Survival rates for victims of traumatic cardiac arrest range
|
|
|
- Meagan Lester
- 10 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE The heart of the matter: Utility of ultrasound of cardiac activity during traumatic arrest Elizabeth L. Cureton, MD, Louise Y. Yeung, MD, Rita O. Kwan, MD, MPH, Emily J. Miraflor, MD, Javid Sadjadi, MD, FACS, Daniel D. Price, MD, and Gregory P. Victorino, MD, FACS, Oakland, California BACKGROUND: METHODS: RESULTS: CONCLUSION: LEVEL OF EVIDENCE: KEY WORDS: The clinical utility of determining cardiac motion on ultrasound has been reported for patients presenting in pulseless medical cardiac arrest. However, the relationship between ultrasound-documented cardiac activity and the probability of surviving pulseless electrical activity has not been examined in populations with trauma. We hypothesized that cardiac activity on ultrasound predicts survival for patients presenting in pulseless traumatic arrest. We conducted a retrospective analysis at our university-based urban trauma center of adult patients with trauma, who were pulseless on hospital arrival. Results of cardiac ultrasound performed during trauma resuscitations were compared with the electrocardiogram (EKG) rhythm and survival. Among 318 pulseless patients with trauma, 162 had both EKG tracings and a cardiac ultrasound, and 4.3% of these 162 patients survived to hospital admission. Survival was higher for those with cardiac motion than for those without it (23.5% vs. 1.9% for patients with EKG electrical activity, p = 0.002, and 66.7% vs. 0% for patients without EKG electrical activity, p G 0.001). The sensitivity of ultrasound cardiac motion to predict survival to hospital admission was 86% (specificity, 91%; positive predictive value, 30%; negative predictive value, 99%). When examined by mechanism, sensitivity was 100% for the 111 patients with penetrating trauma and 75% for the 50 patients with blunt trauma. Survival in pulseless traumatic arrest is very low, but survival for patients with no cardiac motion on ultrasound is also exceedingly rare. Cardiac ultrasound had a negative predictive value approaching 100% for survival to hospital admission. For patients with prolonged prehospital cardiopulmonary resuscitation, ultrasound evaluation of cardiac motion in pulseless patients with trauma may be a rapid way to help determine which patients have no chance of survival in the setting of lethal injuries, so that futile resuscitations can be stopped. (. 2012;73: 102Y110. Copyright * 2012 by Lippincott Williams & Wilkins) Diagnostic study, level III. Ultrasound; trauma; cardiac; FAST; pulseless. Survival rates for victims of traumatic cardiac arrest range from 0% to 3.7%. 1 Current guidelines exist for resuscitation of patients with blunt trauma and patients with penetrating trauma in cardiac arrest. According to the National Association of EMS Physicians and the American College of Surgeons joint position statement, patients with blunt trauma and cardiac arrest at the scene, and patients with penetrating trauma who have no signs of life at the scene, (i.e., pulseless, apneic, and without pupillary reflexes, spontaneous movement or organized electrocardiogram [EKG] activity) should not be resuscitated. 2 However, the decision to stop futile resuscitations for patients with lethal injuries can be difficult considering the complexity of the situation and the desire to save a life. Patients in traumatic arrest are evaluated by prehospital cardiopulmonary resuscitation (CPR) duration, an absent pulse Submitted: October 28, 2011; Revised: January 11, 2012; Accepted: January 19, From the Department of Surgery (E.L.C., L.Y.Y., R.O.K., E.J.M., J.S., G.P.V.), University of California, San Francisco-East Bay; and Department of Emergency Medicine (D.D.P.), Alameda County Medical Center, Oakland, California. This study was performed at the University of California, San Francisco-East Bay, Alameda County Medical Center, Oakland, California. Address for reprints: Gregory P. Victorino, MD, FACS, Department of Surgery, University of California, San Francisco-East Bay, 1411 East 31st St, Oakland, CA 94602; [email protected]. DOI: /TA.0b013e ebc 102 on physical examination, and EKG rhythm morphology. Cardiac ultrasound is increasingly being used and can rapidly assess cardiac motion. In pulseless patients with trauma whose prehospital CPR times are prolonged, ultrasound evaluation of cardiac motion may provide essential information to guide resuscitations when injuries are lethal. Previous studies in pulseless patients in medical cardiac arrest indicate that survival to hospital admission was 67% and survival to hospital discharge was 3% when cardiac activity was demonstrated by ultrasound. 3 For patients whose medical cardiac arrest occurs out of the hospital and who present to the emergency department (ED), ultrasound activity has been proposed to distinguish between patients with electromechanical dissociation (EMD), and those with pseudo-emd, where the cause of pulseless electrical activity (PEA) is potentially reversible. 4 The American Heart Association describes echocardiography as being potentially useful for patients in PEA cardiac arrest (in-house or in the ED); cardiac contractions could be a possible indication for continued CPR. 5 According to a small study of cardiac ultrasound performed by medical house officers on patients having in-house medical PEA arrest, the house officers readings largely agreed with the cardiologists in ascertaining when patients had a normal study or had no cardiac motion. 6 One group has proposed that ultrasound be a part of an algorithm ( Cardiac Arrest Ultrasound Exam [C.A.U.S.E.] ) for the resuscitation of patients in primary nonarrhythmogenic
2 Cureton et al. cardiac arrest. 7 The same group emphasizes the use of ultrasound to identify potential causes of cardiac arrest, including cardiac tamponade, hypovolemia, and pulmonary embolism. Taken together, these studies support the use of ultrasound as a fast, noninvasive, and accurate way to decide whether continuing resuscitation of a patient in medical arrest is futile or helpful. The clinical utility of determining cardiac motion on ultrasound has been suggested for patients in medical pulseless arrest. 3Y7 However, the relationship between cardiac activity documented by ultrasound and the probability of surviving PEA has not yet been examined for patients presenting in pulseless traumatic arrest, in which causes of PEA may be treatable. We hypothesized that cardiac activity on ultrasound predicts survival for patients presenting in pulseless traumatic arrest. PATIENTS AND METHODS Institutional review board approval was obtained for this retrospective study. We analyzed our institutional trauma database and ED records of all trauma patients, presenting without a pulse at our university-based urban trauma center from January 2002 to September 2008, who were older than 18 years. The results of cardiac ultrasound performed during the trauma resuscitation were compared with EKG rhythm and survival. The sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) were calculated to ascertain whether cardiac motion on ultrasound predicted whether a patient survived long enough to be admitted from the trauma bay to the hospital. Downtime and code duration were compared among subgroups of patients. Downtime was defined as the time interval in minutes between loss of pulse (or arrival of the emergency medical services [EMS]on scene if patient had no pulse when EMS arrived) and arrival in the trauma bay, all as recorded on the EMS prehospital records document. When the runsheet was unavailable, an estimated time was used if the downtime was reported verbally to a hospital staff and recorded in the medical record. Code duration was defined as the time interval in the ED in minutes between arrival in the trauma bay and the end of the code, that is, the time of death or, in the case of survivors, the documented time when a pulse returned. Survival was either defined as leaving the ED alive (i.e., survival to hospital admission) or survival to hospital discharge. Focused assessment with sonography for trauma (FAST) isreadilyavailableatourinstitutionintheedandmaybe immediately performed at the request of the trauma team, trauma surgical attending staff, or emergency medicine attending staff. FAST is performed by a surgeon or emergency medicine physician member of the trauma team who has received ultrasound training under the direct supervision of a FAST credentialed emergency medicine attending or trauma surgeon. Because cardiac ultrasound is not a routine part of our institutional trauma resuscitation workup and FAST is done at the discretion of the trauma team and attending surgeons, not all patients received an ultrasound. For example, patients who arrived at our institution clearly deceased or those who had an obvious case of pulselessness that was immediately corrected, may not have undergone a cardiac ultrasound. As a general guideline for the use of ED resuscitative thoracotomy, at our institution, we refer to the series from Denver. 