The use of osseointegrated implants as a foundation for the prosthetic replacement
|
|
|
- Ethelbert Russell
- 8 years ago
- Views:
Transcription
1 The Association Between the Failure of Dental Implants and Cigarette Smoking Crawford A. Bain, BDS, DDS, MSEd/Peter K. Moy, BSc, DMD This paper reviews the outcome of 2,194 Brånemark implants placed in 540 patients by one of the authors over a 6-year period. The overall failure rate of 5.92% is consistent with other studies; however, when patients were subdivided into smokers and nonsmokers, it was found that a significantly greater percentage of failures occurred in smokers (11.28%) than in nonsmokers (4.76%) (P <.001). These differences were significant for all areas except the posterior mandible. While failure rates decreased with increasing implant length, failure rates for each implant length were consistently higher in smokers than in nonsmokers. The possible mechanisms of failure in smokers are discussed, and a protocol for cessation of smoking around the time of surgery is proposed. (INT J ORAL MAXILLOFAC IMPLANTS 1993;8: ) Key words: Brånemark implants, failure, implant length, implant location, osseointegration, smoking/adverse effects The use of osseointegrated implants as a foundation for the prosthetic replacement of missing teeth has become widespread in the last decade. By the use of a gentle surgical technique in sterile conditions, a healing period free of loading, and the development of macroretentive commercially pure titanium implants, a predictable level of success in the integration of implants with bone has been achieved. Since 1977, several retrospective studies have reviewed success rates of both individual implants and implant-supported prostheses, initially in completely edentulous and more recently in partially edentulous patients.1-12 While these studies present large sample sizes and important data on longer-term implant success, they have generally focused on the high levels of success and spent little time analyzing factors involved in the failures that occurred. Although the 5- to 9-year success rates of Adell et al2 are impressive and widely quoted, the authors offer little discussion on the much higher failure rates in the first 5 years of the study. Similarly, van Steenberghe and coworkers' multi-centered study of partially edentulous patients mentions two patients who lost all seven implants placed, but these were not included in the statistical analysis because of incomplete data.9 Several case reports identify patients who have lost an above-average number of implants9,13,14; but in general, retrospective studies have focused on success rates. A notable exception is Jaffin and Berman's paper,15 which identified a much higher failure rate in type IV bone than in all other bone types. Our own unpublished data
2 confirm this, though our failure rate in type IV bone (13.51%) was somewhat lower. Most surgical technique publications identify various local anatomic factors, as well as a few general systemic conditions, that may decrease the possibility of successful integration. Commonly, poor bone quality and quantity, as well as proximity to vital structures, are cited as negative factors. Uncontrolled diabetes, blood dyscrasias, osteoporosis, alcoholism, psychiatric conditions, high levels of head and neck radiotherapy, and general surgical contraindications are among factors that may systemically decrease the potential for implant success Few, if any, studies exist that show a lower implant success rate when patients are treated in the presence of such systemic factors. Smoking has long been identified as harmful to general health. Smokers have a much higher incidence of lung cancer and cardiovascular diseases, together with several other conditions.19 In both animal and human studies, it has repeatedly been shown that smoking compromises healing potential in the treatment of duodenal ulcers,20 plastic surgery21,22 and vascular surgery.23 In the dental field, Meeghan et al24 identified smoking as a major predisposing factor in the occurrence of painful sockets after tooth extraction. They showed that blood fill in postoperative sockets was significantly reduced in smokers, and that maxillary sockets filled more poorly than those in the mandible. Smoking has also been associated with poorer healing after mucogingival surgery25 and is associated with higher rates of refractory periodontitis.26 Cryer et al27 demonstrated an increase in serum levels of norepinephrine and epinephrine in smokers, while Mosely et al28 showed that nicotine inhibited wound healing in a rabbit ear model. Clarke et al29 showed a severe reduction in gingival circulation in rabbits exposed to intra-arterial nicotine. The direct cutaneous vasoconstrictive action of nicotine; increased platelet aggregation; increased levels of fibrinogen, hemoglobin, and blood viscosity; excess levels of carboxyhemoglobin in blood; compromised polymorphonuclear neutrophil (PMN) leukocyte function 30,31; as well as increased platelet adhesiveness have also been hypothesized as mechanisms by which smoking compromises wound healing.32,33 To date, no evaluation has been made of the outcome of dental implants placed in smokers as compared with nonsmokers. The purpose of this study was to evaluate the influence of smoking on the failure rate of Brånemark dental implants placed by one of the authors (PKM) over a period of 6 years. Materials and Methods A total of 2,194 Brånemark implants (Nobelpharma USA, Chicago) were placed in 540 patients between 1984 and These included completely and partially edentulous arches, as well as single-tooth replacements. Both fixed and removable (overdenture) prostheses were included. The patient population consisted of 311 women (57.6%) and 229 men (42.4%).
3 After a complete medical and dental history, thorough clinical and radiographic evaluations including, as indicated, periapical, panoramic, conventional, and computerized tomographic films; diagnostic casts; and consultation with the restorative dentist were carried out. Patients were presented with treatment options and advised of the potential problems associated with dental implants, and an informed consent form was signed. Patients were not accepted for implant surgery if they were medically contraindicated for elective surgery or had unrealistic expectations. All implants were placed under sterile conditions, following the Brånemark protocol, which has been described elsewhere.34 After the appropriate healing period, the implants were exposed, abutments were connected, and patients became involved in the prosthetic stage of therapy. To be included in this study, patients completed abutment connection by March 31, 1991, and postabutment connection radiographs had to be available. These were generally panoramic radiographs or, on occasion, periapical radiographs. All patient records, histories, and radiographs were reviewed; all implant locations were recorded appropriately as posterior maxilla, anterior maxilla, posterior mandible, or anterior mandible; and all implant failures were recorded. While the criteria for failure outlined by Albrektsson et al35 were considered to be optimal, it was not feasible to assess mobility in a study based on radiographic and chart review. Accordingly, an implant was considered to be a failure when: 1. It had been removed for any reason. 2. Radiographic bone loss in excess of 50% of the fixture length was seen on nonstandardized post-treatment radiographs. These criteria may preclude identifying some failing implants according to the Albrektsson et al criteria35; however, they are considered to be realistic and practical in identifying unambiguous implant failure in a chart-review-based study. As part of their medical history, patients were asked whether they smoked. This information was assessed in relation to the success or failure of each implant, and a failure rate was established for both smoking and nonsmoking groups. No attempt was made to quantify the smoking, since this information could be considered unreliable. Data were assessed in relation to location (by sextant) and to implant length. Since bone quality was only recorded routinely after 1985, it was not evaluated in this study. A computerized chi square test was used to compare the two groups by whole mouth and by sextant. Assessment was by individual implant, rather than by patient, since implants placed in each patient were often of various lengths and placed in sites of differing bone quality.
