Emergency Neurological Life Support: Spinal Cord Compression (SCC)
|
|
|
- Brianna Bryant
- 10 years ago
- Views:
Transcription
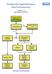
1 DOI /s REVIEW ARTICLE Emergency Neurological Life Support: Spinal Cord Compression (SCC) Kristine H. O Phelan E. Bradshaw Bunney Scott D. Weingart Wade S. Smith Ó Neurocritical Care Society 2012 Abstract Acute spinal cord compression (SCC) is the most serious of the diseases of the cord and should be accorded special attention in neurocritical care. Patients with SCC have a combination of motor and sensory dysfunction that has a distribution referable to one, or a few contiguous, spinal levels. Bowel and bladder dysfunction and neck or back pain are usually part of the clinical presentation but are not uniformly present. Because interventions are time-sensitive, the recognition and treatment of SCC was chosen as an ENLS protocol. Keywords Myelopathy Epidural infection Epidural abscess Paraplegia Quadriplegia Protocol The ENLS suggested algorithm for the initial management of SCC is shown in Fig. 1. Suggested items to complete within the first hour of evaluating a patient with SCC are shown in Table 1. K. H. O Phelan (&) Department of Neurology, University of Miami, Miller School of Medicine, Miami, FL, USA [email protected] E. B. Bunney Department of Emergency Medicine, University of Illinois at Chicago, Chicago, IL, USA S. D. Weingart ENLS Course Co-Chair, Division of ED Critical Care, Mount Sinai School of Medicine, New York, NY, USA W. S. Smith ENLS Course Co-Chair, Department of Neurology, University of California, San Francisco, CA, USA [email protected] Quadriplegia Quadriplegia represents the most serious presentation of SCC. In an alert and responsive patient, quadriplegia indicates a cervical lesion. Depending on the level of the cervical lesion, there may also be respiratory failure. Pulmonary function tests such as negative inspiratory force or vital capacity may be helpful in assessing this status (see the Acute Weakness protocol for indications on intubation). The patient s own assessment of his respiratory status by way of dyspnea is frequently accurate but becomes unreliable if the patient requires pain medication or sedation. When in doubt, the airway should be secured by intubation and assisted with ventilation, particularly if the clinical syndrome is rapidly progressing. The degree of recovery is often fixed at h after injury [1]. Therefore, if the history and physical exam narrow the possible etiology to infectious or metastatic processes, it is prudent to begin antibiotics or steroids if there will be a delay in establishing the cause of cord compression by imaging. If cervical instability is suspected on the basis of spondylolisthesis, traumatic ligamentous injury or multiple destructive bone lesions in one spinal segment, particularly in the posterior elements, the patient should be placed in a cervical collar until imaging can determine cervical stability. Emergent Transfer Advanced imaging as well as specialists in neurology, neurosurgery, radiation oncology, and infectious diseases may be needed to insure the best possible outcome for a patient with SCC [2]. Emergency departments and other
2 should be established for use of ground transportation when weather conditions will not allow flying. Whenever a delay in transfer or lengthy transport is anticipated, empirical therapy should be considered even if the diagnosis is not confirmed. Where an infectious cause is suspected, antibiotics should be started before transfer. If a metastatic lesion is suspected, steroids should be discussed with the accepting physician at the tertiary care facility and started if deemed appropriate. Imaging Not Available Some acute care facilities do not have magnetic resonance imaging (MRI) available continuously, or at all. In these cases, computed tomography (CT) may be helpful if a bony lesion is suspected. However, if a hematoma or neoplastic or infectious cause is suspected, CT may not provide adequate diagnostic information. Therefore, an acute care facility that does not have around-the-clock MRI availability should have an arrangement with a facility that does. Owing to the rapid progression of some acute SCC syndromes, these transfer agreements should be pre-established so as to avoid prolonged attempts to find a facility. Cancer Fig. 1 ENLS spinal cord compression protocol Table 1 Spinal cord compression checklist for the first hour Quadriplegia? Insure proper ventilation Attain emergent spine imaging (MRI unless contraindicated) Alert spine surgeon if indicated Labs: CBC, platelets, PT, PTT, creatinine Suspected metastatic disease, contact radiation oncology; administer steroids if spinal metastasis with SCC is confirmed Suspect epidural infection: ESR, start antibiotics acute care facilities should have arrangements with tertiary care facilities that can provide these resources rapidly. Distances between hospitals may be far enough to warrant transport via aircraft. In these cases, additional considerations such as landing areas for helicopters or ground transport to and from fixed wing aircrafts should be resolved well in advance and articulated in a pre-determined transportation plan. Finally, a contingency plan Patients with a known history of cancer and a high suspicion for metastatic disease to the spine with cord compression should be given high-dose corticosteroids during transfer to a center with MRI services (dosing is discussed below under the Acute Disk Herniation section). Infection Patients with evidence of infection such as fever, leukocytosis, intravenous (IV) drug use, or a known infectious source should be started on empiric antibiotics after blood cultures are drawn. Anti-microbial coverage should include Staphylococcus, Streptococcus, and methicillin resistant Staphylococcus aureus (MRSA). If there is a history of a recent neurosurgical procedure, coverage for gram negative organisms should be added. These empiric therapies may be coordinated with the accepting facility s physicians. Imaging Available Imaging of the spine is essential in identifying which compressive lesions may benefit from surgical treatment.