8 Typically patients will undergo resuscitative thoracotomy if the prehospital duration of CPR is less than 15 minutes for penetrating trauma and less than 5 minutes for blunt trauma. Cardiac ultrasound was typically used for patients with prehospital CPR times that were longer than these time periods. All examinations were performed using a SonoSite MicroMaxx ultrasound scanner (SonoSite, Bothell, WA) with images recorded in DICOM format. Subxiphoid views were obtained using a 5-MHz curvilinear probe. In instances where there was obviously no cardiac movement, one view of the heart was obtained. If there was any question of movement or if the cardiac ultrasound was being conducted as part of a FAST examination, two views of the heart were obtained to evaluate for pericardial fluid. All ultrasound images are routinely reviewed by the fellowship-trained emergency medicine ultrasound director. Cardiac activity was defined as presence of any organized, nonfibrillating motion. Data were analyzed statistically using Fisher s exact tests, W 2 tests, or t tests as appropriate. RESULTS Overall Patient Characteristics and Survival Outcome A flowchart depicting a total of all 318 patients with trauma who are presenting without pulses (Fig. 1) shows that, of the 135 patients with electrical activity on electrocardiography, 71 had an ultrasound completed, 17 of whom had cardiac motion. Of these 17 patients, 4 survived to hospital admission. Of the 54 patients with electrical activity on electrocardiography but no cardiac motion on ultrasound, only 1 survived to hospital admission. Of the 64 patients with electrical activity but no ultrasound performed, 4 (6%) survived to hospital admission after the operation, one of whom also survived to hospital discharge and was seen for follow-up visits in our clinic. This patient had a brachial artery injury from a cut by glass and arrived in PEA. Because of the obvious source of bleeding and recent loss of pulse, the patient was resuscitated, was transfused, immediately underwent successful arterial repair, and subsequently had a functionally normal outcome. To calculate the clinical utility of cardiac ultrasound in pulseless patients with trauma, only patients who received an ultrasound were included in the analysis. Figure 2 shows the 162 pulseless patients with trauma who received both electrocardiography and a cardiac ultrasound. Of these, 71 patients had electrical activity, and 91 did not. Of the 71 patients who had electrical activity on electrocardiography, 17 patients also had cardiac motion on ultrasound, whereas54hadnocardiac motion. Of the 91 patients who had no electrical activity on electrocardiography, 3 patients had cardiac motion on ultrasound, and 88 had no cardiac motion. Among all of the 162 pulseless patients with trauma who received both EKG tracing and cardiac ultrasound, 4.3% survived to hospital admission (23.5% of those with electrical activity and cardiac motion vs. 1.9% with electrical activity but no cardiac motion * 2012 Lippincott Williams & Wilkins 103
3 Cureton et al. Figure 1. The 318 patients with pulseless traumatic arrest were categorized according to presence or absence of electrical activity and whether ultrasound was performed and showed cardiac motion. Survival was defined as survival to hospital admission. [p = 0.002] and 66.7% of those with no electrical activity but with cardiac motion vs. 0% with neither electrical activity nor cardiac motion [p G 0.001]; Table 1). The sensitivity of ultrasound cardiac motion to predict survival to hospital admission was 86%, with a specificity of 91%, PPV of 30%, and NPV of 99%. All survivors had either electrical activity, or cardiac motion, or both; while 100% of patients without cardiac motion and electrical activity died. Survival in Patients With Penetrating Trauma A flowchart depicting the 111 patients with penetrating trauma who received both EKG tracing and cardiac ultrasound Figure 2. There were 162 patients with pulseless arrest who underwent both electrocardiography and ultrasound. These patients were categorized according to presence or absence of electrical activity and whether ultrasound showed cardiac motion. Survival was defined as survival to hospital admission. 104 * 2012 Lippincott Williams & Wilkins
4 Cureton et al. TABLE 1. Patient Characteristics, Resource Use, and Survival to Hospital Admission for All Patients Who Underwent Electrocardiography and US All Patients With Trauma Who Underwent Electrocardiography and US With EKG Electrical Activity Without EKG Electrical Activity With US Cardiac Without US Cardiac With US Cardiac Without US Cardiac Motion Motion p Motion Motion p n Downtime, mean 15.8 (0.8) 13.1 (2.6) 14.6 (1.2) (1.0) Code duration mean 6.0 (0.4) 13.1 (2.6) 6.7 (0.7) (0) 4.1 (0.3) 0.2 Underwent EDT, 8 (5) 3 (18) 4 (7) (1) 0.9 Transfused, 14 (9) 6 (35) 4 (7) (33) 1 (1) G0.001 Underwent operation, 3 (2) 3 (18) 0 (0) (0) 0 (0) NA 7 (4) 4 (24) 1 (2) (67) 0 (0) G0.001 Survived to hospital admission, Downtime is the time between loss of pulse and arrival in the trauma bay per emergency medical providers records. Code duration is the time between arrival and time of end of code (i.e., time of death if patient died). p values are for the comparisons between patients with US cardiac motion versus no US cardiac motion. NA, not applicable; US, ultrasound. (Fig. 3) shows that 45 patients had electrical activity on electrocardiography, with 14 patients showing cardiac motion. Of these 14 patients, 3 survived to hospital admission. Of the 66 patients who had no electrical activity on electrocardiography and an ultrasound completed, only 1 patient showed cardiac motion; this patient did not survive. The sensitivity of ultrasound cardiac motion to predict survival to hospital admission in pulseless patients with penetrating trauma was 100%, with a specificity of 89%, PPV of 20%, and NPV of 100%. Survival in Patients With Blunt Trauma A flowchart depicting the 50 patients with blunt trauma who received both EKG tracing and cardiac ultrasound (Fig. 4) shows that 26 patients (52%) had electrical activity on electrocardiography, with 3 patients having cardiac motion. One of these patients survived to hospital admission. Interestingly, of the 23 patients with electrical activity but no cardiac motion, 1 survived to hospital admission, and the remaining 22 died. Of the 24 patients who had no electrical activity on electrocardiography and an ultrasound completed, 2 patients showed cardiac motion and survived. The remaining 22 patients who had neither electrical activity nor cardiac motion did not survive. The sensitivity of ultrasound cardiac motion to predict survival to hospital admission in pulseless patients with blunt trauma was 75%, with a specificity of 96%, PPVof 60%, and NPV of 98%. One patient in the database had missing Figure 3. There were 111 patients with pulseless arrest from penetrating trauma who had both electrocardiography and ultrasound performed. They were categorized according to presence or absence of electrical activity, and whether ultrasound showed cardiac motion. Survival was defined as survival to hospital admission. * 2012 Lippincott Williams & Wilkins 105
5 Cureton et al. Figure 4. There were 50 patients with pulseless arrest from blunt trauma who underwent both electrocardiography and ultrasound. They were categorized according to presence or absence of electrical activity and whether ultrasound showed cardiac motion. Survival was defined as survival to hospital admission. information on the mechanism of injury and thus was omitted from analysis. Downtime, Code Duration, and Resource Use Table 1 shows that, for all pulseless patients with both EKG tracings and cardiac ultrasound, resource use was generally higher in those patients who exhibited cardiac motion. Mean code duration was longer for patients with both EKG activity and cardiac motion on ultrasound compared to those with only EKG activity and no cardiac motion (mean [SEM], 13.1 [2.6] minutes vs. 6.7 [0.7] minutes; p = 0.003). Although approximately equal numbers of patients underwent ED thoracotomy (EDT) regardless of cardiac motion, more patients with cardiac motion on ultrasound received blood transfusions (six patients vs. four patients, p = 0.004), underwent operation (three patients vs. no patient, p = 0.002) and ultimately survived to hospital admission (six patients vs. one patient, p = 0.002). EDT was performed in 5% (8 of 162) patients who received both EKG tracings and a cardiac ultrasound. This represented 15% (8 of 55) of the total number of EDT s done for all trauma activations at our institution during the study period. Fifty-three percent (29 of 55) of EDTs were done on patients who did not have either EKG tracings or ultrasounds TABLE 2. Patient Characteristics, Resource Use, and Survival to Hospital Admission for Patients With Penetrating Trauma Who Underwent Electrocardiography and US Patients With Penetrating Trauma With EKG and US With EKG Electrical Activity Without EKG Electrical Activity With US Cardiac Without US Cardiac With US Cardiac Without US Cardiac Motion Motion p Motion Motion p n Downtime, mean 16.7 (0.9) 9.7 (2.6) 15.0 (1.5) (1.2) NA Code duration mean 5.7 (0.5) 12.8 (2.8) 6.5 (0.9) (0) 4.0 (0.3) NA Underwent EDT, 8 (7) 3 (21) 4 (13) (2) 0.9 Transfused, 10 (9) 6 (43) 3 (10) (0) 1 (2) 0.9 Underwent operation, 3 (3) 3 (21) 0 (0) (0) 0 (0) NA 3 (3) 3 (21) 0 (0) (0) 0 (0) NA Survived to hospital admission, Downtime is the time between loss of pulse and arrival in the trauma bay per emergency medical providers records. Code duration is the time between arrival and time of end of code (i.e., time of death if patient died). p values are for the comparisons between patients with US cardiac motion versus no US cardiac motion. 106 * 2012 Lippincott Williams & Wilkins
