Role of FDG PET and PET/CT Imaging in Indeterminate Pulmonary Nodules and Lung Cancer
|
|
|
- Ilene Watkins
- 8 years ago
- Views:
Transcription
1 Role of FDG PET and PET/CT Imaging in Indeterminate Pulmonary Nodules and Lung Cancer Dominique Delbeke, MD, PhD Vanderbilt University Medical Center Nashville, Tennessee Congreso Chileno de Medicina Nuclear, Santiago, Chile Noviembre 2008
2 Outline PET/CT protocols Indeterminate lung nodules Lung cancer Staging Monitoring therapy Restaging Mesothelioma Small cell carcinoma Impact on radiation therapy planning
3 Integrated PET/CT Imaging System Benefit of the combined technique: 1) Attenuation correction with CT 2) Anatomical localization PET CT Discovery LS (GE Healthcare) Anatomical localization Attenuation Correction
4 Integrated PET/CT Systems: Protocols Field of view: base of skull to mid-thigh When When clinical relevant Include extremities and/or brain Limited field of view for SPN Patient positioning: Arms-up Optimal CT protocols: mas? IV IV contrast? Breathing pattern?
5 Optimal CT protocol is still debated CT for attenuation correction: High quality maps because of high photon flux Low current (10 mas): satisfactory attenuation maps. CT for anatomical localization: Reduced ma (~80 mas) = compromise for limited radiation dose Optimized diagnostic CT: CT protocol optimized for indication IV contrast: Problems of overcorrection Great vessels Beyer T, et al. J Nucl Med 2004;45 (Suppl( Suppl): 25S Semin Ultrasound CT MR 2008; Aug 29(4).
6 Issues regarding Phase of Respiration for CT Diagnostic CT: Breath-hold hold at inspiration PET: Respiratory motion misregistration in region of diaphragm Curvilinear artifacts along diaphragm Inaccurate localization of lesion in the region of diaphragm (dome of liver versus lung bases) in 2% of patients Recommendation for transmission CT: Breath-holding holding at end tidal volume Respiratory gating Goerres GW et al. Radiology 2003;226: Osman MM et al. Eur J Nucl Med 2003;30: Osman MM et al. J Nucl Med 2003;44:
7 Lung Cancer Global epidemic estimated 3 million deaths annually associated with tobacco use Leading cause of cancer deaths in western world 215,020 new cases and 161,840 deaths in the U.S. annually (2008 data) Histological types: Non-small cell: ~80% Squamous cell Adenocarcinoma (including bronchioalveolar Large cell Small cell: ~20% Jemal et al. CA Cancer J Clin 2005;55:10
8 Evaluation of Lung Nodules Accounts for 20% of newly diagnosed lung cancer* In the US: 150,000 new SPN/year 30-50% are malignant CXR and CT: not accurate to differentiate benign from malignant non-calcified pulmonary nodules that are between cm in diameter Morphologic stability over 2 years: reliable sign of benignity: Doubling time of malignant nodules: days Doubling in volume results in 26% increase in diameter Mack MJ et al. Ann Thorac Surg 1993;56:825. Gurney JW et al. Radiology 1993;186:405.
9 Evaluation of Lung Nodules Bayesian analysis can be used to stratify risk (based on clinical information and imaging characteristics) and guide management: Probability of cancer < 5%: monitoring Probability of cancer between 5%-60%: biopsy Probability of cancer >60%: resection Mack MJ et al. Ann Thorac Surg 1993;56:825. Gurney JW et al. Radiology 1993;186:405.
