Keratoconus is a noninflammatory ectasia of the cornea with
|
|
|
- Posy Flowers
- 10 years ago
- Views:
Transcription
1 CLINICAL SCIENCE Morphological and Immunohistochemical Changes After Corneal Cross-Linking Elisabeth M. Messmer, MD,* Peter Meyer, MD, Martina C. Herwig, MD, Karin U. Loeffler, MD, Frank Schirra, MD, Berthold Seitz, MD, Michael Thiel, MD, Thomas Reinhard, MD,k Anselm Kampik, MD,* and Claudia Auw-Haedrich, MDk Purpose: To present light and electron microscopic as well as immunohistochemical findings after corneal cross-linking (CXL). Methods: Six keratoconus corneas after CXL, 12 keratoconus corneas without CXL, and 7 normal corneas were examined by light microscopy, indirect immunohistochemistry using antibodies against proapoptotic BAX, antiapoptotic survivin, and BCL-2, and anti smooth muscle actin and, in part, by transmission electron microscopy. Direct immunofluorescence with 496-diamidino-2-phenylindole was performed to analyze keratocytes/area in the anterior, middle, posterior, peripheral, and central corneal stroma. Results: The period between CXL and keratoplasty ranged from 5 to 30 months. All keratoconus corneas showed the typical histological changes. Increased proapoptotic BAX expression and/or antiapoptotic survivin expression were noticed in keratocytes and endothelium in 2 keratoconus specimens after CXL. Smooth muscle actin was only observed in subepithelial scar tissue of 2 keratoconus corneas without CXL. Keratoconus corneas after CXL revealed a significant reduction in keratocyte counts in the entire cornea (P = 0.003) compared with keratoconus corneas without CXL and normal corneas. This difference was because of a loss of keratocytes in the anterior (P =0.014)and middle (P = 0.024) corneal stroma. Keratocytes in CXL corneas were reduced in the center (P = 0.028) and the periphery (P =0.047). Conclusions: CXL in human keratoconus can cause considerable morphologic corneal changes up to 30 months postoperatively. Especially noteworthy is a long-lasting, maybe permanent, keratocyte loss in the anterior and middle corneal stroma involving the central and peripheral cornea. As long-term corneal damage after CXL is of genuine concern, particular care should be taken to perform this procedure only in accordance with investigational protocols. Key Words: keratoconus, corneal cross-linking, keratocytes (Cornea 2013;32: ) Received for publication September 9, 2011; revision received January 20, 2012; accepted January 27, From the *Department of Ophthalmology, Ludwig-Maximilians-University, Munich, Germany; University Eye Hospital, Basel, Switzerland; University Eye Hospital, Bonn, Germany; University Eye Hospital, Homburg-Saar, Germany; Eye Hospital, Luzern, Switzerland; and kuniversity Eye Hospital, Freiburg, Germany. The authors state that they have no funding or conflicts of interest to disclose. Reprints: Elisabeth M. Messmer, Department of Ophthalmology, Ludwig- Maximilians-University, Mathildenstr 8, Munich, Germany ( [email protected]). Copyright 2012 by Lippincott Williams & Wilkins Keratoconus is a noninflammatory ectasia of the cornea with documented changes in corneal epithelial basement membrane structure 1 3 ; in stromal collagen composition, distribution, and organization leading to lamellar and/or fibrillar slippage 2,4 7 ; in extracellular matrix components 3 ; and in keratocyte morphology and cell matrix interactions In addition, collagen loss, proteoglycan changes, and the upregulation of degradative enzymes have been shown in keratoconus and support the occurrence of additional biochemical changes Histopathologic studies of keratoconus corneas reported fragmentation of the epithelial basement membrane, superficial linear ruptures in Bowman layer filled with fibrotic connective tissue, and folds in Descemet membrane. 15 Therapeutic options for patients with keratoconus include rigid gas permeable contact lenses, intracorneal ring segments, and topography-guided photorefractive keratectomy. 16,17 In approximately 20% of cases, keratoconus progresses to the extent that corneal transplantation is unavoidable. 18 In 2003, corneal cross-linking (CXL) using the photosensitizer riboflavin and UVA light to increase the biomechanical stability of the cornea and the resistance to collagenases was shown to halt progression of keratoconus. 19 In CXL-treated eyes, maximal keratometry readings and refractive errors remained stable or decreased, whereas visual acuity improved. Corneal transparency and endothelial cell density remained unchanged by CXL. 19 These findings in keratoconus were confirmed by others, and the indication for CXL was extended to corneal melting, 23,24 keratitis refractive to therapy, 25 and laser in situ keratomileusis induced keratectasia. 26,27 Extrapolating from rabbit experiments, a minimal corneal thickness of 400 mm was postulated also in human CXL by Wollensak et al 28,29 to prevent endothelial damage. In vivo confocal microscopic examination after CXL showed a loss of keratocytes in the anterior and intermediate stroma, associated with stromal edema immediately after treatment. Gradual keratocyte repopulation of the corneal stroma, starting between the second and third postoperative month, becoming complete after 6 months, and continuing thereafter was reported by Mazotta et al. 30 Between the third and the sixth months after CXL, increased density with hyperreflectivity of the extracellular matrix combined with activated keratocyte nuclei and elongated cell processes was seen. In late scans 2 years after the procedure, bridge - and needle- shaped hyperreflective bands compatible with newly Cornea Volume 32, Number 2, February
2 Messmer et al Cornea Volume 32, Number 2, February 2013 replaced collagen and different lamellar interconnections were documented. 31,32 This is in accordance with the histological findings in rabbit corneas after CXL, where repopulating keratocytes were observed to repair the cytotoxic effects in 6-weeks time. 33 Recently, histology of one normal human cornea 24 hours after CXL was reported. It confirmed the complete loss of keratocytes down to a depth of 250 to 280 mm with normal keratocyte densities beneath in the immediate postoperative course. 34 We report for the first time histological, immunohistological, and electron microscopic findings in 6 corneas treated with CXL 5 to 30 months before keratoplasty and compare these findings with normal corneas and keratoconic corneas without CXL treatment. PATIENTS AND METHODS All 6 CXL procedures were performed elsewhere, and preoperative data were provided retrospectively by the corresponding surgeons. Clinical patients characteristics are given in Table 1. CXL was performed using a standard protocol with 0.1% riboflavin application every 2 minutes for 60 minutes and concomitant UVA irradiation (370 nm; 3 mw/cm 2 ) for the last 30 minutes in all patients. In 2 patients, hypoosmolar riboflavin was added to increase corneal thickness intraoperatively to a minimum of 400 mm. Additional procedures were performed in 2 patients. One patient underwent photorefractive keratectomy 21 months after CXL, and a second CXL procedure was performed 4 months later (patient 4). In a second patient, corneal ring implantation was performed 12 months after CXL (patient 6). However, a small corneal perforation intraoperatively necessitated the immediate explantation of the ring segment. Corneal transplantation was required in all 6 patients because of further decrease in visual acuity associated with increased astigmatism and/or worsened corneal scarring 5 to 30 months after CXL. For comparison, 12 keratoconic corneas without CXL were obtained after keratoplasty for progressive disease. In addition, 7 normal corneas were taken from eyes enucleated for intraocular melanoma. Specimens were fixed in 4% formaldehyde in M phosphate buffer for 24 hours, dehydrated in increasing concentrations of ethanol (70% 99%), and infiltrated with paraffin (Merck, Darmstadt, Germany) at 60 C. Sections with a thickness of 3 mm were cut and floated on deionized water at 45 C and mounted as single sections on Superfrost Plus glass slides (Menzel-Gläser, Braunschweig, Germany). Slides were subsequently dried at 60 C for 1 hour and stained with hematoxylin and eosin, periodic-acid Schiff, and Alcian blue. For immunohistochemistry, formalin-fixed corneal buttons were mounted on Super Frost Plus slides, deparaffinized and steamed in target retrieval solution for 30 minutes. The tissue was immunostained using the alkaline phosphatase antialkaline phosphatase method (APAAP). Primary antibodies and dilutions used are listed in Table 2. Briefly, the primary antibody was applied for 30 minutes. Thereafter, the tissue was incubated with biotinylated secondary antibodies (Dako ChemMate Detection Kit APAAP, Mouse) and APAAP