of endoscopic versus external repair of orbital
|
|
|
- Tracy Chapman
- 8 years ago
- Views:
Transcription
1 Otolaryngology Head and Neck Surgery (2007) 136, ORIGINAL RESEARCH Endoscopic versus external repair of orbital blowout fractures Hong-Ryul Jin, MD, Je-Yeob Yeon, MD, See-Ok Shin, MD, Young-Seok Choi, MD, and Dong-Wook Lee, MD, Seoul and Cheongju, Korea OBJECTIVES: This study evaluates the usefulness of endoscopic repair compared to external repair in the treatment of blowout fracture (BOF) of the orbit. STUDY DESIGN AND SETTING: This retrospective study comprised 100 patients who had had surgical repair of orbital BOF since Forty-eight of the 100 had undergone endoscopic repair, 48 patients had had external repair, and four patients underwent surgery that combined the two approaches. The two basic approaches were evaluated and compared with respect to technique, results and complications. RESULTS: Endoscopically, transnasal and transantral approaches had been used for reduction and support of fractured medial and inferior walls, respectively. In the external approach, various transorbital incisions were made and the fractured wall was repaired with alloplastic or autologous materials. Complete or partial resolution of preoperative diplopia was achieved in 94% of the endoscopic group and 83% of the external group (NS). Enophthalmos was improved in 89% of the endoscopic group and 76% of the external group (NS). Though the endoscopic group had no significant complications, the external group had ectropions, significant facial scars, extrusion of inserted Medpor, and intra-orbital hematoma. CONCLUSIONS: Endoscopic repair appears to be a safe and effective technique for the treatment of BOF of the orbit American Academy of Otolaryngology Head and Neck Surgery Foundation. All rights reserved. Traditionally, external transorbital approaches have been used in the repair of blowout fracture (BOF) of the orbit. External approaches generally require either a medial canthal incision, a subciliary incision, or a transconjunctival incision, depending on the location, extent, and complexity of the fracture. External repairs with transorbital incisions have known complications that include external scars, ectropion, and a frequent need for alloplastic materials to 1-3 support the fractured wall. Because the application of endoscopic surgery has been extended to the diverse fields of head and neck surgery including facial trauma, many reports about the endoscopic repair of medial and inferior orbital BOF have been published These reports either discuss endonasal repair of medial BOF or transantral repair of inferior BOF. However, studies that include both endoscopic approaches are rare. Moreover, these studies generally have been case series or preliminary reports on cadavers combined with small numbers of surgical patients. To date, there are no published studies that examine the advantages and disadvantages of endoscopic versus external repair of orbital BOF in an adequate number of surgical cases. This study evaluates the usefulness of endoscopic repair compared with external repair of BOF of the orbit; the primary outcomes are resolution of diplopia and enophthalmos. In addition, the advantages and limitations of endoscopic repair will be discussed, and the surgical techniques described in comparison with the external approach. PATIENTS AND METHODS From 1992 to 2004, 316 patients with BOF of the orbit were managed at the Department of Otolaryngology of Chungbuk National University Hospital. All of the fractures were di- From the Department of Otorhinolaryngology (Dr Jin); Seoul National University Boramae Hospital, Seoul; and the Department of Otolaryngology (Drs Yeon, Shin, Choi, and Lee); Chungbuk National University Hospital, Cheongju, Korea. Presented at the 2005 Annual Meeting of the AAO-HNS in Los Angeles, California. Reprint requests: Hong-Ryul Jin, MD, Department of Otorhinolaryngology, Seoul National University Boramae Hospital, 425 Shindaebangdong, Dongjak-gu, Seoul, Korea. address: hrjin@paran.com /$ American Academy of Otolaryngology Head and Neck Surgery Foundation. All rights reserved. doi: /j.otohns
2 Jin et al Endoscopic versus external repair of orbital Table 1 Demographics of the 100 surgical patients Method of repair Average age (years) Male Sex Female Endoscopic (n 48) External (n 48) Combined (n 4) Total agnosed by computed tomography (CT) scan. Of these, 203 patients were managed conservatively and 113 patients underwent surgery by the senior author or chief residents under the supervision of the senior author. A retrospective chart review was performed for the 113 surgical patients with a predetermined check list. All information was collected from the medical records and CT scans with prior approval from the Chungbuk Research Internal Review Board. The patient s age, sex, site of the fracture, presenting symptoms and signs, surgical method and results, complications, and follow-up period were included in the check list. Two residents of our department performed the chart review while blinded to the objectives of the study. Thirteen patients were excluded from the study mainly because of a short follow-up period or inadequate data including a CT scan that did not meet study criteria; the remaining 100 patients were available for further review and analysis. Among the 100 patients reviewed, there were 76 males and 24 females; their mean age was 30 years (Table 1). Injuries were on the left side in 65 patients and on the right side in 35 patients. Fracture sites involved the inferior wall in 45 (45%) patients, medial wall in 32 (32%) patients, and both walls in 23 (23%) patients (Table 2). The follow-up period varied from three months to four years with an average of seven months. Surgical methods and timing, surgical techniques, surgical results that included improvement of diplopia and enophthalmos, and complications associated with the surgery were evaluated and analyzed. Improvement of preoperative diplopia was categorized into three groups: complete resolution, partial resolution, and residual deformity. Complete resolution was defined as no diplopia at all; partial resolution as slightly remaining diplopia within 30 of the primary gaze, especially in upward gaze with no discomfort in daily life; and residual deformity as persistent diplopia that causes discomfort in daily life. Complete and partial resolutions were considered to be a surgical success. The degree of enophthalmos was measured with a Herthel exophthalmometer. Intergroup differences in improvement of diplopia and enophthalmos were assessed with chi-square test and Fisher s exact test. A P value 0.05 was considered statistically significant. RESULTS Management Principle Initial management started with ophthalmologic consultation and supportive care that included cold pack application and intake of analgesics although steroids were not used routinely. Visual acuity, ocular motility, exophthalmometry, and forced duction testing were checked regularly until the day before surgery. Persistent diplopia that lasts two weeks after injury, restriction of eye movement with CT evidence of extraocular muscle entrapment, and an enophthalmos of greater than 2 mm were treated as indications for surgery. Final evaluation for the presence of diplopia and the degree of enophthalmos was performed three months after surgery. Selection of Surgical Method The selection of surgical approach in management of BOF mainly depended on the time of injury. From 1992 to 1996, only external repair was used to treat all orbital BOF. Starting in 1997, endoscopic repair replaced external repair to treat medial BOF. From 1997 to 1999, inferior BOF was still managed with an external approach whereas medial BOF was managed endoscopically. Endoscopic repair of inferior BOF started in 2000, and since then inferior BOF largely has been managed endoscopically although a few cases with severe periorbital laceration and associated tripod fracture were managed with an external approach. Overall, an endoscopic repair was used in 48 patients (endoscopic group), an external repair in 48 patients (external group), and both approaches in four patients (combined group). In the endoscopic group, an endonasal reduction was used in 25 patients, a transantral reduction in 20 patients, and both endonasal and transantral reductions were used in three patients with simultaneous medial and inferior BOFs (Table 2). In the external group, 28 patients had inferior BOF, 12 had medial BOF, and eight had both medial and inferior BOFs. There were four patients with simultaneous medial and inferior BOFs who were treated with both endoscopic and external repairs. Table 2 Methods of repair and sites of blowout fracture in 100 surgical patients Method of repair Medial Inferior Site of fracture Medial and inferior Total Endoscopic Endonasal Transantral Endonasal transantral External Combined Total
