Income Distribution
 Chapter 4 Specific Factors and Income Distribution Chapter Organization Introduction The Specific Factors Model International Trade in the Specific Factors Model Income Distribution and the Gains from
Chapter 4 Specific Factors and Income Distribution Chapter Organization Introduction The Specific Factors Model International Trade in the Specific Factors Model Income Distribution and the Gains from
PUBLIC HEALTH OPTOMETRY ECONOMICS. Kevin D. Frick, PhD
 Chapter Overview PUBLIC HEALTH OPTOMETRY ECONOMICS Kevin D. Frick, PhD This chapter on public health optometry economics describes the positive and normative uses of economic science. The terms positive
Chapter Overview PUBLIC HEALTH OPTOMETRY ECONOMICS Kevin D. Frick, PhD This chapter on public health optometry economics describes the positive and normative uses of economic science. The terms positive
Social Insurance Arises, In Part, Because of Asymmetric Information
 Social Arises, In Part, Because of Asymmetric Information Assume there are 2 groups, each with 100 people. The first group has 5% chance of getting injured, and the second group has a 0.5% chance. The
Social Arises, In Part, Because of Asymmetric Information Assume there are 2 groups, each with 100 people. The first group has 5% chance of getting injured, and the second group has a 0.5% chance. The
We never talked directly about the next two questions, but THINK about them they are related to everything we ve talked about during the past week:
 ECO 220 Intermediate Microeconomics Professor Mike Rizzo Third COLLECTED Problem Set SOLUTIONS This is an assignment that WILL be collected and graded. Please feel free to talk about the assignment with
ECO 220 Intermediate Microeconomics Professor Mike Rizzo Third COLLECTED Problem Set SOLUTIONS This is an assignment that WILL be collected and graded. Please feel free to talk about the assignment with
Optimal Health Insurance for Prevention and Treatment
 Optimal Health Insurance for Prevention and Treatment Randall P. Ellis Department of Economics Boston University Willard G. Manning Harris School of Public Policy Studies The University of Chicago We thank
Optimal Health Insurance for Prevention and Treatment Randall P. Ellis Department of Economics Boston University Willard G. Manning Harris School of Public Policy Studies The University of Chicago We thank
The Free Market Approach. The Health Care Market. Sellers of Health Care. The Free Market Approach. Real Income
 The Health Care Market Who are the buyers and sellers? Everyone is a potential buyer (consumer) of health care At any moment a buyer would be anybody who is ill or wanted preventive treatment such as a
The Health Care Market Who are the buyers and sellers? Everyone is a potential buyer (consumer) of health care At any moment a buyer would be anybody who is ill or wanted preventive treatment such as a
Swe den Structure, delive ry, administration He althcare Financing Me chanisms and Health Expenditures Quality of Bene fits, C hoice, Access
 Sweden Single payer, universal healthcare system, with 21 county councils as the primary payer (reimburser) Administration of healthcare plan is decentralized in the hands of the county councils Central
Sweden Single payer, universal healthcare system, with 21 county councils as the primary payer (reimburser) Administration of healthcare plan is decentralized in the hands of the county councils Central
EDUCATION AND EXAMINATION COMMITTEE SOCIETY OF ACTUARIES RISK AND INSURANCE. Copyright 2005 by the Society of Actuaries
 EDUCATION AND EXAMINATION COMMITTEE OF THE SOCIET OF ACTUARIES RISK AND INSURANCE by Judy Feldman Anderson, FSA and Robert L. Brown, FSA Copyright 25 by the Society of Actuaries The Education and Examination
EDUCATION AND EXAMINATION COMMITTEE OF THE SOCIET OF ACTUARIES RISK AND INSURANCE by Judy Feldman Anderson, FSA and Robert L. Brown, FSA Copyright 25 by the Society of Actuaries The Education and Examination
Choice under Uncertainty
 Choice under Uncertainty Part 1: Expected Utility Function, Attitudes towards Risk, Demand for Insurance Slide 1 Choice under Uncertainty We ll analyze the underlying assumptions of expected utility theory
Choice under Uncertainty Part 1: Expected Utility Function, Attitudes towards Risk, Demand for Insurance Slide 1 Choice under Uncertainty We ll analyze the underlying assumptions of expected utility theory
EC306 Labour Economics. Chapter 3" Labour Supply and Public Policy
