istent Trabecular Micro-Bypass Stent Reimbursement Guide
|
|
|
- Elvin Potter
- 10 years ago
- Views:
Transcription
1 istent Trabecular Micro-Bypass Stent Reimbursement Guide
2 Table of Contents Overview Coding 2 3 Coding Overview Procedure Coding Device Coding Additional Coding Information Coverage Payment 8 9 Payment Overview Medicare Payment Physicians Facilities Private Payer Payment Physicians Facilities Frequently Asked Questions 12 Appendix 14 2
3 Overview This guide provides coding and billing information to facilities and physicians submitting claims for procedures using the istent Trabecular Micro-Bypass Stent (the istent ). Approved Indication The istent Trabecular Micro-Bypass Stent Model GTS100R/L is indicated for use in conjunction with cataract surgery for the reduction of IOP in subjects with mild to moderate open-angle glaucoma currently treated with ocular hypotensive medication. Disclaimer This reimbursement information is intended to provide health care professionals with information related to billing, coding, and reimbursement requirements that may apply to Glaukos products. It is being provided for general informational and educational purposes only, and is not intended, and does not constitute, reimbursement or legal advice. Use of codes identified here does not guarantee coverage or payment at any specific level and is not intended to increase or maximize payment by any payer. Laws, regulations and coverage policies are complex and updated frequently. In addition, reimbursement policies vary widely from insurer to insurer and will reflect different patient conditions. You should check the current law and regulations and insurer's policies to confirm the most current coverage, coding or billing requirements. Any questions should be directed to your attorneys or reimbursement specialist. The health care professional is responsible for all aspects of reimbursement, including using codes that accurately reflect the patient's condition, procedures performed, and products used and ensuring the veracity of all claims submitted to third party payers. 3
4 Coding Coding Overview Medical billing codes convert a narrative description of a procedure, device, drug or disease into an alphanumeric or numeric code that health care providers use to report medical services rendered to patients to payers. When submitting claims to Medicare and other third party payers, facilities (e.g., hospitals and ASCs) and physicians list codes that describe patient condition and reflect procedures performed. The following sections of this guide will review some of the codes that may be appropriate for billing the istent and associated procedures. However, providers are ultimately responsible for choosing diagnosis and procedure codes that accurately describe the patient s condition, underlying disease and treatment. The key in all coding and billing to payers is to be truthful and not misleading and make full disclosures to the payer about how the product has been used and the procedures necessary to deploy and remove the product when seeking reimbursement for any product or procedure. A table providing an overview of the types of codes that will most commonly be used when billing for the istent and associated procedures is displayed below. Table 1: Reimbursement Code Overview CODE TYPES CPT codes Healthcare Common Procedure Coding System (HCPCS) ICD-9-CM diagnosis codes CODE DESCRIPTION Describes procedures performed and are used on claims submitted by physicians, Ambulatory Surgical Centers (ASC) and Hospital Outpatient Departments (HOPD) Describes items used in a patient s treatment, such as devices or drugs Describes patient condition or underlying disease Revenue codes Describes the location where a procedure was performed, and the type of item, if applicable Procedure Coding Category I CPT codes are 5-digit numeric, permanent codes used to describe established procedures or services. Category III CPT codes are temporary codes that describe emerging technologies or services. Category III CPT codes allow for data collection and tracking for these specific services/procedures and if available, Category III CPT codes must be reported instead of unlisted Category I CPT codes. Physicians and facilities need to establish a charge amount to be submitted with a Category III CPT code. Both Category I and Category III CPT codes are eligible for coverage and reimbursement by payers. 4
5 When Category III CPT codes are submitted on claims, they are often subject to manual review by payers to make a determination on medical necessity and therefore payment. Coverage and reimbursement is not guaranteed, and the use of such codes typically requires additional documentation to be submitted to payers in order to justify the medical necessity of the procedure performed. istent Procedure Coding (Physicians and Facilities) Table 2 below identifies the possible CPT code(s) that may be used to describe the istent implantation procedure. Category III CPT code 0191T became effective for use July 1, 2008 and describes the insertion of glaucoma drainage devices using an ab interno approach. Physicians and facilities are responsible for accurately selecting CPT procedure codes to describe the procedures performed. Table 2: Potential CPT Code(s) CPT CODE 0191T DESCRIPTION Insertion of anterior segment aqueous drainage device, without extraocular reservoir, internal approach, into the trabecular meshwork The use of Category III CPT codes may require the submission of additional documentation to payers for them to assess medical necessity and determine appropriate payment levels. Such documentation may include: A letter of medical necessity Product description, including FDA approval letter The patient s medical records A copy of the surgical/operative report with clear documentation of the procedure in question having been performed Clinical literature Cataract Procedure Coding (Physicians and Facilities) The istent device is indicated for use in conjunction with cataract surgery. Standard cataract surgery with implantation of an IOL is most commonly reported with CPT code 66984, although a number of other CPT codes may apply depending on the actual services performed. Table 3 identifies possible Category I CPT codes that may be used to describe the cataract surgery procedure(s) performed in conjunction with the istent insertion procedure. Table 3: Potential CPT Code(s) CPT CODE DESCRIPTION Intracapsular cataract extraction with insertion of intraocular lens prosthesis (1 stage procedure) Extracapsular cataract removal with insertion of intraocular lens prosthesis (1 stage procedure), manual or mechanical technique (eg, irrigation and aspiration or phacoemulsification) 5
6 Device Coding (Facilities Only) Level II HCPCS codes are five-digit alphanumeric codes that include a single letter followed by four numeric digits. They are used primarily to identify a variety of medical supplies, drugs and equipment. HCPCS codes are billed by facilities and should not be included on claims for physician services only. Table 4 below identifies the possible HCPCS code(s) that may be used by ASCs and HOPDs to report the istent device itself. Table 4: Potential HCPCS Code(s) HCPCS CODE L8699 DESCRIPTION Prosthetic implant, not otherwise specified Additional Coding Information Modifiers Depending on the actual procedure(s) performed with the istent, it may be necessary to append certain modifiers to the procedure codes indicated on claim forms. Modifiers are designed to provide payers with additional information that may be necessary in order to process claims. Modifiers are used to clarify the intent, duration, or scope of a procedure billed. Modifiers are two-digit alphanumeric codes that are appended to CPT codes when necessary to indicate that the procedure performed has been modified in some way from its original definition. Healthcare providers may consider the coding options listed in Table 5 below and select the appropriate modifiers based on the procedure(s) performed. Table 5: Potential Modifiers MODIFIER RT LT -51 DESCRIPTION Used to indicate that the procedure was performed on the right side of the body Used to indicate that the procedure was performed on the left side of the body Used to indicate multiple procedures were performed during the same surgical session Revenue Codes Revenue codes are three-digit numeric codes reported on a UB-04 facility claim form to describe general categories of services provided and items furnished to a patient in a facility setting. Facilities are required to report revenue codes to provide a description of the specific service or item related to each revenue code reported. Revenue codes are used for tracking purposes and are not reimbursable codes. Table 6 below identifies the possible revenue code(s) that may be used to report the istent device in the HOPD setting of care. Table 6: Potential Revenue Code(s) SETTING OF CARE DEVICE CODE DESCRIPTION Hospital Outpatient 278 Other implant 6
