Managing the Developing Occlusion. A guide for dental practitioners
|
|
|
- Howard Holland
- 9 years ago
- Views:
Transcription
1 Managing the Developing Occlusion A guide for dental practitioners
2 INTRODUCTION Whether knowingly or not, every dentist who treats children practices orthodontics. It is not enough to think of orthodontics as being solely concerned with appliances. Orthodontics is the longitudinal care of the developing occlusion and any problems associated with it. All qualified dental practitioners should be encouraged to consider the orthodontic requirements of their patients. This booklet is designed to help general dental practitioners examine children from an orthodontic viewpoint. It will highlight the assessment of patients at different stages of dental development and will outline the interceptive procedures and treatments available to deal with the conditions most commonly encountered. Before specific assessment and treatments are considered, a general view of the developing dentition and face is advisable. This should rely on common sense as well as experience and ability. ORTHODONTIC ADVICE First, when considering potential orthodontic advice for the patient, the dental practitioner should consider the following general questions: 1. Is the patient s basic dental health under control and is the parent available for consultation? 2. Is the orthodontic condition minor, moderate or severe in nature and does it cause the patient concern? 3. Can the practitioner provide adequate advice in the short, medium and long term, or is specialist advice required and, if so, at what level? 4. Would the patient and parent prefer a specialist opinion? TREATMENT Secondly, when considering potential orthodontic treatment for patients, the dental practitioner should consider the following general questions: 1. Does the patient want the condition changed? 2. Is the patient receptive to the idea of, and available for, orthodontic treatment? 3. Is specialist treatment required and, if so, at what level? ADVICE Following these general questions, the newly qualified dental practitioner may feel that further advice is required. This may be available from the following sources: 1. The Dental Practice Principal The principal may have a particular interest in orthodontic therapy or, failing this, should be able to advise on the orthodontic facilities that are available in the local area. 2. An Orthodontic Specialist Practitioner Orthodontic specialists in practice have usually undergone a formal postgraduate course of training leading to a higher qualification in orthodontics (M.Orth or D.Orth). The primary function of a specialist is to offer treatment but advice will also be available for general dental practitioners. 2
3 INTRODUCTION 3. A Community Orthodontist Community orthodontists have undergone a formal postgraduate course of training leading to a higher qualification in orthodontics (M.Orth or D.Orth). Community orthodontists are salaried specialists who work in the community dental clinics and, in some districts, only treat community service patients. In other districts, referral for treatment from general dental practitioners are accepted. Again, the emphasis is likely to be on the provision of treatment rather than delegated treatment planning. 4. A Consultant Orthodontist Consultant orthodontists have completed a formal course of training leading to a higher qualification in orthodontics (M.Orth or D.Orth) and have also undergone an additional period of higher specialist training. Consultant orthodontists are trained to provide a full diagnostic, treatment planning and advice service for general dental practitioners. Hospital consultant orthodontists are likely to limit the type of treatment available in their departments to patients with more severe orthodontic problems. As a result, they may delegate suitable treatment plans to any of the above mentioned colleagues. REFERRAL LETTERS The preferred method of communication between practitioner and orthodontic specialist is by referral letter or a specific proforma. Many PCTs/ LHBs have brought in their own standardised referral proforma which all local practitioners are required to use. This letter should include the following basic information: 1. Patient s full name; surname and first names. Which is which should be clearly identified. 2. Patient s address including the postcode. The postcode identifies patients who cross district health boundaries for treatment. This enables the provider unit to be reimbursed by the Primary Care Trust or Local Health Board in which the patient is resident. Most patient administration systems (PAS) will not accept a referral without the postcode. 3. Patient s date of birth. 4. Patient s telephone number. This will enable the specialist to contact the patient at short notice. 6. Any reference (coded at the top of letter) from previous correspondence. This immediately identifies the patient as having had a previous assessment and ensures their notes are retrieved rapidly and the appropriate action taken. 7. The letter should contain the specific reason for the referral. A concise and relevant medical, dental and social history should be included along with the patient s main cause for concern and their likely co-operation with an anticipated treatment plan and orthodontic appliances. 8. Ideally, the patient should be dentally fit and caries-free with excellent oral hygiene and periodontal condition. This is a basic requirement that should be met before an orthodontic referral is made. However, on occasions, early advice can be sought first from an orthodontic specialist regarding the likely need for extractions in patients with carious teeth of dubious long-term prognosis. In addition, any recent radiographs of the patient (e.g. bitewings, periapicals, OPT) that pertain to the reason for referral should be sent along with the referral letter. 9. A copy of the referral letter should be kept in the patient s notes. It is worth emphasising to the patient and parent that the orthodontic specialist will only provide an assessment at the first appointment. Many patients expect more! Dentistry is a small profession and practitioners can sometimes become isolated. It is both professional and sociable for new practitioners to introduce themselves to the orthodontic specialists in the local area and vice versa. This will enable a discussion to take place on the services available and to clarify such points as the range of treatments available, costs and relevant waiting lists. Many areas are developing Managed Clinical Networks (MCNs) locally to ensure good communication between all orthodontic providers and their referring practitioners. With this information you should be able to refer patients to the appropriate specialist with some idea of what to expect. Communication is enhanced if the practitioner and orthodontic specialist have been previously acquainted. 5. Patient s general medical practitioner. This information is needed to register the patient in the case of hospital referrals - again a PAS requirement. 3
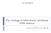
4 MANAGING THE 1. A supplemental B in the deciduous dentition is to be succeeded by a supplemental 2. 1 DECIDUOUS TO MIXED DENTITION The general dental practitioner is responsible for recognising any deviations from normal in the dental development of his/her child patient. The recognition of abnormality is the first important stage in providing treatment to rectify the situation and requires an understanding of normal dental development. Spacing is normal between the anterior teeth in the deciduous dentition. These spaces occur most frequently mesial to the upper canine and distal to the lower canine, the so-called primate spaces. Generalised anterior spacing can be present from the time of eruption of the deciduous teeth, but tends to increase with growth of the alveolus. Lack of spacing in the deciduous dentition may be a cause for concern, since crowding of the permanent dentition is a likely sequel. The deciduous dentition is a time for observation. Characteristics of the deciduous dentition are reproduced or amplified in the permanent dentition. Small overjets become larger whilst reverse overjets and cross-bites invariably reappear in the permanent dentition. However, it is very seldom that any active treatment is indicated for a child in the deciduous dentition. Supernumerary teeth occur in the deciduous dentition but nearly always erupt and require no intervention. They are followed by extra teeth in the same location in the permanent dentition in 35-50% of cases. THE TRANSITION FROM DECIDUOUS TO MIXED DENTITION The transition from the deciduous to the mixed dentition begins at around the age of six with the eruption of the lower central incisors (Table 1). 1 Normal Eruption Sequence Ages TABLE 1. Transition from the deciduous to mixed dentition begins around the age of six years with the eruption of the lower central incisors. The permanent teeth erupt in groups with two main periods of activity. The first occurs between the dental ages of 6 and 8 years when the permanent incisors and first permanent molars erupt; the second between the ages 11 and 12 when permanent canines, premolars and second molars erupt. It should be remembered, however, that the dental age of a patient may differ quite widely from their chronological age and a generalised delay in eruption may be of no consequence. A change in the sequence of eruption or an asymmetrical eruption pattern may indicate a possible abnormality and should be investigated further both clinically and radiographically. Of the first group of permanent teeth to erupt, the most likely to go astray is the upper central incisor. The permanent incisors and canines are usually larger than the corresponding deciduous teeth, whereas the premolars are smaller (leeway space). The combined mesio-distal widths of the upper permanent teeth are about 3mm greater than the deciduous teeth; the lower permanent teeth are about 1mm larger than their deciduous predecessors. The extra size of the permanent teeth is accommodated in three ways: i) Spacing of the deciduous dentition. ii) Growth of the alveolus. iii) The eruptive path of the upper incisors The increase in width of the dental arches occurs predominantly in two phases, the first being at the stage of eruption of the permanent incisors and then later with the eruption of the permanent canines. The upper incisors erupt into a slightly 4
