Comparative Effectiveness Study of Patient-Reported Outcomes After Proton Therapy or Intensity-Modulated Radiotherapy for Prostate Cancer
|
|
|
- Jessica Patterson
- 8 years ago
- Views:
Transcription
1 Comparative Effectiveness Study of Patient-Reported Outcomes After Proton Therapy or Intensity-Modulated Radiotherapy for Prostate Cancer Bradford S. Hoppe, MD, MPH 1 ; Jeff M. Michalski, MD 2 ; Nancy P. Mendenhall, MD 1 ; Christopher G. Morris, MS 1 ; Randal H. Henderson, MD 1 ; Romaine C. Nichols, MD 1 ; William M. Mendenhall, MD 1 ; Christopher R. Williams, MD 3 ; Meredith M. Regan, ScD 4 ; Jonathan J. Chipman, MS 4 ; Catrina M. Crociani, MPH 5 ; Howard M. Sandler, MD 6 ; Martin G. Sanda, MD 7 ; and Daniel A. Hamstra, MD, PhD 8 BACKGROUND: Data continue to emerge on the relative merits of different treatment modalities for prostate cancer. The objective of this study was to compare patient-reported quality-of-life (QOL) outcomes after proton therapy (PT) and intensity-modulated radiation therapy (IMRT) for prostate cancer. METHODS: A comparison was performed of prospectively collected QOL data using the Expanded Prostate Cancer Index Composite (EPIC) questionnaire. QOL data were collected during the first 2 years after treatment for men who received PT and IMRT. PT was delivered to 1243 men at a single center at doses from 76 grays (Gy) to 82 Gy. IMRT was delivered to 204 men who were included in the Prostate Cancer Outcomes and Satisfaction with Treatment Quality Assessment (PROSTQA) study in doses from 75.6 Gy to 79.4 Gy. The Wilcoxon rank-sum test was used to compare EPIC outcomes by modality using baseline-adjusted scores at different time points. Individual questions were assessed by converting to binary outcomes and testing with generalized estimating equations. RESULTS: No differences were observed in summary score changes for bowel, urinary incontinence, urinary irritative=obstructive, and sexual domains between the 2 cohorts. However, more men who received IMRT reported moderate=big problems with rectal urgency (P ) and frequent bowel movements (P ) than men who received PT. CONCLUSIONS: There were no differences in QOL summary scores between the IMRT and PT cohorts during early follow-up (up to 2-years). Response to individual questions suggests possible differences in specific bowel symptoms between the 2 cohorts. These outcomes highlight the need for further comparative studies of PT and IMRT. Cancer 2014;120: VC 2013 The Authors. Cancer published by Wiley Periodicals, Inc. on behalf of American Cancer Society. This is an open access article under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs License, which permits use and distribution in any medium, provided the original work is properly cited, the use is non- commercial and no modifications or adaptations are made. KEYWORDS: proton therapy, intensity-modulated radiotherapy, prostate cancer, outcomes, genitourinary. INTRODUCTION Conformal radiotherapy (RT) techniques for prostate cancer are expected to reduce urinary and rectal toxicity 1 and improve disease control through facilitation of dose escalation. 2 The increased costs associated with these techniques 3 have led payors and insurers to demand clinical data demonstrating improved disease control and=or less toxicity. Corresponding author: Bradford Hoppe, MD, MPH, University of Florida Proton Therapy Institute, 2015 North Jefferson Street, Jacksonville, FL 32206; Fax: (904) ; bhoppe@floridaproton.org 1 University of Florida Proton Therapy Institute, Jacksonville, Florida; 2 Department of Radiation Oncology, Washington University, St. Louis, Missouri; 3 Department of Urology, University of Florida, Jacksonville, Florida; 4 Department of Biostatistics and Computational Biology, Dana-Farber Cancer Institute, Boston, Massachusetts; 5 Division of Urology, Department of Surgery, Beth Israel Deaconess Medical Center, Boston, Massachusetts; 6 Department of Radiation Oncology, Cedars Sinai Medical Center, Los Angeles, California; 7 Department of Urology, Emory University, Atlanta, Georgia; 8 Department of Radiation Oncology, University of Michigan, Ann Arbor, Michigan Presented at the 55th Annual Meeting of the American Society for Radiation Oncology; Atlanta, Georgia; September 22-25, The Prostate Cancer Outcomes and Satisfaction with Treatment Quality Assessment (PROSTQA) Consortium includes contributions in cohort design, patient accrual, and follow-up from the following investigators: Larry Hembroff (Michigan State University, East Lansing, Mich); John T. Wei and Laurel Northouse (University of Michigan, Ann Arbor, Mich); Eric A. Klein and Jay Ciezki (Cleveland Clinic, Cleveland, Ohio); Gerald Andriole (Washington University, St. Louis, Mo); Mark Litwin and Chris Saigal (University of California-Los Angeles Medical Center, Los Angeles, Calif); Thomas Greenfield, PhD (Berkeley, Calif); Louis Pisters and Deborah Kuban (The University of Texas MD Anderson Cancer Center, Houston, Tex); Jim Hu and Adam Kibel (Brigham and Women s Hospital, Boston, Mass); Douglas Dahl and Anthony Zietman (Massachusetts General Hospital, Boston, Mass); and Peter Chang and Irving Kaplan (Beth Israel Deaconess Medical Center, Boston, Mass). We acknowledge PROSTQA Data Coordinating Center Project Management by Jill Hardy, MS (Michigan State University, East Lansing, Mich) and Erin Najuch (Dana Farber Cancer Institute, Boston, Mass); grant administration by Beth Doiron, BA (Beth Israel Deaconess Medical Center, Boston, Mass); and technical support from coordinators at each clinical site. DOI: /cncr.28536, Received: October 8, 2013; Revised: November 21, 2013; Accepted: November 25, 2013, Published online December 30, 2013 in Wiley Online Library (wileyonlinelibrary.com) 1076 Cancer April 1, 2014
2 Outcomes After PT or IMRT/Hoppe et al Several comparative-effectiveness studies of conventional radiation therapy, 3-dimensional conformal radiation therapy (3DCRT), intensity-modulated RT (IMRT), and proton therapy (PT) have been reported. Those studies have in common a reliance on Medicare claims as surrogates for actual clinical outcomes, but they differ somewhat in their findings. 4-7 The use of Medicare claims rather than medical records may be a weakness, because medical claims codes identify interventions that may not reflect the relevant endpoints of disease control, specific treatment-related toxicity, or patient-reported quality of life (QOL). Some of the reports have attracted considerable criticism, 8,9 and the authors of 1 study acknowledge the limitations of the Medicare database and the need for patient-reported QOL outcomes. 7 A randomized trial comparing PT and IMRT has been opened, but the comparative impact on late effects will not be known for some years (registered as National Clinical Trial NCT ). We compared prospectively collected QOL outcomes of >1400 men from 2 databases who received treatment with PT or IMRT. MATERIALS AND METHODS Materials and Patients The Expanded Prostate Cancer Index Composite (EPIC)- 26 questionnaire is a validated instrument that has 5 domains, including urinary incontinence (UI) (4 questions), urinary irritative=obstructive (UO) (4 questions), bowel function (BS) (6 questions), sexual function (SS) (6 questions), and hormonal function (HF) (5 questions); each subscale is scored from 0 to 100, in which 100 represents no problems and 0 represents substantial and significant problems with the specific subscale. 10 Prospectively collected data from EPIC questionnaires from 2 patient cohorts that received PT and IMRT, respectively, were compared. The University of Florida Institutional Review Board approved the study, which included 1482 men with localized prostate cancer who were treated at the University of Florida with passively scattered PT between 2006 and Patients were excluded if they failed to complete treatment (n 5 6), did not consent to study inclusion (n 5 19), or received hypofractionated PT at 2.5 cobalt gray equivalent per fraction or weekly docetaxel on treatment protocols (n 5 71), or pelvic lymph node irradiation (n 5 45), leaving a total of 1243 men in the PT cohort. The EPIC questionnaires were collected on paper forms (before March 2009) or by a secure online medical records portal accessed over the Internet (after March 2009) at 6 months, 1 year, then annually. Specific details of the PT simulation and treatment have been previously reported. 