Widespread Tau and Amyloid-Beta Pathology Many Years After a Single Traumatic Brain Injury in Humans
|
|
|
- Thomasina Anthony
- 8 years ago
- Views:
Transcription
1 Brain Pathology ISSN RESEARCH ARTICLE bpa_ Widespread Tau and Amyloid-Beta Pathology Many Years After a Single Traumatic Brain Injury in Humans Victoria E. Johnson, MBChB 1,2 ; William Stewart, MBChB, PhD 2,3 *; Douglas H. Smith, MD 1 * 1 Penn Center for Brain Injury and Repair and Department of Neurosurgery, University of Pennsylvania, Philadelphia, Pa. 2 Division of Clinical Neurosciences, University of Glasgow. 3 Department of Neuropathology, Institute of Neurological Sciences, Southern General Hospital, Glasgow, UK. Keywords amyloid beta plaques, head injury, long-term survival, neurodegeneration, neurofibrillary tangles, traumatic brain injury. Corresponding author: Douglas H. Smith, MD, Department of Neurosurgery, 105 Hayden Hall, 3320 Smith Walk, University of Pennsylvania, Philadelphia, PA ( smithdou@ mail.med.upenn.edu) Received 23 November 2010; accepted 31 May * These authors have contributed equally to this article. doi: /j x Abstract While a history of a single traumatic brain injury (TBI) is associated with the later development of syndromes of cognitive impairment such as Alzheimer s disease, the long-term pathology evolving after single TBI is poorly understood. However, a progressive tauopathy, chronic traumatic encephalopathy, is described in selected cohorts with a history of repetitive concussive/mild head injury. Here, post-mortem brains from long-term survivors of just a single TBI (1 47 years survival; n = 39) vs. uninjured, age-matched controls (n = 47) were examined for neurofibrillary tangles (NFTs) and amyloid-b (Ab) plaques using immunohistochemistry and thioflavine-s staining. Detailed maps of findings permitted classification of pathology using semiquantitative scoring systems. NFTs were exceptionally rare in young, uninjured controls, yet were abundant and widely distributed in approximately one-third of TBI cases. In addition, Ab-plaques were found in a greater density following TBI vs. controls. Moreover, thioflavine-s staining revealed that while all plaque-positive control cases displayed predominantly diffuse plaques, 64% of plaque-positive TBI cases displayed predominantly thioflavine-s-positive plaques or a mixed thioflavine-s-positive/diffuse pattern. These data demonstrate that widespread NFT and Ab plaque pathologies are present in up to a third of patients following survival of a year or more from a single TBI. This suggests that a single TBI induces long-term neuropathological changes akin to those found in neurodegenerative disease. INTRODUCTION Representing a major health issue, 1.7 million people in the United States suffer a traumatic brain injury (TBI) each year (9). In addition to the acute effects, there is growing concern that a single TBI may initiate long-term processes that further damage the brain (20). Indeed, in epidemiological studies, TBI is recognized as a major risk factor for the later development of syndromes of cognitive impairment, such as Alzheimer s disease (AD) (14, 16, 26 28, 30, 33, 38, 39). While a long-term pathological link between a single TBI and neurodegenerative disease has not been identified, a tau pathology, currently referred to as chronic traumatic encephalopathy (CTE; formerly dementia pugilistica), has been described in the brains of individuals exposed to repetitive, often mild or concussive, head injury such as boxers (7, 8, 10, 35, 43) and, more recently, professional American football players (23, 24, 31, 32). In contrast, thus far, neurofibrillary tangles (NFTs) have not been identified following a single TBI in humans; although the only study examining this was limited to patients dying within 4 weeks of injury (40). Thus, it remains unclear whether tau pathology may appear as a late phenomenon following a single TBI or if it is a manifestation unique to repetitive injury. In contrast to NFTs, amyloid-beta (Ab) plaques, a hallmark pathology of AD, have been identified following a single TBI in approximately 30% of patients (6, 18, 19, 36, 37, 41, 45). Notably, plaques found acutely following TBI are