Insurance 101. Infant and Toddler Coordinators Association. July 28, 2012 Capital City Hyatt. Laura Pizza Plum Plum Healthcare Consulting
|
|
|
- Amberlynn Johnston
- 8 years ago
- Views:
Transcription
1 Insurance 101 Infant and Toddler Coordinators Association July 28, 2012 Capital City Hyatt Laura Pizza Plum 1
2 Agenda Basics of Health Insurance Frequently Asked Questions Early Intervention and working with Insurance Companies Questions 2
3 Definitions Eligibility Verification for participation Member Cost Sharing Copayment or copay is a payment defined in the insurance policy and paid by the insured person each time a medical service is accessed. Copayments do not usually contribute towards any policy out-ofpocket maximums whereas coinsurance payments do. Member Cost Sharing Deductible is the amount of expenses that must be paid out of pocket before an insurer will pay any expenses. It is normally quoted as a fixed dollar amount. The deductible must be paid by the insured, before the benefits of the policy can apply. Typically, a general rule is: the higher the deductible, the lower the premium, and vice versa. Depending on the policy, the deductible may apply per covered incident, or per year. 3
4 Referral Definitions is the transfer of care for a patient from one clinician to another service. Authorization are typically required for specific items and services under most health plans. Specific benefits may vary by product and/or employer group. It is always recommended that you reference appropriate member materials (e.g., the Benefit Handbook, Certificate of Coverage and/or on line Provider Manual) for member-specific benefit information for each insurer. Billing Electronic billing, also called EBP or electronic bill and payment, is the process in which the bill is sent to the customer and/or the insurance company over the internet. 4
5 Definitions Procedure Codes Physicians bill their services using procedure codes developed by a seventeen member committee known as the CPT Editorial Panel. The AMA nominates eleven of the members while the remaining seats are nominated by the BCBS Association, Health Insurance Association of America, CMS and the American Hospital Association. The CPT Committee issues new codes two times per year. Current Procedural Terminology (CPT) The CPT code set is maintained by the AMA CPT Editorial Panel. The CPT code set describes medical, surgical, and diagnostic services and is designed to communicate uniform information about medical services and procedures among physicians, patients, accreditation organizations, and payers for administrative and financial purposes. New editions are released annually, each October. CPT codes are typically referred to as Level 1 codes. Healthcare Common Procedure Coding System (HCPCS) The HCPCS code set is based on CPT coding. HCPCS includes two levels of codes: Level I consists of the CPT codes and is numeric. Level II codes are alphanumeric and primarily include non-physician services for example, ambulance services and durable medical equipment devices, and represent items and supplies not covered by CPT. 5
6 Definitions Relative Value Unit (RVU) is a measure of value used by Medicare as a reimbursement formula for physician services. Before RVUs were used, Medicare paid for physician services using usual and customary charges, which led to payment variability. The Consolidated Omnibus Budget Reconciliation Act of 1985 enacted a Medicare fee schedule. There currently about 7,000 distinct physician services listed. Resource-based relative value scale (RBRVS) is a methodology used to determine how much money medical providers should be paid. It is used by Medicare and many health insurance companies in the US to determine fee schedules. For each service, a payment formula contains three RVUs, one for physician work, one for practice expense, and one for malpractice expense. RBRVS assigns procedures performed by a physician or other medical provider a relative value which is adjusted by geographic region (so a procedure performed in NH may be worth more than a procedure performed in MA). This value is then multiplied by a fixed conversion factor, which changes annually, to determine the amount of payment. 6
7 Diagnostic Codes Definitions are used to group and identify diseases, disorders, and/or symptoms, and are used to measure morbidity and mortality. There is typically not one code for all purposes. The National Centers for Health Statistics (NCHS) and CMS are responsible for overseeing all changes and modifications. The codes may be frequently revised as new knowledge is attained. Diagnosis codes are sometimes referred to as ICD-9 (International Classification of Diseases) codes or ICD-10 (implementation in October 2013). New editions are released annually, each October. 7
8 The Revenue Cycle (enrollment, claims and customer service)
9 Self-service and best practices Throughout the revenue cycle Scheduling & Patient Visit Verify eligibility Member cost sharing Referral/Authorizations Other Policies/Procedures Clinical Programs Preventive Health Disease + Health Risk Management Clinical Guidelines Claim Submission Re-verify Eligibility Referral/Authorization Submit Claim Policies Reduce Outstanding Account Receivables Claim Status Timely appeals/corrections AR Reports/Trending Policies Work In-Process or Rejected Claims Response Report/ File Claim Status Eligibility Policies Electronic Claim Remittance Advice Auto post remittance 9
10 Frequently Asked Questions 10
11 What are the type of insurers? There are two categories of insurers: Private or Commercial (privately held companies) Public or CMS; Centers for Medicare & Medicaid Services (maintained by federal and state government) 11
12 What is 3 rd party payer reimbursement? Health care finance experts make reference to third party payment or third party payers. The first party is the patient. The second party is the physician, clinic, hospital, nursing home or other heath care entity also known as the provider. The third party is the insurance company or health agency that pays the provider or second party for the care or services rendered to the patient or first party. 12
13 What kinds of reimbursement limitations are there? Reimbursement is limited in many ways By medical policies and benefits -- the patient through their insurer, certain diagnosis and procedures are covered and others are not. By networks of providers. In order for patients to receive the maximum benefits (as well as the provider performing the service), patients should stay in network. Providers must participate in the insurance plan (Medicare, Medicaid or a commercial plan) in order to be paid according the established fee schedule. By the fee schedule established by the insurer for providers participating in their network. For maximum reimbursement the provider should be participating in the insurance plan. Some benefit packages limit the number of sessions a particular service can be provided, e.g., 40 therapy visits per calendar year or one annual well visit per year. Additionally, many services require prior authorization or referrals from the PCP prior to the service or procedure being performed. Payment could be denied if the proper steps are not taken in advance. 13
14 Why do insurance companies have their own rates vs. Medicare/Medicaid? Medicare is divided into jurisdictions and each jurisdiction is managed by a fiscal intermediary. In MA, the fiscal intermediary is National Heritage Insurance Company. This company is responsible for Medicare enrollment and providers rate setting following Medicare guidelines and claims processing and payment. Federal Medicaid law does not set precise requirements for reimbursement, hence each state has the ability to set its own Medicaid rates. In most states, Medicaid rates are lower than Medicare rates. Medicare pays less than commercial payers. Most insurance companies set their own rates using Medicare and/or Medicaid as their benchmark. Rates are set based on the regional need and demands of the provider community for reimbursement. 14
