230s Abstract printing supported by. Visit Chiesi at Stand B2.10
|
|
|
- Anabel Mabel Todd
- 8 years ago
- Views:
Transcription
1 120. Clinical issues in malignant pleural effusions P1253 Mesothelioma diagnosis in a district general hospital Shashank Sharma, Katie Wimble, Behdad Shambayati, Michael Wood. Respiratory Medicine, St. Peters Hospital, Chertsey, Surrey, United Kingdom Background: Malignant mesothelioma(mm) is a rare cancer with poor prognosis, posing a diagnostic challenge to respiratory physicians. Aim: We analysed our current diagnostic process for MM to assess the diagnostic yield of different investigative modalities. Methods: We analysed the effectiveness of various diagnostic modalities including pleural fluid cytology, CT or ultrasound guided(usg) core and thoracoscopically guided pleural biopsy over the last five years. Results: Of 55 patients diagnosed with MM since January 2007, 54 patients had confirmed cytological or histological diagnosis. 33(60%) patients had pleural fluid sent for cytology of which 17(51%) were positive for MM, 11(33%) negative, 3(9%) suspicious, 2(6%) showed a lung primary which eventually turned out to be MM and 3% inconclusive. 15 patients presented with pleural thickening or mass without pleural effusion. These patients were diagnosed with CT or USG biopsies. 26 patients underwent VATS. Interestingly, the percentage of patients that have been diagnosed positively on cytology has risen year on year(fig.1). PET scanning identifed an appropriate biopsy site in 4 of 8 patients scanned. Conclusion: We attribute the progressive increase in the cytological diagnoses made in our hospital to the increasing confidence of our cytologists in recognition of cytological features and use of wider immunocytochemical panels. PET can be instrumental in achieving the diagnosis in difficult cases. P1254 Malignant mesothelioma. A survival analysis of 123 consecutive cases at an occupational clinic Ellen Skammeritz 1, Lars Haukali Omland 2, Jens Peter Johansen 1, Øyvind Omland 1. 1 Dept. of Occupational Medicine, Aalborg Hospital, Århus University Hospital, Aalborg, Denmark; 2 Dept. of Infectious Diseases, Rigshospitalet, Copenhagen, Denmark Aim: To describe the asbestos exposure, to identify factors associated to the prognosis, and to calculate the medial survival time in 123 consecutive patients ( ) with patological verified diagnosis of malignant mesothelioma (MM). Method: From medical records we identified age, sex, asbestos fibres exposure, localisation and subtypes of MM, performance status, and treatment. Results: Median age was 65 years (min max. 90) and 111 (90.2%) were men and 12 (9.8%) were women. We identified asbestos exposure in 112 (91%) patients. Major contributers were industries of shipbuilding (30%), construction (22%), asbestos-cement (17%), metal (8%), and automobile repair (6%). 2 years survival for MM in pleura % (95% CI) were: 19 (12-30), peritoneum: 24 (8-74), pleura and peritoneum/pericardium: 25 (5-100), and tunica vaginalis: 100 ( ). In Cox regression survival analysis for all cases but tunica vaginalis (N=120) significant variables for mortality rate ratio (MRR) (95% CI) were male sex: 2.26 ( ) and performance status > 2: 5.01 ( ). In a model restricted to MM in pleura (N=78) significant variables were male sex: 6.95 ( ), sakromatiod subtype: 6.10 ( ), performance status > 1: 4.64 ( ), and time after trimodal treatment 0.25 ( ). Conclusion: Asbestos exposure was identified in 91% of the patients, shipbuilding-, constructing-, and asbestos-cement industry accounted for >2/3 of the cases. 2 years survival for MM was 19% to 25% in pleura and peritoneum, in tunica vaginalis 100%. Male sex, low performance status, and sarkomatiod subtype lower while trimodal treatment enhance survival time. 230s
2 P1255 Prognostic factors and survival in malignant pleural mesothelioma at a large tertiary referral center in Turkey Berna Komurcuoglu, Kadri A. Cirak, Nur Yucel, Gulru Polat, Ozan Usluer. Pulmonology, Dr. Suat Seren Education Hospital for Chest Disease and Surgery, Izmir, Turkey Malignant pleural mesothelioma is a rare tumor but increasing incidance and poor prognosis despite new therapy modalities. In this study we aimed to investigate the effects of various pretreatment clinical and laboratory characteristics on survival of patients with malignant pleural mesothelioma (MPM). During last five years, 125 histological proven MPM cases were evaluated at large tertiary refferal center in eastern part of Turkey. Patients age, gender, performance score, histology, asbestos exposure, smoking history, sympyoms, plasma platelet count, haemoglobin, white blood cell (WBC), plasma LDH level, stages were evaluted in both multivariate and univariate analysis. Univariate analysis showed that patients with extensive stage, N2 nodal invasion and M1 metastasis have a worse prognosis. Multivariate Cox regression analysis showed that sarcomatous histology has found to be indicators of worse prognosis (HR 1, % 95 CI , p= 0.017). As a result; The patients with extensive stage, n2 nodal inavsion and M1 metastasis were found to related with shorter survival. Sarcomatous histology were found as an indipendent worse prognostic factor in MPM. P1256 Malignant pleural mesothelioma stage III and IV: Retrospective analysis of ten years in a central hospital Claudia Lares dos Santos, Ines Sanches, Ligia Fernandes, Filipa Cruz e Costa, Fernando Barata. Pulmonology Department, Centro Hospitalar Universitário de Coimbra, CHC, Coimbra, Portugal Introduction: Pleural mesothelioma (PM) is the most frequent malignant primary tumor of pleura. The incidence in Western Europe is still rising due to the prolonged latency of the disease. Aims: Determine demographic, epidemiological, histological and therapeutical aspects of malignant PM in stage III and IV. Evaluate survival rates. Methods: The study was conducted in an European central hospital covering approximately inhabitants. We performed a retrospective analysis of cases diagnosed in our department over a period of 10 years. Survival analysis was performed using Kaplan Meier method and Cox regression. Results: We diagnosed 32 cases in stages III/IV (91,5% of total), 84.4% men, mean age 65.5±10.2 years, 50% with current or past exposure to tobacco. Exposure to asbestos was reported in 56.3% and had occurred, on average, 41.4±10.8 years before. Approximately 56% of exposures were associated with building construction and mechanics. In 87.5% the diagnosis was obtained with videoassisted thoracic surgery. Histology was epithelioid in 84%. All patients received chemotherapy: 53.1% carboplatin+gemcitabine, 37.5% pemetrexed+cisplatin and 9.4% cisplatin+gemcitabine. Hematological toxicity occurred in 18.8% and non haematological toxicity in 12.5% (grade 3/4). Prophylactic local radiotherapy was performed in 75%. Median survival was 51.6±9.4 weeks. There was no statistically significant difference according to chemotherapy regimen. Conclusion: Malignant PM must be considered, particularly in men involved in mechanics, even with unrecognized or remote exposure to asbestos. In our series no difference was seen combining platinum analogs with gemcitabine or pemetrexed. P1257 Pleural atypical mesothelial hyperplasia: An early stage of pleural malignant mesothelioma? Thomas Vandemoortele 1, Sophie Laroumagne 1, Olivier Bylicki 1, Sophie Giusiano 2,HervéDutau 1, Philippe Astoul 1. 1 Department of Thoracic Oncology, Pleural Diseases, and Interventional Pulmonology, Hôpital Nord, Marseille, France; 2 Department of Pathology, Hôpital Nord, Marseille, France Mesothelioma is a neoplastic process most often secondary to asbestos exposure. Atypical mesothelial hyperplasia (AMH) is thought to be a benign process in reaction to various processes, including infectious pleurisy and recurring transudative pleural effusion. However, it is unknown if there might be a link between AMH and malignant pleural mesothelioma (MPM). Herein, we present the case of a 69 year-old patient with documented asbestos exposure in whom MPM was diagnosed four months after a first diagnosis of AMH. Thoracoscopy showed inflammation of the posterior parietal pleura and white lymphangitis of the anterior pleura, without nodule or any other suspicious lesion. Biopsies taken from the anterior pleura showed AMH. Two months later, the patient returned with a recurring right sided effusion. CT-scan revealed a subcarinal lymph node measuring 15x8mm and a pleural effusion with partial atelectasis of the right lower and middle lobes. Repeat thoracoscopy was performed, four months after the initial one. The pleura was dramatically changed, with numerous nodules and neoplastic lymphangitis. Multiple biopsies were performed on the diaphragmatic and posterior pleura. Histologic features were compatible with epithelioid MPM. How MPM evolves from normal pleura is still debated, despite the acknowledgement of the causal relation with asbestos. Whether mesothelioma evolves from atypical hyperplasia, as epithelium-derived cancer of other origins, remains to be elucidated. Conclusion: Diagnosis of MPM relies on pleural biopsy specimens. Thoracoscopy is particularly useful in guiding pleural biopsies and in symptomatic improvement if talc pleurodesis is performed. P1258 Role of medical thoracoscopy in diagnosis of recurrent undiagnosed pleural effusion Ramadan Bakr, Ibrahim Elmahallawy, Osama Mansour, Ahmad Ali, Samy El-Dahdouh. Chest Department, Menoufiya University, Shebin Elkom, Menoufiya, Egypt Background: The urge for the resurgence of thoracoscopic techniques came essentially from the depressive situation of chronic exudates not diagnosed in 20-40% of cases after using the ordinary diagnostic methods. Methods: This study comprised 20 cases with exudative pleural effusion, all of them were subjected to full history taking, clinical examination, laboratory investigations, radiological examination (chest x- ray and CT), abdominal US, chest US if needed, tuberculin test, sputum for AFB, ABG and ECG. For all patients, pleural tapping and biochemical, cytological, bacteriological and immunological examinations for the pleural aspirates, as well as blind Abrams needle pleural biopsy and histopathological examination were done. The etiologic diagnosis of pleural effusion was not settled after all these investigations, and thus, medical thoracoscopy, under local anesthesia, was carried out for each patient. Results: The mean age of patients was 57.6 years. The diagnosis was achieved in 85% of cases, while 15% of cases diagnosed as non specific pleuritis. The result of biopsies were 65% malignancy (20% mesothelioma, 35% metastatic adenocarcinoma, 5% of either lymphoma or thymoma), and 35% of cases were nonmalignant, 15% undiagnosed, 10% TB, 5% of either empyma or RA). 20% of cases had complication in the form of 10% malposition of the intercostal tube and 5% of either hematoma or infection at the site of tube entry. Conclusion: Medical thoracoscopy, under local anesthesia and conscious sedation, is an effective procedure for diagnosing the underlying etiology of recurrent pleural effusion of unknown etiology, with minimal complications. P1259 Study of thoracoscopic pleural biopsy for nondiagnostic pleural effusion YuJin Kim, Sun Young Kyung, Sang Pyo Lee, Sung Hwan Jeong, Shin Myung Kang, Sang Min Lee, Jeong-Woong Park. Division of Pulmonology and Critical Care Medicine, Department of Internal Medicine, Gachon University Gil Hospital, Incheon, Korea Background: We performed thoracentesis and pleural biopsy by cope needle to find cause of exudative pleural effusion. Usually about 20% of them can t find cause. We study thoracoscopic biopsy for nondianostic patients and charateristics of diseases. Method: We enrolled patients from April 2004 to May We included patients with nondiagnostic pleural effusion through sputum study, thoracentesis, washing microbiologic study and cytology by bronchoscopy. Twenty-six patients were performed thoracoscopic pleural biopsy. Result: Twenty-four patients were identified. Their mean age was 60.5±15.3years, and 16(66.7%) of the patients were men. Four patients weren t performed thoracentesis. Charateristics of pleural effusion were lymphodominent (15; 75%), poly-dominent(2;10%), eosinophil dominant (1;5%) and unknown(2;10%). Final diagnosis of patients with undiagnostic pleural effusion were malignant