Gastrointestinal (GI) bleeding
|
|
|
- Hector Moore
- 10 years ago
- Views:
Transcription
1 Gastrointestinal (GI) bleeding Somchai Leelakusolvong, M.D. Div of Gastroenterology, Dept of Medicine, Siriraj Endoscopy Center address: RCPT อ ตรด ตถ
2 GI Bleeding Objective: To understand how to assess a patient who has upper GI and Mid-GI bleeding To tell the current medical treatment for upper GI and Mid-GI bleeding patients
3 Gastrointestinal (GI) Bleeding: Epidemiology USA : upper GI hemorrhage ~ : 100,000 cases Male : Female ~ 2 :1 Acute GI hemorrhage > chronic Upper GI hemorrhage > lower GI hemorrhage Mortality Upper GI hemorrhage ~ 3.5-7% Lower GI hemorrhage ~ 3.6% Surgery ~ 10% Rebleeding ~ 20%
4 Causes of UGI Bleeding Peptic ulcer disease % Erosive gastritis/duodenitis % Varices 8-15 % Mallory-Weiss Syndrome 8-15 % Esophagitis 6 % Neoplasm 3 % Miscellaneous 7 %
5 Gastrointestinal (GI) Hemorrhage: Classification Classification Upper GI hemorrhage = bleeding above Ligament of Treitz Lower GI hemorrhage = bleeding below Ligament of Treitz
6 Raju GS, et al. Gastroenterology 2007;133: Gastrointestinal bleeding Upper GI bleeding = bleeding above the ampulla of Vater Mid GI bleeding = bleeding from the ampulla of Vater to the terminal ileum Lower GI bleeding = colonic bleeding
7 Hematemesis / Melena Initial Assessment and Resuscitation Risk Stratification Low Risk 4. Supportive Treatment and Monitoring 5. Elective Endoscopy 6. PPI for Suspected Non-variceal Bleeding High Risk Endoscopy Available Yes 8. No Ulcer bleeding Variceal bleeding Others Refer
8 ockall scoring system for risk of rebleeding and death after admission to hospital for acute UGIB score ariable ge(y) < hock No shock (SBP>100,P< Tachycardia (SBP>100, Hypotension (SBP<100, P>100) 100) P>100) omorbidity Nil major Cardiac failure, ischemic heart disease, any major comorbidity Renal failure, liver failure, disseminated malignancy iagnosis MWT, no lesion, and All other diagnosis Malignancy of upper GI tract no SRH ajor SRH None or dark spot Blood in UGI tract, adherent clot, visible spurting vessel ch variable is scored and the total score calculated by simple addition H,stigmata of recent hemorrhage. MWT,Mallory Weiss tear
9 Correlation between Rockall score and rebleeding and mortality A total score of <3 is associated with excellent outcome, where as a score >8 carries a high mortality Risk score n Rebleed (%) Mortality (%) (5) 9(3) 18 (5) 50 (11) 76 (14) 83 (24) 102 (33) 113 (44) 101 (42) 0(0) 0(0) 1 (0.2) 13 (3) 28 (5) 49 (11) 54 (17) 72 (27) 78 (41) Rockall et al. Gut 1996; 38: Sanders DS. Am J Gastroenterol 2002
10 Endoscopic treatment. Evaluate of SRH at ulcer bases SRH of Ulcer Rebleeding Surgery Death lean base 5% 0.5% 2% pot 10% 6% 3% dherent clot 22% 10% 7% BVV 43% 34% 11% ctive bleeding 55% 35% 11% Clean base Spot Adherent clot NBVV Active bleeding
11 Demographic data overall low risk high risk p-value Age 62± 16 58±17 70±11 <0.0001* Sex (Male) 287(71%) 203(71%) 84(71%) 0.93 Underlying disease -Heart disease 120 (22.3%) 71(22.3%) 49(22.2%) 0.04* -Renal disease 30(5.5%) 17(5.3%) 13 (5.9%) Liver disease 34(6.3%) 19(6%) 15(6.9%) 0.04* -Malignancy 27(5%) 13(4.1%) 14(6.3%) 0.007* -Stroke 47(8.7%) 30(9.4%) 17(7.7%) COPD 16(3%) 9(2.8%) 7(3.2%) DM 99(18.4%) 55(17.3%) 44(19.9%) * -Hypertension 166(30.8%) 104(32.7%) 62(28.1%) 0.002* Drugs use -Aspirin 109(27%) 66(23%) 43(36%) 0.006* -Clopidogrel 31(8%) 15(5%) 16(14%) 0.004* -NSAIDs 115(28%) 86(30%) 29(25%) 0.27 Alcohol drinking 0.01* - never 230(57%) 151(52%) 79(67%) - active drinker 171(42%) 134(47%) 37(31%) - ex-drinker 4(1%) 2(1%) 2(2%) Bleeding before admission(hours) 35±41 39±44 25± *
12 Presenting symptoms of non-variceal Laosanguanek N, Bubthamala J, Leelakusolvong S, Charuscharoenwitthaya P. 201 upper GI Bleeding in Thai patients Presenting symptom overall low risk high risk -Coffee ground 70(17%) 51(18%) 19(16%) -Hematemesis 129(32%) 88(31%) 41(35%) -Melena 190(47%) 136(47%) 54(46%) -Hematochezia 16(4%) 12(4%) 4(3%)
13 Causes of NVUGIHg in Thai patients Cause of bleeding overall low risk high risk Clean based ulcer 170(42%) 142(49%) 28(24%) Hemorrhagic spot ulcer 28(7%) 23(8%) 5(4%) Adherent clot with ulcer 12(3%) 4(1%) 8(7%) NBVV with ulcer 54(13%) 17(6%) 37(31%) Active ulcer bleeding 17(4%) 6(2%) 11(9%) Esophageal ulcer 12(3%) 8(3%) 4(3%) Gastroduodenitis 50(12%) 42(15%) 8(7%) Esophagitis 10(2.5%) 9(3%) 1(1%) Mallory Weiss tear 15(3.7%) 13(5%) 2(2%) Dieulafoy's lesion 3(0.7%) 2(0.7%) 1(1%) Angiodysplasia 3(0.7%) 1(0.4%) 2(2%) GI malignancy 13(3.2%) 5(1.7%) 8(7%)
14 Hematemesis / Melena Initial Assessment and Resuscitation Risk Stratification Low Risk High Risk Supportive Treatment and Monitoring PPI for Suspected Non-variceal Bleeding Somatostatin for Suspected Variceal Bleeding Elective Endoscopy Endoscopy Available Yes 8. No Ulcer bleeding Variceal bleeding Others Refer
15 Non-variceal and Variceal Bleeding Pongprasobchai S. World J Gastroenterology 2009;15:
16 Pongprasobchai S. World J Gastroenterology 2009;15: Non-variceal and Variceal Bleeding Accuracy 82%
17 Management goals for upper GI bleeding Resuscitation Identification of bleeding site Cessation of active bleeding Prevention of recurrence of bleeding
