James J. Jaber, MD, PhD, John P. Leonetti, MD, Amy E. Lawrason, and Paul J. Feustel, PhD, Maywood, IL; and Albany, NY
|
|
|
- Isabella Arnold
- 8 years ago
- Views:
Transcription
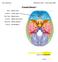
1 Otolaryngology Head and Neck Surgery (2008) 138, ORIGINAL RESEARCH GENERAL OTOLARYNGOLOGY Cervical spine causes for referred otalgia James J. Jaber, MD, PhD, John P. Leonetti, MD, Amy E. Lawrason, and Paul J. Feustel, PhD, Maywood, IL; and Albany, NY OBJECTIVE: Present experience in diagnosis and treatment for referred otalgia secondary to cervical spine degenerative disease (CSDD). STUDY DESIGN: A retrospective study of 123 patients with ear pain. SUBJECTS AND METHODS: All patients had a normal otologic examination and diagnosed with unspecified otalgia. The causes for referred otalgia were categorized into Group I: otalgia from non cervical spine disease (n 72), and Group II: cervical spine disease referred otalgia (n 51). Pain relief following cervical spine physical therapy (CSPT) was assessed. RESULTS: The most common cause for referred otalgia in Group I was Temporomandibular joint (TMJ) dysfunction (46%); most common cervical spine finding in Group II was CSDD (88%). CSPT in those documented patients all reported subjective pain relief. CONCLUSION: As the population in America ages, CSDD in the elderly will begin to emerge as a major etiologic source for referred otalgia. With a targeted medical history and physical examination one can use directed studies to diagnose CSDDreferred otalgia, and this pain can be alleviated with CSPT American Academy of Otolaryngology Head and Neck Surgery Foundation. All rights reserved. Otalgia can be classified as otogenic (primary) or nonotogenic (referred). 1-3 External and middle ear infections are associated with primary otogenic pain, which most otolaryngologists and primary care physicians are trained to diagnose. A negative otologic exam and persistent otalgia should suggest the possibility of referred otalgia. Referred otalgia or pain that is sensed by the ear but originates from a nonotologic source poses a difficult diagnostic challenge to even the most experienced otolaryngologist. Referred pain is an unpleasant sensation localized to an area separate from the site of the causative injury or other noxious stimulation. Often, referred pain is caused by nerve compression or irritation. In this circumstance, the sensation of pain will generally be felt in the territory that the nerve serves (ie, somatic dermatone) even though the damage originates elsewhere (ie,visceral tissue). 4 The ear is unique in that no other structure in the body of comparable size is supplied by so many sensory nerves from so many neural segments. As shown in Figure 1, the sensory innervation of the ear is supplied through a combination of four cranial nerves (CN V, VII, IX, and X) and two superior cervical plexus nerves (C2 and C3). Presumably this complex innervation serves as an evolutionary advantage as hearing is a necessary survival tool, and any pain perceived in that area causes a heightened sense of alarm. The differential diagnosis is specifically related to the sensory innervation of the ear, and therefore it is imperative that the otolaryngologist have a working knowledge of the complex neuroanatomic innervation of the external and middle ear. Among all causes of referred otalgia, dental pathology, which transmits referred otalgia via a branch of the trigeminal nerve, is the most common source of nonotogenic pain. 5 This was demonstrated by a previous study by the author (JPL), where the most common cause of referred otalgia with a normal-appearing ear was dental (74%). 6 Furthermore, the cause of referred otalgia can also be referred pain from the mouth, teeth, larynx, or thyroid gland; neural, vascular, or lymphatic structures of neck; or the esophagus. 7,8 However, with the aging population, physicians must also consider cervical spine degenerative disease (CSDD) as an increasingly common cause of referred otalgia involving the upper cervical plexus (greater auricular and lesser occipital nerve). 9 In this retrospective study, we have reviewed the complex neuroanatomic basis of nonotogenic ear pain, the prevalences of various etiological causes that have elicited this type of pain among our patient population, and presented our own experience in the diagnosis and treatment of referred otalgia secondary to CSDD. Nerve Pathways and Etiologies in Referred Otalgia 1-4,10 Auriculotemporal nerve (CN V). The auriculotemporal nerve derived from the mandibular division of the trigeminal nerve courses with the superficial temporal artery anteriorly to the external ear. The auriculotemporal nerve supplies sensory afferents to the tragus, anterior auricle, anterior wall of the external canal, and anterior portion of the lateral tympanic membrane. Due to the length and extensive distribution of the auriculotemporal nerve, it is the nerve that is most commonly involved in referred otalgia. Received September 4, 2007; revised December 14, 2007; accepted December 28, /$ American Academy of Otolaryngology Head and Neck Surgery Foundation. All rights reserved. doi: /j.otohns