10 PIOPILN Study Prospective investigation of PET in lung nodules 90 patients from 5 centers with indeterminate nodules (CT) Size range: 0.7 to 4 cm All nodules had histology: 67% were malignant PIOPLIN and other studies: SUV > 2.5 = visual Sensitivity: % Specificity: 69-95% 95% False positive: Active granuloma False negative: Bronchioalveolar,, mucinous carcinoma, carcinoid Hyperglycemia (decreases uptake by up to 50%). Lowe VJ et al. J Clin Oncol 1998;16: Nomori H et al. Lung cancer 2004;45: Herder GJ et al. Eur J Nucl Med Mol Imag 2004;31: Lowe VJ et al. J Nucl Med 1994;35: Nomori H et al. Ann Thorac Surg 2005;79:
11 Middle-aged woman with a 1.5 cm lung nodule
12 Question What should be done next? A. Follow-up B. Biopsy C. Chemotherapy D. Antibiotics
13 Question What should be done next? A. Follow-up B. Biopsy C. Chemotherapy D. Antibiotics
14 Middle-aged woman with a 1.5 cm lung nodule
15 Question What should be done next? A. Biopsy B. Reassure the patient that the nodule is benign C. Follow-up with CT at months interval for 2 years D. Follow-up with chest X-ray X in 6 months
16 Question What should be done next? A. Biopsy B. Reassure the patient that the nodule is benign C. Follow-up with CT at months intervals for 2 years D. Follow-up with chest X-ray X in 6 months
17 Middle-aged woman with an infiltrative lung nodule
18 Question What is in the differential diagnosis? A. Neuroendocrine tumor B. Bronchioalveolar carcinoma C. Infection D. All of the above
19 Question What is in the differential diagnosis? A. Neuroendocrine tumor B. Bronchioalveolar carcinoma C. Infection D. All of the above
20 Middle-aged woman with an infiltrative lung nodule Biopsy: Bronchioalveolar carcinoma (Sensitivity FDG PET ~ 50% for bronchioalveolar and carcinoid) Lee KS et al. Radiographics 1997;17: Erasmus JJ et al. AJR 1998;170:
21 Recurrent lung carcinoid Daniels CE et al. Chest 2007, 131(1):
22 48 year-old female with a remote history of early stage melanoma presented with a pulmonary mass Granuloma
23 49 year-old male presented for evaluation of known sarcoidosis Active sarcoidosis: lung, vertebral bodies Love C. et al. Radiographics 2005;25:1357
24 45-year year-old with an apical SPN and pulmonary fibrosis Diagnosis: 1) SPN was negative 2) Patchy FDG uptake in pulmonary fibrosis Alavi A et al. Semin Nucl Med 2003;32 (4):
25 Meta-Analysis of Accuracy of FDG PET for Evaluation of Pulmonary Nodules Includes 40 studies (dedicated and gamma- camera based PET) and 1,474 focal pulmonary lesions: Maximum joint sensitivity and specificity of ROC curve: 91% Practically to decrease F-, F FDG PET operates at sensitivity of 96% and specificity 78% Optimal visual criterion: Greater that mediastinal uptake for nodules > 1 cm Any uptake worrisome for smaller nodules Gould MK et al. JAMA 2001;285:
26 Diagnostic Accuracy of FDG PET and CT for the Characterization of Lung Nodule 344 patients for which definite diagnosis was obtained Prevalence of malignancy: 53% Average size: 16 mm Sensitivity Specificity ROC PET 91.7% 82.3% 0.93 CT 95.6% 40.6% 0.82 Fletcher JW et al. J Nucl Med 2008;49 (2):
27 ROC Meta-Analysis of Accuracy of Cross-sectional sectional Imaging for Evaluation of Pulmonary Nodules 40 studies between Jan 1990 and Dec 2005 Sensitivity Specificity PPV NPV Odds ratio Dynamic CT 93% 76% 80% 95% Dynamic MRI 94% 79% 86% 93% Cronin P et al. Radiology 2008;246 (3): FDG PET 95% 82% 91% 90% mTc- depreotide 95% 82% 90% 91%
28 How about small nodules? 66 year-old female referred for evaluation of a 8 mm SPN
29 Small Pulmonary nodules Early Lung Cancer Action Project (ELCAP) CT screening study : Non-calcified nodules < 5 mm are rarely malignant Annual repeat screening is recommended Phantom-study: detection of nodules < 7 mm is unreliable Screening CT study on 911 patients 14% had non-calcified nodules > 5 mm 3.6% had non-calcified nodules > 10 mm Follow-up: 11 NSCLC (all stage I), 1 SCLC FDG PET accuracy = 76% (19/25, size range mm) FDG sensitivity = 69%, specificity = 91%, PPV = 90%, NPV = 71% Nodules > 10 mm: 95% Henschke CI et al. Radiology 2004;231: Coleman RE et al. Radiology 1999;210: Bastarrika G et al. Am J Respir Crit Care Med 2005;171:
30 ACCP Evidenced-Based Clinical Practice Guidelines: Recommendation for FDG PET PET recommended: Probability of cancer low to moderate (5%-60%) and an indeterminate nodule measures at least mm. PET NOT recommended: SPN that has a high probability of malignancy (> 60%) or nodule < mm Silvestri GA et al. Chest 2007;132:178S-201S 201S
31 T staging: : tumor size Staging NSCLC T1 < 3 cm T2 > 3 cm T3 > 3 cm with chest wall, pleural, or pericardial extension T4 with invasion of adjacent organs N staging: : nodal metastases N0: no nodes N1: ipsilateral hilar nodes N2: ipsilateral mediastinal or subcarinal nodes N3: contralateral nodes or scalene/supraclavicular nodes M Staging: : distant metastases M0: no distant metastases M1: distant metastases present
