TPA / Carrier Questionnaire GENERAL INFORMATION: Questions must be answered for each coverage you are quoting.
|
|
|
- Violet Morris
- 10 years ago
- Views:
Transcription
1 GENERAL INFORMATION: Questions must be answered for each coverage you are quoting. 1. Describe the history, organization and ownership of your company. 2. Explain your ownership, listing all separate legal entities and their relationships. Describe all major shareholders and owners and give percentage of ownership for each. 3. Do you contemplate any agreements, or are agreements being negotiated between you and other parties, which may affect the plan s ownership, corporate structure or management during the next year? 4. Provide the name and address of your company and all outside vendors used in this RFP. Include local, toll-free telephone and fax numbers. 5. Supply an organizational chart identifying the functions and reporting relationships of key people directly responsible for administrative services to. 6. Give the name and title of the person(s) with overall responsibility for planning, supervising, and performing the day-to-day administrative services for. 7. Will you assign an underwriter or another group benefit professional with similar knowledge and experience to? 8. Will Filice Insurance have direct contact and access to all of the above named person(s)? 9. Explain in detail the steps you anticipate will be needed to ensure a smooth implementation. Include a definition of specific activities and a timetable of events. The timetable should assume an award notification date and plan implementation schedule, which includes completion of all enrollment packets, enrollment meetings, system updates and ID card issuance by. 10. Provide a detailed work plan specifying all critical milestones and identifying persons from your organization who will be responsible for each major task. 11. Provide recommendations concerning the following situations: a. Eligible dependent students residing out of area b. Eligible dependent children residing with a separated or divorced parent and living out of area c. Eligible dependents enrolled in a U.S. school but studying outside of the U.S. 12. If you are selected as the administrator, will you permit claim audits at your claim office by a third-party auditor? If so, is there a charge for the time spent by your claims people in meeting with the auditor? 13. requires that you provide year-end financial information and renewal rates and fees 120 days prior to the policy anniversary date. Additionally, Filice Insurance will be provided all service agreements, contracts, amendments, reports, and claims data. Will you agree to this? 14. Will you agree to performance-based administrative fee structures as outlined in this RFP? 15. Will you agree to provide raw claims data to Filice Insurance in a format consistent with their system? See format requirements in the Attachment section of this RFP. 16. Describe any previous or pending material lawsuits in the last 10 years. 17. Have any of the principals in your firm or any of your employees (former or current) ever been indicted or convicted of mishandling/misappropriating any insurance company or client funds? If yes, please explain. 18. Are you HIPAA EDI compliant? 1
2 Please respond to the following questions, recognizing that your organization will be expected to underwrite and administer the program as stated in this RFP unless specifically noted here. 1. Will your organization insure and/or administer the program exactly as shown in this RFP? 2. Will your organization require any additional information or impose restrictions on benefit selections? 3. Does your organization agree to the performance objectives outlined in this RFP? 4. Does your organization agree to cooperate and ensure successful interface of all data with an outside vendor? This assumes that awards coverages to an outside vendor. 2
3 REFERENCES 1. Please provide three references of current clients and two references of clients you have lost in the past two years. Ideally, these references would be similar in size to. 2. What percent of your ASO clients have 1, 000-3,000 covered employees? 3. What percent of your ASO clients have covered lives? 4. What percent of your ASO clients have covered lines? 5. Please provide a reference from a fully insured client. 6. Please provide a reference from a similar product or service offering. 3
4 CLAIM FACILITY AND PERSONNEL 1. How many full-time employees work in this office? 2. How many processors report to one supervisor? 3. What additional responsibilities do the claim processors have (telephone inquiries, correspondence, filing, opening mail, etc.)? 4. What is the case load per processor? What is the number of claims that each processor is expected to process? 5. What is the average length of experience for those claims processors who would be servicing a new large account? 6. What is the claim processor turnover rate at your company? 4
5 CLAIMS PROCESSING AND ADMINISTRATION 1. Do you have an automated claim processing and payments system? 2. How long has this system been operational? 3. What future enhancements are planned for this system? 4. Can all plan design options and provisions automatically be calculated by this system? Please note exceptions. 5. Are there automatic system edits for plan age limits? 6. Does this system track and report overrides? 7. How are processors limited to specific dollar level payments? What other payments require supervisory approval? 8. What are the capabilities of the system relating to tape eligibility feed? 9. Who can add or change eligibility information? 10. How does the system keep track of non-covered expenses? Are all denied claims tracked? 11. How is hard copy stored? How long is it retained? 12. Does the system accumulate annual and lifetime maximums? 13. Are accumulations and claim history information automatically updated by adjustments? 14. How are providers identified (TIN, name/zip, phone number, other)? 15. Does the system track carry over deductible amounts and adjust out-of-pocket sequence claims? 16. Do you use CPT-4 coding? If no, what do you use? 17. Can the system screen for different plan versions based on the incurred date? 18. What frequency edits can be programmed? 19. How are duplicate charges identified by the system? 20. Does your system automatically update the file immediately after a transaction is entered? 21. Define turnaround time for claim processing purposes. 22. Indicate the administrative service targets and actual [year1] and [year2] performance in each of the areas listed below for the proposed facility: a. Turnaround time b. Financial accuracy c. Payment accuracy d. Processing accuracy e. Resolution time for telephone and written inquiries 5
6 23. What should be the minimum standards with respect to each of the administrative service areas listed above? What portion of the quoted rates/fees would be returned to if these standards are not achieved? a. Turnaround time b. Financial accuracy c. Payment accuracy d. Processing accuracy e. Resolution time for telephone and written inquiries 24. Describe the procedures for administering COB in-network vs. out-of-network, specifying whether COB is systemcalculated or manually calculated. 25. Indicate your organization s ability to administer various types of COB. 26. Describe how COB for an in-network with negotiated fees is calculated. 27. What is the current collection/return rate for COB? (as a percent of paid claims). 28. Do you routinely capture, maintain, and access a spouse s coverage and employment data for COB? What specific data elements do you store in these files? How do you update them? 29. Describe the quality management program which is applied to the claims administration function (e.g., coding, processing, paying), specifying audit procedures and error categories. 6
