Optimal injection volume of epinephrine for endoscopic treatment of peptic ulcer bleeding
|
|
|
- Brett Singleton
- 8 years ago
- Views:
Transcription
1 PO Box 2345, Beijing , China World J Gastroenterol 2006 May 21; 12(19): World Journal of Gastroenterology ISSN wjg@wjgnet.com 2006 The WJG Press. All rights reserved. RAPID COMMUNICATION Optimal injection volume of epinephrine for endoscopic treatment of peptic ulcer bleeding Tai-Cherng Liou, Shee-Chan Lin, Horng-Yuan Wang, Wen-Hsiung Chang Tai-Cherng Liou, Shee-Chan Lin, Horng-Yuan Wang, Wen- Hsiung Chang, Division of Gastroenterology, Department of Internal Medicine, Mackay Memorial Hospital, Mackay Medicine, Nursing and Management College, Taipei, Taiwan, China Correspondence to: Dr. Tai-Cherng Liou, Division of Gastroenterology, Department of Internal Medicine, Mackay Memorial Hospital, No. 92, Section 2, Chungshan North Road, Taipei, Taiwan, China. ltc@ms2.mmh.org.tw Telephone: Fax: Received: Accepted: Abstract AIM: To define the optimal injection volume of epinephrine with high efficacy for hemostasis and low complication rate in patients with actively bleeding ulcers. METHODS: This prospective, randomized, comparative trial was conducted in a medical center. A total of 228 patients with actively bleeding ulcers (spurting or oozing) were randomly assigned to three groups with 20, 30 and 40 ml endoscopic injections of an 1: solution of epinephrine. The hemostatic effects and clinical outcomes were compared between the three groups. RESULTS: There were no significant differences in all background variables between the three groups. Initial hemostasis was achieved in 97.4%, 98.7% and 100% of patients respectively in the 20, 30 and 40 ml epinephrine groups. There were no significant differences in the rate of initial hemostasis between the three groups. The rate of peptic ulcer perforation was significantly higher in the 40 ml epinephrine group than in the 20 and 30 ml epinephrine groups (P < 0.05). The rate of recurrent bleeding was significantly higher in the 20 ml epinephrine group (20.3%) than in the 30 (5.3%) and 40 ml (2.8 %) epinephrine groups (P < 0.01). There were no significant differences in the rates of surgical intervention, the amount of transfusion requirements, the days of hospitalization, the deaths from bleeding and 30 d mortality between the three groups. The number of patients who developed epigastric pain due to endoscopic injection, was significantly higher in the 40 ml epinephrine group (51/76) than in the 20 (2/76) and 30 ml (5/76) epinephrine groups (P < 0.001). Significant elevation of systolic blood pressure after endoscopic injection was observed in the 40 ml epinephrine group (P < 0.01). Significant decreasing and normalization of pulse rates after endoscopic injections were observed in the 20 ml and 30 ml epinephrine groups (P < 0.01). CONCLUSION: Injection of 30 ml diluted epinephrine (1:10 000) can effectively prevent recurrent bleeding with a low rate of complications. The optimal injection volume of epinephrine for endoscopic treatment of an actively bleeding ulcer (spurting or oozing) is 30 ml The WJG Press. All rights reserved. Key words: Endoscopic injection; Epinephrine; Volume; Peptic ulcer bleeding Liou TC, Lin SC, Wang HY, Chang WH. Optimal injection volume of epinephrine for endoscopic treatment of peptic ulcer bleeding. World J Gastroenterol 2006; 12(19): INTRODUCTION Endoscopic injection of epinephrine is considered a highly effective and simple hemostatic technique for non-variceal upper gastrointestinal (GI) bleeding [1-3]. Although the rate of initial hemostasis is high, rebleeding occurs in 6% - 36% of patients [4-7]. Rebleeding after initial endoscopic hemostasis remains an important determinant of poor prognosis in patients with hemorrhaging ulcers [8, 9]. The wide variation in rates of recurrent bleeding may result from the different volumes (2-30 ml) of epinephrine injected to achieve hemostasis in various studies [4-7]. Clinical trials in patients with bleeding ulcers disclosed that injection of normal saline solution [10] or distilled water [11] is as effective as absolute alcohol [10] or an epinephrine [11] solution for endoscopic therapy. These findings suggest that tamponade plays a primary role in hemostasis with endoscopic injection therapy, and that injection of larger volumes of epinephrine may be beneficial for preventing recurrent bleeding by prolonging the hemostatic effect of local compression. Lin et al [12] found that injection of a large volume (13-20 ml) of 1:10000 solution of epinephrine can reduce the rate of recurrent bleeding in patients with high-risk peptic ulcers and is superior to an injection of lesser volumes (5-10 ml) of epinephrine (15.4% vs 30.8%). Park et al [13] also reported that injection of ml of an 1:10000 solution of epinephrine is more effective in preventing recurrent bleeding from ulcers in the gastric body than injection of ml of the same solution (0% vs 17.1%). However,
2 Liou TC et al. Optimal volume of epinephrine for endoscopic injection 3109 what is the optimal injection volume of epinephrine for the prevention of recurrent bleeding is not clear. The aim of our study was to define the optimal injection volume of epinephrine with high efficacy for hemostasis and low complication rate in patients with actively bleeding ulcers. MATERIALS AND METHODS Patients This prospective, randomized, comparative trial was conducted in a medical center. Patients with active bleeding ulcers between January 2003 and June 2005 were admitted to our hospital. Emergency endoscopies were performed in the first day of admission, patients were enrolled in this study if the endoscopy revealed an ulcer with active bleeding defined by the Forrest classification [14] as stage Ia (spurting bleeding) or stage Ib (oozing). Patients were excluded if they were under 18 years of age, pregnant, unable or unwilling to give written informed consent, on anticoagulation therapy, or had a bleeding tendency (platelet count < /mm 3, prothrombin time >2.0 by international normalized ratio [INR], and activated partial thromboplastin time > 60 s), bleeding gastric malignancy and multiple potential sources of bleeding. Possible complications of endoscopic treatment were discussed with patients and their relatives, and written informed consent was obtained before entry into the trial. The protocol was approved by the Clinical Research Committee of our hospital. Clinical characteristics, including age, gender, use of non-steroidal anti-inflammatory drugs (NSAID), blood pressure, pulse rate, comorbid diseases, coagulopathy (platelet count 20000/mm /mm 3, prothrombin time by INR), and Hb level were recorded. Shock was defined as systolic pressure less than 100 mmhg and pulse rate greater than 100 beats/min accompanying cold skin, sweating, pallor, and oliguria. Endoscopic