Post-operative rehabilitation guidelines Latissimus Dorsi Transfer to Posterosuperior Cuff
|
|
|
- Tobias Bailey
- 10 years ago
- Views:
Transcription
1 Post-operative rehabilitation guidelines Latissimus Dorsi Transfer to Posterosuperior Cuff Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must demonstrate all exercises to a patient. We cannot be held liable for the outcome of you undertaking any of the exercises outlined here independently of direct supervision from the RNOH. Please read these guidelines with consideration to the specific physiotherapy discharge report that will be sent to the physiotherapist concerned. There may be individual variation that is patient specific in which case these general guidelines will have to be modified as appropriate by the physiotherapist. At RNOH, our emphasis is patient-specific, not condition-specific rehabilitation which encourages recognition of those patients who may progress slower than others. We also want to encourage clinical reasoning based on the continuum concept of shoulder rehabilitation i.e. similar rehabilitation tools are used for each shoulder procedure but the time of intervention varies according to the status of the tissues at pre-op, at surgery and the post-op restrictions. Most of our procedures at RNOH have guidelines that fall into categories loosely based on the Matsen classification of shoulder dysfunction rather than having specific guidelines for each of our more established procedures however, as this particular procedure is often used to supplement another it is difficult to necessarily generalise and suggest which classification it should be in therefore, for now, these guidelines stand alone! Our hope is that by providing guidelines and treatment ideas, it will promote an equitable rehabilitation service to all of our patients and improve the overall understanding of the unique challenges that rehabilitation of the shoulder complex presents. Milestone driven Apart from phase one of the post-operative care which is based upon tissue healing times and surgical opinion, these guidelines are milestone driven and designed to provide an equitable rehabilitation service to all of our patients. The time periods documented at the beginning of each phase are purely there as a rough guide. We hope the guidelines will limit unnecessary visits to the outpatient clinic at the RNOH by helping the patient and therapist to identify when specialist review is required. If the patient and the therapist feel that rehabilitation is progressing satisfactorily and there are no concerns, the patient may cancel and re-book their follow up for a later date. Failure to progress or variations from the norm should be the main reason for clinic attendance. Both patients and therapists can book clinic visits by contacting the numbers given in this document. It is essential you contact us if you have any concerns:
2 Physiotherapy Team /5519 Occupational Therapy Team Consultant Team Secretaries /5727 Surgical Indications for Latissimus Dorsi Transfer to Posterior Cuff Inability to actively place and hold the arm in a functional position in front of the body at waist level due to lack of active external rotation at the shoulder. - e.g. following Brachial Plexus Injury/Neurological Compromise, Irreparable Massive Cuff Tears. Being unable to place the arm in this position will prevent the ability to achieve the starting positions required for an Anterior Deltoid Programme should it be required. Inability to * snug the humeral head on initiation of abduction. This can lead to pain and decreased function in elevation. - e.g. secondary to posterosuperior cuff failure. * Snugging of the humeral head is a term we often use to explain the normal subtle movement of the humeral head as it centres towards the glenoid prior to any movement of the GHJ. This action is normally produced by a functioning cuff. It is tested with gently resisted abduction of the shoulder and the down and in motion of the humeral head is observed. Possible surgical complications Infection Neurovascular compromise Joint stiffness Failure of the transfer Expected long-term outcome When used to supplement a rotator cuff repair, expected outcome may take 9-24 months to achieve. Post neurological injury/bpl our experience shows that changes can continue to develop for up to 4-5 years post transfer. For patients who have had the transfer to supplement a cuff repair, the expected long term outcome should be similar to that of a standard cuff repair, but the time taken to achieve it will be longer due to the early restrictions and the time taken to re-educate the function of the Latissimus Dorsi muscle. This operation is sometimes undertaken in conjunction with other operative procedures such as Total Shoulder Replacements (TSR) therefore it is imperative that all components and limitations of the surgery are taken into consideration. A standard goal for all patients is to report a pain-free shoulder (other underlying pathology to be considered) that can be held comfortably in neutral rotation at waist level allowing for increased functional activity. Further progress from this stage and long-term functional outcome is dependent on the underlying pathology/neuropathology/additional surgery rather than purely the latissimus transfer itself and it is important that the patient s goals and expectations are realistic at the outset.