3 Magnetic resonance imaging (MRI) is the preferred technique because it demonstrates the surrounding supporting structures of the spinal column and the intrinsic aspects of the cord adjacent to the spinal lesion [3]. MRI can demonstrate abnormalities of the soft tissues around the spine and in the discrete regions (extradural, intradural extramedulary, and intramedulary) of the spinal canal itself. In addition, MRI allows the evaluation of long segments of the spine and spinal cord in a single examination. The inclusion of a contrast enhanced study may be required to identify infectious, inflammatory, and neoplastic lesions. Myelography and CT may be used to identify traumatic and compressive lesions in patients who are not eligible for MRI. The initial imaging studies should be oriented to begin at least two spinal segments above the level of the clinical deficit and continue down to the conus. Many patients will present with back pain without signs of a clear motor or sensory level or sphincter dysfunction [4 6]. For this reason, in patients with an active or recent cancer or a high suspicion of metastatic disease, the entire spine should be imaged. Neoplastic Disease In patients with metastatic SCC, motor function is the most important factor in determining outcome [4]. These lesions most frequently present in the thoracic spine (60 %) and less frequently in the lumbosacral (30 %) or cervical (10 %), reflecting the number of segments in each region and their blood supplies [5]. SCC can be the presenting symptom of cancer in 20 % of patients; in other words, an evident diagnosis of malignancy is not always present. Tumors of the lung, breast, and prostate, as well as lymphoma and renal cell cancer, are the most common neoplasms causing metastatic SCC. Metastatic disease occurs most often by hematogenous spread to the marrow of the vertebral bodies. There is contiguous spread from paraspinal tumors in less than 15 % of compressive metastatic lesions; this occurs particularly with Pancoast tumors and lymphomas. Compression of venous structures may also contribute to vasogenic edema and spinal cord infarcts [7]. Primary spinal cord tumors such as multiple myeloma, chordoma, chondrosarcoma, Ewing s sarcoma, and osteogenic sarcoma have also been associated with SCC though they represent only 10 % of cases of extradural SCC. Meningiomas and nerve sheath tumors are the most common intradural extramedullary lesions causing compressive symptoms, and ependymoma and astrocytomas are the most common intramedullary tumors. Intramedullary spinal cord metastases can occur from primary lung neoplasm and breast cancer and rarely from lymphoma. Patients with intramedulary tumors can present with variants of a hemicord syndrome, which typically includes ipsilateral hemiplegia, loss of vibratory sense, and fine touch with contralateral loss of pain and temperature sensation [8]. Multiple cranial or spinal nerve dysfunction and signs of meningeal irritation suggest leptomeningeal metastases. This occurs in up to 8 % of cancer patients, and prognosis is poor [9]. Symptoms may include motor or sensory deficits in several non-contiguous sites in the central nervous system. Bowel and bladder involvement is less common. These patients often have abnormal spinal fluid studies that show an elevated protein level and pleocytosis with hypoglycorrhachia. Cerebral spinal fluid should also be sent for cytology in such cases. A combination of radiotherapy and surgical treatment is recommended for metastatic SCC [10]. In addition, patients with leptomeningeal metastasis can be treated with intrathecal chemotherapy. Chemotherapy for tumors of the spinal column may also be reasonable for those with tumors known to be chemosensitive such as lymphoma, breast cancer, and neuroblastoma [11, 12]. Surgery may be particular beneficial for patients with a single region of spinal compression or instability. Timely referral for surgical evaluation facilitates rapid alleviation of compressive neural damage and prevents further decline [13]. Though patients who are non-ambulatory at presentation have a shorter life expectancy, even those with significant disease at presentation may benefit from palliative surgical stabilization or radiation to mitigate symptoms [14, 15]. There are few useful studies, but some suggest that there is an advantage to surgical decompression within 24 h in patients who have lost the ability to walk or have rapidly declining ambulation. After that period, there may not be the same urgency, and the surgical efficacy has not been established. The overall prognosis for patients with metastatic SCC is poor: the one-year survival rate is 30 % [16]. However, older age is a prognostic factor and may favor radiation over surgery. Patients without a previous history of cancer should have a complete blood count, sedimentation rate or CRP, electrolytes, liver function tests, serum light chains, immunoglobulins and electropheresis, urinary Bence-Jones proteins, and a chest radiograph. CT scans of the chest, abdomen, and pelvis should be obtained, but should not delay treatment. Tumor markers are not specific enough to diagnose cancer but, if they are significantly elevated, may be used to suggest possible primary sites of malignancy [16]. Patients found at presentation to have compressive spinal lesions due to metastases and motor symptoms