2 480 Otolaryngology Head and Neck Surgery, Vol 138, No 4, April 2008 Figure 1 Complex sensory innervation of the ear and periauricular structures and various etiological causes in referred otalgia. Temporomandibular joint (TMJ) disease and dental pathologies are associated with referred otalgia by way of the auriculotemporal nerve. Posterior auricular nerve (CN VII). The posterior auricular nerve, which is the first extracranial branch of the facial nerve, sends sensory afferents that provide innervation of the posterior wall of the external auditory canal, posterior lateral surface of the tympanic membrane, and posterior skin of the auricle. Otalgia referred from the facial nerve may also occur following an outbreak of herpes zoster (prior to vesicle eruption). Jacobson s nerve (CN IX). Jacobson s nerve, a derivative from the glossopharyngeal nerve, joins with the caroticotympanic branches from the sympathetic plexus to form the tympanic plexus. This plexus provides sensation to the middle ear, upper eustachian tube, and medial surface of the tympanic membrane. Referred otalgia transmitted by the glossopharyngeal nerve may be secondary to lesions and/or inflammatory processes of the nasopharynx, palatine tonsil, soft palate, or posterior one-third of the tongue. Arnold s nerve (CN X). Arnold s nerve, the auricular branch from the vagus, divides into a superior branch, which sends a small branch to the facial nerve sheath, and an inferior branch, which is joined by a small branch from the facial nerve. The inferior branch provides sensation to the inferior and posterior aspects of the external auditory canal, to the concavity of the concha, and finally to the lateral surface of the tympanic membrane. Thyroiditis, thyroid tumors, laryngeal carcinomas, and gastroesophageal reflux can present as referred otalgia secondary to irritation of the superior laryngeal nerve, a branch of the vagus nerve. Greater auricular and lesser occipital nerve (cervical plexus). The greater auricular and lesser occipital nerves, derivatives from C2 and C3 of the cervical plexus, course over the
3 Jaber et al Cervical spine causes for referred otalgia sternocleidomastoid muscle to innervate the posterior auricle and the skin overlying the mastoid bone and parotid gland. Pathology of the cervical spine that may present as referred otalgia includes cervical spine degenerative diseases (eg, osteoarthritis, cervical facet syndrome, spondylosis, disc herniation, and stenosis), whiplash injury, and cervical meningiomas. METHODOLOGY Following approval by the Loyola Research Institutional Review Board, a retrospective study and chart review of 133 adults diagnosed with unspecified ear pain at a tertiary-level academic medical center and seen by the senior author (JPL) between January 2002 and November 2006 was conducted. Patients were selected based on a normal otoscopic examination and given the initial diagnosis of unspecified otalgia, ICD-9 code Exclusion criteria included those patients who had undergone previous ear surgery (n 10). The distributions of all diagnosed etiologic causes for referred otalgia (n 123) with their respective nerve pathways were categorized. In addition, patients were separated into two cohorts. Group I consisted of those with referred otalgia from an etiologic source other than cervical spine disease (n 72), and Group II included those with clinical and/or radiographic evidence of cervical spine disease as the cause of their referred ear pain (n 51). A positive imaging study showing CSDD at or above C4 was assumed to be positive but did not exclude the diagnosis of CSDD based on clinical evidence. Age, gender, ethnicity, and ear pain location (right vs left) were analyzed between the two cohorts. In addition two predictors, 1) a significant past medical history of some type of rheumatologic disease, and/or 2) concomitant or recurrent neck pain, and their association with positive imaging study were analyzed in Group II. A P value less than or equal to 0.05 was selected as significant. Student paired t tests were used in testing for group differences unless the expected number in any cell was less than 5, in which case Fisher exact test was used. Statistics 6.0 from Statsoft (Tulsa, OK) was used for all tests. RESULTS The distributions of diagnosed etiologic causes for ear pain with their respective sensory innervations are shown in Table 1. All cranial and cervical ear sensory nerves are represented within our patient population, with the majority of patients experiencing subjective ear pain secondary to TMJ/dental disease (n 44, 37%) or cervical spine degenerative disease (n 45, 37%). One patient was diagnosed with psychogenic otalgia. Group I and Group II patient characteristics are outlined in Table 2. Both groups shared similar demographics, with Table 1 Distribution of referred nerve pathways and etiological causes (n 123) Referred nerve pathway, n (%) Etiological causes in referred otalgia, n (%) Auriculotemporal nerve (CN V), 56 (46%) TMJ dysfunction, 33 (28) Dental, 11 (9) Trigeminal neuralgia, 4 (3) Mandibular osteomyelitis/tumor, 4 (3) Parotid tumor/infection, 4 (3) Posterior auricular nerve (CN VII), 3 (2%) Acoustic neuroma, 2 (2) Herpes zoster, 1 (1) Jacobson s nerve (CN IX), 8 (7%) Tonsillitis/pharyngitis, 2 (2) Sinusitis, 4 (3) Pharyngeal tumor, 1 (1) Glossopharnygeal neuroma, 1 (1) Arnold s nerve (CN X), 4 (3%) LPR, 2 (2) Cricopharyngeal spasm, 1 (1) Vagal stimulator, 1 (1) Greater auricular, lesser occipital nerve (C2, C3), 51 (42%) CSDD, 45 (37) Cervical root cysts, 1 (1) Arnold-Chiari type I, 1 (1) Whiplash, 2 (2) Vascular, 1 (1) Fibromyalgia, 1 (1) Other, 1 (1%) Psychogenic, 1 (1) TMJ, temporal mandibular joint; LPR, laryngeal pharyngeal reflux; CSDD, cervical spine degenerative disease; C2,C3, cervical plexus.