typically diffuse in nature and in contrast to the thioflavine-s-positive neuritic plaques characteristic of advanced AD. While similarly diffuse plaques can be observed as part of so called normal aging (12, 34, 37, 44), TBI appears capable of inducing diffuse plaque formation within hours of injury, even in children (13, 19, 37). However, few plaques are observed following survival of several months from injury (6), perhaps indicating that the plaques observed initially following TBI may be a limited acute phase response. Alternatively, it is possible that increased severity of injury associated with early mortality is an important determinant of plaque pathology. Nonetheless, as with tau pathologies, Ab plaques have not been evaluated years after a single TBI. METHODS We examined the brains of long-term survivors (1 47 years) following a single TBI to evaluate the presence of NFTs and Ab-plaques. Brains were selected from the comprehensive TBI brain archive of the Department of Neuropathology, Southern 142 Brain Pathology 22 (2012)
2 Johnson et al Long-Term AD-Like Pathology after Single TBI Table 1. Demographic and clinical data for cases. Abbreviations: PM = post-mortem; TBI = traumatic brain injury; SUDEP = sudden unexpected death in epilepsy; GI = gastrointestinal; ARDS = acute respiratory distress syndrome; GSW = gun shot wound; MVC = motor vehicle collision; * = 3 unknown. TBI cases (n = 39) Controls (n = 47) Mean age (Range) (Years) 53 (19 89) 47 (14 92) Males 35 (89.7%) 30 (64.8%) Mean PM delay (Range) (Hours) 64 (12 184)* 57 (5 264) Mean survival interval (Range) (Years) 8.2 (1 47) Not applicable Cause of TBI Assault 8 (20.5%) Not applicable: controls had no known history of TBI Fall 16 (41.0%) MVC 8 (20.5%) Unknown 7 (17.9%) Cause of death Pulmonary (Including pneumonia) 9 (23.1%) SUDEP 14 (29.8%) Chronic heart failure 6 (15.4%) Pulmonary (Including pneumonia) 9 (19.1%) SUDEP 6 (15.4%) Acute cardiovascular 7 (14.9%) Acute cardiovascular 4 (10.3%) Drug overdose 4 (8.5%) GI disease (Including liver failure) 3 (7.7%) Chronic heart failure 4 (8.5%) Renal disease (Including pyelonephritis) 3 (7.7%) Sepsis 2 (4.3%) Unknown 3 (7.7%) Malignancy 2 (4.3%) Malignancy 2 (5.1%) Hypothermia 1 (2.1%) Acute intracerebral hemorrhage 1 (2.6%) Vasculitis 1 (2.1%) ARDS 1 (2.6%) GSW chest 1 (2.1%) Hypothermia 1 (2.6%) GI disease (Including liver failure) 1 (2.1%) Myasthenia gravis 1 (2.1%) General Hospital, Glasgow, UK. Approval for the use of tissue was granted by the South Glasgow and Clyde Research Ethics Committee. Cases were selected with a history of a single TBI (n = 39) and were compared to age-matched controls (n = 47). Detailed reports from the diagnostic post-mortem and/or forensic reports were available for all cases and confirmed a history of a single moderate to severe TBI, which was confirmed at diagnostic post-mortem. Following a single TBI, all cases were discharged from hospitalization following recovery and, ultimately, died from causes of death unrelated to TBI or trauma. None were in a persistent vegetative state prior to death. Cases with a history of amateur or professional boxing were excluded. From the same archive, age-matched controls were selected with no documented history of neurological disease, neurodegenerative disease or TBI, and no autopsy evidence to support previous TBI (Table 1). All material was obtained following routine diagnostic autopsy examination at the same institution serving a distinct regional location. Brain tissue preparation Whole brains were immersion fixed in 10% formol saline for a minimum of 3 weeks then dissected, sampled following a standardized block selection protocol and processed to paraffin using standard techniques. Three blocks from the coronal plane at midthalamic level were selected to include: (i) hippocampus at the level of the lateral geniculate nucleus extending through the entorhinal cortex including the inferior temporal gyrus; (ii) corpus callosum and cingulate gyrus; and (iii) insula. Regions of analysis were standardized based on the hypothesis that TBI is capable of inducing widespread neuropathological changes long-term following injury, regardless of the location of any focal lesion. Specific