Network Security & Privacy Risks in the Health Care Industry
|
|
|
- Juniper Johns
- 8 years ago
- Views:
Transcription
1 Network Security & Privacy Risks in the Health Care Industry May 2012 Aon Broking - Professional Risk Solutions 2012 Aon plc Brief Description: Conditions are ripe for health care organizations to fall prey to cyber risk. Many individuals have access to PHI and PII, both inside and outside any given health care organization. Networks and systems must be configured so that these parties can access information with speed and accuracy, while minimizing the risk of this information being compromised. The desires for enhanced efficiency and improvements in patient care (as well as HITECH incentives) have led to an explosion in the adoption of advanced health information technology. The convenience and promise of mobile and tablet computing in a clinical setting have also led to a proliferation of new, potentially less secure methods of accessing and sharing this information. Finally, due in part to budgetary pressures, health care entities are relying on outsourced service providers, ranging in scale from payment processing to lab test processing. Lax procedures by a vendor can lead to catastrophic damage to a covered entity. While insurance products professing to address these risks have been around for years, they have recently become increasingly responsive to real claim situations, and proactive health care entities have made a cyber or network security and privacy liability program a standard purchase. It is critical to work with a broker specializing in this coverage, as policy forms and insurer appetites are incredibly dynamic, just like the risks themselves.
2 Introduction Potential privacy liability risks are not limited to those organizations that directly provide health care services. Any organization that touches or handles Personally Identifiable Information (PII) and/or Protected Health Information (PHI) is exposed to these risks in some form, regardless of whether or not they are subject to the Security and Privacy Rules in the Health Insurance Portability and Accountability Act (HIPAA). There is a long list of potentially affected organizations: patient care organizations (providers), insurance companies (payors), third party administrators, technology firms creating software and hardware for the health care industry, pharmacy benefit managers, outsourced network service providers, data storage firms, Health Information Exchanges, etc. This paper is intended to give the reader a concise view of the privacy risk landscape for the health care industry. We begin with the unique and rapidly evolving risk profile, we then summarize the regulatory and enforcement environment, provide examples of some high-profile actual incidents, and offer risk management solutions, and finally, discuss the risk transfer marketplace. Key Terms Protected Health Information (PHI) as defined by HIPAA Individually identifiable health information is information that is a subset of health information, including demographic information collected from an individual, and: Is created or received by a health care provider, health plan, employer, or health care clearinghouse; and Relates to the past, present, or future physical or mental health or condition of an individual; the provision of health care to an individual; or the past, present, or future payment for the provision of health care to an individual; and o That identifies the individual; or o With respect to which there is a reasonable basis to believe the information can be used to identify the individual. Personally Identifiable Information (PII) There is no single, definitive statutory definition of PII. Various laws and various insurance carriers may each define the term in a slightly different way. Generally, it means any non-public personal information from which an individual can be reliably and uniquely identified as an individual, such as name in combination with address, telephone number, or social security number. 1
3 Risk Profile & Exposure Channels Due to the nature of operations and the use of PII/PHI in almost all facets of the organization, health care firms have more channels of exposure than those in many other industries, including: Many Users Many individuals have access to PII/PHI both within a health care organization (physicians, nurses, accounts receivable, etc.), and externally (pharmacies, insurance companies, outsourced service providers). Additionally, the continued introduction of new services, such as sizeable client facing web interfaces, opens new and evolving channels of exposure. These numerous users of PII/PHI heighten the probability of error leading to a breach. The human dynamic is critical to the exposure equation, as illustrated by a recent study that concluded that 40% of all major PHI breaches in 2011 were caused by human error 1. Scope of Network Operations In order to facilitate availability for the numerous parties described above, network systems must be configured to allow for multiple points of access. Outsourced Information Technology (IT) entities and other service providers may also have direct access to the health care organization s network, thus increasing exposures. Additionally, some larger health care entities have semiautonomous subsidiaries with little or no connectivity to the master network, which increases the perceived risk of the parent organization. Business Associates HIPAA defines third parties with access to the PHI collected by health plans, health care clearinghouses, and certain health care providers (i.e. Covered Entities) as Business Associates. These Business Associates may perform a variety of functions for or on behalf of a Covered Entity, and they are becoming increasingly prevalent. The nature of services or outsourced operations may range in scale from payment processing, to utilization review, to lab test processing. The cost savings of outsourcing arrangements can be very attractive, but these arrangements also change the organization s risk profile because of the increase in number of users, additional access and transfer points, loss of control, and potential inconsistencies in network security and privacy protocols. Information Technology Implementation Much like outsourcing, the modernization of operations and implementation of the latest technologies can result in tremendous cost savings if performed effectively. The downside, however, can be system integration problems, employee training hurdles, and unknown bugs or system glitches that can facilitate a breach of confidential information. A great deal of the focus in health care technology surrounds the creation and implementation of Electronic Health Records (EHRs) and Personal Health Records (PHRs). These efforts began in 2004 when a presidential mandate created the Office of the National Coordinator for Health Information Technology (ONC), a group dedicated to the advancement and development of 2
4 Health care industry IT. The creation of ONC also triggered an explosion of government committees and industry alliances that have produced volumes of guidance on EHR standards, which focus on functionality, availability, interoperability, and security. The original focus of Health IT initiatives was national interoperability, but information security and privacy have become top priorities for entities wishing to avoid the increasing probability of audits and fines. Every entity subject to HIPAA regulation should be keenly aware of compliance with the Security Rule (HIPAA established standards and implementation specifics that organizations must meet in order to become compliant) and must work to make sure the conversion to EHRs is accomplished with proper security protocols in place. Health IT meaningful use incentives in the Health Information Technology for Economic and Clinical Health Act (HITECH Act, discussed further below) have sped the adoption of EHR and e-prescribing systems. Accountable Care Organizations and Health Information Exchanges With the advent of Accountable Care Organizations (ACOs), experts anticipate that Electronic Health Information Exchanges (HIEs) will become critical to enhancing patient outcomes and care. Increased reliance on electronic information sharing and technology support tools will be as critically important to ACOs deriving value from government incentives, as well as delivering better patient outcomes. As ACOs seek to rely on evidence-based medicine, they will need to develop and utilize more electronic information repositories. Additionally, as they engage patients, they may reach out and create new forms of social media discussion with individual patients, as well as rely on electronic and mobile communication at new levels. For efficiency purposes, reporting on quality and cost will certainly need to be automated through electronic reporting mechanisms. Finally, coordination of care will lean on technologies beyond electronic health records and electronic health information exchanges, such as remote patient monitoring systems and web-based patient-provider interaction. In order to maintain patient trust and safety, as well as to maintain compliance with applicable state and federal law, the privacy and security of new technologies must be front and center for every ACO. Coordination of information and systems will be a challenge in an ACO context as there are likely to be several distinct providers, payors, technology service providers, and potentially one or more health information exchanges sharing data. Each of these stakeholders may have its own Information Security personnel and philosophy, and beyond ensuring that the electronic systems are interoperable, those departments must work together to ensure that they are also sufficiently private and secure. State and federal consumer reporting requirements in the event of a breach may also be complicated due to overlapping business associate agreements requiring notification to affected consumers, applicable covered entities, regulatory agencies, or all three. It is critical for ACOs to ensure that contractual arrangements between unrelated parties specifically address who will take responsibility and bear the cost of notification and consumer communication in the event of a breach of confidential information. Miscellaneous Numerous other factors can also contribute to liability scenarios, including whether a health care organization provides any services to unrelated entities. For example, many community hospitals hire larger health systems to provide services which include implementing, installing, and servicing IT platforms for clinical care and billing. The larger health system may do the training, the sales, the onsite installation, or miscellaneous functions, thus increasing its liability exposure. Additionally, if the services provided include the use or handling of the PII/PHI of the client, the service provider is likely to be held 3
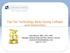
5 responsible for any breaches. The smaller entity on the receiving end of such services should ensure that contractual allocations of liability and insurance provisions are drafted to provide maximum protection. Major Regulatory Concerns The protection of PII in general is currently governed by a patchwork of state and federal laws that target different exposures and different entities. Some of these statutes include HIPAA, Gramm-Leach Bliley Act (GLBA), Fair Credit Reporting Act, Sarbanes-Oxley Act (SOX), Privacy Act of 1974, and others. There are a multitude of regulations in place, but those most applicable to the health care industry in the United States can be separated into federal and state regulation. While we do not outline the international privacy regulatory landscape in this paper, it is important for any U.S. based health care entity treating international patients or doing business outside the U.S. to be cognizant that a variety of a privacy laws exist outside the U.S. U.S. Federal Laws Health Insurance Portability and Accountability Act (HIPAA) Passed in 1996, HIPAA was one of the first statutes that specifically addressed any form of confidential or personal information. The HIPAA framework contains both a Privacy Rule (passed in 2002) that outlines and limits the way PHI in any form can be disclosed, and a Security Rule (passed in 2003) that loosely dictates protocols for the protection of electronic PHI, and, as well as provisions for fines or penalties in the event of non-compliance with either rule. Organizations violating this regulation went without penalty for years, but about the time of the passage of the HITECH Act in 2009, HIPAA finally gained teeth, and enforcement by the Office of Civil Rights (OCR) increased significantly. HIPAA Resolved Complaints/Investigations & Fines (Office of Civil Rights Enforcement Data 2 ) $6,000,000 $5,000,000 $4,000,000 $3,000,000 $2,000,000 $1,000,000 $0 10,000 9,000 8,000 7,000 6,000 5,000 4,000 3,000 2,000 1,000 0 Total Fines ($) Total Resolutions (#) 4