7 CLAIM ADMINISTRATION AND ADJUDICATION 1. Where will you process medical claims? Where will drafts and EOBs be issued? 2. Describe the organization, methods, and procedures for responding to routine claim inquires from employees. 3. Do you routinely pursue subrogation opportunities? If yes, what are your criteria for evaluating subrogation potential? Describe the methods and procedures for investigating. What percent of recoveries would you credit to s account? 4. How do claim processors flag a possible pre-existing condition? What steps do they take to verify a pre-existing condition? 5. Do you process and pay some or all of your managed health care claims (proprietary PPO, HMO) with your indemnity claim adjudication system? If yes, how would the claim processor know a contracted provider treated the patient? Does your claim system automatically determine reimbursement for contracting providers or is this a manual function? If you use other autonomous claim systems to process and pay your managed care claims, where are they? Who manages and operates them? How do you coordinate claim processing for network claims and non-network claims? Do you compile a comprehensive database (network and non-network) for statistical analyses? 6. What is the name of the software system you are using? Who developed it? What year? 7. Is your software leased or owned? If owned, when was it purchased? 8. What is the name of your hardware? Is your hardware leased or owned? 9. Have you changed/upgraded systems within last 12 months? 10. What is your payment accuracy objective? Statistical: number of claims paid? Financial: dollar amount paid without error? 11. Describe the payment authority limitation for the claims staff and the criteria for internal audits. 12. What is your payment accuracy performance during the last 12 months? 13. What is your turnaround objective? 14. What was your turnaround time over the last 12 months? 15. R&C is based upon: HIAA, MDR, Internal, Med-Index, Other? 16. Is your R&C database on-line? 17. How often is R&C data updated? 18. Describe your procedures for auditing and/or negotiating provider bills. 7
8 AUDITING PRACTICES 1. What are your standard claim audit procedures for claims in process and those that are already paid? 2. How are overpayments handled, and to what extent does your company go to recover those overpayments? 3. System security and audit procedures: Describe security for master file Describe security for client funds Describe record retention program for enrollment card, billing files, etc. Describe back-up system in the event the computer master file is destroyed. 4. Has the department been audited by a third party for accuracy/security? 8
9 UTILIZATION REVIEW SERVICES 1. To what extent do you involve the patient and/or family in the review process? Be specific. 2. What percent of all cases are reviewed by a physician and what determines whether a physician becomes involved? 3. Describe your review criteria for: a. Medical necessity for proposed care b. Medical necessity for admission c. Necessity for continued stay d. Length of stay e. Mental health care (inpatient and outpatient) f. Chemical dependency treatment (inpatient and outpatient) g. Necessity for surgical procedures (inpatient and outpatient) h. Case management i. Outpatient services 4. Describe how your UR system is integrated with claim payment. 5. Describe your appeal process for members and physicians. 6. How do you define case management? 7. What specific cost containment programs are you actively involved in? Describe fully. 8. Describe your disease management programs in detail. How do you calculate ROI? Do you offer client specific disease management reports? 9. What is your fee structure? Do you charge on a monthly or case rate? 10. What are your predictive modeling capabilities? 11. Is your utilization provider URAC-accredited? 9
10 NETWORKS 1. Provide a response for the following questions describing the capabilities for each PPO network that would be applicable to this RFP. a. PPO network b. Location(s) c. Date established a. Total enrollment b. Average hospital discount breakdown inpatient/outpatient c. Average professional discount d. Percent PCPs Board Certified 2. What is your service area? Please describe by county & zip code. 3. Provide a Geo Access report indicating the coverage provided by the proposed networks based on zip code information on enclosed census based on the following criteria: a. Within 5 and 10 miles - 2 PCP, 1 OB-GYN, 1 Pediatrician 4. Please explain the access standards used for the report (e.g. from center of zip code to employee s home or provider office, and use of 3 or 5 digit zip codes). 5. Describe any network modifications that are underway or are planned for the future, specifying the modifications, status, and target date for completion. 6. Centers of Excellence a. Indicate the "Centers of Excellence" services and providers currently available in the network. 7. Chiropractic a. Indicate the chiropractic services currently available. b. Describe the method used by subscribers to access such services. 8. Do you have the capability to coordinate a drug testing program for all locations? If yes, is there a separate cost? If not, would you be willing to develop a program? If yes, is there a separate cost? 10
11 9. Please indicate whether your physician application and credentialing process requires the following; a. Written verification of education and experience b. Verification of current license and DEA certificate c. Investigation for adverse action on license and/or hospital privileges d. Verification of letters of recommendation e. Regular recertification of participating physicians f. Verification that physicians complete continuing education requirements g. Documentation on malpractice claims, settlements, and judgments for the previous five years. 10. Explain in detail the process and frequency of recertification credentialing. 11. Do you selectively drop individual physicians in a medical group or physician association while continuing to contract with the entire medical group or association? 12. Do you have dedicated provider relations staff to answer questions for physician office personnel regarding administrative policies and procedures? 13. Are physicians prevented from balance billing? 14. How are radiology services reimbursed? 15. How are laboratory services reimbursed? 16. How are anesthesiology services reimbursed? 17. What screens do you use to audit coding accuracy? 18. What physician services are not available through the network? How are they handled? 11
12 DENTAL CLAIM SYSTEM 1. Explain if this is the same system as the medical system and how (if the two systems interface). 2. Does the system maintain historical information on submitted expenses and paid claims? How long is claim history maintained on-line? On microfilm? On hard copy? 3. Are claims routinely coded using standard ADA codes? What other coding protocols are used? 4. Will the system automatically deny any (all) non-covered items based on the procedure codes entered by the processor? 5. Describe your organization s use of dental consultants. 6. At what percentile of UCRs are dental claims paid? 12
13 PRESCRIPTION PROGRAM CAPABILITIES & SYSTEMS 1. Describe your network capabilities. 2. Describe the process by which you adjudicate claims and verify eligibility. 3. Discuss the variations in plan design that your network system can administer. 4. How many participating pharmacies are currently in your network? 5. Describe the prescription drug program you would suggest for members who do not live within a reasonable distance of your network pharmacies. 6. Provide a list of the retail prescription drug chains that currently participate in your network program. Do members have access via the web to find retail pharmacies within their area? 7. What are your procedures in the event of member termination? 8. Describe the procedures a network pharmacist would follow to verify eligibility, collect the proper copay and process the claim in routine circumstances, and where there was a problem accessing the computer network system. 9. Provide a list of drugs/items which you would recommend not be covered. 10. Describe the programs available to maximize generic substitution. 11. Describe your Drug Utilization Review (DUR) procedures. 12. Explain how your computerized patient medication profiles are maintained and used. 13. Describe your adverse drug reaction reporting program, if available. 14. How do you screen for duplicate prescriptions, therapeutic overlaps, early refill and vacation refills? 15. What customer service protocols are in place for an irate member call? What happens when the member and client are on a call regarding an escalated issue? 16. How are consumer-driven or high deductible plans administered with the company? How is connectivity established between vendors? How often is claims data shared? 17. How are biotech or specialty drugs processed? Is there any additional communication to the member regarding the specific therapy and how to administer medications? 13