3 In-patient post op care plan The RNOH Shoulder Physiotherapy Service follows this care plan prior to discharge. Goals: 1. To educate the patient on post operative instructions and expected outcomes following surgical procedure this may include explaining the purpose of an in-patient rehabilitation admission for initiating Phase 2 in the future. 2. To explain the purpose of the patient s specific support ie spica or abduction pillow and demonstrate ideal positioning/how to alter and remove components of spica/abduction pillow for exercises - within post-operative restrictions. 3. To ensure patient is safe mobilizing on ward with arm immobilized in spica or abduction pillow and feels they can manage stairs/check they can manage stairs, with arm immobilized (as appropriate). 4. To teach scapular setting and hand/wrist/elbow ROM exercises (where appropriate). 5. To teach and ensure that the patient and/or carers are competent with the post operative exercise programme and can maintain the programme post discharge. 6. To ensure all patients requiring further physiotherapy are given a copy of their outpatient referral prior to discharge and are aware that they can contact the Shoulder Service if local services fail to provide a timely appointment. 7. To fax/send physiotherapy referral with patient specific guidelines and information about accessing generic guidelines to local physiotherapy team (as appropriate). Initial rehabilitation phase one: For Latissimus Dorsi Transfer to Posterosuperior Cuff Discharge 8 (or 12) weeks (Dependent on patient specific post-op instructions)
4 If additional major surgery was carried out in conjunction with the transfer, the guidelines may vary. The integrity and tension of the graft will drive the decisions regarding Phase One. Goals: 1. Ensure Wound/Tissue Healing (as able, according to method of immobilization ie spica or abduction pillow). 2. Encourage effective pain control. 3. Ensure patient is safe mobilizing with spica/abduction pillow. 4. Maintain/Increase Passive/Active-Assisted ROM -ranges will be documented on patient specific referral. 5. Initiate scapular control. 6. Continue Isometrics (IR+ER) and eccentric ER -only if documented on patient specific referral. Restrictions: 1. The patient is not to lower the arm from the abduction pillow or remove abduction pillow or spica. 2. No exercises to be carried out, other than those outlined in the post-op plan, that would affect the graft. 3. Exercise should remain relatively pain-free. Education: Patient education on anatomy of shoulder complex, post-op restrictions, progression of short/long term goals in conjunction with guidelines, postural advice/retraining. Milestones to progress to phase two: 1. Adequate pain control. 2. Adequate scapular control. 3. Achieved time specific goals specified on individual referral. Often, to initiate this next phase, the patient will be brought into RNOH rehabilitation ward for one week especially if they have been immobilised in a plaster spica, if this is not due to happen, please progress.. Goals: Rehabilitation phase two: Approx weeks 8 (or 12) to 9 months
5 Restrictions: 1. To hold and maintain at least 30 degrees ER with the elbow supported on the abduction pillow (ie with the arm resting at approx 40 degrees scaption). 2. To be able to eccentrically control the arm from 30 degrees ER position on abduction pillow, back to rest on abduction pillow. 3. (After achieving 1 & 2 above) To wean off the abduction pillow, deflating it, lowering the arm on the support, whist ensuring some control is still achievable as the abduction component decreases. 4. To start to use the arm at waist level for functional activity. 1. Where possible, minimize exercises that may exacerbate pain. 2. Once in this phase, even prior to gaining control, the patient can remove the support for washing/dressing etc, but should return to the abducted/ neutral rotation position at other times so as not to over-stretch the graft, making it harder to gain activity this resting position can be on an armchair or table at times if the patient prefers. 3. Avoid removing the abduction pillow too quickly even though the patient will want to be rid of it! Continue using it for resting and exercises until the patient is able to isometrically hold at approx 30 degrees ER so as to avoid stretching the graft and therefore compromising the ability to recruit to the muscle. 4. Avoid GHJ stretching other than to achieve the ranges required for the goals above. Advice: It is important to remember that when working through these very basic stages, the exercises are not about just strengthening the muscle the muscle/tendon transfer itself would have been of adequate quality and strength in it s previous position and function, and although it has been disrupted and immoblised and therefore weakened, strengthening as such, is not the main focus. The important concept is that of developing the neuromuscular control of the muscle in its new roles as an external rotator and posterosuperior stabilizer of the humeral head. Latissimus Dorsi has always worked predominantly as an internal rotator and adductor of the GHJ and as a depressor of the shoulder girdle. In its new role, it will still depress the shoulder girdle and adduct the GHJ, but it now has to externally rotate the shoulder and assist the remaining cuff (if applicable) to *snug the humeral head onto the glenoid. You will need to initially get cognitive control of the new role and then eventually, as neuroplasticity takes place, it will hopefully become more automatic. Some ideas to assist the exercise progression: In the 40/45 degrees position on the abduction pillow, assist the ER movement to 30/40 degrees as able and encourage holding with the addition of some adduction/depression i.e. using part of the old role to