15 How is billing done? Billing is done via a claim form which varies by the place of service. For a hospital service billed under the hospital Tax Identification Number, a UB 04 form is used. For clinic or individual physicians or free standing ancillary provider, a HCFA 1500 form is used. Each payer including Medicare and Medicaid have their own billing guidelines. Most commercial payers mirror Medicare billing protocols with a few caveats. Most billing protocols are available on line or by calling the claims or provider service department of the payer. In all cases a TID and an NPI number (National Provider Identifier) are required on the form along with diagnosis codes and procedure codes. The provider of service must be entered into the payer claims system and in many cases a W-9 form is required prior to payment of claims. 15
16 Affordable Care Act The Affordable Care Act (commonly known as the health reform law) encourages the formation of medical homes and accountable care organizations (ACOs), in the belief that they will improve health care quality and slow the growth of health care spending in America. By organizing health care teams, technology and knowledge around patient needs, Accountable Care can help the system realize its full potential. The Affordable Care Act includes a provision that allows Medicare to reward health care organizations with a share of the savings that would result from improving care quality and reducing cost. To participate in this shared savings programs, health care organizations need to become Accountable Care Organizations (ACOs). Generally, an ACO can be defined as a set of healthcare providers --- including primary care physicians, specialists, and hospitals --- that work together collaboratively and accept collective accountability for the cost and quality of care delivered to a population of patients. The ACO concept that has been widely discussed among health researchers. According to the Commonwealth Fund, 54 percent of health care leaders believe that ACOs are an effective model of care. The Congressional Budget Office projects that the shared savings program will save $5 billion over 5 years ( ). 16
17 Affordable Care Act The Patient-Centered Medical Home model was proposed by the American Academy of Family Physicians, American Academy of Pediatrics, American College of Physicians, and American Osteopathic Association in Patient-Centered Medical Home is an enhanced primary care delivery model that strives to achieve better access, coordination of care, prevention, quality, and safety within the primary care practice, and strives to create a strong partnership between the patient and primary care physician. The Accountable Care Organization is also based around a strong primary care core. But ACOs are comprised of many medical homes, i.e., many primary care providers and/or practices that work together. The difference is that ACOs would be accountable for the cost and quality of care both within and outside of the primary care relationship. As such, ACOs must include specialists and hospitals in order to be able to control costs and improve health outcomes across the entire care continuum. ACOs by nature would be larger than a single medical home or physician s office. 17
18 EI and working with Insurance Companies 18
19 EI and working with Insurance Companies EI coverage varies by State Know your insurance companies How best to work with your providers and insurance companies 19
20 Questions 20
Glossary of Insurance and Medical Billing Terms
 A Accept Assignment Provider has agreed to accept the insurance company allowed amount as full payment for the covered services. Adjudication The final determination of the issues involving settlement
A Accept Assignment Provider has agreed to accept the insurance company allowed amount as full payment for the covered services. Adjudication The final determination of the issues involving settlement
Billing and Claim Billing and Claim Submission Boot Camp Submission Boot Camp Beverly Remm Beverly Remm
 Billing and Claim Submission Boot Camp Presented by: Beverly Remm Orion Healthcare Technology Billing and Claim Submission Boot Camp Presented by: Beverly Remm Orion Healthcare Technology The presentation
Billing and Claim Submission Boot Camp Presented by: Beverly Remm Orion Healthcare Technology Billing and Claim Submission Boot Camp Presented by: Beverly Remm Orion Healthcare Technology The presentation
Glossary of Frequently Used Billing and Coding Terms
 Glossary of Frequently Used Billing and Coding Terms Accountable Care Organization (ACO) Accounts Receivable Reports All Inclusive Fees Allowances and Adjustments Capitation Payments Care Coordination
Glossary of Frequently Used Billing and Coding Terms Accountable Care Organization (ACO) Accounts Receivable Reports All Inclusive Fees Allowances and Adjustments Capitation Payments Care Coordination
Glossary. Adults: Individuals ages 19 through 64. Allowed amounts: See prices paid. Allowed costs: See prices paid.
 Glossary Acute inpatient: A subservice category of the inpatient facility clams that have excluded skilled nursing facilities (SNF), hospice, and ungroupable claims. This subcategory was previously known
Glossary Acute inpatient: A subservice category of the inpatient facility clams that have excluded skilled nursing facilities (SNF), hospice, and ungroupable claims. This subcategory was previously known
Compensation and Claims Processing
 Compensation and Claims Processing Compensation The network rate for eligible outpatient visits is reimbursed to you at the lesser of (1) your customary charge, less any applicable co-payments, coinsurance
Compensation and Claims Processing Compensation The network rate for eligible outpatient visits is reimbursed to you at the lesser of (1) your customary charge, less any applicable co-payments, coinsurance
HIPAA Glossary of Terms
 ANSI - American National Standards Institute (ANSI): An organization that accredits various standards-setting committees, and monitors their compliance with the open rule-making process that they must
ANSI - American National Standards Institute (ANSI): An organization that accredits various standards-setting committees, and monitors their compliance with the open rule-making process that they must
University of Mississippi Medical Center. Access Management. Patient Access Specialists II
 Financial Terminology in Access Management University of Mississippi Medical Center Access Management Patient Access Specialists II As a Patient Access Specialist You are the FIRST STAGE in the Revenue
Financial Terminology in Access Management University of Mississippi Medical Center Access Management Patient Access Specialists II As a Patient Access Specialist You are the FIRST STAGE in the Revenue
Initial Preventive Physical Examination
 Initial Preventive Physical Examination Overview The Medicare Prescription Drug, Improvement, and Modernization Act (MMA) of 2003 expanded Medicare's coverage of preventive services. Central to the Centers
Initial Preventive Physical Examination Overview The Medicare Prescription Drug, Improvement, and Modernization Act (MMA) of 2003 expanded Medicare's coverage of preventive services. Central to the Centers
RVU BASED PHYSICIAN COMPENSATION AND PRODUCTIVITY
 RVU BASED PHYSICIAN COMPENSATION AND PRODUCTIVITY Ten Recommendations for Determining Physician Compensation/Productivity Through Relative Value Units 2011 Merritt Hawkins 5001 Statesman Drive Irving,
RVU BASED PHYSICIAN COMPENSATION AND PRODUCTIVITY Ten Recommendations for Determining Physician Compensation/Productivity Through Relative Value Units 2011 Merritt Hawkins 5001 Statesman Drive Irving,
Medicare Chronic Care Management Service Essentials
 Medicare Chronic Care Management Service Essentials As part of an ongoing effort to enhance care coordination for Medicare beneficiaries, the Centers for Medicare & Medicaid Services (CMS) established
Medicare Chronic Care Management Service Essentials As part of an ongoing effort to enhance care coordination for Medicare beneficiaries, the Centers for Medicare & Medicaid Services (CMS) established
Chiropractic Assistants Insurance Verification Training Guide
 Chiropractic Assistants Insurance Verification Training Guide What You Will Learn: How to Obtain Maximum Chiropractic Benefits Tools Needed to Verify Benefits Understanding Why You Are Verifying Understanding
Chiropractic Assistants Insurance Verification Training Guide What You Will Learn: How to Obtain Maximum Chiropractic Benefits Tools Needed to Verify Benefits Understanding Why You Are Verifying Understanding