6 Cureton et al. TABLE 3. Patient Characteristics, Resource Use, and Survival to Hospital Admission for Patients With Blunt Trauma Who Underwent Electrocardiography and US Patients With Blunt Trauma Who Underwent Electrocardiography and US With EKG Electrical Activity Without EKG Electrical Activity With US Cardiac Without US Cardiac With US Cardiac Without US Cardiac Motion Motion p Motion Motion p n Downtime, mean 16.3 (1.5) 25 (3.5) 14.2 (2.0) (2.0) 0.01 Code duration mean 6.2 (0.8) 14.5 (10.4) 7.1 (1.1) 0.1 Unknown 4.4 (0.9) NA Underwent EDT, 0 (0) 0 (0) 0 (0) NA 0 (0) 0 (0) NA Transfused, 3 (6) 1 (33) 1 (4) (50) 0 (0) G0.001 Underwent operation, 0 (0) 0 (0) 0 (0) NA 0 (0) 0 (0) NA 4 (8) 1 (33) 1 (4) (100) 0 (0) G0.001 Survived to hospital admission, Downtime is the time between loss of pulse and arrival in the trauma bay per emergency medical providers records. Code duration is the time between arrival and time of end of code (i.e., time of death if patient died). p values are for the comparisons between patients with US cardiac motion versus no US cardiac motion. obtained and, so these patients were not included in the analysis. Of the remaining 26 patients, 18 patients had only EKG tracings monitored and did not receive a cardiac ultrasound before undergoing EDT. The mean downtime in our study for patients undergoing EDT was 11 minutes, whereas the overall mean downtime for all patients in the study was 16 minutes. However, among those who underwent EDT and survived, the mean downtime was 2 minutes. Subgroup analysis of patients with only penetrating injuries (Table 2) continued to show that, for patients with EKG activity, those who also exhibited cardiac motion had a longer mean code duration (mean [SEM], 12.8 [2.8] minutes vs. 6.5 [0.9] minutes, p = 0.01), were more likely to receive blood transfusions (six patients vs. three patients, p =0.01), were more likely to undergo operation (three patients vs. no patient, p = 0.008), and were more likely to survive to hospital admission (three patients vs. no patient, p =0.008).Those patients with blunt injuries still had poor outcomes overall, but those found to still have cardiac motion on ultrasound were more likely to receive blood transfusions and survive to hospital admission (Table 3). To see if isolated patient injuries may impact outcomes, we analyzed the patients who sustained isolated head injuries separately. None of these patients received an EDT. Only 21% of these patients survived to hospital admission, and unfortunately none survived to hospital discharge. TABLE 4. All Pulseless Patients With Trauma Who Underwent Both Electrocardiography and Cardiac US and Survived to Hospital Admission Mechanism Downtime, min Electrical Activity at Admission Cardiac Motion on US Clinical Course GSW to abdomen 4 Yes (PEA, rate 112) Yes Return of pulse after EDT; aortic, IVC, colon, and liver injuries repaired; died in ICU 4 h 4 min after arrival GSW to abdomen 3 Yes (PEA, rate 52) Yes EDT, then to OR. Aortic, IVC, liver, spleen injuries repaired; died in OR 1 h 2 min after arrival GSW to chest 4 Yes (PEA, bradycardia) Yes EDT; subclavian artery injury repaired in OR; died in OR 52 min after arrival Bicycle accident 0 (lost pulse on arrival) Yes (PEA, rate 30) No motion Found asystolic in field; then sinus rhythm en route. Pulse returned 1 min after US completed. Anoxic brain injury; C2 fracture, cervical spinal cord disruption. Died in ICU 2 d after arrival No Yes Asystole then ventricular tachycardia; pulse returned; lived for 52 min in ICU. Pelvic fracture, IVC tear. Crush injury/fall 0 (lost pulse on arrival) Blunt head injury Unknown No Yes Found asystolic outside hospital. Pulse returned 6 min after arrival, anoxic brain injury, lived 2 d in ICU; qualified to be organ donor Blunt head injury 10 Yes (PEA, rate 84) Yes Initially ventricular fibrillation, then asystolic in field. Lived 32 h in ICU; organ donor GSW, gunshot wound; ICU, intensive care unit; IVC, inferior vena cava; OR, operating room. * 2012 Lippincott Williams & Wilkins 107
7 Cureton et al. Table 4 lists the mechanism, downtime, electrical activity, and cardiac motion at admission, and clinical course of all pulseless patients with both electrocardiography and cardiac ultrasound who survived to hospital admission. DISCUSSION Cardiac ultrasound is used as an extension of the FAST examination to evaluate patients with trauma in extremis. It has a 100% sensitivity, 97% specificity, and 97% accuracy for identifying hemopericardium after penetrating injury to the trunk. 9 Cardiac ultrasound has been used in many studies of patients with medical cardiac arrest, 3,4,6,7,10,11 and is increasingly being used in our center and elsewhere to examine pulseless trauma patients for the presence of cardiac motion. However, the significance of what this cardiac motion means in pulseless patients with trauma remains unknown. In our retrospective study of more than 300 patients (the largest to date), we found that absence of cardiac motion in pulseless patients with trauma predicted death with NPV of 99%. Although we found that cardiac ultrasound has a high negative predicative value, it is still critically important to maintain management priorities when treating pulseless patients with trauma. ED resuscitative thoracotomy has been recommended in patients with trauma who are pulseless on hospital arrival and have a prehospital CPR time of less than 5 minutes in blunt trauma or less than 15 minutes in penetrating trauma. 8 These are the guidelines that we use at our institution. New guidelines from the Western Trauma Association recommend expanding the indications for resuscitative thoracotomy in patients with blunt trauma with a prehospital CPR time of less than 10 minutes. 12 Itisessentialtoadheretothese potentially life-saving guidelines instead of obtaining a cardiac ultrasound. As such, of the 55 ED resuscitative thoracotomies that were performed during the study period, only 8 had ultrasound assessment of cardiac motion before initiation of the thoracotomy. This means that 85% (47 of 55) of ED resuscitative thoracotomies were completed without cardiac ultrasound and speaks to the importance of moving immediately to the resuscitative thoracotomy without spending time on ultrasound assessment. Considering that the absence of cardiac motion on ultrasound in pulseless patients with trauma predicted death with an NPV of 99%, the increased utility of cardiac ultrasound may be in those patients who fall outside the guidelines for ED resuscitative thoracotomy. Therefore, we use cardiac ultrasound for pulseless patients with trauma with longer prehospital CPR times, to help confirm death, with the goal of preventing prolonged and unnecessary resuscitative efforts. Because trauma teams are programmed to do everything possible to save lives, it is often emotionally difficult to declare the patient dead and stop the resuscitation. Prolonged resuscitation efforts often result in the unnecessary use of resources. Cardiac ultrasound may be used during these circumstances to provide additional evidence that the patient is dead, to convince the trauma team that nothing else can be done, and thereby confirming that it is reasonable to stop the resuscitation. 108 Our overall rate of survival to hospital discharge was 0.003%, which is on the lower range of previously published reports on pulseless patients with trauma, which cite hospital discharge rates of 0% to 2.6% for pulseless patients with trauma. 