Urgent Colonoscopy for Evaluation and Management of Acute Lower Gastrointestinal Hemorrhage: A Randomized Controlled Trial
|
|
|
- Milton Poole
- 8 years ago
- Views:
Transcription
1 American Journal of Gastroenterology ISSN C 2005 by Am. Coll. of Gastroenterology doi: /j x Published by Blackwell Publishing Urgent for Evaluation and Management of Acute Lower Gastrointestinal Hemorrhage: A Randomized Controlled Trial Bryan T. Green, M.D., Don C. Rockey, M.D., G. Portwood, M.D., Paul R. Tarnasky, M.D., Steve Guarisco, M.D., Malcolm S. Branch, M.D., Joseph Leung, M.D., and Paul Jowell, M.D. Division of Gastroenterology, Department of Medicine, Duke University Medical Center, Durham, North Carolina OBJECTIVES: METHODS: RESULTS: CONCLUSION: We hypothesized that early intervention in patients with lower gastrointestinal bleeding (LGIB) would improve outcomes and therefore conducted a prospective randomized study comparing urgent colonoscopy to standard care. Consecutive patients presenting with LGIB without upper or anorectal bleeding sources were randomized to urgent purge preparation followed immediately by colonoscopy or a standard care algorithm based on angiographic intervention and expectant colonoscopy. A total of 50 patients were randomized to each group. A definite source of bleeding was found more often in urgent colonoscopy patients (diverticula, 13; angioectasia, 4; colitis, 4) than in the standard care group (diverticula, 8; colitis, 3) (the odds ratio for the difference among the groups was 2.6; 95% CI ). In the urgent colonoscopy group, 17 patients received endoscopic therapy; in the standard care group, 10 patients had angiographic hemostasis. There was no difference in outcomes among the two groups including: mortality 2% versus 4%, hospital stay 5.8 versus 6.6 days, ICU stay 1.8 versus 2.4 days, transfusion requirements 4.2 versus 5 units, early rebleeding 22% versus 30%, surgery 14% versus 12%, or late rebleeding 16% versus 14% (mean follow-up of 62 and 58 months). Although urgent colonoscopy identified a definite source of LGIB more often than a standard care algorithm based on angiography and expectant colonoscopy, the approaches are not significantly different with regard to important outcomes. Thus, decisions concerning care for patients with acute LGIB should be based on individual experience and local expertise. (Am J Gastroenterol 2005;100: ) INTRODUCTION Acute lower gastrointestinal bleeding (LGIB) is a common disorder, requiring hospitalization in 21 adults per 100,000/yr (1). Diverticula are the most common cause of acute LGIB and account for 42 56% of episodes (1 3). Other lesions (colonic vascular ectasis, or angiodysplasias, rectal or colonic ulcers, colonic varices, vasculitis, neoplasia, colitis, intussusception, or small intestinal lesions) account for the remaining identifiable causes of LGIB. A major problem in LGIB is that approximately 10 40% of patients will have recurrent hemorrhage, usually within the first 48 h of the index bleed (1, 4). This is often treated by surgical resection. Since the major causes of acute LGIB (diverticulosis and vascular ectasis) are most prevalent in the elderly, surgery often entails a high morbidity and mortality. Although early endoscopy for the diagnosis and, in particular, treatment of upper gastrointestinal bleeding is widely accepted, early endoscopy has not been similarly applied to LGIB. is often performed after the bleeding has stopped and the patient adequately prepared, generally several days after presentation (3). However, a major problem with colonoscopy in this setting has been the low detection rate of bleeding lesions, thus not allowing endoscopic hemostasis. It has been widely reported that urgent colonoscopy is safe and yields a specific diagnosis in a high proportion of cases (5 7). Further, a number of case series have demonstrated that endoscopic therapy during urgent colonoscopy allows initial hemostasis, especially in diverticular bleeding, although follow up has been lacking (8 13). Endoscopic therapy of vascular ectasis has also been shown to be safe and effective (14, 15). A recent nonrandomized study demonstrated a dramatic reduction in rebleeding and the need for surgery with urgent endoscopic therapy in diverticular hemorrhage (7). However, other nonrandomized studies have failed to demonstrate improvement in outcomes after urgent colonoscopy (16, 17). 2395
2 2396 Green et al. Despite the lack of data from randomized controlled studies, urgent colonoscopy is widely recommended and employed by some experts (7). At our institution, the standard care for LGIB, after excluding an upper or anorectal source, is to perform a technetium labeled red cell scan if active bleeding is suspected, followed by visceral angiography for positive scans. Expectant colonoscopy is performed if bleeding is felt to be inactive. We hypothesized that urgent colonoscopy would improve early rebleeding and also the secondary outcomes measures of length of stay and transfusion requirements. We present the results of a prospective, randomized, controlled trial of urgent colonoscopy compared to a standard protocol commonly implemented at this institution in patients with acute LGIB. Positive Angiographic Hemostasis Positive Visceral Angiography Yes Technetium RBC Scan Negative Ongoing bleeding Negative No ME THODS This study was approved by the Duke University Medical Center and Durham Veterans Affairs Medical Center Institutional Review Boards, and fulfilled all criteria for clinical research as set forth in the Declaration of Helsinki (18). All patients gave written informed consent. Patients presenting with hematochezia who were admitted to our hospitals were eligible for the study. Prior to randomization all patients had upper gastrointestinal sources of bleeding excluded by nasogastric lavage and/or esophagogastroduodenoscopy. An upper endoscopy was performed if there was nobile present in the gastric lavage fluid, there was a high suspicion of upper gastrointestinal hemorrhage, there was a history of peptic ulcer disease, or a history of previous upper gastrointestinal bleed. Anorectal sources of bleeding were excluded by anoscopy and/or proctoscopy, one or both of which was performed in all participants. Patients were randomized to a standard care algorithm or to purge preparation colonoscopy (Fig. 1). Inclusion criteria were as follows: (1) the last bloody bowel movement was within 24 h of presentation; (2) there was clinical or laboratory evidence of significant blood loss, manifested by any one of the following: (a) >3 bloody bowel movements in <8 h;(b) admission to the intensive care unit; (c) decrease of more than 5% hematocrit points in <12 h; (d) transfusion of >3 units of packed red blood cells; (e) hemodynamic instability in previous 6 h defined by: angina, syncope, presyncope, orthostatic vital signs, mean arterial blood pressure <80 mmhg, or resting pulse >110. Patients meeting the following criteria were excluded: (1) age <18 yr; (2) known or suspected inflammatory bowel disease; (3) abdominal surgery within previous 10 days; (4) endoscopic polypectomy within the previous 10 days; (5) known or suspected ischemic bowel, perforation, or peritonitis; (6) refractory angina or suspected myocardial infarction; (7) hemodynamic instability refractory to resuscitation; (8) coagulopathy refractory to correction; (9) acquired immune deficiency syndrome or neutropenia; (10) documented pregnancy; (11) inability to provide informed consent. The num- Figure 1. Standard care algorithm. Technetium RBC scanning was performed on patients with suspected active bleeding while those without active bleeding had an elective colonoscopy. Patients with a positive technetium scan went to visceral angiography while those with a negative scan had an elective colonoscopy. Active bleeding on angiography was treated. All patients receiving angiography (whether positive or negative) had an elective colonoscopy. ber of comorbidities were recorded and scored to determine the Charlson comorbidity index (19). The Charlson index is a measure of the number of associated comorbid medical conditions that predicts