effusion (n=14, 58.3%), Tb pleuray(n=3, 12.5%), chronic inflammation and fibrosis(n=5, 20.8%) and hemorrhagic effusion and eosinophilic effusion (n=2, 8.3%). The most common cause of malignant effusion was secondary not primary lung cancer. Metastatic effusion were 5 patients (35.7%). Malignant mesothelioma were 3patients (21.4%). adenocarcinoma of unknown origin were 2patients (14.3%). Primary lung cancer were 4patients (25.8%). Conclusion: Fifteen patients(58.3%) of nondianostic effusion were diagnosed malignant effusion. In These 15 patients, secondary malignant effusion were 10. patients(74.3%). In Conclusion, we consider thoracoscopic biopsy and systemic examination to identified nondianostic pleural effusion. P1260 Medical thoracoscopy experience: 3 years on Burhan Khan, Hamid Aminy Raouf, Majid Mushtaq. Department of Respiratory Medicine, Darent Valley Hospital, Dartford, Kent, United Kingdom Aim: To describe the qualitative and quantitative experience and outcomes at 3 years of medical thoracoscopy (MT) in a DGH. Methods: Retrospective case series review of all consecutive adult patients undergoing MT. Results: To date, 39 MTs have been done between Sept 09 and Sept 11. Median age 71 yrs (range: years); 28 (72%) male. Median age of patients with malignancy 70 (range: years); 15 male (65%). MT was non-diagnostic in 3 cases (7.7%) with one confirmed as metastatic carcinoma on CTGBx. 9/10 MPM were pleurodesed; 8(89%) successful All 13 non-mpm were pleurodesed; 9(70%) 231s
3 P1262 In an era where VATS and medical thoracoscopy is readily accessible Does diagnostic thoracocentesis still have a role in diagnosing malignant pleural effusions? Kerry Woolnough. Respiratory Medicine, University Hospital of North Staffordshire, Stoke on Trent, United Kingdom Figure 1 Introduction: The diagnostic sensitivity of medical thoracoscopy is reported as 92.6% and is approximately 95% for video-assisted thoracoscopic surgery (VATS). Complication rates are acceptably low (2.3% for medical thoracoscopy and <1% for VATS). We wished to ascertain the sensitivity of diagnostic thoracocentesis, compared to VATS for malignant pleural effusions. Method: We retrospectively looked at all pleural fluid samples taken from a diagnostic thoracocentesis and specimens sent from a VATS procedure over a 12 month period in patients who had a confirmed diagnosis of malignancy. The presence of malignant cells, pathological diagnosis and the primary site of malignancy was recorded. Results: Over a 12 month period 34 patients underwent VATs and an additional 88 patients had a diagnostic thoracocentesis performed for a malignant pleural effusion. 88.2% (N=30) had a pathological diagnosis made in samples taken during VATs and 73.6% (n=64) had a diagnosis of pleural malignancy confirmed on cytology taken from a diagnostic aspirate. Conclusion: With the increased availability of medical thoracoscopy and VATS it is tempting to incorporate these into the first step of a diagnostic algorithm for suspected malignant effusions. However the high diagnostic yield revealed by our retrospective analysis of pleural fluid cytology illustrates that diagnostic thoracocentesis and pleural fluid cytology remains a valid initial step in the diagnostic pathway. It is more cost effective, less time consuming and less invasive for the patient. Figure 2 successful. Overall pleurodesis success rate was 77.3%. Excluding the two patients who died within 30 days, pleurodesis success rate is 85% (17/20) for all malignant pleural effusion. Conclusions: Success rates are reported in literature 82.1% - 95% in patients having a single procedure and one pleurodesis only, similar to ours but for the 2 patients aged 72 and 76 years who died; having significant co-morbidities and confirmed metastatic carcinomas with poor pre-op performance status of 3. MT was well tolerated in our cohort of patients who had median age of 70, and success rates varied dependent on pathology; better in MPM than carcinoma. Qualitatively, the most significant result was the duration of pleural fluid recurrence free days that patients achieved, thus mitigating symptoms and avoiding further or repeated invasive pleural interventions. P1261 Results of treatment of the metastatic pleural effusion Goran Kondov 1, Zoran Spirpovski 1, Risto Colanceski 1, Sasko Jovev 1, Biserka Caeva 2, Borislav Kondov 1. 1 Thoracic Surgery, University Clinic for Thoracic and Vascular Surgery, Skopje, Macedonia, The Former Yugoslav Republic of; 2 Pulmology, University Clinic for Pulmology, Skopje, Macedonia, The Former Yugoslav Republic of Metastatic pleural effusion is big health, social and personal problem. Prognosis of patients is 1 to 60 months which is according underling disease, stage of the disease, treatment response, characteristics of the patients and their reserve. We analyze 60patients with confirmedmalignant pleural effusion: 28 patients with breast cancer, 14 with lung cancer, 8 with mesotelioma, 5 with gastric carcinoma, and 5 with other malignant lesions. Mean age were 56 years. At this 60 patients we have done 194 procedures. We analyze effects of thoracocentesis only (60), placing pleurocat (37), placing of thoracic drain (54), VATS with talk pudrage(13) and thoracic drain and thoracic drainage with slurry talk pleurodesis (14). Recurrence of pleural effusion, febrile condition, appearing of the empyema, problems with heart, dispnea, life treating conditions were followed at all patients. Results: Recurrence of pleural effusion were detected at 71,2%, where the best results were with use of VATS with talk pudrage (53,8%), than is thoracic drainage with slurry talk pleurodesis with success rate of 50%. With only placing of drain success rate was 29,6% or with pleurocat placing 27%. With thoracocentesis only, no one has had success. Unwanted conditions were detected the most frequently at thoracic drainage with slurry talk pleurodesis where were detected 14,3% heart problems, 35,7% dispnea and respiratory symptoms, 35,7% febrile conditions with septic conditions. Conclusion: VATS with talk pudrage give the best results with control of the malignant pleural effusion, but need hospitalization and general anesthesia procedure, procedure which was not recommended for many patients which is in bad general conditions. P1263 Effectiveness and safety of endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA) in the diagnosis of mediastinal and hilar lymphoadenopathy Yuuki Tenjin 1, Junji Hamamoto 2, Shinya Sakata 1,RyoSato 1, Sho Saeki 1, Hidenori Ichiyasu 1, Kazuhiko Fujii 1, Naoki Saita 1, Hirotsugu Kohrogi 1. 