Emergency Neurological Life Support: Approach to the Patient with Coma
|
|
|
- Branden Morris
- 10 years ago
- Views:
Transcription
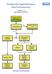
1 DOI /s REVIEW ARTICLE Emergency Neurological Life Support: Approach to the Patient with Coma J. Stephen Huff Robert D. Stevens Scott D. Weingart Wade S. Smith Ó Neurocritical Care Society 2012 Abstract Coma is an acute failure of neuronal systems governing arousal and awareness and represents a neurological emergency. When encountering a comatose patient, the clinician must have an organized approach to detect easily remedial causes, prevent ongoing neurologic injury, and determine a hierarchy of diagnostic tests, treatments, and neuromonitoring. Coma was chosen as an Emergency Neurological Life Support (ENLS) protocol because timely medical and surgical interventions can be life-saving, and the initial work-up of such patients is critical to establishing a correct diagnosis. Keywords Coma Herniation Osmolar therapy Mannitol Hypertonic saline J. S. Huff (&) Departments of Emergency Medicine and Neurology, University of Virginia School of Medicine, Charlottesville, VA, USA [email protected] R. D. Stevens Departments of Anesthesiology and Critical Care Medicine, Neurology, Neurosurgery, and Radiology, Johns Hopkins University School of Medicine, Baltimore, MD, USA S. D. Weingart Division of ED Critical Care, Mount Sinai School of Medicine, New York, NY, USA W. S. Smith Department of Neurology, University of California, San Francisco, San Francisco, CA, USA [email protected] Introduction Coma is characterized by the absence of arousal (wakefulness, vigilance) and of awareness of self and environment [1]. Comatose patients have closed eyes, do not speak, and do not arouse to verbal, tactile, or noxious stimulus. Some causes of coma are readily identified while others may require extensive testing to discover an etiology. Diagnostic and therapeutic steps should occur simultaneously. An organized and sequential plan can form the basis for discovering common causes of unresponsiveness and prioritizing studies for less common causes of coma [2]. The Emergency Neurological Life Support (ENLS) suggested algorithm for the initial management of coma is shown in Fig. 1. Suggested items to complete within the first hour of evaluating a patient with coma are shown in Table 1. Unresponsive Patient Coma may be operationally defined as an eyes-closed state with reflexive, non-purposeful or absent responsiveness to environmental stimuli. The examiner determines the level of responsiveness with stimuli of increasing intensity. A verbal cue, such as Are you OK? or What is your name?, may be used first. Other auditory stimuli may include a handclap or other loud noises. Escalation of stimulation with tactile stimulation of body parts that have large cortical representations, such as the face, follow if needed. If there is no clear response with these approaches, noxious stimuli may be applied that should be intense but not cause tissue injury. Recommended maneuvers include
2 over his or her face, is released. In a conscious patient without motor deficits, the falling arm will be moved and not contact the face. ABCs and C-Spine The unconscious patient s airway, breathing and circulation should be quickly assessed and concurrently treated (see the Airway, Ventilation, and Sedation protocol). Ensuring patency of the airway is an overriding initial priority to allow oxygenation and ventilation. The patient s cervical spine should be immobilized if there is a possibility of injury. A rapid initial survey should follow, looking for injury or other notable physical findings of the head and neck, chest, abdomen, and extremities. Intravenous (IV) access should be established quickly. Bedside blood glucose testing should be performed in all unconscious patients. If the blood glucose is <70 mg/dl, 50 ml of 50 % dextrose should be administered intravenously. Thiamine (100 mg) should be given intravenously with the dextrose in patients at risk for nutritional deficiency (e.g., chronic ethanol users, bariatric surgery patients, patients with malabsorption states). If there is clinical suspicion of opioid toxicity (e.g., history of illicit drug use, apnea or bradypnea, small pupils), naloxone mg IV should be administered and repeated as needed, up to 4 mg. Other antidotes, such as physostigmine, may be administered for anticholinergic toxicity in selected patients. Fig. 1 ENLS coma protocol Table 1 Coma checklist for the first hour ABCs and C-spine Blood sugar Consider narcotic overdose Chemistries, ABG, urine toxicology screen Head CT if presumed structural etiology or uncertain sternal rub, nail bed pressure, pressure applied to the supraorbital ridge, or pressure to the posterior aspect of the mandibular ramus. There is no evidence to support one maneuver over another. An attempt by the examiner to open the eyelids of the patient is a simple test. Resistance by the patient to eyelid opening that increases with increasing effort by the examiner suggests a feigned or functional etiology of unresponsiveness. Another test of the veracity of unresponsiveness is arm-dropping; the patient s arm, suspended General and Neurologic Assessment A general physical examination should be performed, including assessment of vital signs. If hypotension is present, the cause should be pursued while fluid repletion is started. Blood pressure elevation in the comatose patient may be a sign of an underlying life-threatening process, such as intracranial hypertension or stroke, which must be identified and treated. Recommendations for the management of blood pressure in stroke are discussed in the Ischemic Stroke protocol and in published guidelines [3]. A search for signs of trauma and other conditions that might require emergent surgical management are central goals of the initial survey. The symmetry or focal nature of neurological findings is a critical differentiating characteristic in coma assessment. Asymmetric findings on physical examination suggest a focal brain lesion or disturbance. Unconscious patients with a unilateral dilated un-reactive pupil, asymmetric eye movements, or asymmetric motor responses should be rapidly evaluated with imaging to identify a potential herniation syndrome or stroke.
