Evaluation of an Algorithmic Approach to Pediatric Back Pain
|
|
|
- Bruno Allison
- 8 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Evaluation of an Algorithmic Approach to Pediatric Back Pain David S. Feldman, MD, Joseph J. Straight, MD, Mohammad I. Badra, MD, Ahamed Mohaideen, MD, and Sanjeev S. Madan, MD Abstract: Pediatric patients require a systematic approach to treating back pain that minimizes the number of diagnostic studies without missing specific diagnoses. This study reviews an algorithm for the evaluation of pediatric back pain and assesses critical factors in the history and physical examination that are predictive of specific diagnoses. Eighty-seven pediatric patients with thoracic and/or lumbar back pain were treated utilizing this algorithm. If initial plain radiographs were positive, patients were considered to have a specific diagnosis. If negative, patients with constant pain, night pain, radicular pain, and/or an abnormal neurological examination obtained a follow-up magnetic resonance imaging. Patients with negative radiographs and intermittent pain were diagnosed with nonspecific back pain. Twenty-one (24%) of 87 patients had positive radiographs and were treated for their specific diagnoses. Nineteen (29%) of 66 patients with negative radiographs had constant pain, night pain, radicular pain, and/or an abnormal neurological examination. Ten of these 19 patients had a specific diagnosis determined by magnetic resonance imaging. Therefore, 31 (36%) of 87 patients had a specific diagnosis. Back pain of other 56 patients was of a nonspecific nature. No specific diagnoses were missed at latest follow-up. Specificity for determining a specific diagnosis was very high for radicular pain (100%), abnormal neurological examination (100%), and night pain (95%). Radicular pain and an abnormal neurological examination also had high positive predictive value (100%). Lumbar pain was the most sensitive (67%) and had the highest negative predictive value (75%). This algorithm seems to be an effective tool for diagnosing pediatric back pain, and this should help to reduce costs and patient/family anxiety and to avoid unnecessary radiation exposure. Key Words: pediatric patients, back pain, radiographs, algorithm (J Pediatr Orthop 2006;26:353Y357) Back pain has traditionally been considered an uncommon complaint among children and adolescents. 1 However, the recent literature has shown that the incidence of back pain in From the Division of Pediatric Orthopaedic Surgery, New York University Hospital for Joint Diseases, New York, NY. Study conducted at the Center for Children, NYU Hospital for Joint Diseases, New York, NY. None of the authors received financial support for this study. Reprints: David S. Feldman, MD, Chief, Pediatric Orthopaedic Surgery, Center for Children, NYU Hospital for Joint Diseases, New York, NY ( david.feldman@med.nyu.edu). Copyright * 2006 by Lippincott Williams & Wilkins these age groups occurs more frequently than previously reported. 2Y4 Clinically, it is common for a child to have symptoms of back pain that are severe enough to warrant a medical consultation. A complaint of back pain in a child, unlike in an adult, has been considered a serious issue, and every effort has been made to determine its cause. 5,6 Physicians have been inclined to use every available test to reach a diagnosis. Undoubtedly, there are cases of back pain in children that are caused by serious diseases, but it is also well recognized that there are many cases associated with less serious conditions. Physicians need to be able to distinguish between benign and pathological causes of back pain. No single sign, symptom, or test reliably differentiates between these 2 groups. In the evaluation of back pain, physicians should follow a systematic approach using the minimum number of diagnostic studies, which would have the benefit of reducing radiation exposure, cost, and patient/family anxiety. An algorithm to assist physicians in the assessment of pediatric back pain was developed by the senior author (DSF). The purpose of this study was to demonstrate the ability of an algorithm to detect specific major spinal pathology, such as tumor or infection, in pediatric patients presenting with a chief complaint of back pain. MATERIALS AND METHODS From January 1995 to January 2002, 95 consecutive children (44 boys, 51 girls) with an average age of 13.4 years (range, 4Y18 years) presented with a chief complaint of thoracic and/or lumbar back pain. Patients who were referred for scoliosis evaluation or had a history of trauma (fall, motor vehicle injury) within 3 weeks of his or her initial visit were excluded. Institutional Review Board approval was obtained before the study. Upon the patient_s initial presentation, the senior author followed an algorithm (Fig. 1) which included a detailed history, a thorough physical examination, blood tests [complete blood count (CBC)], and plain radiographs. CBC was recommended in patients younger than 10 years because of the association of back pain and leukemia in young children. If the radiographs were positive and adequately corresponded to the patient`s history and examination, treatment was based on the specific diagnosis. If the radiographs were negative and the patient reported constant pain, night pain, radicular pain, and/or demonstrated an abnormal neurological examination, a magnetic resonance imaging () was obtained. Constant pain was defined as pain present at all times, night pain was pain that awoke a J Pediatr Orthop & Volume 26, Number 3, May/June