13Y16 This may be caused by patient selection because our study included patients with longer prehospital CPR times. In one study of patients arriving in the ED in cardiac arrest that was not specified as medical or surgical, 27% of those with cardiac motion on ultrasound versus 3% of those with no motion survived to hospital admission. 11 Another study of pulseless medical patients arriving in the ED in cardiac arrest had a 100% PPV for death if no cardiac motion was seen on parasternal cardiac ultrasound, with a 58% NPV for death if cardiac motion was present. 3 In a study that examined cardiac ultrasound in 28 patients with trauma who either presented in PEA on arrival or developed PEA after arrival, 12 patients had organized cardiac motion on ultrasound. 15 Three of those patients survived to hospital admission; all three had organized motion on ultrasound, and two had narrow complex rhythms. The presence of cardiac activity was not a statistically significant predictor of survival; the absence of cardiac activity was 69% sensitive and 100% specific for lack of return of pulse, and the negative likelihood ratio was 0.3 for not regaining a pulse without activity on ultrasound. The inability of cardiac motion on ultrasound to predict survival may be caused by a lack of power in this small study. This study also differed from ours in that we focused only on patients who arrived without a pulse, often with unknown downtime, and for whom the presence of any type of cardiac motion raises questions of possible viability. The differences in downtime between patients with cardiac motion versus those without it, or between patients with electrical activity and those without it, could imply that these subgroups of patients are merely at different points along a common continuum of decline. Prolonged downtime itself is a predictor of death, 17 and asystole as the initial rhythm portends extremely poor prognosis in patients with traumatic arrest, whereas 2% to 6% of patients who survive traumatic arrest arrived at the hospital in some other rhythm (e.g., PEA and ventricular fibrillation) 13,17 or with a heart rate of more than 40 beats per minute. 13 Although it may be argued that patients who were found pulseless by EMS have an unknown accurate downtime, EMS records are the earliest consistent recorded time available. Special consideration should be given to patients in whom pericardial tamponade is suspected because the pericardial fluid may affect the interpretation of the cardiac ultrasound. Although studies of echocardiography in medical patients with pericardial effusion and clinical tamponade generally show that wall and valve motion occur despite the sonographic signs of tamponade, 18 there is variability in cardiac motion that can range from limited heart-wall movement to increased cardiac motion. 19 In such cases, treatment of the cardiac tamponade should be completed first before any attempts to categorize the patient as having lack of cardiac motion are undertaken. Despite our best efforts to maintain consistency and objectivity with training and supervision by an ultrasound certified attending physician, one difficulty in our study was * 2012 Lippincott Williams & Wilkins
8 Cureton et al. standardizing how cardiac motion was quantified. None of the pulseless patients who had cardiac motion on ultrasound had brisk cardiac contractions. Possibly, the same degree of very minimal motion could be described as no motion by one clinician, and positive motion or a twitch of motion by another. Moreover, this subjective description of motion could be described as positive or negative according to whether the clinician thought the motion had an appearance associated with survivability, thereby potentially influencing whether a code was continued. In addition, although it has been our practice to use cardiac ultrasound to help confirm death during prolonged downtimes, owing to the retrospective nature of the study, it is difficult to prove that the EKG and FAST findings altered clinical management. The subjective categorization among patients with and without cardiac activity may also be an imprecise view of what is actually occurring in the heart electrically. For example, there is likely to be a continuum of patients considered to have a barely perceptible electrical signal, which some clinicians may call asystole. A lack of agreement may exist regarding the term agonal, and even the terms pulseless electrical activity or electromechanical dissociation.peacan be defined as the presence of organized electrical activity but no pulse. 20 In a previous study, cardiac ultrasound motion has been documented in 86% of patients in EMD who have electrical activity but no pulse. 21 EMD is conventionally thought of as organized electrical activity in the absence of simultaneous muscular activity, and it can be distinguished from pseudo-emd where there is contractile activity, but not enough of it to generate a pulse. 22 The American Heart Association refers to PEA as including multiple types of rhythms, including pseudo-emd, idioventricular rhythms, and others, which demonstrate mechanical contractions too weak to generate a pulse. 23 Patients who are brain dead after devastating traumatic injuries have the potential to be organ donors, and cardiac ultrasound may help identify those who have physiologic potential for survival under intensive care until organ donation is possible. In our study, of the 11 survivors, 2 became organ donors and another qualified for organ donation, but the family declined. All three patients had head injuries. Although the potential for organ donation exists for patients who survive to hospital admission, most die quickly, and in our study, all but one patient who survived to hospital admission died in the hospital. That only one patient survived to hospital discharge reinforces how lethal the condition of these patients is and how important it is to limit futile resuscitations. In a resource-limited environment where maximum efficiency is required, we should strive to save our resources to ensure they are available to be used for patients who will benefit from them as well as limit futile procedures that may worsen patient conditions or present unnecessary risks to health care staff. In a busy trauma center or ED, there are often multiple codes or trauma activations that can occur simultaneously. Knowing which patients can benefit from our efforts assists us in managing finite numbers of staff and limited resources at any one time. The data collected in our study allows us to propose an algorithm that could be applied to patients in pulseless traumatic arrest who have more than 15 minutes of prehospital CPR for penetrating trauma and more than 5 minutes for blunt trauma. These patients should have an initial evaluation of their cardiac function by electrical rhythm and cardiac ultrasound. Those found to be asystolic with no motion on cardiac ultrasound should be declared dead. Those with a rhythm other than asystole and with no motion on cardiac ultrasound should be declared dead because lack of cardiac motion is highly predictive of death. Continued resuscitation of patients with cardiac motion on ultrasound can be justified, acknowledging the small rate of survival to hospital admission and the even smaller rate of survival to hospital discharge. However, the finding of no cardiac motion, especially for patients without electrical activity, can reliably predict death. CONCLUSIONS The rate of ultimate survival for patients in pulseless traumatic arrest is quite low, but survival for patients with no cardiac motion on ultrasound is exceedingly rare. Our study showed that the absence of cardiac motion and especially the absence of both cardiac motion and electrical activity were highly predictive of death. Cardiac ultrasound had an NPV approaching 100% for survival to hospital admission. Ultrasound evaluation of cardiac motion in pulseless patients with trauma with prolonged prehospital CPR may be a rapid way to help determine which patients have no chance of survival in the setting of lethal injuries, so that futile resuscitations can be stopped. AUTHORSHIP All authors participated in designing this study. E.L.C. and L.Y.Y. conducted the literature searches. E.L.C., R.O.K., and E.J.M. collected the data, which all authors assisted in interpreting. E.L.C. and L.Y.Y. performed statistical analyses. D.P.P. provided ultrasound interpretation. E.L.C., L.Y.Y., and G.P.V. prepared the manuscript, which R.O.K., E.J.M., D.P.P., and G.P.V. reviewed. G.P.V. provided oversight of the study. DISCLOSURE Dr. Price has been a consultant with SonoSite and Philips and was involved in but not a direct recipient of grant funding by SonoSite and Philips for an unrelated study. For the remaining authors, no conflicts were declared. REFERENCES 1. Lockey D, Crewdson K, Davies G. Traumatic cardiac arrest: who are the survivors? Ann Emerg Med. 2006;48:240Y Hopson LR, Hirsh E, Delgado J, Domeier RM, McSwain NE, Krohmer J. Guidelines for withholding or termination of resuscitation in prehospital traumatic cardiopulmonary arrest: joint position statement of the National Association of EMS Physicians and the American College of Surgeons Committee on Trauma. J Am Coll Surg. 2003;196:106Y Blaivas M, Fox JC. Outcome in cardiac arrest patients found to have cardiac standstill on the bedside emergency department echocardiogram. Acad Emerg Med. 2001;8:616Y Sanders AB, Kern KB, Berg RA. Searching for a predictive rule for terminating cardiopulmonary resuscitation. Acad Emerg Med. 2001;8:654Y Neumar RW, Otto CW, Link MS, Kronick SL, Shuster M, Callaway CW, Kudenchuk PJ, Ornato JP, McNally B, Silvers SM, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010:122:S729YS Niendorff DF, Rassias AJ, Palac R, Beach ML, Costa S, Greenburg M. Rapid cardiac ultrasound of inpatients suffering PEA arrest performed by nonexpert sonographers. Resuscitation. 2005;67:81Y87. * 2012 Lippincott Williams & Wilkins 109
