Consensus report: Pretreatment minimal staging and treatment of potentially resectable malignant pleural mesothelioma
|
|
|
- Solomon Fowler
- 8 years ago
- Views:
Transcription
1 Lung Cancer (2005) 49S1, S123 S127 Consensus report: Pretreatment minimal staging and treatment of potentially resectable malignant pleural mesothelioma Jan P. van Meerbeeck a,,michael Boyer b a University Hospital,De Pintelaan 185, B-9000 Ghent, Belgium b Sydney Cancer Centre, Missenden Road,2050 Camperdown, NSW, Australia 1. Introduction The panel decided to discuss successivelythe issues of staging classification, pretreatment assessment and treatment of potentiallyresectable malignant pleural mesothelioma (MPM). Whenever possible a consensus was agreed and areas of further research were identified based on issues on which no agreement could be obtained. Recommendations were formulated based on the areas of consensus and disagreement. 2. Staging classification Earlier staging systems of MPM reflect the experiences of individual investigators or institutions in their respective patient populations. There is considerable discrepancybetween the various staging systems, resulting in non-uniformity of results reporting. Moreover, these earlier * Corresponding author. addresses: jan.vanmeerbeeck@ugent.be (J.P. van Meerbeeck), michael.boyer@cs.nsw.gov.au (M. Boyer). systems tend to concentrate either on resectable (Butchart, Brigham) or on advanced MPM [1 8]. A new staging system was devised by members of the International Mesothelioma Interest Group (IMIG) and approved byconsensus at the Tri-Annual Meeting of the International Association for the Studyof Lung Cancer (IASLC, Colorado Springs, 1997). This staging system is quite complex reflecting the complex presentation and modes of spread of this unique neoplasm [9,10]. The two most important purposes of the classification were to: 1. Separate out that relativelysmall group of patients with earlympm who maybe potentially curable byaggressive surgical means. 2. Distinguish between later stage presentation of MPM, which is still at a resectable stage, and late MPM, which is unresectable. This classification is hence mainlya surgical pathological one. In view of the limited therapeutic alternatives to surgery, there was little need for further refinement at that time. About 10 years later, with active chemotherapeutic /$ see front matter 2005 Elsevier Ireland Ltd. All rights reserved. doi: /j.lungcan
2 S124 J.P. van Meerbeeck, M. Boyer drugs available and multimodal protocols being activated, the classification is not anymore being considered adequate based on the following arguments: 1. The data base on which it is based is unknown. 2. Its validation has been limited and in a retrospective fashion only [11,16]. 3. The system is not designed to take into account the realityof cross-sectional imaging methodology. Many of the distinctions which the staging system makes: for example, distinguishing visceral from parietal pleural involvement, involvement of endothoracic fascia, transmural versus non-transmural pericardial involvement, cannot be distinguished with the resolution of computed tomography(ct)/ magnetic resonance imaging (MRI) [12]. 4. The complex anatomic presentation of this neoplasm with frequent diffuse, bulkytumour masses involving the pleural surfaces prevents visualization of regional nodal spread. In fact the accuracyof CT/MRI in predicting surgical findings is 55 75% [12]. 5. The regional lymphatic drainage of MPM was thought to mirror the lung cancer one but is in realitymore complex and hence is not reflected in the regional nodal spread (N1, N2 and N3) [13]. With the advent of multislice spiral CT and PET- CT scan, intrathoracic spatial resolution and the qualityof the coronal and sagittal image reconstruction byvoxel isotropism have improved. The application of these techniques in mesothelioma might result in more adequate clinical staging but has insufficientlybeen validated yet [14]. In view of the abovementioned, the consensus panel could not agree on a common staging classification in MPM. 3. Pretreatment minimal assessment 3.1. Assumptions: in reaching its consensus,the panel members made the following assumptions 1. The optimal pretreatment assessment protocol should: a. Be simple and widelyapplicable, without being limited to the lowest denominator. b. Be sequential and logical, unnecessaryinvasive and/or expensive tests should be avoided. c. Identifycandidates for radical locoregional, combined modalitytreatment and palliative treatment. d. Be applicable to good clinical practice with all forms of therapy. There should be no restriction on institutional preference for additional investigations, nor additional requirements for trial purposes. If physical signs or laboratoryinvestigations indicate metastasis and/or invasion, further investigations are indicated onlyif clinicallyrelevant. e. Refer to patients with MPM only. 2. The diagnosis of MPM is alreadyestablished or, at least, the clinical presentation is highlysuspicious for the presence of MPM. 3. Everypatient is fit for all forms of therapy: the suitabilityof individual patients for different forms of therapyshould be separatelyassessed (i.e. cardiac and/or pulmonaryfunction) Pretreatment workup: the pretreatment assessment is ideally split into three steps,which are to some degree overlapping Whether a patient goes through all three steps depends stronglyon the results of the procedures and the consequences for the choice of treatment with radical or palliative intent only Step I,to be considered in all patients at presentation or diagnosis Investigations Including Confirmatory tests Demographics Gender and age Clinical historyperformance As appropriate status, presence/absence of chest pain, dyspnea, change in bodyweight or BMI* Physical examination Presence or absence of shrinking As appropriate Radiological investigations Blood tests hemithorax Chest X-ray: PA/lateral in-/expiration, pre-/post drainage of pleural fluid Hemoglobin, leucocytes, platelets, basic biochemistry *BMI, bodymass index.
