Diabetes in the Competitive Athlete
|
|
|
- James Warren
- 10 years ago
- Views:
Transcription
1 COMPETITIVE SPORTS Diabetes in the Competitive Athlete George D. Harris, MD, MS and Russell D. White, MD, FACSM Abstract Diabetes mellitus is the most common group of metabolic diseases and is characterized by hyperglycemia resulting from defects in insulin secretion, insulin action, or both. Most patients with diabetes are type 2 (90%); the remaining patients have type 1 disease. Athletes with diabetes range from the athlete participating in various youth sports to the competitive Olympic athlete and present a significant challenge to themselves and the medical staff who care for them on a daily basis. Each sport and the type of exercise have their own effects on diabetes management with numerous factors that significantly affect glucose levels, including stress, level of hydration, the rate of glycogenolysis and gluconeogenesis, and the secretion of counterregulatory hormones. This article provides a general overview of diabetes mellitus, the effects of exercise on glucose levels, and a detailed review of the potential complications encountered in the management of diabetes in the athlete. Introduction Athletes with diabetes range from the athlete participating in various youth sports to the competitive Olympic athlete. Each athlete presents a significant challenge to themselves and the medical staff caring for them. They are at risk for acute hypoglycemia or ketoacidosis and chronic complications involving microvascular and macrovascular disease. As a physician caring for athletes with diabetes, it is important to inquire about the athlete s thoughts on their performance at different levels of blood glucose, attitudes about judging blood glucose by how it feels versus testing with a blood glucose meter, and their fears about hypoglycemia (7). The athlete s daily management deals with the physiological demands induced by intense exercise and training, their nutritional needs and varied meal timing, their training regimens and competition as well as the stress of competition (22). Unfortunately for the physician evaluating and managing these athletes, there are limited published well-controlled studies that supplement our knowledge for the formulation of effective treatment plans. There are only a number of Department of Community & Family Medicine, Sports Medicine Fellowship Program, University of Missouri V Kansas City School of Medicine, Kansas City, MO Address for correspondence: Russell D. White, MD, FACSM, University of Missouri V Kansas City School of Medicine, 7900 Lees Summit Road, Kansas City, MO; [email protected] x/1106/309Y315 Current Sports Medicine Reports Copyright * 2012 by the American College of Sports Medicine anecdotal descriptions of management strategies and published case reports. In addition to the usual management challenges encountered in a medical practice for diabetic patients, the demands of training and competition for diabetic athletes can affect glucose homeostasis in a different manner. This can lead to concerns about the athlete s safety during athletic participation, including adequate monitoring of blood glucose, and adjustments to diet and insulin to allow for safe and effective athletic performance (14). Another consideration for the athlete is awareness of the chosen sport and includes 1) how much aerobic and anaerobic exercise is involved, 2) how intensively the athlete practices and competes, 3) duration of the exercise, and 4) the risk of injury or morbidity to self or others if the athlete becomes hypoglycemic (7). The athlete with diabetes needs to understand the effect this disease has on their entire body and take individual responsibility for the daily management of his glucose levels. This component of the athlete s care is one of the greatest challenges physicians face in dealing with the young athletes with diabetes. Lastly, an area often overlooked is identifying the attitudes, abilities, methods, and willingness of the athlete s teammates and coaches to assist them in their diabetes management in order for them to have a successful plan for participation (7). The Types of Diabetes and the Athlete Diabetes mellitus is the most common metabolic disease characterized by hyperglycemia resulting from defects in insulin secretion, insulin action, or both. Most patients with diabetes are type 2 (90%), while the remaining patients have type 1 disease (12). Type 1 diabetes mellitus (T1DM) can occur at any age but is most often diagnosed in children, adolescents, or young adults and is caused by loss of insulin secretion due to progressive loss of insulin production (2). Type 1A is an autoimmune disease characterized by cellular antibodies that may form against islet cells (ICA), insulin (IAA), and glutamic acid decarboxylase (GAD 65 ). Type 1B is an idiopathic, nonautoimmune disease state with loss of beta cell function (16). Type 1 patients demonstrate hyperglycemia and weight loss and are prone to ketoacidosis. Death may occur if exogenous Current Sports Medicine Reports 309
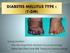
2 insulin is not administered and the acidosis is reversed. Typical onset is before the age of 30 years with peak incidence during adolescence. Therefore, many athletic encounters involve individuals with T1DM. Type 2 diabetes mellitus (T2DM) is characterized by defects in both insulin secretion and resistance to insulin action, resulting in impaired insulin secretion, increased hepatic glucose production, and decreased muscle glucose uptake. T2DM is usually a disease of adults and is due to both genetic (family history or familial hyperlipidemia) and environmental (sedentary lifestyle or inappropriate diet with increased caloric intake) factors. Insulin resistance is associated with obesity, hypertension, hyperlipidemia, and type 2 diabetes and may precede the onset of diagnosed diabetes by 10 to 20 years (35). There are many variations of the mentioned clinical scenario, but most patients are older than 40 years when diabetes develops (38). T2DM is not as common in the competitive, well-fit athlete but occurs in those athletes with an increased body mass for their particular sport (football lineman or rugby players) or those who do not remain fit (baseball players). For both the type 1 and type 2 athletes, the general benefits of physical activity include enhancement of physical fitness, reduction in cardiovascular disease risk, and improved social and emotional well-being (20). The primary risks of physical activity in type 1 patients are exerciseinduced hypoglycemia and aggravation of hyperglycemia and ketosis. Some of the challenges managing athletes with diabetes are related to their individual goals. The reasons why athletes with diabetes participate in sports include the pleasure of competition, improved physical fitness, personal achievement, team atmosphere, improvement of performance, and potential for financial rewards (college scholarships, professional sports contracts, and endorsements). These goals are perceived by the athlete as being far more important than blood glucose control or avoidance of complications and can compromise their blood glucose control and general health. As a physician, our goals are to prevent not only short-term complications (hypoglycemia) but also long-term complications (renal failure, blindness, peripheral vascular disease, and peripheral neuropathy). The athlete may practice unsafe dietary patterns, use nutritional supplements with no benefit or even detrimental effects, and use illegal drugs. The physician needs to be aware of nutritional problems in the female athlete (amenorrhea, osteoporosis, and eating disorder), rapid weight loss to make weight, and excessive consumption of a single macronutrient (carbohydrate, protein, or fat). In sports with weight categories (wrestling, boxing, and weightlifting), a common practice is omission of insulin. By withholding insulin, the athlete can lose weight prior to their weigh-in, leading to poor glucose control and the risk of ketoacidosis (14). Unfortunately, most competitive athletes learn to manage their diabetes during training and competition by trial and error while sharing personal experiences with other athletes (33). Studies suggest that some athletes with type 1 diabetes are not achieving good blood glucose control prior to their competitive event intentionally (31) and have increased lipid utilization (8). This approach often may prevent exercise-induced hypoglycemia. The metabolic demands of the recommended aerobic activity for healthy adults and for the management of patients with T2DM are a percentage of the V O 2max and are intended to minimize contributions of the anaerobic energy systems (14,25,29) (Figure). The physical activity recommendations for healthy adults and for patients with T2DM are similar. The American College of Sports Medicine and American Diabetes Association recommend aerobic exercise at an intensityof40%to70%ofv O 2max and anaerobic exercise Figure: Classification of sports by energy expenditure [Adapted from Mitchell JH, Haskell W, Snell P, et al. Task force 8: classification of sports. J. Am. Coll. Cardiol. 2005; 45:1364Y7. Used with permission.] 310 Volume 11 & Number 6 & November/December 2012 Glucose Management and Monitoring in Sports