regions were selected based on previous published observations of acute plaque formation following injury and brain regions with known vulnerability in both TBI and neurodegenerative disorders. Immunohistochemistry Following deparaffinization and rehydration to dh 2O, sections were immersed in 3% aqueous H 2O 2 (10 minutes) to quench endogenous peroxidase activity. Antigen retrieval on all sections (8 mm) was performed via microwave. Additional antigen retrieval for Ab staining included 5 minutes immersion in 77% formic acid. Blocking was then performed using one drop of normal horse serum (Vector Labs, Burlingame, CA, USA) per 5 ml of Optimax buffer (BioGenex, San Ramon, CA, USA) for 30 minutes. Incubation with the primary antibody was then performed for 20 h at 4 C. Immunostaining for tau was performed with a polyclonal antibody (Dako, Carpinteria, CA, USA; 1:7500) and for Ab, the antibody 6F3D specific for the N-terminal epitope of the peptide was used (Dako; 1:500). Visualization was achieved using a DAB kit (Vector Labs) and sections analyzed using a Leica DMRB light microscope (Leica Microsystems, Wetzlar, Germany). Thioflavine-S staining To identify beta-pleated sheet conformations of tau and Ab, a modified thioflavine-s staining technique was performed (15). Briefly, 8-mm sections of tissue were deparaffinized, rehydrated to dh 2O and immersed in phosphate-buffered saline (PBS) for 5 minutes. Sections were then immersed in 0.05% KMnO 4 in PBS for 20 minutes. Following rinsing, tissue was destained in 0.2% K 2S 2O 5/0.2% Oxalic acid/pbs and subsequently immersed in Brain Pathology 22 (2012)
3 Long-Term AD-Like Pathology after Single TBI Johnson et al % thioflavine-s (Sigma-Aldrich, St Louis, MO, USA; in 40% EtOH/60% PBS). Tissue was then differentiated in 50% EtOH/50% PBS. Following rinsing, sections were cover-slipped using a fluorescence mounting medium (Dako) and analyzed using a Leitz Laberlux-K microscope (Leica Microsystems, Wetzlar, Germany) using a fluorescein isothiocyanate filter. Pathological classification of findings Observations were conducted blind to the demographic and clinical information for all cases. Detailed maps of NFTs and plaques were generated for each region to classify each case in accordance with standardized scoring systems. NFTs NFTs revealed by tau immunohistochemistry were semiquantitatively assessed and classified based on their extent and distribution. Group 1 pathology comprised cases with NFTs of sparse to moderate density in the transentorhinal cortex with or without small numbers in the CA1 sector of the hippocampus. Group 2 pathology included NFTs as described in Group 1 together with NFTs extending into the fusiform gyrus (lateral to entorhinal cortex) and sparse tangles in the isocortex (cingulate/insular blocks). Group 3 pathology contained NFTs in more widespread sectors of the hippocampus and subiculum and with extensive isocortical involvement. Ab plaques Semiquantitative assessments of age-adjusted plaque density were generated based on the mean plaque score across the three regions assessed. Thus, using standard protocols for assessment of plaque density with respect to age (25), sections with no (0), sparse (1), moderate (2) and frequent (3) plaques were identified. Statistical analysis Statistical analysis comparing cohorts for the presence of pathology was performed using the chi-square test. Figure 1. Representative immunohistochemical and thioflavine-s staining for neurofibrillary tangles (NFTs). A. NFTs in the parahippocampal gyrus of a 49-year-old male 1 year post-traumatic brain injury (TBI). B. Representative thioflavine- S-positive staining in the same case as A. C. NFTs in the fusiform gyrus of a 27-year-old male 1.5 years after TBI. D. NFTs in the frontal lobe of a case of advanced Alzheimer s disease (positive control). E, G. Representative images showing prevalent NFTs in the superficial layers of the cortex of the medial temporal lobe. F. Extensive neuropil threads and occasional NFTs in a 53-year-old individual who died 8 years following TBI. H, I. Representative images showing isolated clusters of NFTs within the depth of sulci. J. Uninjured control case displaying no neurons positive for tau immunostaining in the hippocampal region CA1. All scale bars approximately 100 mm. 144 Brain Pathology 22 (2012)
