Proximal Humeral Fracture Repair and Rehabilitation
|
|
|
- Richard Harper
- 8 years ago
- Views:
Transcription
1 1 Proximal Humeral Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: Numerous types of proximal humeral fractures can occur each of which have separate surgical indications and considerations. Proximal humeral fractures commonly occur along the physeal lines. Thus, fractures may involve the tubercles (greater and/or lesser), surgical neck, or anatomical neck of the humerus. The surgical neck lies between the tuberosities and the shaft while the anatomical neck is the junction between the humeral head and the tuberosities. Fortunately, surgical neck fractures are more common. Anatomical neck fractures typically have a less favorable prognosis due to their result in devascularization of the humeral head. Between the two tuberosities of humerus lies a groove in which the biceps tendon lies. It is through this groove that the terminal branches of the ascending division of the anterior humeral circumflex artery enter the humeral head. Fractures that split the tuberosities from the head disrupt this small arterial complex and can result in osteonecrosis of the humeral head. The most recognized and used standard for assessing proximal fractures is the 4-part Neer classification system. It is used for both treatment and prognosis. The 4-part classification: One-part fractures Eight of ten proximal humeral fractures are of this type and include all fractures of the proximal humerus, regardless of the level or number of fracture lines, in which no segment is displaced more than 1cm or angulated more than 45. Two-part fractures The two-part fracture includes those proximal humeral fractures with a single displacement at the anatomic neck, surgical neck, lesser tuberosity, or greater tuberosity. The fracture is named by the structure that is displaced (Two-part surgical neck fracture). Three-part fractures The three-part fracture includes all proximal humeral fractures with a displaced surgical neck and either a greater or lesser tuberosity displacement fracture. Four-part fractures Four-part fractures are proximal humeral fractures with three displaced, fractured segments including both tuberosities and typically the surgical neck. Avascular necrosis is common in these types of fractures. The anatomical positioning of the neural and vascular structures of the arm can cause complications in these types of fractures. Severe displacement of the structures of the shoulder with these types of injury can cause damage to the brachial plexus (most commonly a traction injury of the axillary nerve) or vascular structures (commonly effecting the axillary artery). Avascular necrosis is also a complication causing bone cell death when the blood supply is cut off from a fractured region of bone as mentioned above.
2 2 Pathogenesis: Bone fractures when the mechanical forces exceed the physiologic capacity of the bone. Intrinsic weakening of bone increases the risk of such pathology. Weakening of proximal humeral bone tissue may occur due to repetitive stress (as occurs in little leaguer s shoulder and stress fractures), endocrine functioning (as is the case in osteoporosis), pathology (such as sickle cell anemia, tumors, or cancer), or nutritional deficits (as found in cases of Rickets and osteomalacia). External forces commonly leading to proximal humerus fractures include a fall on the outstretched arm, excessive rotation in the abducted position, a direct blow to the lateral aspect of the shoulder, dislocation leading to subsequent avulsion fracture(s), electrical shock, and muscular forces of seizures (subscapularis can avulse the lesser tuberosity). Biomechanically with a fall on the outstretched arm, the most common cause of proximal humeral fractures, the shoulder and limb remain medially rotated. Normally, to accomplish full abduction, the humerus must externally rotate. If external rotation is blocked, as in a fall, the proximal humerus becomes impinged against the acromion. The acromion acts as a fulcrum of a lever and the depending on the quality of the tissues of the shoulder complex the humerus may fracture, dislocate, or both dislocate and fracture. Epidemiology: Proximal humeral fractures are relatively common. They represent about 4% of all fractures seen in the average orthopedic clinic. These fractures occur in all ages but are most common in relatively fit elderly. The injury is more common in females and the highest agespecific incidence occurs in women between 80 and 89 years of age. Not surprisingly these injuries are more commonly caused by sport and road traffic accidents in younger generations, while over the age of 30 the chief cause of proximal humeral fractures is a standing height fall. ~49% of proximal humeral fractures are part-one, ~28% are part-two surgical neck fractures, ~9% are three-part greater tuberosity and surgical neck fractures. Four-part fractures and fracture dislocations account for ~3% of proximal humeral fractures. Diagnosis Mechanism of injury is usually consistent with a fall on an out stretched arm or blow to the shoulder during a traumatic or sports related event Severe point tenderness over the fracture site can be found with palpation, caution should be used to prevent further damage at the fracture site Swelling usually appears immediately about the shoulder and upper arm while ecchymosis generally appears hrs later. Ecchymosis may spread to the chest wall, flank, and forearm. Confirmation of the fracture can be made with radiographic images. CT scan is indicated in selected cases. Non-operative Versus Operative Management: Treatment of proximal humeral fractures vary depending on the type and severity of the fracture as well as the activity level, health, age, quality of bone, and motivation of the patient. Generally, most unstable/displaced fractures or fractures with accompanying vascular insult require surgical intervention. Various methods of treatment include closed reduction, casts, splints, percutaneous pinning, external fixation, open reduction and internal fixation, and humeral head replacement.