mortality risk at 1 yr. Higher scores represent an increased risk of mortality. Patients were randomized from July 1993 through June Eligible patients were randomized to either purge prep colonoscopy or the standard care algorithm (defined later) by a computergenerated randomization list. All patients were admitted to either the intensive care unit or to telemetry units and managed by a team of internists, intensivists, and general surgeons in consultation with gastroenterologists. Investigators were not primarily involved in the care or decision making for the patients; in some instances, investigators served as consultants to the primary care team. Patients were transferred out of the intensive care unit after hemodynamical stability had been achieved and maintained. Anticoagulants and nonsteroidal anti-inflammatory drugs (NSAIDs), including aspirin, were discontinued during hospitalization in all patients. Packed red blood cells were transfused to correct severe anemia (transfusion threshold hemoglobin <8 g/dl) or to help achieve hemodynamic stability in massive bleeding. Coagulopathy was corrected with platelet and/or fresh frozen plasma transfusion. Urgent Purge Preparation Patients randomized to urgent colonoscopy underwent colonic preparation with a polyethelyne glycol based purgative (Golytely, Braintree Laboratories, Braintree, MA) administered either orally (25 patients) (one cup every 15 min)
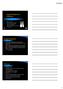
3 Urgent for LGIB 2397 or by nasogastric tube (25 patients) (250 ml every 15 min). Oral administration was the preferred route and only when patients were unable to comply was the preparation administered via nasogastric tube. Four to six liters of purge and 3 4 h were required to clean the colon. was performed within 2 h after the clearance of stool and large clots and within 8 h of hospitalization or the diagnosis of hematochezia. Patients received conscious sedation with meperidine and diazepam while monitoring heart rate, blood pressure, and oxygen saturation. A standard video colonoscope (Olympus, Tokyo, Japan) was used for all procedures. The colonoscope was advanced to the cecum in all cases. The terminal ileum was intubated when possible. The quality of the preparation was graded as excellent if there was no stool, blood, or clots covering the mucosa, fair if less than 25% of the mucosa was obscured by stool, blood, or clots, and poor if there was formed stool or if greater than 25% of the mucosa was obscured by stool or blood. The colon was carefully examined on withdrawal with careful attention to washing any obscured mucosa. Diverticula or angioectasia with active bleeding or with stigmata of recent hemorrhage (see below for definitions) were treated endoscopically. In patients with active bleeding, 1 or 2 ml aliquots of epinephrine (dilution, 1:10,000) was injected into each of four quadrants around the lesion to control bleeding. Lesions were then treated with bipolar electrocautery with 10 to 15 W of power, moderate appositional pressure, and one-second pulses until coagulation and/or flattening of the vessel was achieved. Patients with stigmata of bleeding were treated with bipolar electrocautery alone. Endoscopic therapy was considered successful if bleeding ceased at the end of the procedure or for non-bleeding lesions if the underlying stigmata were obliterated. After recovery from sedation, patients were managed by their primary team as their clinical status dictated. Definition of Endoscopic Lesions and of a Definite Bleeding Source Active bleeding was defined as visualization of blood emanating from a specific, distinct, readily identifiable lesion, and in which bleeding continued after vigorous irrigation. A visible vessel was defined as a protuberant, purple or red, punctate, lesion. Stigmata of recent hemorrhage was defined as present in the setting of non-bleeding visible vessel or as a densely adherent clot that remained present after vigorous washing. A definite source of bleeding was defined as a lesion visualized by either endoscopy or angiography that was either actively bleeding or had clear stigmata of recent bleeding (as described previously). Lesions were classified as a presumptive source of bleeding if they did not have active bleeding or stigmata of bleeding but after colonoscopy, upper endoscopy, and small bowel enteroscopy with a 210-cm video enteroscope (Olympus), no other potential bleeding sites were identified. The source of bleeding was considered unknown only after colonoscopy with an adequate preparation (fair or excellent as assessed by the aforementioned scale), upper endoscopy, and small bowel enteroscopy all failed to reveal a potential source of bleeding. Small bowel follow through radiographs were obtained at later time points in patients with an unknown source of bleeding. Standard Algorithm The standard care algorithm is shown in Figure 1. Patients with suspected ongoing bleeding underwent technetium labeled red cell scanning. The presence of ongoing bleeding was based on clinical judgment made by the primary team in consultation with the gastroenterology team, and was defined as the continued passage of bloody stools during medical evaluation or as persistently unstable vital signs despite resuscitation (the presence of unstable vitals signs was judged as above). Patients with positive scans proceeded to angiography while those with negative scans underwent elective colonoscopy. colonoscopy was defined as that performed after routine preparation (4 6 L of polyethelyne glycol based purgative, administered orally beginning the night prior to the procedure) within four days of admission. Active bleeding found on visceral angiography was treated with intra-arterial infusion of vasopressin. Super-selective embolization was not performed. Angiographic therapy was considered successful if extravasation of contrast ceased at the conclusion of the procedure. Patients without active bleeding on angiography underwent elective colonoscopy. Follow-Up Patients and their outcomes were prospectively assessed during the index hospitalization. Outpatient follow-up was with either an attending gastroenterologist or the patient s primary physician. These records as well as hospital records were retrospectively reviewed and abstracted to obtain late rebleeding and mortality data. Patients with definitive or presumed bleeding from diverticula were advised to avoid prescription or over the counter nonsteroidal anti-inflammatory agents (including aspirin) as well as anticoagulants. The mean duration of follow-up was 62 and 58 months for the urgent colonoscopy and standard therapy groups, respectively. End Points The primary end point was rebleeding. This was classified as either early rebleeding (prior to hospital discharge) or late rebleeding (after hospital discharge). Secondary end points were duration of hospital and intensive care unit stay, blood transfusion requirements, need for surgery, and mortality. Rebleeding was defined as hematochezia developing after index colonoscopy or angiography was defined as that occurring after clinical cessation of the index bleeding event (using criteria for bleeding as above). Statistical Analysis Apower calculation was performed using available estimates of the diagnostic yield for the two strategies examined here. It was estimated that urgent, purge prepped colonoscopy would identify a source of bleeding at 0.75 (P1) while the alternative