4 should generally be treated with corticosteroids. While this therapy did not extend survival in several studies, it has consistently been associated with improvement in ambulation compared with placebo [17]. Whether there is an advantage to the massive doses in the range of 100 mg of dexamethasone used by some units is unknown. There is some evidence that high dose steroid regimens before radiation may have some clinical advantages, but this approach is also associated with a higher risk of complications including psychosis and gastric ulcers with hemorrhage [18]. Protein pump inhibitors are administered in parallel with corticosteroids. Management of patients includes urinary catheterization for patients with urinary retention, hydration and attention to nutritional status, and prevention of pressure ulcers and thromboembolism. Prophylaxis is given for venous thrombosis with heparin or fractionated heparin. Analgesia to control pain and bowel regimens to prevent constipation are also fundamental to improving quality of life for these patients [19]. Acute Spinal Hemorrhage Spinal hematomas can present with rapidly developing paraparesis or tetraparesis with local or radicular pain. The most common causes of non-traumatic spinal cord hematoma are vascular malformations, coagulopathy, inflammatory myelitis, spinal tumors, and syringomyelia [20, 22]. In rare cases, spinal hematoma can be a late complication after radiotherapy, presumably due to bleeding from telangiectasia caused by the radiotherapy [21]. MRI with and without gadolinium are used to evaluate the spinal hematoma, as it will demonstrate both the hematoma and any associated underlying pathology. Because this is relatively rare, the literature consists mainly of case reports and case series. There are little evidencebased data available to guide therapy, and most approaches are empiric. There is considerable variation among surgeons regarding the timing of surgical intervention. Some surgeons choose to evacuate the clot early to relieve compression, while others believe it is best to allow the neurologic symptoms to plateau before surgical intervention to prevent further damage to viable tissue. Regardless of timing, the underlying cause must be addressed, particularly correction of coagulopathy. Acute Disk Herniation Back pain that is localized or radicular is often associated with disk herniation. This symptom is occasionally accompanied by loss of sensory or motor function, which is usually referable to the radiculopathy. Acute non-traumatic myelopathy from a herniated disk is rare, but has been reported [22]. The pain is typically worse when standing or sitting and better in the recumbent position. This is distinct from the pain associated with epidural tumors, which is typically worse when the patient lies down. Acute myelopathy from disk herniations in the cervical and thoracic regions is caused by direct compression of the spinal cord as well as by compression of the blood supply to the cord. MRI will demonstrate the herniated disk as well as signal changes in the injured cord on T2 signal sequences. Patients with acute neurologic deficits from disk herniation should have evaluation for surgical treatment. There is currently no consensus regarding recommendations for the timing of decompression or type of surgery recommended, but most experts operate quickly after signs of cord compression have become evident. Steroids are often given to treat pain and inflammation in patients with disk herniations and radicular symptoms. In cases of severe acute deterioration in motor function with an upper motor neuron distribution, methylprednisolone may be given if started within the first 8 h. The prevailing dosage recommendation is 30 mg/kg IV bolus followed by 5.4 mg/kg/h by 23 h. However, this is a weak, level 2C recommendation based on evidence from the national acute spinal cord injury Study 2, a randomized controlled trial that has been criticized as flawed [23]. Infectious Lesion Suppurative infections of the spinal epidural space can cause injury to the spinal cord through direct compression and also by the involvement of the vascular supply to the spinal cord. Diagnosis is often delayed because the initial symptom may only be back pain. The classic triad of fever, back pain, and neurologic deficit is not seen in most patients [24]. Symptoms may include localized back pain, radiculopathy, weakness, sensory changes, and sphincter dysfunction. The mechanism of spread of bacteria is probably hematogenous; therefore, a history of IV drug use or an indwelling catheter is important. Direct spread of infection from vertebral osteomyelitis can occur. Most epidural abscesses occur in the posterior epidural space, which contains fat, small arteries, and the venous plexus. The anterior epidural space is more difficult to invade. Staphyloccocus aureus is the most commonly reported pathogen though many other bacteria such as gram negative