4 Results A total of 2,194 implants in 540 patients met the inclusion criteria for the study. Of these, 1,255 implants were placed in 311 female patients and 939 implants in 229 male patients. The average age of the female patients was years (range 12 to 86) and of the male patients years (range 15 to 84). There was no significant difference between the mean ages of males and females, nor between the number of implants per patient placed in each group. No difference was found in the age, gender, number of implants per patient, or average implant length between smoking and nonsmoking groups. The time following stage 2 surgery ranged from 1 to 81 months, with a mean of months (36.59 months in smokers and months in nonsmokers). Based on the criteria for failure outlined above, 130 of the 2,194 implants were classified as failures. An additional 23 implants remained buried and were classified as "sleepers." Thus the overall failure rate was 5.92% (excluding "sleepers"), which is consistent with other studies. When patients were divided into smoking and nonsmoking groups, it was found that 390 implants (17.78%) had been placed in smokers and 1,804 implants (82.22%) in nonsmokers. Of the 390 implants placed in smokers, 44 were classified as failures (a failure rate of 11.28%), while of the 1,804 implants placed in nonsmokers, only 86 implants failed (a failure rate of 4.76%). There was a statistically significant difference between the failure rate in the smoking and nonsmoking groups (P <.001). Analysis of the different regions of the mouth revealed that overall failure rates were highest in the posterior maxilla and lowest in the anterior mandible (Table 1). Smokers had higher failure rates in all regions. Only in the posterior mandible was there no significant difference between smokers and nonsmokers (Table 2). The 23 "sleeping" implants were all radiographically healthy and were distributed between smokers (7) and nonsmokers (16). If these were included in the overall failure rate, it increased to 6.97%. Since they all appeared to be integrated from the radiographic perspective and were left unconnected for either positional, esthetic, or psychological reasons, it was felt inappropriate to include them as "failures" when assessing the individual groups. When fixture length was considered, it was found that in the maxilla, failure rates of shorter implants in smokers were extremely high and in several cases exceeded the 25% rate, which is Albrektsson et al's proposal for a maximum acceptable level of failure (Tables 3 to 6). Discussion The findings of this study for the first time identify smoking as a major factor in implant failure. This is not surprising when one considers other areas of the medical 36
5 and dental literature. Smoking has been identified by Battalia et al36 as the most important risk factor for both nonhealing (P =.04) and recurrence (P =.0025) of gastric ulcers. Mosely and Finseth37 found that when arteriosclerotic patients continued to smoke, healing of hand wounds was impaired. They further suggest that this impaired healing is also found in smokers without arteriosclerosis.28 Siana et al 38 found unsatisfactory scarring after gynecological surgery in 14 of 69 smokers and 0 of 51 nonsmokers (P <.002). In the area of microvascular surgery, Herring et al23 showed a much higher deterioration in both Dacron arterial grafts (P=.008) and vein grafts when the patients were smokers. In the plastic surgery literature, Rees et al39 reported a higher rate of skin slough after rhytidectomy in smokers, while Riefkohl et al21 identified an association between cutaneous occlusive vascular disease, cigarette smoking, and skin slough after rhytidectomy. In the dental literature, smoking has been shown to compromise healing after mucogingival surgery,40 and to be associated with greater pocket depth and loss of attachment when age-matched groups of smokers and nonsmokers were compared.41 Preber42 showed a significantly greater reduction in pocket depth after scaling and curettage in nonsmokers than in smokers. Smoking has also been associated with a higher incidence of refractory periodontitis,26 with significant reductions in postextraction sockets filling with blood (P <.01) and with a higher incidence of painful sockets (P <.02).24 As to the actual mechanism of implant failure associated with smoking, a retrospective clinical study can only offer conjecture. Cryer et al27 demonstrated a significant increase in plasma levels of both norepinephrine (P <.01) and epinephrine (P <.05) immediately after 10 minutes of smoking, which persisted for the remaining 20 minutes of the study. Sarin et al43 also showed that smoking a single cigarette reduced the velocity of blood flow to the fingers by over 40% for up to 1 hour. Although nicotine has been shown to cause increased urinary catecholamine excretion in laboratory animals,44 it should also be noted that urinary epinephrine excretion also increased after smoking of nicotine-free cigarettes,45 suggesting an additional influence of other byproducts and/or tars. It has also been shown that smokers have a compromised PMN function when compared with nonsmokers,26,30,31 which may be responsible for a compromised healing response and/or a higher risk of infection in smokers after implant placement. While the systemic vasoconstrictive effect andlor PMN dysfunction induced by smoking may well influence initial wound healing adjacent to newly placed implants, Shuler,46 and Armitage and Turner47 showed that nicotine also had a localized vasoconstrictive effect by being absorbed through the oral mucosa into the blood vessels during smoking. Thus the dental implant may be doubly at risk. If local absorption was a significant factor it could well account for lower failures in smokers in the posterior mandible, which is the area most remote and protected by the tongue from local influences of smoking. This hypothesis is currently being
6 investigated by comparison of the failure rates described in this study with failure rates in extraoral sites of osseointegrated implants in smokers and nonsmokers,25 and if validated, may give some encouragement for smokers who use a nicotine patch around the time of implant placement. If one accepts that smoking has a detrimental effect on implant prognosis, the next logical question is how long the potential implant patient who smokes will have to abstain to have an equal prognosis with the nonsmoker. To establish this with any certainty, a future prospective study will be necessary. However, it may well be feasible to first confirm that smoking is equally detrimental in an animal model system, then evaluate the effects of different periods of abstinence on implant prognosis. A method similar to Brånemark's original vital microscopic studies48 of vascular function might also be useful for evaluating the effects of smoking on the microvascular system adjacent to an integrating implant in an animal model. This could establish whether vasoconstriction and/or platelet aggregation in the proximity of the implant were influenced by smoking. In the absence of any directly related dental literature, one is left to extrapolate guidelines for smoking abstinence from medicine. Webster et al22 suggest that patients cease smoking for several weeks before and at least 2 weeks after plastic surgery, while in the same discipline Kaye49 advises abstinence 2 weeks before and 1 week after surgery. Riefkohl et al21 suggest that cessation from the day before until 5 days after plastic surgery will allow nicotine clearance and an elimination of increased vasoconstriction, as well as a resolution of any carboxyhemoglobin-induced hypoxia. They feel that 5 days postoperatively will be sufficient to allow flap revascularization. All of