UnitedHealthcare Community Plan (UHCCP) PSYCHOSOCIAL REHAB RECORD AUDIT TOOL
|
|
|
- Gervais Phelps
- 10 years ago
- Views:
Transcription
1 October-15 UnitedHealthcare Community Plan (UHCCP) PSYCHOSOCIAL REHAB RECORD AUDIT TOOL Provider Name: Reviewer Name: Date of Review: Rating Scale: NA = Not Applicable Y = Yes N = No Y N NA General Documentation Standards 1 Each member has a separate record. 2 Each record includes the member's address, employer or school, home and work telephone numbers including emergency contacts, relationship or legal status, and guardianship information if relevant. 3 All entries in the record include the responsible service provider's name, professional degree and relevant identification number, if applicable, and dated and signed where appropriate. 4 The record is clearly legible to someone other than the writer. 5 There is evidence of a Consent for Treatment or Informed Consent in the record that is signed by the member and/or legal guardian. 6 There is documentation that the service provider provides education to member/family about service planning, discharge planning, supportive community services, behavioral health problems, and care options. 7 There is documentation that the potential risks of not following treatment recommendations are discussed with the member and/or family or legal guardian.
2 Initial Assessment 8 The reasons for initiation of services are documented. 9 A psychiatric diagnosis is included in the record. 10 A behavioral health history is in the record. 11 A medical history and/or physical exam, along with documentation of any infectious diseases, is in the record. 12 Was a current medical condition identified? This is a non-scored question. (If #11 is no, then 12 is NA) 13 If a medical condition was identified, there is documentation that communication/collaboration with the treating medical clinician occurred. This is a non-scored question. 14 If a medical condition was identified, there is documentation that the member/guardian refused consent for the release of information to the treating medical clinician. This is a non-scored question. 15 The presence or absence of drug allergies and food allergies, including adverse reactions, is clearly documented. 16 The assessment documents the spiritual variables that may impact services
3 17 The assessment documents the cultural variables that may impact services 18 An educational assessment appropriate to the age of the member and level of service is documented. 19 The assessment includes evidence the member identified the skills and resources they wanted to develop. 20 There is documentation of an assessment of the member's level of functioning in the domains of Activities of Daily Living. 21 For members 12 years and older, a screening is in evidence of use or exposure to alcohol, nicotine, and/or illicit drugs. 22 The record documents the presence or absence of relevant legal issues of the member and/or family. 23 There is documentation that the member was asked about community resources (support groups, social services, school based services, other social supports) that they are currently utilizing. 24 There is documentation of a screening for risk issues in the record. 25 When risk issues are identified, there is evidence that an initial safety plan has been developed. Service Planning
4 26 There is evidence that the results of the assessment are considered in the development of the service plan. 27 The service plan is consistent with diagnosis and has BOTH objective and measurable goals. short and long term goals. 28 The service plan is consistent with diagnosis and has BOTH short and long term goals. 29 The service plan includes a safety plan when active risk issues are identified. 30 There is evidence the service plan was reviewed with the member; there is evidence that the member agrees with the service plan. 31 There is evidence that the service plan is reviewed and updated at regular intervals. Progress Notes 32 All progress notes include the date of service. 33 All progress notes include the time of service provided. 34 Progress notes include assessment of how activities relate to the service plan goals. 35 The progress notes describe progress or lack of progress towards service plan goals.
5 36 All progress notes include who rendered services. 37 All progress notes include ongoing monitoring of risk issues, including, but not limited to self-harm or harm to others. 38 Progress notes include an ongoing assessment of the member's capacity to complete ADL's. 39 As appropriate, progress notes document assessment of any additional services needed by the member. Coordination of Care 40 Does the member have a medical physician (PCP)? This is a non-scored question. 41 The record documents that the member was asked whether they have a PCP. Y or N Only 42 If the member has a PCP there is documentation that communication/collaboration occurred. 43 If the member has a PCP, there is documentation that the member/guardian refused consent for the release of information to the PCP. 44 Is the member being seen by another behavioral health clinician (e.g. psychiatrist and social worker, psychologist and substance abuse counselor). This is a non-scored question.
6 45 The record documents that the member was asked whether they are being seen by another behavioral health clinician. Y or N Only 46 If the member is being seen by another behavioral health clinician, there is documentation that communication/collaboration occurred. 47 If the member is being seen by another behavioral health clinician, there is documentation that the member/guardian refused consent for the release of information to the behavioral health clinician. Discharge and Transfer 48 Was the member transferred/discharged to another clinician or program? This is a non-scored question. 49 If the member was transferred/discharged to another clinician or program, there is documentation that communication/collaboration occurred with the receiving clinician/program. 50 If the member was transferred/discharged to another clinician or program, there is documentation that the member/guardian refused consent for release of information to the receiving clinician/program. 51 Prompt referrals to the appropriate level of care are documented when member cannot be safely treated at their current level of care secondary to homicidal or suicidal risk or an inability to conduct activities of daily living. 52 The discharge plan summarizes the reason(s) for treatment and the extent to which treatment goals were met. 53 The discharge/aftercare/safety plan describes specific follow up activities.
7 54 Clinical records are completed within 30 days following discharge.