5 organisms and Mycobacterium tuberculosis can cause a subacute spinal epidural abscess [25]. It may be difficult to distinguish infections from leptomeningeal metastases, particularly in immunosuppressed patients or those with lymphoma who may be susceptible to both. Patients with infections tend to develop cranial nerve and spinal abnormalities later in the course of illness as compared with patients with leptomeningeal neoplasm. Plain radiographs of the spine that show abnormalities involving two vertebral bodies across a disk space indicate an infectious process as it is rare for metastatic tumor to cross the disk space. The work-up for suspected epidural abscess includes complete blood count (CBC), erythrocyte sedimentation rate (ESR), blood cultures, and preoperative lab studies. However, abnormalities of the CBC and ESR are nonspecific: two-thirds of patients have a leukocytosis, and some may have a highly elevated ESR [24]. Spinal fluid studies may show elevated protein and leukocyte levels, but may also be within normal ranges. However, an ESR of less than 20 has excellent sensitivity for excluding a diagnosis of spinal epidural abscess [24]. Treatment of epidural abscess includes both medical and surgical therapies. Surgical decompression and drainage of the abscess is often indicated, and a surgical evaluation should be requested. Antibiotic coverage should include anti-staphylococcal coverage, including coverage for methicillin-resistant Staphylococcus aureus. If there is a history of recent neurosurgical procedure, antibiotic coverage should be broadened to include gram negative organisms (third generation cephalosporin and aminoglycoside) until culture results can definitively guide therapy. The recommendation to delay antibiotics until cultures are obtained in patients who have a mechanically stable spine and a stable neurologic examination is controversial [26]. CT guided aspiration of the epidural space is occasionally used to obtain cultures in patients without neurologic deficits. Cultures should be sent for aerobic and anaerobic bacteria, fungi, and tuberculosis. However, cultures may remain negative in % of cases. Steroids may be used during the course of treatment if the infection involves the spinal cord itself (intramedulary) to reduce associated spinal cord edema. Dexamethasone is most frequently used in doses ranging from 4 10 mg every 6 h. Non-Compressive Acute Spinal Lesions Patients with acute and severe symptoms of spinal cord dysfunction may have spinal cord infarct; inflammatory, infectious, and parainfectious myelitis; or demyelinating diseases. The leading causes of this syndrome are infarctive Table 2 Spinal cord compression communication regarding assessment and referral Airway status Abnormal vital signs Onset and duration of symptoms Bowel or bladder involvement Clinical spinal level of pathology Results of any imaging Coexistence of cancer, systemic illness Which therapy has been started Inquire which further therapy to start now and are all uncommon; they are cartilaginous disk embolus, atherosclerotic disease of the aorta, and the ischemic effects of a dural arteriovenous fistula. These forms of spinal cord ischemia are difficult to diagnose and require further imaging with spinal angiography to identify arteriovenous malformation, and serum and cerebral spinal fluid (CSF) studies should usually be sent for diagnosis of infection and vasculitis. IgG index in CSF and serum as well as oligoclonal bands may be suggestive of an intrathecal infectious or inflammatory process (See the Acute Non-Traumatic Weakness protocol). Normal Imaging MRI that is unrevealing in a patient with acute disturbance of motor and or sensory function should prompt evaluation of the peripheral nerves and neuromuscular junction. Electrophysiologic studies may establish a diagnosis of acute demyelinating or axonal polyradiculopathy, myasthenia gravis, or Lambert Eaton syndrome or motorneuron disease (see the Acute Non-Traumatic Weakness protocol). Communication When communicating to an accepting or referring physician about this patient, consider including the key elements listed in Table 2. References 1. Wuermser LA, Ho CH, Chiodo AE, Priebe MM, Kirshblum SC, Scelza WM. Spinal cord injury medicine. 2. Acute care management of traumatic and nontraumatic injury. Arch Phys Med Rehabil. 2007;88:S Schmidt RD, Markovchick V. Nontraumatic spinal cord compression. J Emerg Med. 1992;10: Bammer R, Fazekas F. Diffusion imaging of the human spinal cord and the vertebral column. Top Magn Reson Imaging. 2003;14:
