Total Knee Arthroplasty Rehabilitation
|
|
|
- Shanon Owens
- 9 years ago
- Views:
Transcription
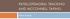
1 1 Total Knee Arthroplasty Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The knee is composed of the distal end of the femur, proximal portion of the tibia, and the patella. It has a medial and lateral meniscus in between the femur and tibia to cushion the joint, absorb and transmit weigh-bearing forces. Four ligaments, the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament (MCL) and lateral collateral ligament (LCL) provide anterior-posterior and medial-lateral support. The knee is an unstable joint, relying on ligaments, menisci, and balanced muscles on all sides of the joint, particularly the hamstrings and quadriceps, for cushioning and stability. It is more than a simple hinge joint, as the bone surfaces roll, glide, and rotate on each other. Pathogenesis: Wear and tear of the knee joint is part of the normal aging process, however, osteoarthritis (OA) accelerates the degenerative wear of the meniscus. This form of arthritis usually results from some predisposing factor, such as an injury or deformity. Whether of unknown origin or secondary to trauma or disease, poor alignment of the leg bones may cause unequal weight distribution. This leads to excessive wear on one side of the joint surface versus another, and any irregularity of the knee joint results in wear and tear of the menisci. Over time, the menisci no longer function as an effective shock absorber/transmitter for the knee. Excessive localized pressure and damage to the joint result, possibly leading to bone-on-bone contact, causing symptoms of increased knee stiffness and pain. Remodeling of bone may also occur due to bone-on-bone contact, causing bony spurs. These spurs contribute to increased pressures within the joint, leading to pain and decreased function. Rheumatoid arthritis is an inflammatory joint disease that is destructive to articular cartilage lining the surfaces of the knee joint. The inflammatory process can cause joint instability and deformity, muscle atrophy and weakness, swelling, stiffness, and pain. Epidemiology: Total knee arthroplasty (TKA) is one of the most common orthopedic procedures: 171,335 primary total knee replacements occurred in Nearly 90% of patients who elected to have TKA had OA of the knee, 2/3 were female, and 1/3 were considered obese. Although patients as young as late-40 s and as old as mid-90 s have received total knee replacements, the ideal knee replacement candidate is between the ages of 65-75, as patients are healthy enough to recover well from surgery, yet old enough so replacement most likely lasts the rest of their lives (15-20 years). Obesity is the most modifiable risk factor, but prior knee injuries/trauma, and extreme physical or repetitive activity can also contribute to increased incidence of knee OA. Other causes of knee dysfunction leading to TKA include rheumatoid arthritis, trauma, congenital/acquired joint deformity, and tumors.
2 2 Diagnosis/Indications For Surgery Severe joint pain with weight bearing or motion that compromises functional activities (severity of pain correlates poorly with radiographic and structural changes in the joint) Extensive destruction of articular cartilage of the knee secondary to advanced arthritis Gross instability or limitation of motion Marked deformity of the knee such as genu varum or valgum Knee pain that does not respond to conservative therapy (medication, injections, physical therapy > six months) Previous failed surgical procedure Nonoperative Versus Operative Management: There are typically four major groups of nonsurgical treatments: 1) Health and behavior modification, including weight loss and patient education about behavior changes to reduce impact of disease, physical therapy and exercise to stretch, strengthen muscles surrounding the knee. Deyle et al concluded that a combination of manual physical therapy and supervised exercise is more effective than no treatment in improving walking distance and decreasing pain, dysfunction, and stiffness in patients with OA of the knee, possibly deferring or decreasing the need for surgical intervention. Vad et al proposed a progressive five-stage rehabilitation program for managing knee OA that ranges from protected mobilization to exercises to improve neuromuscular coordination, timing, and joint protection. Taping and bracing to support and protect the knee joint, foot orthoses to correct imbalances contributing to unequal weight bearing forces across the knee joint, and use of TENS for pain control are also included under this category. 