6 Health Information Technology for Economic and Clinical Health Act (HITECH) Included as part of the American Recovery and Reinvestment Act of 2009 (ARRA), HITECH was intended to stimulate the adoption of electronic health records, accelerate the development of a nationwide health information exchange, and strengthen the privacy and security of PHI. HITECH expanded the reach of HIPAA in several important ways that have significantly affected the way Covered Entities and Business Associates view security and privacy liability insurance buying decisions and coverage. HITECH subjected Business Associates, and not just Covered Entities, to HIPAA s Privacy Rule and the Security Rule, both of which loosely govern the ways these entities must protect PHI. Consequently, civil and criminal penalties under HIPAA are now applicable to Business Associates as well as Covered Entities. HITECH also created the first federal breach disclosure law, and all entities suffering a breach of 500 or more individuals now must report the details and see them immortalized on the OCR website s wall of shame 3. U.S. State Laws State Breach Disclosure Laws Until HITECH, there was no federal breach disclosure mandate, but many of the 49 U.S. state and territory breach notification statutes already covered PHI. While some states allow exceptions for breaches involving encrypted data, most require swift public disclosure of any potential breach of personally identifiable information. Some of these statutes have provisions that exempt entities subject to HIPAA, but only to the extent that the offending entity already has security, privacy, and notification policies in place. State Data Protection Laws (MN, MA, NV, WA) Minnesota amended its data breach notification law to hold entities suffering a breach, as opposed to the issuing banks, responsible for the costs of re-issuing credit cards in the event of a data breach. The law, which was passed in the wake of the TJX security breach, can certainly pertain to health care organizations as it applies to any entity accepting credit cards, debit cards, or other stored value cards. The statute requires companies to reimburse card-issuing financial institutions for the costs of reasonable actions to both protect its cardholders information and to provide post-breach services to its cardholders. Washington has passed a similar law, HB 1149, which allows financial institutions to seek card reissuance costs from a breached entity. Interestingly, Washington s law offers safe harbor if the breached entity was found to be PCI compliant in the preceding year, but does not require entities to comply with PCI. Nevada s SB 227 modifies the state s breach disclosure law to include a requirement for compliance with PCI, a requirement for encryption, and a very limited safe harbor from liability. As of January 1, 2010, Massachusetts began enforcing its new, strict data protection regulations. The Massachusetts Regulation impacts almost every business that stores personal data of Massachusetts employees and residents (whether or not the company operates in Massachusetts, over the Internet or otherwise) and will require significant security and policy changes for most businesses. The Massachusetts Regulation requires, among other things, the encryption of wireless transmissions of personal information and the encryption of personal information stored on portable devices carrying personal information such as laptops, flash drives and PDAs. 5
7 Confidentiality of Medical Information Act (CMIA; CA) California s Confidentiality of Medical Information Act (CMIA) requires health care providers to maintain the privacy and confidentiality of medical information. CMIA allows certain disclosures without patient authorization, such as disclosures to a payor for reimbursement purposes, or disclosures ordered by a court. This law is worth specifically noting because it provides a private right of action and related statutory damages of $1,000 - $3,000 per record wrongfully disclosed. It also contains provisions for civil penalties up to $250,000. Violations of CMIA have been cited in many high profile data breach lawsuits in the past year, including those against Stanford Hospital and Sutter Health, and the statutory damage amounts have even been referenced as a benchmark in data breach cases in other states. Health Care Privacy Incidents Health care privacy incidents can involve PHI and PII in any form or media, whether electronic, paper or oral. According to the Ponemon Institute s December 2011 Patient Privacy & Data Security Study 4, health care data breaches cost breached organizations an average of $2.2M. However, it is clear from high-profile breach incidents that a catastrophic breach with an unfavorable legal or regulatory outcome or a unique incident investigation fact pattern may cost an organization far more. Some of these incidents are further detailed below: Government Health Care Organization A laptop and external hard drive containing sensitive data (name, date of birth, and social security numbers) on over 26,500,000 veterans were stolen from an employee s home. Incident response & investigation The FBI launched an investigation, and the equipment was subsequently anonymously returned. Several of the organization s employees left the company due to public outrage over the breach, however it was eventually determined that no information on the devices had been improperly accessed. Litigation & Settlement After three years of litigation by the victims of this data breach, a federal judge approved a $20,000,000 settlement. Health Care Network In two separate incidents, the unencrypted confidential information of over 4,200,000 patients was compromised due to theft. Incident response The company set up a website and call center where affected individuals could call for additional information. Since the information did not include social security numbers or financial 6
8 information, typical credit monitoring services were not offered. The website also assured patients that the company was accelerating efforts to deploy encryption across the organization. Litigation / enforcement proceedings The initial class action complaint was filed on the same day as the patient notifications were mailed, causing many to call it a zero-day lawsuit. 12 additional class action lawsuits were filed, and all such complaints were consolidated within three months. Regulatory actions are likely to follow. Health Insurance Plan Hard drives containing close to 1,000,000 member records were stolen from an off-site facility. Incident response The company hired outside forensic experts and temporary employees to perform a manual review of backup files and assess the scope of the breach and identify the individuals affected, as well as sent written notification including an offer of credit protection services to the individuals. The company publicly disclosed that their cost for breach response exceeded $10,000,000. Litigation / enforcement proceedings HHS OCR initiated an investigation into the incident, and eventually levied a $1,500,000 fine, even though there was no evidence that any affected consumers had actually been harmed. Several state AGs have requested additional information. Outcome The company s proactive and open communication throughout the breach response has been cited as a model response by multiple experts, and the fact that they were still fined could be an unwelcome harbinger of the future direction of HIPAA enforcement. Risk Management Strategies Technology & Strategy It is critical that each health care organization use technology that complements its security policy and a multitude of products have been specifically designed to fit the changing needs of the health care community. Additionally, because health care is an ever-changing industry and also one that is guided by stringent regulations, the technologies employed must keep pace with the current environment. Health care organizations have struggled to combine standards like HIPAA, ISO 27001/27002 (formerly 27799), COBIT, PCI, and their own best practices into a comprehensive framework for information security and privacy. An innovative group called the HITRUST Alliance has created what they hope will 7
9 become the industry standard Common Security Framework. The group was formed with input from many industry leaders and is a good resource for those responsible for IT and risk management. Health care Information and Management Systems (HIMSS) is a not for profit organization dedicated to advancing Health Information Technology. HIMSS provides thought leadership and guidance on a wide variety of Health IT topics. It s important for health care providers to ensure that any new technology being implemented has been fully tested and certified. Only six organizations 5 are currently approved to certify that Health IT systems meet meaningful use requirements, including security provisions. One such approved body is Certification Commission for Health Care Information Technology (CCHIT), which was developed jointly by HHS and several leading industry groups in CCHIT certifies technology vendors and their products for effective use in the health care community and compliance with the meaningful use requirements in the ARRA and is also a great resource for those responsible for HIT procurement. Contractual Allocation of Risk An increasing number of data privacy incidents are attributed to business associates one study found that 59% of 2011 breaches involved external partners, consultants, outsourcers and contractors. Although it is critical to determine the proper allocation of liability when PII/PHI is shared for business purposes, many providers focus largely on compliance with requirements to have a business associate agreement (BAA) in place, rather than maximizing the vendor risk assessment opportunity and risk transfer that a well crafted BAA can provide. The failure to address these issues proactively can result in confusion and disarray when a breach occurs. Here are two real life examples of outsourced services with breach scenarios that even the most creative risk manager might not have imagined: TranscriptionStat handled the large hospital s transcription work for over twenty years until a rogue transcriptionist outsourced her work to a Pakistani sub-contractor without the approval of her employer or the hospital. The sub-contractor then threatened to post the confidential medical information unless she was paid a certain amount of money. 6 Thankfully, this debacle was resolved before the information was exposed. More recently, Stanford Hospital & Clinics was brought into a high-profile lawsuit as a result of an outside vendor, Multi-Specialty Collection Services, improperly sharing actual patient data with its marketing vendor, Corcino & Associates. The marketing vendor shared a spreadsheet containing the PHI of 20,000 emergency room patients with a job applicant to test her computer skills. She in turn posted the spreadsheet on a public homework help website, where it was discovered by a patient. 8
10 Both were governed by a standard outsourcing arrangement and both highlight the unforeseen liability issues health care firms face. Appropriate contractual provisions in business associate agreements and outsourced services arrangements can mitigate the effect of these situations by clearly defining responsibility, ensuring the proper precautions are taken when the information is out of the control of the health care organization, and limiting the liability of, or ensuring indemnity for, the health care organization in the unfortunate event of a data breach. While an organization should first rely on pre-negotiated indemnification from the vendor in such a situation, we strongly recommend that insurance requirements be put in place to help ensure that the vendor is able to back up its obligations. We suggest starting with a broadly defined, but specific insurance provision along the following lines: Errors & Omissions/Professional Liability Insurance, in an amount not less than $X,000,000 per claim and annual aggregate, covering all acts, errors, omissions, negligence, infringement of intellectual property (except patent and trade secret); network security and privacy risks, including but not limited to unauthorized access, failure of security, breach of privacy perils, wrongful disclosure, collection, or other negligence in the handling of confidential information, privacy perils, and including coverage for related regulatory defense and penalties; data breach expenses, in an amount not less than $X,000,000 and payable whether incurred by <Client> or <Vendor>, including but not limited to consumer notification, whether or not required by law, computer forensic investigations, public relations and crisis management firm fees, credit file or identity monitoring or remediation services in the performance of services for <Client> or on behalf of <Client> hereunder. The policy shall contain an affirmative coverage grant for contingent bodily injury and property damage emanating from the failure of the technology services or an error or omission in the content/information provided. If a sub-limit applies to any elements of coverage, the certificate of insurance evidencing the coverage above must specify the coverage section and the amount of the sub-limit. Such insurance shall be maintained in force at all times during the term of the agreement and for a period of X years thereafter for services completed during the term of the agreement. <Client> shall be given at least 30 days notice of the cancellation or expiration of the aforementioned insurance for any reason. Depending on the specific situation, for example if the Business Associate won t be providing a professional service, the requirement may be scoped down accordingly. It is critical that companies work collaboratively with legal counsel and insurance professionals to ensure the pieces of the contractual risk allocation puzzle mesh correctly. 9