3 Symmetric posturing, either extensor ( decerebrate ) or flexor ( decorticate ), may occur in either structural or metabolic coma. Generalized or symmetric findings raise the possibility of a toxic or metabolic process, or a lesion involving brainstem or diencephalic arousal centers is a possibility. Psychoactive and anti-epileptic drugs have been associated with depressed vestibulo-ocular responses. The neurological assessment of the unconscious patient has four parts [1]: level of consciousness, brainstem assessment, and assessment of motor and breathing patterns. Arousal is assessed by looking for spontaneous opening of the eyes, visual fixation or visual pursuit (tracking), and spontaneous and purposeful movements of the extremities. The level of consciousness can be expressed quantitatively by the Glasgow Coma Scale (GCS) (see Table 2)[4]. The GCS is most valuable for trending sequential examination responses of a particular patient. However, the GCS has many limitations, as it does not account for alterations in brainstem function, hemiparesis, or aphasia. Moreover, patients with identical total GCS scores may have very different clinical presentations due to different combinations in the motor, visual, and eye sub-scores. Therefore, recording the total score and sub-scores is recommended. The Full Outline of Unresponsiveness (FOUR) score incorporates more detailed information on brainstem responses and has been validated in a variety of clinical settings [5, 6]. Testing of cranial nerves is valuable to assess the afferent limb of the reflex; brainstem nuclei and interconnections; and efferent tracts [2]. Brainstem responses include pupils (size, reactivity, and symmetry should be determined in all cases), corneal reflex, visual threat response, oculocephalic reflex (Doll s eyes assessment only if no suspicion of cervical trauma or instability), vestibulo-ocular reflex (cold caloric testing), gag reflex, and cough reflex. Pinpoint pupils are suggestive of pontine damage, usually from hemorrhage or infarction. Enlarged and un-reactive pupils suggest damage to the midbrain or focal compression of the third nerve. Spontaneously roving eyes suggest cortical depression and an intact brainstem. Skew or dysconjugate resting gaze may occur with structural or metabolic processes. Jerky, nystagmoid movement may indicate non-convulsive status epilepticus. Fundoscopy may reveal retinal hemorrhages or papilledema, suggesting elevated intracranial pressure. Cold caloric testing should only be performed after disease or trauma to the external auditory canal and tympanum have been ruled out. This is a reflex arc involving cranial nerve VIII, medial longitudinal fasciculus, parapontine reticular formation (pons), frontal eye field projections, and the efferent motor neurons of cranial nerves III and VI. In the comatose patient with functioning Table 2 Glasgow coma scale (GCS) Eye opening Spontaneous 4 To speech 3 To pain 2 No response 1 Best motor response Obeys 6 Localizes 5 Withdraws 4 Abnormal flexion 3 Abnormal extension 2 No response 1 Best verbal response Oriented 5 Confused conversation 4 Inappropriate words 3 Incomprehensible sounds 2 No response 1 GCS range 3 15 brainstem, afferent (VIII), and efferent (III, VI) cranial nerves, the response is that of tonic deviation of both eyes toward the side of cold irrigation. An asymmetric caloric response is consistent with a structural abnormality. Nystagmus is not seen in the comatose patient. In the patient who is awake, a rapid corrective eye deflection in the direction away from the stimulus, mediated via the frontal eye fields, is observed. Caloric testing may be helpful to unmask pseudocoma or psychogenic coma; presence of the corrective eye deflection is suggestive of wakefulness. Motor function is assessed by observing any spontaneous movements or posturing, the motor response to verbal command, and the response to noxious stimulation. Muscle tone of the extremities may be assessed by passive movement of the limbs. The examiner should distinguish purposeful from reflex activity. Examples of purposeful activity include following of commands, pushing the examiner away, reaching for the tracheal tube, or localizing to noxious stimulation. Examples of reflexive activity include withdrawal, or abnormal flexion or extensor posturing to noxious stimulation. Deep tendon and cutaneous reflexes should be performed with particular attention to briskness and symmetry of findings. Breathing patterns may have localizing value: after airway assessment and stabilization, breathing patterns observed may include central neurogenic hyperventilation from lesions of the pons or midbrain, or cluster (Biot s) breathing from lesions of the pons. Medullary lesions are suggested by the absence of spontaneous breathing or ataxic breathing.
4 Following this initial assessment, unconscious patients should be triaged into likely structural or toxic metabolic causes of coma a critical early distinction, since structural coma may require emergent surgical intervention and/ or invasive neuromonitoring (see Tables 3, 4). Focused History/PMH Historical information, elicited from witnesses, friends, family, co-workers, or emergency medical services (EMS) personnel, will often suggest the cause of coma. EMS personnel may have valuable details about the circumstances in which the patient was found, since they are trained to perform brief information gathering, including a quick search for pill bottles and any suicide notes, at the scene. The time course of the alteration in consciousness may be helpful in suggesting an etiology. An abrupt onset of symptoms suggests a stroke, seizure, or a cardiac event with impaired cerebral perfusion. A more gradual onset of coma suggests a metabolic or possibly infectious process. Past medical, surgical, and psychiatric history; alcohol or Table 3 Neurologic etiologies of coma Trauma Subdural hematoma Epidural hematoma Parenchymal hemorrhages Diffuse axonal injury Cardiovascular Intracerebral hemorrhage Subarachnoid hemorrhage Ischemic stroke Anoxic-ischemic encephalopathy CNS infections Meningitis Encephalitis Abscess Neuroinflammatory disorders Acute disseminated encephalomyelitis Autoimmune encephalitis Neoplasms Metastatic Primary CNS Carcinomatous meningitis Seizures Non-convulsive status epilepticus Postictal state Other Posterior reversible