4 2398 Green et al. algorithm would lead to a detection rate of Based on these estimates, to have 80% power (β + 0.2)/α set at 0.05 (2-tailed), 58 subjects would be required for each group. Enrollment for the study terminated early because of the difficulty in recruiting and because several of the key investigators left Duke. The data were analyzed by the first two authors (BTG and DCR). Statistical analysis was performed with the Student s t-test and the Mann-Whitney test for continuous variables and Fisher s exact test for categorical variables. A p value of <0.05 was considered to be statistically significant. Odds ratios were calculated using the approximation of Woolf. RESULTS A total of 112 patients were screened by the investigators for potential participation in the study. Seven were excluded prior to randomization for the following reasons: Four had upper gastrointestinal sources of bleeding identified on upper endoscopy and three had anorectal sources identified when anoscopy was performed during their initial examination. One hundred and five patients were randomized, however 5 dropped out prior to completing their initial diagnostic evaluation (all patients dropped out because they decided that they did not wish to participate and before any diagnostic testing was performed). Of these 5 participants, 3 were randomized to the urgent colonoscopy group and 2 to the standard care group. All patients in the study underwent anoscopy at the time of initial evaluation. Two patients were found to have hemorrhoids, and 1 patient had proctitis, and thus were excluded from possible randomization. Eight patients underwent upper endoscopies, of whom 4 had lesions detected (and were not enrolled) and another 4 had negative studies (and were enrolled). Thus, 50 patients were randomized to each of the urgent colonoscopy and standard care groups. The number of patients undergoing specific procedures is highlighted in Figure 2. The demographic and clinical characteristics are shown in Table 1. Overall, 16% of patients had a history of previous LGIB and 55% were using NSAIDs or aspirin. On presentation 59% of all patients had ongoing bleeding and 64% had unstable hemodynamics. Among patients randomized to urgent colonoscopy, the mean time from presentation to the procedure was 7.2 h ( h) compared to 38.1 h ( h) in patients randomized to standard care. The endoscopic view during urgent and elective colonoscopy was rated (by the previously stated scale) as excellent in 36% and 38%, fair in 56% and 52%, and poor in 8% and 10% of patients (respectively). There was fresh blood present during colonoscopy in 44% of urgent colonoscopy patients and 12% of standard care patients. Ongoing bleeding was suspected in 27 (57%) of patients randomized to urgent colonoscopy. Diverticula or angioectasia with either active bleeding or stigmata of recent bleeding were found in 17 patients in the urgent colonoscopy group. Endoscopic Hemostasis n=17 Angiographic Hemostasis n=10 n=8 Urgent n=50 Enrolled and randomized Hematochezia n=105 No Endoscopic Hemostasis n=33 n=100 Visceral Angiography n=18 Technetium RBC Scan n=36 Withdrew n=5 n=8 Standard Care n=50 Ongoing bleeding n=18 n=14 Figure 2. Study flow. The number of patients having specific diagnostic and therapeutic interventions is shown. Bleeding diverticula (8 with active bleeding and 5 with stigmata of bleeding) were located as follows: 5 in the left colon, 1inthe transverse colon, and 7 in the right colon. All 4 of the identified vascular ectasias (3 with active bleeding and 1 with stigmata) were located in the right colon. All underwent endoscopic treatment according to the protocol outlined in Methods section. The flow of patients through the standard care algorithm is shown in Figure 1. Ongoing bleeding was suspected in 36 patients (72%) randomized to standard care; all underwent technetium labeled RBC scans. These scans were positive in 18 patients (50%). Visceral angiography was performed in all of these patients and revealed putative sites of bleeding in 10 (56%). In 8 of these patients, diverticula were presumed to be the cause of bleeding. However, the source could not be identified with certainty in the other 2 patients. The bleeding diverticula were located as follows: 3 in the left colon, 1 in the transverse colon, and 4 in the right colon. Vasopressin was administered to all 10 patients and successfully caused bleeding to stop in 8 (80%). Both patients in whom it was unsuccessful went
5 Urgent for LGIB 2399 Table 1. Baseline Patient Characteristics Urgent Standard Care (n = 50) (n = 50) Men/women 27/23 32/18 Age (yr) Race White Black Other 1 3 History of LGIB 6 10 Comorbidities NSAID Duration of bleeding prior to presentation (h) Ongoing bleeding 27 (54%) 36 (72%) Initially unstable Hemodynamics 30 (60%) 34 (68%) Initial hematocrit (%) Transfusion resuscitation only (units of PRBC) There was no significant difference between values. Data are expressed as mean + standard deviation. LGIB = lower gastrointestinal bleeding; NSAIDs = nonsteroidal anti-inflammatory drugs; PRBC = packed red blood cells; ns = not significant. to emergent surgery (1 subtotal colectomy and 1 segmented resection). was performed in 15 patients in this group. No lesions with stigmata of bleeding were identified. The sources of bleeding in each group are shown in Table 2. The likelihood of identifying a definite source of bleeding was greater in the urgent colonoscopy group (21 patients (42%)) than in the standard care group (11 patients (22%)) (odds ratio 2.6; 95% CI ). Diverticula were considered to be a definite source of bleeding in 8 patients in the standard care group (all diagnosed by angiography). Ischemic colitis was considered the definite source of bleeding in 3 standard care patients due to stigmata of recent bleeding (not amendable to endoscopic hemostasis) identified on routine colonoscopy. All definite and presumptive diagnoses in the urgent colonoscopy group were made during the ini- Table 2. Identified Bleeding Sources Urgent Standard Care (n = 50) (n = 50) OR; 95% CI Definite Diverticula 13 8 Angioectasia 4 0 Ischemic colitis 4 3 Total 21 (42%) 11 (22%) 2.6; Presumptive Diverticula ; Angioectasia (colon) 0 1 Angioectasia (jejunum) 1 0 Colitis 0 3 Polyp 0 2 Ulcer (colon) 0 1 Total 27 (54%) 27 (54%) 1.0; Unknown 2 12 Table 3. Outcomes Urgent Standard Care (n = 50) (n = 50) Early rebleed 11 (22%) 15 (30%) Late rebleed 8 (16%) 7 (14%) Mortality LGIB 1 (2%) 2 (4%) Other 0 2 Hospital stay (days) Total ICU Total PRBC (u) Surgery 7 (14%) 6 (12%) Subtotal colectomy 0 3 Hemicolectomy 5 2 Segmental 2 1 Complications 1 0 Data are expressed as mean + standard deviation. LGIB = lower gastrointestinal bleeding; ICU = intensive care unit; PRBC = packed red blood cells; u = units; ns = not significant. tial colonoscopy. Small bowel enteroscopy was performed in all patients with either a presumptive or unknown source of bleeding. A large angioectasia in the jejunum was considered the presumptive source of bleeding in 1 patient in the urgent colonoscopy group. Two patients in the urgent colonoscopy group and 5 patients in the standard care group with either a presumed or unknown source of bleeding had a poor preparation and all underwent repeat colonoscopy during the index hospitalization; a definite bleeding source could not be identified in any of these patients. In 9 patients with an unknown source of bleeding, small bowel followthrough radiographs were obtained as outpatients were unrevealing in all cases. None of the 14 patients with an unknown source of bleeding experienced either early or late rebleeding. Clinical outcomes are shown in Table 3. Early rebleeding did not appear to be different between the urgent colonoscopy and standard care groups (11 (22%) and 15 (30%), respectively; odds ratio 0.7; 95% CI ). Over a mean followup period of 62 and 58 months in the urgent colonoscopy and standard care groups, respectively, late rebleeding was not different (8 (16%) and 7 (14%), respectively). All episodes of late rebleeding in both groups were due to diverticula. Total hospital and intensive care unit stay was also not significantly different between the groups. The mean total blood requirement per patient was lower in the urgent colonoscopy group (4.2 U vs 5.0 U, respectively), but it did not reach statistical significance (p = 0.09). The need for surgery was not different between the groups. The mean duration of stay in the intensive care unit was shorter in the endoscopic hemostasis group than in the angiographic hemostasis group (1.9 days vs 3.9 days, respectively), but this was not statistically significant (p = 0.62). The mean total blood requirement per patient appeared to be less in the endoscopic hemostasis group than in the angiographic hemostasis (5.4 U vs 9 U,respectively), but the difference did not reach statistical significance (p = 0.165).