Behavioral Health Services. Provider Manual
 Behavioral Health Provider Manual Provider Behavioral Health 1 May 1, 2014 TABLE OF CONTENTS Chapter I. General Program Policies Chapter II. Member Eligibility Chapter IV. Billing Iowa Medicaid Appendix
Behavioral Health Provider Manual Provider Behavioral Health 1 May 1, 2014 TABLE OF CONTENTS Chapter I. General Program Policies Chapter II. Member Eligibility Chapter IV. Billing Iowa Medicaid Appendix
What You Need to Know for the Upcoming Transition to ICD-10. Written by the AMA CPT Medical Informatics Department
 What You Need to Know for the Upcoming Transition to ICD-10 Written by the AMA CPT Medical Informatics Department W H I T E P A P E R J U N E 2 0 1 2 This white paper is for educational purposes only and
What You Need to Know for the Upcoming Transition to ICD-10 Written by the AMA CPT Medical Informatics Department W H I T E P A P E R J U N E 2 0 1 2 This white paper is for educational purposes only and
Cracking the Code Billing Beyond MNT ADA Coding and Coverage Committee
 Cracking the Code Billing Beyond MNT ADA Coding and Coverage Committee Billing Primer To successfully bill for nutrition services provided by RDs, practitioners need to become familiar with certain terms
Cracking the Code Billing Beyond MNT ADA Coding and Coverage Committee Billing Primer To successfully bill for nutrition services provided by RDs, practitioners need to become familiar with certain terms
Compensation and Claims Processing
 Compensation and Claims Processing Compensation The network rate for eligible outpatient visits is reimbursed to you at the lesser of (1) your customary charge, less any applicable co-payments, coinsurance
Compensation and Claims Processing Compensation The network rate for eligible outpatient visits is reimbursed to you at the lesser of (1) your customary charge, less any applicable co-payments, coinsurance
Medical Practitioner Reimbursement
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Medical Practitioner Reimbursement L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 6 P U B L I S H E D : F E B R U A R Y 25,
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Medical Practitioner Reimbursement L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 6 P U B L I S H E D : F E B R U A R Y 25,
Screening, Brief Intervention and Referral to Treatment SBIRT Coding, Billing and Reimbursement Manual
 Screening, Brief Intervention and Referral to Treatment SBIRT Coding, Billing and Reimbursement Manual Prepared For: Wisconsin Initiative to Promote Healthy Lifestyles (WIPHL) January 2010 Table of Contents
Screening, Brief Intervention and Referral to Treatment SBIRT Coding, Billing and Reimbursement Manual Prepared For: Wisconsin Initiative to Promote Healthy Lifestyles (WIPHL) January 2010 Table of Contents
1. How do I calculate the reimbursement rate for medical services and treatment?
 MEDICAL SERVICES AND TREATMENT HOW TO CALCULATE REIMBURSEMENT RATES 1. How do I calculate the reimbursement rate for medical services and treatment? The reimbursement rate for medical services and treatment
MEDICAL SERVICES AND TREATMENT HOW TO CALCULATE REIMBURSEMENT RATES 1. How do I calculate the reimbursement rate for medical services and treatment? The reimbursement rate for medical services and treatment
FAQs on Billing for Health and Behavior Services
 FAQs on Billing for Health and Behavior Services by Government Relations Staff January 29, 2009 Practicing psychologists are eligible to bill for applicable services and receive reimbursement from Medicare
FAQs on Billing for Health and Behavior Services by Government Relations Staff January 29, 2009 Practicing psychologists are eligible to bill for applicable services and receive reimbursement from Medicare
Understanding the HIPAA standard transactions: The HIPAA Transactions and Code Set rule
 Understanding the HIPAA standard transactions: The HIPAA Transactions and Code Set rule Many physician practices recognize the Health Information Portability and Accountability Act (HIPAA) as both a patient
Understanding the HIPAA standard transactions: The HIPAA Transactions and Code Set rule Many physician practices recognize the Health Information Portability and Accountability Act (HIPAA) as both a patient
CLAIM FORM REQUIREMENTS
 CLAIM FORM REQUIREMENTS When billing for services, please pay attention to the following points: Submit claims on a current CMS 1500 or UB04 form. Please include the following information: 1. Patient s
CLAIM FORM REQUIREMENTS When billing for services, please pay attention to the following points: Submit claims on a current CMS 1500 or UB04 form. Please include the following information: 1. Patient s
Basics of the Healthcare Professional s Revenue Cycle
 Basics of the Healthcare Professional s Revenue Cycle Payer View of the Claim and Payment Workflow Brenda Fielder, Cigna May 1, 2012 Objective Explain the claim workflow from the initial interaction through
Basics of the Healthcare Professional s Revenue Cycle Payer View of the Claim and Payment Workflow Brenda Fielder, Cigna May 1, 2012 Objective Explain the claim workflow from the initial interaction through
Medicaid Purchasing Administration (MPA) Diabetes Education Program Billing Instructions. ProviderOne Readiness Edition
 Medicaid Purchasing Administration (MPA) Diabetes Education Program Billing Instructions ProviderOne Readiness Edition About This Publication This publication supersedes all previous Department/MPA Diabetes
Medicaid Purchasing Administration (MPA) Diabetes Education Program Billing Instructions ProviderOne Readiness Edition About This Publication This publication supersedes all previous Department/MPA Diabetes
GLOSSARY OF MEDICAL AND INSURANCE TERMS
 GLOSSARY OF MEDICAL AND INSURANCE TERMS At Westfield Family Physicians we are aware that there are lots of words and phrases we used every day that may not be familiar to you, our patients. We are providing
GLOSSARY OF MEDICAL AND INSURANCE TERMS At Westfield Family Physicians we are aware that there are lots of words and phrases we used every day that may not be familiar to you, our patients. We are providing
Premera Blue Cross Medicare Advantage Provider Reference Manual
 Premera Blue Cross Medicare Advantage Provider Reference Manual Introduction to Premera Blue Cross Medicare Advantage Plans Premera Blue Cross offers Medicare Advantage (MA) plans in King, Pierce, Snohomish,
Premera Blue Cross Medicare Advantage Provider Reference Manual Introduction to Premera Blue Cross Medicare Advantage Plans Premera Blue Cross offers Medicare Advantage (MA) plans in King, Pierce, Snohomish,
HIPAA: AN OVERVIEW September 2013
 HIPAA: AN OVERVIEW September 2013 Introduction The Health Insurance Portability and Accountability Act of 1996, known as HIPAA, was enacted on August 21, 1996. The overall goal was to simplify and streamline
HIPAA: AN OVERVIEW September 2013 Introduction The Health Insurance Portability and Accountability Act of 1996, known as HIPAA, was enacted on August 21, 1996. The overall goal was to simplify and streamline
National Correct Coding Initiative Policy Manual for Medicare Services Revision Date: January 1, 2014
 National Correct Coding Initiative Policy Manual for Medicare Services Revision Date: January 1, 2014 Current Procedural Terminology 2013 American Medical Association. All Rights Reserved. Current Procedural
National Correct Coding Initiative Policy Manual for Medicare Services Revision Date: January 1, 2014 Current Procedural Terminology 2013 American Medical Association. All Rights Reserved. Current Procedural
Revenue Cycle Management: The steps Title X agencies must take to get paid
 Revenue Cycle Management: The steps Title X agencies must take to get paid Webinar 2: Revenue Cycle Management: After the Client Visit August 7 th, 2013 Intended Audience Title X Grantee and sub-recipient
Revenue Cycle Management: The steps Title X agencies must take to get paid Webinar 2: Revenue Cycle Management: After the Client Visit August 7 th, 2013 Intended Audience Title X Grantee and sub-recipient
Copayment: The amount you must pay for each medical visit to a participating doctor or other healthcare provider, usually at this time service.