characteristics, including type of stigma, ulcer size and location were recorded. One biopsy was obtained from the gastric antrum and one from the gastric body after cessation of bleeding. The presence of helicobacter pylori infection was assessed with a rapid urease test. Methods Patients were randomly assigned to three groups with 20, 30 and 40 ml endoscopic injections of an 1: solution of epinephrine. Randomization was performed by using a computer-generated randomization list and sealed envelopes. A single experienced senior gastroenterologist performed all endoscopic hemostatic treatments. The post-procedure care of the patients was conducted by other physicians. A commercially available endoscope (GIF-XQ240, Olympus Optical Co., Ltd., Tokyo, Japan) and a 4 mm, 23 G injector needle (NM-8L, Olympus) were used. An 1: solution of epinephrine was injected around the bleeding site (2 ml/injection at 2 mm-3 mm from the point of bleeding) until a total volume of 20, 30 and 40 ml respectively in three groups. Initial hemostasis was defined as endoscopically verified cessation of bleeding for at least 5 min. Pain in the epigastric area that developed during endoscopic injection and lasted for more than one hour after the injection was considered to be induced by the epinephrine injection. Patients who complained of epigastric pain due to endoscopic injection were recorded. Throughout the period of endoscopic injection, electrocardiographic monitoring and pulse oximeter monitoring were used to detect arrhythmia and signs of ischemia or hypoxemia. Patients who continued bleeding, despite an injection of the total volume of epinephrine, underwent additional endoscopic treatment with heater probe thermocoagulation, and were then given emergent surgery if they failed to achieve successful hemostasis. After initial endoscopic hemostasis, all patients received acid suppressive therapy with 40 mg omeprazole, intravenously every 12 h for 3 d, then orally (20 mg/d) for 2 mo. If Helicobacter pylori infection was confirmed by the rapid urease test, the patient was treated for 1 wk with a triple drug regimen (omeprazole, amoxicillin and clarithromycin) as soon as possible. Recurrent bleeding was defined as a subsequent ulcer bleeding that occurred after the initial bleeding stopped. Rebleeding was suspected if one or more signs of ongoing bleeding were found, including fresh hematemesis, melena or bloody stools, aspiration of fresh blood via nasogastric tube, unstable vital signs, and a reduction of Hb by more than 20 g/l within 24 h after initial hemostasis. Patients with rebleeding were confirmed by endoscopy and treated with a second therapeutic endoscopy (epinephrine injection plus heater probe thermocoagulation), and then underwent surgery if they failed to achieve successful hemostasis. The end points of this study were (a) endoscopic therapy failure, i.e., a combination of persistent bleeding and recurrent bleeding during follow-up or (b) death of the patient. Statistical analysis Unless otherwise indicated, values were expressed as mean ± SD. The Student t test was used to compare the mean values of continuous variables. The chi-square test with Yates correction for continuity and the Fisher s exact test were used when appropriate to compare the categorical variables. Clinical, laboratory and endoscopic parameters were analysed. All statistical analyses were performed using SPSS statistical package (version 11.0) on a personal computer. A p value less than 0.05 was considered statistically significant. Any frequency of death was considered as an adverse outcome. Therefore, if a death occurred, the cause was determined. If death was due to recurrent bleeding, a decision of whether to stop the study early was made. Clinical outcomes compared between the three groups were initial hemostatic rate, recurrent bleeding rate, perforated peptic ulcer, need for emergency operation, transfusion requirements, bleeding-related deaths, 30-day mortality, and admission duration. RESULTS A total of 284 patients with actively bleeding ulcers (spurting or oozing) were enrolled in the study. Of these, 56 were excluded because of the absence of informed consent, bleeding tendency, gastric malignancy, or multiple potential bleeding sources at endoscopy. There were 228 patients who were included in the study, 76 in each group. Clinical and endoscopic data obtained for patients at study
3 3110 ISSN CN / R World J Gastroenterol May 21, 2006 Volume 12 Number 19 Table 1 Clinical and endoscopic variables of patients at study entry (n = 76, mean±sd) Epinephrine Epinephrine Epinephrine (20 ml) n (%) (30 ml) n (%) (40 ml) n (%) Age (yr) 61.5 ± ± ± 12.5 Gender (M/F) 56/20 53/23 55/21 NSAID ingestion 26 (34.2) 24 (31.6) 27 (35.5) Shock 20 (26.3) 23 (30.3) 21 (27.6) Comorbid illness 43 (56.6) 41 (53.9) 45 (59.2) Hb level (g/dl) 7.2 ± ± ± 2.7 Coagulopathy 12 (15.8) 10 (13.2) 13 (17.1) Positive H pylori 44 (57.9) 43 (56.6) 47 (61.8) Forrest class Ia 18 (23.7) 20 (26.3) 19 (25.0) Ib 58 (76.3) 56 (73.7) 57 (75.0) Ulcer size 2 cm 20 (26.3) 22 (28.9) 23 (30.3) Table 2 Clinical outcomes of endoscopic injection therapy Epinephrine Epinephrine Epinephrine (20 ml) n (%) (30 ml) n (%) (40 ml) n (%) Initial hemostasis 74 (97.4) 75 (98.7) 76 (100) Recurrent bleeding 15/74 (20.3) b 4/75 (5.3) 2/72 (2.8) Perforated peptic ulcer 0 (0) 0 (0) 4 (5.3) a Surgical intervention 4 (5.3) 2 (2.6) 5 (6.6) Transfusion requirement (units) 4.7 ± ± ± 3.6 Total hospital stay (days) 10.8 ± ± ± 3.1 Deaths from bleeding 0 (0) 0 (0) 0 (0) 30-d mortality 3 (3.9) 2 (2.6) 4 (5.3) No. of patients that felt pain' 2 (2.6) 5 (6.6) 51 (67.1) d a P < 0.05 vs the 20 ml and 30 ml epinephrine groups; b P < 0.01 vs the 30 ml and 40 ml epinephrine groups; d P < vs the 20 ml and 30 ml epinephrine groups;' Epigastric pain induced by endoscopic injection of epinephrine. <2 cm 56 (73.7) 54 (71.1) 53 (69.7) Location of ulcer Stomach 41 (53.9) 40 (52.6) 44 (57.9) Duodenum 32 (42.1) 34 (44.7) 30 (39.5) Stoma 3 (3.9) 2 (2.6) 2 (2.6) NSAID: non-steroid anti-inflammatory drug. P > 0.05 for all variables between the three groups. entry are outlined in Table 1. There were no significant differences in age, gender, NSAID ingestion, shock, comorbid diseases, Hb level, coagulopathy, positive H pylori status, bleeding stigma, ulcer size or ulcer location between the three groups. The 3 groups were well matched for factors that could potentially affect outcomes (Table 1). Initial hemostasis was achieved in 74 of 76 patients (97.4%) in the 20 ml epinephrine group, 75 of 76 patients (98.7%) in the 30 ml epinephrine group and 76 of 76 patients (100%) in the 40 ml epinephrine group. There were no significant differences in the rate of initial hemostasis between the three groups (Table 2). Three patients with spurting bleeding from gastric ulcers, two in the 20 ml epinephrine group and one in the 30 