11 Patients received 1.8 to 2 grays (Gy) per fraction, and the majority (99%; n ) received between 78 Gy and 82 Gy (relative biologic effectiveness) at 2 Gy (relative biologic effectiveness) per fraction. The second cohort included 204 men from the previously reported Prostate Cancer Outcomes and Satisfaction with Treatment Quality Assessment (PROSTQA) study who were treated at 9 university-affiliated hospitals with IMRT and who had completed EPIC-26 questionnaires before treatment and then at 2 months, 6 months, 12 months, and 24 months after treatment. These patients received treatment between March 2003 and March 2006, according to individual institutional policies, which consisted of IMRT to the prostate, with or without seminal vesicles, without pelvic RT, at doses from 75.6 to 79.2Gy at 1.8 to 2.0 Gy per fraction. 12 Data on actual doses delivered to the IMRT patients were not available, but minimum and maximum doses to the planning target volume (PTV) were available for comparison with the same dose parameters in the PT cohort. Because of variability in hormone use between the cohorts, differences in hormonal function or hormonal questions were not investigated. Statistics SAS and JMP software were used for all statistical analyses (SAS Institute, Cary, NC). Differences between the 2 cohorts of patients in pretreatment patient-specific, disease-specific, and treatment-specific characteristics were assessed using the Fisher exact test for categorical variables and the Wilcoxon rank-sum test for continuous variables (Table 1). Scores for the EPIC were calculated as previously described. 13,14 The 6-month, 1-year, and 2-year post-treatment scores for each modality were compared with the baseline data for that modality using the Wilcoxon signed-rank sum test, which is a nonparametric analog to a t test for paired data. Differences from pretreatment values >50% of the standard deviation 15 at any point in time were considered to represent the minimally detectable difference. Differences in pretreatment scores for the various subscales between the 2 cohorts were assessed with the Wilcoxon rank-sum test. The same method was used to compare baseline-adjusted outcomes between the 2 modalities at 6 months, 1 year, and 2 years after treatment; baseline adjustment for each patient and each domain was accomplished by subtracting the Cancer April 1,
3 TABLE 1. Patient-Specific, Cancer-Specific, and Treatment-Specific Characteristics Characteristic No. of Patients (%) IMRT (n 5 204) PT (n ) P Age: Mean [range], y 69 [46 84] 66 [40 to >89] <.001 Body mass index: Mean 6 SD, kg/m 2 Prostate size: Mean 6 SD, ml Race <.001 White 166 (81) 1132 (91) Black 34 (17) 77 (6) Other 4 (2) 34 (3) PSA, ng/ml.12 <4 37 (17) 205 (17) (63) 862 (69) >10 39 (19) 176 (14) Gleason score.28 <7 104 (51) 659 (53) 7 86 (42) 466 (37) >7 14 (7) 118 (10) Clinical tumor classification a.61 T1 148 (73) 922 (74) T2 56 (27) 317 (26) T3 0 (0) 3 (<1) Overall risk level.41 Low 83 (41) 567 (46) Intermediate 94 (46) 532 (43) High 27 (13) 143 (11) ADT 49 (24) 181 (15).001 PTVmin: Median 70.9 [ ] 74.1 [ ] <.001 [range], Gy PTVmax: Median [range], Gy 81.5 [ ] 83.2 [ ] <.001 Abbreviations: ADT, androgen-deprivation therapy; Gy, grays; IMRT, intensity-modulated radiotherapy; PSA, prostate-specific antigen; PT, proton therapy; PTVmin, minimum dose to the planned target volume; PTVmax, maximum dose to the planned target volume; SD, standard deviation. a One patient who received proton therapy had no tumor classification information available. baseline score from the 6-month, 1-year, and 2-year scores. Patients without a baseline score were excluded from the analysis. Because multiple domains were assessed for each patient, a post hoc Bonferroni adjustment was applied to the resulting P values (Tables 2 and 3). An adjusted P value <.05 was considered statistically significant. Two approaches were used to analyze dichotomized responses to each question covering urinary, bowel, and sexual function, as previously reported. 16 Baseline differences in individual question responses between the 2 modalities were assessed with the Fisher exact test. Sixmonth, 1-year, and 2-year responses were assessed simultaneously using repeated-measures generalized estimating equations with unstructured correlation through PROC GENMOD in SAS (Table 4). The primary prognostic TABLE 2. Raw Expanded Prostate Cancer Index Composite (EPIC) Scores With Adjusted P Values (Absolute Shift Compared With Baseline) Proton Therapy EPIC Score IMRT EPIC Domain at Follow-Up Median Min Max Median Min Max P a Bowel summary 6mo y y Urinary incontinence 6mo y y Urinary irritative/obstructive 6mo y y Sexual summary b 6mo y y Abbreviations: EPIC, Expanded Prostate Cancer Index Composite; IMRT, intensity-modulated radiotherapy; Max, maximum; Min, minimum. a P values were determined using the Wilcoxon rank-sum test with Bonferroni adjustment. b Sexual summary scores were calculated for men who did not receive androgen-deprivation therapy. TABLE 3. Percentage of Men With Minimally Detectable Differences From Their Baseline Expanded Prostate Cancer Index Composite Scores a EPIC Domain at Follow-Up Periods PT, % IMRT, % P b Bowel summary 6 mo y y Urinary incontinence 6 mo y y Urinary irritative/obstructive 6 mo y y Sexual summary 6 mo y y Abbreviations: EPIC, Expanded Prostate Cancer Index Composite; IMRT, intensity-modulated radiotherapy; PT, Proton Therapy. a These represent declines in scores >50% from baseline. b P values were determined using the Wilcoxon rank-sum test with Bonferonni adjustment. factor in each model was treatment modality, but baseline response, use of androgen-deprivation therapy (ADT), age (<65 years vs 65 years), and prostate size were entered into the models as covariates to control. A post 1078 Cancer April 1, 2014
4 Outcomes After PT or IMRT/Hoppe et al TABLE 4. Outcomes by Specific Expanded Prostate Cancer Index Composite Question Baseline 6 Months 1 Year 2 Years Question IMRT, % PT, % P a IMRT, % PT, % IMRT, % PT, % IMRT, % PT, % P b P c No. of patients answering EPIC d Urinary irritation/obstruction Dysuria Hematuria Weak stream Frequency Urinary incontinence Leaking > daily Frequent dribbling Any pad use Leaking problem Overall urinary problem Bowel function Urgency Frequency Fecal incontinence Bloody stools Rectal pain Overall bowel problem Sexual function e Poor erections Difficulty with orgasm Erection not firm < Erections not reliable Poor sexual function Overall sexuality problem Abbreviations: EPIC, Expanded Prostate Cancer Index Composite; IMRT, intensity-modulated radiotherapy; PT, proton therapy. a These P values were determined using the Fisher exact test. b These P values were determined using a generalized estimating equation with the values adjusted for baseline difference, androgen-deprivation therapy, age, and prostate size. c These P values also were determined using a generalized estimating equation with the values adjusted for baseline difference, androgen-deprivation therapy, age, and prostate size but included the addition of a Bonferroni adjustment for 21 questions. d These were recorded in absolute numbers. e Sexual function was reported for patients who did not receive androgen-deprivation therapy. hoc Bonferroni adjustment also was included to adjust for the 21 questions evaluated (excluding the hormone function questions, which were not used). RESULTS Patient-specific and treatment-specific characteristics are illustrated in Table 1. IMRT patients treated were older (median age, 69 vs 66 years; P <.001), had larger prostate volumes (mean, 49.5 vs 41.5 g; P ), were less likely to be white (81% vs 91% white; P <.001), were more likely to receive ADT (24% vs 15%; P ), and received both a lower minimum dose to the PTV (median, 70.9 vs 74.1 Gy; P <.001) and a lower maximum PTV dose (median, 81.5 vs 83.2Gy; P <.001). EPIC summary scores at baseline, 6 months, 1 year, and 2 years after treatment are depicted in Figure 1A-D for the PT and IMRT cohorts. After treatment, the only changes in summary scores from baseline that met the minimally detectable difference were observed for bowel summary at 6 months, 1 year, and 2 years for IMRT and for bowel summary at 1 year and 2 years for PT (Fig. 1A- D). Both groups had declines in bowel summary scores, but there were no statistically significant differences in QOL changes between groups for BS, UI, UO, or SS (SS was analyzed only among men who did not receive ADT) at any time (Table 2). When examining the percentage of men who had a minimally detectable difference at the various time points for the different summary scores, the only remarkable difference between the IMRT and PT cohorts was for the bowel summary component at the 6- month follow-up (Table 3). An analysis of individual items comprising each domain also was planned and performed. At baseline, the only differences between the 2 cohorts were that men in the IMRT cohort were more likely to report baseline moderate=big problems with hematuria (P ), daily urinary leakage (P 5.02), bloody stools (P 5.02), and rectal pain (P 5.04). Men in the IMRT cohort also reported more moderate=big problems within the sexual domain, including poor erections, difficulty with Cancer April 1,