Technical Assistance Document 5
 Technical Assistance Document 5 Information Sharing with Family Members of Adult Behavioral Health Recipients Developed by the Arizona Department of Health Services Division of Behavioral Health Services
Technical Assistance Document 5 Information Sharing with Family Members of Adult Behavioral Health Recipients Developed by the Arizona Department of Health Services Division of Behavioral Health Services
Substance Abuse Services (Outpatient)
 RYAN WHITE PART B PEER REVIEW 2009-2010 Virginia Department of Health Division of Disease Prevention HIV Care Services Chart Review Substance Abuse Services (Outpatient) ID# 1. Is there referral in the
RYAN WHITE PART B PEER REVIEW 2009-2010 Virginia Department of Health Division of Disease Prevention HIV Care Services Chart Review Substance Abuse Services (Outpatient) ID# 1. Is there referral in the
Addiction Psychiatry Fellowship Rotation Goals & Objectives
 Addiction Psychiatry Fellowship Rotation Goals & Objectives Table of Contents University Neuropsychiatric Institute (UNI) Training Site 2 Inpatient addiction psychiatry rotation.....2 Outpatient addiction
Addiction Psychiatry Fellowship Rotation Goals & Objectives Table of Contents University Neuropsychiatric Institute (UNI) Training Site 2 Inpatient addiction psychiatry rotation.....2 Outpatient addiction
Administrative Guide
 Community Plan KanCare Program Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide Doc#: PCA15026_20141201 UHCCommunityPlan.com Welcome to UnitedHealthcare This administrative
Community Plan KanCare Program Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide Doc#: PCA15026_20141201 UHCCommunityPlan.com Welcome to UnitedHealthcare This administrative
Policy and Procedure Manual
 Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 RA-13 Admission. History, Physicals and Routine Health Care
Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 RA-13 Admission. History, Physicals and Routine Health Care
TEXAS FAMILY CODE CHAPTER 32. CONSENT TO TREATMENT OF CHILD BY NON PARENT OR CHILD
 TEXAS FAMILY CODE CHAPTER 32. CONSENT TO TREATMENT OF CHILD BY NON PARENT OR CHILD SUBCHAPTER A. CONSENT TO MEDICAL, DENTAL, PSYCHOLOGICAL, AND SURGICAL TREATMENT 32.001. Consent by Non-Parent (a) The
TEXAS FAMILY CODE CHAPTER 32. CONSENT TO TREATMENT OF CHILD BY NON PARENT OR CHILD SUBCHAPTER A. CONSENT TO MEDICAL, DENTAL, PSYCHOLOGICAL, AND SURGICAL TREATMENT 32.001. Consent by Non-Parent (a) The
Policy and Procedure Manual
 Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 Physical Health Services Dental Services Initial Nursing Summary
Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 Physical Health Services Dental Services Initial Nursing Summary
Provider Evaluation of Performance. Plan. Tennessee
 Provider Evaluation of Performance Plan Tennessee 2015 Executive Summary UnitedHealthcare Community Plan is committed to ensuring the services members receive from network providers meet the requirements
Provider Evaluation of Performance Plan Tennessee 2015 Executive Summary UnitedHealthcare Community Plan is committed to ensuring the services members receive from network providers meet the requirements
Psychiatric Consultants of Atlanta, P.C. 1835 Savoy Drive Suite 101 Atlanta, Georgia 30341 Phone: 770-234-0981 Fax: 770-234-0252 www.pcatl.
 Psychiatric Consultants of Atlanta, P.C. 1835 Savoy Drive Suite 101 Atlanta, Georgia 30341 Phone: 770-234-0981 Fax: 770-234-0252 www.pcatl.com CONTACT INFORMATION AND PERSONAL DATA Name: Date of Birth:
Psychiatric Consultants of Atlanta, P.C. 1835 Savoy Drive Suite 101 Atlanta, Georgia 30341 Phone: 770-234-0981 Fax: 770-234-0252 www.pcatl.com CONTACT INFORMATION AND PERSONAL DATA Name: Date of Birth:
Transitional Grant Area (TGA) Definition
 S OF CARE Oakland Transitional Grant Area Care and Treatment Services O CTOBER 2006 Office of AIDS Administration 1000 Broadway, Suite 310 Oakland, CA 94607 Tel: 510.268.7630 Fax: 510.268.7631 AREAS OF
S OF CARE Oakland Transitional Grant Area Care and Treatment Services O CTOBER 2006 Office of AIDS Administration 1000 Broadway, Suite 310 Oakland, CA 94607 Tel: 510.268.7630 Fax: 510.268.7631 AREAS OF
Substance Abuse Treatment Record Review Presentation
 Substance Abuse Treatment Record Review Presentation January 15, 2015 Presented by Melissa Reagan, M.S.W., L.S.W., Quality Management Specialist & Rebecca Rager, M.S.W., Quality Management Specialist Please
Substance Abuse Treatment Record Review Presentation January 15, 2015 Presented by Melissa Reagan, M.S.W., L.S.W., Quality Management Specialist & Rebecca Rager, M.S.W., Quality Management Specialist Please
Assessment of depression in adults in primary care
 Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
McLean Ambulatory Treatment Center Adult Partial Hospital and Residential Program for Alcohol and Drug Abuse 11 Mill Street Belmont, MA 02478-9106
 Program Description Staffed by highly experienced psychiatrists, psychologists, social workers, nurses and addiction specialists, we are committed to working collaboratively with referring providers. Program
Program Description Staffed by highly experienced psychiatrists, psychologists, social workers, nurses and addiction specialists, we are committed to working collaboratively with referring providers. Program
Performance Standards
 Performance Standards Outpatient Performance Standards are intended to provide a foundation and serve as a tool to promote continuous quality improvement and progression toward best practice performances,
Performance Standards Outpatient Performance Standards are intended to provide a foundation and serve as a tool to promote continuous quality improvement and progression toward best practice performances,
Provider Manual Section 4.0 Office Standards
 Provider Manual Section 4.0 Office Standards Table of Contents 4.1 Appointment Scheduling Standards 4.2 After-Hours Telephone Coverage 4.3 Member to Practitioner Ratio Maximum 4.4 Provider Office Standards
Provider Manual Section 4.0 Office Standards Table of Contents 4.1 Appointment Scheduling Standards 4.2 After-Hours Telephone Coverage 4.3 Member to Practitioner Ratio Maximum 4.4 Provider Office Standards
Minor Rights: Access and Consent to Health Care