1 Department of Respiratory Medicine, Kumamoto University Hospital, Kumamoto, Japan; 2 Department of Respiratory Medicine, Kumamoto Saishunso National Hospital, Kumamoto, Japan Endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA) is used to biopsy of enlarged lymphnodes in the mediastinum and hili for staging of patients with lung cancer and definitive diagnosis of lymphadenopathy. EBUS-TBNA has been reported as less-invasive examination compared with mediastinoscopy and as high sensitivity and specifity in the diagnosis. To study the usefulness of EBUS-TBNA in diagnosis of lymphadenopathy in the mediastinum and hili, we analyzed the 90 cases of EBUS-TBNA which were performed in our hospital from August 2007 to July There were 90 cases of undiagnosed lymphadenopathy in the mediastinum and hili. They were 53 cases of suspected metastasis of lung cancer, 37 cases of suspected sarcoidosis. In the cases of suspected metastasis of lung cancer, the sensitivity of EBUS-TBNA was 85.4%, and the specificity was 100% and the accuracy was 86.5%. In the cases of suspected sarcoidosis, the sensitivity was 92%, the specificity was 90% and accuracy was 92.3%. Furthermore, we made diagnosis of EGFR gene mutation and EML4-ALK fusion gene by the specimen obtained by EBUS-TBNA. As adverse effects, one case of lymphadenitis was observed, but mediastinitis was not induced. We conclude that EBUS-TBNA is a powerful instrument for diagnosis and staging of lung cancer and for diagnosis of sarcoidosis and other inflammatory and granulomatous diseases with lymphadenopathy manifested in the mediastinum and hili, and that EBUS-TBNA is safe and less-invasive. P1264 WITHDRAWN 232s
4 P1265 Combination therapy with intrapleural doxycycline and talc in reduced doses for pleurodesis Khaled Hassaan. Pulmonary Medicine, Zagazig University Hospital, Zagazig, Egypt Background: We hypothesized that combining doxycycline and talc in half the usual doses would be synergistic in inducing pleurodesis. Objective: The aim of the study was to evaluate safety and efficacy of low-dose doxycycline combined with low-dose talc for pleurodesis. Methods: In a prospective study, 20 consecutive patients with recurrent and biopsy-proven malignant effusions and 4 patients with recurrent pneumothorax were included. All pleurodesis was performed with talc plus doxycycline as the sclerosing agents. Doses of doxycycline (250 mg) and talc (2.5 grams) were half the usual doses. the sclerosing agents were administered via tube thoracostomy. Post-pleurodesis postero-anterior (PA) radiographs were obtained after tube removal and 30 days following the procedure. Successful therapy was defined as a complete absence or minor re-accumulation of pleural effusion one month after pleurodesis. Results: Twenty four cases were identified (8 women, 16 men, Mean age was 65.2 years). No immediate perioperative complications were noted. Chest tube duration averaged 4.3±2.5 days. Length of stay after the procedure 4.8±3.2 days. Eight patients (33%) reported persistence or worsening dyspnea in the immediate postoperative period. Only one developed respiratory distress; no any parenchymal changes on chest radiography and no required ventilatory support. Other immediate postoperative events included chest pain in 10 patients (42%) and fever in 2(8%) patients. Twenty patients (83%) had successful pleurodesis and 4 (17%) failed. Conclusions: The combination of low-dose doxycycline with low-dose talc appears to be a safe and rational approach to pleurodesis with reasonable side-effects. effusion was diagnosed in 33 patients (5.64%). Paramalignant effusion was found in 17 patients with squamous cell ca (4.7%), in 9 patients with SCLC (6.5%) and in 3 patients with adenoca (3.6%). No statistical significance was found when correlating frequency ofparamalignant effusion to hystological type of lung cancer (p>0.05). Malignant effusion was diagnosed in 55 patients. Malignant effusion was the most common in pts suffering from adenoca (found in 26 patients 30.6%, p<0.01), while malignant effusions were found in 13 pts with squamous cell ca (3.6%), and in SCLC in 9 patients (6.5%). Discussion: No statistical significance was found when trying to correlate frequency of paramalignant effusion in different histological types of lung cancer. In the group of patients with malignant effusion adenoca is the most common causal factor of spread of malignant disease to pleura. P1268 Chloroma as a mediastinal mass with bronchial infiltration and severe stenosis of the left main bronchus Joao Pedro Steinhauser Motta, Axel Tobias Kempa, Franz Stanzel, Jörn Brune. Pneumologie, Lungenklinik Hemer, Nordrhein Westfalen, Germany We report the case of a 46 years old women, who presented to our hospital with cough, chest pain and exertional dyspnea for 1 month. The physical examination showed inspiratory stridor located on the left hemithorax. The laboratory tests showed no pathological changes. The thorax computer tomography showed a large mediastinal mass with compression of the left main bronchus. P1266 Iodopovidone: An effective agent pleurodesis used through chest tube Kotti Amina, Daghfous Hafaoua, Snan Houda, Saad Soumaya, Kahloul Olfa, Tritar Fatma. Pneumolgy C, Abderrahmane Mami Hospital, Ariana, Tunisia Pneumolgy C, Abderrahmane Mami Hospital, Ariana, Tunisia Pneumolgy C, Abderrahmane Mami Hospital, Ariana, Tunisia Pneumolgy C, Abderrahmane Mami Hospital, Ariana, Tunisia Pneumology C, Abderrahmane Mami Hospital, Ariana, Tunisia Pneumology C, Abderrahmane Mami Hospital, Ariana, Tunisia Background: Most variety of pleural irritants have been used for pleurodesis, the ideal agent should produce pleurodesis effectively, safely, and in shortest possible time. Objective: Compare efficacy and safety of iodopovidone used