ml epinephrine group, failed to achieve initial hemostasis after injection of 20 ml or 30 ml of the 1: solution of epinephrine. Bleeding was controlled in all patients by additional heater probe thermocoagulation. Four patients in the 40 ml epinephrine group developed perforation of peptic ulcers and underwent emergent operations within 24 h after endoscopic injection. The rate of peptic ulcer perforation was significantly higher in the 40 ml epinephrine group than in the 20 ml and 30 ml epinephrine groups (P < 0.05, Table 2). The rate of recurrent bleeding was 20.3% (15/74) in the 20 ml epinephrine group, 5.3% (4/75) in the 30 ml epinephrine group and 2.8 % (2/72) in the 40 ml epinephrine group. The rate of recurrent bleeding was significantly higher in the 20 ml epinephrine group than in the 30 and 40 ml epinephrine groups (P < 0.01, Table 2). Fifteen patients in the 20 ml epinephrine group had recurrent bleeding. Bleeding was controlled in 11 patients by epinephrine injection plus heater probe thermocoagulation, and in 4 by surgical intervention. Four patients in the 30 ml epinephrine group had recurrent bleeding. Bleeding was controlled in 2 patients by epinephrine injection plus heater probe thermocoagulation, and in 2 by surgical intervention. Two patients in the 40 ml epinephrine group had recurrent bleeding. Bleeding was controlled in one patient by epinephrine injection plus heater probe thermocoagulation, and in the other by surgical intervention. The rate of 30-d mortality was 3.9% (3/76), 2.6% (2/76) and 5.3% (4/76) in the 20, 30 and 40 ml epinephrine groups respectively. The causes of death included severe pneumonia with respiration failure in 3 patients, terminal lung cancer in 1 patient, advanced hepatoma with hepatic failure in 3 patients, advanced colon cancer with sepsis in 1 patient and uremia in 1 patient. There was no death due to peptic ulcer bleeding in the three groups. There were no significant differences in the rates of surgical intervention, the amount of transfusion requirements, the days of hospitalization, the deaths due to bleeding and 30-d mortality between the three groups (Table 2). The number of patients who complained of epigastric pain during the procedure of endoscopic injection, was significantly higher in the 40 ml epinephrine group (51/76) than in the 20 ml (2/76) and 30 ml (5/76) epinephrine groups (P < 0.001, Table 2). There was no procedure-related cardiovascular or respiratory complication in three groups. Electrocardiographic monitoring did not record any cardiac arrhythmia, and no abrupt change occurred in oxygen saturation. However, significant elevation of systolic blood pressure after endoscopic injection was observed in the 40 ml epinephrine group (P < 0.01), while there were no significant changes in systolic blood pressure after endoscopic injection in the 20 and 30 ml epinephrine groups (Table 3). Significant decreasing and normalization of pulse rates after endoscopic injections were also observed in the 20 and
4 Liou TC et al. Optimal volume of epinephrine for endoscopic injection 3111 Table 3 Changes in systolic blood pressure and pulse before and after endoscopic injection therapy (n = 76, mean±sd) Epinephrine (20 ml) n (%) Epinephrine (30 ml) n (%) Epinephrine (40 ml) n (%) Pressure (mmhg) Before treatment ± ± ± 30.7 b After treatment ± ± ± 25.8 b Pulse (/min) Before treatment 96.5 ± 14.7 d 98.2 ± 15.3 d 96.7 ± 14.3 After treatment 84.8 ± 12.8 d 86.3 ± 12.5 d ± 15.2 b P < 0.01 (paired t-test) in the 40 ml epinephrine group; d P < 0.01 (paired t-test) in the 20 ml and 30 ml epinephrine groups. 30 ml epinephrine groups (P < 0.01) as compared to the 40 ml epinephrine group (Table 3). DISCUSSION Peptic ulcer bleeding remains a disease with a considerable morbidity and mortality. The mortality rate is high especially for patients with spurting or oozing bleeding [2, 3, 15]. Endoscopic injection of epinephrine, which is the most widely used method, can significantly reduce rates of further bleeding in non-variceal upper GI [1-3]. Although high rates of initial hemostasis have been obtained, rebleeding occurs in 6% to 36% of patients [4-7]. The wide variation in rates of recurrent bleeding may result from the different clinical features and endoscopic findings between enrolled patients and also the different volumes (2-30 ml) of epinephrine injected to achieve hemostasis in various studies [4-7]. Some factors may be associated with the rate of recurrent bleeding in actively bleeding ulcers after endoscopic injection, including age, shock, comorbid illness, ulcer size, ulcer location and stigmata of hemorrhage [2, 9, 16], which were similar between the 3 groups in the present study, suggesting that the outcomes of endoscopic therapy are unlikely influenced by these factors. A number of agents have been used to achieve hemostasis in endoscopic therapy. However, what is the best solution for the prevention of recurrent bleeding remains unclear. Lai et al [11] demonstrated that a local tamponade with distilled water is as effective as epinephrine solution (11.3 ± 4.7 ml) in endoscopic injection therapy. Lin et al [10] have also disclosed similar hemostatic effects of injection with normal saline solution, 3% NaCl solution, 50% glucose water, and pure alcohol. These studies suggested local tamponade is the major effect on sustained hemostasis. Although the mechanisms of hemostasis are different among various agents, clinical studies comparing various agents have demonstrated that no single solution is superior to the others [2, 10, 11]. Laine and Estrada [17] found that local tamponade with normal saline (30 ± 3 ml) solution is less effective than thermal therapy. However, Chung et al [18] found that epinephrine injection (1.5 to 19.5 ml) and thermocoagulation have comparable rebleeding rates, indicating that epinephrine injection is technically easier to perform and has a higher initial hemostatic rate. Although the most important mechanism underlying hemostasis in response to epinephrine solution is local tamponade, which is similar to normal saline solution, epinephrine solution offers additional hemostatic effects, including vasoconstriction and platelet aggregation [19]. In a patient with massive active bleeding, it is often difficult to achieve hemostasis with the application of contact devices or laser emergently when visualization of the bleeding site is unsatisfactory. In addition, these methods may not be available in rural hospitals. In our study, the initial hemostatic rate in the 20 ml epinephrine group (97.4%) was as high as that in the 30 ml (98.7%) and 40 ml (100%) epinephrine groups, suggesting that epinephrine solution can be used as a first-line injection solution and hemostatic method for the initial arrest of active bleeding. Because epinephrine produces vessel compression, vasoconstriction, and platelet