Message from The President
|
|
|
- Julie Flynn
- 10 years ago
- Views:
Transcription
1 Issue 01 Volume 01 January 2013 Official e-newsletter of Indian Academy of Pediatrics ISSN No: Editorial Board Chief Advisors CP Bansal Piyush Gupta Sailesh Gupta Editor-in-chief Praveen Kumar Co-editors: Dheeraj Shah Deepak Bansal Sriram Krishnamurthy Jaydeep Choudhury Rhishikesh Thakre National Advisors Rohit Agrawal Vijay N Yewale TU Sukumaran Deepak Ugra Panna Choudhury AK Patwari Apurba Ghosh NK Subramanya AK Rawat Advisory EB Board CM Chhajer (East) Digant Shastri (West) RK Gupta (North) NK Kalappanavar (South) SS Rawat (Central) International Advisors Sergio Augusto Cabral Andreas Constantopoulos Zulfiqar Bhutta William Keenan Official Sponsor for 2013: Eris Montana A Division of Eris Life Sciences Message from The President Many, many congratulations on our brand new initiative Child India, an e- Newsletter which I believe will act as a phenomenal awakening and will continually serve as a very powerful impetus for us in our quest to make our nation a much safer abode for children. This e-newsletter will be a spellbinding source of knowledge and a very easy way to update oneself. It will feature everything from review articles to case reports, an extremely informative images section, and a separate section that will have answers to the frequent queries by the readers. This initiative will be of interest and use for post graduate students as well as private practitioners, and importantly fills a large void. I am sure it is a step with huge potential and a beautiful intention. Your suggestions and inputs are more than welcome. The strength and unity of an organization reflects in each member and we wish to make ours the best. This is just the beginning; we wish to take this journal and IAP to much greater heights and hope you all will benefit from it and contribute to it. I must congratulate IAP National Publishing House, Gwalior for their wonderful work. My sincere thanks and congratulations to Dr Praveen Kumar and the entire editorial board to make my dream come true. Dr. CP Bansal, President, IAP-2013 Dear friends, From the Desk of Editor-In-Chief With the advancement in Information Technology, electronic media are slowly becoming the most popular way to spread knowledge. Information in digital format is much more accessible in the era of electronic gadgets. We also believe that this format is more interactive as readers can send their feedback much faster. To utilize this advancement, our IAP President Dr. CP Bansal came up with the concept of e- Newsletter Child India. It is indeed a privilege for me to work for our beloved Indian Academy of Pediatrics by serving for Child India. Child India editorial team has planned contents of this issue to reach our private practitioners and post graduate students. We have included review article on MLD, an interesting case report, practice tips, quiz to brush up your memory and opinion poll on an important health issue. There are dedicated pages for our postgraduates. From next issue we also wish to include sections on case based discussion and 'Ask your query'. My sincere thanks are due to Dr Piyush Gupta for guiding me at each step and Co-editors Dheeraj, Deepak, Sriram, Jaydeep and Rhishikesh for their valuable contributions. Thanks to IAP National Publishing team for giving Child India a beautiful real Indian look. My sincere request to all members will be to please read Child India and send us feedback and suggestions at [email protected]. I am sure that your feedback and guidance will help editorial team to meet expectations of our President and members. Praveen Kumar
2 2 Abstract: propionic, isovaleric, etc.), urea cycle defects (UCD), sugar intolerances (galactosemia, hereditary fructose Increasing number of metabolic liver diseases like intolerance {HFI}) and metal intoxication (WD, Neonatal Wilson disease, Galactosemia, Glycogen storage Hematochromatosis {NH}). These conditions do not diseases, Lysosomal storage diseases are being interfere with the intrauterine development and present diagnosed in Institutions with good diagnostic with a symptom-free interval before clinical signs of facilities. However this is likely that many cases are 'intoxication' appear, which may be acute (vomiting, missed due to lack of awareness and lack of coma, liver failure, thromboembolic complications) or diagnostic facilities. There are scanty literatures on chronic (failure to thrive, developmental delay, ectopia this aspect from India. In this review attempt has been lentis, cardiomyopathy). Circumstances that can provoke made to discuss different clinical presentation of acute metabolic attacks include catabolism, fever, metabolic liver disease. This review also includes intercurrent illness and food intake. Most of these protocol based approach to various presentations disorders are treatable and require emergency removal of which will help in selecting appropriate investigations the toxin by special diets, extracorporeal procedures, for a specific presentation. cleansing drugs or vitamins [9, 10]. Key Words: liver transplant, liver failure, Wilson 2. Inborn errors of intermediary metabolism with disease, galactosemia INTRODUCTION: symptoms due at least partly to a deficiency in energy production or utilization within liver, myocardium, muscle, brain or other tissues. This group can be divided into the more severe mitochondrial, and the less severe Inborn errors of metabolism, where hepatomegaly and/ or cytoplasmic energy defects. The mitochondrial energy abnormal liver function form part of the clinical disease, are defects encompass the congenital lactic acidemias, collectively referred to as Metabolic liver disease (MLD). respiratory chain disorders, pyruvate oxidation defects Diagnosis is often problematic on account of inadequate and fatty acid oxidation defects (FAOD). Cytoplasmic availability of investigations, failure to identify metabolic energy defects include disorders of glycolysis, glycogen defect and lack of definitive diagnostic tests. Dietary metabolism, gluconeogenesis and the pentose phosphate exclusions, antioxidants and chelation therapy with pathways. Some of the mitochondrial disorders and immunoglobulins can offer good outcome in some of the pentose phosphate pathway defects can interfere with the treatable MLDs. Liver transplantation for MLD shows embryofetal development and give rise to dysmorphism, markedly improved outcome [1,2].Various studies have shown dysplasia and malformations. that MLDs like Wilson Disease (WD), Galactosemia, 3. Involvement of cellular organelles: Lysosomal Lysosomal storage disorder (LSD), Glycogen storage disease (Wolman's disease & cholesteryl ester storage disorder), (GSD) are not uncommon in India [4-7]. Other MLDs are also peroxisomal (Zellweger's syndrome), glycosylation being increasingly diagnosed in Institutions with better (congenital defect of glycosylation {CDG}), and diagnostic facilities. A recent study, among survivors of cholesterol synthesis defects belong to this group. Reye's syndrome in Australia (where salicylates are rarely used in children), has revealed that 26% had inherited diseases of fatty acid oxidation or carnitine metabolism [8]. CLINICAL FEATURES: PATHOPHYSIOLOGY: R E V I E W A R T I C L E Metabolic liver disease in Neonates, Infants and children : Clinical profile, diagnostic approach and management Seema Alam Additional Professor (Pediatric Hepatology), Institute of Liver and Biliary Sciences DI Vasant Kunj, New Delhi-70, Phone : (M) (O) (R) [email protected] From the therapeutic view, the MLD can be divided into three groups: 1. Defect in the intermediary metabolic pathway leading to the accumulation of toxic metabolite (formed at the preceding step) which causes liver failure. Example- Tyrosinemia, organic acidemias (methylmalonic, The MLDs can present at any age, from prenatal, neonatal, infancy to adolescence and even adulthood. The time of presentation coincides with the time of maximum catabolism e.g. neonatal age, at the time of infections, puberty and pregnancy. The diagnosis is often delayed as the symptoms may be intermittent, and in the period between episodes of decompensation, the patient may be free of clinical or biochemical abnormalities. Clinical features that should arouse the suspicion of MLD are depicted in Box-1. History of
3 3 Box 1: Clinical Profile Suggestive of Metabolic Liver Disease Recurrence of the clinical presentation in times of catabolic stress Recurrent vomiting, diarrhea, failure to thrive, short stature, dysmorphic features, edema. Specific food avoidance: Sweet food avoided in hereditary fructose intolerance (HFI) and high protein diet in urea cycle defects. Jaundice, hepatosplenomegaly and hepatic failure, hypoglycemia, lactic acidemia, hyperammonemia and coagulopathy. Developmental delay, hypotonia and seizures, cataract, unusual odors, rickets, and renal tubulopathy. Very few males in the family: x-linked disorder Suggestive family history: Fatty liver of pregnancy and HELLP (Hemolysis, elevated liver enzymes and low platelet) in the mother, consanguinity, miscarriages, neonatal deaths, sudden infant death syndrome (SIDS) and psychiatric illnesses. primary lactic acidemia associated with milder liver dysfunction 3. Cholestatic liver disease. 4. Organomegaly: Hepatomegaly or hepatosplenomegaly 5. Cirrhosis with or without portal hypertension PHYSICAL SIGNS: The age of presentation in a sick neonate, infant or child helps in pinpointing the etiology (Table I). A newborn presenting with liver failure within a week from birth could be NH. HFI is related to introduction of sucrose or fructose to the diet [13] or even syrups of medications with associated episodes of diarrhea and vomiting. WD is more common in the 5-15 years age group, 17% of which may present as fulminant hepatic failure [14]. The various common presentations of a MLD before and at birth are depicted in Table II. Hydrops fetalis can be more commonly seen in NH, Wolman's disease and CDG [15]. Encephalopathy is difficult to diagnose in children and could be the only physical sign in case of UCD, organic acidemias and other primary lactic acidemias. Some UCD defects can cause acute liver failure [16]. Characteristic dysmorphic features in CDG are inverted, hypoplastic and widely spaced nipples, abnormal fat pads, orange peel skin and mild facial dysmorphisms including large ears, high forehead and thin upper lip. It is a multisystem disease and can present with a wide range of systemic manifestations like cardiomyopathy, pericardial effusion, failure to thrive, liver acute fatty liver of pregnancy or hemolysis, elevated liver enzymes and low platelets in the mother is associated with a possibility of long-chain hydroxyl acyl-coa dehydrogenase disease, nephritic syndrome and coagulation disorders [17]. deficiency (LCHAD) in the fetus [11]. Mental retardation, cardiomyopathy, renal tubulopathy in a The presentations of an MLD in an infant or child can be varied hypotonic child with convulsive disorder with or without and may be categorized in the following five presentations: treatment with valproic acid could be a setting for pediatric acute liver failure (PALF) related to mitochondrial disorders. 1. Pediatric acute liver failure (PALF): defined as acute liver injury with coagulopathy with or without encephalopathy [12]. 2. Encephalopathy due to hyperammonemia and/or Table I: Common Metabolic Liver Diseases (MLDs) in Neonates, Infants and Children. The first sign of cholestasis usually appear before 3 months of age and tend to appear earlier in PFIC2 than in PFIC1. No clear-cut difference in jaundice evolution pattern, Neonates Pediatric acute liver failure and acute decompensation of chronic liver disease Neonatal hemochromatosis, Galactosemia, Tyrosinemia type 1, Mitochondrial cytopathy and Wolman's disease Encephalopathy with liver dysfunction Organic acidemias, FAOD, gluconeogenetic disorders, mitochondrial cytopathies and UCD Infants Tyrosinemia type I, FAOD, Mitochondrial cytopathy, Galactosemia, Hereditary fructose intolerance, UCD and Congenital disorders of glycosyllation Organic acidemias, FAOD, gluconeogenetic disorders, UCD, Congenital disorders of glycosylation and mitochondrial cytopathies Children Wilson's disease, FAOD, mitochondrial cytopathy, hereditary fructose intolerance, UCD and Congenital disorders of glycosylation UCD, FAOD, Congenital disorders of glycosylation, gluconeogenetic disorders and mitochondrial cytopathies
4 4 Table II : Various Presentations of different Metabolic Liver Disease before and/at birth. Ascites / Hydrops fetalis Dysmorphism Encephalopathy or Seizure and Apnea Hypotonia Neonatal hemochromatosis Peroxisomal biogenesis disorders Peroxisomal biogenesis disorders Peroxisomal biogenesis disorders Lysosomal disorders Lysosomal disorders Urea cycle defect Congenital defect of N-glycosylation Congenital defect of N- glycosylation Congenital defect of N- glycosylation Congenital lactic acidemia Congenital lactic acidemia Glycogen storage disease type IV Disorders of cholesterol synthesis Organic acidemia development of pruritus, hepatomegaly, or splenomegaly, is seen between PFIC1 and PFIC2. More than half of the PFIC1 patients present with extrahepatic symptoms during disease evolution, such as diarrhea, pancreatitis and deafness. PFIC2 patients are notable for the early presence of signs of fat soluble vitamin deficiencies, including rickets or bleeding, and for cholelithiasis that would be present in one third of children [18]. A MDR3 (PFIC3) defect is also likely to be involved in some cases of transient neonatal cholestasis and adult idiopathic cirrhosis [19]. A cholestatic child or adult without pruritis could be bile acid synthetic defect. Majority of cystic fibrosis presents with biliary cirrhosis in second decade of life while just over 1% may present as neonatal cholestasis, where repeated pneumonia can guide to the diagnosis. Children presenting with only hepatomegaly could be glycogen storage disorder and cholesterol storage disorder. Presence of dolls like face, renal rickets and growth failure would be more prominent in GSD type 1 then type 3. Majority present in infancy but GSD type 1 could even present in neonatal period. Liver symptoms may disappear with puberty in GSD type 3. If splenomegaly is prominently present in an infant with liver dysfunction, then lipid storage (Niemann- Pick disease, Gauchers) or lysosomal disorders (Wolman disease) are more likely. History of prolonged neonatal jaundice and subsequent progressive neurological manifestations like vertical gaze palsy, delayed speech, ataxia, uncontrolled seizures and gelastic cataplexy are suggestive of Niemann- Pick disease, type C. Cherry red spot on fundal examination would be suggestive of Niemann- Pick disease and Gauchers disease. Juvenile Hemochromatosis is characterized by severe iron overload usually associated with liver damage, cardiomyopathy and/or hypogonadotrophic hypogonadism. Table III depicts the list of clinical pointers to various MLDs. DIAGNOSTIC APPROACH: The diagnostic approach should be based upon the mode of presentation. Differentiation on the basis of physical signs, laboratory workup, and confirmatory tests would make the approach easier [20].Approach to children with different presentations are depicted in Figure1-5. LABORATORY WORK UP: Tests for synthetic function (prothrombin time and serum albumin) are disproportionately more affected than the transaminases and bilirubin in MLD. Hence, even in a setting of normal to slightly raised transaminases and bilirubin, disproportionate coagulopathy and hypoproteinemia should raise the suspicion of MLD. Initial screening with fasting blood sugar, blood ammonia, blood gases, and urinary sugars as well as ketones could help in the differential diagnosis of both encephalopathic sick infant and PALF (Figure 1&2). While sending the specimens, it is prudent to mention the feeds, drug or blood transfusions given. Hypoglycemia is a key feature of gluconeogenesis defects accompanied by hepatomegaly and marked lactic acidosis; the latter rapidly resolving with dextrose administration is another important diagnostic clue. In gluconeogenesis disorders, both hypoglycemia and lactic acidosis may be intermittently present in the fasting state e.g. glycogen storage disorder. Persistent and severe hypoglycemia should indicate the differential diagnosis of galactosemia, tyrosinemia, HFI, FAOD, organic acidemia, and CDG. Hyperammonemia is prominent in FAOD and organic academia whereas galactosemia, HFI and CDG would more commonly present with liver failure. Presence of gram negative sepsis would indicate galactosemia [21]. HFI should be suspected if there is hypoglycemia with positive non glucose reducing substance in urine. Oral fructose tolerance test reveals worsening of hypoglycemia with increasing serum uric acid and magnesium associated with hypophosphatemia [22]. Either hypoglycaemia or hyperglycaemia may be seen in organic acidemias.