 Basic Terms How to calculate Out of Pocket Costs on a Hospital Stay: If you have a $2000 deductible and 30% coinsurance health insurance plan. If you have a $10,000 emergency room or hospital stay your
Basic Terms How to calculate Out of Pocket Costs on a Hospital Stay: If you have a $2000 deductible and 30% coinsurance health insurance plan. If you have a $10,000 emergency room or hospital stay your
Glossary of Terms. Account Number/Client Code. Adjudication ANSI. Assignment of Benefits
 Account Number/Client Code Adjudication ANSI Assignment of Benefits Billing Provider/Pay-to-Provider Billing Service Business Associate Agreement Clean Claim Clearinghouse CLIA Number (Clinical Laboratory
Account Number/Client Code Adjudication ANSI Assignment of Benefits Billing Provider/Pay-to-Provider Billing Service Business Associate Agreement Clean Claim Clearinghouse CLIA Number (Clinical Laboratory
Collaborative Care Tips for Sustainability. Virna Little, PsyD, LCSW r, SAP The Institute for Family Health NYS Collaborative Care Initiative
 Collaborative Care Tips for Sustainability Virna Little, PsyD, LCSW r, SAP The Institute for Family Health NYS Collaborative Care Initiative Teamwork Applies to Billing Too!!! Combine with other initiatives
Collaborative Care Tips for Sustainability Virna Little, PsyD, LCSW r, SAP The Institute for Family Health NYS Collaborative Care Initiative Teamwork Applies to Billing Too!!! Combine with other initiatives
Transitioning from ICD-9-CM to ICD-10-CM. Tidewater Physicians Multispecialty Group Williamsburg, VA
 Transitioning from ICD-9-CM to ICD-10-CM Tidewater Physicians Multispecialty Group Williamsburg, VA February 22, 2014 Our Agenda Some guidelines for this morning s presentation Our Transformational Point
Transitioning from ICD-9-CM to ICD-10-CM Tidewater Physicians Multispecialty Group Williamsburg, VA February 22, 2014 Our Agenda Some guidelines for this morning s presentation Our Transformational Point
Informational Series. Community TM. Glossary of Health Insurance & Medical Terminology. (855) 624-6463 HealthOptions.
 Informational Series Glossary of Health Insurance & Medical Terminology How to use this glossary This glossary has many commonly used terms, but isn t a full list. These glossary terms and definitions
Informational Series Glossary of Health Insurance & Medical Terminology How to use this glossary This glossary has many commonly used terms, but isn t a full list. These glossary terms and definitions
MEDICARE CROSSOVER PROCESS FREQUENTLY ASKED QUESTIONS
 MEDICARE CROSSOVER PROCESS FREQUENTLY ASKED QUESTIONS QUESTION 1. What is meant by the crossover payment? ANSWER When Medicaid providers submit claims to Medicare for Medicare/Medicaid beneficiaries, Medicare
MEDICARE CROSSOVER PROCESS FREQUENTLY ASKED QUESTIONS QUESTION 1. What is meant by the crossover payment? ANSWER When Medicaid providers submit claims to Medicare for Medicare/Medicaid beneficiaries, Medicare
To submit electronic claims, use the HIPAA 837 Institutional transaction
 3.1 Claim Billing 3.1.1 Which Claim Form to Use Claims that do not require attachments may be billed electronically using Provider Electronic Solutions (PES) software (provided by Electronic Data Systems
3.1 Claim Billing 3.1.1 Which Claim Form to Use Claims that do not require attachments may be billed electronically using Provider Electronic Solutions (PES) software (provided by Electronic Data Systems
410-130-0005 Federally Qualified Primary Care Provider NEW RULE
 410-130-0005 Federally Qualified Primary Care Provider NEW RULE Federally Qualified Primary Care Provider (1) Section 1202 of the Affordable Care Act (ACA) amended sections 1902(a)(13), 1902(jj), 1905(dd)
410-130-0005 Federally Qualified Primary Care Provider NEW RULE Federally Qualified Primary Care Provider (1) Section 1202 of the Affordable Care Act (ACA) amended sections 1902(a)(13), 1902(jj), 1905(dd)
The benefits of electronic claims submission improve practice efficiencies
 The benefits of electronic claims submission improve practice efficiencies Electronic claims submission vs. manual claims submission An electronic claim is a paperless patient claim form generated by computer
The benefits of electronic claims submission improve practice efficiencies Electronic claims submission vs. manual claims submission An electronic claim is a paperless patient claim form generated by computer
COM Compliance Policy No. 3
 COM Compliance Policy No. 3 THE UNIVERSITY OF ILLINOIS AT CHICAGO NO.: 3 UIC College of Medicine DATE: 8/5/10 Chicago, Illinois PAGE: 1of 7 UNIVERSITY OF ILLINOIS COLLEGE OF MEDICINE CODING AND DOCUMENTATION
COM Compliance Policy No. 3 THE UNIVERSITY OF ILLINOIS AT CHICAGO NO.: 3 UIC College of Medicine DATE: 8/5/10 Chicago, Illinois PAGE: 1of 7 UNIVERSITY OF ILLINOIS COLLEGE OF MEDICINE CODING AND DOCUMENTATION
The American Academy of Pediatrics - A Review
 Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children POLICY STATEMENT Application of the Resource-Based Relative Value Scale System to Pediatrics
Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children POLICY STATEMENT Application of the Resource-Based Relative Value Scale System to Pediatrics
PROTOCOLS FOR PHYSICAL THERAPY PROVIDERS
 PROTOCOLS FOR PHYSICAL THERAPY PROVIDERS A Member may access Physical Therapy services (PT) when treatment is prescribed by a physician to restore or improve a person s ability to undertake activities
PROTOCOLS FOR PHYSICAL THERAPY PROVIDERS A Member may access Physical Therapy services (PT) when treatment is prescribed by a physician to restore or improve a person s ability to undertake activities
The Hospital Billing Process The purpose of this chapter is to provide an overview of the hospital billing process. The
 3 Section One: Section Title Chapter 5 The Hospital Billing Process The purpose of this chapter is to provide an overview of the hospital billing process. The billing process includes submitting charges
3 Section One: Section Title Chapter 5 The Hospital Billing Process The purpose of this chapter is to provide an overview of the hospital billing process. The billing process includes submitting charges
A. CPT Coding System B. CPT Categories, Subcategories, and Headings
 OST 148 MEDICAL CODING, BILLING AND INSURANCE COURSE DESCRIPTION: Prerequisites: None Corequisites: None This course introduces CPT and ICD coding as they apply to medical insurance and billing. Emphasis
OST 148 MEDICAL CODING, BILLING AND INSURANCE COURSE DESCRIPTION: Prerequisites: None Corequisites: None This course introduces CPT and ICD coding as they apply to medical insurance and billing. Emphasis
Reimbursement for Medical Products: Ensuring Marketplace