4 Johnson et al Long-Term AD-Like Pathology after Single TBI RESULTS NFT pathology NFT pathology was observed more widely across the age spectrum following TBI than in controls, being present in cases aged as young as 27 years (Figures 1 and 2A). In addition, NFTs were more common following TBI, with 18 of 39 (46%) cases containing tangles compared with 16 of 47 (34%) controls (Figure 2A); although in assessing the full cohort, including material from individuals at all ages, this difference did not reach statistical significance. However, in comparison with TBI cases, virtually all the controls displaying NFT pathology were aged over 60 years. As such, when material from patients aged greater than 60 is excluded from analysis, a clear difference is observed in the presence of NFTs following TBI vs. controls. Specifically, 11 of the 32 (34%) TBI cases aged 60 years or younger displayed NFT pathology compared with just three of the 32 (9%) controls (P = 0.015; chisquare) (Figure 2A). Of these three control cases, two were aged 60 and one was aged 55. Notably, following TBI, NFTs were commonly observed in the superficial cortical layers, with clustering of NFTs among the depths of the sulci and at points of geometric inflection. Indeed, following TBI, well-defined clusters of NFTs could be found in the cingulate gyrus extending through the superior frontal gyrus and also within the insular cortex. This pattern was not observed in controls who rarely displayed pathology outside the transentorhinal cortex and CA1. In addition, in those cases with NFTs, glia immunoreactive for tau could also be observed following TBI and, to a lesser extent, in control cases, although these were not independently quantified. The distribution of NFTs in both TBI cases and controls permitted classification using a semiquantitative protocol reflecting the density and distribution of tau pathology. Following TBI, cases displayed more extensive pathology than controls (Figure 2B). Specifically six of 18 (33%) cases met the criteria for Group 1, with tangles in the transentorhinal cortex and CA1 of hippocampus; eight of 18 (44%) were Group 2, with NFTs in the same regions as Group 1, but with extension into the fusiform gyrus; the remaining four of 18 (22%) were Group 3, with NFTs more widespread in the hippocampus and subiculum and with more extensive isocortical involvement. In comparison, the distribution of NFTs in controls was consistent with the published literature for so called normal aging (34, 44), with 13 of the 16 (81%) controls with NFTs displaying Group 1 pathology, two cases (13%) with Group 2 pathology and just a single example displaying Group 3 pathology. Thus, in addition to being more prevalent at an earlier age, the extent and distribution of NFTs, as assessed by this semiquantitative protocol, is significantly greater in material from individuals surviving a year or more post-tbi than in controls (P = 0.019; chi-square). Figure 2. Graphical representation of findings regarding neurofibrillary tangles (NFTs). A. Percentage of cases with NFTs in entire cohort/cohort with those aged >60 excluded: traumatic brain injury (TBI) vs. controls. B. Extent and distribution of NFTs in TBI positive cases vs. controls by pathological group. Group 1 (minimal pathology): NFTs of sparse to moderate density in the transentorhinal cortex with or without small numbers in the CA1 sector of the hippocampus. Group 2 (moderate pathology): as described in Group 1, together with NFTs extending into the fusiform gyrus (lateral to entorhinal cortex) and sparse tangles in the isocortex (cingulate/insular blocks). Group 3 (extensive pathology): NFTs in more widespread sectors of the hippocampus and subiculum and with extensive isocortical involvement. Ab plaque pathology Ab plaques were observed in 13 of 47 (28%) controls vs. 11 of 39 (28%) TBI cases (Figure 3). While the incidence of plaque pathology was not statistically different between controls and TBI cases, the extent of plaques differed greatly. Specifically, following TBI, age-adjusted plaque density was moderate (27%; three of 11 cases) or, more commonly, high (73%; eight of 11 cases), whereas in controls 31% (four of 13 cases) had sparse plaque, 31% (four of 13 cases) moderate and just 38% (five of 13 cases) high (Figure 4A). While this observation failed to reach statistical significance (P = 0.095; chi-square), there is a clear trend to a wider distribution and a higher density of Ab plaques (either diffuse or thioflavine-spositive) following survival from TBI. Brain Pathology 22 (2012)