18 Initial Management Early intensive-care monitoring* Reduce time to hemodynamic stabilization Reduce mortality rate UGI bleeding team** Improve overall MR 8% compared with 14% *Baradarian R. Am J Gastroenterol. 2004
19 Stevens. Gastrointest Endosc 1997 Barkun A.Ann Intern med 2003 GI Bleeding Team Versus General GI for treatment of bleeding ulcers GI team General GI N=45 N=45 p Rebleeding 16% 31% <0.05 Surgery 4% 20% <0.05 Mortality 4% 11% <0.10 Length of stay <0.05 Hospital charge $29,819 $76,935 <0.05
20 Hemostasis Initial hemostasis - Endoscopic therapy - Pharmacologic therapy Prevent rebleeding - Pharmacologic therapy - Second look endoscopy
21 nternational Consensus on Nonvariceal Barkun AN, et al. Ann Intern Med 2010;152: Upper Gastrointestinal Bleeding A. Resuscitation, risk assessment, and preendoscopy management A1. Immediately evaluate and initiate appropriate resuscitation. A2. Prognostic scales are recommended for early stratification of patients into low- and high-risk categories for rebleeding and mortality. A3. Consider placement of a nasogastric tube in selected patients because the findings may have prognostic value. A4. Blood transfusions should be administered to a patient with a hemoglobin level 70 g/l. A5. In patients receiving anticoagulants, correction of coagulopathy is recommended but should not delay endoscopy.
22 1. Hematemesis / Melena 2. Initial Assessment and Resuscitation 3. Risk Stratification 3A Low Risk 3B High Risk 4. supportive Treatment and Monitoring 6. PPI for Suspected Non-variceal Bleeding 7. Somatostatin for Suspected Variceal Bleeding 5. Elective Endoscopy Endoscopy Available Yes 8. No Ulcer bleeding Variceal bleeding Others Refer
23 Empirical Therapy Nonvariceal upper GI haemorrhage - Acid related disease: > 75% - Bleeding peptic ulcer ~ 75% stop spontaneously ~ 25% recurrent bleeding Laine L, N Engl J Med, 1994
24 Treatments of Non-variceal UGIH Medical treatment Endoscopic treatment Radiology intervention Surgical treatment
25 Pharmacologic Therapy Acid suppressing agents H 2 -receptor antagonists (H 2 RAs), proton pump inhibitors (PPIs) Splanchnic blood pressure modifiers vasopressin, somatostatin, octreotide Anti-fibrinolytic agents tranexamic acid
26 Role of PPI in Non-variceal Upper GiHg sk stratification TIME Day 0 Day 1 Day 2 Day 3 PPI Before PPI After endoscopy pper Gi Hg Endoscopy + Therapeutics
27 Timing for endoscopy in high risk nonvariceal upper GIHg Study compare 0-6 hr and 6-24 hr for endoscopy Retrospective review in 169 patients (77 patients 0-6 hr and 92 patients 6-24 hr) No difference in Rebleeding Surgery Mortality Readmission within 30 days Targownik LE, et al. Can J Gastroenterol 2007;21:425
28 PPI before Endoscopy in non-variceal Upper Gastrointestinal Hemorrhage Pooled rate (%) PPI (IV or Oral) Control 0 4 RCTs Mortality OR=1.12 ( ) Total n =1,512 Re-bleeding OR=0.81 ( ) Surgery OR=0.96 ( ) Reduced proportion of patient with SRH OR=0.67( ) Dorward S et al. Cochrane Review 2006 issue 4
29 Omeprazole before endoscopy in patients with GI bleeding 80 mg iv bolus then 8mg/hr infusion n=319 n=319 Omeprazole 80 mg iv bolus then 8 mg/hr ns ns ns
30 PPI treatment for acute peptic ulcer bleeding Parameters No Mortality Rebleeding Surgery study (OR) (OR) (OR) 04 Type of control 04.1 PPI vs H 2 RA ( ) 04.2 PPI vs placebo ( ) 0.61 ( ) 05 Route of PPI administration 05.1 Oral PPI ( ) 0.38 ( ) 05.2 iv. PPI ( ) 0.69 ( ) 06 PPI dose 06.1 High dose PPI ( ) 0.61 ( ) 06.2 Low dose PPI ( ) 0.61 ( ) (oral or low iv. Dose) Leontiadis GI et al. Cochrane Review 2006
31 PPI treatment for acute peptic ulcer bleeding Parameters No study Mortality (OR) Rebleeding (OR) Surgery (OR) 07 Initial endoscopic hemostatic treatment 07.1 With initial EHT ( ) 0.60 ( ) 07.2 Without initial EHT ( ) 0.62 ( ) 08 PPI dose for studies allowing initial endoscopic hemostatic treatment 08.1 Oral or low ( ) dose iv. PPI 08.2 High dose iv. PPI ( ) 0.61 ( ) Leontiadis GI et al. Cochrane Review 2006
32 nternational Consensus on Nonvariceal Upper Gastrointestinal Bleeding A. Resuscitation, risk assessment, and preendoscopy management A6. Promotility agents should not be used routinely before endoscopy to increase the diagnostic yield. A7. Selected patients with acute ulcer bleeding who are at low risk for rebleeding on the basis of clinical and endoscopic criteria may be discharged promptly after endoscopy. A8. Preendoscopic PPI therapy may be considered to downstage the endoscopic lesion and decrease the need for endoscopic intervention but should not delay endoscopy. Barkun AN, et al. Ann Intern Med 2010;152:
33 Barkun AN, et al. Ann Intern Med 2010;152: nternational Consensus on Nonvariceal Upper Gastrointestinal Bleeding B. Endoscopic management B1. Develop institution-specific protocols for multidisciplinary management. Include access to an endoscopist trained in endoscopic hemostasis. B2. Have available on an urgent basis support staff trained to assist in endoscopy. B3. Early endoscopy (within 24 hours of presentation) is recommended for most patients with acute upper gastrointestinal bleeding. B4. Endoscopic hemostatic therapy is not indicated for patients with low-risk stigmata (a clean-based ulcer or a nonprotuberant pigmented dot in an ulcer bed).
