TREATMENTS FOR MODERATE OR SEVERE PSORIASIS
|
|
|
- Cecil French
- 8 years ago
- Views:
Transcription
1 TREATMENTS FOR MODERATE OR SEVERE PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with creams and ointments, which are applied to the skin. These are discussed in a separate leaflet ( Topical treatments for psoriasis ). Sometimes other forms of treatment are needed and this leaflet has been written to help you to understand more about them. It tells you what they are, how they are used, and where you can find out more about them. What types of treatment are available? They include: 1. Phototherapy. Ultraviolet light can be used in several different ways to treat psoriasis. 2. Treatments with a variety of tablets. The idea of a tablet to treat psoriasis is attractive, but most of the tablets used have potentially severe side effects. Most are likely to be started by a dermatologist, and some can be prescribed only from a hospital. o They require regular clinical and blood test checks. o Most have the potential to interfere with other medicines, and so you should always let your doctor know if other medicines are changed whilst you are taking tablets for psoriasis. o Female patients should not become pregnant while on any of the tablets used to treat psoriasis; in addition, it is important that male patients taking some of these tablets should not father a child. These pregnancy issues may apply for some time after stopping the tablets. Treatments with tablets tend to be used: o When psoriasis has failed to respond to topical treatments, or comes back quickly after clearing with them. o If the psoriasis is severe. o If its pattern is an awkward one for treatment with creams and ointments.
2 Which of these treatments is most suitable for my psoriasis? The various treatments with light and tablets are discussed individually below, and would also be discussed with you in detail by your dermatologist if you were to start on them. All are effective, but the choice will vary from patient to patient for reasons that are outlined below. All of them carry some potential risks, so they are not used for psoriasis that can sensibly by kept under control with simpler measures. Most patients will need to use some topical therapies as well. Phototherapy What types of phototherapy are available? Two types are used, known as UVB and PUVA. UV stands for ultraviolet - UVA and UVB are different parts of normal sunlight. With both of these treatments it is important that you let the staff know about any tablets that you are taking, as some can make the skin unduly sensitive to sunlight, and particularly about any changes in these tablets during your course of treatment. Tablets for joint problems, water tablets (diuretics), and tablets for diabetes are examples of those that can make the skin sensitive to light. It is also important that you remind staff if you have had a gap in treatment, as this may require the dose of light to be reduced. 1. UVB What is UVB? Ultraviolet light occurs naturally in the sun's rays. The shorter wavelengths of ultraviolet light are known as UVB. Treatment with UVB is the simplest of the treatments discussed in this leaflet, as it involves no tablets. How is treatment with UVB given? UVB can be given by various machines, most of which have fluorescent tubes that look like those used in strip lighting or sunbeds. However, the type of light produced by the tubes used for UVB treatment differs from these, as it concentrates on the burning part of sunlight. Indeed sun beds, which aim to avoid the burning parts of sunlight, are of limited or even of no value in psoriasis. There are various different forms of UVB: one type being used more often now is known as narrow band and comes from TL-01 tubes. It focuses on a single wavelength or colour of ultraviolet, picking out the best part of the spectrum for treating psoriasis while avoiding some of the potentially harmful wavelengths. What sort of psoriasis is treated with UVB? UVB is one of the first steps on from topical treatment, in patients whose psoriasis has failed to respond. It is particularly useful when there are numerous scattered patches of psoriasis, which can be difficult to treat topically,
3 and it is particularly useful in guttate psoriasis, which often gets better on its own but which is difficult to treat with creams because it is made up of lots of tiny spots. UVB is generally not used: o For very inflamed psoriasis. o For psoriasis on areas such as the feet because there is a lack of suitable machinery. o In the treatment of psoriasis on hair-bearing areas such as the scalp. o For patients who live a long way from a treatment centre, or who find it hard to attend several times a week. How frequently will I have to attend for UVB treatment? Treatment is usually given 3 times weekly, sometimes twice weekly, and for 4-6 weeks. Each treatment takes only a few minutes, although it may be combined with other treatments such as creams. As with natural sunlight, treatment times are shorter initially and build up - test doses may be performed to see how easily you burn with UVB. Most dermatologists stop UVB treatment when the psoriasis has cleared or improved significantly, and it is seldom continued as an ongoing ('maintenance') form of treatment, although some patients need repeated courses. Does UVB have any side effects? The skin may burn - as with any form of sunlight. This can generally be avoided by the use of either test doses or small initial doses, and by building up treatment times gradually. Some redness of the skin and subsequent tanning is likely, but you should let the staff in the dermatology department know if you develop any burning sensations (usually hours after treatment). Remember also to tell the staff about any tablets that you are already taking, and about any new ones that you start during your course of treatment. Remind the staff too if you have had a gap in treatment, as this may require the dose of light to be reduced. As with any form of sunlight, there are at least theoretical risks that UVB might cause skin cancers. However these risks are thought to be low. They are difficult to tell from the effects natural sunlight has on the skin over a period of years, but provide a reason why UVB is not used for every patient with psoriasis in preference to creams and ointments, and why UVB is generally not given long-term without careful consideration. The risk of developing skin cancer may be lower with narrow band UVB than with PUVA (discussed below).
4 2. PUVA What is PUVA? PUVA is the term used for a combined treatment with Psoralen (P) and long wavelength ultraviolet A light (UVA). In the presence of UVA, the psoralen combines with the cells in the skin to slow down their rate of division. In psoriasis, these skin cells are multiplying too quickly. The psoralen may be taken as tablets or applied externally to the skin. What are psoralens? Psoralens are a group of naturally occurring chemicals that are found in more than 30 plants (including lemon, celery, parsley, figs and cloves); but the amounts in these are too small to help psoriasis. In PUVA therapy, the psoralen acts by making the skin highly sensitive to sunlight - and in particular to the long wave UVA. What is UVA? The longer wavelengths of the ultraviolet light are known as UVA. In most parts of the world, only small amounts of UVA reach the earth's surface. PUVA therapy needs large amounts of UVA, so this has to be provided by special machines. What is a PUVA cabinet? This is the machine that produces the UVA for PUVA treatment. The UVA comes from specially coated lamps that look like ordinary fluorescent tubes. These are usually built into a box rather like a shower cabinet into which you step for treatment. Some patients dislike the feeling of being inside these cabinets, but most get used to it quickly. Elderly patients may find it difficult or uncomfortable to stand for the time required. Fans are built into the cabinets to control ventilation and temperature. How is the psoralen given? o PUVA tablets. The psoralen drug (usually 8-methoxy psoralen, sometimes known as "8 MOP") is taken in capsule form, 2 hours before the treatment with UVA. With some preparations, the time interval may be different. If the capsules make you feel sick, they should be taken with a light meal or a glass of milk, and sometimes the dose or the type of psoralen may have to be altered to an alternative drug 5 MOP. The level of psoralen in the blood reaches a maximum after about 2 hours, so you will need to be accurate about the times you take the tablets and have the UVA light exposure. Tell the nurse or hospital doctor when you need more capsules, as these are only available from the hospital pharmacy. o Bath PUVA. Another option is to use a form of psoralen that is added to bath water. Usually this involves soaking in a bath for about minutes, followed by the exposure to UVA. As the UVA is given shortly
5 after the bath, and as the concentration of psoralen needs to be measured accurately, the psoralen bath will be given in the dermatology department. o Other forms of PUVA. For localised areas of psoriasis, especially areas such as the hands or feet, psoralen may be applied as a gel or cream, usually about 30 minutes before the exposure to UVA. How long will the PUVA treatment take: and how often will I have to attend for it? o You will attend for PUVA therapy as an outpatient, and so it should not interfere too much with your work or schooling. If you have difficulty in getting time off, your doctor may write to those concerned. o Treatment times depend mainly on your skin type and how it reacts to sunlight. Fair-skinned people who burn easily will have shorter treatment times than dark-skinned individuals who rarely burn in the sun. Treatment times will often be worked out using the results of an initial light test on the skin. o Your treatment sessions will gradually increase from a few minutes to a maximum of minutes if your skin tolerates the treatment. If you notice any burning or irritation, tell the nurse before you start further treatment as the treatment time may have to be reduced, or the affected area may have to be covered up. o Most doctors prescribe therapy twice a week, and the psoriasis is usually much better after 5-8 weeks of treatment. Some people find they can then stop the treatment. o Continuous PUVA therapy should be avoided to reduce the cumulative effects of the UVA. Has PUVA any side effects? It can have: they are divided into short-term and long-term ones. Short-term side effects: o Some patients feel sick after they take their psoralen tablets. o Burning of the skin is sometimes a problem with PUVA, particularly at the start of the treatment course. Test doses may be performed at the start of treatment. Unlike ordinary sunburn, the redness from PUVA can take 2 or 3 days to appear, and can last for more than a week. Remember to let the staff know if you have had a gap in treatment, as this may require the dose of light to be reduced. o The skin may become itchy and dry, but this usually responds to moisturisers. o Some patients develop prominent freckles anywhere on the skin.