7 Diagnosis Codes The International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) diagnosis codes are reported on hospital and physician claims to report the patient s medical condition. Payers use this information to evaluate the episode of care and the appropriateness of the treatment the patient received. ICD-9-CM diagnosis codes are used in all settings of care. Table 7 includes ICD-9-CM diagnosis codes that describe conditions that may be reported on istent claim forms. Table 7: Potential ICD-9-CM Diagnosis Codes ICD-9-CM Code Description Open angle glaucoma, unspecified Primary open angle glaucoma Residual stage of open angle glaucoma Glaucoma associated with other lens disorders The ICD-9-CM diagnosis codes listed in this table may be commonly associated with istent patients but are not intended to be an exhaustive list of all possible diagnosis codes. Please refer to the ICD-9-CM book for a comprehensive list of diagnosis codes. Note that in all cases, it is ultimately the responsibility of the provider to report the ICD-9-CM diagnosis code that most accurately describes the patient s condition. 7
8 Coverage Use of the istent must meet the requirements established by Medicare and other third party payers to be a covered service. Payer coverage policies are available in either benefit policy manuals (Medicare) or insurance contracts (private payers) which identify the products and services eligible for payment. Health insurers generally provide coverage for services when they are medically reasonable and necessary for treatment or diagnosis of illness or injury. The istent represents the latest technology in treating glaucoma and, like other new technologies, is in the early stages of securing widespread coverage from payers. Currently most payers have not established coverage guidelines for the istent. Glaukos is currently working with payers to obtain specific guidance on the istent for its customers and will provide updates when new information becomes available. In the meantime, providers are strongly encouraged to contact their local Medicare carriers and other insurers to clarify coverage guidelines specific to their patients. In the absence of established coverage policies, payers will review claims and determine coverage on a case-by-case basis. Private payers may need to be contacted to obtain prior authorization prior to performing the procedure(s). Additionally, because Category III CPT codes are often used to identify emerging technology, insurers unfamiliar with the istent may request additional materials to support coverage when submitting claims. For information regarding payer coverage in your area, please consult with your Glaukos Regional Business Manager. 8
9 Payment Payment Overview Healthcare providers are provided payment by payers for the products and services they provide to patients during an episode of care. Two types of payments are generally made: a payment for facility resources and a payment for professional services. Facilities such as hospitals and ambulatory surgery centers are paid for the resources used in an episode of care. Physicians are paid for the services they provide in treating patients. Medicare Payment Physician Payment Medicare provides payment to physicians for services based on a fee schedule called the Medicare Physician Fee Schedule (MPFS). CMS assigns national payment rates on the MPFS for Category I CPT codes. As Category III CPT codes typically reflect new and emerging technologies, CMS does not establish national payment rates on the MPFS for these types of procedures. Payment for Category III CPT codes will be determined by individual Medicare contractors on a case-bycase basis. Physicians need to establish a charge amount to be submitted with these types of codes. Claims for professional services submitted under Category III CPT codes are often manually reviewed by payers. The payment methodology for a procedure submitted under a Category III CPT code varies. In some instances, Medicare will calculate payment based on the amount charged on the claim. In other cases, payment will be determined by comparing work involved with the istent to other similar procedures. To determine the payment amount for specific codes on the MPFS, visit the Medicare MPFS Lookup feature at this website: Facility Payment Medicare pays ASCs for services under a prospective payment system called the ASC Payment System. Under this payment system, Medicare assigns procedure codes, which may be performed in the ASC setting of care, to an ASC payment group. This payment group determines the amount that a facility will be paid by Medicare for services provided. To determine the payment amount for the istent procedure and associated cataract procedure in the ASC and to obtain additional information related to the ASC Payment System, visit the CMS website: Medicare pays hospitals for outpatient services under a prospective payment system Hospital Outpatient Prospective Payment System (HOPPS). HOPPS is a payment system that groups payment for drugs and services into ambulatory payment classifications (APCs). The HOPPS provides a fixed, bundled payment for hospital outpatient procedures or services that are assigned to a particular APC (See Table 8). The system determines only the hospital payment and does not affect payment to physicians who perform services in the hospital outpatient setting. To determine the payment amount for the istent procedure and associated cataract procedure in the HOPD and to obtain additional information related to HOPPS, visit the CMS website: 9
10 Table 8: APC assignment for CPT 0191T APC DESCRIPTION 0673 Level V Anterior Segment Eye Procedures While there is a HCPCS code that can be used to bill for the istent device itself, Medicare does not provide separate payment for the device. Under Medicare, payment for the istent and other implantable devices is bundled into the payment for the implantation procedure itself in the ASC and HOPD. It is still important that facilities include the istent device on their claim forms to payers as this permits appropriate tracking of the full costs of the procedure(s). Private Payer Payment Physician Payment Private payers typically establish their own payment rates for services and procedures and may provide this information on a publicly accessible fee schedule. As with Medicare, payment for Category III CPT codes will be determined by private payers on a case-bycase basis. Physicians need to establish a charge amount to be submitted with these types of codes. Claims for professional services submitted under Category III CPT codes are often manually reviewed by payers. The payment methodology for a procedure submitted under a Category III CPT code varies. In some instances, private payers will calculate payment based on the amount charged on the claim. In other cases, payment will be determined by comparing work involved with the istent to other similar procedures. Payment rates for specific CPT codes may be obtained from the payer s published physician fee schedule or by contacting the payer directly. Facility Payment Private payers each employ their own methodology to determine payment amounts for facility services based on the CPT, ICD-9 and HCPCS codes billed on the claim. Facility billing departments should check the service contracts with individual private payers or contact each payer directly to verify the applicable reimbursement methodologies and/or amounts for the istent implantation, the associated cataract procedure and for the istent device itself. As with Medicare, it is important that facilities include the istent device on their claim forms to payers in order to capture the full cost of providing the service. 10
11 Setting Charges Providers must determine a charge for Category III CPT codes. There are many variables that may account for the determination of a charge for a particular service. For example, the American Academy of Orthopedic Surgeons suggests that providers consider the following when establishing a charge to submit for a Category III CPT code: Time, effort, equipment, RVUs, and cost related to geographic variability of the procedure Referencing another CPT code of similar complexity to that of the procedure Comparing the preoperative, intraoperative, and postoperative services of the similar procedure to that of the new procedure Contrasting the factors that differentiate the services (more difficult or less difficult) and setting the charges accordingly 1 Additionally, the Practice Management Information Corporation 2 suggests that the following additional resources may also be helpful when determining appropriate charges. Payer policies Current coding books Relative value data for existing Category I CPT codes Medicare Fee Schedules for existing Category I CPT codes Whichever process the provider uses, it should be described in the supporting documentation that accompanies the claim. 1 LeGrand, Mary. Category III Code Updates. American Academy of Orthopedic Surgeons. (2008). 2 Practice Management Information Corporation. Medical Fees. Los Angeles, CA;