2 Feldman et al J Pediatr Orthop & Volume 26, Number 3, May/June 2006 BACK PAIN HISTORY, PHYSICAL EXAM, BLOOD TESTS NEGATIVE X-RAYS POSITIVE X-RAYS INTERMITTENT PAIN ONLY CONSTANT, NIGHT, OR RADICULAR PAIN, and/or ABNORMAL NEUROLOGIC EXAM NONSPECIFIC BACK PAIN NEGATIVE POSITIVE SPECIFIC DIAGNOSIS TREAT WITH REST, PT, and/or NSAID TREAT AS DIAGNOSED FIGURE 1. Pediatric back pain algorithm. patient from sleep, and radicular pain was pain distributed in a radicular pattern. Patients who had negative radiographs and only reported intermittent pain were diagnosed with nonspecific back pain and treated with rest, physical therapy, and/or nonsteroidal anti-inflammatory medications. If a patient with negative radiographs was found to have a positive finding on, he/she was treated for that specific diagnosis. Specific diagnoses included spondylolisthesis, spondylolysis, scoliosis, herniated nucleus pulposus, and tumors. Those who had both negative radiographs and a negative were treated for nonspecific back pain. Nonspecific diagnoses included strains, sprains, and overuse syndrome. A chart review was performed, and the following data were recorded: sex, age, frequency (constant or intermittent) and location of pain (thoracic, thoracolumbar, or lumbar), presence of radicular or night pain, neurological examination (normal or abnormal), presence of scoliosis, results of all radiological studies, and diagnosis. Patients who were diagnosed with nonspecific back pain or who did not have a follow-up visit were interviewed by telephone to determine if they had developed any new signs or symptoms that suggest a change in their diagnosis. After all the data were collected, each patient was placed into the treatment algorithm. The efficacy of the algorithm was assessed by examining the ability of certain signs, symptoms, and tests to predict the presence of a specific diagnosis and by determining if any specific diagnoses such as tumors, infection, or other significant pathology were missed. 354 Statistical Analysis The sensitivity, specificity, positive predictive value, and negative predictive value of the signs and symptoms (constant pain, night pain, radicular pain, thoracic pain, thoracolumbar pain, lumbar pain, abnormal neurological examination, and scoliosis) of adolescent back pain were analyzed to determine the ability of each of these variables to detect the presence of a specific diagnosis. Using constant pain, night pain, radicular pain, and abnormal neurological examination as predictors, the predicted probability of having a specific diagnosis on the basis of the number of these variables present was calculated. The frequencies of the following were determined: (1) patients with specific diagnoses, (2) specific diagnoses made by radiograph, (3) specific diagnoses in patients with a negative radiograph, (4) specific diagnoses in patients with a negative radiograph and who had a follow-up, and (5) patients in which a specific diagnosis was missed. RESULTS Eighty-seven of the 95 patients with thoracic and/or lumbar back pain were treated utilizing this algorithm (Fig. 1). Five patients who were not available for follow-up, 2 who failed to obtain an, and 1 who had and computed tomography (CT) scan done previously were excluded. Follow-up data were obtained at an average of 3.3 years (range, 2Y8 years) after initial visit. * 2006 Lippincott Williams & Wilkins
3 J Pediatr Orthop & Volume 26, Number 3, May/June 2006 An Algorithmic Approach to Pediatric Back Pain Twenty-one patients had initial radiographs that were positive for a specific diagnosis, including spondylolisthesis, scoliosis, and tumors. Of these 21 patients, 8 had follow-up confirming the diagnosis. Three of these 8 patients who had additionally had CT scans. All 21 patients were treated for their specific diagnosis. Sixty-six patients had negative findings on initial radiographs. Nineteen (29%) of the 66 patients reported having constant pain, night pain, radicular pain, and/or demonstrated an abnormality on neurological examination. Utilizing the algorithm, these 19 patients obtained an. Ten (53%) of the 19 patients had findings that were positive for a specific diagnosis, including spondylolysis, herniated nucleus pulposus, and osteoid osteoma. Five of the 10 patients also had CT scans that confirmed the diagnosis and aided in treatment decision making. The other 9 patients, who had negative, did not undergo further diagnostic testing and were given the diagnosis of nonspecific back pain. These patients were contacted and reported that their symptoms had not changed. The remaining 47 patients with negative radiographs only had intermittent pain and were diagnosed with nonspecific back pain. These patients were contacted and reported no change in their symptoms. Collectively, the 56 patients diagnosed with nonspecific back pain were treated with rest, physical therapy, and/or nonsteroidal anti-inflammatory medications. In summary, 31 (36%) of the 87 patients were found to have a specific diagnosis (Table 1). Twenty-one (68%) of these 31 patients had a positive finding on his or her initial radiographs. The other 10 patients, who had negative radiographs, were found to have a specific diagnosis by. All 10 patients reported having constant pain, night pain, radicular pain, and/or had an abnormal neurological examination. The sensitivity, specificity, positive predictive value, and negative predictive value of the location of pain, type of pain, scoliosis, and abnormal neurological examination for predicting a specific diagnosis are shown in Table 2. The specificity and positive predictive value of both radicular pain and an abnormal neurological examination were 100%. Night pain also had a very high specificity (95%) for determining a specific diagnosis. Lumbar back pain was found to be the most sensitive (67%) and to have the largest negative predictive value (75%) of the variables. TABLE 1. Frequency of Specific Diagnoses Diagnoses No. Patients Spondylolisthesis 10 Herniated nucleus pulposus 6 Scoliosis 5 Spondylolysis 3 Osteoid osteoma 2 Scheuermann kyphosis 1 Masson tumor 1 Congenital spinal dysraphism 1 Degenerative disc changes 2 The predicted probability of having a specific diagnosis using the 4 predictors (constant pain, night pain, radicular pain, and abnormal neurological examination) was 100% when a patient had 3 of the predictors, 85.7% for 2 predictors, 61.1% for 1 predictor, and 18.6% for zero predictors (Table 3). DISCUSSION Pediatric back pain has been more extensively evaluated in the recent literature as the result of the documentation of a higher prevalence than those previously described. In a longitudinal study that included 216 adolescents over a 5-year period, Burton et al 7 found an annual incidence of lumbar pain of 12% at the age of 12 years and 21.5% at the age of 15 years. Similarly, Brattberg 8 reported a 20% incidence over a 2-year period, and Nissinen et al 9 found an annual incidence of low back pain of 17.6% in 859 children aged 12.8 years, with 4.4% requiring medical care. Many physicians believe that the complaint of back pain in a child is a red flag, and every effort should be made to reach a diagnosis that they believe is caused by an organic pathology. 