 Minor Rights: Access and Consent to Health Care A resource for providers, parents and educators Not a legal document. This resource is intended to provide basic information about minors ability to consent
Minor Rights: Access and Consent to Health Care A resource for providers, parents and educators Not a legal document. This resource is intended to provide basic information about minors ability to consent
MEDICAL POLICY No. 91608-R1 MENTAL HEALTH RESIDENTIAL TREATMENT: ADULT
 MENTAL HEALTH RESIDENTIAL TREATMENT: ADULT Effective Date: June 4, 2015 Review Dates: 5/14, 5/15 Date Of Origin: May 12, 2014 Status: Current Summary of Changes Clarifications: Pg 4, Description, updated
MENTAL HEALTH RESIDENTIAL TREATMENT: ADULT Effective Date: June 4, 2015 Review Dates: 5/14, 5/15 Date Of Origin: May 12, 2014 Status: Current Summary of Changes Clarifications: Pg 4, Description, updated
McLean Ambulatory Treatment Center Adult Partial Hospital and Residential Program for Alcohol and Drug Abuse 115 Mill Street Belmont, MA 02478-9106
 Program Description Staffed by highly experienced psychiatrists, psychologists, social workers, nurses and addiction specialists, we are committed to working collaboratively with referring providers. Program
Program Description Staffed by highly experienced psychiatrists, psychologists, social workers, nurses and addiction specialists, we are committed to working collaboratively with referring providers. Program
Medical Record Documentation Standards
 Medical Record Documentation Standards Medical Record Documentation Standards and Performance Measures Compliance with the Standards is monitored as part of our Quality Improvement Program. Practitioner
Medical Record Documentation Standards Medical Record Documentation Standards and Performance Measures Compliance with the Standards is monitored as part of our Quality Improvement Program. Practitioner
Pediatric and Adolescent Medical Record Review Tool
 Pediatric and Adolescent Medical Record Review Tool Primary Care Provider: Member Name: DOB: Provider Name: Provider ID #: Product: Date of Review: Initials of Reviewer: The Medical Record contains the
Pediatric and Adolescent Medical Record Review Tool Primary Care Provider: Member Name: DOB: Provider Name: Provider ID #: Product: Date of Review: Initials of Reviewer: The Medical Record contains the
SENATE BILL 850. By Black BE IT ENACTED BY THE GENERAL ASSEMBLY OF THE STATE OF TENNESSEE:
 SENATE BILL 850 By Black AN ACT to amend Tennessee Code Annotated, Title 9, Chapter 4 and Title 49, Chapter 2, Part 1, relative to mental health testing. BE IT ENACTED BY THE GENERAL ASSEMBLY OF THE STATE
SENATE BILL 850 By Black AN ACT to amend Tennessee Code Annotated, Title 9, Chapter 4 and Title 49, Chapter 2, Part 1, relative to mental health testing. BE IT ENACTED BY THE GENERAL ASSEMBLY OF THE STATE
Downloadable Forms: Otsego County Chemical Dependencies Clinic. Client Handbook. Revised 04/10
 Downloadable Forms: Otsego County Chemical Dependencies Clinic Client Handbook Revised 04/10 OTSEGO CHEMICAL DEPENDENCIES CLINIC 242 Main St, 2 nd Floor Oneonta, New York 13820 Tel. (607) 431-1030 Fax.
Downloadable Forms: Otsego County Chemical Dependencies Clinic Client Handbook Revised 04/10 OTSEGO CHEMICAL DEPENDENCIES CLINIC 242 Main St, 2 nd Floor Oneonta, New York 13820 Tel. (607) 431-1030 Fax.
Outline. Drug and Alcohol Counseling 1 Module 1 Basics of Abuse & Addiction
 Outline Drug and Alcohol Counseling 1 Module 1 Basics of Abuse & Addiction About Substance Abuse The Cost of Chemical Abuse/Addiction Society's Response The Continuum of Chemical Use Definitions of Terms
Outline Drug and Alcohol Counseling 1 Module 1 Basics of Abuse & Addiction About Substance Abuse The Cost of Chemical Abuse/Addiction Society's Response The Continuum of Chemical Use Definitions of Terms
Who Can Diagnose R9-20-204. Staff Member and Employee Qualifications and Records
 "Behavioral health paraprofessional" means an individual who meets the applicable requirements in R9-20-204 and has: a. An associate's degree, b. A high school diploma, or c. A high school equivalency
"Behavioral health paraprofessional" means an individual who meets the applicable requirements in R9-20-204 and has: a. An associate's degree, b. A high school diploma, or c. A high school equivalency
Steele Street Treatment and Rehabilitation Residence
 Steele Street Referral Package 1 Program overview Steele Street Treatment and Rehabilitation Residence The Steele Street Treatment and Rehabilitation residence is one of the services offered by St. Joseph
Steele Street Referral Package 1 Program overview Steele Street Treatment and Rehabilitation Residence The Steele Street Treatment and Rehabilitation residence is one of the services offered by St. Joseph
Admission Application
 Admission Application Kids in Focus Girls in Focus Little Kids in Focus Little Kids in Focus II Kids in Focus II Instructions: When completing the application please do not leave blanks. If the requested
Admission Application Kids in Focus Girls in Focus Little Kids in Focus Little Kids in Focus II Kids in Focus II Instructions: When completing the application please do not leave blanks. If the requested
Fax # s for CAMH programs and services
 INFORMATION AND INSTRUCTIONS STEP 1 BEFORE COMPLETING THE REFERRAL FORM CATS Program / General Psychiatry Memory Clinic, Geriatric Mental Health Program Go to www.camh.net for detailed information on each
INFORMATION AND INSTRUCTIONS STEP 1 BEFORE COMPLETING THE REFERRAL FORM CATS Program / General Psychiatry Memory Clinic, Geriatric Mental Health Program Go to www.camh.net for detailed information on each
Title 10 DEPARTMENT OF HEALTH AND MENTAL HYGIENE
 FINAL Maryland Register Issue Date: November 1, 2013 Volume 40 Issue 22 Page 1878 Title 10 DEPARTMENT OF HEALTH AND MENTAL HYGIENE Subtitle 58 BOARD OF PROFESSIONAL COUNSELORS AND THERAPISTS 10.58.14 Supervision
FINAL Maryland Register Issue Date: November 1, 2013 Volume 40 Issue 22 Page 1878 Title 10 DEPARTMENT OF HEALTH AND MENTAL HYGIENE Subtitle 58 BOARD OF PROFESSIONAL COUNSELORS AND THERAPISTS 10.58.14 Supervision
Day Treatment Mental Health Adult
 Day Treatment Mental Health Adult Definition Day Treatment provides a community based, coordinated set of individualized treatment services to individuals with psychiatric disorders who are not able to