3 Consensus report S Step II,to be considered in patients being candidate for any kind of active treatment Investigations Including Confirmatorytests CT scan of chest and upper abdomen Spiral technique, with iv contrast, including lowest costophrenic angles, after drainage of pleural fluid Pulmonaryfunction tests Forced vital capacity(fvc), forced expiratoryvolume 1 sec (FEV1) Bone scan Not routine, to be considered on clinical suspicion onlystandard X-rayor CT/MRI to confirm dubious findings Brain CT/MRI Not routine, to be considered on clinical suspicion only After having gone through the investigations of step I and II, it is usuallyclear if further tests are necessaryto finalize the process of patient selection for combined modalityor radical locoregional treatment. It was the opinion of the panel that this would be onlythe case in a minority( 10%) of patients with MPM. This is reflected in the paucity of data, reflecting different institutional practice. Among the investigations to be considered are mediastinoscopy, MRI of the chest, Video Assisted Thoracoscopy(VATS) and laparoscopy. To some degree these investigations are complementaryto each other and in the absence of comparative trials no formal advice regarding their respective efficacy can be given. Esophageal Ultrasound with fine needle aspiration (EUS-FNA) and PET-CT scan are new techniques that are not uniformlyavailable and need further confirmation of their validityin the pretreatment evaluation. 3. Further research is done with regard to the comparative efficacyof the different intrathoracic techniques (mediastinoscopy, VATS, EUS- FNA) and the value of the newer ones (PET-CT, EUS-FNA). 4. Treatment of potentially resectable disease In considering the management of patients with potentiallyresectable disease, there was acknowledgement bythe panel that the lack of data from adequatelyperformed, prospective, clinical trials limited the conclusions, which could be drawn. Notwithstanding this fact, the panel considered which patients were candidates for surgical resection, and what form the resection and associated management should take. Area Investigation Patient group Confirmatorytests Diaphragm Chest X-ray, in-/expiration Every patient considered Fluoroscopy for radical treatment Extrathoracic, excluding occult M1 Full ring FDG-PET scan Everypatient considered for radical treatment Biopsyof suspected extrathoracic lesions LaparoscopyAccording to institutional practice Mediastinum, excluding T4, N2/3 involvement Cervical mediastinoscopy, VATS, contralateral VATS According to institutional practice MRI of the chest, Gadolinium enhanced EUS-FNA Investigational PET-CT Investigational Step III: to be considered only in patients being candidate for radical treatment The consensus panel further agrees on that: 1. The interval within which the assessment has to be finalized should be as short as possible. 2. Recent (<1-month-old) imaging studies should be available prior to invasive procedures Patient selection Patients were divided into three groups based on the extent of their disease: 1. Patients with distant metastatic disease, those with involvement of mediastinal structures, and those with diffuse chest wall invasion are not considered to be candidates for resection.