through chest tube to other agents used via thoracoscopy. Patients and methods: Fifty six patients (35 men and 21 women) with malignant pleural effusion (n=40) or pneumothorax (n=10) aged from 5 to 76 years, were distributed into 2 groups: G1: 40 patients treated with injecting iodopovidone 3 successively days (20 ml iodopovidone + 30 ml saline solution) via chest tube G2: 16 patients had pleurodesis through thoracoscopy using talc. Results: Time to pleurodesis was similar in 2 groups (8±3 vs6±2 days).asthe mean length of hospitalization (31,13±22 vs 27,4±15 days) and mean length of drainage (8,8±6,1 days vs 10,6±8,1 days), there is no statistically difference in the 2 groups. A complete response with no recurrence was similar in 2 groups obtained in 44 (78,5%) of cases. After instillation of the sclerosing agent, intense cough and dyspnea were noted only in G1 (n= 3), and 2 patients had systemic hypotension and intense pleuritic pain. Local complications were observed in 10 cases (18%) with no statistically difference in 2 groups: pneumothorax (n= 7) and empyema (n= 3). Chest pain evaluated with visual scale measurement after removed tube was similar in 2 groups. As the mean length of follow-up, there is no statistically difference (5±2.9 and 6,3±1,8 months). Conclusion: Iodopovidone is an effective, safe, cheap, easily available alternative to achieve chemical pleurodesis in cases of recurrent, incapacitating effusions, regardless of etiology. P1267 Pleural effusions in lung cancer Milic Medenica, Redzep Kraja, Miras Medenica. Bronchology, Hospital for Lung Diseases Brezovik, Niksic, Montenegro, Serbia Bronchology, Hospital for Lung Diseases Brezovik, Niksic, Montenegro, Serbia Student at School of Medicine, University of St Andrews, United Kingdom The most common cause of malignant effusions in males is lung cancer. Malignant effusions are the result of spread of lung cancer to pleura or dissemination of metastatic tumour to one of the pleural surfaces. Paramalignant effusions are the result of lung cancer, but not a result of spread of malignant diseases to pleura. Methods: The study group comprised of patients in territory of Montenegro, in time period from to All patients with pleural effusions had their pleural liquid citologically tested, and histological processing of samples of pleural tissue obtained by blind needle biopsy (66 patients) or VATS (8 patients) was done. Descriptive statistical method and retrospective study were used. Results: Total number of newly diagnosed cases of lung cancer was 585 (squamous cell ca (62%); SCLC- 139 (23.5%) adenoca 85 (14.5%)). Paramalignant Bronchoscopy revealed an almost complete obstruction of the left main stem bronchus with extensive infiltration of the mucosa by tumorous tissue. The EBUS- TBNA biopsies demonstrated the suspect of a neoplasm of hematologic origin. The patient was transferred to a referral center for hemato-oncology and underwent a bone narrow biopsy. It could be diagnosed an acute myeloid leukemia. The mediastinal mass and bronchial infiltration corresponded to a chloroma (myeloid sarcoma) as a rare and severe initial manifestation of the disease. Chloroma is an extramedullary, solid tumor which occurs in association with myeloproliferative or leukemic disorders. It affects 3-8% of patients with acute myeloid leukemia and can present as the initial manifestation of hematologic malignicy. The anatomic distribution includes bone, nerve, lymph node, and skin, but may involve a variety of soft tissues. Pulmonary and mediastinal involvement is rare. Just one case has yet been reported in literature with an identical pattern of airway infiltration. P1269 Ectopic heterotopic mediastinal thyroid tissue mimicking lung cancer Kalliopi Athanassiadi 1, Maria-Styliani Kolokotroni 1, Ilias Samiotis 1, Despina Violidaki 2, Konstantina Sotiriou 3, Dimitra Rondogianni 2, Ion Bellenis 1. 1 Thoracic Surgery, General Hospital Evangelismos, Athens, Greece; 2 Pathology, General Hospital Evangelismos, Athens, Greece; 3 Anaesthesiology, General Hospital Evangelismos, Athens, Greece Objective: Ectopic intrathoracic thyroid is a very rare presentation of a mediastinal mass, comprising 1% of mediastinal tumors and can be distinguished from restosternal goiter or secondary intrathoracic goiter from the fact that the former receives its blood supply from mediastinal vessels rather than the neck and is not connected to the cervical thyroid. We present a series of 9 patients with heterotopic mediastinal thyroid mimicking lung cancer. Material: Nine patients, 5 male and 4 female ranging in age between 56 and 79 years were admitted at our hospital. All patients but two were asymptomatic. Chest radiography revealed a mass in the superior middle or posterior mediastinum, in 2 cases with tracheal deviation. CT scan revealed a mass and further investigation took place with MRI. Preoperative staging was negative for metastatic disease in all cases and ultrasonography, scintigram and I131 uptake precluded the possible existence of thyroid tissue. Thyroid function tests were also normal. Results: All patients were led to surgery and were submitted either to lateral mini-thoracotomy (n=5), or cervical incision (n=3) or thoracoscopy (n=1). In all cases there was an encapsulated mass with blood supply from intrathoracic vessels 233s