5,10,11 This has led many children to undergo extensive and often unnecessary investigations, resulting in an increase in radiation exposure, patient/family anxiety, and cost. Certainly, the complaint of back pain in a child may be caused by a serious pathology, but it may also be caused by a benign disease. Feldman et al 12 have demonstrated a high frequency of benign pediatric back pain in that 78.3% of their cases did not have a specific diagnosis to explain their pain. In evaluating pediatric back pain, physicians should aim at differentiating between nonspecific (benign) and specific (pathological) causes using as few diagnostic tests as possible. Included in the differential diagnosis are developmental abnormalities (scoliosis, Scheuermann kyphosis, spondylolysis, spondylolisthesis), mechanical derangement (posture, muscle strain, herniated nucleus pulposus), infection (diskitis, vertebral osteomyelitis), benign neoplasms (osteoid osteoma, osteoblastoma, aneurysmal bone cyst), or malignant neoplasms (leukemia, lymphoma, sarcoma). 5,13 A detailed history should be obtained from the patient and his or her parents inquiring about the onset, duration, frequency, and location of pain, including any exacerbating and alleviating factors. A careful and thorough physical examination should be conducted, including a neurological examination and gait evaluation. The initial radiographic assessment should consist of anteroposterior and lateral plain radiographs of the spine. Simple hematological tests such as CBC and sedimentation rate can be helpful to rule out certain diagnoses, such as infection or leukemia. On the basis of the patient s signs and symptoms, the physician should decide which additional laboratory tests and imaging studies will assist in reaching a diagnosis, such as oblique radiographs of the spine to rule out spondylolysis. When the signs and symptoms do not point to a specific diagnosis and the above-mentioned investigations are normal, the physician is faced with the dilemma of deciding whether to proceed with more extensive and often more expensive tests or to consider the symptoms to be not worrisome and provide conservative treatment. Turner et al 11 recommended that in the absence of neurological signs, patients with a * 2006 Lippincott Williams & Wilkins 355
4 Feldman et al J Pediatr Orthop & Volume 26, Number 3, May/June 2006 TABLE 2. Usefulness of the Type and Location of Pain, Scoliosis, and an Abnormal Neurological Examination in Predicting a Specific Diagnosis Sensitivity (%) Specificity (%) Positive Predictive Value (%) Negative Predictive Value (%) Constant pain Night pain Radicular pain Thoracic pain Thoracolumbar pain Lumbar pain Scoliosis Abnormal neurological examination mobile spine should be treated with a Bwait-and-see[ policy. If their symptoms persist in the presence of clinical suspicion, they suggested that other investigations such as skeletal scintigraphy, myelography, or CT scans are warranted. Controversy exists in the literature regarding the best radiographic modality to use after plain radiographs. According to Turner et al, 11 the greatest diagnostic yield in these patients comes from myelography, which is an invasive, expensive, and uncomfortable test. Richards et al 13 suggested that when the plain radiographs and the neurological examination are normal, a technetium bone scan or singlephoton emission CT should be the next imaging study to be obtained. If the neurological examination is abnormal, an is the optimal study to follow plain radiography to assess the neural axis. When a bone lesion is detected on plain radiography or bone scan, the investigators recommended doing a complete scan to clarify the extent of the lesion. Feldman et al 12 found that the bone scan alone was positive in only 22% of the patients and had low sensitivity and specificity. Five of their patients with both normal plain radiographs and a single-photon emission CT had spinal neoplasms. According to the authors, the main indication for a bone scan is to evaluate patients with suspected spondylolysis and spondylolisthesis presenting with negative plain radiographs or to determine if the lysis is the probable cause of pain. The authors could not state whether an should be part of the routine assessment of children with back pain because the patients in their study inconsistently received. Our algorithm to diagnose specific causes of back pain included initial work-up of history, physical examination, and plain radiographs of the spine. If the radiographs were positive, the patient was given a specific diagnosis based on the radiographic findings and was treated according to the diagnosis. If the radiographs were negative and no diagnostic physical signs were present, then the patient was treated as having nonspecific back pain. These patients were observed and symptomatically treated with rest, physical therapy, and/ or nonsteroidal anti-inflammatory medications. Patients who had a negative radiograph, constant pain, night pain, radicular pain, and/or abnormal neurological examination were evaluated further with. By following this algorithm, we found that we did not miss any specific major spinal pathology such as tumor or infection, and at the last followup, none of the patients who were labeled as having nonspecific back pain had a change in their diagnosis. Similar to the previously noted results of Feldman et al, 12 64% (56/87) of our patients presenting with a chief complaint of back pain had a nondemonstrable cause for their symptoms and were labeled as having nonspecific back pain and treated conservatively. Among the patients who had a specific diagnosis, 21 (68%) of 31 patients were diagnosed by simple plain radiograph. Although some of these patients had other radiographic modalities (CT scans, ) to confirm the diagnosis, the abnormality was seen initially on plain radiographs. We strongly agree with the recommendation that all children presenting with back pain have plain radiographs as their initial radiographic assessment 10,14 and disagree with Selbst et al 1, who found that plain radiographs of the spine were rarely helpful. Plain radiographs are a cost-effective, easily performed modality with a high yield. Our results also showed that certain parameters in the history and physical examination were associated with the presence or absence of specific diagnoses. Constant pain, radicular pain, night pain, and abnormal neurological examination were found to have high specificity, that is, the absence of these parameters would have a high true negative rate for the presence of specific diagnosis. The presence of these clinical markers should alert the physician to possible TABLE 3. Predicted Probability of a Specific Diagnosis on the Basis of the Number of Predictors Present No. Predictors Patients with Nonspecific Diagnosis [n (%)] Patients with Specific Diagnosis [n (%)] Predicted Probability of Specific Diagnosis (%) 0 48 (85.7) 11 (35.5) (12.5) 11 (35.5) (1.8) 6 (19.3) (9.7) Y 356 * 2006 Lippincott Williams & Wilkins