5 5 Table III : Clinical pointers to various metabolic liver diseases Clinical Features Hemolytic DCT negative anemia Cataract, overwhelming gram negative sepsis Hydrops fetalis Cardiomyopathy and skeletal muscle involvement Adrenal calcifications on imaging Hypotonia, convulsions, strabismus, protein losing enteropathy, inverted nipples and abnormal distribution of fat. Presentation by 24 hrs with irritability, poor feeding followed by coma Node-like appearance of fragile hair, which usually responds to arginine supplementation (Trichorrhexis nodosa) X-linked disorder Episodic symptoms, cyclic vomiting Floppy, abnormal facies, optic atrophy Metabolic Liver Disease Wilson's disease Galactosemia NH, CDG, Lysosomal disorders LCHAD, Systemic carnitine deficiency Wolman's disease Congenital disorders of glycosylation (CDG) Urea cycle defects (UCD) Arginosuccinic lyase deficiency Ornithine transcarbamylase deficiency UCD, organic acidemias, FAOD Peroxisomal disorders Blood gas analysis may reveal respiratory alkalosis due to respiratory stimulation by hyerammonemia. Intermittent fasting hypoglycaemia with elevated lactates would suggest GSD. Metabolic acidosis is frequently present in a sick child, but if associated with hypoglycemia, absence of urinary ketones and the normal anion gap, it suggests possibility of FAOD. Ketosis in a similar setting would suggest mitochondrial cytopathies or organic acidemias. Ketosis is a common accompaniment of acidosis, although in the neonate, marked ketosis is unusual and may indicate an organic acidemia. Galactosemia, tyrosinemia type 1 and HFI can all be associated with renal tubular acidosis. The clinical presentation of acute liver failure, hemolysis (anemia, reticulocytosis, low haptoglobin and high LDH levels) and low ceruloplasmin should prompt investigative work up for WD. HISTOPATHOLOGY: Bone-morrow examination can reveal presence of storage cells suggestive for Gaucher's or Niemann-Pick disease. Liver biopsy done during infancy usually shows no or mild portal and lobular fibrosis, no necrosis, and no or few giant transformation of hepatocytes in PFIC1 patients. Presence of numerous giant cell transformations of hepatocytes is more often seen in PFIC2. BASD should be suspected in cases with severe cholestasis and giant cell transformation especially in the presence of serum bile acids <0.5mmol/L. Liver biopsy in GSD shows uniform distension of hepatocytes with glycogen & lipid vacuoles with no fibrosis except in GSD type III and IV. The deposits are PAS positive and diastase sensitive. RADIOIMAGING: The MRI (T2 weighted) demonstrates attenuated signal (dark) from the liver and pancreas relative to the spleen, indicating increased iron content which is pathognomic of NH. Adrenal calcifications on x-ray abdomen or ultrasonography would indicate Wolman's disease. MRI study can be suggestive of undermyelination in Niemann- Pick disease and Gauchers disease. CONFIRMATORY TESTS: If a neonate presents with acute liver failure (ALF) at birth then high serum ferritin levels (>3500µmol/L) [13] and iron deposits on buccal biopsy would be confirmatory for NH. If a child has hypoglycemia and urinary nonglucose reducing sugar (NGRS) positive, then low or absent galactose transferase in blood and mutations [23] would confirm the diagnosis. Sometimes a normal galactose 1 phosphate uridyl transferase (GALT) levels may confuse the picture. In such a scenario either false negative tests due to blood transfusions or epimerase deficiency should be considered [24]. If alfafetoprotein is disproportionately high, elevated urinary succinyl acetone test would clinch the diagnosis of tyrosinemia type 1. WD diagnosis should be established with serum ceruloplasmin, KF ring and 24hrs Urinary copper estimation [25]. HFI can be confirmed by fructo-aldolase enzyme assay
6 6 Fig 1: Approach to a Child with Encephalopathy Fig 4: Approach to a child with Organomegaly Protocol 1 Ammonia FBS, urine sugar ABG, Ketones Enegy deficient presents immediately after birth toxic variety presents after a gap Child with encephalopathy or Reye s syndrome or cyclic vomitings Hyperammonemia No Yes MA or Lactate incr? Yes Hypoglycemia? Urea cycle defects Yes No No FAOD Yes Gluconeogenetic Ketonemia Complete enzyme deficiency presents earlier in neonatal agegroup MA or Lactate incr? Hypoglycemia? Yes No Mitochondrial energy defects Mitochondrial disorders Organic acidemias Protocol 4 Present Hepatomegaly Hypoglycemia Elevated lactate Urine NGRS Absent GSD Types 1 / 3 Present HFI Absent Child with organomegaly with suspected MLD Wilson disease CESD Alpha-l AT def Liver biopsy with specific enzyme estimation Hepatosplenomegaly Bone marrow aspiration & Bx Niemann Pick type C Gaucher s ds CFSD GSD Type 1 / 3 present in older infants Rest may present at any age Fig 2: Approach to Pediatric Acute Liver failure (PALF) Fig 5: Approach to a child with Cirrhosis Protocol 2 FBS, urine sugar AFP ABG, Ketones A F P Utinary succinyl acelone Tyrosinemia type I GALT PALF Radioimaging High Ammonia & Plasma amino acids Acylcannitine & carnitine Hypoglycemia+ Iactate Non glucose reducing sugar in urine Galactosemia NH & Wolman s presents within few, wks of life Neimann Pick C Wolman s disease Urea cycle defects FAOD MITOCHONDROPATHY High ferritin & buccal blopsy Fructose tolerance test Heriditary Fructose Intolerance Galactosemia & Tyrosinemia within months Neonatal Hemochromatosis Protocol 5 Absent Hypoglycemia GSD Types 4 Present Present HFI Cirrhotic Child with suspected MLD Elevated lactate Absent Wilson disease Gaucher s ds Juvenile hemochromatosis Alpha-I AT def Porphyria Liver biopsy with copper estimation, Perl s & PAS-Diastase stain, enzyme estimation ± Portal HTN (Splenomegaly, vx, collaterals) GSD Type 4 usually presents as older infant Rest may present at any age Bone marrow Ferritin Alpha-1 AT phenotype Urine porphobilinogens Fig 3: Approach to Cholestatic infant or child Protocol 3 Normal / Low PIFC 1 / 2 GGT Yes High PIFC 3 Cholestaic child with suspected MLD Pruritus Liver biopsy with immuno histochemistry, Electron microscopy No Low BASD PFIC 3 presents at any age Rest present as infantile cholestasis GGT Normal / High Galactosemia Tyrosinemia Cystic fibrosis Citrullinemia Hyperam onemia Plasma aminoacids Low urea Sweat Chloride test and the mutations on genetic analysis [26]. Skeletal muscle and more recently buccal biopsies can confirm the diagnosis of mitochondrial cytopathy [27]. Very low urea level may suggest UCD. Abnormal urinary organic acids and plasma acylcarnitine profile would confirm either FAOD or organic acidemia. As of now the immunohistochemistry for BSEP (PFIC type 2) and MDR3 (PFIC type 3) would be confirmatory along with the genetic analysis but both are not freely available. In BASD, specific diagnosis can be made by analysis of body fluids (bile, blood, and urine) using fast atom bombardment-mass spectroscopy and gas chromatographymass spectroscopy. Lysosomal enzyme study from leucocytes carried out for â-glucosidase and acid-sphingomyelinase would be confirmatory for Gauchers and Niemann-Pick disease type A or B. Skin fibroblast for demonstration of unesterified cholesterol accumulation in cultured cells by filipin staining method, which is the characteristic of Niemann- Pick disease type C. GSD-Ia is confirmed by a liver biopsy and enzyme assay or, more recently, by mutation
7 7 analysis. The definitive diagnosis of GSD-III is made by demonstrating enzyme deficiency in the liver or muscle and also in other tissues, such as the heart, erythrocytes and cultured fibroblasts [28]. POST MORTEM DIAGNOSIS: It is important to remember that enzymes degrade rapidly secondary to autolysis post death and therefore useful interpretation of samples taken some hours after death is impossible. One would therefore recommend that muscle and liver biopsies, if indicated, are snap frozen in liquid nitrogen within an hour of death. Skin biopsies can be taken up to 48 h after death. SUPPORTIVE AND SPECIFIC MANAGEMENT: Apart from the standard management of encephalopathy and PALF, management of the suspected case of MLD would be largely supportive till diagnosis is established. Hyperammonemia, hypoglycemia, acid base imbalance, electrolyte imbalance and coagulopathy should be corrected. Appropiate antibiotics for sepsis would be needed in some cases like galactosemia where gram negative sepsis is commonly associated. Exclude lactose, fat, and protein from the diet for hours till a diagnosis is established. Lactose free formula could be added in galactosemia while awaiting the GALT report. The main aim of treatment is to stop further decompensation and the accumulation of potentially toxic metabolites and therefore feeds are stopped; but same time anabolism must be promoted to avoid further catabolic breakdown of body stores that further add to the toxicity. IV infusion of 10% dextrose as a basic fluid with required electrolyte additives is appropriate for most cases. The exception is congenital lactic acidosis and mitochondrial disorders where a 5% dextrose-based solution is used as high carbohydrate supply may exacerbate the lactic acidosis. If FAOD has been excluded, then intralipid should be added at 1 g/kg/day to boost calories. Restriction of protein to g per kg per day (half in form of essential amino acids) is line of management for UCD. is preferred. Ursodeoxycholic acid is the only treatment available for PFIC and BASD. Biliary diversions can decrease the pruritus in PFIC type 2. Wilson's disease should be managed with copper chelating agents and zinc titrating to the need and side effects. The mainstay of treatment in GSD is to prevent hypoglycemia either by continuously providing a dietary supply of glucose, or by frequent ingestion of cornstarch during day and night or nocturnal intragastric feeding. This is achievedin GSD-I by frequent meals high in carbohydrates and cornstarch supplements alone or with gastric tube feedings. For patients with myopathy, in addition to management of hypoglycemia, a high protein diet is recommended. Only effective therapeutic approach presently available for GSD-IV patients with progressive liver disease is liver transplantation. Liver transplantation may be helpful not only for liver disease but also for muscular involvement. LIVER TRANSPLANTATION: Liver transplantation is often the last resort in all MLDs. Studies have shown that there is a higher graft and overall survival in a liver transplant undertaken in metabolic liver disease as compared to non metabolic liver disease [1, 2]. Hepatocyte transplantation is moderately successful for liverbased metabolic disease and acute liver failure as a bridge to liver transplantation [30]. Genetic counselling is important for parents who have a child with a metabolic liver disease. Depending on the mode of inheritance of the disorder, x- linked or autosomal (recessive or dominant), the possibility of the next child being affected can be discussed. CONCLUSION: MLD is not a rare etiology and should be suspected specially in a case with relevant family history and clinical profile. Approach to a case with MLD should be protocol based so as to avoid unnecessary investigations and improve morbidity as well as mortality. Treatable etiologies should be prioritised. Liver transplantation has improved the outcome of MLD markedly. Spironolactone (3 mg/kg/day), fluid restriction and albumin REFERENCES: (1g/kg) would help reduce retention of fluid. Cocktail 1. Arnon R, Kerkar N, Davis MK, Anand R, Yin W, González-Peralta RP; administration in NH with N acetylcysteine, selenium, vitamin SPLIT Research Group. Liver transplantation in children with metabolic E supplements and chelation are not very effective and diseases: the studies of pediatric liver transplantation experience. Pediatr treatment of choice would be liver transplantation [29]. Early Transplant. 2010; 14(6): referral to a tertiary care centre is essential to increase survival 2. Stevenson T, Millan MT, Wayman K, Berquist WE, Sarwal M, Johnston of these children with NH. In the urea cycle defects, sodium EE, et al. Long-term outcome following pediatric liver transplantation benzoate and sodium phenylbutyrate conjugate with glycine for metabolic disorders. Pediatr Transplant. 2010; 14(2): and glutamine, respectively, allowing them to be directly 3. Eghtesad B, Nezakatgoo N, Geraci LC, Jabbour N, Irish WD, Marsh W, et al. Liver transplantation for Wilson's disease: a single center excreted via the kidney. Carnitine is used in the case of organic experience. Liver Transpl Surg. 1999; 5: acidemias to conjugate with the organic acid increasing 4. Arora NK, Arora S, Ahuja A, Mathur P, Maheshwari M, Das MK, et al. solubility and therefore renal clearance. Continuous Alpha 1 antitrypsin deficiency in children with chronic liver disease in venovenous haemofiltration is preferred to remove the toxic North India. Indian Pediatr. 2010; 47(12): metabolites. In neonates weighing <2.5 kg, peritoneal dialysis 5. Poddar U, Thapa BR, Das A, Bhattacharya A, Rao KL, Singh K.