3 foraminimumofonesetof10to15repetitionsusing8to 10 resistance exercises for most patients with T2DM with modifications depending on the patient s co-morbidities (1). Managing the Athlete With Diabetes Sport Physiology and Diabetes Each sport and the type of exercise have their own effects on diabetes management. It is known that moderate aerobic exercise is associated with hypoglycemia while bursts of anaerobic exercise may raise blood glucose (5). The table of exercise exchanges and carbohydrate use from Riddell and Bar-or (30) (minutes of exercise requiring 15 g of carbohydrate based on size and type of exercise) provides a beneficial resource in managing the athlete. The initiation of exercise elicits hormonal responses and the release of body fuels, glucose from liver glycogen, glucose stored as glycogen in muscle, the generation of lactic acid that is cycled through the liver to make new glucose, and mobilization of fatty acids and gluconeogenesis from amino acids (7). Exercise augments the effect of insulin, facilitating glucose transport across the cell membrane and increasing muscle glucose uptake 20-fold. The main facilitator, glucose transporter 4 (GLUT-4), is impaired in obesity and diabetes. Its activity is enhanced by insulin-like growth factors, thyroid hormone, bradykinins, nitric oxide, biguanides, thiazolidinediones, and exercise (32). A single exercise session (45 min) may increase insulin sensitivity by 40% and continue for the subsequent 48 h. This glucose-lowering effect via exercise helps normal persons and type 1 and type 2 patients with diabetes; type 2 patients seem to benefit the most (32,38). This metabolic response for the nondiabetic individual is a near instantaneous insulin modulation to keep blood glucose levels within normal range during exercise. However, the athlete with diabetes taking exogenous insulin has insulin absorption from subcutaneous depots with various release patterns along with the increased exposure of insulin to receptors on muscle cells as blood flow increases. This increases the risk of hyperglycemia during the initial exercise and hypoglycemia later as the level of injected insulin is unable to respond to a falling level of glucose (7). Glucose Monitoring During Exercise The athlete, athletic trainer, and team physician should have agreed-upon predetermined blood glucose levels that determine when the athlete participates and when the athlete is not permitted to participate. For example, if the preexercise level is less than 100 mgidl j1, carbohydrate supplementation should take place, and if glucose levels are over 180 mgidl j1,the athlete should consume a non-carbohydrate-containing fluid to prevent dehydration and monitor glucose levels to avoid excessive hyperglycemia and ketosis. Athletes should be educated and questioned about frequent blood glucose monitoring, which should be done two to three times at 30-min intervals before exercise to trend direction of blood glucose levels. During exercise, glucose levels should be checked every 30 min; additional monitoring occurring every 2 h for up to 4 h postexertion to monitor for delayed hypoglycemia (17) should be performed. If preexercise blood glucose is 100 to 250 mgidl j1,itis generally safe to begin exercising (9). Most athletes with T1DM maintain blood glucose levels between 120 and 180 mgidl j1 and regulate their glycemic response to exercise and avoid exercise if their fasting glucose is greater than 250 mgidl j1 and ketosis is present. They use caution if the glucose is greater than 300 mgidl j1 with no ketosis and ingest added carbohydrates (CHO) if glucose levels are less than 100 mgidl j1. Preventing and Managing Hypoglycemia A number of physiological regulatory and counterregulatory mechanisms are in place to allow both fasting and nonfasting serum glucose levels to be maintained within a relatively narrow range, despite the impact of eating and physical activity. With exercise, there are numerous factors that significantly affect glucose levels, including stress, level of hydration, the rate of glycogenolysis and gluconeogenesis, and the secretion of counter-regulatory hormones (19). Hypoglycemia in the diabetic athlete can be either immediate or delayed. Immediate hypoglycemia occurs during or shortly after exercise and is most common in the type 1 patient due to inadequate caloric intake to meet metabolic demands. Other causes include excessive exogenous insulin administration or injection of insulin into the site of exercising muscle or overlying subcutaneous tissue resulting in increased absorption rate (38). Symptoms and signs of hypoglycemia are principally due to either adrenergic causes (from the release of sympathomimetic mediators) and neuroglycopenic causes (from an inadequate amount of glucose being available to support brain activity) (6). Both main causes have considerable overlap with symptoms caused by strenuous or prolonged physical activity, which may make recognition of low blood glucose difficult during athletic activity. Adrenergic signs and symptoms consist of hunger, anxiety, sweating, tremor, tachycardia, palpitations, and/or a feeling of impending doom. Neuroglycopenic symptoms and signs likely are to include weakness or fatigue, slow or slurred speech, impaired performance of tasks, lack of coordination, blurred vision, odd behavior, confusion, vertigo, paresthesias, and/or stupor (6). The severe signs of neuroglycopenia are seizures and loss of consciousness, although these are less common in adults than in children (4). To prevent immediate hypoglycemia, one should avoid injection of insulin into an area of exercising muscles (e.g.,use of anterior thigh in a runner) (10) and instead inject into the abdominal area. This effect is seen much less with analog insulin preparations (27). Calories should be replaced continually during a period of prolonged activity. Careful glucose monitoring during activities allows the athlete to determine individual caloric requirements and make adjustments. To avoid weight gain, the runner may emphasize insulin adjustment rather than supplemental calories. Exercising at a lower exercise intensity but for a longer period of time or in cold weather may require more calories, while in a hot environment, athletes with diabetes may experience hypoglycemia due to poor appetite and decreased caloric intake (36). The best approach in the management of hypoglycemia during exercise is preventing its occurrence. When dealing with athletes with various levels of maturity, commitment to the sport, and personal accountability, one must be prepared for the recognition and management of hypoglycemia. When an athlete self-recognizes symptoms of hypoglycemia Current Sports Medicine Reports 311
4 or a teammate or coach suspects a low glucose level, the athlete should be removed from play and encouraged to measure the fingerstick glucose. Hypoglycemia should be treated with 15 to 20 g of fast-acting carbohydrate, preferably glucose tablets designed to treat hypoglycemia or a sugar-sweetened beverage or juice. This treatment can be repeated if there is no improvement in symptoms or glucose level after 15 min. If conditions are present that suggest hypoglycemia might recur once the athlete resumes play, additional complex carbohydrates should be consumed before returning to the activity. Hypoglycemia provokes a counter-regulatory hormonal response, so excessive carbohydrate intake should be avoided to prevent a significant hyperglycemic rebound (19). Severe hypoglycemia with the loss of consciousness or seizures is a life-threatening condition requiring prompt treatment. Once an athlete with hypoglycemia has become unresponsive, emergency response personnel should be summoned urgently. No attempt to force oral consumption of carbohydrates should be made. Instead, glucagon should be injected parenterally (subcutaneously, intramuscularly, or intravenously) or glucose by intravenous administration of one to three ampules of 50% dextrose (one ampule contains 25 g of glucose in 50 ml of water) in water (D50 W) in the field while evaluating and resuscitating the athlete (19). Delayed Hypoglycemia Delayed hypoglycemia (also known as nocturnal hypoglycemia) usually occurs 6 to 12 h after exercise and has been reported up to 28 h postexercise (21). It often occurs at nighttime when the athlete is to perceive or recognize least likely this condition and is associated with seizures, cardiac arrhythmias, unconsciousness, and death (11). The pathophysiology involves vigorous exercise severely depleting body glycogen stores, followed by inadequate replacement of glycogen stores in the postexercise interval ( golden replenishment period ). The athlete either underestimates caloric requirements or ingests limited calories and defers eating until later (38). Over the ensuing hours, liver and muscle tissues extract circulating blood glucose to replenish depleted glycogen stores and glycogen synthetase is activated (24). In addition, the peripheral muscle tissues are more sensitive to any available insulin postexercise (15). The subsequent severe and persistent delayed hypoglycemia often requires the assistance of another person, parenteral glucagon, and continuous caloric intake over several hours to correct and replenish depleted glycogen stores. Glycemic Control and Management Ideally athletes with diabetes perform best at glucose levels between 70 and 150 mgidl j1. Practically most athletes with T1DM maintain blood glucose levels between 120 and 180 mgidl j1. Based on the training program, the athlete learns the personal glucose response to exercise duration and intensity. Hypoglycemia in athletes with T1DM occurs due to 1) lack of physiological decline in insulin secretion with energy utilization due to exogenous insulin administration, 2) loss of physiologic autonomic regulation of glucose levels due to dysregulation (loss of counter-regulatory autonomic function), and 3) possible increased absorption of exogenous insulin with exercise (13). Comparison of blood glucose levels in normal, nonketotic diabetic, and ketotic diabetic athletes by Wahren et al. (34) found that stimulation of the counter-regulatory hormones in the insulinopenic, ketotic state worsens this condition. A similar effect was found by Berger (3), who studied athletes with diabetes subjected to 3 h of exercise when compared with normal controls. T1DM Anaerobic, short-distance, sprint activity events rarely cause metabolic control problems for the type 1 athlete. Proper hydration and maintenance of glucose levels as noted previously often maximizes performance. Hyperglycemia may occur in some athletes due to acute catecholamine release, but delayed hypoglycemia is rare (26). Adjustment of insulin dosing for these events is usually unnecessary. Some endurance athletes choose to set the basal rate of insulin infusion via continuous subcutaneous insulin infusion (CSII) or insulin pump at a lower rate or select a decreased dosage amount of a long-acting basal insulin dosage and then ingest carbohydrates over a period to match the athlete s energy utilization with exercise (37). This method is utilized by some distance cyclists and runners. By developing a steady-state balance between the exercise requirement, the basal insulin infusion, and ingestion of energy (carbohydrates), the glucose level is held constant (e.g., 130 to 150 mgidl j1 ) over several hours. If the cyclist or runner with T1DM encounters a demanding, incline section of the course, either the basal rate can be adjusted downward or extra energy (calories) ingested to maintain optimal glycemic levels. Many endurance sports commence in the morning. This schedule results in less frequent hypoglycemia due to physiologically elevated diurnal cortisol and growth hormone levels. When events occur later in the day, adjustments must be made accordingly. Practically, training at a time of the day similar to the scheduled competitive event allows the athlete to develop personal adjustments of food and insulin. Athletes with T1DM learn their personal requirements from training and apply these results. To counteract hypoglycemia, runners and cyclists who are prone to hypoglycemia often perform a series of anaerobic sprints or resistance exercise prior to the aerobic endurance event. Bussau et al. (5) have found this anaerobic practice lowers the incidence of subsequent hypoglycemia during the later endurance event. A recent article confirmed a similar effect following aerobic exercise (39). Thus, short bursts of anaerobic exercise before or after aerobic exercise may help prevent subsequent hypoglycemia. If the type 1 diabetic athlete is insulin deficient and blood glucose is elevated, endurance running may exacerbate this diabetic state. Osmotic diuresis with relative dehydration also affects performance. As blood glucose rises, the risk of causing even higher blood glucose levels increases (3,26). Further exercise may exacerbate or precipitate ketoacidosis. Athletes with T1DM will always require some insulin. When the athlete is utilizing human insulin isophane suspension (NPH) or analog long-acting insulin (insulin glargine or insulin detemir) combined with either human short-acting (regular) or analog rapid-acting insulin (insulin lispro, insulin aspart, insulin glulisine), the human intermediate insulin or analog long-acting insulin is often decreased by 50% and 312 Volume 11 & Number 6 & November/December 2012 Glucose Management and Monitoring in Sports
5 the analog rapid-acting or human short-acting insulin is decreased by 25% to 75%, depending on the distance, the time of exercise, and the individual s training response to similar exercise (3). Analog rapid-acting insulins are very predictable in their absorption kinetic profiles (27). In an endurance event, e.g., marathon, total daily insulin dose may need to be reduced more than 80%. One study of halfmarathon runners with type 1 diabetes found that athletes must consume adequate carbohydrates and will often reduce insulin dosages far less than traditionally recommended (28). In longer duration events, energy sources are critical; carbohydrate-containing fluids and other solid fuel sources are necessary. Finally, adequate replenishment of glycogen stores (1.5 g of carbohydrate per kilogram of body weight) at the finish line is critical in the golden recovery period (13). If glycogen stores are not replaced, the risk of delayed hypoglycemia is high (21). T2DM The management of athletes with T2DM depends on the sport and duration of the diagnosed diabetes state. Early in the disease, the athlete maintains some endogenous insulin production or secretion and requires little, if any, exogenous insulin. These athletes maintain the ability to decrease or increase physiologically endogenous insulin secretion and are able to have optimal glucose levels maintained in the desired range. As the disease state progresses and endogenous insulin secretion diminishes, exogenous insulin administration becomes necessary. In these athletes with T2DM, the exogenous insulin will require adjustment to prevent hypoglycemia. With active training, it is not uncommon in these athletes for the exogenous insulin requirement to decrease by 50% or greater, and with competition, the requirement may decrease further based on training requirements. Also important in the athletes with T2DM is that other agents (e.g., insulin secretagogues, insulin sensitizers) are often decreased due to 1) regular training exercise, 2) increased insulin sensitivity, 3) decrease in body fat, and 4) increase in lean body mass. With the given changes, some fit athletes with T2DM note a plateau in medicine requirements for treating their diabetes due to the ability to perform at competitive levels while utilizing less supplemental energy. Special Situations Travel Preparations Travel preparations should be a coordinated effort between the athlete, the team physician, and the athletic trainer. A labeled travel kit should contain unused syringes, blood glucose meters, lancets, test strips, alcohol swabs, insulin, insulin pump with supplies (if needed), glucagon emergency kit, and ketone testing supplies. The athlete should ensure the kit has at least twice as much medication and testing equipment as anticipated for travel. Supplies should be carried with the athlete at all times and not with checked luggage. Additionally, extra prescriptions for these supplies should be carried with the athlete as a precaution along with prepackaged meals or snacks. A letter from the athlete s physician stating the medical condition, necessity of supplies including a red sharps container, athlete s health insurance card, and emergency contact numbers should be included. The athlete should carry an identification card or medical bracelet stating the medical condition (17). Athletes Competing in Specific Sports Altitude Sports Glycemic control decreases in athletes with T1DM and may affect some patients with T2DM at high altitudes. This hyperglycemia is due to 1) increased sympathetic tone with subsequent increased hepatic glucose production, 2) increased insulin resistance, and 3) loss of appetite at high altitude. Other problems encountered by these athletes include variation of glucose monitor reliability and adequate protection of insulin from temperature extremes. As the insulin temperature approaches freezing, it is no longer active (36). Mountain climbers and winter athletes should maintain insulin close to their body to maintain optimal temperature of the insulin. Water Sports, Swimming, or Scuba Participation in water sports limits the use of insulin pumps and continuous glucose monitors depending on the specific device and company model. While insulin pumps are water resistant and one model is water proof to 12 ft for 24 h, other models do not withstand pressure. Insulin pumps usually are removed prior to showering or bathing while continuous skin sensors may remain in place. The separate external glucose monitor device is not waterproof. Scuba diving is discouraged for those with T1DM, although many accomplished divers dive with partners who are aware of their condition. Since recreational dives usually last 30 to 45 min, glucose monitoring can be done on an interval basis at the surface level. Ice Hockey, Wrestling, or Football Use of external devices is discouraged in these sports. Wrestling and football competition could be detrimental to insulin pumps or external glucose monitors. While these devices are not prohibited by USA Hockey, participants cannot wear any equipment that would be harmful to another player. In addition, a letter from a health care provider is required for any special medical equipment. In these sports, the athlete often resorts to intermittent insulin injection and glucose monitoring outside the competition area. Baseball or Softball These sports are ideal for persons with diabetes and require bursts of anaerobic energy without prolonged exercise periods. In the dugout, each inning, the athletes may test their glucose levels, ingest carbohydrates, and maintain hydration. Some position players have worn insulin pumps successfully while playing these sports. Distance Running or Endurance Sports Distance running and other endurance sports require careful management of fuel sources and insulin management for the type 1 athlete (23). When their metabolic derangements are controlled, type 1 patients demonstrate a normal exercise capacity (29). Endurance runners often strive for optimal prerun blood glucose of 120 to 180 mgidl j1,take minimal insulin, and estimate a glucose decrease of 10 to Current Sports Medicine Reports 313
6 15 mgidl j1 per mile (38). When running for periods of 30 to 60 min, self-monitoring of blood glucose or continuous glucose monitoring (CGM) during the training period will delineate the individual s predicted response. If a type 1 endurance runner experiences difficulty in maintaining satisfactory blood glucose levels, rapid-acting insulin and longacting insulin will require adjustment and may require changing to more frequent insulin injections or CSII (insulin pump) to improve control. With longer distances, external fuel sources become more important. The risk of hypoglycemia is increased since insulin levels do not wane in the type 1 diabetic runner as in the runner with normal hormonal control. Carbohydratecontaining fluids and exogenous fuel sources will be required as exercise progresses. Adequate replacement of depleted glycogen stores is crucial in recovery. The use of CGM has improved the ability of athletes with T1DM to compete in many endurance sports. Type 2 diabetic runners may participate in endurance running events since some may have achieved weight loss and improved their cardiovascular fitness. The risk of either immediate or delayed hypoglycemia is far less in these individuals. The period of increased insulin sensitivity should persist for 12 to 48 h without clinical hypoglycemia (18). Those athletes treated with agents predisposing them to hypoglycemia may require a reduction in dosage as they train, reduce body fat, improve physical fitness, and decrease insulin resistance. Triathlons Triathletes who have diabetes and take insulin have competed successfully. Most participants have T1DM and, via training, learn to manage the insulin and glucose satisfactorily and make insulin adjustments for the days of competition based on training experiences. During the swimming element, either a waterproof pump is worn or the insulin pump and glucose monitor are removed. After exiting the water, many athletes attach the external glucose monitor and the insulin pump. This process requires 10 s or less. Then, the athlete may suspend, continue, or increase the same infusion based on the glucose monitor reading without ceasing activity. With special permission from race officials, team members along the course route may pass off glucose supplements to the athlete, if necessary. Conclusion With improved insulin analog formulations and specific oral and parenteral medications, the athlete with T1DM or T2DM is able to compete in most sports with specific medicine adjustments and proper training. The athlete with diabetes is able to participate at all levels of competition with successful outcomes while minimizing hypoglycemia and hyperglycemia. The authors declare no conflict of interest and do not have any financial disclosures. References 1. Albright A, Franz M, Hornsby G, et al. American College of Sports Medicine Position Stand: exercise and type 2 diabetes. Med. Sci. Sports Exerc. 