6 activate the LD muscle, but assist the new ER position as the patient is able to hold it isometrically, try to decrease the active adduction component. Don t request a maximum contraction it is not about strength but activating the muscle appropriately perhaps try 30% effort as a starting point. Use biofeedback if you have the facility, placed on the belly of the LD transfer, to give visual feedback as to when the transfer is working and encourage the holding even if still supported Use FES in a similar way to the biofeedback, giving sensation feedback as to how to activate the muscle join in with it. Place a hand on the area to give proprioceptive feedback so the patient knows where the contraction should be happening and can get some feedback. Manually facilitate the adduction/depression component that you are trying to activate whilst the patient joins in. Repetition! Repetition! Repetition! Use degrees of ER as this is roughly the mid to inner range of the transfer and therefore, from a length-tension relationship point of view, it should be easier! However, if the patient is struggling, vary the degree of ER. Once you have the isometric hold, work on eccentric lowering back to neutral rotation i.e. back to the abduction pillow gaining control this way will prevent hitching /elevating of the scapula and it appears to gain control more easily than working concentrically. Hydrotherapy can be useful to assist with the upper limb control and also with general scapulothoracic control, core stability etc Education: Patient education about the reasoning behind the exercises and the need for continuing abduction/er support, ongoing postural education. Milestones to progress to Phase Three: (if this is much sooner than 9 months please still progress that is the purpose of milestones rather than specified time periods) 1. To be able to hold the arm at approx 30 degrees ER with the arm resting at approx 40 degrees scaption/abduction. 2. To be able to eccentrically control the arm from approx 30 degrees ER position back to neutral when resting at approx 40 degrees scaption/ abduction. 3. To have weaned off the abduction pillow and be using arm at low level for light activities. Once these milestones have been achieved, if there are no other reasons for restricting it, driving can be restarted if the patient feels safe to do so. Rehabilitation phase three: Approx 9 months+ (Dependent on underlying pathology and other rehab requirements)
7 Regardless of whatever additional operation your patient has had, the information below incorporates the final progression of the LD transfer +/- other operations. At this stage if your patient has also had an additional Total Shoulder Replacement or Rotator Cuff Repair see Smooth and Weak Guidelines for more specific guidance if required, and work through the phases according to the milestones outlined. Goals: For those without an existing, functioning Rotator Cuff: 1. To restore full active range of movement (patient specific). 2. To achieve MMT grade 3/5 from an internally rotated position to neutral rotation at 0 degrees abduction achieving a comfortable neutral position, but not necessarily being able to achieve full MMT grade 3/5 through full passive ER range. 3. To develop automatic control of ER and endurance of appropriate muscle groups (patient specific) and relate to functional tasks. For those without an existing, functioning Rotator Cuff, but a functioning Deltoid: 1. To restore full active range of movement (patient specific). 2. To achieve MMT grade 3/5 from an internally rotated position to neutral rotation at 0 degrees abduction achieving a comfortable neutral position, but not necessarily being able to achieve full MMT grade 3/5 through full passive ER range. 3. To develop automatic control of ER and endurance of appropriate muscle groups (patient specific) and relate to functional tasks. 4. To work through an Eccentric Deltoid Programme and maximize functional range. For those who have had the transfer to supplement an existing cuff/cuff repair: 1. To restore full active range of movement (patient specific). 2. To achieve grade MMT 3/5 through rotation range. 3. To develop automatic control of ER and endurance of appropriate muscle groups (patient specific) and relate to functional tasks. 4. To recruit the LD transfer to achieve snugging of the humeral head automatically on the initiation of abduction. 5. To progress Rotator Cuff/Transfer control initially to the exclusion of Deltoid in varying positions through range and without inappropriate muscle patterning (Pecs, Traps, etc) and then to progress control through full functional range with addition of Deltoid. For all patients - try to restore scapulohumeral rhythm, maintain core and postural control and address all other aspects of the kinetic chain as required to maximize function. Restrictions: 1. Where possible minimize exercises that may exacerbate pain.
