Rheumatoid arthritis (RA) is the
|
|
|
- Morgan Copeland
- 10 years ago
- Views:
Transcription
1 Diagnosis and Management of Rheumatoid Arthritis AMY M. WASSERMAN, MD, Boston University School of Medicine, Boston, Massachusetts Rheumatoid arthritis is the most commonly diagnosed systemic inflammatory arthritis. Women, smokers, and those with a family history of the disease are most often affected. Criteria for diagnosis include having at least one joint with definite swelling that is not explained by another disease. The likelihood of a rheumatoid arthritis diagnosis increases with the number of small joints involved. In a patient with inflammatory arthritis, the presence of a rheumatoid factor or anti-citrullinated protein antibody, or elevated C-reactive protein level or erythrocyte sedimentation rate suggests a diagnosis of rheumatoid arthritis. Initial laboratory evaluation should also include complete blood count with differential and assessment of renal and hepatic function. Patients taking biologic agents should be tested for hepatitis B, hepatitis C, and tuberculosis. Earlier diagnosis of rheumatoid arthritis allows for earlier treatment with diseasemodifying antirheumatic agents. Combinations of medications are often used to control the disease. Methotrexate is typically the first-line drug for rheumatoid arthritis. Biologic agents, such as tumor necrosis factor inhibitors, are generally considered second-line agents or can be added for dual therapy. The goals of treatment include minimization of joint pain and swelling, prevention of radiographic damage and visible deformity, and continuation of work and personal activities. Joint replacement is indicated for patients with severe joint damage whose symptoms are poorly controlled by medical management. (Am Fam Physician. 2011;84(11): Copyright 2011 American Academy of Family Physicians.) Patient information: A handout on this topic is available at doctor.org/876. Rheumatoid arthritis (RA) is the most common inflammatory arthritis, with a lifetime prevalence of up to 1 percent worldwide. 1 Onset can occur at any age, but peaks between 30 and 50 years. 2 Disability is common and significant. In a large U.S. cohort, 35 percent of patients with RA had work disability after 10 years. 3 Etiology and Pathophysiology Like many autoimmune diseases, the etiology of RA is multifactorial. Genetic susceptibility is evident in familial clustering and monozygotic twin studies, with 50 percent of RA risk attributable to genetic factors. 4 Genetic associations for RA include human leukocyte antigen-dr4 5 and -DRB1, and a variety of alleles called the shared epitope. 6,7 Genome-wide association studies have identified additional genetic signatures that increase the risk of RA and other autoimmune diseases, including STAT4 gene and CD40 locus. 5 Smoking is the major environmental trigger for RA, especially in those with a genetic predisposition. 8 Although infections may unmask an autoimmune response, no particular pathogen has been proven to cause RA. 9 RA is characterized by inflammatory pathways that lead to proliferation of synovial cells in joints. Subsequent pannus formation may lead to underlying cartilage destruction and bony erosions. Overproduction of proinflammatory cytokines, including tumor necrosis factor (TNF) and interleukin-6, drives the destructive process. 10 RISK FACTORS Older age, a family history of the disease, and female sex are associated with increased risk of RA, although the sex differential is less prominent in older patients. 1 Both current and prior cigarette smoking increases the risk of RA (relative risk [RR] = 1.4, up to 2.2 for more than 40-pack-year smokers). 11 Pregnancy often causes RA remission, likely because of immunologic tolerance. 12 Parity may have long-lasting impact; RA is less likely to be diagnosed in parous women than in nulliparous women (RR = 0.61). 13,14 Breastfeeding decreases the risk of RA (RR = 0.5 in women who breastfeed for at least 24 months), whereas early menarche Downloaded from the American Family Physician Web site at Copyright 2011 American Academy of Family Physicians. For the private, noncommercial December 1, use 2011 of one individual Volume user 84, of Number the Web 11 site. All other rights reserved. Contact [email protected] for copyright questions American and/or Family permission Physician requests. 1245
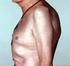
2 In addition, Dutch researchers have developed and validated a clinical prediction rule for RA (Table 2). 17,18 The purpose of this rule is to help identify patients with undifferentiated arthritis that is most likely to progress to RA, and to guide follow-up and referral. Figure 1. Boggy swelling in proximal interphalangeal and metacarpophalangeal joints (more prominent on patient s right hand) in a patient with new-onset rheumatoid arthritis. Note that with joint swelling, the skin creases over the proximal interphalangeal joints become less apparent. (RR = 1.3 for those with menarche at 10 years of age or younger) and very irregular menstrual periods (RR = 1.5) increase risk. 14 Use of oral contraceptive pills or vitamin E does not affect RA risk. 15 Diagnosis TYPICAL PRESENTATION Patients with RA typically present with pain and stiffness in multiple joints. The wrists, proximal interphalangeal joints, and metacarpophalangeal joints are most commonly involved. Morning stiffness lasting more than one hour suggests an inflammatory etiology. Boggy swelling due to synovitis may be visible (Figure 1), or subtle synovial thickening may be palpable on joint examination. Patients may also present with more indolent arthralgias before the onset of clinically apparent joint swelling. Systemic symptoms of fatigue, weight loss, and low-grade fever may occur with active disease. DIAGNOSTIC CRITERIA In 2010, the American College of Rheumatology and European League Against Rheumatism collaborated to create new classification criteria for RA (Table 1). 16 The new criteria are an effort to diagnose RA earlier in patients who may not meet the 1987 American College of Rheumatology classification criteria. The 2010 criteria do not include presence of rheumatoid nodules or radiographic erosive changes, both of which are less likely in early RA. Symmetric arthritis is also not required in the 2010 criteria, allowing for early asymmetric presentation. DIAGNOSTIC TESTS Autoimmune diseases such as RA are often characterized by the presence of autoantibodies. Rheumatoid factor is not specific for RA and may be present in patients with other diseases, such as hepatitis C, and in healthy older persons. Anti-citrullinated protein antibody is more specific for RA and may play a role in disease pathogenesis. 6 Approximately 50 to 80 percent of persons with RA have rheumatoid factor, anti-citrullinated protein antibody, or both. 10 Patients with RA may have a positive antinuclear antibody test result, and the test is of prognostic importance in juvenile forms of this disease. 19 C-reactive protein levels and erythrocyte sedimentation rate are often increased with active RA, and these acute phase reactants are part of the new RA classification criteria. 16 C-reactive protein levels and erythrocyte sedimentation rate may also be used to follow disease activity and response to medication. Baseline complete blood count with differential and assessment of renal and hepatic function are helpful because the results may influence treatment options (e.g., a patient with renal insufficiency or significant thrombocytopenia likely would not be prescribed a nonsteroidal antiinflammatory drug [NSAID]). Mild anemia of chronic disease occurs in 33 to 60 percent of all patients with RA, 20 although gastrointestinal blood loss should also be considered in patients taking corticosteroids or NSAIDs. Methotrexate is contraindicated in patients with hepatic disease, such as hepatitis C, and in patients with significant renal impairment. 21 Biologic therapy, such as a TNF inhibitor, requires a negative tuberculin test or treatment for latent tuberculosis. Hepatitis B reactivation can also occur with TNF inhibitor use. 22 Radiography of hands and feet should be performed to evaluate for characteristic periarticular erosive changes, 1246 American Family Physician Volume 84, Number 11 December 1, 2011