5 Long-Term AD-Like Pathology after Single TBI Johnson et al Figure 3. Representative immunohistochemical and thioflavine-s staining for amyloid-beta (Ab) plaques. A. Plaques in the inferior temporal gyrus of a 55-year-old female 47 years post- traumatic brain injury. B. Representative thioflavine- S-positive staining in the same cases as A. C. Plaques in the frontal lobe of a case of advanced Alzheimer s disease. D. Uninjured control displaying no Ab immunostaining. All scale bars approximately 50 mm. Typically cases could broadly be described as having either (i) widespread and relatively evenly distributed plaques dispersed throughout all layers of the cortex vs. (ii) isolated clusters of plaques scattered throughout the cortex with interspersed, plaquefree regions. Typically, following TBI, cases were less likely to display smaller clustered regions of plaques and more likely to have widespread plaques across the entire cortical region examined. This was particularly true extending from the cingulate gyrus through the superior frontal gyrus, which frequently displayed extensive and widespread pathology after TBI. However, while plaques could often be observed in the entorhinal cortex, throughout the fusiform gyrus and the inferior temporal gyrus, there were comparatively minimal plaques in the hippocampus and subiculum. Cases demonstrating involvement of the hippocampus and subiculum universally displayed extensive plaque pathology throughout all other regions analyzed, potentially indicating a relative sparing of this region in early disease. In addition to an increased density of plaques revealed by immunohistochemistry, thioflavine-s staining revealed that the nature of Ab plaques following TBI also differed from controls. Specifically, while all 13 of the controls with Ab plaques displayed predominantly diffuse plaques with very occasional, isolated fibrillar plaques, in seven of the 11 (64%) plaque-positive TBI cases, plaques were predominantly fibrillar in nature or displayed a mixed diffuse/fibrillar pattern (P = 0.003; chi-square) (Figure 4B). DISCUSSION This study demonstrates that NFTs are present at a higher density and in a wider distribution in brains of patients surviving greater than 1 year following just a single TBI when compared with agematched controls from the same archive. Similarly, there is evidence of more extensive Ab plaque pathology, often fibrillary in nature, in survivors of TBI. These observations raise the intriguing possibility that the pathological mechanisms leading to neurodegenerative disease may be initiated or accelerated as part of the chronic pathological milieu following survival post-tbi, with the pathology emerging even in young adults. Although a previous study failed to find NFTs following a single TBI, analysis was limited to within 4 weeks of injury (40). By extending the examination to years after injury, the present data demonstrate that NFTs can indeed emerge following just a single TBI. Appearing in over 30% of individuals aged less than 60 years, NFTs were often regionally widespread and extensive. This finding is in contrast to the minimal pathology observed in controls. Indeed, NFTs observed in the control group were almost exclusively observed in cases aged 60 or greater at a frequency highly consistent with a large cohort of 2661 nonselected autopsy cases reported by Braak and Braak (3). Specifically, according to this large data set, 91.6% of cases over the age of 60 displayed NFT pathology to some extent. For the control group presented here, this number is 91.2% indicating a high level of consistency with the largest series in the literature. Only one control case aged less than 60 (age 55) was determined to have