4 482 Otolaryngology Head and Neck Surgery, Vol 138, No 4, April 2008 Table 2 Patient characteristics: Group I vs Group II Group I Non cervical spine causes of referred otalgia (n 72) Group II Cervical spine causes of referred otalgia (n 51) Age (y, SD)* Caucasian [n (%)] 61 (85) 44 (86) Gender [n (%)] Female 58 (81) 41 (80) Male 14 (19) 10 (20) Pain location [n (%)] Right 35 (49) 21 (41) Left 28 (39) 24 (47) Bilateral 9 (12) 6 (12) *Student s paired t test: P P value not significant between groups. the majority of patients being of Caucasian origin and of female gender (4:1, female:male) with roughly an equal distribution of subjective ear pain location experienced among the two patient populations. However, one notable difference exists between the two groups; age in Group II was shown to be statistically higher, with a mean age of vs in Group I (P 0.002, Student s paired t test). Forty-eight patients in Group II underwent diagnostic imaging of their cervical spine, with 83% (n 40) showing positive findings for some type of cervical spine pathology that can be attributed to their nonotogenic ear pain: 37, cervical spine degenerative disease (eg, disc changes and herniation, osteophytes, spinal/foramen stenosis, facet disease) with radiographic changes at C4 and above (Fig 2); 1, cervical root cyst; 1, Arnold-Chiari I; and 1, vascular, with the majority undergoing magnetic resonance imaging (85% MRI, 9% x-ray, 6% CT, Table 3). Of the eight negative imaging studies the following diagnoses were made: fibromyalgia (1), whiplash following a motor vehicle accident (2), CSDD based on clinical evidence (1), and probable CSDD with evidence of lower cervical spine pathology on imaging (4). Three patients had previously documented CSDD and did not undergo any diagnostic imaging study. With the majority of patients in Group II having a positive imaging study, subgroup analysis was warranted to elucidate pattern recognition for future diagnoses in this class of referred otalgia. Through a comprehensive retrospective chart review, including documented visits to other medical disciplines, two identifying factors appeared to correlate with a positive imaging study: 1) a significant past medical history of rheumatologic disease, eg, arthritis, certain autoimmune diseases, musculoskeletal pain disorders; Figure 2 Right foramenal stenosis (arrow) at C3 due to large osteophyte in a 69-year-old female with right-sided otalgia. Table 3 Predictors of cervical spine causes for referred otalgia (n 48)* Positive imaging [n (%)] Negative imaging [n (%)] MRI, CT, or x-ray All (n 48) 40 (83) 8 (17) CSDD (n 42) 37 (88) 5 (12) Significant medical history All ( ) history 28 (88) 4 (12) ( ) history 12 (75) 4 (25) CSDD ( ) history 28 (97) 1 (3) ( ) history 9 (69) 4 (31) Neck pain All ( ) pain 32 (89) 4 (11) ( ) pain 8 (67) 4 (33) CSDD ( ) pain 30 (97) 1 (3) ( ) pain 7 (64) 4 (36) *Three patients had previously documented CSDD and did not undergo imaging. All tests were conducted using Fisher exact P, two-tailed. CSDD, cervical spine degenerative disease; cervical degeneration at C4 or above positive. P P P P and 2) concomitant or recurrent neck pain on physical exam. Of those Group II patients who had a significant past medical history or neck pain, 88% (n 28) and 89% (n 32),
5 Jaber et al Cervical spine causes for referred otalgia respectively, were found to have a positive imaging study. Although these predictors correlated with a positive imaging study, there was no statistical significance observed in this group (P 0.41, significant history; and P 0.09, neck pain, Fisher exact test, two-tailed). However, when the six non-csdd patients were removed and a subgroup analysis was conducted, a statistically significant association was demonstrated between a positive imaging study and a significant medical history (97%, P 0.02) and/or neck pain (97%, P 0.01). Cervical spine physical therapy (CSPT) was recommended to all patients diagnosed with CSDD (n 45, radiographic or clinical). Follow-up and compliance was difficult and consequently documentation for only 20 patients could be obtained. Nonetheless, all 20 individuals expressed subjective pain relief following CSPT. DISCUSSION Despite published awareness regarding the many potential causes of referred otalgia, diagnosis often eludes the most experienced physician. 11 This may be due, in part, to the complex neuroanatomic innervation of the ear, head, and neck, and therefore the inherent limitless sources for referred ear pain. Two cohorts were categorized in this study, Group I (non cervical spine causes of referred otalgia) and Group II (cervical spine causes), in which we documented no fewer than 23 causes of referred otalgia representing all five nerve pathways (vide infra), with women reporting otalgia 4 times more frequently than men. These causes ranged from the benign etiology of whiplash (cervical spine nerves) to the more serious mandibular tumor (CN V). The two most common nerve pathways for secondary otalgia were the trigeminal nerve (n 56, 46%) and the superior cervical plexus nerves (n 51, 42%). The most common etiology in Group I was TMJ dysfunction and in Group II, CSDD. Due to the length and extensive distribution of the trigeminal nerve, it is not surprising that this nerve is most commonly involved in referred otalgia. This type of nonotogenic ear pain, especially involving disorders of the temporal mandibular joint, is well documented throughout oral surgery, otolaryngology, and pain journals Surprisingly, one group of patients with nonotogenic otalgia often overlooked are those diagnosed with cervical spine sources, in particular CSDD. 9,15 Referred otalgia due to cervical spine disease usually is described as retroauricular or infra-auricular pain, which is constant and often related to changes in neck position. As the population in America ages, CSDD in the elderly will begin to emerge as a major etiological source for referred ear pain. A case report has been published implicating cervical spine arthritis with ear pain, which improved with injection of the facet joint using a local anestheticcorticosteroid solution. 9 In this current study we have shown that CSDD, diagnosed either through radiographic or clinical evidence, is a major contributor to referred otalgia. CSDD-referred otalgia represented 37% of our patient population and was shown to be statistically higher in an elderly population (Group I vs Group II, P 0.002). Imaging studies evaluate anatomy, rather than function, and are prone to false-positive and false-negative results. For example, Boden s cervical MR study cites abnormalities in nearly 20% of asymptomatic subjects. 