3 40 Otolaryngology Head and Neck Surgery, Vol 136, No 1, January 2007 Table 3 Timing of surgical repair Method of repair and site of fracture* Days from the injury Endoscopic (n 48) 7 (15%) 27 (56%) 8 (17%) 4 (8%) 2 (4%) Medial (n 20) Inferior (n 17) Both (n 11) External (n 48) 4 (8%) 29 (60%) 7 (15%) 6 (13%) 2 (4%) Medial (n 12) Inferior (n 28) Both (n 8) Combined (n 4) Both (n 4) 0 1 (25%) 2 (50%) 1 (25%) 0 *No statistical difference in the timing of surgical repair between the endoscopic group and external group (P 0.05). Timing of Surgery The time to surgical repair was stratified by weekly intervals (Table 3). In the endoscopic group, 34 patients had surgery within two weeks from the injury; 14 patients had surgery two weeks after their injury. In the external group, 33 patients had surgery within two weeks of the injury whereas 15 patients had surgery two weeks after the injury. There was no statistical difference in the timing of surgery between the two groups (P 0.05). In the combined group, one patient had surgery within two weeks after the injury, and three patients had surgery two weeks after the injury. Operative Techniques of Endoscopic Repair Surgery was performed under general or local anesthesia, determined by the extent of the fracture and the status of the patient. Either a 0-degree or 30-degree, 4-mm diameter endoscope (Karl Storz GmBH & Co, Tuttlingen, Germany) was used. In medial BOF, the herniated orbital tissue was approached through the ethmoid cavity. After topical and infiltration anesthesia, an uncinectomy was performed. Care was taken during this procedure not to incise or remove orbital tissue that herniated into the ethmoid cavity when fractures were severe. If necessary, an ethmoidectomy was performed to clearly delineate the fracture site from herniated orbital tissue. Bony fragments that did not interfere with normal muscle action were preserved to obtain a more rigid medial orbital wall postoperatively. On occasion, herniated orbital tissue had adhered to the ethmoid sinus mucosa; it was separated by careful dissection with the use of an elevator. Compressing the orbit gently during surgery helped to identify herniated orbital tissue. After herniated orbital tissue was reduced to its original position, a silastic sheet was sculpted to fit the ethmoid cavity and inserted as an inverted U-shape. Merocel (Xomed, Jacksonville, Fla) soaked with an antibiotic and steroid solution was inserted to fill the cavity evenly to the ethmoid roof (Fig 1). Care was taken to fully reduce the fracture and evenly pack the Merocel to prevent the protrusion of orbital tissue into the unreduced or unpacked site. Care also was taken not to obstruct the middle meatal antrostomy site and the frontal sinus ostium, because this may predispose the patient to postoperative sinusitis. Excessively tight packing was avoided because it generally causes orbital pain after surgery. In inferior BOF, the orbital floor was approached through a small bony window ( cm) made at the anterior wall of the maxillary sinus after gingivobuccal incision. The orbital floor, herniated orbital tissue, maxillary sinus ostium, and infraorbital nerve indentation were carefully observed with the endoscope. While gentle pressure was applied to the affected eyeball, fracture size and patterns were observed with the endoscope. In a trapdoor-type fracture, herniated orbital tissue was repositioned into its premorbid position together with the bone flap, with an appropriately sized elevator or a cotton ball held in place by a small Kelly clamp. Care was taken not to strangulate herniated orbital tissue during the reduction. In a large fracture with orbital floor disruption, a decision was made whether to use the implant for floor support after careful inspection with the elevator. If a large bony fragment had been preserved, it was left in place for floor support after reduction of the orbital contents. In large fractures without any useful bony frag- Figure 1 Design of a silastic sheet and Merocel that are packed at the ethmoid cavity.
4 Jin et al Endoscopic versus external repair of orbital Figure 2 Balloon made with a surgical glove and a pediatric feeding tube. ments for floor support, harvested anterior maxillary wall or a Medpor implant (Porex Surgical Inc, College Park, Ga) was inserted below the reduced orbital tissue and supported by the remaining stable bony shelves. After reduction, the mucosal flap was repositioned and the wall was supported with a balloon catheter inserted through the enlarged maxillary ostium. The balloon catheter was constructed of a surgical glove and a pediatric feeding tube (Fig 2). After surgery, visual acuity and ocular motility were checked. Mild orbital pain subsided spontaneously. The packed Merocel in the endonasal group was kept dry with frequent suctioning during the hospital admission. After discharge, weekly follow-up and oral antibiotics were recommended until removal of the Merocel or balloon catheter. The balloon catheter was easily removed through the nose after removing the saline filling the balloon at the outpatient clinic. Under usual circumstances, the Merocel or the balloon was removed three to four weeks after surgery. After this removal, a routine ophthalmologic examination, including exophthalmometry, was carried out. Surgical Outcomes Diplopia and enophthalmos measurements of the day before surgery and three months after surgery were compared to evaluate the outcome. Before surgery, diplopia was present in 76 (76%) patients (endoscopic group, 37; external group, 35; combined group, 4) (Table 4). In the endoscopic group, complete resolution of diplopia was achieved in 26 (70%) patients and partial resolution in nine (24%) patients for an overall rate of improvement in preoperative diplopia of 94%. In the external group, complete resolution was achieved in 15 (43%) patients and partial resolution in 14 (40%) patients for an overall rate of improvement in preoperative diplopia of 83% (Table 4). The rate of complete resolution was significantly higher in the endoscopic group (P 0.05) versus the external group; however, the overall rate of surgical success, including both complete and partial resolution, was not significantly different. In the combined group, complete resolution was achieved in 1 (25%) patient and partial resolution in two (50%) patients, for an overall rate of improvement in preoperative diplopia of 75 percent. In both endoscopic and external groups, there was no statistical difference in the rate of residual deformity according to the site of fracture P ( 0.05) (Table 4). Preoperatively, an enophthalmos of greater than 2 mm was present in 38 (38%) patients (endoscopic group, 19; external group, 17; combined group, 2) (Table 5). The severity of preoperative enophthalmos was not significantly different between the endoscopic group and external group (2.7 mm vs 2.9 mm) (P 0.05). Preoperative enophthalmos was corrected in 31 (82%) of 38 patients. Enophthalmos was corrected in 17 (89%) of 19 patients in the endoscopic group and 13 (76%) of 17 patients in the external group with no statistical difference between the 2 groups (P 0.05) (Table 5). In the combined group, enophthalmos was corrected in one (50%) of two patients. In both endoscopic and external groups, there was no statistical difference in the rate of enophthalmos correction according to the site of Table 4 Improvement of diplopia after surgical repair Method of repair and site of fracture* Before surgery After surgery Complete resolution Partial resolution Residual deformity Endoscopic (n 48) 37 (100%) 26 (70%) 9 (24%) 2 (6%) Medial (n 20) Inferior (n 17) Both (n 11) External (n 48) 35 (100%) 15 (43%) 14 (40%) 6 (17%) Medial (n 12) Inferior (n 28) Both (n 8) Combined (n 4) Both (n 4) 4 (100%) 1 (25%) 2 (50%) 1 (25%) *No statistical difference in the ratio of residual deformity according to the method of repair or site of fracture (P 0.05). Statistical difference between the endoscopic and external groups (P 0.05).
