Total Knee Replacement
|
|
|
- Timothy Page
- 8 years ago
- Views:
Transcription
1 Total Knee Replacement Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures. Since the 1970 s, while total joint techniques and methodologies have evolved and improved, one thing at DMOS has remained the same: the commitment to specialized, compassionate orthopaedic care for every patient. As the largest and most comprehensive total joint center in Iowa, you can be assured that your surgeon and their colleagues experience in the science and techniques of total joint replacement is at the forefront of exceptional care. In addition to the thousands of total joints performed, DMOS surgeons have published hundreds of articles explaining and exploring the science of total joint replacements. As a result, the Joint Replacement Center at DMOS is second to none in the area. We thank you for choosing DMOS and look forward to helping you gain mobility and get back to life with your total joint.
2 Introduction to Knee replacement surgery has been available to arthritic patients for more than 35 years. Fortunately, this surgical procedure has proven to be a very effective and reliable treatment for arthritis of the knee. The purpose of this pamphlet is to help you better understand knee replacement surgery. We will discuss how arthritis affects the knee and causes pain, stiffness, and disability. Further, we will describe knee replacement surgery and the usual recovery process. Finally, we will explain typical results of the operation and possible complications that may occur. It is our hope and intention that this knowledge will assist you in making an informed decision when you consider knee replacement. Once you have made the decision to have your knee replacement and your surgery has been scheduled, we ask that all patients preparing for a joint replacement participate in a Joint Replacement Class. Depending on the hospital facility where your surgery will be performed, the hospital will offer a Joint Replacement Program for you and a family member to attend. This program will provide a more comprehensive review of how to prepare for your surgery, what to expect, what your post-operative care may entail, and how to return to an active lifestyle, and more. We recommend that a member of your family participate in/view this program with you. The physicians of Des Moines Orthopaedic Surgeons (DMOS) consist of a large group of orthopaedic specialists. In order to provide care for you that is as current and skilled as possible, each of the surgeons has chosen to emphasize surgical care of a few specific orthopaedic conditions. The group has vast experience with the procedures of total hip and total knee replacement. Since the early 1970s, surgeons of DMOS have performed over 16,000 total hip replacements and over 24,000 total knee replacements. This experience is unparalleled in our area.
3 KNEE ANATOMY AND FUNCTION The knee joint is the largest joint in the body. It is a hinge-type joint formed by the meeting of two bones, the femur (thighbone) and the tibia (shinbone). The patella (kneecap) is also an important part of the knee joint. Ligaments and muscles secure these bones together and provide joint stability. All of the moving surfaces of the knee joint are covered with a smooth firm lining known as the articular, or surface, cartilage (Fig. 1). The contact of cartilage on cartilage provides a cushioned, low-friction surface. The combined structure of bone, cartilage, and muscle allows smooth, painless motion as you walk, bend, and straighten your knee. EFFECTS OF ARTHRITIS Arthritis is a condition that results from gradual deterioration and loss of the joint surface cartilage (Fig. 2). This deterioration of cartilage may occur due to the effects of previous injury or from progressive wear and tear, which occurs with aging. This process is called osteoarthritis or degenerative joint disease. In addition, inflammatory conditions, such as rheumatoid arthritis, may destroy joint surface cartilage. Previous injury, such as a fracture or major ligament injuries, may lead to joint deterioration and is called posttraumatic arthritis. Mild arthritis causes joint stiffness and some discomfort. As the cartilage deterioration process progresses, nearly constant pain and permanent stiffness occur. At this point, normal activities of daily living become difficult to carry out. Patients with advanced arthritis are only able to walk short distances before needing to rest, have difficulty going up and down stairs, and need assistance getting out of a chair or car. These patients often walk with a limp and may require the use of an assistance device, such as a cane or walker.