34 Leontiadis GI et al. Cochrane Review 20 PPI treatment for acute peptic ulcer bleeding Conclusions PPI treatment in PU bleeding reduces rebleeding and surgery compared with placebo or H2RA but not on all-cause mortality All-cause mortality was reduced only in Asian studies; reductions in rebleeding and surgery were quantitatively greater in Asian studies.
35 The use of vasoconstrictor therapy in non-variceal upper GI bleeds Meta-analysis of 14 RCTs show good evidence for Somatostatin to reduce rebleeding Trend for reducing surgery Rebleeding with NNT 11 2 octreotide studies in meta-analysis have completely different conclusions The blinded trial showing no effect on outcome The non-blinded trial concluded that it stopped PU bleed Decrease Tx requirements Need for surgery Not superior to ranitidine* May G et al. Emerg Med J 2006;23:722
36 Meta-analysis Tranexamic acid vs Placebo : all-cause mortality N = 1754 patients 7 trials, compared with placebo Gluud LL et al. APT 2008 Feb
37 Barkun AN, et al. Ann Intern Med 2010;152: nternational Consensus on Nonvariceal Upper Gastrointestinal Bleeding. Pharmacologic management C1. H 2 RAs are not recommended for patients with acute ulce leeding. C2. Somatostatin and octreotide are not routinely ecommended for patients with acute ulcer bleeding. C3. An intravenous bolus followed by continuous-infusion PI therapy should be used to decrease rebleeding and ortality in patients with high-risk stigmata who have ndergone successful endoscopic therapy. C4. Patients should be discharged with a prescription for a ingle daily-dose oral PPI for a duration as dictated by the nderlying etiology.
38 nternational Consensus on Nonvariceal Upper Gastrointestinal Bleeding D. Nonendoscopic and nonpharmacologic inhospital management D1. Patients at low risk after endoscopy can be fed within 24 hours. D2. Most patients who have undergone endoscopic hemostasis for high-risk stigmata should be hospitalized for at least 72 hours thereafter. D3. Seek surgical consultation for patients for whom endoscopic therapy has failed. D4. Percutaneous embolization can be considered as an alternative to surgery for patients for whom endoscopic therapy has failed. D5. Patients with bleeding peptic ulcers should be tested for H. pylori and receive eradication therapy if it is present, with confirmation of eradication. D6. Negative H. pylori diagnostic tests obtained in the acute setting should be repeated.