5 M A N A G I N G T H E more proclined (forward) position than their deciduous counterparts. This is responsible for some of the increase in dental arch length. Delayed eruption of one or more of the incisors may lead to space loss. In the presence of crowding, the adjacent teeth tend to drift into the space required for the unerupted teeth. In the majority of children, the permanent incisors erupt into mildly crowded positions and anxious parents first become aware of crooked teeth. Their alignment frequently improves with subsequent alveolar growth. Reassurance may be all that is required at this stage. There are other aspects of normal development that can occur in some individuals: i) More severe lower incisor imbrication may improve following the exfoliation of the deciduous canines (see later); in most cases it is too early to consider the extraction of deciduous canines. ii) The "Ugly Duckling" stage: described as "a fanning out of the crowns of the upper permanent incisors, particularly the lateral incisors, sometimes with a median diastema". It is caused by the position and convergence of their roots prior to the eruption of the permanent canines. The spacing usually closes spontaneously following eruption of the canines. It is important for the general dental practitioner to recognise these characteristics of normal development so that the patient and their parents can be reassured. It is important to differentiate between a median diastema associated with the ugly duckling stage and other possible causes of median diastema (listed below). These may prompt further investigations: i) Family/racial characteristic ii) Unerupted supernumeraries iii) Basal narrowness of maxilla iv) Small teeth, large jaws v) Developmentally (congenitally) missing 22 vi) Misplaced 22 due to crowding vii) Peg-shaped 22 viii) Proclination of ix) Abnormal fraenum An asymmetrical eruption pattern should prompt further investigations. An occlusal or periapical X-ray of BA will usually indicate the reason for the delayed eruption of Failure of eruption can be due to a number of causes. The most common is the presence of an unerupted supernumerary tooth. These are not always easily visible on radiographs. 4 & 5. In the presence of crowding, delayed eruption results in space loss. Although CA AC have been removed, together with the unerupted supernumeraries related to 1 1, these teeth are unlikely to erupt until space has been regained with appliance therapy. 5 5
6 MANAGING THE 6. The non-vital A has been retained, 2 has erupted in advance of 1 and space has been lost. The extraction of A alone will not rectify the situation. 1. Investigate causes of delayed eruption e.g. supernumerary and remedy, i.e. remove. 2. Recreate space for Surgical exposure in combination with the placing of an orthodontic bracket and traction may be needed to encourage some less favourable teeth to erupt. An early orthodontic assessment, around the period of eruption of the permanent incisors, is a useful exercise as a number of simple interceptive measures are available to the orthodontist, which could significantly reduce the later complexity of many developing malocclusions. A radiographic examination may be considered if the occlusion appears not to be developing normally. Early orthodontic assessment is used to monitor: 1. Normal eruption of permanent incisors and first permanent molars and to investigate causes of failure of eruption. A tooth will normally erupt within six months of its contra-lateral number. 2. Presence of malocclusion i) Crowding of incisors ii) Significant displacement of incisors labially or lingually (incisors inside the bite) iii) Posterior crossbites iv) Coincidence of upper and lower centre lines v) Severe skeletal discrepancies especially Class II cases; these may be suitable for functional appliance treatment in the late mixed or early permanent dentition. 3. Long term prognosis of first permanent molars 4. Trauma to permanent incisors 5. Persistent thumb or finger sucking habits The occlusion is in a relatively dynamic state throughout the mixed dentition. Premature loss of deciduous teeth may cause shifts of centre lines and molar relationships, which are responsible for the development of many localised problems. 6 The plasticity of the occlusion can, however, be used to our advantage. Centre line shifts, caused by deciduous tooth loss, can be corrected by the extraction of the contra-lateral deciduous tooth. Indeed, most of the available interceptive measures rely on space availability and drifting. The aim at this stage of dental development, around the age of 8 ½ years, is to achieve the complete eruption of upper and lower permanent incisors, in reasonable alignment, with coincident centre lines. Further details on the management of unerupted upper incisors are available in the form of published national clinical guidelines on the Faculty of Dental Surgery (Eng.) website at: POSSIBLE INTERCEPTIVE MEASURES Interceptive treatment is often the first stage of a more complex treatment plan. The aim is to aid the development of an ideal occlusion and minimise any deviation from normal. Inappropriate intervention may, in fact, complicate matters, especially if excessive space loss has been allowed to occur. If in any doubt, seek further advice. 1. Extract deciduous teeth displacing their permanent successors. 2. Balance the loss of one deciduous canine with the extraction of the contra-lateral tooth to prevent the centre line shifting to the side of the missing tooth. 3. Observe the effects on centre lines of the loss of first deciduous molars. Consider extracting the contra-lateral deciduous canine if this occurs. 4. Appliances to discourage thumb sucking at this stage are found to be less valuable than gentle dissuasion, encouragement and advice. POSSIBLE TREATMENT MEASURES 1. Surgical removal of supernumerary teeth related to unerupted incisors. Refer to an orthodontist for assessment of eruption sequence and space availability. 2. Appliance therapy to correct: i) incisors in crossbite ii) unilateral buccal crossbite causing displacement iii) to recreate space for unerupted incisors Space maintainers at this stage are seldom indicated. The best space maintainer is the patient s own deciduous dentition! Upper second deciduous molars should be preserved, whenever possible, to prevent mesial movement of 6 6 and loss of arch length.
7 MANAGING THE WHAT TO REFER FOR SPECIALIST ADVICE OR TREATMENT The types of problems that specialists would prefer to see early (i.e. at 7-9 years of age), rather than late, are listed below: 1. Delayed eruption of permanent incisors, whether or not related to supernumerary teeth. Always refer to an orthodontic professional. 2. Supplemental incisors - if you are unsure which tooth to extract. 3. Developmental (congenital) absence: commonly affects lower central and upper lateral incisors and second premolars. Consideration must be given to the eventual position of the upper canines, if lateral incisors are absent. 4. One or more upper incisors in crossbite. This may indicate a developing Class III jaw relationship which would benefit from early orthopaedic treatment. 5. Impaction or failure of complete eruption of one or more first permanent molars. 6. Severe crowding. 7. Severe skeletal discrepancies - especially Class II (small lower jaw) and Class III (small upper jaw) children , 9 & 10. Retained or submerged deciduous teeth, severe crowding and teeth of abnormal form, may prompt referral for specialist advice. 2 LATE MIXED DENTITION As discussed on page 4, the permanent teeth erupt in groups with two main periods of activity. The second phase occurs between ages 11 and 12 when the canines, premolars and second molars erupt. This second period of eruptive activity provides another opportunity for taking interceptive measures designed to reduce the severity of a developing malocclusion. THE NORMAL TRANSITION FROM MIXED TO PERMANENT DENTITION In contrast to the anterior teeth, the premolars are smaller than their deciduous predecessors. The resultant leeway space of about 2.5mm on each side of the lower arch and 1.5mm in the upper arch, is usually spontaneously taken up by the forward movement (mesial drift) of the first permanent molars. The deciduous molars normally meet cusp-to-cusp. Greater forward movement of the lower first permanent molar and differential mandibular growth in this period result in the development of the Class I molar occlusion of the permanent dentition. The late mixed dentition is characterised by the eruption of two further groups of teeth as illustrated in the eruption chart (Table 1- page 4). The lower canines and upper and lower first premolars all erupt more or less together at a dental age of 11 years. Dental age and chronological age correlate only moderately well and greater attention should be taken of the sequence of eruption as opposed to the timing. It is useful to remember when assessing dental age and development that permanent teeth usually erupt when three-quarters of their roots are complete. VARIATIONS FROM NORMAL DEVELOPMENT Crowding is the most common cause of variation from the norm. It often first manifests itself with the eruption of the incisors. The upper central incisors frequently erupt normally, leaving insufficient space for the lateral incisors, which subsequently erupt in displaced positions. They may be displaced palatally, so reflecting their developmental positions, or labially or rotated within the line of the dental arch. The last tooth of a group of teeth to erupt is often the one most affected by crowding. Consequently, in the late mixed dentition, the permanent canines or second premolars are the most frequently affected teeth. These teeth may be displaced palatally or buccally or simply fail to erupt altogether due to a shortage of space and subsequent impaction. 10 7
8 MANAGING THE 11. Retained, non-vital deciduous teeth frequently cause their permanent successors to be displaced. 12. The favourable unerupted canine can usually be seen or palpated buccally. 13. The assessment of unerupted canines can be difficult. Seek further advice as necessary OTHER CAUSES OF DELAYED ERUPTION OF PERMANENT TEETH 1. Abnormal developmental position 2. Presence of supernumerary teeth or odontomes 3. Trauma to deciduous teeth causing: i) Ankylosis ii) Displacement of permanent teeth iii) Dilaceration 4. Retained deciduous teeth 5. Impaction 6. Eruption cysts THE ECTOPIC PERMANENT CANINE Of the group of permanent teeth erupting during the late mixed dentition stage, the upper permanent canine is the most likely to stray from its normal eruptive path. The incidence of an ectopic maxillary canine is 1-2% of the population. Of these, 85% are displaced palatally. If ectopic eruption is suspected, early localisation using clinical (palpation) and radiographic methods is recommended so that interceptive measures to encourage eruption can be instituted as soon as possible. Should these fail, time must be available for alternative treatment options. The later an ectopic canine is spotted, the less likely it is that treatment will be successfully completed Do not leave it this late! The attrition to C and the over eruption of 3, together with the lack of space for the unerupted 3 make this a difficult problem to correct. The appearance of the retained deciduous tooth, its root morphology and its occlusion with opposing teeth, all require regular assessment at dental check-up appointments Parallax technique Two radiographs taken with a shift in the cone position between the two views i.e. OPG and upper anterior occlusal (vertical parallax) or two periapical views (horizontal parallax). As the cone shifts between the two views, the ectopic tooth will change its position in relation to the adjacent teeth. If the ectopic tooth moves in the same direction as the tube shift, then the tooth is palatally displaced. It is important to assess the position of the unerupted canine early (before 11 years of age), since the simple extraction of the deciduous canine tooth may result in a significant spontaneous improvement in the position of the majority of palatally displaced canines. Fortunately, ectopically displaced canines are frequently unilateral, resulting in an identifiable asymmetry on manual palpation. The favourable canine is usually palpable buccal to the resorbing deciduous tooth by the age of The angulation of the crowns of the adjacent teeth (especially the lateral incisor) also helps to localise the unerupted canine.