4 ORTHOPAEDIC EVALUATION & TREATMENT ALTERNATIVES X-rays are very useful in determining the severity of arthritis (Fig. 3). As arthritis and cartilage deterioration progress, the cartilage space between the bones decreases in size and may disappear altogether (bone rubbing on bone). This cartilage deterioration may be confined to a limited area of the knee joint (one compartment) or may involve the entire joint. After completion of the orthopaedic examination (symptoms, exam, X-rays), the various treatment options, along with any specific recommendations, will be discussed. With mild arthritis, some modification of activities and arthritis medications may be adequate. The occasional use of a cane may also be helpful. If you are overweight, we encourage weight loss. Your orthopaedic evaluation assesses the severity of your arthritis and leads to a treatment recommendation. The evaluation begins with questions concerning the severity of your knee pain. We attempt to discover how your knee pain and stiffness limit your daily activities, such as walking, stair climbing, and driving or riding in a car. We also ask about previous treatment, such as medications, cortisone or other injections, and the use of a cane. Examination of the knee includes assessment of the knee range of motions (stiffness) and any knee deformity (bowlegged or knock-kneed). In addition, ability to walk and the presence of a limp are noted. Fig. 3 Normal Knee X-Ray (Note: Normal Cartilage Space) Arthritic Knee X-Ray (Note: Loss of Cartilage Space)
5 Injections of various substances into the knee joint may give temporary relief of arthritic symptoms. Cortisone injections have been utilized for more than 40 years and provide very reliable, albeit temporary, relief of arthritis pain. More recently, lubricating substances (viscosupplementation, which contains hyaluronic acid) have become available. These treatments are given in a series of one to three weekly injections into the knee joint. These injections can be effective for patients with mild or moderate osteoarthritis but are usually not effective for patients with severe osteoarthritis. Many patients ask about the use of the nutrients glucosamine and chondroitin sulfate. These two substances may promote the growth or regeneration of articular cartilage and may also have an antiinflammatory effect. Like viscosupplementation, the efficacy of this treatment is not documented at this time. These substances appear to be very safe and can be obtained without prescription at most pharmacies and nutraceutical retailers. With more severe or constant pain and inability to carry out daily activities, surgery with total knee replacement is often the recommended treatment. Age itself is not a major consideration in total knee replacement. The severity of the patient s pain and restriction in activities is the primary consideration. Younger patients must be aware that they need to moderate their activities if they are to enjoy comfortable use of their knee replacement for many years. Older patients whose health remains satisfactory should be able to tolerate a major operation and benefit from it. NONSURGICAL TREATMENT OF ARTHRITIS Weight Loss Modification of Activity Arthritis Medication Glucosamine Cortisone Injection Viscosupplementation Injection Cane KNEE PROSTHESIS Total knee replacement surgery requires replacement of the damaged cartilage joint surfaces with metal and plastic components (prostheses). Metal on plastic artificial joints have proven to be self-lubricating and show minimal effects of wear despite years of use. Nearly all knee replacements require the use of three parts or components (Fig. 4): 1. The femoral component is made of metal (chromecobalt) and covers the end of the femur (thighbone). 2. The tibial component is high-molecular weight polyethylene (plastic) that is reinforced by a metal base plate (titanium or chrome-cobalt) and sits atop the tibia (shinbone). 3. The patellar component is polyethylene and covers the undersurface of the kneecap. In some circumstances, the cartilage of the kneecap remains satisfactory, and in that situation, the patellar component may not be utilized.
6 Femoral Component Femoral Component Tibial Component Tibial Component Fig. 4 - Total Knee Replacement Fig. 5 - Unicompartmental Knee Replacement Actually, very little bone is removed in the preparation for placement of the total knee components. The patient s own muscles and ligaments are preserved and continue to function and allow the new knee to work. Thus, the knee replacement provides new artificial surfaces to replace the worn cartilage. In select circumstances, unicompartmental knee replacement (partial knee replacement) may be the best option (Fig. 5). Often, the knee arthritis condition affects only one area of the knee severely so your surgeon may recommend that only the affected area of the joint be replaced. With this type of prosthesis, femoral and tibial components are smaller but still composed of the same materials. Unicompartmental knee replacement has the advantages of a slightly easier recovery and more normal function following recovery. This type of knee replacement has received considerable attention in the media in recent years and is one type of minimally invasive knee replacement. Surgeons at DMOS feel this type of knee replacement has significant advantages in appropriately selected cases. difficulty with stairs, inclines, and rising from a seated position. A limited replacement for just the patellofemoral joint is now also available and has shown favorable results. New design and materials utilized in the knee joint replacement are slowly evolving. The plastic (ultrahigh molecular weight polyethylene) material has been substantially improved (cross-linked polyethylene) in the last five years to enhance its wear resistance. This improvement has become frequently utilized in knee replacements at this time. Design changes of the tibial component (mobile bearing) have occurred and the appropriate use of these designs has yet to be determined. Your DMOS surgeon will select a design appropriate for your case. Typically, the artificial knee components are held to the bone with acrylic cement. Fortunately, this cement has been found to be very durable for years and years. In occasional cases, knee components, which allow fixations by bone ingrowths, will be placed without cement. Your doctor will discuss these options with you prior to surgery. In other patients, only the patella (kneecap) is severely damaged by arthritis. These patients have particular
7 RESULTS OF TOTAL KNEE REPLACEMENT People with a complete knee replacement are typically able to bend their knee well beyond the right angle (90 degrees). Kneeling is possible after knee replacement, but many may find it difficult. ACTIVITIES AFTER TOTAL KNEE REPLACEMENT Walking Hiking Bicycling Swimming Golf Bowling After a knee replacement, you can expect significant improvement in your knee pain. While an artificial knee is not a normal knee, you can expect to resume most activities of daily living with comfort and ease. Studies have confirmed that approximately 90% of all knee replacements can expect a very good result. Unlimited walking tolerance is the goal and is usually achieved. Most patients are able to climb stairs foot over foot and get out of a chair or car without help. Excessive weight or other medical conditions can certainly affect these activities, however. Recreational activities like walking, bicycling, swimming, bowling, and golf are likely to be possible. More strenuous activities, such as jogging, tennis, racquet sports, and skiing, could damage the artificial knee and are not usually recommended.