2) Drug treatments, including simple pain relievers, nonsteroidal anti-inflammatory drugs (NSAIDs), COX-2 inhibitors, opiates, and glucosamine and/or chondroitin sulfate are several types of drugs used to treat knee OA. 3) Intra-articular treatments involve one or more injections into the knee joint. Corticosteroid injections, limited to four or less per year, are helpful for significant swelling causing moderate to severe pain. Typically corticosteroid injections are not helpful if arthritis affects joint mechanics. Viscosupplementation with hyaluronic acid, a molecule that is found in joints of the body, is a way of adding fluid to lubricate the joint and make it easier to move. It can be helpful for people whose arthritis does not respond to behavior modification or basic drug treatments. Three to five weekly shots are needed to reduce the pain, but relief is not permanent. 4) Alternative therapies include the use of acupuncture and magnetic pulse therapy. Acupuncture is adapted from a Chinese medical practice. It uses fine needles to stimulate specific body areas to relieve pain or temporarily numb an area. Magnetic pulse therapy is painless and works by applying a pulsed signal to the knee, which is placed in an electromagnetic field. Because the body produces electrical signals, proponents think that magnetic pulse therapy may stimulate the production of new cartilage. Many forms
3 3 of therapy are unproven but reasonable to try provided they are through a qualified practitioner and the primary physician is informed of the patient s decision to try these therapies. Elective total knee replacement is, more often than not, the last effort in managing joint pain and dysfunction caused by arthritis when non-operative treatment of knee pain is not effective. When erosion of articular joint surfaces becomes severe, TKA is the surgical procedure of choice to decrease pain, correct deformity, and improve functional movement. Surgical Procedure: An incision is made down the front of the leg from mid-thigh to several inches below the knee. The quadriceps muscles are either split down the middle or shifted, along with the patella, to the side of the thigh. The distal end of the femur and proximal end of the tibia are sawed off; the menisci and ACL are excised as well. The PCL may also be cut; the pros and cons of sparing the PCL is currently of debate in knee replacement surgery. The knee replacement consists of three components that help the surgeon tailor the device to the patient. A curved femoral component is usually made of shiny chrome alloy; it is attached to the femur and replaces the femoral condyles. The metal tibial component has a flat top with a spike that goes into a 2 hole that the surgeon drills into the tibia. A disc, made of polyethylene, is cemented to the top of the tibial component. Depending on its condition, the patella is either left intact or the inside resurfaced- the patella is never totally replaced. If the patella is resurfaced, polyethylene is also used to cover the inside. Total knee arthroplasty components are either held in place with bone cement (cemented fixation), utilize bone ingrowth via a porous prosthesis (uncemented fixation), or combine cemented fixation of the tibial component and uncemented fixation of the femoral component (hybrid). Uncemented fixation has been used primarily for the active patient in whom the risk of prosthetic loosening over time is most likely, however, the ultimate decision rests with the attending surgeon. Preoperative Rehabilitation Ensure adequate strength of trunk and upper extremities for support during use of assistive devices Instruction in use of walker/crutches/or cane to maintain desired postoperative weight bearing status (touchdown weight bearing for uncemented or hybrid replacements, weight bearing as tolerated for cemented replacements) Review of post-operative exercises, bed mobility and transfers, use of continuous passive motion (CPM) machine as indicated per physician General strengthening, flexibility, and aerobic conditioning While it seems reasonable to believe patients undergoing TKA would benefit from preoperative strengthening exercises, there is no evidence to support this assumption, either in improving functional outcome or shortening hospital stay (D Lima et al., Rodgers et al.). However, a study by Jones et al showed that patients who have greater preoperative dysfunction may require more intensive physical therapy intervention after surgery because they are less likely to achieve similar functional outcomes to those of patients who have less preoperative