3 3 Non-operative: Non-displaced or minimally displaced fractures as well as patients with medical illnesses that preclude them from surgery should be treated conservatively. They can be managed nonsurgically, by immobilizing the arm in a sling for comfort and instituting early range of motion exercises when pain permits. See protocol for treatment below. Operative: Isolated two-part fractures of the tuberosities are difficult to perform closed reduction on secondary to the forces created by the attached rotator cuff muscles. The greater tuberosity fracture is treated nonoperatively for fractures with less than.5 cm of superior displacement or 1cm of posterior displacement. If greater, these fractures are generally treated with open reduction internal fixation to prevent subacromial impingement and malunions. The rare isolated lesser trochanteric fracture is treated with open reduction internal fixation when the fragment is large and blocks medical rotation. Two-Part Surgical Neck Fractures are generally treated with open reduction internal fixation for younger patients with good bone quality and ability to comply with postoperative therapy. Rigid internal fixation devices often fail when applied to thin porous bone so hemiarthroplasty is often a better treatment choice for elderly patients. Percutaneous internal fixation is often chosen for displaced two-part fractures that can be reduced with closed manipulation. Intramedullary fixation has been completed successfully by some but concern of torsional rigidity, risk of displacement, and impingement by a prominent rod deters many from this technique. Three part fractures also have multiple treatment choices including internal fixation options of interfragmentary fixation with sutures or wire, percutaneous pinning, plate-and-screw fixation, and intramedullary fixation with and without suture supplementation. Reduction can be completed closed but are difficult to manage. Open reduction is the more common management. Rarely, prosthetic hemi-arthroplasty is used. Four-part fracture treatment options range from early mobilization to percutaneous reduction and internal fixation, open reduction and internal fixation, and hemiarthroplasty. Nonoperative treatment is typically reserved for those in which surgery is contraindicated secondary to the fact that this treatment often results in malunion and pain. There is conflicting evidence recorded on the most effective treatment for this injury.
4 4 NONOPERATIVE AND POSTOPERATIVE REHABILITATION Note: The following rehabilitation progression is a summary of the guidelines provided by Basti, Dionysian, Sherman, and Bigliani. Refer to their publication to obtain further information regarding criteria to progress from one phase to the next, anticipated impairments and functional limitations, interventions, goals, and rationales. REHABILITATION FOR NON-OPERATIVE HUMERAL FRACTURES Early Passive Motion: (7-10 days post fracture) Goals: Control pain and edema Protect fracture site Minimize deconditioning Maintain range in joints around the effected region (wrist, hand, and neck) Prevent glenohumeral adhesive capsulitis and muscle flexibility deficits Modalities, such as TENS and ice, for pain control Splint/Sling as direct by MD Monitor use and weight bearing instructions per MD Cardiovascular conditioning Gentle range of motion exercises of the neck, wrist, and hand Pendulum exercises Passive forward elevation of the shoulder Passive external rotation of the shoulder Early Passive Motion: (10 days to 3 weeks post fracture) When pain has diminished and the patient is less apprehensive. Goals: Same as above in addition to above Active assistive forward elevation Active assistive external rotation to 40 Phase I: (3-6 weeks post fracture) Goals: Continue to control pain and edema as needed Minimize deconditioning Regain full range of motion Prevent muscle atrophy