8 2. If the patient has an active Rotator Cuff, ensure it is functioning well at a low level and the humeral head is snugging into the glenoid prior to progressing to active exercises above shoulder level. Education: Patient education around pacing of activity. Return to sporting activity initially non contact. Caution to be taken with previously aggravating activities. Ongoing postural education. Normal movement with functional activities. To remind regarding the purpose of the LD transfer for each individual patient so that expectations are realistic. Some ideas to assist the exercise progression (as appropriate): When stretching, start with active-assisted stretches into range considering the expected outcome as to how much range is going to be needed for long term goals. Maintain and monitor the ER control that has been gained closely as you start to stretch the GHJ as you are now stretching the graft and could lose control if you stretch too quickly. Use capsular stretches as required for anterior and posterior capsule again, monitoring the active ER gains that have been made and ensuring these are maintained. Use slings and springs or hydrotherapy to offload the arm, allowing low level cuff exercises (as appropriate), now treating the LD transfer as posterosuperior cuff, add resistance and decrease support as control improves. If using therabands, use a maximum strength of a yellow band if you are trying to target just the cuff itself. Monitor the transfer activity during exercises (with biofeedback/palpation) to ensure that it is now activating appropriately as posterosuperior cuff. Still use the concepts of initiating old functions of LD while trying to achieve new functions to recruit appropriately as in Phase Two assisting with manual, visual, proprioceptive feedback and facilitation where required. As the control improves at waist level, incorporate more functional activities to try to make the transition from cognitive control of the graft to automatic control. Use a closed and open chain exercise programme. Address and strengthen LD s original and ongoing action of scapula depression, GHJ adduction and extension from a flexed position For information on cuff exercises and Anterior Deltoid exercises see Smooth and Weak Guidelines and exercise examples on the RNOH web page. Address general core control and proprioceptive deficits - consider Kibler et al, Principles of Kinetic chain and the incorporation of lower limb exercises. Failure to progress: If a patient is failing to progress, then consider the following:
9 Possible problem Action Pain Inhibition Adequate analgesia Maintain pain free exercises Return to passive stretches if appropriate Slow rehab programme If severe night/resting pain then refer to Shoulder Unit Inability to gain any activity in Try exercise ideas outlined in phase two and if no LD Graft flicker can be elicited at all by six months, refer to Shoulder Unit Poor Rotator Cuff Control Ensure snugging is taking place ie the transfer is once Transfer seems to be working automatically as posterosuperior cuff if not working reasonably well in revert back to ideas in phase three isolation Ensure passive range is gained Isometrics through range Rotation dissociation (cuff control without additional muscle assistance or scapula movement) through range with decreasing levels of support and increasing resistance Slow progression through theraband resistances (e.g. Yellow/white tend to bias cuff and green tend to incorporate deltoid) Inability to activate Deltoid Ensure there is innervation to Deltoid i.e. check for for an Eccentric Deltoid history of nerve damage Programme Try activating a static contraction at low level to give (having checked Smooth patient feedback as to which muscle should be and Weak Guidelines and working Eccentric Deltoid Exercises Ensure the humeral head is located beneath the for ideas) acromion in passive elevation Try to maximize passive ER at 90 degrees flexion, to ensure the position is encouraging anterior Deltoid activity Ensure that at least 100 degrees passive flexion can be achieved with ease, and more if possible, as in positions lower than 90 degrees, the weight of the limb acting through a longer lever against gravity will increase the work of Deltoid If still concerned, refer to Shoulder Unit Poor Scapular Control Work on scapular setting through range without pec and/or lat overactivity Try closed chain exercises to increase proprioception Consider prone lying to develop control/awareness Poor Core Stability Develop patient appropriate stability programme Secondary frozen shoulder Maintain passive ROM as able specifically in flexion Use manual mobilizations if appropriate