complex (Dako ChemMate Detection Kit APAAP) as a tertiary reagent for 20 minutes each. The slides were developed for 10 minutes in a solution of chromogen Fast Red substrate (DakoCytomation, Hamburg, Germany). Tris-buffered normal saline (ph 7.6) was used as wash buffer between steps and as negative control. Antibody dilutions were made with readymade antibody diluent (DakoCytomation) for primary antibodies. All slides were counterstained with hemalaun and mounted in Malinol (Waldeck GmbH & Co Division Chroma, Münster, Germany). Tissue from a conjunctival intraepithelial carcinoma and a basal cell carcinoma was used as a positive control. For direct immunofluorescence, 3-mm unstained sections were deparaffinized and immunostained with 496-diamidino-2-phenylindole (Vector Laboratories Ltd, Peterborough, UK) as a nuclear stain to analyze keratocyte densities. A JenOptic ProGress camera attached to a Leica Fluorescence DM 2500 microscope was used to document sections. Images were processed further with Adobe Photoshop CS5.1 to split corneal stromal images into 9 areas: 2 peripheral corneal sections, 1 central corneal section, anterior corneal stroma, middle corneal stroma, and posterior corneal stroma. Adobe Photoshop CS5.1 software was also used to count keratocytes manually and analyze referring corneal stromal areas to obtain keratocyte counts per area (1 mio pixel). Transmission Electron Microscopy Tissue specimens of 3 keratoconus patients after CXL were postfixed in 2% osmium tetroxide, processed through TABLE 1. Clinical Characteristics of Patients Undergoing CXL Patient Number Age (yr) Sex Preoperative Corneal Thickness (mm) Preoperative VA Hypoosmolar Riboflavin Additional Procedures Period CXL KP (mo) Astigmatism Postoperative Scarring Postoperative 1 59 F 540 1/50 No No 6 [ 2 20 M /400 No No 9 Y [ 3 15 M /50 Yes No 5 [ [ 4 24 M n.k. n.k. n.k. PRK, 2CXL 30/23 [ [ 5 34 M /100 No No 6 [ 6 53 M /40 Yes Corneal ring implant 26 [ 2CXL, second crosslinking procedure; F, female; KP, keratoplasty; M, male; n.k., not known; PRK, photorefractive keratectomy; VA, visual acuity Ó 2012 Lippincott Williams & Wilkins
3 Cornea Volume 32, Number 2, February 2013 Morphological Corneal Changes After CXL TABLE 2. Characteristics of Antibodies Used Antibody Company Host Dilution BAX DAKO Polyclonal rabbit 1:50 Survivin DAKO Monoclonal mouse 1:10 BCL-2 DAKO Monoclonal mouse 1:200 Smooth muscle actin DAKO Monoclonal mouse 1:100 alcohol and propylene oxide for embedding in Araldite or acetone Durcupan and sectioned with a Reichert-Jung ultratome. Semithin sections were stained with toluidine blue, whereas ultrathin sections were stained with uranyl acetate and lead citrate and examined under a Zeiss transmission electron microscope. Statistics were performed using x 2 and Kruskal Wallis tests, as well as Spearman correlations. The results were considered statistically significant at P, RESULTS Histology Histological findings in all keratoconus specimens after CXL included thinning of the central corneal epithelium with an intact epithelial basement membrane, breaks in Bowman layer, a thinned (para-) central corneal stroma with reduction of keratocytes, as well as an unaffected Descemet membrane with an intact endothelium (Fig. 1). Collagen structure did not differ between keratoconus with and without CXL by light microscopy. In 1 cornea (patient 4), which had undergone several surgical procedures, the Alcian blue stain revealed deposits of acid mucopolysaccharides in the corneal stroma, in keratocytes, and in endothelial cells. Immunohistochemistry BAX, Survivin, BCL-2 Proapoptotic BAX stained positive in the epithelium of 1 normal cornea, and in 8 of 12 keratoconus epithelia without CXL. Corneal epithelium of keratoconus specimens after CXL was negative for BAX. BAX did not stain the keratocytes or the endothelium in any normal cornea or any keratoconus cornea without CXL, but was positive in keratocytes and endothelium in 2 keratoconus corneas after CXL (Fig. 2A). Antiapoptotic survivin positivity was observed in the epithelium of 4 keratoconus corneas without CXL, and in 1 keratoconus cornea with CXL. In addition, survivin expression was present in the endothelium of 1 keratoconus cornea after CXL. In 1 normal cornea, antiapoptotic BCL-2 was present in several keratocytes. All other corneas were negative for this marker. Smooth Muscle Actin Smooth muscle actin stained positive only in subepithelial scar tissues of 2 keratoconus corneas without CXL (Fig. 2B). Neither normal corneas nor keratoconus corneas after CXL demonstrated any keratocytes positive for smooth muscle actin keratocytes. FIGURE 1. A, Keratoconus cornea 6 months after CXL with centrally thinned corneal epithelium, breaks in Bowman layer, and thinned corneal stroma with near complete loss of keratocytes. The endothelium seems normal (hematoxylin eosin, original magnification 20). B, Keratoconus cornea 5 months after CXL. The corneal stroma is thinned centrally with a significant loss of keratocytes in the anterior stroma (hematoxylin eosin, original magnification 20). Transmission Electron Microscopy Electron microscopy was performed in 3 keratoconus specimens after CXL. It showed a compact collagenous matrix containing few cellular elements in the anterior stroma with thin vacuolated cytoplasmic processes: Moreover, degenerative changes of keratocytes were observed in the anterior stroma with loss of osmiophilic staining. The posterior stroma and the endothelium seemed relatively unremarkable, but an increased number of intracellular vacuoles were present in posterior keratocytes and endothelial cells. Keratocyte Counts Overall keratocyte counts per area were significantly decreased in keratoconus corneas after CXL (P = 0.033) Ó 2012 Lippincott Williams & Wilkins 113
4 Messmer et al Cornea Volume 32, Number 2, February 2013 FIGURE 3. A, Keratoconus cornea without CXL. Normal distribution of keratocytes in the corneal stroma (DAPI stain, original magnification 10). B, Keratoconus cornea 6 months after CXL. Near complete loss of keratocytes in the anterior and middle stroma (DAPI stain, original magnification 10). FIGURE 2. A, Keratoconus cornea after CXL. BAX-positive keratocytes in the deep corneal stroma (asterisk) and BAXpositive endothelial cells (arrow; original magnification 40). B, Smooth muscle actin positive myofibroblasts in subepithelial scar tissue of keratoconus cornea without CXL. compared with normal corneas and keratoconus corneas without CXL (Fig. 3). Keratocytes per 1 mio pixel were 328 (±81) cells in normal corneas, 398 (±97) cells in keratoconus corneas without CXL and 244 (±145) cells in keratoconus corneas after CXL. This difference was especially obvious in the anterior (P = 0.014) and middle (P = 0.024) corneal stroma (Fig. 4). Keratocyte counts in the anterior stroma averaged 399 (±119) in normal corneas, 378 (±96) in keratoconus without CXL, and 187 (±127) in keratoconus with CXL. In the middle stroma, measurements were 347 (±74) keratocytes for normal corneas, 426 (±123) keratocytes for keratoconus corneas without CXL, and 274 (±213) keratocytes for keratoconus after CXL. In the posterior stroma, keratocyte counts were not significantly decreased in keratoconus corneas after CXL compared with normal corneas and keratoconus corneas without CXL. Interestingly, keratocytes were reduced after CXL in the peripheral (P = 0.047) and the central corneal stroma (P = 0.028; Fig. 5). No correlation was evident between keratocyte counts and time since CXL. CXL corneas in which hypoosmolar riboflavin was used in addition to swelling the corneal stroma did not show a significant difference in keratocyte counts compared with corneas that underwent CXL according to the standard protocol. The same was true for corneas that underwent a second procedure including photorefractive keratectomy, corneal ring implantation, or a second CXL. DISCUSSION CXL by combined riboflavin UVA treatment was introduced in 2003 as a promising new therapy in keratoconus to stop progression and delay keratoplasty. 19 Histological changes in keratoconus patients after this procedure have not been published. We observed long-term toxic effects of CXL treatment in keratoconus corneas. In cell culture experiments and rabbits, riboflavin UVA was shown to lead to dose-dependent apoptotic keratocyte damage 24 hours postoperatively by the formation of reactive oxygen species. 33,35,36 According to Wollensak et al, 35,36 keratocyte damage can be expected in human corneas down to a depth of 300 mm using the standard surface UVA irradiance of 3 mw/cm 2 (5.4 J/cm 2 ). And indeed, complete loss of keratocytes down to a depth of 250 to 280 mm with normal keratocyte density beneath was shown in a normal human cornea 24 hours after CXL. 34 Endothelial necrosis and apoptosis occurred in rabbit cornea with a corneal thickness less than 400 mm. 28 Therefore, a minimum corneal thickness of 400 mm Ó 2012 Lippincott Williams & Wilkins