aggregation, but not induce vessel thrombosis, the addition of sclerosing agents such as ethanol, ethalonamie or polidocanol would be advantageous in theory. However, clinical trials have not definitively demonstrated a benefit for this combination therapy [6, 20-22]. Likewise, the addition of thrombin or fibrin sealant also dose not reduce the risk of rebleeding [23, 24]. Lin et al [12] found that injection of a large volume (13-20 ml) of epinephrine can reduce the rate of recurrent bleeding in patients with high-risk peptic ulcer and is superior to injection of lesser volumes (5-10 ml) of epinephrine (15.4% vs 30.8%). Park et al [13] also reported that injection of ml of an 1: solution of epinephrine is more effective in preventing recurrent bleeding from ulcers in the gastric body than an injection of ml of the same solution (0% vs 17.1%). These findings suggest that a continuous injection of larger volumes of epinephrine even after the bleeding stopped is beneficial for preventing recurrent bleeding by prolonging the hemostatic effect of local tamponade, vasoconstriction, and platelet aggregation. However, what is the optimal volume of epinephrine that can achieve permanent hemostasis still remains unknown. In our study, the rate of recurrent bleeding was significantly higher in the 20 ml epinephrine group than in the 30 ml and 40 ml epinephrine groups (P < 0.01), while there was no significant difference in the rate of recurrent bleeding between these two groups. The studies of Lin et al [12] and Park et al [13] enrolled peptic ulcers with spurting, oozing or non-bleeding visible vessels, and found that only 48.7% (38/78) and 52.8% (19/36) of ulcers are active bleeders (spurting or oozing) in the larger-volume injection group respectively. Because our study only enrolled patients with active bleeding (spurting or oozing), the rates of recurrent bleeding in the 30 and 40 ml epinephrine groups were higher than those reported by Park et al [13]. However, with a larger injection volume, the rebleeding rate in our study was lower than that reported by Lin et al [12] Our study disclosed that an injection of 30 ml epinephrine was an optimal volume for sustained hemostasis and equally beneficial for preventing recurrent bleeding as a 40 ml epinephrine injection. Sung et al [25] found that immediately after the endoscopic injection of a small volume (3-11 ml) of 1: epinephrine solution, the plasma epinephrine level is increased by 4-5 times above the basal level. In addition, hypertensive emergency and ventricular tachycardia after epinephrine injection have been reported [26]. In our study,
5 3112 ISSN CN / R World J Gastroenterol May 21, 2006 Volume 12 Number 19 significant elevation of systolic blood pressure after endoscopic injection was observed in the 40 ml epinephrine group (P < 0.01), while there were no significant changes in systolic blood pressure after endoscopic injection in the 20 and 30 ml epinephrine groups. Significant decreasing and normalization of pulse rates after endoscopic injections were also observed in the 20 and 30 ml epinephrine groups (P < 0.01) as compared to the 40 ml epinephrine group. Therefore, the potential risk of inducing a hypertensive crisis and arrhythmia in patients with underlying cardiovascular diseases by using 40 ml of epinephrine as a hemostatic solution should not be overlooked. Although it has been confirmed that endoscopic injection of epinephrine is safe [6, 20, 23], the injection volume of epinephrine should not be unlimited, because the systemic absorption of epinephrine does occur during endoscopic injection. For large-volume epinephrine injection, electrocardiographic and pulse oximeter monitoring should be used to detect arrhythmias and signs of ischemia or hypoxemia. Our study demonstrated that injection of 30 ml epinephrine was safer than injection of 40 ml epinephrine concerning the potential risk of inducing a cardiovascular event. The epigastric pain induced by large-volume epinephrine injection is rarely reported in literature. In our study, the number of patients who developed epigastric pain due to endoscopic injection, was significantly higher in the 40 ml epinephrine group (51/76) than in the 20 (2/76) and 30 ml (5/76) epinephrine groups (P < 0.001). The epigastric pain induced by large-volume epinephrine injection may be due to tissue ischemia as well as swelling of the ulcer. In addition, injection with a large volume [4, 22, 27] of epinephrine may result in severe tissue necrosis or GI perforation [21, 24, 28]. Perforation of duodenal ulcer in a patient injected a large-volume (35 ml) epinephrine has been reported by Park et al [13]. In our study, the rate of peptic ulcer perforation was significantly higher in the 40 ml epinephrine group than in the 20 and 30 ml epinephrine groups (P < 0.05). Among the four patients who developed perforation of peptic ulcers, three had deep duodenal ulcers (two with spurting bleeding and one with oozing), the other one had spurting bleeding from a deep and big ulcer (4 cm) in the antrum of the stomach. The size of all the perforated ulcers is greater than 2 cm before endoscopic injection. The cause of perforation may be due to severe tissue necrosis and prolonged inflation in the limited space of the duodenal bulb during the endoscopic procedure. Our study revealed that injection with 30 ml epinephrine was safer than 40 ml epinephrine concerning the potential risk of inducing severe tissue necrosis or peptic ulcer perforation. In conclusion, diluted epinephrine (1:10000) solution is good as a first-line injection solution for arrest of active bleeding with a high initial hemostatic rate. Injection of 30 ml epinephrine is optimal for sustained hemostasis with a low rebleeding rate. A 30 ml epinephrine injection is safer than a 40 ml epinephrine injection concerning the potential risk of inducing cardiovascular event and severe tissue necrosis or peptic ulcer perforation. Injection of 30 ml diluted epinephrine (1:10000) can effectively prevent recurrent bleeding with a low rate of complications. The optimal injection volume of epinephrine for endoscopic treatment of an actively bleeding ulcer (spurting or oozing) is 30 ml. REFERENCES 1 Ogra R, Lane M, Wong P, Fraser A. Endoscopic injection therapy for non-variceal upper gastrointestinal bleeding at Auckland Hospital. N Z Med J 2002; 115: U255 2 Barkun A, Bardou M, Marshall JK. Consensus recommendations for managing patients with nonvariceal upper gastrointestinal bleeding. Ann Intern Med 2003; 139: Rollhauser C, Fleischer DE. Nonvariceal upper gastrointestinal bleeding. Endoscopy 2004; 36: Sollano JD, Ang VN, Moreno JA. Endoscopic hemostasis of bleeding peptic ulcers: 1:10000 adrenalin injection vs 1:10000 adrenalin +1% aethoxysclerol injection vs. heater probe. Gastroenterol Jpn 1991; 26 Suppl 3: Loizou LA, Bown SG. Endoscopic treatment