encephalopathy syndrome Osmotic demylenation syndrome illicit drug use history; and any environmental toxic exposures should be included in information gathering. Medication history is paramount; not only may this suggest a possibility of overdose, but current medications provide valuable clues to the medical history in the absence of any detailed information. The electronic medical record may provide rapid access to the patient s past medical history if the patient can be reliably identified. Stat Labs Unless a readily reversible cause of unresponsiveness, such as hypoglycemia, has been discovered and corrected, additional laboratory work should be obtained. Serum chemistries, basic hematological panel, and blood gas analysis should be considered, as well as co-oximetry in selected patents. Toxicologic testing, such as ethanol level and urine toxicology screen, should be obtained (note that some toxins which cause unconsciousness are not detectable in common toxicologic screens, and that substances tested for in toxicologic screens vary among institutions). Microbiologic studies, including cultures of blood and urine may be helpful. Initial Formulation: Structural, Non-Structural, or Unclear Causes of Coma The differential diagnosis of coma is broad. Information obtained with initial stabilization, general physical examination, neurological assessment, focused history, and stat laboratory results will typically allow sorting of patients into likely structural or non-structural causes of coma and suggest whether and what additional testing is needed. If there is any concern for a structural etiology of coma, or if the cause of coma cannot be identified after initial assessment, cranial computed tomography (CT) should be sought immediately. Brain Imaging Non-contrast cranial CT should be obtained emergently in unconscious patients with presumed structural cause of coma and in patients with an unclear cause of coma after initial assessment. CT allows discovery of potential causes such as focal hypodensity suggestive of a cerebral infarct; intracranial hemorrhage; brain mass; brain edema; and acute hydrocephalus. If acute ischemic stroke is being considered, CT angiography and CT perfusion can provide valuable information on the cerebral vasculature and regional perfusion. Non-contrast CT imaging in the hyperacute phase of ischemic stroke is often normal; in this setting, clinical diagnosis of stroke is still valid. Ischemic stroke does not
5 Table 4 Toxic metabolic etiologies of coma Metabolic encephalopathies Hypoglycemia Hypoxia, hypercapnia Diabetic ketoacidosis; hyperosmolar non-ketotic hyperglycemia Hepatic encephalopathy Uremia Hyponatremia Hypernatremia Myxedema Adrenal failure Hypercalcemia Wernicke s disease Sepsis Drug/medication overdose Drugs of abuse (opioids, alcohol, methanol, ethylene glycol, amphetamines, cocaine) Sedative-hypnotics Narcotics Aspirin Acetaminophen SSRI Tricyclic antidepressants Antipsychotics Carbon monoxide Anticonvulsants Environmental causes Heat stroke Hypothermia Carbon monoxide typically cause coma acutely unless it occurs within arousal systems located in the brainstem or diencephalon (e.g., basilar artery thrombosis); sub-acutely, coma may develop due to progression of a hemispheric infarct with transtentorial herniation. When a central nervous system (CNS) infection is being considered, cranial CT with and without contrast may be ordered to evaluate for abscess, extra-axial fluid collections, hydrocephalus, hemorrhagic changes, and infarctions prior to lumbar puncture and cerebrospinal fluid analysis. Non-structural Coma Common non-structural causes of coma include anoxicischemic encephalopathy, seizures, metabolic alterations, endocrinopathies, systemic infections, CNS infections, overdose of medications, illicit drug and alcohol use, and exposure to toxins (Table 4). Treatment is guided by the underlying etiology. Where appropriate, specific antagonists or antidotes should be administered. For example, the opioid toxidrome should prompt administration of naloxone as discussed in the ABCs and C-Spine section above. Acetaminophen ingestion is treated with N-acetylcysteine. In some cases, a metabolic encephalopathy may evolve toward a structural process, such as such as acute liver failure leading to cerebral edema and herniation. In patients with new seizures or change in seizure pattern, a structural cause must be carefully searched for with CT and magnetic resonance imaging (MRI) if the CT is negative. CNS infections, such as bacterial meningitis, may have no structural correlation present on contrast CT scan (though the test should be obtained to exclude brain abscess). Where there is high suspicion of acute bacterial meningitis, appropriate antibiotics and dexamethasone should be administered before CT and lumbar puncture. Persisting Uncertainty If diagnostic uncertainty persists after initial diagnostic steps, non-contrast CT scan should be obtained. Lumbar puncture is performed if there is suspicion of CNS infection, inflammation, or complications of lymphoma or other cancers. In addition, when there is clinical suspicion of subarachnoid hemorrhage, lumbar puncture should be obtained if the CT is negative for subarachnoid hemorrhage. MRI is obtained if there is a presumption of hyperacute ischemic stroke or when the cause of coma is not explained by other tests. A few less common causes of coma deserve special mention. Non-convulsive status epilepticus may be suspected if there is a seizure history or if a seizure was observed in the clinical course. There may be subtle physical examination findings, such as an eyelid twitch or finger movement, but the patient does not have tonic clonic activity. In these cases, EEG is required for diagnosis. Cerebellar hemorrhage may cause rapid unresponsiveness from brainstem compression. A history of sudden headache followed by inability to walk, or severe nausea and vomiting, may be key to diagnosis. Non-contrast CT is diagnostic. Ischemic stroke involving the basilar artery may produce sudden unresponsiveness [7]. Abnormal eye findings may be present on examination. CT-angiography may reveal the basilar clot, and the non-contrast CT may show a hyperdense basilar artery. Communication When communicating to an accepting or referring physician about this patient, consider including the key elements listed in Table 5.