6 Long-term side effects: PUVA treatment, if given in excess, can lead to premature ageing of the skin, and to an increased risk of developing certain forms of skin cancer. The risks from a few courses of treatment (less than 5) are small and should not cause undue concern. The risks are higher for those who receive or request PUVA treatment over several years, and especially for people with fair or freckled skin. For this reason, we prefer to stop PUVA treatment once the psoriasis has cleared. What precautions should I take during a course of PUVA treatment? o Eye protection Psoralen capsules make the eyes as well as the skin more sensitive to sunlight. You will be given goggles to wear during treatment, but the eyes also need to be protected by wearing UVA protective glasses whenever you go outside for 24 hours from the time you take the tablets. You need not wear your sunglasses indoors, except in rooms lit by natural sunlight or unshielded fluorescent tubes. All Polaroid-type sunglasses provide adequate eye protection. Your own sunglasses can be tested at the hospital to make sure that they are suitable. Some nontinted glasses or specially coated glasses also provide adequate protection but may be expensive: the hospital can give you details about them if you wish. o Genital protection Underpants of the same size for each treatment or other suitable covering should be worn during the UVA light treatment to protect the male genital area. o Sunbathing and sunbeds Avoid sun exposure on treatment days, and wear suitable clothing to protect your skin from sunlight. Avoid other artificial sun lamps during the course of PUVA treatment. o Other skin treatments Your scalp should continue to be treated with prescribed topical applications, as the UVA may not penetrate the hair enough to help it. Moisturisers can be used in the bath or applied to your skin during PUVA and TL-01 phototherapy. Some moisturisers block UV light, so they are best avoided in the few hours before treatment. Other ointments and creams can often be used but it is best to check with the nurses or doctors at the PUVA unit. Perfumes and aftershaves can cause a skin reaction with the UVA light and should not be used on treatment days. o Other prescribed medications and diet Remember to let the staff know about any tablets that you are taking, or any new tablets that start during your course of treatment, as some may make the skin sensitive to light. Some foods, such as celery, contain psoralens and should not be eaten in excess during PUVA treatment.
7 o Contraception It is very important that women do not become pregnant while having PUVA: efficient contraception should be used throughout. Tablets used to treat severe psoriasis 1. ACITRETIN What is acitretin? Acitretin (trade name Neotigason) is one of a group of drugs known as retinoids, which are related to Vitamin A. Acitretin is the one usually selected for psoriasis. It is prescribed only in hospitals and is hardly ever used in women of childbearing age. How is acitretin taken? It is taken daily, as capsules, either on its own or combined with PUVA or topical therapy. How does acitretin work? It slows down rapidly dividing skin cells and calms the inflammation of psoriasis. Approximately 40% of patients (i.e. 4 out of every 10 people) derive significant benefit What are the possible unwanted side effects of acitretin? The side effects of acitretin are generally mild, and reversible if treatment is stopped. Most depend on the dose that is used. They include: o Harmful effects in pregnancy - see below. o Dryness of the lips, eyes, and face. This can usually be relieved by the use of moisturisers. A lip salve should be used from the start of therapy. o Nose bleeds. o Thinning of the scalp hair. o Muscle aches and pains, especially after vigorous exercise, which can be treated with paracetamol if necessary. o Headaches, usually relieved with paracetamol. The acitretin should be stopped if they persist. o Bone changes can occur after long-term use. What precautions should I take while taking acitretin? o Because retinoids severely damage an unborn baby, pregnancy must be avoided whilst on therapy, and for 2 years after the therapy has stopped. Efficient contraception is essential during this time period. o For this reason male patients must also avoid sharing their tablets and donating blood for a similar period. o Some antibiotics (tetracyclines) should be avoided as they can exacerbate headaches.
8 o The skin becomes more sensitive to sunlight, so that caution is needed to avoid sunburn. What other tests may be needed? A pregnancy test will be needed before you start treatment to exclude the possibility of an early pregnancy. At the start, you will be given a blood test to check your lipids, liver and kidney function; and this will be repeated at intervals. An X-ray of certain joints may be taken every 1 or 2 years. How long will the treatment last? Until the skin has improved and usually for several months thereafter to keep the psoriasis at bay. 2. CICLOSPORIN Further information on ciclosporin can be found in the specific leaflet on this drug found on the website You should read this if you are starting on ciclosporin What is ciclosporin? Ciclosporin (previously called cyclosporin: trade name "Neoral") has been used extensively for many years for patients with kidney or other transplants to prevent organ rejection. It is also effective in controlling severe psoriasis. It may take 3-4 weeks before you see benefit from ciclosporin treatment. How does ciclosporin work? Ciclosporin is an immunosuppressive drug. It reduces the inflammation seen in psoriasis and subsequently reduces the scaling. How is ciclosporin taken? Ciclosporin is taken as capsules, or as a solution by mouth. Your doctor will tell you exactly how much to take and how often you should take it each day. Many tablets can interfere with ciclosporin and reduce its effect. Some increase the risk of side effects. Lists of these 'drug interactions' are readily available for doctors to check if required. It is important that you tell your own doctor, or any other doctor looking after you, that you are on this medication, so that you are not prescribed any therapy that might interfere with it. Most cases of psoriasis can be cleared or substantially improved with ciclosporin in the short term. With monitoring, it is often used for 2 years or can be used intermittently. However, it is generally not considered safe to take ciclosporin for much longer periods of time, and in most cases, the psoriasis recurs on stopping treatment. Different people respond differently; and some can be treated for much longer periods with careful monitoring.