5 42 Otolaryngology Head and Neck Surgery, Vol 136, No 1, January 2007 Table 5 Incidence of enophthalmos before and after surgical repair Method of repair and site of fracture* fracture (P 0.05) (Table 5). Satisfactorily reduced orbital walls could be observed by nasal endoscopy or by CT scan (Figs 3 A and B and Fig 4). Surgical Complications In the endoscopic group, no significant intraoperative or postoperative complications were discovered except for one patient who developed orbital cellulitis that resolved with antibiotic treatment; transient mild orbital pain and decreased sensation of the cheek improved over time. In the external group, two patients developed transient ectropion that improved with massage; one patient developed an unsightly medial canthal scar; one patient had extrusion of inserted Medpor; and one patient developed an intra-orbital hematoma. DISCUSSION Before surgery After surgery Endoscopic (n 48) 19 (100%) 2 (11%) Medial (n 20) 8 1 Inferior (n 17) 4 0 Both (n 11) 7 1 External (n 48) 17 (100%) 4 (24%) Medial (n 12) 3 1 Inferior (n 28) 10 3 Both (n 8) 4 0 Combined (n 4) Both (n 4) 2 (100%) 1 (50%) *No statistical difference in the rate of enophthalmos correction according to the method of repair or site of fracture (P 0.05). Endoscopic repair of BOF of the orbit has been reported to provide surgeons with several advantages over conventional external repair First, it provides excellent visualization of the medial and inferior walls of the orbit, which enables safe removal of bony fragments and clear anatomic reduction of fractures. Second, the use of intraocular alloplastic implants, commonly used with external repairs, can be avoided or minimized. Third, endoscopy virtually eliminates the risk of significantly visible facial scarring and eyelid complications, complications reported with transorbital incisions. Fourth, endoscopic surgery can be performed under local anesthesia, which makes intra-operative evaluation of ocular movements and diplopia possible. Some of the advantages of endoscopic repair were evident in our study. In our endoscopic group, there were no postoperative complications associated with transorbital incisions, such as ectropion or unsightly facial scars that were observed in the external group. A case of Medpor extrusion into the ethmoid cavity after external repair of a medial BOF was managed successfully with endoscopic endonasal reduction after Medpor removal. When the anterior maxillary wall or Medpor is used to support the orbital floor, an endoscope enables clear identification of the bony shelves so that the implant can be placed safely and with adequate support. No specific major disadvantages have been reported for 4-13 endoscopic repair of BOF. In endonasal repair of the medial wall, maxillary and/or frontal sinusitis can be caused by obstruction of the sinus ostium. This can be avoided by careful insertion of a silastic sheet and Merocel and administration of antibiotics until the packing is removed. In our study, transantral repair of an orbital floor fracture resulted in transient numbness of the cheek, but symptoms slowly resolved over time. One potential difficulty with transantral repair of inferior BOF is in the fabrication and maintenance of a balloon that conforms to the shape of the orbital floor to support the reduced orbital tissue. In our experience, this can be overcome by using a self-made balloon fashioned from the fingers of a surgical glove and a pediatric feeding tube. With a small diameter catheter to facilitate the posi- Figure 3 (A) Preoperative CT scan shows a large blowout fracture of the right medial orbital wall with herniation of orbital tissue. (B) CT scan taken at 8 weeks after surgery shows a well-reduced medial orbital wall.
6 Jin et al Endoscopic versus external repair of orbital Figure 4 (A) Preoperative CT scan shows an inferior blowout fracture of the right orbit. (B) CT scan taken at two months after surgery shows a well-reduced orbital floor. tioning of the balloon, you can avoid the inconvenience to the patient of a large diameter foley catheter. Under usual circumstances, the Merocel or the balloon is removed three to four weeks after surgery, though the timing of removal depends on the type and extent of the fracture and whether supporting materials were used. In medial BOF, the Merocel can be removed early if the fracture is small or if only those bony fragments that might interfere with ocular muscle function are removed. In inferior BOF, the balloon can be removed early when a trapdoor type fracture is reduced with the bony fragment intact or when the fracture site is supported by a large bony fragment or implant. Usually, the Merocel packing that supports the medial wall can be removed earlier than a balloon catheter that supports the inferior wall because the inferior wall must be rigid enough to support the orbit against gravity. Failure of diplopia to improve after adequate repositioning of orbital tissue is not an infrequent outcome after surgery for BOF, as we found in our study. There are a few explanations for residual diplopia even after adequate surgery. The first possible explanation is that entrapment, contusion, or hematoma of ocular muscle by fractured bony fragments may influence muscle function even after adequate repositioning. 15 Second, there may be an undetected, 16,17 persistent palsy of the oculomotor nerve. Third, altered orbit position may occur. In this study, the endoscopic group was statistically more likely to experience complete resolution of diplopia than the external group, though the percentage in the two groups who experienced either complete or partial resolution was not different. The apparent improvement in complete resolution rate might be explained by improved visualization and anatomic reconstruction of the fracture in the endoscopic group. Enophthalmos of greater than 2 mm is another indication for surgery, mostly for cosmetic reasons. Though there was no intergroup difference in the success rate for enophthalmos correction, only two Medpor implants were required to support the fractured inferior wall. This suggests that our endoscopic repair technique provides sufficient strength to support the repositioned orbital tissue with minimal use of any artificial implants even with large inferior fractures. When observed through the endoscope postoperatively, usually the reduced medial wall was strong enough to hold the orbital tissue in place. Although the inferior wall could not be observed through the endoscope, a well-aligned inferior wall was observed by CT scan. CONCLUSIONS Endoscopic repair of orbital blowout fractures represents an innovative and highly successful and safe alternative to external repairs. Prospective, randomized studies are warranted to study this new technique further. REFERENCES 1. Zingg M, Chowdhury K, Ladrach K, et al. Treatment of 813 zygomalateral orbital complex fractures. Arch Otolaryngol Head Neck Surg 1991;117: (Grade B). 2. Appling WD, Patrinely JR, Salzer TA. Transconjunctival approach vs. subciliary skin-muscle flap approach for orbital fracture repair. Arch Otolaryngol Head Neck Surg 1993;119: (Grade B). 3. Mullins JB, Holds JB, Branham GH, et al. Complications of the transconjunctival approach: a review of 400 cases. Arch Otolaryngol Head Neck Surg 1997;123: (Grade C). 4. Yamaguchi N, Arai S, Mitani H, et al. Endoscopic endonasal techniques of the blowout fracture of the medial orbital wall. Oper Techniq Otolaryngol Head Neck Surg 1991;2: (Grade C). 5. Michel O. Medial orbital wall fracture: results of minimally invasive endoscopically controlled endonasal surgical technique. Laryngorhinootologie 1993;72: (Grade C). 6. Jin HR, Shin SO, Choo MJ, et al. Endonasal endoscopic reduction of blowout fractures of the medial orbital wall. J Oral Maxillofac Surg 2000;58: (Grade C). 7. Rhee JS, Lynch J, Loehrl TA. Intranasal endoscopy-assisted repair of medial orbital wall fractures. Arch Facial Plast Surg 2000;2: (Grade D).