4 S126 J.P. van Meerbeeck, M. Boyer 2. Patients with focal chest wall invasion are considered to be potential candidates for resection. 3. Patients with localized disease are considered to be candidates for resection. No agreement could be reached bythe panel on the implications of N2 nodal involvement on resectability. Although technically resectable, the outcomes for patients with involved N2 nodes have been verypoor in the experience of some groups [11,16], leading these groups to exclude such patients from initial resection. Other groups continue to resect tumors, which are associated with involved nodes. Consideration was also given to the impact of histological sub-type on the potential for resection. There was agreement that outcomes seemed to be best for patients with epithelioid tumours [11,16]. However, it was also felt there was insufficient evidence to exclude patients with bi-phasic or sarcomatoid tumor types from consideration for surgical resection Surgical treatment There was general agreement amongst the panel that the goal of surgeryin the management of potentiallyresectable mesothelioma was to improve local control bymaximallydebulking the disease. There was no agreement about the optimal type of surgery (pleuro-pneumonectomy, pleurectomy, or pleurodesis), the need for radiation therapy, or the need for combined modalitytreatment incorporating chemotherapy. Several centres have extensive experience with pleuropneumonectomy, radiation therapyand the addition of chemotherapyto these other modalities [15 18]. However, the lack of appropriatelydesigned prospective trials means that it is difficult to be certain how much patient selection contributes to the results seen after treatment. There was general agreement that prospective trials are needed urgentlyin order to assess different treatment approaches. A necessaryprerequisite for these trials is the development of a generallyagreed-upon staging system, to ensure that patients included in different trials are comparable. Although multimodal therapy, incorporating surgery, radiation therapyand chemotherapyhas become widelyused there was also no agreement as to whether this improved outcomes, and if so, what the optimal sequence and types of treatment were. Further trials are required to evaluate these questions. 5. Recommendations The panel members formulated the following recommendations: 1. A new robust and uniform clinical staging system has to be developed and validated. This new staging classification: a. Should preferentiallybe TNM-compatible. b. Encompass the existing surgical pathologic staging systems (IMIG, Brigham), that should be preferentiallytelescoped. c. Be based on a large database, consisting of a registryof retrospective surgical data (e.g. The International Registryof Lung Metastases [19]), added with prospective collection of clinical and pathological data of new cases. The IASLC was regarded as the organization of choice to develop this new classification as it has a current similar effort being conducted regarding the staging classification of lung cancer [20]. 2. Further research, ideallycomprising multicentre randomized controlled trials, is required to define preciselythe optimal surgical management of mesothelioma. In addition, trials are also required to evaluate the other components of therapyincluding radiation therapyand chemotherapy. 3. Extrapleural pneumonectomyshould onlybe carried out as part of a prospective clinical trial, in centres with experience in the procedure, and with the support of a multidisciplinaryteam. 4. Credentialing processes should be developed for the surgical and radiation management of malignant pleural mesothelioma, in order to maximize the effectiveness and minimize the toxicity of treatment. Appendix A. Members of consensus group Name Country Dienemann, Hendrik Kestenholz, Peter Steele, JeremyUK Stevens, Craig Schmitt-Opitz, Isabelle Müller, Michael Austria Gaafar, Rabab Egypt Waller, David UK Facciolo Francesco Sorensen, Jens Benn Denmark Van Schil, Paul Belgium Pinto, Carmine