5 Cornea Volume 32, Number 2, February 2013 Morphological Corneal Changes After CXL FIGURE 4. Mean keratocytes/area in anterior, middle, and posterior corneal stroma in normal corneas, keratoconus corneas without CXL, and keratoconus corneas after CXL. A significant difference was evident between keratocyte counts in keratoconus corneas with and without CXL in the anterior (P = 0.05) and the middle stroma (P = 0.018). In addition, significantly reduced keratocytes were present in the anterior stroma of keratoconus corneas after CXL compared with normal corneas (P = 0.014). (without epithelium) was postulated to be safe in human CXL treatment. Preoperative swelling of the cornea with hypoosmolar riboflavin, however, has been shown to be effective and safe in keratoconus patients with thinner corneas. 37 Wound healing experiments in approximately 300 mm thin rabbit corneas after CXL showed a complete loss of endothelial cells and stromal keratocytes by day 3. On day 7, the endothelium was intact again, and keratocyte repopulation of the posterior stroma began. By week 4, keratocyte repopulation of the anterior stroma was observed, with normal cytoarchitecture by week In vivo confocal microscopy in humans after CXL also demonstrated a reduction in anterior and intermediate stromal keratocytes followed by a gradual repopulation until up to 6 months. 30 In our study, keratocyte loss was still evident 5 to 30 months after CXL in keratoconus patients. The cell loss was mainly confined to the anterior and middle stroma, but it involved the central and the peripheral cornea. This finding is in complete disagreement to animal studies and in vivo confocal studies in humans. Additional procedures, such as photorefractive keratectomy, corneal ring implantation, or a second CXL procedure were not responsible for this keratocyte loss. In addition, the use of hypoosmolar riboflavin to increase stromal thickness to a minimum of 400 mm for treatment was not associated with FIGURE 5. Mean keratocytes/area in the peripheral and central corneal stroma in normal corneas, keratoconus corneas without CXL, and keratoconus corneas after CXL. A significant reduction of keratocytes was observed in keratoconus corneas after CXL in the central (P = 0.018) and peripheral (P = 0.024) corneal stroma compared with keratoconus corneas without CXL. a further keratocyte reduction compared with patients treated with the standard protocol. We were surprised to find keratocytes and endothelial cells staining for proapoptotic BAX and antiapoptotic survivin in keratoconus specimens after CXL compared with normal corneas and keratoconus corneas without CXL. The CXL procedure itself does not seem to be responsible because these markers are typically expressed only for a short time after wounding. It may be a feature associated with keratoconus itself, as Kaldawy et al 8 could also demonstrate apoptotic cells in all 3 layers of the keratoconus corneas. However, our keratoconus specimens without CXL did not express any apoptosis markers in the stroma or endothelium. Thus, it may be speculated that the CXL procedure may be indirectly involved. Further research is certainly warranted to explain these findings. Keratocyte apoptosis and necrosis are also known to occur after mechanical epithelial debridement or incision through the epithelium as performed as part of the CXL procedure or in the case of keratoplasty. However, this observation is only made in the anterior 50 mm of the corneal stroma, is typically seen early after the trauma, and the subsequent repopulation by activated stromal keratocytes is complete in several days after the injury In our study, no difference was observed in keratocyte counts in the peripheral cornea in keratoconus buttons without CXL and normal corneas confirming that the trephine cut was not responsible for the loss of keratocytes in the corneal periphery after CXL. Ó 2012 Lippincott Williams & Wilkins 115
6 Messmer et al Cornea Volume 32, Number 2, February 2013 Chronic keratocyte apoptosis associated with the ongoing epithelial injury may be an important pathophysiological factor in keratoconus mediated by interleukin-1 and Fasligand. 8,41,43 But keratocyte counts were not significantly different in keratoconus specimens without CXL and normal corneas indicating that indeed CXL is responsible for the keratocyte loss observed in our study. Wollensak et al 33 identified a-actin-positive myofibroblasts, especially in the periphery of the irradiated areas, by weeks 4 and 6 after CXL in rabbit corneas. The presence of these cells is interesting because myofibroblasts, presumed derivatives of keratocytes responding to transforming growth factor beta, are a critical component of the wound healing cascade. 44 They play a comprehensive role in collagen and extracellular matrix remodeling through production of collagen, glycosaminoglycans, collagenases, gelatinases, and matrix metalloproteinases The regression of keratectasia in keratoconus patients after CXL might be explained in part by the action of myofibroblasts. 33 Five to 30 months after CXL, we could not identify any actin-positive myofibroblasts in the corneal stroma. The wound healing process after CXL seems to be complete by that time. It may parallel wound healing after photorefractive keratectomy, where myofibroblasts are typically observed for 3 months. 47 The increase in biomechanical stiffness in corneas after CXL is paralleled by an increase in corneal collagen diameter in animal experiments. 48 In vivo confocal microscopy confirmed an increased density of the anterior extracellular corneal matrix starting between the third and sixth month postoperatively with bridge-like and needle-shaped hyperreflective bands in humans after CXL. 31 In our study, CXL corneas did not show any obvious changes in collagen structure by light microscopy, but the anterior corneal stroma was unusually compact by transmission electron microscopy. Special measurements to document changes in collagen diameter thickness were not performed. Our results demonstrate that CXL can cause considerable long-term changes to keratoconus corneas. Our series of cases having consisted of surgically removed corneas for keratoconus is biased for poor outcome, but permanent keratocyte loss after CXL is a potentially serious consequence of the procedure that deserves further study. To exclude additional negative influential factors, CXL treatment should only be performed under investigational protocol. REFERENCES 1. Tuori AJ, Virtanen I, Aine E, et al. The immunohistochemical composition of corneal basement membrane in keratoconus. Curr Eye Res. 1997;16: Cheng EL, Maruyama I, SundarRaj N, et al. Expression of type XII collagen and hemidesmosome-associated proteins in keratoconus corneas. Curr Eye Res. 2001;22: Kenney MC, Nesburn AB, Burgeson RE, et al. Abnormalities of the extracellular matrix in keratoconus corneas. Cornea. 1997;16: Daxer A, Fratzl P. Collagen fibril orientation in the human corneal stroma and its implication in keratoconus. Invest Ophthalmol Vis Sci. 1997;38: Radner W, Zehetmayer M, Skorpik C, et al. Altered organization of collagen in the apex of keratoconus corneas. Ophthalmic Res. 1998;30: Meek KM, Tuft SJ, Huang Y, et al. Changes in collagen orientation and distribution in keratoconus corneas. Invest Ophthalmol Vis Sci. 2005;46: Hayes S, Boote C, Tuft SJ, et al. A study of corneal thickness, shape and collagen organisation in keratoconus using videokeratography and X-ray scattering techniques. Exp Eye Res. 2007;84: Kaldawy RM, Wagner J, Ching S, et al. Evidence of apoptotic cell death in keratoconus. Cornea. 2002;21: Rock ME, Moore MN, Anderson JA, et al. 3-D computer models of human keratocytes. CLAO J. 1995;21: Yue BY, Baum JL, Smith BD. Identification of collagens synthesized by cultures of normal human corneal and keratoconus stromal cells. Biochim Biophys Acta. 1983;755: Balasubramanian SA, Pye DC, Willcox MD. Are proteinases the reason for keratoconus? Curr Eye Res. 2010;35: Kao WW, Vergnes JP, Ebert J, et al. Increased collagenase and gelatinase activities in keratoconus. Biochem Biophys Res Commun. 1982;107: Rehany U, Lahav M, Shoshan S. Collagenolytic activity in keratoconus. Ann Ophthalmol. 1982;14: Collier SA. Is the corneal degradation in keratoconus caused by matrixmetalloproteinases? Clin Experiment Ophthalmol. 2001;29: Pouliquen Y. Doyne lecture keratoconus. Eye (Lond). 1987;1(pt 1): Kanellopoulos AJ. Comparison of sequential vs same-day simultaneous collagen cross-linking and topography-guided PRK for treatment of keratoconus. J Refract Surg. 2009;25:S812 S Coskunseven E, Jankov MR II, Hafezi F, et al. Effect of treatment sequence in combined intrastromal corneal rings and corneal collagen crosslinking for keratoconus. J Cataract Refract Surg. 2009;35: Kennedy RH, Bourne WM, Dyer JA. A 48-year clinical and epidemiologic study of keratoconus. Am J Ophthalmol. 