12 Frequently Asked Questions Q1. How can I tell whether a private payer will cover the istent implantation procedure? I can t tell from their coverage policies. A1. When it is unclear whether a private payer will cover the istent, the provider may choose to obtain prior authorization for the patient s istent implantation procedure. Q2. How can I tell whether Medicare will cover the istent implantation procedure? I can t tell from their local coverage determinations. A2. Because Medicare does not have a process to review prior authorization requests, a provider may be required to complete an ABN. Note that an ABN is required for both assigned and nonassigned claims and modifier GA should be appended to the appropriate CPT or HCPCS code. By signing an ABN, the Medicare beneficiary is acknowledging that he or she has been informed that Medicare might not pay for the services being rendered and agrees to be responsible for payment in the event that Medicare does not pay. For a copy of the ABN, please see the Appendix. In addition, please check with your Glaukos Regional Business Manager for the most current information regarding coverage of implantation of the istent by your local Medicare contractor. Q3. Can I bill for the implant of the istent (0191T) and cataract surgery (66983 or 66984) on the same day for the same patient? A3. The National Medicare Correct Coding Initiative (CCI) edits do not prohibit billing 0191T and or on the same day for the same patient. Q4: My patient is covered through our local Medicare Administrative Contractor (MAC), and I don t think they will cover the istent implantation procedure. What should I do? A4. If your local Medicare Administrative Contractor (MAC) is not yet routinely covering the implantation of the istent, you may consider having the patient sign an ABN. For a copy of the ABN, please see the Appendix. Q5. My claim for the istent procedure was denied. What should I do? A5. Since Category III CPT codes represent newer and lesser-known technologies, payers may request additional documentation showing medical necessity before paying a claim with a Category III CPT code. Providers are advised to pursue an appeal via the appeals process, which usually involves providing product information, clinical literature, and an explanation describing why the procedure was medically necessary for the patient. Contact the payer in question to get information on the appeals process and the materials they require to show medical necessity. To see whether you qualify for Glaukos assistance with your istent medical necessity appeal, contact your Glaukos Regional Business Manager. 12
13 Q6. How do I bill Medicare for the istent when used in the hospital outpatient setting of care? A6. Hospital outpatient facilities should use revenue code 278 on the UB-04 claim form to bill for the istent in this setting. Medicare reimbursement for hospital outpatient departments is based on the APC payment system. CPT code 0191T maps to APC Q7. What diagnosis codes are covered for use with the istent? I have a patient who I think would be a good candidate but I don t know whether his condition would result in on- or off-label use of the istent. A7. Providers should check with a patient s insurer to determine which indications are currently covered, and the appropriate course of action when submitting claims for non-covered indications. Q8. What procedure code should I use to report the implantation of the istent? A8. Providers should bill for the istent implantation procedure using the Category III CPT code 0191T. As payers typically flag claims with Category III CPT codes for manual review, you should be prepared to provide product information, clinical literature, and an explanation describing why the procedure was medically necessary for the patient. 13
14 Appendix Sample Physician Claim Form (CMS-1500) Sample ASC Claim Form (CMS-1500) Sample Hospital Claim Form (UB-04) CMS Advance Beneficiary Notice (ABN) Form 14
istent Trabecular Micro-Bypass Stent Reimbursement Guide
 istent Trabecular Micro-Bypass Stent Reimbursement Guide Table of Contents Overview Coding 3 4 Coding Overview Procedure Coding Device Coding Additional Coding Information Coverage Payment 10 11 Payment
istent Trabecular Micro-Bypass Stent Reimbursement Guide Table of Contents Overview Coding 3 4 Coding Overview Procedure Coding Device Coding Additional Coding Information Coverage Payment 10 11 Payment
CODING. Neighborhood Health Plan 1 Provider Payment Guidelines
 CODING Policy The terms of this policy set forth the guidelines for reporting the provision of care rendered by NHP participating providers, including but not limited to use of standard diagnosis and procedure
CODING Policy The terms of this policy set forth the guidelines for reporting the provision of care rendered by NHP participating providers, including but not limited to use of standard diagnosis and procedure
NOVOSTE BETA-CATH SYSTEM
 HOSPITAL INPATIENT AND OUTPATIENT BILLING GUIDE FOR THE NOVOSTE BETA-CATH SYSTEM INTRAVASCULAR BRACHYTHERAPY DEVICE This guide is intended solely for use as a tool to help hospital billing staff resolve
HOSPITAL INPATIENT AND OUTPATIENT BILLING GUIDE FOR THE NOVOSTE BETA-CATH SYSTEM INTRAVASCULAR BRACHYTHERAPY DEVICE This guide is intended solely for use as a tool to help hospital billing staff resolve
Advanced Monitoring Parameters 2015 Quick Guide to Hospital Coding, Coverage and Payment
 Advanced Monitoring Parameters 2015 Quick Guide to Hospital Coding, Coverage and Payment The information in this quick guide is provided by our Healthcare Economics Department, which supports Respiratory
Advanced Monitoring Parameters 2015 Quick Guide to Hospital Coding, Coverage and Payment The information in this quick guide is provided by our Healthcare Economics Department, which supports Respiratory
Rotator Cuff Repair Surgical Procedures
 Rotator Cuff Repair Surgical Procedures 2011 Reimbursement and Coding Reference Guide for Physicians and Hospitals This coding reference guide is intended to illustrate the common CPT * codes, ICD-9 CM
Rotator Cuff Repair Surgical Procedures 2011 Reimbursement and Coding Reference Guide for Physicians and Hospitals This coding reference guide is intended to illustrate the common CPT * codes, ICD-9 CM
Physician Fee Schedule BCBSRI follows CMS Physician Fee Schedule (PFS) Relative Value Units (RVU) for details relating to
 Policy Coding and Guidelines EFFECTIVE DATE: 09 01 2015 POLICY LAST UPDATED: 09 02 2015 OVERVIEW This Policy provides an overview of coding and guidelines as they pertain to claims submitted to Blue Cross
Policy Coding and Guidelines EFFECTIVE DATE: 09 01 2015 POLICY LAST UPDATED: 09 02 2015 OVERVIEW This Policy provides an overview of coding and guidelines as they pertain to claims submitted to Blue Cross
Zimmer Payer Coverage Approval Process Guide
 Zimmer Payer Coverage Approval Process Guide Market Access You ve Got Questions. We ve Got Answers. INSURANCE VERIFICATION PROCESS ELIGIBILITY AND BENEFITS VERIFICATION Understanding and verifying a patient
Zimmer Payer Coverage Approval Process Guide Market Access You ve Got Questions. We ve Got Answers. INSURANCE VERIFICATION PROCESS ELIGIBILITY AND BENEFITS VERIFICATION Understanding and verifying a patient
1) There are 0 indicator edits, which are never correctly reported together;
 Medical Coverage Policy Coding and Guidelines sad EFFECTIVE DATE: 11/15/2011 POLICY LAST UPDATED: 11/1/2013 OVERVIEW This Policy provides an overview of coding and guidelines as they pertain to claims
Medical Coverage Policy Coding and Guidelines sad EFFECTIVE DATE: 11/15/2011 POLICY LAST UPDATED: 11/1/2013 OVERVIEW This Policy provides an overview of coding and guidelines as they pertain to claims
Global Surgery Fact Sheet
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services R Global Surgery Fact Sheet Fact Sheet Definition of a Global Surgical Package Medicare established a national definition
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services R Global Surgery Fact Sheet Fact Sheet Definition of a Global Surgical Package Medicare established a national definition
Medicare Controversies in Cataract Coding One Consultant s Opinion. Riva Lee Asbell Philadelphia, PA
 Medicare Controversies in Cataract Coding One Consultant s Opinion INTRODUCTION Riva Lee Asbell Philadelphia, PA It would seem that coding for cataract surgery is a straightforward affair not so at all.
Medicare Controversies in Cataract Coding One Consultant s Opinion INTRODUCTION Riva Lee Asbell Philadelphia, PA It would seem that coding for cataract surgery is a straightforward affair not so at all.
Suppliers are to follow The Health Plan requirements for precertification, as applicable.