32 Regional Lymph Node Classification for Lung Cancer Staging* Clifton F. Mountain, MD, FCCP; and Carolyn M. Dresler,, MD, FCCP Recommendations for classifying regional lymph node stations for lung cancer staging have been adopted by the American Joint Committee on Cancer (AJCC) and the Union Internationale Contre le Cancer. (CHEST 1997; 111: )
33 Staging NSCLC Stage I: no nodes or mets T1 or T2; N0; M0 40% 5-year 5 survival Stage II: regional nodes T1 N1 or T2 N1 M0 20% 5-year 5 survival Stage IIIa: extrapulmonary extension T3 N0 or N1; T1-3 3 N2 15% 5-year 5 survival Stage IIIb: more extensive mediastinal involvement T4 any N; any T N3, malignant pleural effusion 5% 5-year 5 survival; 40% 1-year 1 survival
34 FDG PET for Staging T staging: CT and MRI: best to demonstrate the extension of the tumor, relationship to adjacent organs & vessels FDG PET: limited for T staging due to poor anatomic resolution, lack of anatomical landmark. N staging: CT and MRI: limited by size criteria. FDG PET: : best to detect tumor in normal size lymph nodes M Staging: FDG PET: : detect metastases > ~7 mm when CT and MRI are normal or equivocal. Whole body technique: unsuspected metastases
35 Staging NSCLC: N-staging N critical Early stage NSCLC including ipsilateral nodal involvement: Surgical resection is the treatment of choice Accurate staging is essential for management. Study of 235 patient: If CT negative: ~20% ~20% have positive mediastinoscopy Invasive diagnostic methods remains necessary Webb WR, et al: Radiology 1991;178: De Leyn P et al. Eur J Cardiothor Surg 1997; 12:
36 Staging NSCLC: Invasive Methods Accurate assessment of malignancy has traditionally required invasive diagnostic methods Needle biopsy 10% sampling error; 15% pneumothorax Bronchoscopy low sensitivity; occasional pneumothorax Mediastinoscopy Surgical procedure; limited to anterior mediastinum Study of 859 patients: If mediastinoscopy negative: ~15% have N2 disease at thoracotomy Thoracotomy open surgery; 1-3% 1 mortality De Leyn P et al. Eur J Cardiothorac Surg 1996;10:
37 N-Staging NSCLC:FDG PET Meta-analysis analysis for FDG PET and CT: Includes 14 studies (514 patients) for FDG PET and 29 studies (2,226 patients) for CT: Sensitivity of FDG PET = 79%, CT = 60% Specificity of FDG PET = 91%, CT = 77% Prospective study of 102 patients: Sensitivity of FDG PET = 91%, CT = 75% Specificity of FDG PET = 86%, CT = 77% FDG PET detected distant metastases in 10% patients FDG PET changed the stage in 60% patients Cost effectiveness of FDG PET has been demonstrated* Dwamena BA et al. Radiology 1999;213: Peterman RM et al N Engl J Med 2000;343: *Gambhir SS, et al:j Nucl Med 1996;37:
38 ACCP Evidenced-Based Practice Guidelines FDG PET compared to CT for mediastinal Staging Silvestri GA et al. Chest 2007;132:178S-201S 201S
39 ACCP Evidenced-Based Clinical Practice Guidelines: Recommendations for FDG PET Stage IA being treated with curative intend Stage IB-IIIB IIIB treated with curative intend If PET is abnormal, biopsy is recommended Silvestri GA et al. Chest 2007;132:178S-201S 201S
40 66 year-old with right hilar mass Primary lung ca with atelectasis AP window LN
41 66 year-old with right hilar mass
42 Staging NSCLC: FDG PET Stage IV: Distant metastases Common metastases to adrenals, skeleton, liver, brain. FDG PET is superior to conventional imaging: Detect unsuspected distant metastases: ~13% of patients Stage I: 7.5% Stage II: 18% Stage III: 24% Change management: 18% of these Peterman RM et al N Engl J Med 2000;343: Baum RP et al. Q J Nucl Med 2004;48:
43 Staging NSCLC: FDG PET Stage IV: Indeterminate Adrenal Masses Patients with malignancy: ~ 30% are malignant. Patients without known malignancy: rarely malignant. Contrast-CT CT with delayed washout images and MRI with T2-weighted images: accurate but requires additional imaging FDG PET: high accuracy Study of 27 patients with NSCLC: Sensitivity = 100%, specificity = 80% Boland GW et al. Radiology 1995;194: Erasmus JJ et al. AJR 1997;168:
44 63-year year-old male with newly diagnosed lung ca Lung cancer and mediastinal metastasis Left adrenal metastasis Left vocal cord paralysis Urine diversion in ileal loop From Delbeke D. Diagnostic Imaging 2003
45 Staging NSCLC: FDG PET Stage IV: Detection of Skeletal Metastases 110 patients comparing bone scintigraphy and FDG PET 43 patients with metastases, 21 of which with bone metastases proven with other imaging studies or biopsy Modality PPV NPV Acc BS 90% 61% 66% FDG PET 90% 98% 96% Specificity PET (95%) > BS (61%) FDG PET better for lytic metastases Bone scintigraphy better for blastic metastases Bury T et al. Eur J Nucl Med 1998;25:
46 50 year-old female with lung cancer Pleural metastasis Rib metastasis Sacral metastasis