6 Table 5 Coma communication regarding assessment and referral Coma communication regarding assessment and referral Clinical presentation Relevant PMH/PSH Neurological exam Brain imaging, LP, or EEG results (if available) Treatments administered so far References 1. Plum F, Posner JB. The diagnosis of stupor and coma. 3rd ed. Philadelphia: F. A. Davis Co; Stevens RD, Bhardwaj A. Approach to the comatose patient. Crit Care Med. 2006;34: Adams HP Jr, del Zoppo G, Alberts MJ, et al. Guidelines for the early management of adults with ischemic stroke: a guideline from the American Heart Association/American Stroke Association Stroke Council, Clinical Cardiology Council, Cardiovascular Radiology and Intervention Council, and the Atherosclerotic Peripheral Vascular Disease and Quality of Care Outcomes in Research Interdisciplinary Working Groups: The American Academy of Neurology affirms the value of this guideline as an educational tool for neurologists. Circulation. 2007;115:e Teasdale G, Jennett B. Assessment of coma and impaired consciousness. A practical scale. Lancet. 1974;2: Wijdicks EF, Rabinstein AA, Bamlet WR, Mandrekar JN. FOUR score and Glasgow Coma Scale in predicting outcome of comatose patients: a pooled analysis. Neurology. 2011;77: Wijdicks EF, Bamlet WR, Maramattom BV, Manno EM, McClelland RL. Validation of a new coma scale: the FOUR score. Ann Neurol. 2005;58: Ferbert A, Bruckmann H, Drummen R. Clinical features of proven basilar artery occlusion. Stroke. 1990;21:
The Clinical Evaluation of the Comatose Patient in the Emergency Department
 The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
Neurology Clerkship Learning Objectives
 Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
Neurology Clerkship Learning Objectives Clinical skills Perform a neurological screening examination of the cranial nerves, motor system, reflexes, and sensory system under the observation and guidance
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]
![SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]](/thumbs/27/9667060.jpg) SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
Coma and Brain Death (Dr. Merchut) Coma. 1. Clinical features of coma
 Coma and Brain Death (Dr. Merchut) Coma 1. Clinical features of coma Coma is defined as a sleep-like, unarousable, unresponsive state. Other patients with impaired consciousness but some limited degree
Coma and Brain Death (Dr. Merchut) Coma 1. Clinical features of coma Coma is defined as a sleep-like, unarousable, unresponsive state. Other patients with impaired consciousness but some limited degree
PE finding: Left side extremities mild weakness No traumatic wound No bloody otorrhea, nor rhinorrhea
 Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
TRAUMATIC BRAIN INJURY (TBI)
 Background: Traumatic Brain Injury (TBI) is one of the leading causes of trauma related disability and death in the U.S. TBIs can occur as either blunt, penetrating, or a combination of both depending
Background: Traumatic Brain Injury (TBI) is one of the leading causes of trauma related disability and death in the U.S. TBIs can occur as either blunt, penetrating, or a combination of both depending
DIAGNOSTIC CRITERIA OF STROKE
 DIAGNOSTIC CRITERIA OF STROKE Diagnostic criteria are used to validate clinical diagnoses. Here below MONICA diagnostic criteria are reported. MONICA - MONItoring trends and determinants of CArdiovascular
DIAGNOSTIC CRITERIA OF STROKE Diagnostic criteria are used to validate clinical diagnoses. Here below MONICA diagnostic criteria are reported. MONICA - MONItoring trends and determinants of CArdiovascular
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease.
 Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Overview. Geriatric Overview. Chapter 26. Geriatrics 9/11/2012
 Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Types of Brain Injury
 Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
Diabetic Emergencies. David Hill, D.O.
 Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Acute Myocardial Infarction (the formulary thrombolytic for AMI at AAMC is TNK, please see the TNK monograph in this manual for information)
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
Practice Guideline. Neuropsychological Evaluations
 Practice Guideline Neuropsychological Evaluations Adapted from the practice guideline of the same name by the Arizona Department of Health Services Division of Behavioral Health Services Effective: 06/30/2006
Practice Guideline Neuropsychological Evaluations Adapted from the practice guideline of the same name by the Arizona Department of Health Services Division of Behavioral Health Services Effective: 06/30/2006
Diabetes Expert Witness on: Diabetic Hypoglycemia in Nursing Homes
 Diabetes Expert Witness on: Diabetic Hypoglycemia in Nursing Homes Nursing home patients with diabetes treated with insulin and certain oral diabetes medications (i.e. sulfonylureas and glitinides) are
Diabetes Expert Witness on: Diabetic Hypoglycemia in Nursing Homes Nursing home patients with diabetes treated with insulin and certain oral diabetes medications (i.e. sulfonylureas and glitinides) are
75-09.1-08-02. Program criteria. A social detoxi cation program must provide:
 CHAPTER 75-09.1-08 SOCIAL DETOXIFICATION ASAM LEVEL III.2-D Section 75-09.1-08-01 De nitions 75-09.1-08-02 Program Criteria 75-09.1-08-03 Provider Criteria 75-09.1-08-04 Admission and Continued Stay Criteria
CHAPTER 75-09.1-08 SOCIAL DETOXIFICATION ASAM LEVEL III.2-D Section 75-09.1-08-01 De nitions 75-09.1-08-02 Program Criteria 75-09.1-08-03 Provider Criteria 75-09.1-08-04 Admission and Continued Stay Criteria
Headache: Differential diagnosis and Evaluation. Raymond Rios PGY-1 Pediatrics
 Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Headache: Differential diagnosis and Evaluation Raymond Rios PGY-1 Pediatrics You are evaluating a 9 year old male patient at the ED brought by his mother, who says that her son has had a fever, cough,
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Interval: [ ] Baseline [ ] 2 hours post treatment [ ] 24 hours post onset of symptoms ±20 minutes [ ] 7-10 days [ ] 3 months [ ] Other ( )
![Interval: [ ] Baseline [ ] 2 hours post treatment [ ] 24 hours post onset of symptoms ±20 minutes [ ] 7-10 days [ ] 3 months [ ] Other ( ) Interval: [ ] Baseline [ ] 2 hours post treatment [ ] 24 hours post onset of symptoms ±20 minutes [ ] 7-10 days [ ] 3 months [ ] Other ( )](/thumbs/29/13263233.jpg) Patient Identification. - - Pt. Date of Birth / / Hospital ( - ) Date of Exam / / Interval: [ ] Baseline [ ] 2 hours post treatment [ ] 24 hours post onset of symptoms ±20 minutes [ ] 7-10 days [ ] 3 months
Patient Identification. - - Pt. Date of Birth / / Hospital ( - ) Date of Exam / / Interval: [ ] Baseline [ ] 2 hours post treatment [ ] 24 hours post onset of symptoms ±20 minutes [ ] 7-10 days [ ] 3 months
Update on Therapeutics in Neurology Evaluation Tabulation
 Update on Therapeutics in Neurology Evaluation Tabulation June 23, 2011 Georgetown, Washington, D.C. I am a: What was your overall rating of the faculty Jeffrey Frank, MD? The learning objectives designated
Update on Therapeutics in Neurology Evaluation Tabulation June 23, 2011 Georgetown, Washington, D.C. I am a: What was your overall rating of the faculty Jeffrey Frank, MD? The learning objectives designated
Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy
 Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy Emily S. Birkholz, MD, and Michael Wall, MD December 30, 2009 CC: 44 year old male with diplopia HPI: This 44 year old man with a history
Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy Emily S. Birkholz, MD, and Michael Wall, MD December 30, 2009 CC: 44 year old male with diplopia HPI: This 44 year old man with a history
Examination Approach. Case 1: Mental Status. Examination Approach. The Neurological Exam In the ICU: High Yield Techniques 5/30/2013
 The Neurological Exam In the ICU: High Yield Techniques S. Andrew Josephson MD Carmen Castro-Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Vice Chairman, Parnassus Programs
The Neurological Exam In the ICU: High Yield Techniques S. Andrew Josephson MD Carmen Castro-Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Vice Chairman, Parnassus Programs
Traumatic Head Injuries
 Traumatic Brain Injury (TBI) Traumatic Head Injuries Major contributing cause of trauma deaths Many survivors have permanent disability Commonly occurs in young adults (mostly males) Spokane County EMS
Traumatic Brain Injury (TBI) Traumatic Head Injuries Major contributing cause of trauma deaths Many survivors have permanent disability Commonly occurs in young adults (mostly males) Spokane County EMS
Common Questions and Answers About Severe Brain Injury
 Common Questions and Answers About Severe Brain Injury What you should know about severe brain injuries The purpose of this publication is to provide you with information about severe brain injuries. Such
Common Questions and Answers About Severe Brain Injury What you should know about severe brain injuries The purpose of this publication is to provide you with information about severe brain injuries. Such
APPROACH TO THE CHILD WITH A SEIZURE
 APPROACH TO THE CHILD WITH A SEIZURE 1. Background... 1 2. Questions to ask... 1 a) Pre-ictal... 2 b) Ictal... 2 c) Post-ictal... 2 d) Other questions to ask... 2 3. Diagnosis... 3 a) Clinical categories...