9 MANAGING THE The incidence of ectopic maxillary canines increases markedly in the presence of any abnormality of the lateral incisor. 5% of ectopic canines are associated with an absent lateral incisor, whereas 11.5% are associated with a peg-shaped tooth. 48% of palatally displaced canines are related to anomalous lateral incisors. Clinical and radiographic indications for intervention include: i) Permanent canine not palpable in labial sulcus by age 10. ii) Deciduous canine root resorption not progressing. iii) Radiographs indicate ectopic position or damage to adjacent teeth. iv) Canine crown overlaps the most distal incisor root. v) Enlargement of canine follicle. If you suspect an ectopic canine, refer to an appropriate orthodontic professional. Published national clinical guidelines on this topic are available from the Faculty of Dental Surgery (Eng.) website at: v) Unilateral extraction of Cs and Ds is likely to cause a shift of the centre line; this tendency is greater in the lower arch than the upper. The loss of a deciduous canine on one side should be balanced by the extraction of the contra-lateral tooth, so as: i) to prevent centre line shifts and ii) to allow spontaneous alignment of the incisors. There is no justification for balancing the extraction of second deciduous molars when one or more have to be lost. This would lead to space being lost in the buccal segments to no advantage. POOR QUALITY FIRST PERMANENT MOLARS The first permanent molar continues to be the most caries prone member of the permanent dentition. Its early loss or poor long-term prognosis frequently complicates orthodontic treatment planning. THE RESULTS OF EARLY LOSS OF DECIDUOUS TEETH Space loss resulting from the early extraction of deciduous teeth is usually attributed to mesial drift of the molars. However, in the canine region, it can also be due to distal drift of anterior teeth. Most space loss occurs after extraction of the deciduous teeth, markedly so in the case of second deciduous molars. The consequences of early loss are summarised below: 1. In cases where crowding is absent, early loss of deciduous teeth will have little or no effect on the permanent dentition. 2. Where crowding is present: i) Space loss is always greater in the upper arch than the lower. ii) Loss of second deciduous molars leads to a greater loss of space than loss of the first deciduous molars. iii) Very early loss of second deciduous molars, before the eruption of the first permanent molars, can lead to almost complete loss of the second premolar space. iv) Extractions after the age of 10 can cause relatively little space loss. 15. Early loss of second deciduous molars has resulted in severe space loss. First molars have tilted mesially. Although past the optimum age for extraction of first molars, their loss, due to poor quality, will provide the space where it is needed When assessing the prognosis of first permanent molars, remember to also look at the buccal surfaces of upper and the lingual surfaces of lower molars, which are caries prone areas. 9
10 MANAGING THE 17 & 18. Extraction of deciduous canines. Age 8 years 6 months. Lower 2 2 erupted and rotated. 2 2 unerupted and short of space. All deciduous canines extracted. 19 & 20. Extraction of deciduous canines. Age 9 years 6 months. Incisor alignment much improved one year later If more than one of the first permanent molars has a doubtful prognosis, then extraction of all four first molars may be indicated. Optimal space closure occurs when the timing of these extractions is carefully managed and the advice of a specialist should be sought. The best results are achieved if the following combination of factors co-exists at the time of extractions: 1. Chronological Age. Best results are achieved at around the age of 9 and 10 years. 2. Dental Age. Lateral incisors and first premolars should have erupted but not the remaining buccal teeth. Calcification of the bifurcation of the roots of the second permanent molars should have just commenced. 3. Radiographic examination must be carried out to confirm the presence of successional teeth. 4. Crowding should be present. Ideally, the crowding should be located in the buccal segments, as the extraction of first molars does little to relieve anterior crowding. As active orthodontic treatment is required to relieve anterior crowding or reduce an increased overjet, it may be better to retain the upper first molars until the start of active treatment so that no useful space is lost. Where the extraction of a single first permanent molar has been necessary, advice regarding the status of the remaining first molars should be sought. Further information on this topic is available from the National Clinical Guidelines section of the Faculty of Dental Surgery (Eng.) website at: 19 THE EXTRACTION OF ALL DECIDUOUS CANINES It is not uncommon to extract all four deciduous canines in the following circumstances: 1. To provide space so that a crowded but unerupted maxillary lateral incisor may erupt without being deflected into lingual occlusion. Once a positive overbite has been obtained, such teeth will not correct spontaneously even when space is made available. Early intervention is therefore crucial. 2. To provide space for crowded maxillary incisors, which are already in lingual occlusion, to be corrected in the early mixed dentition To provide space for severely crowded lower incisors to align spontaneously - if the crowding is more of a displacement than a rotation, and the lateral incisors are less than half erupted. 4. To ensure that incisors delayed by the presence
11 MANAGING THE of a supernumerary tooth have sufficient space to allow their full eruption. 5. To encourage a palatally ectopic maxillary canine to erupt. SERIAL EXTRACTION The full serial extraction procedure is seldom recommended these days since the prospect of having 12 teeth extracted must be daunting to any child. However, all first premolars can be extracted as the permanent canines emerge in order to provide sufficient space for them to erupt in the line of the arch. It is particularly important to check that the upper canines are favourably placed (i.e. mesially inclined and buccally positioned). The premolars should not be extracted too early as undue space loss may occur. Driftodontics is the term used to describe the judiciously timed removal of teeth to enable some spontaneous improvement in the eruption and alignment of the permanent dentition to occur. It may avoid, minimize or simplify the need for future active orthodontic treatment. In some crowded Class I cases, it may be prudent to extract the fully erupted first premolars to allow sufficient space for the canines and second premolars to erupt into the line of the arch. Always seek orthodontic advice first before proceeding. GENERAL ANAESTHETICS The extraction of deciduous teeth for orthodontic purposes seldom justifies a general anaesthetic (Poswillo recommendations). If a child will not accept extractions under local anaesthetic, they should be referred for a specialist paediatric dental opinion. It may be better to avoid extractions rather than expose the child to the risk of a general anaesthetic. POSSIBLE INTERCEPTIVE MEASURES The permanent teeth erupt into a dynamic and changing environment. During the period of eruption, changes occur as a result of skeletal growth, premature tooth contacts, sucking habits and soft tissue adaptations. It may be possible to influence some of these factors by interceptive measures. Remember to confirm the presence of all permanent teeth before any extractions are carried out Extraction of deciduous canines. Age 10 years 6 months. Incisors well aligned and crowding transferred to the buccal segments. This patient will probably require orthodontic therapy and permanent extractions in due course. 1. Extraction of deciduous teeth. i) To relieve significant incisor crowding. ii) To prevent or improve centre line problems. iii) If the permanent successor is being displaced. 2. Active treatment i) To correct incisors in crossbite. ii) Early correction of buccal crossbite. WHAT TO REFER FOR SPECIALIST ADVICE OR TREATMENT There are numerous anomalies occurring in the mixed dentition, which should be referred early (i.e. at 7-9 years of age) for specialist advice. These include the following: 1. Severe skeletal problems where early treatment may be appropriate - particularly developing Class III (small upper jaw) children. 2. Unfavourably positioned canines or other teeth. 3. Developmentally missing (congenitally absent) permanent teeth. 4. Poor quality first permanent molars or other teeth of poor prognosis where timing of extractions may simplify subsequent treatment. The Index of Orthodontic Treatment Need (IOTN) is an internationally used measure to assess the need and eligibility of patients for NHS orthodontic treatment. There are two components to this index: i) Dental Health Component (DHC) grades 1 to 5 see Table 2 ii) Aesthetic Component (AC) - graded 1 to 10. The Aesthetic Component is a scale of 10 colour photographs showing different levels of dental attractiveness. The general dental practitioner should choose one of the photographs which he or she feels best grades (matches) the malocclusion of the child being assessed. It can also be used as a counselling tool with patients with mild problems to see where 11
12 Managing the developing occlusion TABLE 2. The Dental Health Component of the Index of Orthodontic Treatment Need they think they fit on the scale. Currently, to be eligible for NHS treatment a patient must score a minimum DHC score of 3 along with an AC grading of 6 or above. 3 EARLY PERMANENT DENTITION The early permanent dentition is the best time to carry out treatment for the majority of patients. There are obvious social advantages at this age. The alveolar bone is readily remodeled during periods of active growth. This facilitates the tooth movements produced by orthodontic appliances. This is the ideal time for a full orthodontic assessment to be carried out in order to determine whether active orthodontic treatment is indicated. ORTHODONTIC ASSESSMENT Severe malocclusions are obvious even to the untrained eye. Less severe problems may not be so readily apparent, but they may be just as difficult to treat. A system for the clinical assessment of malocclusion needs to be simple yet methodical to ensure that all abnormalities are noted. The following sequential examination is recommended: 1. Lower labial segment - check for alignment and crowding. 2. Upper labial segment. Note the presence and position of all anterior teeth and the inclination of the incisors. 12 GRADE 5 (Need treatment) 5.i Impeded eruption of teeth (except for third molars) due to crowding, displacement, the presence of supernumerary teeth, retained deciduous teeth and any pathological cause. 5.h Extensive hypodontia with restorative implications (more that 1 tooth missing in any quadrant) requiring prerestorative orthodontics. 5.a Increased overjet greater than 9mm. 5.m Reverse overjet greater than 3.5min with reported masticatory and speech difficulties. 5.p Defects of cleft lip and palate and other craniofacial anomalies. 5.s Submerged deciduous teeth. GRADE 4 (Need treatment) 4.h Less extensive hypodontia requiring pre-restorative orthodontics or orthodontic space closure to obviate the need for a prosthesis. 4.a Increased overjet greater than 6mm but less than or equal to 9mm. 4.b Reverse overjet greater than 3.5mm with no masticatory or speech difficulties. 4.m Reverse overjet greater than 1mm but less than 3.5mm with recorded masticatory and speech difficulties. 4.c Anterior or posterior crossbites with greater than 2mm discrepancy between retruded contact position and intercuspal position. 4.l Posterior lingual crossbite with no functional occlusal contact in one or both buccal segments. 4.d Severe contact point displacements greater than 4mm. 4.e Extreme lateral or anterior open bites greater than 4mm. 4.f Increased and complete overbite with gingival or palatal trauma. 4.t Partially erupted teeth, tipped and impacted against adjacent teeth. 4.x Presence of supernumerary teeth. GRADE 3 (Borderline need) 3.a Increased overjet greater than 3.5mm but less than or equal to 6mm with incompetent lips. 3.b Reverse overjet greater than 1mm but less than or equal to 3.5mm. 3.c Anterior or posterior crossbites with greater than 1mm but less than or equal to 2mm discrepancy between retruded contact position and intercuspal position. 3.d Contact point displacements greater than 2mm but less than or equal to 4mm. 3.e Lateral or anterior open bite greater than 2mm but less than or equal to 4mm. 3.f Deep overbite complete on gingival or palatal tissues but no trauma. GRADE 2 (Little) 2.a Increased overjet greater than 3.5mm but less than or equal to 6mm with competent lips. 2.b Reverse overjet greater than 0mm but less than or equal to 1mm. 2.c Anterior or posterior crossbite with less than or equal to 1mm discrepancy between retruded contact position and intercuspal position. 2.d Contact point displacements greater than 1mm but less than or equal to 2mm. 2.e Anterior or posterior openbite greater than 1mm but less than or equal to 2mm. 2.f Increased overbite greater than or equal to 3.5mm without gingival contact. 2.g Pre-normal or post-normal occlusions with no other anomalies (includes up to half a unit discrepancy). GRADE 1 (None) 1. Extremely minor malocclusions including contact point displacements less than 1mm.