6 2400 Green et al. One patient in the urgent colonoscopy group had a colonic perforation after endoscopic treatment of an angioectasia in the cecum and required surgery. Finally, we compared the outcomes of the 17 patients undergoing endoscopic hemostasis to the 10 patients undergoing angiographic therapy. These groups were nearly identical in terms of baseline characteristics. The initial hemostasis rate, early rebleeding rate, late rebleeding rate, surgical intervention rate, length of hospital stay, transfusion requirement, complication rate, and mortality rate was identical in each group. Comparisons between groups were additionally analyzed based on an intention to treat basis (53 and 52 patients in the urgent colonoscopy and standard care groups, respectively). The primary end point of early rebleeding still did not differ between the urgent colonoscopy and standard care groups (11 (21%) and 15 (29%), respectively). This analysis also revealed identical results for other end points as compared to the primary analysis. DISCUSSION This study demonstrated that urgent colonoscopy identified a definite source of lower gastrointestinal hemorrhage more often than a standard care algorithm that utilized elective colonoscopy. Despite this apparent improvement in diagnosis, in this study, urgent colonoscopy did not significantly improve important outcomes such as either early or late rebleeding. While it is tempting to extrapolate the well documented benefits of urgent endoscopy with hemostatic treatment in acute upper gastrointestinal bleeding (20, 21) to LGIB, it should be emphasized that such an extrapolation may not necessarily be valid. There are several distinctions between the two types of bleeding. For upper gastrointestinal bleeding lesions such as ulcers and varices, these lesions may be readily identified, and thus, endoscopic therapy can be readily applied. However, in lesions that cause LGIH are often difficult to identify, and may be different pathologically (the colon is different than the stomach and duodenum, diverticula are different anatomically than ulcers) so that it remains unproven whether endoscopic therapy is effective. Additionally, unlike gastric or duodenal ulcers in which therapy after control of the acute bleeding leads may lead to elimination of the causal agent (i.e., NSAIDs, acid, or Helicobacter pylori), the same is not necessarily true for the lesions that cause LGIB. While it has been suggested that lifestyle modifications such as high fiber diets and avoidance of foods with small seeds may alter the natural history of existing diverticuli, this remains speculative. In addition, the pathophysiology of diverticular and vascular ectasia bleeding is such that treatment of an individual lesion may be effective, however, other lesions may bleed. Our results differ from a recent nonrandomized study (7) that demonstrated an apparent beneficial effect for urgent colonoscopy in LGIH. In this previous study (7), endoscopic treatment of bleeding diverticula led to a reduction in rebleeding. In the current study, 13 patients received endoscopic treatment to culprit diverticula and yet 5 rebled early and 2 rebled late. This finding could be related to a variety of technical factors, but this was unlikely given standardization of the techniques utilized. The most notable difference in the two studies was that the current study was randomized. The previous study (7) compared therapy in two different time periods, and One drawback of such an approach includes the possibility that changes in clinical care such as improvements in intensive care, improved endoscopic techniques, divergent transfusion practices, updated general medical care, and different thresholds for surgical intervention. Further, differences in the acuity of bleeding could have accounted for the differences in study outcome. For example, our study included all patients admitted with hematochezia and hemodynamically significant blood loss. Finally, follow-up for the current study was nearly twice as long (57 months) as that in the previous study (34 months). The standard care group required angiography and although this is a small number of patients, there were no complications from angiography. The absence of complications in this group was surprising, but could be related to the emphasis on vascular radiology procedures at our institution. All patients requiring angiographic hemostasis had intraarterial vasopressin infusion, as was standard at the time. Recently, super-selective embolization techniques have been introduced, and may reduce the rebleeding rate (i.e., from approximately 40% to as low as 7% in expert hands) (22 24). Thus, it is possible that super-selective embolization could improve outcomes in the standard care group. Although urgent colonoscopy did not alter the primary end point of rebleeding, its use could be justified if it improved secondary end points such as hospital stay, transfusion requirements, or the need for surgery. Previous work has demonstrated that urgent colonoscopy may reduce hospital stay (3, 25). Although there was a trend toward lower total blood transfusion requirements in the urgent colonoscopy group (4.2 units vs 5 units), this difference did not reach statistical significance (p = 0.09). The requirement for surgery and length of hospital stay (total or ICU) were not different in the two groups. It has been suggested that urgent colonoscopy might provide better localization of bleeding sites, thus allowing a more focused surgical resection for lesions that continue to bleed. Indeed, no patients in the urgent colonoscopy group required subtotal colectomy compared to three in the standard care group. Although this comparison is attractive, the number of patients seen in this study are too small to allow us to make firm conclusions. A definite source of bleeding was identified in 42% of patients in the urgent colonoscopy group, compared to only 22% in the standard care group. Other studies investigating urgent colonoscopy have found this approach to yield a definite bleeding site in % of patients (2, 6, 7, 17, 26 28). The wide discrepancy reported in the literature almost
7 Urgent for LGIB 2401 certainly is reflective of a number of inherent biases. For example, definitions of a definite bleeding site are likely to vary. Some required, as we did, active bleeding or stigmata of recent bleeding (6, 16) while others were less stringent (2, 6). Additionally, differences in the ability to assess lesions, as well as differences in equipment, timing and quality of the preparation among studies, likely translate into variability in detection of lesions. There are several important strengths of this study, including that it is the first randomized study evaluating urgent colonoscopy in acute LGIB, it had long-term follow-up, the patient management was standardized, and that a homogeneous patient population was studied. Nonetheless, there are several important weaknesses of this study. The greatest weakness is that because the sample size is modest, we are unable to exclude differences in outcomes due to a type II statistical error (unfortunately, the study did not reach its planned size because the study was terminated early). Indeed, the possibility of a type II statistical error may be insurmountable without a study employing a multicenter design that allows recruitment of an extremely large sample size. A further weakness of this study was that physicians caring for patients were not blinded to randomization or specific interventions (because withholding the findings of endoscopy or radiology procedures to the responsible physicians was felt to be unethical with regard to delivery of quality patient care). Thus, the unblinded study design could have introduced any of a number of biases, although there is no reason to presuppose a priori that patients in one group or the other were handled differently because of their randomization assignment. For example, routine care such as transfusion practices, criteria for intensive care unit, endoscopic techniques, and the like were standardized. colonoscopy in the standard care group was performed at a range of 1 4 days after admission and thus could have potentially caused some variability in the total hospital stay if patients were kept in the hospital awaiting a colonoscopy. It is not however, standard practice at our institution to prolong patient hospitalization for an elective procedure. Finally, initial enrollment in this study was begun approximately 10 yr ago and it is possible that some aspects of care have improved. For example, it is possible that intensive care unit treatment, surgical techniques, transfusion, and early hospital discharge criteria have all improved. In this situation, it is likely that such improvements would affect both intervention groups equally, thus improving the outcomes for all patients but not altering the comparison between groups. In summary, the data from this study suggest that for patients with substantial lower gastrointestinal hemorrhage, outcomes are similar whether urgent colonoscopy or expectant colonoscopy is performed as part of a standard care algorithm. Except for diagnosis, urgent colonoscopy proved to provide no advantage over radiographic intervention. Thus, we suggest that the choice of these two approaches should be based on local expertise and available resources. ACKNOWLEDGMENTS We thank the Nurses, the Housestaff, and the Fellows and Faculty involved in the care of these patients for their assistance. This work was supported by the Burroughs Welcome Fund (DCR is the recipient of a BWF Translational Scientist Award) and in part by a grant from the American College of Gastroenterology. Reprint requests and correspondence: Don C. Rockey, M.D., Division of Digestive and Liver Diseases, University of Texas Southwestern Medical Center, 5323 Harry Hines Blvd., Dallas, TX Received August 27, 2004; accepted May 23, REFERENCES 1. Longstreth GF. Epidemiology and outcome of patients hospitalized with acute lower gastrointestinal hemorrhage: A population based study. Am J Gastroenterol 1997;92(3): Wilcox CM, Clark S. Causes and outcome of upper and lower gastrointestinal bleeding: The Grady Hospital experience. South Med J 1999;92(1): Schmulewitz N, Fisher DA, Rockey DC. Early colonoscopy for acute lower GI bleeding predicts shorter hospital stay: A retrospective study of experience in a single center. Gastrointest Endosc 2003;58: McGuire HH. Bleeding colonic diverticuli. A reappraisal of natural history and management. Ann Surg 1994;220: Kok KY, Kum CK, Goh PM. Colonoscopic evaluation of severe hematochezia in an Oriental population. Endoscopy 1998;30: Chaudry V, Hyser MJ, Gracias VH, et al. : The initial test for acute lower gastrointestinal bleeding. Am Surg 1998;64: Jenson DM, Machicado GA, Jutabha R, et al. Urgent colonoscopy for the diagnosis and treatment of severe diverticular hemorrhage [see comments]. N Engl J Med 2000;342: Johnson JJ, Sones J. Endoscopic heater probe coagulation of the bleeding colonic diverticulum. Gastrointest Endosc 1986;32:168A. 9. Pardole PM, Neubrand S. Injection control of colonic hemorrhage with hypertonic saline-epinephrine solution. Am J Gastroenterol 1989;84:1193A. 10. Kim YI, Marcon NE. Injection therapy for colonic diverticular bleeding. A case study. J Clin Gastroenterol 1993;17(1): Savides TJ, Jensen DM. Colonoscopic hemostasis for recurrent diverticular hemorrhage associated with a visible vessel: A report of three cases. Gastrointest Endosc 1994;40(1): Foutch PG, Zimmerman K. Diverticular bleeding and the pigmented protuberance (sentinel clot): Clinical implications, histopathological correlation, and results of endoscopic intervention. Am J Gastroenterol 1996;91(12): Pakash C, Chokshi H, Walden DT, et al. Endoscopic hemostasis in acute diverticular bleeding. Endoscopy 1999;31(6):460 3.