5 Consensus report S127 Appendix A (Continued ) Name Favaretto, Adolfo Treasure, Tom Johnston, Michael Shepherd, Frances Bueno, Raphael Tin, Mo Mo Passlick, Bernward Weder, Walter Reck, Martin Münter, Marc Salih, Emri Hillerdal, Gunnar Armato, Sam Steinert, Hans Byrne, Michael References Country UK Canada Canada Australia Turkey Sweden Australia [1] Butchart EG, Ashcroft T, BarnsleyWC, Holden MP. Pleuropneumonectomyin the management of diffuse malignant mesothelioma of the pleura: experience with 29 patients. Thorax 1976;31: [2] Mattson K. Natural historyand clinical staging of malignant mesothelioma (abstract). Eur J Respir Dis 1982;(Suppl): [3] Rusch VW, Ginsberg RJ. New concepts in the staging of mesotheliomas. In: Deslauriers J, Lacquet LK, editors. Thoracic surgery: surgical management of pleural diseases. St. Louis: Mosby; p [4] Boutin C, ReyF, Gouvernet J, Viallat JR, Astoul P, LedorayV. Thoracoscopyin pleural malignant mesothelioma: a prospective studyof 188 consecutive patients II. Prognosis and staging. Cancer 1993;72: [5] Dimitrov NV, McMahon S. Presentation, diagnostic methods, staging, and natural historyof malignant mesothelioma. In: Antman K, Aisner J, editors. Asbestos-related malignancy. Orlando, FL: Grune and Stratton; p [6] Tammilehto L, Kivisaari L, Salminen US, Maasilta P, Mattson K. Evaluation of the clinical TNM staging system for malignant pleural mesothelioma: an assessment in 88 patients. Lung Cancer 1995;12: [7] Patz Jr EF, Shaffer K, Piwnica-Worms DR, Jochelson M, Sarin M, Sugarbaker DJ, et al. Malignant pleural mesothelioma: value of CT and MR imaging in predicting resectability. Am J Roentgenol 1992;159: [8] Sugarbaker DJ, Garcia JP, Richards WG. Extrapleural pneumonectomyin the multimodalitytherapyof malignant pleural mesothelioma Results in 120 consecutive patients. Ann Surg 1996;224: [9] Rusch VW (Ed.), The International Mesothelioma Interest Group. A proposed new international TNM staging system for malignant pleural mesothelioma. Chest 1995;108: [10] Patz Jr EF, Rusch VW, Heelan RT. The proposed new international TNM staging system for malignant pleural mesothelioma: application to imaging. Am J Roentgenol 1996;66: [11] Rusch VW, Venkatraman ES. Important prognostic factors in patients with malignant pleural mesothelioma managed surgically. Ann Thorac Surg 1999;68: [12] Heelan RT, Rusch VW, Begg CB, Panicek DM, Caravelli JF, Eisen C. Staging of malignant pleural mesothelioma: comparison of CT and MR imaging. Am J Roentgenol 1999;172: [13] Sharma A, Fidias P, Hayman LA, Loomis SL, Taber KT, Aquino SL. Patterns of lymphadenopathy in thoracic malignancies. RadioGraphics 2004;24: [14] Zubelia J, Abou-Zied M, Nabi H. Evaluation of patients with known mesothelioma with 18F-fluorodeoxyglucose and PET Comparison with computed tomography. Clin Positron Imag 2000;3:165. [15] Grondin SC, Sugarbaker DJ. Pleuropneumonectomyin the treatment of malignant pleural mesothelioma. Chest 1999;116(Suppl. 6):450S 4S. [16] Sugarbaker DJ, Flores RM, Jaklitsch MT, et al. resection margins, extrapleural nodal status, and cell type determine postoperative long-term survival in trimodalitytherapyof malignant pleural mesothelioma: results in 183 patients. J Thor Cardiovasc Surg 1999;117: [17] Ahamad A, Stevens CW, Smythe WR, et al. promising early local control of malignant pleural mesothelioma following postoperative intensitymodulated radiotherapy(imrt) to the chest. Cancer J 2003;9: [18] Weder W, Kestenholz P, Taverna C, et al. Neoadjuvant chemotherapyfollowed byextrapleural pneumonectomyin malignant pleural mesothelioma. J Clin Oncol 2004;22: [19] Anonymous. Long-term results of lung metastasectomy: prognostic analyses based on 5206 cases. The International Registryof Lung Metastases. J Thorac Cardiovasc Surg January1997;113(1): [20] Goldstraw P. The IASLC staging revision project. Lung Cancer 2003;41:S3 41.
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
The Proposed New International TNM Staging System for Malignant Pleural Mesothelioma: Application to Imaging
 323.....:. #{149} :. #{149}..: #{149}. #{149}. :- : Received June 22, 1995; accepted after revision September 12, 1995. 1 Department of Radiology, Duke University Medical Center, Box 3808, Dunham, NC 2771
323.....:. #{149} :. #{149}..: #{149}. #{149}. :- : Received June 22, 1995; accepted after revision September 12, 1995. 1 Department of Radiology, Duke University Medical Center, Box 3808, Dunham, NC 2771
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project
 INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Malignant Pleural Mesothelioma in Singapore
 RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Mesothelioma Current Approaches to a Difficult Problem. Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database
 Featured Article Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database Valerie W. Rusch 1, Dorothy Giroux 2 1 Memorial Sloan-Kettering Cancer Center, New
Featured Article Do we need a revised staging system for malignant pleural mesothelioma? Analysis of the IASLC database Valerie W. Rusch 1, Dorothy Giroux 2 1 Memorial Sloan-Kettering Cancer Center, New
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases
 Original Article Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases William G. Richards, PhD 1,2 ; John J. Godleski, MD 2,3 ; Beow Y.
Original Article Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases William G. Richards, PhD 1,2 ; John J. Godleski, MD 2,3 ; Beow Y.