7 44 Otolaryngology Head and Neck Surgery, Vol 136, No 1, January Lee MJ, Kang YS, Yang JY, et al. Endoscopic transnasal approach for the treatment of medial orbital blow-out fracture: a technique for controlling the fractured wall with a balloon catheter and Merocel. Plast Reconstr Surg 2002;110: (Grade C). 9. Saunders CJ, Whetzel TP, Stokes RB, et al. Transantral endoscopic orbital floor exploration: a cadaver and clinical study. Plast Reconstr Surg 1997;100: (Grade C). 10. Ikeda K, Suzuki H, Oshima T, et al. Endoscopic endonasal repair of orbital floor fracture. Arch Otolaryngol Head Neck Surg 1999;125: (Grade C). 11. Chen CT, Chen YR. Endoscopically assisted repair of orbital floor fractures. Plast Reconstr Surg 2001;108: (Grade C). 12. Persons BL, Wong GB. Transantral endoscopic orbital floor repair using resorbable plate. J Craniofac Surg 2002;13: (Grade C). 13. Strong EB, Kim KK, Diaz RC. Endoscopic approach to orbital blowout fracture. Otolaryngol Head Neck Surg 2004;131: (Grade C). 14. Dulley B, Fells P. Long-term follow up of orbital blowout fracture with or without surgery. Mod Probl Ophthalmol 1970;19: (Grade B). 15. Lyon DB, Newman SA. Evidence of direct damage to extraocular muscles as a cause of diplopia following orbital trauma. Ophthal Plast Reconstr Surg 1989;5: (Grade C). 16. Thering HR, Bogart JN. Blowout fracture of the medial orbital wall with entrapment of the medial rectus muscle. Plast Reconstr Surg 1979;63: (Grade C). 17. Wojno TH. The incidence of extraocular muscle and cranial nerve palsy in orbital floor blow-out fractures. Ophthalmology 1987;94: (Grade B).
ORIGINAL RESEARCH FACIAL PLASTIC AND RECONSTRUCTIVE SURGERY METHODS
 Otolaryngology Head and Neck Surgery (2009) 140, 849-854 ORIGINAL RESEARCH FACIAL PLASTIC AND RECONSTRUCTIVE SURGERY Endoscopic transantral repair of orbital floor fractures Yadranko Ducic, MD, and Daniel
Otolaryngology Head and Neck Surgery (2009) 140, 849-854 ORIGINAL RESEARCH FACIAL PLASTIC AND RECONSTRUCTIVE SURGERY Endoscopic transantral repair of orbital floor fractures Yadranko Ducic, MD, and Daniel
By James D. Gould, MD FACS
 By James D. Gould, MD FACS BACKGROUND Balloon devices enlarge narrowed sinus ostia and outflow tracts by remodeling the surrounding bone and paranasal sinus structures. Multiple studies have demonstrated
By James D. Gould, MD FACS BACKGROUND Balloon devices enlarge narrowed sinus ostia and outflow tracts by remodeling the surrounding bone and paranasal sinus structures. Multiple studies have demonstrated
La décompression orbitaire dans la maladie de Basedow
 La décompression orbitaire dans la maladie de Basedow P. Mahy 1, C. Daumerie 2, A. Boschi 3 Services de stomatologie et chirurgie maxillo-faciale 1 d endocrinologie et de nutrition 2 et d ophtalmologie
La décompression orbitaire dans la maladie de Basedow P. Mahy 1, C. Daumerie 2, A. Boschi 3 Services de stomatologie et chirurgie maxillo-faciale 1 d endocrinologie et de nutrition 2 et d ophtalmologie
Surgery of the Frontal Sinus
 Surgery of the Frontal Sinus Steven D. Pletcher MD Assistant Professor Department of Otolaryngology Head and Neck Surgery University of California, San Francisco Disclosures Co-author patent application
Surgery of the Frontal Sinus Steven D. Pletcher MD Assistant Professor Department of Otolaryngology Head and Neck Surgery University of California, San Francisco Disclosures Co-author patent application
Lateral Canthoplasty by the Micro-Mitek Anchor System: 10-Year Review of 96 Patients
 CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY J Oral Maxillofac Surg 69:1745-1749, 2011 Lateral Canthoplasty by the Micro-Mitek Anchor System: 10-Year Review of 96 Patients Carmine Alfano, MD,* Stefano
CRANIOMAXILLOFACIAL DEFORMITIES/COSMETIC SURGERY J Oral Maxillofac Surg 69:1745-1749, 2011 Lateral Canthoplasty by the Micro-Mitek Anchor System: 10-Year Review of 96 Patients Carmine Alfano, MD,* Stefano
PROTOCOLS FOR INJURIES TO THE EYE
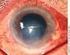 CORNEAL ABRASION PROTOCOLS FOR INJURIES TO THE EYE A corneal abrasion is usually caused by a foreign body or other object striking the eye. This results in a disruption of the corneal epithelium. Patients
CORNEAL ABRASION PROTOCOLS FOR INJURIES TO THE EYE A corneal abrasion is usually caused by a foreign body or other object striking the eye. This results in a disruption of the corneal epithelium. Patients
Fourth Nerve Palsy (a.k.a. Superior Oblique Palsy)
 Hypertropia Hypertropia is a type of strabismus characterized by vertical misalignment of the eyes. Among the many causes of vertical strabismus, one of the most common is a fourth nerve palsy (also known
Hypertropia Hypertropia is a type of strabismus characterized by vertical misalignment of the eyes. Among the many causes of vertical strabismus, one of the most common is a fourth nerve palsy (also known
Chapter 10. All chapters, full text, free download, available at http://www.divingmedicine.info SINUS BAROTRAUMA ANATOMY OF THE SINUSES
 Chapter 10 All chapters, full text, free download, available at http://www.divingmedicine.info SINUS BAROTRAUMA ANATOMY OF THE SINUSES The sinuses are air filled cavities contained within the bones of
Chapter 10 All chapters, full text, free download, available at http://www.divingmedicine.info SINUS BAROTRAUMA ANATOMY OF THE SINUSES The sinuses are air filled cavities contained within the bones of
YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY
 YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY What is functional endoscopic sinus surgery (FESS)? Functional endoscopic sinus surgery
YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY What is functional endoscopic sinus surgery (FESS)? Functional endoscopic sinus surgery
Surgical Treatment of Chronic Rhinosinusitis in. Children
 Surgical Treatment of Chronic Rhinosinusitis in Children Fuad M. Baroody, M.D., F.A.C.S. Professor of Otolaryngology-Head and Neck Surgery and Pediatrics The University of Chicago Medicine and Biological
Surgical Treatment of Chronic Rhinosinusitis in Children Fuad M. Baroody, M.D., F.A.C.S. Professor of Otolaryngology-Head and Neck Surgery and Pediatrics The University of Chicago Medicine and Biological
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
What is Balloon Sinuplasty?
 What is Balloon Sinuplasty? The painful symptoms associated with chronic sinusitis can be overwhelming. If symptoms are difficult to control with medications alone, your primary doctor may refer you to
What is Balloon Sinuplasty? The painful symptoms associated with chronic sinusitis can be overwhelming. If symptoms are difficult to control with medications alone, your primary doctor may refer you to
Titanium Wire with Barb and Needle. For canthal tendon procedures.