 Eye Prostheses Adopted from the National Government Services website. For any item to be covered by The Health Plan, it must: 1. Be eligible for a defined Medicare or Health Plan benefit category 2. Be
Eye Prostheses Adopted from the National Government Services website. For any item to be covered by The Health Plan, it must: 1. Be eligible for a defined Medicare or Health Plan benefit category 2. Be
Tips on Glaucoma Surgical Coding for Medicare. Riva Lee Asbell Philadelphia, PA
 Tips on Glaucoma Surgical Coding for Medicare Riva Lee Asbell Philadelphia, PA INTRODUCTION Glaucoma surgical coding is usually rather straightforward, but occasionally some problems occur. Although the
Tips on Glaucoma Surgical Coding for Medicare Riva Lee Asbell Philadelphia, PA INTRODUCTION Glaucoma surgical coding is usually rather straightforward, but occasionally some problems occur. Although the
Medico-Legal Considerations and Coding and Billing of Laser Procedures. Marcus G. Piccolo, OD
 Medico-Legal Considerations and Coding and Billing of Laser Procedures Marcus G. Piccolo, OD Invasive Patient Procedures First Do No Harm Informed Consent Part of any medical procedure no matter how minor
Medico-Legal Considerations and Coding and Billing of Laser Procedures Marcus G. Piccolo, OD Invasive Patient Procedures First Do No Harm Informed Consent Part of any medical procedure no matter how minor
Reimbursement Guide 2011
 Reimbursement Guide 2011 IMPORTANT SAFETY INFORMATION HYALGAN is indicated for the treatment of pain in osteoarthritis (OA) of the knee in patients who have failed to respond adequately to conservative
Reimbursement Guide 2011 IMPORTANT SAFETY INFORMATION HYALGAN is indicated for the treatment of pain in osteoarthritis (OA) of the knee in patients who have failed to respond adequately to conservative
Contractor Number 11302. Oversight Region Region IV
 Local Coverage Determination (LCD): Spinal Cord Stimulators for Chronic Pain (L32549) Contractor Information Contractor Name Palmetto GBA opens in new window Contractor Number 11302 Contractor Type MAC
Local Coverage Determination (LCD): Spinal Cord Stimulators for Chronic Pain (L32549) Contractor Information Contractor Name Palmetto GBA opens in new window Contractor Number 11302 Contractor Type MAC
COM Compliance Policy No. 3
 COM Compliance Policy No. 3 THE UNIVERSITY OF ILLINOIS AT CHICAGO NO.: 3 UIC College of Medicine DATE: 8/5/10 Chicago, Illinois PAGE: 1of 7 UNIVERSITY OF ILLINOIS COLLEGE OF MEDICINE CODING AND DOCUMENTATION
COM Compliance Policy No. 3 THE UNIVERSITY OF ILLINOIS AT CHICAGO NO.: 3 UIC College of Medicine DATE: 8/5/10 Chicago, Illinois PAGE: 1of 7 UNIVERSITY OF ILLINOIS COLLEGE OF MEDICINE CODING AND DOCUMENTATION
WELLCARE CLAIM PAYMENT POLICIES
 WellCare and Harmony Health Plan s claim payment policies are based on publicly distributed guidelines from established industry sources such as the Centers for Medicare and Medicaid Services (CMS), the
WellCare and Harmony Health Plan s claim payment policies are based on publicly distributed guidelines from established industry sources such as the Centers for Medicare and Medicaid Services (CMS), the
eskbook Emerging Life Sciences Companies second edition Chapter 18 Medicare Reimbursement for Drugs and Devices
 eskbook Emerging Life Sciences Companies second edition Chapter 18 Medicare Reimbursement for Drugs and Devices Chapter 18 MEDICARE REIMBURSEMENT FOR DRUGS AND DEVICES Coverage Coding There is no reimbursement
eskbook Emerging Life Sciences Companies second edition Chapter 18 Medicare Reimbursement for Drugs and Devices Chapter 18 MEDICARE REIMBURSEMENT FOR DRUGS AND DEVICES Coverage Coding There is no reimbursement
2006 Provider Coding/Billing Information. www.novoseven-us.com
 2006 Provider Coding/Billing Information 2 3 Contents About NovoSeven...2 Coverage...4 Coding...4 Reimbursement...8 Establishing Medical Necessity and Appealing Denied Claims...10 Claims Materials...12
2006 Provider Coding/Billing Information 2 3 Contents About NovoSeven...2 Coverage...4 Coding...4 Reimbursement...8 Establishing Medical Necessity and Appealing Denied Claims...10 Claims Materials...12
Highlights of the Florida Medicaid Ambulatory Surgical Center Services Coverage and Limitations Handbook
 Highlights of the Florida Medicaid Ambulatory Surgical Center Services Coverage and Limitations Handbook Agency for Health Care Administration July 2013 1 Learning Objectives Provide an overview of the
Highlights of the Florida Medicaid Ambulatory Surgical Center Services Coverage and Limitations Handbook Agency for Health Care Administration July 2013 1 Learning Objectives Provide an overview of the
Medicare 101: Basics of CPT. Part B Provider Outreach and Education February 11, 2015
 Medicare 101: Basics of CPT Part B Provider Outreach and Education February 11, 2015 Housekeeping Tips When you called in, did you enter your attendee code? Dial-in number: 1-800-791-2345 Attendee (participant)
Medicare 101: Basics of CPT Part B Provider Outreach and Education February 11, 2015 Housekeeping Tips When you called in, did you enter your attendee code? Dial-in number: 1-800-791-2345 Attendee (participant)
ICD-9 CM. ICD-9 9 CM stands for International Classification of Diseases, 9 th revision, clinical modifications
 Ophthalmology Coding ICD-9 9 CM & CPT By Alice Landry, Registered Health Information Administrator and Certified Procedural Coder Harvey & Bernice Jones Eye Institute University of Arkansas for Medical
Ophthalmology Coding ICD-9 9 CM & CPT By Alice Landry, Registered Health Information Administrator and Certified Procedural Coder Harvey & Bernice Jones Eye Institute University of Arkansas for Medical
Biodesign ADVANCED TISSUE REPAIR
 Biodesign ADVANCED TISSUE REPAIR 2013 CODING AND REIMBURSEMENT GUIDE FOR RECTOVAGINAL FISTULA The information provided herein reflects Cook Medical's understanding of the procedure(s) and/or devices(s)
Biodesign ADVANCED TISSUE REPAIR 2013 CODING AND REIMBURSEMENT GUIDE FOR RECTOVAGINAL FISTULA The information provided herein reflects Cook Medical's understanding of the procedure(s) and/or devices(s)
Intra-operative Nerve Monitoring Coding Guide. March 1, 2011
 Intra-operative Nerve Monitoring Coding Guide March 1, 2011 Please direct any questions to: Patty Telgener, RN Vice President, Reimbursement Services Emerson Consultants (303) 526-7604 (office) (303) 570-2159
Intra-operative Nerve Monitoring Coding Guide March 1, 2011 Please direct any questions to: Patty Telgener, RN Vice President, Reimbursement Services Emerson Consultants (303) 526-7604 (office) (303) 570-2159
Financial Disclosure. Modifiers Getting It Right! Modifiers. Modifiers. Medicare Expected Frequency. Common Modifiers Used Only with Office Visits
 Financial Disclosure Modifiers Getting It Right! Donna McCune is a consultant for Corcoran Consulting Group and acknowledges a financial interest in the subject matter of this presentation. Donna McCune,
Financial Disclosure Modifiers Getting It Right! Donna McCune is a consultant for Corcoran Consulting Group and acknowledges a financial interest in the subject matter of this presentation. Donna McCune,
Medical Necessity: Can You Please Define That? Part I. Riva Lee Asbell Philadelphia, PA
 Medical Necessity: Can You Please Define That? Part I Riva Lee Asbell Philadelphia, PA INTRODUCTION One of Medicare=s most elusive concepts is the term Amedical necessity@. Yet, lack thereof is the reason
Medical Necessity: Can You Please Define That? Part I Riva Lee Asbell Philadelphia, PA INTRODUCTION One of Medicare=s most elusive concepts is the term Amedical necessity@. Yet, lack thereof is the reason
Status Active. Assistant Surgeons. This policy addresses reimbursement for assistant surgical procedures during the same operative session.