2000; 32:1345Y Atkinson MA, Maclaren NK. The pathogenesis of insulin-dependent diabetes mellitus. N. Engl. J. Med. 1994; 331:1428Y Berger M. Adjustment of insulin and oral agent therapy. In: Handbook of Exercise in Diabetes. 2nd ed. Alexandria: American Diabetes Association, Inc., 2002, pp. 365Y Bognetti E, Brunelli A, Meschi F, et al. Frequency and correlates of severe hypoglycaemia in children and adolescents with diabetes mellitus. Eur. J. Pediatr. 1997; 156:589Y Bussau VA, Ferreira LD, Jones TW, et al. The 10-s maximal sprint: a novel approach to counter an exercise-mediated fall in glycemia in individuals with type 1 diabetes. Diabetes Care. 2006; 29:601Y6. 6. Cryer PE. Glucose homeostasis and hypoglycemia. In: Kronenberg HM, Melmed S, Polonsky KS, et al, editors. Williams Textbook of Endocrinology. 11th edition, Philadelphia: Saunders; pp. 1503Y Drazin MB. Managing the adolescent athlete with type 1 diabetes mellitus. Pediatr. Clin. North Am. 2010; 57:829Y Ebeling P, Tuominen JA, Bourey R, et al. Athletes with IDDM exhibit impaired metabolic control and increased lipid utilization with no increase insulin sensitivity. Diabetes. 1995; 44:471Y7. 9. Flood L, Constance A. Diabetes and exercise safety. Am. J. Nurs. 2002; 102:47Y Frid A, Ostman J, Linde B. Hypoglycemia risk during exercise after intramuscular injection of insulin in the thigh in IDDM. Diabetes Care. 1990; 11:410Y Gill GV, Woodward A, Casson IF, et al. Cardiac arrhythmia and nocturnal hypoglycaemia in type 1 diabetes V the dead in bed syndrome revisited. Diabetologia. 2009; 52:42Y Harris MI, Zimmet P. Classification of diabetes mellitus and other categories of glucose intolerance. In: Alberti KGMN, Zimmet P, DeFronzo RA, editors. International Textbook of Diabetes Mellitus. 2nd edition, London: John Wiley and Sons, Ltd.; p Hirsch I B, Marker JC, Smith LJ, et al. Insulinandglucagoninpreventionof hypoglycemia during exercise in humans. Am. J. Physiol. 1991; 260:E695Y Hornsby WG Jr, Chetlin RD. Management of competitive athletes with diabetes. Diabetes Spectr. 2005; 18:102Y Hough DO. Diabetes mellitus in sports. Med. Clin. North Am. 1994; 78:423Y Imagawa A, Hanafusa T, Miyagawa J, et al. A novel subtype of type 1 diabetes mellitus characterized by a rapid onset and an absence of diabetesrelated antibodies. N. Engl. J. Med. 2000; 342:301Y Jimenez CC, Corcoran MH, Crawley JT, et al. National athletic trainers association position statement: management of the athlete with type I diabetes mellitus. J. Athl. Train. 2007; 42:536Y Kelley DE, Goodpaster BH. Effects of exercise on glucose homeostasis in type 2 diabetes mellitus. Med. Sci. Sports Exerc. 2001; 33:S495Y501; discussion S528Y Kirk SE. Hypoglycemia in athletes with diabetes. Clin. Sports Med. 2009; 28:455Y Lehmann R, Kaplan V, Bingisser R, et al. Impact of physical activity on cardiovascular risk factors in IDDM. Diabetes Care. 1997; 20:1603Y MacDonald MJ. Postexercise late-onset hypoglycemia in insulin-dependent diabetic patients. Diabetes Care. 1987; 10:584Y MacKnight JM, Dilaawar JM, Pastors JG, et al. The daily management of athletes with diabetes. Clin. Sports Med. 2009; 28:479Y Mayer-Davis EJ, D Agostino R, Karter AJ, et al. Intensity and amount of physical activity in relation to insulin sensitivity: the Insulin Resistance Atherosclerosis Study. JAMA. 1998; 279:669Y Mikines KJ, Sonne B. Insulin sensitivity and responsiveness after acute exercise in man. Clin. Physiol. 1985; 5(4 suppl):a Mitchell JH, Haskell W, Snell P, et al. Task force 8: classification of sports. J. Am. Coll. Cardiol. 2005; 45:1364Y Mitchell TH, Abraham G, Schiffrin A, et al. Hyperglycemia after intense exercise in IDDM subjects during continuous subcutaneous insulin infusion. Diabetes Care. 1988; 11:311Y Mudaliar SR, Lindberg FA, Joyce M, et al. Insulin aspart (B28 asp-insulin): a fast-acting analog of human insulin: absorption kinetics and action profile compared with regular human insulin in healthy nondiabetic subjects. Diabetes Care. 1999; 22:1501Y Murillo S, Brugnara L, Novialsa A. One year follow-up in a group of halfmarathon runners with type-1 diabetes treated with analogues. J. Sports Med. Phys. Fitness. 2010; 50:506Y Richter EA, Turcotte L, Hespel P, et al. Metabolic responses to exercise. Effects of endurance training and implications for diabetes. Diabetes Care. 1992; 15:1767Y Volume 11 & Number 6 & November/December 2012 Glucose Management and Monitoring in Sports
7 30. Riddell MC, Bar-or O. Children and adolescents. In: Ruderman N, Devlin JT, Schneider SH, et al, editors. Handbook of Exercise in Diabetes. Alexandria (Egypt): American Diabetes Association; pp. 547Y Sane T, Helve E, Pelkonen R, Koivisto VA. The adjustment of diet and insulin dose during long-term endurance exercise in type 1 (insulin-dependent) diabetic men. Diabetologia. 1988; 31:35Y Shepherd PR, Kahn BB. Glucose transporters and insulin actionv implications for insulin resistance and diabetes mellitus. N. Engl. J. Med. 1999; 341:248Y Thurm U, Harper PN. I m running on insulin: summary of the history of the International Diabetic Athletes Association. Diabetes Care. 1992; 15:1811Y Wahren J, Hagenfeldt L, Felig P. Splanchnic and leg exchange of glucose, amino acids, and free fatty acids during exercise in diabetes mellitus. J. Clin. Invest. 1975; 55:1303Y Warram JH, Martin BC, Krolewaski AS, et al. Slow glucose removal rate and hyperinsulinemia precede the development of type II diabetes in the offspring of diabetic parents. Ann. Intern. Med. 1990; 113:909Y White R, Cardone D, Berg K. The athlete with diabetes. In: Madden C, Young C, Putukian M, McCarty E, editors. Netter s Sports Medicine. Philadelphia: Elsevier Publishing, Inc.; pp. 223Y White RD. Insulin pump therapy (continuous subcutaneous insulin infusion). Prim. Care. 2007; 34:845Y White RD, Harris GD, Daily JP. The runner with diabetes. In: Wilder RP, O Connor FG, editors. The Textbook of Running Medicine. Champaign (IL): Human Kinetics Inc., 2012 (in press). 39. Yardley JE, Kenny GP, Perkins B, et al. Effects of performing resistance exercise before versus after aerobic exercise on glycemia in type 1 diabetes. Diabetes Care. 2012; 35:669Y75. Current Sports Medicine Reports 315
Diabetes mellitus. Lecture Outline
 Diabetes mellitus Lecture Outline I. Diagnosis II. Epidemiology III. Causes of diabetes IV. Health Problems and Diabetes V. Treating Diabetes VI. Physical activity and diabetes 1 Diabetes Disorder characterized
Diabetes mellitus Lecture Outline I. Diagnosis II. Epidemiology III. Causes of diabetes IV. Health Problems and Diabetes V. Treating Diabetes VI. Physical activity and diabetes 1 Diabetes Disorder characterized
Managing Diabetes in the Athletic Population
 Managing Diabetes in the Athletic Population Michael Prybicien, LA, ATC, CSCS, CES, PES Athletic Trainer, Passaic High School Overlook Medical Center & Adjunct Faculty, William Paterson University Dedicated
Managing Diabetes in the Athletic Population Michael Prybicien, LA, ATC, CSCS, CES, PES Athletic Trainer, Passaic High School Overlook Medical Center & Adjunct Faculty, William Paterson University Dedicated
ETIOLOGIC CLASSIFICATION. Type I diabetes Type II diabetes
 DIABETES MELLITUS DEFINITION It is a common, chronic, metabolic syndrome characterized by hyperglycemia as a cardinal biochemical feature. Resulting from absolute lack of insulin. Abnormal metabolism of
DIABETES MELLITUS DEFINITION It is a common, chronic, metabolic syndrome characterized by hyperglycemia as a cardinal biochemical feature. Resulting from absolute lack of insulin. Abnormal metabolism of
Abdulaziz Al-Subaie. Anfal Al-Shalwi
 Abdulaziz Al-Subaie Anfal Al-Shalwi Introduction what is diabetes mellitus? A chronic metabolic disorder characterized by high blood glucose level caused by insulin deficiency and sometimes accompanied
Abdulaziz Al-Subaie Anfal Al-Shalwi Introduction what is diabetes mellitus? A chronic metabolic disorder characterized by high blood glucose level caused by insulin deficiency and sometimes accompanied
INJEX Self Study Program Part 1
 INJEX Self Study Program Part 1 What is Diabetes? Diabetes is a disease in which the body does not produce or properly use insulin. Diabetes is a disorder of metabolism -- the way our bodies use digested
INJEX Self Study Program Part 1 What is Diabetes? Diabetes is a disease in which the body does not produce or properly use insulin. Diabetes is a disorder of metabolism -- the way our bodies use digested
2. What Should Advocates Know About Diabetes? O
 2. What Should Advocates Know About Diabetes? O ften a school district s failure to properly address the needs of a student with diabetes is due not to bad faith, but to ignorance or a lack of accurate
2. What Should Advocates Know About Diabetes? O ften a school district s failure to properly address the needs of a student with diabetes is due not to bad faith, but to ignorance or a lack of accurate
CYCLING AND DIABETES Conrad Earnest, PhD, FACSM
 CYCLING AND DIABETES Conrad Earnest, PhD, FACSM Working with a diabetic cyclist can at first be intimidating simply owing to ones unfamiliarity with the disease. However, a few basic guidelines will help
CYCLING AND DIABETES Conrad Earnest, PhD, FACSM Working with a diabetic cyclist can at first be intimidating simply owing to ones unfamiliarity with the disease. However, a few basic guidelines will help
Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both.
 Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
GLUCOSE HOMEOSTASIS-II: An Overview
 GLUCOSE HOMEOSTASIS-II: An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology, M Med Part I
GLUCOSE HOMEOSTASIS-II: An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology, M Med Part I
Causes, incidence, and risk factors
 Causes, incidence, and risk factors Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both. To understand diabetes,
Causes, incidence, and risk factors Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both. To understand diabetes,
CLASS OBJECTIVES. Describe the history of insulin discovery List types of insulin Define indications and dosages Review case studies
 Insulins CLASS OBJECTIVES Describe the history of insulin discovery List types of insulin Define indications and dosages Review case studies INVENTION OF INSULIN 1921 The first stills used to make insulin
Insulins CLASS OBJECTIVES Describe the history of insulin discovery List types of insulin Define indications and dosages Review case studies INVENTION OF INSULIN 1921 The first stills used to make insulin
Insulin therapy and exercise
 DIABETES RESEARCH A ND CLINICAL PRACTICE 93S (2011) S73 S77 Insulin therapy and exercise Georgios I. Kourtoglou * St. Luke s General Hospital, Panorama, Thessaloniki, Greece ARTICLE INFO ABSTRACT Keywords:
DIABETES RESEARCH A ND CLINICAL PRACTICE 93S (2011) S73 S77 Insulin therapy and exercise Georgios I. Kourtoglou * St. Luke s General Hospital, Panorama, Thessaloniki, Greece ARTICLE INFO ABSTRACT Keywords:
Intensive Insulin Therapy in Diabetes Management
 Intensive Insulin Therapy in Diabetes Management Lillian F. Lien, MD Medical Director, Duke Inpatient Diabetes Management Assistant Professor of Medicine Division of Endocrinology, Metabolism, & Nutrition
Intensive Insulin Therapy in Diabetes Management Lillian F. Lien, MD Medical Director, Duke Inpatient Diabetes Management Assistant Professor of Medicine Division of Endocrinology, Metabolism, & Nutrition
8/7/2015. Disclosure to Participants. Type 1 Diabetes and Physical Activity: Integrating Data. Successful T1 Diabetic Athletes
 8/7/2015 Sheri R. Colberg PhD, FACSM Professor of Exercise Science Old Dominion University Norfolk, VA Disclosure to Participants Notice of Requirements For Successful Completion Please refer to learning
8/7/2015 Sheri R. Colberg PhD, FACSM Professor of Exercise Science Old Dominion University Norfolk, VA Disclosure to Participants Notice of Requirements For Successful Completion Please refer to learning
Regulation of Metabolism. By Dr. Carmen Rexach Physiology Mt San Antonio College
 Regulation of Metabolism By Dr. Carmen Rexach Physiology Mt San Antonio College Energy Constant need in living cells Measured in kcal carbohydrates and proteins = 4kcal/g Fats = 9kcal/g Most diets are
Regulation of Metabolism By Dr. Carmen Rexach Physiology Mt San Antonio College Energy Constant need in living cells Measured in kcal carbohydrates and proteins = 4kcal/g Fats = 9kcal/g Most diets are
There seem to be inconsistencies regarding diabetic management in
 Society of Ambulatory Anesthesia (SAMBA) Consensus Statement on Perioperative Blood Glucose Management in Diabetic Patients Undergoing Ambulatory Surgery Review of the consensus statement and additional
Society of Ambulatory Anesthesia (SAMBA) Consensus Statement on Perioperative Blood Glucose Management in Diabetic Patients Undergoing Ambulatory Surgery Review of the consensus statement and additional
DIABETES MELLITUS. By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria
 DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
INPATIENT DIABETES MANAGEMENT Robert J. Rushakoff, MD Professor of Medicine Director, Inpatient Diabetes University of California, San Francisco
 INPATIENT DIABETES MANAGEMENT Robert J. Rushakoff, MD Professor of Medicine Director, Inpatient Diabetes University of California, San Francisco CLINICAL RECOGNITION Background: Appropriate inpatient glycemic
INPATIENT DIABETES MANAGEMENT Robert J. Rushakoff, MD Professor of Medicine Director, Inpatient Diabetes University of California, San Francisco CLINICAL RECOGNITION Background: Appropriate inpatient glycemic
Diabetes Fundamentals
 Diabetes Fundamentals Prevalence of Diabetes in the U.S. Undiagnosed 10.7% of all people 20+ 23.1% of all people 60+ (12.2 million) Slide provided by Roche Diagnostics Sources: ADA, WHO statistics Prevalence
Diabetes Fundamentals Prevalence of Diabetes in the U.S. Undiagnosed 10.7% of all people 20+ 23.1% of all people 60+ (12.2 million) Slide provided by Roche Diagnostics Sources: ADA, WHO statistics Prevalence
Department Of Biochemistry. Subject: Diabetes Mellitus. Supervisor: Dr.Hazim Allawi & Dr.Omar Akram Prepared by : Shahad Ismael. 2 nd stage.
 Department Of Biochemistry Subject: Diabetes Mellitus Supervisor: Dr.Hazim Allawi & Dr.Omar Akram Prepared by : Shahad Ismael. 2 nd stage. Diabetes mellitus : Type 1 & Type 2 What is diabestes mellitus?
Department Of Biochemistry Subject: Diabetes Mellitus Supervisor: Dr.Hazim Allawi & Dr.Omar Akram Prepared by : Shahad Ismael. 2 nd stage. Diabetes mellitus : Type 1 & Type 2 What is diabestes mellitus?
X-Plain Hypoglycemia Reference Summary
 X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
Section 504 Plan (pg 1 of 8)
 Section 504 Plan (pg 1 of 8) of Birth School Today s Section 504 Plan for: Disability: Diabetes School Year: Grade: Homeroom Teacher: Bus Number: Background Objectives The student has type diabetes. Diabetes
Section 504 Plan (pg 1 of 8) of Birth School Today s Section 504 Plan for: Disability: Diabetes School Year: Grade: Homeroom Teacher: Bus Number: Background Objectives The student has type diabetes. Diabetes
Diabetes Expert Witness on: Diabetic Hypoglycemia in Nursing Homes
 Diabetes Expert Witness on: Diabetic Hypoglycemia in Nursing Homes Nursing home patients with diabetes treated with insulin and certain oral diabetes medications (i.e. sulfonylureas and glitinides) are
Diabetes Expert Witness on: Diabetic Hypoglycemia in Nursing Homes Nursing home patients with diabetes treated with insulin and certain oral diabetes medications (i.e. sulfonylureas and glitinides) are
CME Test for AMDA Clinical Practice Guideline. Diabetes Mellitus
 CME Test for AMDA Clinical Practice Guideline Diabetes Mellitus Part I: 1. Which one of the following statements about type 2 diabetes is not accurate? a. Diabetics are at increased risk of experiencing
CME Test for AMDA Clinical Practice Guideline Diabetes Mellitus Part I: 1. Which one of the following statements about type 2 diabetes is not accurate? a. Diabetics are at increased risk of experiencing
Type 1 Diabetes. Pennington Nutrition Series. Overview. About Insulin
 Pennington Nutrition Series Healthier lives through education in nutrition and preventive medicine Pub No. 32 Type 1 Diabetes Overview Type 1 Diabetes (DM) is usually diagnosed in children and young adults.
Pennington Nutrition Series Healthier lives through education in nutrition and preventive medicine Pub No. 32 Type 1 Diabetes Overview Type 1 Diabetes (DM) is usually diagnosed in children and young adults.