1986;101: Wollensak G, Spoerl E, Seiler T. Riboflavin/ultraviolet-a-induced collagen crosslinking for the treatment of keratoconus. Am J Ophthalmol. 2003;135: Caporossi A, Mazzotta C, Baiocchi S, et al. Long-term results of riboflavin ultraviolet a corneal collagen cross-linking for keratoconus in Italy: the Siena eye cross study. Am J Ophthalmol. 2010;149: Koller T, Mrochen M, Seiler T. Complication and failure rates after corneal crosslinking. J Cataract Refract Surg. 2009;35: Wittig-Silva C, Whiting M, Lamoureux E, et al. A randomized controlled trial of corneal collagen cross-linking in progressive keratoconus: preliminary results. J Refract Surg. 2008;24:S720 S Al-Sabai N, Koppen C, Tassignon MJ. UVA/riboflavin crosslinking as treatment for corneal melting. Bull Soc Belge Ophtalmol. 2010(315): Schnitzler E, Spörl E, Seiler T. Irradiation of cornea with ultraviolet light and riboflavin administration as a new treatment for erosive corneal processes, preliminary results in four patients [in German]. Klin Monbl Augenheilkd. 2000;217: Makdoumi K, Mortensen J, Crafoord S. Infectious keratitis treated with corneal crosslinking. Cornea. 2010;29: Hafezi F, Kanellopoulos J, Wiltfang R, et al. Corneal collagen crosslinking with riboflavin and ultraviolet A to treat induced keratectasia after laser in situ keratomileusis. J Cataract Refract Surg. 2007;33: Kohlhaas M, Spoerl E, Speck A, et al. A new treatment of keratectasia after LASIK by using collagen with riboflavin/uva light cross-linking [in German]. Klin Monbl Augenheilkd. 2005;222: Wollensak G, Spoerl E, Wilsch M, et al. Endothelial cell damage after riboflavin-ultraviolet-a treatment in the rabbit. J Cataract Refract Surg. 2003;29: Wollensak G, Spörl E, Reber F, et al. Corneal endothelial cytotoxicity of riboflavin/uva treatment in vitro. Ophthalmic Res. 2003;35: Mazzotta C, Balestrazzi A, Traversi C, et al. Treatment of progressive keratoconus by riboflavin-uva-induced cross-linking of corneal collagen: ultrastructural analysis by Heidelberg Retinal Tomograph II in vivo confocal microscopy in humans. Cornea. 2007;26: Mazzotta C, Traversi C, Baiocchi S, et al. Corneal healing after riboflavin ultraviolet-a collagen cross-linking determined by confocal laser scanning microscopy in vivo: early and late modifications. Am J Ophthalmol. 2008;146: Mazzotta C, Caporossi T, Denaro R, et al. Morphological and functional correlations in riboflavin UV A corneal collagen cross-linking for keratoconus. Acta Ophthalmol. [published online ahead of print April 23, 2010.] doi: /j x Ó 2012 Lippincott Williams & Wilkins
7 Cornea Volume 32, Number 2, February 2013 Morphological Corneal Changes After CXL 33. Wollensak G, Iomdina E, Dittert DD, et al. Wound healing in the rabbit cornea after corneal collagen cross-linking with riboflavin and UVA. Cornea. 2007;26: Wollensak G. Histological changes in human cornea after cross-linking with riboflavin and ultraviolet A. Acta Ophthalmol. 2010;88:e17 e Wollensak G, Spoerl E, Wilsch M, et al. Keratocyte apoptosis after corneal collagen cross-linking using riboflavin/uva treatment. Cornea. 2004;23: Wollensak G, Spoerl E, Reber F, et al. Keratocyte cytotoxicity of riboflavin/uva-treatment in vitro. Eye (Lond). 2004;18: Hafezi F, Mrochen M, Iseli HP, et al. Collagen crosslinking with ultraviolet-a and hypoosmolar riboflavin solution in thin corneas. J Cataract Refract Surg. 2009;35: Ambrósio R Jr, Kara-José N, Wilson SE. Early keratocyte apoptosis after epithelial scrape injury in the human cornea. Exp Eye Res. 2009;89: Dohlman CH, Gasset AR, Rose J. The effect of the absence of corneal epithelium or endothelium on the stromal keratocytes. Invest Ophthalmol. 1968;7: Helena MC, Baerveldt F, Kim WJ, et al. Keratocyte apoptosis after corneal surgery. Invest Ophthalmol Vis Sci. 1998;39: Wilson SE, He YG, Weng J, et al. Epithelial injury induces keratocyte apoptosis: hypothesized role for the interleukin-1 system in the modulation of corneal tissue organization and wound healing. Exp Eye Res. 1996;62: Wilson SE, Mohan RR, Mohan RR, et al. The corneal wound healing response: cytokine-mediated interaction of the epithelium, stroma, and inflammatory cells. Prog Retin Eye Res. 2001;20: Kim WJ, Rabinowitz YS, Meisler DM, et al. Keratocyte apoptosis associated with keratoconus. Exp Eye Res. 1999;69: Jester JV, Ho-Chang J. Modulation of cultured corneal keratocyte phenotype by growth factors/cytokines control in vitro contractility and extracellular matrix contraction. Exp Eye Res. 2003;77: Dupps WJ Jr, Wilson SE. Biomechanics and wound healing in the cornea. Exp Eye Res. 2006;83: Jester JV, Petroll WM, Cavanagh HD. Corneal stromal wound healing in refractive surgery: the role of myofibroblasts. Prog Retin Eye Res. 1999; 18: Mohan RR, Hutcheon AE, Choi R, et al. Apoptosis, necrosis, proliferation, and myofibroblast generation in the stroma following LASIK and PRK. Exp Eye Res. 2003;76: Wollensak G, Wilsch M, Spoerl E, et al. Collagen fiber diameter in the rabbit cornea after collagen crosslinking by riboflavin/uva. Cornea. 2004;23: Ó 2012 Lippincott Williams & Wilkins 117
Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus
 Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus Michelle Cho, M.D. 1 Anastasios John Kanellopoulos, M.D 1,2 New York University
Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus Michelle Cho, M.D. 1 Anastasios John Kanellopoulos, M.D 1,2 New York University
Short and long term complications of combined. Protocol) in 412 keratoconus eyes (2 7 years follow up)
 Short and long term complications of combined topography guided PRK and CXL (the Athens Protocol) in 412 keratoconus eyes (2 7 years follow up) Anastasios John Kanellopoulos, MD Director, Laservision.gr
Short and long term complications of combined topography guided PRK and CXL (the Athens Protocol) in 412 keratoconus eyes (2 7 years follow up) Anastasios John Kanellopoulos, MD Director, Laservision.gr
Keratoconus. Progressive bilateral ectasia. Onset puberty. Prevalence 1:2000. 20% progress to transplantation. Pathogenesis unclear
 Keratoconus Progressive bilateral ectasia Onset puberty Prevalence 1:2000 20% progress to transplantation Pathogenesis unclear Increased pepsin and catalase Decreased collagen crosslinking cf normal Conventional
Keratoconus Progressive bilateral ectasia Onset puberty Prevalence 1:2000 20% progress to transplantation Pathogenesis unclear Increased pepsin and catalase Decreased collagen crosslinking cf normal Conventional
Overview of Refractive Surgery
 Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Transepithelial Crosslinking vs. Corneal Pocket Crosslinking. Christoph Kranemann MD Anna Yu OD
 Transepithelial Crosslinking vs. Corneal Pocket Crosslinking Christoph Kranemann MD Anna Yu OD Rome 2013 We have no financial interests in this presentation. Corneal collagen cross linking Creates new
Transepithelial Crosslinking vs. Corneal Pocket Crosslinking Christoph Kranemann MD Anna Yu OD Rome 2013 We have no financial interests in this presentation. Corneal collagen cross linking Creates new
Diego Fernando Suárez Sierra, MD Fellow Cornea and Refractive Surgery Fellow Lens and Ocular Surface Vejarano Laser Vision Center
 Corneal crosslinking with riboflavin and ultraviolet light before or after subepithelial keratectomy laser-assisted (LASEK) in patients with thin corneas. Diego Fernando Suárez Sierra, MD Fellow Cornea
Corneal crosslinking with riboflavin and ultraviolet light before or after subepithelial keratectomy laser-assisted (LASEK) in patients with thin corneas. Diego Fernando Suárez Sierra, MD Fellow Cornea
How To Test For Cxl
 ARTICLE Complication and failure rates after corneal crosslinking Tobias Koller, MD, Michael Mrochen, PhD, Theo Seiler, MD, PhD PURPOSE: To evaluate the complication rate of corneal crosslinking (CXL)
ARTICLE Complication and failure rates after corneal crosslinking Tobias Koller, MD, Michael Mrochen, PhD, Theo Seiler, MD, PhD PURPOSE: To evaluate the complication rate of corneal crosslinking (CXL)
Collagen cross-linking should be done separately. Canan Asli Utine, MD, MSc, FICO Yeditepe University, Istanbul, Turkey
 Collagen cross-linking should be done separately Canan Asli Utine, MD, MSc, FICO Yeditepe University, Istanbul, Turkey Collagen cross linking 1st established tx addressing the pathophysiology of corneal
Collagen cross-linking should be done separately Canan Asli Utine, MD, MSc, FICO Yeditepe University, Istanbul, Turkey Collagen cross linking 1st established tx addressing the pathophysiology of corneal
CXL With the Epithelium on or off: Which Is Better?