 Reimbursement for Medical Products: Ensuring Marketplace Success by Securing Coverage and Payment Christopher J. Panarites, Ph.D. Director, Endovascular Products Health Economics and Outcomes Research
Reimbursement for Medical Products: Ensuring Marketplace Success by Securing Coverage and Payment Christopher J. Panarites, Ph.D. Director, Endovascular Products Health Economics and Outcomes Research
Frequently Asked Questions about ICD-10
 Frequently Asked Questions about -10 Q: What is the current status of -10? A: The U.S. Department of Health and Human Services (HHS) has issued its final rule that the -9-CM code sets be replaced with
Frequently Asked Questions about -10 Q: What is the current status of -10? A: The U.S. Department of Health and Human Services (HHS) has issued its final rule that the -9-CM code sets be replaced with
Insurance Coverage for ABA in Texas. Kate Johnson-Patagoc, M.S., BCBA Kelle Rich, M.Ed., BCBA Wesley H. Dotson, Ph.D., BCBA
 Insurance Coverage for ABA in Texas Kate Johnson-Patagoc, M.S., BCBA Kelle Rich, M.Ed., BCBA Wesley H. Dotson, Ph.D., BCBA About the Presenters Kate Johnson-Patagoc, MS, BCBA Director of Specialized Services,
Insurance Coverage for ABA in Texas Kate Johnson-Patagoc, M.S., BCBA Kelle Rich, M.Ed., BCBA Wesley H. Dotson, Ph.D., BCBA About the Presenters Kate Johnson-Patagoc, MS, BCBA Director of Specialized Services,
Section 9. Claims Claim Submission Molina Healthcare PO Box 22815 Long Beach, CA 90801
 Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Molina Healthcare of Ohio, Inc. PO Box 22712 Long Beach, CA 90801
 Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Revenue Cycle Responsibilities. Revenue Cycle. Objectives 4/9/2013
 Revenue Cycle Kathryn DeVault, RHIA, CCS, CCS-P AHIMA 2013 Objectives Identify responsibilities within the Revenue Cycle Focus on management of the revenue cycle process Discuss the revenue cycle process
Revenue Cycle Kathryn DeVault, RHIA, CCS, CCS-P AHIMA 2013 Objectives Identify responsibilities within the Revenue Cycle Focus on management of the revenue cycle process Discuss the revenue cycle process
VEI Consulting Services. 2013 Evaluation and Management Update. Effective January 1, 2013
 VEI Consulting Services 2013 Evaluation and Management Update Effective January 1, 2013 Pat Schmitter CPC, CPC-I Sr. Healthcare Consultant Instructor Professional Medical Coding Curriculum AHIMA Approved
VEI Consulting Services 2013 Evaluation and Management Update Effective January 1, 2013 Pat Schmitter CPC, CPC-I Sr. Healthcare Consultant Instructor Professional Medical Coding Curriculum AHIMA Approved
* Dignity Health. Success
 * Dignity Health. Tools for Success Table of Contents ICD 10 Overview Physician Practice Checklist Financial Planning for ICD 10 ICD 10 Education for Physicians ICD 10 Education for Staff ICD 10 Impacts
* Dignity Health. Tools for Success Table of Contents ICD 10 Overview Physician Practice Checklist Financial Planning for ICD 10 ICD 10 Education for Physicians ICD 10 Education for Staff ICD 10 Impacts
INTERMEDIATE ADMINISTRATIVE SIMPLIFICATION CENTERS FOR MEDICARE & MEDICAID SERVICES. Online Guide to: ADMINISTRATIVE SIMPLIFICATION
 02 INTERMEDIATE» Online Guide to: CENTERS FOR MEDICARE & MEDICAID SERVICES Last Updated: February 2014 TABLE OF CONTENTS INTRODUCTION: ABOUT THIS GUIDE... i About Administrative Simplification... 2 Why
02 INTERMEDIATE» Online Guide to: CENTERS FOR MEDICARE & MEDICAID SERVICES Last Updated: February 2014 TABLE OF CONTENTS INTRODUCTION: ABOUT THIS GUIDE... i About Administrative Simplification... 2 Why
CODING. Neighborhood Health Plan 1 Provider Payment Guidelines
 CODING Policy The terms of this policy set forth the guidelines for reporting the provision of care rendered by NHP participating providers, including but not limited to use of standard diagnosis and procedure
CODING Policy The terms of this policy set forth the guidelines for reporting the provision of care rendered by NHP participating providers, including but not limited to use of standard diagnosis and procedure
Position Paper on. Evaluation and Management Services (E/M) with Osteopathic Manipulative Treatment (OMT)
 Position Paper on Evaluation and Management Services (E/M) with Osteopathic Manipulative Treatment (OMT) Revised July 2006 AOA Division of Socioeconomic Affairs AOA POSITION ON E/M AND OMT SERVICES The
Position Paper on Evaluation and Management Services (E/M) with Osteopathic Manipulative Treatment (OMT) Revised July 2006 AOA Division of Socioeconomic Affairs AOA POSITION ON E/M AND OMT SERVICES The
Top 50 Billing Error Reason Codes With Common Resolutions (09-12)
 Top 50 Billing Error Reason Codes With Common Resolutions (09-12) On the following table you will find the top 50 Error Reason Codes with Common Resolutions for denied claims at Virginia Medicaid. This
Top 50 Billing Error Reason Codes With Common Resolutions (09-12) On the following table you will find the top 50 Error Reason Codes with Common Resolutions for denied claims at Virginia Medicaid. This
Senate-Passed Bill (Patient Protection and Affordable Care Act H.R. 3590)**
 Prevention and Screening Services Cost-sharing Eliminates cost sharing requirements for requirements for all preventive services (including prevention and colorectal cancer screening) that have a screening
Prevention and Screening Services Cost-sharing Eliminates cost sharing requirements for requirements for all preventive services (including prevention and colorectal cancer screening) that have a screening
Zimmer Payer Coverage Approval Process Guide
 Zimmer Payer Coverage Approval Process Guide Market Access You ve Got Questions. We ve Got Answers. INSURANCE VERIFICATION PROCESS ELIGIBILITY AND BENEFITS VERIFICATION Understanding and verifying a patient
Zimmer Payer Coverage Approval Process Guide Market Access You ve Got Questions. We ve Got Answers. INSURANCE VERIFICATION PROCESS ELIGIBILITY AND BENEFITS VERIFICATION Understanding and verifying a patient
Fundamental Guide to Understanding Healthcare Payments
 Fundamental Guide to Understanding Healthcare Payments Monday April 22 nd 9:30 10:30am Stuart Hanson Director, Healthcare Solutions Executive Citi Enterprise Payments Irfan Ahmad VP, Healthcare Payments
Fundamental Guide to Understanding Healthcare Payments Monday April 22 nd 9:30 10:30am Stuart Hanson Director, Healthcare Solutions Executive Citi Enterprise Payments Irfan Ahmad VP, Healthcare Payments
Accountable Care Organization Workgroup Glossary
 Accountable Care Organization Workgroup Glossary Accountable care organization (ACO) a group of coordinated health care providers that care for all or some of the health care needs of a defined population.