8 LONG-TERM EXPECTATIONS OF KNEE REPLACEMENTS Most patients wish to know how long they can expect their artificial knee replacement to last. Long-term scientific studies have confirmed that over 90% of knee joint replacements are still functioning well at 10 years, and over 80% of knee joint replacements are still functioning quite well at 20 years. Over time, a knee replacement may deteriorate or fail for a number of reasons. Wear or deterioration of the plastic polyethylene component may cause inflammation within the joint, which can lead to discomfort, swelling, and some deterioration of the bone, called osteolysis (Fig. 6). The risk of this occurrence may well be decreasing due to the improved polyethylene materials now available. Knee joint failure may also occur if the cement bond between the component and the bone deteriorates. This process is often termed loosening. It is the most common cause of failure and requires surgery to repair. Infection of a total joint replacement is a particularly serious problem and may require several surgeries to resolve. Fortunately, this complication occurs in less than 0.5% of knee replacement patients. Repeat surgery on a knee replacement is commonly called revision joint replacement surgery. These procedures are becoming more common due to the vast number of patients having completed knee joint replacement surgery in the last 40 years. Revision becomes necessary because of osteolysis, loosening, and/or infection. Generally speaking, revision surgery is more complex and more difficult than the primary surgery and may often be associated with a longer recovery and less favorable results than the initial surgery. LONG-TERM RESULTS 90% of knee joint replacements are still functioning well at ten years. Over 80% of knee replacements are still functioning well at 20 years. Fig. 6 - Osteolysis
9 RISKS OF KNEE REPLACEMENTS No surgery is without risk. Understanding the risks is necessary in order for you to make an informed decision about your desire for surgery. MEDICAL COMPLICATIONS. Anesthesia and surgeryrelated complications such as heart attack, stroke, death, or loss of limb (less than 1 in 10,000 chance), may occur. Fortunately, these events occur extremely rarely. A thorough medical examination prior to surgery minimizes these risks. INFECTION. Infection is very serious complication of any joint replacement surgery. Many precautions are taken to avoid infection and as a result, the risk of infection is very low (less than half of a percent). These precautions include the use of antibiotics at the time of surgery. Use of designated operating rooms with special air-handling filters, and in some instances, the use of space suits by the surgeons and nurses. Further surgery would be necessary if an infection should occur and the successful treatment of infection could require many months of treatment. BLOOD LOSS. Following knee replacement surgery, and particularly following bilateral knee joint replacement surgery, a blood transfusion may be required. Patients undergoing a single joint replacement have a less than a 5% risk of requiring a transfusion. Patients undergoing bilateral (right and left) replacements, however, have a greater than 10% chance of requiring blood transfusion. Bloodborne diseases (AIDS, hepatitis, etc.) and adverse allergic reactions are the major hazards of blood transfusions. Our blood bank screening is as modern and thorough as possible and therefore, the risks are exceedingly small. In fact, the risk of dying from a blood transfusion is hundreds of times lower than that of driving your car for one day. There are many options available to lower your chance of needing a blood transfusion.
10 OBESITY. Excessive weight can make the actual surgical procedure more difficult and increases your risk of complications, such as wound healing and infection. Expectations following knee replacement surgery in obese patients are diminished. Patients of large size generally will not be able to walk as far; stair climbing and rising from a chair will remain more difficult, and the knee joint will have less flexion (bend). Excessive weight may also shorten the life of the prosthesis. However, patients with excessive weight generally are pleased with their joint replacement. NERVE, ARTERY, OR BONE INJURY. Though rare, other complications could include artery or nerve damage or fractures of the bones near the knee. BLOOD CLOTS. Blood clots or deep vein thromboses may occur following any lower extremity surgery, including knee joint replacement. These clots cause increased swelling in the legs and although rare, can travel to the lung and cause more severe illness or even sudden death. The risks of these events are minimized by several important treatments. All patients are given appropriate blood thinner soon after surgery. Generally, you will be required to take small injections of blood thinner (Lovenox or Fragmin) daily or you will use an oral blood thinner (Coumadin or Pradaxa). Adult-strength aspirin is becoming the preferred protection from blood clots. Either of these medications will be continued after your discharge from the hospital. In addition to these medications, we minimize the risk of blood clots by the use of foot pumps, used while in bed, or by getting you up and moving very soon after surgery. BILATERAL SURGERY Frequently, both right and left knees are affected by similar arthritis. Under these circumstances, the best results are only obtained if each knee undergoes a total knee replacement. We have found that it is sometimes desirable to complete both knee replacements during the same hospitalization, although certainly the second knee replacement can be delayed many months. Replacing both knees in one operation on the same day is occasionally possible, but generally, we find it is too stressful for most patients. We have found, however, that two knee replacements can be completed within one week with great success. Your surgeon will discuss this option if both of your knees are severely affected by the arthritis. This, of course, will prolong your hospital stay by two to three days.