 EC306 Labour Economics Chapter 3" Labour Supply and Public Policy 1 Objectives Income/payroll Taxes Income Maintenance Schemes Demogrant Social assistance/welfare Programs Negative Income Tax Wage Subsidy
EC306 Labour Economics Chapter 3" Labour Supply and Public Policy 1 Objectives Income/payroll Taxes Income Maintenance Schemes Demogrant Social assistance/welfare Programs Negative Income Tax Wage Subsidy
Corporate Income Taxation
 Corporate Income Taxation We have stressed that tax incidence must be traced to people, since corporations cannot bear the burden of a tax. Why then tax corporations at all? There are several possible
Corporate Income Taxation We have stressed that tax incidence must be traced to people, since corporations cannot bear the burden of a tax. Why then tax corporations at all? There are several possible
How To Determine The Impact Of The Health Care Law On Insurance In Indiana
 ACA Impact on Premium Rates in the Individual and Small Group Markets Paul R. Houchens, FSA, MAAA BACKGROUND The Patient Protection and Affordable Care Act (ACA) introduces significant changes in covered
ACA Impact on Premium Rates in the Individual and Small Group Markets Paul R. Houchens, FSA, MAAA BACKGROUND The Patient Protection and Affordable Care Act (ACA) introduces significant changes in covered
TRENDS AND ISSUES EARLY RETIREE HEALTH INSURANCE ISSUES. By Marilyn Moon, American Institutes for Research and TIAA-CREF Institute Fellow
 EARLY RETIREE HEALTH INSURANCE ISSUES By Marilyn Moon, American Institutes for Research and TIAA-CREF Institute Fellow March 2007 EXECUTIVE SUMMARY Individuals considering early retirement, i.e., retirement
EARLY RETIREE HEALTH INSURANCE ISSUES By Marilyn Moon, American Institutes for Research and TIAA-CREF Institute Fellow March 2007 EXECUTIVE SUMMARY Individuals considering early retirement, i.e., retirement
Lecture 7: Policy Design: Health Insurance & Adverse Selection
 Health Insurance Spending & Health Adverse Selection Lecture 7: Policy Design: Health Insurance & Adverse Selection Johannes Spinnewijn London School of Economics Lecture Notes for Ec426 1 / 25 Health
Health Insurance Spending & Health Adverse Selection Lecture 7: Policy Design: Health Insurance & Adverse Selection Johannes Spinnewijn London School of Economics Lecture Notes for Ec426 1 / 25 Health
Chapter 12: Economics of Information
 Chapter 11: probs #1, #3, and #4, p. 298 Problem set 4: due week of Feb 20-24 Chapter 12: probs #1 a-b-c-d, #2, #3, pp. 320-321 Future problem sets Chapter 13: probs #1, #2 a-b-c-d, #3, #5, pp. 347-348
Chapter 11: probs #1, #3, and #4, p. 298 Problem set 4: due week of Feb 20-24 Chapter 12: probs #1 a-b-c-d, #2, #3, pp. 320-321 Future problem sets Chapter 13: probs #1, #2 a-b-c-d, #3, #5, pp. 347-348
Organization of Health Insurance Markets
 Organization of Health Insurance Markets In Canada, can characterize healthcare as Universal healthcare Most medical services and tests Hospital stays in ward rooms Supplemental health insurance Prescription
Organization of Health Insurance Markets In Canada, can characterize healthcare as Universal healthcare Most medical services and tests Hospital stays in ward rooms Supplemental health insurance Prescription
Theoretical Tools of Public Economics. Part-2
 Theoretical Tools of Public Economics Part-2 Previous Lecture Definitions and Properties Utility functions Marginal utility: positive (negative) if x is a good ( bad ) Diminishing marginal utility Indifferences
Theoretical Tools of Public Economics Part-2 Previous Lecture Definitions and Properties Utility functions Marginal utility: positive (negative) if x is a good ( bad ) Diminishing marginal utility Indifferences
Sarah Dickson Otago University Degree: Law and BA majoring in Economics
 Sarah Dickson Otago University Degree: Law and BA majoring in Economics The health sector faces a dual problem. The first is essentially an economic question; the issue of how to keep public health spending
Sarah Dickson Otago University Degree: Law and BA majoring in Economics The health sector faces a dual problem. The first is essentially an economic question; the issue of how to keep public health spending
The Analysis of Health Care Coverage through Transition Matrices Using a One Factor Model
 Journal of Data Science 8(2010), 619-630 The Analysis of Health Care Coverage through Transition Matrices Using a One Factor Model Eric D. Olson 1, Billie S. Anderson 2 and J. Michael Hardin 1 1 University