10 Patient exercising too Education on pacing, risks of flare-up scenario vigorously Poor patient compliance with Set functional based goals HEP Return to ADL too soon Reduce activity levels Cervical/thoracic referred Assess and treat pain Altered neurodynamics Assess and treat Many thanks for your help The Shoulder Unit, RNOH References of interest: Iannotti J, et al (2006) Latissimus Dorsi Tendon Transfer for Irreparable Posterosuperior Rotator Cuff Tears: Factors Affecting Outcome, The Journal of Bone and Joint Surgery (American);88: This (albeit small study) suggests that there is a better clinical result when there is synchronous contraction of the transfer present with ER and flexion Aoki M, et al (1996) Transfer of Latissimus Dorsi for Irreparable Rotator-Cuff Tears The Journal of Bone and Joint Surgery [Br];78-B: Again, it is noted that the patients with the poorer results demonstrated nonsynergistic action of the transferred Latissimus Dorsi and the supraspinatus Gerber (1992) Latissimus Dorsi Transfer for the Treatment of Irreparable Tears of the Rotator Cuff, Clinical Orthopaedics and Related Research: 275: Holt M, et al GOST3: Guide for Orthopaedic Surgeons and Therapists, 3rd Ed, Liverpool Upper Limb Unit and South Manchester University Hospitals Trust, Biomet-Merck. - Very useful resource for sample exercises especially glenohumeral rotation control and closed kinetic chain. Contact Biomet-Merck for copies. Kibler W B, et al (2001) 'Shoulder rehabilitation strategies, guidelines and practice', Orthopaedic Clinics of North America, 32, 3, McMullen J and Uhl T, (2000) 'A kinetic chain approach for shoulder rehabilitation', Journal of Athletic Training, 35, 3, Tania Douglas Updated May 2009 (review date May 2011)
Rehabilitation Guidelines for Post-Operative Stiff Shoulder
 Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair
 Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist
Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Arthroscopic Rotator Cuff Repair Postoperative Rehab Protocol Starting the first day after surgery you should remove the sling 3-4 times per day to perform pendulum exercises and elbow/wrist range of motion
Arthroscopic Rotator Cuff Repair Postoperative Rehab Protocol Starting the first day after surgery you should remove the sling 3-4 times per day to perform pendulum exercises and elbow/wrist range of motion
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Rotator Cuff Repair
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com
 North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior
 Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Rehabilitation Protocol: SLAP Superior Labral Lesion Anterior to Posterior Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes
 SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It
SLAP Lesion Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It
Biceps Tenodesis Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463
 Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
Phase I Passive Range of Motion Phase (postop week 1-2) Minimize shoulder pain and inflammatory response Achieve gradual restoration of gentle active range of motion Enhance/ensure adequate scapular function
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
2. Repair of the deltoid - the amount deltoid was released and security of repair
 Johns Hopkins Shoulder Surgery Rotator Cuff Rehabilitation Program Johns Hopkins Shoulder Surgeons INTRODUCTION: This program is designed for rotator cuff repairs involving fixation of the tendon to bone,
Johns Hopkins Shoulder Surgery Rotator Cuff Rehabilitation Program Johns Hopkins Shoulder Surgeons INTRODUCTION: This program is designed for rotator cuff repairs involving fixation of the tendon to bone,
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair
 Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm
 Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm *It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual
Combined SLAP with Arthroscopic Rotator Cuff Repair Large to Massive Tears = or > 3 cm *It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual
Copeland Surface Replacement Arthroplasty (Hannan Mullett)
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
10/1/2007. Philosophy. Pune Shoulder Rehabilitation Programme (PSRP) 9 th Annual TRAC meeting, Budapest. Principles -I. Design. Study-I.
 Dr. Ashish Babhulkar D.Orth., DNB(Orth.), MCh.Orth.(Liverpool,UK.),FRCS(Tr. & Orth.) Shoulder & Joint Replacement Surgeon Pune, India Pune Shoulder Rehabilitation Programme (PSRP) Philosophy Design an
Dr. Ashish Babhulkar D.Orth., DNB(Orth.), MCh.Orth.(Liverpool,UK.),FRCS(Tr. & Orth.) Shoulder & Joint Replacement Surgeon Pune, India Pune Shoulder Rehabilitation Programme (PSRP) Philosophy Design an
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital we recognise that our broad and often complex patient
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Department of Rehabilitation Services Physical Therapy This protocol has been adopted from Brotzman & Wilk, which has been published in Brotzman SB, Wilk KE, Clinical Orthopeadic Rehabilitation. Philadelphia,
Department of Rehabilitation Services Physical Therapy This protocol has been adopted from Brotzman & Wilk, which has been published in Brotzman SB, Wilk KE, Clinical Orthopeadic Rehabilitation. Philadelphia,
Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood
 Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood Indications: Posterior shoulder instability is a relatively uncommon finding in normal adult shoulders. The most common
Postoperative Protocol For Posterior Labral Repair/ Capsular Plication-- Dr. Trueblood Indications: Posterior shoulder instability is a relatively uncommon finding in normal adult shoulders. The most common
Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes
 Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic anterior stabilization procedure.