8 2402 Green et al. 14. Gupta N, Longo WE, Vernava AM. Angiodysplasia of the lower gastrointestinal tract: An entity readily diagnosed by colonoscopy and primarily managed nonoperatively. Dis Colon Rectum 1995;38: Bemvenuti GA, Julich MM. Ethanolamine injection for sclerotherapy of angiodysplasia of the colon. Endoscopy 1998;30: Bloomfeld R, Shetzline M, Rockey DC. Urgent colonoscopy for the diagnosis and treatment of severe diverticular hemorrhage. N Engl J Med 2000;342: Angtuaco TL, Reddy SK, Drapkin S, et al. The utility of urgent colonoscopy in the evaluation of acute lower gastrointestinal tract bleeding: A 2-year experience from a single center. Am J Gastroenterol 2001;96: World Medical Association Declaration of Helsinki. Recommendations guiding physicians in biomedical research involving human subjects. JAMA 1997;277: Charlson ME, Pompei P, Ales KL, et al. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J Chronic Dis 1987;40: Laine L. Multipolar electrocoagulation in the treatment of active upper gastrointestinal tract hemorrhage. A prospective controlled trial. N Engl J Med 1987;316: Cook DJ, Guyatt GH, Salena BJ, et al. Endoscopic therapy for acute nonvariceal upper gastrointestinal hemorrhage: A meta-analysis. Gastroenterology 1992;102: DeBarros J, Rosas L, Cohen J, et al. The changing paradigm for the treatment of colonic hemorrhage: Super-selective angiographic embolization. Dis Colon Rectum 2002;45: Ledermann HP, Schoch E, Jost R, et al. Superselctive coil embolization in acute gastrointestinal hemorrhage: Personal experience in 10 patients and review of the literature [see comments]. J Vasc Interv Radiol 1998;9: Peck DJ, McLoughlin RF, Hughson MN, et al. Percutaneous embolotherapy of lower gastrointestinal hemorrhage [see comments]. J Vasc Interv Radiol 1998;9: Strate LL, Syngal S. Timing of colonoscopy: Impact on length of hospital stay in patients with acute lower intestinal bleeding. Am J Gastroenterol 2003;98: Zuckerman GR, Prakash C. Acute lower intestinal bleeding. Part II: Etiology, therapy, and outcomes. Gastrointest Endosc 1999;49: Jensen DM, Machicado GA. for diagnosis and treatment of severe lower gastrointestinal bleeding. Routine outcomes and cost analysis. Gastrointest Endosc Clin N Am 1997;7: Jensen DM, Machicado G. Diagnosis and treatment of severe hematochezia: The role of urgent colonoscopy after purge. Gastroenterology 1988;95:
ORIGINAL ARTICLE: Clinical Endoscopy
 ORIGINAL ARTICLE: Clinical Endoscopy Immediate unprepared hydroflush colonoscopy for severe lower GI bleeding: a feasibility study Aparna Repaka, MD, Matthew R. Atkinson, MD, Ashley L. Faulx, MD, Gerard
ORIGINAL ARTICLE: Clinical Endoscopy Immediate unprepared hydroflush colonoscopy for severe lower GI bleeding: a feasibility study Aparna Repaka, MD, Matthew R. Atkinson, MD, Ashley L. Faulx, MD, Gerard
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
Rebleeding and survival after acute lower gastrointestinal bleeding
 The American Journal of Surgery 188 (2004) 485 490 Scientific paper Rebleeding and survival after acute lower gastrointestinal bleeding Thomas Anthony, M.D.*, Pradeep Penta, B.S., Robert D. Todd, B.S.,
The American Journal of Surgery 188 (2004) 485 490 Scientific paper Rebleeding and survival after acute lower gastrointestinal bleeding Thomas Anthony, M.D.*, Pradeep Penta, B.S., Robert D. Todd, B.S.,
Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage
 Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage Brian P. Bosworth A. Outcomes in Lower Gastrointestinal Bleeding Acute
Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage Brian P. Bosworth A. Outcomes in Lower Gastrointestinal Bleeding Acute
LOWER GASTROINTESTINAL BLEEDING GED/05/08
 LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
Surgical Management of GI Bleeding. VA Case Presentation. 0-24 hours 9/18/2012
 Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
HOW I DO IT Approach to lower gastrointestinal bleeding
 HOW I DO IT Approach to lower gastrointestinal AUTHORSHIP How I do it: Roque Sáenz MD Eduardo Valdivieso MD, MSc The Latin-American Advanced Gastrointestinal Endoscopy Training Center Clínica Alemana,
HOW I DO IT Approach to lower gastrointestinal AUTHORSHIP How I do it: Roque Sáenz MD Eduardo Valdivieso MD, MSc The Latin-American Advanced Gastrointestinal Endoscopy Training Center Clínica Alemana,
Acute lower gastrointestinal bleeding (LGIB) is distinct clinically from upper
 Gastroenterol Clin N Am 34 (2005) 665 678 GASTROENTEROLOGY CLINICS OF NORTH AMERICA Lower Gastrointestinal Bleeding Management Bryan T. Green, MD a, *, Don C. Rockey, MD b a Division of Gastroenterology,
Gastroenterol Clin N Am 34 (2005) 665 678 GASTROENTEROLOGY CLINICS OF NORTH AMERICA Lower Gastrointestinal Bleeding Management Bryan T. Green, MD a, *, Don C. Rockey, MD b a Division of Gastroenterology,
Vikram S. Kumar Gillian Lieberman, MD. September 2002. Lower GI Bleeds. Vikram Sheel Kumar, Harvard Medical School Year III Gillian Lieberman, MD
 September 2002 Lower GI Bleeds Vikram Sheel Kumar, Harvard Medical School Year III Index Case maroon/bright red: think lower GI bleed Mr. X, 78 years old, presents w/ maroon stool and eighteen hours of
September 2002 Lower GI Bleeds Vikram Sheel Kumar, Harvard Medical School Year III Index Case maroon/bright red: think lower GI bleed Mr. X, 78 years old, presents w/ maroon stool and eighteen hours of
GI Bleeding. Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics
 GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD
 Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
UGI Tract Hemorrhage. GI Tract Emergencies. UGI Hemorrhage. David D. Markowitz, MD. UGI tract hemorrhage Comorbid disease
 UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
Endoscopic diagnosis and treatment of severe lower gastrointestinal bleeding. Gustavo A Machicado, Dennis M Jensen
 Endoscopic diagnosis and treatment of severe lower gastrointestinal bleeding Gustavo A Machicado, Dennis M Jensen UCLA Center for the Health Sciences, Veteran s Administration Greater Los Angeles Healthcare
Endoscopic diagnosis and treatment of severe lower gastrointestinal bleeding Gustavo A Machicado, Dennis M Jensen UCLA Center for the Health Sciences, Veteran s Administration Greater Los Angeles Healthcare
ASGE Guideline: the role of endoscopy in the patient with lower-gi bleeding
 GUIDELINE ASGE Guideline: the role of endoscopy in the patient with lower-gi bleeding This is one of a series of statements discussing the utilization of GI endoscopy in common clinical situations. The
GUIDELINE ASGE Guideline: the role of endoscopy in the patient with lower-gi bleeding This is one of a series of statements discussing the utilization of GI endoscopy in common clinical situations. The