14 SELF-FUNDED QUOTATION ASSUMPTION/CONDITIONS 1. Are the fees quoted for firm and guaranteed for: a. Administrative service? b. Individual stop loss? c. Aggregate stop loss? 2. If not, what are the conditions or assumptions, and what is the fee impact if these are not met for: a. Administrative services? b. Individual stop loss? c. Aggregate stop loss? 3. Are the stop loss attachment points quoted for firm and guaranteed? a. If not, what are the conditions or assumptions, and what is the impact to the attachment point(s) if they are not met? 4. Do quoted rates and fees include all services described within this RFP? If not, please indicate which services are not included. 5. Will individual medical underwriting of self-funded members ever be required? Under what circumstances? 6. What is the maximum percentage the quoted fees will increase for: a. Administrative services? b. Individual stop loss? c. Aggregate stop loss? 7. Please outline the reimbursement process and banking arrangements for your self-funded quotes. Attach copies of any agreements related to this process. Include in the response answers to the following: a. Do you require a specific bank be used, or does have the choice? b. Is an initial deposit required? A minimum balance? c. What is the frequency of claim transfers? d. How often is the claim paying account reconciled? 8. Please describe the process and timing of reimbursements to when the stop loss threshold has been exceeded for: a. Individual stop loss b. Aggregate stop loss 9. Does individual and aggregate stop loss coverage include: a. COBRA participants? b. All other covered members as of the effective date? 14
15 10. Please describe any actively at work, pre-existing conditions or other limitations (other than those requested) that apply to: a. Individual stop loss b. Aggregate stop loss 11. With your proposal please submit copies of your most recent financial ratings to include AM Best and one of the following: Moody's, Standard & Poor's, Duff & Phelps or Weiss Research, as well as ratings for stop loss carriers and any other outside vendors in your proposal. Your prompt response is appreciated. Please return the above items to: Filice Insurance 738 North First Street San Jose, CA Phone Fax Zywave, Inc
Independent Accountants Report on Applying Agreed-Upon Procedures
 Independent Accountants Report on Applying Agreed-Upon Procedures Honorable Members of the District School Board District School Board of Osceola County, Florida Kissimmee, Florida Dear Members: We have
Independent Accountants Report on Applying Agreed-Upon Procedures Honorable Members of the District School Board District School Board of Osceola County, Florida Kissimmee, Florida Dear Members: We have
Summary of Benefits and Coverage What this Plan Covers & What it Costs - 2015
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan document at www.mpiphp.org or by calling 1-855-275-4674. Important Questions Answers
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan document at www.mpiphp.org or by calling 1-855-275-4674. Important Questions Answers
407-767-8554 Fax 407-767-9121
 Florida Consumers Notice of Rights Health Insurance, F.S.C.A.I, F.S.C.A.I., FL 32832, FL 32703 Introduction The Office of the Insurance Consumer Advocate has created this guide to inform consumers of some
Florida Consumers Notice of Rights Health Insurance, F.S.C.A.I, F.S.C.A.I., FL 32832, FL 32703 Introduction The Office of the Insurance Consumer Advocate has created this guide to inform consumers of some
Summary of Benefits and Coverage What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan document at www.mpiphp.org or by calling 1-855-275-4674. Important Questions Answers
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan document at www.mpiphp.org or by calling 1-855-275-4674. Important Questions Answers
Northeastern University 2015 Medical Benefits
 Northeastern University 2015 Medical Benefits Northeastern s 2015 Open Enrollment Effective Date: January 1, 2015 2015 Medical Plan Options Blue Choice New England Core POS Plan New Plan Blue Choice New
Northeastern University 2015 Medical Benefits Northeastern s 2015 Open Enrollment Effective Date: January 1, 2015 2015 Medical Plan Options Blue Choice New England Core POS Plan New Plan Blue Choice New
Chiropractic Assistants Insurance Verification Training Guide
 Chiropractic Assistants Insurance Verification Training Guide What You Will Learn: How to Obtain Maximum Chiropractic Benefits Tools Needed to Verify Benefits Understanding Why You Are Verifying Understanding
Chiropractic Assistants Insurance Verification Training Guide What You Will Learn: How to Obtain Maximum Chiropractic Benefits Tools Needed to Verify Benefits Understanding Why You Are Verifying Understanding
2013 IBM Health Benefit Comparison Charts
 203 IBM Health Benefit Comparison Charts for IBM Active Employees These Health Benefit Comparison Charts provide a summary overview of the coverage available for medical services, mental health/substance
203 IBM Health Benefit Comparison Charts for IBM Active Employees These Health Benefit Comparison Charts provide a summary overview of the coverage available for medical services, mental health/substance
Health Insurance After Graduation: Individual Health Insurance in California
 Health Insurance After Graduation: Individual Health Insurance in California University of California, Berkeley Student Health Insurance Office Tang Center Fall Semester 2013 Health Care vs. Health Insurance
Health Insurance After Graduation: Individual Health Insurance in California University of California, Berkeley Student Health Insurance Office Tang Center Fall Semester 2013 Health Care vs. Health Insurance
SCHEDULE OF BENEFITS. Group Access Care Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
FREQUENTLY ASKED QUESTIONS ID CARDS / ELIGIBILITY / ENROLLMENT
 FREQUENTLY ASKED QUESTIONS ID CARDS / ELIGIBILITY / ENROLLMENT BENEFIT INFORMATION CLAIMS STATUS/INFORMATION GENERAL INFORMATION PROVIDERS THE SIGNATURE 90 ACCOUNT PLAN THE SIGNATURE 80 PLAN USING YOUR
FREQUENTLY ASKED QUESTIONS ID CARDS / ELIGIBILITY / ENROLLMENT BENEFIT INFORMATION CLAIMS STATUS/INFORMATION GENERAL INFORMATION PROVIDERS THE SIGNATURE 90 ACCOUNT PLAN THE SIGNATURE 80 PLAN USING YOUR
2015 IBM Health Benefit Comparison Charts for IBM Active Employees
 2015 IBM Health Benefit Comparison Charts for IBM Active Employees These Health Benefit Comparison Charts provide a summary overview of the coverage available for medical, mental health/substance care
2015 IBM Health Benefit Comparison Charts for IBM Active Employees These Health Benefit Comparison Charts provide a summary overview of the coverage available for medical, mental health/substance care
Health Insurance. A Small Business Guide. New York State Insurance Department
 Health Insurance A Small Business Guide New York State Insurance Department Health Insurance A Small Business Guide The Key Health insurance is a key benefit of employment. Most organizations with more
Health Insurance A Small Business Guide New York State Insurance Department Health Insurance A Small Business Guide The Key Health insurance is a key benefit of employment. Most organizations with more
Available to Those who ARE Medicare Eligible
 LACERA is proud to offer comprehensive medical plans to Los Angeles County retirees and their eligible dependents. Eligibility for some plans depends on whether the person being insured is eligible for
LACERA is proud to offer comprehensive medical plans to Los Angeles County retirees and their eligible dependents. Eligibility for some plans depends on whether the person being insured is eligible for
1) How does my provider network work with Sanford Health Plan?