Day Treatment Mental Health Adult Definition Day Treatment provides a community based, coordinated set of individualized treatment services to individuals with psychiatric disorders who are not able to
[Provider or Facility Name]
![[Provider or Facility Name] [Provider or Facility Name]](/thumbs/24/2833314.jpg) [Provider or Facility Name] SECTION: [Facility Name] Residential Treatment Facility (RTF) SUBJECT: Psychiatric Security Review Board (PSRB) In compliance with OAR 309-032-0450 Purpose and Statutory Authority
[Provider or Facility Name] SECTION: [Facility Name] Residential Treatment Facility (RTF) SUBJECT: Psychiatric Security Review Board (PSRB) In compliance with OAR 309-032-0450 Purpose and Statutory Authority
SUBSTANCE ABUSE OUTPATIENT SERVICES
 SUBSTANCE ABUSE OUTPATIENT SERVICES A. DEFINITION: Substance Abuse Outpatient is the provision of medical or other treatment and/or counseling to address substance abuse problems (i.e., alcohol and/or
SUBSTANCE ABUSE OUTPATIENT SERVICES A. DEFINITION: Substance Abuse Outpatient is the provision of medical or other treatment and/or counseling to address substance abuse problems (i.e., alcohol and/or
American Society of Addiction Medicine
 American Society of Addiction Medicine Public Policy Statement on Treatment for Alcohol and Other Drug Addiction 1 I. General Definitions of Addiction Treatment Addiction Treatment is the use of any planned,
American Society of Addiction Medicine Public Policy Statement on Treatment for Alcohol and Other Drug Addiction 1 I. General Definitions of Addiction Treatment Addiction Treatment is the use of any planned,
ADULT REGISTRATION FORM. Last Name First Name Middle Initial. Date of Birth Age Identified Gender. Street Address. City State Zip Code
 ADULT REGISTRATION FORM Last Name First Name Middle Initial Date of Birth Age Identified Gender Street Address City State Zip Code Home Phone Cell Phone FINANCIALLY RESPONSIBLE PARTY (If different from
ADULT REGISTRATION FORM Last Name First Name Middle Initial Date of Birth Age Identified Gender Street Address City State Zip Code Home Phone Cell Phone FINANCIALLY RESPONSIBLE PARTY (If different from
Parent Intake Packet 11 pages total 1 Atlanta Center for Eating Disorders Patient Registration Information. Patient Name: Date:
 Parent Intake Packet 11 pages total 1 Patient Registration Information Patient Name: Date: Address: City: State: Zip: Phone# Home ( ) Work ( ) Cell ( ) May we leave you a message at home? at work? on cell?
Parent Intake Packet 11 pages total 1 Patient Registration Information Patient Name: Date: Address: City: State: Zip: Phone# Home ( ) Work ( ) Cell ( ) May we leave you a message at home? at work? on cell?
IRVING & ASSOCIATES IN BEHAVIORAL HEALTH, P.C. 5151 Mochel Drive, Suite 307 Downers Grove, IL 60515
 : / / Client Name: _ SSN: / / of Birth: Age: Sex: Male Female Address: City/State/Zip: Home Phone Number Is it okay to leave a message here? Y/N Work Number Is it okay to leave a message here? Y/N Cell
: / / Client Name: _ SSN: / / of Birth: Age: Sex: Male Female Address: City/State/Zip: Home Phone Number Is it okay to leave a message here? Y/N Work Number Is it okay to leave a message here? Y/N Cell
REFERRAL INFORMATION CHILD, YOUTH AND FAMILY PROGRAM
 Please Note the following information: WE DO NOT OFFER EMERGENCY OR CRISIS SERVICE Please print clearly and ensure contact information is correct. Complete all forms. We will contact the family to set
Please Note the following information: WE DO NOT OFFER EMERGENCY OR CRISIS SERVICE Please print clearly and ensure contact information is correct. Complete all forms. We will contact the family to set
AmeriHealth Caritas District of Columbia Psychiatric Residential Treatment Facility Referral
 AmeriHealth Caritas District of Columbia Psychiatric Residential Treatment Facility Referral Date of referral: Psychiatric Residential Treatment Facility (PRTF) Referral Information Referral contact: Phone
AmeriHealth Caritas District of Columbia Psychiatric Residential Treatment Facility Referral Date of referral: Psychiatric Residential Treatment Facility (PRTF) Referral Information Referral contact: Phone
Patient Registration Please Print Patient Name Last First Middle
 Patient Registration Please Print Patient Name Last First Middle Address City Zip Home Phone Work Ext Cell Birthdate - - Social Security # - - Gender Marital Status Employer Referred by_emergency Contact
Patient Registration Please Print Patient Name Last First Middle Address City Zip Home Phone Work Ext Cell Birthdate - - Social Security # - - Gender Marital Status Employer Referred by_emergency Contact
Working Together HEALTH SERVICES FOR CHILDREN IN FOSTER CARE
 Chapter Eight Maintaining Health Records Maintaining the health records of children in foster care is critical to providing and monitoring health care on an ongoing basis. When health records are maintained
Chapter Eight Maintaining Health Records Maintaining the health records of children in foster care is critical to providing and monitoring health care on an ongoing basis. When health records are maintained
CONSENT FOR HEALTHCARE SERVICES OF A MINOR
 Wellness Center CONSENT FOR HEALTHCARE SERVICES OF A MINOR I, the parent/guardian/legal representative, agree to the following on behalf of myself and the patient: 1. Scope of Available Services. I have
Wellness Center CONSENT FOR HEALTHCARE SERVICES OF A MINOR I, the parent/guardian/legal representative, agree to the following on behalf of myself and the patient: 1. Scope of Available Services. I have
Partial Hospitalization - MH - Adult (Managed Medicaid only Service)
 Partial Hospitalization - MH - Adult (Managed Medicaid only Service) Definition Partial hospitalization is a nonresidential treatment program that is hospital-based. The program provides diagnostic and
Partial Hospitalization - MH - Adult (Managed Medicaid only Service) Definition Partial hospitalization is a nonresidential treatment program that is hospital-based. The program provides diagnostic and
Intensive Outpatient Psychotherapy - Adult
 Intensive Outpatient Psychotherapy - Adult Definition Intensive Outpatient Psychotherapy services provide group based, non-residential, intensive, structured interventions consisting primarily of counseling