3 Table 1. The 2010 American College of Rheumatology/European League Against Rheumatism Classification Criteria for RA Target population (who should be tested?): patients who 1) have at least one joint with definite clinical synovitis (swelling)* 2) with the synovitis not better explained by another disease Classification criteria for RA (score-based algorithm: add score of categories A through D; a score of 6 out of 10 is needed for classification of a patient as having definite RA) A. Joint involvement One large joint 0 Two to 10 large joints 1 One to three small joints (with or without involvement of large joints) 2 Four to 10 small joints (with or without involvement of large joints) 3 > 10 joints (at least one small joint)** 5 B. Serology (at least one test result is needed for classification) Negative RF and negative ACPA 0 Low positive RF or low positive ACPA 2 High positive RF or high positive ACPA 3 C. Acute phase reactants (at least one test result is needed for classification) Normal CRP and normal ESR 0 Abnormal CRP or normal ESR 1 D. Duration of symptoms < six weeks 0 six weeks 1 Score ACPA = anti-citrullinated protein antibody; CRP = C-reactive protein; ESR = erythrocyte sedimentation rate; * The criteria are aimed at classification of newly presenting patients. In addition, patients with erosive disease typical of RA with a history compatible with prior fulfillment of the 2010 criteria should be classified as having RA. Patients with long-standing disease, including those whose disease is inactive (with or without treatment), who, based on retrospectively available data, have previously fulfilled the 2010 criteria should be classified as having RA. Differential diagnoses differ in patients with different presentations, but may include conditions such as systemic lupus erythematosus, psoriatic arthritis, and gout. If it is unclear about the relevant differential diagnoses to consider, an expert rheumatologist should be consulted. Although patients with a score of less than 6 out of 10 are not classifiable as having RA, their status can be re assessed, and the criteria might be fulfilled cumulatively over time. Joint involvement refers to any swollen or tender joint on examination, which may be confirmed by imaging evidence of synovitis. Distal interphalangeal joints, first carpometacarpal joints, and first metatarsophalangeal joints are excluded from assessment. Categories of joint distribution are classified according to the location and number of involved joints, with placement into the highest category possible based on the pattern of joint involvement. Large joints refers to shoulders, elbows, hips, knees, and ankles. Small joints refers to the metacarpophalangeal joints, proximal interphalangeal joints, second to fifth metatarsophalangeal joints, thumb interphalangeal joints, and wrists. ** In this category, at least one of the involved joints must be a small joint; the other joints can include any combination of large and additional small joints, as well as other joints not specifically listed elsewhere (e.g., temporomandibular, acromioclavicular, sternoclavicular). Negative refers to international unit values that are less than or equal to the upper limit of normal for the laboratory and assay; low positive refers to international unit values that are higher than the upper limit of normal but three or less times the upper limit of normal for the laboratory and assay; high positive refers to international unit values that are more than three times the upper limit of normal for the laboratory and assay. When rheumatoid factor information is only available as positive or negative, a positive result should be scored as low positive for rheumatoid factor. Normal/abnormal is determined by local laboratory standards. Duration of symptoms refers to patient self-report of the duration of signs or symptoms of synovitis (e.g., pain, swelling, tenderness) of joints that are clinically involved at the time of assessment, regardless of treatment status. Adapted with permission from Aletaha D, Neogi T, Silman AJ, et al rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative [published correction appears in Ann Rheum Dis. 2010;69(10):1892]. Ann Rheum Dis. 2010;69(9):1583. December 1, 2011 Volume 84, Number 11 American Family Physician 1247
4 Table 2. Clinical Rule for Predicting the Risk of RA in Patients with Undifferentiated Arthritis Patient characteristics which may be indicative of a more aggressive RA subtype. 10 DIFFERENTIAL DIAGNOSIS Points Age Years 0.02 Female sex 1.0 Distribution of affected joints (patients may receive points for more than one item) Small joints of hands or feet 0.5 Symmetric 0.5 Upper extremities 1.0 Upper and lower extremities 1.5 Score for morning stiffness on a 100-mm visual analog scale 26 to 90 mm 1.0 > 90 mm 2.0 Number of tender joints Four to Number of swollen joints Four to C-reactive protein level 5 to 50 mg per L (47.62 to nmol per L) mg per L ( nmol per L) 1.5 Positive for rheumatoid factor 1.0 Positive for anti-citrullinated protein antibody 2.0 Score* Number with RA Number without RA Likelihood ratio Total: 0 to to to * Score rounded to the nearest number ending in 0 or 0.5. Percentage with RA at one year Adapted with permission from van der Helm-van Mil AH, le Cessie S, van Dongen H, et al. A prediction rule for disease outcome in patients with recent-onset undifferentiated arthritis. Arthritis Rheum. 2007;56(2):436, with scoring information from reference 18. Skin findings suggest systemic lupus erythematosus, systemic sclerosis, or psoriatic arthritis. Polymyalgia rheumatica should be considered in an older patient with symptoms primarily in the shoulder and hip, and the patient should be asked questions related to associated temporal arteritis. Chest radiography is helpful to evaluate for sarcoidosis as an etiology of arthritis. Patients with inflammatory back symptoms, a history of inflammatory bowel disease, or inflammatory eye disease may have spondyloarthropathy. Persons with less than six weeks of symptoms may have a viral process, such as parvovirus. Recurrent self-limited episodes of acute joint swelling suggest crystal arthropathy, and arthrocentesis should be performed to evaluate for monosodium urate monohydrate or calcium pyrophosphate dihydrate crystals. The presence of numerous myofascial trigger points and somatic symptoms may suggest fibromyalgia, which can coexist with RA. To help guide diagnosis and determine treatment strategy, patients with inflammatory arthritis should be promptly referred to a rheumatology subspecialist. 16,17 Treatment After RA has been diagnosed and an initial evaluation performed, treatment should begin. Recent guidelines have addressed the management of RA, 21,22 but patient preference also plays an important role. There are special considerations for women of childbearing age because many medications have deleterious effects on pregnancy. Goals of therapy include minimizing joint pain and swelling, preventing deformity (such as ulnar deviation) and radiographic damage (such as erosions), maintaining quality of life (personal and work), and controlling extra-articular manifestations. Diseasemodifying antirheumatic drugs (DMARDs) are the mainstay of RA therapy. DMARDS DMARDs can be biologic or nonbiologic (Table 3). 23 Biologic agents include monoclonal antibodies and recombinant receptors to block cytokines that promote the inflammatory cascade responsible for RA symptoms. Methotrexate is recommended as the firstline treatment in patients with active RA, unless contraindicated or not tolerated. 21 Leflunomide (Arava) may be used as an alternative to methotrexate, although gastrointestinal adverse effects are more common. Sulfasalazine (Azulfidine) or hydroxychloroquine (Plaquenil) is recommended as monotherapy in patients with low disease 1248 American Family Physician Volume 84, Number 11 December 1, 2011