13 MANAGING THE 3. How they meet, i.e. incisor relationship. i) Overjet normal, increased, reduced, edge-to-edge. ii) Overbite complete, incomplete, open. iii) Centre lines. 4. Buccal segments. Note crowding. Presence/ absence, position and quality of all posterior teeth. 5. How they meet, i.e. buccal occlusion. i) Antero-posteriorly: Class I, Class II molars. ii) Transversely: for presence of crossbites. iii) Vertically: for open bites, etc. iv) Mandibular displacement. 6. Skeletal Pattern. i) Antero-posteriorly: to determine if the mandible is posterior to the maxilla and to what extent. This can be assessed by digital palpation with the patient sitting upright in the dental chair with their Frankfort Plane (FP) horizontal. ii) Vertically: An assessment of the Frankfort- Mandibular Plane Angle (FMPA) gives some idea of the difficulty of the case. Both extremes tend to be difficult. A very low FMPA suggests difficulty in reducing a deep overbite or spaces in the arch that would be difficult to close. A high angle indicates an increased lower facial height with concomitant reduction in the lip competence. Post-treatment stability may be questionable. iii) Transversely: note any chin or nasal asymmetry. 7. Soft Tissues. The soft tissues of the lips and tongue often adapt to an abnormal tooth position and may exacerbate a malocclusion caused primarily by the skeletal pattern. For example, the lower lip may rest behind the upper incisors to help form an anterior oral seal. This can cause the upper incisors to procline further. 8. If as a result of the clinical assessment there are findings which require further investigation, then appropriate radiographs may be justified (see Orthodontic Radiographs Guidelines 3rd Ed 2008 BOS). The vast majority of abnormalities fall into one or other of the categories discussed earlier. It is relatively simple to progress from this diagnostic analysis to a problem list and on to a provisional treatment plan. Your initial assessment might indicate that a malocclusion is present which could be corrected with treatment. However, the patient and parent may not be aware that a problem exists. It is important to ascertain at this stage whether treatment would be appropriate, bearing in mind the severity of the occlusal problem as well as the patient s attitude, motivation and oral health. The following questions may help in this decision process: 1. Is the orthodontic condition a genuine problem, and to whom? 2. Is orthodontic advice required and can you provide it? 3. If not, at what level is specialist advice required? The nature of the problem should be explained to the child/parent(s) together with possible solutions. In addition, you should discuss with the child/ parent(s) what is expected of them in terms of compliance, the appliances likely to be required, the duration of treatment and the need for retention following active orthodontic treatment The advantages and shortcomings of various types of treatment should also be discussed, where appropriate, before deciding on further action. Time taken to counsel the patient and parent at this stage is time well spent. If you consider that removable appliance therapy is indicated, are you confident that a significant and stable improvement will be achieved? Remember that extracted teeth cannot be replaced. Above all, it is imperative that you do no harm. If in any doubt, seek specialist advice SOFT TISSUES. The variation in lip morphology and behaviour is almost infinite. There are, however, some characteristic patterns to be aware of. 22. The very active ("strap-like") lower lip which pulls back against the lower incisors. Here, any overjet is likely to be partly due to retroclined lower incisors. 23. The lower lip which rests behind the upper incisors is likely to procline them and contribute to any increase in overjet. 24. A short upper lip length or high upper lip line will contribute to a lips-apart posture. The stability of any overjet reduction in these cases will be in some doubt. 13
14 TREATMENT PLANNING 1 SPACE CONSIDERATIONS The alignment of crowded or rotated teeth or the reduction of an increased overjet frequently requires space. This may be provided either by expansion of the arches or by the extraction of permanent teeth. Throughout the first half of the last century, the proponents of both extraction and non-extraction therapies were in vehement opposition. These two schools of thought persisted until the latter part of the 20th Century when common sense prevailed. It is now recognised that each method has its place in contemporary orthodontic practice. In cases with crowding of less than 4mm, sufficient space may be gained by expansion but stability may be a problem in the long term. Patients with crowding of more than 4mm are more difficult to categorise and may be treated either by extraction or expansion techniques. The choice is normally made on an individual basis on the grounds of the type of malocclusion, facial aesthetics and stability. It is governed by the position of the teeth and the anticipated soft tissue response to any changes in tooth position. Although expansion is now accepted as a legitimate method of space creation, it must be carried out carefully and within prescribed limits. In general, to be confident of long-term stability, a maximum of 2mm forward movement of incisors, 2-3mm lateral expansion of premolars and molars and zero inter-canine expansion is all that can be permitted. 25. Remember to confirm the presence, position and morphology of all permanent teeth before any extractions. The unerupted UL5 is being deflected into the UL4 space and could easily be extracted in error EXTRACTIONS Lower incisor crowding is so prevalent that it may be regarded as the norm. It is not the result of pressure from erupting permanent third molars but is due to late growth changes and soft tissue maturation. Mild crowding is probably more difficult to treat than severe crowding, since the loss of one tooth in each quadrant will leave excessive residual spacing. If the appearance of the teeth is satisfactory, it may be wise to accept a mild degree of crowding rather than embarking on prolonged and unwanted treatment with fixed appliances. It must be remembered that if the first premolars are extracted there is a risk of increased overbite and reduction of intercanine width; residual space is also likely to be a problem in the absence of treatment. It is worth seeking specialist advice if there is any doubt regarding extractions. Planning Extractions Look at the lower arch first. If moderate crowding of the lower incisors is present, it may be necessary to extract in the lower arch. If the degree of crowding is such that extractions are considered necessary, then either the first or second premolars are likely to be the teeth of choice for extraction. The final choice of extraction pattern will be determined by the degree of crowding as well as the condition and position of the remaining permanent teeth. The ectopic position of the permanent canine or the hypoplastic nature of a second premolar may dictate their loss. Similarly, a lower incisor may be non-vital and discoloured or severely misplaced. These features complicate treatment planning and are ample justification for seeking specialist advice. Consider the upper arch. If extractions are required in the lower arch, then extractions will usually be required in the upper arch. Once again, the first or second premolars are likely to be the teeth of choice for extraction, unless second premolars are absent or hypoplastic or first permanent molars are of poor quality. If space is tight and the molar relationship is Class II, anchorage reinforcement or distal movement with extra-oral traction (i.e. headgear) or orthodontic mini-screws may be indicated. If the lower arch is well aligned, it may be possible to carry out treatment by extracting in the upper arch only. Alternatively, it may be possible to recreate space in the upper arch by moving the upper buccal segments distally with headgear. 14
15 TREATMENT PLANNING 3 WHAT TO REFER FOR SPECIALIST ADVICE 1. Severe skeletal problems, including those where functional appliances may be indicated in the late mixed dentition stage of dental development. 2. Patients with unerupted teeth of doubtful prognosis, especially impacted maxillary canines. 3. Uncertain choice of extraction patterns. 4. Teeth which require derotation or bodily movement. Retention Any treatment more complex than pushing a single incisor over the bite requires a period of retention. At the end of active treatment, there is an almost universal tendency for the teeth to relapse. It is important to remember that the mouth is a complex biological system, which undergoes constant change throughout an individual s life. The fibres of the periodontal ligament and gingivae are put under tension or pressure during the active stages of treatment. Research has shown that it takes 9-12 months for these fibres to re-attach so that tension no longer exists. A period of retention is essential during this re-orientation process. This is normally provided by some form of passive removable appliance. It is difficult to offer hard and fast rules for the ideal length of retention period as it varies from patient to patient depending on the specific features of their original malocclusion. The minimum period is usually 3-6 months full-time followed by six months night-time wear. Even after a period of retention, there is likely to be some slight movement (relapse/ deterioration) of the position of the teeth. Corrected rotated teeth may require some form of permanent retention. Patients are often advised to wear their removable retainers one or two nights each week for the rest of their lives if they want their teeth to remain straight. There is an increasing tendency to use prolonged or indefinite retention regimes nowadays. Adult Orthodontics Although the majority of orthodontic treatment is carried out on adolescents during their active skeletal growth period, it would be wrong to advise adults that orthodontic treatment is not possible for them. Many adults are now prepared to undergo complicated orthodontic treatment. However, they should be advised that treatment will take several months longer that the equivalent treatment for a child. Adult teeth move less readily through denser bone and the multidisciplinary nature of adult orthodontics makes their treatment more complex and demanding. Refer adults to an orthodontic specialist for further advice Recommended Reading An Introduction to Orthodontics. L. Mitchell. 3rd ed. Oxford University Press 2007 ISBN Handbook of Orthodontics. M. Cobourne & A. DiBiase. Mosby ISBN Orthodontics at a Glance. D.S. Gill. Blackwell ISBN A Clinical Guide to Orthodontics. D. Roberts-Harry & J. Sandy. BDJ series ISBN Interceptive Orthodontics. A. Richardson. 4th ed. BDJ ISBN Royal College of England Faculty of Dental Surgery National Clinical Guidelines at: ,27 & 28. This case illustrates the degree of improvement that can be routinely achieved with fixed appliance therapy Scrupulous oral hygiene and dietary control are essential during fixed appliance therapy to avoid possible damage to the teeth caused by plaque collecting around the brackets and acid erosion from soft fizzy drinks. 15
16 This booklet is designed to assist general dental practitioners with their examination of children from an orthodontic point of view. It highlights the assessment of children at the different stages of their dental development and outlines the interceptive procedures and treatments available to deal with those conditions most commonly encountered in general practice. Produced by Members of the Clinical Standards Committee of the British Orthodontic Society. Edited by Annalise McNair and David Morris. British Orthodontic Society 2010 Revised and Updated February 2010 ISBN All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means, electronic, mechanical, photocopying, recording or otherwise, without the prior permission of the British Orthodontic Society. British Orthodontic Society (Registered Charity Number ) 12 Bridewell Place London EC4V 6AP Tel: +44 (0) Fax:+44 (0)
Guidelines for Referrals for Orthodontic Treatment
 Advice for General Dental Practitioners, PCTs and LHBs Guidelines for Referrals for Orthodontic Treatment This document has been produced by the British Orthodontic Society Guidelines for Referrals for
Advice for General Dental Practitioners, PCTs and LHBs Guidelines for Referrals for Orthodontic Treatment This document has been produced by the British Orthodontic Society Guidelines for Referrals for
Clinical Practice Guideline For Orthodontics
 Clinical Practice Guideline For Orthodontics MOH- Oral Health CSN -Orthodontics -2010 Page 1 of 15 Orthodontic Management Guidelines 1. Definitions: Orthodontics is the branch of dentistry concerned with
Clinical Practice Guideline For Orthodontics MOH- Oral Health CSN -Orthodontics -2010 Page 1 of 15 Orthodontic Management Guidelines 1. Definitions: Orthodontics is the branch of dentistry concerned with
Classification of Malocclusion
 Classification of Malocclusion What s going on here? How would you describe this? Dr. Robert Gallois REFERENCE: Where Do We Begin? ESSENTIALS FOR ORTHODONTIC PRACTICE By Riolo and Avery Chapter 6 pages
Classification of Malocclusion What s going on here? How would you describe this? Dr. Robert Gallois REFERENCE: Where Do We Begin? ESSENTIALS FOR ORTHODONTIC PRACTICE By Riolo and Avery Chapter 6 pages
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery. Consequences of tooth loss.
 Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Headgear Appliances. Dentofacial Orthopedics and Orthodontics. A Common Misconception. What is Headgear? Ideal Orthodontic Treatment Sequence
 Ideal Orthodontic Treatment Sequence Headgear Appliances Natalie A. Capan, D.M.D. 580 Sylvan Avenue, Suite 1M Englewood Cliffs, New Jersey 07632 (201)569-9055 www.capanorthodontics.com [email protected]
Ideal Orthodontic Treatment Sequence Headgear Appliances Natalie A. Capan, D.M.D. 580 Sylvan Avenue, Suite 1M Englewood Cliffs, New Jersey 07632 (201)569-9055 www.capanorthodontics.com [email protected]
Removable appliances II. Functional jaw orthopedics
 Removable appliances II. Functional jaw orthopedics Melinda Madléna DMD, PhD Associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification
Removable appliances II. Functional jaw orthopedics Melinda Madléna DMD, PhD Associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification
A. DEVELOPMENT OF THE DENTAL ORGAN (ENAMEL ORGAN):
 A. DEVELOPMENT OF THE DENTAL ORGAN (ENAMEL ORGAN): AS EARLY AS THE SECOND MONTH OF FETAL LIFE, THE DEVELOPMENT OF THE DECIDUOUS TEETH MAY FIRST BECOME EVIDENT. 1. Dental lamina and Bud stage At about six
A. DEVELOPMENT OF THE DENTAL ORGAN (ENAMEL ORGAN): AS EARLY AS THE SECOND MONTH OF FETAL LIFE, THE DEVELOPMENT OF THE DECIDUOUS TEETH MAY FIRST BECOME EVIDENT. 1. Dental lamina and Bud stage At about six
Objectives. Objectives. Objectives. Objectives. Describe Class II div 1
 Class II div 1 Malocclusion Class II div 1 Malocclusion Objectives OR What can we do about Goofy? Objectives Describe Class II div 1 Objectives Describe Class II div 1 Describe principles of treatment
Class II div 1 Malocclusion Class II div 1 Malocclusion Objectives OR What can we do about Goofy? Objectives Describe Class II div 1 Objectives Describe Class II div 1 Describe principles of treatment
Bitewing Radiography B.E. DIXON. B.D.S., M.Sc., D.P.D.S.
 Bitewing Radiography B.E. DIXON B.D.S., M.Sc., D.P.D.S. Main Indications Detection of Dental Caries Monitoring progression of caries Assessment of existing restorations Assessment of Periodontal status
Bitewing Radiography B.E. DIXON B.D.S., M.Sc., D.P.D.S. Main Indications Detection of Dental Caries Monitoring progression of caries Assessment of existing restorations Assessment of Periodontal status
The etiology of orthodontic problems Fifth session
 بنام خداوند جان و خرد The etiology of orthodontic problems Fifth session دکتر مھتاب نوری دانشيار گروه ارتدنسی Course Outline( 5 sessions) Specific causes of malocclusion Genetic Influences Environmental
بنام خداوند جان و خرد The etiology of orthodontic problems Fifth session دکتر مھتاب نوری دانشيار گروه ارتدنسی Course Outline( 5 sessions) Specific causes of malocclusion Genetic Influences Environmental
Orthodontic mini-implants, or temporary anchorage devices
 Anchors, away by John Marshall Grady, DMD, Dan E. Kastner, DMD, and Matthew C. Gornick, DMD Drs. John Marshall Grady (center), Dan E. Kastner (left), and Matthew C. Gornick (right). Drs. John Marshall
Anchors, away by John Marshall Grady, DMD, Dan E. Kastner, DMD, and Matthew C. Gornick, DMD Drs. John Marshall Grady (center), Dan E. Kastner (left), and Matthew C. Gornick (right). Drs. John Marshall
Appendix 1 Orthodontic Referral Guidelines for referring practitioners
 Appendix 1 Orthodontic Referral Guidelines for referring practitioners These guidelines are intended to assist General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists and Primary Care
Appendix 1 Orthodontic Referral Guidelines for referring practitioners These guidelines are intended to assist General Dental Practitioners (GDPs), Community Dental Service (CDS) Dentists and Primary Care
SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656
 SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656 ORTHODONTIC CLASSIFICATION / DIAGNOSIS Goal of diagnosis: An orderly reduction of the data base to a useful list of the patient s problems Useful??
SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656 ORTHODONTIC CLASSIFICATION / DIAGNOSIS Goal of diagnosis: An orderly reduction of the data base to a useful list of the patient s problems Useful??
Topics for the Orthodontics Board Exam
 Topics for the Orthodontics Board Exam I. Diagnostics, relations to paediatric dentistry, prevention 1. Etiology of dental anomalies. 2. Orthodontic anomalies, relationship between orthodontic treatment
Topics for the Orthodontics Board Exam I. Diagnostics, relations to paediatric dentistry, prevention 1. Etiology of dental anomalies. 2. Orthodontic anomalies, relationship between orthodontic treatment
ABSTRACT INTRODUCTION. Facial Esthetics. Dental Esthetics
 ABSTRACT The FACE philosophy is characterized by clearly defined treatment goals. This increases diagnostic ability and improves the quality and stability of the end result. The objective is to establish
ABSTRACT The FACE philosophy is characterized by clearly defined treatment goals. This increases diagnostic ability and improves the quality and stability of the end result. The objective is to establish
Dr. Park's Publications
 Dr. Park's Publications Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D. Diplomate, American Board of Orthodontics Editor-in-Chief, Pacific Coast Society of Orthodontists Chief Editor, Computed Tomography: New
Dr. Park's Publications Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D. Diplomate, American Board of Orthodontics Editor-in-Chief, Pacific Coast Society of Orthodontists Chief Editor, Computed Tomography: New
Retrospective analysis of factors influencing the eruption of delayed permanent incisors after supernumerary tooth removal
 Retrospective analysis of factors influencing the eruption of delayed permanent incisors after supernumerary tooth removal R.A.E. BRYAN*, B.O.I. COLE**, R.R. WELBURY* ABSTRACT. Aim This was to assess the
Retrospective analysis of factors influencing the eruption of delayed permanent incisors after supernumerary tooth removal R.A.E. BRYAN*, B.O.I. COLE**, R.R. WELBURY* ABSTRACT. Aim This was to assess the
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION
 MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
Guideline on Management of the Developing Dentition and Occlusion in Pediatric Dentistry
 Guideline on Management of the Developing Dentition and Occlusion in Pediatric Dentistry Originating Committee Clinical Affairs Committee Developing Dentition Subcommittee Review Council Council on Clinical
Guideline on Management of the Developing Dentition and Occlusion in Pediatric Dentistry Originating Committee Clinical Affairs Committee Developing Dentition Subcommittee Review Council Council on Clinical
ORTHODONTIC SCREENING GUIDE FOR NORTH DAKOTA HEALTH TRACKS NURSES
 ORTHODONTIC SCREENING GUIDE FOR NORTH DAKOTA HEALTH TRACKS NURSES The North Dakota Department of Human Services Medical Services Division and the North Dakota Department of Health s Oral Health Program
ORTHODONTIC SCREENING GUIDE FOR NORTH DAKOTA HEALTH TRACKS NURSES The North Dakota Department of Human Services Medical Services Division and the North Dakota Department of Health s Oral Health Program
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Use of variable torque brackets to enhance treatment outcomes
 Use of variable torque brackets to enhance treatment outcomes Ralph Nicassio DDS Many clinicians performing Orthodontics for their patients are missing an opportunity to get better results because they
Use of variable torque brackets to enhance treatment outcomes Ralph Nicassio DDS Many clinicians performing Orthodontics for their patients are missing an opportunity to get better results because they
Congenital absence of mandibular second premolars
 CLINICIAN S CORNER Congenitally missing mandibular second premolars: Clinical options Vincent G. Kokich a and Vincent O. Kokich b Seattle, Wash Introduction: Congenital absence of mandibular second premolars
CLINICIAN S CORNER Congenitally missing mandibular second premolars: Clinical options Vincent G. Kokich a and Vincent O. Kokich b Seattle, Wash Introduction: Congenital absence of mandibular second premolars
General Explanation of the Straight Wire Appliance in the Treatment of Young People and Adults Publication for the Journal du Dentiste in Belgium
 General Explanation of the Straight Wire Appliance in the Treatment of Young People and Adults Publication for the Journal du Dentiste in Belgium Today, our dental patients are asking us to provide them,
General Explanation of the Straight Wire Appliance in the Treatment of Young People and Adults Publication for the Journal du Dentiste in Belgium Today, our dental patients are asking us to provide them,
ORTHODONTIC TREATMENT
 ORTHODONTIC TREATMENT Informed Consent for the Orthodontic Patient As a general rule, positive orthodontic results can be achieved by informed and cooperative patients. Thus, the following information
ORTHODONTIC TREATMENT Informed Consent for the Orthodontic Patient As a general rule, positive orthodontic results can be achieved by informed and cooperative patients. Thus, the following information
CRANIOFACIAL ABNORMALITIES
 CRANIOFACIAL ABNORMALITIES It is well documented that mouth-breathing children grow longer faces. A paper by Tourne entitled The long face syndrome and impairment of the nasopharyngeal airway, recognised
CRANIOFACIAL ABNORMALITIES It is well documented that mouth-breathing children grow longer faces. A paper by Tourne entitled The long face syndrome and impairment of the nasopharyngeal airway, recognised
Anatomic Anomalies. Anomalies. Anomalies. Anomalies. Supernumerary Teeth. Supernumerary Teeth. Steven R. Singer, DDS 212.305.5674 srs2@columbia.