 CXL With the Epithelium on or off: Which Is Better? Transepithelial CXL Is Gaining Ground By Roy S. Rubinfeld, MD, and the CXL-USA Study Group At its simplest, corneal collagen cross-linking (CXL) is a
CXL With the Epithelium on or off: Which Is Better? Transepithelial CXL Is Gaining Ground By Roy S. Rubinfeld, MD, and the CXL-USA Study Group At its simplest, corneal collagen cross-linking (CXL) is a
Original Article Corneal Collagen Cross Linking Pak Armed Forces Med J 2015; 65(1): 105-9
 Original Article Corneal Collagen Cross Linking Pak Armed Forces Med J 2015; 65(1): 105-9 COMPARISON OF RAPID AND CONVENTIONAL CORNEAL COLLAGEN CROSS LINKING IN PATIENTS HAVING KERATOCONUS Intisar ul Haq,
Original Article Corneal Collagen Cross Linking Pak Armed Forces Med J 2015; 65(1): 105-9 COMPARISON OF RAPID AND CONVENTIONAL CORNEAL COLLAGEN CROSS LINKING IN PATIENTS HAVING KERATOCONUS Intisar ul Haq,
Surgical Advances in Keratoconus. Keratoconus. Innovations in Ophthalmology. New Surgical Advances. Diagnosis of Keratoconus. Scheimpflug imaging
 Surgical Advances in Keratoconus Keratoconus Ectatic disorder 1 in 1,000 individuals Starts in adolescence & early adulthood Uncertain cause 20% require corneal transplant Innovations in Ophthalmology
Surgical Advances in Keratoconus Keratoconus Ectatic disorder 1 in 1,000 individuals Starts in adolescence & early adulthood Uncertain cause 20% require corneal transplant Innovations in Ophthalmology
Management of Unpredictable Post-PRK Corneal Ectasia with Intacs Implantation
 Management of Unpredictable Post-PRK Corneal Ectasia with Intacs Implantation Mohammad Naser Hashemian, MD 1 Mahdi AliZadeh, MD 2 Hassan Hashemi, MD 1,3 Firoozeh Rahimi, MD 4 Abstract Purpose: To present
Management of Unpredictable Post-PRK Corneal Ectasia with Intacs Implantation Mohammad Naser Hashemian, MD 1 Mahdi AliZadeh, MD 2 Hassan Hashemi, MD 1,3 Firoozeh Rahimi, MD 4 Abstract Purpose: To present
Natural history of corneal haze after collagen crosslinking for keratoconus and corneal ectasia: Scheimpflug and biomicroscopic analysis
 ARTICLE Natural history of corneal haze after collagen crosslinking for keratoconus and corneal ectasia: Scheimpflug and biomicroscopic analysis Steven A. Greenstein, Kristen L. Fry, OD, MS, Jalpa Bhatt,
ARTICLE Natural history of corneal haze after collagen crosslinking for keratoconus and corneal ectasia: Scheimpflug and biomicroscopic analysis Steven A. Greenstein, Kristen L. Fry, OD, MS, Jalpa Bhatt,
BY A. JOHN KANELLOPOULOS, MD
 Sequential Versus Simultaneous CXL and Topography-Guided PRK Simultaneous treatment appears to provide superior rehabilitation of keratoconus. BY A. JOHN KANELLOPOULOS, MD * Editor s note: The following
Sequential Versus Simultaneous CXL and Topography-Guided PRK Simultaneous treatment appears to provide superior rehabilitation of keratoconus. BY A. JOHN KANELLOPOULOS, MD * Editor s note: The following
Case Reports Post-LASIK ectasia treated with intrastromal corneal ring segments and corneal crosslinking
 Case Reports Post-LASIK ectasia treated with intrastromal corneal ring segments and corneal crosslinking Kay Lam, MD, Dan B. Rootman, MSc, Alejandro Lichtinger, and David S. Rootman, MD, FRCSC Author affiliations:
Case Reports Post-LASIK ectasia treated with intrastromal corneal ring segments and corneal crosslinking Kay Lam, MD, Dan B. Rootman, MSc, Alejandro Lichtinger, and David S. Rootman, MD, FRCSC Author affiliations:
Corneal Collagen Cross-Linking (CXL) With Riboflavin
 Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Simultaneous Photorefractive keratectomy (PRK) with Corneal Cross Linking (CXL) For Treatment of Early Keratoconus.
 Simultaneous Photorefractive keratectomy (PRK) with Corneal Cross Linking (CXL) For Treatment of Early Keratoconus. Mahmoud M Saleh, Ahmed I Galhoom, Mohamed A El-Malah, Abdelgany Ib Abdelgany Department
Simultaneous Photorefractive keratectomy (PRK) with Corneal Cross Linking (CXL) For Treatment of Early Keratoconus. Mahmoud M Saleh, Ahmed I Galhoom, Mohamed A El-Malah, Abdelgany Ib Abdelgany Department
Corneal Collagen Crosslinking: An Introduction to the New Paradigm in Keratoconus. Michael Waggoner DO McDonald Eye Associates Fayetteville AR
 Corneal Collagen Crosslinking: An Introduction to the New Paradigm in Keratoconus Michael Waggoner DO McDonald Eye Associates Fayetteville AR Learning Objectives Gain knowledge in: The history of the development
Corneal Collagen Crosslinking: An Introduction to the New Paradigm in Keratoconus Michael Waggoner DO McDonald Eye Associates Fayetteville AR Learning Objectives Gain knowledge in: The history of the development
Simultaneous Topography-guided PRK Followed by Corneal Collagen Cross-linking for Keratoconus
 Simultaneous Topography-guided PRK Followed by Corneal Collagen Cross-linking for Keratoconus George D. Kymionis, MD, PhD; Georgios A. Kontadakis, MD, MSc; George A. Kounis, PhD; Dimitra M. Portaliou,
Simultaneous Topography-guided PRK Followed by Corneal Collagen Cross-linking for Keratoconus George D. Kymionis, MD, PhD; Georgios A. Kontadakis, MD, MSc; George A. Kounis, PhD; Dimitra M. Portaliou,
9/15/2013. Naturally-existing Corneal Pathology Forme Fruste Keratoconus Keratoconus Pellucid Marginal Degeneration
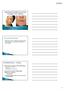 Bill Tullo, OD, FAAO Diplomate Vice-President of Clinical Services TLC Vision 33386-PO 1 Hour Bill Tullo, OD has no financial interests in any of the products or companies discussed in this program Naturally-existing
Bill Tullo, OD, FAAO Diplomate Vice-President of Clinical Services TLC Vision 33386-PO 1 Hour Bill Tullo, OD has no financial interests in any of the products or companies discussed in this program Naturally-existing
Intracorneal Ring Segments Implantation Followed by Same-day Topography-guided PRK and Corneal Collagen CXL in Low to Moderate Keratoconus
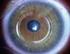 SURGICAL TECHNIQUE Intracorneal Ring Segments Implantation Followed by Same-day Topography-guided PRK and Corneal Collagen CXL in Low to Moderate Keratoconus Waleed Al-Tuwairqi, MD; Mazen M. Sinjab, MD,
SURGICAL TECHNIQUE Intracorneal Ring Segments Implantation Followed by Same-day Topography-guided PRK and Corneal Collagen CXL in Low to Moderate Keratoconus Waleed Al-Tuwairqi, MD; Mazen M. Sinjab, MD,
Ectasia after laser in-situ keratomileusis (LASIK)
 Ectasia after laser in-situ keratomileusis (LASIK) 長 庚 紀 念 醫 院 眼 科 蕭 靜 熹 Post-LASIK ectasia A rare complication of LASIK Manhattan jury awarded a former investment banker a record $7.25 million for post-lasik
Ectasia after laser in-situ keratomileusis (LASIK) 長 庚 紀 念 醫 院 眼 科 蕭 靜 熹 Post-LASIK ectasia A rare complication of LASIK Manhattan jury awarded a former investment banker a record $7.25 million for post-lasik
Post LASIK Ectasia. Examination: Gina M. Rogers, MD and Kenneth M. Goins, MD
 Post LASIK Ectasia Gina M. Rogers, MD and Kenneth M. Goins, MD October 6, 2012 Chief Complaint: Decreasing vision after laser- assisted in- situ keratomileusis (LASIK) History of Present Illness: This
Post LASIK Ectasia Gina M. Rogers, MD and Kenneth M. Goins, MD October 6, 2012 Chief Complaint: Decreasing vision after laser- assisted in- situ keratomileusis (LASIK) History of Present Illness: This