39 Endoscopic hemostasis : Cook et al. Gastroenterol 1992;102: Endpoint Meta-analysis OR (95% CI) Rebleeding 0.38 ( ) Surgery 0.36 ( ) Death 0.55 ( ) Endoscopy Better 1 ODDS Ratio No Endoscopy Better
40 Endoscopic hemostatic methods Thermal Bipolar probe Heater probe Laser Argon plasma coagulation Monopolar probe Microwave Injection Epinephrine Alcohol Ethanolamine Cyanoacrylate Polidocanol Thrombin Mechanical Hemoclips Sewing Band ligation Endoloop Combination Epinephrine+thermal Epinephrine+hemoclips hemoclips Epinephrine+laser
41 Injection Therapy Epinephrine(1:10,000-20,000) Saline : hypertonic saline Absolute alcohol Water Ethanolamine Cyanoacrylate Polidocanol Thrombin Fibrin
42 Thermal Coaptive Therapy Heater probe, Multipolar probe Mechanism Physically compress & tamponade Thermal energy sealing the wall of vessel
43 Heater probe
44 Mechanical Devices Clips, band ligators, Endo-loop Mechanism Mechanical closure of bleeding vessel
45
46 Clip Best suitable for spurting bleed and visible vessels Lower rebleeding rate Minor tissue damage May be the only option in large vessels >1mm 15.7% technical difficulties Location - tangential, retroflex position of endoscope Lesion - fibrotic scar
47 Is a second look necessary? A meta-analysis Marmo et al. found that routine second look (24 hr later) endoscopy with retreatment as appropriate, significantly reduced the risk of recurrent bleeding, but did not substantially reduce the rates of surgery or mortality The absolute risk reduction in re-bleeding was 6.2% (P < 0.01) Absolute risk reductions for surgery and mortality were, respectively, 1.7% and 1.0% (P=N.S.) Thus, second look endoscopy has failed to prove that it has an effect on key outcome parameters Marmo 7. et al. Gastrointest Endosc 2003; 57: 62 Messmann et al, Endoscopy. 1998
48 Failure Endoscopic Therapy Risk factors associated with treatment failure with combination injection therapy and heater probe; Hypertension Hb < 10 g/dl Fresh blood in the stomach Ulcer with active bleeding Ulcer > 2 cm Wong SK, et al. Gut 2002;50:
49 Indication for Surgery 1. Continued active bleeding and unable to perform endoscopy 2. Require blood transfusion > 6 units/24 hr 3. Failure of endoscopic treatment 3. Rebleeding after successful endoscopic treatment
50 Classification of Gastric Varices GOV2 16% GOV1 74% IGV1 6% IGV2 2%
51 Esophageal variceal treatment Package
52 Seng-Staken Blakemore tube
53 Gastric Varices Pretreatment cyanoacrylate Post-treatment cyanoacrylate
54 ENDOSCOPIC IMAGES OF MILD AND SEVERE PORTAL HYPERTENSIVE GASTROPATHY Carpinelli et al. Ital J Gastroenterol Hepatol 1997; 29:533 Mild Severe Mosaic pattern Mosaic pattern + red spots
55 Gastric varix injection with Glue
56 Treatment of Variceal Bleeding Endoscopic treatment Somatostatin S-B tube Stop bleed Rebleeding Complicat n Onset Cost 70-90% 20% 2-22% immediate % 40% Low 1-2 hrs % 50% 15-68% immediate +
57 Recommendation for treatment acute variceal hemorrhage Variceal bleeding should be managed in the ICU Blood volume replacement should be performed using Concentrated erythrocytes, to obtain a hemoglobin level of about g/l Plasma expanders (crystalloid or colloid), to maintain hemodynamic stability renal perfusion pressure) Antibiotic prophylaxis should be given to all patients Endoscopy should be performed as soon as possible (within 12 h after hospital admission) Garcia-Tsao G, et al. Hepatology 2007;46:922
58 Recommendation for treatment acute variceal hemorrhage Specific treatment should consist of combination therapy with a vasoactive drug and endoscopic treatment: Intravenous vasoactive therapy with one of the following drugs should be started as soon as possible after hospital admission, before diagnostic endoscopy, and maintained for 2(3)-5 d: Terlipressin: #1-2 mg every 4 h Somatostatin: bolus of 250 µg following by infusion of 250 µg/h Octreotide: infusion of µg/h, possibly preceded by bolus of µg Vapreotide: #bolus of 50 µg followed by infusion of 50 µg/h Garcia-Tsao G, et al. Hepatology 2007;46:922
59 Recommendation for treatment acute variceal hemorrhage Either EVL or EVS can be performed but EVL is the recommended first-line treatment In cases of acute gastric variceal bleeding, variceal obturation with a tissue adhesive (N-2-butyl-cyanoacrylate) is recommended If combined therapy fails, endoscopic treatment should be repeated or TIPS performed (second-line treatment). If repeat endoscopic treatment fails, TIPS is justified Note: TIPS = transjugular intrahepatic portosystemic shunt. *These recommendations are based on information from recent consensus statements on the management of portal hypertension. Garcia-Tsao G, et al. Hepatology 2007;46:922
60 lgorithm for treatment acute variceal hemorrhage Variceal bleeding suspected Early vasoactive drug therapy, endoscopic screening (within 12 h after admission) and antibiotic prophylaxis Variceal bleeding confirmed Endoscopic therapy: maintain vasoactive drug therapy for 2(3)-5 d Bleeding controlled Secondary prophylaxis by 5 days Bleeding not controlled Second attempt at endoscopic therapy Nonselective Beta-blocker therapy or endoscopic band ligation or both arcia-tsao G, et al. Hepatology 2007;46:922 Bleeding not controlled TIPS; if massive bleeding, conduct
61 Antibiotic Prophylaxis Antibiotic prophylaxis after endoscopy for UGIB - Norfloxacin 400 mg BID X 7 days after endoscopy or iv. Ciprofloxacin* - In patients with advanced cirrhosis iv. ceftriaxone (1gm/day) may be preferable particularly in centers with high prevalence of quinolone-resistant organisms* - rate of bacterial infection 19% - rate of SBP 7% - mortality rate 9% - Standard recommendation *Garcia-Tsao G, et al. Hepatology 2007;46:922 Bernard B, et al. Hepatology 1999; 29: Rimola A, et al. J Hepatol 2000; 32:
62 Obscure GI bleeding: Definition Obscure GI bleeding = bleeding from the GI tract that persists or recurs without an obvious etiology after esophagogastroduodenoscopy (EGD) colonoscopy, and radiologic evaluation of the small bowel such as small bowel follow-through or enteroclysis categorized into obscure overt obscure occult Raju GS, et al. Gastroenterology 2007;133:
63 Double balloon enteroscopy (DBE)
64 Single balloon enteroscopy (SBE)
65 Spiral enteroscopy
66 Enteroscopy: Indications Indications: Included all patients who were evaluated for small bowel pathology Diagnosis Treatment Surveillance: Polyposis syndrome Relative contraindications: Adhesion bands from prior surgery Underlying disease: Crohn s disease Large esophageal varices (antegrade approach) Absolute contraindications: Perforation Not suitable condition: Shock
67 Etiology of Obscure GI Bleeding Upper GI and lower GI bleeding overlooked Mid GI bleeding Upper GI lesions Younger than 40 years of age Cameron s erosions Tumors Fundic varices Meckel s diverticulum Peptic ulcer Dieulafoy s lesion Angiectasia Crohn s disease Dieulafoy s lesion Celiac disease Gastric antral vascular ectasia Older than 40 years of age Lower GI lesions Angiectasia Angiectasia NSAID enteropathy Neoplasms Celiac disease Uncommon Hemobilia Hemosuccus pancreaticus Aortoenteric fistula