5 5 Pendulum Active assistive forward elevation Active assistive external rotation Isometrics: Internal and external rotation, flexion, extension, and abduction in a neutral position (at 4 weeks) Active assistive hyper extension (at 6 weeks) Gripping exercises Phase II: (6-8 weeks post fracture) Goals: Regain full Range of motion Actively work within newly gained range of motion Increase strength Active forward elevation in supine Active forward elevation with weights in supine Forward elevation in standing with stick Pulleys with eccentric lowering of involved arm Phase III: (8 weeks post fracture) Goals: Increase strength (especially at end range) Gain adequate strength in the rotator cuff to allow for humeral head depression necessary to avoid impingement Strengthen scapular rotators to allow for proper scapulohumeral rhythm Resistive exercises: standing forward press, theraband resisted (flexion, internal rotation, external rotation and abduction) exercises, and rowing Self stretching: flexion/abduction combined, internal rotation, flexion, abduction/external rotation combined, bilateral hanging stretches Advanced internal rotation, shoulder flexion, external rotation and horizontal abduction stretching
6 6 REHABILITATION FOR OPEN REDUCTION/INTERNAL FIXATION AND HUMERAL HEAD REPLACEMENT Preoperative Rehabilitation Injury is protected with immobilization through casting, splinting and/or placed in a sling Patient is instructed of post-operative rehabilitation goals and plan Early Passive Motion: (3-5 days post op) Goals: Control pain and edema Protect fracture site Minimize cardiovascular deconditioning Maintain range in joints around the effected region (wrist, hand, and neck) Prevent glenohumeral adhesive capsulitis and muscle flexibility deficies Modalities, such as TENS and ice, for pain control Splint/Sling as direct by MD Monitor use and weight bearing instructions per MD Cardiovascular conditioning Gentle range of motion exercises of the neck, wrist, and hand Passive supine external rotation to 40 Passive supine forward elevation Phase Ia: (7-10 days post op) and Phase Ib: (3 weeks post op) Goals: Continue to control pain and edema as needed Minimize deconditioning Regain full range of motion Prevent muscle atrophy Phase Ia Pendulum Passive external rotation with stick or pulleys Passive forward elevation with assist from non involved arm or pulleys Passive internal rotation and hyperextension with stick (not to be done with tuberosity fracture) Cardiovascular conditioning
7 7 Interventions: Phase Ib Isometrics: Internal rotation, external rotation, flexion, extension, abduction in a neutral position Phase II: (4-6 weeks post op) Goals: Regain full Range of motion Actively work within newly gained range of motion Increase strength Active forward elevation in supine Active forward elevation with weights in supine Forward elevation in standing with stick Pulleys with eccentric lowering of involved arm Phase III: (12 weeks post op) Goals: Increase strength (especially at end range) Gain adequate strength in the rotator cuff to allow for humeral head depression necessary to avoid impingement Strengthen scapular rotators to allow for proper scapulohumeral rhythm Resistive exercises: Standing forward press, theraband resisted (flexion, internal rotation, external rotation and abduction) exercises, and rowing Self stretching: flexion/abduction combined, internal rotation, flexion, abduction/external rotation combined, bilateral hanging stretches Advanced internal rotation, shoulder flexion, external rotation and horizontal abduction stretching
8 8 Selected References: Basti JJ, Dionysian E, Sherman PW, Bigliani LU. Management of proximal humeral fractures. J Hand Ther. 1994;7: Cornell N, Schneider K. Proximal Humerus. In Koval K, Zuckerman J, eds., Fractures in the Elderly. Philadelphia, Lippincott-Raven Court-Brown CM, Garg A, McQueen MM. The epidemiology of proximal humeral fractures. Acta Orthop Scand. 2001;72: Curwin S. Shoulder Injuries. In Zachazewski JE, Magee DJ, Quillen WS, eds. Athletic Injuries and Rehabilitation. Philadelphia, 1996, WB Saunders. Goldman RT, Koval KJ, Cuomo F, Gallagher MA, Zuckerman JD. Functional outcome after humeral head replacement for acute three- and four-part proximal humeral fractures. J Shoulder Elbow Surg. 1995;4: Green A, Izzi J. Isolated fractures of the greater tuberosity of the proximal humerus. J Shoulder Elbow Surg. 2003;12: Iannotti JP, Ramsey ML, Williams GR, Warner JP. Nonprosthetic management of proximal humeral fractures. J Bone Joint Surgery. 2003;8: Neer CS. Four-segment classification of proximal humeral fractures: purpose and reliable use. J Shoulder Elbow Surg. 2002;11: Visser C, et al. Nerve lesions in proximal humeral fractures. J Shoulder Elbow Surg. 2001;10: Zyto K, Wallace WA, Frostick SP, Preston BJ. Outcome after hemiarthroplasy for three-and four-part fractures of the proximal humerus. J Shoulder Elbow Surg. 1998;7:85-89.