11 Insurance Coverage All insureds should review their traditional insurance policies to determine the exact scope of coverage for data breaches. However, carriers who offer traditional property and casualty policies are rapidly creating stand-alone Network Security & Privacy Liability (NSP) offerings. In order to promote adoption of these specialized policies, they are inserting more and more broad exclusionary language in traditional policies. General Liability and Property Policies Changes in 2004 to the Insurance Service Organization ( ISO ) forms, as well as some insurance litigation, have limited the coverage available under traditional general liability and property forms and exclusions are becoming more common as general liability carriers offer standalone network security and privacy policies. Additionally, an increasing number of health care Risk Retention Groups are formalizing exclusions for all Cyber Risks. Health Care Provider Professional Liability In the health care space, Professional Liability policies are intended to cover third party damages and personal/bodily injury from errors, omissions or negligent acts in the course of medical care and related administrative services. It is possible to endorse security and privacy coverage on to some Health Care Professional Liability policies. Most health care entities have elected to keep their Security and Privacy programs separate to avoid a shared limit and retention and to take full advantage of the marketplace, because only a limited number of carriers will combine the programs. Other Insurance Policies Depending upon the facts of the data breach and the particular wording of the policies, some coverage could exist in various other policies, including Commercial Crime Policies, Employment Related Practices Policies, Data Processing Policies, Computer Fraud Policies, Advertising, or Kidnap and Ransom Policies. For instance, if a hacker claims that confidential information will be distributed on the Internet unless the insured pays some type of extortion fee, some Kidnap and Ransom policies may provide defense and indemnity coverage. In general, such policies were not intended to cover privacy/data breaches and there are significant coverage gaps in each. Security & Privacy Liability Coverage Most dedicated policies are provided on a modular basis, so we ve summarized each module below. Breach Event Expenses Triggered by discovery of an privacy incident This component of coverage provides reimbursement for the insured s costs to respond to a data privacy or security incident. This module is triggered either by the discovery of such an event, or a statutory obligation to notify consumers of such an event. Covered expenses can include breach-related legal assistance, computer forensics expenses, costs for a public relations firm and related advertising to restore your reputation, consumer notification, and consumer credit monitoring services. Carriers provide 10
12 widely varying levels of control and service in this area. Most carriers provide this coverage as a sublimit within the overall policy aggregate, though some offer outside the limit. Liability Coverage Parts Triggered by a third party demand or suit Security Liability This module covers defense costs and damages suffered by others resulting from a failure of computer security, including liability caused by theft or disclosure of confidential information, unauthorized access, unauthorized use, denial of service attack or transmission of a computer virus. It is almost always combined with the Privacy Liability module below. Privacy Liability This module covers defense costs and damages suffered by others for any failure to protect personally identifiable or confidential corporate information, whether or not due to a failure of network security. Some policies include: unintentional violations of the insured s privacy policy, actions of rogue employees, and/or the alleged wrongful collection of confidential information. Regulatory Proceedings This coverage, which is generally a sub-set of the Security and Privacy modules, covers defense costs for proceedings brought by a governmental agency in connection with a failure to protect private information and/or a failure of network security. Coverage is typically sub-limited and may include (depending on insurer) coverage for fines and penalties to the extent insurable by law. Compensatory damages, i.e. amounts the insured is required by a regulator to deposit into a consumer redress fund, may be covered at full limits depending on the insurer. Media Liability This module can extend the scope of the insured s personal and advertising injury coverage in a general liability policy. The module covers defense costs and damages suffered by others for content-based injuries such as libel, slander, defamation, copyright infringement, trademark infringement, or invasion of privacy. The scope of covered media is variable and can range from the insured s website only to all content in any medium. Cyber Extortion Triggered by a threat to cause a security failure or privacy breach This component, also called Network Extortion, reimburses the insured for expenses incurred in the investigation of a cyber threat and any extortion payments made to prevent or resolve the threat. Payments are generally subject to full discretion by insurer, and insurers offer varying levels of service along with the reimbursement. 11
13 First Party Coverage Parts Business Interruption This section reimburses the insured for actual lost income caused by a computer network security failure, as well as associated extra expense. Dependent business interruption is also available, but it is often subject to a sub-limit. In addition to a dollar amount retention, a waiting period retention of between 6 to 24 hours is usually applied. Digital Asset Protection This module reimburses the insured for costs incurred to restore or recollect intangible, non-physical assets (software or data) that are corrupted, destroyed or deleted due to a covered computer network security failure. Health care entities considering this coverage should note that the Business Interruption and Digital Asset coverage parts have not been especially relevant to the health care industry. There are exceptions, however, and one example is an entity whose primary revenue stream is from network/internet activities, such as online pharmacies. Additionally, there have been very few first party claims paid by any insurer and significant hurdles to coverage exist, such as waiting periods of 6-24 hours before coverage applies and difficulty in valuing intangible assets and business interruption costs. Evaluating Coverage Features and Exclusions Each carrier addresses the risks in a different manner, so it is essential that the insured review the policy form and work with their broker to customize it to their specific exposures. There are many other distinct issues to consider on a case by case basis, but the following basic checklist can be used in the initial evaluation process: Does the policy include media liability? Is it broader than our GL policy s AI/PI grant? Does it contemplate social media exposure? How does the policy treat coverage for rogue employees? Employee claimants? Will the policy respond if our vendor causes a breach? Is there a separate retention for breach response expenses? How broad is the regulatory claim trigger? Are fines and penalties covered? If we make an acquisition, how does the policy respond? Will we be able to use our preferred law firm in the event of a claim? Will their rates be fully covered? Does the carrier have a duty to defend? Does it apply to claims as well as regulatory actions? What exclusions exist for breaches that we aren t aware of, but may already be ongoing? When do I provide notice of a claim or incident, and what qualifies as a covered claim? Does the policy exclude unencrypted or unprotected data or devices? 12
14 What other exclusions should we be specifically concerned about, and what corresponding uncovered claim scenarios could arise? Breach response expenses are perhaps the most differentiated area of coverage, and a specific set of questions apply to that element: Is the trigger a reasonable belief that identity theft may occur as a result of a particular incident, or is it tied to statutory obligations only? Does the policy only pay those costs the insured is required to incur by law or does it provide for voluntary expenses such as providing credit monitoring in a state where the law does not require it? Is the insurer s prior written consent required before coverage will apply? Is there a reasonableness standard for consent? Are costs incurred solely to mitigate damage to the insured s reputation covered? What time constraints apply? Can the insured recover costs under this coverage part more than one year after a breach? Does coverage apply on a per individual basis or is a set dollar amount available? Does coverage erode the available limit of liability or is it provided outside and in addition to the limit? Do the covered expenses mesh with the insured s crisis response plan? Are the insured s preferred crisis management vendors pre-approved? Insurance Marketplace & Benchmarking The market for Security and Privacy Liability remains competitive, with favorable risks with clean loss history renewing flat, and carriers continuing to solicit new insureds. Many experienced markets have now paid large claims and regulatory costs, and are becoming more inquisitive in their underwriting process and wary of taking on insureds without state of the art controls. Benchmarking in this area is of limited value as it is difficult to categorize insureds and because each underwriting situation is based on many different factors such as revenues, patient statistics, loss history, information security posture, contractual allocation of liability and number/accessibility of data records. Many forward looking health care entities are basing their limit and retention decisions on data breach cost modeling, such as the ID Experts PHIve 7 method, which quantifies the value of PHI for both risk transfer and IT security investment purposes, or on modeling based on peer loss experience. There are at least fifteen carriers that can provide a primary program for health care entities, with capacity to build in excess of $100,000,000 in total limits. Retentions generally fall in the $250,000 - $500,000 range, but can be as low as $10,000 or as high as $10,000,000 depending on risk tolerance and exposure. Pricing for a stand alone program varies widely but usually falls within a range of $10,000 to $35,000 per million of coverage. Very large organizations or those with weaker security and privacy controls may be forced to take higher retentions and pay premiums in excess of $50,000 per million. 13
15 Underwriting Process The first step in the underwriting process is the completion of an application and/or self-assessment. It is important that the risk management team engage the appropriate information security and privacy personnel in the application process to provide complete and accurate information. The assessment and application process also provides an opportunity to critically examine an entity s information risk management strategies. In conjunction with the base application, a potential insured should be prepared to provide the following: Copies of privacy policies Standard contracts and Business Associate Agreements Results of any external or internal audits or assessments that illustrate the information security posture Details of any security breach incidents and the response to them, including any new protocols put in place to prevent similar incidents Financial information Patient statistics Aon recommends that, as part of a comprehensive risk management strategy, health care entities work with experienced brokers who are experts in Security and Privacy coverage and the corresponding legal issues and who have a thorough understanding of the evolving dynamics of both health care and the insurance marketplace. The underwriting process must be skillfully managed and the complexity of coverage demands innovation and expertise. Those companies who successfully utilize these resources in their risk management process will realize the benefits of this enhanced coverage. 14
16 Contact Information Sarah Stephens Vice President Aon Risk Solutions Financial Services Group Professional Risk Solutions 199 Fremont, Suite 1500 San Francisco, CA t sarah.stephens@aon.com How to cite this publication Individuals are encouraged to cite this report and any accompanying graphics in printed matter, publications, or any other medium, as long as the information is attributed to the cited source or to Aon plc. About Aon Aon plc (NYSE: AON) is the leading global provider of risk management, insurance and reinsurance brokerage, and human resources solutions and outsourcing services. Through its more than 61,000 colleagues worldwide, Aon unites to empower results for clients in over 120 countries via innovative and effective risk and people solutions and through industry-leading global resources and technical expertise. Aon has been named repeatedly as the world's best broker, best insurance intermediary, reinsurance intermediary, captives manager and best employee benefits consulting firm by multiple industry sources. Visit for more information on Aon and to learn about Aon's global partnership and shirt sponsorship with Manchester United. 1 Breach Report 2011; Protected Health Information Protecting PHI and Responding to Data Thefts, Davis Wright Tremaine LLP, Randy Gainer and John McGrory
Cyber and Privacy Risk What Are the Trends? Is Insurance the Answer?