68 Single or Double Balloon Enteroscope
69
70 Enteroscopy: Indication (Siriraj experience) Small bowel ulcer 3% Other 13% # of patients =97 # of procedures=107 Male =55 Female =42 Partial small bowel obstruction 4% Antegrade =100 Retrograde =7 IBD (Crohn and UC) 4% Tumor 4% GI Bleeding 56% Chronic diarrhea 16% Leelakusolvong S, et al. 2010
71 62 y/o female with AML in complete remission, 10 bouts of melena with negative prior bidirectional endoscopy and CE
72 70 y/o male with repeated melena and maroon stoo and negative bidirectional endoscopy
73 70 y/o male with repeated melena and maroon stoo with negative bidirectional endoscopy
74 SBE: Results (Siriraj experience, N=107 Finding Number (%) Ulcer 17 (16) Diverticulosis (Jejunal=6, colon=4) 10 (9) IBD (Crohn s=5, UC=1) 6 (6) Jejunal polyp 4 (4) Lymphangiectasia 4 (4) Small bowel cancer 3 (3) Enteritis 3 (3) Angiodysplasia 3 (3) Small bowel TB 3 (3) CBD stone 2 (2) Capillariasis 1 (1) Lymphoma 1 (1) Normal finding 50 (45)
75
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD
 Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
GI Bleeding. Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics
 GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
UGI Tract Hemorrhage. GI Tract Emergencies. UGI Hemorrhage. David D. Markowitz, MD. UGI tract hemorrhage Comorbid disease
 UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding
 Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Management and Prevention of Upper GI Bleeding
 Management and Prevention of Upper GI Bleeding By Jiwon Kim, Pharm.D., BCPS, FCSHP Reviewed by Clarence Chant, Pharm.D., FCSHP, FCCP, BCPS; and Steven E. Pass, Pharm.D., FCCP, FCCM, BCPS Learning Objectives
Management and Prevention of Upper GI Bleeding By Jiwon Kim, Pharm.D., BCPS, FCSHP Reviewed by Clarence Chant, Pharm.D., FCSHP, FCCP, BCPS; and Steven E. Pass, Pharm.D., FCCP, FCCM, BCPS Learning Objectives
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Surgical Management of GI Bleeding. VA Case Presentation. 0-24 hours 9/18/2012
 Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
SIGN. Management of acute upper and lower gastrointestinal bleeding. September 2008. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
New Anticoagulants and GI bleeding
 New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
AASLD PRACTICE GUIDELINES Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis
 AASLD PRACTICE GUIDELINES Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis Guadalupe Garcia-Tsao, 1 Arun J. Sanyal, 2 Norman D. Grace, 3 William Carey, 4 and the
AASLD PRACTICE GUIDELINES Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis Guadalupe Garcia-Tsao, 1 Arun J. Sanyal, 2 Norman D. Grace, 3 William Carey, 4 and the
HemoClip: Guidelines & Atlas
 HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas
 Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial
 Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
TEST QUESTIONS GASTROINTESTINAL BLEEDING
 TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
Acute Gastrointestinal Bleeding
 EMERGENCY MEDICINE BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, PUBLISHER Bruce M. White EXECUTIVE EDITOR Debra Dreger SENIOR EDITOR Bobbie Lewis EDITOR Robert Litchkofski ASSISTANT EDITOR Melissa Frederick
EMERGENCY MEDICINE BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, PUBLISHER Bruce M. White EXECUTIVE EDITOR Debra Dreger SENIOR EDITOR Bobbie Lewis EDITOR Robert Litchkofski ASSISTANT EDITOR Melissa Frederick
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
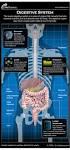 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
American Journal of Gastroenterology ISSN 0002-9270
 American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Gastrointestinal bleeding
 Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
How to Effectively Code for Endoscopic Procedures in Gastroenterology
 How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
Evaluation and Prognosis of Patients with Cirrhosis
 Evaluation and Prognosis of Patients with Cirrhosis Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded
Evaluation and Prognosis of Patients with Cirrhosis Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded
June 11, 2015 Tim Halterman
 June 11, 2015 Tim Halterman Defini&on Histologic change + loss of liver function Derives from Greek word kirrhos meaning yellow, tawny First named by Rene Laennec in 1819 Laennec s cirrhosis=alcoholic
June 11, 2015 Tim Halterman Defini&on Histologic change + loss of liver function Derives from Greek word kirrhos meaning yellow, tawny First named by Rene Laennec in 1819 Laennec s cirrhosis=alcoholic
LOWER GASTROINTESTINAL BLEEDING GED/05/08
 LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
Screening for Varices and Prevention of Bleeding
 Hepatitis C Online PDF created August 24, 2016, 3:30 am Screening for Varices and Prevention of Bleeding Module 3: Lesson 3: Contents: Management of Cirrhosis-Related Complications Screening for Varices
Hepatitis C Online PDF created August 24, 2016, 3:30 am Screening for Varices and Prevention of Bleeding Module 3: Lesson 3: Contents: Management of Cirrhosis-Related Complications Screening for Varices
1802 CLINICAL REVIEWS
 1802 CLINICAL S nature publishing group Management and Treatment of Patients With Cirrhosis and Portal Hypertension: Recommendations From the Department of Veterans Affairs Hepatitis C Resource Center
1802 CLINICAL S nature publishing group Management and Treatment of Patients With Cirrhosis and Portal Hypertension: Recommendations From the Department of Veterans Affairs Hepatitis C Resource Center
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Endoscopic Management of Acute Lower Gastrointestinal Bleeding
 American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2008.02075.x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management
American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2008.02075.x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management
New Treatments for Stroke Prevention in Atrial Fibrillation. John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013
 New Treatments for Stroke Prevention in Atrial Fibrillation John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013 Classification Paroxysmal atrial fibrillation (AF) Last < 7
New Treatments for Stroke Prevention in Atrial Fibrillation John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013 Classification Paroxysmal atrial fibrillation (AF) Last < 7
GASTRO-INTESTINAL BLEEDING
 Introduction Site of Bleeding History Physical Examination Laboratory Tests Investigation Treatment References Introduction Gastrointestinal bleeding is an uncommon but important sign in paediatric patients.