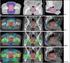
5 Figure 1. Expanded Prostate Cancer Index Composite (EPIC) summary scores are illustrated over time for men who received intensity-modulated radiotherapy (IMRT) or proton therapy (PT) for prostate cancer. Bar-and-whisker graphs at baseline and at 6 months (6M), 1 year (1Y), and 2 years (2Y) after proton therapy or intensity-modulated radiotherapy illustrate (A) bowel summary scores, (B) urinary incontinence scores, (C) urinary irritative=obstructive scores, and (D) sexual summary scores (no androgendeprivation therapy). The bottom whisker represents the cutoff score for the lowest 5%, the bottom bar represents the cutoff score for the lowest quartile, the blue line represents the median score, the top of the bar represents the cutoff score for the top quartile, and the top of the whisker represents the cutoff score for the top 5%. At the bottom of the graph, an asterisk indicates a statistically significant change from baseline score for each treatment modality and time point, and a pound sign indicates a statistically significant and minimally detectable change (>50% of the baseline standard deviation) from the baseline score. orgasms, erections not sufficient for intercourse, and unreliable erections (all P <.01) (Table 4). When comparisons over time were controlled for differences between groups in age, prostate size, and ADT use as well as baseline QOL, there were no significant differences between the cohorts except for more frequent reports in the IMRT cohort of moderate or big problems with rectal urgency (P 5.02) and bowel frequency (P 5.05). DISCUSSION The study reported herein compares patient-reported QOL outcomes in PT and IMRT cohorts using the EPIC questionnaire. No significant differences were observed in QOL EPIC summary scores for bowel, urinary, or sexual function between the IMRT and PT cohorts, despite higher minimum and maximum PTV doses in the PT cohort, a factor that is expected to be associated with higher toxicity. EPIC urinary summary scores were similar between the IMRT and PT cohorts in this study, concurring with similar urinary toxicity rates between IMRT and PT suggested by surrogate data reported in the Medicare studies. 5,6,17 However, the EPIC bowel outcomes in this study did not correlate with findings in 2 of the Medicare studies, 5,6 which suggested worse bowel toxicity with PT than with IMRT. The Medicare studies have been criticized for their reliance on surrogate data rather than actual clinical data, such as using colonoscopy claims to conclude rectal toxicity. Furthermore, absence of any clinical and treatment details in the Medicare studies also may have confounded conclusions, because radiation dose, dose fractionation, and dose distribution, the most important predictive factors for gastrointestinal toxicity, were not available and could have been significantly impacted by the dose-escalation studies being performed during the study period at the 2 proton centers. 12,18 In contrast to the Medicare studies, the current study is based on prospectively collected, actual patient-reported clinical outcomes using the same QOL instrument and acquisition times between the PT and IMRT cohorts, and, as such, 1080 Cancer April 1, 2014
6 Outcomes After PT or IMRT/Hoppe et al should provide a more reliable comparison of functional outcomes. In this study, bowel summary scores were similar between the groups, correlating with the findings by Yu et al, 7 who reported on a more recent Medicare patient population that included patients who received treatment at different proton centers. The results also are similar to those recently reported by Gray et al, 19 who compared QOL outcomes of 95 men who received PT at Massachusetts General Hospital using the Talcott Prostate Symptom Index 20 with men who received IMRT from the PROSTQA database using the EPIC questionnaire; those authors reported that little difference was demonstrated in bowel problems >6 months after treatment. IMRT and PT both produce high radiation dose volumes that conform to the target; IMRT does so at the expense of exposing a larger volume of nontargeted tissue to low and moderate radiation doses. 21,22 Thus, toxicities and functional outcomes related to high radiation dose exposure, such as rectal bleeding, are expected to be similar between IMRT and PT if target doses and daily doses are similar. 22,23 Conversely, the rate of toxicities related to larger volumes of nontargeted tissue receiving low-dose and moderate-dose radiation exposure might be expected to be higher with IMRT than with PT. In the current study, the rate of rectal bleeding tended to being worse in the PT cohort, which may be explained by the higher prescription doses received in the PT cohort. Studies investigating rectal toxicities other than bleeding such as rectal syndrome (which includes rectal urgency), frequency, and incontinence have demonstrated correlations with the volumes of the rectum receiving both high and low to moderate doses. 18,24,25 Those studies focused on patients who received 3DCRT rather than IMRT, but the dose-volume relations serve to demonstrate the type of toxicity improvements that might be expected with reductions in the volume of rectum exposed to low to moderate radiation doses using PT compared with IMRT. Therefore, a potentially important finding of the current study is the analysis that identified significantly worse bowel urgency and bowel frequency in the IMRT group, a problem that affects QOL and can persist more than 10 years after radiation. 26 Nevertheless, alternate explanations, such as differing use of image-guided therapy, differing use of aspirin or other anticoagulants, target margins, interobserver variability, older age, or larger prostate volumes in the IMRT cohort, also could influence these results. 27 Recent research has investigated the impact of different rectal complications on global QOL after radiation therapy for prostate cancer. Krol et al 28 evaluated anorectal function in 85 men at least 1 year after conventionaldose prostate RT using the EPIC questionnaire, the Fecal Incontinence QOL scale, and anal manometry. Those authors observed that fecal incontinence and rectal urgency most greatly influenced overall QOL along with impaired anal resting pressure. It was also demonstrated that urgency of defecation has a more severe impact on patient-reported QOL than rectal bleeding, despite clinicians greater concern with rectal bleeding, which can be treated and resolved, compared with urgency, which can worsen over time and for which there is little treatment for its symptomology. 29 Therefore, these differences in discreet rectal symptoms between PT and IMRT treatments, as assessed from patient-reported outcomes, are intriguing and warrant further evaluation. The strengths of the current study are the prospective design for data collection, the use of patient-reported outcomes (PRO) from contemporary IMRT and PT series, the use of a common QOL instrument, and the collaborative effort between institutions that use IMRT and those that use PT. Although patients were not randomized to RT modalities, baseline information on clinical factors, QOL, and RT details permitted some adjustments for differences between the cohorts. Nevertheless, no level of statistical manipulation can account for how PT patients may have sought out (and traveled) to receive treatment in expectation of fewer side effects and better QOL. This exact criticism, however, can be made for the Medicare studies, which also were unable to statistically account for these differences. Another potential weakness is that the patients receiving PT were treated consistently at a single academic center, whereas the patients receiving IMRT were treated at 9 different academic centers; however, the same could be said for the Medicare studies, in which the vast majority of patients who were treated before 2008 would have been treated at 1 institution. 18 Additional weaknesses include that our comparative analysis plan was post hoc, although the QOL data were collected prospectively, and the difference in EPIC data collection between the cohorts with patients who received IMRT undergoing a telephone-assisted interview whereas those who received PT read and completed their questionnaires without assistance potentially could lead to bias in either direction. The findings from this study provide evidence of excellent and comparable QOL outcomes for patients with prostate cancer who receive either contemporary IMRT or PT. Although similar bowel, urinary, and sexual scores were observed with IMRT and PT, potential Cancer April 1,