 Status Active Reimbursement Policy Section: Surgery/Interventional Procedure Policy Number: RP - Surgery/Interventional Procedure - 001 Assistant Surgeons Effective Date: June 1, 2015 Assistant Surgeons
Status Active Reimbursement Policy Section: Surgery/Interventional Procedure Policy Number: RP - Surgery/Interventional Procedure - 001 Assistant Surgeons Effective Date: June 1, 2015 Assistant Surgeons
Unlisted Procedure Codes Frequently Asked Questions
 Unlisted Procedure Codes Frequently Asked Questions Use of an unlisted code is common when a physician performs a new procedure or utilizes new technology when no other CPT code adequately describes the
Unlisted Procedure Codes Frequently Asked Questions Use of an unlisted code is common when a physician performs a new procedure or utilizes new technology when no other CPT code adequately describes the
APR,:2 0 2009. Charlene Frizzera Acting Administrator Centers for Medicare & Medicaid Services. FROM: Daniel R. Levinson ~,u,l, ~.~ Inspector General
 DEPARTMENT OF HEALTH &. HUMAN SERVICES Office of Inspector General Washington, D.C. 20201 APR,:2 0 2009 TO: Charlene Frizzera Acting Administrator Centers for Medicare & Medicaid Services FROM: Daniel
DEPARTMENT OF HEALTH &. HUMAN SERVICES Office of Inspector General Washington, D.C. 20201 APR,:2 0 2009 TO: Charlene Frizzera Acting Administrator Centers for Medicare & Medicaid Services FROM: Daniel
100.1 - Payment for Physician Services in Teaching Settings Under the MPFS. 100.1.1 - Evaluation and Management (E/M) Services
 MEDICARE CLAIMS PROCESSING MANUAL Accessed September 25, 2005 100.1 - Payment for Physician Services in Teaching Settings Under the MPFS Payment is made for physician services furnished in teaching settings
MEDICARE CLAIMS PROCESSING MANUAL Accessed September 25, 2005 100.1 - Payment for Physician Services in Teaching Settings Under the MPFS Payment is made for physician services furnished in teaching settings
Article from: Health Section News. October 2002 Issue No. 44
 Article from: Health Section News October 2002 Issue No. 44 Outpatient Facility Reimbursement by Brian G. Small Outpatient Charge Levels Today s outpatient care can be every bit as intense and expensive
Article from: Health Section News October 2002 Issue No. 44 Outpatient Facility Reimbursement by Brian G. Small Outpatient Charge Levels Today s outpatient care can be every bit as intense and expensive
5/2/2014. Beginning Biller / Coder 101 Thursday, May 8 1:00 p.m. to 2:30 p.m. Disclaimer. Stay in touch through Facebook Please note
 Disclaimer Beginning Biller / Coder 101 Thursday, May 8 1:00 p.m. to 2:30 p.m. Presented by: Judy B Breuker, CPC, CPMA, CCS P, CDIP, CHC, CHCA, CEMC, AHIMA Approved ICD 10 CM/PCS Trainer The class is intended
Disclaimer Beginning Biller / Coder 101 Thursday, May 8 1:00 p.m. to 2:30 p.m. Presented by: Judy B Breuker, CPC, CPMA, CCS P, CDIP, CHC, CHCA, CEMC, AHIMA Approved ICD 10 CM/PCS Trainer The class is intended
Local Coverage Article: Venipuncture Necessitating Physician s Skill for Specimen Collection Supplemental Instructions Article (A50852)
 Local Coverage Article: Venipuncture Necessitating Physician s Skill for Specimen Collection Supplemental Instructions Article (A50852) Contractor Information Contractor Name CGS Administrators, LLC Article
Local Coverage Article: Venipuncture Necessitating Physician s Skill for Specimen Collection Supplemental Instructions Article (A50852) Contractor Information Contractor Name CGS Administrators, LLC Article
Class Action Settlement Recap
 Class Action Settlement Recap Enhancements to Claim Payment Policy, Processing and Payment Disclosure, and an Appeals Process for Class Action Settlement Providers The following enhancements are effective
Class Action Settlement Recap Enhancements to Claim Payment Policy, Processing and Payment Disclosure, and an Appeals Process for Class Action Settlement Providers The following enhancements are effective
FAQs on Billing for Health and Behavior Services
 FAQs on Billing for Health and Behavior Services by Government Relations Staff January 29, 2009 Practicing psychologists are eligible to bill for applicable services and receive reimbursement from Medicare
FAQs on Billing for Health and Behavior Services by Government Relations Staff January 29, 2009 Practicing psychologists are eligible to bill for applicable services and receive reimbursement from Medicare
Common Billing Mistakes Costing Your ASC Money and Correct Modifier & Revenue Code Usage for ASC Claims
 Common Billing Mistakes Costing Your ASC Money and Correct Modifier & Revenue Code Usage for ASC Claims October 2013 Beckers 20 th Annual ASC Conference Presenter: Stephanie Ellis, R.N., CPC, Speaker Ellis
Common Billing Mistakes Costing Your ASC Money and Correct Modifier & Revenue Code Usage for ASC Claims October 2013 Beckers 20 th Annual ASC Conference Presenter: Stephanie Ellis, R.N., CPC, Speaker Ellis
Medicare Physician Fee Schedule Modifiers
 Basics of MPFS Part 3 Medicare Physician Fee Schedule Modifiers Presented by Part B Provider Outreach and Education July 16, 2013 Disclaimer This information released is the property of Cahaba GBA and
Basics of MPFS Part 3 Medicare Physician Fee Schedule Modifiers Presented by Part B Provider Outreach and Education July 16, 2013 Disclaimer This information released is the property of Cahaba GBA and
Payment Policy. Evaluation and Management
 Purpose Payment Policy Evaluation and Management The purpose of this payment policy is to define how Health New England (HNE) reimburses for Evaluation and Management Services. Applicable Plans Definitions
Purpose Payment Policy Evaluation and Management The purpose of this payment policy is to define how Health New England (HNE) reimburses for Evaluation and Management Services. Applicable Plans Definitions
Medicare 101: Basics of Modifier Billing. Part B Provider Outreach and Education February 26, 2014
 Medicare 101: Basics of Modifier Billing Part B Provider Outreach and Education February 26, 2014 Housekeeping Tips When you called in, did you enter your attendee code? Dial-in number: 1-800-791-2345
Medicare 101: Basics of Modifier Billing Part B Provider Outreach and Education February 26, 2014 Housekeeping Tips When you called in, did you enter your attendee code? Dial-in number: 1-800-791-2345
SECTION 4. A. Balance Billing Policies. B. Claim Form
 SECTION 4 Participating Physicians, hospitals and ancillary providers shall be entitled to payment for covered services that are provided to a DMC Care member. Payment is made at the established and prevailing
SECTION 4 Participating Physicians, hospitals and ancillary providers shall be entitled to payment for covered services that are provided to a DMC Care member. Payment is made at the established and prevailing
Glossary of Insurance and Medical Billing Terms
 A Accept Assignment Provider has agreed to accept the insurance company allowed amount as full payment for the covered services. Adjudication The final determination of the issues involving settlement
A Accept Assignment Provider has agreed to accept the insurance company allowed amount as full payment for the covered services. Adjudication The final determination of the issues involving settlement
1500 Claims Processing Manual DHMP Health Insurance Claim Form CMS-1500
 DENVER HEALTH MEDICAL PLAN, INC. 1500 Claims Processing Manual DHMP Health Insurance Claim Form CMS-1500 Box 1 Medicare, Medicaid, Group Health Plan or other insurance Information Show the type of health
DENVER HEALTH MEDICAL PLAN, INC. 1500 Claims Processing Manual DHMP Health Insurance Claim Form CMS-1500 Box 1 Medicare, Medicaid, Group Health Plan or other insurance Information Show the type of health
Note: This article was updated on June 5, 2013, to reflect current Web addresses. All other information remains unchanged.
 MLN Matters Number: MM3816 Related Change Request (CR) #: 3816 Related CR Release Date: June 7, 2005 Effective Date: April 1, 2006 Related CR Transmittal #: R25DEMO Implementation Date: April 3, 2006 Note:
MLN Matters Number: MM3816 Related Change Request (CR) #: 3816 Related CR Release Date: June 7, 2005 Effective Date: April 1, 2006 Related CR Transmittal #: R25DEMO Implementation Date: April 3, 2006 Note:
Compensation and Claims Processing
 Compensation and Claims Processing Compensation The network rate for eligible outpatient visits is reimbursed to you at the lesser of (1) your customary charge, less any applicable co-payments, coinsurance
Compensation and Claims Processing Compensation The network rate for eligible outpatient visits is reimbursed to you at the lesser of (1) your customary charge, less any applicable co-payments, coinsurance
National Coverage Determination. Vagus Nerve Stimulation (VNS)
 National Coverage Determination Vagus Nerve Stimulation (VNS) Number NEURO-004 Contractor Name Wisconsin Physicians Service Insurance Corporation AMA CPT Copyright Statement CPT codes, descriptions and
National Coverage Determination Vagus Nerve Stimulation (VNS) Number NEURO-004 Contractor Name Wisconsin Physicians Service Insurance Corporation AMA CPT Copyright Statement CPT codes, descriptions and
Page 1 of 11. MLN Matters Number: SE1010 REVISED Related Change Request (CR) #: 6740. Related CR Release Date: N/A Effective Date: January 1, 2010
 News Flash Version 3.0 of the Measures Groups Specifications Manual released in November 2009 for 2010 PQRI has been revised. Version 3.1 of the 2010 PQRI Measures Groups Specifications Manual and Release
News Flash Version 3.0 of the Measures Groups Specifications Manual released in November 2009 for 2010 PQRI has been revised. Version 3.1 of the 2010 PQRI Measures Groups Specifications Manual and Release
How to Overcome the 5 Biggest Reimbursement Challenges in Joint & Spine Coding
 How to Overcome the 5 Biggest Reimbursement Challenges in Joint & Spine Coding Presented by: Carolyn Neumann, CPC Senior Manager Coding and Coverage Access The opinions and codes denoted within are suggestions
How to Overcome the 5 Biggest Reimbursement Challenges in Joint & Spine Coding Presented by: Carolyn Neumann, CPC Senior Manager Coding and Coverage Access The opinions and codes denoted within are suggestions
Modifiers 58, 78, and 79 Staged, Related, and Unrelated Procedures
 Manual: Policy Title: Reimbursement Policy Modifiers 58, 78, and 79 Staged, Related, and Unrelated Procedures Section: Modifiers Subsection: None Date of Origin: 9/22/2004 Policy Number: RPM010 Last Updated:
Manual: Policy Title: Reimbursement Policy Modifiers 58, 78, and 79 Staged, Related, and Unrelated Procedures Section: Modifiers Subsection: None Date of Origin: 9/22/2004 Policy Number: RPM010 Last Updated:
Ambulatory Surgery Center Coding and Payment Guide 2015
 Targeted Drug Delivery Ambulatory Surgery Center Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party
Targeted Drug Delivery Ambulatory Surgery Center Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party
New Outpatient Therapy Evaluation and Intervention E&I Codes. An introduction to the new policy and new claims coding requirements
 New Outpatient Therapy Evaluation and Intervention E&I Codes An introduction to the new policy and new claims coding requirements Disclaimer Contents of this presentation are for educational purposes only.