16 Consequently, results of imaging studies must be interpreted within the context of each clinical case, with the converse being equally valid. Although both clinical and radiographic evidence were used to support the diagnosis of referred otalgia from cervical spine causes (Group II), we also analyzed Group II independently for positive predictors in only those who had undergone imaging studies implicating cervical spine causes for referred otalgia. After ruling out non cervical spine causes of referred ear pain, a targeted medical history of some type of rheumatological disease, recurrent or concomitant neck pain coupled with a normal otologic exam highly correlated with a positive imaging study of CSDD (P 0.02, rheumatologic disease; P 0.01, neck pain). Kuttila et al have also described an association of several predictors, including and not limited to neck pain, general arthrosis, bruxism, age, and active need for TMJ disease treatment, with secondary otalgia in an adult population. 17 Similar to this study, they reported that women presented with otalgia more often than men. This published report very nicely outlines several general predictors in secondary otalgia similar to our observations but falls short in implicating cervical spine causes as a cause of ear pain. The authors of this report believe that CSDD-referred otalgia is propagated through disease of the cervical vertebrae and therefore is postural. This ear pain can be ameliorated with physical therapy, and most studies support conservative treatment, such as cervicothoracic stabilization programs, combined with aerobic conditioning in treating cervical spine disorders. 18,19 With this in mind, we recommended outpatient physical therapy to all our patients with CSDD-referred otalgia. Although documentation could be ascertained for only 20 patients, all patients reported subjective pain relief. A prospective study is currently underway at our institution to further assess the long-term effects of CSPT for the treatment of referred otalgia due to degenerative changes in this anatomic location. With the current study data in hand, a diagnostic and treatment algorithm can be proposed and is outlined in Figure 3. If a female greater than 60 years of age with persistent otalgia and a negative otolaryngologic and dental work-up presents with similar characteristics outlined in this study, ie, rheumatologic disease and/or neck pain, a CT or MRI of the cervical spine has
6 484 Otolaryngology Head and Neck Surgery, Vol 138, No 4, April 2008 Figure 3 Diagnostic and treatment algorithm for cervical spine degenerative disease referred otalgia. been shown to implicate degenerative changes as a source for her ear pain. In that case CSPT is indicated as a conservative and effective treatment strategy. CONCLUSION The complex sensory innervation of the ear and the many etiological factors that can elicit nonotogenic ear pain may result in a diagnostic challenge. Elderly citizens aged 65 and over constitute over 13% of the United States population and as a consequence cervical spine degenerative diseases in the elderly will begin to emerge as a major etiological source for referred ear pain. Our review clearly shows that with a targeted medical history and physical examination, one can use directed studies to elucidate the cause of pain as being secondary to CSDD. Conservative medical management involving cervical spine physical therapy can help improve or eliminate this type of referred otalgia. A prospective pilot study is currently underway to assess the current treatment strategy. AUTHOR INFORMATION From Loyola University Medical Center, Department of Otolaryngology Head and Neck Surgery (Drs Jaber and Leonetti), Maywood, IL; Loyola University Chicago, Stritch School of Medicine (Ms Lawrason), Chicago, IL; and the Center for Neuropharmacology and Neuroscience (Dr Feustel), Albany Medical College. Corresponding author: John P. Leonetti, MD, Loyola University Medical Center, Department of Otolaryngology-Head and Neck Surgery, 2160 S. First Ave, Maguire Building, Maywood, IL address: jleonet@lumc.edu. AUTHOR CONTRIBUTIONS John P. Leonetti, major author, original designer of study, clinician; James J. Jaber, chart review, analysis, and majority author; Amy Lawrason, chart review, minor author; Paul J. Feustel, statistical analysis, minor author. FINANCIAL DISCLOSURE None. REFERENCES 1. Shah RK, Blevins NH. Otalgia. Otolaryngol Clin North Am 2003;36: Olsen KD. The many causes of otalgia. Infection, trauma, cancer. Postgrad Med 1986;80:50 2., 55 6, Thaller SR. Otalgia with a normal ear. Am Fam Physician 1987;36:
7 Jaber et al Cervical spine causes for referred otalgia Powers WH, Britton BH. Nonotogenic otalgia: diagnosis and treatment. Am J Otol 1980;2: Kreisberg MK, Turner J. Dental causes of referred otalgia. Ear Nose Throat J 1987 Oct;66: Leonetti JP, Li J, Donzelli J. Otalgia in a normal appearing ear [poster]. Otolaryngol Head Neck Surg 117:P Scarbrough TJ, Day TA, Williams TE, et al. Referred otalgia in head and neck cancer: a unifying schema. Am J Clin Oncol 2003;26:e Yanagisawa K, Kveton JF. Referred otalgia. Am J Otolaryngol 1992; 13: Tamer TJ. Ear pain due to cervical spine arthritis: treatment with cervical facet injection. Headache 199;31: Wazen JJ. Referred otalgia. Otolaryngol Clin North Am 1989;22: Janetta PJ. Pain problems of significance in the head and face, some of which often are misdiagnosed. Curr Probl Surg 1973; Keersmaekers K, De Boever JA, Van Den Berghe L. Otalgia in patients with temporomandibular joint disorders. J Prosthet Dent 1996; 75: Kuttila S, Kuttila M, Le Bell Y, et al. Aural symptoms and signs of temporomandibular disorder in association with treatment need and visits to physician. Laryngoscope 1999;109: Ciancaglini R, Loreti P, Radalli G. Ear, nose and throat symptoms in patients with TMD: the association of symptoms according to severity of arthropathy. J Orofac Pain 1994;8: Danish, SF, Zager EL. Cervical spine meningioma presenting as otalgia: case report. Neurosurgery 2005;56(3):E Boden SD, McCowin PR, Davis DO, et al. Abnormal magneticresonance scans of the cervical spine in asymptomatic subjects. A prospective investigation. J Bone Joint Surg Am 1990;72: Kuttila SJ, Kuttila MH, Niemi PM, et al. Arch Otolaryngol Head Neck Surg 2001;127: Saal JS, Saal JA, Yurth EF. Nonoperative management of herniated cervical intervertebral disc with radiculopathy. Spine 1996;21: Grant RN, McKenzie RA. Mechanical diagnosis and therapy for cervical and thoracic spine. In: Grant R, editor. Physical therapy of the cervical and thoracic spine. New York: Churchill Livingstone; p