7 differences in specific functional outcomes, such as bleeding, rectal urgency, and bowel frequency, also were observed and may reflect differences in radiation dose distributions between IMRT and PT, differences in patient characteristics, or both. Further investigation will be necessary to validate these findings and to identify the underlying mechanisms that account for them. FUNDING SUPPORT This work was supported by grants from the National Institute of Health (RO1 CA95662 and 1RC1CA14596) and the American College of Radiology-Radiation Therapy Oncology Group. CONFLICT OF INTEREST DISCLOSURES Dr. Hoppe reports receiving an honorarium from ProCure for lectures, and he serves on the board of the Proton Collaborative Group. Dr. Sandler is a board member of Eviti and he reports payment from Medivation, Millennium, Bayer Health, and Varian Health for consultant services. Dr. Sanda is a board member of Medicametrix, and he reports payment from Sanofi-Aventis for lectures. Dr. Hamstra reports payment from Myriad Health and Bayer Health for consultant services and payment from Varian Health for lectures. REFERENCES 1. Zelefsky MJ, Fuks Z, Hunt M, et al. High-dose intensity modulated radiation therapy for prostate cancer: early toxicity and biochemical outcome in 772 patients. Int J Radiat Oncol Biol Phys. 2002;53: Zietman AL, Bae K, Slater JD, et al. Randomized trial comparing conventional-dose with high-dose conformal radiation therapy in early stage adenocarcinoma of the prostate: long-term results from Proton Radiation Oncology Group=American College of Radiology J Clin Oncol. 2010;28: Nguyen PL, Gu X, Lipsitz SR, et al. Cost implications of the rapid adoption of newer technologies for treating prostate cancer. J Clin Oncol. 2011;29: Bekelman JE, Mitra N, Efstathiou J, et al. Outcomes after intensitymodulated versus conformal radiotherapy in older men with nonmetastatic prostate cancer [serial online]. Int J Radiat Oncol Biol Phys. 2011;81:e325-e Sheets NC, Goldin GH, Meyer AM, et al. Intensity-modulated radiation therapy, proton therapy, or conformal radiation therapy and morbidity and disease control in localized prostate cancer. JAMA. 2012;307: Kim S, Shen S, Moore DF, et al. Late gastrointestinal toxicities following radiation therapy for prostate cancer. Eur Urol. 2011;60: Yu JB, Soulos PR, Herrin J, et al. Proton versus intensity-modulated radiotherapy for prostate cancer: patterns of care and early toxicity. J Natl Cancer Inst. 2013;105: Deville C, Ben-Josef E, Vapiwala N. Radiation therapy modalities for prostate cancer [letter]. JAMA308:451, 2012; author reply Mendenhall NP, Schild S, Slater J. Radiation therapy modalities for prostate cancer [letter]. JAMA. 2012;308: ; author reply Szymanski KM, Wei JT, Dunn RL, et al. Development and validation of an abbreviated version of the Expanded Prostate Cancer Index Composite instrument for measuring health-related quality of life among prostate cancer survivors. Urology. 2010;76: Mendenhall NP, Li Z, Hoppe BS, et al. Early outcomes from 3 prospective trials of image-guided proton therapy for prostate cancer. Int J Radiat Oncol Biol Phys. 2012;82: Sandler HM, Liu PY, Dunn RL, et al. Reduction in patient-reported acute morbidity in prostate cancer patients treated with 81-Gy intensity-modulated radiotherapy using reduced planning target volume margins and electromagnetic tracking: assessing the impact of margin reduction study. Urology. 2010;75: Wei JT, Dunn RL, Litwin MS, et al. Development and validation of the Expanded Prostate Cancer Index Composite (EPIC) for comprehensive assessment of health-related quality of life in men with prostate cancer. Urology. 2000;56: Miller DC, Sanda MG, Dunn RL, et al. Long-term outcomes among localized prostate cancer survivors: health-related quality-oflife changes after radical prostatectomy, external radiation, and brachytherapy. J Clin Oncol. 2005;23: Norman GR, Sloan JA, Wyrwich KW. Interpretation of changes in health-related quality of life: the remarkable universality of half a standard deviation. Med Care. 2003;41: Sanda MG, Dunn RL, Michalski J, et al. Quality of life and satisfaction with outcome among prostate-cancer survivors. N Engl J Med. 2008;358: Hoppe BS, Nichols RC, Henderson RH, et al. Erectile function, incontinence, and other quality of life outcomes following proton therapy for prostate cancer in men 60 years old and younger. Cancer. 2012;118: Fiorino C, Fellin G, Rancati T, et al. Clinical and dosimetric predictors of late rectal syndrome after 3D-CRT for localized prostate cancer: preliminary results of a multicenter prospective study. Int J Radiat Oncol Biol Phys. 2008;70: Gray PJ, Paly JJ, Yeap BY, et al. Patient-reported outcomes after 3- dimensional conformal, intensity-modulated, or proton beam radiotherapy for localized prostate cancer. Cancer. 2013;119: Clark JA, Talcott JA. Symptom indexes to assess outcomes of treatment for early prostate cancer. Med Care. 2001;39: Vargas C, Fryer A, Mahajan C, et al. Dose-volume comparison of proton therapy and intensity-modulated radiotherapy for prostate cancer. Int J Radiat Oncol Biol Phys. 2008;70: Trofimov A, Nguyen PL, Coen JJ, et al. Radiotherapy treatment of early stage prostate cancer with IMRT and protons: a treatment planning comparison. Int J Radiat Oncol Biol Phys. 2007;69: Tucker SL, Dong L, Michalski JM, et al. Do intermediate radiation doses contribute to late rectal toxicity? An analysis of data from radiation therapy oncology group protocol Int J Radiat Oncol Biol Phys. 2012;84: Peeters ST, Lebesque JV, Heemsbergen WD, et al. Localized volume effects for late rectal and anal toxicity after radiotherapy for prostate cancer. Int J Radiat Oncol Biol Phys. 2006;64: al-abany M, Helgason AR, Cronqvist AK, et al. Toward a definition of a threshold for harmless doses to the anal-sphincter region and the rectum. Int J Radiat Oncol Biol Phys. 2005;61: Resnick MJ, Koyama T, Fan KH, et al. Long-term functional outcomes after treatment for localized prostate cancer. N Engl J Med. 2013;368: Hamstra DA, Stenmark MJ, Ritter T, et al. Age and comorbid illness are associated with late rectal toxicity following dose-escalated radiation therapy for prostate cancer. Int J Radiat Oncol Biol Phys. 2013;85: Krol R, Smeenk RJ, van Lin EN, et al. Impact of late anorectal dysfunction on quality of life after pelvic radiotherapy. Int J Colorectal Dis. 2013;28: Yeoh EK, Holloway RH, Fraser RJ, et al. Pathophysiology and natural history of anorectal sequelae following radiation therapy for carcinoma of the prostate [serial online]. Int J Radiat Oncol Biol Phys. 2012;84:e593-e Cancer April 1, 2014
Erectile Function, Incontinence, and Other Quality of Life Outcomes Following Proton Therapy for Prostate Cancer in Men 60 Years Old and Younger
 Erectile Function, Incontinence, and Other Quality of Life Outcomes Following Proton Therapy for Prostate Cancer in Men 60 Years Old and Younger Bradford S. Hoppe, MD, MPH 1 ; Romaine C. Nichols, MD 1
Erectile Function, Incontinence, and Other Quality of Life Outcomes Following Proton Therapy for Prostate Cancer in Men 60 Years Old and Younger Bradford S. Hoppe, MD, MPH 1 ; Romaine C. Nichols, MD 1
PROTON THERAPY FOR PROSTATE CANCER: THE INITIAL LOMA LINDA UNIVERSITY EXPERIENCE
 doi:10.1016/j.ijrobp.2003.10.011 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 2, pp. 348 352, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
doi:10.1016/j.ijrobp.2003.10.011 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 2, pp. 348 352, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