APPROACH TO THE CHILD WITH A SEIZURE 1. Background... 1 2. Questions to ask... 1 a) Pre-ictal... 2 b) Ictal... 2 c) Post-ictal... 2 d) Other questions to ask... 2 3. Diagnosis... 3 a) Clinical categories...
REHABILITATION STANDARD: COMMUNICATION
 REHABILITATION STANDARD: COMMUNICATION Residents of Vancouver Island Health Authority (VIHA) will have reasonable access to consistent, integrated, measurable, evidence based rehabilitation services. This
REHABILITATION STANDARD: COMMUNICATION Residents of Vancouver Island Health Authority (VIHA) will have reasonable access to consistent, integrated, measurable, evidence based rehabilitation services. This
What Medical Emergencies Should a Dental Office be Prepared to Handle?
 What Medical Emergencies Should a Dental Office be Prepared to Handle? Gary Cuttrell, DDS, JD, University of NM Division of Dental Services Santiago Macias, MD, First Choice Community Healthcare Dentists
What Medical Emergencies Should a Dental Office be Prepared to Handle? Gary Cuttrell, DDS, JD, University of NM Division of Dental Services Santiago Macias, MD, First Choice Community Healthcare Dentists
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Level III Stroke Center Data Collection Requirements
 Who? Level III Stroke Center Data Collection Requirements All LERN Level III Stroke Centers. LERN Level I and II Stroke Centers have reporting requirements to The Joint Commission or other Board approved
Who? Level III Stroke Center Data Collection Requirements All LERN Level III Stroke Centers. LERN Level I and II Stroke Centers have reporting requirements to The Joint Commission or other Board approved
Practice Protocol. Neuropsychological Evaluations
 Practice Protocol Neuropsychological Evaluations Jointly Developed by the Arizona Department of Health Services/Division of Behavioral Health Services and AHCCCS/Health Plans Effective June 30, 2006 Revised
Practice Protocol Neuropsychological Evaluations Jointly Developed by the Arizona Department of Health Services/Division of Behavioral Health Services and AHCCCS/Health Plans Effective June 30, 2006 Revised
Developing a Dynamic Team Approach to Stroke Care. Emergency Medical Services 2015
 Developing a Dynamic Team Approach to Stroke Care Emergency Medical Services 2015 Why Stroke, Why now? A recent study showed that 80 percent of people in the United States live within an hour s drive of
Developing a Dynamic Team Approach to Stroke Care Emergency Medical Services 2015 Why Stroke, Why now? A recent study showed that 80 percent of people in the United States live within an hour s drive of
Adult CCRN/CCRN E/CCRN K Certification Review Course: Endocrine 12/2015. Endocrine 1. Disclosures. Nothing to disclose
 Adult CCRN/CCRN E/CCRN K Certification Review Course: Carol Rauen RN BC, MS, PCCN, CCRN, CEN Disclosures Nothing to disclose 1 Body Harmony disorders and emergencies Body Harmony (cont) Introduction Disorders
Adult CCRN/CCRN E/CCRN K Certification Review Course: Carol Rauen RN BC, MS, PCCN, CCRN, CEN Disclosures Nothing to disclose 1 Body Harmony disorders and emergencies Body Harmony (cont) Introduction Disorders
NEUROLOCALIZATION MADE EASY
 NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
NEUROLOGICAL ASSESSMENT
 Components of a Neurological Assessment: 1. Interview 2. Level of Consciousness 3. Pupillary Assessment 4. Cranial Nerve Testing 5. Vital signs 6. Motor Function 7. Sensory Function 8. Tone 9. Cerebral
Components of a Neurological Assessment: 1. Interview 2. Level of Consciousness 3. Pupillary Assessment 4. Cranial Nerve Testing 5. Vital signs 6. Motor Function 7. Sensory Function 8. Tone 9. Cerebral
Diuretics: You may get diuretic medicine to help decrease swelling in your brain. This may help your brain get better blood flow.
 Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
TYPE OF INJURY and CURRENT SABS Paraplegia/ Tetraplegia
 Paraplegia/ Tetraplegia (a) paraplegia or quadriplegia; (a) paraplegia or tetraplegia that meets the following criteria i and ii, and either iii or iv: i. ii. iii i. The Insured Person is currently participating
Paraplegia/ Tetraplegia (a) paraplegia or quadriplegia; (a) paraplegia or tetraplegia that meets the following criteria i and ii, and either iii or iv: i. ii. iii i. The Insured Person is currently participating
Emergency Neurological Life Support. Spinal Cord Compression. Version: 1.0 Last Updated: 8/3/2014. Checklist & Communication
 Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
1. According to recent US national estimates, which of the following substances is associated
 1 Chapter 36. Substance-Related, Self-Assessment Questions 1. According to recent US national estimates, which of the following substances is associated with the highest incidence of new drug initiates
1 Chapter 36. Substance-Related, Self-Assessment Questions 1. According to recent US national estimates, which of the following substances is associated with the highest incidence of new drug initiates
Chapter 7: The Nervous System
 Chapter 7: The Nervous System I. Organization of the Nervous System Objectives: List the general functions of the nervous system Explain the structural and functional classifications of the nervous system
Chapter 7: The Nervous System I. Organization of the Nervous System Objectives: List the general functions of the nervous system Explain the structural and functional classifications of the nervous system
Defining and classifying syncope. Clinical Autonomic Research 2004;14 (Suppl 1): 4 8
 Defining and classifying syncope Roland D. Thijs, 1 Wouter Wieling, 2 Horacio Kaufmann, 3 J. Gert van Dijk 1 Clinical Autonomic Research 2004;14 (Suppl 1): 4 8 [1] Department of Neurology and Clinical
Defining and classifying syncope Roland D. Thijs, 1 Wouter Wieling, 2 Horacio Kaufmann, 3 J. Gert van Dijk 1 Clinical Autonomic Research 2004;14 (Suppl 1): 4 8 [1] Department of Neurology and Clinical
Is this pt s brain dysfunction due to ischemia? Onset & progression of sx; location of deficit
 CEREBROVASCULAR ACCIDENTS & TIA s Maggie Kelly History: Onset of symptoms exact time Previous sxs suggestive of TIA s Progression of symptoms Headache? Medications Past history of CVA, clotting events
CEREBROVASCULAR ACCIDENTS & TIA s Maggie Kelly History: Onset of symptoms exact time Previous sxs suggestive of TIA s Progression of symptoms Headache? Medications Past history of CVA, clotting events
LIMITED BENEFIT HEALTH COVERAGE FOR SPECIFIED CRITICAL ILLNESS. OUTLINE OF COVERAGE (Applicable to Policy Form CI-1.0-NC)
 COLONIAL LIFE & ACCIDENT INSURANCE COMPANY 1200 Colonial Life Boulevard, P.O. Box 1365, Columbia, South Carolina 29202 1.800.325.4368 www.coloniallife.com A Stock Company LIMITED BENEFIT HEALTH COVERAGE
COLONIAL LIFE & ACCIDENT INSURANCE COMPANY 1200 Colonial Life Boulevard, P.O. Box 1365, Columbia, South Carolina 29202 1.800.325.4368 www.coloniallife.com A Stock Company LIMITED BENEFIT HEALTH COVERAGE
LECTURE 16 NEUROPATHOPHYSIOLOGY (HEAD INJURY)
 LECTURE 16 Copyright 2000 by Bowman O. Davis, Jr. The approach and organization of this material was developed by Bowman O. Davis, Jr. for specific use in online instruction. All rights reserved. No part
LECTURE 16 Copyright 2000 by Bowman O. Davis, Jr. The approach and organization of this material was developed by Bowman O. Davis, Jr. for specific use in online instruction. All rights reserved. No part
Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
 Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Epilepsy 101: Getting Started
 American Epilepsy Society 1 Epilepsy 101 for nurses has been developed by the American Epilepsy Society to prepare professional nurses to understand the general issues, concerns and needs of people with
American Epilepsy Society 1 Epilepsy 101 for nurses has been developed by the American Epilepsy Society to prepare professional nurses to understand the general issues, concerns and needs of people with
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE
 STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STATEMENT OF STANDARD
 OHSU HEALTH CARE SYSTEM PRACTICE STANDARD Acute Stroke Practice Standard for the Emergency Department (includes ischemic stroke, TIAs, intracerebral hemorrhage, and non-subarachnoid hemorrhage), PS 01.11
OHSU HEALTH CARE SYSTEM PRACTICE STANDARD Acute Stroke Practice Standard for the Emergency Department (includes ischemic stroke, TIAs, intracerebral hemorrhage, and non-subarachnoid hemorrhage), PS 01.11
Approved: Acute Stroke Ready Hospital Advanced Certification Program
 Approved: Acute Stroke Ready Hospital Advanced Certification Program The Joint Commission recently developed a new Disease- Specific Care Advanced Certification program for Acute Stroke Ready Hospitals
Approved: Acute Stroke Ready Hospital Advanced Certification Program The Joint Commission recently developed a new Disease- Specific Care Advanced Certification program for Acute Stroke Ready Hospitals
PHSW Procedural Sedation Post-Test Answer Key. For the following questions, circle the letter of the correct answer(s) or the word true or false.
 PHSW Procedural Sedation Post-Test Answer Key 1 1. Define Procedural (Conscious) Sedation: A medically controlled state of depressed consciousness where the patient retains the ability to continuously
PHSW Procedural Sedation Post-Test Answer Key 1 1. Define Procedural (Conscious) Sedation: A medically controlled state of depressed consciousness where the patient retains the ability to continuously
Master of Physician Assistant Studies Course Descriptions for Year I
 FALL TERM COURSES: Master of Physician Assistant Studies Course Descriptions for Year I PHAC 7230 Fundamentals in Pharmacology for Health Care I Credit Hrs: 3 This course will build on foundational knowledge
FALL TERM COURSES: Master of Physician Assistant Studies Course Descriptions for Year I PHAC 7230 Fundamentals in Pharmacology for Health Care I Credit Hrs: 3 This course will build on foundational knowledge
Functions of the Brain
 Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
ARTICLE #1 PLEASE RETURN AT THE END OF THE HOUR
 ARTICLE #1 PLEASE RETURN AT THE END OF THE HOUR Alcoholism By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/alcoholism/ds00340 Definition Alcoholism is a chronic and often progressive
ARTICLE #1 PLEASE RETURN AT THE END OF THE HOUR Alcoholism By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/alcoholism/ds00340 Definition Alcoholism is a chronic and often progressive
Discovery of an Aneurysm Following a Motorcycle Accident. Maya Babu, MSIII Gillian Lieberman, M.D.