these recommendations relate to soft tissue healing and are essentially untested in any prospective study. It seems likely that the longer time frame associated with osseous healing and the osseointegration process would require a longer period of abstinence. In the absence of any research-based data, we would suggest that the patient cease smoking at least 1 week prior to surgery to allow reversal of higher levels of platelet adhesion and blood viscosity, as well as the shorter-term effects associated with nicotine. The patient should continue to avoid tobacco for at least 2 months after implant placement, by which time bony healing will have progressed to the osteoblastic phase, and early osseointegration should be established. It is realized that this period will be perceived by some as unrealistic as far as compliance is concerned; however, it has a biologic rationale. When informed consent is obtained, careful clarification of the harmful effects of smoking, together with an establishment of the patient's responsibilities in achieving the best prognosis, will ensure the best obtainable level of compliance as well as cover the clinician in the event of implant failure in a noncompliant patient. These recommendations, while based on a sound biologic rationale, are as yet not substantiated by clinical research data. While this study establishes smoking as a significant factor in the failure of
7 dental implants, it would be naive to assume that it is either the only or the most significant factor. Further research is necessary to identify other possible factors that contribute to failure, as well as the possible relationship of the coexistence of several factors in the same individual. Once these factors have been identified, it may then be feasible to use multiple regression analysis to develop a formula whereby a more meaningful, customized prognosis is established for each patient. It is hoped that second-generation clinical research in implant dentistry will focus more on identifying causes for failure than on presenting high success rates, manipulated by creative statistical analysis to present the various systems in the best possible light. It is a well-worn truism that more is learned from failures than successes, and it appears likely that the selection of one implant system over another has less potential to increase success rates than does careful and comprehensive patient selection based on a clear understanding of factors that have been shown to contribute to implant failure. This, combined with an honest presentation of the individual patient's prognosis based on evaluation of the pertinent factors, can only enhance overall success and patient satisfaction. Conclusions This study identifies smoking as a significant factor in increasing the potential failure rate of dental implants. The overall failure rate of 5.92% is consistent with other reported studies. This study further identifies that implant success is poorest in the posterior maxilla and best in the anterior mandible. In all areas except the posterior mandible, the failure rate in smokers was significantly higher than in nonsmokers. When implant length was considered, smokers had consistently higher failure rates than nonsmokers. The maxillary failure rates for shorter implants in smokers exceeded previously proposed acceptable levels. To date, no clear evidence exists as to the mechanism whereby smoking contributes to the failure of dental implants. This paper identifies potential areas of future research to investigate this mechanism and recommends a cessation protocol that, though based on a sound biologic rationale, requires experimental verification in a prospective study. More research is also necessary into other factors that contribute to implant failure, and to potential interrelationships where more than one factor is present in any given patient.
8 1. Brånemark P-I, Hansson BO, Adell R, Breine U, Lindstrom J, Hallen O, Ohman A. Osseointegrated implants in the treatment of the edentulous jaw. Scand J Plast Reconstr Surg 1977;11(suppl 16). 2. Adell R, Lekholm U, Rockler B, Brånemark P-I. A 15-year study of osseointegrated implants in the treatment of the edentuous jaw. Int J Oral Surg 1981;l0: Adell R, Eriksson B, Lekholm U, Brånemark P-I, Jemt T. A long-term follow-up study of osseointegrated implants in the treatment of totally edentuous jaws. Int J Oral Maxillofac Implants 1990;5: Albrektsson T, Dahl E, Enbom L, Engevall S, Engquist B, Eriksson AR, et al. A Swedish multi-centered study of 8139 consecutively inserted Nobelpharma implants. J Periodontol 1988;59: Albrektsson T. A multi-centered report on osseointegrated oral implants. J Prosthet Dent 1988;60: Zarb G, Schmitt A. The longitudinal clinical effectiveness of osseointegrated dental implants: The Toronto study, Part 1. Surgical results. J Prosthet Dent 1990;63: Zarb G, Schmitt A. The longitudinal clinical effectiveness of osseointegrated dental implants: The Toronto study, Part 2. The prosthetic results. J Prosthet Dent 1990;64: Buser DA, Schroeder A, Sutter F, Lang NP. The new concept of ITI hollow-cylinder screw implants: Part 2. Clinical aspects, indications and early clinical results. Int J Oral Maxillofac Implants 1988;3: Kirsch A, Ackerman KL. The IMZ osseointegrated implant system. Dent Clin North Am 1989;33: Patrick D, Zosky J, Lubar R, Buchs A. The longitudinal clinical effectiveness of Core-Vent dental implants. A 5 year report. J Oral Implantol 1989;15: Kent JN, Block MS, Finger IM, Guerra L, Larsen H, Misiek DJ. Biointegrated hydroxyapatite-coated dental implants: 5 year clinical observations. J Am Dent Assoc 1990;121: van Steenberghe D. A retrospective multicenter evaluation of survival rate of osseointegrated implant fixtures supporting fixed partial prostheses in the treatment of partial edentulism. J Prosthet Dent 1989;61: Engquist B, Bergendal T, Kallus T, Linden U. A retrospective multicenter evaluation of osseointegrated implants supporting overdentures. Int J Oral Maxillofac Implants 1988;3:
9 14. Malmstrom HS, Fritz ME, Timmis DP, VanDyke TE. Osseo-integrated implant treatment of a patient with rapidly progressive periodontitis. J Periodontol 1990;61: Jaffin RA, Bemlan CL. The excessive loss of Brånemark fixtures in type IV bone. J Periodontol 1991;62: Laney WR. Selecting edentulous patients for tissue-integrated prostheses. Int J Oral Maxillofac Implants 1986;1: Lekholm U, Zarb GA. Patient selection and preparation. In: Brånemark P-I, Zarb GA, Albrektsson T (eds). Tissue-lntegrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence, 1987: Beumer J III, Lewis SG. Patient selection and treatment planning. In: Beumer J III, Lewis SG (eds). The Brånemark Implant System: Clinical and Laboratory Procedures. St Louis: Ishiyaku EuroAmerica, 1989: Ball K, Turner R. Smoking and the heart; the basis for action. Lancet 1974;2: Kikendahl JW, Evaul J, Johnson LF. Effects of cigarette smoking on gastrointestinal physiology and non-neoplastic digestive disease. J Clin Gastroenterol 1984;6: Riefkohl R, Wolfe JA, Cox EB, McCarthy KS Jr. Association between cutaneous occlusive vascular disease, cigarette smoking and skin sloughing after rhytidectomy. Plast Reconstr Surg 1986;77: Webster RC, Kazda G, Hamdan US, Fuleihan NS, Smith RC. Cigarette smoking and facelift: Conservative vs. wide undenmining. Plast Reconstr Surg 1986;77: Herring M, Gardener A, Glover J Seeding human arterial prostheses with mechanically derived endothelium The detrimental effect of smoking. J Vasc Surg 1984;1: Meechan JG, MacGregor DM, Rogers SM, Hobson RS, Bates JPC, Dennison M. The effect of smoking on immediate post-extraction socket filling with blood and on the incidence of painful sockets. Br J Oral Maxillofac Surg 1988;26: Moy PK, Bain CA, Sagai T, Beumer J III. Effects of smoking on osseointegrated implants in oral and extra-oral sites. In preparation. 26. MacFarlane GD, Herzberg MC, Wolff LF, Hardie NA. Refractory periodontitis associated with abnormal PMN leukocyte phagocytosis and cigarette smoking. J Periodontol 1992;63: Cryer PE, Haymond MW, Santiago JV, Shah SD. Norepinephrine and epinephrine