 Minnesota Society for Healthcare Risk Management September 22, 2011 Cyber and Privacy Risk What Are the Trends? Is Insurance the Answer? Melissa Krasnow, Partner, Dorsey & Whitney, and Certified Information
Minnesota Society for Healthcare Risk Management September 22, 2011 Cyber and Privacy Risk What Are the Trends? Is Insurance the Answer? Melissa Krasnow, Partner, Dorsey & Whitney, and Certified Information
Data breach, cyber and privacy risks. Brian Wright Lloyd Wright Consultants Ltd
 Data breach, cyber and privacy risks Brian Wright Lloyd Wright Consultants Ltd Contents Data definitions and facts Understanding how a breach occurs How insurance can help to manage potential exposures
Data breach, cyber and privacy risks Brian Wright Lloyd Wright Consultants Ltd Contents Data definitions and facts Understanding how a breach occurs How insurance can help to manage potential exposures
Joe A. Ramirez Catherine Crane
 RIMS/RMAFP PRESENTATION Joe A. Ramirez Catherine Crane RISK TRANSFER VIA INSURANCE Most Common Method Involves Assessment of Risk and Loss Potential Risk of Loss Transferred For a Premium Insurance Contract
RIMS/RMAFP PRESENTATION Joe A. Ramirez Catherine Crane RISK TRANSFER VIA INSURANCE Most Common Method Involves Assessment of Risk and Loss Potential Risk of Loss Transferred For a Premium Insurance Contract
Insurance Considerations Related to Data Security and Breach in Outsourcing Agreements
 Insurance Considerations Related to Data Security and Breach in Outsourcing Agreements Greater New York Chapter Association of Corporate Counsel November 19, 2015 Stephen D. Becker, Executive Vice President
Insurance Considerations Related to Data Security and Breach in Outsourcing Agreements Greater New York Chapter Association of Corporate Counsel November 19, 2015 Stephen D. Becker, Executive Vice President
Cyber Exposure for Credit Unions
 Cyber Exposure for Credit Unions What it is and how to protect yourself L O C K T O N 2 0 1 2 www.lockton.com Add Cyber Title Exposure Here Overview #1 financial risk for Credit Unions Average cost of
Cyber Exposure for Credit Unions What it is and how to protect yourself L O C K T O N 2 0 1 2 www.lockton.com Add Cyber Title Exposure Here Overview #1 financial risk for Credit Unions Average cost of
GALLAGHER CYBER LIABILITY PRACTICE. Tailored Solutions for Cyber Liability and Professional Liability
 GALLAGHER CYBER LIABILITY PRACTICE Tailored Solutions for Cyber Liability and Professional Liability Are you exposed to cyber risk? Like nearly every other business, you have probably capitalized on the
GALLAGHER CYBER LIABILITY PRACTICE Tailored Solutions for Cyber Liability and Professional Liability Are you exposed to cyber risk? Like nearly every other business, you have probably capitalized on the
Coverage is subject to a Deductible
 Frank Cowan Company Limited 75 Main Street North, Princeton, ON N0J 1V0 Phone: 519-458-4331 Fax: 519-458-4366 Toll Free: 1-800-265-4000 www.frankcowan.com CYBER RISK INSURANCE DETAILED APPLICATION Notes:
Frank Cowan Company Limited 75 Main Street North, Princeton, ON N0J 1V0 Phone: 519-458-4331 Fax: 519-458-4366 Toll Free: 1-800-265-4000 www.frankcowan.com CYBER RISK INSURANCE DETAILED APPLICATION Notes:
CYBER & PRIVACY LIABILITY INSURANCE GUIDE
 CYBER & PRIVACY LIABILITY INSURANCE GUIDE 01110000 01110010 011010010111011001100001 01100 01110000 01110010 011010010111011001100001 0110 Author Gamelah Palagonia, Founder CIPM, CIPT, CIPP/US, CIPP/G,
CYBER & PRIVACY LIABILITY INSURANCE GUIDE 01110000 01110010 011010010111011001100001 01100 01110000 01110010 011010010111011001100001 0110 Author Gamelah Palagonia, Founder CIPM, CIPT, CIPP/US, CIPP/G,
RISKY BUSINESS SEMINAR CYBER LIABILITY DISCUSSION
 RISKY BUSINESS SEMINAR CYBER LIABILITY DISCUSSION October 23, 2015 THREAT ENVIRONMENT Growing incentive for insiders to abuse access to sensitive data for financial gain Disgruntled current and former
RISKY BUSINESS SEMINAR CYBER LIABILITY DISCUSSION October 23, 2015 THREAT ENVIRONMENT Growing incentive for insiders to abuse access to sensitive data for financial gain Disgruntled current and former
Data Security Breaches: Learn more about two new regulations and how to help reduce your risks
 Data Security Breaches: Learn more about two new regulations and how to help reduce your risks By Susan Salpeter, Vice President, Zurich Healthcare Risk Management News stories about data security breaches
Data Security Breaches: Learn more about two new regulations and how to help reduce your risks By Susan Salpeter, Vice President, Zurich Healthcare Risk Management News stories about data security breaches
2009 HIMSS Analytics Report: Evaluating HITECH s Impact on Healthcare Privacy and Security
 2009 HIMSS Analytics Report: Evaluating HITECH s Impact on Healthcare Privacy and Security Commissioned by ID Experts November 2009 INTRODUCTION Healthcare breaches are on the rise; according to the 2009
2009 HIMSS Analytics Report: Evaluating HITECH s Impact on Healthcare Privacy and Security Commissioned by ID Experts November 2009 INTRODUCTION Healthcare breaches are on the rise; according to the 2009
Data breach! cyber and privacy risks. Brian Wright Michael Guidry Lloyd Guidry LLC
 Data breach! cyber and privacy risks Brian Wright Michael Guidry Lloyd Guidry LLC Collaborative approach Objective: To develop your understanding of a data breach, and risk transfer options to help you
Data breach! cyber and privacy risks Brian Wright Michael Guidry Lloyd Guidry LLC Collaborative approach Objective: To develop your understanding of a data breach, and risk transfer options to help you
Data Breach and Senior Living Communities May 29, 2015
 Data Breach and Senior Living Communities May 29, 2015 Todays Objectives: 1. Discuss Current Data Breach Trends & Issues 2. Understanding Why The Senior Living Industry May Be A Target 3. Data Breach Costs
Data Breach and Senior Living Communities May 29, 2015 Todays Objectives: 1. Discuss Current Data Breach Trends & Issues 2. Understanding Why The Senior Living Industry May Be A Target 3. Data Breach Costs
Cyber-Technology Policy Comparisons
 Cyber-Technology Policy Comparisons ABA Insurance Internet/Electronic Banking Liability Insurance Policy (04/01) January, 2011 Endorsements Topic ACE Computer & Technology Products and Services Professional
Cyber-Technology Policy Comparisons ABA Insurance Internet/Electronic Banking Liability Insurance Policy (04/01) January, 2011 Endorsements Topic ACE Computer & Technology Products and Services Professional
Cyber Liability. AlaHA Annual Meeting 2013
 Cyber Liability AlaHA Annual Meeting 2013 Disclaimer We are not providing legal advise. This Presentation is a broad overview of health care cyber loss exposures, the process in the event of loss and coverages
Cyber Liability AlaHA Annual Meeting 2013 Disclaimer We are not providing legal advise. This Presentation is a broad overview of health care cyber loss exposures, the process in the event of loss and coverages
Discussion on Network Security & Privacy Liability Exposures and Insurance
 Discussion on Network Security & Privacy Liability Exposures and Insurance Presented By: Kevin Violette Errors & Omissions Senior Broker, R.T. Specialty, LLC February, 25 2014 HFMA Washington-Alaska Chapter
Discussion on Network Security & Privacy Liability Exposures and Insurance Presented By: Kevin Violette Errors & Omissions Senior Broker, R.T. Specialty, LLC February, 25 2014 HFMA Washington-Alaska Chapter
Information Protection Framework: Data Security Compliance and Today s Healthcare Industry
 Information Protection Framework: Data Security Compliance and Today s Healthcare Industry Executive Summary Today s Healthcare industry is facing complex privacy and data security requirements. The movement
Information Protection Framework: Data Security Compliance and Today s Healthcare Industry Executive Summary Today s Healthcare industry is facing complex privacy and data security requirements. The movement
Managing Cyber & Privacy Risks
 Managing Cyber & Privacy Risks NAATP Conference 2013 NSM Insurance Group Sean Conaboy Rich Willetts SEAN CONABOY INSURANCE BROKER NSM INSURANCE GROUP o Sean has been with NSM Insurance Group for the past
Managing Cyber & Privacy Risks NAATP Conference 2013 NSM Insurance Group Sean Conaboy Rich Willetts SEAN CONABOY INSURANCE BROKER NSM INSURANCE GROUP o Sean has been with NSM Insurance Group for the past
Hit ratios are still very low for Security & Privacy coverage: What are companies waiting for?
 Hit ratios are still very low for Security & Privacy coverage: What are companies waiting for? Authored by Neeraj Sahni and Tim Stapleton Neeraj Sahni is Director, Insurance Channel at Kroll Cyber Investigations
Hit ratios are still very low for Security & Privacy coverage: What are companies waiting for? Authored by Neeraj Sahni and Tim Stapleton Neeraj Sahni is Director, Insurance Channel at Kroll Cyber Investigations
Reducing Risk. Raising Expectations. CyberRisk and Professional Liability
 Reducing Risk. Raising Expectations. CyberRisk and Professional Liability Are you exposed to CyberRisk? Like nearly every other business, you have likely capitalized on the advancements in technology today
Reducing Risk. Raising Expectations. CyberRisk and Professional Liability Are you exposed to CyberRisk? Like nearly every other business, you have likely capitalized on the advancements in technology today
Cyber Liability. Michael Cavanaugh, RPLU Vice President, Director of Production Apogee Insurance Group 877-337-3200 Ext. 7029
 Cyber Liability Michael Cavanaugh, RPLU Vice President, Director of Production Apogee Insurance Group 877-337-3200 Ext. 7029 Today s Agenda What is Cyber Liability? What are the exposures? Reality of a
Cyber Liability Michael Cavanaugh, RPLU Vice President, Director of Production Apogee Insurance Group 877-337-3200 Ext. 7029 Today s Agenda What is Cyber Liability? What are the exposures? Reality of a
INFORMATION SECURITY & PRIVACY INSURANCE WITH BREACH RESPONSE SERVICES
 INFORMATION SECURITY & PRIVACY INSURANCE WITH BREACH RESPONSE SERVICES NOTICE: INSURING AGREEMENTS I.A., I.C. AND I.D. OF THIS POLICY PROVIDE COVERAGE ON A CLAIMS MADE AND REPORTED BASIS AND APPLY ONLY
INFORMATION SECURITY & PRIVACY INSURANCE WITH BREACH RESPONSE SERVICES NOTICE: INSURING AGREEMENTS I.A., I.C. AND I.D. OF THIS POLICY PROVIDE COVERAGE ON A CLAIMS MADE AND REPORTED BASIS AND APPLY ONLY
ISO? ISO? ISO? LTD ISO?