LATE MORBIDITY PROFILES IN PROSTATE CANCER PATIENTS TREATED TO 79 84 GY BY A SIMPLE FOUR-FIELD COPLANAR BEAM ARRANGEMENT
 PII S0360-3016(02)03822-1 Int. J. Radiation Oncology Biol. Phys., Vol. 55, No. 1, pp. 71 77, 2003 Copyright 2003 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/03/$ see front matter
PII S0360-3016(02)03822-1 Int. J. Radiation Oncology Biol. Phys., Vol. 55, No. 1, pp. 71 77, 2003 Copyright 2003 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/03/$ see front matter
Implementation Date: April 2015 Clinical Operations
 National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
Subject: Proton Beam Therapy for Prostate Cancer
 Subject: Proton Beam Therapy for Prostate Cancer Guidance Number: MCG-153 Revision Date(s): Original Effective Date: 10/30/13 Medical Coverage Guidance Approval Date: 10/30/13 PREFACE This Medical Guidance
Subject: Proton Beam Therapy for Prostate Cancer Guidance Number: MCG-153 Revision Date(s): Original Effective Date: 10/30/13 Medical Coverage Guidance Approval Date: 10/30/13 PREFACE This Medical Guidance
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引
 馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
The Science behind Proton Beam Therapy
 The Science behind Proton Beam Therapy Anthony Zietman MD Shipley Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School Principles underlying Radiotherapy Radiation related
The Science behind Proton Beam Therapy Anthony Zietman MD Shipley Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School Principles underlying Radiotherapy Radiation related
Cyberknife Information Guide. Prostate Cancer Treatment
 Cyberknife Information Guide Prostate Cancer Treatment CYBERKNIFE INFORMATION GUIDE PROSTATE CANCER TREATMENT As a patient recently diagnosed with localized prostate cancer, it is important that you familiarize
Cyberknife Information Guide Prostate Cancer Treatment CYBERKNIFE INFORMATION GUIDE PROSTATE CANCER TREATMENT As a patient recently diagnosed with localized prostate cancer, it is important that you familiarize
Proton Therapy for Prostate Cancer
 BRADFORD HOPPE, MD, MPH 1 RANDAL HENDERSON, MD, MBA 1 WILLIAM M. MENDENHALL, MD 1 ROMAINE C. NICHOLS, MD 1 ZUOFENG LI, PhD 1 NANCY P. MENDENHALL, MD 1 Proton Therapy for Prostate Cancer Abstract: Proton
BRADFORD HOPPE, MD, MPH 1 RANDAL HENDERSON, MD, MBA 1 WILLIAM M. MENDENHALL, MD 1 ROMAINE C. NICHOLS, MD 1 ZUOFENG LI, PhD 1 NANCY P. MENDENHALL, MD 1 Proton Therapy for Prostate Cancer Abstract: Proton
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
1 of 6 6/13/11 12:40 PM
 ONCOLOGY. Vol. 25 No. 7 REVIEW ARTICLE Proton Therapy for Prostate Cancer By Bradford Hoppe, MD, MPH 1, Randal Henderson, MD, MBA 1, William M. Mendenhall, MD 1, Romaine C. Nichols, MD 1, Zuofeng Li, PhD
ONCOLOGY. Vol. 25 No. 7 REVIEW ARTICLE Proton Therapy for Prostate Cancer By Bradford Hoppe, MD, MPH 1, Randal Henderson, MD, MBA 1, William M. Mendenhall, MD 1, Romaine C. Nichols, MD 1, Zuofeng Li, PhD
Michael J. Zelefsky,*, Heather Chan, Margie Hunt, Yoshiya Yamada, Alison M. Shippy and Howard Amols
 Long-Term Outcome of High Dose Intensity Modulated Radiation Therapy for Patients With Clinically Localized Prostate Cancer Michael J. Zelefsky,*, Heather Chan, Margie Hunt, Yoshiya Yamada, Alison M. Shippy
Long-Term Outcome of High Dose Intensity Modulated Radiation Therapy for Patients With Clinically Localized Prostate Cancer Michael J. Zelefsky,*, Heather Chan, Margie Hunt, Yoshiya Yamada, Alison M. Shippy
Proton Beam Therapy. Methods Literature for this article was obtained using the Touro College Online library, in particular PubMed.
 Is Proton Beam Therapy more Effective than Intensity- Modulated Radiotherapy in Prostate Cancer Treatment? Daniel Zelefsky Daniel will graduate in June 2015 with an Honors Biology B.S. degree. Abstract
Is Proton Beam Therapy more Effective than Intensity- Modulated Radiotherapy in Prostate Cancer Treatment? Daniel Zelefsky Daniel will graduate in June 2015 with an Honors Biology B.S. degree. Abstract
Prostate Cancer Treatment: What s Best for You?
 Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Radiation Therapy for Prostate Cancer: Treatment options and future directions
 Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
4/8/13. Pre-test Audience Response. Prostate Cancer 2012. Screening and Treatment of Prostate Cancer: The 2013 Perspective
 Pre-test Audience Response Screening and Treatment of Prostate Cancer: The 2013 Perspective 1. I do not offer routine PSA screening, and the USPSTF D recommendation will not change my practice. 2. In light
Pre-test Audience Response Screening and Treatment of Prostate Cancer: The 2013 Perspective 1. I do not offer routine PSA screening, and the USPSTF D recommendation will not change my practice. 2. In light
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate
 Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Prostate cancer is the most common cause of death from cancer in men over age 75. Prostate cancer is rarely found in men younger than 40.
 A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
PROTON BEAM THERAPY FOR PROSTATE CANCER. A Technology Assessment
 PROTON BEAM THERAPY FOR PROSTATE CANCER A Technology Assessment INTRODUCTION The California Technology Assessment Forum is requested to review the scientific evidence for the use of proton therapy for
PROTON BEAM THERAPY FOR PROSTATE CANCER A Technology Assessment INTRODUCTION The California Technology Assessment Forum is requested to review the scientific evidence for the use of proton therapy for
Patient-reported Hip Symptoms following Treatment with Proton Therapy for Prostate Cancer
 Patient-reported Hip Symptoms following Treatment with Proton Therapy for Prostate Cancer Whoon J. Kil, MD 1 ; Nancy P. Mendenhall, MD 1 ; Christopher G. Morris, MS 1 ;R. Charles Nichols, MD 1 ; Randal
Patient-reported Hip Symptoms following Treatment with Proton Therapy for Prostate Cancer Whoon J. Kil, MD 1 ; Nancy P. Mendenhall, MD 1 ; Christopher G. Morris, MS 1 ;R. Charles Nichols, MD 1 ; Randal
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results. Alan Katz MD JD Flushing, NY USA
 CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results Alan Katz MD JD Flushing, NY USA Prostate Ablative Therapy Over the last 10 years our therapy has improved bned rates for LDR/HDR
CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results Alan Katz MD JD Flushing, NY USA Prostate Ablative Therapy Over the last 10 years our therapy has improved bned rates for LDR/HDR
Prostate Cancer Patients Report on Benefits of Proton Therapy
 Prostate Cancer Patients Report on Benefits of Proton Therapy Dobson DaVanzo & Associates, LLC Vienna, VA 703.260.1760 www.dobsondavanzo.com Prostate Cancer Patients Report on Benefits of Proton Therapy
Prostate Cancer Patients Report on Benefits of Proton Therapy Dobson DaVanzo & Associates, LLC Vienna, VA 703.260.1760 www.dobsondavanzo.com Prostate Cancer Patients Report on Benefits of Proton Therapy
Proton Therapy for Prostate Cancer
 Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director, Proton Therapy Center Associate Professor Department of Radiation Oncology M.D. Anderson Cancer Center Randomized studies showing benefit
Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director, Proton Therapy Center Associate Professor Department of Radiation Oncology M.D. Anderson Cancer Center Randomized studies showing benefit
Intensity-Modulated Radiation Therapy Leads to Survival Benefit Only in Patients with High-Risk Prostate Cancer: a Population-Based Study
 Annals of Oncology Advance Access published February 22, 2014 1 Intensity-Modulated Radiation Therapy Leads to Survival Benefit Only in Patients with High-Risk Prostate Cancer: a Population-Based Study
Annals of Oncology Advance Access published February 22, 2014 1 Intensity-Modulated Radiation Therapy Leads to Survival Benefit Only in Patients with High-Risk Prostate Cancer: a Population-Based Study
ONLINE CONTINUING EDUCATION ACTIVITY
 ONLINE CONTINUING EDUCATION ACTIVITY Take free quizzes online at acsjournals.com/ce ARTICLE TITLE: Progress and Controversies: Radiation Therapy for Prostate Cancer CONTINUING MEDICAL EDUCATION ACCREDITATION
ONLINE CONTINUING EDUCATION ACTIVITY Take free quizzes online at acsjournals.com/ce ARTICLE TITLE: Progress and Controversies: Radiation Therapy for Prostate Cancer CONTINUING MEDICAL EDUCATION ACCREDITATION
Ryan C. Hedgepeth,* Jessica Labo, LingLing Zhang and David P. Wood, Jr.