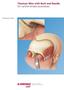 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Institute of Ophthalmology. Thyroid Eye Disease. aka Thyroid Associated Ophthalmopathy
 Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Endoscopic Orbital and Optic Nerve Decompression
 Otolaryngol Clin N Am 39 (2006) 551 561 Endoscopic Orbital and Optic Nerve Decompression Ralph Metson, MD a,b, *, Steven D. Pletcher, MD b a Department of Otology and Laryngology, Harvard Medical School,
Otolaryngol Clin N Am 39 (2006) 551 561 Endoscopic Orbital and Optic Nerve Decompression Ralph Metson, MD a,b, *, Steven D. Pletcher, MD b a Department of Otology and Laryngology, Harvard Medical School,
New treatment options for chronic sinusitis
 New treatment options for chronic sinusitis Balloon Sinuplasty Technology Vishram Jalukar, MD Mason City Clinic ENT & Allergy MKT01014 Rev. D Sinusitis Overview Inflammation of the sinus lining caused
New treatment options for chronic sinusitis Balloon Sinuplasty Technology Vishram Jalukar, MD Mason City Clinic ENT & Allergy MKT01014 Rev. D Sinusitis Overview Inflammation of the sinus lining caused
Unilateral Nasal Polyps
 Unilateral Nasal Polyps This tutorial follows on from the rhinosinusitis tutorial but only concerns itself with the unilateral nasal polyp. The majority of unilateral nasal polyps form in the same way
Unilateral Nasal Polyps This tutorial follows on from the rhinosinusitis tutorial but only concerns itself with the unilateral nasal polyp. The majority of unilateral nasal polyps form in the same way
Introduction. 31 million Americans suffer from chronic sinusitis Surgical treatment for chronic sinusitis has evolved tremendously since its inception
 Balloon Sinuplasty Ki-Hong Kevin Ho, MD Faculty Advisor: Patricia Maeso, MD Department of Otolaryngology The University of Texas Medical Branch Grand Rounds Presentation December 16, 2009 Introduction
Balloon Sinuplasty Ki-Hong Kevin Ho, MD Faculty Advisor: Patricia Maeso, MD Department of Otolaryngology The University of Texas Medical Branch Grand Rounds Presentation December 16, 2009 Introduction
Thyroid eye disease (TED)
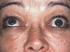 Thyroid eye disease (TED) Mr David H Verity, MD MA FRCOphth Consultant Ophthalmic Surgeon Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy This information leaflet
Thyroid eye disease (TED) Mr David H Verity, MD MA FRCOphth Consultant Ophthalmic Surgeon Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy This information leaflet
Cheekbone (zygoma) and/or eye socket (orbit) fracture surgery
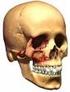 Ambulatory Care & Local Networks Cheekbone (zygoma) and/or eye socket (orbit) fracture surgery Information for patients You have been treated in the Emergency Department for a broken (fractured) cheekbone
Ambulatory Care & Local Networks Cheekbone (zygoma) and/or eye socket (orbit) fracture surgery Information for patients You have been treated in the Emergency Department for a broken (fractured) cheekbone
Thyroid eye disease (TED) Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy
 Thyroid eye disease (TED) Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy This information leaflet briefly covers the following issues in TED: What is TED? When
Thyroid eye disease (TED) Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy This information leaflet briefly covers the following issues in TED: What is TED? When
How To Harvest Fat From The Infratemporal Fossila
 Techniques in Cosmetic Surgery Harvesting Fat from the Infratemporal Fossa Bahman Guyuron, M.D., and Kevin Rose, M.D. Cleveland, Ohio As part of forehead rejuvenation and surgical treatment of migraine
Techniques in Cosmetic Surgery Harvesting Fat from the Infratemporal Fossa Bahman Guyuron, M.D., and Kevin Rose, M.D. Cleveland, Ohio As part of forehead rejuvenation and surgical treatment of migraine
Heel Pain Syndromes DELLON INSTITUTES FOR PERIPHERAL NERVE SURGERY
 Heel Pain s 5 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Pain, numbness or burning in your heel. The timing of this pain and
Heel Pain s 5 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Pain, numbness or burning in your heel. The timing of this pain and
GUIDELINE Sinusitis. David M. Poetker MD, MA Associate Professor. Division of Rhinology and Sinus Surgery
 GUIDELINE Sinusitis David M. Poetker MD, MA Associate Professor Division of Rhinology and Sinus Surgery Guideline Fokkens et al. The European Position Paper on Rhinosinusitis and Nasal Polyps 2012. Rhinology.
GUIDELINE Sinusitis David M. Poetker MD, MA Associate Professor Division of Rhinology and Sinus Surgery Guideline Fokkens et al. The European Position Paper on Rhinosinusitis and Nasal Polyps 2012. Rhinology.
X-Plain Sinus Surgery Reference Summary
 X-Plain Sinus Surgery Reference Summary Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus
X-Plain Sinus Surgery Reference Summary Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus
Coding Endoscopic Sinus Surgery
 Coding Endoscopic Sinus Surgery Audio Seminar/Webinar July 31, 2008 Practical Tools for Seminar Learning Copyright 2008 American Health Information Management Association. All rights reserved. Disclaimer
Coding Endoscopic Sinus Surgery Audio Seminar/Webinar July 31, 2008 Practical Tools for Seminar Learning Copyright 2008 American Health Information Management Association. All rights reserved. Disclaimer
Blepharoplasty & Cosmetic eyelid surgery
 Our cosmetic surgery team at The USF Eye Institute offers a wide variety of cosmetic procedures of the eyelids and face with the goal of obtaining a natural and rejuvenated appearance. Dr.Leyngold has
Our cosmetic surgery team at The USF Eye Institute offers a wide variety of cosmetic procedures of the eyelids and face with the goal of obtaining a natural and rejuvenated appearance. Dr.Leyngold has
Facial Nerve Paralysis: Management of the Eye
 Facial Nerve Paralysis: Management of the Eye Facial Nerve Paralysis: Management of the Eye Introduction Anatomy Options Discussion of Literature Introduction-Facial Nerve Paralysis Functional and cosmetic
Facial Nerve Paralysis: Management of the Eye Facial Nerve Paralysis: Management of the Eye Introduction Anatomy Options Discussion of Literature Introduction-Facial Nerve Paralysis Functional and cosmetic
Disclosure Statement. I have no financial interest in any of material presented today
 The eyes have it PEARLS IN EVALUATION, TREATMENT, AND REFERRAL OF PEDIATRIC OCULAR CONDITIONS AND TRAUMA MICHAEL G. HUNT, MD PEDIATRIC EYE SPECIALISTS, LLP Disclosure Statement I have no financial interest
The eyes have it PEARLS IN EVALUATION, TREATMENT, AND REFERRAL OF PEDIATRIC OCULAR CONDITIONS AND TRAUMA MICHAEL G. HUNT, MD PEDIATRIC EYE SPECIALISTS, LLP Disclosure Statement I have no financial interest
Facial Sports Injuries
 Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com
 Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Royal National Throat, Nose and Ear Hospital. Functional endoscopic sinus surgery (FESS) Ear, Nose and Throat Surgery
 Royal National Throat, Nose and Ear Hospital Functional endoscopic sinus surgery (FESS) Ear, Nose and Throat Surgery 31 If you need a large print, audio or translated copy of the document, please contact
Royal National Throat, Nose and Ear Hospital Functional endoscopic sinus surgery (FESS) Ear, Nose and Throat Surgery 31 If you need a large print, audio or translated copy of the document, please contact
UNMH Oral and Maxillofacial Surgery Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
Prevention and Management of Complications in Maxillary Sinus Surgery
 Prevention and Management of Complications in Maxillary Sinus Surgery Esther Kim, MD, James A. Duncavage, MD* KEYWORDS Maxillary antrostomy Management of complications Prevention of complications Caldwell-Luc
Prevention and Management of Complications in Maxillary Sinus Surgery Esther Kim, MD, James A. Duncavage, MD* KEYWORDS Maxillary antrostomy Management of complications Prevention of complications Caldwell-Luc
Surgical Coding Errors & English 101. Riva Lee Asbell. Fort Lauderdale, FL