Anterior Shoulder Instability Surgical Repair Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic anterior stabilization procedure.
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF)
 ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF) Phase I Immediate Post Surgical Phase (Weeks 1-4): Maintain integrity of repair Diminish pain and inflammation Prevent muscular inhibition Independent
ARTHROSCOPIC ROTATOR CUFF REPAIR PROTOCOL (DR. ROLF) Phase I Immediate Post Surgical Phase (Weeks 1-4): Maintain integrity of repair Diminish pain and inflammation Prevent muscular inhibition Independent
Rehabilitation Guidelines For SLAP Lesion Repair
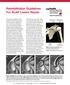 Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears)
 SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears) This protocol has been modified and is being used with permission from the BWH Sports and Shoulder Service. The
SLAP Repair Protocol Arthroscopic Labral Repair Protocols (Type II, IV and Complex Tears) This protocol has been modified and is being used with permission from the BWH Sports and Shoulder Service. The
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
Important rehabilitation management concepts to consider for a postoperative physical therapy rtsa program are:
 : General Information: Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff
: General Information: Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair
 Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Dr. Benjamin Hewitt. Shoulder Stabilisation
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Shoulder Stabilisation The shoulder is the most flexible joint in the body, allowing
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Shoulder Stabilisation The shoulder is the most flexible joint in the body, allowing
Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
 LUKE S. CHOI, M.D. 14825 N. Outer Forty Road, Suite 360 Chesterfield, MO 63017 Office: (314) 392-5063 Fax: (314) 336-2571 Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
LUKE S. CHOI, M.D. 14825 N. Outer Forty Road, Suite 360 Chesterfield, MO 63017 Office: (314) 392-5063 Fax: (314) 336-2571 Shoulder Arthroscopy Combined Arthoscopic Labrum Repair Rehabilitation Protocol
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair
 UW Health SpoRTS Rehabilitation Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair The anatomic configuration of the shoulder joint (glenohumeral joint)
UW Health SpoRTS Rehabilitation Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair The anatomic configuration of the shoulder joint (glenohumeral joint)
POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL
 POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL The goal of this rehabilitation program is to return the patient/athlete to their activity/sport as quickly and safely as possible while maintaining a stable
POSTERIOR CAPSULAR SHIFT REHABILITATION PROTOCOL The goal of this rehabilitation program is to return the patient/athlete to their activity/sport as quickly and safely as possible while maintaining a stable
LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ
LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
 ORTHOPAEDIC WARD: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
ORTHOPAEDIC WARD: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY/ SHOULDER DECOMPRESSION
Overhead Strength Training for the Shoulder: Guidelines for Injury Prevention and Performance Training Success
 Overhead Strength Training for the Shoulder: Guidelines for Injury Prevention and Performance Training Success Robert Panariello MS, PT, ATC, CSCS Strength training is an important component in the overall
Overhead Strength Training for the Shoulder: Guidelines for Injury Prevention and Performance Training Success Robert Panariello MS, PT, ATC, CSCS Strength training is an important component in the overall
ROTATOR CUFF TEARS SMALL
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
REVERSE SHOULDER ARTHROPLASTY
 William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.com REVERSE SHOULDER ARTHROPLASTY The shoulder is a ball
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.com REVERSE SHOULDER ARTHROPLASTY The shoulder is a ball
POST OPERATIVE ROTATOR CUFF REPAIR PROTOCOL. Therapist Instructions
 MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
J F de Beer, K van Rooyen, D Bhatia. Rotator Cuff Tears
 1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
.org. Rotator Cuff Tears: Surgical Treatment Options. When Rotator Cuff Surgery is Recommended. Surgical Repair Options
 Rotator Cuff Tears: Surgical Treatment Options Page ( 1 ) The following article provides in-depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article Rotator
Rotator Cuff Tears: Surgical Treatment Options Page ( 1 ) The following article provides in-depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article Rotator
SHOULDER INSTABILITY IN PATIENTS WITH EDS
 EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
Post-operative Rehabilitation Following Arthroscopic Rotator Cuff Repair
 Post-op ARCR - Ticker/Egan 1 Post-operative Rehabilitation Following Arthroscopic Rotator Cuff Repair Jonathan B. Ticker, MD Long Island Shoulder Clinic Island Orthopaedics & Sports Medicine, PC Massapequa,
Post-op ARCR - Ticker/Egan 1 Post-operative Rehabilitation Following Arthroscopic Rotator Cuff Repair Jonathan B. Ticker, MD Long Island Shoulder Clinic Island Orthopaedics & Sports Medicine, PC Massapequa,
Reverse Shoulder Replacement
 Reverse Shoulder Replacement An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Reverse Shoulder Replacement An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Muscle Energy Technique. Applied to the Shoulder