6 4. Husband DJ. Malignant spinal cord compression: prospective study of delays in referral and treatment. BMJ. 1998;317: Klimo P Jr, Thompson CJ, Kestle JR, Schmidt MH. A metaanalysis of surgery versus conventional radiotherapy for the treatment of metastatic spinal epidural disease. Neuro Oncol. 2005;7: Gilbert RW, Kim JH, Posner JB. Epidural spinal cord compression from metastatic tumor: diagnosis and treatment. Ann Neurol. 1978;3: Bach F, Larsen BH, Rohde K, et al. Metastatic spinal cord compression. Occurrence, symptoms, clinical presentations and prognosis in 398 patients with spinal cord compression. Acta Neurochir (Wien). 1990;107: Schiff D, O Neill BP. Intramedullary spinal cord metastases: clinical features and treatment outcome. Neurology. 1996;47: Mut M, Schiff D, Shaffrey ME. Metastasis to nervous system: spinal epidural and intramedullary metastases. J Neurooncol. 2005;75: Sundaresan N, Sachdev VP, Holland JF, et al. Surgical treatment of spinal cord compression from epidural metastasis. J Clin Oncol. 1995;13: Burch PA, Grossman SA. Treatment of epidural cord compressions from Hodgkin s disease with chemotherapy. A report of two cases and a review of the literature. Am J Med. 1988;84: Boogerd W, van der Sande JJ, Kroger R, Bruning PF, Somers R. Effective systemic therapy for spinal epidural metastases from breast carcinoma. Eur J Cancer Clin Oncol. 1989;25: Chen YJ, Chang GC, Chen HT, et al. Surgical results of metastatic spinal cord compression secondary to non-small cell lung cancer. Spine (Phila Pa 1976). 2007;32:E Patchell RA, Tibbs PA, Regine WF, et al. Direct decompressive surgical resection in the treatment of spinal cord compression caused by metastatic cancer: a randomised trial. Lancet. 2005; 366: Mannion RJ, Wilby M, Godward S, Lyratzopoulos G, Laing RJ. The surgical management of metastatic spinal disease: prospective assessment and long-term follow-up. Br J Neurosurg. 2007;21: Walji N, Chan AK, Peake DR. Common acute oncological emergencies: diagnosis, investigation and management. Postgrad Med J. 2008;84: Delattre JY, Arbit E, Rosenblum MK, et al. High dose versus low dose dexamethasone in experimental epidural spinal cord compression. Neurosurgery. 1988;22: Sorensen S, Helweg-Larsen S, Mouridsen H, Hansen HH. Effect of high-dose dexamethasone in carcinomatous metastatic spinal cord compression treated with radiotherapy: a randomised trial. Eur J Cancer. 1994;30A: Loblaw DA, Perry J, Chambers A, Laperriere NJ. Systematic review of the diagnosis and management of malignant extradural spinal cord compression: the cancer care ontario practice guidelines initiative s neuro-oncology disease site group. J Clin Oncol. 2005;23: Rodesch G, Hurth M, Alvarez H, Tadie M, Lasjaunias P. Spinal cord intradural arteriovenous fistulae: anatomic, clinical, and therapeutic considerations in a series of 32 consecutive patients seen between 1981 and 2000 with emphasis on endovascular therapy. Neurosurgery. 2005;57:973 83; discussion Allen JC, Miller DC, Budzilovich GN, Epstein FJ. Brain and spinal cord hemorrhage in long-term survivors of malignant pediatric brain tumors: a possible late effect of therapy. Neurology. 1991;41: Suzuki T, Abe E, Murai H, Kobayashi T. Nontraumatic acute complete paraplegia resulting from cervical disc herniation: a case report. Spine. 2003;28:E Bracken MB, Holford TR. Effects of timing of methylprednisolone or naloxone administration on recovery of segmental and long-tract neurological function in NASCIS 2. J Neurosurg. 1993;79: Mehta SH, Shih R. Cervical epidural abscess associated with massively elevated erythrocyte sedimentation rate. J Emerg Med. 2004;26: Joshi SM, Hatfield RH, Martin J, Taylor W. Spinal epidural abscess: a diagnostic challenge. Br J Neurosurg. 2003;17: Pradilla G, Ardila GP, Hsu W, Rigamonti D. Epidural abscesses of the CNS. Lancet Neurol. 2009;8:
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Emergency Neurological Life Support. Spinal Cord Compression. Version: 1.0 Last Updated: 8/3/2014. Checklist & Communication
 Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
MALIGNANT SPINAL CORD COMPRESSION. Kate Hamilton Head of Medical Oncology Ballarat Health Services
 MALIGNANT SPINAL CORD COMPRESSION Kate Hamilton Head of Medical Oncology Ballarat Health Services OVERVIEW Background Epidemiology Pathophysiology Diagnosis Investigation Differential Diagnosis Management
MALIGNANT SPINAL CORD COMPRESSION Kate Hamilton Head of Medical Oncology Ballarat Health Services OVERVIEW Background Epidemiology Pathophysiology Diagnosis Investigation Differential Diagnosis Management
Advanced Practice Provider Academy
 (+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
(+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
.org. Metastatic Bone Disease. Description
 Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Hospice Palliative Care Program Symptom Guidelines. Spinal Cord Compression
 Hospice Palliative Care Program Symptom Guidelines Spinal Cord Compression Spinal Cord Compression Rationale This guideline is adapted for inter-professional primary care providers working in various
Hospice Palliative Care Program Symptom Guidelines Spinal Cord Compression Spinal Cord Compression Rationale This guideline is adapted for inter-professional primary care providers working in various
Brown-Sequard Syndrome Caused by Cervical Disc Herniation
 62 CASE REPORT Brown-Sequard Syndrome Caused by Cervical Disc Herniation Chih-Hsiu Wang, Chun-Chung Chen, Der-Yang Cho Department of Neurosurgery, China Medical University Hospital, Taichung, Taiwan, R.O.C.