Introduction Site of Bleeding History Physical Examination Laboratory Tests Investigation Treatment References Introduction Gastrointestinal bleeding is an uncommon but important sign in paediatric patients.
Long term anticoagulant therapy in patients with atrial fibrillation at high risk of stroke: a new scenario after RE-LY trial
 Long term anticoagulant therapy in patients with atrial fibrillation at high risk of stroke: a new scenario after RE-LY trial Camillo Autore Università di Roma Sapienza II Facoltà di Medicina e Chirurgia
Long term anticoagulant therapy in patients with atrial fibrillation at high risk of stroke: a new scenario after RE-LY trial Camillo Autore Università di Roma Sapienza II Facoltà di Medicina e Chirurgia
Inhibit terminal acid secretion from parietal cells by blocking H + /K + - ATPase pump
 Chris J. Taylor, Pharm.D., BCPS Clinical Pharmacist Phoenix VA Health Care System Review pharmacology of PPIs Discuss possible association between PPI use and development of the following: Pneumonia (community-acquired
Chris J. Taylor, Pharm.D., BCPS Clinical Pharmacist Phoenix VA Health Care System Review pharmacology of PPIs Discuss possible association between PPI use and development of the following: Pneumonia (community-acquired
HOW I DO IT Approach to lower gastrointestinal bleeding
 HOW I DO IT Approach to lower gastrointestinal AUTHORSHIP How I do it: Roque Sáenz MD Eduardo Valdivieso MD, MSc The Latin-American Advanced Gastrointestinal Endoscopy Training Center Clínica Alemana,
HOW I DO IT Approach to lower gastrointestinal AUTHORSHIP How I do it: Roque Sáenz MD Eduardo Valdivieso MD, MSc The Latin-American Advanced Gastrointestinal Endoscopy Training Center Clínica Alemana,
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
After the Cure: Long-Term Management of HCV Liver Disease Norah A. Terrault, MD, MPH
 After the Cure: Long-Term Management of HCV Liver Disease Norah A. Terrault, MD, MPH Professor of Medicine Department of Gastroenterology Director, Viral Hepatitis Center University of California San Francisco
After the Cure: Long-Term Management of HCV Liver Disease Norah A. Terrault, MD, MPH Professor of Medicine Department of Gastroenterology Director, Viral Hepatitis Center University of California San Francisco
STROKE PREVENTION IN ATRIAL FIBRILLATION. TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: ABBREVIATIONS: BACKGROUND:
 STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
Awareness of the inappropriate use of GI prophylaxis and its cost. Adverse effects of proton pump inhibitor
 Understand the indication for stress ulcer/gi prophylaxis Awareness of the inappropriate use of GI prophylaxis and its cost Adverse effects of proton pump inhibitor A. 65yo w/ HTN and ESRD on HD p/w left
Understand the indication for stress ulcer/gi prophylaxis Awareness of the inappropriate use of GI prophylaxis and its cost Adverse effects of proton pump inhibitor A. 65yo w/ HTN and ESRD on HD p/w left
Learning Luncheon 7: Endoscopic Mucosal Resection: When, Where and How?
 Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Evolution of Barrett s esophagus
 Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department!
 Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding.
 Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding. Through innovation and continuous educational support, we offer a wide range
Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding. Through innovation and continuous educational support, we offer a wide range
CLINICAL CONSEQUENCES OF PORTAL HYPERTENSION
 Página 1 de 10 CLINICAL CONSEQUENCES OF PORTAL HYPERTENSION Part of "11 - PORTAL HYPERTENSION" The portal hypertensive syndrome is responsible for many of the manifestations of advanced, decompensated
Página 1 de 10 CLINICAL CONSEQUENCES OF PORTAL HYPERTENSION Part of "11 - PORTAL HYPERTENSION" The portal hypertensive syndrome is responsible for many of the manifestations of advanced, decompensated
National Digestive Diseases Information Clearinghouse
 Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
REVIEW CLINICAL REVIEWS
 1802 CLINICAL S nature publishing group Management and Treatment of Patients With Cirrhosis and Portal Hypertension: Recommendations From the Department of Veterans Affairs Hepatitis C Resource Center
1802 CLINICAL S nature publishing group Management and Treatment of Patients With Cirrhosis and Portal Hypertension: Recommendations From the Department of Veterans Affairs Hepatitis C Resource Center
Antiplatelet and Antithrombotic Therapy. Dr Curry Grant Stroke Prevention Clinic Quinte Health Care
 Antiplatelet and Antithrombotic Therapy Dr Curry Grant Stroke Prevention Clinic Quinte Health Care Disclosure of Potential for Conflict of Interest Dr. F.C. Grant Atrial Fibrillation FINANCIAL DISCLOSURE:
Antiplatelet and Antithrombotic Therapy Dr Curry Grant Stroke Prevention Clinic Quinte Health Care Disclosure of Potential for Conflict of Interest Dr. F.C. Grant Atrial Fibrillation FINANCIAL DISCLOSURE:
New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation. Joy Wahawisan, Pharm.D., BCPS April 25, 2012
 New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation Joy Wahawisan, Pharm.D., BCPS April 25, 2012 Stroke in Atrial Fibrillation % Stroke 1991;22:983. Age Range (years) CHADS 2 Risk
New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation Joy Wahawisan, Pharm.D., BCPS April 25, 2012 Stroke in Atrial Fibrillation % Stroke 1991;22:983. Age Range (years) CHADS 2 Risk
Duration of Dual Antiplatelet Therapy After Coronary Stenting
 Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013
 Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013 Family physician with Rivergrove Medical Clinic Practice in the north end since 1985 Medical Director of the Wellness
Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013 Family physician with Rivergrove Medical Clinic Practice in the north end since 1985 Medical Director of the Wellness
Damage Control in Abdominal Trauma
 Damage Control in Abdominal Trauma Steven Stylianos, MD Surgeon-in-Chief, Morgan Stanley Children s Hospital Rudolph Schullinger Professor of Surgery, Columbia University College of Physicians & Surgeons
Damage Control in Abdominal Trauma Steven Stylianos, MD Surgeon-in-Chief, Morgan Stanley Children s Hospital Rudolph Schullinger Professor of Surgery, Columbia University College of Physicians & Surgeons
Optimal injection volume of epinephrine for endoscopic treatment of peptic ulcer bleeding
 PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 May 21; 12(19): 3108-3113 World Journal of Gastroenterology ISSN 1007-9327 [email protected] 2006 The WJG Press. All rights reserved. RAPID COMMUNICATION
PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 May 21; 12(19): 3108-3113 World Journal of Gastroenterology ISSN 1007-9327 [email protected] 2006 The WJG Press. All rights reserved. RAPID COMMUNICATION
Dual Antiplatelet Therapy. Stephen Monroe, MD FACC Chattanooga Heart Institute
 Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
The author has no disclosures
 Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 [email protected] This presentation will discuss unlabeled and investigational use of products The author
Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 [email protected] This presentation will discuss unlabeled and investigational use of products The author
CLINICAL PRACTICE GUIDELINES
 CLINICAL PRACTICE GUIDELINES April 2003 MOH/P/PAK/ (GU) MANAGEMENT OF NON-VARICEAL UPPER GASTROINTESTINAL BLEEDING MINISTRY OF HEALTH MALAYSIAN SOCIETY ACADEMY OF MEDICINE, MALAYSIA OF MALAYS IA GASTROENTEROLOGY
CLINICAL PRACTICE GUIDELINES April 2003 MOH/P/PAK/ (GU) MANAGEMENT OF NON-VARICEAL UPPER GASTROINTESTINAL BLEEDING MINISTRY OF HEALTH MALAYSIAN SOCIETY ACADEMY OF MEDICINE, MALAYSIA OF MALAYS IA GASTROENTEROLOGY
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Acute Myocardial Infarction (the formulary thrombolytic for AMI at AAMC is TNK, please see the TNK monograph in this manual for information)
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
Articles Presented. Journal Presentation. Dr Albert Lo. Dr Albert Lo
 * This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
* This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
Vikram S. Kumar Gillian Lieberman, MD. September 2002. Lower GI Bleeds. Vikram Sheel Kumar, Harvard Medical School Year III Gillian Lieberman, MD
 September 2002 Lower GI Bleeds Vikram Sheel Kumar, Harvard Medical School Year III Index Case maroon/bright red: think lower GI bleed Mr. X, 78 years old, presents w/ maroon stool and eighteen hours of
September 2002 Lower GI Bleeds Vikram Sheel Kumar, Harvard Medical School Year III Index Case maroon/bright red: think lower GI bleed Mr. X, 78 years old, presents w/ maroon stool and eighteen hours of
COMPLICATIONS OF CIRRHOSIS COMPLICATIONS OF CIRRHOSIS OBSERVATIONS OF AN AGING HEPATOLOGIST. Philip C. Delich, M.D.