Radial Head Fracture Repair and Rehabilitation
 1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
SCAPULAR FRACTURES. Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading.
 SCAPULAR FRACTURES Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading. Aims Anatomy Incidence/Importance Mechanism Classification Principles of treatment Specific variations Conclusion Anatomy
SCAPULAR FRACTURES Jai Relwani, Shoulder Fellow, Reading Shoulder Unit, Reading. Aims Anatomy Incidence/Importance Mechanism Classification Principles of treatment Specific variations Conclusion Anatomy
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior
 Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Biceps Tenodesis Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Shoulder Pain and Weakness
 Shoulder Pain and Weakness John D. Kelly IV, MD THE PHYSICIAN AND SPORTSMEDICINE - VOL 32 - NO. 11 - NOVEMBER 2004 For CME accreditation information, instructions and learning objectives, click here. A
Shoulder Pain and Weakness John D. Kelly IV, MD THE PHYSICIAN AND SPORTSMEDICINE - VOL 32 - NO. 11 - NOVEMBER 2004 For CME accreditation information, instructions and learning objectives, click here. A
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com
 North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
Rotator Cuff Tears in Football
 Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Rehabilitation Guidelines For SLAP Lesion Repair
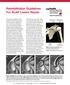 Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
A Patient s Guide to Shoulder Pain
 A Patient s Guide to Shoulder Pain Part 2 Evaluating the Patient James T. Mazzara, M.D. Shoulder and Elbow Surgery Sports Medicine Occupational Orthopedics Patient Education Disclaimer This presentation
A Patient s Guide to Shoulder Pain Part 2 Evaluating the Patient James T. Mazzara, M.D. Shoulder and Elbow Surgery Sports Medicine Occupational Orthopedics Patient Education Disclaimer This presentation
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Arthroscopic Rotator Cuff Repair Postoperative Rehab Protocol Starting the first day after surgery you should remove the sling 3-4 times per day to perform pendulum exercises and elbow/wrist range of motion
Arthroscopic Rotator Cuff Repair Postoperative Rehab Protocol Starting the first day after surgery you should remove the sling 3-4 times per day to perform pendulum exercises and elbow/wrist range of motion
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Hand and Upper Extremity Injuries in Outdoor Activities. John A. Schneider, M.D.
 Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Biceps Brachii Tendon Proximal Rupture
 1 Biceps Brachii Tendon Proximal Rupture Surgical Indications and Considerations Anatomical Considerations: Biceps brachii, one of the dominant muscles of the arm, is involved in functional activities
1 Biceps Brachii Tendon Proximal Rupture Surgical Indications and Considerations Anatomical Considerations: Biceps brachii, one of the dominant muscles of the arm, is involved in functional activities
Rotator Cuff Repair and Rehabilitation
 1 Rotator Cuff Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The rotator cuff complex is comprised of four tendons from four muscles: supraspinatus, infraspinatus,
1 Rotator Cuff Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The rotator cuff complex is comprised of four tendons from four muscles: supraspinatus, infraspinatus,
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair
 Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
Total Elbow Arthroplasty and Rehabilitation
 Total Elbow Arthroplasty and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: There are three bones and four joint articulations that have a high degree of congruence in
Total Elbow Arthroplasty and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: There are three bones and four joint articulations that have a high degree of congruence in
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463
 Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes
 SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It
SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair
 Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Nonoperative Treatment of Proximal. Humerus Fractures
 Nonoperative Treatment of Proximal 2 Humerus Fractures Todd Twiss Introduction Proximal humerus fractures are common but debilitating injuries, which result in significant dysfunction for the patient and
Nonoperative Treatment of Proximal 2 Humerus Fractures Todd Twiss Introduction Proximal humerus fractures are common but debilitating injuries, which result in significant dysfunction for the patient and
Arthroscopic Labrum Repair of the Shoulder (SLAP)
 Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Rotator Cuff Repair
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Upper Limb QUESTIONS UPPER LIMB: QUESTIONS
 1 Upper Limb QUESTIONS 1.1 Which of the following statements best describes the scapula? a. It usually overlies the 2nd to 9th ribs. b. The spine continues laterally as the coracoid process. c. The suprascapular
1 Upper Limb QUESTIONS 1.1 Which of the following statements best describes the scapula? a. It usually overlies the 2nd to 9th ribs. b. The spine continues laterally as the coracoid process. c. The suprascapular
A Simplified Approach to Common Shoulder Problems
 A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
Rehabilitation Guidelines for Post-Operative Stiff Shoulder
 Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Management of common upper limb fractures in Adults and Children. Dr Matthew Sherlock Shoulder and Elbow Orthopaedic Surgeon
 Management of common upper limb fractures in Adults and Children Dr Matthew Sherlock Shoulder and Elbow Orthopaedic Surgeon Outline Immobilisation choices Adults Clavicle Fractures Proximal Humeral Fractures
Management of common upper limb fractures in Adults and Children Dr Matthew Sherlock Shoulder and Elbow Orthopaedic Surgeon Outline Immobilisation choices Adults Clavicle Fractures Proximal Humeral Fractures
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Department of Rehabilitation Services Physical Therapy This protocol has been adopted from Brotzman & Wilk, which has been published in Brotzman SB, Wilk KE, Clinical Orthopeadic Rehabilitation. Philadelphia,
Department of Rehabilitation Services Physical Therapy This protocol has been adopted from Brotzman & Wilk, which has been published in Brotzman SB, Wilk KE, Clinical Orthopeadic Rehabilitation. Philadelphia,
Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation
 1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma. Magee, 2008. pg.
 PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
2. Repair of the deltoid - the amount deltoid was released and security of repair
 Johns Hopkins Shoulder Surgery Rotator Cuff Rehabilitation Program Johns Hopkins Shoulder Surgeons INTRODUCTION: This program is designed for rotator cuff repairs involving fixation of the tendon to bone,
Johns Hopkins Shoulder Surgery Rotator Cuff Rehabilitation Program Johns Hopkins Shoulder Surgeons INTRODUCTION: This program is designed for rotator cuff repairs involving fixation of the tendon to bone,
Important rehabilitation management concepts to consider for a postoperative physical therapy rtsa program are:
 : General Information: Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff
: General Information: Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff
Rehabilitation Guidelines for Biceps Tenodesis
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Biceps Tenodesis The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms a flat, shallow surface.
UW Health Sports Rehabilitation Rehabilitation Guidelines for Biceps Tenodesis The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms a flat, shallow surface.