Intensive Outpatient Psychotherapy - Adult Definition Intensive Outpatient Psychotherapy services provide group based, non-residential, intensive, structured interventions consisting primarily of counseling
Behavioral Health Medical Necessity Criteria
 Behavioral Health Medical Necessity Criteria Revised: 7/14/05 2 nd Revision: 9/14/06 3 rd Revision: 8/23/07 4 th Revision: 8/28/08; 11/20/08 5 th Revision: 8/27/09 Anthem Blue Cross and Blue Shield 2 Gannett
Behavioral Health Medical Necessity Criteria Revised: 7/14/05 2 nd Revision: 9/14/06 3 rd Revision: 8/23/07 4 th Revision: 8/28/08; 11/20/08 5 th Revision: 8/27/09 Anthem Blue Cross and Blue Shield 2 Gannett
Behavioral Health Services 14.0
 Behavioral Health Services 14.0 Kaiser Permanente s Behavioral Health Services operates within the multi-specialty Mid- Atlantic Permanente Medical Group (MAPMG). It is a regional service committed to
Behavioral Health Services 14.0 Kaiser Permanente s Behavioral Health Services operates within the multi-specialty Mid- Atlantic Permanente Medical Group (MAPMG). It is a regional service committed to
How To Get A Mental Health Care Plan In Vermont
 Agency of Human Services STANDARD OPERATING PROCEDURES MANUAL FOR VERMONT MEDICAID INPATIENT PSYCHIATRIC AND DETOXIFICATION AUTHORIZATIONS Department of Vermont Health Access Department of Mental Health
Agency of Human Services STANDARD OPERATING PROCEDURES MANUAL FOR VERMONT MEDICAID INPATIENT PSYCHIATRIC AND DETOXIFICATION AUTHORIZATIONS Department of Vermont Health Access Department of Mental Health
Numerator Details. - An acute or nonacute inpatient admission with a diagnosis of AOD (AOD Dependence
 Description Measure 0004: Initiation and Engagement of Alcohol and Other Drug Dependence Treatment (IET) (National Committee for Quality Assurance) The percentage of adolescent and adult patients with
Description Measure 0004: Initiation and Engagement of Alcohol and Other Drug Dependence Treatment (IET) (National Committee for Quality Assurance) The percentage of adolescent and adult patients with
STANDARD OPERATING PROCEDURES MANUAL FOR VERMONT MEDICAID INPATIENT PSYCHIATRIC AND DETOXIFICATION AUTHORIZATIONS
 Agency of Human Services STANDARD OPERATING PROCEDURES MANUAL FOR VERMONT MEDICAID INPATIENT PSYCHIATRIC AND DETOXIFICATION AUTHORIZATIONS Department of Vermont Health Access Department of Mental Health
Agency of Human Services STANDARD OPERATING PROCEDURES MANUAL FOR VERMONT MEDICAID INPATIENT PSYCHIATRIC AND DETOXIFICATION AUTHORIZATIONS Department of Vermont Health Access Department of Mental Health
Telemedicine, Wellness, Intervention, Triage and Referral
 Telemedicine, Wellness, Intervention, Triage and Referral Travis Hanson, JD, MS Executive Director, TTUHSC Innovative Healthcare Transformation 2013-2015 TWITR Project. The Texas Office of the Governor
Telemedicine, Wellness, Intervention, Triage and Referral Travis Hanson, JD, MS Executive Director, TTUHSC Innovative Healthcare Transformation 2013-2015 TWITR Project. The Texas Office of the Governor
BEACON HEALTH STRATEGIES, LLC TELEHEALTH PROGRAM SPECIFICATION
 BEACON HEALTH STRATEGIES, LLC TELEHEALTH PROGRAM SPECIFICATION Providers contracted for the telehealth service will be expected to comply with all requirements of the performance specifications. Additionally,
BEACON HEALTH STRATEGIES, LLC TELEHEALTH PROGRAM SPECIFICATION Providers contracted for the telehealth service will be expected to comply with all requirements of the performance specifications. Additionally,
DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource
 E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
James A. Purvis, Ph.D. Psychotherapy Services Agreement
 James A. Purvis, Ph.D. Psychotherapy Services Agreement PSYCHOLOGICAL SERVICES Psychotherapy is not easily described in general statements. It varies depending on the personalities of the psychologist
James A. Purvis, Ph.D. Psychotherapy Services Agreement PSYCHOLOGICAL SERVICES Psychotherapy is not easily described in general statements. It varies depending on the personalities of the psychologist
Mosaic Arlington Counseling Center 817 W. Park Row Arlington, Texas 76013 Phone: (817) 929-3408 NEW CLIENT INFORMATION
 NEW CLIENT INFORMATION (Please Print) / / Client Name M/ F of Birth Address City/State Zip Home ( ) Work ( ) Cell ( ) Email Address: (Circle One) Minor Single Married Divorced Separated Widow Living Together
NEW CLIENT INFORMATION (Please Print) / / Client Name M/ F of Birth Address City/State Zip Home ( ) Work ( ) Cell ( ) Email Address: (Circle One) Minor Single Married Divorced Separated Widow Living Together
Mental Disorders (Except initial PTSD and Eating Disorders) Examination
 Mental Disorders (Except initial PTSD and Eating Disorders) Examination Name: Date of Exam: SSN: C-number: Place of Exam: The following health care providers can perform initial examinations for Mental
Mental Disorders (Except initial PTSD and Eating Disorders) Examination Name: Date of Exam: SSN: C-number: Place of Exam: The following health care providers can perform initial examinations for Mental
Dartmouth Medical School Curricular Content in Addiction Medicine for Medical Students (DCAMMS) Keyed to LCME Core Competency Domains ***Draft***
 Dartmouth Medical School Curricular Content in Addiction Medicine for Medical Students (DCAMMS) Keyed to LCME Core Competency Domains ***Draft*** This content, sorted by LCME competencies is intended to
Dartmouth Medical School Curricular Content in Addiction Medicine for Medical Students (DCAMMS) Keyed to LCME Core Competency Domains ***Draft*** This content, sorted by LCME competencies is intended to
REHAB XCEL, LLC. NEW PATIENT INFORMATION
 REHAB XCEL, LLC. NEW PATIENT INFORMATION DATE: NAME: LAST: FIRST: MID: MAIL ADDRESS: HOME PHONE: CELL PHONE: WORK PHONE: DATE OF BIRTH: SS# SEX: M OR F EMERGENCY CONTACT: PHONE: MARITAL STATUS: M OR S
REHAB XCEL, LLC. NEW PATIENT INFORMATION DATE: NAME: LAST: FIRST: MID: MAIL ADDRESS: HOME PHONE: CELL PHONE: WORK PHONE: DATE OF BIRTH: SS# SEX: M OR F EMERGENCY CONTACT: PHONE: MARITAL STATUS: M OR S
Performance Standards
 Performance Standards Clinical Telemedicine Services Performance Standards are intended to provide a foundation and serve as a tool to promote continuous quality improvement and progression toward best