9 Cureton et al. 7. Hernandez C, Shuler K, Hannan H, Sonyika C, Likourezos A, Marshall J. C.A.U.S.E.: cardiac arrest ultra-sound examva better approach to managing patients in primary non-arrythmogenic cardiac arrest. Resuscitation. 2008;76:198Y Powell D, Moore E, Clothren C, Ciesla D, Burch J, Moore J, Johnson J. Is emergency department resuscitative thoracotomy futile care for the critically injured patient requiring prehospital cardiopulmonary resuscitation? JAmCollSurg. 2004;199:211Y Rozycki GS, Feliciano DV, Ochsner MG, Knudson MM, Hoyt DB, Davis F, Hammerman D, Figueredo V, Harviel JD, Han DC, et al. The role of ultrasound in patients with possible penetrating cardiac wounds: a prospective multicenter study. JTrauma.1999;46:543Y551; discussion 551Y Salen P, Melniker L, Choolijian C, Rose J, Alteveer J, Reed J, Heller M. Does the presence or absence of sonographically identified cardiac activity predict resuscitation outcomes of cardiac arrest patients? Am J Emerg Med. 2005;23:459Y Salen P, O Connor R, Sierzenski P, Passarello B, Pancu D, Melanson S, Arcona S, Reed J, Heller M. Can cardiac sonography and capnography be used independently and in combination to predict resuscitation outcomes? Acad Emerg Med. 2001;8:610Y Moore EE, Knudson MM, Burlew CC, Inaba K, Dicker RA, Biffl WL, Malhotra AK, Schreiber MA, Browder TD, Coimbra R, et al. Defining the limits of resuscitative emergency department thoracotomy: a contemporary Western Trauma Association perspective. JTrauma. 2011;70: 334Y Battistella FD, Nugent W, Owings JT, Anderson JT. Field triage of the pulseless trauma patient. Arch Surg. 1999;134:742Y Rosemurgy AS, Norris P, Olson S, Hurst J, Albrink M. Prehospital traumatic cardiac arrest: the cost of futility. J Trauma. 1993;35:468Y Schuster KM, Lofthouse R, Moore C, Lui F, Kaplan LJ, Davis KA. Pulseless electrical activity, focused abdominal sonography for trauma, and cardiac contractile activity as predictors of survival after trauma. J Trauma. 2009;67:1154Y Martin SK, Shatney CH, Sherck JP, Ho CC, Homan SJ, Neff J, Moore EE. Blunt trauma patients with prehospital pulseless electrical activity (PEA): poor ending assured. J Trauma. 2002;53:876Y880; discussion 880Y Fulton R, Voigt W, Hilakos A. Confusion surrounding the treatment of cardiac arrest. J Am Coll Surg. 1995;181:209Y Naggar CZ, Dillon WD, Butterly JR, Malacoff RF. Echocardiographic manifestations of tense pericardial effusion. J Am Coll Cardiol. 1985;6: 467Y Feigenbaum H, Zaky A, Grabhorn LL. Cardiac motion in patients with pericardial effusion. A study using reflected ultrasound. Circulation. 1966;34:611Y Desbiens NA. Simplifying the diagnosis and management of pulseless electrical activity in adults: a qualitative review. Crit Care Med. 2008;36: 391Y Bocka JJ, Overton DT, Hauser A. Electromechanical dissociation in human beings: an echocardiographic evaluation. Ann Emerg Med. 1988; 17:450Y Paradis NA, Martin GB, Goetting MG, Rivers EP, Feingold M, Nowak RM. Aortic pressure during human cardiac arrest. Identification of pseudoelectromechanical dissociation. Chest. 1992;101:123Y ECC Committee, Subcommittees and Task Forces of the American Heart Association American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care: management of cardiac arrest. Circulation. 2005;112:IV58YIV * 2012 Lippincott Williams & Wilkins
CARDIAC MOVEMENT IDENTIFIED ON PREHOSPITAL ECHOCARDIOGRAPHY PREDICTS OUTCOME IN CARDIAC ARREST PATIENTS
 CARDIAC MOVEMENT IDENTIFIED ON PREHOSPITAL ECHOCARDIOGRAPHY PREDICTS OUTCOME IN CARDIAC ARREST PATIENTS Gernot Aichinger, MD, Peter Michael Zechner, MD, Gerhard Prause, MD, Florian Sacherer, Gernot Wildner,
CARDIAC MOVEMENT IDENTIFIED ON PREHOSPITAL ECHOCARDIOGRAPHY PREDICTS OUTCOME IN CARDIAC ARREST PATIENTS Gernot Aichinger, MD, Peter Michael Zechner, MD, Gerhard Prause, MD, Florian Sacherer, Gernot Wildner,
Sonography in Cardiac Arrest
 Sonography in Cardiac Arrest Real-time Assessment and Evaluation with Sonography - Outcomes Network (REASON) Dr. Paul Atkinson MB MA FRCEM Professor and Research Program Director Emergency Medicine Dalhousie
Sonography in Cardiac Arrest Real-time Assessment and Evaluation with Sonography - Outcomes Network (REASON) Dr. Paul Atkinson MB MA FRCEM Professor and Research Program Director Emergency Medicine Dalhousie
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Case III. Disscussion. the UHP ultrasound protocol. Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient
 The UHP Ultrasound Protocol: A Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient JOHN S. ROSE, MD,* AARON E. BAIR, MD,* DIKU MANDAVIA, MD, AND DONNA J. KINSER,
The UHP Ultrasound Protocol: A Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient JOHN S. ROSE, MD,* AARON E. BAIR, MD,* DIKU MANDAVIA, MD, AND DONNA J. KINSER,
STATE OF CONNECTICUT
 STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
CARDIAC ARREST ULTRASOUND
 ADIA AEST ULTASOUND Phillip Andrus, MD, FAEP Department of Emergency Medicine Division of Emergency Ultrasound Mount Sinai School of Medicine Point of are Ultrasound provides important diagnostic, procedural
ADIA AEST ULTASOUND Phillip Andrus, MD, FAEP Department of Emergency Medicine Division of Emergency Ultrasound Mount Sinai School of Medicine Point of are Ultrasound provides important diagnostic, procedural
The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes
 The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes Reporter: Intern 鄭 琬 蓉 Supervisor: Dr. 朱 健 銘 Date: Sep. 16th, 2014 The nonspecific
The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes Reporter: Intern 鄭 琬 蓉 Supervisor: Dr. 朱 健 銘 Date: Sep. 16th, 2014 The nonspecific
Traumatic Cardiac Tamponade. Shane KF Seal 19 November 2003 POS
 Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION. ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements
 TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements 836 IAC 1.5-1 Purpose Affected: [IC 10-14-3-12; IC 16-18; IC 16-21-2; IC 16-31-2-9;
TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements 836 IAC 1.5-1 Purpose Affected: [IC 10-14-3-12; IC 16-18; IC 16-21-2; IC 16-31-2-9;
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010
 Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Outcomes of Rapid Defibrillation by Security Officers after Cardiac Arrest in Casinos
 Outcomes of Rapid Defibrillation by Security Officers after Cardiac Arrest in Casinos Terence D. Valenzuela, M.D., M.P.H., Denise J. Roe, Dr.P.H., Graham Nichol, M.D., M.P.H., Lani L. Clark, B.S., Daniel
Outcomes of Rapid Defibrillation by Security Officers after Cardiac Arrest in Casinos Terence D. Valenzuela, M.D., M.P.H., Denise J. Roe, Dr.P.H., Graham Nichol, M.D., M.P.H., Lani L. Clark, B.S., Daniel
How To Teach An Integrated Ultrasound
 University of South Carolina School of Medicine Integrated Ultrasound Curriculum iusc Richard Hoppmann The Integrated Ultrasound Curriculum Initiated 2006 First (M1) and Second (M2) Year Medical Students
University of South Carolina School of Medicine Integrated Ultrasound Curriculum iusc Richard Hoppmann The Integrated Ultrasound Curriculum Initiated 2006 First (M1) and Second (M2) Year Medical Students
Focused assessment of sonography in trauma
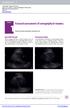 Chapter1 Focused assessment of sonography in trauma Patricia Fermin and John Christian Fox Epicardial fat pad When imaging the heart, careful attention must be made in identifying any surrounding fluid.
Chapter1 Focused assessment of sonography in trauma Patricia Fermin and John Christian Fox Epicardial fat pad When imaging the heart, careful attention must be made in identifying any surrounding fluid.