 NDPERS FAQ Summary Non-Medicare Members Last Updated: 8/5/2015 PROVIDER NETWORK 1) How does my provider network work with Sanford Health Plan? Sanford Health Plan is offering you the same PPO network you
NDPERS FAQ Summary Non-Medicare Members Last Updated: 8/5/2015 PROVIDER NETWORK 1) How does my provider network work with Sanford Health Plan? Sanford Health Plan is offering you the same PPO network you
August 2014. SutterSelect Administrative Manual
 August 2014 SutterSelect Administrative Manual Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
August 2014 SutterSelect Administrative Manual Introduction This SutterSelect Administrative Manual has been prepared as a resource for providers who are caring for members of SutterSelect health plans.
SCHEDULE OF BENEFITS (continued) Group LINK Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68 ] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68 ] Family Coverage [$1,210.66]] Benefit
Health Insurance Matrix 01/01/16-12/31/16
 Employee Contributions Family Monthly : $121.20 Bi-Weekly : $60.60 Monthly : $290.53 Bi-Weekly : $145.26 Monthly : $431.53 Bi-Weekly : $215.76 Monthly : $743.77 Bi-Weekly : $371.88 Employee Contributions
Employee Contributions Family Monthly : $121.20 Bi-Weekly : $60.60 Monthly : $290.53 Bi-Weekly : $145.26 Monthly : $431.53 Bi-Weekly : $215.76 Monthly : $743.77 Bi-Weekly : $371.88 Employee Contributions
Gilsbar 360 Alliance PROVIDER MANUAL. Gilsbar. www.gilsbar360alliance.com
 Gilsbar 360 Alliance PROVIDER MANUAL Gilsbar www.gilsbar360alliance.com Dear Provider: Gilsbar is building a PPO network that gives providers and employers the opportunity to truly work together. We ve
Gilsbar 360 Alliance PROVIDER MANUAL Gilsbar www.gilsbar360alliance.com Dear Provider: Gilsbar is building a PPO network that gives providers and employers the opportunity to truly work together. We ve
SCHEDULE OF BENEFITS. Group LINK Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
benefit summary BAXTER COUNTY
 benefit summary BAXTER COUNTY benefit summary Effective Date: BAXTER COUNTY 01/01/2015 welcome Arkansas Blue Cross and Blue Shield is pleased to be your health insurance company. This Benefit Summary gives
benefit summary BAXTER COUNTY benefit summary Effective Date: BAXTER COUNTY 01/01/2015 welcome Arkansas Blue Cross and Blue Shield is pleased to be your health insurance company. This Benefit Summary gives
SCHEDULE OF BENEFITS. Group Access Care Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
Insurance Benefits For Employees C H E S T E R F I E L D C O U N T Y P U B L I C S C H O O L S
 CCPS Insurance Benefits For Employees 2015 C H E S T E R F I E L D C O U N T Y P U B L I C S C H O O L S CHESTERFIELD COUNTY PUBLIC SCHOOLS BENEFITS DEPARTMENT Enrollment or Changes in Coverage 748-1226,
CCPS Insurance Benefits For Employees 2015 C H E S T E R F I E L D C O U N T Y P U B L I C S C H O O L S CHESTERFIELD COUNTY PUBLIC SCHOOLS BENEFITS DEPARTMENT Enrollment or Changes in Coverage 748-1226,
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN
 SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN January 1, 2014-December 31, 2014 Call APS Healthcare Toll-Free: 1-877-239-1458 Customer Service for Hearing Impaired TTY: 1-877-334-0489
SUMMARY OF MARYLAND STATE EMPLOYEES & RETIREES BEHAVIORAL HEALTH PLAN January 1, 2014-December 31, 2014 Call APS Healthcare Toll-Free: 1-877-239-1458 Customer Service for Hearing Impaired TTY: 1-877-334-0489
Terms Defined. Participating/Non-Participating Provider. Benefits Coverage Charts. Prescription Drug Purchases. Pre-Authorization
 Medical Coverage Terms Defined Participating/Non-Participating Provider Benefits Coverage Charts Prescription Drug Purchases Section Two MEDICAL COVERAGE Pre-Authorization Coordination of Benefits Questions
Medical Coverage Terms Defined Participating/Non-Participating Provider Benefits Coverage Charts Prescription Drug Purchases Section Two MEDICAL COVERAGE Pre-Authorization Coordination of Benefits Questions
Consumer Guide to. Health Insurance. Oregon Insurance Division
 Consumer Guide to Health Insurance Oregon Insurance Division The Department of Consumer and Business Services, Oregon s largest business regulatory and consumer protection agency, produced this guide.
Consumer Guide to Health Insurance Oregon Insurance Division The Department of Consumer and Business Services, Oregon s largest business regulatory and consumer protection agency, produced this guide.