5 Table 3. Biologic and Nonbiologic Disease-Modifying Antirheumatic Drugs Rheumatoid Arthritis Drug* Mechanism for rheumatoid arthritis Adverse effects Monthly cost Nonbiologic More commonly used Methotrexate Inhibits dihydrofolate reductase Liver effects, teratogenesis, hair loss, oral ulcers $ Leflunomide (Arava) Inhibits pyrimidine synthesis Liver effects, gastrointestinal effects, teratogenesis $ Hydroxychloroquine (Plaquenil) Antimalarial, blocks toll-like receptors Rare ocular toxicity $$ Sulfasalazine (Azulfidine) Minocycline (Minocin) Less commonly used Gold sodium thiomalate Penicillamine (Cuprimine) Cyclophosphamide Cyclosporine (Sandimmune) Biologic Anti-TNF agents Folate depletion, other mechanisms unknown Antimicrobial, other mechanisms unknown Inhibits antigen processing, decreases cytokines (TNF, interleukin-6) Chelates metal, other mechanisms unknown Nitrogen mustard alkylating agent, cross-links DNA Calcineurin inhibitor, decreases interleukin-2 Anemia in G6PD deficiency, gastrointestinal effects Drug-induced lupus erythematosus, Clostridium difficile colitis Skin, heme, renal effects $$ Heme, renal effects $$ Infertility, cancer, hemorrhagic cystitis $$ Hypertension, renal effects, hirsutism $$ Adalimumab (Humira) Anti-TNF-α TB, opportunistic infection $$$ Certolizumab pegol (Cimzia) Anti-TNF-α, pegylated TB, opportunistic infection $$$ Etanercept (Enbrel) Anti-TNF-α, receptor TB, opportunistic infection $$$ Golimumab (Simponi) Anti-TNF-α TB, opportunistic infection $$$ Infliximab (Remicade) Anti-TNF-α TB, opportunistic infection, infusion reaction $$$ Other biologic agents Abatacept (Orencia) Costimulator blocker, cytotoxic T lymphocyte antigen 4 Opportunistic infection $$$ Anakinra (Kineret) Anti-interleukin-1 receptor blocker Opportunistic infection, injection site pain $$$ Rituximab (Rituxan) Anti-CD20, eliminates B cells Infusion reaction, opportunistic infection, progressive multifocal leukoencephalopathy Tocilizumab (Actemra) Anti-interleukin-6 receptor blocker Opportunistic infection $$$ $ $ $$$$ G6PD = glucose-6-phosphate dehydrogenase; TB = tuberculosis; TNF = tumor necrosis factor. * Nonbiologic drugs listed in approximate order of priority, biologic drugs listed in alphabetical order. $ = $30 to $100; $$ = $100 to $1,000; $$$ = $1,000 to $5,000; $$$$ = more than $5,000. Information from reference 23. activity or without poor prognostic features (e.g., seronegative, nonerosive RA). 21,22 Combination therapy with two or more DMARDs is more effective than monotherapy; however, adverse effects may also be greater. 24 If RA is not well controlled with a nonbiologic DMARD, a biologic DMARD should be initiated. 21,22 TNF inhibitors are the first-line biologic therapy and are the most studied of these agents. If TNF inhibitors are ineffective, additional biologic therapies can be considered. Simultaneous use of more than one biologic therapy (e.g., adalimumab [Humira] with abatacept [Orencia]) is not recommended because of an unacceptable rate of adverse effects. 21 NSAIDS AND CORTICOSTEROIDS Drug therapy for RA may involve NSAIDs and oral, intramuscular, or intra-articular corticosteroids for controlling pain and inflammation. Ideally, NSAIDs and corticosteroids are used only for short-term management. DMARDs are the preferred therapy. 21,22 COMPLEMENTARY THERAPIES Dietary interventions, including vegetarian and Mediterranean diets, have been December 1, 2011 Volume 84, Number 11 American Family Physician 1249
6 Table 4. Extra-Articular Manifestations of RA Manifestation Characteristics Cardiac Accelerated atherosclerosis Pericarditis Eye Episcleritis/scleritis Keratoconjunctivitis sicca Peripheral ulcerative keratitis Hematologic Amyloidosis Felty syndrome Nervous system Cervical myelopathy Neuropathy Pulmonary Caplan syndrome Interstitial lung disease Pleural effusion Pulmonary nodules Skin Rheumatoid nodules Vasculitis Leading cause of death in patients with RA Present in 30 to 50 percent of persons with RA on autopsy, rarely leads to tamponade Acute, red, painful eye; occurs in less than 1 percent of patients with RA Secondary Sjögren syndrome, dry mouth may also occur More severe scleritis, if untreated can perforate anterior chamber Caused by chronic inflammation Splenomegaly, neutropenia, and thrombocytopenia Caused by C1-C2 subluxation, seen on flexionextension radiography Carpal tunnel, mononeuritis multiplex (foot drop) Nodules and pneumoconiosis (e.g., in coal miners) May resemble bronchiolitis obliterans with organizing pneumonia, idiopathic pulmonary fibrosis, patient may also have pulmonary arterial hypertension Exudative effusion with markedly low glucose level Can be asymptomatic Information from references 1, 2, and 10. Firm or rubbery, located on pressure areas (e.g., olecranon) Poor prognosis, increased mortality, rare but occurs with severe RA (i.e., erosive, deforming, and seropositive disease) studied in the treatment of RA without convincing evidence of benefit. 25,26 Despite some favorable outcomes, there is a lack of evidence for the effectiveness of acupuncture in placebo-controlled trials of patients with RA. 27,28 In addition, thermotherapy and therapeutic ultrasound for RA have not been studied adequately. 29,30 A Cochrane review of herbal treatments for RA concluded that gamma-linolenic acid (from evening primrose or black currant seed oil) and Tripterygium wilfordii (thunder god vine) have potential benefits. 31 It is important to inform patients that serious adverse effects have been reported with use of herbal therapy. 31 EXERCISE AND PHYSICAL THERAPY Results of randomized controlled trials support physical exercise to improve quality of life and muscle strength in patients with RA. 32,33 Exercise training programs have not been shown to have deleterious effects on RA disease activity, pain scores, or radiographic joint damage. 34 Tai chi has been shown to improve ankle range of motion in persons with RA, although randomized trials are limited. 35 Randomized controlled trials of Iyengar yoga in young adults with RA are underway. 36 DURATION OF TREATMENT Remission is obtainable in 10 to 50 percent of patients with RA, depending on how remission is defined and the intensity of therapy. 10 Remission is more likely in males, nonsmokers, persons younger than 40 years, and in those with late-onset disease (patients older than 65 years), with shorter duration of disease, with milder disease activity, without elevated acute phase reactants, and without positive rheumatoid factor or anticitrullinated protein antibody findings. 37 After the disease is controlled, medication dosages may be cautiously decreased to the minimum amount necessary. Patients will require frequent monitoring to ensure stable symptoms, and prompt increase in medication is recommended with disease flare-ups. 22 JOINT REPLACEMENT Joint replacement is indicated when there is severe joint damage and unsatisfactory control of symptoms with medical management. Long-term outcomes are good, with only 4 to 13 percent of large joint replacements requiring revision within 10 years. 38 The hip and knee are the most commonly replaced joints. Long-term Monitoring Although RA is considered a disease of the joints, it is also a systemic disease capable of involving multiple organ systems. Extraarticular manifestations of RA are included in Table 4. 1,2,10 Patients with RA have a twofold increased risk of lymphoma, which is thought to be caused by the underlying inflammatory 1250 American Family Physician Volume 84, Number 11 December 1, 2011
7 Table 5. Complications of RA and Its Treatments Complication Comments process, and not a consequence of medical treatment. 39 Patients with RA are also at an increased risk of coronary artery disease, and physicians should work with patients to modify risk factors, such as smoking, high blood pressure, and high cholesterol. 40,41 Class III or IV congestive heart failure (CHF) is a contraindication for using TNF inhibitors, which can worsen CHF outcomes. 21 In patients with RA and malignancy, caution is needed with continued use of DMARDs, especially TNF inhibitors. Biologic DMARDs, methotrexate, and leflunomide should not be initiated in patients with active herpes zoster, significant fungal infection, or bacterial infection requiring antibiotics. 21 Complications of RA and its treatments are listed in Table 5. 1,2,10 Prognosis Patients with RA live three to 12 years less than the general population. 40 Increased mortality in these patients is mainly due to accelerated cardiovascular disease, especially in those with high disease activity and chronic inflammation. The relatively new biologic therapies may reverse progression of atherosclerosis and extend life in those with RA. 41 Data Sources: A PubMed search was completed in Clinical Queries using the key terms rheumatoid arthritis, extra-articular manifestations, and disease-modifying antirheumatic agents. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality evidence reports, Clinical Evidence, the Cochrane database, Essential Evidence, and UpToDate. Search date: September 20, The Author AMY M. WASSERMAN, MD, is an assistant professor of medicine at Boston (Mass.) University School of Medicine. Address correspondence to Amy M. Wasserman, MD, Boston University, 72 E. Concord St., Evans 501, Boston, MA ( [email protected]). Reprints are not available from the author. Author disclosure: No relevant financial affiliations to disclose. REFERENCES 1. Etiology and pathogenesis of rheumatoid arthritis. In: Firestein GS, Kelley WN, eds. Kelley s Textbook of Rheumatology. 