8 8 Neonatal cholestasis: differentiation of biliary atresia from neonatal Hollander, S M Willems, et al. Congenital disorder of glycosylation type hepatitis in a developing country. Acta Paediatr. 2009; 98(8): Ia presenting with hydrops fetalis. J Med Genet 2007; 44: Shah I, Bhatnagar S. Clinical profile of chronic hepatobiliary disorders 18. Davit-Spraul A, Fabre M, Branchereau S, Baussan C, Gonzales E,,et al. in children: experience from tertiary referral centre in Western India. ATP8B1 and ABCB11 analysis in 62 children with normal gamma- Trop Gastroenterol. 2010; 31 (2): glutamyl transferase progressive familial intrahepatic cholestasis 7. Verma IC. Burden of genetic disorders in India. Indian J Pediatr. 2000; (PFIC): phenotypic differences between PFIC1 and PFIC2 and natural 67(12): history. Hepatology. 2010; 51(5): Orlowski JP. Whatever happened to Reye's syndrome? Did it ever really 19. Davit-Spraul A, Gonzales E, Baussan C, Jacquemin E. Progressive exist? Crit Care Med 1999; 27: familial intrahepatic cholestasis. Orphanet J Rare Dis ;4:1 9. Boles RG, Buck EA, Blitzer MG, Platt MS, Cowan TM, Martin SK, et al. 20. Squires RH, Acute liver failure in children. Seminars in liver disease Retrospective biochemical screening of fatty acid oxidation disorders in 2008 ; 28(2): postmortem livers of 418 cases of sudden death in the first year of life. J 21. Rathi N, Rathi A. Galactosemia presenting as recurrent sepsis. J Trop Pediatr 1998; 132: Pediatr. 2011; 57(6): Bonilla S, Prozialeck JD, Malladi P, Pan X, Yu S, Melin-Aldana H, et al. 22. Bouteldja N, Timson DJ. The biochemical basis of hereditary fructose Neonatal iron overload and tissue siderosis due to gestational intolerance. J Inherit Metab Dis. 2010; 33(2): alloimmune liver disease. J Hepatol. 2012; 56(6): , Kaur G, Thapa BR, Prasad R, Kulkarni K. A case of classical 11. Eskelin PM, Laitinen KA, Tyni TA. Elevated hydroxyacylcarnitines in a galactosemia: Identification and characterization of 3 distinct mutations carrier of LCHAD deficiency during acute liver disease of pregnancy - a in galactose-1-phosphate uridyl transferase (GALT) gene in a single common feature of the pregnancy complication? Mol Genet Metab. family. Indian J Pediatr. 2011; 78(7): ; 100 (2): Sarkar M, Bose SS, Mondal G, Chatterjee S. Generalized epimerase 12. Squires RH Jr, Shneider BL, Bucuvalas J, Alonso E, Sokol RJ, deficiency galactosemia. Indian J Pediatr. 2010; 77(8): Narkewicz MR, et al. Acute Liver Failure in Children: The First Roberts EA, Schilsk ML; American Association for Study of Liver Patients in the Pediatric Acute Liver Failure Study Group. J Pediatr. Diseases (AASLD). Diagnosis and treatment of Wilson disease: an 2006; 148(5): update. Hepatolog. 2008; 47(6): Choi HW, Lee YJ, Oh SH, Kim KM, Ryu JM, Lee BH, et al. A Novel 26. Coffee EM, Tolan DR. Mutations in the promoter region of the aldolase Frame shift Mutation of the ALDOB Gene in a Korean Girl Presenting B gene that cause hereditary fructose intolerance. J Inherit Metab Dis. with Recurrent Hepatitis Diagnosed as Hereditary Fructose Intolerance. 2010; 33(6): Gut Liver. 2012; 6(1): Vedrenne V, Galmiche L, Chretien D, de Lonlay P, Munnich A, Rötig A. 14. Jiménez G, Cambronero V, Morales C, Mora A, Guzmán C, Jiménez- Mutation in the mitochondrial translation elongation factor EFTs results Rivera C. Wilson's disease: pediatric experience in Costa Rica. in severe infantile liver failure. J Hepatol. 2012; 56(1): Gastroenterol Hepatol. 2009; 32(4): Ozen H. Glycogen storage diseases: new perspectives. World J 15. Léticée N, Bessières-Grattagliano B, Dupré T, Vuillaumier-Barrot S, de Gastroenterol. 2007; 13(18): Lonlay P, Razavi F, et al. Should PMM2-deficiency (CDG Ia) be searched in every case of unexplained hydrops fetalis? Mol Genet 29. Grabhorn E, Richter A, Burdelski M, Rogiers X, Ganschow R. Neonatal Metab. 2010; 101(2-3): hemochromatosis: long-term experience with favorable outcome. Pediatrics. 2006; 118(5): Mustafa A, Clark JT. Ornithine transcarbamoylase deficiency presenting with acute liver failure. J Inherit Metab Dis. 2006; 29 (4): Hughes RD, Mitry RR, Dhawan. A Current status of hepatocyte transplantation. Transplantation. 2012; 93(4): J M van de Kamp, D J Lefeber, G J G Ruijter, S J Steggerda, N S den Dear IAP members submitted. Image should clearly identify the condition and have the classical characteristics of the clinical condition. Photographs should You will be happy to know that Indian Academy of Pediatrics has started be high quality, high resolution (>300 dpi). The following file types are to publish a bimonthly e-newsletter Child India from January 2013 acceptable: TIFF, and JPEG. A short text of about 150 words under Presidential Action Plan. This e-newsletter will be will be sent to all depicting the condition is needed. No references are needed. the 20,000 members, electronically, free of cost. Child India will contain Review article/symposium on topics relevant to practice of pediatrics in 5. Short write up on recently published International / National the Indian context. It will also feature sections for both Post graduate guidelines related to diagnosis/management of common pediatric students and the Practitioners. Another endeavor of the newsletter will conditions in 250 words, with the link for free download, if any. be to disseminate the important international and national Guidelines related to management of relevant issues in child health. Practitioner Preparation & Submission of the Manuscript section will also include clinical quiz/ images and 'Ask your query'. Manuscript should contain (i) the title of the article; (ii) initials and Editorial board invites papers for following categories surname of each author with the highest academic degree(s) and designation at the time when the work was done; (iii) 1. Review Article: State-of-the-art review articles or name of department(s) and institution(s) to which the work systematic, critical assessments of literature are invited. FOR should be attributed; (iv) disclaimers, if any; (vii) name, The typical length for review articles should be 3000 address, telephone, fax, address of the words (excluding tables, figures, and references). PAPERS corresponding author, (v) declaration on competing Authors submitting review manuscripts should include an interests; and vi) Also, indicate on top the category (i.e. unstructured abstract of up to 200 words describing the Review, Case Report, Images), for which the article is being main findings. Up to 40 references can be included. submitted. Once a manuscript has been accepted for publication, it will undergo editing, typesetting, and reference 2. Case Reports: Clinical cases highlighting uncommon condition or validation by section editors presentation. The text should not exceed 1000 words and should be arranged as introduction, case report and discussion. 3. Reader's Forum: Questions of common interest from members are invited. Editorial board will try to elicit answers from the experts; and publish them, if found suitable. CALL M a n u s c r i p t s s h o u l d b e s u b m i t t e d b y e m a i l t o [email protected] with a copy to [email protected] Editor-in-Chief : Dr Praveen Kumar Section Editors: Dr Dheeraj Shah, Dr Deepak Bansal, 4. Images section: Only clinical photographs with/without Dr Sriram Krishnamurthy, accompanying skiagrams or pathological images should be Dr Jaydeep Choudhury, Dr Rhishikesh Thakre
9 9 Abstract Incomplete form of Pachydermoperiostosis : A rare cause of finger clubbing Pachydermoperiostosis (PDP), the primary form of hypertrophic osteoarthropathy (HOA) is a rare genodermatosis characterized by digital clubbing, arthropathy and periostosis of long tubular bones and pachyderma. The absence of pachyderma defines the incomplete form. We report an 11-year boy who presented with clubbing of fingers/toes since birth and hyperhidrosis. There was no skin thickening, arthritis or cardio-pulmonary disease. Radiographic evidence of acro-osteolysis of distal phalanges/toes and evidence of periosteal new bone formation was present. Wormian bones were seen in each lambdoid suture. The search for a secondary cause remained negative. Although rare, primary HOA without cutaneous involvement as a rare cause of clubbing should be kept in mind. Key Words- Digital clubbing, Hyperhidrosis, Wormian bones INTRODUCTION: Hypertrophic osteoarthropathy (HOA) is a syndrome characterized by clubbing, p e r i o s t o s i s a n d a r t h r i t i s. Pachydermoperiostosis (PDP), the primary form is a rare genodermatosis characterized by pachydermia, digital clubbing and periostosis [1]. We report a child with incomplete form of PDP who had digital clubbing, acro-osteolysis, wormian bones, and hyperhidrosis without pachyderma. CASE REPORT Ankit Parakh, Anand Prakash Dubey, S. Sudha Department of Paediatrics, Maulana Azad Medical College and Associated Hospitals, New Delhi , India Corresponding Author Ankit Parakh, Jain's B-52, Ashoka Niketan, IP Extension II, Delhi , ID: [email protected] PDP is characterized by pachydermia (thickening of the skin and seborrhea of the skin of the face and/or forehead) (45.6%), digital clubbing (94%) and periostosis (swelling of periarticular tissue and subperiosteal new bone formation) (1). Other associated features include hyperhidrosis (27%), acro- osteolysis (10%), arthritis/arthralgia (32.8%), gastric ulcer (11%), cutis verticus gyrata (10.3%), blepharoptosis (8.7%), joint effusion/ hemarthrosis (17.6%), seborrhea (28.6%), acne (4.8%) and eczema (35%) [5]. An eleven years old boy presented with fever, pain abdomen and loose stools. There was no history of consanguinity. On examination he had clubbing of fingers and toes (Fig 1a), which was apparently present since birth. There was no history of any long standing systemic illness but there was history of increased sweating over the palms and soles (hyperhidrosis), which occasionally used to interfere with writing. Child was neurodevelopmentally normal.. The mother reported that her sister's daughter 13 years old also had similar deformities of fingers and toes. However she could not be brought for examination. No other member of the fourgeneration pedigree was affected. The child had a normal shaped skull with normal facies and no obvious clavicle or limb deformity. Dentition was normal. Hyperhidrosis could be appreciated over the palms and the CASE REPORT soles. Joints and skin were normal. Cardiovascular, respiratory and abdomen examination were normal. Central nervous system including sensory system was also normal. Routine blood investigations including complete blood counts, urea, ESR, CRP, creatinine, electrolytes, serum calcium, phosphate, alkaline phosphatase and serum proteins were normal. Thyroid function tests, chest X-ray and electrocardiogram were normal. The radiographs showed evidence of acro-osteolysis of distal phalanges in the hand & foot (Fig 1b), wormian bones in each lambdoid suture in the skull (Fig 1c) and periosteal new bone formation in all long bones (Fig 1d & e). All joints and spine were normal. Pachydermoperiostosis diagnosis was set up on 3 out of the 4 Borochowitz criteria [2]. DISCUSSION Hypertrophic osteoarthropathy (HOA) is a syndrome characterized by clubbing, periostosis and arthritis. PDP, the primary form of HOA is a rare genodermatosis and accounts for 5% of all cases of HOA. The more common secondary form is associated with several systemic diseases (usually cardiopulmonary diseases) and sometimes occurs as paraneoplastic syndrome. Primary HOA was originally described by Friedreich (1868) in two affected brothers as 'hyperostosis of the entire skeleton' [3]. In 1935, Touraine, et al individualized PDP as the primary form of HOA, distinct from the more common secondary HOA and proposed a classification describing 3 forms of PDP: (i) a complete form presenting with full-blown phenotype with pachydermia and periostitis (ii) an incomplete form with evidence of bone abnormalities but lacking pachydermia and (iii) a forme fruste with prominent pachydermia and minimal-to-absent skeletal changes [4]. PDP is a rare hereditary disorder and the precise incidence is unknown. It is more common in African-Americans than in whites with a male-to-female ratio of approximately 7:1. Typically, men are affected more severely than women.