5 J Pediatr Orthop & Volume 26, Number 3, May/June 2006 An Algorithmic Approach to Pediatric Back Pain underlying pathology and indicate that further investigations are warranted. With respect to the location of pain, lumbar pain had the highest sensitivity (67%) and was, therefore, associated with a specific diagnosis. Although lumbar pain was not included in our algorithm to plan for further investigations, our findings suggest that referral of pain specifically to the lumbar area is a relatively important marker that might warrant further evaluation. The presence of scoliosis was found on radiographs in 18% (16/87) of our cases. Five (31%) of these 16 patients had no other underlying pathology to explain their symptoms, and therefore, scoliosis was considered to be the direct cause of their back pain. The association between scoliosis and back pain has been demonstrated by Ramirez et al 15 who found that 23% of patients with adolescent idiopathic scoliosis at initial time of presentation had back pain, and an additional 9% developed back pain during the period of observation. In conclusion, although we cannot rule out missing an occult specific diagnosis, the patients were followed for an average of 3 years without the development of additional signs or symptoms to suggest the presence of a serious pathological condition. Our study suggests that history and physical examination with plain radiographs and an when indicated should be the evaluation for back pain. has supplanted bone scan as a screening tool, and bone scan is used to rule out metastatic disease or determine activity of a spondylolysis. This algorithmic approach provided a systematic methodology of selecting patients for further diagnostic studies. A child who has back pain in which a diagnosis cannot be firmly established based on history, physical examination, and plain radiographs should be further evaluated with of the spine provided that he/she shows certain clinical markers, including constant pain, radicular pain, night pain, and/or abnormal neurological examination. This strategy should reduce costs, decrease patient /family anxiety, and avoid unnecessary radiation exposure. REFERENCES 1. Selbst SM, Lavelle JM, Soyupak SK, et al. Back pain in children who present to the emergency department. Clin Pediatr. 1999;38:401Y Balaque F, Dutoit G, Waldburger M. Low back pain in school children. An epidemiological study. Scand J Rehabil Med Suppl. 1988;20: 175Y Olsen TL, Anderson RL, Dearwater SR, et al. The epidemiology of low back pain in an adolescent population. Am J Public Health. 1992;82: 606Y Salminen JJ, Penti J, Terho P. Low back pain and disability in 14-year old school children. Acta Paediatr. 1992;81:1035Y Bunnell WP. Back pain in children. Orthop Clin North Am. 1982;13: 587Y Combs JA, Caskey PM. Back pain in children and adolescents. A retrospective review of 648 patients. South J Med. 1997;90:789Y Burton AK, Clarke RD, McClune TD, et al. The natural history of low back pain in adolescents. Spine. 1996;21:2323Y Brattberg G. The incidence of back pain and headache among Swedish school children. Qual Life Res. 1994;3:S27YS Nissinen M, Heliovaara M, Seitsamo J, et al. Anthropometric measurements and the incidence of low back pain in a cohort of pubertal children. Spine. 1994;12:1367Y King HA. Evaluating the child with back pain. Pediatr Clin North Am. 1986;33:1489Y Turner PG, Green JH, Galasko SB. Back pain in childhood. Spine. 1989;14:812Y Feldman DS, Hedden DM, Wright JG. The use of bone scan to investigate back pain in children and adolescents. J Pediatr Orthop. 2000;20:790Y Richards BS, McCarthy RE, Akbarnia BA. Back pain in childhood and adolescence. Instr Course Lect. 1999;48:525Y Hoppenfeld S. Back pain. Pediatr Clin North Am. 1977;24:881Y Ramirez N, Johnston CE, Browne RH. The prevalence of back pain in children who have idiopathic scoliosis. J Bone Joint Surg Am. 1997;79: 364Y368. * 2006 Lippincott Williams & Wilkins 357
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Back Pain in Children and Adolescents: Clinically and Cost Effective Treatment
 Back Pain in Children and Adolescents: Clinically and Cost Effective Treatment Matthew E. Oetgen, MD Department of Orthopaedics and Sports Medicine Children s National Medical Center Children s National
Back Pain in Children and Adolescents: Clinically and Cost Effective Treatment Matthew E. Oetgen, MD Department of Orthopaedics and Sports Medicine Children s National Medical Center Children s National
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Health Benchmarks Program Clinical Quality Indicator Specification 2013
 Health Benchmarks Program Clinical Quality Indicator Specification 2013 Measure Title USE OF IMAGING STUDIES FOR LOW BACK PAIN Disease State Musculoskeletal Indicator Classification Utilization Strength
Health Benchmarks Program Clinical Quality Indicator Specification 2013 Measure Title USE OF IMAGING STUDIES FOR LOW BACK PAIN Disease State Musculoskeletal Indicator Classification Utilization Strength
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Test Request Tip Sheet
 With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Advanced Practice Provider Academy
 (+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
(+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
Treatment of Young Athletes with Spine Injuries