47 Staging NSCLC: FDG PET Stage IV: Detection of Cerebral Metastases Cerebral cortex uses only glucose as substrate high background uptake in cortex Metastases can hyper-,, iso- or hypometabolic compared to cortex:~ 60% are easily detectable on FDG PET images MRI is the standard of care for evaluation of brain metastases Study of 1,026 oncology patients: Abnormal findings: 3.9 % Unsuspected metastases: 0.4% Ludwig V et al. Mol Imag Biol 2002;4:
48 Staging Lung Cancer: PET/CT versus PET or CT Prospective analysis of 49 consecutive patients with NSCLC Conventional staging vs PET + CT vs integrated PET-CT Surgery in 40/49 (82%) Integrated PET-CT provided additional info in 20/49 (41%) Location of LN s s in 9 patients Accurate determination of chest wall infiltration in 3 Accurate determination of mediastinal invasion in 3 Differentiation of tumor vs atelectasis/inflammation in 7 Location of distant metastases in 2 Lardinois D et al. N Engl J Med 2003;348:
49 FDG PET in The Preoperative Assessment of NSCLC: The PLUS Multicenter Randomized Trial 188 patients from 9 hospitals were randomized to Conventional work-up (CWU) CWU + PET End point: futile (unnecessary) thoracotomy Results CWU: 41% futile thoracotomy CWU + PET: 21% futile thoracotomy Decrease of unnecessary surgery by 50% Decrease cost of healthcare! Van Tinteren H et al. Lancet 2002;359 (9315):
50 Detection of Unknown Primary FDG PET In a study of 44 patients presenting with cervical metastasis FDG PET detected the primary tumor in 34% (15/44) of patients, 7 (47%) of which were in the lung. Bohuslavizki et al. J Nucl Med 2000;41:
51 Carcinoma of unknown primary metastatic to the liver NSCLC mistaken for esophagus on CT From: Delbeke D et al (eds( eds): Practical FDG Imaging: A teaching File Springer-Verlag 2002.
52 Mesothelioma: FDG PET FDG-avid Change in clinical stage (15 patients) Upstage: 13% Downstage: 27% Change in management: 20% Study of 29 patient Major impact on M-stagingM Prognosis SUV > 4: 3 times higher risk of death Nanni C et al. Cancer Biother Radiopharm 2004; Erasmuss JJ et al. J Thorac Cardiovasc Surg 2005;129: Flores RM et al. Lung Cancer 2005;49 (suppl( suppl): S27-S32. S32.
53 Small Cell Lung Carcinoma Neuroendocrine aggressive tumor VA Lung Cancer Study Group:Two stage classification: Limited: tumor confined to unilateral chest Treatment: Chemoradiation Extensive: Contralateral or distant disease Treatment: Chemotherapy alone Change of management due to FDG PET: 8-29% 8 Abrams J et al. Semin Oncol 1988;15: Kamel EM et al. J Nucl Med 2003;44: Blum R et al. Am J Clin Oncol 2004;27: Bradley JD et al. J Clin Oncol 2004;22:
54 70 year-old male referred for initial staging of SCLC
55 Impact of PET/CT on Radiation Therapy 39 patients with various solid tumors Comparison Gross Target Volume (GTV) delineated on CT, then with PET overlay PET changed GTV in 56% of patients GTV increased by 25% or more because of PET GTV was reduced by 25% or more because of PET GTV variability between 2 independent oncologists decreased from a mean volume difference of 25 cm 3 to 9 cm 3. PET/CT change treatment from curative to palliative because of distant metastases in 16% of patients Ciernik F et al. Int J Radiation Oncol Biol Phys;2003;57:
56 PTV Changes for Lung Radiation Therapy PET overlay over CT: 1) Decreased ROI over atelectasis mistaken for tumor on CT 2) Increased ROI over metastatic mediastinal LN missed on CT Courtesy of Dr Caggiano,, Holy Name Hospital
57 FDG PET for Lung Carcinoma: Conclusions Indeterminate Pulmonary Nodule: High NPV: FDG- monitoring F+ granulomatous disease: FDG+ biopsy False bronchioalveolar and mucinous adenocarcinoma, carcinoid, small lesions Staging NSCLC: Stage I, II and III: Mediastinoscopy recommended when FDG PET is positive FDG help guide mediastinal biopsy FDG help select other invasive procedures Detection of unsuspected distant metastases: ~ 15% Impact on therapy: ~40%
58 FDG PET for Lung Carcinoma: Conclusions Monitoring therapy Early prediction of response Late after completion: Good predictor of prognosis Planning radiation therapy Potential new tracers: Hypoxia: 18 F-MISO, Cu-ATSM Cell proliferation: 18 F-FLTFLT Potential role: SCLC Mesothelioma
59 ACCP Evidenced-Based Clinical Practice Guidelines: Recommendations for FDG PET Stage IA being treated with curative intent Stage IB-IIIB IIIB treated with curative intent If PET is abnormal, biopsy is recommended Stage IIIA-IIIB: IIIB: routine imaging for extrathoracic disease with most appropriate study (see below) Patients with abnormal clinical evaluation: Site specific symptoms warrant evaluation with most appropriate study. Head CT/MRI Whole body PET Bone scintigraphy Abdominal CT Silvestri GA et al. Chest 2007;132:178S-201S 201S
60 Breast cancer Colorectal cancer Lung cancer Lymphoma Podoloff DA et al. J Natl Compr Canc Netw 2007;May;5 Suppl 1: S1-S22. S22.