Accountable Care Organization Workgroup Glossary Accountable care organization (ACO) a group of coordinated health care providers that care for all or some of the health care needs of a defined population.
Molina Healthcare of Washington, Inc. CLAIMS
 CLAIMS As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your reference:
CLAIMS As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your reference:
Status Active. Assistant Surgeons. This policy addresses reimbursement for assistant surgical procedures during the same operative session.
 Status Active Reimbursement Policy Section: Surgery/Interventional Procedure Policy Number: RP - Surgery/Interventional Procedure - 001 Assistant Surgeons Effective Date: June 1, 2015 Assistant Surgeons
Status Active Reimbursement Policy Section: Surgery/Interventional Procedure Policy Number: RP - Surgery/Interventional Procedure - 001 Assistant Surgeons Effective Date: June 1, 2015 Assistant Surgeons
ICD-10 Preparation for Dental Providers. July 2014
 ICD-10 Preparation for Dental Providers July 2014 What is ICD-10? The International Classification of Diseases (ICD) is a set of codes used worldwide to classify medical diagnoses and inpatient procedures.
ICD-10 Preparation for Dental Providers July 2014 What is ICD-10? The International Classification of Diseases (ICD) is a set of codes used worldwide to classify medical diagnoses and inpatient procedures.
This information is current as of the training dates.
 Welcome to this training on Billing Basics for Washington State Local Health Jurisdictions. This training will help you understand basic principles and processes needed for billing private insurance. This
Welcome to this training on Billing Basics for Washington State Local Health Jurisdictions. This training will help you understand basic principles and processes needed for billing private insurance. This
How Health Reform Will Affect Health Care Quality and the Delivery of Services
 Fact Sheet AARP Public Policy Institute How Health Reform Will Affect Health Care Quality and the Delivery of Services The recently enacted Affordable Care Act contains provisions to improve health care
Fact Sheet AARP Public Policy Institute How Health Reform Will Affect Health Care Quality and the Delivery of Services The recently enacted Affordable Care Act contains provisions to improve health care
Disclaimer CODING 101 BOOT CAMP CODING SEMINAR FOR NEW PHYSICIANS
 CODING 101 BOOT CAMP CODING SEMINAR FOR NEW PHYSICIANS AND STAFF Chicago Dermatological Society January 26, 2013 Presented by Joy Newby, LPN, CPC, PCS Newby Consulting, Inc. 5725 Park Plaza Court Indianapolis,
CODING 101 BOOT CAMP CODING SEMINAR FOR NEW PHYSICIANS AND STAFF Chicago Dermatological Society January 26, 2013 Presented by Joy Newby, LPN, CPC, PCS Newby Consulting, Inc. 5725 Park Plaza Court Indianapolis,
HOW TO PREVENT AND MANAGE MEDICAL CLAIM DENIALS TO INCREASE REVENUE
 Billing & Reimbursement Revenue Cycle Management HOW TO PREVENT AND MANAGE MEDICAL CLAIM DENIALS TO INCREASE REVENUE Billing and Reimbursement for Physician Offices, Ambulatory Surgery Centers and Hospitals
Billing & Reimbursement Revenue Cycle Management HOW TO PREVENT AND MANAGE MEDICAL CLAIM DENIALS TO INCREASE REVENUE Billing and Reimbursement for Physician Offices, Ambulatory Surgery Centers and Hospitals
Medicare Supplemental Insurance - Medigap Plans
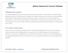 Medicare Supplemental Insurance (Medigap) All Medigap s A through N The available supplemental insurance plans that are offered are lettered plans A-N. Each plan offers a different benefits package and
Medicare Supplemental Insurance (Medigap) All Medigap s A through N The available supplemental insurance plans that are offered are lettered plans A-N. Each plan offers a different benefits package and
Common Medicare Billing Mistakes Systems and protocols necessary to help prevent and overpayment Best practices in resolving an overpayment
 Bill J. Ulrich, President / CEO Consolidated Billing Services Inc. Pat Newberry, Director of Clinical Education AIS Inc. Common Medicare Billing Mistakes Systems and protocols necessary to help prevent
Bill J. Ulrich, President / CEO Consolidated Billing Services Inc. Pat Newberry, Director of Clinical Education AIS Inc. Common Medicare Billing Mistakes Systems and protocols necessary to help prevent
PROTOCOLS FOR OCCUPATIONAL THERAPY PROVIDERS
 PROTOCOLS FOR OCCUPATIONAL THERAPY PROVIDERS Type of Services Provided Services provided by Occupational Therapy providers are covered for Santa Barbara Health Initiative (SBHI), San Luis Obispo Health
PROTOCOLS FOR OCCUPATIONAL THERAPY PROVIDERS Type of Services Provided Services provided by Occupational Therapy providers are covered for Santa Barbara Health Initiative (SBHI), San Luis Obispo Health
ICD-10-CM and ICD-10-PCS Frequently asked questions for HIM and Patient Financial Services Leaders
 ICD-10-CM and ICD-10-PCS Frequently asked questions for HIM and Patient Financial Services Leaders Executive questions What is the current status of ICD-10? The U.S. Department of Health and Human Services
ICD-10-CM and ICD-10-PCS Frequently asked questions for HIM and Patient Financial Services Leaders Executive questions What is the current status of ICD-10? The U.S. Department of Health and Human Services
Reimbursement Guide 2011
 Reimbursement Guide 2011 IMPORTANT SAFETY INFORMATION HYALGAN is indicated for the treatment of pain in osteoarthritis (OA) of the knee in patients who have failed to respond adequately to conservative
Reimbursement Guide 2011 IMPORTANT SAFETY INFORMATION HYALGAN is indicated for the treatment of pain in osteoarthritis (OA) of the knee in patients who have failed to respond adequately to conservative
Title: Coding Documentation for IHS Affiliated Physician Practices
 Affiliated Physician Practices Effective Date: 11/03; Rev. 4/06, 7/08, 7/10 POLICY: IHS affiliated physician practices will code diagnoses utilizing the International Classification of Diseases, Ninth
Affiliated Physician Practices Effective Date: 11/03; Rev. 4/06, 7/08, 7/10 POLICY: IHS affiliated physician practices will code diagnoses utilizing the International Classification of Diseases, Ninth
Comparison of the Prospective Payment System Methodologies Currently Utilized in the United States
 Comparison of the Prospective Payment System Methodologies Currently Utilized in the United States 1 Can you speak the jargon of Prospective Payment Systems? MS- DRGs APCs IPF-PPS RBRVS HHRGs RUGs MS-LTC