 Muscle Energy Technique Applied to the Shoulder MUSCLE ENERGY Theory Muscle energy technique is a manual therapy procedure which involves the voluntary contraction of a muscle in a precisely controlled
Muscle Energy Technique Applied to the Shoulder MUSCLE ENERGY Theory Muscle energy technique is a manual therapy procedure which involves the voluntary contraction of a muscle in a precisely controlled
ROTATOR CUFF TEARS LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
SLAP repair. An information guide for patients. Delivering the best in care. UHB is a no smoking Trust
 SLAP repair An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
SLAP repair An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Arthroscopic Labrum Repair of the Shoulder (SLAP)
 Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Ms. Ruth Delaney ROTATOR CUFF DISEASE Orthopaedic Surgeon, Shoulder Specialist
 WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
SHOULDER INSTABILITY. E. Edward Khalfayan, MD
 SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER - TORN ROTATOR CUFF
 175 Cambridge Street, 4 th floor ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade
175 Cambridge Street, 4 th floor ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade
Dr. Benjamin Hewitt. Subacramial Decompression & Rotator Cuff Repair
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Subacramial Decompression & Rotator Cuff Repair The Rotator Cuff consists of four
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Subacramial Decompression & Rotator Cuff Repair The Rotator Cuff consists of four
Biceps Tenodesis. An information guide for patients. Delivering the best in care. UHB is a no smoking Trust
 Biceps Tenodesis An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Biceps Tenodesis An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
POSTERIOR LABRAL (BANKART) REPAIRS
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
MOON SHOULDER GROUP. Rotator Cuff Home Exercise Program. MOON Shoulder Group
 MOON Shoulder Group For information regarding the MOON Shoulder Group, talk to your doctor or contact: Rosemary Sanders 1215 21 st Avenue South 6100 Medical Center East Vanderbilt University Medical Center
MOON Shoulder Group For information regarding the MOON Shoulder Group, talk to your doctor or contact: Rosemary Sanders 1215 21 st Avenue South 6100 Medical Center East Vanderbilt University Medical Center
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Elbow Arthroplasty
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Indications... 3 7.2 Types of
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Indications... 3 7.2 Types of
Rotator Cuff Home Exercise Program MOON SHOULDER GROUP
 Rotator Cuff Home Exercise Program MOON SHOULDER GROUP Introduction The MOON Shoulder group is a Multi-center Orthopaedic Outcomes Network. In other words, it is a group of doctors from around the country
Rotator Cuff Home Exercise Program MOON SHOULDER GROUP Introduction The MOON Shoulder group is a Multi-center Orthopaedic Outcomes Network. In other words, it is a group of doctors from around the country
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
UHealth Sports Medicine
 UHealth Sports Medicine REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames
UHealth Sports Medicine REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames
GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL INTRODUCTION The ulnar collateral ligament reconstruction is a tendon transfer procedure. No muscles are transected during
GALLAND/KIRBY UCL RECONSTRUCTION (TOMMY JOHN) POST-SURGICAL REHABILITATION PROTOCOL INTRODUCTION The ulnar collateral ligament reconstruction is a tendon transfer procedure. No muscles are transected during
Cervical Fusion Protocol
 REHABILITATION DEPARTMENT Cervical Fusion Protocol The following protocol for physical therapy rehabilitation was designed based on the typical patient seen at the Texas Back Institute for the procedure
REHABILITATION DEPARTMENT Cervical Fusion Protocol The following protocol for physical therapy rehabilitation was designed based on the typical patient seen at the Texas Back Institute for the procedure
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Rotator Cuff and Shoulder Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES
 OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior
 Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior glenohumeral instability and glenoid labral tear. Background:
Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior glenohumeral instability and glenoid labral tear. Background:
Strength Training for the Shoulder
 Strength Training for the Shoulder This handout is a guide to help you safely build strength and establish an effective weighttraining program for the shoulder. Starting Your Weight Training Program Start
Strength Training for the Shoulder This handout is a guide to help you safely build strength and establish an effective weighttraining program for the shoulder. Starting Your Weight Training Program Start
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
ACL plastik, erfarenheter av. tidig kirurgisk behandling. tidig kirurgisk behandling 6/12/2013
 in sports Per Renström, MD, PhD Professor emeritus,,, Sweden Member ATP and ITF Sports Science and Medical Committees Physician Swedish Football Association Presentation at the IOC Advanced team physician
in sports Per Renström, MD, PhD Professor emeritus,,, Sweden Member ATP and ITF Sports Science and Medical Committees Physician Swedish Football Association Presentation at the IOC Advanced team physician
Rehabilitation Guidelines for Biceps Tenodesis
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Biceps Tenodesis The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms a flat, shallow surface.