NFTs, which again is consistent with the comprehensive data by Braak and Braak (3). In contrast, following survival of a year or more from a moderate to severe TBI, NFTs were observed in autopsy-derived brain material from individuals dying in their third to fourth decade. The apparent delayed appearance of NFTs after trauma suggests that even a single TBI may, in the long term, be associated with a neurodegenerative process. Moreover, this finding provides a potential pathological substrate for the epidemiological observation of an increased risk of developing syndromes of cognitive impairment, such as AD, following TBI (14, 16, 26 28, 30, 33, 38, 39). A similar tau pathology has been observed in autopsy-acquired brains from athletes involved in contact sports, thought to be a consequence of repetitive TBI (7, 8, 10, 23, 31, 32, 35, 43). NFTs observed in the current, relatively large cohort of patients following a single moderate/severe TBI suggest tau pathology may not be exclusive to situations where there is a history of repetitive injury. 146 Brain Pathology 22 (2012)
6 Johnson et al Long-Term AD-Like Pathology after Single TBI Figure 4. Graphical representation of findings regarding amyloid-beta plaques. A. Age-adjusted plaque density in plaque-positive traumatic brain injury (TBI) cases (11 of 39; 28%) vs. controls (13 of 47; 28%). B. Percentage of plaque-positive cases displaying thioflavine-s-positive staining in TBI cases vs. controls. Of note, although cases with a known history of repetitive injury, such as boxing, were excluded, it is difficult to determine with complete certainty whether any of the cases within this study experienced repeat head injury because of the retrospective nature of the archive and available clinical information. However, a large age and demographically matched control group for which tissue was accrued at the same institution was included for comparison and failed to display pathology at the same frequency or extent. The observation of NFTs in relatively young individuals long after just a single TBI supports epidemiological studies suggesting that TBI may act to accelerate the clinical onset of neurodegenerative disease (11, 29, 39, 42). Notably, analysis of over 1200 TBI survivors demonstrated that the time to onset of AD was significantly reduced in those who sustained TBI (29). The median time to onset from TBI to the development of AD in that cohort was 10 years a finding that is consistent with the NFTs encountered post-tbi in this study. The regional distribution of NFTs observed post-trauma follows a similar hierarchical progression to that of AD (1, 2). However, in AD, the deep cortical layers are predominantly affected (2), whereas in CTE it is the superficial layers (17). While NFT pathology in our cohort was not uniformly superficial, this was a common finding, possibly indicating a pattern of tau pathology specific to trauma and common to both single and repetitive head injury. Furthermore, at points of geometric inflection, such as the depths of sulci, clustering of NFTs was frequently found. Although not typical of AD, similar clustering has been demonstrated in CTE (5, 23). Potentially unique to TBI, this may arise as the brain is rapidly deformed, producing concentrations of mechanical stress at inflection points that, ultimately, may lead to more severe cellular pathology, such as the formation of NFTs. Interestingly, glial cells immunoreactive for tau were also observed more commonly following TBI, typically in regions where NFTs were observed. Although not directly quantified, this is a finding worthy of further exploration with regards to delineating the mechanisms of tau accumulation and, possibly, clearance. Previous investigations of the link between TBI and neurodegenerative disease primarily focused on Ab plaques as these were found in approximately 30% of cases in the immediate period after injury (20). However, the long-term Ab plaque pathology following TBI had been in doubt as a consequence of the observation that, in contrast to the acute phase, few plaques are seen in the months following TBI (6). Plaque regression mediated by the Ab-clearing enzyme neprilysin has been suggested as a