for bleeding peptic ulcers: randomised comparison of adrenaline injection and adrenaline injection + Nd:YAG laser photocoagulation. Gut 1991; 32: Chung SC, Leong HT, Chan AC, Lau JY, Yung MY, Leung JW, Li AK. Epinephrine or epinephrine plus alcohol for injection of bleeding ulcers: a prospective randomized trial. Gastrointest Endosc 1996; 43: Lin HJ, Tseng GY, Perng CL, Lee FY, Chang FY, Lee SD. Comparison of adrenaline injection and bipolar electrocoagulation for the arrest of peptic ulcer bleeding. Gut 1999; 44: Rockall TA, Logan RF, Devlin HB, Northfield TC. Risk assessment after acute upper gastrointestinal haemorrhage. Gut 1996; 38: Wong SK, Yu LM, Lau JY, Lam YH, Chan AC, Ng EK, Sung JJ, Chung SC. Prediction of therapeutic failure after adrenaline injection plus heater probe treatment in patients with bleeding peptic ulcer. Gut 2002; 50: Lin HJ, Perng CL, Lee FY, Chan CY, Huang ZC, Lee SD, Lee CH. Endoscopic injection for the arrest of peptic ulcer hemorrhage: final results of a prospective, randomized comparative trial. Gastrointest Endosc 1993; 39: Lai KH, Peng SN, Guo WS, Lee FY, Chang FY, Malik U, Wang JY, Lo GH, Cheng JS, Lee SD. Endoscopic injection for the treatment of bleeding ulcers: local tamponade or drug effect? Endoscopy 1994; 26: Lin HJ, Hsieh YH, Tseng GY, Perng CL, Chang FY, Lee SD. A prospective, randomized trial of large- versus small-volume endoscopic injection of epinephrine for peptic ulcer bleeding. Gastrointest Endosc 2002; 55: Park CH, Lee SJ, Park JH, Park JH, Lee WS, Joo YE, Kim HS, Choi SK, Rew JS, Kim SJ. Optimal injection volume of epinephrine for endoscopic prevention of recurrent peptic ulcer bleeding. Gastrointest Endosc 2004; 60: Forrest JA, Finlayson ND, Shearman DJ. Endoscopy in gastrointestinal bleeding. Lancet 1974; 2: van Leerdam ME, Vreeburg EM, Rauws EA, Geraedts AA, Tijssen JG, Reitsma JB, Tytgat GN. Acute upper GI bleeding: did anything change? Time trend analysis of incidence and outcome of acute upper GI bleeding between 1993/1994 and Am J Gastroenterol 2003; 98: Guglielmi A, Ruzzenente A, Sandri M, Kind R, Lombardo F, Rodella L, Catalano F, de Manzoni G, Cordiano C. Risk assessment and prediction of rebleeding in bleeding gastroduodenal ulcer. Endoscopy 2002; 34: Laine L, Estrada R. Randomized trial of normal saline solution injection versus bipolar electrocoagulation for treatment of patients with high-risk bleeding ulcers: is local tamponade enough? Gastrointest Endosc 2002; 55: Chung SC, Leung JW, Sung JY, Lo KK, Li AK. Injection or heat probe for bleeding ulcer. Gastroenterology 1991; 100: O Brien JR. Some effects of adrenaline and anti-adrenaline compounds on platelets in vitro and in vivo. Nature 1963; 200: Choudari CP, Palmer KR. Endoscopic injection therapy for
6 Liou TC et al. Optimal volume of epinephrine for endoscopic injection 3113 bleeding peptic ulcer; a comparison of adrenaline alone with adrenaline plus ethanolamine oleate. Gut 1994; 35: Villanueva C, Balanzo J, Espinos JC, Fabrega E, Sainz S, Gonzalez D, Vilardell F. Endoscopic injection therapy of bleeding ulcer: a prospective and randomized comparison of adrenaline alone or with polidocanol. J Clin Gastroenterol 1993; 17: Chung SC, Leung JW, Leong HT, Lo KK, Li AK. Adding a sclerosant to endoscopic epinephrine injection in actively bleeding ulcers: a randomized trial. Gastrointest Endosc 1993; 39: Kubba AK, Murphy W, Palmer KR. Endoscopic injection for bleeding peptic ulcer: a comparison of adrenaline alone with adrenaline plus human thrombin. Gastroenterology 1996; 111: Pescatore P, Jornod P, Borovicka J, Pantoflickova D, Suter W, Meyenberger C, Blum AL, Dorta G. Epinephrine versus epinephrine plus fibrin glue injection in peptic ulcer bleeding: a prospective randomized trial. Gastrointest Endosc 2002; 55: Sung JY, Chung SC, Low JM, Cocks R, Ip SM, Tan P, Leung JW, Li AK, Oh TE. Systemic absorption of epinephrine after endoscopic submucosal injection in patients with bleeding peptic ulcers. Gastrointest Endosc 1993; 39: Stevens PD, Lebwohl O. Hypertensive emergency and ventricular tachycardia after endoscopic epinephrine injection of a Mallory-Weiss tear. Gastrointest Endosc 1994; 40: Loperfido S, Patelli G, La Torre L. Extensive necrosis of gastric mucosa following injection therapy of bleeding peptic ulcer. Endoscopy 1990; 22: Bedford RA, van Stolk R, Sivak MV Jr, Chung RS, Van Dam J. Gastric perforation after endoscopic treatment of a Dieulafoy s lesion. Am J Gastroenterol 1992; 87: S- Editor Wang J L- Editor Wang XL E- Editor Zhang Y
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD
 Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
American Journal of Gastroenterology ISSN 0002-9270
 American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial
 Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
Rob Enns University of British Columbia, Vancouver. Grigorios Leontiadis McMaster University, Hamilton
 Rob Enns University of British Columbia, Vancouver Grigorios Leontiadis McMaster University, Hamilton Accreditation This event has been approved as an accredited (Section1) group learning activity as defined
Rob Enns University of British Columbia, Vancouver Grigorios Leontiadis McMaster University, Hamilton Accreditation This event has been approved as an accredited (Section1) group learning activity as defined
Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points
 372 Gut 2001;49:372 379 Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points G M Hawkey, A T Cole, A S McIntyre, R G Long, C J Hawkey Division of Gastroenterology,
372 Gut 2001;49:372 379 Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points G M Hawkey, A T Cole, A S McIntyre, R G Long, C J Hawkey Division of Gastroenterology,
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding
 Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
GI Bleeding. Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics
 GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Management by the intensivist of gastrointestinal bleeding in adults and children
 Osman et al. Annals of Intensive Care 2012, 2:46 REVIEW Open Access Management by the intensivist of gastrointestinal bleeding in adults and children David Osman 1*, Michel Djibré 2, Daniel Da Silva 3,
Osman et al. Annals of Intensive Care 2012, 2:46 REVIEW Open Access Management by the intensivist of gastrointestinal bleeding in adults and children David Osman 1*, Michel Djibré 2, Daniel Da Silva 3,
Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage
 Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage Brian P. Bosworth A. Outcomes in Lower Gastrointestinal Bleeding Acute
Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage Brian P. Bosworth A. Outcomes in Lower Gastrointestinal Bleeding Acute
Inpatient Anticoagulation Safety. To provide safe and effective anticoagulation therapy through a collaborative approach.