Surgical/ASC Claims Revenue Cycle Management: An Introduction to Our Processes and Protocols
 Surgical/ASC Claims Revenue Cycle Management: An Introduction to Our Processes and Protocols 200 Old Country Road, Suite 470 Mineola, NY 11501 Phone: 516-294-4118 Fax: 516-294-9268 www.businessdynamicslimited.com
Surgical/ASC Claims Revenue Cycle Management: An Introduction to Our Processes and Protocols 200 Old Country Road, Suite 470 Mineola, NY 11501 Phone: 516-294-4118 Fax: 516-294-9268 www.businessdynamicslimited.com
What Your Plan Covers and How Benefits are Paid BENEFIT PLAN. Prepared Exclusively for Vanderbilt University. Aetna Choice POS II Health Fund Plan
 BENEFIT PLAN Prepared Exclusively for Vanderbilt University What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Health Fund Plan Table of Contents Schedule of Benefits... Issued with Your
BENEFIT PLAN Prepared Exclusively for Vanderbilt University What Your Plan Covers and How Benefits are Paid Aetna Choice POS II Health Fund Plan Table of Contents Schedule of Benefits... Issued with Your
52ND LEGISLATURE - STATE OF NEW MEXICO - FIRST SESSION, 2015
 SENATE JUDICIARY COMMITTEE SUBSTITUTE FOR SENATE BILL ND LEGISLATURE - STATE OF NEW MEXICO - FIRST SESSION, AN ACT RELATING TO MANAGED HEALTH CARE; AMENDING AND ENACTING SECTIONS OF THE NEW MEXICO INSURANCE
SENATE JUDICIARY COMMITTEE SUBSTITUTE FOR SENATE BILL ND LEGISLATURE - STATE OF NEW MEXICO - FIRST SESSION, AN ACT RELATING TO MANAGED HEALTH CARE; AMENDING AND ENACTING SECTIONS OF THE NEW MEXICO INSURANCE
Retiree Considerations Medicare 101. June 26, 2012
 Retiree Considerations Medicare 101 June 26, 2012 Agenda Goal: Present information regarding Medicare and related products to assist you in evaluating options Key Topics: Eligibility Rules Enrollment Rules
Retiree Considerations Medicare 101 June 26, 2012 Agenda Goal: Present information regarding Medicare and related products to assist you in evaluating options Key Topics: Eligibility Rules Enrollment Rules
Benefit Coverage Chart & Rates
 Benefit Coverage Chart & Rates Effective July 1, 2014- June 30, 2015 PPO Medical Coverage by Category The following coverages are included with the PPO plan: o Prescription o Vision Additional Benefits
Benefit Coverage Chart & Rates Effective July 1, 2014- June 30, 2015 PPO Medical Coverage by Category The following coverages are included with the PPO plan: o Prescription o Vision Additional Benefits
Pharmacy Operating Guidelines & Information
 Pharmacy Operating Guidelines & Information RxAMERICA PHARMACY BENEFIT MANAGEMENT Pharmacy Operating Guidelines & Information Table of Contents I. Quick Reference List...3 C. D. E. Important Phone Numbers...
Pharmacy Operating Guidelines & Information RxAMERICA PHARMACY BENEFIT MANAGEMENT Pharmacy Operating Guidelines & Information Table of Contents I. Quick Reference List...3 C. D. E. Important Phone Numbers...
FUNDAMENTALS OF HEALTH INSURANCE: What Health Insurance Products Are Available?
 http://www.naic.org/ FUNDAMENTALS OF HEALTH INSURANCE: PURPOSE The purpose of this session is to acquaint the participants with the basic principles of health insurance, areas of health insurance regulation
http://www.naic.org/ FUNDAMENTALS OF HEALTH INSURANCE: PURPOSE The purpose of this session is to acquaint the participants with the basic principles of health insurance, areas of health insurance regulation
1) How does my provider network work with Sanford Health Plan?
 NDPERS FAQ Summary Non-Medicare Members Last Updated: 7/20/2015 PROVIDER NETWORK 1) How does my provider network work with Sanford Health Plan? Sanford Health Plan is offering you the same PPO network
NDPERS FAQ Summary Non-Medicare Members Last Updated: 7/20/2015 PROVIDER NETWORK 1) How does my provider network work with Sanford Health Plan? Sanford Health Plan is offering you the same PPO network
Medical and Rx Claims Procedures
 This section of the Stryker Benefits Summary describes the procedures for filing a claim for medical and prescription drug benefits and how to appeal denied claims. Medical and Rx Benefits In-Network Providers
This section of the Stryker Benefits Summary describes the procedures for filing a claim for medical and prescription drug benefits and how to appeal denied claims. Medical and Rx Benefits In-Network Providers
SECTION 4. A. Balance Billing Policies. B. Claim Form
 SECTION 4 Participating Physicians, hospitals and ancillary providers shall be entitled to payment for covered services that are provided to a DMC Care member. Payment is made at the established and prevailing
SECTION 4 Participating Physicians, hospitals and ancillary providers shall be entitled to payment for covered services that are provided to a DMC Care member. Payment is made at the established and prevailing
2014 Southcoast Health Plan Frequently Asked Questions
 2014 Southcoast Health Plan Frequently Asked Questions What does Southcoast Health Plan offer me? Southcoast Health Plan provides members with broad access to quality health care at an affordable price.
2014 Southcoast Health Plan Frequently Asked Questions What does Southcoast Health Plan offer me? Southcoast Health Plan provides members with broad access to quality health care at an affordable price.
Fee-for-Service. Medicare Supplemental Retiree Health Plans
 Sheet Metal Workers Health Plan of Southern California, Arizona & Nevada April 2011 Summary Comparison Of Benefits Available under the Fee-for-Service and Medicare Supplemental Retiree Health Plans Important:
Sheet Metal Workers Health Plan of Southern California, Arizona & Nevada April 2011 Summary Comparison Of Benefits Available under the Fee-for-Service and Medicare Supplemental Retiree Health Plans Important:
Patient Resource Guide for Billing and Insurance Information
 Patient Resource Guide for Billing and Insurance Information 17 Patient Account Payment Policies July 2012 Update Lexington Clinic Central Business Office Payment Policies Customer service...2 Check-in...2
Patient Resource Guide for Billing and Insurance Information 17 Patient Account Payment Policies July 2012 Update Lexington Clinic Central Business Office Payment Policies Customer service...2 Check-in...2
Kraft Foods Group, Inc. Retiree Medical and Prescription Plan Summary High Deductible Health Plan
 General Provisions Deductible (eligible medical and prescription drug expenses apply to the deductible) Kraft Foods Group, Inc. Retiree Medical and Prescription Plan Summary Care can be obtained in-network
General Provisions Deductible (eligible medical and prescription drug expenses apply to the deductible) Kraft Foods Group, Inc. Retiree Medical and Prescription Plan Summary Care can be obtained in-network
Banner Health - Choice Plus Coverage Period: 1/1/2015-12/31/2015
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan document at www.bannerbenefits.com by clicking on the Resources tab and then Plan
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan document at www.bannerbenefits.com by clicking on the Resources tab and then Plan
Health Alliance Plan. Coverage Period: 01/01/2015-12/31/2015. document at www.hap.org or by calling 1-800-422-4641.