61 PET/CT in NCCN Practice Guidelines Summary of Recommendations: NSCLC Recommended: Diagnosis of in patients with one or two pulmonary nodules Initial staging except if multiple distant metastases Restaging stage III and IV after 2 to 3 months after treatment or before surgery Restaging in patients with symptoms suggestive of recurrence Radiation therapy
62
63 Thank YOU!
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Thoracic 18F-FDG PETCT
 Thoracic 18F-FDG PETCT RAD Magazine, 41, 482, 13-16 Dr Allanah arker Specialist registrar radiology Dr Nagmi Qureshi Consultant cardiothoracic radiologist Papworth Hospital, Cambridge email: allanahbarker@nhs.net
Thoracic 18F-FDG PETCT RAD Magazine, 41, 482, 13-16 Dr Allanah arker Specialist registrar radiology Dr Nagmi Qureshi Consultant cardiothoracic radiologist Papworth Hospital, Cambridge email: allanahbarker@nhs.net
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
False positive PET in lymphoma
 False positive PET in lymphoma Thomas Krause Introduction and conclusion 2 3 Introduction 4 FDG-PET in staging of lymphoma 34 studies with 2227 Patients CT FDG-PET Sensitivity 63 % 89 % (58%-100%) (63%-100%)
False positive PET in lymphoma Thomas Krause Introduction and conclusion 2 3 Introduction 4 FDG-PET in staging of lymphoma 34 studies with 2227 Patients CT FDG-PET Sensitivity 63 % 89 % (58%-100%) (63%-100%)
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines
 Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Low-dose CT Imaging. Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital
 Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Practice Guidelines in Oncology. A summary of the recommendations and practice guidelines of professional groups. April 2013 EXECUTIVE SUMMARY
 18 F-fluorodeoxyglucose (FDG) PET and PET/CT Practice Guidelines in Oncology A summary of the recommendations and practice guidelines of professional groups April 2013 The recommendations and practice
18 F-fluorodeoxyglucose (FDG) PET and PET/CT Practice Guidelines in Oncology A summary of the recommendations and practice guidelines of professional groups April 2013 The recommendations and practice
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
An Update on Lung Cancer Diagnosis
 An Update on Lung Cancer Diagnosis Dr Michael Fanning MBBS FRACGP FRACP RESPIRATORY AND SLEEP PHYSICIAN Mater Medical Centre Outline Risk factors for lung cancer Screening for lung cancer Radiologic follow-up
An Update on Lung Cancer Diagnosis Dr Michael Fanning MBBS FRACGP FRACP RESPIRATORY AND SLEEP PHYSICIAN Mater Medical Centre Outline Risk factors for lung cancer Screening for lung cancer Radiologic follow-up
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
PET/CT: Basic Principles, Applications in Oncology
 PET/CT: Basic Principles, Applications in Oncology Mabel Djang, HMS III Overview PET Basics and Limitations PET/CT - Advantages and Limitations Applications of PET/CT in oncology Summary 2 Principles of
PET/CT: Basic Principles, Applications in Oncology Mabel Djang, HMS III Overview PET Basics and Limitations PET/CT - Advantages and Limitations Applications of PET/CT in oncology Summary 2 Principles of
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
PET. Can we afford PET-CT. Positron annihilation. PET-CT scanner. PET detection
 PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
Post-recurrence survival in completely resected stage I non-small cell lung cancer with local recurrence
 Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Adjuvant Therapy Non Small Cell Lung Cancer. Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015
 Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
In the last hundred years, lung cancer has risen from a
 CONTINUING EDUCATION PET Evaluation of Lung Cancer* Tira Bunyaviroch, MD 1 ; and R. Edward Coleman, MD 2 1 Boston University School of Medicine and Boston Medical Center, Boston, Massachusetts; and 2 Duke
CONTINUING EDUCATION PET Evaluation of Lung Cancer* Tira Bunyaviroch, MD 1 ; and R. Edward Coleman, MD 2 1 Boston University School of Medicine and Boston Medical Center, Boston, Massachusetts; and 2 Duke
PET/CT in Breast Cancer
 PET/CT in Breast Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria Overview Introduction Locorregional
PET/CT in Breast Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria Overview Introduction Locorregional
Patterns of nodal spread in thoracic malignancies
 Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC
 Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Lung Cancer and Mesothelioma
 Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice
 Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice By Howard (Jack) West, MD May, 2009 Hello and welcome to the GRACE audio podcast on PET scanning. This one is with Dr. David
Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice By Howard (Jack) West, MD May, 2009 Hello and welcome to the GRACE audio podcast on PET scanning. This one is with Dr. David
The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options
 Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer
 In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer Prostate cancer is the second most common cancer in men worldwide, accounting for 15% of all new cancer cases. 1 Great strides have
In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer Prostate cancer is the second most common cancer in men worldwide, accounting for 15% of all new cancer cases. 1 Great strides have
Elements of PET/CT Reporting
 Elements of PET/CT Reporting 1. Clinical History a. Indication i. tumor type ii. abnormality to be evaluated iii. specific clinical question b. Relevent history i. biopsy results ii. chemotherapy iii.