10 10 Disease onset is often at puberty, with progressive thickening and furrowing of the skin on the face and the scalp (pachydermia), enlargement of the fingertips (digital clubbing), swelling of periarticular tissue and shaggy periosteal new bone formation of the long bones (periostosis). These changes usually progress for 5 20 years and remain stable afterwards. The major complication is joint involvement, consisting of arthralgia, arthritis and hydrarthrosis/haemarthrosis. (5). PDP is often familial. It is believed to be inherited in an autosomal dominant pattern with variable penetrance; however, autosomal recessive forms have been reported. The two forms may differ in clinical severity, intrafamilial variability and prevalence of some features. Radiographic features include subperiosteal new bone formation of the long bones. This feature is mainly seen in the distal tibia, the fibula, the radius, the ulna, the metacarpals, the phalanges, and less frequently the metatarsals. Acro-osteolysis and ossification of the ligaments and interosseus membranes may also occur. Cortical thickening without narrowing of the medullary cavity, enlargement of the paranasal sinuses and soft tissue swellings have also been described. Most important differential diagnosis is secondary HOA, which must be excluded. Several conditions such as acromegaly, thyroid acropachy, syphilitic periostosis, lepromatous leprosy and other high bone density skeletal dysplasias may mimic PDP and must be carefully differentiated. Our case is unique from the usual forms of PDP as the age of onset was at birth or early infancy. The age of onset has been reported to be at birth in 4 and in infancy in 8 of the 68 pedigrees although in the classical form the process is reported to start around puberty. Wormian bones are also reported as a very rare feature in PDP. Figure 1: (a) Showing digital clubbing (b) radiograph of hands and feet showing acro-osteolysis (c) radiograph of skull showing Wormian Bones (d) radiograph of leg showing periosteal reaction in the tibia and fibula(e) radiograph of arm showing periosteal reaction in the radius and ulna REFERENCES 1. Auger M, Stavrianeas N. Pachydermoperiostosis. Orphanet Encyclopedia, Accessed August 2005, from 2. Borochowitz Z, Rimoin DL. Pachydermoperiostosis. Birth Defects Encyclopaedia 1990: Friedreich N. Hyperostose des gesammten skelettes. Virchows Arch [a] 1868: 43: Touraine A, Solente G, Gole L. Un syndrome oste odermopathique: la pachydermie plicature e avec pachype riostose des extre mite s. Presse Med 1935: 43: Castori M, Sinibaldi M, Mingarelli R, Lachman RM, Rimoin RL, Dallapiccola M. Pachydermoperiostosis: an update. Clin Genet 2005: 68: O P I N I O N P O L L The obesity epidemic calls for urgent attention of health professionals, researchers and public health advocates. The "food environment" what foods are easily available to us, how much they cost, how they are marketed has a large influence on what we eat and in turn, our obesity risk. The food preference that children develop can last well into adulthood &these are largely influenced by the family and society dietary choices. Further just as employed adults spend most of their day at work, children spend much of their day at school and whatever is available in the school has impact on their choices. Several researchers have shown correlation between use of Junk foods and sugar sweetened beverages with obesity epidemic. Some researchers argue that recent shifts in cultural norms have led to eating and physical activity habits that promote overweight but at the same time it cannot be ignored that these food items are addictive. There is a strong psychological craving for these foods /beverages. Junk foods and sugary beverage companies use all the P's of marketing to increase sales: product, promotion, packaging, placement, and pricing. Education about the risks of junk foods and sugary beverages which increases risk of obesity is absolutely necessary, but the continued growth of the obesity epidemic makes it clear that education alone is not sufficient to solve this problem. If we are to end this epidemic, we will also need a food environment in country. What should be done to bring back safe food environment in our country? a) Heavy tax on junk foods and sugary beverages b) Regulations to ban advertisement of these items on TV/at Public places c) Education of people but no regulation d) Voluntary declaration by manufacturers of junk foods and sugary beverages about risk of obesity Send your opinion and view to [email protected]
11 11 Pseudoascites: Pitfalls in diagnosis ABSTRACT The term pseudoascites denoted a clinical impression of ascites when in fact there is no free fluid in the peritoneal cavity. We are reporting two cases of omental and mesenteric cyst that were masquerading clinically as ascites. One of these cases even received anti tubercular treatment (ATT) for ascites with no response. These cases illustrate the clinical and diagnostic pitfalls faced in investigating and managing patients of massive abdominal distension. Keywords: omental cyst; mesenteric cyst INTRODUCTION Anu Maheshwari, Prathik BH, Satinder Aneja, Praveen Kumar, Archana Puri, Rajeev Chaddha, Nitin Pant, Monisha Choudhury Department of Pediatrics, Department of Pediatric Surgery, Department of Pathology, Lady Hardinge Medical College and associated Smt Sucheta Kriplani Hospital, New Delhi-01, India Address for Correspondence Dr Anu Maheshwari, Assistant Professor, Department of Pediatrics, Lady Hardinge Medical College, New Delhi [email protected]. Ascites is one of the common clinical conditions encountered in routine clinical practice. The term 'ascites' refers to detectable and pathological collection of fluid in the peritoneal cavity. Clinically ascites is suggested by physical signs like abdominal distension with flank fullness and shifting dullness and, fluid thrill. Ultrasonographic examination is the best modality to detect small amount of intra-peritoneal fluid in patients who present with mild abdominal distension. The aetiology is usually apparent after history, physical examination and basic investigations. During evaluation of patients who have obvious ascites, those conditions that produce physical signs of ascites without actually causing fluid accumulation in the peritoneal cavity are not usually considered. We are reporting two cases of omental and mesenteric cyst that were masquerading clinically as ascites. One of these cases even received anti tubercular treatment (ATT) with no response. These cases highlight pitfalls in differentiating causes of abdominal distension. We should look for these rare causes of abdominal distension when common causes are excluded. CASE 1 A 2 yr 9 months male, presented with complaints of gradually progressive abdominal distension noticed since the age of 18 months. There was no history of abdominal pain, vomiting, urinary problem, breathing difficulty, chest pain, jaundice or swelling over the body. There was no history of koch's contact, any significant illness or trauma in the past. CASE REPORT On examination, vitals were stable. His weight and height were normal for his age. There was no pallor, icterus, cyanosis, lymphadenopathy or pedal edema. Per abdomen examination revealed gross distension with fluid thrill. There was no hepato-splenomegaly, distended veins, spider naevi, or palmar erythema. Other systemic examination was normal. Investigations showed normal hemogram, serum electrolytes, renal and liver function. Total serum protein and albumin were 7.6gm% and 4.6gm% respectively. Lipid profile showed total cholesterol of 153mg/dl and triglyceride was 223 mg/dl. Serology for HIV, hepatitis B and C were non-reactive. The work up for tuberculosis was negative. Ultrasound abdomen revealed normal sized liver with normal echo texture andportal vein diameter of 4.3 mm. The gall bladder, spleen, pancreas, kidneys and retro-peritoneum were normal. There was free fluid in abdomen with internal echoes, and septations. Ascitic tap was done which revealed golden brown fluid. Cytology revealed few mesothelial cells and occasional lymphocytes with no evidence of malignant cells. Protein and sugar were 3.5gm/dl and 113mg/dl respectively. Fluid ADA (adenosine deaminase) was U/L and cultures weresterile. MRI (magnetic resonance imaging) abdomen with MRCP (magnetic resonance cholecystography) revealed free fluid in the abdomen with no other abnormality (figure 1). Diagnostic laparoscopy was planned. It revealed a large omental cyst of 20x30 cm filled with hemorrhagic fluid and approximately 2 litres of fluid was drained and the cyst was completely excised. The histopathology was suggestive of lymphangiomatous type of omental cyst. Follow up after 3 months revealed no apparent recurrence on ultrasound and the child was asymptomatic. CASE 2 A 13 year old male was referred with p r o g r e s s i v e a b d o m i n a l distension since 2years (figure 2). He was receiving ATT for 4 months. Even after receiving ATT t h e r e w a s n o improvement in a b d o m i n a l distension. There Figure 1 : MRI showing free fluids
12 12 was no history of fever, j a u n d i c e, c h r o n i c diarrhoea, weight loss, pallor or anorexia. He had no breathlessness, swelling or recurrent cough. There was no family history of tuberculosis. There was no significant illness or trauma in the past. General physical examination revealed stable vitals and Figure-2 : absence of pallor, icterus, Child with gross abdominal distension e d e m a o r lymphadenopathy. Per abdomen examination revealed generalized abdominal distension with bulging flanks. There was no organomegaly but fluid thrill was positive. There were no distended veins, spider naevi, or palmar erythema. Other systemic examination was normal. Investigations revealed haemoglobin of 12.3 g/dl, TLC 13.6 x /µl and platelet 267x10 /µl. Erythrocyte sedimentation st rate (ESR) was 16 mm/1 hour. Renal function tests, liver function tests and serum electrolytes were normal. Totalserum protein and albumin were 7.8 g/dl and 4.8 g/dl respectively. Coagulation profile was also normal. His chest X- ray was normal and mantoux test was negative. Serology for HIV, hepatitis B and C were non-reactive. A diagnostic paracentesis was done which showed no cells on microscopy, protein of 78mg/dl and sugar of 60 mg/dl, suggestive of transudative fluid. Culture and gram stain was sterile. No acid fast bacilli were demonstrated. Ultrasound abdomen was done which showed slightly enlarged liver with normal echotexture with no evidence of portal hypertension. Rest of the intra-abdominal findings were normal except for gross ascites with few internal septations. Contrast enhanced computed tomography (CECT) abdomen showed gross ascites with centrally displaced small bowel loops in which showed diffuse wall thickening (figure 3). Figure-3 : CT abdomen showing gross fluid collection with displaced small bowel loops A diagnostic laparoscopy was followed by laparatomy. Intraoperatively multiple mesenteric cysts were revealed. There were 2 huge intra-peritoneal cysts with multiple small cysts (figure 4). Adhesions were present to the mesentery of small bowel, predominantly ileum and to large b o w e l. T h e r e w a s n o communication with bowel or biliary system. The cyst was completely excised and sent for histopathological examination which confirmed the benign n a t u r e o f t h e l e s i o n, lymphomatous in origin. During follow up he is asymptomatic. DISCUSSION The term pseudo ascites denotes the condition w h e r e t h e c l i n i c a l impression of ascites is present, but in fact free fluid is not present in the peritoneal cavity.[1] There are many conditions which p r o d u c e s i g n s a n d symptoms similar to ascites without accumulation of free fluid in peritoneal cavity. Pseudoascites is a rare condition and the Figure-4: Intra-peritoneal cyst correct diagnosis is made pre-operatively in only 15-35% of cases.[1] The correct diagnosis is usually made after surgical exploration. The concept of peudoascites should be remembered as it may explain the clinical situation in cases where diagnosis remains elusive. The most frequently reported aetiology of pseudoascites in order of occurrence is omental, mesenteric and ovarian cysts. Omental and mesenteric cyst are believed to be of lymphatic origin. They may develop slowly or rapidly depending on inciting factors like infection and haemorrhage. The first omental cyst was described by Gairdner in 1951.[2] It is a rare intra-abdominal lesion in paediatric population with an incidence of approximately 1 in 140,000.[3] The true incidence is much higher because only cysts of clinical importance are reported. The most common type is cystic lymphangioma which has male preponderance and mean age of presentation is about 2.2 years.[4] Proposed aetiologies include failure of embryonic vessels of mesentery to join the central lymphatic and venous system, benign proliferation of ectopic lymphatics, trauma and degeneration of lymph nodes.[5,6] They can be single or multiple, unilocular or multilocular and they may contain hemorrhagic, serous or chylous fluid. In large cysts a fluid wave may be detected, leading to erroneous diagnosis of st ascites as in our 1 case. Lack of involvement of flanks is more indicative of cystic mass rather than ascites, but in our case, the flanks were not spared clinically and even in the MRI possibly due to large size of the cyst and flaccid consistency which tends to flow out and fill out the dependent parts of the abdominal cavity and interposes between the structures.[7] Mesenteric cysts are also rare abdominal lesions with an incidence of nearly 1 in 20,000 in children. It was first observed in 1507 by an Italian anatomist Benevieni.[8] Although mesenteric cysts can occur at any age; they are common in people between 40 and 70 years and in children less than 10 years old. The exact pathogenesis of the disease remains unknown but is similar to that of the omental cysts. They can occur anywhere between duodenum and rectum but are most common in the small bowel mesentery (60%), especially the ileum, followed by mesocolon (24%) and the retroperitoneum (14.5%), while it is indefinite in 1.5% of cases.[7] They can be single or multiple, unilocular or multilocular and they may contain hemorrhagic, serous or chylous fluid. Multiple mesenteric cysts are less common compared to single cysts. In our case 2 huge cysts along with multiple small cysts were present containing fluid with biliary tinge in one of the large Contd...17
13 13 HOW TO WRITE THESIS PROTOCOL - PRAVEEN KUMAR, SATINDER ANEJA Department of Pediatrics, Lady Hardinge Medical College and associated Kalawati Saran Children's Hospital, New Delhi Research is an integral part of the training for all postgraduates 3. AIMS & OBJECTIVES : pursuing Doctor of Medicine and registered for Diplomate of The aim is what you want to achieve, and the objective National Board degree. According to both MCI and National describes how you are going to achieve that aim. Make Board, every candidate during their training shall carry out sure that each aim is matched with specific objectives. work on an assigned research project under the guidance of a Aim and Objectives should be presented concisely and recognized supervisor. The research project shall be written up briefly. It should be able to answer the research question, and submitted to the University /Board in the form of a thesis. should be realistic about what one can accomplish in the Thesis teaches the fundamentals of research methodology & duration of the project considering the other stimulates interest in research. It also contributes in the commitments. development of a spirit of enquiry, critical analysis, Research question is a question that needs to be answered acquaintance with the latest advances in medical science and by the planned study. A good research question has well the manner of identifying and consulting available literature. defined PICO (participants, intervention, control and As per MCI and National Board guideline, thesis needs to be outcome). Research question is based on some submitted at least six months before the theoretical and hypothesis. Hypothesis is nothing but an idea, which is clinical/ practical examination. yet to be proved. 'Null Hypothesis', also known as statistical hypothesis states exactly opposite of the WHERE AND HOW TO START? research hypothesis. Null hypothesis is the one that will be tested by the statistical significance tests and is either Each student is supposed to select a topic for thesis and develop rejected or not rejected. This hypothesis if not rejected protocol in consultation with his/her guide and the head of concludes that the observed results could be due to chance department. alone. On the other hand its rejection signifies that the observed result is statistically significant indeed. USEFUL HINTS FOR THE SELECTION OF A TOPIC: Objectives are broadly divided into two parts- primary and secondary. Primary objective is the objective which Avoid topics on which thesis has already been carried out in the must be achieved. It dictates design, methods and sample previous 5years, in the University. Candidates should try to size. Secondary objectives are of interest but not essential. select a topic, which requires minimal help from other Characteristic of objectives are described as S.M.A.R.T. departments (equipments or personnel). If unavoidable then (specific, measurable, attainable, reliable, time limited). official appointment of a co-guide from the collaborating department will be useful. The thesis protocol should be presented first in the department where other faculty members 4. BRIEF 'REVIEW OF LITERATURE' are present. Their inputs will always be helpful in Review of literature reveals those aspects of topics on improvement of the protocol. which research has not been carried out. It helps in Most universities require thesis protocol in following format knowing the strengths and weaknesses of other studies 1. TITLE: which will serve as guide for the proposed study. By good review, investigators are able to know the requirements Title of thesis should be brief, clear and focus on the and difficulties for the proposed study. Information about relevance of the topic. dose of the drug, side effects, sample size, statistical methods used also come from review. 2. INTRODUCTION: What should be reviewed? In this section the topic is introduced. Candidates explain - Text Books why this topic was chosen by describing the problem - Journals under consideration. A brief review of literature and justification is given in the form of what is already known, Which studies should be included in review? what are gaps in the current knowledge and how present Those that study will contribute to the current knowledge. - Help to define the problem
14 14 - Describe its magnitude Study questionnaire and formats: Submit a copy of - Provide data for / against the research hypothesis study questionnaire in annexure which you will use in your study and case study proforma for recording the - Provide Indian data findings. information in a systematic manner (placed in annexure) 5. MATERIAL AND METHODS Describe data collection methods This section of the thesis protocol gives information about - Clearly define all variables Study design and setting - Mention how you will ensure quality control - Descriptive Data management and statistical analysis - Analytical Describe procedure to enter data - Interventional Software to be used for data entry and statistical analysis - Observational Missing data handling Study period It is good idea to prepare dummy tables for data Study subjects: Inclusion and exclusion criteria with analysis case definitions Ethical consideration- Institutional ethical clearance Sample size: is compulsory for all studies, even the ones without Basis of sample size: Sample size should be based on intervention. primary objective. In case it is not feasible to take desired Competing interest if any- disclose source of funding, sample due to time constraints or availability of subjects association etc. then lower sample size should be taken but should be stated clearly in the protocol. Method of recruitment 6. BIBLIOGRAPHY (REFERENCES): Randomization, if applicable Write references in Vancouver style. Sequence generation Format for reference from a journal: Author's surname Initials. Title of article. Title of Journal.[abbreviated] Allocation concealment Year of publication; Volume Number:page numbers. Blinding/ masking Format for reference from a book; Author's surname Intervention if any- discuss in detail Initials. Title of chapter. In: Record the co-interventions/ confounders Editor's surname Initials, editor. Title of the book. # ed.[if not 1st] Place of publication: Publisher's name; Year of Follow up of the study participants, if applicable. If publication. p. #. [page numbers of chapter] there are multiple measurements, it is good to provide a table with the measurements and the time. Method of measurement of Outcome of interest- 7. ANNEXURES: Outcome variable (Primary and secondary) should be clearly defined You should add a copy of questionnaires/ measurement tools, patient/ parent information sheet and consent form: both in english and local languages as annexures. Corresponding Author: Dr Praveen Kumar, Department of Pediatrics, Lady Hardinge Medical College and associated Kalawati Saran Children's Hospital, New Delhi Who Should Be Tested for Celiac Disease? Revised ESPGHAN guideline 2012 recommends testing for CD in the following group of patients: Group 1:Symptomatic children and adolescents (unexplained chronic or intermittent diarrhoea, failure to thrive, weight loss, stunted growth, delayed puberty, iron-deficiency anemia, chronic abdominal pain or distension, chronic constipation, chronic fatigue, recurrent aphthous stomatitis (mouth ulcers), dermatitis herpetiformis like rash, osteopenia/osteoporosis, and abnormal liver biochemistry. Group 2: Asymptomatic children and adolescents with an increased risk for CD such as type 1 diabetes mellitus (IDDM),Down syndrome, autoimmune thyroid disease, Turner syndrome, Williams syndrome, selective immunoglobulin A (IgA)deficiency, autoimmune liver disease, and first-degree relatives of CD patients.