 Treatment of Young Athletes with Spine Injuries North American Spine Society Public Education Series Treatment of the Young Athlete Although not common, low back injuries can occur in young athletes who
Treatment of Young Athletes with Spine Injuries North American Spine Society Public Education Series Treatment of the Young Athlete Although not common, low back injuries can occur in young athletes who
Orthopaedic Approach to Back Pain. Seth Cheatham, MD
 Orthopaedic Approach to Back Pain Seth Cheatham, MD 262 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures. Focus on clinical situations where a referral to an orthopaedic surgeon
Orthopaedic Approach to Back Pain Seth Cheatham, MD 262 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures. Focus on clinical situations where a referral to an orthopaedic surgeon
LOW BACK PAIN; MECHANICAL
 1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
DUKE ORTHOPAEDIC SURGERY GOALS AND OBJECTIVES SPINE SERVICE
 GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
Effects of vertebral axial decompression on intradiscal pressure
 This article is reprinted with the permission of the authors from the Journal of Neurosurgery, Volume 81. J Neurosurg 81:350-353, 1994 Effects of vertebral axial decompression on intradiscal pressure GUSTAVO
This article is reprinted with the permission of the authors from the Journal of Neurosurgery, Volume 81. J Neurosurg 81:350-353, 1994 Effects of vertebral axial decompression on intradiscal pressure GUSTAVO
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
How To Get An Mri Of The Lumbar Spine W/O Contrast
 Date notice sent to all parties: May 27, 2014 IRO CASE #: ReviewTex, Inc. 1818 Mountjoy Drive San Antonio, TX 78232 (phone) 210-598-9381 (fax) 210-598-9382 reviewtex@hotmail.com Notice of Independent Review
Date notice sent to all parties: May 27, 2014 IRO CASE #: ReviewTex, Inc. 1818 Mountjoy Drive San Antonio, TX 78232 (phone) 210-598-9381 (fax) 210-598-9382 reviewtex@hotmail.com Notice of Independent Review
Spine Injury and Back Pain in Sports
 Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Clinical Guideline. Low Back Pain Orthopaedics. Princess Alexandra Hospital Emergency Department. 1 Purpose. 2 Background
 Princess Alexandra Hospital Emergency Department Clinical Guideline Orthopaedics Review Officer: Katherine Isoardi Version no: 1 Approval date: 18/03/2015 Review date: 18/03/2017 Approving Officer Dr James
Princess Alexandra Hospital Emergency Department Clinical Guideline Orthopaedics Review Officer: Katherine Isoardi Version no: 1 Approval date: 18/03/2015 Review date: 18/03/2017 Approving Officer Dr James
Lumbar Back Pain in Young Athletes
 Lumbar Back Pain in Young Athletes MS CAQ in Sports Medicine Blair Orthopedics Altoona, PA OMED 2012 San Diego CA AOASM Tuesday October 9 th 1:00pm Lumbar Back Pain in Learning ObjecKves Epidemiology Anatomy
Lumbar Back Pain in Young Athletes MS CAQ in Sports Medicine Blair Orthopedics Altoona, PA OMED 2012 San Diego CA AOASM Tuesday October 9 th 1:00pm Lumbar Back Pain in Learning ObjecKves Epidemiology Anatomy
Diagnosis and Management for Chronic Back Pain: Critical for your Recovery
 Diagnosis and Management for Chronic Back Pain: Critical for your Recovery Dr. Connie D Astolfo, DC, PhD (candidate) In past articles I have stressed that the causes of back pain can be very complex. This
Diagnosis and Management for Chronic Back Pain: Critical for your Recovery Dr. Connie D Astolfo, DC, PhD (candidate) In past articles I have stressed that the causes of back pain can be very complex. This
Headaches in Children
 Children s s Hospital Headaches in Children Manikum Moodley, MD, FRCP Section of Pediatric Neurology The Cleveland Clinic Foundation Introduction Headaches are common in children Most headaches are benign
Children s s Hospital Headaches in Children Manikum Moodley, MD, FRCP Section of Pediatric Neurology The Cleveland Clinic Foundation Introduction Headaches are common in children Most headaches are benign
STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION
 In the matter of STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation XXXXX Petitioner
In the matter of STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation XXXXX Petitioner
The goals of modern spinal surgery are to maximize
 SPRING 2013 Robot-Guided Spine Surgery Christopher R. Good, M.D., F.A.C.S. and Blair K. Snyder, P.A.-C. The goals of modern spinal surgery are to maximize patient function and accelerate a return to a
SPRING 2013 Robot-Guided Spine Surgery Christopher R. Good, M.D., F.A.C.S. and Blair K. Snyder, P.A.-C. The goals of modern spinal surgery are to maximize patient function and accelerate a return to a
LOW BACK PAIN. common of these conditions include: muscle strain ( pulled muscle ), weak core muscles
 LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
Chronic Low Back Pain
 Chronic Low Back Pain North American Spine Society Public Education Series What is Chronic Pain? Low back pain is considered to be chronic if it has been present for longer than three months. Chronic low
Chronic Low Back Pain North American Spine Society Public Education Series What is Chronic Pain? Low back pain is considered to be chronic if it has been present for longer than three months. Chronic low
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
How To Write An Icd10
 Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015
 Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease)
 Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease) 2 Introduction Kummel's disease is a collapse of the vertebrae (the bones that make up the spine). It is also called vertebral osteonecrosis.
Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease) 2 Introduction Kummel's disease is a collapse of the vertebrae (the bones that make up the spine). It is also called vertebral osteonecrosis.
Neck and Back Pain in VA Incidence and Prevalence in VA Users
 Neck and Back Pain in VA Incidence and Prevalence in VA Users Spotlight on Pain Management: Patsi Sinnott, PT, PhD, MPH Sharon Dally, MS, Tigran Avoundjian, MPH, Jody Trafton, PhD, Todd Wagner, PhD Dec.
Neck and Back Pain in VA Incidence and Prevalence in VA Users Spotlight on Pain Management: Patsi Sinnott, PT, PhD, MPH Sharon Dally, MS, Tigran Avoundjian, MPH, Jody Trafton, PhD, Todd Wagner, PhD Dec.