 Expanded Prostate Cancer Index Composite Versus Incontinence Symptom Index and Sexual Health Inventory for Men to Measure Functional Outcomes After Prostatectomy Ryan C. Hedgepeth,* Jessica Labo, LingLing
Expanded Prostate Cancer Index Composite Versus Incontinence Symptom Index and Sexual Health Inventory for Men to Measure Functional Outcomes After Prostatectomy Ryan C. Hedgepeth,* Jessica Labo, LingLing
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
Does my patient need more therapy after prostate cancer surgery?
 Does my patient need more therapy after prostate cancer surgery? Contact the GenomeDx Patient Care Team at: 1.888.792.1601 (toll-free) or e-mail: client.service@genomedx.com Prostate Cancer Classifier
Does my patient need more therapy after prostate cancer surgery? Contact the GenomeDx Patient Care Team at: 1.888.792.1601 (toll-free) or e-mail: client.service@genomedx.com Prostate Cancer Classifier
Proton Therapy for Prostate Cancer: Your Questions, Our Answers.
 Proton Therapy for Prostate Cancer: Your Questions, Our Answers. When you re looking for the right treatment for your prostate cancer, nothing s more important than accurate information. Read on, and learn
Proton Therapy for Prostate Cancer: Your Questions, Our Answers. When you re looking for the right treatment for your prostate cancer, nothing s more important than accurate information. Read on, and learn
Issues Concerning Development of Products for Treatment of Non-Metastatic Castration- Resistant Prostate Cancer (NM-CRPC)
 Issues Concerning Development of Products for Treatment of Non-Metastatic Castration- Resistant Prostate Cancer (NM-CRPC) FDA Presentation ODAC Meeting September 14, 2011 1 Review Team Paul G. Kluetz,
Issues Concerning Development of Products for Treatment of Non-Metastatic Castration- Resistant Prostate Cancer (NM-CRPC) FDA Presentation ODAC Meeting September 14, 2011 1 Review Team Paul G. Kluetz,
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
Prostatectomy, pelvic lymphadenect. Med age 63 years Mean followup 53 months No other cancer related therapy before recurrence. Negative.
 Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer
 Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer Adam R. Kuykendal, MD; Laura H. Hendrix, MS; Ramzi G. Salloum, PhD; Paul A. Godley, MD, PhD; Ronald C. Chen, MD, MPH No conflicts
Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer Adam R. Kuykendal, MD; Laura H. Hendrix, MS; Ramzi G. Salloum, PhD; Paul A. Godley, MD, PhD; Ronald C. Chen, MD, MPH No conflicts
Optimizing Adoption of Advanced Technology to Achieve High Value Cancer Care: The Case of Proton Therapy ECRI NCI Conference November 17, 2015
 Optimizing Adoption of Advanced Technology to Achieve High Value Cancer Care: The Case of Proton Therapy ECRI NCI Conference November 17, 2015 Justin E. Bekelman, MD Associate Professor, Radiation Oncology
Optimizing Adoption of Advanced Technology to Achieve High Value Cancer Care: The Case of Proton Therapy ECRI NCI Conference November 17, 2015 Justin E. Bekelman, MD Associate Professor, Radiation Oncology
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
Prostate Cancer Treatment Comparison
 Prostate Cancer Treatment Comparison Treatment Comparative Data Outcome Comparison: Surgery vs. Radiotherapy Outcome Radical Prostatectomy* Radiation** Survival duration compared to conservative disease
Prostate Cancer Treatment Comparison Treatment Comparative Data Outcome Comparison: Surgery vs. Radiotherapy Outcome Radical Prostatectomy* Radiation** Survival duration compared to conservative disease
Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021
 Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021 Introduction Prostate is one of the treatment sites that is well suited for IMRT. For
Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021 Introduction Prostate is one of the treatment sites that is well suited for IMRT. For
Role of Radiation after Radical Prostatectomy Review of Literature
 Vol. 9, No: 1 Jan - Jun 2013. Page 1-44 Role of Radiation after Radical Prostatectomy Review of Literature S.K. Raghunath, N. Srivatsa Abstract Biochemical relapse after radical prostatectomy occurs in
Vol. 9, No: 1 Jan - Jun 2013. Page 1-44 Role of Radiation after Radical Prostatectomy Review of Literature S.K. Raghunath, N. Srivatsa Abstract Biochemical relapse after radical prostatectomy occurs in
Neoadjuvant hormonal therapy in prostate cancer impact of PSA level before radiotherapy
 JBUON 2013; 18(4): 949-953 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Neoadjuvant hormonal therapy in prostate cancer impact of PSA level
JBUON 2013; 18(4): 949-953 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Neoadjuvant hormonal therapy in prostate cancer impact of PSA level
American College of Radiology ACR Appropriateness Criteria DEFINITIVE EXTERNAL-BEAM IRRADIATION IN STAGE T1 AND T2 PROSTATE CANCER
 American College of Radiology ACR Appropriateness Criteria Date of origin: 1996 Last review date: 2013 DEFINITIVE EXTERNAL-BEAM IRRADIATION IN STAGE T1 AND T2 PROSTATE CANCER Expert Panel on Radiation
American College of Radiology ACR Appropriateness Criteria Date of origin: 1996 Last review date: 2013 DEFINITIVE EXTERNAL-BEAM IRRADIATION IN STAGE T1 AND T2 PROSTATE CANCER Expert Panel on Radiation
Defining Sexual Outcomes after Treatment for Localized Prostate Carcinoma
 1773 Defining Sexual Outcomes after Treatment for Localized Prostate Carcinoma Leslie R. Schover, Ph.D. 1 Rachel T. Fouladi, Ph.D. 1 Carla L. Warneke, M.S. 1 Leah Neese, M.A. 1 Eric A. Klein, M.D. 2 Craig
1773 Defining Sexual Outcomes after Treatment for Localized Prostate Carcinoma Leslie R. Schover, Ph.D. 1 Rachel T. Fouladi, Ph.D. 1 Carla L. Warneke, M.S. 1 Leah Neese, M.A. 1 Eric A. Klein, M.D. 2 Craig
Historical Basis for Concern
 Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
PRIOR AUTHORIZATION Prior authorization is recommended and obtained via the online tool for participating providers.
 Medical Coverage Policy Intensity-Modulated Radiotherapy of the Prostate EFFECTIVE DATE: 02 15 2016 POLICY LAST UPDATED: 03 23 2016 OVERVIEW Radiotherapy (RT) is an integral component in the treatment
Medical Coverage Policy Intensity-Modulated Radiotherapy of the Prostate EFFECTIVE DATE: 02 15 2016 POLICY LAST UPDATED: 03 23 2016 OVERVIEW Radiotherapy (RT) is an integral component in the treatment
The Business of Prostate Cancer Care: A Clinician-Researcher s Perspective
 The Business of Prostate Cancer Care: A Clinician-Researcher s Perspective David F. Penson, MD, MPH Departments of Urology and Preventive Medicine Keck School of Medicine University of Southern California
The Business of Prostate Cancer Care: A Clinician-Researcher s Perspective David F. Penson, MD, MPH Departments of Urology and Preventive Medicine Keck School of Medicine University of Southern California
Protons vs. CyberKnife. Protons vs. CyberKnife. Page 1 UC SF. What are. Alexander R. Gottschalk, M.D., Ph.D.