15 15 INTRODUCTION: - Bleeding time and clotting time. Renal biopsy is an important investigation in the diagnosis and management of a subset of children with renal diseases. Renal biopsy is more difficult in children than in adults due to size variation and different levels of co-operation. A final histopathological diagnosis is based on a synthesis of information on light microscopic findings, immunofluorescence and electron microscopy [1]. INDICATIONS FOR RENAL BIOPSY IN CHILDREN [1-5] Recognition of the underlying etiology is essential for the prompt diagnosis and initiation of therapeutic interventions in many renal diseases. Box-1 depicts the indications of renal biopsy in childhood renal diseases. CONTRAINDICATIONS RADIOLOGICAL EVALUATION Ultrasonography should be done to look for the size, shape and position of the kidneys. PROCEDURE Usually, percutaneous renal biopsies are outpatient procedures, except in infants, children with solitary kidney and chronic kidney disease. Percutaneous renal biopsy may be done under ultrasound guided imaging or as a blind procedure, with sedation. PRECAUTIONS 1. Avoid ketamine for sedation in children with respiratory illnesses or young infants Though there are no absolute contraindications to renal biopsy, 2. Avoid treatment with non-steroidal anti-inflammatory it is imperative that caution be exercised in the presence of the drugs or warfarin 5-7 days before surgery. following: 3. In patients on hemodialysis requiring a kidney biopsy, the a) Bleeding or clotting disorders (including procedure should be done 6 hours after hemodialysis. The thrombocytopenia, haemophilia or recent medications use of anticoagulants should be avoided for next 24 hours. that increase bleeding risk) 4. Post biopsy bleeding risk can be reduced in patients with b) Uncontrolled hypertension (since the risk of bleeding is uremia or prolonged bleeding time by administration of increased) intravenous desmopressin 30 minutes prior, or nasal c) Solitary kidney desmopressin 2 hours before the procedure. d) Active kidney infection PRE-BIOPSY EVALUATION Prior to biopsy, the medical history, clinical examination and investigations should be reviewed. Clinical evaluation (History and examination) The history should be reviewed for bleeding disorders, drug allergies and cardiac or respiratory illnesses. During clinical examination, emphasis should be laid on detection of hypertension, subcutaneous infection over the biopsy site, spine abnormalities and ascites. Laboratory tests Renal biopsy in children Sriram Krishnamurthy Department of Pediatrics, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Dhanvantari Nagar, Pondicherry, , India The hemoglobin level should be more than 8 g/dl and platelet 3 counts more than 75,000/mm. The other investigations needed are: - Blood urea and serum creatinine (very high levels of blood urea can interfere with platelet function) - Prothrombin time (INR should be less than 1.5, at least 24 hour prior to the biopsy, especially if the patient has been receiving oral anticoagulants) BIOPSY EQUIPMENTS The equipment used is a semi-automatic kidney biopsy needle (e.g Bard Biopsy gun). Alternatively, a Trucut biopsy needle can be used. Either a 16 or 18 gauge needle can be used. SEDATION AND POSITIONING Most children need conscious sedation with monitoring of vital signs. Patient is biopsied in prone position. An intravenous access should be established. Medications administered for the sedation include: a) Midazolam mg/kg i.v. b) Atropine 0.01 mg/kg i.v. is administered 1-2 minutes prior to midazolam to reduce excessive secretions c) Ketamine 0.5 mg/kg is given 3-5 minutes after midazolam, just before the biopsy. PREPARATION OF SURFACE AND LOCAL ANAESTHESIA Betadine and spirit (70% alcohol) are used in succession to clean the site and adjoining area centrifugally. Drapes are used.
16 16 Lidocaine is injected locally (1% i. v.) (0.5 ml/kg). ULTRASOUND GUIDED BIOPSY In case ultrasound guided biopsy is chosen to be done, the biopsy needle is inserted from a posterior approach in a trajectory that avoids the lungs, adjacent organs and the central renal collecting system. A trajectory that passes vertically down to the lower pole renal cortex avoiding the central echogenic hilum is chosen to avoid vascular injury. IF ULTRASOUND GUIDED BIOPSY FACILITIES NOT AVAILABLE A probing needle (1.5 inch, 23 gauge) is used to locate the renal th capsule at the lower pole (below 12 rib, lateral to the sacrospinalis muscle). Next, a stab incision is given at the proposed site with a 11 gauge surgical blade. The kidney biopsy needle is then passed to the required depth and the cores are taken. SPECIMEN COLLECTION Two or three cores are taken for light microscopy, immunofluorescence and if possible, electron microscopy. The tissue for light microscopy is transported in 10% formalin, while immunofluorescence in special media (e.g Michel) and snap frozen in the laboratory. Electron microscopy sample is transported in glutaraldehyde. MONITORING OF THE CHILD POST-PROCEDURE It is essential that heart rate, respiratory rate, blood pressure are monitored every 15 minutes for the first hour, then half hourly for 2 hours and then hourly for 4-6 hours. The patient is kept supine and orally allowed when conscious. Each urine specimen is inspected for hematuria. Microscopic hematuria is common. DISCHARGE FROM HOSPITAL The child should stay in hospital 8-24 hours after the procedure. Bed rest is advised for 24 hours. Contact sports, cycling or lifting heavy objects should be avoided for 1 week. Paracetamol is given for pain relief. At discharge, the vital signs should be normal and there should be no gross hematuria. POTENTIAL COMPLICATIONS Though renal biopsy is generally a safe procedure, complications may rarely occur. These are as follows: a) Gross Hematuria: % b) Perinephric hematoma: 16% - 42% (1% clinically significant) c) Bleeding and hypotension: 0.87% d) Blood transfusion secondary to bleeding: 0.42% Box-1: Indications for renal biopsy in children 1. Acute Glomerulonephritis a. Delayed resolution Oliguria, hypertension, azotemia persisting beyond 2 weeks Macroscopic hematuria persisting beyond 4 weeks Hypocomplementemia (low C3) beyond 8 weeks Nephrotic range proteinuria persisting beyond 8 weeks b. Absence of hypocomplementemia at admission c. Severe acute kidney injury, rising serum creatinine with normal sized kidneys d. Systemic features like skin rashes, joint pains, hepatosplenomegaly or persistent fever 2. Nephrotic syndrome At Onset Age of onset <1 year. Gross hematuria, persistent microscopic hematuria or low serum C3. Sustained hypertension. Renal failure not attributable to hypovolemia. Suspected secondary causes of nephrotic syndrome. After Initial Treatment Proteinuria persisting despite 4-weeks of daily corticosteroid therapy. Before treatment with cyclosporin A or tacrolimus. 3. Acute kidney injury Unremitting acute kidney injury lasting more than 2 to 3 weeks Suspected drug induced renal failure; acute interstitial nephritis Etiology of acute kidney injury unascertained 4. Hematuria Persistent glomerular hematuria (2+ or more, red blood casts, dysmorphic red cell casts, or azotemia) Microscopic hematuria of unknown etiology persisting beyond 2 years 5. Asymptomatic proteinuria Nephrotic range proteinuria Persistent non-nephrotic range proteinuria with hematuria 6. Systemic diseases Systemic lupus erythematosus, Henoch Schonlein purpura, microscopic polyarteritis 7. Following renal transplantation
17 17 e) Embolisation to stop bleeding: 0.1% REFERENCES st f) Damage to surrounding organs such as liver and intestine: 1. Renal biopsy. In: Protocols in Pediatric Nephrology. 1 edition. Eds Bagga A, Sinha A, Gulati A. CBS Publishers and Distributors Pvt. Ltd., 0.78% Delhi 2012 p g) Arteriovenous fistula: 0.05% 2. Vijayakumar M. Acute and crescentic glomerulonephritis. Indian J Pediatr ; 69(12): h) Infection: 0.93% 3. Hussain F, Mallik M, Marks SD, Watson AR; British Association of i) Nephrectomy (partial or total): < 0.1% Paediatric Nephrology. Renal biopsies in children: current practice and audit of outcomes.nephrol Dial Transplant. 2010; 25(2): In the presence of gross hematuria, an ultrasound examination 4. Mahajan V, Suri D, Saxena A, Nada R. Should ultrasound guided is done to look for bleeds, clots or perinephric hematomas. percutaneous renal biopsy in children be done in a day care setting? Packed cells should be given if hemoglobin falls by more than Indian J Nephrol ;20(1): % from baseline. Adequate hydration is ensured. 5. Walker PD, Cavallo T, Bonsib SM; Ad Hoc Committee on Renal Biopsy Desmopressin may be given if coagulation profile is deranged. Guidelines of the Renal Pathology Society. Practice guidelines for the If hematuria persists then arteriovenous fistula should be renal biopsy. Mod Pathol ;17(12): suspected, which may require embolization or surgical 6. Indian Pediatric Nephrology Group, Indian Academy of Pediatrics, intervention. Bagga A, Ali U, Banerjee S, Kanitkar M, Phadke KD, Senguttuvan P, et al. Management of steroid sensitive nephrotic syndrome: revised guidelines. Indian Pediatr. 2008;45(3): Pseudoascites: Pitfalls in diagnosis... (Contd...) cysts and other had brownish fluid with jelly like material. ATT in view of bowel wall thickening apparent on CT. When Adhesions were present to the mesentery of bowel he did not respond to treatment, surgical exploration was done, predominantly distal ileum. There was no communication to thereby delaying definitive diagnosis and treatment. bowel or with biliary system. In summary pseudo ascites cannot be distinguished Abdominal ultrasonography is the imaging modality of choice consistently from massive ascites by history, physical in suspected omental or mesenteric cysts. It usually reveals examination or by laboratory investigations. Even advanced fluid filled cystic structures, commonly with thin internal imaging techniques are often non-contributory. Strong clinical septae and sometimes with internal echoes from debris, suspicion is necessary and it should be kept in the differential hemmorhage or infection. An anterior fluid collection with diagnosis of ascites. Early laparoscopy and laparotomy should internal septae (which might be mistaken for loculated ascites) be considered when the exact aetiology is not found. is the typical sonographic appearance of an omental cyst. Omental cyst tends to displace the bowels posteriorly. Ultrasound can easily identify internal septations in the cyst REFERENCES which may be missed by CT scan.[2,9]abdominal CT or MRI 1. Fiedorek SC, Casteel HB, Reddy G, Graham DY. The aetiology and adds minimal additional information, although it can reveal clinical significance of pseudoascites. J Gen Intern Med Jan-Feb; that cyst is not arising from another organ such as kidney, 6(1): pancreas or ovary. Paracentesis should be done only after 2. Prasad KK, Jain M, Gupta RK. Omental cyst in children presenting as pseudoascites: Report of two cases and review of the literature. Indian confirmation of diagnosis by ultrasound or CT, because when a Pathol Microbiol. 2001; large omental cyst is imaged after paracentesis, a mistaken 3. NettMH, Vo NJ, Chapman T. Large omental cyst. Radiology case reports diagnosis of 2010; 5:2. 4. Ricketts RR (1998) Mesenteric and omental cysts. In O'Neill JA, Rowe ascites might be made and the origin of the peritoneal fluid MI, Grosfeld JL, Fonkalsrud EW, Coran AG, editors. Pediatric Surgery. from a cystic mass overlooked. Indeed imaging after 5th ed. Chicago: Mosby paracentesis may be normal if the cyst contents have been 5. Joshi N, YadavS, Singh.B, Gupta A: Omental cyst presenting as resorbed through the peritoneum.[10] tubercular ascites. J Infect Dev Ctries Mar 29; 4(3): Kaya M, Sakarya MH. Pseudoascites: reports of three cases. Turk J Tubercular ascites is usually the first differential diagnosis we Gastroenterol 2009; 20: consider in the developing world while evaluating the cases 7. Dulger C, AdaliE,AvcuS, Kurdoglu Z. Large mesenteric cyst mimicking tuberculous ascites. Case Report Med. 2010; 2010: with long standing ascites when other causes have been 8. MoraliogluS, SonmezK, TurkyilmazZ, Basaklar AC, Kale N. A child excluded and when exact aetiology is not found. Most of these with a gaintomental cyst. Acta Chir Belg. 2007; 107(6): are treated by a trail of ATT (Table I) with disappointing 9. Gairdner WT. A remarkable cyst in the omentum. Transpatholsci (lond) results. Moreover peritoneal fluid ADA value may be falsely 1851; 3:374 elevated in mesenteric and omental cysts thereby creating 10. Gyves-ray k, Hernandez RJ, Hillemeier AC. Pseudoascites: Unusual presentation of omental cyst. Pediatrradiol 1990; 20: more confusion and leading to further delay in diagnosis and 11. Debnath B, Biswas SK, Mallick AK. Omental cyst masquerading as increases the morbidity and risk of complications. However in ascites. J Indian Med Assoc. 2008; 106: st our 1 case fluid ADA was not suggestive of tuberculosis and 12. Menon p, Rao KLN. Giant Omental Cyst Masquerading as Hemorrhagic we were more confident to undertake diagnostic laparoscopy Ascites. Indian Pediatrics 2005; 42:395-6 nd as the diagnosis was not apparent. But our 2 case received
18 18 Choice of intravenous fluids for resuscitation and maintenance in children a) Resuscitation: Children severely dehydrated or with signs of shock should be resuscitated using isotonic intravenous (IV) solutions such as sodium chloride 0.9% or ringers lactate. b) Intravenous maintenance fluid: For children who require IV fluids for maintenance, options include ringers lactate solution with 5% dextrose, sodium chloride 0.45% with glucose 5%, sodium chloride 0.45% with glucose 2.5%, or 0.9% sodium chloride with glucose 5%. c) Low sodium-containing solutions, such as sodium chloride 0.18% with glucose 4%, or 5% glucose in water, should not be used as there is an increased risk of hyponatraemia leading to cerebral oedema Skin-to-skin contact in the first hour of life Newborns without complications should be kept in skin-to-skin contact with their mothers during the first hour after birth to prevent hypothermia and promote breastfeeding Empirical antibiotics for suspected neonatal sepsis a) Neonates with signs of sepsis should be treated with ampicillin (or penicillin) and gentamicin as the first line antibiotic treatment for at least 10 days. b) If a neonate with sepsis is at greater risk of staphylococcus infection (e.g. extensive skin pustules, abscess, or omphalitis in addition to signs of sepsis), they should be given cloxacillin and gentamicin instead of penicillin and gentamicin. c) Where possible, blood cultures should be obtained before starting antibiotics. If an infant does not improve in 2 3 days, antibiotic treatment should be changed, or the infant should be referred for further management. Head or whole body cooling in management of hypoxic ischaemic encephalopathy Head or whole body cooling should not be done outside well-resourced, tertiary neonatal intensive care units, because there is potential for harm from this therapy in low-resource settings. Kangaroo Mother Care Low birth weight (LBW) neonates weighing < 2000 g who are clinically stable should be provided Kangaroo Mother Care (KMC) early in the first week of life. Prevention of hypothermia immediately after birth in LBW infants LBW neonates weighing >1200g who do not have complications and are clinically stable should be put in skin-to-skin contact with the mother soon after birth and after drying them thoroughly to prevent neonatal hypothermia. Clippings from WHO 2012 recommendations for management of common childhood conditions