New Onset Seizure Clinic
 New Onset Seizure Clinic Timely Care from the Region s Experts The New Onset Seizure Clinic at UH Rainbow Babies & Children s Hospital provides expert diagnostic services, referrals, treatment and follow-up
New Onset Seizure Clinic Timely Care from the Region s Experts The New Onset Seizure Clinic at UH Rainbow Babies & Children s Hospital provides expert diagnostic services, referrals, treatment and follow-up
International Postprofessional Doctoral of Physical Therapy (DPT) in Musculoskeletal Management Program (non US/Canada) Curriculum
 International Postprofessional Doctoral of Physical Therapy (DPT) in Musculoskeletal Management Program (non US/Canada) Curriculum Effective: July 2015 INTERNATIONAL POSTPROFESSIONAL DOCTORAL OF PHYSICAL
International Postprofessional Doctoral of Physical Therapy (DPT) in Musculoskeletal Management Program (non US/Canada) Curriculum Effective: July 2015 INTERNATIONAL POSTPROFESSIONAL DOCTORAL OF PHYSICAL
Low Back Pain Protocols
 Low Back Pain Protocols Introduction: Diagnostic Triage And 1. Patient Group Adults aged 18 years and over with routine low back problems. Patients who have had recent surgery should be referred directly
Low Back Pain Protocols Introduction: Diagnostic Triage And 1. Patient Group Adults aged 18 years and over with routine low back problems. Patients who have had recent surgery should be referred directly
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure
 Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Headache: Differential diagnosis and Evaluation. Raymond Rios PGY-1 Pediatrics
 Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Maricopa Integrated Health System: Administrative Policy & Procedure
 Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Radiologic Diagnosis of Spinal Metastases
 September 2002 Radiologic Diagnosis of Spinal Metastases Natalie J. M. Dailey, Harvard Medical Student Year III Our Patient s Presenting Story 70 year old male Presents to the hospital for laparascopic
September 2002 Radiologic Diagnosis of Spinal Metastases Natalie J. M. Dailey, Harvard Medical Student Year III Our Patient s Presenting Story 70 year old male Presents to the hospital for laparascopic
Etiology of Long-term Failures of Lumbar Spine Surgery
 PAIN MEDICINE Volume 3 Number 1 2002 Etiology of Long-term Failures of Lumbar Spine Surgery Alexis Waguespack, MD, Jerome Schofferman, MD, Paul Slosar, MD, and James Reynolds, MD SpineCare Medical Group,
PAIN MEDICINE Volume 3 Number 1 2002 Etiology of Long-term Failures of Lumbar Spine Surgery Alexis Waguespack, MD, Jerome Schofferman, MD, Paul Slosar, MD, and James Reynolds, MD SpineCare Medical Group,
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Spinal Decompression
 Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis
 Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis 1 Mason Hohl, MD FROM ABSTRACT: Journal of Bone and Joint Surgery (American) December 1974;56(8):1675-1682 Five years
Soft-tissue injuries of the neck in automobile accidents: Factors influencing prognosis 1 Mason Hohl, MD FROM ABSTRACT: Journal of Bone and Joint Surgery (American) December 1974;56(8):1675-1682 Five years
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Choosing Wisely Recommendation Analysis: Prioritizing Opportunities for Reducing Inappropriate Care
 Choosing Wisely Recommendation Analysis: Prioritizing Opportunities for Reducing Inappropriate Care IMAGING FOR NONSPECIFIC LOW BACK PAIN Sarah Jane Reed, MSc and Steven Pearson, MD, MSc INSTITUTE FOR
Choosing Wisely Recommendation Analysis: Prioritizing Opportunities for Reducing Inappropriate Care IMAGING FOR NONSPECIFIC LOW BACK PAIN Sarah Jane Reed, MSc and Steven Pearson, MD, MSc INSTITUTE FOR
Back Pain in a Gymnast An understanding of its cause and treatment
 Back Pain in a Gymnast An understanding of its cause and treatment David Kruse, M.D. Former Senior Men s National Team Member USAG Men s National Team Physician Assistant Clinical Professor & Director
Back Pain in a Gymnast An understanding of its cause and treatment David Kruse, M.D. Former Senior Men s National Team Member USAG Men s National Team Physician Assistant Clinical Professor & Director
A pediatric case of single level idiopathic cervical intervertebral disc. calcification with symptom relapse one year after initial onset
 Title Author(s) Citation A pediatric case of single-level id calcification with symptom relapse Sasagawa, Takeshi; Hashimoto, Fumio Yoshinobu; Matsumoto, Naoyuki; Sega Goshima, Kenichi; Murakami, Hideki;
Title Author(s) Citation A pediatric case of single-level id calcification with symptom relapse Sasagawa, Takeshi; Hashimoto, Fumio Yoshinobu; Matsumoto, Naoyuki; Sega Goshima, Kenichi; Murakami, Hideki;
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
United States Department of Labor Employees Compensation Appeals Board DECISION AND ORDER
 United States Department of Labor V.L., Appellant and DEPARTMENT OF JUSTICE, U.S. PROBATION DEPARTMENT, New York City, NY, Employer Appearances: Alan J. Shapiro, Esq., for the appellant Office of Solicitor,
United States Department of Labor V.L., Appellant and DEPARTMENT OF JUSTICE, U.S. PROBATION DEPARTMENT, New York City, NY, Employer Appearances: Alan J. Shapiro, Esq., for the appellant Office of Solicitor,
What types of scoliosis are there?