CENTRO OFTALMOLOGICO GUSTAVO TAMAYO BOGOTA COLOMBIA LASIK XTRA GUSTAVO TAMAYO MD CLAUDIA CASTELL MD PILAR VARGAS MD
 CENTRO OFTALMOLOGICO GUSTAVO TAMAYO BOGOTA COLOMBIA LASIK XTRA GUSTAVO TAMAYO MD CLAUDIA CASTELL MD PILAR VARGAS MD From: BOGOTA LASER REFRACTIVE INSTITUTE Bogota, Colombia DISCLOSURES FOR GUSTAVO TAMAYO
CENTRO OFTALMOLOGICO GUSTAVO TAMAYO BOGOTA COLOMBIA LASIK XTRA GUSTAVO TAMAYO MD CLAUDIA CASTELL MD PILAR VARGAS MD From: BOGOTA LASER REFRACTIVE INSTITUTE Bogota, Colombia DISCLOSURES FOR GUSTAVO TAMAYO
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL
 REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
5/24/2013 ESOIRS 2013. Moderator: Alaa Ghaith, MD. Faculty: Ahmed El Masri, MD Mohamed Shafik, MD Mohamed El Kateb, MD
 ESOIRS 2013 Moderator: Alaa Ghaith, MD Faculty: Ahmed El Masri, MD Mohamed Shafik, MD Mohamed El Kateb, MD 1 A systematic approach to the management of Keratoconus through the presentation of different
ESOIRS 2013 Moderator: Alaa Ghaith, MD Faculty: Ahmed El Masri, MD Mohamed Shafik, MD Mohamed El Kateb, MD 1 A systematic approach to the management of Keratoconus through the presentation of different
Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments
 Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments File Name: Origination: Last CAP Review: Next CAP Review: Last Review: implantation_of_intrastromal_corneal_ring_segments 8/2008
Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments File Name: Origination: Last CAP Review: Next CAP Review: Last Review: implantation_of_intrastromal_corneal_ring_segments 8/2008
Corneal Collagen Cross-Linking for Ectasia after LASIK and Photorefractive Keratectomy
 Corneal Collagen Cross-Linking for Ectasia after LASIK and Photorefractive Keratectomy Long-Term Results Olivier Richoz, MD, 1 Nikolaos Mavrakanas, MD, 1 Bojan Pajic, MD, PhD, 1 Farhad Hafezi, MD, PhD
Corneal Collagen Cross-Linking for Ectasia after LASIK and Photorefractive Keratectomy Long-Term Results Olivier Richoz, MD, 1 Nikolaos Mavrakanas, MD, 1 Bojan Pajic, MD, PhD, 1 Farhad Hafezi, MD, PhD
Corneal thickness changes after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results
 ARTICLE Corneal thickness changes after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results Steven A. Greenstein, BA, Vinnie P. Shah, MD, Kristen L. Fry, OD, MS, Peter S.
ARTICLE Corneal thickness changes after corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results Steven A. Greenstein, BA, Vinnie P. Shah, MD, Kristen L. Fry, OD, MS, Peter S.
Descemet s Stripping Endothelial Keratoplasty (DSEK)
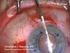 Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Managing Post-Operative Complications for LASIK and PRK
 Managing Post-Operative Complications for LASIK and PRK LASIK Flap Complications Epithelial defects o Cause Basement membrane dystrophy Recurrent erosion syndrome Dry eyes Trauma PRK as alternative Pre-treat
Managing Post-Operative Complications for LASIK and PRK LASIK Flap Complications Epithelial defects o Cause Basement membrane dystrophy Recurrent erosion syndrome Dry eyes Trauma PRK as alternative Pre-treat
Irregular astigmatism can occur naturally or due to
 Combined Topography- Guided Transepithelial PRK and CXL in Patients With Keratoconus The combined procedure strengthens the cornea and regularizes the anterior surface. BY MIRKO R. JANKOV II, MD, PHD;
Combined Topography- Guided Transepithelial PRK and CXL in Patients With Keratoconus The combined procedure strengthens the cornea and regularizes the anterior surface. BY MIRKO R. JANKOV II, MD, PHD;
Keratoconus is a bilateral, nonsymmetric, and noninflammatory
 CASE REPORT Collagen Cross-Linking (CCL) With Sequential Topography-Guided PRK A Temporizing Alternative for Keratoconus to Penetrating Keratoplasty A. John Kanellopoulos, MD* and Perry S. Binder, MS,
CASE REPORT Collagen Cross-Linking (CCL) With Sequential Topography-Guided PRK A Temporizing Alternative for Keratoconus to Penetrating Keratoplasty A. John Kanellopoulos, MD* and Perry S. Binder, MS,
Short and long term complications of combined. Protocol) in 412 keratoconus eyes (2 7 years follow up)
 Short and long term complications of combined topography guided PRK and CXL (the Athens Protocol) in 412 keratoconus eyes (2 7 years follow up) Anastasios John Kanellopoulos, MD Director, Laservision.gr
Short and long term complications of combined topography guided PRK and CXL (the Athens Protocol) in 412 keratoconus eyes (2 7 years follow up) Anastasios John Kanellopoulos, MD Director, Laservision.gr
By Dr Waleed Al-Tuwairqi, MD Dr Omnia Sherif, MD Ophthalmology Consultants, Elite Medical & Surgical Center Riyadh -KSA.
 By Dr Waleed Al-Tuwairqi, MD Dr Omnia Sherif, MD Ophthalmology Consultants, Elite Medical & Surgical Center Riyadh -KSA Rome, Italy 2013 بسم الرحمن الرحيم In the name of Allah, Most Gracious, Most Merciful
By Dr Waleed Al-Tuwairqi, MD Dr Omnia Sherif, MD Ophthalmology Consultants, Elite Medical & Surgical Center Riyadh -KSA Rome, Italy 2013 بسم الرحمن الرحيم In the name of Allah, Most Gracious, Most Merciful
Medical Director, Shinagawa LASIK Center, Tokyo, Japan Adjunct Professor, Department of Ophthalmology, Wenzhou Medical College, Wenzhou, China
 Medical Director,, Tokyo, Japan Adjunct Professor, Department of Ophthalmology, Wenzhou Medical College, Wenzhou, China Financial disclosure: Ziemer Group AG, Switzerland AcuFocus, CA Schwind Eye-Tech-Solutions,
Medical Director,, Tokyo, Japan Adjunct Professor, Department of Ophthalmology, Wenzhou Medical College, Wenzhou, China Financial disclosure: Ziemer Group AG, Switzerland AcuFocus, CA Schwind Eye-Tech-Solutions,
How To Implant A Keraring
 Corneal Remodeling Using the Keraring A variety of thicknesses, arc lengths, and optical zone sizes allows tailoring of the procedure to the individual patient. BY DOMINIQUE PIETRINI, MD; AND TONY GUEDJ
Corneal Remodeling Using the Keraring A variety of thicknesses, arc lengths, and optical zone sizes allows tailoring of the procedure to the individual patient. BY DOMINIQUE PIETRINI, MD; AND TONY GUEDJ
Keratometric Changes after Corneal Collagen Cross linking for Keratoconus
 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Keratometric Changes after Corneal Collagen Cross linking for Keratoconus Muhemmed Swadique 1, Priya S 2, Sanju TS 3 1 Associate Professor, Dept.
Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Keratometric Changes after Corneal Collagen Cross linking for Keratoconus Muhemmed Swadique 1, Priya S 2, Sanju TS 3 1 Associate Professor, Dept.
New and Improved Femtosecond Laser Applications. Karl Stonecipher, MD Wavefront Congress 2008
 New and Improved Femtosecond Laser Applications Karl Stonecipher, MD Wavefront Congress 2008 When birds don t fly, neither should you. When cows bunch together in a field, a storm is coming. When ants
New and Improved Femtosecond Laser Applications Karl Stonecipher, MD Wavefront Congress 2008 When birds don t fly, neither should you. When cows bunch together in a field, a storm is coming. When ants
Collagen Cross-linking combined with PRK and LASIK
 Collagen Cross-linking combined with PRK and LASIK./*0&1#*!"#$%%&'&(%&)2*+,* +$345"%*,46$57&62*8")$694)4&#/:6*;#)%4#45"%*?6&@$))&62*ABC*8"#:&#$*+$345"%*D51&&%2*AB!"#$%%&'&(%&)*+,!