Comparison of the Prospective Payment System Methodologies Currently Utilized in the United States 1 Can you speak the jargon of Prospective Payment Systems? MS- DRGs APCs IPF-PPS RBRVS HHRGs RUGs MS-LTC
Reimbursement Questions and Answers for IBCLCs Judith L. Gutowski, BA, IBCLC, RLC Chair, USLCA Licensure and Reimbursement Committee June 2012
 Reimbursement Questions and Answers for IBCLCs Judith L. Gutowski, BA, IBCLC, RLC Chair, USLCA Licensure and Reimbursement Committee June 2012 The USLCA often receives inquiries about insurance and Medicaid
Reimbursement Questions and Answers for IBCLCs Judith L. Gutowski, BA, IBCLC, RLC Chair, USLCA Licensure and Reimbursement Committee June 2012 The USLCA often receives inquiries about insurance and Medicaid
REIMBURSEMENT POLICY CMS-1500 Physical Medicine & Rehabilitation: Multiple Therapy Procedure Reduction Policy 2/13/2013
 Policy Number REIMBURSEMENT POLICY CMS-1500 Physical Medicine & Rehabilitation: Multiple Therapy Procedure Reduction Policy 2013R0121C Annual Approval Date 2/13/2013 Approved By National Reimbursement
Policy Number REIMBURSEMENT POLICY CMS-1500 Physical Medicine & Rehabilitation: Multiple Therapy Procedure Reduction Policy 2013R0121C Annual Approval Date 2/13/2013 Approved By National Reimbursement
Molina Healthcare of Puerto Rico (MHPR) Non-Participating Provider Information
 Molina Healthcare of Puerto Rico (MHPR) Non-Participating Provider Information Please refer to Carta Normativa 15-0326 Re Transicion for details regarding the ASES-established Transition of Care and Reimbursement
Molina Healthcare of Puerto Rico (MHPR) Non-Participating Provider Information Please refer to Carta Normativa 15-0326 Re Transicion for details regarding the ASES-established Transition of Care and Reimbursement
List of Insurance Terms and Definitions for Uniform Translation
 Term actuarial value Affordable Care Act allowed charge Definition The percentage of total average costs for covered benefits that a plan will cover. For example, if a plan has an actuarial value of 70%,
Term actuarial value Affordable Care Act allowed charge Definition The percentage of total average costs for covered benefits that a plan will cover. For example, if a plan has an actuarial value of 70%,
on the status of a claim previously submitted to CMS for processing. A code that identifies the category a claim falls within.
 270 Health Care Eligibility Benefit Inquiry 271 Health Care Eligibility Benefit Response 276 Health Care Claims Status Request 277 Health Care Claims Status Response 278 Health Care Services Request for
270 Health Care Eligibility Benefit Inquiry 271 Health Care Eligibility Benefit Response 276 Health Care Claims Status Request 277 Health Care Claims Status Response 278 Health Care Services Request for
Physician payment: present and future The devil of the details
 Physician payment: present and future The devil of the details John D. Goodson MD, FACP Massachusetts General Hospital Harvard Medical School The future of PC MD payments 2000 2005 2010 2015 2020 2025
Physician payment: present and future The devil of the details John D. Goodson MD, FACP Massachusetts General Hospital Harvard Medical School The future of PC MD payments 2000 2005 2010 2015 2020 2025
2006 Provider Coding/Billing Information. www.novoseven-us.com
 2006 Provider Coding/Billing Information 2 3 Contents About NovoSeven...2 Coverage...4 Coding...4 Reimbursement...8 Establishing Medical Necessity and Appealing Denied Claims...10 Claims Materials...12
2006 Provider Coding/Billing Information 2 3 Contents About NovoSeven...2 Coverage...4 Coding...4 Reimbursement...8 Establishing Medical Necessity and Appealing Denied Claims...10 Claims Materials...12
NOVOSTE BETA-CATH SYSTEM
 HOSPITAL INPATIENT AND OUTPATIENT BILLING GUIDE FOR THE NOVOSTE BETA-CATH SYSTEM INTRAVASCULAR BRACHYTHERAPY DEVICE This guide is intended solely for use as a tool to help hospital billing staff resolve
HOSPITAL INPATIENT AND OUTPATIENT BILLING GUIDE FOR THE NOVOSTE BETA-CATH SYSTEM INTRAVASCULAR BRACHYTHERAPY DEVICE This guide is intended solely for use as a tool to help hospital billing staff resolve
Payment Policy. Evaluation and Management
 Purpose Payment Policy Evaluation and Management The purpose of this payment policy is to define how Health New England (HNE) reimburses for Evaluation and Management Services. Applicable Plans Definitions
Purpose Payment Policy Evaluation and Management The purpose of this payment policy is to define how Health New England (HNE) reimburses for Evaluation and Management Services. Applicable Plans Definitions
Medical Assisting Review
 Fifth Edition Medical Assisting Review Passing the CMA, RMA, and CCMA Exams Chapter 14 Medical Insurance 14-2 Learning Outcomes 14.1 Define terminology used in association with medical insurance. 14.2
Fifth Edition Medical Assisting Review Passing the CMA, RMA, and CCMA Exams Chapter 14 Medical Insurance 14-2 Learning Outcomes 14.1 Define terminology used in association with medical insurance. 14.2
MEDICARE SUPPLEMENT OUTLINE OF BENEFIT COVERAGE
 Shaded Sections show Benefit Plans A, B, C, F, High Deductible F*, M and N which are available These charts show the benefits included in each of the standard Medicare Supplement plans. Every company must
Shaded Sections show Benefit Plans A, B, C, F, High Deductible F*, M and N which are available These charts show the benefits included in each of the standard Medicare Supplement plans. Every company must
Medicare 101 for the Clinician and RTS. Medicare - What Is It? Who is Eligible? 4/5/2011. Federally managed medical insurance plan.
 Medicare 101 for the Clinician and RTS Medtrade d Spring 2011 Presented by: Elizabeth Cole, MSPT Director of Clinical Rehab Services U.S. Rehab Medicare - What Is It? Federally managed medical insurance
Medicare 101 for the Clinician and RTS Medtrade d Spring 2011 Presented by: Elizabeth Cole, MSPT Director of Clinical Rehab Services U.S. Rehab Medicare - What Is It? Federally managed medical insurance
1. Long Term Care Facility
 Table of Contents 1.... 1 1.1. Introduction... 1 1.1.1. General Policy... 1 1.1.2. Advance Directives... 1 1.1.3. Customary Fees... 1 1.1.4. Covered Services... 1 1.1.5. Swing Bed General Policy... 2 1.2.
Table of Contents 1.... 1 1.1. Introduction... 1 1.1.1. General Policy... 1 1.1.2. Advance Directives... 1 1.1.3. Customary Fees... 1 1.1.4. Covered Services... 1 1.1.5. Swing Bed General Policy... 2 1.2.