 Anatomic Anomalies Steven R. Singer, DDS 212.305.5674 [email protected] Anomalies! Anomalies are variations in the:! Size! Morphology! Number! Eruption of the teeth Anomalies Anomalies There are two categories:!
Anatomic Anomalies Steven R. Singer, DDS 212.305.5674 [email protected] Anomalies! Anomalies are variations in the:! Size! Morphology! Number! Eruption of the teeth Anomalies Anomalies There are two categories:!
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
The Current Concepts of Orthodontic Discrepancy Stability
 Open Journal of Stomatology, 2014, 4, 184-196 Published Online April 2014 in SciRes. http://www.scirp.org/journal/ojst http://dx.doi.org/10.4236/ojst.2014.44028 The Current Concepts of Orthodontic Discrepancy
Open Journal of Stomatology, 2014, 4, 184-196 Published Online April 2014 in SciRes. http://www.scirp.org/journal/ojst http://dx.doi.org/10.4236/ojst.2014.44028 The Current Concepts of Orthodontic Discrepancy
Periapical radiography
 8 Periapical radiography Periapical radiography describes intraoral techniques designed to show individual teeth and the tissues around the apices. Each film usually shows two to four teeth and provides
8 Periapical radiography Periapical radiography describes intraoral techniques designed to show individual teeth and the tissues around the apices. Each film usually shows two to four teeth and provides
About the Doctor. Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D.
 About the Doctor Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D. Dr. Jae Hyun Park is a highly regarded, Board Certified Orthodontist with a strong commitment to clinical education, patient care and research.
About the Doctor Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D. Dr. Jae Hyun Park is a highly regarded, Board Certified Orthodontist with a strong commitment to clinical education, patient care and research.
Introduction to Dental Anatomy
 Introduction to Dental Anatomy Vickie P. Overman, RDH, MEd Continuing Education Units: N/A This continuing education course is intended for dental students and dental hygiene students. Maintaining the
Introduction to Dental Anatomy Vickie P. Overman, RDH, MEd Continuing Education Units: N/A This continuing education course is intended for dental students and dental hygiene students. Maintaining the
A Guideline for the Extraction of First Permanent Molars in Children.
 A Guideline for the Extraction of First Permanent Molars in Children. Introduction The relative timing of coronal development associated with first permanent molars makes them susceptible to chronological
A Guideline for the Extraction of First Permanent Molars in Children. Introduction The relative timing of coronal development associated with first permanent molars makes them susceptible to chronological
Wired for Learning - Orthodontic Basics
 Wired for Learning - Orthodontic Basics Lori Garland Parker, BS, MAOM, RDAEF, CDA, COA Continuing Education Units: 3 hours Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce365/ce365.aspx
Wired for Learning - Orthodontic Basics Lori Garland Parker, BS, MAOM, RDAEF, CDA, COA Continuing Education Units: 3 hours Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce365/ce365.aspx
OCCLUSION IN COMPLETE DENTURES
 1 OCCLUSION IN COMPLETE DENTURES C P Owen Introduction Occlusion has been described as the most important subject in all the disciplines of dentistry, and for good reason, because the way the teeth come
1 OCCLUSION IN COMPLETE DENTURES C P Owen Introduction Occlusion has been described as the most important subject in all the disciplines of dentistry, and for good reason, because the way the teeth come
Position Classification Standard for Dental Officer Series, GS-0680
 Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
ANGEL DENTAL CARE Implant Consent
 This information is to help you make an informed decision about having implant treatment. You should take as much time as you wish to make the decision in relation to signing the following consent form.
This information is to help you make an informed decision about having implant treatment. You should take as much time as you wish to make the decision in relation to signing the following consent form.
Preventive Pediatric Dental Care. Lawrence A. Kotlow DDS Practice Limited to Pediatric Dental Care 340 Fuller Road Albany, New York 12203
 Preventive Pediatric Dental Care Lawrence A. Kotlow DDS Practice Limited to Pediatric Dental Care 340 Fuller Road Albany, New York 12203 Patient comfort and safety 1. All children are treated using the
Preventive Pediatric Dental Care Lawrence A. Kotlow DDS Practice Limited to Pediatric Dental Care 340 Fuller Road Albany, New York 12203 Patient comfort and safety 1. All children are treated using the
DENTAL FOR EVERYONE SUMMARY OF BENEFITS, LIMITATIONS AND EXCLUSIONS
 DENTAL FOR EVERYONE SUMMARY OF BENEFITS, LIMITATIONS AND EXCLUSIONS DEDUCTIBLE The dental plan features a deductible. This is an amount the Enrollee must pay out-of-pocket before Benefits are paid. The
DENTAL FOR EVERYONE SUMMARY OF BENEFITS, LIMITATIONS AND EXCLUSIONS DEDUCTIBLE The dental plan features a deductible. This is an amount the Enrollee must pay out-of-pocket before Benefits are paid. The
In Class IV arch: Fulcrum line passes through two abutments adjacent to single edentulous space.
 It is that part of removable partial denture which assists the direct retainers in preventing displacement of distal extension denture bases by resisting lever action from the opposite side of the fulcrum
It is that part of removable partial denture which assists the direct retainers in preventing displacement of distal extension denture bases by resisting lever action from the opposite side of the fulcrum
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Humana Health Plans of Florida. Important:
 Humana Health Plans of Florida Important: Dental discount membership in Florida is determined by viewing the member s ID card and verifying that the Humana Logo and Medicare name is listed with an effective
Humana Health Plans of Florida Important: Dental discount membership in Florida is determined by viewing the member s ID card and verifying that the Humana Logo and Medicare name is listed with an effective
CHAPTER 10 RESTS AND PREPARATIONS. 4. Serve as a reference point for evaluating the fit of the framework to the teeth.
 CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
OVERVIEW The MetLife Dental Plan for Retirees
 OVERVIEW The MetLife Dental Plan for Retirees IN NETWORK: Staying in network saves you money. 1 Participating dentists have agreed to MetLife s negotiated fees which are typically 15% to 45% below the
OVERVIEW The MetLife Dental Plan for Retirees IN NETWORK: Staying in network saves you money. 1 Participating dentists have agreed to MetLife s negotiated fees which are typically 15% to 45% below the
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
Page 1 of 10 BDS FINAL PROFESSIONAL EXAMINATION 2007 Prosthodontics (MCQs) Model Paper SECTION I
 Page 1 of 10 COMPLETE DENTURES ANATOMICAL LANDMARKS SECTION I 1. There are many landmarks in the oral cavity which helps in designing complete dentures. One of the important landmarks is fovea palatini.
Page 1 of 10 COMPLETE DENTURES ANATOMICAL LANDMARKS SECTION I 1. There are many landmarks in the oral cavity which helps in designing complete dentures. One of the important landmarks is fovea palatini.
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
2007 Insurance Benefits Guide. Dental and Dental Plus. Dental and. Dental Plus. www.eip.sc.gov Employee Insurance Program 91
 Dental and www.eip.sc.gov Employee Insurance Program 91 Table of Contents Introduction...93 Your Dental Benefits at a Glance...94 Claim Examples (using Class III procedure claims)...95 How to File a Dental
Dental and www.eip.sc.gov Employee Insurance Program 91 Table of Contents Introduction...93 Your Dental Benefits at a Glance...94 Claim Examples (using Class III procedure claims)...95 How to File a Dental
The Dahl principle in everyday dentistry
 The Dahl principle in everyday dentistry Using two clinical case studies, Dr Tif Qureshi revisits differential tooth wear, the Inman aligner, the Dahl principle and an alternative to preparo-mental dentistry
The Dahl principle in everyday dentistry Using two clinical case studies, Dr Tif Qureshi revisits differential tooth wear, the Inman aligner, the Dahl principle and an alternative to preparo-mental dentistry
Non-carious dental conditions
 Non-carious dental conditions Children s Dental Health in the United Kingdom, 2003 Barbara Chadwick, Liz Pendry October 2004 Crown copyright 2004 Office for National Statistics 1 Drummond Gate London SW1V
Non-carious dental conditions Children s Dental Health in the United Kingdom, 2003 Barbara Chadwick, Liz Pendry October 2004 Crown copyright 2004 Office for National Statistics 1 Drummond Gate London SW1V
Dental Services Rider Harbor Choice Plus, a product of Harbor Health Plan, Inc.