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to
Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm
 Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm *It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual
Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm *It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual
Arthroscopic Labral Repair (SLAP)
 Arthroscopic Labral Repair (SLAP) Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Anatomy The shoulder joint involves three bones: the scapula
Arthroscopic Labral Repair (SLAP) Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Anatomy The shoulder joint involves three bones: the scapula
Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood
 Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood Indications: Posterior shoulder instability is a relatively uncommon finding in normal adult shoulders. The most common
Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood Indications: Posterior shoulder instability is a relatively uncommon finding in normal adult shoulders. The most common
Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior
 Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior glenohumeral instability and glenoid labral tear. Background:
Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior glenohumeral instability and glenoid labral tear. Background:
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T
 THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL
 POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL The goal of this rehabilitation program is to return the patient/athlete to their activity/sport as quickly and safely as possible while maintaining a stable
POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL The goal of this rehabilitation program is to return the patient/athlete to their activity/sport as quickly and safely as possible while maintaining a stable
Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
 LUKE S. CHOI, M.D. 14825 N. Outer Forty Road, Suite 360 Chesterfield, MO 63017 Office: (314) 392-5063 Fax: (314) 336-2571 Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
LUKE S. CHOI, M.D. 14825 N. Outer Forty Road, Suite 360 Chesterfield, MO 63017 Office: (314) 392-5063 Fax: (314) 336-2571 Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair
 UW Health SpoRTS Rehabilitation Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair The anatomic configuration of the shoulder joint (glenohumeral joint)
UW Health SpoRTS Rehabilitation Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair The anatomic configuration of the shoulder joint (glenohumeral joint)
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Ms. Ruth Delaney ROTATOR CUFF DISEASE Orthopaedic Surgeon, Shoulder Specialist
 WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
Arthroscopic Shoulder Procedures. David C. Neuschwander MD. Shoulder Instability. Allegheny Health Network Orthopedic Associates of Pittsburgh
 Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
Upper limb injuries. Traumatology RHS 231 Dr. Einas Al-Eisa
 Upper limb injuries Traumatology RHS 231 Dr. Einas Al-Eisa Pain in the limbs: May be classified under 4 headings: 1. Joint pain 2. Soft tissue pain 3. Neurogenic pain 4. Orthopaedic causes (fractures,
Upper limb injuries Traumatology RHS 231 Dr. Einas Al-Eisa Pain in the limbs: May be classified under 4 headings: 1. Joint pain 2. Soft tissue pain 3. Neurogenic pain 4. Orthopaedic causes (fractures,
Hamstring Apophyseal Injuries in Adolescent Athletes
 Hamstring Apophyseal Injuries in Adolescent Athletes Kyle Nagle, MD MPH University of Colorado Department of Orthopedics Children s Hospital Colorado Orthopedics Institute June 14, 2014 Disclosures I have
Hamstring Apophyseal Injuries in Adolescent Athletes Kyle Nagle, MD MPH University of Colorado Department of Orthopedics Children s Hospital Colorado Orthopedics Institute June 14, 2014 Disclosures I have
J F de Beer, K van Rooyen, D Bhatia. Rotator Cuff Tears
 1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
28% have partial tear of the rotator cuff.
 ROTATOR CUFF TENDON RUPTURE Anatomy: 1. Rotator cuff consists of: Subscapularis anteriorly, Supraspinatus superiorly and Infraspinatus and Teres minor posteriorly. 2 Biceps tendon is present in the rotator
ROTATOR CUFF TENDON RUPTURE Anatomy: 1. Rotator cuff consists of: Subscapularis anteriorly, Supraspinatus superiorly and Infraspinatus and Teres minor posteriorly. 2 Biceps tendon is present in the rotator
Wrist Fracture. Please stick addressograph here
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
Copeland Surface Replacement Arthroplasty (Hannan Mullett)
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Rehabilitation After Arthroscopic Bankart Repair And Anterior Stabilization Procedures Phase 0: 0 to 2 weeks after Surgery
 Rehabilitation After Arthroscopic Bankart Repair And Anterior Stabilization Procedures Phase 0: 0 to 2 weeks after Surgery POSTOPERATIVE INSTRUCTIONS Brett Sanders, MD Center For Sports Medicine and Orthopaedic
Rehabilitation After Arthroscopic Bankart Repair And Anterior Stabilization Procedures Phase 0: 0 to 2 weeks after Surgery POSTOPERATIVE INSTRUCTIONS Brett Sanders, MD Center For Sports Medicine and Orthopaedic
LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ
LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ
ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF)
 ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF) Phase I Immediate Post Surgical Phase (Weeks 1-4): Maintain integrity of repair Diminish pain and inflammation Prevent muscular inhibition Independent
ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF) Phase I Immediate Post Surgical Phase (Weeks 1-4): Maintain integrity of repair Diminish pain and inflammation Prevent muscular inhibition Independent
Shoulder Injuries. Why Bother? QAS Injury Prevalence. Screening Injury 29.2% 12 month cumulative injury prevalence. Dr Simon Locke
 Shoulder Injuries Dr Simon Locke Why Bother? Are shoulder and upper limb injuries common? Some anatomy What, where, what sports? How do they happen? Treatment, advances? QAS Injury Prevalence Screening
Shoulder Injuries Dr Simon Locke Why Bother? Are shoulder and upper limb injuries common? Some anatomy What, where, what sports? How do they happen? Treatment, advances? QAS Injury Prevalence Screening
POST OPERATIVE ROTATOR CUFF REPAIR PROTOCOL. Therapist Instructions
 MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes
 Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic anterior stabilization procedure.
Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic anterior stabilization procedure.
9/7/14. I do not have a financial relationship with any orthopedic manufacturing organization
 I do not have a financial relationship with any orthopedic manufacturing organization Timothy M. Geib, MD Oklahoma Sports & Orthopedic Institute September 27, 2014 Despite what you may have heard, I am
I do not have a financial relationship with any orthopedic manufacturing organization Timothy M. Geib, MD Oklahoma Sports & Orthopedic Institute September 27, 2014 Despite what you may have heard, I am
ROTATOR CUFF TEARS SMALL
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
ASOP Exams PO Box 7440 Seminole, FL 33775. The Manual of Fracture Casting & Bracing Exam 80% Passing ID # Name Title. Address. City State Zip.
 The Manual of Fracture Casting & Bracing Exam 80% Passing ID # Name Title Address City State Zip Tel# Email Certification Organization Cert# Mail a copy of your completed exam to: ASOP Exams PO Box 7440
The Manual of Fracture Casting & Bracing Exam 80% Passing ID # Name Title Address City State Zip Tel# Email Certification Organization Cert# Mail a copy of your completed exam to: ASOP Exams PO Box 7440
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
POSTERIOR LABRAL (BANKART) REPAIRS
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
SHOULDER INSTABILITY. E. Edward Khalfayan, MD
 SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears)
 SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears) This protocol has been modified and is being used with permission from the BWH Sports and Shoulder Service. The
SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears) This protocol has been modified and is being used with permission from the BWH Sports and Shoulder Service. The
Diagnosis of Acromioclavicular Joint Injuries
 PO Box 15 Rocky Hill, CT 06067 (860) 463-9003 Chiroeducation@aol.com www.chirocredit.com ChiroCredit.com is proud to present a section from one of our continuing education programs: Physical Diagnosis
PO Box 15 Rocky Hill, CT 06067 (860) 463-9003 Chiroeducation@aol.com www.chirocredit.com ChiroCredit.com is proud to present a section from one of our continuing education programs: Physical Diagnosis
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Clavicle Fracture (Broken Collarbone)
 617-726-7500 www2.massgeneral.org/sports Clavicle Fracture (Broken Collarbone) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages.
617-726-7500 www2.massgeneral.org/sports Clavicle Fracture (Broken Collarbone) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages.
Forearm Fractures 09/18/2013. Mechanism: Usually a fall on an outstretched arm. Incidence. Mechansim
 September 20, 2013 Amanda Taylor PA-C Children s Orthopaedics of Louisville Forearm Fractures Incidence 40-50% of all pediatric fractures Mechansim Wide range of mechanism Mechanism: Usually a fall on
September 20, 2013 Amanda Taylor PA-C Children s Orthopaedics of Louisville Forearm Fractures Incidence 40-50% of all pediatric fractures Mechansim Wide range of mechanism Mechanism: Usually a fall on
Clients w/ Orthopedic, Injury and Rehabilitation Concerns. Chapter 21
 Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
SHOULDER INSTABILITY IN PATIENTS WITH EDS
 EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
.org. Rotator Cuff Tears. Anatomy. Description
 Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
Refer to Specialist. The Diagnosis and Management of Shoulder Pain 1. SLAP lesions, types 1 through 4
 The Diagnosis Management of Shoulder Pain 1 Significant Hisry -Age -Extremity Dominance -Hisry of trauma, dislocation, subluxation -Weakness, numbness, paresthesias -Sports participation -Past medical
The Diagnosis Management of Shoulder Pain 1 Significant Hisry -Age -Extremity Dominance -Hisry of trauma, dislocation, subluxation -Weakness, numbness, paresthesias -Sports participation -Past medical
Injuries to Upper Limb
 Injuries to Upper Limb 1 The following is a list of common sporting conditions and injuries. The severity of each condition may lead to different treatment protocols and certainly varying levels of intervention.