MANAGEMENT OF TYPE - 1 DIABETES MELLITUS
 MANAGEMENT OF TYPE - 1 DIABETES MELLITUS INVESTIGATIONS AND TREATMENT MANSI NAIK VII SEMESTER INVESTIGATIONS FASTING BLOOD SUGAR PLASMA GLUCOSE HEMOGLOBIN A 1c SYMPTOMS OF TYPE 1 DIABETES MELLITUS Polyuria
MANAGEMENT OF TYPE - 1 DIABETES MELLITUS INVESTIGATIONS AND TREATMENT MANSI NAIK VII SEMESTER INVESTIGATIONS FASTING BLOOD SUGAR PLASMA GLUCOSE HEMOGLOBIN A 1c SYMPTOMS OF TYPE 1 DIABETES MELLITUS Polyuria
Mind the Gap: Navigating the Underground World of DKA. Objectives. Back That Train Up! 9/26/2014
 Mind the Gap: Navigating the Underground World of DKA Christina Canfield, MSN, RN, ACNS-BC, CCRN Clinical Nurse Specialist Cleveland Clinic Respiratory Institute Objectives Upon completion of this activity
Mind the Gap: Navigating the Underground World of DKA Christina Canfield, MSN, RN, ACNS-BC, CCRN Clinical Nurse Specialist Cleveland Clinic Respiratory Institute Objectives Upon completion of this activity
Section 5: Type 2 Diabetes
 SECTION OVERVIEW Definition and Symptoms Blood Glucose Monitoring Healthy Eating Physical Activity Oral Medication Insulin Sharps Disposal Definition and Symptoms Type 2 diabetes is occurring more frequently
SECTION OVERVIEW Definition and Symptoms Blood Glucose Monitoring Healthy Eating Physical Activity Oral Medication Insulin Sharps Disposal Definition and Symptoms Type 2 diabetes is occurring more frequently
Endocrine Responses to Resistance Exercise
 chapter 3 Endocrine Responses to Resistance Exercise Chapter Objectives Understand basic concepts of endocrinology. Explain the physiological roles of anabolic hormones. Describe hormonal responses to
chapter 3 Endocrine Responses to Resistance Exercise Chapter Objectives Understand basic concepts of endocrinology. Explain the physiological roles of anabolic hormones. Describe hormonal responses to
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
DRUGS FOR GLUCOSE MANAGEMENT AND DIABETES
 Page 1 DRUGS FOR GLUCOSE MANAGEMENT AND DIABETES Drugs to know are: Actrapid HM Humulin R, L, U Penmix SUNALI MEHTA The three principal hormones produced by the pancreas are: Insulin: nutrient metabolism:
Page 1 DRUGS FOR GLUCOSE MANAGEMENT AND DIABETES Drugs to know are: Actrapid HM Humulin R, L, U Penmix SUNALI MEHTA The three principal hormones produced by the pancreas are: Insulin: nutrient metabolism:
Diabetes Mellitus. Melissa Meredith M.D. Diabetes Mellitus
 Melissa Meredith M.D. Diabetes mellitus is a group of metabolic diseases characterized by high blood glucose resulting from defects in insulin secretion, insulin action, or both Diabetes is a chronic,
Melissa Meredith M.D. Diabetes mellitus is a group of metabolic diseases characterized by high blood glucose resulting from defects in insulin secretion, insulin action, or both Diabetes is a chronic,
Diabetes mellitus 1 عبد هللا الزعبي. pharmacology. Shatha Khalil Shahwan. 1 P a g e
 Diabetes mellitus 1 pharmacology عبد هللا الزعبي 1 P a g e 4 Shatha Khalil Shahwan Diabetes mellitus The goals of the treatment of diabetes 1. Treating symptoms 2. Treating and Preventing acute complications
Diabetes mellitus 1 pharmacology عبد هللا الزعبي 1 P a g e 4 Shatha Khalil Shahwan Diabetes mellitus The goals of the treatment of diabetes 1. Treating symptoms 2. Treating and Preventing acute complications
1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net
 1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net Diabetes Mellitus (in cats) Diabetes, sugar Affected Animals: Most diabetic cats are older than 10 years of age when they are
1333 Plaza Blvd, Suite E, Central Point, OR 97502 * www.mountainviewvet.net Diabetes Mellitus (in cats) Diabetes, sugar Affected Animals: Most diabetic cats are older than 10 years of age when they are
Diagnosis, classification and prevention of diabetes
 Diagnosis, classification and prevention of diabetes Section 1 1 of 4 Curriculum Module II 1 Diagnosis, classification and presentation of diabetes Slide 2 of 48 Polyurea Definition of diabetes Slide 3
Diagnosis, classification and prevention of diabetes Section 1 1 of 4 Curriculum Module II 1 Diagnosis, classification and presentation of diabetes Slide 2 of 48 Polyurea Definition of diabetes Slide 3
Insulin s Effects on Testosterone, Growth Hormone and IGF I Following Resistance Training
 Insulin s Effects on Testosterone, Growth Hormone and IGF I Following Resistance Training By: Jason Dudley Summary Nutrition supplements with a combination of carbohydrate and protein (with a ratio of
Insulin s Effects on Testosterone, Growth Hormone and IGF I Following Resistance Training By: Jason Dudley Summary Nutrition supplements with a combination of carbohydrate and protein (with a ratio of
Diabetes Mellitus: Type 1
 Diabetes Mellitus: Type 1 What is type 1 diabetes mellitus? Type 1 diabetes is a disorder that happens when your body produces little or no insulin. The lack of insulin causes the level of sugar in your
Diabetes Mellitus: Type 1 What is type 1 diabetes mellitus? Type 1 diabetes is a disorder that happens when your body produces little or no insulin. The lack of insulin causes the level of sugar in your
Overview of Diabetes Management. By Cindy Daversa, M.S.,R.D.,C.D.E. UCI Health
 Overview of Diabetes Management By Cindy Daversa, M.S.,R.D.,C.D.E. UCI Health Objectives: Describe the pathophysiology of diabetes. From a multiorgan systems viewpoint. Identify the types of diabetes.
Overview of Diabetes Management By Cindy Daversa, M.S.,R.D.,C.D.E. UCI Health Objectives: Describe the pathophysiology of diabetes. From a multiorgan systems viewpoint. Identify the types of diabetes.
Reactive Hypoglycemia- is it a real phenomena among endurance athletes? by Dr. Trent Stellingwerff, PhD
 Reactive Hypoglycemia- is it a real phenomena among endurance athletes? by Dr. Trent Stellingwerff, PhD Are you an athlete that periodically experiences episodes of extreme hypoglycemia (low blood sugar)
Reactive Hypoglycemia- is it a real phenomena among endurance athletes? by Dr. Trent Stellingwerff, PhD Are you an athlete that periodically experiences episodes of extreme hypoglycemia (low blood sugar)
Disability Evaluation Under Social Security
 Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY. 12a. FOCUS ON Your Risk for Diabetes. Copyright 2011 Pearson Education, Inc.
 PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY 12a FOCUS ON Your Risk for Diabetes Your Risk for Diabetes! Since 1980,Diabetes has increased by 50 %. Diabetes has increased by 70 percent
PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY 12a FOCUS ON Your Risk for Diabetes Your Risk for Diabetes! Since 1980,Diabetes has increased by 50 %. Diabetes has increased by 70 percent
Management of Clients with Diabetes Mellitus
 Management of Clients with Diabetes Mellitus Black, J.M. & Hawks, J.H. (2005) Chapters 47, (pp 1243-1288) 1288) Baptist Health School of Nursing NSG 4037: Adult Nursing III Carole Mackey, MNSc,, RN, PNP
Management of Clients with Diabetes Mellitus Black, J.M. & Hawks, J.H. (2005) Chapters 47, (pp 1243-1288) 1288) Baptist Health School of Nursing NSG 4037: Adult Nursing III Carole Mackey, MNSc,, RN, PNP
Introduction. We hope this guide will aide you and your staff in creating a safe and supportive environment for your students challenged by diabetes.
 Introduction Diabetes is a chronic disease that affects the body s ability to metabolize food. The body converts much of the food we eat into glucose, the body s main source of energy. Glucose is carried
Introduction Diabetes is a chronic disease that affects the body s ability to metabolize food. The body converts much of the food we eat into glucose, the body s main source of energy. Glucose is carried
EFFIMET 1000 XR Metformin Hydrochloride extended release tablet
 BRAND NAME: Effimet XR. THERAPEUTIC CATEGORY: Anti-Diabetic PHARMACOLOGIC CLASS: Biguanides EFFIMET 1000 XR Metformin Hydrochloride extended release tablet COMPOSITION AND PRESENTATION Composition Each
BRAND NAME: Effimet XR. THERAPEUTIC CATEGORY: Anti-Diabetic PHARMACOLOGIC CLASS: Biguanides EFFIMET 1000 XR Metformin Hydrochloride extended release tablet COMPOSITION AND PRESENTATION Composition Each
Blood Glucose Management
 Blood Glucose Management What Influences Blood Sugar Levels? There are three main things that influence your blood sugar: Nutrition Exercise Medication What Influences Blood Sugar Levels? NUTRITION 4 Meal
Blood Glucose Management What Influences Blood Sugar Levels? There are three main things that influence your blood sugar: Nutrition Exercise Medication What Influences Blood Sugar Levels? NUTRITION 4 Meal
Section 6: Diabetes Emergencies
 Section 6: Diabetes Emergencies SECTION OVERVIEW General Overview Low Blood Glucose (Hypoglycemia) Glucagon High Blood Glucose (Hyperglycemia) Diabetic Ketoacidosis Monitoring Ketones Emergency Medical
Section 6: Diabetes Emergencies SECTION OVERVIEW General Overview Low Blood Glucose (Hypoglycemia) Glucagon High Blood Glucose (Hyperglycemia) Diabetic Ketoacidosis Monitoring Ketones Emergency Medical
X-Plain Diabetes - Introduction Reference Summary
 X-Plain Diabetes - Introduction Reference Summary Introduction Diabetes is a disease that affects millions of Americans every year. Your doctor may have informed you that you have diabetes. Although there
X-Plain Diabetes - Introduction Reference Summary Introduction Diabetes is a disease that affects millions of Americans every year. Your doctor may have informed you that you have diabetes. Although there
N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993
 N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993 The Jail Bulletin is a monthly feature of the Crime Commission Update. The Bulletin may be used as a supplement to your jail in-service training program
N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993 The Jail Bulletin is a monthly feature of the Crime Commission Update. The Bulletin may be used as a supplement to your jail in-service training program
Insulin onset, peak and duration of action
 Insulin onset, peak and duration of action Insulin was first discovered in the early 190 s. Before then, diabetes could not be treated. Insulin was then taken from cow and pig pancreases, but nearly all
Insulin onset, peak and duration of action Insulin was first discovered in the early 190 s. Before then, diabetes could not be treated. Insulin was then taken from cow and pig pancreases, but nearly all
Management of Diabetes Mellitus in Custody
 Recommendations The medico-legal guidelines and recommendations published by the Faculty are for general information only. Appropriate specific advice should be sought from your medical defence organisation
Recommendations The medico-legal guidelines and recommendations published by the Faculty are for general information only. Appropriate specific advice should be sought from your medical defence organisation
written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org
 written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org What Is Insulin? The cells of your body need energy and one source of energy is sugar in your blood. Insulin
written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org What Is Insulin? The cells of your body need energy and one source of energy is sugar in your blood. Insulin
Cardiovascular Disease Risk Factors Part XII Insulin Resistance By James L. Holly, MD Your Life Your Health The Examiner September 15, 2005
 Cardiovascular Disease Risk Factors Part XII By James L. Holly, MD Your Life Your Health The Examiner September 15, 2005 As we approach the end of our extended series on cardiovascular disease risk factors,
Cardiovascular Disease Risk Factors Part XII By James L. Holly, MD Your Life Your Health The Examiner September 15, 2005 As we approach the end of our extended series on cardiovascular disease risk factors,
INSULIN AND INCRETIN THERAPIES: WHAT COMBINATIONS ARE RIGHT FOR YOUR PATIENT?