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
How To Learn To Perform An Ultrasound
 CAE ICCU E-Learning CAE VIMEDIX Ultrasound Simulator Master Ultrasonography of the Thoracic, Abdominal and Pelvic Cavities An Engaging Learning Solution for Ultrasound Hands-on Simulation, Multimedia Content,
CAE ICCU E-Learning CAE VIMEDIX Ultrasound Simulator Master Ultrasonography of the Thoracic, Abdominal and Pelvic Cavities An Engaging Learning Solution for Ultrasound Hands-on Simulation, Multimedia Content,
Dr Anne Weaver London s Air Ambulance CODE RED THE BLEEDING PATIENT
 Dr Anne Weaver London s Air Ambulance CODE RED THE BLEEDING PATIENT Objectives Describe the background to Code Red Describe our Standard Operating Procedure Share our data The bleeding problem Major haemorrhage
Dr Anne Weaver London s Air Ambulance CODE RED THE BLEEDING PATIENT Objectives Describe the background to Code Red Describe our Standard Operating Procedure Share our data The bleeding problem Major haemorrhage
Organ Donation: A Call for Greater Palliative Care Involvement
 Organ Donation: A Call for Greater Palliative Care Involvement Heather A. Harris, M.D. Associate Medical Director, Supportive & Palliative Care Service San Francisco General Hospital & Trauma Center Associate
Organ Donation: A Call for Greater Palliative Care Involvement Heather A. Harris, M.D. Associate Medical Director, Supportive & Palliative Care Service San Francisco General Hospital & Trauma Center Associate
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
EMS POLICIES AND PROCEDURES
 EMS POLICIES AND PROCEDURES POLICY #: 13 EFFECT DATE: xx/xx/05 PAGE: 1 of 4 *** DRAFT *** SUBJECT: TRIAGE OF TRAUMA PATIENTS *** DRAFT *** APPROVED BY: I. PURPOSE Art Lathrop, EMS Director Joseph A. Barger,
EMS POLICIES AND PROCEDURES POLICY #: 13 EFFECT DATE: xx/xx/05 PAGE: 1 of 4 *** DRAFT *** SUBJECT: TRIAGE OF TRAUMA PATIENTS *** DRAFT *** APPROVED BY: I. PURPOSE Art Lathrop, EMS Director Joseph A. Barger,
TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4
 ROTATION LIAISON: INSTITUTION: LEVEL(S): TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4 I. GENERAL INFORMATION The General Surgery Department at Orlando Regional Health has three full
ROTATION LIAISON: INSTITUTION: LEVEL(S): TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4 I. GENERAL INFORMATION The General Surgery Department at Orlando Regional Health has three full
Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For. KGH Patients And Their Families
 Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For KGH Patients And Their Families The goal of this pamphlet is to provide information about cardiopulmonary resuscitation (CPR) so you can be adequately
Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For KGH Patients And Their Families The goal of this pamphlet is to provide information about cardiopulmonary resuscitation (CPR) so you can be adequately
REFERRAL HOSPITAL. The Importance of Door In Door Out Time DIDO
 REFERRAL HOSPITAL The Importance of Door In Door Out Time DIDO Time to Treatment is critical for STEMI patients For patients with ST-segment elevation myocardial infarction (STEMI), percutaneous coronary
REFERRAL HOSPITAL The Importance of Door In Door Out Time DIDO Time to Treatment is critical for STEMI patients For patients with ST-segment elevation myocardial infarction (STEMI), percutaneous coronary
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Convincing Deans that Ultrasound should be in the Medical Student Curriculum. Richard Hoppmann Dean University of South Carolina School of Medicine
 Convincing Deans that Ultrasound should be in the Medical Student Curriculum Richard Hoppmann Dean University of South Carolina School of Medicine Convincing Deans that Ultrasound should be in the Medical
Convincing Deans that Ultrasound should be in the Medical Student Curriculum Richard Hoppmann Dean University of South Carolina School of Medicine Convincing Deans that Ultrasound should be in the Medical
Ruchika D. Husa, MD, MS Assistant t Professor of Medicine in the Division of Cardiology The Ohio State University Wexner Medical Center
 Modified Early Warning Score (MEWS) Ruchika D. Husa, MD, MS Assistant t Professor of Medicine i in the Division of Cardiology The Ohio State University Wexner Medical Center MEWS Simple physiological scoring
Modified Early Warning Score (MEWS) Ruchika D. Husa, MD, MS Assistant t Professor of Medicine i in the Division of Cardiology The Ohio State University Wexner Medical Center MEWS Simple physiological scoring
Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults
 PS46 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults 1. INTRODUCTION Ultrasound imaging of the heart is
PS46 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults 1. INTRODUCTION Ultrasound imaging of the heart is
ALLOW NATURAL DEATH/WITHHOLDING AND/OR WITHDRAWING L I F E - S U S T A I N I N G T R E A T M E N T / NON-BENEFICIAL CARE AND RESUSCITATION POLICY
 PURPOSE SUPPORTIVE DATA To specify the parameters within which decisions regarding the withholding and/or withdrawing of life-sustaining treatment/non beneficial care and/or no initiation of cardiopulmonary
PURPOSE SUPPORTIVE DATA To specify the parameters within which decisions regarding the withholding and/or withdrawing of life-sustaining treatment/non beneficial care and/or no initiation of cardiopulmonary
HEMS in an urbansetting. Anne Weaver RESUS 2013, Limerick 27 th April 2013
 HEMS in an urbansetting Anne Weaver RESUS 2013, Limerick 27 th April 2013 Car at night 12 minutes by air 40 minutes by road 10 million people 25 mile radius London HEMS Pan London service Operates as
HEMS in an urbansetting Anne Weaver RESUS 2013, Limerick 27 th April 2013 Car at night 12 minutes by air 40 minutes by road 10 million people 25 mile radius London HEMS Pan London service Operates as
Cardiac Arrest: General Considerations
 Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Emergency Ultrasound Course
 Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 5: Credentialing 1 Why all the fuss? Why credential in point-of-care US (POCUS)? POCUS is quite a different skill to traditional US in the Radiology
Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 5: Credentialing 1 Why all the fuss? Why credential in point-of-care US (POCUS)? POCUS is quite a different skill to traditional US in the Radiology
ITLS & PHTLS: A Comparison
 ITLS & PHTLS: A Comparison International Trauma Life Support (ITLS) is a global organization dedicated to preventing death and disability from trauma through education and emergency care. ITLS educates
ITLS & PHTLS: A Comparison International Trauma Life Support (ITLS) is a global organization dedicated to preventing death and disability from trauma through education and emergency care. ITLS educates
CARDIAC SONOGRAPHER SERIES
 CARDIAC SONOGRAPHER SERIES Occ. Work Prob. Effective Code No. Class Title Area Area Period Date 4636 Cardiac Sonographer I 02 447 6 mo. 04/15/05 4637 Cardiac Sonographer II 02 447 6 mo. 04/15/05 4638 Cardiac
CARDIAC SONOGRAPHER SERIES Occ. Work Prob. Effective Code No. Class Title Area Area Period Date 4636 Cardiac Sonographer I 02 447 6 mo. 04/15/05 4637 Cardiac Sonographer II 02 447 6 mo. 04/15/05 4638 Cardiac
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
LIFE CARE planning. Advance Health Care Directive. my values, my choices, my care WASHINGTON. kp.org/lifecareplan
 Advance Health Care Directive WASHINGTON LIFE CARE planning kp.org/lifecareplan 60418811_NW All plans offered and underwritten by Kaiser Foundation Health Plan of the Northwest. 500 NE Multnomah St., Suite
Advance Health Care Directive WASHINGTON LIFE CARE planning kp.org/lifecareplan 60418811_NW All plans offered and underwritten by Kaiser Foundation Health Plan of the Northwest. 500 NE Multnomah St., Suite
Prehospital Endotracheal Intubation of Children by Paramedics
 PEDIATRICS/ORIGINAL CONTRIBUTION Prehospital Endotracheal Intubation of Children by Paramedics From the Department of Pediatrics*, Epidemiology ~, and Medicine ~, University of Washington; the Children's
PEDIATRICS/ORIGINAL CONTRIBUTION Prehospital Endotracheal Intubation of Children by Paramedics From the Department of Pediatrics*, Epidemiology ~, and Medicine ~, University of Washington; the Children's
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
All Intraosseous Sites Are Not Equal
 All Intraosseous Sites Are Not Equal Clinical Data Suggests the Sternal IO Route Improves Patient Outcomes Current Guidelines, (such as AHA) indicate that Intraosseous Infusion (IO) is a rapid, safe and
All Intraosseous Sites Are Not Equal Clinical Data Suggests the Sternal IO Route Improves Patient Outcomes Current Guidelines, (such as AHA) indicate that Intraosseous Infusion (IO) is a rapid, safe and
Pennsylvania Trauma Nursing Core Curriculum. Posted to PTSF Website: 10/30/2014