9 What are the side effects of ciclosporin? o The most common side effects are nausea, headaches and indigestion. These rarely necessitate stopping the ciclosporin. o Serious side effects can occur so blood tests are carefully monitored. o Long-term treatment may damage the kidneys and may cause high blood pressure. It is very important that you attend regularly for your hospital appointments so that relevant blood and urine tests can be done to check your kidneys, and your blood pressure can be measured. o Ciclosporin may cause growth retardation in a baby if you become pregnant, so you must not become pregnant while you are taking it. It is important that you discuss contraception, if necessary, with your doctor before you start treatment. What precautions should I take while on ciclosporin? Many medicines can interfere with ciclosporin. Always check with your doctor before taking any medicine whilst on this treatment. 3. METHOTREXATE Further information on methotrexate can be found in the specific leaflet on this drug found on the website We recommend that you read this if starting on methotrexate. How does methotrexate work? Methotrexate has a number of actions that account for its helpful effects in psoriasis. It slows down the skin cells that are dividing so rapidly in psoriasis, and also reduces inflammation by altering the way the immune system works. Methotrexate is usually effective and most patients find their psoriasis clears completely, or nearly so, within 8 weeks. How is methotrexate taken? Methotrexate is usually taken by mouth as a single weekly dose. Tablets of different strengths may look very similar so always check the dose carefully. If it is effective, methotrexate can be taken continuously for many years. What are the possible side effects of methotrexate? Although methotrexate has been used safely in the treatment of severe psoriasis for about 30 years, it can occasionally have adverse side effects. o Nausea may occur in the 24 hours after taking the tablets. o Methotrexate can affect the bone marrow where blood cells are made. This can lead to anaemia and a risk of infections or excessive bleeding. For these reasons, while taking methotrexate, you will need regular blood checks - usually weekly at first, but perhaps every 8-12 weeks once your psoriasis is well under control. o With long-term use, methotrexate can damage the liver. If liver damage is detected early, it is not likely to get worse and may well recover. This
10 is looked for using special blood tests, and occasionally it may be necessary to biopsy (sample) your liver. What precautions should I take while on methotrexate? o Avoid pregnancy: methotrexate affects male and female reproductive function. You must not become pregnant, or father a child, whilst you are on methotrexate or for six months afterwards. o Avoid alcohol: the risk of damaging your liver can be greatly reduced by avoiding alcohol while you are taking methotrexate. The best policy is to drink no alcohol at all except on very rare special occasions. o Several medicines interfere with methotrexate and increase the risk of side effects. You should be given a list of the ones to avoid. They include aspirin, some painkillers and cold remedies, and some antibiotics. 4. HYDROXYCARBAMIDE (previously called hydroxyurea) Further information on hydroxycarbamide can be found in the specific leaflet on this drug found on the website We recommend that you read this if starting on hydroxycarbamide. How does hydroxycarbamide work? Hydroxycarbamide (trade name "Hydrea") slows down the rapid division of skin cells that is characteristic of psoriasis, towards their normal rate. Most patients notice an improvement of their psoriasis within 8 weeks of starting treatment. Sometimes however, the dose of hydroxycarbamide needed to clear psoriasis also affects the bone marrow (see below). When effective, hydroxycarbamide can be used long-term. What are the possible side effects of hydroxycarbamide? o As hydroxycarbamide also reduces the growth of bone marrow cells it can occasionally make you anaemic or prone to infections. For this reason, while you are having hydroxycarbamide, you will require regular blood checks (initially weekly, then less often - perhaps every 8 weeks). o Adequate contraception is essential for women, both while they are taking hydroxycarbamide and for 2 months after it has been stopped. Men must not father a child for this time period. How is treatment given? o Hydroxycarbamide is prescribed as capsules and you will usually be asked to take 2 or 3 per day. o If you have not responded well in 12 weeks, alternative therapies will be discussed with you. If you respond well, treatment will continue for 6 months or more. o From time to time, your doctor will probably decide to stop the therapy to see if you still need it.
11 5. ROTATIONAL THERAPY Most patients with severe psoriasis will be helped by at least one of these therapies, but from time to time your doctor may stop or change the treatment to control the disease better and to minimise the risk of side effects. 6. NEW TREATMENTS Other new, or less commonly used treatments for psoriasis include other medicines that alter the immune system. Some of these, such as mycophenolate mofetil and azathioprine, have been used for some time, but mainly for other conditions. Some of the newer treatments are still being assessed, and some have to be given through a drip into a vein (infliximab) or as injections into the skin (efalizumab and etanercept). Efalizumab (Raptiva) and Etanercept (Enbrel) are two new injection treatments licensed for use in psoriasis. However, they are currently used only for patients with very severe psoriasis who are unable to take one of the standard treatments listed above or who have failed to respond to them. It is particularly important to know as much as possible about these new treatments, and the British Association of Dermatologists will soon be able to post information about them on its website. Until then the instructions that come with these treatments are good and detailed. Where can I get more information about psoriasis and its treatment? o The Psoriasis Association: Milton House 7 Milton Street Northampton NN2 7JG Tel: (01604) Fax: (01604) mail@psoriasis.demon.co.uk Web: o The Psoriatic Arthropathy Alliance: P O Box 111 St Albans Herts. AL2 3JQ Tel: (0870) Fax: As Above Business Line: (0870) info@paalliance.org Web:
12 o The British Association of Dermatologists has several other Patient Information Leaflets on its website that deal with psoriasis: 1. Psoriasis an overview. 2. Topical treatments for psoriasis 3. Ciclosporin 4. Methotrexate 5. Hydroxycarbamide 6. Etanercept 7. Efalizumab. 8. Infliximab (Whilst every effort has been made to ensure that the information given in this leaflet is accurate, not every treatment will be suitable or effective for every person. Your own doctor will be able to advise in greater detail.) BRITISH ASSOCIATION OF DERMATOLOGISTS PATIENT INFORMATION LEAFLET PRODUCED MARCH 2005
Treating your skin condition with narrowband ultraviolet B radiation (NB-UVB)
 Treating your skin condition with narrowband ultraviolet B radiation (NB-UVB) Your doctor has referred you to the Dowling Day Treatment Centre for a course of narrow band ultraviolet treatment for your
Treating your skin condition with narrowband ultraviolet B radiation (NB-UVB) Your doctor has referred you to the Dowling Day Treatment Centre for a course of narrow band ultraviolet treatment for your
Department of Dermatology, Churchill Hospital PUVA Treatment
 Oxford University Hospitals NHS Trust Department of Dermatology, Churchill Hospital PUVA Treatment information for patients CONTENTS What is PUVA 3 What conditions are treated with PUVA? 3 How is PUVA
Oxford University Hospitals NHS Trust Department of Dermatology, Churchill Hospital PUVA Treatment information for patients CONTENTS What is PUVA 3 What conditions are treated with PUVA? 3 How is PUVA
X-Plain Psoriasis Reference Summary
 X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
Treatment options a simple guide
 Guide Treatment options a simple guide To decide which treatment is right for you, a good starting point is to know what options you have and to understand the pros and cons of each one. People respond
Guide Treatment options a simple guide To decide which treatment is right for you, a good starting point is to know what options you have and to understand the pros and cons of each one. People respond
PATIENT RESOURCES: PSORIASIS
 PATIENT RESOURCES: PSORIASIS Psoriasis is a persistent skin disorder in which there are red, thickened areas with silvery scales, most often on the scalp, elbows, knees, and lower back. Some cases, of
PATIENT RESOURCES: PSORIASIS Psoriasis is a persistent skin disorder in which there are red, thickened areas with silvery scales, most often on the scalp, elbows, knees, and lower back. Some cases, of
Psoriasis is a skin condition that causes scaly red patches on your skin. There's no cure for psoriasis, but there are treatments that can help.
 Patient information from the BMJ Group Psoriasis What is it? What are the symptoms? How is it diagnosed? How common is it? What treatments work? What will happen? Questions to ask Psoriasis If you get
Patient information from the BMJ Group Psoriasis What is it? What are the symptoms? How is it diagnosed? How common is it? What treatments work? What will happen? Questions to ask Psoriasis If you get
Professor Andrew Wright,
 Professor Andrew Wright, Systemic treatments are drugs taken as tablets or injections that travel through the bloodstream, dampening down the immune system to reach and treat eczema all over the body.
Professor Andrew Wright, Systemic treatments are drugs taken as tablets or injections that travel through the bloodstream, dampening down the immune system to reach and treat eczema all over the body.