Malignant pleural mesothelioma: outcome of limited surgical management
 Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma
 Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Surgical therapy of. who should be operated
 SAMO Interdisciplinary Workshop on Chest Tumors Lucerne, 13th and 14th January 2012 Surgical therapy of mesothelioma, who should be operated Walter Weder MD Professor of Surgery University Hospital Zurich
SAMO Interdisciplinary Workshop on Chest Tumors Lucerne, 13th and 14th January 2012 Surgical therapy of mesothelioma, who should be operated Walter Weder MD Professor of Surgery University Hospital Zurich
Recommendations for the Reporting of Pleural Mesothelioma
 Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Treatment of mesothelioma in Bloemfontein, South Africa
 European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
Sternotomy and removal of the tumor
 Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Malignant pleural mesothelioma P/D vs. EPP
 3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines
 Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
Post-operative intrapleural chemotherapy for mesothelioma
 Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
System for Malignant Pleural Mesothelioma'
 A Proposed New International TNM Staging System for Malignant Pleural Mesothelioma' From the International Mesothelioma Interest Group* Study objective: Investigation of the behavior and treatment of diffuse
A Proposed New International TNM Staging System for Malignant Pleural Mesothelioma' From the International Mesothelioma Interest Group* Study objective: Investigation of the behavior and treatment of diffuse
Surgical treatment for malignant pleural mesothelioma: extrapleural pneumonectomy, pleurectomy/decortication or extended pleurectomy?
 JBUON 2015; 20(2): 376-380 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com REVIEW ARTICLE Surgical treatment for malignant pleural mesothelioma: extrapleural pneumonectomy,
JBUON 2015; 20(2): 376-380 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com REVIEW ARTICLE Surgical treatment for malignant pleural mesothelioma: extrapleural pneumonectomy,
Post-recurrence survival in completely resected stage I non-small cell lung cancer with local recurrence
 Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Patterns of nodal spread in thoracic malignancies
 Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
Plueral Malignancy: Radiologic-pathologic
 Plueral Malignancy: Radiologic-pathologic Correlation Ritu R. Gill, MD Pleural Malignancies: Radiologic-Pathologic Correlation Ritu R Gill MD Brigham and Women s Hospital Boston, Massachusetts Pleural
Plueral Malignancy: Radiologic-pathologic Correlation Ritu R. Gill, MD Pleural Malignancies: Radiologic-Pathologic Correlation Ritu R Gill MD Brigham and Women s Hospital Boston, Massachusetts Pleural
Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline
 Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
What is the best way to diagnose and stage malignant pleural mesothelioma?
 doi:10.1510/icvts.2010.255893 Interactive CardioVascular and Thoracic Surgery 12 (2011) 254 259 Best evidence topic - Thoracic oncologic What is the best way to diagnose and stage malignant pleural mesothelioma?
doi:10.1510/icvts.2010.255893 Interactive CardioVascular and Thoracic Surgery 12 (2011) 254 259 Best evidence topic - Thoracic oncologic What is the best way to diagnose and stage malignant pleural mesothelioma?
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE MESOTHELIOMA Lung Site Group Mesothelioma Date Guideline Created: April 2013 Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE MESOTHELIOMA Lung Site Group Mesothelioma Date Guideline Created: April 2013 Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1.
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Brigham and Women s Hospital, Boston, MA, USA; 2 Verastem, Inc., Boston, MA, USA
 Determination of Biomarker Response in a Phase II Window of Opportunity Study of Defactinib (VS 6063), a Focal Adhesion Kinase (FAK) Inhibitor, in Patients with Resectable Malignant Pleural Mesothelioma
Determination of Biomarker Response in a Phase II Window of Opportunity Study of Defactinib (VS 6063), a Focal Adhesion Kinase (FAK) Inhibitor, in Patients with Resectable Malignant Pleural Mesothelioma
How To Treat A Cancer With A Radical
 Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
Use of imaging in the management of malignant pleural mesothelioma
 Clinical Radiology (2005) 60, 1237 1247 REVIEW Use of imaging in the management of malignant pleural mesothelioma R.E. Benamore a, M.J. O Doherty b, J.J. Entwisle a, * a Department of Radiology, University
Clinical Radiology (2005) 60, 1237 1247 REVIEW Use of imaging in the management of malignant pleural mesothelioma R.E. Benamore a, M.J. O Doherty b, J.J. Entwisle a, * a Department of Radiology, University
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
The National Clinical Lung Cancer Audit (LUCADA)
 The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Screening, early referral and treatment for asbestos related cancer
 Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Characteristics of Malignant Pleural Mesothelioma in Women
 Characteristics of Malignant Pleural Mesothelioma in Women Andrea S. Wolf, MD, MPH, William G. Richards, PhD, Tamara R. Tilleman, MD, PhD, Lucian Chirieac, MD, Shelley Hurwitz, PhD, Raphael Bueno, MD,