11 PREPARATIONS FOR SURGERY ROUTINE LABORATORY TESTS are generally performed with your pre-surgical medical exam prior to surgery. These include necessary blood tests, possibly X-rays, and an EKG. PRE-SURGERY JOINT REPLACEMENT PROGRAM. The hospital offers a Pre-Surgery Joint Replacement Program class for you and a family member to attend. It is necessary that all joint replacement patients attend this pre-surgery class. The program will provide useful information concerning your hospitalization for your total knee replacement and will answer many of your questions. In addition to your attendance, we strongly encourage a family member to attend the program with you as well. Your surgeon and his/her staff will provide you with more information about the Pre-Surgery Joint Replacement Program class. Once you have made the decision to proceed with knee replacement surgery, a number of necessary events will be scheduled. A DATE FOR SURGERY will be determined and scheduled at the hospital by your surgeon. If you need to contact the program coordinator or would like more information about the class, the contact information is below: METHODIST WEST: (515) IOWA LUTHERAN HOSPITAL: (515) ST. ANTHONY REGIONAL HOSPITAL: (712) A PRE-SURGICAL MEDICAL EXAMINATION will be scheduled. This examination should be carried out in the weeks prior to the scheduled surgery. In most cases, your age and medical condition will require a complete medical exam by an internal medicine specialist and/or a cardiologist, who will then be available to assist in your care during your post-operative hospital stay. We will provide additional information concerning these exams and schedule your evaluation.
12 BLOOD TRANSFUSION. A blood transfusion may be necessary after a total knee replacement. The need for a blood transfusion following a single total knee replacement is less than 5%, thus we do not generally recommend donating your own blood prior to surgery. If you would require blood after surgery, it will be supplied from the blood bank. The blood is carefully screened for disease and cross-matched to you prior to the transfusion. As a result, the risk of disease transmission or allergic reaction is extremely rare. With bilateral knee replacement, the need for a blood transfusion increases by 10%. HOME MEDICATIONS MEDICATIONS PRIOR TO SURGERY. If you are taking aspirin or anti-inflammatory medications, please discontinue use seven days prior to surgery. Your surgeon may have additional recommendations concerning your iron and/ or other supplements prior to surgery. TO DO BEFORE SURGERY: Pre-Op History & Physical Find Family Member or Coach to Accompany Me to Total Joint Class and to Assist Me at Home Starting Post-Op Day #1 Attend Total Joint Class
13 SURGERY & HOSPITAL STAY DAY OF SURGERY Patients are usually admitted to the hospital on the day of surgery. If your procedure is at Methodist West, Iowa Methodist Medical Center, or Iowa Lutheran Hospital, you will be contacted to confirm the time of your surgery and time of arrival. If you have not received a call by 3 p.m., please contact the hospital outpatient surgery center or surgery scheduling desk. If your procedure is at St. Anthony Regional Hospital, you will learn your surgery time and time of arrival three to four days prior. Please expect to arrive two hours prior to your surgery time. You should report to the Outpatient Surgery Department at the hospital in which your procedure is being performed. Listed below is the location of the Outpatient Surgery Department at each hospital: METHODIST WEST: Main entrance, east side of hospital. Check in at Surgery Department IOWA METHODIST MEDICAL CENTER: Entrance #7, east end of the hospital, level A IOWA LUTHERAN HOSPITAL: Main entrance of hospital, south side of building ST. ANTHONY REGIONAL HOSPITAL: Report to Same Day Surgery Center (3rd floor of parking garage) You will be assigned a room following surgery. The patient should bring sleepwear, a good pair of walking shoes, and personal hygiene supplies with them. You should not eat or drink after midnight the evening before surgery. If you take medications every morning, discuss these medications with your primary care physician or surgeon, as they may have you take these medications with a small sip of water on the morning of surgery. Total knee replacement is either performed under a spinal anesthetic or a general anesthetic. You will have an opportunity to discuss these options with an anesthesiologist prior to your surgery. There are several factors that determine the type of anesthetic that should be used, but the patient s preference is also taken into account. The surgical procedure, including the time for preparation, is approximately two hours. You will also spend approximately one to two hours in the recovery room area before you are taken to your room. Following completion of the knee replacement surgery, your leg is placed in a bandage that extends from the toes to the upper thigh. When you return to your room, you will begin to experience some discomfort in your knee. The onset of this pain can vary considerably depending on whether you had a general anesthetic or a spinal anesthetic. We have had great success in managing pain with a combination of primarily oral, but also intravenous (IV), medication. Some of these medications will be given on a predetermined schedule, while others will be given at your request depending on your pain level.