Performance Standards Clinical Telemedicine Services Performance Standards are intended to provide a foundation and serve as a tool to promote continuous quality improvement and progression toward best
David A. Wang, MD Primary Care Sports Medicine Physician PRINT NAME: ADDRESS: DOB: AGE: SEX: SS# HOME: MOBILE PHONE: WORK: FAX:
 David A. Wang, MD Primary Care Sports Medicine Physician PRINT NAME: ADDRESS: DOB: AGE: SEX: SS# HOME: MOBILE PHONE: WORK: FAX: INSURANCE INFORMATION Did you injure yourself at work or is this injury a
David A. Wang, MD Primary Care Sports Medicine Physician PRINT NAME: ADDRESS: DOB: AGE: SEX: SS# HOME: MOBILE PHONE: WORK: FAX: INSURANCE INFORMATION Did you injure yourself at work or is this injury a
Self-Advocacy Guide: Individual Service Planning for Individuals with a Serious Mental Illness in Arizona s Public Behavioral Health System
 Self-Advocacy Guide: Individual Service Planning for Individuals with a Serious Mental Illness in Arizona s Public Behavioral Health System Arizona Department of Health Services/Division of Behavioral
Self-Advocacy Guide: Individual Service Planning for Individuals with a Serious Mental Illness in Arizona s Public Behavioral Health System Arizona Department of Health Services/Division of Behavioral
Initial Evaluation for Post-Traumatic Stress Disorder Examination
 Initial Evaluation for Post-Traumatic Stress Disorder Examination Name: Date of Exam: SSN: C-number: Place of Exam: The following health care providers can perform initial examinations for PTSD. a board-certified
Initial Evaluation for Post-Traumatic Stress Disorder Examination Name: Date of Exam: SSN: C-number: Place of Exam: The following health care providers can perform initial examinations for PTSD. a board-certified
Pain Management Regulations Affect More Than Pain Management Specialists January 2012. Of counsel to
 Pain Management Regulations Affect More Than Pain Management Specialists January 2012 LINDA A. KEEN MSN, JD, LHCRM LAW OFFICE OF LINDA A. KEEN P.A. TALLAHASSEE, FL Of counsel to Pain Management Regulations
Pain Management Regulations Affect More Than Pain Management Specialists January 2012 LINDA A. KEEN MSN, JD, LHCRM LAW OFFICE OF LINDA A. KEEN P.A. TALLAHASSEE, FL Of counsel to Pain Management Regulations
Instructions for Funding Authorization/Reauthorization Process. Residential Alcohol and Other Drug Treatment Programs
 Instructions for Funding Authorization/Reauthorization Process Clinician Instructions: Residential Alcohol and Other Drug Treatment Programs For initial authorization or authorization of continued stay,
Instructions for Funding Authorization/Reauthorization Process Clinician Instructions: Residential Alcohol and Other Drug Treatment Programs For initial authorization or authorization of continued stay,
D. Clinical indicators for psychiatric evaluation are established by one or more of the following criteria. The consumer is:
 MCCMH MCO Policy 2-015 Date: 4/21/11 V. Standards A. A psychiatric evaluation shall be done as an integral part of the assessment process. It serves as the guide to the identification of medical and psychiatric
MCCMH MCO Policy 2-015 Date: 4/21/11 V. Standards A. A psychiatric evaluation shall be done as an integral part of the assessment process. It serves as the guide to the identification of medical and psychiatric
Professional Practice Medical Record Documentation Guidelines
 Professional Practice Medical Record Documentation Guidelines INTRODUCTION Consistent and complete documentation in the medical record is an essential component of quality patient care. All Participating
Professional Practice Medical Record Documentation Guidelines INTRODUCTION Consistent and complete documentation in the medical record is an essential component of quality patient care. All Participating
PRIOR AUTHORIZATION GUIDELINES FOR PSYCHOSOCIAL REHABILITATION SERVICES BEGINNING AUGUST 1, 2014
 PRIOR AUTHORIZATION GUIDELINES FOR PSYCHOSOCIAL REHABILITATION SERVICES BEGINNING AUGUST 1, 2014 PREFACE The criteria and procedures outlined herein apply only to mental health Psychosocial Rehabilitation
PRIOR AUTHORIZATION GUIDELINES FOR PSYCHOSOCIAL REHABILITATION SERVICES BEGINNING AUGUST 1, 2014 PREFACE The criteria and procedures outlined herein apply only to mental health Psychosocial Rehabilitation
TREATMENT PLAN UNDER MHL SECTION 9.60 Article 28 Facilities
 TREATMENT PLAN UNDER MHL SECTION 9.60 Article 28 Facilities Subject of the Petition Name: Subject Also Known As : Subject Home/Residence Address D/O/B: Physician s Name:, M.D.. Board eligible: [ ] Board
TREATMENT PLAN UNDER MHL SECTION 9.60 Article 28 Facilities Subject of the Petition Name: Subject Also Known As : Subject Home/Residence Address D/O/B: Physician s Name:, M.D.. Board eligible: [ ] Board
Disability Insurance Claim Packet Instructions. Your Disability Benefit Claim. How To Apply For Benefits
 Claim Packet Instructions Your Disability Benefit Claim This packet contains the forms necessary to apply for disability benefits. It also addresses common questions about Disability claims. Please save
Claim Packet Instructions Your Disability Benefit Claim This packet contains the forms necessary to apply for disability benefits. It also addresses common questions about Disability claims. Please save
Brantford Native Housing Residential Support/ Addiction Treatment Program
 Brantford Native Housing Residential Support/ Addiction Treatment Program Application Package Ojistoh House or Karahkwa House 318 Colborne Street East Brantford, ON N3S 3M9 (519) 753-5408 x 235 T (519)
Brantford Native Housing Residential Support/ Addiction Treatment Program Application Package Ojistoh House or Karahkwa House 318 Colborne Street East Brantford, ON N3S 3M9 (519) 753-5408 x 235 T (519)
Medical Malpractice Treatment Alprazolam benzodiazepine - A Case Study
 Improving Outcomes in Patients Who are Prescribed Alprazolam with Concurrent Use of Opioids Pik-Sai Yung, M.D. Staff Psychiatrist Center for Counseling at Walton Background and Rationale Alprazolam is
Improving Outcomes in Patients Who are Prescribed Alprazolam with Concurrent Use of Opioids Pik-Sai Yung, M.D. Staff Psychiatrist Center for Counseling at Walton Background and Rationale Alprazolam is
CHEMICAL DEPENDENCE INPATIENT REHABILITATION SERVICES. [Statutory Authority: Mental Hygiene Law Sections 19.07(e), 19.09(b), 19.40, 32.01, 32.