Gastrointestinal bleeding
 Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Endoscopic Management of Acute Lower Gastrointestinal Bleeding
 American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2008.02075.x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management
American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2008.02075.x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management
ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding
 PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas
 Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Management of the Adult Patient With Acute Lower Gastrointestinal Bleeding
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 93, No. 8, 1998 Copyright 1998 by Am. Coll. of Gastroenterology ISSN 0002-9270/98/$19.00 Published by Elsevier Science Inc. PII S0002-9270(98)00276-7 Practice
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 93, No. 8, 1998 Copyright 1998 by Am. Coll. of Gastroenterology ISSN 0002-9270/98/$19.00 Published by Elsevier Science Inc. PII S0002-9270(98)00276-7 Practice
Diagnosis and management of lower gastrointestinal bleeding
 Diagnosis and management of lower gastrointestinal bleeding Jürgen Barnert and Helmut Messmann abstract Lower gastrointestinal bleeding (LGIB) can present as an acute and life threatening event or as chronic
Diagnosis and management of lower gastrointestinal bleeding Jürgen Barnert and Helmut Messmann abstract Lower gastrointestinal bleeding (LGIB) can present as an acute and life threatening event or as chronic
Colonoscopy Data Collection Form
 Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
How to Effectively Code for Endoscopic Procedures in Gastroenterology
 How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
Cost-Saving Approach to Patients on Long-Term Anticoagulation Who Need Endoscopy: A Decision Analysis
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 8, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Inc. doi:10.1016/s0002-9270(03)00445-3 Cost-Saving Approach
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 8, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Inc. doi:10.1016/s0002-9270(03)00445-3 Cost-Saving Approach
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
understanding GI bleeding
 understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D.
 Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
SIGN. Management of acute upper and lower gastrointestinal bleeding. September 2008. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
New Anticoagulants and GI bleeding
 New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial
 Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding
 Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Management by the intensivist of gastrointestinal bleeding in adults and children
 Osman et al. Annals of Intensive Care 2012, 2:46 REVIEW Open Access Management by the intensivist of gastrointestinal bleeding in adults and children David Osman 1*, Michel Djibré 2, Daniel Da Silva 3,
Osman et al. Annals of Intensive Care 2012, 2:46 REVIEW Open Access Management by the intensivist of gastrointestinal bleeding in adults and children David Osman 1*, Michel Djibré 2, Daniel Da Silva 3,
Lower Gastrointestinal Bleeding Author: Burt Cagir, MD, FACS; Chief Editor: Julian Katz, MD
 Lower Gastrointestinal Bleeding Author: Burt Cagir, MD, FACS; Chief Editor: Julian Katz, MD Reprinted with permission from Emedicine.com New users to emedicine.com will be required to register for free
Lower Gastrointestinal Bleeding Author: Burt Cagir, MD, FACS; Chief Editor: Julian Katz, MD Reprinted with permission from Emedicine.com New users to emedicine.com will be required to register for free
ESD for colorectal lesions I am in favour. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
Acute Gastrointestinal Bleeding
 EMERGENCY MEDICINE BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, PUBLISHER Bruce M. White EXECUTIVE EDITOR Debra Dreger SENIOR EDITOR Bobbie Lewis EDITOR Robert Litchkofski ASSISTANT EDITOR Melissa Frederick
EMERGENCY MEDICINE BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, PUBLISHER Bruce M. White EXECUTIVE EDITOR Debra Dreger SENIOR EDITOR Bobbie Lewis EDITOR Robert Litchkofski ASSISTANT EDITOR Melissa Frederick
TEST QUESTIONS GASTROINTESTINAL BLEEDING
 TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
The Forzani MacPhail Colon Cancer Screening Centre Frequently Asked Questions. What is the Forzani MacPhail Colon Cancer Screening Centre?
 The Forzani MacPhail Colon Cancer Screening Centre Frequently Asked Questions What is the Forzani MacPhail Colon Cancer Screening Centre? The Forzani and MacPhail Colon Cancer Screening Centre (CCSC) is
The Forzani MacPhail Colon Cancer Screening Centre Frequently Asked Questions What is the Forzani MacPhail Colon Cancer Screening Centre? The Forzani and MacPhail Colon Cancer Screening Centre (CCSC) is
HemoClip: Guidelines & Atlas
 HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
Epi procolon The Blood Test for Colorectal Cancer Screening
 Epi procolon The Blood Test for Colorectal Cancer Screening Epi procolon is an approved blood test for colorectal cancer screening. The US Preventive Services Task Force, the American Cancer Society and
Epi procolon The Blood Test for Colorectal Cancer Screening Epi procolon is an approved blood test for colorectal cancer screening. The US Preventive Services Task Force, the American Cancer Society and
Acute Lower Gastrointestinal Bleeding in Crohn s Disease: Characteristics of a Unique Series of 34 Patients
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 94, No. 8, 1999 1999 by Am. Coll. of Gastroenterology ISSN 0002-9270/99/$20.00 Published by Elsevier Science Inc. PII S0002-9270(99)00347-0 Acute Lower Gastrointestinal
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 94, No. 8, 1999 1999 by Am. Coll. of Gastroenterology ISSN 0002-9270/99/$20.00 Published by Elsevier Science Inc. PII S0002-9270(99)00347-0 Acute Lower Gastrointestinal
Flexible sigmoidoscopy the procedure explained Please bring this booklet with you
 Flexible sigmoidoscopy the procedure explained Please bring this booklet with you Exceptional healthcare, personally delivered Introduction You have been advised by your GP or hospital doctor to have an
Flexible sigmoidoscopy the procedure explained Please bring this booklet with you Exceptional healthcare, personally delivered Introduction You have been advised by your GP or hospital doctor to have an
Clinical question: what is the role of colonoscopy in the diagnosis of ischemic colitis?