Journal of Data Science 8(2010), 619-630 The Analysis of Health Care Coverage through Transition Matrices Using a One Factor Model Eric D. Olson 1, Billie S. Anderson 2 and J. Michael Hardin 1 1 University
Asymmetric Information
 Chapter 12 Asymmetric Information CHAPTER SUMMARY In situations of asymmetric information, the allocation of resources will not be economically efficient. The asymmetry can be resolved directly through
Chapter 12 Asymmetric Information CHAPTER SUMMARY In situations of asymmetric information, the allocation of resources will not be economically efficient. The asymmetry can be resolved directly through
The Large Business Guide to Health Care Law
 The Large Business Guide to Health Care Law How the new changes in health care law will affect you and your employees Table of contents Introduction 3 Part I: A general overview of the health care law
The Large Business Guide to Health Care Law How the new changes in health care law will affect you and your employees Table of contents Introduction 3 Part I: A general overview of the health care law
C(t) (1 + y) 4. t=1. For the 4 year bond considered above, assume that the price today is 900$. The yield to maturity will then be the y that solves
 Economics 7344, Spring 2013 Bent E. Sørensen INTEREST RATE THEORY We will cover fixed income securities. The major categories of long-term fixed income securities are federal government bonds, corporate
Economics 7344, Spring 2013 Bent E. Sørensen INTEREST RATE THEORY We will cover fixed income securities. The major categories of long-term fixed income securities are federal government bonds, corporate
Chapter 12. Aggregate Expenditure and Output in the Short Run
 Chapter 12. Aggregate Expenditure and Output in the Short Run Instructor: JINKOOK LEE Department of Economics / Texas A&M University ECON 203 502 Principles of Macroeconomics Aggregate Expenditure (AE)
Chapter 12. Aggregate Expenditure and Output in the Short Run Instructor: JINKOOK LEE Department of Economics / Texas A&M University ECON 203 502 Principles of Macroeconomics Aggregate Expenditure (AE)
Imperfect information Up to now, consider only firms and consumers who are perfectly informed about market conditions: 1. prices, range of products
 Imperfect information Up to now, consider only firms and consumers who are perfectly informed about market conditions: 1. prices, range of products available 2. characteristics or relative qualities of
Imperfect information Up to now, consider only firms and consumers who are perfectly informed about market conditions: 1. prices, range of products available 2. characteristics or relative qualities of
6. Budget Deficits and Fiscal Policy
 Prof. Dr. Thomas Steger Advanced Macroeconomics II Lecture SS 2012 6. Budget Deficits and Fiscal Policy Introduction Ricardian equivalence Distorting taxes Debt crises Introduction (1) Ricardian equivalence
Prof. Dr. Thomas Steger Advanced Macroeconomics II Lecture SS 2012 6. Budget Deficits and Fiscal Policy Introduction Ricardian equivalence Distorting taxes Debt crises Introduction (1) Ricardian equivalence
How To Find Out How To Balance The Two-Country Economy
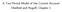 A Two-Period Model of the Current Account Obstfeld and Rogo, Chapter 1 1 Small Open Endowment Economy 1.1 Consumption Optimization problem maximize U i 1 = u c i 1 + u c i 2 < 1 subject to the budget constraint
A Two-Period Model of the Current Account Obstfeld and Rogo, Chapter 1 1 Small Open Endowment Economy 1.1 Consumption Optimization problem maximize U i 1 = u c i 1 + u c i 2 < 1 subject to the budget constraint
Work incentives and household insurance: Sequential contracting with altruistic individuals and moral hazard
 Work incentives and household insurance: Sequential contracting with altruistic individuals and moral hazard Cécile Aubert Abstract Two agents sequentially contracts with different principals under moral
Work incentives and household insurance: Sequential contracting with altruistic individuals and moral hazard Cécile Aubert Abstract Two agents sequentially contracts with different principals under moral
SUPPLEMENTARY GREEN BOOK GUIDANCE
 SUPPLEMENTARY GREEN BOOK GUIDANCE ADJUSTING FOR TAXATION IN PFI vs PSC COMPARISONS 1 INTRODUCTION 1.1 This guidance looks at the differential tax receipts that arise from the use of the Private Finance