 PART 818 CHEMICAL DEPENDENCE INPATIENT REHABILITATION SERVICES [Statutory Authority: Mental Hygiene Law Sections 19.07(e), 19.09(b), 19.40, 32.01, 32.07(a)] Notice: The following regulations are provided
PART 818 CHEMICAL DEPENDENCE INPATIENT REHABILITATION SERVICES [Statutory Authority: Mental Hygiene Law Sections 19.07(e), 19.09(b), 19.40, 32.01, 32.07(a)] Notice: The following regulations are provided
Section 2. Purpose. Section 3. Alcohol Crisis Teams.
 CVR 13-100-003 CODE OF VERMONT RULES Copyright (c) 2014 Matthew Bender & Company, Inc. A member of the LexisNexis Group. All rights reserved. *** This document reflects changes current through July 11,
CVR 13-100-003 CODE OF VERMONT RULES Copyright (c) 2014 Matthew Bender & Company, Inc. A member of the LexisNexis Group. All rights reserved. *** This document reflects changes current through July 11,
Glen Davis PhD Maine Child Psychology 2 Elm Street, Waterville, ME 04901 Telephone: (207) 221-2631 Fax: (207) 221-3368 MaineChildPsych.
 Dear Parent, Glen Davis PhD Maine Child Psychology 2 Elm Street, Waterville, ME 04901 Telephone: (207) 221-2631 Fax: (207) 221-3368 MaineChildPsych.com Thank you for your interest in psychological services
Dear Parent, Glen Davis PhD Maine Child Psychology 2 Elm Street, Waterville, ME 04901 Telephone: (207) 221-2631 Fax: (207) 221-3368 MaineChildPsych.com Thank you for your interest in psychological services
PART 822 CHEMICAL DEPENDENCE OUTPATIENT SERVICES INDIVIDUAL TREATMENT PLAN
 INDIVIDUAL TREATMENT PLAN PATIENT NAME: John Doe PATIENT ID # 9078 ADMISSION 6-28-11 AXIS AXIS I: 303.9, 304.3 II: 799.9 Deferred I: III: Nicotine use I: IV: Legal Issues; family issues Axis I co-occurring
INDIVIDUAL TREATMENT PLAN PATIENT NAME: John Doe PATIENT ID # 9078 ADMISSION 6-28-11 AXIS AXIS I: 303.9, 304.3 II: 799.9 Deferred I: III: Nicotine use I: IV: Legal Issues; family issues Axis I co-occurring
Going the Distance with Behavioral Health Core Measures Workflow Changes to Canopy. Go-Live: July 23, 2015
 Going the Distance with Behavioral Health Core Measures Workflow Changes to Canopy Go-Live: July 23, 2015 Learning Objectives Provide an overview of core measures and their importance Describe the enhancements
Going the Distance with Behavioral Health Core Measures Workflow Changes to Canopy Go-Live: July 23, 2015 Learning Objectives Provide an overview of core measures and their importance Describe the enhancements
Understanding Coding & Reimbursement for SBI. Presented By: Jen Cohrs CPC, CPMA, CGIC Director of Educational Strategies Wisconsin Medical Society
 Understanding Coding & Reimbursement for SBI Presented By: Jen Cohrs CPC, CPMA, CGIC Director of Educational Strategies Wisconsin Medical Society CPT codes, descriptions and material only are Copyright
Understanding Coding & Reimbursement for SBI Presented By: Jen Cohrs CPC, CPMA, CGIC Director of Educational Strategies Wisconsin Medical Society CPT codes, descriptions and material only are Copyright
DRAFT A Comparison of Targeted Case Management Positions with Community Integration Specialists in Maine
 Service Definitions DRAFT A Comparison of Targeted Case Management Positions with in Maine All TCM Positions Case Management are those covered services provided by a social services or health professional,
Service Definitions DRAFT A Comparison of Targeted Case Management Positions with in Maine All TCM Positions Case Management are those covered services provided by a social services or health professional,
Clinical Considerations for Involuntary Mental Health Treatment of Adults in Oklahoma
 Clinical Considerations for Involuntary Mental Health Treatment of Adults in Oklahoma Brandon Schader, M.D. Medical Director for Crisis Stabilization Oklahoma County Crisis Intervention Center Oklahoma
Clinical Considerations for Involuntary Mental Health Treatment of Adults in Oklahoma Brandon Schader, M.D. Medical Director for Crisis Stabilization Oklahoma County Crisis Intervention Center Oklahoma
ARTICLE 10. OUTPATIENT TREATMENT CENTERS
 Section R9-10-1001. R9-10-1002. R9-10-1003. R9-10-1004. R9-10-1005. R9-10-1006. R9-10-1007. R9-10-1008. R9-10-1009. R9-10-1010. R9-10-1011. R9-10-1012. R9-10-1013. R9-10-1014. R9-10-1015. R9-10-1016. R9-10-1017.
Section R9-10-1001. R9-10-1002. R9-10-1003. R9-10-1004. R9-10-1005. R9-10-1006. R9-10-1007. R9-10-1008. R9-10-1009. R9-10-1010. R9-10-1011. R9-10-1012. R9-10-1013. R9-10-1014. R9-10-1015. R9-10-1016. R9-10-1017.