62 CASE REPORT Brown-Sequard Syndrome Caused by Cervical Disc Herniation Chih-Hsiu Wang, Chun-Chung Chen, Der-Yang Cho Department of Neurosurgery, China Medical University Hospital, Taichung, Taiwan, R.O.C.
Radiotherapy in locally advanced & metastatic NSC lung cancer
 Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
4.2 Spinal Cord Compression
 4.2 Spinal Cord Compression AO Protocol Name: Metastatic Spinal Cord Compression (MSCC) AO Type: Type I (New Cancer), Type III (Cancer Complication) Author: ST Introduction: MSCC can cause irreversible
4.2 Spinal Cord Compression AO Protocol Name: Metastatic Spinal Cord Compression (MSCC) AO Type: Type I (New Cancer), Type III (Cancer Complication) Author: ST Introduction: MSCC can cause irreversible
Clinical Guideline. Low Back Pain Orthopaedics. Princess Alexandra Hospital Emergency Department. 1 Purpose. 2 Background
 Princess Alexandra Hospital Emergency Department Clinical Guideline Orthopaedics Review Officer: Katherine Isoardi Version no: 1 Approval date: 18/03/2015 Review date: 18/03/2017 Approving Officer Dr James
Princess Alexandra Hospital Emergency Department Clinical Guideline Orthopaedics Review Officer: Katherine Isoardi Version no: 1 Approval date: 18/03/2015 Review date: 18/03/2017 Approving Officer Dr James
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease)
 Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease) 2 Introduction Kummel's disease is a collapse of the vertebrae (the bones that make up the spine). It is also called vertebral osteonecrosis.
Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease) 2 Introduction Kummel's disease is a collapse of the vertebrae (the bones that make up the spine). It is also called vertebral osteonecrosis.
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
The Lewin Group undertook the following steps to identify the guidelines relevant to the 11 targeted procedures:
 Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Spinal Cord Diseases in Bernese Mountain Dogs
 Spinal Cord Diseases in Bernese Mountain Dogs 0 A N O V E R V I E W F O R BERNER O W N E R S O R G A N I Z E D B Y N A N C Y M E L O N E, P H. D. Based on materials obtained from the Berner Garde Foundation
Spinal Cord Diseases in Bernese Mountain Dogs 0 A N O V E R V I E W F O R BERNER O W N E R S O R G A N I Z E D B Y N A N C Y M E L O N E, P H. D. Based on materials obtained from the Berner Garde Foundation
2011 Radiology Diagnosis Coding Update Questions and Answers
 2011 Radiology Diagnosis Coding Update Questions and Answers How can we subscribe to the Coding Clinic for ICD-9 guidelines and updates? The American Hospital Association publishes this quarterly newsletter.
2011 Radiology Diagnosis Coding Update Questions and Answers How can we subscribe to the Coding Clinic for ICD-9 guidelines and updates? The American Hospital Association publishes this quarterly newsletter.
CT scans and IV contrast (radiographic iodinated contrast) utilization in adults
 CT scans and IV contrast (radiographic iodinated contrast) utilization in adults At United Radiology Group, a majority of CT exams are performed either with IV contrast or without while just a few exams
CT scans and IV contrast (radiographic iodinated contrast) utilization in adults At United Radiology Group, a majority of CT exams are performed either with IV contrast or without while just a few exams
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Stage I, II Non Small Cell Lung Cancer
 Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
ICD-9-CM coding for patients with Spinal Cord Injury*
 ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Nonsurgical treatment of an upper thoracic spinal subdural hemorrhage
 (2001) 39, 657 ± 661 ã 2001 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/01 $15.00 www.nature.com/sc Case Report Nonsurgical treatment of an upper thoracic spinal subdural
(2001) 39, 657 ± 661 ã 2001 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/01 $15.00 www.nature.com/sc Case Report Nonsurgical treatment of an upper thoracic spinal subdural
University College Hospital. Metastatic spinal cord compression (MSCC) information for patients at risk of developing MSCC.
 University College Hospital Metastatic spinal cord compression (MSCC) information for patients at risk of developing MSCC Cancer Services 2 If you would like this document in another language or format,
University College Hospital Metastatic spinal cord compression (MSCC) information for patients at risk of developing MSCC Cancer Services 2 If you would like this document in another language or format,
The Brain and Spine CenTer
 The Br ain and Spine Center Choosing the right treatment partner is important for patients facing tumors involving the brain, spine or skull base. The Brain and Spine Center at The University of Texas
The Br ain and Spine Center Choosing the right treatment partner is important for patients facing tumors involving the brain, spine or skull base. The Brain and Spine Center at The University of Texas
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Thymus Cancer. This reference summary will help you better understand what thymus cancer is and what treatment options are available.
 Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain. Seth Cheatham, MD
 Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 [email protected]
 Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 [email protected] CURRENT PRACTICE September 2009-present University of Miami School of Medicine Assistant Professor, Department of
Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 [email protected] CURRENT PRACTICE September 2009-present University of Miami School of Medicine Assistant Professor, Department of
Hepatocellular Carcinoma (HCC)
 Abhishek Vadalia Introduction Chemoembolization is being used with increasing frequency in the treatment of solid hepatic tumors such as Hepatocellular Carinoma (HCC) & rare Cholangiocellular Carcinoma
Abhishek Vadalia Introduction Chemoembolization is being used with increasing frequency in the treatment of solid hepatic tumors such as Hepatocellular Carinoma (HCC) & rare Cholangiocellular Carcinoma
The Spine Center at Beth Israel Deaconess
 Spinal Pain The Spine Center at Beth Israel Deaconess Medical Center developed the following detailed eplanation of our care pathways for primary care providers to help support your interactions with patients
Spinal Pain The Spine Center at Beth Israel Deaconess Medical Center developed the following detailed eplanation of our care pathways for primary care providers to help support your interactions with patients
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. CP57 Version: V3
 GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: CP57 Version: V3 Dr V. Misra Accountable Committee: Acute Oncology Group Network
GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: CP57 Version: V3 Dr V. Misra Accountable Committee: Acute Oncology Group Network
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
OHTAC Recommendation
 OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
III./8.4.2: Spinal trauma. III./8.4.2.1 Injury of the spinal cord
 III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
Khaled s Radiology report
 Khaled s Radiology report Patient Name: Khaled Adli Moustafa Date 06/15/2014 The patient is not present. And the following report is based upon what was in the MRI of the cervical and lumbar spine report
Khaled s Radiology report Patient Name: Khaled Adli Moustafa Date 06/15/2014 The patient is not present. And the following report is based upon what was in the MRI of the cervical and lumbar spine report
Radiologic Diagnosis of Spinal Metastases
 September 2002 Radiologic Diagnosis of Spinal Metastases Natalie J. M. Dailey, Harvard Medical Student Year III Our Patient s Presenting Story 70 year old male Presents to the hospital for laparascopic
September 2002 Radiologic Diagnosis of Spinal Metastases Natalie J. M. Dailey, Harvard Medical Student Year III Our Patient s Presenting Story 70 year old male Presents to the hospital for laparascopic
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Standard of Care: Cervical Radiculopathy
 Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Brain Cancer. This reference summary will help you understand how brain tumors are diagnosed and what options are available to treat them.
 Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
CHAPTER 2. Neoplasms (C00-D49) March 2014. 2014 MVP Health Care, Inc.
 Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Smoking and misuse of certain pain medicines can affect the risk of developing renal cell cancer.
 Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
LOW BACK PAIN; MECHANICAL
 1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862
 Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
Low Back Pain Protocols
 Low Back Pain Protocols Introduction: Diagnostic Triage And 1. Patient Group Adults aged 18 years and over with routine low back problems. Patients who have had recent surgery should be referred directly
Low Back Pain Protocols Introduction: Diagnostic Triage And 1. Patient Group Adults aged 18 years and over with routine low back problems. Patients who have had recent surgery should be referred directly
PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION
 PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION This booklet was designed to help you and the important people in your life understand the treatment of high dose chemotherapy with stem cell support: a procedure
PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION This booklet was designed to help you and the important people in your life understand the treatment of high dose chemotherapy with stem cell support: a procedure
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Evaluation of an Algorithmic Approach to Pediatric Back Pain
 ORIGINAL ARTICLE Evaluation of an Algorithmic Approach to Pediatric Back Pain David S. Feldman, MD, Joseph J. Straight, MD, Mohammad I. Badra, MD, Ahamed Mohaideen, MD, and Sanjeev S. Madan, MD Abstract:
ORIGINAL ARTICLE Evaluation of an Algorithmic Approach to Pediatric Back Pain David S. Feldman, MD, Joseph J. Straight, MD, Mohammad I. Badra, MD, Ahamed Mohaideen, MD, and Sanjeev S. Madan, MD Abstract:
BACK PAIN PATHWAY DEFINTIONS
 BACK PAIN PATHWAY DEFINTIONS Cauda Equina Syndrome (CES) Current or imminent compression of the sacral nerve roots resulting in neurogenic bladder and bowel dysfunction. Symptoms typically include: severe