14 Your IV line is usually left in place for hours so that you can be given adequate fluids and also so that necessary antibiotics can be given. Antibiotics help to prevent infection in your knee. Most patients will be allowed and encouraged to get up out of bed on the day of surgery. At a minimum, you will sit or stand at the bedside and/or to a chair or commode. Voiding is usually difficult following spinal anesthesia. Therefore, many patients will have a catheter placed in the OR, and it is usually removed the morning after surgery. Your surgical bandages will be removed early afternoon of your first post-op day. You will now begin the important rehabilitation process. The success of this program greatly depends on the cooperation and enthusiasm of the patient. The goals of physical therapy are to increase knee range of motion, build muscle strength and endurance, learn to walk with crutches, and to become independent with daily activities. Physical therapists will work with you each day, emphasizing the importance of muscle strengthening and knee mobility. You will be instructed to a limited number of exercises, which you will continue throughout your hospitalization and upon your return home. They will also initiate walking with a walker or crutches. Finally, they will teach you to navigate stairs safely. Nurses and other clinic personnel will assist the patient in walking with either a walker or crutches at least three times per day. Some patients may use a CPM (continuous passive motion) machine, which is a motorized device that helps you bend your knee. Typically, this device will be used twice a day for one to two hours. The knee motion allowed by the CPM will be increased with each use. It is very important that you fully extend or straighten your knee while using the CPM. DAY 1 All patients will be up and walking the first day after surgery. Your diet will be progressed as long as you are not nauseated. The surgical dressing will be removed and a small fish net dressing will be applied. This knee dressing will be changed each day, and the wound will be cleaned with alcohol. You can expect a moderate amount of swelling and bruising of the knee at this time. It will take several months for this swelling to completely resolve. An IV line will be continued through which fluids and antibiotics will be given for the first hours. Blood transfusions, if necessary, will be given through the same IV.
15 The use of blood thinner begins on the day of surgery. This will either require a small injection daily or the use of Coumadin or aspirin by mouth. In addition, many patients will use the foot pumps, which enhance circulation and diminish the risk of blood clots. These foot pumps are used at all times while in bed. Because of advanced surgical techniques and pain management advances, some patients are able to be discharged home the day after surgery. This is a decision that will be made between you and your surgeon. DAY 2 The intravenous (IV) line will be discontinued on the second day. A physical therapist will again work with you on knee mobility and strengthening exercises as well as ambulation with walker or crutches. The nursing staff and a PT will continue your walking activities at least three times per day. It is our hope that you will be able to walk a greater distance each time. You are allowed and encouraged to place as much weight as is comfortable on the operating leg. A walker or crutches are merely for balance and security. Additional blood tests will be obtained periodically during your hospitalization. Patients will be ready for discharge from the hospital when they have demonstrated satisfactory independence with their walking and necessary daily activities. Most patients are ready for discharge the afternoon or evening of the second day after surgery. DAYS 3-4 In the unlikely event that progress is slower than expected, one or two additional days of hospitalization may be helpful. Your rehabilitation program, including physical therapy, occupational therapy, and ambulation, will progress. HELP AFTER SURGERY HOME OR REHABILITATION FACILITY Nurses and social services will begin to help you make plans for any additional help you might need after returning home. We strongly encourage a capable family member or friend to be available 24/7 for the first week at home. If you need further assistance with your rehabilitation, you may go to a skilled nursing facility at your physician s recommendation. Patients who live alone or who have undergone bilateral knee replacement surgery are more likely to require a short stay in a skilled nursing facility. At the skilled nursing facility, you will be given assistance with your daily activities and will undergo additional physical therapy until you become independent with necessary activities. Most people stay for 5 to 10 days. These arrangements are completed at the hospital by a social worker. Upon your physician s recommendation, the social worker will make contact with you and discuss skilled nursing facility options. Whenever possible, the social worker will take your facility preferences into consideration. Transportation to the skilled facility is generally not covered by insurance companies and is the responsibility of the patient and their family.