MEDICAL STAFF RULES & REGULATIONS
 MEDICAL STAFF RULES & REGULATIONS PURPOSE: Rules and Regulations shall set standards of practice that are to be required of each individual exercising clinical privileges in the hospital, and shall act
MEDICAL STAFF RULES & REGULATIONS PURPOSE: Rules and Regulations shall set standards of practice that are to be required of each individual exercising clinical privileges in the hospital, and shall act
16 Rankings On First Page. 30 Total Keywords. KEYWORD RANKINGS We are tracking Benchmark Date and Current Ranking. Ranking Changes Improved
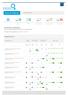 Keyword Rankings harmonygroup.co.za 0 Total Keywords 8 Rankings On First Page 6 Rankings On First Page 7 Rankings On Second Page 7 Ranking Changes Improved NA Ranking Changes Declined KEYWORD RANKINGS
Keyword Rankings harmonygroup.co.za 0 Total Keywords 8 Rankings On First Page 6 Rankings On First Page 7 Rankings On Second Page 7 Ranking Changes Improved NA Ranking Changes Declined KEYWORD RANKINGS
ST. CLAIR COUNTY COMMUNITY MENTAL HEALTH Date Issued: 07/09 Date Revised: 09/11;03/13;06/14;07/15
 ST. CLAIR COUNTY COMMUNITY MENTAL HEALTH Date Issued: 07/09 Date Revised: 09/11;/13;06/14;07/15 WRITTEN BY Jim Johnson Page 1 REVISED BY AUTHORIZED BY Jessica Moeller Debra Johnson I. APPLICATION: THUMB
ST. CLAIR COUNTY COMMUNITY MENTAL HEALTH Date Issued: 07/09 Date Revised: 09/11;/13;06/14;07/15 WRITTEN BY Jim Johnson Page 1 REVISED BY AUTHORIZED BY Jessica Moeller Debra Johnson I. APPLICATION: THUMB
How To Know If You Can Get Help For An Addiction
 2014 FLORIDA SUBSTANCE ABUSE LEVEL OF CARE CLINICAL CRITERIA SUBSTANCE ABUSE LEVEL OF CARE CLINICAL CRITERIA Overview Psychcare strives to provide quality care in the least restrictive environment. An
2014 FLORIDA SUBSTANCE ABUSE LEVEL OF CARE CLINICAL CRITERIA SUBSTANCE ABUSE LEVEL OF CARE CLINICAL CRITERIA Overview Psychcare strives to provide quality care in the least restrictive environment. An
HEALTH INFORMATION FORM FOR STUDY ABROAD PARTICIPANTS
 HEALTH INFORMATION FORM FOR STUDY ABROAD PARTICIPANTS Student: Last name: First Name: Middle Initial: Period of intended study abroad: Year(s): Fall Spring Academic Year Country Foreign Institution or
HEALTH INFORMATION FORM FOR STUDY ABROAD PARTICIPANTS Student: Last name: First Name: Middle Initial: Period of intended study abroad: Year(s): Fall Spring Academic Year Country Foreign Institution or
New Substance Abuse Screening and Intervention Benefit Covered by BadgerCare Plus and Medicaid
 Update December 2009 No. 2009-96 Affected Programs: BadgerCare Plus, Medicaid To: All Providers, HMOs and Other Managed Care Programs New Substance Abuse Screening and Intervention Benefit Covered by BadgerCare
Update December 2009 No. 2009-96 Affected Programs: BadgerCare Plus, Medicaid To: All Providers, HMOs and Other Managed Care Programs New Substance Abuse Screening and Intervention Benefit Covered by BadgerCare
Care Programme Approach (CPA)
 Care Programme Approach (CPA) The Care Programme Approach (CPA) is used to plan many people s mental health care. This factsheet explains what it is, when you should get and when it might stop. The Care
Care Programme Approach (CPA) The Care Programme Approach (CPA) is used to plan many people s mental health care. This factsheet explains what it is, when you should get and when it might stop. The Care
AGREEMENT AND INFORMATION
 AGREEMENT AND INFORMATION We would like to welcome you to our office. Please review this Agreement and Information sheet to assist you in understanding our office policies. Our therapists are private practitioners.
AGREEMENT AND INFORMATION We would like to welcome you to our office. Please review this Agreement and Information sheet to assist you in understanding our office policies. Our therapists are private practitioners.
Dr. Tina Parkman LPC, CAADC 7 points to Total Recovery!
 Dr. Tina Parkman LPC, CAADC 7 points to Total Recovery! } I. Individualized Integrated Care and Services for Co- occurring Disorders } II. The disease progression of Substance Abuse } III. The disease
Dr. Tina Parkman LPC, CAADC 7 points to Total Recovery! } I. Individualized Integrated Care and Services for Co- occurring Disorders } II. The disease progression of Substance Abuse } III. The disease
Search for Compliance Documentation Requirements Part 1: Consent Forms and Treatment Plans. Melissa S. Hooks Director of Program Integrity
 Search for Compliance Documentation Requirements Part 1: Consent Forms and Treatment Plans Melissa S. Hooks Director of Program Integrity Overview of Presentation Background of Compliance Importance of
Search for Compliance Documentation Requirements Part 1: Consent Forms and Treatment Plans Melissa S. Hooks Director of Program Integrity Overview of Presentation Background of Compliance Importance of
PATIENT REGISTRATION Date:
 PATIENT REGISTRATION Date: PLEASE PRESENT YOUR DRIVER S LICENSE AND INSURANCE CARDS TO RECEPTION DESK. INSURANCE CO-PAYMENTS ARE EXPECTED BEFORE SERVICES ARE RENDERED. PAYMENT IN FULL IS EXPECTED WHEN
PATIENT REGISTRATION Date: PLEASE PRESENT YOUR DRIVER S LICENSE AND INSURANCE CARDS TO RECEPTION DESK. INSURANCE CO-PAYMENTS ARE EXPECTED BEFORE SERVICES ARE RENDERED. PAYMENT IN FULL IS EXPECTED WHEN
The Field of Counseling. Veterans Administration one of the most honorable places to practice counseling is with the
 Gainful Employment Information The Field of Counseling Job Outlook Veterans Administration one of the most honorable places to practice counseling is with the VA. Over recent years, the Veteran s Administration
Gainful Employment Information The Field of Counseling Job Outlook Veterans Administration one of the most honorable places to practice counseling is with the VA. Over recent years, the Veteran s Administration
Client s Rights and Counselor Responsibilities
 Client s Right to Give Informed Consent Client s Rights and Counselor Responsibilities Chapter 5 Psychology 475 Professional Ethics in Addictions Counseling Listen to the audio lecture while viewing these
Client s Right to Give Informed Consent Client s Rights and Counselor Responsibilities Chapter 5 Psychology 475 Professional Ethics in Addictions Counseling Listen to the audio lecture while viewing these