 Pennsylvania Trauma Nursing Core Curriculum Posted to PTSF Website: 10/30/2014 PREFACE Care of the trauma patient has evolved since 1985, when the Pennsylvania Trauma Systems Foundation (PTSF) Board of
Pennsylvania Trauma Nursing Core Curriculum Posted to PTSF Website: 10/30/2014 PREFACE Care of the trauma patient has evolved since 1985, when the Pennsylvania Trauma Systems Foundation (PTSF) Board of
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Patient conditions to notify physician. The ALS RN or ALS RT will immediately notify the physician:
 1 CURRENT EFFECTIVE DATE March 1995 REVISED DATE June 2011 MANUAL: NICU/PICU ALS TRANSPORT TRACKING # [ ] P O L I C Y/PROCEDURE [ X] STANDARDIZED PROCEDURE [ ] PLAN [ ] GUIDELINE [ ] PLAN Specialty Review
1 CURRENT EFFECTIVE DATE March 1995 REVISED DATE June 2011 MANUAL: NICU/PICU ALS TRANSPORT TRACKING # [ ] P O L I C Y/PROCEDURE [ X] STANDARDIZED PROCEDURE [ ] PLAN [ ] GUIDELINE [ ] PLAN Specialty Review
Listen to your heart: Good Cardiovascular Health for Life
 Listen to your heart: Good Cardiovascular Health for Life Luis R. Castellanos MD, MPH Assistant Clinical Professor of Medicine University of California San Diego School of Medicine Sulpizio Family Cardiovascular
Listen to your heart: Good Cardiovascular Health for Life Luis R. Castellanos MD, MPH Assistant Clinical Professor of Medicine University of California San Diego School of Medicine Sulpizio Family Cardiovascular
Heart Center Packages
 Heart Center Packages For more information and appointments, Please contact The Heart Center of Excellence at the American Hospital Dubai Tel: +971-4-377-6571 Email: [email protected] www.ahdubai.com
Heart Center Packages For more information and appointments, Please contact The Heart Center of Excellence at the American Hospital Dubai Tel: +971-4-377-6571 Email: [email protected] www.ahdubai.com
Guidelines for the Operation of Burn Centers
 C h a p t e r 1 4 Guidelines for the Operation of Burn Centers............................................................. Each year in the United States, burn injuries result in more than 500,000 hospital
C h a p t e r 1 4 Guidelines for the Operation of Burn Centers............................................................. Each year in the United States, burn injuries result in more than 500,000 hospital
Common Questions and Answers About Severe Brain Injury
 Common Questions and Answers About Severe Brain Injury What you should know about severe brain injuries The purpose of this publication is to provide you with information about severe brain injuries. Such
Common Questions and Answers About Severe Brain Injury What you should know about severe brain injuries The purpose of this publication is to provide you with information about severe brain injuries. Such
Sonography for Trauma
 Sonography for Trauma Christine Butts and Justin Cook 9 KEY POINTS Focused abdominal sonography for trauma (FAST) is sensitive and specific for the detection of intraperitoneal free fluid, but it has poor
Sonography for Trauma Christine Butts and Justin Cook 9 KEY POINTS Focused abdominal sonography for trauma (FAST) is sensitive and specific for the detection of intraperitoneal free fluid, but it has poor
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE
 ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
Cardiac and Pulmonary Issues in the Elite Athlete. Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015
 Cardiac and Pulmonary Issues in the Elite Athlete Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015 THORACIC EMERGENCIES Hockey related thoracic trauma is blunt Injury to the boney
Cardiac and Pulmonary Issues in the Elite Athlete Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015 THORACIC EMERGENCIES Hockey related thoracic trauma is blunt Injury to the boney
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
Information for Patients. Advance Health Care Directive Kit A guide to help you express your health care wishes
 Information for Patients Advance Health Care Directive Kit A guide to help you express your health care wishes Table of contents PART I - REQUIRED Selection of a decision maker Who will make health care
Information for Patients Advance Health Care Directive Kit A guide to help you express your health care wishes Table of contents PART I - REQUIRED Selection of a decision maker Who will make health care
January-February 2008 Volume 27 Number 1. Case Study Peer Reviewed Perimortem cesarean section in the helicopter EMS setting: A case report
 January-February 2008 Volume 27 Number 1 Case Study Peer Reviewed Perimortem cesarean section in the helicopter EMS setting: A case report http://www2.us.elsevierhealth.com/inst/serve?retrieve=pii/s1067-991x(07)00164-2&arttype=full#head1
January-February 2008 Volume 27 Number 1 Case Study Peer Reviewed Perimortem cesarean section in the helicopter EMS setting: A case report http://www2.us.elsevierhealth.com/inst/serve?retrieve=pii/s1067-991x(07)00164-2&arttype=full#head1
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
Overview. Geriatric Overview. Chapter 26. Geriatrics 9/11/2012
 Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Impact of Manual CPR on Increasing Coronary Perfusion Pressure
 Impact of Manual CPR on Increasing Coronary Perfusion Pressure In sudden cardiac arrest cases, the ability to adequately perfuse the brain and heart during resuscitation is of critical importance. The
Impact of Manual CPR on Increasing Coronary Perfusion Pressure In sudden cardiac arrest cases, the ability to adequately perfuse the brain and heart during resuscitation is of critical importance. The
SAEM ETHICS CURRICULUM Module 3: End of Life Issues
 SAEM ETHICS CURRICULUM Module 3: End of Life Issues SAEM Ethics Committee, 2010-12 Primary Author: Ryan Paterson, MD, Emergency Medicine, University of Colorado SOM Review date: April, 2012 Updated: March,
SAEM ETHICS CURRICULUM Module 3: End of Life Issues SAEM Ethics Committee, 2010-12 Primary Author: Ryan Paterson, MD, Emergency Medicine, University of Colorado SOM Review date: April, 2012 Updated: March,
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography
 Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography Anthony M.-H. Ho, Lester A. H. Critchley, Patricia Kan, Sylvia Au, Siu Keung Ng, Simon K. C. Chan, Philip Lam, Gordon Choi, Alex Lee,
Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography Anthony M.-H. Ho, Lester A. H. Critchley, Patricia Kan, Sylvia Au, Siu Keung Ng, Simon K. C. Chan, Philip Lam, Gordon Choi, Alex Lee,
Physician Insertion via Helicopter Emergency Medical Services (HEMS) to Improve patient care in the time of disaster response.
 Physician Insertion via Helicopter Emergency Medical Services (HEMS) to Improve patient care in the time of disaster response. JD Boston University Medical School Practicum Each of us should strive "to
Physician Insertion via Helicopter Emergency Medical Services (HEMS) to Improve patient care in the time of disaster response. JD Boston University Medical School Practicum Each of us should strive "to
Electrocardiographic Issues in Williams Syndrome
 Electrocardiographic Issues in Williams Syndrome R. Thomas Collins II, MD Assistant Professor, Pediatrics and Internal Medicine University of Arkansas for Medical Sciences Arkansas Children s Hospital
Electrocardiographic Issues in Williams Syndrome R. Thomas Collins II, MD Assistant Professor, Pediatrics and Internal Medicine University of Arkansas for Medical Sciences Arkansas Children s Hospital
Teaching Medical Students Diagnostic Sonography
 Article Teaching Medical Students Diagnostic Sonography Peter H. Arger, MD, Susan M. Schultz, RDMS, Chandra M. Sehgal, PhD, Theodore W. Cary, Judith Aronchick, MD Objective. The purpose of this pilot project
Article Teaching Medical Students Diagnostic Sonography Peter H. Arger, MD, Susan M. Schultz, RDMS, Chandra M. Sehgal, PhD, Theodore W. Cary, Judith Aronchick, MD Objective. The purpose of this pilot project
Advance Health Care Directive Form Instructions
 Advance Health Care Directive Form Instructions You have the right to give instructions about your own health care. You also have the right to name someone else to make health care decisions for you. The
Advance Health Care Directive Form Instructions You have the right to give instructions about your own health care. You also have the right to name someone else to make health care decisions for you. The
Aktuelle Literatur aus der Notfallmedizin
 05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
Management of Pacing Wires After Cardiac Surgery
 Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
Field Trauma Triage & Air Ambulance Utilization. SWORBHP Answers
 Field Trauma Triage & Air Ambulance Utilization SWORBHP Answers Presented by : Dr. Mike Lewell, Regional Medical Director Dr. Mike Peddle, Local Medical Director Introduction/History What s this all about?