19 19 Q1. A newly born baby has presented with hypertrophied left lower limb since birth. There is a nevus noticed over the lateral aspect of the left thigh. What is the diagnosis? pq PHOTO QUIZ Readers are requested to mail their answer with name and place to [email protected] Names of first 10 people sending correct answer will be published in next issue (March 2013) Q2. A 13 month old child has presented with multiple hard nodular swellings over the scalp, abdomen and limbs. The peripheral smear shows 40% blast cells. What is the diagnosis? DO YOU Cord clamping should be delayed for at least 1 minute in babies who do not require resuscitation. Advantage of delayed cord clamping: Improved iron status and reduced anemia at 4 months (Ref: Curr Opin Pediatr 2012;24:147-53) American Academy of Pediatrics (2010) recommends iron supplementation at 1 mg/kg/day from 4 months of age in all exclusively breast-fed, full-term neonates, until appropriate iron-containing complementary foods are introduced in diet. (Ref: Pediatrics 2010; 126: ) KNOW? Private cord blood banking for unidentified possible future use is not currently recommended by The American Academy of Pediatrics or The American College of Obstetricians and Gynecologists Private cord blood banking and any form of advertisement is illegal in France and Italy (Ref: Am Fam Physician 2011;84:661-6) Deepak Bansal Hematology/Oncology unit, Dept. of Pediatrics,Advanced Pediatric Center, Postgraduate Institute of Medical Education & Research, Chandigarh
20 20 e-learning training course on Programming for Infant and Young Child Feeding UNICEF's nutrition section, in collaboration with Cornell University, has launched a new e-learning training course on Programming for Infant and Young Child Feeding. The course is free of charge. After completing the unit tests for all 12 units, the final exam and a course evaluation survey, you will receive a personalized certificate. You need to register as a member of Cornell Nutrition Works in order to access the course. Once you have been given access, you will have 3 months to complete the course. If you do not complete it within the 3 months, your access will expire and you will need to register again and start the course. You can register for the course by visiting. < Malnutrition e-learning course Caring for children with acute Malnutrition University of Southampton has developed an elearning course to cater individualized learning for health professionals on management of severe acute malnutrition both at community and facility level. It targets all health professionals who have any responsibility for child care, especially pediatricians, nurses, medical students and nursing students. It has 3 modules. You do not need to finish the course at once. Your answers will be stored in a database and be retrieved next time you log in. So, you can plan your study in a way suitable for you. After completion you will need to write to course providers for a certificate. The course is free and available at < Address for Correspondence Dr. Praveen Kumar, Professor, Department of Pediatrics, Lady Hardinge Medical College & Assoc. Hospitals,New Delhi [email protected], [email protected] Designed by: NANDINI GRAPHICS,
Fatty Acid Oxidation Disorders Galactosemia Biotinidase Deficiency
 Fatty Acid Oxidation Disorders Galactosemia Biotinidase Deficiency Dr. Kathy Grange, MD Division of Genetics and Genomic Medicine Department of Pediatrics Washington University School of Medicine What
Fatty Acid Oxidation Disorders Galactosemia Biotinidase Deficiency Dr. Kathy Grange, MD Division of Genetics and Genomic Medicine Department of Pediatrics Washington University School of Medicine What
Liver Function Tests. Dr Stephen Butler Paediatric Advance Trainee TDHB
 Liver Function Tests Dr Stephen Butler Paediatric Advance Trainee TDHB Introduction Case presentation What is the liver? Overview of tests used to measure liver function RJ 10 month old European girl
Liver Function Tests Dr Stephen Butler Paediatric Advance Trainee TDHB Introduction Case presentation What is the liver? Overview of tests used to measure liver function RJ 10 month old European girl
NORD Guides for Physicians #1. Physician s Guide to. Tyrosinemia. Type 1
 NORD Guides for Physicians #1 The National Organization for Rare Disorders Physician s Guide to Tyrosinemia Type 1 The original version of this booklet was made possible by donations in honor of Danielle
NORD Guides for Physicians #1 The National Organization for Rare Disorders Physician s Guide to Tyrosinemia Type 1 The original version of this booklet was made possible by donations in honor of Danielle
The child with abnormal liver function tests
 The child with abnormal liver function tests Dr Jane Hartley Consultant Paediatric Hepatologist Birmingham Children s Hospital, UK 1 st Global Congress CIP, Paris 2011 Contents Over view of liver anatomy,
The child with abnormal liver function tests Dr Jane Hartley Consultant Paediatric Hepatologist Birmingham Children s Hospital, UK 1 st Global Congress CIP, Paris 2011 Contents Over view of liver anatomy,
Laboratory Monitoring of Adult Hospital Patients Receiving Parenteral Nutrition
 Laboratory Monitoring of Adult Hospital Patients Receiving Parenteral Nutrition Copy 1 Location of copies Web based only The following guideline is for use by medical staff caring for the patient and members
Laboratory Monitoring of Adult Hospital Patients Receiving Parenteral Nutrition Copy 1 Location of copies Web based only The following guideline is for use by medical staff caring for the patient and members
Acute Pancreatitis. Questionnaire. if yes: amount (cigarettes/day): since when (year): Drug consumption: yes / no if yes: type of drug:. amount:.
 The physical examination has to be done AT ADMISSION! The blood for laboratory parameters has to be drawn AT ADMISSION! This form has to be filled AT ADMISSION! Questionnaire Country: 1. Patient personal
The physical examination has to be done AT ADMISSION! The blood for laboratory parameters has to be drawn AT ADMISSION! This form has to be filled AT ADMISSION! Questionnaire Country: 1. Patient personal
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS
 Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
ETIOLOGIC CLASSIFICATION. Type I diabetes Type II diabetes
 DIABETES MELLITUS DEFINITION It is a common, chronic, metabolic syndrome characterized by hyperglycemia as a cardinal biochemical feature. Resulting from absolute lack of insulin. Abnormal metabolism of
DIABETES MELLITUS DEFINITION It is a common, chronic, metabolic syndrome characterized by hyperglycemia as a cardinal biochemical feature. Resulting from absolute lack of insulin. Abnormal metabolism of
OMG my LFT s! How to Interpret and Use Them. OMG my LFT s! OMG my LFT s!
 How to Interpret and Use Them René Romero, M.D. Clinical Director, Pediatric Hepatology CPG Gastroenterology, Hepatology and Nutrition Emory University School of Medicine Objectives Understand the anatomy
How to Interpret and Use Them René Romero, M.D. Clinical Director, Pediatric Hepatology CPG Gastroenterology, Hepatology and Nutrition Emory University School of Medicine Objectives Understand the anatomy
Liver, Gallbladder, Exocrine Pancreas KNH 406
 Liver, Gallbladder, Exocrine Pancreas KNH 406 2007 Thomson - Wadsworth LIVER Anatomy - functions With disease blood flow becomes obstructed Bile All bile drains into common hepatic duct Liver Bile complex
Liver, Gallbladder, Exocrine Pancreas KNH 406 2007 Thomson - Wadsworth LIVER Anatomy - functions With disease blood flow becomes obstructed Bile All bile drains into common hepatic duct Liver Bile complex
Approach to Abnormal Liver Tests
 Approach to Abnormal Liver Tests Naga P. Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of Gastroenterology and Hepatology Indiana University School
Approach to Abnormal Liver Tests Naga P. Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of Gastroenterology and Hepatology Indiana University School
Inborn Errors of Metabolism
 351 Inborn Errors of Metabolism Definition/ cut-off value Inherited metabolic disorders caused by a defect in the enzymes or their cofactors that metabolize protein, carbohydrate, or fat. Inborn errors
351 Inborn Errors of Metabolism Definition/ cut-off value Inherited metabolic disorders caused by a defect in the enzymes or their cofactors that metabolize protein, carbohydrate, or fat. Inborn errors
Liver Failure. Nora Aziz. www.3bv.org. Bones, Brains & Blood Vessels
 Liver Failure Nora Aziz www.3bv.org Bones, Brains & Blood Vessels Severe deterioration in liver function Looses ability to regenerate/repair decompensated Liver extensively damaged before it fails Equal
Liver Failure Nora Aziz www.3bv.org Bones, Brains & Blood Vessels Severe deterioration in liver function Looses ability to regenerate/repair decompensated Liver extensively damaged before it fails Equal
Chapter 25: Metabolism and Nutrition
 Chapter 25: Metabolism and Nutrition Chapter Objectives INTRODUCTION 1. Generalize the way in which nutrients are processed through the three major metabolic fates in order to perform various energetic
Chapter 25: Metabolism and Nutrition Chapter Objectives INTRODUCTION 1. Generalize the way in which nutrients are processed through the three major metabolic fates in order to perform various energetic
NUTRITION OF THE BODY
 5 Training Objectives:! Knowledge of the most important function of nutrients! Description of both, mechanism and function of gluconeogenesis! Knowledge of the difference between essential and conditionally
5 Training Objectives:! Knowledge of the most important function of nutrients! Description of both, mechanism and function of gluconeogenesis! Knowledge of the difference between essential and conditionally
Inborn Errors of Metabolism
 Intensive Care Nursery House Staff Manual Inborn Errors of Metabolism INTRODUCTION and PATHOPHYSIOLOGY: Inborn Errors of Metabolism (IEM) comprise a group of disorders in which a single gene defect causes
Intensive Care Nursery House Staff Manual Inborn Errors of Metabolism INTRODUCTION and PATHOPHYSIOLOGY: Inborn Errors of Metabolism (IEM) comprise a group of disorders in which a single gene defect causes
ICD-9-CM/ICD-10-CM Codes for MNT
 / Codes for MNT ICD (International Classification of Diseases) codes are used by physicians and medical coders to assign medical diagnoses to individual patients. It is not within the scope of practice
/ Codes for MNT ICD (International Classification of Diseases) codes are used by physicians and medical coders to assign medical diagnoses to individual patients. It is not within the scope of practice
NUTRITION IN LIVER DISEASES
 NUTRITION IN LIVER DISEASES 1. HEPATITIS: Definition: - Viral inflammation of liver cells. Types: a. HAV& HEV, transmitted by fecal-oral route. b. HBV & HCV, transmitted by blood and body fluids. c. HDV
NUTRITION IN LIVER DISEASES 1. HEPATITIS: Definition: - Viral inflammation of liver cells. Types: a. HAV& HEV, transmitted by fecal-oral route. b. HBV & HCV, transmitted by blood and body fluids. c. HDV
LIVER CANCER AND TUMOURS
 LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
Indications in Hepatology and Liver Diseases
 exclusively working in Health Care sananet GmbH Tilo Stolzke Breite Str. 6-8 23562 Lübeck Germany Telefon : +49 451 400 8301 Telefax : +49 451 400 8302 E-Mail : [email protected] Internet : www.sananet.com
exclusively working in Health Care sananet GmbH Tilo Stolzke Breite Str. 6-8 23562 Lübeck Germany Telefon : +49 451 400 8301 Telefax : +49 451 400 8302 E-Mail : [email protected] Internet : www.sananet.com
What to do with abnormal LFTs? Andrew M Smith Hepatobiliary Surgeon
 What to do with abnormal LFTs? Andrew M Smith Hepatobiliary Surgeon "it looks like there's something wrong.with your television set. Matt Groenig, creator of The Simpsons Probability of an abnormal screening
What to do with abnormal LFTs? Andrew M Smith Hepatobiliary Surgeon "it looks like there's something wrong.with your television set. Matt Groenig, creator of The Simpsons Probability of an abnormal screening
Diabetes mellitus. Lecture Outline
 Diabetes mellitus Lecture Outline I. Diagnosis II. Epidemiology III. Causes of diabetes IV. Health Problems and Diabetes V. Treating Diabetes VI. Physical activity and diabetes 1 Diabetes Disorder characterized
Diabetes mellitus Lecture Outline I. Diagnosis II. Epidemiology III. Causes of diabetes IV. Health Problems and Diabetes V. Treating Diabetes VI. Physical activity and diabetes 1 Diabetes Disorder characterized
1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net
 1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net Diabetes Mellitus (in cats) Diabetes, sugar Affected Animals: Most diabetic cats are older than 10 years of age when they are
1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net Diabetes Mellitus (in cats) Diabetes, sugar Affected Animals: Most diabetic cats are older than 10 years of age when they are
Wilson Disease. National Digestive Diseases Information Clearinghouse
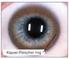 Wilson Disease National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Wilson disease? Wilson disease is a genetic disorder
Wilson Disease National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Wilson disease? Wilson disease is a genetic disorder
Bile Duct Diseases and Problems
 Bile Duct Diseases and Problems Introduction A bile duct is a tube that carries bile between the liver and gallbladder and the intestine. Bile is a substance made by the liver that helps with digestion.