10 release and androgenic mediation of smoking associated hemodynamic and metabolic events. New Engl J Med 1976;295: Mosely LH, Finseth F, Goody M. Nicotine and its effects on wound healing. Plast Reconstr Surg 1978;61: Clarke NG, Shephard BC, Hirsch RS. The effects of intra-arterial epinephrine and nicotine on gingival circulation. Oral Surg 1981;52: Noble RC, Penny BB. Comparison of leukocyte count and function in smoking and non-smoking young men. Infect Immun 1975;12: Kenney EB, Kraal JH, Saxe SR, Jones J. The effect of cigarette smoke on human polymorphonuclear leukocytes. J Periodont Res 1977;12: Nadler JL, Velasco JS, Horton R. Cigarette smoking inhibits prostacycline formation. Lancet 1983;1: Lawrence WT, Murphy RC, Robson MC, Heggers JP. The detrimental effect of cigarette smoking on flap survival: An experimental study in the rat. Br J Plast Surg 1984;37: Adell R, Lekholm U, Brånemark P-I. Surgical procedures. In: Brånemark P-I, Zarb GA, Albrektsson T (eds). Tissue-lntegrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence, 1985: Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: A review and proposed criteria for success. Int J Oral Maxillofac Implants 1986;1: Battaglia G, Di Marco F, Piccoli A, Vianello F, Farinati F, Naccarato R. Clinical markers of slow healing and relapsing gastric ulcer. Gut 1987;28: Mosely LH, Finseth F. Cigarette smoking: Impairment of digital blood flow and wound healing in the hand. Hand Clin 1977;9: Siana JE, Rex S, Gottrup F. The effects of cigarette smoking on wound healing. Scand J Plast Reconstr Surg 1989;23: Rees TD, Liverett DM, Guy CL. The effect of cigarette smoking on skin flap survival in the face lift patient. Plast Reconstr Surg 1984;73: Millar PD. Regenerative and reconstrictive periodontal plastic surgery. Dent Clin North Am 1988;32: Bridges RB, Saxe SR, McKean HE. Cigarette smoking and diabetes effects on loss of attachment [abstract 2601]. J Dent Res 1991;70: Preber H. Clinical and therapeutic aspects. In: Preber H (ed). Smoking and Periodontal Disease. Stockholm: Karolinska Institute, 1986:
11 43. Sarin CL, Austin JC, Nickel WO. Effects of smoking on digital blood flow velocity. JAMA 1974;229: Westfall TC, Brase DA. Studies on the mechanism of tolerance of nicotine-induced elevations of urinary catecholamines. Biochem Pharmacol 1971;20: Ague C. Urinary catecholamines, flow rate and tobacco smoking. Biol Physiol 1974;1: Shuler RL. Effects of cigarette smoking on the circulation of the oral mucosa. J Dent Res 1968;47: Armitage AK, Turner DM. Absorption of nicotine in cigarette and cigar smoking through the oral mucosa. Nature 1970;226: Brånemark P-I. Bone marrosv microvascular structure and function. Adv Microcirc 1968;1: Kaye BL. Discussion. Plast Reconstr Surg 1986;77:
12
13
Titanium endosseous implants have
 Smoking and Complications of Endosseous Dental Implants* Devorah Schwartz-Arad, Naama Samet, Nachum Samet, and Avi Mamlider Background: The purpose of this study was to compare the incidence of the complications
Smoking and Complications of Endosseous Dental Implants* Devorah Schwartz-Arad, Naama Samet, Nachum Samet, and Avi Mamlider Background: The purpose of this study was to compare the incidence of the complications
Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan
 Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
An adequate amount of bone, in
 CASE REPORT Immediate Loading of Dental Implant After Sinus Floor Elevation With Osteotome Technique: A Clinical Report and Preliminary Radiographic Results Mario Santagata, MD* Luigi Guariniello, MD,
CASE REPORT Immediate Loading of Dental Implant After Sinus Floor Elevation With Osteotome Technique: A Clinical Report and Preliminary Radiographic Results Mario Santagata, MD* Luigi Guariniello, MD,
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
Leslie Laing Gibbard, BSc, BEd, MSc, PhD, DDS George Zarb, BChD, DDS, MS, MS, FRCD(C)
 A P P L I E D R E S E A R C H A 5-Year Prospective Study of Implant-Supported Single-Tooth Replacements Leslie Laing Gibbard, BSc, BEd, MSc, PhD, DDS George Zarb, BChD, DDS, MS, MS, FRCD(C) A b s t r a
A P P L I E D R E S E A R C H A 5-Year Prospective Study of Implant-Supported Single-Tooth Replacements Leslie Laing Gibbard, BSc, BEd, MSc, PhD, DDS George Zarb, BChD, DDS, MS, MS, FRCD(C) A b s t r a
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
The predictability of attaining osseointegration
 ITI Implant Use in Private Practice: Clinical Results with 5,526 Implants Followed Up to 72+ Months in Function Paul A. Fugazzotto, DDS 1 /James Vlassis, DDS 2 /Bobby Butler, DDS 3 Purpose: To evaluate
ITI Implant Use in Private Practice: Clinical Results with 5,526 Implants Followed Up to 72+ Months in Function Paul A. Fugazzotto, DDS 1 /James Vlassis, DDS 2 /Bobby Butler, DDS 3 Purpose: To evaluate
The rate of success of implants in the edentulous
 Clinical evaluation of single-tooth mini-implant restorations: A five-year retrospective study Paolo Vigolo, Dr Odont, MScD, and Andrea Givani, MD, DDS Vicenza, Italy Statement of problem. Placement of
Clinical evaluation of single-tooth mini-implant restorations: A five-year retrospective study Paolo Vigolo, Dr Odont, MScD, and Andrea Givani, MD, DDS Vicenza, Italy Statement of problem. Placement of
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments
 Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
C HAPTER 4 O RAL AND M AXILLOFACIAL S URGERY
 C HAPTER 4 O RAL AND M AXILLOFACIAL S URGERY I. TREATMENT PLANNING GUIDELINES As part of informed consent, the clinician should carefully explain the risks and benefits of oral and maxillofacial surgery
C HAPTER 4 O RAL AND M AXILLOFACIAL S URGERY I. TREATMENT PLANNING GUIDELINES As part of informed consent, the clinician should carefully explain the risks and benefits of oral and maxillofacial surgery
The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review
 IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
Effects of smoking on the success of dental implants: A literature review
 44 REVIEW ARTICLE Effects of smoking on the success of dental implants: A literature review Manish Goutam 1, Madhvi Singh 2, Deepak Patel 3 1 Intern, Dept. Of Prosthodontics, People's College Of Dental
44 REVIEW ARTICLE Effects of smoking on the success of dental implants: A literature review Manish Goutam 1, Madhvi Singh 2, Deepak Patel 3 1 Intern, Dept. Of Prosthodontics, People's College Of Dental
Implant therapy using osseointegrated implants has
 Natural Tooth Intrusion Phenomenon With Implants: A Survey Lily T. Garcia, DDS, MS*/Larry J. Oesterle, DDS, MS** A common assumption when planning for treatment for a fixed partial denture potentially
Natural Tooth Intrusion Phenomenon With Implants: A Survey Lily T. Garcia, DDS, MS*/Larry J. Oesterle, DDS, MS** A common assumption when planning for treatment for a fixed partial denture potentially
Spedding Dental Clinic. 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk
 DENTAL IMPLANTS Spedding Dental Clinic 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk SPEDDING DENTAL CLINIC Jack Spedding is a partner in Spedding dental clinic. He is a highly
DENTAL IMPLANTS Spedding Dental Clinic 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk SPEDDING DENTAL CLINIC Jack Spedding is a partner in Spedding dental clinic. He is a highly
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Prosthetic treatment planning on the basis of scientific evidence.
 Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Modern Tooth Replacement Strategies & Digital Workflow
 Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Retrospective study on the survival rate of IBS implant
 Retrospective study on the survival rate of IBS implant Date : 30. 05. 2013 Written by : Dr. Je Won Wang, Director of research Approved by : Prof. Min Seung Ki - Contents - 1. Purpose Of Study 2. Materials
Retrospective study on the survival rate of IBS implant Date : 30. 05. 2013 Written by : Dr. Je Won Wang, Director of research Approved by : Prof. Min Seung Ki - Contents - 1. Purpose Of Study 2. Materials
DENT IMPLANT restoring qualit S: of LIfE
 DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
Outcomes of Placing Short Dental Implants in the Posterior Mandible: A Retrospective Study of 124 Cases
 DENTAL IMPLANTS J Oral Maxillofac Surg 67:713-717, 2009 Outcomes of Placing Short Dental in the Posterior Mandible: A Retrospective Study of 124 Cases Bao-Thy N. Grant, DDS,* Franklin X. Pancko, DDS, and
DENTAL IMPLANTS J Oral Maxillofac Surg 67:713-717, 2009 Outcomes of Placing Short Dental in the Posterior Mandible: A Retrospective Study of 124 Cases Bao-Thy N. Grant, DDS,* Franklin X. Pancko, DDS, and
Saudi Fellowship In Dental Implant (SF-DI)
 Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Healing Abutment Selection. Perio Implant Part I. Implant Surface Characteristics. Single Tooth Restorations. Credit and Thanks for Lecture Material
 Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Immediate Molar Implant Placement: A Private Practice Clinical Investigation. Abstract
 Immediate Molar Implant Placement: A Private Practice Clinical Investigation Gargiulo et al Alphonse Gargiulo, DDS, MS 1 Thomas Manos, DDS, MS 2 Mark Kolozenski, DDS, MS 3 Alex Tzanos, DDS, MSD 3 Michael
Immediate Molar Implant Placement: A Private Practice Clinical Investigation Gargiulo et al Alphonse Gargiulo, DDS, MS 1 Thomas Manos, DDS, MS 2 Mark Kolozenski, DDS, MS 3 Alex Tzanos, DDS, MSD 3 Michael
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up
 Article 1 Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up Dr. Gadi Schneider DMD, Specialist in periodontics Dr. Yoram Bruckmayer DMD Long-Term dental Implant Survival
Article 1 Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up Dr. Gadi Schneider DMD, Specialist in periodontics Dr. Yoram Bruckmayer DMD Long-Term dental Implant Survival
Teeth in a Day for the Maxilla and Mandible: Case Report
 Teeth in a Day for the Maxilla and Mandible: Case Report Thomas J. Balshi, DDS, FACP* Glenn J. Wolfinger, DMD, FACP** Abstract Background: A growing body of evidence indicates that successful osseointegration
Teeth in a Day for the Maxilla and Mandible: Case Report Thomas J. Balshi, DDS, FACP* Glenn J. Wolfinger, DMD, FACP** Abstract Background: A growing body of evidence indicates that successful osseointegration
education Although demographic factors and growing patient awareness of the benefits of dental implants
 education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Rehabilitation of Endondontically Failed Anterior teeth by Immediate Replacement and Loading of an Implant supported Crown: A Case Report.