 Health Alliance Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage for: Individual+Family Plan Type: HMO This is only a summary.
Health Alliance Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2015-12/31/2015 Coverage for: Individual+Family Plan Type: HMO This is only a summary.
Retiree Health Care Plan Benefits 2012 Enrollment Guide. Medical Coverage: Pre-Medicare Retirees
 Retiree Health Care Plan Benefits 2012 Enrollment Guide Medical Coverage: Pre-Medicare Retirees You ll choose from four medical plans: Basic, Comprehensive, Health Reimbursement Arrangement (HRA) and Health
Retiree Health Care Plan Benefits 2012 Enrollment Guide Medical Coverage: Pre-Medicare Retirees You ll choose from four medical plans: Basic, Comprehensive, Health Reimbursement Arrangement (HRA) and Health
Anthem Blue Cross: I have not seen 1 alpha prefix and request that you send an email to [email protected] with an example of this.
 QUESTION ANSWER 1 Caller: Will precert authorization be required for emergency ambulance or just hospital admissions? 2 Caller: Can we go over who will be considered the HOST Plan and who would be the
QUESTION ANSWER 1 Caller: Will precert authorization be required for emergency ambulance or just hospital admissions? 2 Caller: Can we go over who will be considered the HOST Plan and who would be the
Copayment: The amount you must pay for each medical visit to a participating doctor or other healthcare provider, usually at this time service.
 Basic Terms How to calculate Out of Pocket Costs on a Hospital Stay: If you have a $2000 deductible and 30% coinsurance health insurance plan. If you have a $10,000 emergency room or hospital stay your
Basic Terms How to calculate Out of Pocket Costs on a Hospital Stay: If you have a $2000 deductible and 30% coinsurance health insurance plan. If you have a $10,000 emergency room or hospital stay your
Boston College Student Blue PPO Plan Coverage Period: 2015-2016
 Boston College Student Blue PPO Plan Coverage Period: 2015-2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This is only a
Boston College Student Blue PPO Plan Coverage Period: 2015-2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This is only a
PHASE II CORE 260 ELIGIBILITY & BENEFITS (270/271) DATA CONTENT RULE VERSION 2.1.0 SECTION 6.2 APPENDIX 2: GLOSSARY OF DATA CONTENT TERMS MARCH 2011
 PHASE II CORE 260 ELIGIBILITY & BENEFITS (270/271) DATA CONTENT RULE VERSION 2.1.0 SECTION 6.2 APPENDIX 2: GLOSSARY OF DATA CONTENT TERMS MARCH 2011 CAQH 2008-2011. All rights reserved. 1 Table of Contents
PHASE II CORE 260 ELIGIBILITY & BENEFITS (270/271) DATA CONTENT RULE VERSION 2.1.0 SECTION 6.2 APPENDIX 2: GLOSSARY OF DATA CONTENT TERMS MARCH 2011 CAQH 2008-2011. All rights reserved. 1 Table of Contents
Health Insurance. INSURANCE FACTS for Pennsylvania Consumers. A Consumer s Guide to. 1-877-881-6388 Toll-free Automated Consumer Line
 INSURANCE FACTS for Pennsylvania Consumers A Consumer s Guide to Health Insurance 1-877-881-6388 Toll-free Automated Consumer Line www.insurance.pa.gov Pennsylvania Insurance Department Website Increases
INSURANCE FACTS for Pennsylvania Consumers A Consumer s Guide to Health Insurance 1-877-881-6388 Toll-free Automated Consumer Line www.insurance.pa.gov Pennsylvania Insurance Department Website Increases
You asked. We answered. 35 things you didn t know about your health plan.
 You asked. We answered. 35 things you didn t know about your health plan. Make the Most of Your Healthcare Coverage At Oxford Health Plans, we believe that helping you understand your healthcare coverage
You asked. We answered. 35 things you didn t know about your health plan. Make the Most of Your Healthcare Coverage At Oxford Health Plans, we believe that helping you understand your healthcare coverage
PHARMACY MANUAL. WHP Health Initiatives, Inc. 2275 Half Day Road, Suite 250 Bannockburn, IL 60015
 PHARMACY MANUAL WHP Health Initiatives, Inc. 2275 Half Day Road, Suite 250 Bannockburn, IL 60015 Welcome WHP Health Initiatives, Inc. ( WHI ) is pleased to welcome you to our network of participating pharmacies.
PHARMACY MANUAL WHP Health Initiatives, Inc. 2275 Half Day Road, Suite 250 Bannockburn, IL 60015 Welcome WHP Health Initiatives, Inc. ( WHI ) is pleased to welcome you to our network of participating pharmacies.