 Property NetProtect 360 SM and NetProtect Essential SM Which one is right for your client? Do your clients Use e-mail? Rely on networks, computers and electronic data to conduct business? Browse the Internet
Property NetProtect 360 SM and NetProtect Essential SM Which one is right for your client? Do your clients Use e-mail? Rely on networks, computers and electronic data to conduct business? Browse the Internet
HIPAA BUSINESS ASSOCIATE AGREEMENT
 HIPAA BUSINESS ASSOCIATE AGREEMENT This HIPAA Business Associate Agreement ("BA AGREEMENT") supplements and is made a part of any and all agreements entered into by and between The Regents of the University
HIPAA BUSINESS ASSOCIATE AGREEMENT This HIPAA Business Associate Agreement ("BA AGREEMENT") supplements and is made a part of any and all agreements entered into by and between The Regents of the University
HIPAA Omnibus Compliance How A Data Loss Prevention Solution Can Help
 HIPAA Omnibus Compliance How A Data Loss Prevention Solution Can Help The Health Information Portability and Accountability Act (HIPAA) Omnibus Rule which will begin to be enforced September 23, 2013,
HIPAA Omnibus Compliance How A Data Loss Prevention Solution Can Help The Health Information Portability and Accountability Act (HIPAA) Omnibus Rule which will begin to be enforced September 23, 2013,
APIP - Cyber Liability Insurance Coverages, Limits, and FAQ
 APIP - Cyber Liability Insurance Coverages, Limits, and FAQ The state of Washington purchases property insurance from Alliant Insurance Services through the Alliant Property Insurance Program (APIP). APIP
APIP - Cyber Liability Insurance Coverages, Limits, and FAQ The state of Washington purchases property insurance from Alliant Insurance Services through the Alliant Property Insurance Program (APIP). APIP
Cyber and data Policy wording
 Please read the schedule to see whether Breach costs, Cyber business interruption, Hacker damage, Cyber extortion, Privacy protection or Media liability are covered by this section. The General terms and
Please read the schedule to see whether Breach costs, Cyber business interruption, Hacker damage, Cyber extortion, Privacy protection or Media liability are covered by this section. The General terms and
INFORMATION SECURITY AND PRIVACY INSURANCE WITH ELECTRONIC MEDIA LIABILITY COVERAGE. I. GENERAL INFORMATION Full Name:
 INFORMATION SECURITY AND PRIVACY INSURANCE WITH ELECTRONIC MEDIA LIABILITY COVERAGE NOTICE: COVERAGE UNDER THIS POLICY IS PROVIDED ON A CLAIMS MADE AND REPORTED BASIS AND APPLIES ONLY TO CLAIMS FIRST MADE
INFORMATION SECURITY AND PRIVACY INSURANCE WITH ELECTRONIC MEDIA LIABILITY COVERAGE NOTICE: COVERAGE UNDER THIS POLICY IS PROVIDED ON A CLAIMS MADE AND REPORTED BASIS AND APPLIES ONLY TO CLAIMS FIRST MADE
Network Security and Data Privacy Insurance for Physician Groups
 Network Security and Data Privacy Insurance for Physician Groups February 2014 Lockton Companies While exposure to medical malpractice remains a principal risk MIKE EGAN, CPCU Senior Vice President Unit
Network Security and Data Privacy Insurance for Physician Groups February 2014 Lockton Companies While exposure to medical malpractice remains a principal risk MIKE EGAN, CPCU Senior Vice President Unit
Business Associate Agreement
 This Business Associate Agreement Is Related To and a Part of the Following Underlying Agreement: Effective Date of Underlying Agreement: Vendor: Business Associate Agreement This Business Associate Agreement
This Business Associate Agreement Is Related To and a Part of the Following Underlying Agreement: Effective Date of Underlying Agreement: Vendor: Business Associate Agreement This Business Associate Agreement
Data Breach Cost. Risks, costs and mitigation strategies for data breaches
 Data Breach Cost Risks, costs and mitigation strategies for data breaches Tim Stapleton, CIPP/US Deputy Global Head of Professional Liability Zurich General Insurance Data Breaches: Greater frequency,
Data Breach Cost Risks, costs and mitigation strategies for data breaches Tim Stapleton, CIPP/US Deputy Global Head of Professional Liability Zurich General Insurance Data Breaches: Greater frequency,
CYBER & PRIVACY INSURANCE FOR FINANCIAL INSTITUTIONS
 CYBER & PRIVACY INSURANCE FOR FINANCIAL INSTITUTIONS 1 As regulators around the world move to tighten compliance requirements for financial institutions, improvement in cyber security controls will become
CYBER & PRIVACY INSURANCE FOR FINANCIAL INSTITUTIONS 1 As regulators around the world move to tighten compliance requirements for financial institutions, improvement in cyber security controls will become
Implementing Electronic Medical Records (EMR): Mitigate Security Risks and Create Peace of Mind
 Page1 Implementing Electronic Medical Records (EMR): Mitigate Security Risks and Create Peace of Mind The use of electronic medical records (EMRs) to maintain patient information is encouraged today and
Page1 Implementing Electronic Medical Records (EMR): Mitigate Security Risks and Create Peace of Mind The use of electronic medical records (EMRs) to maintain patient information is encouraged today and
SINGAPORE HEALTHCARE ENTERPRISE RISK MANAGEMENT CONGRESS 2014 - Data Breach : The Emerging Threat to Healthcare Industry
 SINGAPORE HEALTHCARE ENTERPRISE RISK MANAGEMENT CONGRESS 2014 - Data Breach : The Emerging Threat to Healthcare Industry DATA BREACH A FICTIONAL CASE STUDY THE FIRST SIGNS OF TROUBLE Friday, 5.20 pm :
SINGAPORE HEALTHCARE ENTERPRISE RISK MANAGEMENT CONGRESS 2014 - Data Breach : The Emerging Threat to Healthcare Industry DATA BREACH A FICTIONAL CASE STUDY THE FIRST SIGNS OF TROUBLE Friday, 5.20 pm :
9/13/2011. Miscellaneous Current Topics in Healthcare Professional Liability. Antitrust Notice. Table of Contents. Cyber Liability.
 Miscellaneous Current Topics in Healthcare Professional Liability Josh Zirin, FCAS, MAAA Antitrust Notice The Casualty Actuarial Society is committed to adhering strictly to the letter and spirit of the
Miscellaneous Current Topics in Healthcare Professional Liability Josh Zirin, FCAS, MAAA Antitrust Notice The Casualty Actuarial Society is committed to adhering strictly to the letter and spirit of the
University Healthcare Physicians Compliance and Privacy Policy
 Page 1 of 11 POLICY University Healthcare Physicians (UHP) will enter into business associate agreements in compliance with the provisions of the Health Insurance Portability and Accountability Act of
Page 1 of 11 POLICY University Healthcare Physicians (UHP) will enter into business associate agreements in compliance with the provisions of the Health Insurance Portability and Accountability Act of
cyber invasions cyber risk insurance AFP Exchange
 Cyber Risk With cyber invasions now a common place occurrence, insurance coverage isn t found in your liability policy. So many different types of computer invasions exist, but there is cyber risk insurance
Cyber Risk With cyber invasions now a common place occurrence, insurance coverage isn t found in your liability policy. So many different types of computer invasions exist, but there is cyber risk insurance
Lessons Learned from Recent HIPAA and Big Data Breaches. Briar Andresen Katie Ilten Ann Ladd
 Lessons Learned from Recent HIPAA and Big Data Breaches Briar Andresen Katie Ilten Ann Ladd Recent health care breaches Breach reports to OCR as of February 2015 1,144 breaches involving 500 or more individual
Lessons Learned from Recent HIPAA and Big Data Breaches Briar Andresen Katie Ilten Ann Ladd Recent health care breaches Breach reports to OCR as of February 2015 1,144 breaches involving 500 or more individual
Tools Conference Toronto November 26, 2014 Insurance for NFP s. Presented by Paul Spark HUB International HKMB Limited
 Tools Conference Toronto November 26, 2014 Insurance for NFP s Presented by Paul Spark HUB International HKMB Limited Topics Insurance Policies Basics Directors and Officers Liability Insurance Commercial
Tools Conference Toronto November 26, 2014 Insurance for NFP s Presented by Paul Spark HUB International HKMB Limited Topics Insurance Policies Basics Directors and Officers Liability Insurance Commercial
INFORMATION SECURITY & PRIVACY INSURANCE WITH ELECTRONIC MEDIA LIABILITY APPLICATION
 INFORMATION SECURITY & PRIVACY INSURANCE WITH ELECTRONIC MEDIA LIABILITY APPLICATION NOTICE: COVERAGE UNDER THIS POLICY IS PROVIDED ON A CLAIMS MADE AND REPORTED BASIS AND APPLIES ONLY TO CLAIMS FIRST
INFORMATION SECURITY & PRIVACY INSURANCE WITH ELECTRONIC MEDIA LIABILITY APPLICATION NOTICE: COVERAGE UNDER THIS POLICY IS PROVIDED ON A CLAIMS MADE AND REPORTED BASIS AND APPLIES ONLY TO CLAIMS FIRST
what your business needs to do about the new HIPAA rules
 what your business needs to do about the new HIPAA rules Whether you are an employer that provides health insurance for your employees, a business in the growing health care industry, or a hospital or
what your business needs to do about the new HIPAA rules Whether you are an employer that provides health insurance for your employees, a business in the growing health care industry, or a hospital or
CYBER INSURANCE. Cyber Insurance and Gaps in Traditional Insurance. Cyber and E&O Team Willis FINEX North America
 CYBER INSURANCE Cyber Insurance and Gaps in Traditional Insurance Cyber and E&O Team Willis FINEX North America Privacy & Network Security (Cyber) Insurance COVERAGE MODULES Privacy Expense Consumer Notification
CYBER INSURANCE Cyber Insurance and Gaps in Traditional Insurance Cyber and E&O Team Willis FINEX North America Privacy & Network Security (Cyber) Insurance COVERAGE MODULES Privacy Expense Consumer Notification
Why Lawyers? Why Now?