Bile Duct Diseases and Problems Introduction A bile duct is a tube that carries bile between the liver and gallbladder and the intestine. Bile is a substance made by the liver that helps with digestion.
Enzyme Replacement Therapies for UCD (Liver/ Liver Cell / Stem Cell Transplantation) Pat McKiernan Birmingham Children s Hospital
 Enzyme Replacement Therapies for UCD (Liver/ Liver Cell / Stem Cell Transplantation) Pat McKiernan Birmingham Children s Hospital Survival following liver transplantation for Biliary Atresia at BCH (n=195)
Enzyme Replacement Therapies for UCD (Liver/ Liver Cell / Stem Cell Transplantation) Pat McKiernan Birmingham Children s Hospital Survival following liver transplantation for Biliary Atresia at BCH (n=195)
Organic Acid Disorders
 Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Cystic Fibrosis. Cystic fibrosis affects various systems in children and young adults, including the following:
 Cystic Fibrosis What is cystic fibrosis? Cystic fibrosis (CF) is an inherited disease characterized by an abnormality in the glands that produce sweat and mucus. It is chronic, progressive, and is usually
Cystic Fibrosis What is cystic fibrosis? Cystic fibrosis (CF) is an inherited disease characterized by an abnormality in the glands that produce sweat and mucus. It is chronic, progressive, and is usually
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
The Liver and Alpha-1. Antitrypsin Deficiency (Alpha-1) 1 ALPHA-1 FOUNDATION
 The Liver and Alpha-1 Antitrypsin Deficiency (Alpha-1) 1 ALPHA-1 FOUNDATION What Is Alpha-1 Antitrypsin Deficiency? Alpha-1 is a condition that may result in serious lung disease in adults and/or liver
The Liver and Alpha-1 Antitrypsin Deficiency (Alpha-1) 1 ALPHA-1 FOUNDATION What Is Alpha-1 Antitrypsin Deficiency? Alpha-1 is a condition that may result in serious lung disease in adults and/or liver
Liver Function Essay
 Liver Function Essay Name: Quindoline Ntui Date: April 20, 2009 Professor: Dr. Danil Hammoudi Class: Anatomy and Physiology 2 Liver function The human body consist of many highly organize part working
Liver Function Essay Name: Quindoline Ntui Date: April 20, 2009 Professor: Dr. Danil Hammoudi Class: Anatomy and Physiology 2 Liver function The human body consist of many highly organize part working
Patterns of abnormal LFTs and their differential diagnosis
 Patterns of abnormal LFTs and their differential diagnosis Professor Matthew Cramp South West Liver Unit and Peninsula Schools of Medicine and Dentistry, Plymouth Summary liver function / liver function
Patterns of abnormal LFTs and their differential diagnosis Professor Matthew Cramp South West Liver Unit and Peninsula Schools of Medicine and Dentistry, Plymouth Summary liver function / liver function
Liver, Gallbladder and Pancreas diseases. Premed 2 Pathophysiology
 Liver, Gallbladder and Pancreas diseases Premed 2 Pathophysiology Pancreas Pancreatitis Acute Pancreatitis Autodigestion of the pancreas due to activation of the enzymes Hemorrhagic fat necrosis, calcium
Liver, Gallbladder and Pancreas diseases Premed 2 Pathophysiology Pancreas Pancreatitis Acute Pancreatitis Autodigestion of the pancreas due to activation of the enzymes Hemorrhagic fat necrosis, calcium
X-Plain Hypoglycemia Reference Summary
 X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
Newborn Screening Update for Health Care Practitioners
 Newborn Screening Update for Health Care Practitioners Changes in regulations affecting your practice for newborns transferred to neonatal intensive care units. Changes for newborn screening of premature,
Newborn Screening Update for Health Care Practitioners Changes in regulations affecting your practice for newborns transferred to neonatal intensive care units. Changes for newborn screening of premature,
Routine Investigations for Liver Disease a guide
 fighting childhood liver disease Routine Investigations for Liver Disease a guide Medical Information Series Welcome This leaflet has been written specifically for: Parents/carers of a child with a liver
fighting childhood liver disease Routine Investigations for Liver Disease a guide Medical Information Series Welcome This leaflet has been written specifically for: Parents/carers of a child with a liver
School-age child 5-1 THE BLOOD
 C A S E S T U D Y 5 : School-age child Adapted from Thomson Delmar Learning s Case Study Series: Pediatrics, by Bonita E. Broyles, RN, BSN, MA, PhD. Copyright 2006 Thomson Delmar Learning, Clifton Park,
C A S E S T U D Y 5 : School-age child Adapted from Thomson Delmar Learning s Case Study Series: Pediatrics, by Bonita E. Broyles, RN, BSN, MA, PhD. Copyright 2006 Thomson Delmar Learning, Clifton Park,
LCD for Viral Hepatitis Serology Tests
 LCD for Viral Hepatitis Serology Tests Applicable CPT Code(s): 86692 Antibody; Hepatitis, Delta Agent 86704 Hepatitis B Core Antibody (HBcAb); Total 86705 Hepatitis B Core Antibody (HBcAb); IgM Antibody
LCD for Viral Hepatitis Serology Tests Applicable CPT Code(s): 86692 Antibody; Hepatitis, Delta Agent 86704 Hepatitis B Core Antibody (HBcAb); Total 86705 Hepatitis B Core Antibody (HBcAb); IgM Antibody
Fatty Acid Oxidation Disorder Case Study by Muhammad Ali Pervaiz, MD Clinical Biochemical Genetics Fellow.
 Fatty Acid Oxidation Disorder Case Study by Muhammad Ali Pervaiz, MD Clinical Biochemical Genetics Fellow. FOD/OAA Family Support Groups National Metabolic Conference Atlanta, Georgia July 30 & 31, 2010
Fatty Acid Oxidation Disorder Case Study by Muhammad Ali Pervaiz, MD Clinical Biochemical Genetics Fellow. FOD/OAA Family Support Groups National Metabolic Conference Atlanta, Georgia July 30 & 31, 2010
The Family Library. Understanding Diabetes
 The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
Causes, incidence, and risk factors
 Causes, incidence, and risk factors Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both. To understand diabetes,
Causes, incidence, and risk factors Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both. To understand diabetes,
Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both.
 Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Evaluation and Prognosis of Patients with Cirrhosis
 Evaluation and Prognosis of Patients with Cirrhosis Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded
Evaluation and Prognosis of Patients with Cirrhosis Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded
Hepatic Encephalopathy, Hyperammonemia, and Current Treatment in ICU Room
 Hepatic Encephalopathy, Hyperammonemia, and Current Treatment in ICU Room Assoc.Prof. Chan Sovandy Chairman by : Prof.So Saphy and Assoc Prof, Kim chhoung Hepatic Encephalopathy Hepatic (portal systemic
Hepatic Encephalopathy, Hyperammonemia, and Current Treatment in ICU Room Assoc.Prof. Chan Sovandy Chairman by : Prof.So Saphy and Assoc Prof, Kim chhoung Hepatic Encephalopathy Hepatic (portal systemic
Diabetic Emergencies. David Hill, D.O.
 Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
Is Insulin Effecting Your Weight Loss and Your Health?
 Is Insulin Effecting Your Weight Loss and Your Health? Teressa Alexander, M.D., FACOG Women s Healthcare Associates www.rushcopley.com/whca 630-978-6886 Obesity is Epidemic in the US 2/3rds of U.S. adults
Is Insulin Effecting Your Weight Loss and Your Health? Teressa Alexander, M.D., FACOG Women s Healthcare Associates www.rushcopley.com/whca 630-978-6886 Obesity is Epidemic in the US 2/3rds of U.S. adults
Cardiovascular diseases. pathology
 Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
NURSING GUIDELINES FOR MANAGEMENT OF CHILDREN WITH FATTY ACID OXIDATION DEFECT
 NURSING GUIDELINES FOR MANAGEMENT OF CHILDREN WITH FATTY ACID OXIDATION DEFECT National Centre for Inherited Metabolic Disorders 2.1 NURSING GUIDELINES FOR MANAGEMENT OF CHILDREN WITH FATTY ACID OXIDATION
NURSING GUIDELINES FOR MANAGEMENT OF CHILDREN WITH FATTY ACID OXIDATION DEFECT National Centre for Inherited Metabolic Disorders 2.1 NURSING GUIDELINES FOR MANAGEMENT OF CHILDREN WITH FATTY ACID OXIDATION
MANAGEMENT OF LIVER CIRRHOSIS
 MANAGEMENT OF LIVER CIRRHOSIS Information Leaflet Your Health. Our Priority. Page 2 of 6 What is cirrhosis? Cirrhosis is a result of long-term, continuous damage to the liver and may be due to many different
MANAGEMENT OF LIVER CIRRHOSIS Information Leaflet Your Health. Our Priority. Page 2 of 6 What is cirrhosis? Cirrhosis is a result of long-term, continuous damage to the liver and may be due to many different
INITIATING ORAL AUBAGIO (teriflunomide) THERAPY
 FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
Bariatric Patients, Nutritional Intervention for
 SKILL COMPETENCY CHECKLIST Bariatric Patients, Nutritional Intervention for Link to Dietitian Practice and Skill Standard Met/Initials Prerequisite Skills Competency Areas Knowledge of how to conduct a
SKILL COMPETENCY CHECKLIST Bariatric Patients, Nutritional Intervention for Link to Dietitian Practice and Skill Standard Met/Initials Prerequisite Skills Competency Areas Knowledge of how to conduct a
PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY. 12a. FOCUS ON Your Risk for Diabetes. Copyright 2011 Pearson Education, Inc.
 PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY 12a FOCUS ON Your Risk for Diabetes Your Risk for Diabetes! Since 1980,Diabetes has increased by 50 %. Diabetes has increased by 70 percent
PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY 12a FOCUS ON Your Risk for Diabetes Your Risk for Diabetes! Since 1980,Diabetes has increased by 50 %. Diabetes has increased by 70 percent
Newborn Screening Test
 Important Information for Parents about the Newborn Screening Test Newborn Screening Branch Genetic Disease Screening Program http://cdph.ca.gov/nbs California Department of Public Health Publication Date:
Important Information for Parents about the Newborn Screening Test Newborn Screening Branch Genetic Disease Screening Program http://cdph.ca.gov/nbs California Department of Public Health Publication Date:
1 ALPHA-1. The Liver and Alpha-1 Antitrypsin Deficiency (Alpha-1) FOUNDATION FOUNDATION. A patient s guide to Alpha-1 liver disease
 The Liver and Alpha-1 Antitrypsin Deficiency (Alpha-1) 1 ALPHA-1 FOUNDATION The Alpha-1 Foundation is committed to finding a cure for Alpha-1 Antitrypsin Deficiency and to improving the lives of people
The Liver and Alpha-1 Antitrypsin Deficiency (Alpha-1) 1 ALPHA-1 FOUNDATION The Alpha-1 Foundation is committed to finding a cure for Alpha-1 Antitrypsin Deficiency and to improving the lives of people
How To Treat A Diabetic Coma With Tpn
 GUIDELINES FOR TOTAL PARENTERAL NUTRITION (TPN) IN ADULT BONE MARROW TRANSPLANT PATIENTS TPN Indications TPN is indicated for any patient who is not expected to eat sufficiently for 3-5 days in severe
GUIDELINES FOR TOTAL PARENTERAL NUTRITION (TPN) IN ADULT BONE MARROW TRANSPLANT PATIENTS TPN Indications TPN is indicated for any patient who is not expected to eat sufficiently for 3-5 days in severe
Alanine aminotransferase (serum, plasma)
 Alanine aminotransferase (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Alanine aminotransferase (ALT) 1.2 Alternative names Systematic name L alanine:2 oxoglutarate aminotransferase
Alanine aminotransferase (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Alanine aminotransferase (ALT) 1.2 Alternative names Systematic name L alanine:2 oxoglutarate aminotransferase
Investigation and treatment of liver disease with acute onset Local hospital protocol
 Alastair Baker Page 1 9/7/2013 Investigation and treatment of liver disease with acute onset Local hospital protocol Defined as EITHER sudden onset of jaundice with evidence of liver aetiology OR incidental
Alastair Baker Page 1 9/7/2013 Investigation and treatment of liver disease with acute onset Local hospital protocol Defined as EITHER sudden onset of jaundice with evidence of liver aetiology OR incidental
NP/PA Clinical Hepatology Fellowship Summary of Year-Long Curriculum
 OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
Developmental delay and Cerebral palsy. Present the differential diagnosis of developmental delay.