 Surgical Coding Errors & English 101 Riva Lee Asbell Fort Lauderdale, FL INTRODUCTION Many surgical coding mistakes result from misinterpretation of CPT (Current Procedural Terminology) wording. When the
Surgical Coding Errors & English 101 Riva Lee Asbell Fort Lauderdale, FL INTRODUCTION Many surgical coding mistakes result from misinterpretation of CPT (Current Procedural Terminology) wording. When the
Robert Lingua M.D. Pediatric and Adult Strabismus Surgery www.eye.uci.edu
 Robert Lingua M.D. Pediatric and Adult Strabismus Surgery www.eye.uci.edu Augmented Sinskey Extirpation Procedure for Nystagmus. Robert W. Lingua, MD Updated 12/1/2014 The following information is being
Robert Lingua M.D. Pediatric and Adult Strabismus Surgery www.eye.uci.edu Augmented Sinskey Extirpation Procedure for Nystagmus. Robert W. Lingua, MD Updated 12/1/2014 The following information is being
IN THE UNITED STATES DISTRICT COURT FOR THE EASTERN DISTRICT OF PENNSYLVANIA : : : : : : : : : : FINDINGS OF FACT AND CONCLUSIONS OF LAW
 IN THE UNITED STATES DISTRICT COURT FOR THE EASTERN DISTRICT OF PENNSYLVANIA Harold Miterman, Plaintiff, v. United States of America, Defendant. CIVIL ACTION NO. 01-5352 FINDINGS OF FACT AND CONCLUSIONS
IN THE UNITED STATES DISTRICT COURT FOR THE EASTERN DISTRICT OF PENNSYLVANIA Harold Miterman, Plaintiff, v. United States of America, Defendant. CIVIL ACTION NO. 01-5352 FINDINGS OF FACT AND CONCLUSIONS
Tucson Eye Care, PC. Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens
 Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Open and Endoscopic Forehead Lift. Plastic Surgery. For All Brow and Forehead Lift Procedures. Revolutionizing. Soft-Tissue Fixation
 Plastic Surgery Open and Endoscopic Forehead Lift For All Brow and Forehead Lift Procedures Revolutionizing Soft-Tissue Fixation DESIGNED FOR SIMPLICITY AND PREDICTABILITY The versatile design can be applied
Plastic Surgery Open and Endoscopic Forehead Lift For All Brow and Forehead Lift Procedures Revolutionizing Soft-Tissue Fixation DESIGNED FOR SIMPLICITY AND PREDICTABILITY The versatile design can be applied
ALTERNATIVES TO LASIK
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
FESS surgical technique tips. and hints. Lujber László és a. szerző engedélyé. Prof. Dr. Imre Gerlinger
 FESS surgical technique tips and hints Prof. Dr. Imre Gerlinger 013 szakvizsga kötelező tanfolyam 013 szakvizsga kötelező tanfolyam Importance of cadaver dissection Position of the head Anaesthesia of
FESS surgical technique tips and hints Prof. Dr. Imre Gerlinger 013 szakvizsga kötelező tanfolyam 013 szakvizsga kötelező tanfolyam Importance of cadaver dissection Position of the head Anaesthesia of
Upper Eyelid Gold Weight Implantation in the Asian Patient with Facial Paralysis
 Upper Eyelid Gold Weight Implantation in the Asian Patient with Facial Paralysis Phillip H. Choo, M.D., Susan R. Carter, M.D., and Stuart R. Seiff, M.D. Sacramento and San Francisco, Calif. Patients with
Upper Eyelid Gold Weight Implantation in the Asian Patient with Facial Paralysis Phillip H. Choo, M.D., Susan R. Carter, M.D., and Stuart R. Seiff, M.D. Sacramento and San Francisco, Calif. Patients with
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY NASOLABIAL FLAP FOR ORAL CAVITY RECONSTRUCTION Harry Wright, Scott Stephan, James Netterville Designed as a true myocutaneous flap pedicled
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY NASOLABIAL FLAP FOR ORAL CAVITY RECONSTRUCTION Harry Wright, Scott Stephan, James Netterville Designed as a true myocutaneous flap pedicled
(Immediate) Primary Versus Delayed Reconstruction of Human and Animal Bite
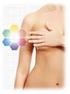 Egypt, J. Plast. Reconstr. Surg., Vol. 35, No. 2, July: 267-271, 2011 (Immediate) Primary Versus Delayed Reconstruction of Human and Animal Bite SAMY ELEOWA, M.D.; AHMED TAHA, M.D.; MOUSTAFA MEKY, M.D.
Egypt, J. Plast. Reconstr. Surg., Vol. 35, No. 2, July: 267-271, 2011 (Immediate) Primary Versus Delayed Reconstruction of Human and Animal Bite SAMY ELEOWA, M.D.; AHMED TAHA, M.D.; MOUSTAFA MEKY, M.D.
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery
 Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
POEM Procedure for. Esophageal Achalasia
 POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
Tissue Reinforcement with Strattice Reconstructive Tissue Matrix following Correction of Severe Breast Deformity
 Tissue Reinforcement with Strattice Reconstructive Tissue Matrix following Correction of Severe Breast Deformity Robert Cohen, MD, FACS* Paradise Valley, AZ Case summary A 41-year old woman with a history
Tissue Reinforcement with Strattice Reconstructive Tissue Matrix following Correction of Severe Breast Deformity Robert Cohen, MD, FACS* Paradise Valley, AZ Case summary A 41-year old woman with a history
Underestimation of Rhinogenic Causes in Patients Presenting to the Emergency Department with Acute Headache
 Original Article 37 Underestimation of Rhinogenic Causes in Patients Presenting to the Emergency Department with Acute Headache Jae-Heon Lee, Hyun-Jik Kim, Young-Ho Hong, Kyung-Soo Kim Abstract- Objectives:
Original Article 37 Underestimation of Rhinogenic Causes in Patients Presenting to the Emergency Department with Acute Headache Jae-Heon Lee, Hyun-Jik Kim, Young-Ho Hong, Kyung-Soo Kim Abstract- Objectives:
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Sinus and Nasal Surgery
 D E C A T U R M E M O R I A L H O S P I T A L Sinus and Nasal Surgery Introduction You are scheduled for sinus and nasal surgery. This helps open your sinuses and restore normal sinus functioning. Usually,
D E C A T U R M E M O R I A L H O S P I T A L Sinus and Nasal Surgery Introduction You are scheduled for sinus and nasal surgery. This helps open your sinuses and restore normal sinus functioning. Usually,
Outcomes of Levator Resection at Tertiary Eye Care Center in Iran: A 10-Year Experience
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(1):1-5 http://dx.doi.org/10.3341/kjo.2012.26.1.1 Original rticle Outcomes of Levator Resection at Tertiary Eye Care Center in Iran: 10-Year
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(1):1-5 http://dx.doi.org/10.3341/kjo.2012.26.1.1 Original rticle Outcomes of Levator Resection at Tertiary Eye Care Center in Iran: 10-Year
Transition Spaces. LJ Mariotti, DO Associate Professor of Surgery The Commonwealth Medical College Scranton, PA
 Transition Spaces LJ Mariotti, DO Associate Professor of Surgery The Commonwealth Medical College Scranton, PA Messerklinger considered these the spaces between the sinus proper and the nose He called
Transition Spaces LJ Mariotti, DO Associate Professor of Surgery The Commonwealth Medical College Scranton, PA Messerklinger considered these the spaces between the sinus proper and the nose He called
Dr. Booth received his medical degree from the University of California: San Diego and his bachelor of science from Stanford University.
 We've developed this handbook to help our patients become better informed about the entire process of laser vision correction. We hope you find it helpful and informative. Dr. Booth received his medical
We've developed this handbook to help our patients become better informed about the entire process of laser vision correction. We hope you find it helpful and informative. Dr. Booth received his medical
Corporate Medical Policy Reconstructive Eyelid Surgery and Brow Lift
 Corporate Medical Policy Reconstructive Eyelid Surgery and Brow Lift File Name: Origination: Last CAP Review: Next CAP Review: Last Review: reconstructive_eyelid_surgery_and_brow_lift 1/2000 9/2015 9/2016
Corporate Medical Policy Reconstructive Eyelid Surgery and Brow Lift File Name: Origination: Last CAP Review: Next CAP Review: Last Review: reconstructive_eyelid_surgery_and_brow_lift 1/2000 9/2015 9/2016
RAPID CLINICAL REPORT
 RAPID CLINICAL REPORT ADVERSE EFFECTS ASSOCIATED WITH THE ABSENCE OF HYALURONIDASE IN ANESTHESIA FOR CATARACT SURGERY Background: Issued February 13, 2001 Hyaluronidase (Wydase ) is a medical preparation
RAPID CLINICAL REPORT ADVERSE EFFECTS ASSOCIATED WITH THE ABSENCE OF HYALURONIDASE IN ANESTHESIA FOR CATARACT SURGERY Background: Issued February 13, 2001 Hyaluronidase (Wydase ) is a medical preparation
Comment prendre en charge une épistaxis sévère en médecine ambulatoire?!