 TODAY S PRESENTERS Why Lawyers? Why Now? New HIPAA regulations go into effect September 23, 2013 Expands HIPAA safeguarding and breach liabilities for business associates (BAs) Lawyer is considered a business
TODAY S PRESENTERS Why Lawyers? Why Now? New HIPAA regulations go into effect September 23, 2013 Expands HIPAA safeguarding and breach liabilities for business associates (BAs) Lawyer is considered a business
MANAGING Cybersecurity Risk AND DISCLOSURE OBLIGATIONS
 MANAGING Cybersecurity Risk AND DISCLOSURE OBLIGATIONS RRD Donnelley SEC Hot Topics Institute May 21, 2014 1 MANAGING CYBERSECURITY RISK AND DISCLOSURE OBLIGATIONS Patrick J. Schultheis Partner Wilson
MANAGING Cybersecurity Risk AND DISCLOSURE OBLIGATIONS RRD Donnelley SEC Hot Topics Institute May 21, 2014 1 MANAGING CYBERSECURITY RISK AND DISCLOSURE OBLIGATIONS Patrick J. Schultheis Partner Wilson
Insuring Innovation. CyberFirst Coverage for Technology Companies
 Insuring Innovation. CyberFirst for Technology Companies TECHNOLOGY IS EVERYWHERE. SO ARE THE THREATS. protection that goes well beyond a traditional general liability policy. CyberFirst CyberFirst is
Insuring Innovation. CyberFirst for Technology Companies TECHNOLOGY IS EVERYWHERE. SO ARE THE THREATS. protection that goes well beyond a traditional general liability policy. CyberFirst CyberFirst is
HITRUST CSF Assurance Program You Need a HITRUST CSF Assessment Now What?
 HITRUST CSF Assurance Program You Need a HITRUST CSF Assessment Now What? Introduction This material is designed to answer some of the commonly asked questions by business associates and other organizations
HITRUST CSF Assurance Program You Need a HITRUST CSF Assessment Now What? Introduction This material is designed to answer some of the commonly asked questions by business associates and other organizations
DATA BREACH COVERAGE
 THIS ENDORSEMENT CHANGES THE POLICY. PLEASE READ THIS CAREFULLY. DATA BREACH COVERAGE SCHEDULE OF COVERAGE LIMITS Coverage Limits of Insurance Data Breach Coverage $50,000 Legal Expense Coverage $5,000
THIS ENDORSEMENT CHANGES THE POLICY. PLEASE READ THIS CAREFULLY. DATA BREACH COVERAGE SCHEDULE OF COVERAGE LIMITS Coverage Limits of Insurance Data Breach Coverage $50,000 Legal Expense Coverage $5,000
CYBER RISK SECURITY, NETWORK & PRIVACY
 CYBER RISK SECURITY, NETWORK & PRIVACY CYBER SECURITY, NETWORK & PRIVACY In the ever-evolving technological landscape in which we live, our lives are dominated by technology. The development and widespread
CYBER RISK SECURITY, NETWORK & PRIVACY CYBER SECURITY, NETWORK & PRIVACY In the ever-evolving technological landscape in which we live, our lives are dominated by technology. The development and widespread
Internet Gaming: The New Face of Cyber Liability. Presented by John M. Link, CPCU Cottingham & Butler
 Internet Gaming: The New Face of Cyber Liability Presented by John M. Link, CPCU Cottingham & Butler 1 Presenter John M. Link, Vice President jlink@cottinghambutler.com 2 What s at Risk? $300 billion in
Internet Gaming: The New Face of Cyber Liability Presented by John M. Link, CPCU Cottingham & Butler 1 Presenter John M. Link, Vice President jlink@cottinghambutler.com 2 What s at Risk? $300 billion in
Specialty Risk Protector
 Specialty Professional Liability and Data and Network Security Insurance is a single policy that makes it easy for companies to secure the multi-faceted E&O protection our networked world requires. A simplified,
Specialty Professional Liability and Data and Network Security Insurance is a single policy that makes it easy for companies to secure the multi-faceted E&O protection our networked world requires. A simplified,
Enterprise PrivaProtector 9.0
 IRONSHORE INSURANCE COMPANIES 75 Federal St Boston, MA 02110 Toll Free: (877) IRON411 Enterprise PrivaProtector 9.0 Network Security and Privacy Insurance Application THE APPLICANT IS APPLYING FOR A CLAIMS
IRONSHORE INSURANCE COMPANIES 75 Federal St Boston, MA 02110 Toll Free: (877) IRON411 Enterprise PrivaProtector 9.0 Network Security and Privacy Insurance Application THE APPLICANT IS APPLYING FOR A CLAIMS
White Paper #6. Privacy and Security
 The Complexity of America s Health Care Industry White Paper #6 Privacy and Security www.nextwavehealthadvisors.com 2015 Next Wave Health Advisors and Lynn Harold Vogel, Ph.D. The Complexity of America
The Complexity of America s Health Care Industry White Paper #6 Privacy and Security www.nextwavehealthadvisors.com 2015 Next Wave Health Advisors and Lynn Harold Vogel, Ph.D. The Complexity of America
The HITECH Act: Implications to HIPAA Covered Entities and Business Associates. Linn F. Freedman, Esq.
 The HITECH Act: Implications to HIPAA Covered Entities and Business Associates Linn F. Freedman, Esq. Introduction and Overview On February 17, 2009, President Obama signed P.L. 111-05, the American Recovery
The HITECH Act: Implications to HIPAA Covered Entities and Business Associates Linn F. Freedman, Esq. Introduction and Overview On February 17, 2009, President Obama signed P.L. 111-05, the American Recovery
Privacy Legislation and Industry Security Standards
 Privacy Legislation and Issue No. 3 01010101 01010101 01010101 Information is generated about and collected from individuals at an unprecedented rate in the ordinary course of business. In most cases,
Privacy Legislation and Issue No. 3 01010101 01010101 01010101 Information is generated about and collected from individuals at an unprecedented rate in the ordinary course of business. In most cases,
Best practices and insight to protect your firm today against tomorrow s cybersecurity breach
 Best practices and insight to protect your firm today against tomorrow s cybersecurity breach July 8, 2015 Baker Tilly Virchow Krause, LLP Baker Tilly refers to Baker Tilly Virchow Krause, LLP, an independently
Best practices and insight to protect your firm today against tomorrow s cybersecurity breach July 8, 2015 Baker Tilly Virchow Krause, LLP Baker Tilly refers to Baker Tilly Virchow Krause, LLP, an independently
Cyberinsurance: Insuring for Data Breach Risk
 View the online version at http://us.practicallaw.com/2-588-8785 Cyberinsurance: Insuring for Data Breach Risk JUDY SELBY AND C. ZACHARY ROSENBERG, BAKER HOSTETLER LLP, WITH PRACTICAL LAW INTELLECTUAL
View the online version at http://us.practicallaw.com/2-588-8785 Cyberinsurance: Insuring for Data Breach Risk JUDY SELBY AND C. ZACHARY ROSENBERG, BAKER HOSTETLER LLP, WITH PRACTICAL LAW INTELLECTUAL
Cyber Liability Insurance: It May Surprise You
 Cyber Liability Insurance: It May Surprise You Moderator Eugene Montgomery, President & CEO Community Financial Insurance Center Panelists Antonio Trotta, Senior Claim Counsel, CNA Specialty William Heinbokel,
Cyber Liability Insurance: It May Surprise You Moderator Eugene Montgomery, President & CEO Community Financial Insurance Center Panelists Antonio Trotta, Senior Claim Counsel, CNA Specialty William Heinbokel,
APPLICATION FOR TECHNOLOGY & PRIVACY PROFESSIONAL LIABILITY
 APPLICATION FOR TECHNOLOGY & PRIVACY PROFESSIONAL LIABILITY GENERAL INFORMATION 1. APPLICANT NAME: 2. PHONE: 3. MAILING ADDRESS: 4. WEB ADDRESS: 5. The following officer of the Applicant is designated
APPLICATION FOR TECHNOLOGY & PRIVACY PROFESSIONAL LIABILITY GENERAL INFORMATION 1. APPLICANT NAME: 2. PHONE: 3. MAILING ADDRESS: 4. WEB ADDRESS: 5. The following officer of the Applicant is designated
GENOA, a QoL HEALTHCARE COMPANY GENOA ONLINE SYSTEM TERMS OF USE
 GENOA, a QoL HEALTHCARE COMPANY GENOA ONLINE SYSTEM TERMS OF USE By using the Genoa Online system (the System ), you acknowledge and accept the following terms of use: This document details the terms of
GENOA, a QoL HEALTHCARE COMPANY GENOA ONLINE SYSTEM TERMS OF USE By using the Genoa Online system (the System ), you acknowledge and accept the following terms of use: This document details the terms of
Data security: A growing liability threat
 Data security: A growing liability threat Data security breaches occur with alarming frequency in today s technology-laden world. Even a comparatively moderate breach can cost a company millions of dollars
Data security: A growing liability threat Data security breaches occur with alarming frequency in today s technology-laden world. Even a comparatively moderate breach can cost a company millions of dollars
Top Ten Technology Risks Facing Colleges and Universities
 Top Ten Technology Risks Facing Colleges and Universities Chris Watson, MBA, CISA, CRISC Manager, Internal Audit and Risk Advisory Services cwatson@schneiderdowns.com April 23, 2012 Overview Technology
Top Ten Technology Risks Facing Colleges and Universities Chris Watson, MBA, CISA, CRISC Manager, Internal Audit and Risk Advisory Services cwatson@schneiderdowns.com April 23, 2012 Overview Technology
Distributor Liability Contract Risk Management THOMAS DOUGLASS APRIL 15, 2015
 Distributor Liability Contract Risk Management THOMAS DOUGLASS APRIL 15, 2015 Today s Agenda What are we talking about today? What is Risk Evolution of risk management Understand the importance of Risk
Distributor Liability Contract Risk Management THOMAS DOUGLASS APRIL 15, 2015 Today s Agenda What are we talking about today? What is Risk Evolution of risk management Understand the importance of Risk
Cyber-Crime Protection
 Cyber-Crime Protection A program of cyber-crime prevention, data breach remedies and data risk liability insurance for houses of worship, camps, schools, denominational/association offices and senior living
Cyber-Crime Protection A program of cyber-crime prevention, data breach remedies and data risk liability insurance for houses of worship, camps, schools, denominational/association offices and senior living
Disclaimer: Template Business Associate Agreement (45 C.F.R. 164.308)
 HIPAA Business Associate Agreement Sample Notice Disclaimer: Template Business Associate Agreement (45 C.F.R. 164.308) The information provided in this document does not constitute, and is no substitute
HIPAA Business Associate Agreement Sample Notice Disclaimer: Template Business Associate Agreement (45 C.F.R. 164.308) The information provided in this document does not constitute, and is no substitute
HIPAA Omnibus Rule Overview. Presented by: Crystal Stanton MicroMD Marketing Communication Specialist
 HIPAA Omnibus Rule Overview Presented by: Crystal Stanton MicroMD Marketing Communication Specialist 1 HIPAA Omnibus Rule - Agenda History of the Omnibus Rule What is the HIPAA Omnibus Rule and its various
HIPAA Omnibus Rule Overview Presented by: Crystal Stanton MicroMD Marketing Communication Specialist 1 HIPAA Omnibus Rule - Agenda History of the Omnibus Rule What is the HIPAA Omnibus Rule and its various
Zip It! Feds, State Strengthen Privacy Protection. Practice Management Feature July 2012. Tex Med. 2012;108(7):33-37.