 RESEARCH AND REVIEWS: JOURNAL OF DENTAL SCIENCES Rehabilitation of Endondontically Failed Anterior teeth by Immediate Replacement and Loading of an Implant supported Crown: A Case Report. Lalit Kumar 1
RESEARCH AND REVIEWS: JOURNAL OF DENTAL SCIENCES Rehabilitation of Endondontically Failed Anterior teeth by Immediate Replacement and Loading of an Implant supported Crown: A Case Report. Lalit Kumar 1
RESEARCH. Key Words: crown-implant ratios, proximal bone-to-implant contact. Journal of Oral Implantology 425
 RESEARCH Crown-to-Implant Ratios of Short-Length Implants Hardeep Birdi, DMD, MS 1 * John Schulte, DDS, MSD 1 Alejandro Kovacs, DDS, MS 1 Meghan Weed, RDH 2 Sung-Kiang Chuang, DMD, MD 3 Excessive crown-implant
RESEARCH Crown-to-Implant Ratios of Short-Length Implants Hardeep Birdi, DMD, MS 1 * John Schulte, DDS, MSD 1 Alejandro Kovacs, DDS, MS 1 Meghan Weed, RDH 2 Sung-Kiang Chuang, DMD, MD 3 Excessive crown-implant
THE EVOLUTION OF EXTERNAL AND INTERNAL IMPLANT/ABUTMENT CONNECTIONS
 CONTINUING EDUCATION 2 5 THE EVOLUTION OF EXTERNAL AND INTERNAL IMPLANT/ABUTMENT CONNECTIONS Israel M. Finger, DDS, MS* Paulino Castellon, DDS Michael Block, DMD Nicolas Elian, DDS FINGER 15 8 SEPTEMBER
CONTINUING EDUCATION 2 5 THE EVOLUTION OF EXTERNAL AND INTERNAL IMPLANT/ABUTMENT CONNECTIONS Israel M. Finger, DDS, MS* Paulino Castellon, DDS Michael Block, DMD Nicolas Elian, DDS FINGER 15 8 SEPTEMBER
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
IMPLANT MENTOR PROGRAM
 THE BRIGHTON INSTITUTE FOR DENTAL IMPLANTS IMPLANT MENTOR PROGRAM WITH DR BRUNO SILVA www.brightonimplantclinic.com www.thebrightonimplantinsitute.com Foreword Osseointegrated implants are enabling dentists
THE BRIGHTON INSTITUTE FOR DENTAL IMPLANTS IMPLANT MENTOR PROGRAM WITH DR BRUNO SILVA www.brightonimplantclinic.com www.thebrightonimplantinsitute.com Foreword Osseointegrated implants are enabling dentists
All-on-4 treatment concept with NobelSpeedy Groovy
 All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
A Comprehensive Explanation
 Dental Implants A Comprehensive Explanation Overview Since the 1980s, dental implants have become more popular among dentists and patients. 1 In some clinical situations, implants may be the best treatment
Dental Implants A Comprehensive Explanation Overview Since the 1980s, dental implants have become more popular among dentists and patients. 1 In some clinical situations, implants may be the best treatment
TRI Product NewsFlash. December 2015
 TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
Retention of maxillary implant overdenture bars of different designs
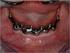 Retention of maxillary implant overdenture bars of different designs Brian H. Williams, DDS, a Kent T. Ochiai, DDS, b Satoru Hojo, DDS, PhD, c Russell Nishimura, DDS, d and Angelo A. Caputo, PhD e School
Retention of maxillary implant overdenture bars of different designs Brian H. Williams, DDS, a Kent T. Ochiai, DDS, b Satoru Hojo, DDS, PhD, c Russell Nishimura, DDS, d and Angelo A. Caputo, PhD e School
The Impact of Oral Implants Past and Future, 1966 2042. Tomas Albrektsson, MD, PhD, ODhc Ann Wennerberg, DDS, PhD
 P R O F E S S I O N A L I S S U E S The Impact of Oral Implants Past and Future, 1966 202 Tomas Albrektsson, MD, PhD, ODhc Ann Wennerberg, DDS, PhD A b s t r a c t This paper traces the history of oral
P R O F E S S I O N A L I S S U E S The Impact of Oral Implants Past and Future, 1966 202 Tomas Albrektsson, MD, PhD, ODhc Ann Wennerberg, DDS, PhD A b s t r a c t This paper traces the history of oral
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
Implants for life? A critical review of implant-supported restorations
 journal of dentistry 35 (2007) 768 772 available at www.sciencedirect.com journal homepage: www.intl.elsevierhealth.com/journals/jden Review Implants for life? A critical review of implant-supported restorations
journal of dentistry 35 (2007) 768 772 available at www.sciencedirect.com journal homepage: www.intl.elsevierhealth.com/journals/jden Review Implants for life? A critical review of implant-supported restorations
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
Curriculum Vitae Frank L. Higginbottom, D.D.S.
 Curriculum Vitae Frank L. Higginbottom, D.D.S. Education Oklahoma University B.S. 1967 Baylor College of Dentistry D.D.S. 1971 Practice Staff Appointments Private Practice of Esthetics, Restorative, and
Curriculum Vitae Frank L. Higginbottom, D.D.S. Education Oklahoma University B.S. 1967 Baylor College of Dentistry D.D.S. 1971 Practice Staff Appointments Private Practice of Esthetics, Restorative, and
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Dental Extractions, Antibiotics and Curettage First, Do no Harm
 Global Journal of Medical research: J Dentistry and Otolaryngology Volume 14 Issue 1 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc.
Global Journal of Medical research: J Dentistry and Otolaryngology Volume 14 Issue 1 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc.
CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT
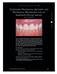 CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
Don t Let Life Pass You By Because Of Missing Teeth
 Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE
 IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 5 JUNE Surgical and restorative techniques that can reduce the loss of hard and soft tissues
IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 5 JUNE Surgical and restorative techniques that can reduce the loss of hard and soft tissues
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment
 Number 3 $1.25 The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment If you are like most people considering dental implants, you probably have
Number 3 $1.25 The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment If you are like most people considering dental implants, you probably have
Dental Implant Failure Rates and Associated Risk Factors
 Dental Implant Failure Rates and Associated Risk Factors Peter K. Moy, DMD 1 /Diana Medina, DDS 2 /Vivek Shetty, DDS, Dr Med Dent 3 /Tara L. Aghaloo, DDS, MD 4 Purpose: To guide treatment planning by analyzing
Dental Implant Failure Rates and Associated Risk Factors Peter K. Moy, DMD 1 /Diana Medina, DDS 2 /Vivek Shetty, DDS, Dr Med Dent 3 /Tara L. Aghaloo, DDS, MD 4 Purpose: To guide treatment planning by analyzing
Osseo-integrated Dental Implant Policy and Guidelines
 Osseo-integrated Dental Implant Policy and Guidelines 1. PURPOSE The purpose of this document is to outline the Department of Veterans Affairs (DVA) policy regarding the provision of dental implant treatment
Osseo-integrated Dental Implant Policy and Guidelines 1. PURPOSE The purpose of this document is to outline the Department of Veterans Affairs (DVA) policy regarding the provision of dental implant treatment
SCD Case Study. Treatment Considerations for Implant Rehabilitation
 SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
Immediate and Delayed Restoration of Dental Implants in Patients with a History of Periodontitis: A Prospective Evaluation up to 5 Years