Characteristics of Malignant Pleural Mesothelioma in Women Andrea S. Wolf, MD, MPH, William G. Richards, PhD, Tamara R. Tilleman, MD, PhD, Lucian Chirieac, MD, Shelley Hurwitz, PhD, Raphael Bueno, MD,
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Malignant pleural mesothelioma: multidisciplinary experience in a public tertiary hospital*
 13 Original Article Malignant pleural mesothelioma: multidisciplinary experience in a public tertiary hospital* Ricardo Mingarini Terra 1, Lisete Ribeiro Teixeira 2, Ricardo Beyruti 1, Teresa Yae Takagaki
13 Original Article Malignant pleural mesothelioma: multidisciplinary experience in a public tertiary hospital* Ricardo Mingarini Terra 1, Lisete Ribeiro Teixeira 2, Ricardo Beyruti 1, Teresa Yae Takagaki
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Analysis of the effect of radiotherapy on malignant pleural mesothelioma when given on adjuvant or palliative basis
 Analysis of the effect of radiotherapy on malignant pleural mesothelioma when given on adjuvant or palliative basis Hesham A. El Hossieny, MD 1, Fatma Aboulkasem, MD 2, Abdel Rahman M.,MD 3. (1) Department
Analysis of the effect of radiotherapy on malignant pleural mesothelioma when given on adjuvant or palliative basis Hesham A. El Hossieny, MD 1, Fatma Aboulkasem, MD 2, Abdel Rahman M.,MD 3. (1) Department
1) Thoracic Surgery, Kyoto University Hospital. 2) Radiation Oncology and Image-Applied Therapy, Kyoto University Hospital
 Title Survival and relapse pattern after malignant pleural mesothelioma. Okubo, Kenichi; Sonobe, Makoto; Fuj Author(s) Tsuyoshi; Sakai, Hiroaki; Miyahara, Hiroshi; Shibuya, Keiko; Hiraoka, M Citation General
Title Survival and relapse pattern after malignant pleural mesothelioma. Okubo, Kenichi; Sonobe, Makoto; Fuj Author(s) Tsuyoshi; Sakai, Hiroaki; Miyahara, Hiroshi; Shibuya, Keiko; Hiraoka, M Citation General
Trimodality therapy for malignant pleural mesothelioma: results from an EORTC phase II multicentre trial
 Eur Respir J 2010; 36: 1362 1369 DOI: 10.1183/09031936.00039510 CopyrightßERS 2010 Trimodality therapy for malignant pleural mesothelioma: results from an EORTC phase II multicentre trial P.E. Van Schil*,
Eur Respir J 2010; 36: 1362 1369 DOI: 10.1183/09031936.00039510 CopyrightßERS 2010 Trimodality therapy for malignant pleural mesothelioma: results from an EORTC phase II multicentre trial P.E. Van Schil*,
Treatment of Malignant Pleural Mesothelioma: Is There a Benefit to Pleuropneumonectomy?
 55 Treatment of Malignant Pleural Mesothelioma: Is There a Benefit to Pleuropneumonectomy? Stacey Su, Michael T. Jaklitsch, and David J. Sugarbaker Malignant pleural mesothelioma (MPM) is a rare but highly
55 Treatment of Malignant Pleural Mesothelioma: Is There a Benefit to Pleuropneumonectomy? Stacey Su, Michael T. Jaklitsch, and David J. Sugarbaker Malignant pleural mesothelioma (MPM) is a rare but highly
A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy and Photodynamic Therapy
 CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.1.36 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:36-40 A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy
CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.1.36 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:36-40 A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy
The New International Staging System Lung Cancer
 The New International Staging System Lung Cancer Valerie W. Rusch, MD Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center Chair, Lung and Esophagus Task Force, American Joint Commission on Cancer
The New International Staging System Lung Cancer Valerie W. Rusch, MD Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center Chair, Lung and Esophagus Task Force, American Joint Commission on Cancer
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Imaging of pleural and chest wall tumors
 Thorac Surg Clin 14 (2004) 15 23 Imaging of pleural and chest wall tumors Michael J. Weyant, MD a, Raja M. Flores, MD a,b, * a Cardiothoracic Surgery, Memorial Sloan-Kettering Cancer Center, 1275 York
Thorac Surg Clin 14 (2004) 15 23 Imaging of pleural and chest wall tumors Michael J. Weyant, MD a, Raja M. Flores, MD a,b, * a Cardiothoracic Surgery, Memorial Sloan-Kettering Cancer Center, 1275 York
Principal Investigator: Valerie W. Rusch, MD, FACS, Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Materials and Methods. Results
 Anatomic Pathology / Malignant Pleural Mesothelioma Histologic Assessment and Prognostic Factors of Malignant Pleural Mesothelioma Treated With Extrapleural Pneumonectomy Andrea V. Arrossi, MD, 1 E. Lin,
Anatomic Pathology / Malignant Pleural Mesothelioma Histologic Assessment and Prognostic Factors of Malignant Pleural Mesothelioma Treated With Extrapleural Pneumonectomy Andrea V. Arrossi, MD, 1 E. Lin,
Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma
 Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma Based on AJCC/UICC TNM, 7th edition Protocol web posting date: February 1, 2011 Procedures Resection Authors
Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma Based on AJCC/UICC TNM, 7th edition Protocol web posting date: February 1, 2011 Procedures Resection Authors
Diagnosis and Prognosis of Pancreatic Cancer
 Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Image. 3.11.3 SW Review the anatomy of the EAC and how this plays a role in the spread of tumors.
 Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Thoracic 18F-FDG PETCT
 Thoracic 18F-FDG PETCT RAD Magazine, 41, 482, 13-16 Dr Allanah arker Specialist registrar radiology Dr Nagmi Qureshi Consultant cardiothoracic radiologist Papworth Hospital, Cambridge email: allanahbarker@nhs.net
Thoracic 18F-FDG PETCT RAD Magazine, 41, 482, 13-16 Dr Allanah arker Specialist registrar radiology Dr Nagmi Qureshi Consultant cardiothoracic radiologist Papworth Hospital, Cambridge email: allanahbarker@nhs.net
What is Mesothelioma?
 What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
MESOTHELIOMA. Not Just a Late Night Commercial. Graciela Hoal, RN, MSN, ACNP-BC
 MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
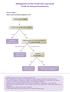 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Staging algorithm for diffuse malignant pleural mesothelioma
 doi:10.1510/icvts.2009.213611 Interactive CardioVascular and Thoracic Surgery 10 (2010) 185 189 report - Pulmonary Staging algorithm for diffuse malignant pleural mesothelioma a, a a b c Marcin Zieliński
doi:10.1510/icvts.2009.213611 Interactive CardioVascular and Thoracic Surgery 10 (2010) 185 189 report - Pulmonary Staging algorithm for diffuse malignant pleural mesothelioma a, a a b c Marcin Zieliński
GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT
 GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT 1) TOPIC OF THE EVENT MALIGNANT PLEURAL DISEASE 2) SUGGESTED TITLE : Approach to Pleural Cancer: State-of-the-Art 3) TYPE OF EVENT Course Native
GRANT APPLICATION FORM: ORGANISING AN ESO EDUCATIONAL EVENT 1) TOPIC OF THE EVENT MALIGNANT PLEURAL DISEASE 2) SUGGESTED TITLE : Approach to Pleural Cancer: State-of-the-Art 3) TYPE OF EVENT Course Native
People Living with Cancer
 Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
PET. Can we afford PET-CT. Positron annihilation. PET-CT scanner. PET detection
 PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
ASBESTOS MANAGEMENT REVIEW A CRITICAL REVIEW OF MEDICAL MANAGEMENT IN MALIGNANT PLEURAL MESOTHELIOMA - AUSTRALIA, 2011
 ASBESTOS MANAGEMENT REVIEW A CRITICAL REVIEW OF MEDICAL MANAGEMENT IN MALIGNANT PLEURAL MESOTHELIOMA - AUSTRALIA, 2011 Dr Malcolm Feigen Senior Radiation Oncologist Radiation Oncology Centre Austin Health
ASBESTOS MANAGEMENT REVIEW A CRITICAL REVIEW OF MEDICAL MANAGEMENT IN MALIGNANT PLEURAL MESOTHELIOMA - AUSTRALIA, 2011 Dr Malcolm Feigen Senior Radiation Oncologist Radiation Oncology Centre Austin Health
Malignant Pleural Mesothelioma. NCCN Guidelines for Patients
 Malignant Pleural Mesothelioma NCCN Guidelines for Patients Presented with support from the national law firm of Baron & Budd Also available at NCCN.com About this booklet Its purpose Learning that you
Malignant Pleural Mesothelioma NCCN Guidelines for Patients Presented with support from the national law firm of Baron & Budd Also available at NCCN.com About this booklet Its purpose Learning that you
Malignant pleural mesothelioma is a rare primary neoplasm,
 Assessment of Malignant Pleural Mesothelioma with F-FDG Dual-Head Gamma-Camera Coincidence Imaging: Comparison with Histopathology Victor H. Gerbaudo, PhD 1 ; David J. Sugarbaker, MD 2 ; Scott Britz-Cunningham,
Assessment of Malignant Pleural Mesothelioma with F-FDG Dual-Head Gamma-Camera Coincidence Imaging: Comparison with Histopathology Victor H. Gerbaudo, PhD 1 ; David J. Sugarbaker, MD 2 ; Scott Britz-Cunningham,
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Research Article Malignant Pleural Mesothelioma Outcomes in the Era of Combined Platinum and Folate Antimetabolite Chemotherapy