 Zip It! Feds, State Strengthen Privacy Protection Practice Management Feature July 2012 Tex Med. 2012;108(7):33-37. By Crystal Conde Associate Editor When it comes to enforcing HIPAA data security and
Zip It! Feds, State Strengthen Privacy Protection Practice Management Feature July 2012 Tex Med. 2012;108(7):33-37. By Crystal Conde Associate Editor When it comes to enforcing HIPAA data security and
THE NEW REALITY OF RISK CYBER RISK: TRENDS AND SOLUTIONS
 THE NEW REALITY OF RISK CYBER RISK: TRENDS AND SOLUTIONS Read the Marsh Risk Management Research Briefing: Cyber Risks Extend Beyond Data and Privacy Exposures To access the report, visit www.marsh.com.
THE NEW REALITY OF RISK CYBER RISK: TRENDS AND SOLUTIONS Read the Marsh Risk Management Research Briefing: Cyber Risks Extend Beyond Data and Privacy Exposures To access the report, visit www.marsh.com.
Understanding HIPAA Privacy and Security Helping Your Practice Select a HIPAA- Compliant IT Provider A White Paper by CMIT Solutions
 Understanding HIPAA Privacy and Security Helping Your Practice Select a HIPAA- Compliant IT Provider A White Paper by CMIT Solutions Table of Contents Understanding HIPAA Privacy and Security... 1 What
Understanding HIPAA Privacy and Security Helping Your Practice Select a HIPAA- Compliant IT Provider A White Paper by CMIT Solutions Table of Contents Understanding HIPAA Privacy and Security... 1 What
CAGNY Spring 2015 Meeting Fundamentals of Cyber Risk. Brad Gow June 9th, 2015 Endurance
 Fundamentals of Cyber Risk Brad Gow June 9th, 2015 Endurance But consider the kickoff chuckle to a speech given to the Wharton School in March 1977 by Sidney Homer of Salomon Brothers, the leading bond
Fundamentals of Cyber Risk Brad Gow June 9th, 2015 Endurance But consider the kickoff chuckle to a speech given to the Wharton School in March 1977 by Sidney Homer of Salomon Brothers, the leading bond
Are You Still HIPAA Compliant? Staying Protected in the Wake of the Omnibus Final Rule Click to edit Master title style.
 Are You Still HIPAA Compliant? Staying Protected in the Wake of the Omnibus Final Rule Click to edit Master title style March 27, 2013 www.mcguirewoods.com Introductions Holly Carnell McGuireWoods LLP
Are You Still HIPAA Compliant? Staying Protected in the Wake of the Omnibus Final Rule Click to edit Master title style March 27, 2013 www.mcguirewoods.com Introductions Holly Carnell McGuireWoods LLP
Risk Management of Outsourced Technology Services. November 28, 2000
 Risk Management of Outsourced Technology Services November 28, 2000 Purpose and Background This statement focuses on the risk management process of identifying, measuring, monitoring, and controlling the
Risk Management of Outsourced Technology Services November 28, 2000 Purpose and Background This statement focuses on the risk management process of identifying, measuring, monitoring, and controlling the
HIPAA Compliance and the Protection of Patient Health Information
 HIPAA Compliance and the Protection of Patient Health Information WHITE PAPER By Swift Systems Inc. April 2015 Swift Systems Inc. 7340 Executive Way, Ste M Frederick MD 21704 1 Contents HIPAA Compliance
HIPAA Compliance and the Protection of Patient Health Information WHITE PAPER By Swift Systems Inc. April 2015 Swift Systems Inc. 7340 Executive Way, Ste M Frederick MD 21704 1 Contents HIPAA Compliance
2/9/2012. 2012 HIPAA Privacy and Security Audit Readiness. Table of contents
 2012 HIPAA Privacy and Security Audit Readiness Mark M. Johnson National HIPAA Services Director Table of contents Page Background 2 Regulatory Background and HITECH Impacts 3 Office of Civil Rights (OCR)
2012 HIPAA Privacy and Security Audit Readiness Mark M. Johnson National HIPAA Services Director Table of contents Page Background 2 Regulatory Background and HITECH Impacts 3 Office of Civil Rights (OCR)
Cyber Risk State of the Art
 Proudly presents Cyber Risk State of the Art Matthew Davies, Chubb Insurance Catherine Dowdall, Canada Post Mike Petersen, Marsh 1 Agenda 1. Who is At Risk? 2. New/Emerging Risk and Trends 3. Canada Post
Proudly presents Cyber Risk State of the Art Matthew Davies, Chubb Insurance Catherine Dowdall, Canada Post Mike Petersen, Marsh 1 Agenda 1. Who is At Risk? 2. New/Emerging Risk and Trends 3. Canada Post
Business Associate Agreement Involving the Access to Protected Health Information
 School/Unit: Rowan University School of Osteopathic Medicine Vendor: Business Associate Agreement Involving the Access to Protected Health Information This Business Associate Agreement ( BAA ) is entered
School/Unit: Rowan University School of Osteopathic Medicine Vendor: Business Associate Agreement Involving the Access to Protected Health Information This Business Associate Agreement ( BAA ) is entered
Understanding the Business Risk
 AAPA Cybersecurity Seminar Andaz Savannah Hotel March 11, 2015 10:30 am Noon Understanding the Business Risk Presenter: Joshua Gold, Esq. (212) 278-1886 jgold@andersonkill.com Disclaimer The views expressed
AAPA Cybersecurity Seminar Andaz Savannah Hotel March 11, 2015 10:30 am Noon Understanding the Business Risk Presenter: Joshua Gold, Esq. (212) 278-1886 jgold@andersonkill.com Disclaimer The views expressed
Protecting Your Assets: How To Safeguard Your Fund Against Cyber Security Attacks
 Protecting Your Assets: How To Safeguard Your Fund Against Cyber Security Attacks Hacks, breaches, stolen data, trade secrets hijacked, privacy violated, ransom demands made; how can you protect your data
Protecting Your Assets: How To Safeguard Your Fund Against Cyber Security Attacks Hacks, breaches, stolen data, trade secrets hijacked, privacy violated, ransom demands made; how can you protect your data
Cyber Liability. What School Districts Need to Know
 Cyber Liability What School Districts Need to Know Data Breaches Growing In Number Between January 1, 2008 and April 4, 2012 314,216,842 reported records containing sensitive personal information have
Cyber Liability What School Districts Need to Know Data Breaches Growing In Number Between January 1, 2008 and April 4, 2012 314,216,842 reported records containing sensitive personal information have
Network Security & Privacy Landscape
 Network Security & Privacy Landscape Presented By: Greg Garijanian Senior Underwriter Professional Liability 1 Agenda Network Security Overview -Latest Threats - Exposure Trends - Regulations Case Studies
Network Security & Privacy Landscape Presented By: Greg Garijanian Senior Underwriter Professional Liability 1 Agenda Network Security Overview -Latest Threats - Exposure Trends - Regulations Case Studies
HIPAA Omnibus Rule Practice Impact. Kristen Heffernan MicroMD Director of Prod Mgt and Marketing
 HIPAA Omnibus Rule Practice Impact Kristen Heffernan MicroMD Director of Prod Mgt and Marketing 1 HIPAA Omnibus Rule Agenda History of the Rule HIPAA Stats Rule Overview Use of Personal Health Information
HIPAA Omnibus Rule Practice Impact Kristen Heffernan MicroMD Director of Prod Mgt and Marketing 1 HIPAA Omnibus Rule Agenda History of the Rule HIPAA Stats Rule Overview Use of Personal Health Information
BUSINESS ASSOCIATE AGREEMENT
 COLUMBIA AGREEMENT BUSINESS ASSOCIATE AGREEMENT This Business Associate Agreement ( Agreement ) is entered into as of ( Effective Date ) by and between The Trustees of Columbia University in the City of
COLUMBIA AGREEMENT BUSINESS ASSOCIATE AGREEMENT This Business Associate Agreement ( Agreement ) is entered into as of ( Effective Date ) by and between The Trustees of Columbia University in the City of
Cyber/ Network Security. FINEX Global
 Cyber/ Network Security FINEX Global ABOUT US >> We are one of the largest insurance brokers in the world >> We have over 180 years of history and experience in insurance; we currently operate in over
Cyber/ Network Security FINEX Global ABOUT US >> We are one of the largest insurance brokers in the world >> We have over 180 years of history and experience in insurance; we currently operate in over
Cyber Threats: Exposures and Breach Costs
 Issue No. 2 THREAT LANDSCAPE Technological developments do not only enhance capabilities for legitimate business they are also tools that may be utilized by those with malicious intent. Cyber-criminals
Issue No. 2 THREAT LANDSCAPE Technological developments do not only enhance capabilities for legitimate business they are also tools that may be utilized by those with malicious intent. Cyber-criminals