 Inpatient Anticoagulation Safety Purpose: Policy: To provide safe and effective anticoagulation therapy through a collaborative approach. Upon the written order of a physician, Heparin, Low Molecular Weight
Inpatient Anticoagulation Safety Purpose: Policy: To provide safe and effective anticoagulation therapy through a collaborative approach. Upon the written order of a physician, Heparin, Low Molecular Weight
Treating delayed endoscopic sphincterotomy-induced bleeding: Epinephrine injection with or without thermotherapy
 Online Submissions: wjg.wjgnet.com World J Gastroenterol 2009 October 14; 15(38): 4823-4828 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.15.4823 2009 The WJG Press and
Online Submissions: wjg.wjgnet.com World J Gastroenterol 2009 October 14; 15(38): 4823-4828 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.15.4823 2009 The WJG Press and
SIGN. Management of acute upper and lower gastrointestinal bleeding. September 2008. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
Management and Prevention of Upper GI Bleeding
 Management and Prevention of Upper GI Bleeding By Jiwon Kim, Pharm.D., BCPS, FCSHP Reviewed by Clarence Chant, Pharm.D., FCSHP, FCCP, BCPS; and Steven E. Pass, Pharm.D., FCCP, FCCM, BCPS Learning Objectives
Management and Prevention of Upper GI Bleeding By Jiwon Kim, Pharm.D., BCPS, FCSHP Reviewed by Clarence Chant, Pharm.D., FCSHP, FCCP, BCPS; and Steven E. Pass, Pharm.D., FCCP, FCCM, BCPS Learning Objectives
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
ORIGINAL ARTICLE: Clinical Endoscopy
 ORIGINAL ARTICLE: Clinical Endoscopy Immediate unprepared hydroflush colonoscopy for severe lower GI bleeding: a feasibility study Aparna Repaka, MD, Matthew R. Atkinson, MD, Ashley L. Faulx, MD, Gerard
ORIGINAL ARTICLE: Clinical Endoscopy Immediate unprepared hydroflush colonoscopy for severe lower GI bleeding: a feasibility study Aparna Repaka, MD, Matthew R. Atkinson, MD, Ashley L. Faulx, MD, Gerard
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Summary and general discussion
 Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
British Society of Gastroenterology. St. Elsewhere's NHS Foundation Trust. National Comparative Audit of Blood Transfusion
 British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood December 2007 St. Elsewhere's NHS Foundation Trust National Comparative Audit of Blood
British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood December 2007 St. Elsewhere's NHS Foundation Trust National Comparative Audit of Blood
New Anticoagulants and GI bleeding
 New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
Articles Presented. Journal Presentation. Dr Albert Lo. Dr Albert Lo
 * This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
* This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
Cilostazol versus Clopidogrel after Coronary Stenting
 Cilostazol versus Clopidogrel after Coronary Stenting Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine Seoul, Korea AMC, 2004 Background
Cilostazol versus Clopidogrel after Coronary Stenting Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine Seoul, Korea AMC, 2004 Background
The degree of liver inflammation or damage (grade) Presence and extent of fatty liver or other metabolic liver diseases
 ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
National Digestive Diseases Information Clearinghouse
 Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a
 AMP particles - absorbable polysaccharide hemostat in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a prospective, randomized
AMP particles - absorbable polysaccharide hemostat in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a prospective, randomized
Presence and extent of fatty liver or other metabolic liver diseases
 UC San Diego Health System Patient Information Sheet: Liver Biopsy What is a Liver Biopsy? A liver biopsy is a procedure where a qualified doctor (typically a hepatologist, radiologist or gastroenterologist)
UC San Diego Health System Patient Information Sheet: Liver Biopsy What is a Liver Biopsy? A liver biopsy is a procedure where a qualified doctor (typically a hepatologist, radiologist or gastroenterologist)
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
A. Ketorolac*** B. Naproxen C. Ibuprofen D. Celecoxib
 1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
Rebleeding and survival after acute lower gastrointestinal bleeding
 The American Journal of Surgery 188 (2004) 485 490 Scientific paper Rebleeding and survival after acute lower gastrointestinal bleeding Thomas Anthony, M.D.*, Pradeep Penta, B.S., Robert D. Todd, B.S.,
The American Journal of Surgery 188 (2004) 485 490 Scientific paper Rebleeding and survival after acute lower gastrointestinal bleeding Thomas Anthony, M.D.*, Pradeep Penta, B.S., Robert D. Todd, B.S.,
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
Dabigatran (Pradaxa) Guidelines
 Dabigatran (Pradaxa) Guidelines Dabigatran is a new anticoagulant for reducing the risk of stroke in patients with atrial fibrillation. Dabigatran is a direct thrombin inhibitor, similar to warfarin, without
Dabigatran (Pradaxa) Guidelines Dabigatran is a new anticoagulant for reducing the risk of stroke in patients with atrial fibrillation. Dabigatran is a direct thrombin inhibitor, similar to warfarin, without
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Appendix G - Identification and Selection of Studies
 FINAL Emergency framework for rationing of blood for massively bleeding patients during a red phase of a Appendix G - Identification and Selection of Studies Inclusion/Exclusion Criteria We included studies
FINAL Emergency framework for rationing of blood for massively bleeding patients during a red phase of a Appendix G - Identification and Selection of Studies Inclusion/Exclusion Criteria We included studies
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Evolution of Barrett s esophagus
 Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Gruppo di lavoro: Malattie Tromboemboliche
 Gruppo di lavoro: Malattie Tromboemboliche 2381 Soluble Recombinant Thrombomodulin Ameliorates Hematological Malignancy-Induced Disseminated Intravascular Coagulation More Promptly Than Conventional Anticoagulant
Gruppo di lavoro: Malattie Tromboemboliche 2381 Soluble Recombinant Thrombomodulin Ameliorates Hematological Malignancy-Induced Disseminated Intravascular Coagulation More Promptly Than Conventional Anticoagulant
Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting
 Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting DATE Educating for Quality Improvement & Patient Safety 1 The Team Division CS&E Participants
Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting DATE Educating for Quality Improvement & Patient Safety 1 The Team Division CS&E Participants
DVT/PE Management with Rivaroxaban (Xarelto)
 DVT/PE Management with Rivaroxaban (Xarelto) Rivaroxaban is FDA approved for the acute treatment of DVT and PE and reduction in risk of recurrence of DVT and PE. FDA approved indications: Non valvular
DVT/PE Management with Rivaroxaban (Xarelto) Rivaroxaban is FDA approved for the acute treatment of DVT and PE and reduction in risk of recurrence of DVT and PE. FDA approved indications: Non valvular
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
ESD for colorectal lesions I am in favour. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
Peptic ulcers are a common cause of nonvariceal upper
 original article ractices in peptic ulcer bleeding controversies among university- versus nonuniversity-affiliated gastroenterologists Justin Cheung MD FRCC 1, Grant Sawisky MD 2, Robert Enns MD FRCC 3,
original article ractices in peptic ulcer bleeding controversies among university- versus nonuniversity-affiliated gastroenterologists Justin Cheung MD FRCC 1, Grant Sawisky MD 2, Robert Enns MD FRCC 3,
CLINICAL PRACTICE GUIDELINES
 CLINICAL PRACTICE GUIDELINES April 2003 MOH/P/PAK/ (GU) MANAGEMENT OF NON-VARICEAL UPPER GASTROINTESTINAL BLEEDING MINISTRY OF HEALTH MALAYSIAN SOCIETY ACADEMY OF MEDICINE, MALAYSIA OF MALAYS IA GASTROENTEROLOGY
CLINICAL PRACTICE GUIDELINES April 2003 MOH/P/PAK/ (GU) MANAGEMENT OF NON-VARICEAL UPPER GASTROINTESTINAL BLEEDING MINISTRY OF HEALTH MALAYSIAN SOCIETY ACADEMY OF MEDICINE, MALAYSIA OF MALAYS IA GASTROENTEROLOGY
STROKE PREVENTION IN ATRIAL FIBRILLATION. TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: ABBREVIATIONS: BACKGROUND:
 STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
Endoscopic Management of Strictures and Leaks. Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center
 Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
Medical Direction and Practices Board WHITE PAPER
 Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
understanding GI bleeding
 understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
The author has no disclosures
 Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 Mary.bradbury@inova.org This presentation will discuss unlabeled and investigational use of products The author
Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 Mary.bradbury@inova.org This presentation will discuss unlabeled and investigational use of products The author
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Comparison of Heart Rate and Blood Pressure administration of anesthesia agent with and without
 ISSN: 2347-3215 Volume 2 Number 9 (September-2014) pp. 153-158 www.ijcrar.com Comparison of Heart Rate and Blood Pressure administration of anesthesia agent with and without Mohammad Ali Ghavimi 1*, Javad
ISSN: 2347-3215 Volume 2 Number 9 (September-2014) pp. 153-158 www.ijcrar.com Comparison of Heart Rate and Blood Pressure administration of anesthesia agent with and without Mohammad Ali Ghavimi 1*, Javad
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
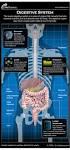 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS
 NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS Date of First Issue 01/12/ 2012 Approved 15/11/2012 Current Issue Date 29/10/2014 Review Date 29/10/2016
NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS Date of First Issue 01/12/ 2012 Approved 15/11/2012 Current Issue Date 29/10/2014 Review Date 29/10/2016
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
POEM Procedure for. Esophageal Achalasia
 POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
SBRT (Elekta), 45 Gy in fractions of 3 Gy 3x/week for 5 weeks (N=22) vs.