Field Trauma Triage & Air Ambulance Utilization SWORBHP Answers Presented by : Dr. Mike Lewell, Regional Medical Director Dr. Mike Peddle, Local Medical Director Introduction/History What s this all about?
RECENT MEDICAL MALPRACTICE CASES By Judge Bryan C. Dixon 1. MERE TELEPHONE CONVERSATION WITH TREATING DOCTOR DOES NOT ESTABLISH DUTY TO PATIENT
 RECENT MEDICAL MALPRACTICE CASES By Judge Bryan C. Dixon 1. MERE TELEPHONE CONVERSATION WITH TREATING DOCTOR DOES NOT ESTABLISH DUTY TO PATIENT Jennings v. Badgett, 2010 OK 7 Facts: Plaintiffs are parents
RECENT MEDICAL MALPRACTICE CASES By Judge Bryan C. Dixon 1. MERE TELEPHONE CONVERSATION WITH TREATING DOCTOR DOES NOT ESTABLISH DUTY TO PATIENT Jennings v. Badgett, 2010 OK 7 Facts: Plaintiffs are parents
State of Ohio Health Care Power of Attorney of
 State of Ohio Health Care Power of Attorney of (Print Full Name) (Birth Date) I state that this is my Health Care Power of Attorney and I revoke any prior Health Care Power of Attorney signed by me. I
State of Ohio Health Care Power of Attorney of (Print Full Name) (Birth Date) I state that this is my Health Care Power of Attorney and I revoke any prior Health Care Power of Attorney signed by me. I
Damage Control in Abdominal Trauma
 Damage Control in Abdominal Trauma Steven Stylianos, MD Surgeon-in-Chief, Morgan Stanley Children s Hospital Rudolph Schullinger Professor of Surgery, Columbia University College of Physicians & Surgeons
Damage Control in Abdominal Trauma Steven Stylianos, MD Surgeon-in-Chief, Morgan Stanley Children s Hospital Rudolph Schullinger Professor of Surgery, Columbia University College of Physicians & Surgeons
Advanced Cardiovascular Life Support Case Scenarios
 Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
Emergency Ultrasound. Emergency Room. EMERGENCY ULTRASOUND reimagined
 in Emergency and Critical Care WORKSHOP Emergency Room The POINT-OF-CARE THINKING and the EMERGENCY ULTRASOUND reimagined Luca Neri, MD & Enrico Storti, MD SSUEm 118 Milano Intenisve Care Unit AO Niguarda
in Emergency and Critical Care WORKSHOP Emergency Room The POINT-OF-CARE THINKING and the EMERGENCY ULTRASOUND reimagined Luca Neri, MD & Enrico Storti, MD SSUEm 118 Milano Intenisve Care Unit AO Niguarda
Emergency Medical Technician - Basic
 Washington State Specific Objectives for Emergency Medical Technician - Basic OFFICE OF EMERGENCY MEDICAL AND TRAUMA PREVENTION September 1996 Emergency Medical Technician - Basic Definition: Emergency
Washington State Specific Objectives for Emergency Medical Technician - Basic OFFICE OF EMERGENCY MEDICAL AND TRAUMA PREVENTION September 1996 Emergency Medical Technician - Basic Definition: Emergency
EMS Subspecialty Certification Review Course. Learning Objectives 2. Medical Oversight of EMS Systems 2.1 Medical Oversight
 EMS Subspecialty Certification Review Course Medical Oversight of EMS Systems 2.1 Medical Oversight Version Date: 7.31.15 Learning Objectives 1 Upon the completion of this program participants will be
EMS Subspecialty Certification Review Course Medical Oversight of EMS Systems 2.1 Medical Oversight Version Date: 7.31.15 Learning Objectives 1 Upon the completion of this program participants will be
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department!
 Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
CALIFORNIA Advance Directive Planning for Important Health Care Decisions
 CALIFORNIA Advance Directive Planning for Important Health Care Decisions CaringInfo 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CaringInfo, a program of the National
CALIFORNIA Advance Directive Planning for Important Health Care Decisions CaringInfo 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CaringInfo, a program of the National
2 North Meridian Street Indianapolis, Indiana 46204 March 1999 Revised May 2004 Revised July 1, 2013 ADVANCE DIRECTIVES YOUR RIGHT TO DECIDE
 2 North Meridian Street Indianapolis, Indiana 46204 March 1999 Revised May 2004 Revised July 1, 2013 ADVANCE DIRECTIVES YOUR RIGHT TO DECIDE The purpose of this brochure is to inform you of ways that you
2 North Meridian Street Indianapolis, Indiana 46204 March 1999 Revised May 2004 Revised July 1, 2013 ADVANCE DIRECTIVES YOUR RIGHT TO DECIDE The purpose of this brochure is to inform you of ways that you
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona
 Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Emergency Medical Services Agency. Report to the Local Agency Formation Commission
 Emergency Medical Services Agency August 8, 2012 Report to the Local Agency Formation Commission The Relationship of Fire First Response to Emergency Medical Services On September 26, 2011, the Contra
Emergency Medical Services Agency August 8, 2012 Report to the Local Agency Formation Commission The Relationship of Fire First Response to Emergency Medical Services On September 26, 2011, the Contra
The Living Will: What Do I Need to Know?
 What is a Living Will? The Living Will: What Do I Need to Know? Simply put, a Living Will is a legal document that tells the doctor that you don t want to be put on a life-support machine when it won t
What is a Living Will? The Living Will: What Do I Need to Know? Simply put, a Living Will is a legal document that tells the doctor that you don t want to be put on a life-support machine when it won t
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
What is the Future of Epinephrine in Cardiac Arrest? Pros and Cons
 What is the Future of Epinephrine in Cardiac Arrest? Pros and Cons Melissa L. Thompson Bastin, PharmD., BCPS Komal A. Pandya, PharmD., BCPS 0 Presenter Disclosure Information Melissa L. Thompson Bastin,
What is the Future of Epinephrine in Cardiac Arrest? Pros and Cons Melissa L. Thompson Bastin, PharmD., BCPS Komal A. Pandya, PharmD., BCPS 0 Presenter Disclosure Information Melissa L. Thompson Bastin,
Utah Advance Directive Form & Instructions
 Utah Advance Directive Form & Instructions 2009 Edition published by Utah Medical Association 310 E. 4500 South, Suite 500 Salt Lake City, UT 84107 Instructions for Completing the Advance Health Care Directive
Utah Advance Directive Form & Instructions 2009 Edition published by Utah Medical Association 310 E. 4500 South, Suite 500 Salt Lake City, UT 84107 Instructions for Completing the Advance Health Care Directive
Power of Attorney for Health Care For
 Power of Attorney for Health Care For Name: Date of Birth: Address: Telephone: This document is on file at Copies of this document have been given to my health care agent(s) and: 1. 2. 3. 4. 5. Courtesy
Power of Attorney for Health Care For Name: Date of Birth: Address: Telephone: This document is on file at Copies of this document have been given to my health care agent(s) and: 1. 2. 3. 4. 5. Courtesy
SUGGESTIONS & REQUIREMENTS For Medical Power of Attorney & Completing the Texas Will to Live Form
 SUGGESTIONS & REQUIREMENTS For Medical Power of Attorney & Completing the Texas Will to Live Form 1. This Medical Power of Attorney (also known as the Health Care Agent Designation Form) allows you to
SUGGESTIONS & REQUIREMENTS For Medical Power of Attorney & Completing the Texas Will to Live Form 1. This Medical Power of Attorney (also known as the Health Care Agent Designation Form) allows you to
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
CARDIAC CARE. Giving you every advantage
 CARDIAC CARE Giving you every advantage Getting to the heart of the matter The Cardiovascular Program at Northwest Hospital & Medical Center is dedicated to the management of cardiovascular disease. The
CARDIAC CARE Giving you every advantage Getting to the heart of the matter The Cardiovascular Program at Northwest Hospital & Medical Center is dedicated to the management of cardiovascular disease. The