 INSULIN AND INCRETIN THERAPIES: WHAT COMBINATIONS ARE RIGHT FOR YOUR PATIENT? MARTHA M. BRINSKO, MSN, ANP-BC CHARLOTTE COMMUNITY HEALTH CLINIC CHARLOTTE, NC Diagnosed and undiagnosed diabetes in the United
INSULIN AND INCRETIN THERAPIES: WHAT COMBINATIONS ARE RIGHT FOR YOUR PATIENT? MARTHA M. BRINSKO, MSN, ANP-BC CHARLOTTE COMMUNITY HEALTH CLINIC CHARLOTTE, NC Diagnosed and undiagnosed diabetes in the United
Kansas Behavioral Health Risk Bulletin
 Kansas Behavioral Health Risk Bulletin Kansas Department of Health and Environment November 7, 1995 Bureau of Chronic Disease and Health Promotion Vol. 1 No. 12 Diabetes Mellitus in Kansas Diabetes mellitus
Kansas Behavioral Health Risk Bulletin Kansas Department of Health and Environment November 7, 1995 Bureau of Chronic Disease and Health Promotion Vol. 1 No. 12 Diabetes Mellitus in Kansas Diabetes mellitus
Diabetes and Obesity. The diabesity epidemic
 Diabetes and Obesity Frank B. Diamond, Jr. M.D. Professor of Pediatrics University of South Florida College of Medicine The diabesity epidemic Prevalence of diabetes worldwide was over 135 million people
Diabetes and Obesity Frank B. Diamond, Jr. M.D. Professor of Pediatrics University of South Florida College of Medicine The diabesity epidemic Prevalence of diabetes worldwide was over 135 million people
tips Insulin Pump Users 1 Early detection of insulin deprivation in continuous subcutaneous 2 Population Study of Pediatric Ketoacidosis in Sweden:
 tips Top International Publications Selection Insulin Pump Users Early detection of insulin deprivation in continuous subcutaneous insulin infusion-treated Patients with TD Population Study of Pediatric
tips Top International Publications Selection Insulin Pump Users Early detection of insulin deprivation in continuous subcutaneous insulin infusion-treated Patients with TD Population Study of Pediatric
INSULIN PRODUCTS. Jack DeRuiter
 INSULIN PRODUCTS Jack DeRuiter The number and types of insulin preparations available in the United States is constantly changing, thus students should refer to recent drug resources for a current list
INSULIN PRODUCTS Jack DeRuiter The number and types of insulin preparations available in the United States is constantly changing, thus students should refer to recent drug resources for a current list
Insulin: A Practice Update. Department of Nursing Staff Development Elizabeth Borgelt, MS, RN
 Insulin: A Practice Update Department of Nursing Staff Development Elizabeth Borgelt, MS, RN Learning Outcome The learner will be able to identify the different types of insulins available, their actions,
Insulin: A Practice Update Department of Nursing Staff Development Elizabeth Borgelt, MS, RN Learning Outcome The learner will be able to identify the different types of insulins available, their actions,
Insulin Therapy In Type 2 DM. Sources of support. Agenda. Michael Fischer, M.D., M.S. The underuse of insulin Insulin definition and types
 Insulin Therapy In Type 2 DM Michael Fischer, M.D., M.S. Sources of support NaRCAD is supported by a grant from the Agency for Healthcare Research and Quality My current research projects are funded by
Insulin Therapy In Type 2 DM Michael Fischer, M.D., M.S. Sources of support NaRCAD is supported by a grant from the Agency for Healthcare Research and Quality My current research projects are funded by
Type 2 Diabetes. What is diabetes? Understanding blood glucose and insulin. What is Type 2 diabetes? Page 1 of 5
 Page 1 of 5 Type 2 Diabetes Type 2 diabetes occurs mainly in people aged over 40. The 'first-line' treatment is diet, weight control and physical activity. If the blood glucose level remains high despite
Page 1 of 5 Type 2 Diabetes Type 2 diabetes occurs mainly in people aged over 40. The 'first-line' treatment is diet, weight control and physical activity. If the blood glucose level remains high despite
DIABETIC EDUCATION MODULE ONE GENERAL OVERVIEW OF TREATMENT AND SAFETY
 DIABETIC EDUCATION MODULE ONE GENERAL OVERVIEW OF TREATMENT AND SAFETY First Edition September 17, 1997 Kevin King R.N., B.S., C.C.R.N. Gregg Kunder R.N., B.S.N., C.C.T.C. 77-120 CHS UCLA Medical Center
DIABETIC EDUCATION MODULE ONE GENERAL OVERVIEW OF TREATMENT AND SAFETY First Edition September 17, 1997 Kevin King R.N., B.S., C.C.R.N. Gregg Kunder R.N., B.S.N., C.C.T.C. 77-120 CHS UCLA Medical Center
Therapy Insulin Practical guide to Health Care Providers Quick Reference F Diabetes Mellitus in Type 2
 Ministry of Health, Malaysia 2010 First published March 2011 Perkhidmatan Diabetes dan Endokrinologi Kementerian Kesihatan Malaysia Practical guide to Insulin Therapy in Type 2 Diabetes Mellitus Quick
Ministry of Health, Malaysia 2010 First published March 2011 Perkhidmatan Diabetes dan Endokrinologi Kementerian Kesihatan Malaysia Practical guide to Insulin Therapy in Type 2 Diabetes Mellitus Quick
Management of Diabetes in the Elderly. Sylvia Shamanna Internal Medicine (R1)
 Management of Diabetes in the Elderly Sylvia Shamanna Internal Medicine (R1) Case 74 year old female with frontal temporal lobe dementia admitted for prolonged delirium and frequent falls (usually in the
Management of Diabetes in the Elderly Sylvia Shamanna Internal Medicine (R1) Case 74 year old female with frontal temporal lobe dementia admitted for prolonged delirium and frequent falls (usually in the
TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY. Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU
 TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU Objectives: 1. To discuss epidemiology and presentation
TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU Objectives: 1. To discuss epidemiology and presentation
Diabetes Management Tube Feeding/Parenteral Nutrition Order Set (Adult)
 Review Due Date: 2016 May PATIENT CARE ORDERS Weight (kg) Known Adverse Reactions or Intolerances DRUG No Yes (list) FOOD No Yes (list) LATEX No Yes ***See Suggestions for Management (on reverse)*** ***If
Review Due Date: 2016 May PATIENT CARE ORDERS Weight (kg) Known Adverse Reactions or Intolerances DRUG No Yes (list) FOOD No Yes (list) LATEX No Yes ***See Suggestions for Management (on reverse)*** ***If
SCHOOL DISTRICT #22 VERNON DIABETES POLICY
 SCHOOL DISTRICT #22 VERNON DIABETES POLICY A student with diabetes does not automatically qualify for additional support. The student may qualify as a temporary D category (chronic health) after diagnosis
SCHOOL DISTRICT #22 VERNON DIABETES POLICY A student with diabetes does not automatically qualify for additional support. The student may qualify as a temporary D category (chronic health) after diagnosis
Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes
 Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes U.S. Department of Health and Human Services Food and Drug Administration Center
Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes U.S. Department of Health and Human Services Food and Drug Administration Center
The first injection of insulin was given on
 EFFECTIVE USE OF INSULIN THERAPY IN TYPE 2 DIABETES * Bernard Zinman, MDCM ABSTRACT Type 2 diabetes is a progressive disease; an individual s ability to secrete insulin in increasing amounts to overcome
EFFECTIVE USE OF INSULIN THERAPY IN TYPE 2 DIABETES * Bernard Zinman, MDCM ABSTRACT Type 2 diabetes is a progressive disease; an individual s ability to secrete insulin in increasing amounts to overcome
Guidelines. for Sick Day Management for People with Diabetes
 Guidelines for Sick Day Management for People with Diabetes When to Follow Sick Day Guidelines These guidelines apply when the person with diabetes is feeling unwell or noticing signs of an illness and/
Guidelines for Sick Day Management for People with Diabetes When to Follow Sick Day Guidelines These guidelines apply when the person with diabetes is feeling unwell or noticing signs of an illness and/
Diabetes. Emergency Checklists. From A Child in Your Care Has Diabetes. A Collection of Information. Copyright 2005 by Elisa Hendel, M.Ed.