 Comment prendre en charge une épistaxis sévère en médecine ambulatoire? Prof. dr. Thibaut. Van Zele Prof. dr. Jean-Baptiste Watelet dienst neus-, keel- en oorheelkunde Universitair Ziekenhuis Gent 2013
Comment prendre en charge une épistaxis sévère en médecine ambulatoire? Prof. dr. Thibaut. Van Zele Prof. dr. Jean-Baptiste Watelet dienst neus-, keel- en oorheelkunde Universitair Ziekenhuis Gent 2013
5 Upper eyelid blepharoplasty
 5 Upper eyelid blepharoplasty INSTRUMENTS Marking pen No. 15 scalpel blade Blade handle Castroviejo needle holder Castroviejo calipers 0.5 fixation forceps Westcott scissors 6-0 prolene suture Bovie cautery
5 Upper eyelid blepharoplasty INSTRUMENTS Marking pen No. 15 scalpel blade Blade handle Castroviejo needle holder Castroviejo calipers 0.5 fixation forceps Westcott scissors 6-0 prolene suture Bovie cautery
Update on Surgical Treatment of Pituitary Tumors. Kristen Riley, MD, FACS Associate Professor, Division of Neurosurgery, Department of Surgery
 Update on Surgical Treatment of Pituitary Tumors Kristen Riley, MD, FACS Associate Professor, Division of Neurosurgery, Department of Surgery Pituitary Tumors Pituitary adenoma: common intracranial neoplasm
Update on Surgical Treatment of Pituitary Tumors Kristen Riley, MD, FACS Associate Professor, Division of Neurosurgery, Department of Surgery Pituitary Tumors Pituitary adenoma: common intracranial neoplasm
Septoplasty and Turbinate Reduction Surgical Information
 Septoplasty and Turbinate Reduction Surgical Information PREOPERATIVE DISCUSSION FOR SEPTOPLASTY and TURBINATE REDUCTION Septoplasty The nasal septum is made of cartilage and bone covered with a lining
Septoplasty and Turbinate Reduction Surgical Information PREOPERATIVE DISCUSSION FOR SEPTOPLASTY and TURBINATE REDUCTION Septoplasty The nasal septum is made of cartilage and bone covered with a lining
Mesh Plug Repair of Inguinal Hernias. Presented by: V.K Ashok, M.D, F.A.C.S
 Mesh Plug Repair of Inguinal Hernias Presented by: V.K Ashok, M.D, F.A.C.S April 2, 2011 About V.K. Ashok, M.D Practicing general and vascular surgeon in private practice based in Freehold, NJ for the
Mesh Plug Repair of Inguinal Hernias Presented by: V.K Ashok, M.D, F.A.C.S April 2, 2011 About V.K. Ashok, M.D Practicing general and vascular surgeon in private practice based in Freehold, NJ for the
Quick Facts about Breast Augmentation with IDEAL IMPLANT Saline-filled Breast Implants
 Quick Facts about Breast Augmentation with IDEAL IMPLANT Saline-filled Breast Implants Important Factors Breast Augmentation Patients Should Consider October 2015 Caution: Federal law restricts this device
Quick Facts about Breast Augmentation with IDEAL IMPLANT Saline-filled Breast Implants Important Factors Breast Augmentation Patients Should Consider October 2015 Caution: Federal law restricts this device
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Laparoscopic Repair of Incisional Hernia. Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds
 Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Balloon catheter sinusotomy: One-year follow-up Outcomes and role in functional endoscopic sinus surgery
 Otolaryngology Head and Neck Surgery (2008) 139, S27-S37 ORIGINAL RESEARCH Balloon catheter sinusotomy: One-year follow-up Outcomes and role in functional endoscopic sinus surgery Frederick A. Kuhn, MD,
Otolaryngology Head and Neck Surgery (2008) 139, S27-S37 ORIGINAL RESEARCH Balloon catheter sinusotomy: One-year follow-up Outcomes and role in functional endoscopic sinus surgery Frederick A. Kuhn, MD,
Surgical Outcome Of Incomitant Exotropia In Patients With Partial Third Nerve Palsy
 Surgical Outcome Of Incomitant Exotropia In Patients With Partial Third Nerve Palsy Amit Mohan, MS ; Sudhir Singh, MS ; Dr V.C. Bhatnagar, MS, DNB Dr Amit Mohan, MS Jr.Consultant Global Hospital Institute
Surgical Outcome Of Incomitant Exotropia In Patients With Partial Third Nerve Palsy Amit Mohan, MS ; Sudhir Singh, MS ; Dr V.C. Bhatnagar, MS, DNB Dr Amit Mohan, MS Jr.Consultant Global Hospital Institute
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
Chapter 24. Evolution of Procedures
 Chapter 24 BREAST SURGERY KEY FIGURES: Saline implant reconstruction Latissimus dorsi reconstruction Free TRAM reconstruction In the developed world, breast reconstruction after mastectomy and breast reduction
Chapter 24 BREAST SURGERY KEY FIGURES: Saline implant reconstruction Latissimus dorsi reconstruction Free TRAM reconstruction In the developed world, breast reconstruction after mastectomy and breast reduction
Lower eyelid retraction, secondary to middle lamellar cicatrix,
 SURGICAL TECHNIQUE En-Glove Lysis of Lower Eyelid Retractors With AlloDerm and Dermis-Fat Grafts in Lower Eyelid Retraction Surgery Heather S. Chang, M.D.*, Diana Lee, B.S.*, Mehryar Taban, M.D.*, Raymond
SURGICAL TECHNIQUE En-Glove Lysis of Lower Eyelid Retractors With AlloDerm and Dermis-Fat Grafts in Lower Eyelid Retraction Surgery Heather S. Chang, M.D.*, Diana Lee, B.S.*, Mehryar Taban, M.D.*, Raymond
IntraLase and LASIK: Risks and Complications
 No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
Balloon Sinuplasty for Chronic Sinusitis: The Latest Recommendations
 Balloon Sinuplasty for Chronic Sinusitis: The Latest Recommendations Shannon Hunter, MD Board-Certified Otolaryngologist Thank you for joining us today We are recording this webinar and will be sending
Balloon Sinuplasty for Chronic Sinusitis: The Latest Recommendations Shannon Hunter, MD Board-Certified Otolaryngologist Thank you for joining us today We are recording this webinar and will be sending
Endoscopic Surgical Treatment of Chronic Maxillary Sinusitis of Dental Origin
 Endoscopic Surgical Treatment of Chronic Maxillary Sinusitis of Dental Origin Fabio Costa, MD,* Enzo Emanuelli, MD, Massimo Robiony, MD, FEBOMS, Nicoletta Zerman, MD, Francesco Polini, MD, and Massimo
Endoscopic Surgical Treatment of Chronic Maxillary Sinusitis of Dental Origin Fabio Costa, MD,* Enzo Emanuelli, MD, Massimo Robiony, MD, FEBOMS, Nicoletta Zerman, MD, Francesco Polini, MD, and Massimo
Clinical Privileges Profile Plastic Surgery. Indu & Raj Soin Medical Center
 Printed Name Clinical Privileges Profile Plastic Surgery Indu & Raj Soin Medical Center Applicant: Check off the Requested box for each privilege requested. Applicants have the burden of producing information
Printed Name Clinical Privileges Profile Plastic Surgery Indu & Raj Soin Medical Center Applicant: Check off the Requested box for each privilege requested. Applicants have the burden of producing information
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Lip Cancer: Treatment & Reconstruction
 Lip Cancer: Treatment & Reconstruction GBMC - Head & Neck Cancer Grand Rounds Elizabeth E. Redd, M.D. With the assistance of Ira Papel, M.D. Patrick Byrne, M.D. Lip Cancer: Treatment & Reconstruction Anatomic