 Uitgangsvraag 6: Wat is de plaats van stereotactische radiotherapiebehandeling (SBRT) bij HCC patiënten? Primaire studies I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary
Uitgangsvraag 6: Wat is de plaats van stereotactische radiotherapiebehandeling (SBRT) bij HCC patiënten? Primaire studies I Study ID II Method III Patient characteristics IV Intervention(s) V Results primary
(ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding?
 (ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding? Dennis M. Jensen 1, Robert Stuart 2, Henrik Ahlbom 3, Stefan Eklund 3, Alan Barkun
(ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding? Dennis M. Jensen 1, Robert Stuart 2, Henrik Ahlbom 3, Stefan Eklund 3, Alan Barkun
Diagnosis and treatment of patients with gastrointestinal bleeding
 Current Anaesthesia & Critical Care (2004) 15, 123 132 ARTICLE IN PRESS www.elsevier.com/locate/cacc MEDICAL Diagnosis and treatment of patients with gastrointestinal bleeding C. Meaden, A.J. Makin* UK
Current Anaesthesia & Critical Care (2004) 15, 123 132 ARTICLE IN PRESS www.elsevier.com/locate/cacc MEDICAL Diagnosis and treatment of patients with gastrointestinal bleeding C. Meaden, A.J. Makin* UK
HemoClip: Guidelines & Atlas
 HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
Duration of Dual Antiplatelet Therapy After Coronary Stenting
 Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
ABOUT XARELTO CLINICAL STUDIES
 ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
How To Screen For Alcohol Dependence
 Commonwealth of Massachusetts Board of Registration in Medicine Quality and Patient Safety Division Advisory Alcohol Screening and Management Protocols July 2013 Background The Quality and Patient Safety
Commonwealth of Massachusetts Board of Registration in Medicine Quality and Patient Safety Division Advisory Alcohol Screening and Management Protocols July 2013 Background The Quality and Patient Safety
Learning Luncheon 7: Endoscopic Mucosal Resection: When, Where and How?
 Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
Undergoing an Oesophageal Endoscopic Resection (ER)
 Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
Contact Information If you have an enquiry about your appointment time/date please contact the Booking Office on 0300 422 6350. For medication enquiries please call 0300 422 8232, this is an answer machine
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Post-DDW OAG Course - Therapeutic Endoscopy
 Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto moskoj@smh.ca Program Name: Post-DDW OAG course CanMEDS
Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto moskoj@smh.ca Program Name: Post-DDW OAG course CanMEDS
Critical Bleeding Reversal Protocol
 Critical Bleeding Reversal Protocol Coagulopathy, either drug related or multifactorial, is a major contributing factor to bleeding related mortality in a variety of clinical settings. Standard therapy
Critical Bleeding Reversal Protocol Coagulopathy, either drug related or multifactorial, is a major contributing factor to bleeding related mortality in a variety of clinical settings. Standard therapy
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
A PATIENT S GUIDE TO DEEP VEIN THROMBOSIS TREATMENT
 A PATIENT S GUIDE TO DEEP VEIN THROMBOSIS TREATMENT This medicine is subject to additional monitoring. This will allow quick identification of new safety information. If you get any side effects, talk
A PATIENT S GUIDE TO DEEP VEIN THROMBOSIS TREATMENT This medicine is subject to additional monitoring. This will allow quick identification of new safety information. If you get any side effects, talk
Gloucestershire Hospitals
 TRUST GUIDELINE In the case of hard copies of this policy the content can only be assured to be accurate on the date of issue marked on the document. The Policy framework requires that the policy is fully
TRUST GUIDELINE In the case of hard copies of this policy the content can only be assured to be accurate on the date of issue marked on the document. The Policy framework requires that the policy is fully
MEDICAL POLICY No. 91104-R7 DETOXIFICATION I. POLICY/CRITERIA
 DETOXIFICATION MEDICAL POLICY Effective Date: January 7, 2013 Review Dates: 1/93, 2/97, 4/99, 2/01, 12/01, 2/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14 Date
DETOXIFICATION MEDICAL POLICY Effective Date: January 7, 2013 Review Dates: 1/93, 2/97, 4/99, 2/01, 12/01, 2/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14 Date
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA
 KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D.
 Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Anticoagulation at the end of life. Rhona Maclean Rhona.maclean@sth.nhs.uk
 Anticoagulation at the end of life Rhona Maclean Rhona.maclean@sth.nhs.uk Content Anticoagulant Therapies Indications for anticoagulation Venous thromboembolism (VTE) Atrial Fibrillation Mechnical Heart
Anticoagulation at the end of life Rhona Maclean Rhona.maclean@sth.nhs.uk Content Anticoagulant Therapies Indications for anticoagulation Venous thromboembolism (VTE) Atrial Fibrillation Mechnical Heart
The largest clinical study of Bayer's Xarelto (rivaroxaban) Wednesday, 14 November 2012 07:38
 Bayer HealthCare has announced the initiation of the COMPASS study, the largest clinical study of its oral anticoagulant Xarelto (rivaroxaban) to date, investigating the prevention of major adverse cardiac
Bayer HealthCare has announced the initiation of the COMPASS study, the largest clinical study of its oral anticoagulant Xarelto (rivaroxaban) to date, investigating the prevention of major adverse cardiac
What are peptic ulcers?