 Patient and Family Education Scoliosis About idiopathic scoliosis and its treatment This handout covers the most common type of scoliosis, adolescent idiopathic scoliosis. Other types of scoliosis may
Patient and Family Education Scoliosis About idiopathic scoliosis and its treatment This handout covers the most common type of scoliosis, adolescent idiopathic scoliosis. Other types of scoliosis may
Spina Bifida Occulta. Lo-Call 1890 20 22 60. Occulta Means Hidden
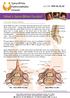 Occulta Means Hidden Spina Bifida Occulta is not easily detected because skin covers the area, such as the spinal cord, spinal bone or nerve roots, which may be affected. Spina Bifida Occulta can affect
Occulta Means Hidden Spina Bifida Occulta is not easily detected because skin covers the area, such as the spinal cord, spinal bone or nerve roots, which may be affected. Spina Bifida Occulta can affect
Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase
 Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase The MedStar Spine Center in Chevy Chase Relief from Pain, Restoration of Function Non-surgical, Minimally Invasive and Complex Surgical
Get Back to the Life You Love! The MedStar Spine Center in Chevy Chase The MedStar Spine Center in Chevy Chase Relief from Pain, Restoration of Function Non-surgical, Minimally Invasive and Complex Surgical
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Hitting a Nerve: The Triggers of Sciatica. Bruce Tranmer MD FRCS FACS
 Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Pathophysiology of Acute and Chronic Low Back Pain
 Pathophysiology of Acute and Chronic Low Back Pain Mary Beth Partyka MSN APN Adult Nurse Practitioner Adult Pain Service Advocate Christ Medical Center Presentation Objectives Review the incidence of acute
Pathophysiology of Acute and Chronic Low Back Pain Mary Beth Partyka MSN APN Adult Nurse Practitioner Adult Pain Service Advocate Christ Medical Center Presentation Objectives Review the incidence of acute
But My Back Hurts Only When I m Standing!
 But My Back Hurts Only When I m Standing! Axial Loading for Spinal Canal Stenosis Matthew Cham, MD; Akio Hiwatashi, MD; Per-Lennart Westesson, MD, PhD, DDS Division of Diagnostic and Interventional Neuroradiology,
But My Back Hurts Only When I m Standing! Axial Loading for Spinal Canal Stenosis Matthew Cham, MD; Akio Hiwatashi, MD; Per-Lennart Westesson, MD, PhD, DDS Division of Diagnostic and Interventional Neuroradiology,
The Lewin Group undertook the following steps to identify the guidelines relevant to the 11 targeted procedures:
 Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Practice Guidelines For Low Back Pain
 Consumers Guide Practice Guidelines For Low Back Pain Copyright 2008 American Chronic Pain Association Page 1 Written by: Penney Cowan Founder Executive Director American Chronic Pain Association Editors:
Consumers Guide Practice Guidelines For Low Back Pain Copyright 2008 American Chronic Pain Association Page 1 Written by: Penney Cowan Founder Executive Director American Chronic Pain Association Editors:
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS
 ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
MN Community Measurement Low Back Pain Measure Impact and Recommendation Document June 2010
 MN Community Measurement Low Back Pain Measure Impact and Recommendation Document June 2010 Impact Relevance to Consumers, Employers and Payers Improvability Inclusiveness Mechanical low back pain (LBP)
MN Community Measurement Low Back Pain Measure Impact and Recommendation Document June 2010 Impact Relevance to Consumers, Employers and Payers Improvability Inclusiveness Mechanical low back pain (LBP)
IMPAIRMENT RATING 5 TH EDITION MODULE II
 IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
Imaging degenerative disk disease in the lumbar spine. Elaine Besancon MS III Dr. Gillian Lieberman
 Imaging degenerative disk disease in the lumbar spine Elaine Besancon MS III Dr. Gillian Lieberman Learning Objectives Anatomy review Pathophysiology of degenerative disc disease Common sequelae of disk
Imaging degenerative disk disease in the lumbar spine Elaine Besancon MS III Dr. Gillian Lieberman Learning Objectives Anatomy review Pathophysiology of degenerative disc disease Common sequelae of disk
Competency Based Goals and Objectives:
 PEDIATRIC SPORTS MEDICINE FELLOWSHIP COMPETENCY-BASED GOALS AND OBJECTIVES & OVERALL EDUCATIONAL GOALS Competency Based Goals and Objectives: Mission: Train fellows to become sports medicine physicians
PEDIATRIC SPORTS MEDICINE FELLOWSHIP COMPETENCY-BASED GOALS AND OBJECTIVES & OVERALL EDUCATIONAL GOALS Competency Based Goals and Objectives: Mission: Train fellows to become sports medicine physicians
Practice Guideline. Neuropsychological Evaluations
 Practice Guideline Neuropsychological Evaluations Adapted from the practice guideline of the same name by the Arizona Department of Health Services Division of Behavioral Health Services Effective: 06/30/2006
Practice Guideline Neuropsychological Evaluations Adapted from the practice guideline of the same name by the Arizona Department of Health Services Division of Behavioral Health Services Effective: 06/30/2006
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 jonrgottlieb@gmail.com
 Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 jonrgottlieb@gmail.com CURRENT PRACTICE September 2009-present University of Miami School of Medicine Assistant Professor, Department of
Jonathan R. Gottlieb, MD 7220 SW 127 Street Pinecrest, FL 33156 jonrgottlieb@gmail.com CURRENT PRACTICE September 2009-present University of Miami School of Medicine Assistant Professor, Department of
The Spine Center at Beth Israel Deaconess
 Spinal Pain The Spine Center at Beth Israel Deaconess Medical Center developed the following detailed eplanation of our care pathways for primary care providers to help support your interactions with patients
Spinal Pain The Spine Center at Beth Israel Deaconess Medical Center developed the following detailed eplanation of our care pathways for primary care providers to help support your interactions with patients
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Spine University s Guide to Kinetic MRIs Detect Disc Herniations
 Spine University s Guide to Kinetic MRIs Detect Disc Herniations 2 Introduction Traditionally, doctors use a procedure called magnetic resonance imaging (MRI) to diagnose disc injuries. Kinetic magnetic
Spine University s Guide to Kinetic MRIs Detect Disc Herniations 2 Introduction Traditionally, doctors use a procedure called magnetic resonance imaging (MRI) to diagnose disc injuries. Kinetic magnetic
BACK PAIN MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: BACK PAIN MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN BACK PAIN MEASURES GROUP: #148. Back Pain: Initial Visit #149. Back Pain: Physical Exam #150. Back Pain: Advice
2014 PQRS OPTIONS F MEASURES GROUPS: BACK PAIN MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN BACK PAIN MEASURES GROUP: #148. Back Pain: Initial Visit #149. Back Pain: Physical Exam #150. Back Pain: Advice
Clarian Health Partners - Marketing Group. Procedure Code Listing by Specialty Report Prepared: February 11, 2011 at 8:50 AM
 IU Health Listing by Abdominal Diagnostic Ultrasound ABDOMDX All Aspects of Spine Care SPINE Amputations AMPUTATE Ankle Arthroscopy ANKLEART Ankle Pain ANKLEPAI Ankle Surgery ANKLESX Arthritic Recon. Proc.