4 4 dysfunction. POSTOPERATIVE REHABILITATION Note: The following rehabilitation progression is a summary of the guidelines provided by Kisner and Colby. Refer to their publication to obtain further information regarding criteria to progress from one phase to the next, anticipated impairments and functional limitations, interventions, and goals. *Use of a CPM device is often initiated by the first day after surgery, per physician protocol. It has been suggested that CPM decreases postoperative pain, promotes wound healing, decreases incidence of deep venous thrombosis (DVT), and enables the patient to regain knee flexion more rapidly during early postoperative days. However, Kumar et al conducted a randomized prospective study that found no statistically significant difference in range of motion gains using a CPM device versus active movement. Continuous passive motion units may be recommended as an adjunct to, not a replacement for, a supervised postoperative rehabilitation program. Phase I: Maximum Protection: Weeks 1-2 Goals: Control postoperative swelling Minimize pain Knee ROM 0-90 Muscle strength 3/5-4/5 Ambulation with or without use of an assistive device Establish home exercise program Intervention: Passive range of motion (PROM)-CPM as indicated per physician Ankle pumps to decrease risk of DVT Bed mobility and transfers usually initiated hours post-surgery, depending on surgical procedure and co-morbidities Heel slides in supine or sitting to increase knee flexion Muscle-setting exercises of the quadriceps, hamstrings, and hip adductors, possibly coupled with neuromuscular electrical stimulation Assisted progressing to active straight-leg raises in supine, prone, and sidelying positions Gravity-assisted knee extension in supine by periodically placing a towel roll under the ankle and leaving the knee unsupported Gentle inferior and superior patellar glides Neuromuscular inhibition techniques such as agonist-contraction techniques to decrease muscle guarding, particularly in the quadriceps, and increase knee flexion Gentle stretches for the hamstrings, calf, and iliotibial band Pain modulation modalities Compressive wrap to control effusion
5 5 Gait training Phase II: Moderate-Minimum Protection: Weeks 3-6 Goals: Diminish swelling and inflammation Increase ROM or more Increased dynamic joint stability/full weight bearing per implant status Muscle strength 4/5-5/5 Return to functional activities Adhere to home exercise program Intervention: Interventions listed in Phase I Patellar mobilizations Tibiofemoral joint mobilization if appropriate and needed Soft tissue mobilization to quadriceps or hamstrings myofascia Incision mobilization after suture removal, when incision is clean and dry Progressive passive stretches to hamstrings, gastrocnemius, soleus, quadriceps within a pain-free range Stationary bike or peddler without resistance to increase flexion ROM Pain-free progressive resisted exercises using ankle weights, theraband/tubing Proprioceptive training such as weight shifting, tandem walking, lateral stepping over/around objects, obstacle courses, lower extremity proprioceptive neuromuscular facilitation (PNF), front and lateral step-ups, closed-kinetic chain activities Closed-kinetic chain strengthening, such as ¼ squats, ¼ front lunges Gait training as needed to decrease limp, wean off assistive device Protected, progressive aerobic exercise, such as cycling without resistance, walking, or swimming Phase III: Return to Activity: Week 6 and beyond Goals: Progress ROM as able, to a functional range for the patient Enhance strength and endurance and motor control of the involved limb Increase cardiovascular fitness Develop a maintenance program and educate patient on the importance of adherence, including methods of joint protection Intervention: Continue interventions of previous phases; advance as appropriate Implement exercises specific to functional tasks, such as transferring from sit-to-stand, lifting, carrying, push/pulling, squat/crouching, return to work tasks, return to sport tasks Improve cardiorespiratory and muscle endurance with activities such as bicycling, walking, or aquatic programs
6 6 Selected References: Avramidis K, Strike P, Taylor P, Swain I. Effects of electrical stimulation of the vastus medialis muscles in the rehabilitation of patients after total knee arthroplasty. Arch Phys Med Rehab. 2003;84: D Lima D, Colwell C, Morris B, Hardwick M, Kozin F. The effect of preoperative exercise on total knee replacement outcomes. Clin Orthop. 1996;1(326): Deyle G, Henderson N, Matekel R, Ryder M, Garber M, Allison S. Effectiveness of manual physical therapy and exercise in osteoarthritis of the knee: A randomized controlled trial. Ann Intern Med. 2000;132: Fitzgerald G, Oatis C. Role of physical therapy in management of knee osteoarthritis. Curr Opin Rheumatol. 