 Clinical question: what is the role of colonoscopy in the diagnosis of ischemic colitis? Filtered resources,, which appraise the quality of studies and often make recommendations for practice, include
Clinical question: what is the role of colonoscopy in the diagnosis of ischemic colitis? Filtered resources,, which appraise the quality of studies and often make recommendations for practice, include
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
British Society of Gastroenterology. St. Elsewhere's NHS Foundation Trust. National Comparative Audit of Blood Transfusion
 British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood December 2007 St. Elsewhere's NHS Foundation Trust National Comparative Audit of Blood
British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood December 2007 St. Elsewhere's NHS Foundation Trust National Comparative Audit of Blood
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Direct Current Therapy for Treatment of Hemorrhoids
 Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Aktuelle Literatur aus der Notfallmedizin
 05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
Flexible Sigmoidoscopy
 Flexible Sigmoidoscopy National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is flexible sigmoidoscopy? Flexible sigmoidoscopy
Flexible Sigmoidoscopy National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is flexible sigmoidoscopy? Flexible sigmoidoscopy
Appendix G - Identification and Selection of Studies
 FINAL Emergency framework for rationing of blood for massively bleeding patients during a red phase of a Appendix G - Identification and Selection of Studies Inclusion/Exclusion Criteria We included studies
FINAL Emergency framework for rationing of blood for massively bleeding patients during a red phase of a Appendix G - Identification and Selection of Studies Inclusion/Exclusion Criteria We included studies
COLORECTAL CANCER SCREENING
 COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
Treatment of acute lower gastrointestinal hemorrhage by superselective transcatheter embolization. Rahul Sheth, Vimal Someshwar, Gireesh Warawdekar
 Original Article Treatment of acute lower gastrointestinal hemorrhage by superselective transcatheter embolization Rahul Sheth, Vimal Someshwar, Gireesh Warawdekar Lilavati Hospital, Sir H N Hospital and
Original Article Treatment of acute lower gastrointestinal hemorrhage by superselective transcatheter embolization Rahul Sheth, Vimal Someshwar, Gireesh Warawdekar Lilavati Hospital, Sir H N Hospital and
(ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding?
 (ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding? Dennis M. Jensen 1, Robert Stuart 2, Henrik Ahlbom 3, Stefan Eklund 3, Alan Barkun
(ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding? Dennis M. Jensen 1, Robert Stuart 2, Henrik Ahlbom 3, Stefan Eklund 3, Alan Barkun
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE
 STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
Main Effect of Screening for Coronary Artery Disease Using CT
 Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
Colic is one of the most dreaded conditions horse owners and trainers encounter with
 Impaction Colic and Hydration Michele Frazer, DVM, DACVIM, DACVECC Impaction Colic Colic is one of the most dreaded conditions horse owners and trainers encounter with their horses. The term colic, however,
Impaction Colic and Hydration Michele Frazer, DVM, DACVIM, DACVECC Impaction Colic Colic is one of the most dreaded conditions horse owners and trainers encounter with their horses. The term colic, however,
Pediatric Gastroenterology Fellowship Pediatric Nutrition Rotation Goals and Objectives - 1 st Year
 Pediatric Nutrition Rotation Goals and Objectives - 1 st Year Goal 1: Gain experience and competency in managing common and rare gastrointestinal, liver and nutritional problems. (Competencies: patient
Pediatric Nutrition Rotation Goals and Objectives - 1 st Year Goal 1: Gain experience and competency in managing common and rare gastrointestinal, liver and nutritional problems. (Competencies: patient
Summary and general discussion
 Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
GASTRO-INTESTINAL BLEEDING
 Introduction Site of Bleeding History Physical Examination Laboratory Tests Investigation Treatment References Introduction Gastrointestinal bleeding is an uncommon but important sign in paediatric patients.
Introduction Site of Bleeding History Physical Examination Laboratory Tests Investigation Treatment References Introduction Gastrointestinal bleeding is an uncommon but important sign in paediatric patients.
Evidence of Crohn s Disease. Case Presentation
 Witt Wait to Treat tutiled Until Endoscopic Evidence of Crohn s Disease Raymond Cross, MD, MS, AGAF Associate Professor of Medicine Director, IBD Program University of Maryland School of Medicine Co-Director,
Witt Wait to Treat tutiled Until Endoscopic Evidence of Crohn s Disease Raymond Cross, MD, MS, AGAF Associate Professor of Medicine Director, IBD Program University of Maryland School of Medicine Co-Director,
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department!
 Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Patients who fail to bring a driver/someone to stay with them for the night will have their procedure cancelled immediately.
 Preparing for your Colonoscopy You must have someone and/or a driver accompany you and stay with you for 24 hours after your procedure. Patients who fail to bring a driver/someone to stay with them for
Preparing for your Colonoscopy You must have someone and/or a driver accompany you and stay with you for 24 hours after your procedure. Patients who fail to bring a driver/someone to stay with them for
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
American Journal of Gastroenterology ISSN 0002-9270
 American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
Lower gastrointestinal bleeding in the elderly
 Online Submissions: http://www.wjgnet.com/1948-5190office wjge@wjgnet.com doi:10.4253/wjge.v2.i5.147 World J Gastrointest Endosc 2010 May 16; 2(5): 147-154 ISSN 1948-5190 (online) 2010 Baishideng. All
Online Submissions: http://www.wjgnet.com/1948-5190office wjge@wjgnet.com doi:10.4253/wjge.v2.i5.147 World J Gastrointest Endosc 2010 May 16; 2(5): 147-154 ISSN 1948-5190 (online) 2010 Baishideng. All
Gastrointestinal (GI) bleeding is one of the major causes of morbidity
 Diagn Interv Radiol 2011; 17:368 373 Turkish Society of Radiology 2011 INTERVENTIONAL RADIOLOGY ORIGINAL ARTICLE Mesenteric angiography of patients with gastrointestinal tract hemorrhages: a single center
Diagn Interv Radiol 2011; 17:368 373 Turkish Society of Radiology 2011 INTERVENTIONAL RADIOLOGY ORIGINAL ARTICLE Mesenteric angiography of patients with gastrointestinal tract hemorrhages: a single center
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
LOWER GI ENDOSCOPIES So why is CMS yanking our chain? General Concepts for all GI Endoscopy Procedures
 LOWER GI ENDOSCOPIES We have lots of changes to lower GI coding for 2015 to talk about. Code definitions have been revised and many new codes have been added to this chapter. First the good news: All these
LOWER GI ENDOSCOPIES We have lots of changes to lower GI coding for 2015 to talk about. Code definitions have been revised and many new codes have been added to this chapter. First the good news: All these
Chronic Gastrointestinal Bleeding of Obscure Origin: Diagnosis and Management
 Clinical Review Article Chronic Gastrointestinal Bleeding of Obscure Origin: Diagnosis and Management Arif Nawaz, MD Ahmed Shehata, MD Imtiaz Mohamed, MD Carylann Hadjiyane, MD, FACG Ali S. Karakurum,
Clinical Review Article Chronic Gastrointestinal Bleeding of Obscure Origin: Diagnosis and Management Arif Nawaz, MD Ahmed Shehata, MD Imtiaz Mohamed, MD Carylann Hadjiyane, MD, FACG Ali S. Karakurum,
2016 Quick Reference Coding Chart
 43197 Trans nasal esophagoscopy 43198 Biospy Trans Nasal Esophagoscopy Esophagoscopy 43200 Esophagoscopy Includes collection of specimen(s) by brushing or washing, when performed. 43201 Submucosal injection
43197 Trans nasal esophagoscopy 43198 Biospy Trans Nasal Esophagoscopy Esophagoscopy 43200 Esophagoscopy Includes collection of specimen(s) by brushing or washing, when performed. 43201 Submucosal injection
GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo
 GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo Educational Purpose: The Hepatology Rotation introduces the fellow to the management of outpatients and inpatients
GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo Educational Purpose: The Hepatology Rotation introduces the fellow to the management of outpatients and inpatients
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI)
 Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
CERTIFICATE OF NEED AND ACUTE CARE LICENSURE PROGRAM. Hospital Licensing Standards: Emergency Department and Trauma Services:
 HEALTH AND SENIOR SERVICES HEALTH CARE QUALITY AND OVERSIGHT BRANCH HEALTH CARE QUALITY AND OVERSIGHT DIVISION ACUTE CARE FACILITY OVERSIGHT CERTIFICATE OF NEED AND ACUTE CARE LICENSURE PROGRAM Hospital
HEALTH AND SENIOR SERVICES HEALTH CARE QUALITY AND OVERSIGHT BRANCH HEALTH CARE QUALITY AND OVERSIGHT DIVISION ACUTE CARE FACILITY OVERSIGHT CERTIFICATE OF NEED AND ACUTE CARE LICENSURE PROGRAM Hospital
Please read the instructions 6 days before your colonoscopy.