 Immediate and Delayed Restoration of Dental Implants in Patients with a History of Periodontitis: A Prospective Evaluation up to 5 Years Jacob Horwitz, DMD 1 /Eli E. Machtei, DMD 2 Purpose: To evaluate
Immediate and Delayed Restoration of Dental Implants in Patients with a History of Periodontitis: A Prospective Evaluation up to 5 Years Jacob Horwitz, DMD 1 /Eli E. Machtei, DMD 2 Purpose: To evaluate
Anatomic limitations in the maxilla provide challenges
 Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Taking the Mystique out of Implant Dentistry. Dr. Michael Weinberg B.Sc., DDS, FICOI
 Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Periodontal Screening and Recording: Early Detection of Periodontal Diseases
 Periodontal Screening and Recording: Early Detection of Periodontal Diseases Tanya Villalpando Mitchell, RDH, MS Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce53/ce53.aspx
Periodontal Screening and Recording: Early Detection of Periodontal Diseases Tanya Villalpando Mitchell, RDH, MS Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce53/ce53.aspx
Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants
 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 62:1418-1422, 2004 Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants Eric D. Ferrara,
CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 62:1418-1422, 2004 Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants Eric D. Ferrara,
Implants and all-ceramic restorations in a patient treated for aggressive periodontitis: a case report
 CASE REPORT J Adv Prosthodont 2010;2:97-101 DOI:10.4047/jap.2010.2.3.97 Implants and all-ceramic restorations in a patient treated for aggressive periodontitis: a case report Jin-Sun Hong, DDS, In-Sung
CASE REPORT J Adv Prosthodont 2010;2:97-101 DOI:10.4047/jap.2010.2.3.97 Implants and all-ceramic restorations in a patient treated for aggressive periodontitis: a case report Jin-Sun Hong, DDS, In-Sung
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
Analysis of the 619 Brånemark System TiUnite Implants: A Retrospective Study
 Kobe J. Med. Sci., Vol. 58, No. 1, pp. E19-E28, 2012 Analysis of the 619 Brånemark System TiUnite Implants: A Retrospective Study YASUYUKI SHIBUYA, DDS, PhD* 1, NAOKI TAKATA, DDS, PhD 1, JUNICHIRO TAKEUCHI,
Kobe J. Med. Sci., Vol. 58, No. 1, pp. E19-E28, 2012 Analysis of the 619 Brånemark System TiUnite Implants: A Retrospective Study YASUYUKI SHIBUYA, DDS, PhD* 1, NAOKI TAKATA, DDS, PhD 1, JUNICHIRO TAKEUCHI,
Adramatic increase in the number of dental practitioners
 Risk Management Aspects of Implant Dentistry Navot Givol, DMD 1 /Shlomo Taicher, DMD 2 /Talia Halamish-Shani, LLB 3 /Gavriel Chaushu, DMD, MSc 4 Purpose: To categorize and review complications related
Risk Management Aspects of Implant Dentistry Navot Givol, DMD 1 /Shlomo Taicher, DMD 2 /Talia Halamish-Shani, LLB 3 /Gavriel Chaushu, DMD, MSc 4 Purpose: To categorize and review complications related
Radiographic Vertical Bone Loss Evaluation around Dental Implants Following One Year of Functional Loading
 Original Article Radiographic Vertical Bone Loss Evaluation around Dental Implants Following One Year of Functional Loading AAR. Rasouli Ghahroudi 1, AR Talaeepour 2, A. Mesgarzadeh 3, AR. Rokn 4, 5, A.
Original Article Radiographic Vertical Bone Loss Evaluation around Dental Implants Following One Year of Functional Loading AAR. Rasouli Ghahroudi 1, AR Talaeepour 2, A. Mesgarzadeh 3, AR. Rokn 4, 5, A.
Amajor limitation in the use of most
 Volume 75 Number 6 A Targeted Review of Study Outcomes With Short ( 7 mm) Endosseous Dental Implants Placed in Partially Edentulous Patients D. Hagi,* D.A. Deporter,* R.M. Pilliar,* and T. Arenovich Background:
Volume 75 Number 6 A Targeted Review of Study Outcomes With Short ( 7 mm) Endosseous Dental Implants Placed in Partially Edentulous Patients D. Hagi,* D.A. Deporter,* R.M. Pilliar,* and T. Arenovich Background:
Teeth and Dental Implants: When to save, and when to extract.
 Teeth and Dental Implants: When to save, and when to extract. One of the most difficult decisions a restorative dentist has to make is when to refer a patient for extraction and placement of dental implants.
Teeth and Dental Implants: When to save, and when to extract. One of the most difficult decisions a restorative dentist has to make is when to refer a patient for extraction and placement of dental implants.
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
DENTAL IMPLANT THERAPY
 DENTAL IMPLANT THERAPY PATIENT WELCOME PACK Dr. Syed Abdullah BDS, MSc (Dental Implants) What are dental implants? In the early 1950s, a Swedish Scientist, Per-Ingvar Branemark observed that titanium metal
DENTAL IMPLANT THERAPY PATIENT WELCOME PACK Dr. Syed Abdullah BDS, MSc (Dental Implants) What are dental implants? In the early 1950s, a Swedish Scientist, Per-Ingvar Branemark observed that titanium metal
2016 Buy Up Dental Care Plan Procedure List
 * This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
* This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
IMPLANT DENTISTRY CLINICAL SYLLABUS
 IMPLANT DENTISTRY CLINICAL SYLLABUS RESD 535 MATS H. KRONSTROM, DDS, PhD Course Director DEPARTMENT OF RESTORATIVE DENTISTRY SCHOOL OF DENTISTRY UNIVERSITY OF WASHINGTON 2008 2009 RD 535 - SCHEDULE FALL
IMPLANT DENTISTRY CLINICAL SYLLABUS RESD 535 MATS H. KRONSTROM, DDS, PhD Course Director DEPARTMENT OF RESTORATIVE DENTISTRY SCHOOL OF DENTISTRY UNIVERSITY OF WASHINGTON 2008 2009 RD 535 - SCHEDULE FALL
THE SINGLE-TOOTH IMPLANT TREATMENT FOR MAXILLARY CENTRAL INCISORS LOSS AFTER TRAUMA: CASE REPORTS
 CLINICAL DENTISTRY AND RESEARCH 2011; 35(1): 47-52 THE SINGLE-TOOTH IMPLANT TREATMENT FOR MAXILLARY CENTRAL INCISORS LOSS AFTER TRAUMA: CASE REPORTS Hakan Tuna, DDS, PhD Assistant Professor, Department
CLINICAL DENTISTRY AND RESEARCH 2011; 35(1): 47-52 THE SINGLE-TOOTH IMPLANT TREATMENT FOR MAXILLARY CENTRAL INCISORS LOSS AFTER TRAUMA: CASE REPORTS Hakan Tuna, DDS, PhD Assistant Professor, Department
Restoring quality to life. Dental implants. A naturally better solution. Patient Education
 Restoring quality to life. Dental implants. A naturally better solution. Patient Education Dental implants: A better treatment option. What are dental implants? Dental implants are a safe, medically proven,
Restoring quality to life. Dental implants. A naturally better solution. Patient Education Dental implants: A better treatment option. What are dental implants? Dental implants are a safe, medically proven,
E. Richard Hughes, D.D.S.
 E. Richard Hughes, D.D.S. Docket No. FDA-2012-N-0677 Blade Form Endosseous Dental Implants E. Richard Hughes, D.D.S. 46440 Benedict Dr.,# 201 Sterling, Va. 20164 USA 703-444-1152 erhughesdds@aol.com Diplomate,
E. Richard Hughes, D.D.S. Docket No. FDA-2012-N-0677 Blade Form Endosseous Dental Implants E. Richard Hughes, D.D.S. 46440 Benedict Dr.,# 201 Sterling, Va. 20164 USA 703-444-1152 erhughesdds@aol.com Diplomate,
Dental Implant Options in Atrophic Jaws
 Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros.