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
HEADACHES AND THE THIRD OCCIPITAL NERVE
 HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies
 Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
Autonomic Nervous System of the Neck. Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW
 Autonomic Nervous System of the Neck Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW Autonomic nervous system sympathetic parasympathetic enteric Autonomic
Autonomic Nervous System of the Neck Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW Autonomic nervous system sympathetic parasympathetic enteric Autonomic
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Neck Pain Overview Causes, Diagnosis and Treatment Options
 Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
TMJ. Problems. Certain headaches and pain in. the ear, jaw, neck, tooth, and. sinus can be the result of a. temporomandibular joint (TMJ)
 DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
On Cervical Zygapophysial Joint Pain After Whiplash. Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199
 On Cervical Zygapophysial Joint Pain After Whiplash 1 Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199 Nikolai Bogduk, MD, PhD FROM ABSTRACT Objective To summarize the evidence that implicates
On Cervical Zygapophysial Joint Pain After Whiplash 1 Spine December 1, 2011; Volume 36, Number 25S, pp S194 S199 Nikolai Bogduk, MD, PhD FROM ABSTRACT Objective To summarize the evidence that implicates
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report
 Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Image. 3.11.3 SW Review the anatomy of the EAC and how this plays a role in the spread of tumors.
 Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California.
 Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California. In this issue, we focus on a 23-year-old female patient referred by her
Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California. In this issue, we focus on a 23-year-old female patient referred by her
Whiplash and Whiplash- Associated Disorders
 Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
CERVICAL SPONDYLOSIS
 CERVICAL SPONDYLOSIS Dr. Sahni B.S Dy. Chief Medical Officer, ONGC Hospital Panvel-410221,Navi Mumbai,India Introduction The cervical spine consists of the top 7 vertebrae of the spine. These are referred
CERVICAL SPONDYLOSIS Dr. Sahni B.S Dy. Chief Medical Officer, ONGC Hospital Panvel-410221,Navi Mumbai,India Introduction The cervical spine consists of the top 7 vertebrae of the spine. These are referred
Cranial Nerve I Name: Foramen: Fiber Type: Function: Branches: Embryo:
 Cranial Nerve I Olfactory nerve Cribiform plate Special sensory Olfactory bulbs, Smell Olfactory filaments CNS (ectoderm) cribiform plate sensory = Cranial Nerve II Other: Optic nerve Optic canal Special
Cranial Nerve I Olfactory nerve Cribiform plate Special sensory Olfactory bulbs, Smell Olfactory filaments CNS (ectoderm) cribiform plate sensory = Cranial Nerve II Other: Optic nerve Optic canal Special
Differential Diagnosis of Craniofacial Pain
 1. Differential Diagnosis of Craniofacial Pain 2. Headache Page - 1 3. International Headache Society International Classification... 4. The Primary Headaches (1-4) Page - 2 5. The Secondary Headaches
1. Differential Diagnosis of Craniofacial Pain 2. Headache Page - 1 3. International Headache Society International Classification... 4. The Primary Headaches (1-4) Page - 2 5. The Secondary Headaches
Pain Management Top Diagnosis Codes (Crosswalk)
 Pain Management Top s (Crosswalk) 274.00 Gout arthropathy, M1000 Idiopathic gout, unspecified site unspecified M10011 Idiopathic gout, right shoulder M10012 Idiopathic gout, left shoulder M10019 Idiopathic
Pain Management Top s (Crosswalk) 274.00 Gout arthropathy, M1000 Idiopathic gout, unspecified site unspecified M10011 Idiopathic gout, right shoulder M10012 Idiopathic gout, left shoulder M10019 Idiopathic
ARTICLES. Prevalence of Herniated Intervertebral Discs of the Cervical Spine in Asymptomatic Subjects Using MRI Scans: A Qualitative Systematic Review
 Please note that this electronic prepublication galley may contain typographical errors and may be missing artwork, such as charts, photographs, etc. Pagination in this version will differ from the published
Please note that this electronic prepublication galley may contain typographical errors and may be missing artwork, such as charts, photographs, etc. Pagination in this version will differ from the published
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ)
 The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
Whiplash Associated Disorder
 Whiplash Associated Disorder The pathology Whiplash is a mechanism of injury, consisting of acceleration-deceleration forces to the neck. Mechanism: Hyperflexion/extension injury Stationary vehicle hit
Whiplash Associated Disorder The pathology Whiplash is a mechanism of injury, consisting of acceleration-deceleration forces to the neck. Mechanism: Hyperflexion/extension injury Stationary vehicle hit
Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy
 Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
Headaches + Facial pain
 Headaches + Facial pain Introduction: Each of us experienced sporadically/ chronically headache 40% worldwide population suffers with severe, disabling headache at least annually Common ailment Presenting
Headaches + Facial pain Introduction: Each of us experienced sporadically/ chronically headache 40% worldwide population suffers with severe, disabling headache at least annually Common ailment Presenting
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
NON SURGICAL SPINAL DECOMPRESSION. Dr. Douglas A. VanderPloeg
 NON SURGICAL SPINAL DECOMPRESSION Dr. Douglas A. VanderPloeg CONTENTS I. Incidence of L.B.P. II. Anatomy Review III. IV. Disc Degeneration, Bulge, and Herniation Non-Surgical Spinal Decompression 1. History
NON SURGICAL SPINAL DECOMPRESSION Dr. Douglas A. VanderPloeg CONTENTS I. Incidence of L.B.P. II. Anatomy Review III. IV. Disc Degeneration, Bulge, and Herniation Non-Surgical Spinal Decompression 1. History
ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015
 Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
SpineFAQs. Whiplash. What causes this condition?