2004;16: Goodman C, Boissonnault W. Pathology: Implications for the Physical Therapist. Philadelphia, W.B. Saunders Company, Jones C, Voaklander DC, Suarez-Almazor ME. Determinants of function after total knee arthroplasty. Phys Ther. 2003;83: Kisner C, Colby LA. Therapeutic Exercise Foundations and Techniques. Philadelphia, F.A. Davis Company, Kramer JF, Speechley M, Bourne R, Rorabeck C, Vaz M. Comparison of clinic- and home-based rehabilitation programs after total knee arthroplasty. Clin Orthop. 2003;1(410): Kumar PJ, McPherson EJ, Dorr L, Wan Z, Baldwin K. Rehabilitation after total knee arthroplasty: A comparison of 2 rehabilitation techniques. Clin Orthop. 1996;1(331): Moore K, Dalley A. Clinically Oriented Anatomy, 4 th ed. Baltimore, Lippincott Williams and Wilkins, Ranawat CS, Ranawat AS, Mehta A. Total knee arthroplasty rehabilitation protocol. What makes the difference? J Arthroplasty. 2003;18(3): Rodgers JA, Garvin KL, Walker CW, Morford D, Urban J, Bedard J. Preoperative physical therapy in primary total knee arthroplasty. J Arthroplasty. 1998;13: Vad V, Hong HM, Zazzali M, Agi N, Basrai D. Exercise recommendations in athletes with early osteoarthritis of the knee. Sports Med. 2002;32(11):
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
ACL Non-Operative Protocol
 ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
Anterior Cruciate Ligament Reconstruction. ACL Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Theodore B. Shybut, M.D. 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521. Sports Medicine
 Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
What is Osteoarthritis? Who gets Osteoarthritis? What can I do when I am diagnosed with Osteoarthritis? What can my doctor do to help me?
 Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
Hip Arthroscopy Post-operative Rehabilitation Protocol
 Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Hamstring Graft/PTG-Accelerated Rehab
 The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
ACL Reconstruction Post Operative Rehabilitation Protocol
 ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol
 Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL
 Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Cincinnati Sportsmedicine and Orthopaedic Center
 Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
Knee Arthroscopy (Meniscectomy)
 Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe
 Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
PREOPERATIVE: POSTOPERATIVE:
 PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions
 Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
Rehabilitation Guidelines for Autologous Chondrocyte Implantation. Ashley Conlin, PT, DPT, SCS, CSCS
 Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty
 Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Structure & Function of the Knee. One of the most complex simple structures in the human body. The middle child of the lower extremity.
 Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Goals of Post-operative operative Rehab. Surgical Procedures. Phase 1 Maximum protection and Mobility (1-4 weeks)
 Hip Arthroscopy - Post-Operative Care and Rehabilitation Franz Valenzuela, DPT, OCS Surgery corrects mechanical problems Rehabilitation corrects functional deficits Surgical Procedures Requires little
Hip Arthroscopy - Post-Operative Care and Rehabilitation Franz Valenzuela, DPT, OCS Surgery corrects mechanical problems Rehabilitation corrects functional deficits Surgical Procedures Requires little
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
MEDIAL PATELLA FEMORAL LIGAMENT RECONSTRUCTION Rehab Protocol
 Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees
 Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
How To Treat A Patella Dislocation
 Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Patellar Dislocation Conservative and Operative Rehabilitation
 1 Patellar Dislocation Conservative and Operative Rehabilitation Surgical Indications and Considerations Anatomical Considerations: Patellar stability is dependent upon two components: bony (trochlear
1 Patellar Dislocation Conservative and Operative Rehabilitation Surgical Indications and Considerations Anatomical Considerations: Patellar stability is dependent upon two components: bony (trochlear
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Dr. O Meara s. Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com
 Dr. O Meara s Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol Hamstring Stretching & Strengthening
Dr. O Meara s Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol Hamstring Stretching & Strengthening
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Why knees hurt, and what you can do about it.