New Outpatient Therapy Evaluation and Intervention E&I Codes An introduction to the new policy and new claims coding requirements Disclaimer Contents of this presentation are for educational purposes only.
Initial Preventive Physical Examination
 Initial Preventive Physical Examination Overview The Medicare Prescription Drug, Improvement, and Modernization Act (MMA) of 2003 expanded Medicare's coverage of preventive services. Central to the Centers
Initial Preventive Physical Examination Overview The Medicare Prescription Drug, Improvement, and Modernization Act (MMA) of 2003 expanded Medicare's coverage of preventive services. Central to the Centers
A. CPT Coding System B. CPT Categories, Subcategories, and Headings
 OST 148 MEDICAL CODING, BILLING AND INSURANCE COURSE DESCRIPTION: Prerequisites: None Corequisites: None This course introduces CPT and ICD coding as they apply to medical insurance and billing. Emphasis
OST 148 MEDICAL CODING, BILLING AND INSURANCE COURSE DESCRIPTION: Prerequisites: None Corequisites: None This course introduces CPT and ICD coding as they apply to medical insurance and billing. Emphasis
Coding and Payment Guide for Anesthesia Services. An essential coding, billing, and reimbursement resource for anesthesiology and pain management
 Coding and Payment Guide for Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2011 Contents Introduction...1 Coding Systems... 1 Claim
Coding and Payment Guide for Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2011 Contents Introduction...1 Coding Systems... 1 Claim
2013 MPFS Indicator Descriptors
 2013 MPFS Indicator Descriptors Here is an overview of the layout. Use the key on the following pages to interpret indicators. Indicator NOTE - # NOTE - C PROCEDURE/MOD PAR Amount NON-PAR Amount Limiting
2013 MPFS Indicator Descriptors Here is an overview of the layout. Use the key on the following pages to interpret indicators. Indicator NOTE - # NOTE - C PROCEDURE/MOD PAR Amount NON-PAR Amount Limiting
Reporting Audiology Quality Measures: A Step-by-Step Guide
 What is PQRS? The Physician Quality Reporting System (PQRS) is a program through the Centers for Medicare and Medicaid Services (CMS) designed to improve the quality of care to Medicare beneficiaries by
What is PQRS? The Physician Quality Reporting System (PQRS) is a program through the Centers for Medicare and Medicaid Services (CMS) designed to improve the quality of care to Medicare beneficiaries by
Revenue Cycle Responsibilities. Revenue Cycle. Objectives 4/9/2013
 Revenue Cycle Kathryn DeVault, RHIA, CCS, CCS-P AHIMA 2013 Objectives Identify responsibilities within the Revenue Cycle Focus on management of the revenue cycle process Discuss the revenue cycle process
Revenue Cycle Kathryn DeVault, RHIA, CCS, CCS-P AHIMA 2013 Objectives Identify responsibilities within the Revenue Cycle Focus on management of the revenue cycle process Discuss the revenue cycle process
Treatment Facilities Amended Date: October 1, 2015. Table of Contents
 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements... 1 2.1 Provisions... 1 2.1.1 General... 1 2.1.2 Specific... 1 2.2 Special
Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements... 1 2.1 Provisions... 1 2.1.1 General... 1 2.1.2 Specific... 1 2.2 Special
Injection, Tendon Sheath, Ligament, Ganglion Cyst, Carpal and Tarsal Tunnel Supplemental Instructions Article (A47720) Contractor Information
 Page 1 of 9 Deborah Rondeau From: Saved by Windows Internet Explorer 7 Sent: Saturday, August 23, 2008 7:42 PM Subject: FUTURE ARTICLE : Injection, Tendon Sheath, Ligament, Ganglion Cyst, Carpal and Tarsal
Page 1 of 9 Deborah Rondeau From: Saved by Windows Internet Explorer 7 Sent: Saturday, August 23, 2008 7:42 PM Subject: FUTURE ARTICLE : Injection, Tendon Sheath, Ligament, Ganglion Cyst, Carpal and Tarsal
Compensation and Claims Processing
 Compensation and Claims Processing Compensation The network rate for eligible outpatient visits is reimbursed to you at the lesser of (1) your customary charge, less any applicable co-payments, coinsurance
Compensation and Claims Processing Compensation The network rate for eligible outpatient visits is reimbursed to you at the lesser of (1) your customary charge, less any applicable co-payments, coinsurance
Title 40. Labor and Employment. Part 1. Workers' Compensation Administration
 Title 40 Labor and Employment Part 1. Workers' Compensation Administration Chapter 3. Electronic Billing 301. Purpose The purpose of this Rule is to provide a legal framework for electronic billing, processing,
Title 40 Labor and Employment Part 1. Workers' Compensation Administration Chapter 3. Electronic Billing 301. Purpose The purpose of this Rule is to provide a legal framework for electronic billing, processing,
Preventive Medicine and Screening Policy
 REIMBURSEMENT POLICY Policy Number 2015R0013C Preventive Medicine and Screening Policy Annual Approval Date 3/11/2015 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
REIMBURSEMENT POLICY Policy Number 2015R0013C Preventive Medicine and Screening Policy Annual Approval Date 3/11/2015 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
KYPHON. Reimbursement Guide. Physician Reimbursement. Balloon Kyphoplasty Procedure. ICD-9-CM Diagnosis Codes. CPT Codes and Payment
 KYPHON Balloon Kyphoplasty Procedure Reimbursement Guide ICD-9-CM Diagnosis Codes Providers should report the ICD-9-CM diagnosis code that most accurately describes the patient s condition. Please refer
KYPHON Balloon Kyphoplasty Procedure Reimbursement Guide ICD-9-CM Diagnosis Codes Providers should report the ICD-9-CM diagnosis code that most accurately describes the patient s condition. Please refer
Reporting of Devices and Leads When a Credit is Received
 Reporting of Devices and Leads When a Credit is Received Cardiac Rhythm Management and Electrophysiology Updated January 2014 Medicare Reporting Requirements For Full or Partial Credits of Devices and
Reporting of Devices and Leads When a Credit is Received Cardiac Rhythm Management and Electrophysiology Updated January 2014 Medicare Reporting Requirements For Full or Partial Credits of Devices and
How To Write A Procedure Code
 Manual: Policy Title: Reimbursement Policy Technical Component (TC), Professional Component (PC/26), and Global Service Billing Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number:
Manual: Policy Title: Reimbursement Policy Technical Component (TC), Professional Component (PC/26), and Global Service Billing Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number:
ICD-10 Preparation for Dental Providers. July 2014
 ICD-10 Preparation for Dental Providers July 2014 What is ICD-10? The International Classification of Diseases (ICD) is a set of codes used worldwide to classify medical diagnoses and inpatient procedures.