 SpineFAQs Whiplash Whiplash is defined as a sudden extension of the cervical spine (backward movement of the neck) and flexion (forward movement of the neck). This type of trauma is also referred to as
SpineFAQs Whiplash Whiplash is defined as a sudden extension of the cervical spine (backward movement of the neck) and flexion (forward movement of the neck). This type of trauma is also referred to as
Diagnosis and Management for Chronic Back Pain: Critical for your Recovery
 Diagnosis and Management for Chronic Back Pain: Critical for your Recovery Dr. Connie D Astolfo, DC, PhD (candidate) In past articles I have stressed that the causes of back pain can be very complex. This
Diagnosis and Management for Chronic Back Pain: Critical for your Recovery Dr. Connie D Astolfo, DC, PhD (candidate) In past articles I have stressed that the causes of back pain can be very complex. This
Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis
 Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis 1 Mason Hohl, MD FROM ABSTRACT: Journal of Bone and Joint Surgery (American) December 1974;56(8):1675-1682 Five years
Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis 1 Mason Hohl, MD FROM ABSTRACT: Journal of Bone and Joint Surgery (American) December 1974;56(8):1675-1682 Five years
Herniated Disk. This reference summary explains herniated disks. It discusses symptoms and causes of the condition, as well as treatment options.
 Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
.org. Cervical Radiculopathy (Pinched Nerve) Anatomy. Cause
 Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Careful Coding: Headaches
 Dynamic Chiropractic March 26, 2012, Vol. 30, Issue 07 Careful Coding: Headaches By K. Jeffrey Miller, DC, DABCO and Ray Tuck, DC Because s are among the most common reasons for seeking chiropractic care,
Dynamic Chiropractic March 26, 2012, Vol. 30, Issue 07 Careful Coding: Headaches By K. Jeffrey Miller, DC, DABCO and Ray Tuck, DC Because s are among the most common reasons for seeking chiropractic care,
How To Treat Pain With Pain Management
 SUTTER PHYSICIANS ALLIANCE (SPA) 2800 L Street, 7 th Floor Sacramento, CA 95816 SPA PCP Treatment & Referral Guidelines Pain Management Developed June 1, 2003 Revised - (Format Revisions) November 13,
SUTTER PHYSICIANS ALLIANCE (SPA) 2800 L Street, 7 th Floor Sacramento, CA 95816 SPA PCP Treatment & Referral Guidelines Pain Management Developed June 1, 2003 Revised - (Format Revisions) November 13,
Colossus Important Diagnoses. Instructions for How to List Diagnoses
 1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
Discogenic Low Backache A clinical and MRI correlative study A DISSERTATION SUBMITTED TO UNIVERSITY OF SEYCHELLES AMERICAN INSTITUTE OF MEDICINE
 Discogenic Low Backache A clinical and MRI correlative study A DISSERTATION SUBMITTED TO UNIVERSITY OF SEYCHELLES AMERICAN INSTITUTE OF MEDICINE IN PARTIAL FULFILLMENT OF THE REGULATIONS FOR THE AWARD
Discogenic Low Backache A clinical and MRI correlative study A DISSERTATION SUBMITTED TO UNIVERSITY OF SEYCHELLES AMERICAN INSTITUTE OF MEDICINE IN PARTIAL FULFILLMENT OF THE REGULATIONS FOR THE AWARD
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
How To Get An Mri Of The Lumbar Spine W/O Contrast
 Date notice sent to all parties: May 27, 2014 IRO CASE #: ReviewTex, Inc. 1818 Mountjoy Drive San Antonio, TX 78232 (phone) 210-598-9381 (fax) 210-598-9382 reviewtex@hotmail.com Notice of Independent Review
Date notice sent to all parties: May 27, 2014 IRO CASE #: ReviewTex, Inc. 1818 Mountjoy Drive San Antonio, TX 78232 (phone) 210-598-9381 (fax) 210-598-9382 reviewtex@hotmail.com Notice of Independent Review
Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase
 Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase The MedStar Spine Center in Chevy Chase Relief from Pain, Restoration of Function Non-surgical, Minimally Invasive and Complex Surgical
Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase The MedStar Spine Center in Chevy Chase Relief from Pain, Restoration of Function Non-surgical, Minimally Invasive and Complex Surgical
*A discrete, hypersensitive nodule within tight band of muscle or fascia that present with classic pattern of pain referral that does not follow
 A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
LOW BACK PAIN; MECHANICAL
 1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Magnetic Resonance Imaging
 Magnetic Resonance Imaging North American Spine Society Public Education Series What Is Magnetic Resonance Imaging (MRI)? Magnetic resonance imaging (MRI) is a valuable diagnostic study that has been used
Magnetic Resonance Imaging North American Spine Society Public Education Series What Is Magnetic Resonance Imaging (MRI)? Magnetic resonance imaging (MRI) is a valuable diagnostic study that has been used
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
DAMAGING EFFECTS OF FORWARD HEAD POSTURE
 DAMAGING EFFECTS OF FORWARD HEAD POSTURE The effect of posture on health is becoming more evident. Spinal pain, headache, mood, blood pressure, pulse and lung capacity are among the functions most easily