 Lung Cancer International Volume 2015, Article ID 590148, 7 pages http://dx.doi.org/10.1155/2015/590148 Research Article Malignant Pleural Mesothelioma Outcomes in the Era of Combined Platinum and Folate
Lung Cancer International Volume 2015, Article ID 590148, 7 pages http://dx.doi.org/10.1155/2015/590148 Research Article Malignant Pleural Mesothelioma Outcomes in the Era of Combined Platinum and Folate
Malignant Mesothelioma: an Update
 Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
General Rules SEER Summary Stage 2000. Objectives. What is Staging? 5/8/2014
 General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
Summary of treatment benefits
 Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer
 In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer Prostate cancer is the second most common cancer in men worldwide, accounting for 15% of all new cancer cases. 1 Great strides have
In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer Prostate cancer is the second most common cancer in men worldwide, accounting for 15% of all new cancer cases. 1 Great strides have
Malignant Mesothelioma
 Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
prognostic scoring systems. We
 Thorax 2000;55:731 735 731 Original articles Prognostic factors for malignant mesothelioma in 142 patients: validation of CALGB and EORTC prognostic scoring systems J G Edwards, K R Abrams, J N Leverment,
Thorax 2000;55:731 735 731 Original articles Prognostic factors for malignant mesothelioma in 142 patients: validation of CALGB and EORTC prognostic scoring systems J G Edwards, K R Abrams, J N Leverment,
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement during Initial Diagnosis
 Case Reports in Pulmonology Volume 2015, Article ID 962504, 4 pages http://dx.doi.org/10.1155/2015/962504 Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement
Case Reports in Pulmonology Volume 2015, Article ID 962504, 4 pages http://dx.doi.org/10.1155/2015/962504 Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement
Contemporary Management of Malignant Pleural Mesothelioma
 Contemporary Management of Malignant Pleural Mesothelioma ERIC G. BUTCHART University Hospital of Wales, Cardiff, United Kingdom Key Words. Mesothelioma Surgery Radiotherapy Chemotherapy Immunology Gene
Contemporary Management of Malignant Pleural Mesothelioma ERIC G. BUTCHART University Hospital of Wales, Cardiff, United Kingdom Key Words. Mesothelioma Surgery Radiotherapy Chemotherapy Immunology Gene
Multimodal therapy of malignant pleural mesothelioma: is the replacement of radical surgery imminent?
 Interactive CardioVascular and Thoracic Surgery Advance Access published November 21, 2012 Interactive CardioVascular and Thoracic Surgery (2012) 1 7 doi:10.1093/icvts/ivs465 ORIGINAL ARTICLE Multimodal
Interactive CardioVascular and Thoracic Surgery Advance Access published November 21, 2012 Interactive CardioVascular and Thoracic Surgery (2012) 1 7 doi:10.1093/icvts/ivs465 ORIGINAL ARTICLE Multimodal
Radical surgery for malignant pleural mesothelioma: results and prognosis
 doi:10.1510/icvts.2007.166322 Interactive CardioVascular and Thoracic Surgery 7 (2008) 102 106 www.icvts.org Institutional report - Thoracic general Radical surgery for malignant pleural mesothelioma:
doi:10.1510/icvts.2007.166322 Interactive CardioVascular and Thoracic Surgery 7 (2008) 102 106 www.icvts.org Institutional report - Thoracic general Radical surgery for malignant pleural mesothelioma:
Lung Cancer and Mesothelioma
 Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