ICD-10 Preparation for Dental Providers July 2014 What is ICD-10? The International Classification of Diseases (ICD) is a set of codes used worldwide to classify medical diagnoses and inpatient procedures.
Status Active. Reimbursement Policy Section: Anesthesia Services Policy Number: RP - Anesthesia - 001 Anesthesia Effective Date: June 1, 2015
 Status Active Reimbursement Policy Section: Anesthesia Services Policy Number: RP - Anesthesia - 001 Anesthesia Effective Date: June 1, 2015 Anesthesia Policy Description: Definitions: This policy addresses
Status Active Reimbursement Policy Section: Anesthesia Services Policy Number: RP - Anesthesia - 001 Anesthesia Effective Date: June 1, 2015 Anesthesia Policy Description: Definitions: This policy addresses
Pennsylvania Workers Compensation Billing Tutorial. Step 1: Find the Charge Classes by Zip Code
 Step 1: Find the Charge Classes by Zip Code http://www.portal.state.pa.us/portal/server.pt/community/charge_classes_by_zip_co de/10428 The Pennsylvania Workers' Compensation Fee Schedule for Part B providers
Step 1: Find the Charge Classes by Zip Code http://www.portal.state.pa.us/portal/server.pt/community/charge_classes_by_zip_co de/10428 The Pennsylvania Workers' Compensation Fee Schedule for Part B providers
HOW TO PREVENT AND MANAGE MEDICAL CLAIM DENIALS TO INCREASE REVENUE
 Billing & Reimbursement Revenue Cycle Management HOW TO PREVENT AND MANAGE MEDICAL CLAIM DENIALS TO INCREASE REVENUE Billing and Reimbursement for Physician Offices, Ambulatory Surgery Centers and Hospitals
Billing & Reimbursement Revenue Cycle Management HOW TO PREVENT AND MANAGE MEDICAL CLAIM DENIALS TO INCREASE REVENUE Billing and Reimbursement for Physician Offices, Ambulatory Surgery Centers and Hospitals
ifuse Implant System Patient Appeal Guide
 ifuse Implant System Patient Appeal Guide Table of Contents PURPOSE OF THIS BOOKLET...................................................... 2 GUIDE TO THE APPEALS PROCESS..................................................
ifuse Implant System Patient Appeal Guide Table of Contents PURPOSE OF THIS BOOKLET...................................................... 2 GUIDE TO THE APPEALS PROCESS..................................................
ICD-10 FAQ. How Long Has ICD-9-CM Been In Use?
 ICD-10 FAQ How Long Has ICD-9-CM Been In Use? What Code Set Does ICD-9-CM Define? What Code Set Does ICD-10 Define? When was ICD-10-CM Created? What agency maintains ICD-10? Why is ICD-10 better than ICD-9?
ICD-10 FAQ How Long Has ICD-9-CM Been In Use? What Code Set Does ICD-9-CM Define? What Code Set Does ICD-10 Define? When was ICD-10-CM Created? What agency maintains ICD-10? Why is ICD-10 better than ICD-9?
Question and Answer Submissions
 AACE Endocrine Coding Webinar Welcome to the Brave New World: Billing for Endocrine E & M Services in 2010 Question and Answer Submissions Q: If a patient returns after a year or so and takes excessive
AACE Endocrine Coding Webinar Welcome to the Brave New World: Billing for Endocrine E & M Services in 2010 Question and Answer Submissions Q: If a patient returns after a year or so and takes excessive
FREQUENTLY ASKED QUESTIONS
 FREQUENTLY ASKED QUESTIONS The American Academy of Dental Sleep Medicine provides support for its members in matters relating to insurance reimbursement for oral appliance therapy. The following section
FREQUENTLY ASKED QUESTIONS The American Academy of Dental Sleep Medicine provides support for its members in matters relating to insurance reimbursement for oral appliance therapy. The following section
CLAIM FORM REQUIREMENTS
 CLAIM FORM REQUIREMENTS When billing for services, please pay attention to the following points: Submit claims on a current CMS 1500 or UB04 form. Please include the following information: 1. Patient s
CLAIM FORM REQUIREMENTS When billing for services, please pay attention to the following points: Submit claims on a current CMS 1500 or UB04 form. Please include the following information: 1. Patient s
Medical Compliance with Billing and Coding 2013: Will your Records Survive an Audit from a Third Party Payer or the OIG?
 Medical Compliance with Billing and Coding 2013: Will your Records Survive an Audit from a Third Party Payer or the OIG? Michael J. McGovern, OD, FAAO; Richard Soden, OD, FAAO American Academy of Optometry
Medical Compliance with Billing and Coding 2013: Will your Records Survive an Audit from a Third Party Payer or the OIG? Michael J. McGovern, OD, FAAO; Richard Soden, OD, FAAO American Academy of Optometry
ANNUAL NOTICE TO PHYSICIANS
 NOVEMBER 2014 ANNUAL NOTICE TO PHYSICIANS Dear Physician Colleague: Genoptix Medical Laboratory is committed to complying with all applicable laws and regulations governing the health care industry. We
NOVEMBER 2014 ANNUAL NOTICE TO PHYSICIANS Dear Physician Colleague: Genoptix Medical Laboratory is committed to complying with all applicable laws and regulations governing the health care industry. We
REIMBURSEMENT GUIDE. 2015 Pacira Pharmaceuticals, Inc. Parsippany, NJ 07054 03/15
 REIMBURSEMENT GUIDE This Reimbursement Guide guide is made available by Pacira Pharmaceuticals, Inc. ( Pacira ) for educational purposes only. You should note that rules concerning International Classification
REIMBURSEMENT GUIDE This Reimbursement Guide guide is made available by Pacira Pharmaceuticals, Inc. ( Pacira ) for educational purposes only. You should note that rules concerning International Classification
Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures
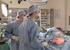 Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures Table 1: Surgeon Billing for Laparoscopic Adjustable Gastric Band Procedures 2012 Medicare Payment 2 43770
Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures Table 1: Surgeon Billing for Laparoscopic Adjustable Gastric Band Procedures 2012 Medicare Payment 2 43770
CODE AUDITING RULES. SAMPLE Medical Policy Rationale
 CODE AUDITING RULES As part of Coventry Health Care of Missouri, Inc s commitment to improve business processes, we are implemented a new payment policy program that applies to claims processed on August
CODE AUDITING RULES As part of Coventry Health Care of Missouri, Inc s commitment to improve business processes, we are implemented a new payment policy program that applies to claims processed on August
Medical Necessity and Coding
 Medical Necessity and Coding NEW MEXICO HEALTH INFORMATION MANAGEMENT ASSOCIATION FALL CODING WORKSHOP September 14, 2012 Hyatt Downtown Albuquerque, NM Presented by: Andrea Busby, RHIA ADHIMA, INC Goals
Medical Necessity and Coding NEW MEXICO HEALTH INFORMATION MANAGEMENT ASSOCIATION FALL CODING WORKSHOP September 14, 2012 Hyatt Downtown Albuquerque, NM Presented by: Andrea Busby, RHIA ADHIMA, INC Goals
How To Transition From Icd 9 To Icd 10
 ICD-10 FAQs for Doctors What is ICD-10? ICD-10 is the 10 th revision of the International Classification of Diseases (ICD), used by health care systems to report diagnoses and procedures for purposes of
ICD-10 FAQs for Doctors What is ICD-10? ICD-10 is the 10 th revision of the International Classification of Diseases (ICD), used by health care systems to report diagnoses and procedures for purposes of
Oregon CO-OP Modifier Table - December 2013
 Oregon CO-OP Modifier Table - December 2013 Modifier Modifier Description Pricing Functionality 22 Increased Procedural Services Modifier 22 should only be reported with procedure codes that have a global
Oregon CO-OP Modifier Table - December 2013 Modifier Modifier Description Pricing Functionality 22 Increased Procedural Services Modifier 22 should only be reported with procedure codes that have a global
Screening, Brief Intervention and Referral to Treatment SBIRT Coding, Billing and Reimbursement Manual
 Screening, Brief Intervention and Referral to Treatment SBIRT Coding, Billing and Reimbursement Manual Prepared For: Wisconsin Initiative to Promote Healthy Lifestyles (WIPHL) January 2010 Table of Contents
Screening, Brief Intervention and Referral to Treatment SBIRT Coding, Billing and Reimbursement Manual Prepared For: Wisconsin Initiative to Promote Healthy Lifestyles (WIPHL) January 2010 Table of Contents
Best ASC Billing Practices & Potential Issues
 Best ASC Billing Practices & Potential Issues Speaker: Stephanie Ellis, R.N., CPC Ellis Medical Consulting, Inc. [email protected] www.ellismedical.com (615) 371-1506 for SourceMedical About STEPHANIE
Best ASC Billing Practices & Potential Issues Speaker: Stephanie Ellis, R.N., CPC Ellis Medical Consulting, Inc. [email protected] www.ellismedical.com (615) 371-1506 for SourceMedical About STEPHANIE
US Reimbursement Guide
 US Reimbursement Guide The information with this notice is general reimbursement information only. It is not legal advice, nor is it about how to code, complete or submit any particular claim for payment.