 Developmental delay and Cerebral palsy objectives 1. developmental delay Define developmental delay Etiologies of developmental delay Present the differential diagnosis of developmental delay. 2. cerebral
Developmental delay and Cerebral palsy objectives 1. developmental delay Define developmental delay Etiologies of developmental delay Present the differential diagnosis of developmental delay. 2. cerebral
EFFIMET 1000 XR Metformin Hydrochloride extended release tablet
 BRAND NAME: Effimet XR. THERAPEUTIC CATEGORY: Anti-Diabetic PHARMACOLOGIC CLASS: Biguanides EFFIMET 1000 XR Metformin Hydrochloride extended release tablet COMPOSITION AND PRESENTATION Composition Each
BRAND NAME: Effimet XR. THERAPEUTIC CATEGORY: Anti-Diabetic PHARMACOLOGIC CLASS: Biguanides EFFIMET 1000 XR Metformin Hydrochloride extended release tablet COMPOSITION AND PRESENTATION Composition Each
EXECUTIVE BLOOD WORK PANEL
 EXECUTIVE BLOOD WORK PANEL Below is a list of all blood and urine testing done on the day of your Executive Medical. MALE Serum Glucose Random Serum Glucose Fasting Creatinine Uric Acid Sodium Potassium
EXECUTIVE BLOOD WORK PANEL Below is a list of all blood and urine testing done on the day of your Executive Medical. MALE Serum Glucose Random Serum Glucose Fasting Creatinine Uric Acid Sodium Potassium
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
LIVER FUNCTION TESTS
 MODULE Liver Function Tests 17 LIVER FUNCTION TESTS 17.1 INTRODUCTION Liver function tests are a group of tests done to assess the functional capacity of the liver as well as any cellular damage to the
MODULE Liver Function Tests 17 LIVER FUNCTION TESTS 17.1 INTRODUCTION Liver function tests are a group of tests done to assess the functional capacity of the liver as well as any cellular damage to the
Diagnostics: Page 2 of 5
 Proteinuria Proteinuria is a condition in which there are increased amounts of protein in the urine. There are a number of different diseases which can result in proteinuria. In the early stages of the
Proteinuria Proteinuria is a condition in which there are increased amounts of protein in the urine. There are a number of different diseases which can result in proteinuria. In the early stages of the
Neonatal Hypotonia. Clinical Approach to Floppy Baby
 Neonatal Hypotonia Clinical Approach to Floppy Baby Hypotonia in the newborn is a common presenting feature of systemic illness or neurologic dysfunction at any level of the central or peripheral nervous
Neonatal Hypotonia Clinical Approach to Floppy Baby Hypotonia in the newborn is a common presenting feature of systemic illness or neurologic dysfunction at any level of the central or peripheral nervous
DIAGNOSING CHILDHOOD MUSCULAR DYSTROPHIES
 DIAGNOSING CHILDHOOD MUSCULAR DYSTROPHIES Extracts from a review article by KN North and KJ Jones: Recent advances in diagnosis of the childhood muscular dystrophies Journal of Paediatrics and Child Health
DIAGNOSING CHILDHOOD MUSCULAR DYSTROPHIES Extracts from a review article by KN North and KJ Jones: Recent advances in diagnosis of the childhood muscular dystrophies Journal of Paediatrics and Child Health
Things You Don t Want to Miss in Multiple Myeloma
 Things You Don t Want to Miss in Multiple Myeloma Sreenivasa Chandana, MD, PhD Attending Hematologist and Medical Oncologist West Michigan Cancer Center Assistant Professor, Western Michigan University
Things You Don t Want to Miss in Multiple Myeloma Sreenivasa Chandana, MD, PhD Attending Hematologist and Medical Oncologist West Michigan Cancer Center Assistant Professor, Western Michigan University
DIABETES MELLITUS. By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria
 DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
Part I Failure to Thrive
 Part I Failure to Thrive Emma and Jacob Miller were so excited at the birth of their baby Matthew. Jacob, he s just so perfect! Just one problem though, it looks like he has your hairline! Emma teased
Part I Failure to Thrive Emma and Jacob Miller were so excited at the birth of their baby Matthew. Jacob, he s just so perfect! Just one problem though, it looks like he has your hairline! Emma teased
Key Facts about Influenza (Flu) & Flu Vaccine
 Key Facts about Influenza (Flu) & Flu Vaccine mouths or noses of people who are nearby. Less often, a person might also get flu by touching a surface or object that has flu virus on it and then touching
Key Facts about Influenza (Flu) & Flu Vaccine mouths or noses of people who are nearby. Less often, a person might also get flu by touching a surface or object that has flu virus on it and then touching
Hepatitis C. Laboratory Tests and Hepatitis C
 Hepatitis C Laboratory Tests and Hepatitis C If you have hepatitis C, your doctor will use laboratory tests to check your health. This handout will help you understand what the major tests are and what
Hepatitis C Laboratory Tests and Hepatitis C If you have hepatitis C, your doctor will use laboratory tests to check your health. This handout will help you understand what the major tests are and what
1. What has a higher stored energy potential per gram, glycogen or triglycerides? Explain.
 Lipid Metabolism 1. What has a higher stored energy potential per gram, glycogen or triglycerides? Explain. 2. How can excess acetyl CoA trapped in the mitochondria, be utilized as a substrate for fatty
Lipid Metabolism 1. What has a higher stored energy potential per gram, glycogen or triglycerides? Explain. 2. How can excess acetyl CoA trapped in the mitochondria, be utilized as a substrate for fatty
DIABETES A chronic, debilitating and often deadly disease A global epidemic Diabetes in Africa
 DIABETES A chronic, debilitating and often deadly disease Diabetes is a chronic condition that arises when the pancreas does not produce enough insulin, or when the body cannot effectively use the insulin
DIABETES A chronic, debilitating and often deadly disease Diabetes is a chronic condition that arises when the pancreas does not produce enough insulin, or when the body cannot effectively use the insulin
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only)
 PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only) 1. What is the main problem that you are having? (If additional space is required, please use the back of this
PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only) 1. What is the main problem that you are having? (If additional space is required, please use the back of this
Evaluation of a Child with Elevated Transaminases. Linda V. Muir, M.D. April 11, 2008 Northwest Pediatric Liver Disease Symposium
 Evaluation of a Child with Elevated Transaminases Linda V. Muir, M.D. April 11, 2008 Northwest Pediatric Liver Disease Symposium Disclosures I do not have a financial interest, arrangement or affiliation
Evaluation of a Child with Elevated Transaminases Linda V. Muir, M.D. April 11, 2008 Northwest Pediatric Liver Disease Symposium Disclosures I do not have a financial interest, arrangement or affiliation
95% of childhood kidney cancer cases are Wilms tumours. Childhood kidney cancer is extremely rare, with only 90 cases a year in
 James Whale Fund for Kidney Cancer Childhood kidney cancer factsheet Kidney cancer rarely afflicts children and about 90 paediatric cases are diagnosed in the UK each year. About 75% of childhood kidney
James Whale Fund for Kidney Cancer Childhood kidney cancer factsheet Kidney cancer rarely afflicts children and about 90 paediatric cases are diagnosed in the UK each year. About 75% of childhood kidney
Endocrine issues in FA SUSAN R. ROSE CINCINNATI CHILDREN S HOSPITAL MEDICAL CENTER
 Endocrine issues in FA SUSAN R. ROSE CINCINNATI CHILDREN S HOSPITAL MEDICAL CENTER 80% of children and adults with FA have an endocrine abnormality Endocrine cells make a hormone (message) Carried in bloodstream
Endocrine issues in FA SUSAN R. ROSE CINCINNATI CHILDREN S HOSPITAL MEDICAL CENTER 80% of children and adults with FA have an endocrine abnormality Endocrine cells make a hormone (message) Carried in bloodstream
APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES. Appendix 5 166
 APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES Appendix 5 166 CORE CURRICULUM IN CHILD HEALTH This document is a guide for undergraduates, and summarises the key knowledge, skills and attitudes that it is
APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES Appendix 5 166 CORE CURRICULUM IN CHILD HEALTH This document is a guide for undergraduates, and summarises the key knowledge, skills and attitudes that it is
INTRODUCTION Thrombophilia deep vein thrombosis DVT pulmonary embolism PE inherited thrombophilia
 INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
ARTICLE #1 PLEASE RETURN AT THE END OF THE HOUR
 ARTICLE #1 PLEASE RETURN AT THE END OF THE HOUR Alcoholism By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/alcoholism/ds00340 Definition Alcoholism is a chronic and often progressive
ARTICLE #1 PLEASE RETURN AT THE END OF THE HOUR Alcoholism By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/alcoholism/ds00340 Definition Alcoholism is a chronic and often progressive
Nutrition. Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT
 1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
Service Definition with all Clinical Terms Service: Laprascopic Cholecystectomy Clinic (No Gallstones in bile duct)
 Service Definition with all Clinical Terms Service: Laprascopic Cholecystectomy Clinic (No Gallstones in bile duct) Section 1 Service Details Service ID: 7540540 Service Comments: Referrer Alert: Service
Service Definition with all Clinical Terms Service: Laprascopic Cholecystectomy Clinic (No Gallstones in bile duct) Section 1 Service Details Service ID: 7540540 Service Comments: Referrer Alert: Service
Preoperative Laboratory and Diagnostic Studies
 Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Disclosures. Interpreting Liver Tests: What Do They Mean? Liver Function Tests. Objectives. Common Tests. Case 1
 Disclosures Interpreting Liver Tests: What Do They Mean? I have no financial disclosures to make. Roman Perri, MD Vanderbilt University Medical Center Nashville, TN Objectives Discuss tests commonly used
Disclosures Interpreting Liver Tests: What Do They Mean? I have no financial disclosures to make. Roman Perri, MD Vanderbilt University Medical Center Nashville, TN Objectives Discuss tests commonly used
X-Plain Diabetes - Introduction Reference Summary
 X-Plain Diabetes - Introduction Reference Summary Introduction Diabetes is a disease that affects millions of Americans every year. Your doctor may have informed you that you have diabetes. Although there
X-Plain Diabetes - Introduction Reference Summary Introduction Diabetes is a disease that affects millions of Americans every year. Your doctor may have informed you that you have diabetes. Although there
Diseases of peritoneum Lect. Al Qassim University, Faculty of Medicine Phase II Year III, CMD 332 Pathology Department 31-32
 Diseases of peritoneum Lect Al Qassim University, Faculty of Medicine Phase II Year III, CMD 332 Pathology Department 31-32 Describe the etiology, pathogenesis and types of peritonitis Define ascites and
Diseases of peritoneum Lect Al Qassim University, Faculty of Medicine Phase II Year III, CMD 332 Pathology Department 31-32 Describe the etiology, pathogenesis and types of peritonitis Define ascites and
Life Insurance Application Form
 Life Insurance Application Form INSTRUCTION To be completed by all applicants PERSONAL DETAILS Surname First name Middle name Sex Female Male Marital status (please tick) Single Married Other Current residential
Life Insurance Application Form INSTRUCTION To be completed by all applicants PERSONAL DETAILS Surname First name Middle name Sex Female Male Marital status (please tick) Single Married Other Current residential
INTRODUCTION Thrombophilia deep vein thrombosis DVT pulmonary embolism PE inherited thrombophilia
 INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS
 WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS This is a patient information booklet providing specific practical information about gall bladder polyps in brief. Its aim is to provide the patient
WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS This is a patient information booklet providing specific practical information about gall bladder polyps in brief. Its aim is to provide the patient
PPS UNDERWRITING GUIDE FOR APPLICANTS
 PPS UNDERWRITING GUIDE FOR APPLICANTS UNDERWRITING guide 2013 WHAT HAPPENS WHEN YOU SUBMIT YOUR APPLICATION FOR INSURANCE? Once an application is submitted it is put through a number of processes to ensure
PPS UNDERWRITING GUIDE FOR APPLICANTS UNDERWRITING guide 2013 WHAT HAPPENS WHEN YOU SUBMIT YOUR APPLICATION FOR INSURANCE? Once an application is submitted it is put through a number of processes to ensure
LIVER FUNCTION TESTS
 LIVER FUNCTION TESTS University of PNG School of Medicine and Health Sciences, Division of Basic Medical Sciences, Discipline of Biochemistry & Molecular Biology VJ Temple 1 What are some of the functions
LIVER FUNCTION TESTS University of PNG School of Medicine and Health Sciences, Division of Basic Medical Sciences, Discipline of Biochemistry & Molecular Biology VJ Temple 1 What are some of the functions
HEPATIC ENCEPHALOPATHY
 HEPATIC ENCEPHALOPATHY Jan Albrecht Department of Neurotoxicology, Medical Research Centre, Polish Academy of Sciences, Warsaw, Poland Brussels, July 14, 2009 DEFINITIONS: - HEPATIC ENCEPHALOPATHY (HE)
HEPATIC ENCEPHALOPATHY Jan Albrecht Department of Neurotoxicology, Medical Research Centre, Polish Academy of Sciences, Warsaw, Poland Brussels, July 14, 2009 DEFINITIONS: - HEPATIC ENCEPHALOPATHY (HE)
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