UW Health Sports Rehabilitation Rehabilitation Guidelines for Biceps Tenodesis The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms a flat, shallow surface.
ROTATOR CUFF HOME EXERCISE PROGRAM
 ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
Shoulder Tendonitis. Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696
 Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
Biceps Brachii Tendon Proximal Rupture
 1 Biceps Brachii Tendon Proximal Rupture Surgical Indications and Considerations Anatomical Considerations: Biceps brachii, one of the dominant muscles of the arm, is involved in functional activities
1 Biceps Brachii Tendon Proximal Rupture Surgical Indications and Considerations Anatomical Considerations: Biceps brachii, one of the dominant muscles of the arm, is involved in functional activities
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
Shoulder stabilisation surgery. Information for patients Orthopaedics
 Shoulder stabilisation surgery Information for patients Orthopaedics page 2 of 20 Introduction The upper limb unit team wants you and your family to understand as much as possible about the operation you
Shoulder stabilisation surgery Information for patients Orthopaedics page 2 of 20 Introduction The upper limb unit team wants you and your family to understand as much as possible about the operation you
SHOULDER - TORN ROTATOR CUFF
 ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The capsule is a broad
ANATOMY AND FUNCTION SHOULDER - TORN ROTATOR CUFF The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The capsule is a broad
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T
 THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
Rotator Cuff Repair and Rehabilitation
 1 Rotator Cuff Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The rotator cuff complex is comprised of four tendons from four muscles: supraspinatus, infraspinatus,
1 Rotator Cuff Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The rotator cuff complex is comprised of four tendons from four muscles: supraspinatus, infraspinatus,
Mini Medical School _ Focus on Orthopaedics
 from The Cleveland Clinic Mini Medical School _ Focus on Orthopaedics Arthritis of the Shoulder: Treatment Options Joseph P. Iannotti MD, PhD Professor and Chairman, Department of Orthopaedic Surgery The
from The Cleveland Clinic Mini Medical School _ Focus on Orthopaedics Arthritis of the Shoulder: Treatment Options Joseph P. Iannotti MD, PhD Professor and Chairman, Department of Orthopaedic Surgery The
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
The Shoulder Complex & Shoulder Girdle
 The Shoulder Complex & Shoulder Girdle The shoulder complex 4 articulations involving The sternum The clavicle The ribs The scapula and The humerus Bony Landmarks provide attachment points for muscles
The Shoulder Complex & Shoulder Girdle The shoulder complex 4 articulations involving The sternum The clavicle The ribs The scapula and The humerus Bony Landmarks provide attachment points for muscles
Clavicle Fracture (Broken Collarbone)
 617-726-7500 www2.massgeneral.org/sports Clavicle Fracture (Broken Collarbone) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages.
617-726-7500 www2.massgeneral.org/sports Clavicle Fracture (Broken Collarbone) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages.
Arthroscopic Labral Repair (SLAP)
 Arthroscopic Labral Repair (SLAP) Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Anatomy The shoulder joint involves three bones: the scapula
Arthroscopic Labral Repair (SLAP) Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Anatomy The shoulder joint involves three bones: the scapula
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