 1 COMPLICATIONS OF CIRRHOSIS OBSERVATIONS OF AN AGING HEPATOLOGIST COMPLICATIONS OF CIRRHOSIS Philip C. Delich, M.D. Faculty Disclosure Dr. Delich has indicated that he does not have any relevant financial
1 COMPLICATIONS OF CIRRHOSIS OBSERVATIONS OF AN AGING HEPATOLOGIST COMPLICATIONS OF CIRRHOSIS Philip C. Delich, M.D. Faculty Disclosure Dr. Delich has indicated that he does not have any relevant financial
RR 0.88 (95% CI: 0.77 1.00) P=0.051 (superiority) 3.75
 ALL-CAUSE MORTALITY RR 0.88 (95% CI: 0.77 1.00) P=0.051 (superiority) Rate per year (%) 5.0 4.0 3.0 2.0 1.0 0 3.64 D150 mg BID 3.75 D110 mg BID RR 0.91 (95% CI: 0.80 1.03) P=0.13 (superiority) 4.13 Warfarin
ALL-CAUSE MORTALITY RR 0.88 (95% CI: 0.77 1.00) P=0.051 (superiority) Rate per year (%) 5.0 4.0 3.0 2.0 1.0 0 3.64 D150 mg BID 3.75 D110 mg BID RR 0.91 (95% CI: 0.80 1.03) P=0.13 (superiority) 4.13 Warfarin
New Anticoagulants: When and Why Should I Use Them? Disclosures
 Winship Cancer Institute of Emory University New Anticoagulants: When and Why Should I Use Them? Christine L. Kempton, MD, MSc Associate Professor of Pediatrics and Hematology and Medical Oncology Hemophilia
Winship Cancer Institute of Emory University New Anticoagulants: When and Why Should I Use Them? Christine L. Kempton, MD, MSc Associate Professor of Pediatrics and Hematology and Medical Oncology Hemophilia
understanding GI bleeding
 understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
New Anticoagulants: What to Use What to Avoid
 New Anticoagulants: What to Use What to Avoid Bruce Davidson, MD, MPH Clinical Professor of Medicine Pulmonary and Critical Care Medicine Division University of Washington School of Medicine Seattle USA
New Anticoagulants: What to Use What to Avoid Bruce Davidson, MD, MPH Clinical Professor of Medicine Pulmonary and Critical Care Medicine Division University of Washington School of Medicine Seattle USA
GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo
 GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo Educational Purpose: The Hepatology Rotation introduces the fellow to the management of outpatients and inpatients
GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo Educational Purpose: The Hepatology Rotation introduces the fellow to the management of outpatients and inpatients
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
9/5/14. Objectives. Atrial Fibrillation (AF)
 Novel Anticoagulation for Prevention of Stroke in Patients with Atrial Fibrillation Objectives 1. Review current evidence on use of warfarin in individuals with atrial fibrillation 2. Compare the three
Novel Anticoagulation for Prevention of Stroke in Patients with Atrial Fibrillation Objectives 1. Review current evidence on use of warfarin in individuals with atrial fibrillation 2. Compare the three
Guidelines for diagnosis and management of acute pulmonary embolism
 Guidelines for diagnosis and management of acute pulmonary embolism By Dr. Ahmed Zaghloul M.D. Anesthesia & Critical Care 2014 Predisposing factors for VTE Predisposing factor Strong predisposing factors
Guidelines for diagnosis and management of acute pulmonary embolism By Dr. Ahmed Zaghloul M.D. Anesthesia & Critical Care 2014 Predisposing factors for VTE Predisposing factor Strong predisposing factors
New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis
 New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis Holster IL, Valkhoff VE, Kuipers EJ, Tjwa ET Departments of Gastroenterology and Hepatology,
New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis Holster IL, Valkhoff VE, Kuipers EJ, Tjwa ET Departments of Gastroenterology and Hepatology,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE
 STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding
 PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
Complications of pediatric endoscopy and colonoscopy. Informed consent. Learning objectives. Complication types. Complications (adults) 10/3/2012
 Complications of pediatric endoscopy and colonoscopy I have no financial relationships with any commercial entity to disclose Petar Mamula, M.D. The Children s Hospital of Philadelphia University of Pennsylvania
Complications of pediatric endoscopy and colonoscopy I have no financial relationships with any commercial entity to disclose Petar Mamula, M.D. The Children s Hospital of Philadelphia University of Pennsylvania
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
OFFICE OF THE STATE CORONER FINDINGS OF INVESTIGATION
 OFFICE OF THE STATE CORONER FINDINGS OF INVESTIGATION CITATION: TITLE OF COURT: JURISDICTION: Non-inquest findings into the death of Mr B Coroner s Court Brisbane DATE: 29 February 2016 FILE NO(s): 2015/1036
OFFICE OF THE STATE CORONER FINDINGS OF INVESTIGATION CITATION: TITLE OF COURT: JURISDICTION: Non-inquest findings into the death of Mr B Coroner s Court Brisbane DATE: 29 February 2016 FILE NO(s): 2015/1036
A. Ketorolac*** B. Naproxen C. Ibuprofen D. Celecoxib
 1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
Post-DDW OAG Course - Therapeutic Endoscopy
 Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto [email protected] Program Name: Post-DDW OAG course CanMEDS
Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto [email protected] Program Name: Post-DDW OAG course CanMEDS
The 50-year Quest to Replace Warfarin: Novel Anticoagulants Define a New Era. CCRN State of the Heart 2012 June 2, 2012
 The 50-year Quest to Replace Warfarin: Novel Anticoagulants Define a New Era CCRN State of the Heart 2012 June 2, 2012 Disclosures I have I have been involved in trials of new anticoagulants and have received
The 50-year Quest to Replace Warfarin: Novel Anticoagulants Define a New Era CCRN State of the Heart 2012 June 2, 2012 Disclosures I have I have been involved in trials of new anticoagulants and have received
PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES.
 PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES. Hossam Bahy, MD (1992 2012), 19 tools have been identified 11 stroke scores 1
PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES. Hossam Bahy, MD (1992 2012), 19 tools have been identified 11 stroke scores 1
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Prescriber Guide. 20mg. 15mg. Simply Protecting More Patients. Simply Protecting More Patients
 Prescriber Guide 20mg Simply Protecting More Patients 15mg Simply Protecting More Patients 1 Dear Doctor, This prescriber guide was produced by Bayer Israel in cooperation with the Ministry of Health as
Prescriber Guide 20mg Simply Protecting More Patients 15mg Simply Protecting More Patients 1 Dear Doctor, This prescriber guide was produced by Bayer Israel in cooperation with the Ministry of Health as
ANESTHESIA FOR PATIENTS WITH CORONARY STENTS FOR NON CARDIAC SURGERY. Dr. Mahesh Vakamudi. Professor and Head
 ANESTHESIA FOR PATIENTS WITH CORONARY STENTS FOR NON CARDIAC SURGERY Dr. Mahesh Vakamudi Professor and Head Department of Anesthesiology, Critical Care and Pain Medicine Sri Ramachandra University INTRODUCTION
ANESTHESIA FOR PATIENTS WITH CORONARY STENTS FOR NON CARDIAC SURGERY Dr. Mahesh Vakamudi Professor and Head Department of Anesthesiology, Critical Care and Pain Medicine Sri Ramachandra University INTRODUCTION