 Your Agreement gives You important information about Your health care benefits. This Dental Services Rider ( Rider ) is issued to You with Your Agreement because the plan you selected includes Other Dental
Your Agreement gives You important information about Your health care benefits. This Dental Services Rider ( Rider ) is issued to You with Your Agreement because the plan you selected includes Other Dental
Dental. Covered services and limitations module
 Dental Covered services and limitations module Dental Covered Services and Limitations Module Covered Dental Services for Patients Under the Age of 21...2 Examinations...2 Radiographs and Diagnostic Imaging...2
Dental Covered services and limitations module Dental Covered Services and Limitations Module Covered Dental Services for Patients Under the Age of 21...2 Examinations...2 Radiographs and Diagnostic Imaging...2
Quintessence Publishing Co, Inc
 EARLY-AGE ORTHODONTIC TREATMENT Aliakbar Bahreman, DDS, MS Clinical Professor Orthodontic and Pediatric Dentistry Programs Eastman Institute for Oral Health University of Rochester Rochester, New York
EARLY-AGE ORTHODONTIC TREATMENT Aliakbar Bahreman, DDS, MS Clinical Professor Orthodontic and Pediatric Dentistry Programs Eastman Institute for Oral Health University of Rochester Rochester, New York
LIP INCOMPETENCE. Robert M. Mason, DMD, PhD
 LIP INCOMPETENCE Robert M. Mason, DMD, PhD If you were to enter an elementary school classroom, you would expect to see a lot of teeth showing as you talk to the students who are (hopefully) sitting quietly
LIP INCOMPETENCE Robert M. Mason, DMD, PhD If you were to enter an elementary school classroom, you would expect to see a lot of teeth showing as you talk to the students who are (hopefully) sitting quietly
HEALTH SERVICES POLICY & PROCEDURE MANUAL. SUBJECT: Types of Dental Treatments Provided EFFECTIVE DATE: July 2014 SUPERCEDES DATE: January 2014
 PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
A Dental Benefit Summary for Rice University
 Aetna Dental presents A Dental Benefit Summary for Rice University CODE CODE Office Visit Copay $5 DIAGNOSTIC CROWNS/BRIDGES D0120 Exam-Periodic No Charge D2510 Inlay, Metallic, One surface $225 D0150
Aetna Dental presents A Dental Benefit Summary for Rice University CODE CODE Office Visit Copay $5 DIAGNOSTIC CROWNS/BRIDGES D0120 Exam-Periodic No Charge D2510 Inlay, Metallic, One surface $225 D0150
05 - DENTAL SURGERY. (02) MS (Oral Surgery) Part II Examination
 05 - DENTAL SURGERY (02) MS (Oral Surgery) Part II Examination 01. October 1990 02. October 1991 03. October 1992 04. October 1993 05. October 1994 06. November 1995 07. October 1996 08. November 1997
05 - DENTAL SURGERY (02) MS (Oral Surgery) Part II Examination 01. October 1990 02. October 1991 03. October 1992 04. October 1993 05. October 1994 06. November 1995 07. October 1996 08. November 1997
TIPS ON FILING INVISALIGN! INSURANCE CLAIMS
 TIPS ON FILING INVISALIGN! INSURANCE CLAIMS Charles Blair, DDS Disclaimer: The codes, rules and their interpretations change. Always refer to the latest code revision, CDT-2007/2008 and use the latest
TIPS ON FILING INVISALIGN! INSURANCE CLAIMS Charles Blair, DDS Disclaimer: The codes, rules and their interpretations change. Always refer to the latest code revision, CDT-2007/2008 and use the latest
4-1-2005. Dental Clinical Criteria and Documentation Requirements
 4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
GUIDELINES FOR AJODO CASE REPORTS
 GUIDELINES FOR AJODO CASE REPORTS Case reports are published on a regular basis in the AJODO. Not only are these short communications interesting to the clinician in private practice, but they provide
GUIDELINES FOR AJODO CASE REPORTS Case reports are published on a regular basis in the AJODO. Not only are these short communications interesting to the clinician in private practice, but they provide
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
ORTHODONTIC PROBLEMS IN PATIENTS WITH HYPODONTIA AND TAURODONTISM OF PERMANENT MOLARS
 Journal of IMAB - Annual Proceeding (Scientific Papers) 2011, vol. 17, book 2 ORTHODONTIC PROBLEMS IN PATIENTS WITH HYPODONTIA AND TAURODONTISM OF PERMANENT MOLARS Miroslava Yordanova 1, Svetlana Yordanova
Journal of IMAB - Annual Proceeding (Scientific Papers) 2011, vol. 17, book 2 ORTHODONTIC PROBLEMS IN PATIENTS WITH HYPODONTIA AND TAURODONTISM OF PERMANENT MOLARS Miroslava Yordanova 1, Svetlana Yordanova
Dental Implant Treatment after Improvement of Oral Environment by Orthodontic Therapy
 Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
Managing worn teeth with composites
 6 Managing worn teeth with composites Clinical details A 50-year-old man presents to you complaining about his worn teeth and would like the appearance improved (Fig. 6.1). He complains of regurgitation
6 Managing worn teeth with composites Clinical details A 50-year-old man presents to you complaining about his worn teeth and would like the appearance improved (Fig. 6.1). He complains of regurgitation
BASIC ORTHODONTICS. And why we believe in THE TIP EDGE TECHNIQUE (Differential Straight Arch)
 BASIC ORTHODONTICS And why we believe in THE TIP EDGE TECHNIQUE (Differential Straight Arch) MOVING TEETH Light force + Time = Tooth Movement Any technique of moving teeth involves light force and time.
BASIC ORTHODONTICS And why we believe in THE TIP EDGE TECHNIQUE (Differential Straight Arch) MOVING TEETH Light force + Time = Tooth Movement Any technique of moving teeth involves light force and time.
Implants in your Laboratory: Abutment Design
 1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
Condylar position in children with functional posterior crossbites: before and after crossbite correction*
 PEDIATRIC DENTISTRY/Copyright 1980 by The American Academy of Pedodontics/Vol. 2, No. 3 Condylar position in children with functional posterior crossbites: before and after crossbite correction* David
PEDIATRIC DENTISTRY/Copyright 1980 by The American Academy of Pedodontics/Vol. 2, No. 3 Condylar position in children with functional posterior crossbites: before and after crossbite correction* David
Universal Screw Removal System (USR)
 Craniomaxillofacial Surgery 3 Universal Screw Removal System (USR) Craniomaxillofacial rigid fixation systems are available from a variety of manufacturers. The USR system is a complete screwdriver array
Craniomaxillofacial Surgery 3 Universal Screw Removal System (USR) Craniomaxillofacial rigid fixation systems are available from a variety of manufacturers. The USR system is a complete screwdriver array
ADA Dental Claim Form (2012 American Dental Association) Completion Instructions Page 1 of 17
 Page 1 of 17 Introduction The ADA Dental Claim Form has been revised to incorporate key changes to the HIPAA standard electronic dental claim transaction. This version of the form, front and reverse sides,
Page 1 of 17 Introduction The ADA Dental Claim Form has been revised to incorporate key changes to the HIPAA standard electronic dental claim transaction. This version of the form, front and reverse sides,
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Tooth preparation J. C. Davenport, 1 R. M. Basker, 2 J. R. Heath, 3 J. P. Ralph, 4 P-O. Glantz, 5 and P. Hammond, 6
 12 5 Tooth preparation J. C. Davenport, 1 R. M. Basker, 2 J. R. Heath, 3 J. P. Ralph, 4 P-O. Glantz, 5 and P. Hammond, 6 This final article in the series describes the modification of teeth to improve
12 5 Tooth preparation J. C. Davenport, 1 R. M. Basker, 2 J. R. Heath, 3 J. P. Ralph, 4 P-O. Glantz, 5 and P. Hammond, 6 This final article in the series describes the modification of teeth to improve
Course Curriculum for the Master Degree in Dentistry/Orthodontics
 Jordan University of Science and Technology Faculty of Graduate Studies Course Curriculum for the Master Degree in Dentistry/Orthodontics The Master Degree in Dentistry/ Orthodontics is awarded by the
Jordan University of Science and Technology Faculty of Graduate Studies Course Curriculum for the Master Degree in Dentistry/Orthodontics The Master Degree in Dentistry/ Orthodontics is awarded by the
ORTHODONTIC CARE IN NAVAL MILITARY TREATMENT FACILITIES
 DEPARTMENT OF THE NAVY BUREAU OF MEDICINE AND SURGERY 2300 E STR EET NW WASHINGTON DC 20372-5300 IN REPL Y REFER TO BUMEDINST 6670.2A BUMED-M3B6 BUMED INSTRUCTION 6670.2A From: Chief, Bureau of Medicine
DEPARTMENT OF THE NAVY BUREAU OF MEDICINE AND SURGERY 2300 E STR EET NW WASHINGTON DC 20372-5300 IN REPL Y REFER TO BUMEDINST 6670.2A BUMED-M3B6 BUMED INSTRUCTION 6670.2A From: Chief, Bureau of Medicine
General Dentist Fees
 General Dentist Fees January 1, 2015 Not all codes are covered benefits. Please check the member s plan for verification and limitations. There are no fee increases for 2015, but new CDT codes have been
General Dentist Fees January 1, 2015 Not all codes are covered benefits. Please check the member s plan for verification and limitations. There are no fee increases for 2015, but new CDT codes have been
Schedule B Indemnity plan People First Plan Code #4084
 : Calendar year deductible Waived for Type I preventive dental services Calendar year maximum Type I, II, III Waiting period Type I, II, III $50 individual $150 family (3 per family) $1,000 per covered
: Calendar year deductible Waived for Type I preventive dental services Calendar year maximum Type I, II, III Waiting period Type I, II, III $50 individual $150 family (3 per family) $1,000 per covered
Case Report Case studies on local orthodontic traction by minis-implants before implant rehabilitation
 Int J Clin Exp Med 2015;8(5):8178-8184 www.ijcem.com /ISSN:1940-5901/IJCEM0006299 Case Report Case studies on local orthodontic traction by minis-implants before implant rehabilitation Pei Shen *, Wei-Feng
Int J Clin Exp Med 2015;8(5):8178-8184 www.ijcem.com /ISSN:1940-5901/IJCEM0006299 Case Report Case studies on local orthodontic traction by minis-implants before implant rehabilitation Pei Shen *, Wei-Feng
SURGICAL ORTHODONTICS: LITERATURE REVIEW AND CASE REPORT
 Orthodontics Piyush Heda, Babita Raghuwanshi, Amit Prakash, Kishore Sonawane SURGICAL ORTHODONTICS: LITERATURE REVIEW AND CASE REPORT Piyush HEDA 1, Babita RAGHUWANSHI 2, Amit PRAKASH 3, Kishore SONAWANE
Orthodontics Piyush Heda, Babita Raghuwanshi, Amit Prakash, Kishore Sonawane SURGICAL ORTHODONTICS: LITERATURE REVIEW AND CASE REPORT Piyush HEDA 1, Babita RAGHUWANSHI 2, Amit PRAKASH 3, Kishore SONAWANE
U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria
 U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria Alcune pubblicazioni della Scuola: Impacted maxillary incisors: diagnosis and predictive measurements. Pavoni C, Mucedero M, Laganà G, Paoloni
U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria Alcune pubblicazioni della Scuola: Impacted maxillary incisors: diagnosis and predictive measurements. Pavoni C, Mucedero M, Laganà G, Paoloni
CLASSIFICATION OF CARIOUS LESIONS AND TOOTH PREPARATION.