Methotrexate treatment
 Methotrexate treatment Oral methotrexate pre-treatment patient information leaflet This leaflet has been prepared to support information given to you as part of your discussions with the doctor, nurse
Methotrexate treatment Oral methotrexate pre-treatment patient information leaflet This leaflet has been prepared to support information given to you as part of your discussions with the doctor, nurse
Temozolomide (oral) with concurrent radiotherapy to the brain
 Temozolomide (oral) with concurrent radiotherapy to the brain Temozolomide (oral) with concurrent radiotherapy to the brain This leaflet is offered as a guide to you and your family. You will find it useful
Temozolomide (oral) with concurrent radiotherapy to the brain Temozolomide (oral) with concurrent radiotherapy to the brain This leaflet is offered as a guide to you and your family. You will find it useful
METHOTREXATE TREATMENT
 METHOTREXATE TREATMENT This leaflet has been prepared to support information given to you as part of your discussions with the doctor, nurse or pharmacist before you start treatment with oral methotrexate.
METHOTREXATE TREATMENT This leaflet has been prepared to support information given to you as part of your discussions with the doctor, nurse or pharmacist before you start treatment with oral methotrexate.
PSORIASIS AND ITS. Learn how vitamin D medications play an important role in managing plaque psoriasis
 PLAQUE PSORIASIS AND ITS TREATMENTS Learn how vitamin D medications play an important role in managing plaque psoriasis 2 Understanding Plaque Psoriasis WHAT CAUSES PLAQUE PSORIASIS? No one knows exactly
PLAQUE PSORIASIS AND ITS TREATMENTS Learn how vitamin D medications play an important role in managing plaque psoriasis 2 Understanding Plaque Psoriasis WHAT CAUSES PLAQUE PSORIASIS? No one knows exactly
MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1%
![MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% MEDICATION GUIDE. PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1%](/thumbs/27/10084771.jpg) MEDICATION GUIDE PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% Read the Medication Guide every time you or a family member gets PROTOPIC Ointment. There may be new information. This Medication
MEDICATION GUIDE PROTOPIC [pro-top-ik] (tacrolimus) Ointment 0.03% Ointment 0.1% Read the Medication Guide every time you or a family member gets PROTOPIC Ointment. There may be new information. This Medication
Graft-versus-host disease (GvHD)
 Graft-versus-host disease (GvHD) This information is an extract from the booklet Understanding donor stem cell (allogeneic) transplants. You may find the full booklet helpful. We can send you a free copy
Graft-versus-host disease (GvHD) This information is an extract from the booklet Understanding donor stem cell (allogeneic) transplants. You may find the full booklet helpful. We can send you a free copy
Other treatments for chronic myeloid leukaemia
 Other treatments for chronic myeloid leukaemia This information is an extract from the booklet Understanding chronic myeloid leukaemia. You may find the full booklet helpful. We can send you a copy free
Other treatments for chronic myeloid leukaemia This information is an extract from the booklet Understanding chronic myeloid leukaemia. You may find the full booklet helpful. We can send you a copy free
MEDICATION GUIDE. SORIATANE (sor-rye-uh-tane) (acitretin) Capsules
 Page 30 Please print: Patient name and address: Telephone: I have fully explained to the patient,, the nature and purpose of the treatment described above and the risks to females of childbearing potential.
Page 30 Please print: Patient name and address: Telephone: I have fully explained to the patient,, the nature and purpose of the treatment described above and the risks to females of childbearing potential.
Teriflunomide (Aubagio) 14mg once daily tablet
 Teriflunomide (Aubagio) 14mg once daily tablet Exceptional healthcare, personally delivered Your Consultant Neurologist has suggested that you may benefit from treatment with Teriflunomide. The decision
Teriflunomide (Aubagio) 14mg once daily tablet Exceptional healthcare, personally delivered Your Consultant Neurologist has suggested that you may benefit from treatment with Teriflunomide. The decision
TOPICAL TREATMENTS FOR PSORIASIS
 TOPICAL TREATMENTS FOR PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with preparations that are applied to the skin. This leaflet has been written to help you
TOPICAL TREATMENTS FOR PSORIASIS What are the aims of this leaflet? Patients with psoriasis are usually treated with preparations that are applied to the skin. This leaflet has been written to help you
Paracetamol apollo +9191 46 950 950. Paracetamol apollo +9191 46 950 950. Paracetamol
 Paracetamol apollo +9191 46 950 950 Paracetamol apollo +9191 46 950 950 Paracetamol CAS Number : 103-90-2 Molecular Weight : 151.17 g/mol Molecular Formula : C8H9NO2 Systematic (IUPAC) : N-(4- hydroxyphenyl)ethanamide
Paracetamol apollo +9191 46 950 950 Paracetamol apollo +9191 46 950 950 Paracetamol CAS Number : 103-90-2 Molecular Weight : 151.17 g/mol Molecular Formula : C8H9NO2 Systematic (IUPAC) : N-(4- hydroxyphenyl)ethanamide
Treating psoriasis and psoriatic arthritis. A booklet for patients and carers
 Treating psoriasis and psoriatic arthritis A booklet for patients and carers Picture credits Cover Stuart Neville Page 4 Dr P. Marazzi/Science Photo Library CNRI/Science Photo Library CID, ISM/Science
Treating psoriasis and psoriatic arthritis A booklet for patients and carers Picture credits Cover Stuart Neville Page 4 Dr P. Marazzi/Science Photo Library CNRI/Science Photo Library CID, ISM/Science
Patient Information Leaflet
 Patient Information Leaflet METHOTREXATE We hope this fact sheet will provide you with some information about Methotrexate and answer some of the questions you may have. Methotrexate is available in tablet
Patient Information Leaflet METHOTREXATE We hope this fact sheet will provide you with some information about Methotrexate and answer some of the questions you may have. Methotrexate is available in tablet
Answering your questions on Chronic Myeloid Leukaemia (CML)
 Answering your questions on Chronic Myeloid Leukaemia (CML) Your guide to understanding CML and Glivec (imatinib) treatment The information in this booklet is designed to help you understand chronic myeloid
Answering your questions on Chronic Myeloid Leukaemia (CML) Your guide to understanding CML and Glivec (imatinib) treatment The information in this booklet is designed to help you understand chronic myeloid
CICLOSPORIN. What are the aims of this leaflet?
 CICLOSPORIN What are the aims of this leaflet? This leaflet has been written to help you understand more about ciclosporin. It tells you what it is, how it works, how it is used to treat skin conditions,
CICLOSPORIN What are the aims of this leaflet? This leaflet has been written to help you understand more about ciclosporin. It tells you what it is, how it works, how it is used to treat skin conditions,
Multiple Myeloma. This reference summary will help you understand multiple myeloma and its treatment options.
 Multiple Myeloma Introduction Multiple myeloma is a type of cancer that affects white blood cells. Each year, thousands of people find out that they have multiple myeloma. This reference summary will help
Multiple Myeloma Introduction Multiple myeloma is a type of cancer that affects white blood cells. Each year, thousands of people find out that they have multiple myeloma. This reference summary will help
Methotrexate. What is methotrexate?