8th ed. Philadelphia, Pa.: Saunders/Elsevier; 2009: Bathon J, Tehlirian C. Rheumatoid arthritis clinical and Depression Infection Malignancy Lymphoma Lung cancer Skin cancer Affects up to 40 percent of patients with RA, can also be caused by corticosteroid use May be caused by RA itself or use of immunosuppressants Risk is double in persons with RA, independent of immunosuppressant use Caused by smoking, underlying interstitial lung disease Risk may be increased with immunosuppressant use Information from references 1, 2, and 10. SORT: KEY RECOMMENDATIONS FOR PRACTICE Clinical recommendation Patients with inflammatory joint disease should be referred to a rheumatology subspecialist, especially if symptoms last more than six weeks. In persons with RA, combination therapy with two or more disease-modifying antirheumatic drugs is more effective than monotherapy. However, more than one biologic agent should not be used at one time (e.g., adalimumab [Humira] with abatacept [Orencia]) because of the high risk of adverse effects. A guided exercise program can improve quality of life and muscle strength in patients with RA. Cardiovascular disease is the main cause of mortality in persons with RA; therefore, risk factors for coronary artery disease should be addressed in these patients. laboratory manifestations. In: Klippel JH, Stone JH, Crofford LJ, et al., eds. Primer on the Rheumatic Diseases. 13th ed. New York, NY: Springer; 2008: Allaire S, Wolfe F, Niu J, et al. Current risk factors for work disability associated with rheumatoid arthritis. Arthritis Rheum. 2009; 61(3): MacGregor AJ, Snieder H, Rigby AS, et al. Characterizing the quantitative genetic contribution to rheumatoid arthritis using data from twins. Arthritis Rheum. 2000; 43(1): Orozco G, Barton A. Update on the genetic risk factors for rheumatoid arthritis. Expert Rev Clin Immunol. 2010; 6(1): Balsa A, Cabezón A, Orozco G, et al. Influence of HLA DRB1 alleles in the susceptibility of rheumatoid arthritis and the regulation of antibodies against citrullinated proteins and rheumatoid factor. Arthritis Res Ther. 2010; 12(2): R62. Evidence rating References C 16, 17 A 21, 22, 24 B 32, 34, 35 C 40, 41 A = consistent, good-quality patient-oriented evidence; B = inconsistent or limitedquality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to December 1, 2011 Volume 84, Number 11 American Family Physician 1251
8 7. McClure A, Lunt M, Eyre S, et al. Investigating the viability of genetic screening/testing for RA susceptibility using combinations of five confirmed risk loci. Rheumatology (Oxford). 2009; 48(11): Bang SY, Lee KH, Cho SK, et al. Smoking increases rheumatoid arthritis susceptibility in individuals carrying the HLA-DRB1 shared epitope, regardless of rheumatoid factor or anti-cyclic citrullinated peptide antibody status. Arthritis Rheum. 2010; 62(2): Wilder RL, Crofford LJ. Do infectious agents cause rheumatoid arthritis? Clin Orthop Relat Res. 1991; (265): Scott DL, Wolfe F, Huizinga TW. Rheumatoid arthritis. Lancet. 2010; 376(9746): Costenbader KH, Feskanich D, Mandl LA, et al. Smoking intensity, duration, and cessation, and the risk of rheumatoid arthritis in women. Am J Med. 2006; 119(6): 503.e1-e Kaaja RJ, Greer IA. Manifestations of chronic disease during pregnancy. JAMA. 2005; 294(21): Guthrie KA, Dugowson CE, Voigt LF, et al. Does pregnancy provide vaccine-like protection against rheumatoid arthritis? Arthritis Rheum. 2010; 62(7): Karlson EW, Mandl LA, Hankinson SE, et al. Do breastfeeding and other reproductive factors influence future risk of rheumatoid arthritis? Results from the Nurses Health Study. Arthritis Rheum. 2004; 50(11): Karlson EW, Shadick NA, Cook NR, et al. Vitamin E in the primary prevention of rheumatoid arthritis: the Women s Health Study. Arthritis Rheum. 2008; 59(11): Aletaha D, Neogi T, Silman AJ, et al rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative [published correction appears in Ann Rheum Dis. 2010; 69(10): 1892]. Ann Rheum Dis. 2010; 69(9): van der Helm-van Mil AH, le Cessie S, van Dongen H, et al. A prediction rule for disease outcome in patients with recent-onset undifferentiated arthritis. Arthritis Rheum. 2007; 56(2): Mochan E, Ebell MH. Predicting rheumatoid arthritis risk in adults with undifferentiated arthritis. Am Fam Physician. 2008;77(10): Ravelli A, Felici E, Magni-Manzoni S, et al. Patients with antinuclear antibody-positive juvenile idiopathic arthritis constitute a homogeneous subgroup irrespective of the course of joint disease. Arthritis Rheum. 2005; 52(3): Wilson A, Yu HT, Goodnough LT, et al. Prevalence and outcomes of anemia in rheumatoid arthritis. Am J Med. 2004; 116(suppl 7A): 50S-57S. 21. Saag KG, Teng GG, Patkar NM, et al. American College of Rheumatology 2008 recommendations for the use of nonbiologic and biologic disease-modifying antirheumatic drugs in rheumatoid arthritis. Arthritis Rheum. 2008; 59(6): Deighton C, O Mahony R, Tosh J, et al.; Guideline Development Group. Management of rheumatoid arthritis: summary of NICE guidance. BMJ. 2009; 338: b AHRQ. Choosing medications for rheumatoid arthritis. April 9, ehc/products/14/85/rheumarthritisclinicianguide.pdf. Accessed June 23, Choy EH, Smith C, Doré CJ, et al. A meta-analysis of the efficacy and toxicity of combining disease-modifying anti-rheumatic drugs in rheumatoid arthritis based on patient withdrawal. Rheumatology (Oxford). 2005; 44(11): Smedslund G, Byfuglien MG, Olsen SU, et al. Effectiveness and safety of dietary interventions for rheumatoid arthritis. J Am Diet Assoc. 2010; 110(5): Hagen KB, Byfuglien MG, Falzon L, et al. Dietary interventions for rheumatoid arthritis. Cochrane Database Syst Rev. 2009; 21(1): CD Wang C, de Pablo P, Chen X, et al. Acupuncture for pain relief in patients with rheumatoid arthritis: a systematic review. Arthritis Rheum. 2008; 59(9): Kelly RB. Acupuncture for pain. Am Fam Physician. 2009; 80(5): Robinson V, Brosseau L, Casimiro L, et al. Thermotherapy for treating rheumatoid arthritis. Cochrane Database Syst Rev. 2002; 2(2): CD Casimiro L, Brosseau L, Robinson V, et al. Therapeutic ultrasound for the treatment of rheumatoid arthritis. Cochrane Database Syst Rev. 2002; 3(3): CD Cameron M, Gagnier JJ, Chrubasik S. Herbal therapy for treating rheumatoid arthritis. Cochrane Database Syst Rev. 2011; (2): CD Brodin N, Eurenius E, Jensen I, et al. Coaching patients with early rheumatoid arthritis to healthy physical activity. Arthritis Rheum. 2008; 59(3): Baillet A, Payraud E, Niderprim VA, et al. A dynamic exercise programme to improve patients disability in rheumatoid arthritis: a prospective randomized controlled trial. Rheumatology (Oxford). 2009; 48(4): Hurkmans E, van der Giesen FJ, Vliet Vlieland TP, et al. Dynamic Exercise programs (aerobic capacity and/or muscle strength training) in patients with rheumatoid arthritis. Cochrane Database Syst Rev. 2009; (4): CD Han A, Robinson V, Judd M, et al. Tai chi for treating rheumatoid arthritis. Cochrane Database Syst Rev. 2004; (3): CD Evans S, Cousins L, Tsao JC, et al. A randomized controlled trial examining Iyengar yoga for young adults with rheumatoid arthritis. Trials. 2011; 12: Katchamart W, Johnson S, Lin HJ, et al. Predictors for remission in rheumatoid arthritis patients: a systematic review. Arthritis Care Res (Hoboken). 2010; 62(8): Wolfe F, Zwillich SH. The long-term outcomes of rheumatoid arthritis: a 23-year prospective, longitudinal study of total joint replacement and its predictors in 1,600 patients with rheumatoid arthritis. Arthritis Rheum. 1998; 41(6): Baecklund E, Iliadou A, Askling J, et al. Association of chronic inflammation, not its treatment, with increased lymphoma risk in rheumatoid arthritis. Arthritis Rheum. 2006; 54(3): Friedewald VE, Ganz P, Kremer JM, et al. AJC editor s consensus: rheumatoid arthritis and atherosclerotic cardiovascular disease. Am J Cardiol. 2010; 106(3): Atzeni F, Turiel M, Caporali R, et al. The effect of pharmacological therapy on the cardiovascular system of patients with systemic rheumatic diseases. Autoimmun Rev. 2010; 9(12): American Family Physician Volume 84, Number 11 December 1, 2011
Rheumatoid Arthritis. Outline. Treatment Goal 4/10/2013. Clinical evaluation New treatment options Future research Discussion
 Rheumatoid Arthritis Robert L. Talbert, Pharm.D., FCCP, BCPS University of Texas at Austin College of Pharmacy University of Texas Health Science Center at San Antonio Outline Clinical evaluation New treatment