IU Health Listing by Abdominal Diagnostic Ultrasound ABDOMDX All Aspects of Spine Care SPINE Amputations AMPUTATE Ankle Arthroscopy ANKLEART Ankle Pain ANKLEPAI Ankle Surgery ANKLESX Arthritic Recon. Proc.
Information on the Chiropractic Care of Lower Back Pain
 Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Worsening thigh pain after blunt trauma
 Images in Radiology Worsening thigh pain after blunt trauma LT Kendall Lane MD MC USN A 19 year-old otherwise healthy male presented with right thigh pain for three weeks after another player s knee struck
Images in Radiology Worsening thigh pain after blunt trauma LT Kendall Lane MD MC USN A 19 year-old otherwise healthy male presented with right thigh pain for three weeks after another player s knee struck
Understanding. Spinal Cord Injury. Tasha, injured in 1997.
 Understanding Spinal Cord Injury Tasha, injured in 1997. What Is Spinal Cord Injury? The spinal cord is the part of the central nervous system that contains the body s longest nerve fibers. It serves as
Understanding Spinal Cord Injury Tasha, injured in 1997. What Is Spinal Cord Injury? The spinal cord is the part of the central nervous system that contains the body s longest nerve fibers. It serves as
INDEPENDENT MEDICAL EXAMINATION. Dr. Jeffery Luther
 INDEPENDENT MEDICAL EXAMINATION Dr. Jeffery Luther What is an Independent Medical Exam? Objective and impartial medical exam Requested by workers compensation insurer or self insured provider Conducted
INDEPENDENT MEDICAL EXAMINATION Dr. Jeffery Luther What is an Independent Medical Exam? Objective and impartial medical exam Requested by workers compensation insurer or self insured provider Conducted
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Facet and Axial Spine Pain
 Facet and Axial Spine Pain Diane M. Rowles, MS, ACNP, BC, CRRN Nurse Practitioner, University Neurosurgery Rush University Medical Center Adjunct Assistant Professor, Feinberg School of Medicine Northwestern
Facet and Axial Spine Pain Diane M. Rowles, MS, ACNP, BC, CRRN Nurse Practitioner, University Neurosurgery Rush University Medical Center Adjunct Assistant Professor, Feinberg School of Medicine Northwestern
IN THE MATTER OF: Docket No. 2012-53891 QHP Case No. DECISION AND ORDER
 STATE OF MICHIGAN MICHIGAN ADMINISTRATIVE HEARING SYSTEM FOR THE DEPARTMENT OF COMMUNITY HEALTH P.O. Box 30763, Lansing, MI 48909 (877) 833-0870; Fax: (517) 334-9505 IN THE MATTER OF: Docket No. 2012-53891
STATE OF MICHIGAN MICHIGAN ADMINISTRATIVE HEARING SYSTEM FOR THE DEPARTMENT OF COMMUNITY HEALTH P.O. Box 30763, Lansing, MI 48909 (877) 833-0870; Fax: (517) 334-9505 IN THE MATTER OF: Docket No. 2012-53891
Employees Compensation Appeals Board
 U. S. DEPARTMENT OF LABOR Employees Compensation Appeals Board In the Matter of BRENDA K. ANDREWS and U.S. POSTAL SERVICE, POST OFFICE, Chillicothe, OH Docket No. 03-780; Submitted on the Record; Issued
U. S. DEPARTMENT OF LABOR Employees Compensation Appeals Board In the Matter of BRENDA K. ANDREWS and U.S. POSTAL SERVICE, POST OFFICE, Chillicothe, OH Docket No. 03-780; Submitted on the Record; Issued
Spine Pain in VA: Right Cohorto Patsi Sinnott. Andrea Shane, Andrew Siroka Todd Wagner, Jodie Trafton July 21, 2010
 Spine Pain in VA: Finding the Complete/ Right Cohorto Patsi Sinnott Andrea Shane, Andrew Siroka Todd Wagner, Jodie Trafton July 21, 2010 Outline Background Methods Results Discussioni 2 Background Musculoskeletal
Spine Pain in VA: Finding the Complete/ Right Cohorto Patsi Sinnott Andrea Shane, Andrew Siroka Todd Wagner, Jodie Trafton July 21, 2010 Outline Background Methods Results Discussioni 2 Background Musculoskeletal
Sinus Headache vs. Migraine
 Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Sodium Fluoride PET/CT Bone Imaging: Theory and Practice
 Sodium Fluoride PET/CT Bone Imaging: Theory and Practice George Segall, M.D. Stanford University Why F-18 Fluoride? Faster Higher Resolution Anatomic Correlation Chemiadsorption Hydroxyapatite Ca10(PO4)6(OH)2
Sodium Fluoride PET/CT Bone Imaging: Theory and Practice George Segall, M.D. Stanford University Why F-18 Fluoride? Faster Higher Resolution Anatomic Correlation Chemiadsorption Hydroxyapatite Ca10(PO4)6(OH)2
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