 Why knees hurt, and what you can do about it. Table of Contents How Knees Work Common Conditions and Treatment Options Surgical Procedures START Start the Journey to Pain-Free Knees START What Sets Us
Why knees hurt, and what you can do about it. Table of Contents How Knees Work Common Conditions and Treatment Options Surgical Procedures START Start the Journey to Pain-Free Knees START What Sets Us
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW Health Sports Rehabilitation Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW Health Sports Rehabilitation Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities
 Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Shoulder Joint Replacement
 Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Clients w/ Orthopedic, Injury and Rehabilitation Concerns. Chapter 21
 Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
REHABILITATION PROTOCOL
 COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation
 1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
PATELLOFEMORAL TRACKING AND MCCONNELL TAPING. Minni Titicula
 PATELLOFEMORAL TRACKING AND MCCONNELL TAPING Minni Titicula PF tracking disorder PF tracking disorder occurs when patella shifts out of the femoral groove during joint motion. most common in the US. affects
PATELLOFEMORAL TRACKING AND MCCONNELL TAPING Minni Titicula PF tracking disorder PF tracking disorder occurs when patella shifts out of the femoral groove during joint motion. most common in the US. affects
Steps to Success: A Guide to Knee Rehabilitation
 Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
Knee Kinematics and Kinetics
 Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
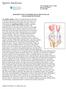 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
KNEES A Physical Therapist s Perspective American Physical Therapy Association
 Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Total Elbow Arthroplasty and Rehabilitation
 Total Elbow Arthroplasty and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: There are three bones and four joint articulations that have a high degree of congruence in
Total Elbow Arthroplasty and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: There are three bones and four joint articulations that have a high degree of congruence in
UK HealthCare Sports Medicine Patient Education December 09
 Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Hip Bursitis/Tendinitis
 Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Anterior Cruciate Ligament Reconstruction
 1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular
UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee.
 Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY
 B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
Rehabilitation Guidelines for Lateral Ankle Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
Post Surgical Care of Patella Luxation Repair
 Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Treatment Guide Knee Pain
 Treatment Guide Knee Pain Choosing Your Care Approximately 18 million patients visit a doctor or a hospital because of knee pain each year. Fortunately, there are many ways to successfully treat knee pain
Treatment Guide Knee Pain Choosing Your Care Approximately 18 million patients visit a doctor or a hospital because of knee pain each year. Fortunately, there are many ways to successfully treat knee pain
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION
 KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI MR GREG CRIAG MR IAN COLLIER DECEMBER, 2004 INTRODUCTION Anterior cruciate ligament reconstruction
AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI MR GREG CRIAG MR IAN COLLIER DECEMBER, 2004 INTRODUCTION Anterior cruciate ligament reconstruction
Post-Operative Exercise Program
 785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Rehabilitation. Modalities and Rehabilitation. Basics of Injury Rehabilitation. Injury Rehabilitation. Vocabulary. Vocabulary
 Modalities and Rehabilitation Rehabilitation Chapter 12: Basics of Injury Rehabilitation Vocabulary Balance: ability to maintain our center of gravity over a base of support Kinesthesia: the ability to
Modalities and Rehabilitation Rehabilitation Chapter 12: Basics of Injury Rehabilitation Vocabulary Balance: ability to maintain our center of gravity over a base of support Kinesthesia: the ability to
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction
 Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
Total Knee Replacement
 Total Knee Replacement Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures.
Total Knee Replacement Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures.