 Protons vs. CyberKnife UC SF Protons vs. CyberKnife UC SF Alexander R. Gottschalk, M.D., Ph.D. Associate Professor and Director of the CyberKnife Radiosurgery Program Department of Radiation Oncology University
Protons vs. CyberKnife UC SF Protons vs. CyberKnife UC SF Alexander R. Gottschalk, M.D., Ph.D. Associate Professor and Director of the CyberKnife Radiosurgery Program Department of Radiation Oncology University
Oncology Annual Report: Prostate Cancer 2005 Update By: John Konefal, MD, Radiation Oncology
 Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Prostate Cancer Screening: Are We There Yet? March 2010 Andrew M.D. Wolf, MD University of Virginia School of Medicine
 Prostate Cancer Screening: Are We There Yet? March 2010 Andrew M.D. Wolf, MD University of Virginia School of Medicine Case #1 A 55 yo white man with well-controlled hypertension presents for his annual
Prostate Cancer Screening: Are We There Yet? March 2010 Andrew M.D. Wolf, MD University of Virginia School of Medicine Case #1 A 55 yo white man with well-controlled hypertension presents for his annual
Key Staff Members EXECUTIVE TEAM Nancy Price Mendenhall, MD Medical Director Stuart Klein, MHA Executive Director Zuofeng Li, DSc Physics Director
 Key Staff Members EXECUTIVE TEAM Nancy Price Mendenhall, MD Medical Director A University of Florida College of Medicine faculty member since 1985, Dr. Mendenhall served as the chair of the Department
Key Staff Members EXECUTIVE TEAM Nancy Price Mendenhall, MD Medical Director A University of Florida College of Medicine faculty member since 1985, Dr. Mendenhall served as the chair of the Department
Focal therapy for prostate cancer: seriously or seriously? Disclosures
 Focal therapy for prostate cancer: seriously or seriously? Mitchell Kamrava, MD Assistant Clinical Professor Department of Radiation Oncology University of California Los Angeles Disclosures Speaking honorarium
Focal therapy for prostate cancer: seriously or seriously? Mitchell Kamrava, MD Assistant Clinical Professor Department of Radiation Oncology University of California Los Angeles Disclosures Speaking honorarium
Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15.
 Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15. CLINICAL CASE The Debate Over Prostate Cancer Screening Guidelines Commentary by Karen E. Hoffman,
Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15. CLINICAL CASE The Debate Over Prostate Cancer Screening Guidelines Commentary by Karen E. Hoffman,
A new score predicting the survival of patients with spinal cord compression from myeloma
 A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
TITLE: The Impact Of Prostate Cancer Treatment-Related Symptoms On Low-Income Latino Couples
 AD Award Number: W81WH-07-1-0069 TITLE: The Impact Of Prostate Cancer Treatment-Related Symptoms On Low-Income Latino Couples PRINCIPAL INVESTIGATOR: Sally L. Maliski, Ph.D., R.N. CONTRACTING ORGANIZATION:
AD Award Number: W81WH-07-1-0069 TITLE: The Impact Of Prostate Cancer Treatment-Related Symptoms On Low-Income Latino Couples PRINCIPAL INVESTIGATOR: Sally L. Maliski, Ph.D., R.N. CONTRACTING ORGANIZATION:
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
BRACHYTHERAPY OR CONFORMAL EXTERNAL RADIOTHERAPY FOR PROSTATE CANCER: A SINGLE-INSTITUTION MATCHED-PAIR ANALYSIS
 doi:10.1016/j.ijrobp.2009.01.081 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No. 1, pp. 43 49, 2010 Copyright Ó 2010 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/10/$ see front
doi:10.1016/j.ijrobp.2009.01.081 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No. 1, pp. 43 49, 2010 Copyright Ó 2010 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/10/$ see front
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
IEHP UM Subcommittee Approved Authorization Guidelines Proton Beam Radiation therapy for Prostate Cancer
 Proton Beam Radiation therapy for Prostate Cancer Policy: The use of Proton Beam Therapy (PBT) in Prostate cancer has not been established as more effective than other forms of External Beam Radiation
Proton Beam Radiation therapy for Prostate Cancer Policy: The use of Proton Beam Therapy (PBT) in Prostate cancer has not been established as more effective than other forms of External Beam Radiation
LONG-TERM URINARY TOXICITY AFTER 3-DIMENSIONAL CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER IN PATIENTS WITH PRIOR HISTORY OF TRANSURETHRAL RESECTION
 PII S0360-3016(00)00714-8 Int. J. Radiation Oncology Biol. Phys., Vol. 48, No. 3, pp. 643 647, 2000 Copyright 2000 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/00/$ see front
PII S0360-3016(00)00714-8 Int. J. Radiation Oncology Biol. Phys., Vol. 48, No. 3, pp. 643 647, 2000 Copyright 2000 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/00/$ see front
DOCTOr. Doctor to HIGHLIGHTS. issue NO. 3 VOLuMe NO. 1
 Doctor to DOCTOr issue NO. 3 VOLuMe NO. 1 PROSTATE CANCER is the most common cancer in men, with 233,000 new cases diagnosed per year. Although prostate cancer remains the second leading cause of cancer
Doctor to DOCTOr issue NO. 3 VOLuMe NO. 1 PROSTATE CANCER is the most common cancer in men, with 233,000 new cases diagnosed per year. Although prostate cancer remains the second leading cause of cancer
Therapies for Prostate Cancer and Treatment Selection
 Prostatic Diseases Therapies for Prostate Cancer and Treatment Selection JMAJ 47(12): 555 560, 2004 Yoichi ARAI Professor and Chairman, Department of Urology, Tohoku University Graduate School of Medicine
Prostatic Diseases Therapies for Prostate Cancer and Treatment Selection JMAJ 47(12): 555 560, 2004 Yoichi ARAI Professor and Chairman, Department of Urology, Tohoku University Graduate School of Medicine
American Urological Association (AUA) Guideline
 1 (AUA) Guideline Approved by the AUA Board of Directors April 2013 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article. 2013 by the American
1 (AUA) Guideline Approved by the AUA Board of Directors April 2013 Authors disclosure of potential conflicts of interest and author/staff contributions appear at the end of the article. 2013 by the American
Prognostic Factors for Late Urinary Toxicity Grade 2-3 after Conformal Radiation Therapy on Patients with Prostate Cancer
 Clinical Urology Toxicity Grade - after Radiation for Prostate Cancer International Braz J Urol Vol. (5): 65-661, September - October, 007 Prognostic Factors for Late Urinary Toxicity Grade - after Conformal
Clinical Urology Toxicity Grade - after Radiation for Prostate Cancer International Braz J Urol Vol. (5): 65-661, September - October, 007 Prognostic Factors for Late Urinary Toxicity Grade - after Conformal
Cancer research in the Midland Region the prostate and bowel cancer projects
 Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
ACCEPTED MANUSCRIPT. Understanding the performance of active surveillance selection criteria in diverse urology practices
 Understanding the performance of active surveillance selection criteria in diverse urology practices Scott R. Hawken BS*,1, Paul R. Womble MD*,1, Lindsey A. Herrel MD 1, Zaojun Ye MS 1, Susan M. Linsell
Understanding the performance of active surveillance selection criteria in diverse urology practices Scott R. Hawken BS*,1, Paul R. Womble MD*,1, Lindsey A. Herrel MD 1, Zaojun Ye MS 1, Susan M. Linsell
1. What is the prostate-specific antigen (PSA) test?
 1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
Prostate Cancer. Treatments as unique as you are
 Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Salvage Conformal Radiotherapy for Biochemical Recurrent Prostate Cancer after Radical Prostatectomy
 Clinical Urology Salvage Conformal Radiotherapy for Prostate Cancer International Braz J Urol Vol. 32 (4): 46-427, July - August, 2006 Salvage Conformal Radiotherapy for Biochemical Recurrent Prostate
Clinical Urology Salvage Conformal Radiotherapy for Prostate Cancer International Braz J Urol Vol. 32 (4): 46-427, July - August, 2006 Salvage Conformal Radiotherapy for Biochemical Recurrent Prostate
Clinical Education A comprehensive and specific training program. carry out effective treatments from day one
 Proton Therapy Clinical Education A comprehensive and specific training program carry out effective treatments from day one Forewarned is forearmed Although over 100,000 patients have been treated in proton
Proton Therapy Clinical Education A comprehensive and specific training program carry out effective treatments from day one Forewarned is forearmed Although over 100,000 patients have been treated in proton
Prostate Cancer Results Study Group 2014 Results Comparing Treatment of. About This Review Study
 Prostate Cancer Results Study Group Results Comparing Treatment of Prostate Cancer Peter Grimm, DO Seattle, WA About This Review Study,000+ prostate studies were published between 00 and June 3, of those
Prostate Cancer Results Study Group Results Comparing Treatment of Prostate Cancer Peter Grimm, DO Seattle, WA About This Review Study,000+ prostate studies were published between 00 and June 3, of those
Prostate Cancer Treatment
 Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD
 MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD Division of Urology, MCP Hahnemann University, Philadelphia, PA
MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD Division of Urology, MCP Hahnemann University, Philadelphia, PA
TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software.
 SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER
 2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER Humboldt County is located on the Redwood Coast of Northern California. U.S census data for 2010 reports county population at 134,623, an increase of
2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER Humboldt County is located on the Redwood Coast of Northern California. U.S census data for 2010 reports county population at 134,623, an increase of
Beyond the PSA: Genomic Testing in Localized Prostate Cancer
 Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Understanding the. Controversies of. testosterone replacement. therapy in hypogonadal men with prostate cancer. controversies surrounding
 Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
MEDICARE. Higher Use of Costly Prostate Cancer Treatment by Providers Who Self- Refer Warrants Scrutiny. Report to Congressional Requesters
 United States Government Accountability Office Report to Congressional Requesters July 2013 MEDICARE Higher Use of Costly Prostate Cancer Treatment by Providers Who Self- Refer Warrants Scrutiny GAO-13-525
United States Government Accountability Office Report to Congressional Requesters July 2013 MEDICARE Higher Use of Costly Prostate Cancer Treatment by Providers Who Self- Refer Warrants Scrutiny GAO-13-525
PSA After Radiation for Prostate Cancer
 Review Article [1] May 01, 2004 By Deborah A. Kuban, MD [2], Howard D. Thames, PhD [3], and Larry B. Levy, MS [4] The introduction of prostate-specific antigen (PSA) as a reliable tumor marker for prostate
Review Article [1] May 01, 2004 By Deborah A. Kuban, MD [2], Howard D. Thames, PhD [3], and Larry B. Levy, MS [4] The introduction of prostate-specific antigen (PSA) as a reliable tumor marker for prostate
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
Particle Therapy for Lung Cancer. Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org
 Particle Therapy for Lung Cancer Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org Content Rationale for Particle Therapy in Lung Cancer Proof of Principle Treatment
Particle Therapy for Lung Cancer Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org Content Rationale for Particle Therapy in Lung Cancer Proof of Principle Treatment
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
Nine Decisions Before Electing RADIATION THERAPY After Radical Prostatectomy
 Nine Decisions Before Electing RADIATION THERAPY After Radical Prostatectomy Who might it help? When should it be done? Understand the risks of side-effects By Nathan Roundy The words the surgeon may not
Nine Decisions Before Electing RADIATION THERAPY After Radical Prostatectomy Who might it help? When should it be done? Understand the risks of side-effects By Nathan Roundy The words the surgeon may not
Early stage prostate cancer: biochemical recurrence after treatment
 REVIEW ARTICLE Vol. 40 (2): 137-145, March - April, 2014 doi: 10.1590/S1677-5538.IBJU.2014.02.02 Early stage prostate cancer: biochemical recurrence after treatment Danielle A. Zanatta, Reginaldo J. Andrade,
REVIEW ARTICLE Vol. 40 (2): 137-145, March - April, 2014 doi: 10.1590/S1677-5538.IBJU.2014.02.02 Early stage prostate cancer: biochemical recurrence after treatment Danielle A. Zanatta, Reginaldo J. Andrade,
Current and Future Trends in Proton Treatment of Prostate Cancer
 Current and Future Trends in Proton Treatment of Prostate Cancer Reinhard W. Schulte Assistant Professor Department of Radiation Medicine Loma Linda University Medical Center Loma Linda, CA, USA Outline
Current and Future Trends in Proton Treatment of Prostate Cancer Reinhard W. Schulte Assistant Professor Department of Radiation Medicine Loma Linda University Medical Center Loma Linda, CA, USA Outline
NATURAL HISTORY OF CLINICALLY STAGED LOW- AND INTERMEDIATE-RISK PROSTATE CANCER TREATED WITH MONOTHERAPEUTIC PERMANENT INTERSTITIAL BRACHYTHERAPY
 doi:1.116/j.ijrobp.9..1 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No., pp. 349 354, 1 Copyright Ó 1 Elsevier Inc. Printed in the USA. All rights reserved 36-316/1/$ see front matter CLINICAL INVESTIGATION
doi:1.116/j.ijrobp.9..1 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No., pp. 349 354, 1 Copyright Ó 1 Elsevier Inc. Printed in the USA. All rights reserved 36-316/1/$ see front matter CLINICAL INVESTIGATION
Proton Therapy: Cutting Edge Treatment for Cancerous Tumors. By: Cherilyn G. Murer, JD, CRA
 Proton Therapy: Cutting Edge Treatment for Cancerous Tumors By: Cherilyn G. Murer, JD, CRA Introduction Put simply, proton therapy is a new cutting edge cancer treatment that promises better outcomes for
Proton Therapy: Cutting Edge Treatment for Cancerous Tumors By: Cherilyn G. Murer, JD, CRA Introduction Put simply, proton therapy is a new cutting edge cancer treatment that promises better outcomes for
Clinical Trials and Radiation Treatment. Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto
 Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Should we use Docetaxel in hormone- naïve prostate cancer? Karim Fizazi, MD, PhD Institut Gustave Roussy Villejuif, France
 Should we use Docetaxel in hormone- naïve prostate cancer? Karim Fizazi, MD, PhD Institut Gustave Roussy Villejuif, France Disclosure Participation to advisory boards/honorarium from: Amgen, Astellas,
Should we use Docetaxel in hormone- naïve prostate cancer? Karim Fizazi, MD, PhD Institut Gustave Roussy Villejuif, France Disclosure Participation to advisory boards/honorarium from: Amgen, Astellas,
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Prostate Cancer. What is prostate cancer?
 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Does Radiation Treatment of Prostate Cancer Increase Risk for Rectal Cancer? The Perfect Storm
 NAACCR Conference, Austin, TX June 13, 2013 In Collaboration with: Does Radiation Treatment of Prostate Cancer Increase Risk for Rectal Cancer? The Perfect Storm John W. Morgan, DrPH, CPH, Brice Jabo,
NAACCR Conference, Austin, TX June 13, 2013 In Collaboration with: Does Radiation Treatment of Prostate Cancer Increase Risk for Rectal Cancer? The Perfect Storm John W. Morgan, DrPH, CPH, Brice Jabo,
Precise, Minimally Invasive Prostate Cancer Removal
 Precise, Minimally Invasive Prostate Cancer Removal Learn why da Vinci Surgery may be your best treatment option 1 Beyond Minimally Invasive For Prostate Cancer 1 Facing Prostate Cancer Prostate cancer
Precise, Minimally Invasive Prostate Cancer Removal Learn why da Vinci Surgery may be your best treatment option 1 Beyond Minimally Invasive For Prostate Cancer 1 Facing Prostate Cancer Prostate cancer
National And Institutional Outcomes In Prostate Cancer Radiotherapy
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2011 National And Institutional Outcomes In Prostate Cancer
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2011 National And Institutional Outcomes In Prostate Cancer
Cancer in Primary Care: Prostate Cancer Screening. How and How often? Should we and in which patients?
 Cancer in Primary Care: Prostate Cancer Screening How and How often? Should we and in which patients? PLCO trial (Prostate, Lung, Colorectal and Ovarian) Results In the screening group, rates of compliance
Cancer in Primary Care: Prostate Cancer Screening How and How often? Should we and in which patients? PLCO trial (Prostate, Lung, Colorectal and Ovarian) Results In the screening group, rates of compliance
Official reprint from UpToDate www.uptodate.com 2013 UpToDate
 Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment. Always seek
Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment. Always seek
Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy
 Brachytherapy - (2012) - Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy Carlos Vargas 1, *, Douglas Swartz 2, Apoorva Vashi 2, Mark Blasser
Brachytherapy - (2012) - Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy Carlos Vargas 1, *, Douglas Swartz 2, Apoorva Vashi 2, Mark Blasser
Prostate Cancer Screening in Taiwan: a must
 Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