 Discovery of an Aneurysm Following a Motorcycle Accident Maya Babu, MSIII Gillian Lieberman, M.D. Patient CC: July 2004 65 yo male transferred to the BI from an OSH s/p motorcycle crash w/o a helmet CC
Discovery of an Aneurysm Following a Motorcycle Accident Maya Babu, MSIII Gillian Lieberman, M.D. Patient CC: July 2004 65 yo male transferred to the BI from an OSH s/p motorcycle crash w/o a helmet CC
Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium
 Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium October 30, 2008 Barry Libman, RHIA, CCS, CCS-P President, Barry Libman Inc. Stroke Coding Issues Outline Medical record documentation
Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium October 30, 2008 Barry Libman, RHIA, CCS, CCS-P President, Barry Libman Inc. Stroke Coding Issues Outline Medical record documentation
What Is an Arteriovenous Malformation (AVM)?
 What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
Seizures (Convulsions, Status Epilepticus) in Dogs
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Seizures (Convulsions, Status Epilepticus) in Dogs Basics OVERVIEW Seizures are
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Seizures (Convulsions, Status Epilepticus) in Dogs Basics OVERVIEW Seizures are
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!!
 Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Short Communications. Alcoholic Intracerebral Hemorrhage
 Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
THE HISTORICAL EVOLUTION OF BRAIN DEATH FROM FORMER DEFINITIONS OF DEATH: THE HARVARD CRITERIA TO THE PRESENT *
 The Signs of Death Pontifical Academy of Sciences, Scripta Varia 110, Vatican City 2007 www.pas.va/content/dam/accademia/pdf/sv110/sv110-daroff.pdf THE HISTORICAL EVOLUTION OF BRAIN DEATH FROM FORMER DEFINITIONS
The Signs of Death Pontifical Academy of Sciences, Scripta Varia 110, Vatican City 2007 www.pas.va/content/dam/accademia/pdf/sv110/sv110-daroff.pdf THE HISTORICAL EVOLUTION OF BRAIN DEATH FROM FORMER DEFINITIONS
Dehydration & Overhydration. Waseem Jerjes
 Dehydration & Overhydration Waseem Jerjes Dehydration 3 Major Types Isotonic - Fluid has the same osmolarity as plasma Hypotonic -Fluid has fewer solutes than plasma Hypertonic-Fluid has more solutes than
Dehydration & Overhydration Waseem Jerjes Dehydration 3 Major Types Isotonic - Fluid has the same osmolarity as plasma Hypotonic -Fluid has fewer solutes than plasma Hypertonic-Fluid has more solutes than
About Brain Injury: A Guide to Brain Anatomy Information from http://www.waiting.com, 1997-2002, Becca, Ltd.
 About Brain Injury: A Guide to Brain Anatomy Information from http://www.waiting.com, 1997-2002, Becca, Ltd. Brain Anatomy Definitions Brainstem: The lower extension of the brain where it connects to the
About Brain Injury: A Guide to Brain Anatomy Information from http://www.waiting.com, 1997-2002, Becca, Ltd. Brain Anatomy Definitions Brainstem: The lower extension of the brain where it connects to the
Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both.
 Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
The Petrylaw Lawsuits Settlements and Injury Settlement Report
 The Petrylaw Lawsuits Settlements and Injury Settlement Report TRAUMATIC BRAIN INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Brain Injury Cases The Petrylaw Lawsuits Settlements
The Petrylaw Lawsuits Settlements and Injury Settlement Report TRAUMATIC BRAIN INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Brain Injury Cases The Petrylaw Lawsuits Settlements
Using the Pupillometer in Clinical Practice
 Using the Pupillometer in Clinical Practice Claude Hemphill MD M.A.S. [email protected] Kathy Johnson RN, MSN [email protected] Mary Kay Bader RN, MSN, CCNS [email protected] Pupillometry: How It
Using the Pupillometer in Clinical Practice Claude Hemphill MD M.A.S. [email protected] Kathy Johnson RN, MSN [email protected] Mary Kay Bader RN, MSN, CCNS [email protected] Pupillometry: How It
2011 Radiology Diagnosis Coding Update Questions and Answers
 2011 Radiology Diagnosis Coding Update Questions and Answers How can we subscribe to the Coding Clinic for ICD-9 guidelines and updates? The American Hospital Association publishes this quarterly newsletter.
2011 Radiology Diagnosis Coding Update Questions and Answers How can we subscribe to the Coding Clinic for ICD-9 guidelines and updates? The American Hospital Association publishes this quarterly newsletter.
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
The Lewin Group undertook the following steps to identify the guidelines relevant to the 11 targeted procedures:
 Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Reflex Physiology. Dr. Ali Ebneshahidi. 2009 Ebneshahidi
 Reflex Physiology Dr. Ali Ebneshahidi Reflex Physiology Reflexes are automatic, subconscious response to changes within or outside the body. a. Reflexes maintain homeostasis (autonomic reflexes) heart
Reflex Physiology Dr. Ali Ebneshahidi Reflex Physiology Reflexes are automatic, subconscious response to changes within or outside the body. a. Reflexes maintain homeostasis (autonomic reflexes) heart
PRACTICE PARAMETERS: ASSESSMENT AND MANAGEMENT OF PATIENTS IN THE PERSISTENT VEGETATIVE STATE. (Summary Statement)
 PRACTICE PARAMETERS: ASSESSMENT AND MANAGEMENT OF PATIENTS IN THE PERSISTENT VEGETATIVE STATE (Summary Statement) Report of the Quality Standards Subcommittee of the American Academy of Neurology Overview.
PRACTICE PARAMETERS: ASSESSMENT AND MANAGEMENT OF PATIENTS IN THE PERSISTENT VEGETATIVE STATE (Summary Statement) Report of the Quality Standards Subcommittee of the American Academy of Neurology Overview.
doi: 10.1016/j.jocn.2010.10.005
 doi: 10.1016/j.jocn.2010.10.005 A remote desktop-based telemedicine system Yasushi Shibata, MD, PhD Department of Neurosurgery, Mito Medical Center, University of Tsukuba Mito, Ibaraki, 310-0015, Japan
doi: 10.1016/j.jocn.2010.10.005 A remote desktop-based telemedicine system Yasushi Shibata, MD, PhD Department of Neurosurgery, Mito Medical Center, University of Tsukuba Mito, Ibaraki, 310-0015, Japan
STROKE INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. A commonly used term for stroke is cerebrovascular accident, typically shortened
STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. A commonly used term for stroke is cerebrovascular accident, typically shortened
Corporate Medical Policy
 File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
Acute Pancreatitis. Questionnaire. if yes: amount (cigarettes/day): since when (year): Drug consumption: yes / no if yes: type of drug:. amount:.