Collagen Cross-linking combined with PRK and LASIK./*0&1#*!"#$%%&'&(%&)2*+,* +$345"%*,46$57&62*8")$694)4&#/:6*;#)%4#45"%*?6&@$))&62*ABC*8"#:&#$*+$345"%*D51&&%2*AB!"#$%%&'&(%&)*+,!
Cornea and Refractive Surgery Update
 Cornea and Refractive Surgery Update Fall 2015 Optometric Education Dinner Sebastian Lesniak MD Matossian Eye Associates Disclosures: None Bio: Anterior Segment and Cornea Surgery Fellowship Wills Eye
Cornea and Refractive Surgery Update Fall 2015 Optometric Education Dinner Sebastian Lesniak MD Matossian Eye Associates Disclosures: None Bio: Anterior Segment and Cornea Surgery Fellowship Wills Eye
Intacs for keratoconus Yaron S. Rabinowitz
 Intacs for keratoconus Yaron S. Rabinowitz Purpose of review The use of Intacs as a therapeutic modality in contact lens intolerant patients with mild to moderate keratoconus is increasingly gaining acceptance
Intacs for keratoconus Yaron S. Rabinowitz Purpose of review The use of Intacs as a therapeutic modality in contact lens intolerant patients with mild to moderate keratoconus is increasingly gaining acceptance
Refractive Surgery Issue. Inlays and Presbyopia: On the Horizon P. 24. Crack a SMILE or Raise a Flap? P. 30. LASIK Xtra: Who Should Get It? P.
 MULTIMODAL IMAGING OF PLACOID DISORDERS P. 42 WILLS RESIDENT CASE SERIES P. 67 NTG: THE NOCTURNAL BLOOD PRESSURE FACTOR P. 54 WISE CHOICES FOR OCULAR DIAGNOSES P. 50 NEW WAYS TO DETECT KERATOCONUS P. 58
MULTIMODAL IMAGING OF PLACOID DISORDERS P. 42 WILLS RESIDENT CASE SERIES P. 67 NTG: THE NOCTURNAL BLOOD PRESSURE FACTOR P. 54 WISE CHOICES FOR OCULAR DIAGNOSES P. 50 NEW WAYS TO DETECT KERATOCONUS P. 58
Clinical Practice. Corneal Crosslinking with Riboflavin and Ultraviolet A. Part II. Clinical Indications and Results
 Clinical Practice JOHN E. SUTPHIN, MD, EDITOR Corneal Crosslinking with Riboflavin and Ultraviolet A. Part II. Clinical Indications and Results FREDERIK RAISKUP, MD, PHD, FEBO, AND EBERHARD SPOERL, PHD
Clinical Practice JOHN E. SUTPHIN, MD, EDITOR Corneal Crosslinking with Riboflavin and Ultraviolet A. Part II. Clinical Indications and Results FREDERIK RAISKUP, MD, PHD, FEBO, AND EBERHARD SPOERL, PHD
Sharjah: Al Zahra Private Hospital, Al Zahra square Tel: 06 5619999, Appointments: 06 5167080, 06 5167081
 Sharjah: Al Zahra Private Hospital, Al Zahra square Tel: 06 5619999, Appointments: 06 5167080, 06 5167081 Email: [email protected] Dubai: Al Zahra Medical Centre, Sheikh Zayed Road Tel: 04 3315000, Appointments:
Sharjah: Al Zahra Private Hospital, Al Zahra square Tel: 06 5619999, Appointments: 06 5167080, 06 5167081 Email: [email protected] Dubai: Al Zahra Medical Centre, Sheikh Zayed Road Tel: 04 3315000, Appointments:
Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery
 Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery Farhad Hafezi, MD; Michael Mrochen, PhD; Franz Fankhauser II, MD; Theo Seiler, MD, PhD
Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery Farhad Hafezi, MD; Michael Mrochen, PhD; Franz Fankhauser II, MD; Theo Seiler, MD, PhD
Corneal Transparency After Cross-linking for Keratoconus: 1-Year Follow-up
 Corneal Transparency After Cross-linking for Keratoconus: 1-Year Follow-up Ramon Gutiérrez, MD, PhD; Inma Lopez, MD; Cesar Villa-Collar, OD, PhD; José Manuel González-Méijome, OD, PhD ABSTRACT PURPOSE:
Corneal Transparency After Cross-linking for Keratoconus: 1-Year Follow-up Ramon Gutiérrez, MD, PhD; Inma Lopez, MD; Cesar Villa-Collar, OD, PhD; José Manuel González-Méijome, OD, PhD ABSTRACT PURPOSE:
Long-Term Outcomes of Flap Amputation After LASIK
 Long-Term Outcomes of Flap Amputation After LASIK Priyanka Chhadva BS, Florence Cabot MD, Anat Galor MD, Sonia H. Yoo MD Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami
Long-Term Outcomes of Flap Amputation After LASIK Priyanka Chhadva BS, Florence Cabot MD, Anat Galor MD, Sonia H. Yoo MD Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami
Refractive Surgery. Evolution of Refractive Error Correction
 Refractive Surgery Techniques that correct for refractive error in the eye have undergone dramatic evolution. The cornea is the easiest place to place a correction, so most techniques have focused on modifying
Refractive Surgery Techniques that correct for refractive error in the eye have undergone dramatic evolution. The cornea is the easiest place to place a correction, so most techniques have focused on modifying
ORIGINAL ARTICLES. Anastasios John Kanellopoulos, MD; Perry S. Binder, MS, MD
 ORIGINAL ARTICLES Management of Corneal Ectasia After LASIK With Combined, Same-day, Topographyguided Partial Transepithelial PRK and Collagen Cross-linking: The Athens Protocol Anastasios John Kanellopoulos,
ORIGINAL ARTICLES Management of Corneal Ectasia After LASIK With Combined, Same-day, Topographyguided Partial Transepithelial PRK and Collagen Cross-linking: The Athens Protocol Anastasios John Kanellopoulos,
Pentacam HR Criteria for Curvature Change in Keratoconus and Postoperative LASIK Ectasia
 Pentacam HR Criteria for Curvature Change in Keratoconus and Postoperative LASIK Ectasia Robert L. Epstein, MD, MSEE; Yi-Lin Chiu, PhD; Greg L. Epstein, BS ABSTRACT PURPOSE: To determine criteria for keratoconus
Pentacam HR Criteria for Curvature Change in Keratoconus and Postoperative LASIK Ectasia Robert L. Epstein, MD, MSEE; Yi-Lin Chiu, PhD; Greg L. Epstein, BS ABSTRACT PURPOSE: To determine criteria for keratoconus
Medicare and Corneal Surgery: Cosmetic versus Functional
 Medicare and Corneal Surgery: Cosmetic versus Functional Riva Lee Asbell INTRODUCTION With the introduction of several new CPT (Current Procedural Terminology) codes for cornea, corneal coding is in the
Medicare and Corneal Surgery: Cosmetic versus Functional Riva Lee Asbell INTRODUCTION With the introduction of several new CPT (Current Procedural Terminology) codes for cornea, corneal coding is in the
Sri Ganesh and Sheetal Brar. 1. Introduction. 2. Materials and Methods
 Ophthalmology Volume 215, Article ID 263412, 7 pages http://dx.doi.org/1.1155/215/263412 Clinical Study Clinical Outcomes of Small Incision Lenticule Extraction with Accelerated Cross-Linking (ReLEx SMILE
Ophthalmology Volume 215, Article ID 263412, 7 pages http://dx.doi.org/1.1155/215/263412 Clinical Study Clinical Outcomes of Small Incision Lenticule Extraction with Accelerated Cross-Linking (ReLEx SMILE
Corneal intrastromal implantation surgery for the treatment of moderate and high myopia
 TECHNIQUE Corneal intrastromal implantation surgery for the treatment of moderate and high myopia Albert Daxer, MD, PhD I describe a corneal intrastromal implantation technique that uses a new type of
TECHNIQUE Corneal intrastromal implantation surgery for the treatment of moderate and high myopia Albert Daxer, MD, PhD I describe a corneal intrastromal implantation technique that uses a new type of
Lasik Xtra Provides Corneal Stability and Improved Outcomes
 DOI 10.1007/s40123-015-0039-x REVIEW Lasik Xtra Provides Corneal Stability and Improved Outcomes Rajesh K. Rajpal. Christine B. Wisecarver. Dawn Williams. Sachin D. Rajpal. Rhonda Kerzner. Nick Nianiaris.