potential mechanism that may drive plaque clearance in the weeks following TBI (6, 21). In this study we observed Ab plaques in long-term TBI survivors at a greater density than in age-matched controls. In contrast to NFTs, plaques were evident in older cases, a feature previously observed with plaques forming in the acute phase post-injury (12, 37). Furthermore, unlike Ab plaques encountered in both normal aging and acutely post-tbi, which are almost universally diffuse in nature in individuals aged less than 75 (12, 34, 37, 44), the plaques observed in this cohort of survivors of a year or more post-tbi were more often fibrillary. While this work indicates a clear association between a history of a single moderate to severe TBI and later development of Ab and tau pathologies, the limitations inherent in a retrospective study such as this based on archival tissue did not permit extensive regional analyses or subanalyses with regard to correlating the specific TBI-induced pathologies, mechanism of injury or therapeutic intervention with observed pathological findings. However, the results do support the establishment of prospective studies with suitably sampled brain tissue to explore these specific points. In addition, detailed analysis of lesion location in relation to pathology may also be of interest. Here, a standardized analysis over three regions was performed to determine whether trauma is capable of inducing a widespread pathology that might be associated with neurodegenerative disease. Specific regions were sampled because of their known vulnerability in both TBI and neurodegenerative disorders, as well as reflecting previous observations of the acute pathology following TBI, such as plaques (6, 18, 19, 36, 37). Notably, previous data examining plaques following acute TBI suggest the location of any focal lesion (e.g., cerebral contusion) Brain Pathology 22 (2012)
7 Long-Term AD-Like Pathology after Single TBI Johnson et al does not influence the regional distribution of plaques, in other words, it would appear it is the diffuse consequences of TBI that may be mechanistically important (6). Again, however, larger scale prospective studies may permit direct comparisons with the pathologies identified here and those of both AD and following repetitive TBI. Collectively, these data demonstrating the presence of widespread and extensive tau and Ab pathology many years after a single moderate to severe TBI may, in part, represent a substrate for the long-term development of neurodegenerative disease, such as AD, known to be at increased incidence in long-term survivors of TBI. There is undoubtedly a need for direct quantitation and exploration of the mechanistic basis underpinning these observations, including potential genetic determinants such as apolipoprotein E genotype. However, these findings may indicate important potential therapeutic considerations for survivors of TBI, such as emerging anti-tau and anti-ab drugs (4, 22). ACKNOWLEDGMENTS This work was supported by NIH grants NS and NS We would like to express our gratitude to Ms Janice E. Stewart who assisted with the tissue preparation and immunohistochemical techniques described in this study. REFERENCES 1. Braak H, Braak E (1990) Neurofibrillary changes confined to the entorhinal region and an abundance of cortical amyloid in cases of presenile and senile dementia. Acta Neuropathol 80: Braak H, Braak E (1991) Neuropathological stageing of Alzheimer-related changes. Acta Neuropathol 82: Braak H, Braak E (1997) Frequency of stages of Alzheimer-related lesions in different age categories. Neurobiol Aging 18: Brunden KR, Trojanowski JQ, Lee VM (2009) Advances in tau-focused drug discovery for Alzheimer s disease and related tauopathies. Nat Rev Drug Discov 8: Buee L, Hof PR, Bouras C, Delacourte A, Perl DP, Morrison JH, Fillit HM (1994) Pathological alterations of the cerebral microvasculature in Alzheimer s disease and related dementing disorders. Acta Neuropathol 87: Chen XH, Johnson VE, Uryu K, Trojanowski JQ, Smith DH (2009) A lack of amyloid beta plaques despite persistent accumulation of amyloid beta in axons of long-term survivors of traumatic brain injury. Brain Pathol 19: Corsellis JA, Bruton CJ, Freeman-Browne D (1973) The aftermath of boxing. Psychol Med 3: Dale GE, Leigh PN, Luthert P, Anderton BH, Roberts GW (1991) Neurofibrillary tangles in dementia pugilistica are ubiquitinated. J Neurol Neurosurg Psychiatry 54: Faul M, Xu L, Wald MM, Coronado VG (2010) Traumatic Brain Injury in the United States: Emergency Department Visits, Hospitalizations, and Deaths. Centers for Disease Control and Prevention, National Center for Injury Prevention and Control: Atlanta. 