Amendment No. 1 to HB0963. Sargent Signature of Sponsor. AMEND Senate Bill No. 937 House Bill No. 963*
 Pensions and Insurance 1 Amendment No. 1 to HB0963 Sargent Signature of Sponsor AMEND Senate Bill No. 937 House Bill No. 963* by deleting all language after the enacting clause and substituting instead
Pensions and Insurance 1 Amendment No. 1 to HB0963 Sargent Signature of Sponsor AMEND Senate Bill No. 937 House Bill No. 963* by deleting all language after the enacting clause and substituting instead
EPEC. Education for Physicians on End-of-life Care. Trainer s Guide
 EPEC Education for Physicians on End-of-life Care Trainer s Guide Procedure/Diagnosis Coding and Reimbursement Mechanisms for Physician Services in Palliative Care EPEC Project, The Robert Wood Johnson
EPEC Education for Physicians on End-of-life Care Trainer s Guide Procedure/Diagnosis Coding and Reimbursement Mechanisms for Physician Services in Palliative Care EPEC Project, The Robert Wood Johnson
HB 159 mandates that private insurance provides the following for individuals diagnosed with Autism spectrum Disorders:
 HB 159 mandates that private insurance provides the following for individuals diagnosed with Autism spectrum Disorders: "Applied behavior analysis" means the design, implementation, and evaluation of environmental
HB 159 mandates that private insurance provides the following for individuals diagnosed with Autism spectrum Disorders: "Applied behavior analysis" means the design, implementation, and evaluation of environmental
2010 Medicare Part B Consultation Coding Changes 1/26/2010 & 1/27/2010
 2010 Medicare Part B Consultation Coding Changes 1/26/2010 & 1/27/2010 Consultations The Centers for Medicare/Medicaid Services (CMS) finalized its proposal to require claims for consultation services
2010 Medicare Part B Consultation Coding Changes 1/26/2010 & 1/27/2010 Consultations The Centers for Medicare/Medicaid Services (CMS) finalized its proposal to require claims for consultation services
How Health Reform Will Help Children with Mental Health Needs
 How Health Reform Will Help Children with Mental Health Needs The new health care reform law, called the Affordable Care Act (or ACA), will give children who have mental health needs better access to the
How Health Reform Will Help Children with Mental Health Needs The new health care reform law, called the Affordable Care Act (or ACA), will give children who have mental health needs better access to the
PA PROMISe 837 Institutional/UB 04 Claim Form
 Table of Contents 2 1 Appendix H Bureau of Provider Support (BPS) Field Operations Review Process Contents: A. General Background B. Explanation of Forms and Terms used in the Field Operations Section
Table of Contents 2 1 Appendix H Bureau of Provider Support (BPS) Field Operations Review Process Contents: A. General Background B. Explanation of Forms and Terms used in the Field Operations Section
Medicare-Medicaid Crossover Claims FAQ
 Medicare-Medicaid Crossover Claims FAQ Table of Contents 1. Benefits of Crossover Claims... 1 2. General Information... 1 3. Medicare Part B Professional Claims and DMERC Claims... 2 4. Professional Miscellaneous...
Medicare-Medicaid Crossover Claims FAQ Table of Contents 1. Benefits of Crossover Claims... 1 2. General Information... 1 3. Medicare Part B Professional Claims and DMERC Claims... 2 4. Professional Miscellaneous...
IWCC 50 ILLINOIS ADMINISTRATIVE CODE 7110 7110.90. Section 7110.90 Illinois Workers' Compensation Commission Medical Fee Schedule
 Section 7110.90 Illinois Workers' Compensation Commission Medical Fee Schedule a) In accordance with Sections 8(a), 8.2 and 16 of the Workers' Compensation Act [820 ILCS 305/8(a), 8.2 and 16] (the Act),
Section 7110.90 Illinois Workers' Compensation Commission Medical Fee Schedule a) In accordance with Sections 8(a), 8.2 and 16 of the Workers' Compensation Act [820 ILCS 305/8(a), 8.2 and 16] (the Act),
Billing, Coding, & Calculating Fees: Finding Success
 Billing, Coding, & Calculating Fees: Finding Success Janet McCarty American Speech-Language-Hearing Association Today s Agenda BILLING: Learn how to bill for your services. CODING: Learn the codes that
Billing, Coding, & Calculating Fees: Finding Success Janet McCarty American Speech-Language-Hearing Association Today s Agenda BILLING: Learn how to bill for your services. CODING: Learn the codes that
Patient Resource Guide for Billing and Insurance Information
 Patient Resource Guide for Billing and Insurance Information 17 Patient Account Payment Policies July 2012 Update Lexington Clinic Central Business Office Payment Policies Customer service...2 Check-in...2
Patient Resource Guide for Billing and Insurance Information 17 Patient Account Payment Policies July 2012 Update Lexington Clinic Central Business Office Payment Policies Customer service...2 Check-in...2
UPDATED NOVEMBER 2015. Providing and Billing Medicare for Chronic Care Management
 UPDATED NOVEMBER 2015 Providing and Billing Medicare for Chronic Care Management Research studies have demonstrated time and again that care management reduces total costs of care for chronic disease patients
UPDATED NOVEMBER 2015 Providing and Billing Medicare for Chronic Care Management Research studies have demonstrated time and again that care management reduces total costs of care for chronic disease patients
CLAIMS Section 5. Overview. Clean Claim. Prompt Payment. Timely Claims Submission. Claim Submission Format
 Overview The Claims department partners with the Provider Relations, Health Services and Customer Service departments to assist providers with any claims-related questions. The focus of the Claims department
Overview The Claims department partners with the Provider Relations, Health Services and Customer Service departments to assist providers with any claims-related questions. The focus of the Claims department
Exhibit 4. Provider Network
 Exhibit 4 Provider Network Provider Contract Requirements ICS must develop, implement, and maintain a comprehensive provider network that assures access to primary and specialty health related care that
Exhibit 4 Provider Network Provider Contract Requirements ICS must develop, implement, and maintain a comprehensive provider network that assures access to primary and specialty health related care that
MEDICAL BILLING & CODING PROGRAM
 ELIM OUTREACH TRAINING CENTER 1820 Ridge Rd Suite 300-301 Homewood, IL 60430 Tel:708-922-9547-Fax: 708-922-9568 E-mail: elim1820@comcast.net Website: elimotc.com MEDICAL BILLING & CODING PROGRAM ELIM OUTREACH
ELIM OUTREACH TRAINING CENTER 1820 Ridge Rd Suite 300-301 Homewood, IL 60430 Tel:708-922-9547-Fax: 708-922-9568 E-mail: elim1820@comcast.net Website: elimotc.com MEDICAL BILLING & CODING PROGRAM ELIM OUTREACH
Ambulance Fees - Impact of the USAmbulance Fees
 Background CY 2012 Ambulance Fee Schedule Public Use Files The Ambulance Fee Schedule was implemented on April 1, 2002. The accompanying public use files reflect updates effective for ambulance claims
Background CY 2012 Ambulance Fee Schedule Public Use Files The Ambulance Fee Schedule was implemented on April 1, 2002. The accompanying public use files reflect updates effective for ambulance claims