 Information about Peptic ulcers www.corecharity.org.uk What are the symptoms? What are the causes? What are peptic ulcers? When should I consult a doctor? What will the doctor do? How should I treat peptic
Information about Peptic ulcers www.corecharity.org.uk What are the symptoms? What are the causes? What are peptic ulcers? When should I consult a doctor? What will the doctor do? How should I treat peptic
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Gastrointestinal bleeding
 Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
FOR THE PREVENTION OF ATRIAL FIBRILLATION RELATED STROKE
 www.bpac.org.nz keyword: warfarinaspirin FOR THE PREVENTION OF ATRIAL FIBRILLATION RELATED STROKE Key Concepts In atrial fibrillation (AF) warfarin is more effective than aspirin for stroke prevention.
www.bpac.org.nz keyword: warfarinaspirin FOR THE PREVENTION OF ATRIAL FIBRILLATION RELATED STROKE Key Concepts In atrial fibrillation (AF) warfarin is more effective than aspirin for stroke prevention.
Enoxaparin for long term anticoagulation in patients unsuitable for oral anticoagulants
 Enoxaparin for long term anticoagulation in patients unsuitable for oral anticoagulants Traffic light classification- Amber 2 Information sheet for Primary Care Prescribers Relevant Licensed Indications
Enoxaparin for long term anticoagulation in patients unsuitable for oral anticoagulants Traffic light classification- Amber 2 Information sheet for Primary Care Prescribers Relevant Licensed Indications
The administration of epinephrine for severe anaphylactic type allergic reactions. Training for Québec first aiders 2008
 The administration of epinephrine for severe anaphylactic type allergic reactions Training for Québec first aiders 2008 2 Acknowledgements AQAA St-John Ambulance Canadian Red Cross CSST Québec Heart and
The administration of epinephrine for severe anaphylactic type allergic reactions Training for Québec first aiders 2008 2 Acknowledgements AQAA St-John Ambulance Canadian Red Cross CSST Québec Heart and
PHENYLEPHRINE HYDROCHLORIDE INJECTION USP
 PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
UGI Tract Hemorrhage. GI Tract Emergencies. UGI Hemorrhage. David D. Markowitz, MD. UGI tract hemorrhage Comorbid disease
 UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
Format for ANSWERING REVIEWERS
 Format for ANSWERING REVIEWERS July 15, 2015 Dear Editor, Please find enclosed the edited manuscript in Word format (file name: 19935-revised manuscript). Title: Management and associated factors of delayed
Format for ANSWERING REVIEWERS July 15, 2015 Dear Editor, Please find enclosed the edited manuscript in Word format (file name: 19935-revised manuscript). Title: Management and associated factors of delayed
OFFICE OF THE STATE CORONER FINDINGS OF INVESTIGATION
 OFFICE OF THE STATE CORONER FINDINGS OF INVESTIGATION CITATION: TITLE OF COURT: JURISDICTION: Non-inquest findings into the death of Mr B Coroner s Court Brisbane DATE: 29 February 2016 FILE NO(s): 2015/1036
OFFICE OF THE STATE CORONER FINDINGS OF INVESTIGATION CITATION: TITLE OF COURT: JURISDICTION: Non-inquest findings into the death of Mr B Coroner s Court Brisbane DATE: 29 February 2016 FILE NO(s): 2015/1036
NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol)
 NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol) Date of First Issue 10/05/2010 Approved 16/06/2010 Current Issue Date 18/11/2015
NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol) Date of First Issue 10/05/2010 Approved 16/06/2010 Current Issue Date 18/11/2015
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Endoscopic Management of Acute Lower Gastrointestinal Bleeding
 American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2008.02075.x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management
American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2008.02075.x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management
Complications of pediatric endoscopy and colonoscopy. Informed consent. Learning objectives. Complication types. Complications (adults) 10/3/2012
 Complications of pediatric endoscopy and colonoscopy I have no financial relationships with any commercial entity to disclose Petar Mamula, M.D. The Children s Hospital of Philadelphia University of Pennsylvania
Complications of pediatric endoscopy and colonoscopy I have no financial relationships with any commercial entity to disclose Petar Mamula, M.D. The Children s Hospital of Philadelphia University of Pennsylvania
Getting smart about dyspnea and life saving drug therapy in ACS patients. Kobi George Kaplan Medical Center Rehovot
 Getting smart about dyspnea and life saving drug therapy in ACS patients Kobi George Kaplan Medical Center Rehovot 78 year old female Case description Presented with resting chest pain and dyspnea Co morbidities:
Getting smart about dyspnea and life saving drug therapy in ACS patients Kobi George Kaplan Medical Center Rehovot 78 year old female Case description Presented with resting chest pain and dyspnea Co morbidities:
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl
 NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl Mikele Wissing, RN June 2014 Introduction until recently, was the unrivaled medication for treatment
NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl Mikele Wissing, RN June 2014 Introduction until recently, was the unrivaled medication for treatment
Peptic Upper Gastrointestinal Bleeding: Diagnosis and Treatment. A Monocentric Experience on a 5 Years Period
 ORIGINAL ARTICLES Peptic Upper Gastrointestinal Bleeding: Diagnosis and Treatment. A Monocentric Experience on a 5 Years Period I. SPOREA 1, DANIELA LAZĂR 1, ALINA POPESCU 1, ROXANA ŞIRLI 1, A. GOLDIŞ
ORIGINAL ARTICLES Peptic Upper Gastrointestinal Bleeding: Diagnosis and Treatment. A Monocentric Experience on a 5 Years Period I. SPOREA 1, DANIELA LAZĂR 1, ALINA POPESCU 1, ROXANA ŞIRLI 1, A. GOLDIŞ
Aktuelle Literatur aus der Notfallmedizin
 05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
Thrombosis and Hemostasis
 Thrombosis and Hemostasis Wendy Lim, MD, MSc, FRCPC Associate Professor, Department of Medicine McMaster University, Hamilton, ON Overview To review the important developments in venous thromboembolism
Thrombosis and Hemostasis Wendy Lim, MD, MSc, FRCPC Associate Professor, Department of Medicine McMaster University, Hamilton, ON Overview To review the important developments in venous thromboembolism
Disclosures. Objective (NRHS) Self Assessment #2
 Development and Implementation of a Protocol for Reversing the Effects of Anticoagulants for Use in a Community Hospital Samantha Sepulveda, Pharm.D. PGY1 Pharmacy Resident Norman Regional Health System
Development and Implementation of a Protocol for Reversing the Effects of Anticoagulants for Use in a Community Hospital Samantha Sepulveda, Pharm.D. PGY1 Pharmacy Resident Norman Regional Health System