Elements of PET/CT Reporting 1. Clinical History a. Indication i. tumor type ii. abnormality to be evaluated iii. specific clinical question b. Relevent history i. biopsy results ii. chemotherapy iii.
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Targeted Therapy What the Surgeon Needs to Know
 Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Understanding Your Surgical Options for Lung Cancer
 Information Booklet for Patients Understanding Your Surgical Options for Lung Cancer Understanding Lung Cancer If you have just been diagnosed with lung cancer, this booklet will serve as an informational
Information Booklet for Patients Understanding Your Surgical Options for Lung Cancer Understanding Lung Cancer If you have just been diagnosed with lung cancer, this booklet will serve as an informational
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH
 9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
Surgeons Role in Symptom Management. A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND
 Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
LUNG CANCER. FCDS 2011 Educational Webcast Series November 17, 2011
 LUNG CANCER FCDS 2011 Educational Webcast Series November 17, 2011 Judy Bonner, RN, MS, CTR and Lynne Pearson, CTR, LHRM Steven Peace, CTR Updated for 2011 Requirements and CSv02.03.02 1 Presentation Outline
LUNG CANCER FCDS 2011 Educational Webcast Series November 17, 2011 Judy Bonner, RN, MS, CTR and Lynne Pearson, CTR, LHRM Steven Peace, CTR Updated for 2011 Requirements and CSv02.03.02 1 Presentation Outline
PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1. Jonathan C. Daniel 2. Kenneth S.
 PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1 Jonathan C. Daniel 2 Kenneth S. Knox 1 Kathleen Williams 1 Departments of Medicine 1 and Surgery 2, University
PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1 Jonathan C. Daniel 2 Kenneth S. Knox 1 Kathleen Williams 1 Departments of Medicine 1 and Surgery 2, University
Lungenkrebs. Lungenkrebs Häufigkeit
 Lungenkrebs Prof. Dr. E.W. Russi Pneumologie 1.9.2008 Lungenkrebs Häufigkeit The Principles and Practice of Medicine William Osler New York D. Appleton and Company 1892 Section IV DISEASE OF THE RESPIRATORY
Lungenkrebs Prof. Dr. E.W. Russi Pneumologie 1.9.2008 Lungenkrebs Häufigkeit The Principles and Practice of Medicine William Osler New York D. Appleton and Company 1892 Section IV DISEASE OF THE RESPIRATORY
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
An Overview of Lung Cancer Symptoms, Pathophysiology, And Treatment Linda H. Yoder
 CE Objectives and Evaluation Form appear on page 235. An Overview of Lung Cancer Symptoms, Pathophysiology, And Treatment Linda H. Yoder Patients with lung cancer can provide treatment challenges for even
CE Objectives and Evaluation Form appear on page 235. An Overview of Lung Cancer Symptoms, Pathophysiology, And Treatment Linda H. Yoder Patients with lung cancer can provide treatment challenges for even
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD
 SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
People Living with Cancer
 Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
The New International Staging System Lung Cancer
 The New International Staging System Lung Cancer Valerie W. Rusch, MD Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center Chair, Lung and Esophagus Task Force, American Joint Commission on Cancer
The New International Staging System Lung Cancer Valerie W. Rusch, MD Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center Chair, Lung and Esophagus Task Force, American Joint Commission on Cancer
How To Know When To Stage Lung Cancer
 WHITE PAPER - SBRT for Non Small Cell Lung Cancer I. Introduction This white paper will focus on non-small cell lung carcinoma with sections one though six comprising a general review of lung cancer from
WHITE PAPER - SBRT for Non Small Cell Lung Cancer I. Introduction This white paper will focus on non-small cell lung carcinoma with sections one though six comprising a general review of lung cancer from
Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method
 Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method Christopher Martel, M.Sc., CHP Lisa Thornhill,, NRRPT, RT(NM) Boston University Medical Center Thyroid Carcinoma New cases and deaths in
Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method Christopher Martel, M.Sc., CHP Lisa Thornhill,, NRRPT, RT(NM) Boston University Medical Center Thyroid Carcinoma New cases and deaths in
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7
 Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7 Authors Ronald C. Walker 1,2, Tracy L. Brown 3, Laurie B. Jones-Jackson
Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7 Authors Ronald C. Walker 1,2, Tracy L. Brown 3, Laurie B. Jones-Jackson
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Lung Cancer: An Overview
 VOL. I Issue 2 2010 Lung Cancer: An Overview By Matthew F. Koscielski, M.D. Lung cancer is the most common cause of cancer mortality worldwide. In the United States there are about 220,000 new cases of
VOL. I Issue 2 2010 Lung Cancer: An Overview By Matthew F. Koscielski, M.D. Lung cancer is the most common cause of cancer mortality worldwide. In the United States there are about 220,000 new cases of
Sternotomy and removal of the tumor
 Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy
 Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy Sarah Hutto,, MSIV Marc Underhill, M.D. January 27, 2009 Past History 45 yo female
Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy Sarah Hutto,, MSIV Marc Underhill, M.D. January 27, 2009 Past History 45 yo female
Survival analysis of 220 patients with completely resected stage II non small cell lung cancer
 窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
Crosswalk for Positron Emission Tomography (PET) Imaging Codes G0230 G0030, G0032, G0034, G0036, G0038, G0040, G0042, G0044, G0046
 Positron Emission Tomography (PET) CPT to HCPCS Level Crosswalk Changes below from CMS Change Request 3741 Transmittals 518 & 31 published on April 1, 2005; mplementation of CPT codes are effective January
Positron Emission Tomography (PET) CPT to HCPCS Level Crosswalk Changes below from CMS Change Request 3741 Transmittals 518 & 31 published on April 1, 2005; mplementation of CPT codes are effective January
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Case Report: Whole-body Oncologic Imaging with syngo TimCT
 Case Report: Whole-body Oncologic Imaging with syngo TimCT Eric Hatfield, M.D. 1 ; Agus Priatna, Ph.D. 2 ; John Kotyk, Ph.D. 1 ; Benjamin Tan, M.D. 1 ; Alto Stemmer 3 ; Stephan Kannengiesser, Ph.D. 3 ;
Case Report: Whole-body Oncologic Imaging with syngo TimCT Eric Hatfield, M.D. 1 ; Agus Priatna, Ph.D. 2 ; John Kotyk, Ph.D. 1 ; Benjamin Tan, M.D. 1 ; Alto Stemmer 3 ; Stephan Kannengiesser, Ph.D. 3 ;
Lung Cancer. Public Outcomes Report. Submitted by Omar A. Majid, MD
 Public Outcomes Report Lung Cancer Submitted by Omar A. Majid, MD Lung cancer is the most common cancer-related cause of death among men and women. It has been estimated that there will be 226,1 new cases
Public Outcomes Report Lung Cancer Submitted by Omar A. Majid, MD Lung cancer is the most common cancer-related cause of death among men and women. It has been estimated that there will be 226,1 new cases
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
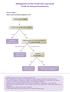 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Guideline for the Referral, Diagnosis and Staging of Patients with Lung Cancer
 Guideline for the Referral, Diagnosis and Staging of Patients with Lung Cancer Incorporating: Guideline for the diagnosis and staging of patients with lung cancer detected within secondary care, guidelines
Guideline for the Referral, Diagnosis and Staging of Patients with Lung Cancer Incorporating: Guideline for the diagnosis and staging of patients with lung cancer detected within secondary care, guidelines
General Rules SEER Summary Stage 2000. Objectives. What is Staging? 5/8/2014
 General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
Part II: NCCN Practice Guidelines Narrative Summary PET and PET/CT
 Part II: NCCN Practice Guidelines Narrative Summary PET and PET/CT NCCN guidelines were reviewed on 3/25/2013 for utilization of 18 F-fluorodeoxyglucose (FDG) PET and PET/CT (available at: http://www.nccn.org/professionals/physician_gls/f_guidelines.asp).
Part II: NCCN Practice Guidelines Narrative Summary PET and PET/CT NCCN guidelines were reviewed on 3/25/2013 for utilization of 18 F-fluorodeoxyglucose (FDG) PET and PET/CT (available at: http://www.nccn.org/professionals/physician_gls/f_guidelines.asp).