 Diabetes Emergency Checklists From A Child in Your Care Has Diabetes. A Collection of Information. Copyright 2005 by Elisa Hendel, M.Ed. Hyperglycemia High Blood Sugar * Hyperglycemia occurs when the blood
Diabetes Emergency Checklists From A Child in Your Care Has Diabetes. A Collection of Information. Copyright 2005 by Elisa Hendel, M.Ed. Hyperglycemia High Blood Sugar * Hyperglycemia occurs when the blood
Insulin pen start checklist
 Insulin pen start checklist Topic Instruction Date & Initials 1. Cognitive Assessment 2. Insulin Delivery loading appropriate mixing priming shot dialing up dose delivery of insulin 3. Insulin type/action
Insulin pen start checklist Topic Instruction Date & Initials 1. Cognitive Assessment 2. Insulin Delivery loading appropriate mixing priming shot dialing up dose delivery of insulin 3. Insulin type/action
The Family Library. Understanding Diabetes
 The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
Basal Insulin Analogues Where are We Now?
 232 Medicine Update 41 Basal Insulin Analogues Where are We Now? S CHANDRU, V MOHAN Insulin is a polypeptide secreted by the beta cells of pancreas and consists of 51 amino acids (AA). It has two polypeptide
232 Medicine Update 41 Basal Insulin Analogues Where are We Now? S CHANDRU, V MOHAN Insulin is a polypeptide secreted by the beta cells of pancreas and consists of 51 amino acids (AA). It has two polypeptide
Diabetic Emergencies. David Hill, D.O.
 Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
Diabetic Emergencies David Hill, D.O. Class Outline Diabetic emergency/glucometer training Identify the different signs of insulin shock Diabetic coma, and HHNK Participants will understand the treatment
Insulin Treatment. J A O Hare. www.3bv.org. Bones, Brains & Blood Vessels
 Insulin Treatment J A O Hare www.3bv.org Bones, Brains & Blood Vessels Indications for Insulin Treatment Diabetic Ketoacidosis Diabetics with unstable acute illness ICU Gestational Diabetes: diet failure
Insulin Treatment J A O Hare www.3bv.org Bones, Brains & Blood Vessels Indications for Insulin Treatment Diabetic Ketoacidosis Diabetics with unstable acute illness ICU Gestational Diabetes: diet failure
Safe use of insulin e- learning module
 Safe use of insulin e- learning module Page 1 Introduction Insulin is a hormone produced by the beta cells in the pancreas, it is released when blood glucose levels are raised for example after a meal.
Safe use of insulin e- learning module Page 1 Introduction Insulin is a hormone produced by the beta cells in the pancreas, it is released when blood glucose levels are raised for example after a meal.
TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION. Robert Dobbins, M.D. Ph.D.
 TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION Robert Dobbins, M.D. Ph.D. Learning Objectives Recognize current trends in the prevalence of type 2 diabetes. Learn differences between type 1 and type
TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION Robert Dobbins, M.D. Ph.D. Learning Objectives Recognize current trends in the prevalence of type 2 diabetes. Learn differences between type 1 and type
Nutrition. Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT
 1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides.
 Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides. Example: = Head Over Heels Take a moment Confer with your neighbour And try to solve the following word
Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides. Example: = Head Over Heels Take a moment Confer with your neighbour And try to solve the following word
CHAPTER V DISCUSSION. normal life provided they keep their diabetes under control. Life style modifications
 CHAPTER V DISCUSSION Background Diabetes mellitus is a chronic condition but people with diabetes can lead a normal life provided they keep their diabetes under control. Life style modifications (LSM)
CHAPTER V DISCUSSION Background Diabetes mellitus is a chronic condition but people with diabetes can lead a normal life provided they keep their diabetes under control. Life style modifications (LSM)
HUMULIN R REGULAR INSULIN HUMAN INJECTION, USP (rdna ORIGIN) 100 UNITS PER ML (U-100)
 1 PATIENT INFORMATION HUMULIN R REGULAR INSULIN HUMAN INJECTION, USP (rdna ORIGIN) 100 UNITS PER ML (U-100) WARNINGS Do not share your syringes with other people, even if the needle has been changed. You
1 PATIENT INFORMATION HUMULIN R REGULAR INSULIN HUMAN INJECTION, USP (rdna ORIGIN) 100 UNITS PER ML (U-100) WARNINGS Do not share your syringes with other people, even if the needle has been changed. You
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Afrezza Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Afrezza (human insulin) Prime Therapeutics will review Prior Authorization requests Prior Authorization
Afrezza Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Afrezza (human insulin) Prime Therapeutics will review Prior Authorization requests Prior Authorization
INSULINThere are. T y p e 1 T y p e 2. many different insulins for
 T y p e 1 T y p e 2 INSULINThere are many different insulins for Characteristics The three characteristics of insulin are: Onset. The length of time before insulin reaches the bloodstream and begins lowering
T y p e 1 T y p e 2 INSULINThere are many different insulins for Characteristics The three characteristics of insulin are: Onset. The length of time before insulin reaches the bloodstream and begins lowering
A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration
 of nurse A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration 1. Check times for point of care meter blood glucose testing. Pre-Breakfast
of nurse A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration 1. Check times for point of care meter blood glucose testing. Pre-Breakfast
Your Life Your Health Cariodmetabolic Risk Syndrome Part VII Inflammation chronic, low-grade By James L. Holly, MD The Examiner January 25, 2007
 Your Life Your Health Cariodmetabolic Risk Syndrome Part VII Inflammation chronic, low-grade By James L. Holly, MD The Examiner January 25, 2007 The cardiometabolic risk syndrome is increasingly recognized
Your Life Your Health Cariodmetabolic Risk Syndrome Part VII Inflammation chronic, low-grade By James L. Holly, MD The Examiner January 25, 2007 The cardiometabolic risk syndrome is increasingly recognized
Faculty. Program Objectives. Introducing the Problem. Diabetes is a Silent Killer. Minorities at Greater Risk of Having Type 2 Diabetes
 Diabetes: The Basics Understanding and Managing Diabetes (Part 1 of 3) Satellite Conference Tuesday, October 18, 2005 2:00-4:00 p.m. (Central Time) Produced by the Alabama Department of Public Health Video
Diabetes: The Basics Understanding and Managing Diabetes (Part 1 of 3) Satellite Conference Tuesday, October 18, 2005 2:00-4:00 p.m. (Central Time) Produced by the Alabama Department of Public Health Video
Shared Care Agreement Insulin Degludec (Tresiba )
 Licensed Indication Shared Care Agreement Insulin Degludec (Tresiba ) Insulin Degludec is licensed for the treatment of diabetes mellitus in adults. Countess of Chester prescribing guidelines Restricting
Licensed Indication Shared Care Agreement Insulin Degludec (Tresiba ) Insulin Degludec is licensed for the treatment of diabetes mellitus in adults. Countess of Chester prescribing guidelines Restricting
Insulin therapy in various type 1 diabetes patients workshop
 Insulin therapy in various type 1 diabetes patients workshop Bruce H.R. Wolffenbuttel, MD PhD Dept of Endocrinology, UMC Groningen website: www.umcg.net & www.gmed.nl Twitter: @bhrw Case no. 1 Male of
Insulin therapy in various type 1 diabetes patients workshop Bruce H.R. Wolffenbuttel, MD PhD Dept of Endocrinology, UMC Groningen website: www.umcg.net & www.gmed.nl Twitter: @bhrw Case no. 1 Male of
Type 2 Diabetes Type 2 Diabetes
 Pennington Nutrition Series Healthier lives through education in nutrition and preventive medicine Pub No. 33 Type 2 is the most common form of diabetes. In this form, the body does not produce enough
Pennington Nutrition Series Healthier lives through education in nutrition and preventive medicine Pub No. 33 Type 2 is the most common form of diabetes. In this form, the body does not produce enough
Practical Applications of Insulin Pump Therapy in Type 2 Diabetes
 Practical Applications of Insulin Pump Therapy in Type 2 Diabetes Wendy Lane, MD For a CME/CEU version of this article please go to www.namcp.org/cmeonline.htm, and then click the activity title. Summary
Practical Applications of Insulin Pump Therapy in Type 2 Diabetes Wendy Lane, MD For a CME/CEU version of this article please go to www.namcp.org/cmeonline.htm, and then click the activity title. Summary
Diabetes Insulin Pump Health Care Plan District Nurse Phone: 262-560-2104 District Nurse Fax: 262-560-2106
 EMPOW ERING A COMMUNITY OF LEARNERS AND LEADERS Diabetes Insulin Pump Health Care Plan District Nurse Phone: 262-560-2104 District Nurse Fax: 262-560-2106 Student DOB School Grade Doctor Phone School Year
EMPOW ERING A COMMUNITY OF LEARNERS AND LEADERS Diabetes Insulin Pump Health Care Plan District Nurse Phone: 262-560-2104 District Nurse Fax: 262-560-2106 Student DOB School Grade Doctor Phone School Year
Understanding and Managing Type 2 Diabetes
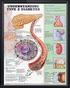 VEA Bringing Learning to Life Program Support Notes Understanding and Managing Type 2 Diabetes Professional Development 32mins Teacher Notes by Anne Hill, Nurse Educator Produced by VEA Pty Ltd Commissioning
VEA Bringing Learning to Life Program Support Notes Understanding and Managing Type 2 Diabetes Professional Development 32mins Teacher Notes by Anne Hill, Nurse Educator Produced by VEA Pty Ltd Commissioning