 CLASSIFICATION OF CARIOUS LESIONS AND TOOTH PREPARATION. ١ G.V. BLACK who is known as the father of operative dentistry,he classified carious lesions into groups according to their locations in permanent
CLASSIFICATION OF CARIOUS LESIONS AND TOOTH PREPARATION. ١ G.V. BLACK who is known as the father of operative dentistry,he classified carious lesions into groups according to their locations in permanent
Dental Plan General Information
 Dental Plan General Information CSU offers two dental plans for employees to choose from: Delta Dental Basic and Delta Dental Plus. Both plans are self-insured and administered, including claims processing,
Dental Plan General Information CSU offers two dental plans for employees to choose from: Delta Dental Basic and Delta Dental Plus. Both plans are self-insured and administered, including claims processing,
What s The Plan? Why Start Now?
 What s The Plan? Just as no two people are exactly alike, no two treatment plans are exactly alike. Dr. Hullings has developed a treatment plan just for you, involving procedures appropriate for your individual
What s The Plan? Just as no two people are exactly alike, no two treatment plans are exactly alike. Dr. Hullings has developed a treatment plan just for you, involving procedures appropriate for your individual
Orthodontic treatment need in the Italian child population
 Orthodontic treatment need in the Italian child population C. GRIPPAUDO, E.G. PAOLANTONIO, R. DELI, G. LA TORRE* ABSTRACT. Aim To assess orthodontic treatment need in the Italian child population using
Orthodontic treatment need in the Italian child population C. GRIPPAUDO, E.G. PAOLANTONIO, R. DELI, G. LA TORRE* ABSTRACT. Aim To assess orthodontic treatment need in the Italian child population using
A collection of pus. Usually forms because of infection. A tooth or tooth structure which is responsible for the anchorage of a bridge or a denture.
 Abscess A collection of pus. Usually forms because of infection. Abutment A tooth or tooth structure which is responsible for the anchorage of a bridge or a denture. Amalgam A silver filling material.
Abscess A collection of pus. Usually forms because of infection. Abutment A tooth or tooth structure which is responsible for the anchorage of a bridge or a denture. Amalgam A silver filling material.
Review Article. International Journal of Advanced Health Sciences September 2014 Vol 1 Issue 5 23
 Interdisciplinary Therapy in Orthodontics: An Overview Khumanthem Savana 1, Akram Ansari 2, Rani Hamsa PR 3, Mukesh Kumar 4, Abhay Jain 5, Ankit Singh 6 1,6 Post Graduate Students, 2,5 Reader, 3 Professor
Interdisciplinary Therapy in Orthodontics: An Overview Khumanthem Savana 1, Akram Ansari 2, Rani Hamsa PR 3, Mukesh Kumar 4, Abhay Jain 5, Ankit Singh 6 1,6 Post Graduate Students, 2,5 Reader, 3 Professor
POLICY HOLDER/SUBSCRIBER INFORMATION
 Dental Claim Form Instructions Claim Field Identification 1. Type of Transaction Statement of Actual Services EPSDT/Title XIX Request for Predetermination 2. Predetermination/ Prior Authorization Code
Dental Claim Form Instructions Claim Field Identification 1. Type of Transaction Statement of Actual Services EPSDT/Title XIX Request for Predetermination 2. Predetermination/ Prior Authorization Code
Bonitas Medical Scheme Dental Benefit Table
 Bonitas Medical Dental Benefit Table 2015 PRIMARY DENTAL BENEFIT TABLE 2015 BONSAVE DENTAL BENEFIT TABLE 2015 STANDARD DENTAL BENEFIT TABLE 2015 BONCOM DENTAL BENEFIT TABLE 2015 Dental benefits are paid
Bonitas Medical Dental Benefit Table 2015 PRIMARY DENTAL BENEFIT TABLE 2015 BONSAVE DENTAL BENEFIT TABLE 2015 STANDARD DENTAL BENEFIT TABLE 2015 BONCOM DENTAL BENEFIT TABLE 2015 Dental benefits are paid
SECURITY LIFE INSURANCE COMPANY OF AMERICA Minnetonka, Minnesota
 SECURITY LIFE INSURANCE COMPANY OF AMERICA Minnetonka, Minnesota COVERAGE SCHEDULE PREFERRED (In-Network) PROVIDER: WE WILL PAY BASED ON THE CONTRACTED FEE FOR SERVICE WITH THE PREFERRED PROVIDER ORGANIZATION
SECURITY LIFE INSURANCE COMPANY OF AMERICA Minnetonka, Minnesota COVERAGE SCHEDULE PREFERRED (In-Network) PROVIDER: WE WILL PAY BASED ON THE CONTRACTED FEE FOR SERVICE WITH THE PREFERRED PROVIDER ORGANIZATION
Activity: Can You Identify the Age?
 Activity: Can You Identify the Age? Skeletons are good age markers because teeth and bones mature at fairly predictable rates. How Teeth Reveal Age For toddler to age 21, teeth are the most accurate age
Activity: Can You Identify the Age? Skeletons are good age markers because teeth and bones mature at fairly predictable rates. How Teeth Reveal Age For toddler to age 21, teeth are the most accurate age
MEDICAL ASSISTANCE PROGRAM DENTAL FEE SCHEDULE
 Dental General Payment Policies Children under 21 years of age are eligible for all medically necessary dental services. For children under 21 years of age who require medically necessary dental services
Dental General Payment Policies Children under 21 years of age are eligible for all medically necessary dental services. For children under 21 years of age who require medically necessary dental services
Basic Training 101 TRAINING FOR THE CLINICAL TEAM WITH CONCENTRATION ON COMMUNICATION SKILLS AND CLINICAL SYSTEMS. By: Charlene White, President
 Basic Training 101 TRAINING FOR THE CLINICAL TEAM WITH CONCENTRATION ON COMMUNICATION SKILLS AND CLINICAL SYSTEMS By: Charlene White, President Progressive Concepts, Inc. Consultations, Seminars, Speaking
Basic Training 101 TRAINING FOR THE CLINICAL TEAM WITH CONCENTRATION ON COMMUNICATION SKILLS AND CLINICAL SYSTEMS By: Charlene White, President Progressive Concepts, Inc. Consultations, Seminars, Speaking
RISK MANAGEMENT MODULE 25 ISSN 1749-7426 (PRINT) Cosmetic dentistry COSMETIC DENTISTRY
 RISK MANAGEMENT MODULE 25 ISSN 1749-7426 (PRINT) Cosmetic dentistry As more dentists become increasingly involved in cosmetic procedures, there is a greater potential for patient dissatisfaction, complaints
RISK MANAGEMENT MODULE 25 ISSN 1749-7426 (PRINT) Cosmetic dentistry As more dentists become increasingly involved in cosmetic procedures, there is a greater potential for patient dissatisfaction, complaints
Chapter. CPT only copyright 2010 American Medical Association. All rights reserved. 14Dental
 14Dental Chapter 14 14.1 Enrollment..................................................................... 14-3 14.2 Benefits, Limitations, and Authorization Requirements........................... 14-3
14Dental Chapter 14 14.1 Enrollment..................................................................... 14-3 14.2 Benefits, Limitations, and Authorization Requirements........................... 14-3
Dental Radiography collimator Ionising radiation image radiolucent area radiopaque area controlled zone scatter radiation intraoral
 Dental Radiography X-rays for dental radiography are produced by high voltages of electricity within an x-ray head and come out through a metal tube called a collimator. This ensures the x-rays only come
Dental Radiography X-rays for dental radiography are produced by high voltages of electricity within an x-ray head and come out through a metal tube called a collimator. This ensures the x-rays only come