 Methotrexate What is methotrexate? Methotrexate is a mild immunosuppressant that also exhibits antiinflammatory activity. Methotrexate is commonly used for the treatment of certain cancers including but
Methotrexate What is methotrexate? Methotrexate is a mild immunosuppressant that also exhibits antiinflammatory activity. Methotrexate is commonly used for the treatment of certain cancers including but
Vincristine by short infusion Doxorubicin by injection Cyclophosphamide by injection Rituximab by an infusion over between 60 minutes to a few hours
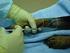 R-CHOP R-CHOP This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy may reduce the risk of the cancer coming back, for others
R-CHOP R-CHOP This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy may reduce the risk of the cancer coming back, for others
ORAL ANTICOAGULANTS RIVAROXABAN (XARELTO) FOR PULMONARY EMBOLISM (PE)
 ORAL ANTICOAGULANTS RIVAROXABAN (XARELTO) FOR PULMONARY EMBOLISM (PE) Information Leaflet Your Health. Our Priority. Page 2 of 6 What Are Anticoagulants And What Do They Do? This information leaflet has
ORAL ANTICOAGULANTS RIVAROXABAN (XARELTO) FOR PULMONARY EMBOLISM (PE) Information Leaflet Your Health. Our Priority. Page 2 of 6 What Are Anticoagulants And What Do They Do? This information leaflet has
FEC chemotherapy. The drugs that are used. How treatment is given
 Macmillan and Cancerbackup have merged. Together we provide free, high quality information for all. FEC chemotherapy This fact sheet is about a chemotherapy treatment for breast cancer called FEC. It describes
Macmillan and Cancerbackup have merged. Together we provide free, high quality information for all. FEC chemotherapy This fact sheet is about a chemotherapy treatment for breast cancer called FEC. It describes
ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR DEEP VEIN THROMBOSIS (DVT)
 ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR DEEP VEIN THROMBOSIS (DVT) Information Leaflet Your Health. Our Priority. Page 2 of 6 What Are Anticoagulants And What Do They Do? This information leaflet
ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR DEEP VEIN THROMBOSIS (DVT) Information Leaflet Your Health. Our Priority. Page 2 of 6 What Are Anticoagulants And What Do They Do? This information leaflet
Medicines for Psoriatic Arthritis. A Review of the Research for Adults
 Medicines for Psoriatic Arthritis A Review of the Research for Adults Is This Information Right for Me? Yes, this information is right for you if: Your doctor* has told you that you have psoriatic (pronounced
Medicines for Psoriatic Arthritis A Review of the Research for Adults Is This Information Right for Me? Yes, this information is right for you if: Your doctor* has told you that you have psoriatic (pronounced
BOWEN S DISEASE (SQUAMOUS CELL CARCINOMA IN SITU)
 BOWEN S DISEASE (SQUAMOUS CELL CARCINOMA IN SITU) What are the aims of this leaflet? This leaflet has been written to help you understand more about squamous cell carcinoma in situ (Bowen s disease). It
BOWEN S DISEASE (SQUAMOUS CELL CARCINOMA IN SITU) What are the aims of this leaflet? This leaflet has been written to help you understand more about squamous cell carcinoma in situ (Bowen s disease). It
Acne (Acne Vulgaris) A common type of bacteria that lives on the skin, known as Propionibacterium acnes, sometimes
 Acne (Acne Vulgaris) Acne, clinically known as acne vulgaris, is the most common skin disease. It affects 85% of teenagers, some as young as 12, and often continues into adulthood. It is also called pimples,
Acne (Acne Vulgaris) Acne, clinically known as acne vulgaris, is the most common skin disease. It affects 85% of teenagers, some as young as 12, and often continues into adulthood. It is also called pimples,
PACKAGE LEAFLET: INFORMATION FOR THE USER. Elidel 10 mg/g Cream. pimecrolimus
 PACKAGE LEAFLET: INFORMATION FOR THE USER Elidel 10 mg/g Cream pimecrolimus Read all of this leaflet carefully before you start using Elidel cream Keep this leaflet. You may need to read it again. If you
PACKAGE LEAFLET: INFORMATION FOR THE USER Elidel 10 mg/g Cream pimecrolimus Read all of this leaflet carefully before you start using Elidel cream Keep this leaflet. You may need to read it again. If you
Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement
 Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement A Copy of this page signed by all three parties should be retained in the
Topical Tacrolimus or Pimecrolimus for the treatment of mild, moderate or severe atopic eczema. Effective Shared Care Agreement A Copy of this page signed by all three parties should be retained in the
Liver Disease & Hepatitis Program Providers: Brian McMahon, MD, Steve Livingston, MD, Lisa Townshend, ANP. Primary Care Provider:
 Liver Disease & Hepatitis Program Providers: Brian McMahon, MD, Steve Livingston, MD, Lisa Townshend, ANP Primary Care Provider: If you are considering hepatitis C treatment, please read this treatment
Liver Disease & Hepatitis Program Providers: Brian McMahon, MD, Steve Livingston, MD, Lisa Townshend, ANP Primary Care Provider: If you are considering hepatitis C treatment, please read this treatment
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
biologics for the treatment of psoriasis
 How to contact us The Psoriasis Association Dick Coles House 2 Queensbridge Northampton NN4 7BF tel: 08456 760 076 (01604) 251 620 fax: (01604) 251 621 email: mail@psoriasis-association.org.uk www.psoriasis-association.org.uk
How to contact us The Psoriasis Association Dick Coles House 2 Queensbridge Northampton NN4 7BF tel: 08456 760 076 (01604) 251 620 fax: (01604) 251 621 email: mail@psoriasis-association.org.uk www.psoriasis-association.org.uk
Nail Psoriasis. A positive approach. to psoriasis and. psoriatic arthritis
 Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What is psoriasis? Psoriasis (Ps) is a long-term (chronic) scaling disease of the skin, which affects 2% 3% of the UK population.
Nail Psoriasis A positive approach to psoriasis and psoriatic arthritis What is psoriasis? Psoriasis (Ps) is a long-term (chronic) scaling disease of the skin, which affects 2% 3% of the UK population.
Psoriatic arthritis FACTSHEET
 1 What is psoriatic arthritis? Psoriatic arthritis (PsA) is a disease where joints around the body become inflamed and sore. It can make moving about difficult and painful. People who have PsA also have
1 What is psoriatic arthritis? Psoriatic arthritis (PsA) is a disease where joints around the body become inflamed and sore. It can make moving about difficult and painful. People who have PsA also have
HIRSUTISM. What are the aims of this leaflet?