US Reimbursement Guide The information with this notice is general reimbursement information only. It is not legal advice, nor is it about how to code, complete or submit any particular claim for payment.
Behavioral Health Services. Provider Manual
 Behavioral Health Provider Manual Provider Behavioral Health 1 May 1, 2014 TABLE OF CONTENTS Chapter I. General Program Policies Chapter II. Member Eligibility Chapter IV. Billing Iowa Medicaid Appendix
Behavioral Health Provider Manual Provider Behavioral Health 1 May 1, 2014 TABLE OF CONTENTS Chapter I. General Program Policies Chapter II. Member Eligibility Chapter IV. Billing Iowa Medicaid Appendix
IWCC 50 ILLINOIS ADMINISTRATIVE CODE 7110 7110.90. Section 7110.90 Illinois Workers' Compensation Commission Medical Fee Schedule
 Section 7110.90 Illinois Workers' Compensation Commission Medical Fee Schedule a) In accordance with Sections 8(a), 8.2 and 16 of the Workers' Compensation Act [820 ILCS 305/8(a), 8.2 and 16] (the Act),
Section 7110.90 Illinois Workers' Compensation Commission Medical Fee Schedule a) In accordance with Sections 8(a), 8.2 and 16 of the Workers' Compensation Act [820 ILCS 305/8(a), 8.2 and 16] (the Act),
HEALTHCARE COMMON PROCEDURE CODING SYSTEM (HCPCS) LEVEL II CODING PROCEDURES
 HEALTHCARE COMMON PROCEDURE CODING SYSTEM (HCPCS) LEVEL II CODING PROCEDURES This information provides a description of the procedures CMS follows in processing HCPCS code applications and making coding
HEALTHCARE COMMON PROCEDURE CODING SYSTEM (HCPCS) LEVEL II CODING PROCEDURES This information provides a description of the procedures CMS follows in processing HCPCS code applications and making coding
CONNECTIONS TESTING FOR ICD-10
 TESTING FOR ICD-10 In conjunction with the Centers for Medicare and Medicaid Services (CMS), Providence Health Plan (PHP) and all major payers will convert from International Classification of Diseases,
TESTING FOR ICD-10 In conjunction with the Centers for Medicare and Medicaid Services (CMS), Providence Health Plan (PHP) and all major payers will convert from International Classification of Diseases,
ASC Coding and Billing Fundamentals. Objectives
 ASC Coding and Billing Fundamentals Brenda Chidester-Palmer CPC, CPCI, CEMC, CASCC Objectives Guidelines/Regulations Covered Surgical Procedures Ancillary Supplies Separately Reportable Correct Use of
ASC Coding and Billing Fundamentals Brenda Chidester-Palmer CPC, CPCI, CEMC, CASCC Objectives Guidelines/Regulations Covered Surgical Procedures Ancillary Supplies Separately Reportable Correct Use of
EXPANDING YOUR HORIZONS
 Glaucoma Therapy EXPANDING YOUR HORIZONS Learn how to control glaucoma with SLT therapy. SLTPATIENT EDUCATION PROGRAM Glaucoma Glaucoma is a degenerative disease that if left untreated can cause permanent
Glaucoma Therapy EXPANDING YOUR HORIZONS Learn how to control glaucoma with SLT therapy. SLTPATIENT EDUCATION PROGRAM Glaucoma Glaucoma is a degenerative disease that if left untreated can cause permanent
Insurance 101. Infant and Toddler Coordinators Association. July 28, 2012 Capital City Hyatt. Laura Pizza Plum Plum Healthcare Consulting
 Insurance 101 Infant and Toddler Coordinators Association July 28, 2012 Capital City Hyatt Laura Pizza Plum 1 Agenda Basics of Health Insurance Frequently Asked Questions Early Intervention and working
Insurance 101 Infant and Toddler Coordinators Association July 28, 2012 Capital City Hyatt Laura Pizza Plum 1 Agenda Basics of Health Insurance Frequently Asked Questions Early Intervention and working
Kevin Corcoran is a consultant for Corcoran Consulting Group and acknowledges a financial interest in the subject matter of this presentation.
 Financial Disclosure Cataract and Premium IOL Surgery Kevin Corcoran is a consultant for Corcoran Consulting Group and acknowledges a financial interest in the subject matter of this presentation. Kevin
Financial Disclosure Cataract and Premium IOL Surgery Kevin Corcoran is a consultant for Corcoran Consulting Group and acknowledges a financial interest in the subject matter of this presentation. Kevin
Title 8, California Code of Regulations, 9789.30 et seq.
 Title 8, California Code of Regulations Chapter 4.5, Division of Workers Compensation Subchapter 1 Administrative Director-Administrative Rules Article 5.3 Official Medical Fee Schedule-Hospital Outpatient
Title 8, California Code of Regulations Chapter 4.5, Division of Workers Compensation Subchapter 1 Administrative Director-Administrative Rules Article 5.3 Official Medical Fee Schedule-Hospital Outpatient
Medical Practitioner Reimbursement
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Medical Practitioner Reimbursement L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 6 P U B L I S H E D : F E B R U A R Y 25,
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Medical Practitioner Reimbursement L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 6 P U B L I S H E D : F E B R U A R Y 25,
Intraoperative Nerve Monitoring Coding Guide. March 1, 2010
 Intraoperative Nerve Monitoring Coding Guide March 1, 2010 Please direct any questions to: Kim Brew Manager Reimbursement and Therapy Access Medtronic ENT (904) 279-7569 Rev 9/10 KB TO OUR PARTNERS IN
Intraoperative Nerve Monitoring Coding Guide March 1, 2010 Please direct any questions to: Kim Brew Manager Reimbursement and Therapy Access Medtronic ENT (904) 279-7569 Rev 9/10 KB TO OUR PARTNERS IN
Modifiers 80, 81, 82, and AS - Assistant At Surgery
 Manual: Policy Title: Reimbursement Policy Modifiers 80, 81, 82, and AS - Assistant At Surgery Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM013 Last Updated: 8/29/2014
Manual: Policy Title: Reimbursement Policy Modifiers 80, 81, 82, and AS - Assistant At Surgery Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM013 Last Updated: 8/29/2014
PROTOCOLS FOR PHYSICAL THERAPY PROVIDERS
 PROTOCOLS FOR PHYSICAL THERAPY PROVIDERS A Member may access Physical Therapy services (PT) when treatment is prescribed by a physician to restore or improve a person s ability to undertake activities
PROTOCOLS FOR PHYSICAL THERAPY PROVIDERS A Member may access Physical Therapy services (PT) when treatment is prescribed by a physician to restore or improve a person s ability to undertake activities
Reimbursement for Medical Products: Ensuring Marketplace
 Reimbursement for Medical Products: Ensuring Marketplace Success by Securing Coverage and Payment Christopher J. Panarites, Ph.D. Director, Endovascular Products Health Economics and Outcomes Research
Reimbursement for Medical Products: Ensuring Marketplace Success by Securing Coverage and Payment Christopher J. Panarites, Ph.D. Director, Endovascular Products Health Economics and Outcomes Research