DAMAGING EFFECTS OF FORWARD HEAD POSTURE The effect of posture on health is becoming more evident. Spinal pain, headache, mood, blood pressure, pulse and lung capacity are among the functions most easily
THE TMJ TREATMENT CENTER
 THE TMJ TREATMENT CENTER TEMPOROMANDIBULAR JOINT DISORDERS, CRANIOFACIAL DISORDERS, CERVICOCRANIAL INSTABILITY & EHLERS-DANLOS SYNDROME ABOUT DR. MITAKIDES & THE TMJ TREATMENT CENTER Dedicated to the diagnosis
THE TMJ TREATMENT CENTER TEMPOROMANDIBULAR JOINT DISORDERS, CRANIOFACIAL DISORDERS, CERVICOCRANIAL INSTABILITY & EHLERS-DANLOS SYNDROME ABOUT DR. MITAKIDES & THE TMJ TREATMENT CENTER Dedicated to the diagnosis
https://www.laserspineinstitute.com/back_problems/foraminal_stenosis/e...
 Questions? Call toll free 1-866-249-1627 Contact us today. We're here for you seven days a week. MRI Review Consultation Live help Call 1-866-249-1627 Chat Live Home Laser Spine Institute Laser Spine Institute's
Questions? Call toll free 1-866-249-1627 Contact us today. We're here for you seven days a week. MRI Review Consultation Live help Call 1-866-249-1627 Chat Live Home Laser Spine Institute Laser Spine Institute's
Angela Wilkin May 2013
 Angela Wilkin May 2013 Upper Motor Neuron v Lower Motor Neuron Lesions UMN Lesion LMN Lesion Forehead usually unaffected (bilateral innervation) Forehead affected Contralateral side Ipsilateral side Often
Angela Wilkin May 2013 Upper Motor Neuron v Lower Motor Neuron Lesions UMN Lesion LMN Lesion Forehead usually unaffected (bilateral innervation) Forehead affected Contralateral side Ipsilateral side Often
CMS Imaging Efficiency Measures Included in Hospital Outpatient Quality Data Reporting Program (HOP QDRP) 2009
 CMS Imaging Efficiency Measures Included in Hospital Outpatient Quality Data Reporting Program (HOP QDRP) 2009 OP 8: MRI LUMBAR SPINE FOR LOW BACK PAIN Measure Description: This measure estimates the percentage
CMS Imaging Efficiency Measures Included in Hospital Outpatient Quality Data Reporting Program (HOP QDRP) 2009 OP 8: MRI LUMBAR SPINE FOR LOW BACK PAIN Measure Description: This measure estimates the percentage
Standard of Care: Cervical Radiculopathy
 Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve,
 Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve, Larynx, Trachea, & Esophageal Management Robert C. Wang,
Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve, Larynx, Trachea, & Esophageal Management Robert C. Wang,
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, The Cervical Spine. What is the Cervical Spine?
 Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Sinus Headache vs. Migraine
 Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
ICD-9-CM coding for patients with Spinal Cord Injury*
 ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE
 TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
Cervical Traction. Distinguishing Features and Benefits 2. Cervical Traction Frequently Asked Questions 2
 Cervical Traction Distinguishing Features and Benefits 2 Cervical Traction Frequently Asked Questions 2 Evidence for Saunders Cervical Traction Protocols in Peer-Reviewed Literature 5 Peer Reviewed Article
Cervical Traction Distinguishing Features and Benefits 2 Cervical Traction Frequently Asked Questions 2 Evidence for Saunders Cervical Traction Protocols in Peer-Reviewed Literature 5 Peer Reviewed Article
Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries
 1 Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries J Bone Joint Surg (Br) 2001 Mar;83(2):226-9 Ide M, Ide J, Yamaga M, Takagi K Department of Orthopaedic Surgery, Kumamoto University
1 Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries J Bone Joint Surg (Br) 2001 Mar;83(2):226-9 Ide M, Ide J, Yamaga M, Takagi K Department of Orthopaedic Surgery, Kumamoto University
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Options for Cervical Disc Degeneration A Guide to the M6-C. clinical study
 Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Electrodiagnostic Testing
 Electrodiagnostic Testing Electromyogram and Nerve Conduction Study North American Spine Society Public Education Series What Is Electrodiagnostic Testing? The term electrodiagnostic testing covers a
Electrodiagnostic Testing Electromyogram and Nerve Conduction Study North American Spine Society Public Education Series What Is Electrodiagnostic Testing? The term electrodiagnostic testing covers a
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
X-Plain Temporomandibular Joint Disorders Reference Summary
 X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Spinal Decompression
 Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Hitting a Nerve: The Triggers of Sciatica. Bruce Tranmer MD FRCS FACS
 Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
First Year. PT7040- Clinical Skills and Examination II
 First Year Summer PT7010 Anatomical Dissection for Physical Therapists This is a dissection-based, radiographic anatomical study of the spine, lower extremity, and upper extremity as related to physical
First Year Summer PT7010 Anatomical Dissection for Physical Therapists This is a dissection-based, radiographic anatomical study of the spine, lower extremity, and upper extremity as related to physical
Basic Cranial Nerve Examination