 HIRSUTISM What are the aims of this leaflet? This leaflet has been written to help you understand more about hirsutism. It tells you what it is, what causes it, what can be done about it, and provides
HIRSUTISM What are the aims of this leaflet? This leaflet has been written to help you understand more about hirsutism. It tells you what it is, what causes it, what can be done about it, and provides
ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR ATRIAL FIBRILLATION
 ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR ATRIAL FIBRILLATION Information Leaflet Your Health. Our Priority. Page 2 of 6 What Are Anticoagulants And What Do They Do? This information leaflet has
ORAL ANTICOAGULANTS - RIVAROXABAN (XARELTO) FOR ATRIAL FIBRILLATION Information Leaflet Your Health. Our Priority. Page 2 of 6 What Are Anticoagulants And What Do They Do? This information leaflet has
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radioactive Ra 223 therapy. Information for patients Weston Park Hospital
 Radioactive Ra 223 therapy Information for patients Weston Park Hospital page 2 of 8 This leaflet contains information about radioactive Ra 223 therapy. If you have any questions about your treatment,
Radioactive Ra 223 therapy Information for patients Weston Park Hospital page 2 of 8 This leaflet contains information about radioactive Ra 223 therapy. If you have any questions about your treatment,
Understanding Cytotoxic Chemotherapy
 Understanding Cytotoxic Chemotherapy Introduction Chemotherapy is part of your continuing treatment. This booklet has been compiled in an effort to help you understand cytotoxic chemotherapy. It is your
Understanding Cytotoxic Chemotherapy Introduction Chemotherapy is part of your continuing treatment. This booklet has been compiled in an effort to help you understand cytotoxic chemotherapy. It is your
Psoriatic Arthritis. Psoriatic Arthritis 3/05
 Psoriatic Arthritis 3/05 Psoriatic Arthritis Arthritis Ireland, 1 Clanwilliam Square, Grand Canal Quay, Dublin 2 T: (01) 661 8188 F: (01) 661 8261 www.arthritisireland.ie What is in this booklet? This
Psoriatic Arthritis 3/05 Psoriatic Arthritis Arthritis Ireland, 1 Clanwilliam Square, Grand Canal Quay, Dublin 2 T: (01) 661 8188 F: (01) 661 8261 www.arthritisireland.ie What is in this booklet? This
Vibramycin Capsules Doxycycline hyclate capsules USP. Vibra-Tabs Film Coated Tablets Doxycycline hyclate tablets USP
 32 READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Vibramycin Capsules Doxycycline hyclate capsules USP Vibra-Tabs Film Coated Tablets Doxycycline hyclate tablets USP
32 READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Vibramycin Capsules Doxycycline hyclate capsules USP Vibra-Tabs Film Coated Tablets Doxycycline hyclate tablets USP
AUBAGIO Conversation Starter
 AUBAGIO Conversation Starter When you are choosing a multiple sclerosis (MS) treatment for the first time or are considering switching your MS therapy, there can be a lot to think about for both you and
AUBAGIO Conversation Starter When you are choosing a multiple sclerosis (MS) treatment for the first time or are considering switching your MS therapy, there can be a lot to think about for both you and
Radiotherapy for a mesothelioma
 Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy for a mesothelioma Information for patients Introduction This leaflet is for people who have been recommended treatment with
Oxford University Hospitals NHS Trust The Radiotherapy Department Radiotherapy for a mesothelioma Information for patients Introduction This leaflet is for people who have been recommended treatment with
How To Deal With The Side Effects Of Radiotherapy
 Radiotherapy to the Bowel (Colo-Rectal Tumours) Information for patients Northern Centre for Cancer Care Freeman Hospital Introduction Your oncologist has advised you to have a course of radiotherapy to
Radiotherapy to the Bowel (Colo-Rectal Tumours) Information for patients Northern Centre for Cancer Care Freeman Hospital Introduction Your oncologist has advised you to have a course of radiotherapy to
VITILIGO Charles Camisa, MD 1/24/12. Vitiligo is a common autoimmune skin disease that causes gradual loss of the natural
 VITILIGO Charles Camisa, MD 1/24/12 What is vitiligo? Vitiligo is a common autoimmune skin disease that causes gradual loss of the natural brown pigment in the skin called melanin. It affects about 1%
VITILIGO Charles Camisa, MD 1/24/12 What is vitiligo? Vitiligo is a common autoimmune skin disease that causes gradual loss of the natural brown pigment in the skin called melanin. It affects about 1%
Oxford University Hospitals. NHS Trust. Dermatology Department Frontal Fibrosing Alopecia. Information for patients
 Oxford University Hospitals NHS Trust Dermatology Department Frontal Fibrosing Alopecia Information for patients What is Frontal Fibrosing Alopecia (FFA)? FFA is a condition which causes hair loss, mainly
Oxford University Hospitals NHS Trust Dermatology Department Frontal Fibrosing Alopecia Information for patients What is Frontal Fibrosing Alopecia (FFA)? FFA is a condition which causes hair loss, mainly
SQUAMOUS CELL CARCINOMA
 SQUAMOUS CELL CARCINOMA What are the aims of this leaflet? This leaflet has been written to help you understand more about squamous cell carcinomas of the skin. It tells you what they are, what causes
SQUAMOUS CELL CARCINOMA What are the aims of this leaflet? This leaflet has been written to help you understand more about squamous cell carcinomas of the skin. It tells you what they are, what causes
Radiation Oncology Patient information. Radiation Therapy for breast cancers
 Radiation Oncology Patient information Radiation Therapy for breast cancers Radiation Therapy for breast cancers 1 Radiation therapy for breast cancer Radiation therapy plays a vital role in treating and
Radiation Oncology Patient information Radiation Therapy for breast cancers Radiation Therapy for breast cancers 1 Radiation therapy for breast cancer Radiation therapy plays a vital role in treating and
How long will it take to work? You may begin to feel better within a few days or it may take up to six weeks after your first treatment session.
 Crohn's and Colitis UK Drug Treatment Information Improving life for people affected by inflammatory bowel diseases Infliximab This information leaflet aims to answer common questions you may have if you
Crohn's and Colitis UK Drug Treatment Information Improving life for people affected by inflammatory bowel diseases Infliximab This information leaflet aims to answer common questions you may have if you
Guide to PUVA Therapy
 Guide to PUVA Therapy Elisabeth Richard, MD Light Therapy for Skin Disease lightandlaser.com 410-847-3700!1 OVERVIEW PUVA therapy consists of taking a medication called psoralen (pronounced soralen with
Guide to PUVA Therapy Elisabeth Richard, MD Light Therapy for Skin Disease lightandlaser.com 410-847-3700!1 OVERVIEW PUVA therapy consists of taking a medication called psoralen (pronounced soralen with
There is a risk of renal impairment in dehydrated children and adolescents.
 PACKAGE LEAFLET: INFORMATION FOR THE USER MELFEN 200mg FILM-COATED TABLETS MELFEN 400mg FILM-COATED TABLETS Ibuprofen Read all of this leaflet carefully before you start taking this medicine because it
PACKAGE LEAFLET: INFORMATION FOR THE USER MELFEN 200mg FILM-COATED TABLETS MELFEN 400mg FILM-COATED TABLETS Ibuprofen Read all of this leaflet carefully before you start taking this medicine because it
Psoriatic Arthritis www.arthritis.org.nz
 Psoriatic Arthritis www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Psoriatic arthritis usually appears in people between the ages of 30 to 50.
Psoriatic Arthritis www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Psoriatic arthritis usually appears in people between the ages of 30 to 50.
Have a shower, rather than a bath to avoid exposing your genitals to the chemicals in your cleaning products for too long. Always empty your bladder
 Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation Information for patients and families. www.anaesthesia.ie 1 This information leaflet is for anyone expecting to have an eye operation with a local anaesthetic.
Local anaesthesia for your eye operation Information for patients and families. www.anaesthesia.ie 1 This information leaflet is for anyone expecting to have an eye operation with a local anaesthetic.
Like cocaine, heroin is a drug that is illegal in some areas of the world. Heroin is highly addictive.
 Heroin Introduction Heroin is a powerful drug that affects the brain. People who use it can form a strong addiction. Addiction is when a drug user can t stop taking a drug, even when he or she wants to.
Heroin Introduction Heroin is a powerful drug that affects the brain. People who use it can form a strong addiction. Addiction is when a drug user can t stop taking a drug, even when he or she wants to.
SKIN CANCER AND TANNING 101. Introduction. There are more than one hundred types of cancer. All the kinds of cancer begin in our cells.
 Introduction There are more than one hundred types of cancer. All the kinds of cancer begin in our cells. Normal cells grow and multiply and then die. Cancer cells grow and multiply and keep growing and
Introduction There are more than one hundred types of cancer. All the kinds of cancer begin in our cells. Normal cells grow and multiply and then die. Cancer cells grow and multiply and keep growing and
UW MEDICINE PATIENT EDUCATION. Xofigo Therapy. For metastatic prostate cancer. What is Xofigo? How does it work?