16 RETURNING HOME assistance. If considerable help is necessary and if you live alone, transferring to an extended care facility where both nursing care and physical therapy are available may be required. ACTIVITY. We encourage you to be as active as possible. You should not spend too much time in bed other than at night to sleep. You should walk several times daily. These walks are by far the most important exercise you can do. As your recovery progresses, you should be able to walk longer distances and with less fatigue. Be careful not to push yourself too hard too quickly. You should continue to use your crutches until you obtain further instructions at your first office visit. Most patients are ready to progress to the use of a cane after only two weeks following surgery. EXERCISES. As noted previously, walking is the most important exercises. In addition, you should continue to work on the exercises that were started in the hospital under the direction of the physical therapist. These exercises are described further in a later section of this pamphlet. By the time of discharge, we expect you to be able to walk independently with crutches (or a walker), bend your knee to nearly 90 degrees (right angle), and lift your leg with the knee extended straight. The following instructions are intended to help make your return home as comfortable as possible. Since everyone s home situation varies, some patients may require additional assistance upon returning home. Either social services or home healthcare can arrange this PHYSICAL THERAPY. Supervised physical therapy following discharge after total knee replacement is determined on a case-by-case basis. Numerous follow-up studies have shown that patients may do just as well with a home exercise program and without the use of a home CPM machine. If needs require, however, we will certainly arrange for outpatient physical therapy. BATHING. You may begin to shower as soon as two days after surgery. Bathing in a tub is acceptable after your wound is healed but is usually difficult for one to two months until your knee becomes more comfortable. Neither a shower nor a bath is harmful to your incision.
17 INCISION. At the time of your discharge, your incision will be swollen and a small amount of drainage will still be present on the dressing. You should clean the wound daily with alcohol and apply a new dressing until the wound is completely dry. In most cases, no skin sutures will need removal. If the incision becomes excessively swollen, red, or begins to drain, you should notify us. It is not unusual for the knee to remain swollen, feeling warm and tight, for several months after surgery. Elevating the knee above the heart will help with swelling. RETURN APPOINTMENT. Your first return examination in our office will occur about days after being discharged from the hospital for the purpose of assessing your progress. In most instances, you will be given an appointment card at the time of your discharge. If for some reason, you do not receive an appointment or if your appointment time is not convenient, please call our office during normal office hours for a new appointment time. for the use of these injections if you are required to use them. Other patients will also be given a prescription for Coumadin (blood thinner) at the time of discharge. Patients requiring the use of Coumadin for an extended period of time will be asked to have their blood monitored with a blood test (PT/INR). Other patients will use aspirin alone. RECOVERY. Keep in mind that, although we expect a patient to be able to walk without crutches or a cane within 4 weeks of their surgery, full recovery and maximum comfort often require 6 or more months. If comfort or weakness requires the use of crutches for longer than 4 weeks, the long-term success of your total joints will not be affected. DRIVING. You need to be able to control your leg well before you resume driving. Typically, this occurs 2 to 4 weeks after surgery. We will advise you when we feel it is appropriate for you to resume driving. TRAVELING. It is reasonable to travel by car or plane soon after leaving the hospital. When traveling long distances, you will be more comfortable if you stop and walk a little every hour. This will also reduce your risk of blood clots. When traveling by air, the artificial joints usually set off airport security metal detectors and will require individual screening. Cards documenting your knee replacement are not necessary to clear airport security. MEDICATIONS. Most patients will require the occasional use of medications following discharge from the hospital. We will provide a prescription for an appropriate medication. In addition, you should resume any other medications you were taking prior to hospitalization unless otherwise instructed by a physician. Some patients will receive a low molecular weight heparin, such as Fragmin or Lovenox, that requires continuing the small injections under the skin. You will be provided with specific home instructions
18 TOTAL KNEE EXERCISE PROGRAM The goals of any knee exercise program are to build muscle strength and endurance and to increase lower extremity mobility and function. These exercises are taught during the post-operative recovery period by your physical therapist. Each exercise should be performed 2 to 3 times per day for at least 3 months following your surgery. Quadriceps Setting 1. Lie on your back with both knees out as straight as possible. 2. Tighten the muscles on top of your thigh by pressing the back of your knee down into the surface. 3. Keep your toes pointed straight up. 4. Hold for 5 seconds, and then relax. 5. Repeat 10 times. Sitting Knee Stretch Bending 1. Sit in a straight chair. Feet flat on the floor. 2. Slide back the foot of your operated leg. 3. Scoot your buttocks to the edge of the chair until a stretch is felt in the knee. Keep both feet flat on the floor. 4. Hold for 10 seconds, and then relax. 5. Repeat 10 times. 6. To assist the knee in bending more, cross the opposite ankle over the operated ankle and use gentle pressure to push the foot back. 7. If a rocking chair is available, slow, gentle motion for 20 minutes twice daily may be beneficial. Sitting Knee Stretch Straightening Straight Leg Raise 1. Lie on your back with the opposite knee bent and foot flat on bed. 2. Tighten the muscle on top of your thigh (do a quad set). 3. Lift the leg about 12 inches off the bed. 4. Keep the knee straight and toes pointed up throughout the exercise. 5. Hold for 5 seconds. 6. Slowly return to the starting position and relax. 7. Repeat 10 times. 1. Sit in a chair with your lower leg placed on another chair or footstool of the same height. 2. Press your knee down until fully straight. Keep your foot pointed up throughout. 3. To do this, tighten the muscles on top of your thigh or gently press down on your thigh. 4. Hold for 30 seconds, and then relax. 5. Repeat 10 times. 6. Decrease the number of repetitions of any exercise that produces pain that is lasting. 7. While leg is in extension, apply a 5-10 lb. soft weight to the top of the knee and leave in extension for 5-10 minutes.