Rheumatoid Arthritis Robert L. Talbert, Pharm.D., FCCP, BCPS University of Texas at Austin College of Pharmacy University of Texas Health Science Center at San Antonio Outline Clinical evaluation New treatment
Rheumatoid Arthritis Information
 Rheumatoid Arthritis Information Definition Rheumatoid arthritis (RA) is a long-term disease that leads to inflammation of the joints and surrounding tissues. It can also affect other organs. Alternative
Rheumatoid Arthritis Information Definition Rheumatoid arthritis (RA) is a long-term disease that leads to inflammation of the joints and surrounding tissues. It can also affect other organs. Alternative
Rheumatoid Arthritis
 Rheumatoid Arthritis While rheumatoid arthritis (RA) has long been feared as one of the most disabling types of arthritis, the outlook has dramatically improved for many newly diagnosed patients. Certainly
Rheumatoid Arthritis While rheumatoid arthritis (RA) has long been feared as one of the most disabling types of arthritis, the outlook has dramatically improved for many newly diagnosed patients. Certainly
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
Biologic Treatments for Rheumatoid Arthritis
 Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Rheumatoid Arthritis
 What is Rheumatoid Arthritis? Rheumatoid Arthritis (RA) is a chronic and systemic disease that causes pain, stiffness, swelling, and limitation in the motion and function of multiple joints. Though joints
What is Rheumatoid Arthritis? Rheumatoid Arthritis (RA) is a chronic and systemic disease that causes pain, stiffness, swelling, and limitation in the motion and function of multiple joints. Though joints
Evidence-based Management of Rheumatoid Arthritis (2009)
 CPLD reviews its distance learning programmes every twelve months to ensure currency. This update has been produced by an expert and should be read in conjunction with the Evidencebased Management of distance
CPLD reviews its distance learning programmes every twelve months to ensure currency. This update has been produced by an expert and should be read in conjunction with the Evidencebased Management of distance
Understanding Rheumatoid Arthritis
 Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Immune modulation in rheumatology. Geoff McColl University of Melbourne/Australian Rheumatology Association
 Immune modulation in rheumatology Geoff McColl University of Melbourne/Australian Rheumatology Association A traditional start to a presentation on biological agents in rheumatic disease is Plasma cell
Immune modulation in rheumatology Geoff McColl University of Melbourne/Australian Rheumatology Association A traditional start to a presentation on biological agents in rheumatic disease is Plasma cell
Rheumatoid Arthritis. Disease RA Final.indd 2 15. 6. 10. 11:23
 Rheumatoid Arthritis Disease RA Final.indd 2 15. 6. 10. 11:23 Understanding what to expect can help you prepare for your transition into treatment. Rheumatoid Arthritis What You Need To Know About Rheumatoid
Rheumatoid Arthritis Disease RA Final.indd 2 15. 6. 10. 11:23 Understanding what to expect can help you prepare for your transition into treatment. Rheumatoid Arthritis What You Need To Know About Rheumatoid
The Most Common Autoimmune Disease: Rheumatoid Arthritis. Bonita S. Libman, M.D.
 The Most Common Autoimmune Disease: Rheumatoid Arthritis Bonita S. Libman, M.D. Disclosures Two googled comics The Normal Immune System Network of cells and proteins that work together Goal: protect against
The Most Common Autoimmune Disease: Rheumatoid Arthritis Bonita S. Libman, M.D. Disclosures Two googled comics The Normal Immune System Network of cells and proteins that work together Goal: protect against
Rheumatoid Arthritis: Constantly Evolving Treatment Approaches
 Rheumatoid Arthritis: Constantly Evolving Treatment Approaches Jody Garry, Pharm.D. Primary Care Pharmacy Resident VA Medical Center - Iowa City Presentation Overview Pathophysiology & epidemiology Diagnostic
Rheumatoid Arthritis: Constantly Evolving Treatment Approaches Jody Garry, Pharm.D. Primary Care Pharmacy Resident VA Medical Center - Iowa City Presentation Overview Pathophysiology & epidemiology Diagnostic
Rheumatology Labs for Primary Care Providers. Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine
 Rheumatology Labs for Primary Care Providers Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine Objectives Review the Indications for and Interpretation of lab testing for the following diseases:
Rheumatology Labs for Primary Care Providers Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine Objectives Review the Indications for and Interpretation of lab testing for the following diseases:
Rheumatoid arthritis: an overview. Christine Pham MD
 Rheumatoid arthritis: an overview Christine Pham MD RA prevalence Chronic inflammatory disease affecting approximately 0.5 1% of the general population Prevalence is higher in North America (approaching
Rheumatoid arthritis: an overview Christine Pham MD RA prevalence Chronic inflammatory disease affecting approximately 0.5 1% of the general population Prevalence is higher in North America (approaching
Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists
 Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists 1. Which of the following matches of biologic targets that contribute to rheumatoid arthritis (RA) and
Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists 1. Which of the following matches of biologic targets that contribute to rheumatoid arthritis (RA) and
Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis
 Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis 奇 美 醫 院 過 敏 免 疫 風 濕 科 陳 宏 安 Rheumatoid arthritis Most common chronic inflammatory joint disease Multisystem autoimmune disease of unknown
Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis 奇 美 醫 院 過 敏 免 疫 風 濕 科 陳 宏 安 Rheumatoid arthritis Most common chronic inflammatory joint disease Multisystem autoimmune disease of unknown
Rheumatoid arthritis
 Rheumatoid arthritis Rheumatoid arthritis Chronic multisystem disease Unknown cause Characteristic feature persistent inflammation of synovia in symmetric peripheral joints Synovial inflammation cartilage
Rheumatoid arthritis Rheumatoid arthritis Chronic multisystem disease Unknown cause Characteristic feature persistent inflammation of synovia in symmetric peripheral joints Synovial inflammation cartilage
Rheumatoid Arthritis. Nicole Klett,, M.D.
 Rheumatoid Arthritis Nicole Klett,, M.D. Rheumatoid Arthritis Systemic Chronic Inflammatory Primarily targets the synovium of diarthrodial joints Etiology likely combination genetic and environmental Diarthrodial
Rheumatoid Arthritis Nicole Klett,, M.D. Rheumatoid Arthritis Systemic Chronic Inflammatory Primarily targets the synovium of diarthrodial joints Etiology likely combination genetic and environmental Diarthrodial
Dr Sarah Levy Consultant Rheumatology Croydon University Hospital
 Dr Sarah Levy Consultant Rheumatology Croydon University Hospital Contents Definition/ epidemiology Diagnosis Importance of early diagnosis/ treatment Guidelines Evidence based treatment protocol Current
Dr Sarah Levy Consultant Rheumatology Croydon University Hospital Contents Definition/ epidemiology Diagnosis Importance of early diagnosis/ treatment Guidelines Evidence based treatment protocol Current
ABOUT RHEUMATOID ARTHRITIS
 MEDIA BACKGROUNDER ABOUT RHEUMATOID ARTHRITIS Rheumatoid arthritis (RA) is a type of arthritis (chronic inflammatory polyarthritis) that typically affects hands and feet, although any joint in the body
MEDIA BACKGROUNDER ABOUT RHEUMATOID ARTHRITIS Rheumatoid arthritis (RA) is a type of arthritis (chronic inflammatory polyarthritis) that typically affects hands and feet, although any joint in the body
Page 1 of 15 Origination Date: 09/14 Revision Date(s): 10/2015, 02/2016 Developed By: Medical Criteria Committee 10/28/2015
 Moda Health Plan, Inc. Medical Necessity Criteria Subject: Actemra (tocilizumab) Page 1 of 15 Origination Date: 09/14 Revision Date(s): 10/2015, 02/2016 Developed By: Medical Criteria Committee 10/28/2015
Moda Health Plan, Inc. Medical Necessity Criteria Subject: Actemra (tocilizumab) Page 1 of 15 Origination Date: 09/14 Revision Date(s): 10/2015, 02/2016 Developed By: Medical Criteria Committee 10/28/2015
DISEASE-MODIFYING ANTIRHEUMATIC DRUG THERAPY FOR RHEUMATOID ARTHRITIS
 DISEASE-MODIFYING ANTIRHEUMATIC DRUG THERAPY FOR RHEUMATOID ARTHRITIS APPLICATIONS OBJECTIVE Purpose of Measure: ELIGIBLE POPULATION Which members are included? STANDARD OF CARE NCQA APPROVED CODES HEDIS