SUPPLEMENTARY GREEN BOOK GUIDANCE ADJUSTING FOR TAXATION IN PFI vs PSC COMPARISONS 1 INTRODUCTION 1.1 This guidance looks at the differential tax receipts that arise from the use of the Private Finance
SELECTION IN INSURANCE MARKETS by Steven E. Landsburg University of Rochester
 SELECTION IN INSURANCE MARKETS by Steven E. Landsburg University of Rochester Consider an insurance market say, for insurance against accidental injuries. Agents face different levels of accident risk,
SELECTION IN INSURANCE MARKETS by Steven E. Landsburg University of Rochester Consider an insurance market say, for insurance against accidental injuries. Agents face different levels of accident risk,
ASSESSING THE RESULTS
 HEALTH REFORM IN MASSACHUSETTS EXPANDING TO HEALTH INSURANCE ASSESSING THE RESULTS March 2014 Health Reform in Massachusetts, Expanding Access to Health Insurance Coverage: Assessing the Results pulls
HEALTH REFORM IN MASSACHUSETTS EXPANDING TO HEALTH INSURANCE ASSESSING THE RESULTS March 2014 Health Reform in Massachusetts, Expanding Access to Health Insurance Coverage: Assessing the Results pulls
Chapter 10 SUPPLEMENTARY FINANCING OPTION (3) MEDICAL SAVINGS ACCOUNTS. Medical Savings Accounts as Supplementary Financing
 Chapter 10 SUPPLEMENTARY FINANCING OPTION (3) MEDICAL SAVINGS ACCOUNTS Medical Savings Accounts as Supplementary Financing 10.1 Medical savings accounts are mandatory employment based and income linked
Chapter 10 SUPPLEMENTARY FINANCING OPTION (3) MEDICAL SAVINGS ACCOUNTS Medical Savings Accounts as Supplementary Financing 10.1 Medical savings accounts are mandatory employment based and income linked
Problem Set #3 Answer Key
 Problem Set #3 Answer Key Economics 305: Macroeconomic Theory Spring 2007 1 Chapter 4, Problem #2 a) To specify an indifference curve, we hold utility constant at ū. Next, rearrange in the form: C = ū
Problem Set #3 Answer Key Economics 305: Macroeconomic Theory Spring 2007 1 Chapter 4, Problem #2 a) To specify an indifference curve, we hold utility constant at ū. Next, rearrange in the form: C = ū
Lecture 1: Asset Allocation
 Lecture 1: Asset Allocation Investments FIN460-Papanikolaou Asset Allocation I 1/ 62 Overview 1. Introduction 2. Investor s Risk Tolerance 3. Allocating Capital Between a Risky and riskless asset 4. Allocating
Lecture 1: Asset Allocation Investments FIN460-Papanikolaou Asset Allocation I 1/ 62 Overview 1. Introduction 2. Investor s Risk Tolerance 3. Allocating Capital Between a Risky and riskless asset 4. Allocating
Legislative Council Panel on Health Services Subcommittee on Health Protection Scheme
 LC Paper No. CB(2)1360/11-12(01) For discussion on 19 March 2012 Legislative Council Panel on Health Services Subcommittee on Health Protection Scheme Roles of Public Funding and Health Insurance in Financing
LC Paper No. CB(2)1360/11-12(01) For discussion on 19 March 2012 Legislative Council Panel on Health Services Subcommittee on Health Protection Scheme Roles of Public Funding and Health Insurance in Financing
The Taxable Income Elasticity and the Implications of Tax Evasion for Deadweight Loss. Jon Bakija, April 2011
 The Taxable Income Elasticity and the Implications of Tax Evasion for Deadweight Loss Jon Bakija, April 2011 I. The Taxable Income Elasticity Literature Traditionally, the microeconometric literature on
The Taxable Income Elasticity and the Implications of Tax Evasion for Deadweight Loss Jon Bakija, April 2011 I. The Taxable Income Elasticity Literature Traditionally, the microeconometric literature on
Health & Government Module 5 i2p Expedition India
 Health & Government Module 5 i2p Expedition India National Emblem of India : Emblem i2p Expedition India India 2011 1 Take Home Points The United Nations has declared access to basic health care a human
Health & Government Module 5 i2p Expedition India National Emblem of India : Emblem i2p Expedition India India 2011 1 Take Home Points The United Nations has declared access to basic health care a human
Introduction. Employer sponsored health insurance, Part 1. This section of class
 ntroduction Employer sponsored health insurance, Part 1 ECON 40447 Fall 2009 1 Most health insurance in this country is provided by employers as a fringe benefit Function of the tax-preferred nature of
ntroduction Employer sponsored health insurance, Part 1 ECON 40447 Fall 2009 1 Most health insurance in this country is provided by employers as a fringe benefit Function of the tax-preferred nature of