 UW MEDICINE PATIENT EDUCATION Xofigo Therapy For metastatic prostate cancer This handout explains how the drug Xofigo is used to treat metastatic prostate cancer. What is Xofigo? Xofigo is a radioactive
UW MEDICINE PATIENT EDUCATION Xofigo Therapy For metastatic prostate cancer This handout explains how the drug Xofigo is used to treat metastatic prostate cancer. What is Xofigo? Xofigo is a radioactive
Patient Information Once Weekly FOSAMAX (FOSS-ah-max) (alendronate sodium) Tablets and Oral Solution
 Patient Information Once Weekly FOSAMAX (FOSS-ah-max) (alendronate sodium) Tablets and Oral Solution Read this information before you start taking FOSAMAX *. Also, read the leaflet each time you refill
Patient Information Once Weekly FOSAMAX (FOSS-ah-max) (alendronate sodium) Tablets and Oral Solution Read this information before you start taking FOSAMAX *. Also, read the leaflet each time you refill
2 What you need to know before you have Ampiclox
 Reason for update: GDS 14 & QRD Updates Response to questions for variation update section 4.1 of SPC MHRA Submission Date: 6 November 2014 MHRA Approval Date: Text Date: October 2014 Text Issue and Draft
Reason for update: GDS 14 & QRD Updates Response to questions for variation update section 4.1 of SPC MHRA Submission Date: 6 November 2014 MHRA Approval Date: Text Date: October 2014 Text Issue and Draft
Leflunomide Leflunomide
 Drug information Leflunomide Leflunomide This leaflet provides information on leflunomide and will answer any questions you have about the treatment. Arthritis Research UK produce and print our booklets
Drug information Leflunomide Leflunomide This leaflet provides information on leflunomide and will answer any questions you have about the treatment. Arthritis Research UK produce and print our booklets
Psoriasis. Student's Name. Institution. Date of Submission
 Running head: PSORIASIS Psoriasis Student's Name Institution Date of Submission PSORIASIS 1 Abstract Psoriasis is a non-contagious chronic skin disease that is characterized by inflammatory and multiplying
Running head: PSORIASIS Psoriasis Student's Name Institution Date of Submission PSORIASIS 1 Abstract Psoriasis is a non-contagious chronic skin disease that is characterized by inflammatory and multiplying
Biologic Treatments for Rheumatoid Arthritis
 Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
MEDICATION GUIDE POMALYST (POM-uh-list) (pomalidomide) capsules. What is the most important information I should know about POMALYST?
 MEDICATION GUIDE POMALYST (POM-uh-list) (pomalidomide) capsules What is the most important information I should know about POMALYST? Before you begin taking POMALYST, you must read and agree to all of
MEDICATION GUIDE POMALYST (POM-uh-list) (pomalidomide) capsules What is the most important information I should know about POMALYST? Before you begin taking POMALYST, you must read and agree to all of
Getting the best result from Opioid medicine. in the management of chronic pain
 Getting the best result from Opioid medicine in the management of chronic pain Your doctor has prescribed you opioid medicine to help you manage your chronic pain. This patient information leaflet gives
Getting the best result from Opioid medicine in the management of chronic pain Your doctor has prescribed you opioid medicine to help you manage your chronic pain. This patient information leaflet gives
Laser Treatment for Acne
 Laser Treatment for Acne Exceptional healthcare, personally delivered Welcome to the Laser Centre of the South West We are part of the Plastic Surgery Department at North Bristol NHS Trust, and were set
Laser Treatment for Acne Exceptional healthcare, personally delivered Welcome to the Laser Centre of the South West We are part of the Plastic Surgery Department at North Bristol NHS Trust, and were set
Treatment for pleural mesothelioma
 Treatment for pleural mesothelioma This information is an extract from the booklet Understanding mesothelioma. You may find the full booklet helpful. We can send you a free copy see page 9. Contents Treatment
Treatment for pleural mesothelioma This information is an extract from the booklet Understanding mesothelioma. You may find the full booklet helpful. We can send you a free copy see page 9. Contents Treatment
THE KIDNEY. Bulb of penis Abdominal aorta Scrotum Adrenal gland Inferior vena cava Urethra Corona glandis. Kidney. Glans penis Testicular vein
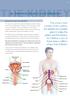 29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
Laser Tattoo Removal. Birmingham Regional Skin Laser Centre
 What is laser tattoo removal? Laser tattoo removal is a treatment to help fade and remove unwanted tattoos. We are able to remove the following types of tattoos: Amateur tattoos - normally formed using
What is laser tattoo removal? Laser tattoo removal is a treatment to help fade and remove unwanted tattoos. We are able to remove the following types of tattoos: Amateur tattoos - normally formed using
Key words: Vitamin D Production, Vitamin D Deficiency, and Vitamin D Treatment
 Title: Vitamin D Author: Kerry Lynn Kuffenkam Date: 4-29-09 Key words: Vitamin D Production, Vitamin D Deficiency, and Vitamin D Treatment Abstract: Since the term Vitamin D contains the word vitamin most
Title: Vitamin D Author: Kerry Lynn Kuffenkam Date: 4-29-09 Key words: Vitamin D Production, Vitamin D Deficiency, and Vitamin D Treatment Abstract: Since the term Vitamin D contains the word vitamin most
VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients
 VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients The Regimen contains: V = vincristine (Oncovin ) A = Adriamycin (doxorubicin) D = Decadron (dexamethasone) How Is This Regimen Given?
VAD Chemotherapy Regimen for Multiple Myeloma Information for Patients The Regimen contains: V = vincristine (Oncovin ) A = Adriamycin (doxorubicin) D = Decadron (dexamethasone) How Is This Regimen Given?
Eastern Health MS Service. Tysabri Therapy. Information for People with MS and their Families
 Eastern Health MS Service Tysabri Therapy Information for People with MS and their Families The Eastern Health MS Service has developed this information for you as a guide through what will happen to you
Eastern Health MS Service Tysabri Therapy Information for People with MS and their Families The Eastern Health MS Service has developed this information for you as a guide through what will happen to you
Lichen Sclerosus. Exceptional healthcare, personally delivered
 Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Lichen Sclerosus Exceptional healthcare, personally delivered Lichen Sclerosus (LS) is an itchy skin condition usually affecting genital skin, but it can occur elsewhere. It affects women more often than
Mycophenolate mofetil (CellCept ): risks of miscarriage and birth defects. Patient guide. Key points to remember
 Mycophenolate (CellCept ): risks of miscarriage and birth defects Patient guide Key points to remember Mycophenolate (CellCept ) causes birth defects and miscarriages Follow the contraceptive advice given
Mycophenolate (CellCept ): risks of miscarriage and birth defects Patient guide Key points to remember Mycophenolate (CellCept ) causes birth defects and miscarriages Follow the contraceptive advice given
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. [new-ka la]
![READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. [new-ka la] READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. [new-ka la]](/thumbs/35/17235501.jpg) READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr NUCALA [new-ka la] mepolizumab lyophilized powder for subcutaneous injection Read this carefully before you start
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr NUCALA [new-ka la] mepolizumab lyophilized powder for subcutaneous injection Read this carefully before you start
about Why You Should Know Melanoma
 about Why You Should Know Melanoma Why You Should Know about Melanoma Each year, more than 3 million Americans are diagnosed with skin cancer. This is the most common form of cancer. Of these, more than
about Why You Should Know Melanoma Why You Should Know about Melanoma Each year, more than 3 million Americans are diagnosed with skin cancer. This is the most common form of cancer. Of these, more than
Psoriasis: Controlled YOUR GUIDE TO BIOLOGICAL TREATMENTS FOR PLAQUE PSORIASIS
 Psoriasis: Controlled YOUR GUIDE TO BIOLOGICAL TREATMENTS FOR PLAQUE PSORIASIS 2 Proudly supported by Disclaimer: Some photographs and models used in this booklet are for illustrative purposes only and