DISEASE-MODIFYING ANTIRHEUMATIC DRUG THERAPY FOR RHEUMATOID ARTHRITIS APPLICATIONS OBJECTIVE Purpose of Measure: ELIGIBLE POPULATION Which members are included? STANDARD OF CARE NCQA APPROVED CODES HEDIS
Let s talk about Arthritis
 Let s talk about Arthritis Osteoarthritis Rheumatoid Arthritis Kam Shojania, MD, FRCPC Clinical Professor and Head, St. Paul s, UBC and VGH Divisions of Rheumatology Slides with thanks to: Cheryl Koehn
Let s talk about Arthritis Osteoarthritis Rheumatoid Arthritis Kam Shojania, MD, FRCPC Clinical Professor and Head, St. Paul s, UBC and VGH Divisions of Rheumatology Slides with thanks to: Cheryl Koehn
Rheumatoid Arthritis: Diagnosis, Management and Monitoring
 Rheumatoid Arthritis: Diagnosis, Management and Monitoring Effective Date: September 30, 2012 Scope This guideline is intended to aid in early recognition, intervention and management of patients with
Rheumatoid Arthritis: Diagnosis, Management and Monitoring Effective Date: September 30, 2012 Scope This guideline is intended to aid in early recognition, intervention and management of patients with
Treatment of Rheumatoid Arthritis in the New Millennium. Neal I. Shparago, D.O., FACP, FACR
 Treatment of Rheumatoid Arthritis in the New Millennium Neal I. Shparago, D.O., FACP, FACR What is RA? Symmetric inflammatory polyarthritis Rheumatoid factor positive in 80% Anti-CCP positive in approximately
Treatment of Rheumatoid Arthritis in the New Millennium Neal I. Shparago, D.O., FACP, FACR What is RA? Symmetric inflammatory polyarthritis Rheumatoid factor positive in 80% Anti-CCP positive in approximately
MEDICATION GUIDE. ACTEMRA (AC-TEM-RA) (tocilizumab) Solution for Intravenous Infusion
 MEDICATION GUIDE ACTEMRA (AC-TEM-RA) (tocilizumab) Solution for Intravenous Infusion ACTEMRA (AC-TEM-RA) (tocilizumab) Injection, Solution for Subcutaneous Administration Read this Medication Guide before
MEDICATION GUIDE ACTEMRA (AC-TEM-RA) (tocilizumab) Solution for Intravenous Infusion ACTEMRA (AC-TEM-RA) (tocilizumab) Injection, Solution for Subcutaneous Administration Read this Medication Guide before
Information on Rheumatoid Arthritis
 Information on Rheumatoid Arthritis Table of Contents About Rheumatoid Arthritis 1 Definition 1 Signs and symptoms 1 Causes 1 Risk factors 1 Test and diagnosis 2 Treatment options 2 Lifestyle 3 References
Information on Rheumatoid Arthritis Table of Contents About Rheumatoid Arthritis 1 Definition 1 Signs and symptoms 1 Causes 1 Risk factors 1 Test and diagnosis 2 Treatment options 2 Lifestyle 3 References
Guidelines for the Pharmaceutical Management of Rheumatoid Arthritis Swedish Society of Rheumatology, April 14, 2011
 Guidelines for the Pharmaceutical Management of Rheumatoid Arthritis Swedish Society of Rheumatology, April 14, 2011 Working party: Eva Baecklund, Helena Forsblad d Elia, Carl Turesson Background Our purpose
Guidelines for the Pharmaceutical Management of Rheumatoid Arthritis Swedish Society of Rheumatology, April 14, 2011 Working party: Eva Baecklund, Helena Forsblad d Elia, Carl Turesson Background Our purpose
Rheumatoid Arthritis www.arthritis.org.nz
 Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
Rheumatoid Arthritis www.arthritis.org.nz Did you know? RA is the second most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most often appears between
RHEUMATOID ARTHRITIS. Semmelweis University 3rd Department of Medicine. György Temesszentandrási MD
 RHEUMATOID ARTHRITIS Semmelweis University 3rd Department of Medicine György Temesszentandrási MD Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease predominantly affecting diarthrodial
RHEUMATOID ARTHRITIS Semmelweis University 3rd Department of Medicine György Temesszentandrási MD Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease predominantly affecting diarthrodial
Rheumatoid Arthritis:
 Rheumatoid Arthritis Update 2014 Mark Hulsey, MD FACR Rheumatoid Arthritis Key Features Symptoms >6 weeks duration Often lasts the remainder of the patient s life Inflammatory synovitis Palpable synovial
Rheumatoid Arthritis Update 2014 Mark Hulsey, MD FACR Rheumatoid Arthritis Key Features Symptoms >6 weeks duration Often lasts the remainder of the patient s life Inflammatory synovitis Palpable synovial
Once the immune system is triggered, cells migrate from the blood into the joints and produce substances that cause inflammation.
 HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
Rheumatoid Arthritis
 Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
Arthritis in Children: Juvenile Rheumatoid Arthritis By Kerry V. Cooke
 Reading Comprehension Read the following essay on juvenile rheumatoid arthritis. Then use the information in the text to answer the questions that follow. Arthritis in Children: Juvenile Rheumatoid Arthritis
Reading Comprehension Read the following essay on juvenile rheumatoid arthritis. Then use the information in the text to answer the questions that follow. Arthritis in Children: Juvenile Rheumatoid Arthritis
Rheumatoid arthritis: diagnosis, treatment and prognosis. Dr David D Cruz MD FRCP Consultant Rheumatologist
 Rheumatoid arthritis: diagnosis, treatment and prognosis Dr David D Cruz MD FRCP Consultant Rheumatologist The Louise Coote Lupus Unit St Thomas Hospital London AMUS meeting London 7 th March 2012 Disclosures
Rheumatoid arthritis: diagnosis, treatment and prognosis Dr David D Cruz MD FRCP Consultant Rheumatologist The Louise Coote Lupus Unit St Thomas Hospital London AMUS meeting London 7 th March 2012 Disclosures
A Genetic Analysis of Rheumatoid Arthritis
 A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
How will we prevent rheumatoid arthritis? Kevin Deane, MD/PhD Division of Rheumatology University of Colorado
 How will we prevent rheumatoid arthritis? Kevin Deane, MD/PhD Division of Rheumatology University of Colorado Outline 1) Brief overview of natural history of RA and how current understanding of disease
How will we prevent rheumatoid arthritis? Kevin Deane, MD/PhD Division of Rheumatology University of Colorado Outline 1) Brief overview of natural history of RA and how current understanding of disease
Disclosures. None. Seth Compton, MD Fellow of Rheumatology University of Mississippi Medical Center. Thank you for coming
 Disclosures None Seth Compton, MD Fellow of Rheumatology University of Mississippi Medical Center Steroids Steroids Thank you for coming 1 Outline Osteoarthritis Rheumatoid Arthritis Monoarthritis Systemic
Disclosures None Seth Compton, MD Fellow of Rheumatology University of Mississippi Medical Center Steroids Steroids Thank you for coming 1 Outline Osteoarthritis Rheumatoid Arthritis Monoarthritis Systemic
Speaking Plainly. Biologic treatment options for rheumatoid arthritis
 in association with Plain English Campaign Speaking Plainly Biologic treatment options for rheumatoid arthritis A guide to help healthcare professionals talking to patients with rheumatoid arthritis Foreword
in association with Plain English Campaign Speaking Plainly Biologic treatment options for rheumatoid arthritis A guide to help healthcare professionals talking to patients with rheumatoid arthritis Foreword
Rheumatoid Arthritis Medicines. A Guide for Adults
 Rheumatoid Arthritis Medicines A Guide for Adults Fast Facts Medicines for rheumatoid arthritis (RA) can slow down the disease and reduce damage to joints. They can relieve pain and make it easier to do
Rheumatoid Arthritis Medicines A Guide for Adults Fast Facts Medicines for rheumatoid arthritis (RA) can slow down the disease and reduce damage to joints. They can relieve pain and make it easier to do
Rheumatoid Arthritis: Key Features
 Rheumatoid Arthritis: Key Features Symptoms >6 weeks duration Often lasts the remainder of the patient s life Inflammatory synovitis Palpable synovial swelling Morning stiffness >1 hour, fatigue Symmetrical
Rheumatoid Arthritis: Key Features Symptoms >6 weeks duration Often lasts the remainder of the patient s life Inflammatory synovitis Palpable synovial swelling Morning stiffness >1 hour, fatigue Symmetrical
RHEUMATOLOGY ICD-10 CROSSWALK
 RHEUMATOLOGY ICD-10 CROSSWALK ICD is revised periodically and is currently in its tenth edition and will be implemented in the United States on October 1, 2015. There is an annual minor update and three-yearly
RHEUMATOLOGY ICD-10 CROSSWALK ICD is revised periodically and is currently in its tenth edition and will be implemented in the United States on October 1, 2015. There is an annual minor update and three-yearly
Do I need a physician referral? Yes, we see patients on referral from a health care provider.
 FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
Medicines for Psoriatic Arthritis. A Review of the Research for Adults
 Medicines for Psoriatic Arthritis A Review of the Research for Adults Is This Information Right for Me? Yes, this information is right for you if: Your doctor* has told you that you have psoriatic (pronounced
Medicines for Psoriatic Arthritis A Review of the Research for Adults Is This Information Right for Me? Yes, this information is right for you if: Your doctor* has told you that you have psoriatic (pronounced
MEDICAL ASSISTANCE HANDBOOK PRIOR AUTHORIZATION OF PHARMACEUTICAL SERVICES `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists
 MEDICAL ASSISTANCE HBOOK `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists A. Prescriptions That Require Prior Authorization All prescriptions for Cytokine and CAM Antagonists must
MEDICAL ASSISTANCE HBOOK `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists A. Prescriptions That Require Prior Authorization All prescriptions for Cytokine and CAM Antagonists must
DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES
 DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES GOAL #1 develop the ability to order and understand interpretation
DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES GOAL #1 develop the ability to order and understand interpretation
(Intro to Arthritis with a. Arthritis) Manager of Education & Services for the Vancouver Island Region of The Arthritis Society
 Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Rheumatic Diseases, Psoriasis, and Crohn s Disease
 Rheumatic Diseases, Psoriasis, and Crohn s Disease What does this handout cover? This handout has information about rheumatic disease, psoriasis, and Crohn s disease. It also has information on how these
Rheumatic Diseases, Psoriasis, and Crohn s Disease What does this handout cover? This handout has information about rheumatic disease, psoriasis, and Crohn s disease. It also has information on how these
Evolution of Classification Criteria for Rheumatoid Arthritis: How Do the 2010 Criteria Perform?
 Evolution of Classification Criteria for Rheumatoid Arthritis: How Do the 2010 Criteria Perform? Elizabeth C. Ortiz, MD*, Shuntaro Shinada, MD KEYWORDS Rheumatoid arthritis Classification criteria Inflammatory
Evolution of Classification Criteria for Rheumatoid Arthritis: How Do the 2010 Criteria Perform? Elizabeth C. Ortiz, MD*, Shuntaro Shinada, MD KEYWORDS Rheumatoid arthritis Classification criteria Inflammatory
subcutaneous initially every 4 weeks then every 12 weeks Coverage Criteria: Express Scripts, Inc. monograph dated 02/24/2010
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Humira (adalimumab subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Humira (adalimumab subcutaneous injection) Commercial HMO/PPO/CDHP
Drug Therapy Guidelines: Humira (adalimumab)
 Drug Therapy Guidelines: Humira (adalimumab) Effective Date: 5/1/08 Committee Review Date: 1/6/01, 9/18/01, 1/15/02, 1/7/03, 1/20/04, 1/18/05, 12/7/05, 10/15/06, 7/2/07, 11/5/07, 3/25/08 Policy Statements:
Drug Therapy Guidelines: Humira (adalimumab) Effective Date: 5/1/08 Committee Review Date: 1/6/01, 9/18/01, 1/15/02, 1/7/03, 1/20/04, 1/18/05, 12/7/05, 10/15/06, 7/2/07, 11/5/07, 3/25/08 Policy Statements:
2010 ACR/EULAR Classification Criteria for Rheumatoid Arthritis
 2010 ACR/EULAR Classification Criteria for Rheumatoid Arthritis Published in the September 2010 Issues of A&Rand ARD Phases of the Project Phase 1 Data analysis Phase 2 Consensus process Predictors of
2010 ACR/EULAR Classification Criteria for Rheumatoid Arthritis Published in the September 2010 Issues of A&Rand ARD Phases of the Project Phase 1 Data analysis Phase 2 Consensus process Predictors of
CLINICAL POLICY Department: Medical Management Document Name: Rheumatoid & Juvenile Arthritis and Ankylosing Spondylitis Treatments
 Page: 1 of 18 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Page: 1 of 18 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Rheumatoid Arthritis. What is rheumatoid arthritis? Understanding joints. What causes rheumatoid arthritis?
 Page 1 of 6 Rheumatoid Arthritis Rheumatoid arthritis causes inflammation, pain, and swelling of joints. In time, affected joints typically become damaged. The severity can vary from mild to severe. Treatments
Page 1 of 6 Rheumatoid Arthritis Rheumatoid arthritis causes inflammation, pain, and swelling of joints. In time, affected joints typically become damaged. The severity can vary from mild to severe. Treatments
Rheumatoid Arthritis www.arthritis.org.nz
 Rheumatoid Arthritis www.arthritis.org.nz Did you know? Rheumatoid arthritis (RA) is the third most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most
Rheumatoid Arthritis www.arthritis.org.nz Did you know? Rheumatoid arthritis (RA) is the third most common form of arthritis Approximately 40,000 New Zealanders have RA RA can occur at any age, but most
Infl ectra for rheumatoid arthritis
 Infl ectra for rheumatoid arthritis Some important information to get you started with your treatment This booklet is intended only for use by patients who have been prescribed Inflectra. Introduction
Infl ectra for rheumatoid arthritis Some important information to get you started with your treatment This booklet is intended only for use by patients who have been prescribed Inflectra. Introduction
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC)
 BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) September 2014 Review date: September 2017 Bulletin 203: Tocilizumab (subcutaneous) in combination with methotrexate or as monotherapy for the treatment
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) September 2014 Review date: September 2017 Bulletin 203: Tocilizumab (subcutaneous) in combination with methotrexate or as monotherapy for the treatment
Testing for RA. The Ideal Lab Test. William M. Wason, MD, PhD 9/24/2010. Confusion Abounds
 Confusion Abounds Rheumatoid arthritis: ulnar deviation and muscle artrophy, hands Poor sensitivity and specificity Hepatitis C causes lots of false + tests Changing technology in how tests are done Historic
Confusion Abounds Rheumatoid arthritis: ulnar deviation and muscle artrophy, hands Poor sensitivity and specificity Hepatitis C causes lots of false + tests Changing technology in how tests are done Historic
Rheumatoid Arthritis: New tests, new treatments and. Christine H Jones MD Assistant Professor of Medicine UVM/FAHC
 Rheumatoid Arthritis: New tests, new treatments and new perspectives Christine H Jones MD Assistant Professor of Medicine UVM/FAHC Objectives Discuss physical and laboratory findings in rheumatoid arthritis
Rheumatoid Arthritis: New tests, new treatments and new perspectives Christine H Jones MD Assistant Professor of Medicine UVM/FAHC Objectives Discuss physical and laboratory findings in rheumatoid arthritis
How To Choose A Biologic Drug
 North Carolina Rheumatology Association Position Statements I. Biologic Agents A. Appropriate delivery, handling, storage and administration of biologic agents B. Indications for biologic agents II. III.
North Carolina Rheumatology Association Position Statements I. Biologic Agents A. Appropriate delivery, handling, storage and administration of biologic agents B. Indications for biologic agents II. III.