 Basic Cranial Nerve Examination WIPE Wash hands Introduce yourself Permission Position (Patient sitting facing you, maintain comparable eye level) Exposure (Face exposed only, i.e. remove hats etc) Identify
Basic Cranial Nerve Examination WIPE Wash hands Introduce yourself Permission Position (Patient sitting facing you, maintain comparable eye level) Exposure (Face exposed only, i.e. remove hats etc) Identify
ICD-10 Cheat Sheet Frequently Used ICD-10 Codes for Musculoskeletal Conditions *
 ICD-10 Cheat Sheet Frequently Used ICD-10 Codes for Musculoskeletal Conditions * Finding the ICD-10 equivalent for an ICD-9 code can be a challenge. This resource of frequently used codes can help when
ICD-10 Cheat Sheet Frequently Used ICD-10 Codes for Musculoskeletal Conditions * Finding the ICD-10 equivalent for an ICD-9 code can be a challenge. This resource of frequently used codes can help when
Intra-operative Nerve Monitoring Coding Guide. March 1, 2011
 Intra-operative Nerve Monitoring Coding Guide March 1, 2011 Please direct any questions to: Patty Telgener, RN Vice President, Reimbursement Services Emerson Consultants (303) 526-7604 (office) (303) 570-2159
Intra-operative Nerve Monitoring Coding Guide March 1, 2011 Please direct any questions to: Patty Telgener, RN Vice President, Reimbursement Services Emerson Consultants (303) 526-7604 (office) (303) 570-2159
Objectives AXIAL SKELETON. 1. Frontal Bone. 2. Parietal Bones. 3. Temporal Bones. CRANIAL BONES (8 total flat bones w/ 2 paired)
 Objectives AXIAL SKELETON SKULL 1. On a skull or diagram, identify and name the bones of the skull 2. Identify the structure and function of the bones of the skull 3. Describe how a fetal skull differs
Objectives AXIAL SKELETON SKULL 1. On a skull or diagram, identify and name the bones of the skull 2. Identify the structure and function of the bones of the skull 3. Describe how a fetal skull differs
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Level IA: Submental Group
 IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Fig. 1 The level system is used for describing the location of lymph nodes in the neck: Level I, submental and submandibular group; Level II, upper jugular
IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Fig. 1 The level system is used for describing the location of lymph nodes in the neck: Level I, submental and submandibular group; Level II, upper jugular
Spinal Anatomy. * MedX research contends that the lumbar region really starts at T-11, based upon the attributes of the vertebra.
 Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Instability concept. Symposium- Cervical Spine. Barcelona, February 2014
 Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
MD 2016. Back Muscles & Movements Applied Anatomy. A/Prof Chris Briggs Anatomy & Neuroscience
 MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
Upper Cervical Spine - Occult Injury and Trigger for CT Exam
 Upper Cervical Spine - Occult Injury and Trigger for CT Exam Bakman M, Chan K, Bang C, Basu A, Seo G, Monu JUV Department of Imaging Sciences University of Rochester Medical Center, Rochester, NY Introduction
Upper Cervical Spine - Occult Injury and Trigger for CT Exam Bakman M, Chan K, Bang C, Basu A, Seo G, Monu JUV Department of Imaging Sciences University of Rochester Medical Center, Rochester, NY Introduction
Online Course Descriptions (degree seeking):
 Online Course Descriptions (degree seeking): BSC 6001 Foundations of Clinical Orthopaedics This is an online self study course discussing the foundations of orthopaedics and manipulative therapy. The history
Online Course Descriptions (degree seeking): BSC 6001 Foundations of Clinical Orthopaedics This is an online self study course discussing the foundations of orthopaedics and manipulative therapy. The history
Dr. Brendan Stack Orthodontist, DDS, MS Washington, DC
 Dr. Brendan Stack Orthodontist, DDS, MS Washington, DC Dr. Stack is a University trained orthodontist (Georgetown University) who, since 1965, has limited his practice in Northern Virginia (Washington,
Dr. Brendan Stack Orthodontist, DDS, MS Washington, DC Dr. Stack is a University trained orthodontist (Georgetown University) who, since 1965, has limited his practice in Northern Virginia (Washington,
Whiplash injuries can be visible by functional magnetic resonance imaging. Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp.
 Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
The Lewin Group undertook the following steps to identify the guidelines relevant to the 11 targeted procedures:
 Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
Oh, 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8
 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
A Look at Two Syndromes:
 TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
24, 2006 RESIDENT PHYSICIAN:
 TITLE: Regional Anesthesia in Head and Neck Surgery SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: May 24, 2006 RESIDENT PHYSICIAN: Jacques Peltier, MD FACULTY ADVISOR: Francis
TITLE: Regional Anesthesia in Head and Neck Surgery SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: May 24, 2006 RESIDENT PHYSICIAN: Jacques Peltier, MD FACULTY ADVISOR: Francis