A How-To Guide for Updating HIPAA Policies & Procedures to Align with ARRA Health Care Provider Edition Version 1
 A How-To Guide for Updating HIPAA Policies & Procedures to Align with ARRA Health Care Provider Edition Version 1 Policy and Procedure Templates Reflects modifications published in the Federal Register
A How-To Guide for Updating HIPAA Policies & Procedures to Align with ARRA Health Care Provider Edition Version 1 Policy and Procedure Templates Reflects modifications published in the Federal Register
HIPAA PRIVACY AND SECURITY RULES BUSINESS ASSOCIATE AGREEMENT BETWEEN. Stewart C. Miller & Co., Inc. (Business Associate) AND
 HIPAA PRIVACY AND SECURITY RULES BUSINESS ASSOCIATE AGREEMENT BETWEEN Stewart C. Miller & Co., Inc. (Business Associate) AND City of West Lafayette Flexible Spending Plan (Covered Entity) TABLE OF CONTENTS
HIPAA PRIVACY AND SECURITY RULES BUSINESS ASSOCIATE AGREEMENT BETWEEN Stewart C. Miller & Co., Inc. (Business Associate) AND City of West Lafayette Flexible Spending Plan (Covered Entity) TABLE OF CONTENTS
Written Information Security Programs: Compliance with the Massachusetts Data Security Regulation
 Written Information Security Programs: Compliance with the Massachusetts Data Security Regulation Melissa J. Krasnow, Dorsey & Whitney LLP A Note discussing written information security programs (WISPs)
Written Information Security Programs: Compliance with the Massachusetts Data Security Regulation Melissa J. Krasnow, Dorsey & Whitney LLP A Note discussing written information security programs (WISPs)
Introduction to Data Security Breach Preparedness with Model Data Security Breach Preparedness Guide
 Introduction to Data Security Breach Preparedness with Model Data Security Breach Preparedness Guide by Christopher Wolf Directors, Privacy and Information Management Practice Hogan Lovells US LLP christopher.wolf@hoganlovells.com
Introduction to Data Security Breach Preparedness with Model Data Security Breach Preparedness Guide by Christopher Wolf Directors, Privacy and Information Management Practice Hogan Lovells US LLP christopher.wolf@hoganlovells.com
Privacy and Data Breach Protection Modular application form
 Instructions The Hiscox Technology, Privacy and Cyber Portfolio Policy may be purchased on an a-la-carte basis. Some organizations may require coverage for their technology errors and omissions, while
Instructions The Hiscox Technology, Privacy and Cyber Portfolio Policy may be purchased on an a-la-carte basis. Some organizations may require coverage for their technology errors and omissions, while
The benefits you need... from the name you know and trust
 The benefits you need... Privacy and Security Best at Practices the price you can afford... Guide from the name you know and trust The Independence Blue Cross (IBC) Privacy and Security Best Practices
The benefits you need... Privacy and Security Best at Practices the price you can afford... Guide from the name you know and trust The Independence Blue Cross (IBC) Privacy and Security Best Practices
VENDOR MANAGEMENT. General Overview
 VENDOR MANAGEMENT General Overview With many organizations outsourcing services to other third-party entities, the issue of vendor management has become a noted topic in today s business world. Vendor
VENDOR MANAGEMENT General Overview With many organizations outsourcing services to other third-party entities, the issue of vendor management has become a noted topic in today s business world. Vendor
Internet Stolen: The Fastest Growing White Collar Crime
 Cyber Liability What you need to know! PRESENTED BY: GALLAGHER / CYBERRISK SERVICES MAY 2014 Most Common Reactions to Cyber Liability Questions: We don t need cyber liability coverage; we have tort immunity
Cyber Liability What you need to know! PRESENTED BY: GALLAGHER / CYBERRISK SERVICES MAY 2014 Most Common Reactions to Cyber Liability Questions: We don t need cyber liability coverage; we have tort immunity
BUSINESS ASSOCIATE AGREEMENT
 BUSINESS ASSOCIATE AGREEMENT This Business Associate Agreement (the Agreement ), is made effective as of the sign up date on the login information page of the CarePICS.com website, by and between CarePICS,
BUSINESS ASSOCIATE AGREEMENT This Business Associate Agreement (the Agreement ), is made effective as of the sign up date on the login information page of the CarePICS.com website, by and between CarePICS,
The Dish on Data and Disks HIPAAPrivacy and Security Breach Developments. Robin B. Campbell Ethan P. Schulman Jennifer S. Romano
 The Dish on Data and Disks HIPAAPrivacy and Security Breach Developments Robin B. Campbell Ethan P. Schulman Jennifer S. Romano HIPAAPrivacy and Security Breach Overview of the Laws Developments Incident
The Dish on Data and Disks HIPAAPrivacy and Security Breach Developments Robin B. Campbell Ethan P. Schulman Jennifer S. Romano HIPAAPrivacy and Security Breach Overview of the Laws Developments Incident
Privacy / Network Security Liability Insurance Discussion. January 30, 2013. Kevin Violette RT ProExec
 Privacy / Network Security Liability Insurance Discussion January 30, 2013 Kevin Violette RT ProExec 1 Irrefutable Laws of Information Security 1) Information wants to be free People want to talk, post,
Privacy / Network Security Liability Insurance Discussion January 30, 2013 Kevin Violette RT ProExec 1 Irrefutable Laws of Information Security 1) Information wants to be free People want to talk, post,
Trust 9/10/2015. Why Does Privacy and Security Matter? Who Must Comply with HIPAA Rules? HIPAA Breaches, Security Risk Analysis, and Audits
 HIPAA Breaches, Security Risk Analysis, and Audits Derrick Hill Senior Health IT Advisor Kentucky REC Why Does Privacy and Security Matter? Trust Who Must Comply with HIPAA Rules? Covered Entities (CE)
HIPAA Breaches, Security Risk Analysis, and Audits Derrick Hill Senior Health IT Advisor Kentucky REC Why Does Privacy and Security Matter? Trust Who Must Comply with HIPAA Rules? Covered Entities (CE)
Compliance Challenges. Ali Pabrai, MSEE, CISSP (ISSMP, ISSAP) Member, FBI InfraGard. Increased Audits & On-site Investigations
 Enabling a HITECH & HIPAA Compliant Organization: Addressing Meaningful Use Mandates & Ensuring Audit Readiness Ali Pabrai, MSEE, CISSP (ISSMP, ISSAP) Member, FBI InfraGard Compliance Mandates Increased
Enabling a HITECH & HIPAA Compliant Organization: Addressing Meaningful Use Mandates & Ensuring Audit Readiness Ali Pabrai, MSEE, CISSP (ISSMP, ISSAP) Member, FBI InfraGard Compliance Mandates Increased
Data Security and Integrity of e-phi. MLCHC Annual Clinical Conference Worcester, MA Wednesday, November 12, 2014 2:15pm 3:30pm
 Electronic Health Records: Data Security and Integrity of e-phi Worcester, MA Wednesday, 2:15pm 3:30pm Agenda Introduction Learning Objectives Overview of HIPAA HIPAA: Privacy and Security HIPAA: The Security
Electronic Health Records: Data Security and Integrity of e-phi Worcester, MA Wednesday, 2:15pm 3:30pm Agenda Introduction Learning Objectives Overview of HIPAA HIPAA: Privacy and Security HIPAA: The Security
BUSINESS ASSOCIATE AGREEMENT
 BUSINESS ASSOCIATE AGREEMENT THIS BUSINESS ASSOCIATE AGREEMENT ( Agreement ) is entered into by and between (the Covered Entity ), and Iowa State Association of Counties (the Business Associate ). RECITALS
BUSINESS ASSOCIATE AGREEMENT THIS BUSINESS ASSOCIATE AGREEMENT ( Agreement ) is entered into by and between (the Covered Entity ), and Iowa State Association of Counties (the Business Associate ). RECITALS
HIPAA Hot Topics. Audits, the Latest on Enforcement and the Impact of Breaches. September 2012. Nashville Knoxville Memphis Washington, D.C.
 HIPAA Hot Topics Audits, the Latest on Enforcement and the Impact of Breaches September 2012 Nashville Knoxville Memphis Washington, D.C. Overview HITECH Act HIPAA Audit Program: update and initial results
HIPAA Hot Topics Audits, the Latest on Enforcement and the Impact of Breaches September 2012 Nashville Knoxville Memphis Washington, D.C. Overview HITECH Act HIPAA Audit Program: update and initial results
Data Breach and Cybersecurity: What Happens If You or Your Vendor Is Hacked
 Data Breach and Cybersecurity: What Happens If You or Your Vendor Is Hacked Linda Vincent, R.N., P.I., CITRMS Vincent & Associates Founder The Identity Advocate San Pedro, California The opinions expressed
Data Breach and Cybersecurity: What Happens If You or Your Vendor Is Hacked Linda Vincent, R.N., P.I., CITRMS Vincent & Associates Founder The Identity Advocate San Pedro, California The opinions expressed