DOI 10.1007/s40123-015-0039-x REVIEW Lasik Xtra Provides Corneal Stability and Improved Outcomes Rajesh K. Rajpal. Christine B. Wisecarver. Dawn Williams. Sachin D. Rajpal. Rhonda Kerzner. Nick Nianiaris.
Daniel F. Goodman, M.D. 2211 Bush Street, 2nd Floor San Francisco, CA 94115 Phone: 415-474-3333 Fax: 415-474-3939
 Daniel F. Goodman, M.D. 2211 Bush Street, 2nd Floor San Francisco, CA 94115 Phone: 415-474-3333 Fax: 415-474-3939 INFORMED CONSENT FOR LASIK (LASER IN SITU KERATOMILEUSIS) and PRK (PHOTOREFRACTIVE KERATECTOMY)
Daniel F. Goodman, M.D. 2211 Bush Street, 2nd Floor San Francisco, CA 94115 Phone: 415-474-3333 Fax: 415-474-3939 INFORMED CONSENT FOR LASIK (LASER IN SITU KERATOMILEUSIS) and PRK (PHOTOREFRACTIVE KERATECTOMY)
Confocal Microscopy of Corneal Stroma and Endothelium After LASIK and PRK
 Confocal Microscopy of Corneal Stroma and Endothelium After LASIK and PRK Javad Amoozadeh, MD; Soheil Aliakbari, MD; Amir-Houshang Behesht-Nejad, MD; Mohammad-Amin Seyedian, MD; Bijan Rezvan, DDS; Hassan
Confocal Microscopy of Corneal Stroma and Endothelium After LASIK and PRK Javad Amoozadeh, MD; Soheil Aliakbari, MD; Amir-Houshang Behesht-Nejad, MD; Mohammad-Amin Seyedian, MD; Bijan Rezvan, DDS; Hassan
Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) John D. Goosey, MD Introduction DSAEK is a corneal transplant technique where the unhealthy, diseased, posterior portion of a patient s cornea
Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) John D. Goosey, MD Introduction DSAEK is a corneal transplant technique where the unhealthy, diseased, posterior portion of a patient s cornea
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment
 Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Page: 1 of 6. Corneal Topography/Computer-Assisted Corneal Topography/ Photokeratoscopy
 Section: Surgery Effective Date: July 15, 2015 Last Review Status/Date: June 2015 Page: 1 of 6 Corneal Topography/ Photokeratoscopy Description Computer-assisted topography/photokeratoscopy provides a
Section: Surgery Effective Date: July 15, 2015 Last Review Status/Date: June 2015 Page: 1 of 6 Corneal Topography/ Photokeratoscopy Description Computer-assisted topography/photokeratoscopy provides a
Keratoconus Lasers, Lenses & Boomerangs (the journey, missing links, and management & treatment options) Moderator: Jan P G Bergmanson, OD, PhD
 2014 AAO CCLRT Section Symposium Keratoconus Lasers, Lenses & Boomerangs (the journey, missing links, and management & treatment options) Moderator: Jan P G Bergmanson, OD, PhD Recurrent Keratoconus: Does
2014 AAO CCLRT Section Symposium Keratoconus Lasers, Lenses & Boomerangs (the journey, missing links, and management & treatment options) Moderator: Jan P G Bergmanson, OD, PhD Recurrent Keratoconus: Does
UPDATE ON AVEDRO CROSSLINKING STUDIES
 UPDATE ON AVEDRO CROSSLINKING STUDIES Peter S. Hersh, M.D. Director, Cornea & Laser Eye Institute CLEI Center for Keratoconus Clinical Professor of Ophthalmology, Rutgers Medical School Visiting Researcher,
UPDATE ON AVEDRO CROSSLINKING STUDIES Peter S. Hersh, M.D. Director, Cornea & Laser Eye Institute CLEI Center for Keratoconus Clinical Professor of Ophthalmology, Rutgers Medical School Visiting Researcher,
Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques
 Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques Julio Narváez MD Associate Professor of Ophthalmology Loma Linda University Non-Refractive Applications of Femtosecond
Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques Julio Narváez MD Associate Professor of Ophthalmology Loma Linda University Non-Refractive Applications of Femtosecond
THE BEST OF BOTH WORLDS Dual-Scheimpflug and Placido Reaching a new level in refractive screening
 THE BEST OF BOTH WORLDS Dual-Scheimpflug and Placido Reaching a new level in refractive screening GALILEI G4 Clinical Applications Corneal Implant Planning The comes with a licensable corneal inlay software
THE BEST OF BOTH WORLDS Dual-Scheimpflug and Placido Reaching a new level in refractive screening GALILEI G4 Clinical Applications Corneal Implant Planning The comes with a licensable corneal inlay software
REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES
 Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM
 1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY
 Thi-Qar Medical Journal (TQMJ): Vol(4) No(4):1(14-21) SUMMARY: LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY Dr. Ali Jawad AL- Gidis (M.B.Ch.B., D.O., F.I.C.O.)* Background: LASIK which
Thi-Qar Medical Journal (TQMJ): Vol(4) No(4):1(14-21) SUMMARY: LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY Dr. Ali Jawad AL- Gidis (M.B.Ch.B., D.O., F.I.C.O.)* Background: LASIK which
ALTERNATIVES TO LASIK
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
Risks and Limitations of LASIK Procedure
 Drs. Fine, Hoffman & Packer, LLC 1550 Oak Street, Suite #5 Eugene, OR 97401 541-687-2110 From Drs. Fine, Hoffman, & Packer Risks and Limitations of LASIK Procedure Infection, serious injury, or even death,
Drs. Fine, Hoffman & Packer, LLC 1550 Oak Street, Suite #5 Eugene, OR 97401 541-687-2110 From Drs. Fine, Hoffman, & Packer Risks and Limitations of LASIK Procedure Infection, serious injury, or even death,
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com
 Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
EPITHELIAL BASEMENT MEMBRANE DYSTROPHY IS THE
 Sloughing of Corneal Epithelium and Wound Healing Complications Associated With Laser In Situ Keratomileusis in Patients With Epithelial Basement Membrane Dystrophy K. ALEXANDER DASTGHEIB, MD, THOMAS E.
Sloughing of Corneal Epithelium and Wound Healing Complications Associated With Laser In Situ Keratomileusis in Patients With Epithelial Basement Membrane Dystrophy K. ALEXANDER DASTGHEIB, MD, THOMAS E.
Laser in situ keratomileusis (LASIK)
 Corneal Stromal Changes Induced by Myopic LASIK Minna Vesaluoma, 1 Juan Pérez Santonja, 2 W. Matthew Petroll, 3 Tuuli Linna, 1 Jorge Alió, 2 and Timo Tervo 1 PURPOSE. Despite the rapidly growing popularity
Corneal Stromal Changes Induced by Myopic LASIK Minna Vesaluoma, 1 Juan Pérez Santonja, 2 W. Matthew Petroll, 3 Tuuli Linna, 1 Jorge Alió, 2 and Timo Tervo 1 PURPOSE. Despite the rapidly growing popularity
LASIK, Epi LASIK and PRK Past present and future
 LASIK, Epi LASIK and PRK Past present and future Ioannis G. Pallikaris MD, PhD Institute of Vision and Optics University of Crete Medical School Heraklion Crete Greece Photorefractive Keratectomy Kerr-Muir
LASIK, Epi LASIK and PRK Past present and future Ioannis G. Pallikaris MD, PhD Institute of Vision and Optics University of Crete Medical School Heraklion Crete Greece Photorefractive Keratectomy Kerr-Muir
The pinnacle of refractive performance.
 Introducing! The pinnacle of refractive performance. REFRACTIVE SURGERY sets a new standard in LASIK outcomes More than 98% of patients would choose it again. 1 It even outperformed glasses and contacts
Introducing! The pinnacle of refractive performance. REFRACTIVE SURGERY sets a new standard in LASIK outcomes More than 98% of patients would choose it again. 1 It even outperformed glasses and contacts
OCT-guided Femtosecond Laser for LASIK and Presbyopia Treatment
 Shinagawa LASIK Center OCT-guided Femtosecond Laser for LASIK and Presbyopia Treatment Minoru Tomita, MD, Ph.D 1) Executive Medical Director at Shinagawa LASIK Center, Tokyo, Japan 2) Clinical Professor
Shinagawa LASIK Center OCT-guided Femtosecond Laser for LASIK and Presbyopia Treatment Minoru Tomita, MD, Ph.D 1) Executive Medical Director at Shinagawa LASIK Center, Tokyo, Japan 2) Clinical Professor