Psoriasis: Controlled YOUR GUIDE TO BIOLOGICAL TREATMENTS FOR PLAQUE PSORIASIS 2 Proudly supported by Disclaimer: Some photographs and models used in this booklet are for illustrative purposes only and
Mitoxantrone. For multiple sclerosis. InfoNEURO INFORMATION FOR PATIENTS. Montreal Neurological Hospital
 i InfoNEURO Montreal Neurological Hospital INFORMATION FOR PATIENTS Mitoxantrone For multiple sclerosis Centre universitaire de santé McGill McGill University Health Centre Collaborators: D. Lowden Clinical
i InfoNEURO Montreal Neurological Hospital INFORMATION FOR PATIENTS Mitoxantrone For multiple sclerosis Centre universitaire de santé McGill McGill University Health Centre Collaborators: D. Lowden Clinical
SHINGLES (Herpes zoster infection)
 SHINGLES (Herpes zoster infection) What are the aims of this leaflet? This leaflet has been written to help you understand more about shingles. It will tell you what it is, what causes it, what can be
SHINGLES (Herpes zoster infection) What are the aims of this leaflet? This leaflet has been written to help you understand more about shingles. It will tell you what it is, what causes it, what can be
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
MEDICATION GUIDE STELARA
 MEDICATION GUIDE STELARA (stel ar a) (ustekinumab) Injection What is the most important information I should know about STELARA? STELARA is a medicine that affects your immune system. STELARA can increase
MEDICATION GUIDE STELARA (stel ar a) (ustekinumab) Injection What is the most important information I should know about STELARA? STELARA is a medicine that affects your immune system. STELARA can increase
TERMINATION OF PREGNANCY- MEDICAL
 TERMINATION OF PREGNANCY- MEDICAL Information Leaflet Your Health. Our Priority. Page 2 of 8 You have been offered a medical termination of pregnancy using mifepristone. You will have been given some verbal
TERMINATION OF PREGNANCY- MEDICAL Information Leaflet Your Health. Our Priority. Page 2 of 8 You have been offered a medical termination of pregnancy using mifepristone. You will have been given some verbal
Psoriasis Treatment Transition Pathway
 Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
CMF: Cyclophosphamide, Methotrexate and Fluorouracil
 PATIENT EDUCATION patienteducation.osumc.edu CMF: Cyclophosphamide, Methotrexate and Fluorouracil What is CMF? This is the short name for the drugs used for this chemotherapy treatment. The three drugs
PATIENT EDUCATION patienteducation.osumc.edu CMF: Cyclophosphamide, Methotrexate and Fluorouracil What is CMF? This is the short name for the drugs used for this chemotherapy treatment. The three drugs
Humulin (HU-mu-lin) R
 1 PATIENT INFORMATION Humulin (HU-mu-lin) R Regular U-500 (Concentrated) insulin human injection, USP (rdna origin) Read the Patient Information that comes with Humulin R U-500 before you start taking
1 PATIENT INFORMATION Humulin (HU-mu-lin) R Regular U-500 (Concentrated) insulin human injection, USP (rdna origin) Read the Patient Information that comes with Humulin R U-500 before you start taking
Vitamin D. Why Vitamin D is important and how to get enough
 Vitamin D Why Vitamin D is important and how to get enough Why is vitamin D vital for health? Vitamin D is needed by the body for both physical and mental health, but is best known for making sure bones
Vitamin D Why Vitamin D is important and how to get enough Why is vitamin D vital for health? Vitamin D is needed by the body for both physical and mental health, but is best known for making sure bones
Local steroid injections
 Drug information Local steroid injections Local steroid injections This leaflet provides information on local steroid injections and will answer any questions you have about the treatment. Arthritis Research
Drug information Local steroid injections Local steroid injections This leaflet provides information on local steroid injections and will answer any questions you have about the treatment. Arthritis Research
Graft Versus Host Disease:
 Graft Versus Host Disease: GvHD Information for young people having a donor stem cell transplant, and their families Children s Cancer and Leukaemia Group - www.cclg.org.uk Edited by Julie Guest, on behalf
Graft Versus Host Disease: GvHD Information for young people having a donor stem cell transplant, and their families Children s Cancer and Leukaemia Group - www.cclg.org.uk Edited by Julie Guest, on behalf
Department of Gynaecology Early medically induced termination of pregnancy. Information for patients
 Department of Gynaecology Early medically induced termination of pregnancy Information for patients Medically induced termination of pregnancy In this procedure the termination of pregnancy is brought
Department of Gynaecology Early medically induced termination of pregnancy Information for patients Medically induced termination of pregnancy In this procedure the termination of pregnancy is brought
AXIRON (AXE-e-RON) CIII
 Medication Guide 1 AXIRON (AXE-e-RON) CIII (testosterone) topical solution Read this Medication Guide before you start using AXIRON and each time you get a refill. There may be new information. This information
Medication Guide 1 AXIRON (AXE-e-RON) CIII (testosterone) topical solution Read this Medication Guide before you start using AXIRON and each time you get a refill. There may be new information. This information
JANUVIA sitagliptin phosphate 25 mg, 50 mg & 100 mg tablets
 JANUVIA sitagliptin phosphate 25 mg, 50 mg & 100 mg tablets What is in this leaflet This leaflet answers some common questions about JANUVIA. It does not contain all the available information. It does
JANUVIA sitagliptin phosphate 25 mg, 50 mg & 100 mg tablets What is in this leaflet This leaflet answers some common questions about JANUVIA. It does not contain all the available information. It does
Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer
 Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer Northern Centre for Cancer Care (NCCC) Freeman Hospital Introduction This leaflet has been written to
Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer Northern Centre for Cancer Care (NCCC) Freeman Hospital Introduction This leaflet has been written to
It can be devastating to be diagnosed with a cancer like multiple myeloma. But there are treatments that can help you live longer and feel better.
 Patient information from the BMJ Group It can be devastating to be diagnosed with a cancer like multiple myeloma. But there are treatments that can help you live longer and feel better. What is multiple
Patient information from the BMJ Group It can be devastating to be diagnosed with a cancer like multiple myeloma. But there are treatments that can help you live longer and feel better. What is multiple
Ruthenium Plaque Treatment
 Information for patients Department of Ophthalmology Royal Hallamshire Hospital Ruthenium Plaque Treatment What is Ruthenium Plaque treatment? This is a treatment whereby a plaque is surgically placed
Information for patients Department of Ophthalmology Royal Hallamshire Hospital Ruthenium Plaque Treatment What is Ruthenium Plaque treatment? This is a treatment whereby a plaque is surgically placed
Sofosbuvir, Pegylated Interferon and Ribavirin for the Treatment of Hepatitis C
 Sofosbuvir, Pegylated Interferon and Ribavirin for the Treatment of Hepatitis C Department of Hepatology Digestive Diseases Centre Patient Information This leaflet is designed to give you important information
Sofosbuvir, Pegylated Interferon and Ribavirin for the Treatment of Hepatitis C Department of Hepatology Digestive Diseases Centre Patient Information This leaflet is designed to give you important information
Psoriatic Arthritis. What is psoriatic arthritis? Understanding joints. Who gets psoriatic arthritis? Page 1 of 5
 Page 1 of 5 Psoriatic Arthritis Psoriatic arthritis causes inflammation, pain, and swelling of joints in some people who have psoriasis. Other parts of the body may also be affected. For example, in many
Page 1 of 5 Psoriatic Arthritis Psoriatic arthritis causes inflammation, pain, and swelling of joints in some people who have psoriasis. Other parts of the body may also be affected. For example, in many
The Menopause and Subtotal Hysterectomy
 Oxford University Hospitals NHS Trust Women s Health The Menopause and Subtotal Hysterectomy Information for patients The menopause At the menopause the ovaries stop working. This means that the female
Oxford University Hospitals NHS Trust Women s Health The Menopause and Subtotal Hysterectomy Information for patients The menopause At the menopause the ovaries stop working. This means that the female