The National Clinical Lung Cancer Audit (LUCADA)
 The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
The Di Bella Method (DBM) improves Survival, Objective Response and Performance Status in Breast Cancer
 BIT's 4th World Cancer Congress 2011 People s Republic of China Dalian The Di Bella Method (DBM) improves Survival, Objective Response and Performance Status in treated with DBM therapy Retrospective observational
BIT's 4th World Cancer Congress 2011 People s Republic of China Dalian The Di Bella Method (DBM) improves Survival, Objective Response and Performance Status in treated with DBM therapy Retrospective observational
Lung Cancer Treatment
 Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
The TV Series. www.healthybodyhealthymind.com INFORMATION TELEVISION NETWORK
 The TV Series www.healthybodyhealthymind.com Produced By: INFORMATION TELEVISION NETWORK ONE PARK PLACE 621 NW 53RD ST BOCA RATON, FL 33428 1-800-INFO-ITV www.itvisus.com 2005 Information Television Network.
The TV Series www.healthybodyhealthymind.com Produced By: INFORMATION TELEVISION NETWORK ONE PARK PLACE 621 NW 53RD ST BOCA RATON, FL 33428 1-800-INFO-ITV www.itvisus.com 2005 Information Television Network.
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project
 INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
Small Cell Lung Cancer
 Small Cell Lung Cancer Lung Practice Guideline Dr. Brian Dingle MSc, MD, FRCPC Approval Date: April 2007 Revised: November 2008 This guideline is a statement of consensus of the Thoracic Disease Site Team
Small Cell Lung Cancer Lung Practice Guideline Dr. Brian Dingle MSc, MD, FRCPC Approval Date: April 2007 Revised: November 2008 This guideline is a statement of consensus of the Thoracic Disease Site Team
Thyroid Cancer: Resection, Dissection, Surveillance and Recurrence. Cord Sturgeon, MD
 Thyroid Cancer: Resection, Dissection, Surveillance and Recurrence Cord Sturgeon, MD Associate Professor of Surgery Northwestern University Feinberg School of Medicine Director of Endocrine Surgery Chicago,
Thyroid Cancer: Resection, Dissection, Surveillance and Recurrence Cord Sturgeon, MD Associate Professor of Surgery Northwestern University Feinberg School of Medicine Director of Endocrine Surgery Chicago,
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Sodium Fluoride PET/CT Bone Imaging: Theory and Practice
 Sodium Fluoride PET/CT Bone Imaging: Theory and Practice George Segall, M.D. Stanford University Why F-18 Fluoride? Faster Higher Resolution Anatomic Correlation Chemiadsorption Hydroxyapatite Ca10(PO4)6(OH)2
Sodium Fluoride PET/CT Bone Imaging: Theory and Practice George Segall, M.D. Stanford University Why F-18 Fluoride? Faster Higher Resolution Anatomic Correlation Chemiadsorption Hydroxyapatite Ca10(PO4)6(OH)2
Invasive Cervical Cancer. Kathleen M. Schmeler, MD Associate Professor Department of Gynecologic Oncology
 Invasive Cervical Cancer Kathleen M. Schmeler, MD Associate Professor Department of Gynecologic Oncology Cervical Cancer Etiology Human Papilloma Virus (HPV): Detected in 99.7% of cervical cancers Cancer
Invasive Cervical Cancer Kathleen M. Schmeler, MD Associate Professor Department of Gynecologic Oncology Cervical Cancer Etiology Human Papilloma Virus (HPV): Detected in 99.7% of cervical cancers Cancer
3.0 With final Comments for presentation at Sub Group Meeting 24. 24.11.10
 Guideline for the Treatment of Lung Cancer Version History 2.0 Endorsed by the Governance Committee as treatment of lung cancer 27.07.09 with radiotherapy and chemotherapy. 2.1 Re-written to include the
Guideline for the Treatment of Lung Cancer Version History 2.0 Endorsed by the Governance Committee as treatment of lung cancer 27.07.09 with radiotherapy and chemotherapy. 2.1 Re-written to include the
Stage I, II Non Small Cell Lung Cancer
 Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
CHAPTER 4: LUNG CANCER DIAGNOSIS AND STAGING
 CHAPTER 4: LUNG CANCER DIAGNOSIS AND STAGING INTRODUCTION The lungs are vital organs. Working with the heart and circulatory system, they provide lifesustaining oxygen and rid the body of carbon dioxide.
CHAPTER 4: LUNG CANCER DIAGNOSIS AND STAGING INTRODUCTION The lungs are vital organs. Working with the heart and circulatory system, they provide lifesustaining oxygen and rid the body of carbon dioxide.
Radiologic Diagnosis of Spinal Metastases
 September 2002 Radiologic Diagnosis of Spinal Metastases Natalie J. M. Dailey, Harvard Medical Student Year III Our Patient s Presenting Story 70 year old male Presents to the hospital for laparascopic
September 2002 Radiologic Diagnosis of Spinal Metastases Natalie J. M. Dailey, Harvard Medical Student Year III Our Patient s Presenting Story 70 year old male Presents to the hospital for laparascopic
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