Lip Cancer: Treatment & Reconstruction GBMC - Head & Neck Cancer Grand Rounds Elizabeth E. Redd, M.D. With the assistance of Ira Papel, M.D. Patrick Byrne, M.D. Lip Cancer: Treatment & Reconstruction Anatomic
INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) USING INTRALASE TM BLADE-FREE TECHNOLOGY
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) USING INTRALASE TM BLADE-FREE
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) USING INTRALASE TM BLADE-FREE
Cranial/Neurosurgical Implants
 MEDPOR Cranial/Neurosurgical Implants MEDPOR Biomaterial MEDPOR Porous Polyethylene Implants provide surgeons with an expanding range of options for reconstruction and augmentation. MEDPOR is a biocompatible,
MEDPOR Cranial/Neurosurgical Implants MEDPOR Biomaterial MEDPOR Porous Polyethylene Implants provide surgeons with an expanding range of options for reconstruction and augmentation. MEDPOR is a biocompatible,
Fat Injection to Correct Contour Deformities in the Reconstructed Breast
 Fat Injection to Correct Contour Deformities in the Reconstructed Breast Scott L. Spear, M.D., Henry B. Wilson, M.D., and Michelle D. Lockwood, M.D. Washington, D.C. Background: A ten-year, single-surgeon
Fat Injection to Correct Contour Deformities in the Reconstructed Breast Scott L. Spear, M.D., Henry B. Wilson, M.D., and Michelle D. Lockwood, M.D. Washington, D.C. Background: A ten-year, single-surgeon
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
a guide to understanding crouzon syndrome a publication of children s craniofacial association
 a guide to understanding crouzon syndrome a publication of children s craniofacial association a guide to understanding crouzon syndrome this parent s guide to Crouzon syndrome is designed to answer questions
a guide to understanding crouzon syndrome a publication of children s craniofacial association a guide to understanding crouzon syndrome this parent s guide to Crouzon syndrome is designed to answer questions
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Sinus Headache vs. Migraine
 Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY
 INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment
 Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Long-Term Outcomes of Flap Amputation After LASIK
 Long-Term Outcomes of Flap Amputation After LASIK Priyanka Chhadva BS, Florence Cabot MD, Anat Galor MD, Sonia H. Yoo MD Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami
Long-Term Outcomes of Flap Amputation After LASIK Priyanka Chhadva BS, Florence Cabot MD, Anat Galor MD, Sonia H. Yoo MD Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami
INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY
 INTRODUCTION INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
INTRODUCTION INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
How To Recover From A Surgical Wound From A Cast
 Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System
 White PAPer Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System Jerome Hester, MD Chief Medical Officer SinuSys Corporation Palo Alto, California USA introduction Establishment
White PAPer Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System Jerome Hester, MD Chief Medical Officer SinuSys Corporation Palo Alto, California USA introduction Establishment
EYE MUSCLE SURGERY. I am on staff and perform surgery at the following facilities: HCA Gulf Coast Surgery Center of Bradenton
 1 EYE MUSCLE SURGERY Prepared by Scott E. Silverman, M.D. Strabismus is a misalignment of the eyes. The eyes may cross or drift up or out. Strabismus may be present from birth or may develop in childhood.
1 EYE MUSCLE SURGERY Prepared by Scott E. Silverman, M.D. Strabismus is a misalignment of the eyes. The eyes may cross or drift up or out. Strabismus may be present from birth or may develop in childhood.
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Post Surgical Care of Patella Luxation Repair
 Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
1 of 6 2/10/12 10:15 AM
 Home Dr. Bitar About Us Events Media Specialties Non Surgical Gallery Fees Contact Us Plastic Surgery Products Magazine, October 2007 Issue Breast Augmentation: The Axillary Approach by George John Bitar,
Home Dr. Bitar About Us Events Media Specialties Non Surgical Gallery Fees Contact Us Plastic Surgery Products Magazine, October 2007 Issue Breast Augmentation: The Axillary Approach by George John Bitar,
BREAST IMPLANTS (enlargement, augmentation) Dr. Benjamin Van Raalte TYPES OF IMPLANTS saline round implants high profiles low profile shaped
 BREAST IMPLANTS (enlargement, augmentation) Dr. Benjamin Van Raalte has 20 years of experience with breast enlargement including axillary incisions and gel implants. Dr. Van Raalte is the first Quad City
BREAST IMPLANTS (enlargement, augmentation) Dr. Benjamin Van Raalte has 20 years of experience with breast enlargement including axillary incisions and gel implants. Dr. Van Raalte is the first Quad City
BRYAN. Cervical Disc System. Patient Information
 BRYAN Cervical Disc System Patient Information 3 BRYAN Cervical Disc System PATIENT INFORMATION BRYAN Cervical Disc System PATIENT INFORMATION 1 BRYAN Cervical Disc System This patient information brochure
BRYAN Cervical Disc System Patient Information 3 BRYAN Cervical Disc System PATIENT INFORMATION BRYAN Cervical Disc System PATIENT INFORMATION 1 BRYAN Cervical Disc System This patient information brochure
Facial Fractures from Dog Bite Injuries
 Facial Fractures from Dog Bite Injuries Alexander H. Tu, B.A., John A. Girotto, M.D., Navin Singh, M.D., Craig R. Dufresne, M.D., Bradley C. Robertson, M.D., D.D.S., Alan E. Seyfer, M.D., Paul N. Manson,
Facial Fractures from Dog Bite Injuries Alexander H. Tu, B.A., John A. Girotto, M.D., Navin Singh, M.D., Craig R. Dufresne, M.D., Bradley C. Robertson, M.D., D.D.S., Alan E. Seyfer, M.D., Paul N. Manson,
SURGICAL TREATMENT OF NASAL CONGESTION AND RHINORRHEA
 SURGICAL TREATMENT OF NASAL CONGESTION AND RHINORRHEA 2010 Allergy Symposium November 6, 2010 David Keschner, MD, JD HNS Orange County General Introduction Overview of material Anatomy and Clinical Features
SURGICAL TREATMENT OF NASAL CONGESTION AND RHINORRHEA 2010 Allergy Symposium November 6, 2010 David Keschner, MD, JD HNS Orange County General Introduction Overview of material Anatomy and Clinical Features
Nasal polyps differ in terms of origin, as well
 Focus on CME at the University of Saskatchewan Clearing the Air on Nasal Polyps By Gordon Franke, MD, BSc, FRCS(C) Presented at the University of Saskatchewan Practical Otolaryngology Conference 2003,
Focus on CME at the University of Saskatchewan Clearing the Air on Nasal Polyps By Gordon Franke, MD, BSc, FRCS(C) Presented at the University of Saskatchewan Practical Otolaryngology Conference 2003,
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