How To Compare A Small Group Plan In Massachusetts
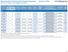 Non- ER Medical Individual/ Family HMO Value 250 $15 $100 $250 $100 No 26% Basic 25 $25 $125 $500 $100 No $2,500/$5,000 17% 500 after after after $500/$1,000 8% 1000 after after after 1 (baseline) * after
Non- ER Medical Individual/ Family HMO Value 250 $15 $100 $250 $100 No 26% Basic 25 $25 $125 $500 $100 No $2,500/$5,000 17% 500 after after after $500/$1,000 8% 1000 after after after 1 (baseline) * after
Blue Care Elect Saver with Coinsurance Northeastern University HDHP Coverage Period: on or after 01/01/2016
 Blue Care Elect Saver with Coinsurance Northeastern University HDHP Coverage Period: on or after 01/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual
Blue Care Elect Saver with Coinsurance Northeastern University HDHP Coverage Period: on or after 01/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual
Frequently Asked Questions For Middlesex Community College Students 2013-2014 Student Health Insurance Plan
 Frequently Asked Questions For Middlesex Community College Students 2013-2014 Student Health Insurance Plan Table of Contents Important Contact Information... 2 I have questions about what is covered,
Frequently Asked Questions For Middlesex Community College Students 2013-2014 Student Health Insurance Plan Table of Contents Important Contact Information... 2 I have questions about what is covered,
Medical Plan Comparison
 For Agent Use Only Medical Plan Comparison Flexible Plan Designs, Lower-Cost Alternatives As an expert in small group healthcare benefits, Starmark provides businesses with two to 50 employees a broad
For Agent Use Only Medical Plan Comparison Flexible Plan Designs, Lower-Cost Alternatives As an expert in small group healthcare benefits, Starmark provides businesses with two to 50 employees a broad
Health Plan Comparison
 A healthier bottom line. For Agent Use Only Starmark Healthy Incentives Health Plan Comparison Self-Funded Health Plans Specifically for Businesses With Five or More Employees PPO Indemnity CDHP PPO CDHP
A healthier bottom line. For Agent Use Only Starmark Healthy Incentives Health Plan Comparison Self-Funded Health Plans Specifically for Businesses With Five or More Employees PPO Indemnity CDHP PPO CDHP
ILWU California Locals 10,13,18, 26, 29, 34, 34-A, 46, 54, 63, 75, 91 and 94 ILWU Oregon Locals 4, 8, 40, and 92
 May 26, 2010 To: From: Subject: ILWU California Locals 10,13,18, 26, 29, 34, 34-A, 46, 54, 63, 75, 91 and 94 ILWU Oregon Locals 4, 8, 40, and 92 Elizabeth Sharpe, Manager, Welfare Plans Kaiser Permanente
May 26, 2010 To: From: Subject: ILWU California Locals 10,13,18, 26, 29, 34, 34-A, 46, 54, 63, 75, 91 and 94 ILWU Oregon Locals 4, 8, 40, and 92 Elizabeth Sharpe, Manager, Welfare Plans Kaiser Permanente
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Prepared Exclusively for Cerner Corporation (Expatriate Employees)
 BENEFIT PLAN Prepared Exclusively for Cerner Corporation (Expatriate Employees) What Your Plan Covers and How Benefits are Paid PPO Medical, PPO Dental, Basic Vision and Pharmacy Aetna Life and Casualty
BENEFIT PLAN Prepared Exclusively for Cerner Corporation (Expatriate Employees) What Your Plan Covers and How Benefits are Paid PPO Medical, PPO Dental, Basic Vision and Pharmacy Aetna Life and Casualty
Name of Company: Contact Name: Address: Telephone Number: Fax Number: Email:
 DEFIANCE COUNTY REQUEST FOR PROPOSALS (RFP) ON-SITE CLINICAL SERVICES (On-site physician clinic which shall provide primary care, including episodic and preventive care; health risk assessments to adult
DEFIANCE COUNTY REQUEST FOR PROPOSALS (RFP) ON-SITE CLINICAL SERVICES (On-site physician clinic which shall provide primary care, including episodic and preventive care; health risk assessments to adult
Pace University CIGNA Medical Detailed Benefit Summaries July 1, 2015 - June 30, 2016
 Consumer Core HDHP In Net $50 (ONLY APPLICABLE TO THOSE Network Core $25 ALREADY ENROLLED) Network Choice Fund In Network In Network In Network Deductible $1,300/$2,600 (Cumulative) N/A N/A Coinsurance
Consumer Core HDHP In Net $50 (ONLY APPLICABLE TO THOSE Network Core $25 ALREADY ENROLLED) Network Choice Fund In Network In Network In Network Deductible $1,300/$2,600 (Cumulative) N/A N/A Coinsurance
How To Pay For Health Care With Bluecrossma
 PPO Student/Affiliate Plan MIT Student/Affiliate Extended Insurance Plan Coverage Period: 2014-2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual, Couple,
PPO Student/Affiliate Plan MIT Student/Affiliate Extended Insurance Plan Coverage Period: 2014-2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual, Couple,
In-network: $5,000 per insured/ $10,000 per family per calendar year. Out-of-network: $10,000 per insured / $20,000
 Regence BlueShield of Idaho: Coverage Period: Beginning on or after 01/01/2014 Regence Individual Direct Bronze HSA Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for:
Regence BlueShield of Idaho: Coverage Period: Beginning on or after 01/01/2014 Regence Individual Direct Bronze HSA Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for:
Even though you pay these expenses, they don t count toward the out-ofpocket limit.
 Commonwealth of Virginia: COVA Care Basic Coverage Period: 07/01/2014 06/30/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO This
Commonwealth of Virginia: COVA Care Basic Coverage Period: 07/01/2014 06/30/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO This
Massachusetts. Coverage Period: 1/1/2015 12/31/2015
 Massachusetts The Harvard Pilgrim Hospital Prefer Best Buy Tiered Copayment HMO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 1/1/2015 12/31/2015 Coverage for:
Massachusetts The Harvard Pilgrim Hospital Prefer Best Buy Tiered Copayment HMO Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 1/1/2015 12/31/2015 Coverage for:
how to choose the health plan that s right for you
 how to choose the health plan that s right for you It s easy to feel a little confused about where to start when choosing a health plan. Some people ask their friends, family, or co-workers for advice.
how to choose the health plan that s right for you It s easy to feel a little confused about where to start when choosing a health plan. Some people ask their friends, family, or co-workers for advice.
Table of Contents. Transmittal Letter...2. Background... 3-4. Objectives and Approach... 5-6. TPA Claim Audit Results... 7-23
 Audit Committee of Brevard County Self Insurance Claims Audit Prepared By: Bray, Beck & Koetter, CPAs P.A. November 30, 2001 Table of Contents Transmittal Letter...2 Background... 3-4 Objectives and Approach...
Audit Committee of Brevard County Self Insurance Claims Audit Prepared By: Bray, Beck & Koetter, CPAs P.A. November 30, 2001 Table of Contents Transmittal Letter...2 Background... 3-4 Objectives and Approach...