Rheumatoid Arthritis monitoring of DMARDs
 www.bpac.org.nz keyword: DMARDS Rheumatoid Arthritis monitoring of DMARDs Key reviewers: Professor John Highton, Head of Section, Department of Medical and Surgical Sciences, Dunedin School of Medicine,
www.bpac.org.nz keyword: DMARDS Rheumatoid Arthritis monitoring of DMARDs Key reviewers: Professor John Highton, Head of Section, Department of Medical and Surgical Sciences, Dunedin School of Medicine,
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 17 December 2003 CPMP/EWP/556/95 rev 1/Final COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 17 December 2003 CPMP/EWP/556/95 rev 1/Final COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
5.07.09. Aubagio. Aubagio (teriflunomide) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
Psoriatic arthritis FACTSHEET
 1 What is psoriatic arthritis? Psoriatic arthritis (PsA) is a disease where joints around the body become inflamed and sore. It can make moving about difficult and painful. People who have PsA also have
1 What is psoriatic arthritis? Psoriatic arthritis (PsA) is a disease where joints around the body become inflamed and sore. It can make moving about difficult and painful. People who have PsA also have
Arthritis and Rheumatology. Antoni Chan MBChB, FRCP, PhD Consultant Rheumatologist Royal Berkshire NHS Foundation Trust
 Antoni Chan MBChB, FRCP, PhD Consultant Rheumatologist Royal Berkshire NHS Foundation Trust Rheumatology Investigation, Diagnosis, Treatment The challenge 8 billion a year in cost 700,000 people suffering
Antoni Chan MBChB, FRCP, PhD Consultant Rheumatologist Royal Berkshire NHS Foundation Trust Rheumatology Investigation, Diagnosis, Treatment The challenge 8 billion a year in cost 700,000 people suffering
Original Policy Date
 MP 5.01.20 Tysabri (natalizumab) Medical Policy Section Prescription Drug Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local Policy/12:2013 Return to Medical Policy Index Disclaimer
MP 5.01.20 Tysabri (natalizumab) Medical Policy Section Prescription Drug Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local Policy/12:2013 Return to Medical Policy Index Disclaimer
Immune Modulating Drugs Prior Authorization Request Form
 Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
What is Rheumatoid Arthritis? Pathogenesis: Overview. Pathogenesis: Joint Inflammation. Risk Factors for RA. Who is Affected by RA?
 What is Rheumatoid Arthritis? Chronic, progressive, and disabling inflammatory disease Affects the synovial tissue of joints, especially of the hands/feet, although any joint can be involved Affects extra-articular
What is Rheumatoid Arthritis? Chronic, progressive, and disabling inflammatory disease Affects the synovial tissue of joints, especially of the hands/feet, although any joint can be involved Affects extra-articular
Rheumatoid Arthritis. Compiled by Darreck My Healing Oils notes
 Rheumatoid Arthritis Compiled by Darreck My Healing Oils notes What is Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease where the body's immune system attacks normal joint tissues,
Rheumatoid Arthritis Compiled by Darreck My Healing Oils notes What is Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease where the body's immune system attacks normal joint tissues,
Systemic Lupus Erythematosus
 Harvard-MIT Division of Health Sciences and Technology HST.021: Musculoskeletal Pathophysiology, IAP 2006 Course Director: Dr. Dwight R. Robinson Systemic Lupus Erythematosus A multi-system autoimmune
Harvard-MIT Division of Health Sciences and Technology HST.021: Musculoskeletal Pathophysiology, IAP 2006 Course Director: Dr. Dwight R. Robinson Systemic Lupus Erythematosus A multi-system autoimmune
Arthritis and Rheumatology Clinics of Kansas Patient Education. Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis
 Arthritis and Rheumatology Clinics of Kansas Patient Education Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis Introduction: For as long as scientists have studied rheumatic disease,
Arthritis and Rheumatology Clinics of Kansas Patient Education Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis Introduction: For as long as scientists have studied rheumatic disease,
Psoriatic Arthritis. Title. Understanding and Managing. in All the Wrong Places. Clinical Features. Etiology of Psoriatic Arthritis
 Focus on CME at Memorial University Understanding and Managing Title Psoriatic Arthritis in All the Wrong Places Proton Rahman MD, MSc, FRCPC Although Baron Jean-Luis Aubert offered the first case description
Focus on CME at Memorial University Understanding and Managing Title Psoriatic Arthritis in All the Wrong Places Proton Rahman MD, MSc, FRCPC Although Baron Jean-Luis Aubert offered the first case description
Media Release. Basel, 11 June 2009. RA patients with enhanced response identified
 Media Release Basel, 11 June 2009 New data demonstrate the ability of MabThera to reduce the progression of joint damage when used as a first-line biologic treatment in rheumatoid arthritis RA patients
Media Release Basel, 11 June 2009 New data demonstrate the ability of MabThera to reduce the progression of joint damage when used as a first-line biologic treatment in rheumatoid arthritis RA patients
RHEUMATOID ARTHRITIS ASSOCIATED SCLERITIS
 RHEUMATOID ARTHRITIS ASSOCIATED SCLERITIS FEHMA TUFAIL M.D Case Report A 77-year-old white male presented with a history of painful, red right eye. The patient was diagnosed with mild iritis in the right
RHEUMATOID ARTHRITIS ASSOCIATED SCLERITIS FEHMA TUFAIL M.D Case Report A 77-year-old white male presented with a history of painful, red right eye. The patient was diagnosed with mild iritis in the right
Critical Issues in School Health Arthritis in the School Setting. Lawrence Zemel MD Tegan Willard RN Connecticut Children s
 Critical Issues in School Health Arthritis in the School Setting Lawrence Zemel MD Tegan Willard RN Connecticut Children s Juvenile Rheumatoid Idiopathic Arthritis Definition of JRA (JIA) Persistent arthritis
Critical Issues in School Health Arthritis in the School Setting Lawrence Zemel MD Tegan Willard RN Connecticut Children s Juvenile Rheumatoid Idiopathic Arthritis Definition of JRA (JIA) Persistent arthritis
Top 50 ICD-10-Codes Description ICD-9-CM Code ICD-10-CM Code 724.5 727.3
 Description ICD-9-CM Code ICD-10-CM Code Backache unspecified 724.5 M54.89 Other dorsalgia Excludes1: o dorsalgia in thoracic region (M54.6) o low back pain (M54.5) M54.9 Dorsalgia, unspecified Other bursitis
Description ICD-9-CM Code ICD-10-CM Code Backache unspecified 724.5 M54.89 Other dorsalgia Excludes1: o dorsalgia in thoracic region (M54.6) o low back pain (M54.5) M54.9 Dorsalgia, unspecified Other bursitis
Cytokine and CAM Antagonists
 Texas Prior Authorization Program Clinical Edit Criteria Drug/Drug Class Clinical Edit Information Included in this Document Actemra (Tocilizumab) Drugs requiring prior authorization: the list of drugs
Texas Prior Authorization Program Clinical Edit Criteria Drug/Drug Class Clinical Edit Information Included in this Document Actemra (Tocilizumab) Drugs requiring prior authorization: the list of drugs
MEDICATION GUIDE REMICADE (Rem-eh-kaid) (infliximab) Read the Medication Guide that comes with REMICADE before you receive the first treatment, and
 MEDICATION GUIDE REMICADE (Rem-eh-kaid) (infliximab) Read the Medication Guide that comes with REMICADE before you receive the first treatment, and before each time you get a treatment of REMICADE. This
MEDICATION GUIDE REMICADE (Rem-eh-kaid) (infliximab) Read the Medication Guide that comes with REMICADE before you receive the first treatment, and before each time you get a treatment of REMICADE. This
Symptoms ongoing for 6/12, initially intermittent in nature.
 Rheumatoid Arthritis Case Study INTRODUCTION Each student will have watched the relevant MDT member carrying out their initial assessment on the same newly diagnosed Rheumatoid Arthritis patient. Videos
Rheumatoid Arthritis Case Study INTRODUCTION Each student will have watched the relevant MDT member carrying out their initial assessment on the same newly diagnosed Rheumatoid Arthritis patient. Videos
Overview of Rheumatology
 Overview of Rheumatology Griffin Hospital Mini Med School Stephen Moses, MD Valley Medical Associates 135 Division St. Ansonia, CT 06401 203.735.9354 Topics I. Anatomy of a Joint II. Osteoarthritis III.
Overview of Rheumatology Griffin Hospital Mini Med School Stephen Moses, MD Valley Medical Associates 135 Division St. Ansonia, CT 06401 203.735.9354 Topics I. Anatomy of a Joint II. Osteoarthritis III.
Autoimmune Diseases More common than you think Randall Stevens, MD
 Autoimmune Diseases More common than you think Randall Stevens, MD picture placeholder Autoimmune Diseases More than 60 different disorders Autoimmune disorders (AID) diseases caused by the immune system
Autoimmune Diseases More common than you think Randall Stevens, MD picture placeholder Autoimmune Diseases More than 60 different disorders Autoimmune disorders (AID) diseases caused by the immune system
Rheumatology. Overview Osteoarthritis Rheumatoid arthritis Psoriatic arthropathy Chronic tophaceous gout Systemic lupus Scleroderma
 Rheumatology This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations. They
Rheumatology This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations. They