Injuries to Upper Limb 1 The following is a list of common sporting conditions and injuries. The severity of each condition may lead to different treatment protocols and certainly varying levels of intervention.
Chapter 5. The Shoulder Joint. The Shoulder Joint. Bones. Bones. Bones
 Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. Chapter 5 The Shoulder Joint Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Structural Kinesiology The Shoulder Joint 5-1 The Shoulder
Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. Chapter 5 The Shoulder Joint Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Structural Kinesiology The Shoulder Joint 5-1 The Shoulder
Combined lesions of the glenoid labrum include labral
 9(1):10 14, 2008 Ó 2008 Lippincott Williams & Wilkins, Philadelphia T E C H N I Q U E Arthroscopic Repair of Combined Labral Lesions MAJ Brett D. Owens, MD, Bradley J. Nelson, MD, and COL Thomas M. DeBerardino,
9(1):10 14, 2008 Ó 2008 Lippincott Williams & Wilkins, Philadelphia T E C H N I Q U E Arthroscopic Repair of Combined Labral Lesions MAJ Brett D. Owens, MD, Bradley J. Nelson, MD, and COL Thomas M. DeBerardino,
ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE
 ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE Christopher Mings, LAT, ATC University of Central Florida Alumnus & Florida Gulf Coast University Graduate
ACUTE AVULSION FRACTURE OF THE ANTERIOR SUPERIOR ILIAC SPINE IN A HIGH SCHOOL TRACK AND FIELD ATHLETE Christopher Mings, LAT, ATC University of Central Florida Alumnus & Florida Gulf Coast University Graduate
Distal Radius Fractures. Lee W Hash, MD Affinity Orthopedics and Sports Medicine
 Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
Bankart Repair Protocol
 Bankart Repair Protocol The Bankart procedure is performed to increase anterior stability of the shoulder. The following is a guideline for progression of post-operative treatment. General Information
Bankart Repair Protocol The Bankart procedure is performed to increase anterior stability of the shoulder. The following is a guideline for progression of post-operative treatment. General Information
Scaphoid Fracture of the Wrist
 Page 1 of 6 Scaphoid Fracture of the Wrist Doctors commonly diagnose a sprained wrist after a patient falls on an outstretched hand. However, if pain and swelling don't go away, doctors become suspicious
Page 1 of 6 Scaphoid Fracture of the Wrist Doctors commonly diagnose a sprained wrist after a patient falls on an outstretched hand. However, if pain and swelling don't go away, doctors become suspicious
SHOULDER - TORN ROTATOR CUFF
 175 Cambridge Street, 4 th floor ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade
175 Cambridge Street, 4 th floor ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA
 Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
RADIOGRAPHIC EVALUATION
 Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
Lateral Epicondylitis Surgical Treatment and Rehabilitation
 1 Lateral Epicondylitis Surgical Treatment and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: Lateral epicondylitis primarily involves the origin of the extensor carpi
1 Lateral Epicondylitis Surgical Treatment and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: Lateral epicondylitis primarily involves the origin of the extensor carpi
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Sports Injuries of the Foot and Ankle. Dr. Travis Kieckbusch August 7, 2014
 Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Shoulder MRI for Rotator Cuff Tears. Conor Kleweno,, Harvard Medical School Year III Gillian Lieberman, MD
 Shoulder MRI for Rotator Cuff Tears Conor Kleweno,, Harvard Medical School Year III Goals of Presentation Shoulder anatomy Function of rotator cuff MRI approach to diagnose cuff tear Anatomy on MRI images
Shoulder MRI for Rotator Cuff Tears Conor Kleweno,, Harvard Medical School Year III Goals of Presentation Shoulder anatomy Function of rotator cuff MRI approach to diagnose cuff tear Anatomy on MRI images
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