Horizon MyWay HSA Horizon Direct Access 100/80/60 Benefit Highlights *
 Horizon MyWay HSA Horizon Direct Access 100/80/60 Benefit Highlights * Office Visit Maximum Out of Pocket Plan** Copayment Deductible Network Non-Network Option 1 Not applicable $1,500 $3,500 $5,250 Option
Horizon MyWay HSA Horizon Direct Access 100/80/60 Benefit Highlights * Office Visit Maximum Out of Pocket Plan** Copayment Deductible Network Non-Network Option 1 Not applicable $1,500 $3,500 $5,250 Option
BridgeSpan Health Company: BridgeSpan Oregon Standard Gold Plan MyChoice Northwest
 BridgeSpan Health Company: BridgeSpan Oregon Standard Gold Plan MyChoice Northwest Summary of Benefits and Coverage: What this Plan Covers & What it Costs Questions: Call 1 (855) 857-9943 or visit us at
BridgeSpan Health Company: BridgeSpan Oregon Standard Gold Plan MyChoice Northwest Summary of Benefits and Coverage: What this Plan Covers & What it Costs Questions: Call 1 (855) 857-9943 or visit us at
Open Enrollment 2015 November 12 November 26
 Open Enrollment 2015 November 12 November 26 November 4 & 6, 2014 1 Brief Review of Affordable Care Act (ACA) What You Need to Know What you Need to do by November 26 What s New or Changing in 2015 Do
Open Enrollment 2015 November 12 November 26 November 4 & 6, 2014 1 Brief Review of Affordable Care Act (ACA) What You Need to Know What you Need to do by November 26 What s New or Changing in 2015 Do
Questionnaire/Compliance Form for COBRA Administration
 Form for COBRA Administration Questionnaire/Compliance 1. General Information 1.1 Total number of employees in your company. 1.2 Your company shall submit renewal fees to the district no later than February
Form for COBRA Administration Questionnaire/Compliance 1. General Information 1.1 Total number of employees in your company. 1.2 Your company shall submit renewal fees to the district no later than February
Medical Insurance Guide
 1 of 12 11-11-20 8:17 AM Medical Insurance Guide Medical Necessity form Frequently Asked Questions Glossary of Insurance Terminology Suggestions for contacting your health plan Links to Major Health Insurance
1 of 12 11-11-20 8:17 AM Medical Insurance Guide Medical Necessity form Frequently Asked Questions Glossary of Insurance Terminology Suggestions for contacting your health plan Links to Major Health Insurance
Flexible. The. benefits plan YOUR HEALTH CARE ADVANTAGE SPD. Summary Plan Description
 The Flexible benefits plan YOUR HEALTH CARE ADVANTAGE SPD Summary Plan Description Table of Contents Overview of the Plan................................................ 1 Eligibility...........................................................
The Flexible benefits plan YOUR HEALTH CARE ADVANTAGE SPD Summary Plan Description Table of Contents Overview of the Plan................................................ 1 Eligibility...........................................................
Graduate Student Insurance Comparison Summary Student Insurance Plan vs. Employer Group Insurance Program
 Graduate Student Insurance Comparison Summary Student Insurance Plan vs. Employer Group Insurance Program Revised 08/20/2015 Graduate Student employees may choose between the Student Insurance Plan administered
Graduate Student Insurance Comparison Summary Student Insurance Plan vs. Employer Group Insurance Program Revised 08/20/2015 Graduate Student employees may choose between the Student Insurance Plan administered
Parent to Parent of NYS Family to Family Health Care Information and Education Center
 Parent to Parent of NYS Family to Family Health Care Information and Education Center September 2005 With funding from Parent to Parent of New York State s Real Choice Systems Change Grant, this publication
Parent to Parent of NYS Family to Family Health Care Information and Education Center September 2005 With funding from Parent to Parent of New York State s Real Choice Systems Change Grant, this publication
OPERATING ENGINEERS HEALTH & WELFARE FUND BENEFIT PLANS SUMMARY COMPARISON FOR ACTIVE and RETIRED PARTICIPANTS
 Employee Premium None None None None None Explanation of Plans and Options Available to You Deductible Annual Out-of-Pocket Calendar Year (Applicable to members who reside in California & Nevada Only.)
Employee Premium None None None None None Explanation of Plans and Options Available to You Deductible Annual Out-of-Pocket Calendar Year (Applicable to members who reside in California & Nevada Only.)
Frequently Asked Questions. High Deductible Health Plan (HDHP) with Health Savings Account (HSA)
 Frequently Asked Questions High Deductible Health Plan (HDHP) with Health Savings Account (HSA) There are two components to the High Deductible Health Plan (HDHP) with HSA Medical Plan the HDHP Health
Frequently Asked Questions High Deductible Health Plan (HDHP) with Health Savings Account (HSA) There are two components to the High Deductible Health Plan (HDHP) with HSA Medical Plan the HDHP Health
Blue Care Elect Preferred 90 Copay Coverage Period: on or after 09/01/2015
 Blue Care Elect Preferred 90 Copay Coverage Period: on or after 09/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Only Plan Type: PPO This is only
Blue Care Elect Preferred 90 Copay Coverage Period: on or after 09/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Only Plan Type: PPO This is only
!"#$%$&!"'()*+,-".-,/ &01*+("12"31+4156"$,+0"!*7("819".5(<(/4*<("&,5( :(()";(,-40"&,5( !"#$%$&!",/)"'()*+,5(
 submitted anytime during the year to your institution HR/Benefits Office, and the tobacco premium will be waived beginning the first of the month following submission of the form. Important: A member is
submitted anytime during the year to your institution HR/Benefits Office, and the tobacco premium will be waived beginning the first of the month following submission of the form. Important: A member is
classic ppo evidence of coverage handbook
 classic ppo evidence of coverage handbook WELCOME TO LOVELACE INSURANCE COMPANY Lovelace Insurance Company is a Health Care Insurer organized under the applicable laws of the State of New Mexico and is
classic ppo evidence of coverage handbook WELCOME TO LOVELACE INSURANCE COMPANY Lovelace Insurance Company is a Health Care Insurer organized under the applicable laws of the State of New Mexico and is
NYU HOSPITALS CENTER. Retirement Plan. Your Health & Welfare Plan Benefits
 NYU HOSPITALS CENTER Retirement Plan Your Health & Welfare Plan Benefits 1 What s Inside Welcome to the NYU Hospitals Center Retiree Health & Welfare Program Retiree Health & Welfare Benefits At-A-Glance...
NYU HOSPITALS CENTER Retirement Plan Your Health & Welfare Plan Benefits 1 What s Inside Welcome to the NYU Hospitals Center Retiree Health & Welfare Program Retiree Health & Welfare Benefits At-A-Glance...