5 and histopathology revealed thyroid. The postoperative course was uneventful and no recurrence was observed in a follow up of 2 months to 4 years. Conclusion: Although malignant transformation in heterotopic thyroid tissue is extremely rare, these masses should be resected in order to put the diagnosis and to avoid later complications such as progressive enlargement, hemorrhage within the mass causing respiratory failure, and compression of vital mediastinal organs. P1270 Endobronchial ultrasound transbronchial needle aspiration at Aberdeen Royal Infirmary: How are we doing? David Miller 1, Pratheega Mahendra 1, Valerie Bruce 1, Keith Kerr 2, Mary McKean 2, Mahendran Chetty 1, Graeme Currie 1. 1 Chest Clinic C, Aberdeen Royal Infirmary, Aberdeen, United Kingdom; 2 Department of Pathology, Aberdeen Royal Infirmary, Aberdeen, United Kingdom Background: Endobronchial ultrasound transbronchial needle aspiration(ebus- TBNA) is a more convenient alternative to mediastinoscopy for sampling mediastinal lymph nodes. We describe the demographics, results and diagnostic sensitivity of EBUS-TBNA in the 1st 100 procedures performed. Methods: Since the service began in 2010, patient age, gender, length of procedure, sedative doses, numbers of passes for each node and results were recorded and retrospectively analysed. Results: Of 100 patients, 66 were male with mean age 62 years (range 22-88). Mean procedure duration was 16 minutes, and median doses of midazolam and fentanyl were 4mg and 100mcg respectively. 142 lymph nodes were sampled with median number of passes of 4 per node. Lymphoid material was obtained from 126 (86%) of all nodes sampled. A pathological abnormality was found in 73 patients: NSCLC (n=34), SCLC (n=20), granulomatous inflammation (n=14), possible lymphoma (n=1) and metastatic neck (n=1), urological (n=2) and breast cancer (n=1). In the remaining 27 patients, no lymph node was sampled in 10 and lymph node was sampled in 17 cases with no abnormality noted; of the latter, 9 were true negatives. The diagnostic sensitivity for all 100 cases was 81% (77% in the first 50 procedures versus 84% in the remainder). Conclusions: A variety of cell types can be identified using EBUS-TBNA. Our overall diagnostic sensitivity was 81% with the top of the learning curve almost reached after 50 procedures. The high diagnostic sensitivity implies that many mediastinoscopies can be avoided with potential financial savings. P1271 Ideal volume sampling in the diagnosis of malignant pleural effusions Vasilis Anastasakos, Mpisirtzoglou Danai, Zetos Athanasio, Mpampoukos Stavros, Marketos Charalampos, Georgios Politis. Respiratory Unit, Agios Savvas Oncological Hospital, Athens, Greece Introduction: Management of pleural effusion is based on established guidelines deriving from scientific committees and experts on pleural diseases all over the world. Nevertheless true consensus on volume sampling in malignant pleural effusions has not yet been achieved. Only few publications have been published over the past 10 years. Further studies should take place in order to clarify this essential point in the management of malignant pleural effusions. Hypothesis: 20 to 40 ml of pleural fluid could improve cytology yield in high risk malignancy patients. Methods and materials: Patients with at least medium sized pleural effusion and high risk for malignancy are enrolled. Pleural fluid is extracted as follows: 1. 10cc of pleural fluid sent for cell typing and ALB, tpr, LDH, CHOL, TG analysis 2. 20cc of pleural fluid extracted and placed as sample A 3. 50cc of pleural fluid extracted and placed as sample B cc of pleural fluid should be extracted and placed as sample C Samples A, B and C are sent for cytology Cytology results include the following: 1. Positivity or negativity for malignancy 2. Malignant cells numerosity (rare, infrequent, frequent, dense) First data in our research strongly support our hypothesis and we feel that with our sample growing we will be able to show that a larger quantity of pleural fluid will not improve results (whilst will affect costs and laboratory man hours), but 20 to 40 ml could play a role in diagnosis and should be the target quantity. We hope our study will help to decrease time to diagnosis, reduce cost (less paracentesis, less adverse effects, less hospitalization time) and provide material for evidence based guideline development in the future. 234s
Surgeons Role in Symptom Management. A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND
 Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
International Journal of Case Reports in Medicine
 International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Therapy of pleural effusions Modern techniques
 Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Malignant Pleural Mesothelioma Diagnosed by Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration
 http://dx.doi.org/10.4046/trd.2013.74.2.74 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:74-78 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2013.74.2.74 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:74-78 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines
 Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1. Jonathan C. Daniel 2. Kenneth S.
 PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1 Jonathan C. Daniel 2 Kenneth S. Knox 1 Kathleen Williams 1 Departments of Medicine 1 and Surgery 2, University
PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1 Jonathan C. Daniel 2 Kenneth S. Knox 1 Kathleen Williams 1 Departments of Medicine 1 and Surgery 2, University
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Malignant Mesothelioma Diagnosed by Bronchoscopic Biopsy
 CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.3.297 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:297-301 Malignant Mesothelioma Diagnosed by Bronchoscopic Biopsy Yeon-Hee Park,
CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.3.297 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:297-301 Malignant Mesothelioma Diagnosed by Bronchoscopic Biopsy Yeon-Hee Park,
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
How To Treat A Cancer With A Radical
 Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Survey of Mesothelioma Associated with Asbestos Exposure in Japan
 The research and development and the dissemination projects related to the 13 fields of occupational injuries and illnesses Survey of Mesothelioma Associated with Asbestos Exposure in Japan Clinical characteristics
The research and development and the dissemination projects related to the 13 fields of occupational injuries and illnesses Survey of Mesothelioma Associated with Asbestos Exposure in Japan Clinical characteristics
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3
 ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
Sternotomy and removal of the tumor
 Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma
 Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
CHAPTER 2. Neoplasms (C00-D49) March 2014. 2014 MVP Health Care, Inc.
 Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Diseases. Inflammations Non-inflammatory pleural effusions Pneumothorax Tumours
 Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Malignant Mesothelioma
 Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Mesothelioma
 Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
An Update on Lung Cancer Diagnosis
 An Update on Lung Cancer Diagnosis Dr Michael Fanning MBBS FRACGP FRACP RESPIRATORY AND SLEEP PHYSICIAN Mater Medical Centre Outline Risk factors for lung cancer Screening for lung cancer Radiologic follow-up
An Update on Lung Cancer Diagnosis Dr Michael Fanning MBBS FRACGP FRACP RESPIRATORY AND SLEEP PHYSICIAN Mater Medical Centre Outline Risk factors for lung cancer Screening for lung cancer Radiologic follow-up
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
Understanding Your Surgical Options for Lung Cancer
 Information Booklet for Patients Understanding Your Surgical Options for Lung Cancer Understanding Lung Cancer If you have just been diagnosed with lung cancer, this booklet will serve as an informational
Information Booklet for Patients Understanding Your Surgical Options for Lung Cancer Understanding Lung Cancer If you have just been diagnosed with lung cancer, this booklet will serve as an informational
Summary of treatment benefits
 Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT
 TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT Introduction : ETB 15-20% Pleural effusion 20% in non HIV Under reporting because of AFB negative in fluid In HIV patients: EPTB 20% PTB + EPTB 50% Pleural Effusion
TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT Introduction : ETB 15-20% Pleural effusion 20% in non HIV Under reporting because of AFB negative in fluid In HIV patients: EPTB 20% PTB + EPTB 50% Pleural Effusion
HEALTH CARE FOR EXPOSURE TO ASBESTOS. 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.
 HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
Lung cancer case study
 Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Principal Investigator: Valerie W. Rusch, MD, FACS, Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Lung Cancer Center: How to Achieve JCI
 07/30/55 1 Lung Cancer Center: How to Achieve JCI Prof. Emeritus Sawang Saenghirunvattana M.D Copyright 2012 07/30/55 2 Technology TECHNOLOGY ROADMAP Emphasis valve EBUS GS AUTOFLUORESCENSE Virtual Bronchoscopy
07/30/55 1 Lung Cancer Center: How to Achieve JCI Prof. Emeritus Sawang Saenghirunvattana M.D Copyright 2012 07/30/55 2 Technology TECHNOLOGY ROADMAP Emphasis valve EBUS GS AUTOFLUORESCENSE Virtual Bronchoscopy
The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options
 Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
YOUR LUNG CANCER PATHOLOGY REPORT
 UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
EPEC -O. Education In Palliative And End-Of-Life Care For Oncology. Self-Study Module 3m: Symptoms; Malignant Pleural Effusions
 EPEC -O Education In Palliative And End-Of-Life Care For Oncology Self-Study Module 3m: Symptoms; Malignant Pleural Effusions Module 3m: Symptoms; Malignant Pleural Effusions Abstract... 3 Introduction...
EPEC -O Education In Palliative And End-Of-Life Care For Oncology Self-Study Module 3m: Symptoms; Malignant Pleural Effusions Module 3m: Symptoms; Malignant Pleural Effusions Abstract... 3 Introduction...
Malignant Pleural Effusions. Introduction. Further Reading. Etiology. Abstract
 372 PLEURAL EFFUSIONS / Malignant Pleural Effusions Further Reading Antony VB and Mohammed KA (1999) Pathophysiology of pleural space infections. Seminars in Respiratory Infections 14(1): 9 17. Colice
372 PLEURAL EFFUSIONS / Malignant Pleural Effusions Further Reading Antony VB and Mohammed KA (1999) Pathophysiology of pleural space infections. Seminars in Respiratory Infections 14(1): 9 17. Colice
Pre-workshop exercise
 Setting research priorities for mesothelioma workshop 10 th November 2014 Pre-workshop exercise Your individual ranking of unanswered questions about the diagnosis, treatment and care of mesothelioma Please
Setting research priorities for mesothelioma workshop 10 th November 2014 Pre-workshop exercise Your individual ranking of unanswered questions about the diagnosis, treatment and care of mesothelioma Please
What is Mesothelioma?
 What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
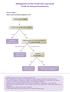 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Treatment of mesothelioma in Bloemfontein, South Africa
 European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement during Initial Diagnosis
 Case Reports in Pulmonology Volume 2015, Article ID 962504, 4 pages http://dx.doi.org/10.1155/2015/962504 Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement
Case Reports in Pulmonology Volume 2015, Article ID 962504, 4 pages http://dx.doi.org/10.1155/2015/962504 Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement
Surgery. Wedge resection only part of the lung, not. not a lobe, is removed. Cancer Council NSW
 The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Lung cancer. A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment
 Lung cancer A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment Contents Contents 2 3 Section 1: Lung Cancer 4 i. Types of lung cancer 4 ii. Causes and risk factors 5 iii. Symptoms
Lung cancer A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment Contents Contents 2 3 Section 1: Lung Cancer 4 i. Types of lung cancer 4 ii. Causes and risk factors 5 iii. Symptoms
Asbestos Related Diseases
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Lung Cancer Understanding your diagnosis
 Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount of information
Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount of information
Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too.
 Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer
 Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer Version History Version Date Summary of Change/Process 0.1 09.01.11
Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer Version History Version Date Summary of Change/Process 0.1 09.01.11
Occupational respiratory diseases due to Asbestos. Dirk Dahmann, IGF, Bochum
 Occupational respiratory diseases due to Asbestos Dirk Dahmann, IGF, Bochum Contents Introduction Diseases Further Effects Preventive Strategies Conclusion Asbestos minerals Woitowitz, 2003 Imports (+
Occupational respiratory diseases due to Asbestos Dirk Dahmann, IGF, Bochum Contents Introduction Diseases Further Effects Preventive Strategies Conclusion Asbestos minerals Woitowitz, 2003 Imports (+
Asbestos and your lungs
 This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium
 Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Rare Thoracic Tumours
 Rare Thoracic Tumours 1. Epithelial Tumour of Trachea 1 1.1 General Results Table 1. Epithelial Tumours of Trachea: Incidence, Trends, Survival Flemish Region 2001-2010 Both Sexes Incidence Trend EAPC
Rare Thoracic Tumours 1. Epithelial Tumour of Trachea 1 1.1 General Results Table 1. Epithelial Tumours of Trachea: Incidence, Trends, Survival Flemish Region 2001-2010 Both Sexes Incidence Trend EAPC
Case Report Pleural Mesothelioma Presenting as Periumbilical Metastasis: The First Clinical Documentation
 Volume 2013, Article ID 198729, 4 pages http://dx.doi.org/10.1155/2013/198729 Case Report Pleural Mesothelioma Presenting as Periumbilical Metastasis: The First Clinical Documentation R. F. Falkenstern-Ge,
Volume 2013, Article ID 198729, 4 pages http://dx.doi.org/10.1155/2013/198729 Case Report Pleural Mesothelioma Presenting as Periumbilical Metastasis: The First Clinical Documentation R. F. Falkenstern-Ge,
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
J of Evidence Based Med & Hlthcare, pissn- 2349-2562, eissn- 2349-2570/ Vol. 2/Issue 33/Aug. 17, 2015 Page 5063
 PERITONEAL MALIGNANT MESOTHELIOMA: A RARE S. R. Dhamotharan 1, S. Shanthi Nirmala 2, F. Celine Foustina Mary 3, M. Arul Raj Kumar 4, R. Vinothprabhu 5 HOW TO CITE THIS ARTICLE: S. R. Dhamotharan, S. Shanthi
PERITONEAL MALIGNANT MESOTHELIOMA: A RARE S. R. Dhamotharan 1, S. Shanthi Nirmala 2, F. Celine Foustina Mary 3, M. Arul Raj Kumar 4, R. Vinothprabhu 5 HOW TO CITE THIS ARTICLE: S. R. Dhamotharan, S. Shanthi
Linfoma maligno pulmonar tratado com Nerium oleander. http://www.drozel.org/eng/diagnosis_malignant_mg.htm CASE REPORT
 Linfoma maligno pulmonar tratado com Nerium oleander http://www.drozel.org/eng/diagnosis_malignant_mg.htm CASE REPORT Diagnosis: Malignant lymphoma, lung cancer A 60-year-old woman experienced pain in
Linfoma maligno pulmonar tratado com Nerium oleander http://www.drozel.org/eng/diagnosis_malignant_mg.htm CASE REPORT Diagnosis: Malignant lymphoma, lung cancer A 60-year-old woman experienced pain in
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
Post-operative intrapleural chemotherapy for mesothelioma
 Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
Malignant Mesothelioma
 Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT
 GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT 1) TOPIC OF THE EVENT MALIGNANT PLEURAL DISEASE 2) SUGGESTED TITLE : Approach to Pleural Cancer: State-of-the-Art 3) TYPE OF EVENT Course Native
GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT 1) TOPIC OF THE EVENT MALIGNANT PLEURAL DISEASE 2) SUGGESTED TITLE : Approach to Pleural Cancer: State-of-the-Art 3) TYPE OF EVENT Course Native
Screening, early referral and treatment for asbestos related cancer
 Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Aggressive lymphomas. Michael Crump Princess Margaret Hospital
 Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
THYROID CANCER. I. Introduction
 THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
Malignant Mesothelioma
 Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD
 SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Patterns of nodal spread in thoracic malignancies
 Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
American Thoracic Society
 American Thoracic Society Management of Malignant Pleural Effusions THIS OFFICIAL STATEMENT OF THE AMERICAN THORACIC SOCIETY WAS ADOPTED BY THE ATS BOARD OF DIRECTORS, MARCH 2000 CONTENTS Incidence Etiology
American Thoracic Society Management of Malignant Pleural Effusions THIS OFFICIAL STATEMENT OF THE AMERICAN THORACIC SOCIETY WAS ADOPTED BY THE ATS BOARD OF DIRECTORS, MARCH 2000 CONTENTS Incidence Etiology
Thoracoscopy in Pleural Malignant Mesothelioma
 Diagnostic and Therapeutic Endoscopy, 1997, Vol. 3, pp. 147-151 Reprints available directly from the publisher Photocopying permitted by license only (C) 1997 OPA (Overseas Publishers Association) Amsterdam
Diagnostic and Therapeutic Endoscopy, 1997, Vol. 3, pp. 147-151 Reprints available directly from the publisher Photocopying permitted by license only (C) 1997 OPA (Overseas Publishers Association) Amsterdam
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 171/08
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 171/08 BEFORE: M.F. Keil : Vice-Chair M. Christie: Member Representative of Employers M. Ferrari: Member Representative of Workers HEARING:
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 171/08 BEFORE: M.F. Keil : Vice-Chair M. Christie: Member Representative of Employers M. Ferrari: Member Representative of Workers HEARING:
This factsheet aims to outline the characteristics of some rare lung cancers, and highlight where each type of lung cancer may be different.
 There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