 979-776-8440 Please read the instructions 6 days before your colonoscopy. COLONOSCOPY MIRALAX PREP SIX DAYS BEFORE THE COLONOSCOPY - Stop iron medications 6 days before your colonoscopy. - Stop taking
979-776-8440 Please read the instructions 6 days before your colonoscopy. COLONOSCOPY MIRALAX PREP SIX DAYS BEFORE THE COLONOSCOPY - Stop iron medications 6 days before your colonoscopy. - Stop taking
1/12/2016. What s in a name? What s in a name? NO.Anti-Coagulation. DOACs in clinical practice. Practical aspects of using
 What s in a name? Practical aspects of using DOACs (Direct Oral Anticoagulants) James L. Sebastian, MD, MACP Professor of Medicine (GIM) Medical College of Wisconsin February 5, 2016 DOAC NOAC NOAC ODI
What s in a name? Practical aspects of using DOACs (Direct Oral Anticoagulants) James L. Sebastian, MD, MACP Professor of Medicine (GIM) Medical College of Wisconsin February 5, 2016 DOAC NOAC NOAC ODI
Dual Antiplatelet Therapy. Stephen Monroe, MD FACC Chattanooga Heart Institute
 Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy
 Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy Judith Long, MD,RWJCS Perelman School of Medicine Philadelphia Veteran Affairs Medical Center Background Objective Overview Methods
Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy Judith Long, MD,RWJCS Perelman School of Medicine Philadelphia Veteran Affairs Medical Center Background Objective Overview Methods
Duration of Dual Antiplatelet Therapy After Coronary Stenting
 Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
MU Inpatient Consult Rotation
 MU Inpatient Consult Rotation I. Description of Rotation and Educational Goal: This is a four-week rotation in which GI fellows gain exposure and acquire expertise in the evaluation and management of adult
MU Inpatient Consult Rotation I. Description of Rotation and Educational Goal: This is a four-week rotation in which GI fellows gain exposure and acquire expertise in the evaluation and management of adult
Articles Presented. Journal Presentation. Dr Albert Lo. Dr Albert Lo
 * This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
* This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
AHS s Headache Coding Corner A user-friendly guide to CPT and ICD coding
 AHS s Headache Coding Corner A user-friendly guide to CPT and ICD coding Stuart Black, MD Part 3 - Medical Decision Making (MDM) coding in Headache As stated in the CPT codebook, the classification of
AHS s Headache Coding Corner A user-friendly guide to CPT and ICD coding Stuart Black, MD Part 3 - Medical Decision Making (MDM) coding in Headache As stated in the CPT codebook, the classification of
Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points
 372 Gut 2001;49:372 379 Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points G M Hawkey, A T Cole, A S McIntyre, R G Long, C J Hawkey Division of Gastroenterology,
372 Gut 2001;49:372 379 Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points G M Hawkey, A T Cole, A S McIntyre, R G Long, C J Hawkey Division of Gastroenterology,
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl
 NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl Mikele Wissing, RN June 2014 Introduction until recently, was the unrivaled medication for treatment
NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl Mikele Wissing, RN June 2014 Introduction until recently, was the unrivaled medication for treatment
in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a
 AMP particles - absorbable polysaccharide hemostat in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a prospective, randomized
AMP particles - absorbable polysaccharide hemostat in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a prospective, randomized
Diagnosis and treatment of patients with gastrointestinal bleeding
 Current Anaesthesia & Critical Care (2004) 15, 123 132 ARTICLE IN PRESS www.elsevier.com/locate/cacc MEDICAL Diagnosis and treatment of patients with gastrointestinal bleeding C. Meaden, A.J. Makin* UK
Current Anaesthesia & Critical Care (2004) 15, 123 132 ARTICLE IN PRESS www.elsevier.com/locate/cacc MEDICAL Diagnosis and treatment of patients with gastrointestinal bleeding C. Meaden, A.J. Makin* UK
Post-DDW OAG Course - Therapeutic Endoscopy
 Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto moskoj@smh.ca Program Name: Post-DDW OAG course CanMEDS
Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto moskoj@smh.ca Program Name: Post-DDW OAG course CanMEDS
Damage Control in Abdominal Trauma
 Damage Control in Abdominal Trauma Steven Stylianos, MD Surgeon-in-Chief, Morgan Stanley Children s Hospital Rudolph Schullinger Professor of Surgery, Columbia University College of Physicians & Surgeons
Damage Control in Abdominal Trauma Steven Stylianos, MD Surgeon-in-Chief, Morgan Stanley Children s Hospital Rudolph Schullinger Professor of Surgery, Columbia University College of Physicians & Surgeons
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16
 Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Ulcerative colitis patients with low grade dysplasia should undergo frequent surveillance colonoscopies
 Ulcerative colitis patients with low grade dysplasia should undergo frequent surveillance colonoscopies David T. Rubin, MD, FACG, AGAF Associate Professor of Medicine Co-Director, Inflammatory Bowel Disease
Ulcerative colitis patients with low grade dysplasia should undergo frequent surveillance colonoscopies David T. Rubin, MD, FACG, AGAF Associate Professor of Medicine Co-Director, Inflammatory Bowel Disease
Results of streamlined regional ambulance transport and subsequent treatment of acute abdominal aortic aneurysm
 CHAPTER 6 Results of streamlined regional ambulance transport and subsequent treatment of acute abdominal aortic aneurysm JW Haveman, A Karliczek, ELG Verhoeven, IFJ Tielliu, R de Vos, JH Zwaveling, JJAM
CHAPTER 6 Results of streamlined regional ambulance transport and subsequent treatment of acute abdominal aortic aneurysm JW Haveman, A Karliczek, ELG Verhoeven, IFJ Tielliu, R de Vos, JH Zwaveling, JJAM
Rob Enns University of British Columbia, Vancouver. Grigorios Leontiadis McMaster University, Hamilton
 Rob Enns University of British Columbia, Vancouver Grigorios Leontiadis McMaster University, Hamilton Accreditation This event has been approved as an accredited (Section1) group learning activity as defined
Rob Enns University of British Columbia, Vancouver Grigorios Leontiadis McMaster University, Hamilton Accreditation This event has been approved as an accredited (Section1) group learning activity as defined
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