 I M P L A N T S in IRRADIATED TISSUES Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros. Adj Associate Professor, National University of Singapore Chair,
I M P L A N T S in IRRADIATED TISSUES Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros. Adj Associate Professor, National University of Singapore Chair,
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Coding and Payment Guide for Dental Services. A comprehensive coding, billing, and reimbursement resource for dental services
 Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Single anterior tooth replacement: clinical approaches
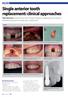 Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Six-Year Survival and Early Failure Rate of 2918 Implants with Hydrophobic and Hydrophilic Enossal Surfaces
 Dent. J. 2015, 3, 15-23; doi:10.3390/dj3010015 Article OPEN ACCESS dentistry journal ISSN 2304-6767 www.mdpi.com/journal/dentistry Six-Year Survival and Early Failure Rate of 2918 Implants with Hydrophobic
Dent. J. 2015, 3, 15-23; doi:10.3390/dj3010015 Article OPEN ACCESS dentistry journal ISSN 2304-6767 www.mdpi.com/journal/dentistry Six-Year Survival and Early Failure Rate of 2918 Implants with Hydrophobic
BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT
 BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT B K Biswas 1 S Bag 2 & S Pal 3 1. Dept. of Dental Surgery, Associate Professor, KPC Medical College & Hospital, Kolkata,
BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT B K Biswas 1 S Bag 2 & S Pal 3 1. Dept. of Dental Surgery, Associate Professor, KPC Medical College & Hospital, Kolkata,
Dental Implant Treatment after Improvement of Oral Environment by Orthodontic Therapy
 Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012
 PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012 Implant placement and restoration involves two major stages: surgical placement of the implant(s) followed by the restoration of the implant after
PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012 Implant placement and restoration involves two major stages: surgical placement of the implant(s) followed by the restoration of the implant after
USE OF DENTAL IMPLANTS IN THE NAVY MEDICAL HEALTH CARE SYSTEM
 DEPARTMENT OF THE NAVY BUR EAU OF MEDICINE AND SURGERY 2300 E STREET NW WASHINGTON DC 20312 5300 I ~ REPt Y REFER TO BUMEDINST 6630.3B BUMED-M3/5 131an2011 BUMED INSTRUCTION 6630.3B From: Chief, Bureau
DEPARTMENT OF THE NAVY BUR EAU OF MEDICINE AND SURGERY 2300 E STREET NW WASHINGTON DC 20312 5300 I ~ REPt Y REFER TO BUMEDINST 6630.3B BUMED-M3/5 131an2011 BUMED INSTRUCTION 6630.3B From: Chief, Bureau
Encode Impression System. Optimization By Design
 The Encode Impression System Optimization By Design Optimization Is Key To Aesthetics The BellaTek Encode Impression System provides optimized solutions to clinicians by eliminating the need for implant
The Encode Impression System Optimization By Design Optimization Is Key To Aesthetics The BellaTek Encode Impression System provides optimized solutions to clinicians by eliminating the need for implant
MINI IMPLANTS FOR LOWER DENTURE STABLIZATION
 MINI IMPLANTS FOR LOWER DENTURE STABLIZATION From the Office of Dr. Michael J. Guy 511A Lakeshore Drive, North Bay ON, P1A 2E3 Mini dental implants (MDI) have become increasingly popular in the past decade
MINI IMPLANTS FOR LOWER DENTURE STABLIZATION From the Office of Dr. Michael J. Guy 511A Lakeshore Drive, North Bay ON, P1A 2E3 Mini dental implants (MDI) have become increasingly popular in the past decade
Replacement of a single front tooth Surgical procedure and three-year results
 Case Report 10 2011 Replacement of a single front tooth Surgical procedure and three-year results Dr Peter Randelzhofer Munich, Germany Prosthetics Dr Peter Randelzhofer studied dentistry in Munich, Germany,
Case Report 10 2011 Replacement of a single front tooth Surgical procedure and three-year results Dr Peter Randelzhofer Munich, Germany Prosthetics Dr Peter Randelzhofer studied dentistry in Munich, Germany,
Straumann. Time-tested
 Straumann Soft TiSSue Level implant System Time-tested Why a Soft Tissue Level implant? Simplicity and efficiency by integrated soft tissue management Straumann Soft Tissue Level implants have a built-in
Straumann Soft TiSSue Level implant System Time-tested Why a Soft Tissue Level implant? Simplicity and efficiency by integrated soft tissue management Straumann Soft Tissue Level implants have a built-in
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Outcomes of dental implant treatment in patients with generalized aggressive periodontitis: a systematic review
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.4.210 Outcomes of dental implant treatment in patients with generalized aggressive periodontitis: a systematic review Kyoung-Kyu Kim*, DDS, MSD, Hun-Mo
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.4.210 Outcomes of dental implant treatment in patients with generalized aggressive periodontitis: a systematic review Kyoung-Kyu Kim*, DDS, MSD, Hun-Mo
BioHorizons Education Programme 2015
 BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
CAD/CAM technology supporting successful implant therapy
 CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
Survival Analysis of Dental Implants. Abstracts
 Survival Analysis of Dental Implants Andrew Kai-Ming Kwan 1,4, Dr. Fu Lee Wang 2, and Dr. Tak-Kun Chow 3 1 Census and Statistics Department, Hong Kong, China 2 Caritas Institute of Higher Education, Hong
Survival Analysis of Dental Implants Andrew Kai-Ming Kwan 1,4, Dr. Fu Lee Wang 2, and Dr. Tak-Kun Chow 3 1 Census and Statistics Department, Hong Kong, China 2 Caritas Institute of Higher Education, Hong
DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI
 Good Morning DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI What is implant? A dental implant is an artificial root that replaces the natural tooth root. Crown Gum Implant Tooth Root Jawbone Parts of implant Cover
Good Morning DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI What is implant? A dental implant is an artificial root that replaces the natural tooth root. Crown Gum Implant Tooth Root Jawbone Parts of implant Cover
While the prosthetic rehabilitation of
 Restoring Mandibular Single Teeth with the Inclusive Tooth Replacement Solution Go online for in-depth content by Bradley C. Bockhorst, DMD While the prosthetic rehabilitation of full-arch cases provides
Restoring Mandibular Single Teeth with the Inclusive Tooth Replacement Solution Go online for in-depth content by Bradley C. Bockhorst, DMD While the prosthetic rehabilitation of full-arch cases provides
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS
 RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION
 MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration
 Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration ROBERT SCHNEIDER, DDS, MS* ABSTRACT The prosthetic restoration of a
Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration ROBERT SCHNEIDER, DDS, MS* ABSTRACT The prosthetic restoration of a