 The physical examination has to be done AT ADMISSION! The blood for laboratory parameters has to be drawn AT ADMISSION! This form has to be filled AT ADMISSION! Questionnaire Country: 1. Patient personal
The physical examination has to be done AT ADMISSION! The blood for laboratory parameters has to be drawn AT ADMISSION! This form has to be filled AT ADMISSION! Questionnaire Country: 1. Patient personal
Department of Veterans Affairs VHA DIRECTIVE 2011-038 Veterans Health Administration Washington, DC 20420 November 2, 2011
 Department of Veterans Affairs VHA DIRECTIVE 2011-038 Veterans Health Administration Washington, DC 20420 TREATMENT OF ACUTE ISCHEMIC STROKE (AIS) 1. PURPOSE: This Veterans Health Administration (VHA)
Department of Veterans Affairs VHA DIRECTIVE 2011-038 Veterans Health Administration Washington, DC 20420 TREATMENT OF ACUTE ISCHEMIC STROKE (AIS) 1. PURPOSE: This Veterans Health Administration (VHA)
Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents
 Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents Approved/ Revised Effective BLS Adult Nerve Agent/Organophosphate Poisoning Antidote
Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents Approved/ Revised Effective BLS Adult Nerve Agent/Organophosphate Poisoning Antidote
Emergencies Related to ETHANOL (ETOH) Alcohol
 University of Wisconsin Hospital and Clinics Emergency Education Center Emergencies Related to ETHANOL (ETOH) Alcohol Alcoholics are in all socio-economical levels of society ~ETOH is one of the most commonly
University of Wisconsin Hospital and Clinics Emergency Education Center Emergencies Related to ETHANOL (ETOH) Alcohol Alcoholics are in all socio-economical levels of society ~ETOH is one of the most commonly
Disability Evaluation Under Social Security
 Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
Implementing Medical Checkups to Prevent. Sports-Related Injuries and Disorders
 Sports-Related Injuries and Disorders Implementing Medical Checkups to Prevent Sports-Related Injuries and Disorders JMAJ 48(1): 1 5, 2005 Hideo MATSUMOTO*, Toshiro OTANI**, Hitoshi ABE*** and Yasunori
Sports-Related Injuries and Disorders Implementing Medical Checkups to Prevent Sports-Related Injuries and Disorders JMAJ 48(1): 1 5, 2005 Hideo MATSUMOTO*, Toshiro OTANI**, Hitoshi ABE*** and Yasunori
Delirium. The signs of delirium are managed by treating the underlying cause of the medical condition causing the delirium.
 Delirium Introduction Delirium is a complex symptom where a person becomes confused and shows significant changes in behavior and mental state. Signs of delirium include problems with attention and awareness,
Delirium Introduction Delirium is a complex symptom where a person becomes confused and shows significant changes in behavior and mental state. Signs of delirium include problems with attention and awareness,
Dallas Neurosurgical and Spine Associates, P.A Patient Health History
 Dallas Neurosurgical and Spine Associates, P.A Patient Health History DOB: Date: Reason for your visit (Chief complaint): Past Medical History Please check corresponding box if you have ever had any of
Dallas Neurosurgical and Spine Associates, P.A Patient Health History DOB: Date: Reason for your visit (Chief complaint): Past Medical History Please check corresponding box if you have ever had any of
Cardiovascular diseases. pathology
 Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
F r e q u e n t l y A s k e d Q u e s t i o n s
 Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Electrodiagnostic Testing
 Electrodiagnostic Testing Electromyogram and Nerve Conduction Study North American Spine Society Public Education Series What Is Electrodiagnostic Testing? The term electrodiagnostic testing covers a
Electrodiagnostic Testing Electromyogram and Nerve Conduction Study North American Spine Society Public Education Series What Is Electrodiagnostic Testing? The term electrodiagnostic testing covers a
HEADACHES IN CHILDREN AND ADOLESCENTS. Brian D. Ryals, M.D.
 HEADACHES IN CHILDREN AND ADOLESCENTS Brian D. Ryals, M.D. Frequency and Type of Headaches in Schoolchildren 8993 children age 7-15 in Sweden Migraine in 4% Frequent Nonmigrainous in 7% Infrequent Nonmigrainous
HEADACHES IN CHILDREN AND ADOLESCENTS Brian D. Ryals, M.D. Frequency and Type of Headaches in Schoolchildren 8993 children age 7-15 in Sweden Migraine in 4% Frequent Nonmigrainous in 7% Infrequent Nonmigrainous
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College
 Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Primary Sources for figures and content: Eastern Campus Marieb,
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Primary Sources for figures and content: Eastern Campus Marieb,
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Workup and Management of Vertigo
 Workup and Management of Vertigo S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 25, 2008 The speaker has no disclosures Two Key Questions 1. What do you
Workup and Management of Vertigo S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 25, 2008 The speaker has no disclosures Two Key Questions 1. What do you
Medical Surgical Nursing (Elsevier)
 1 of 6 I. The Musculoskeletal System Medical Surgical Nursing (Elsevier) 1. Med/Surg: Musculoskeletal System: The Comprehensive Health History 2. Med/Surg: Musculoskeletal System: A Nursing Approach to
1 of 6 I. The Musculoskeletal System Medical Surgical Nursing (Elsevier) 1. Med/Surg: Musculoskeletal System: The Comprehensive Health History 2. Med/Surg: Musculoskeletal System: A Nursing Approach to
Neurological System Best Practice Documentation
 Neurological System Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Dementia Delirium/Encephalopathy Parkinson s Epilepsy /Seizure Migraines
Neurological System Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Dementia Delirium/Encephalopathy Parkinson s Epilepsy /Seizure Migraines