BACK PAIN PATHWAY DEFINTIONS Cauda Equina Syndrome (CES) Current or imminent compression of the sacral nerve roots resulting in neurogenic bladder and bowel dysfunction. Symptoms typically include: severe
Musculoskeletal: Acute Lower Back Pain
 Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Disorders of the Spine & Peripheral Nerves
 Disorders of the Spine & Peripheral Nerves An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Spine Disorders & Neurosurgery Neurosurgery
Disorders of the Spine & Peripheral Nerves An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Spine Disorders & Neurosurgery Neurosurgery
Selective Nerve Root Block
 Selective Nerve Root Block What is a selective nerve root block? Selective nerve root blocks is similar to epidural injections, as the preparation and approach is identical. Epidural refers to the space
Selective Nerve Root Block What is a selective nerve root block? Selective nerve root blocks is similar to epidural injections, as the preparation and approach is identical. Epidural refers to the space
Spine Injury and Back Pain in Sports
 Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Test Request Tip Sheet
 With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
Weakness More diffuse More focal Atrophy Mild, general Severe, focal Atrophy versus weakness
 Spinal Cord Disorders (Dr. Merchut) Clinical signs and symptoms in spinal cord lesions 1. Motor signs and symptoms Lower motor neuron (LMN) signs (Table 1) are found in a limb if some of its muscles are
Spinal Cord Disorders (Dr. Merchut) Clinical signs and symptoms in spinal cord lesions 1. Motor signs and symptoms Lower motor neuron (LMN) signs (Table 1) are found in a limb if some of its muscles are
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation
 UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation Goals of the Program To acquire the knowledge and skills necessary to assess and provide a management plan for
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the Neurology Rotation Goals of the Program To acquire the knowledge and skills necessary to assess and provide a management plan for
Things You Don t Want to Miss in Multiple Myeloma
 Things You Don t Want to Miss in Multiple Myeloma Sreenivasa Chandana, MD, PhD Attending Hematologist and Medical Oncologist West Michigan Cancer Center Assistant Professor, Western Michigan University
Things You Don t Want to Miss in Multiple Myeloma Sreenivasa Chandana, MD, PhD Attending Hematologist and Medical Oncologist West Michigan Cancer Center Assistant Professor, Western Michigan University
Neurosarcoidosis. Jeffrey M. Gelfand, MD
 Neurosarcoidosis WASOG Meeting Cleveland October 2012 Patient Education Session Relevant Financial Disclosures: None Jeffrey M. Gelfand, MD Assistant Professor of Clinical Neurology UCSF MS Center, Dept
Neurosarcoidosis WASOG Meeting Cleveland October 2012 Patient Education Session Relevant Financial Disclosures: None Jeffrey M. Gelfand, MD Assistant Professor of Clinical Neurology UCSF MS Center, Dept
MULTIPLE MYELOMA Review & Update for Primary Care. Dr. Joseph Mignone 21st Century Oncology
 MULTIPLE MYELOMA Review & Update for Primary Care Dr. Joseph Mignone 21st Century Oncology OVERVIEW Identify the diagnostic criteria for multiple myeloma Compare first & second line therapies, using data
MULTIPLE MYELOMA Review & Update for Primary Care Dr. Joseph Mignone 21st Century Oncology OVERVIEW Identify the diagnostic criteria for multiple myeloma Compare first & second line therapies, using data
REFERRAL GUIDELINES: NEUROSURGERY
 Outpatient Referral Guidelines Page 1 1 REFERRAL GUIDELINES: NEUROSURGERY Essential Referral Content Date of birth Demographic Contact details (including mobile phone) Referring GP details Interpreter
Outpatient Referral Guidelines Page 1 1 REFERRAL GUIDELINES: NEUROSURGERY Essential Referral Content Date of birth Demographic Contact details (including mobile phone) Referring GP details Interpreter
Cervical Spine Radiculopathy: Convervative Treatment. Christos K. Yiannakopoulos, MD Orthopaedic Surgeon
 Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Reversibility of Acute Demyelinating Lesions in relapsingremitting
 Reversibility of Acute Demyelinating Lesions in relapsingremitting Multiple Sclerosis Omar A. Khan ( Division of Neuroimmunology, Department of Neurology, Neurology and Research Services. Veterans Affairs
Reversibility of Acute Demyelinating Lesions in relapsingremitting Multiple Sclerosis Omar A. Khan ( Division of Neuroimmunology, Department of Neurology, Neurology and Research Services. Veterans Affairs
Spinal Cord Injury Education. An Overview for Patients, Families, and Caregivers
 Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Headache: Differential diagnosis and Evaluation. Raymond Rios PGY-1 Pediatrics
 Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
SPINAL INFECTIONS. Anatomical Classification. Pathophysiology. Spine Infections. Microbiology. Sharad Rajpal, MD
 Anatomical Classification SPINAL INFECTIONS Sharad Rajpal, MD Vertebral column Intervertebral disc space Pyogenic vertebral osteomyelitis Spontaneous adult discitis Non pyogenic vertebral osteomyelitis
Anatomical Classification SPINAL INFECTIONS Sharad Rajpal, MD Vertebral column Intervertebral disc space Pyogenic vertebral osteomyelitis Spontaneous adult discitis Non pyogenic vertebral osteomyelitis
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