19 COMMON QUESTIONS COMMON QUESTIONS AND CONCERNS FOLLOWING TOTAL KNEE REPLACEMENT 1. Patients will commonly experience a click in their knee. This is normal and should not cause concern and typically disappears. 2. All patients will experience some numbness or diminished feeling over the front of their knee in the area along the scar following the surgery. This numbness will gradually improve over the first year but will never completely disappear. 3. Kneeling and squatting are perfectly acceptable activities but never become as easy as in a normal knee. 4. Stiffness or tightness in the knee is a very common concern but also tends to diminish over time, although, it often never completely resolves. Patients particularly complain of stiffness after a period of sitting or inactivity. 5. It is unlikely that your knee will bend or flex any further than it did prior to your surgery. In some patients with particularly stiff knees, flexion may improve. 6. Some patients experience continued swelling in their joint of a mild degree indefinitely. Rarely is there a good explanation for this situation, but fortunately, it causes only mild symptoms. 7. Remember that you can expect some improvement in pain, swelling, comfort, and motion for a minimum of 6 months, and often 12 months, after the surgery. 8. Patients who experience particular difficulty in regaining their knee flexion may benefit from a knee manipulation with anesthesia. This option will be discussed with you if necessary by your surgeon. SUMMARY Total knee replacement is extremely effective in relieving the pain of arthritis. Most people with a total knee will continue to enjoy pain-free activity for many years after their surgery.
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
HIP & KNEE SURGERY PATIENTS
 HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
.org. Total Knee Replacement. Anatomy
 Total Knee Replacement Page ( 1 ) If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to
Total Knee Replacement Page ( 1 ) If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
What is Osteoarthritis? Who gets Osteoarthritis? What can I do when I am diagnosed with Osteoarthritis? What can my doctor do to help me?
 Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Fine jewelry is rarely reactive, but cheaper watches, bracelets, rings, earrings and necklaces often contain nickel.
 BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
PALM BEACH ORTHOPAEDIC INSTITUTE, P.A. FAQ: OUT-PATIENT SURGERY
 DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
Rehabilitation After Your Total Knee Replacement
 1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard
1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
AFTER TOTAL KNEE REPLACEMENT. Living with Your New Knee
 AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION
 KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Procedure Information Guide
 Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
HIP JOINT REPLACEMENT
 HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Hip Replacement Surgery
 Hip Replacement Surgery Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures.
Hip Replacement Surgery Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures.
Total knee replacement Uni-compartmental knee replacement
 Your Knee Replacement at the Nuffield Orthopaedic Centre A patient s guide to: Total knee replacement Uni-compartmental knee replacement Welcome to Team Two at the NOC. Together you and your surgeon have
Your Knee Replacement at the Nuffield Orthopaedic Centre A patient s guide to: Total knee replacement Uni-compartmental knee replacement Welcome to Team Two at the NOC. Together you and your surgeon have
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
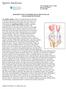 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Total Knee Replacement
 Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Before Surgery You will likely be asked to see your family physician or an internal medicine doctor for a thorough medical evaluation.
 Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee Replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee Replacement or arthritis management. All decisions about
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Should I have a knee replacement?
 Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Rehabilitation After Your Total Hip Replacement
 1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Hip Replacement Whether you have just begun exploring treatment options or have already
1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Hip Replacement Whether you have just begun exploring treatment options or have already
Arthritis www.patientedu.org
 written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Delivering Excellence. Nuffield Orthopaedic Centre NHS Trust. Information for Patients. Hip and Knee service. Total Knee Replacement NHS
 www.noc.nhs.uk/hipandknee/default.aspx Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Total Knee Replacement Information for Patients Hip and Knee service Delivering Excellence Contents Page
www.noc.nhs.uk/hipandknee/default.aspx Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Total Knee Replacement Information for Patients Hip and Knee service Delivering Excellence Contents Page
MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty
 Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Shoulder Joint Replacement
 Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
The Total Ankle Replacement
 The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
Total Knee Replacement
 Chester Knee Clinic at The Grosvenor Nuffield Hospital Wrexham Road Chester CH4 7QP website: www.kneeclinic.info email: info@kneeclinic.info Total Knee Replacement Knee Anatomy Sitting, standing, and walking
Chester Knee Clinic at The Grosvenor Nuffield Hospital Wrexham Road Chester CH4 7QP website: www.kneeclinic.info email: info@kneeclinic.info Total Knee Replacement Knee Anatomy Sitting, standing, and walking
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
Understanding Total Hip Replacement
 Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Further information You can get more information and share your experience at www.aboutmyhealth.org
 OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
PERIACETABULAR OSTEOTOMY SURGERY
 1 PERIACETABULAR OSTEOTOMY SURGERY It is important to us that all of our patients know what to expect before surgery, during their hospitalization and after surgery. Office Visits Planning begins with
1 PERIACETABULAR OSTEOTOMY SURGERY It is important to us that all of our patients know what to expect before surgery, during their hospitalization and after surgery. Office Visits Planning begins with
TOTAL KNEE REPLACEMENT
 PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
Total elbow joint replacement for rheumatoid arthritis: A Patient s Guide
 www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
Total Knee Replacement. Patient Information
 Total Knee Replacement Patient Information Introduction: We would like to thank you for choosing The Institute for Advanced Bone and Joint Surgery at St. Joseph s/ Candler for your Total Joint Replacement
Total Knee Replacement Patient Information Introduction: We would like to thank you for choosing The Institute for Advanced Bone and Joint Surgery at St. Joseph s/ Candler for your Total Joint Replacement
 Total Hip Replacement Hip replacement surgery, or arthroplasty, uses implants to resurface and replace the bones in the joint, re-creating the smooth gliding surfaces that were once intact. Hip replacement
Total Hip Replacement Hip replacement surgery, or arthroplasty, uses implants to resurface and replace the bones in the joint, re-creating the smooth gliding surfaces that were once intact. Hip replacement
Total Knee Replacement
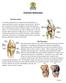 Total Knee Replacement The Knee Joint A total knee replacement, also called total knee arthroplasty, is a surgery performed to remove and replace your knee joint. The knee joint, comprised of the femur
Total Knee Replacement The Knee Joint A total knee replacement, also called total knee arthroplasty, is a surgery performed to remove and replace your knee joint. The knee joint, comprised of the femur
Anterior Approach. to Hip Replacement Surgery
 Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
Post Surgical Care of Patella Luxation Repair
 Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
UK HealthCare Sports Medicine Patient Education December 09
 Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Total Joint Replacement
 Total Joint Replacement Brinceton M. Phipps MD Animas Orthopedic Associates 575 Rivergate Lane, Suite 105 Durango Colorado 970-259-3020 www.brincetonphippsmd.com www.animasorthopedics.com Frequently Asked
Total Joint Replacement Brinceton M. Phipps MD Animas Orthopedic Associates 575 Rivergate Lane, Suite 105 Durango Colorado 970-259-3020 www.brincetonphippsmd.com www.animasorthopedics.com Frequently Asked
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Knee Replacement: Information for Patients and Carers
 Directorate of Surgical Care Department of Orthopaedics Knee Replacement: Information for Patients and Carers This information is for patients who are considering having a knee replacement. What is a Knee
Directorate of Surgical Care Department of Orthopaedics Knee Replacement: Information for Patients and Carers This information is for patients who are considering having a knee replacement. What is a Knee
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
Orthopaedic Surgery Center of Joint Preservation and Replacement After Total Hip Replacement Discharge Instructions
 Congratulations on your new hip! You are going home after a successful total hip replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep
Congratulations on your new hip! You are going home after a successful total hip replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery
 Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Orthopaedic Surgery Center of Joint Preservation and Replacement After Total Knee Replacement Discharge Instructions
 Congratulations! You are going home after a successful total knee replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep breath and relax.
Congratulations! You are going home after a successful total knee replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep breath and relax.
Patella Realignment Tibial Tuberosity Transfer with Lateral Release
 Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
Cartilage Repair Center
 Cartilage Repair Center Tom Minas, MD, MS 850 Boylston Street, Suite 112 Andreas Gomoll, MD Chestnut Hill, MA 02467 Courtney VanArsdale, PA-C P: 617-732-9967 Lindsey Oneto, PA-C F: 617-732-9272 (Minas)
Cartilage Repair Center Tom Minas, MD, MS 850 Boylston Street, Suite 112 Andreas Gomoll, MD Chestnut Hill, MA 02467 Courtney VanArsdale, PA-C P: 617-732-9967 Lindsey Oneto, PA-C F: 617-732-9272 (Minas)
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Post-Operative Exercise Program
 785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