10. Geddes JF, Vowles GH, Nicoll JA, Revesz T (1999) Neuronal cytoskeletal changes are an early consequence of repetitive head injury. Acta Neuropathol 98: Gedye A, Beattie BL, Tuokko H, Horton A, Korsarek E (1989) Severe head injury hastens age of onset of Alzheimer s disease. J Am Geriatr Soc 37: Gentleman SM, Greenberg BD, Savage MJ, Noori M, Newman SJ, Roberts GW et al (1997) A beta 42 is the predominant form of amyloid beta-protein in the brains of short-term survivors of head injury. Neuroreport 8: Graham DI, Gentleman SM, Lynch A, Roberts GW (1995) Distribution of beta-amyloid protein in the brain following severe head injury. Neuropathol Appl Neurobiol 21: Graves AB, White E, Koepsell TD, Reifler BV, van Belle G, Larson EB, Raskind M (1990) The association between head trauma and Alzheimer s disease. Am J Epidemiol 131: Guntern R, Bouras C, Hof PR, Vallet PG (1992) An improved thioflavine S method for staining neurofibrillary tangles and senile plaques in Alzheimer s disease. Experientia 48: Guo Z, Cupples LA, Kurz A, Auerbach SH, Volicer L, Chui H et al (2000) Head injury and the risk of AD in the MIRAGE study. Neurology 54: Hof PR, Bouras C, Buee L, Delacourte A, Perl DP, Morrison JH (1992) Differential distribution of neurofibrillary tangles in the cerebral cortex of dementia pugilistica and Alzheimer s disease cases. Acta Neuropathol 85: Huber AGK, Kelemen J, Cervod-Navarro J (1993) Density of amyloid plaques in brains after head trauma. J Neurotrauma 10(Suppl.):S Ikonomovic MD, Uryu K, Abrahamson EE, Ciallella JR, Trojanowski JQ, Lee VM et al (2004) Alzheimer s pathology in human temporal cortex surgically excised after severe brain injury. Exp Neurol 190: Johnson VE, Stewart W, Smith DH (2010) Traumatic brain injury and amyloid-beta pathology: a link to Alzheimer s disease? Nat Rev Neurosci 11: Johnson VE, Stewart W, Stewart JE, Graham DI, Praestgaard AH, Smith DH (2009) A neprilysin polymorphism and amyloid-beta plaques following traumatic brain injury. J Neurotrauma 26: Loane DJ, Pocivavsek A, Moussa CE, Thompson R, Matsuoka Y, Faden AI et al (2009) Amyloid precursor protein secretases as therapeutic targets for traumatic brain injury. Nat Med 15: McKee AC, Cantu RC, Nowinski CJ, Hedley-Whyte ET, Gavett BE, Budson AE et al (2009) Chronic traumatic encephalopathy in athletes: progressive tauopathy after repetitive head injury. J Neuropathol Exp Neurol 68: McKee AC, Gavett BE, Stern RA, Nowinski CJ, Cantu RC, Kowall NW et al (2010) TDP-43 proteinopathy and motor neuron disease in chronic traumatic encephalopathy. J Neuropathol Exp Neurol 69: Mirra SS, Heyman A, McKeel D, Sumi SM, Crain BJ, Brownlee LM et al (1991) The Consortium to Establish a Registry for Alzheimer s Disease (CERAD). Part II. Standardization of the neuropathologic assessment of Alzheimer s disease. Neurology 41: Molgaard CA, Stanford EP, Morton DJ, Ryden LA, Schubert KR, Golbeck AL (1990) Epidemiology of head trauma and neurocognitive impairment in a multi-ethnic population. Neuroepidemiology 9: Mortimer JA, French LR, Hutton JT, Schuman LM (1985) Head injury as a risk factor for Alzheimer s disease. Neurology 35: Mortimer JA, van Duijn CM, Chandra V, Fratiglioni L, Graves AB, Heyman A et al (1991) Head trauma as a risk factor for Alzheimer s disease: a collaborative re-analysis of case-control studies. EURODEM Risk Factors Research Group. Int J Epidemiol 20(Suppl. 2):S28 S Nemetz PN, Leibson C, Naessens JM, Beard M, Kokmen E, Annegers JF, Kurland LT (1999) Traumatic brain injury and time to onset of Alzheimer s disease: a population-based study. Am J Epidemiol 149: Brain Pathology 22 (2012)
8 Johnson et al Long-Term AD-Like Pathology after Single TBI 30. O Meara ES, Kukull WA, Sheppard L, Bowen JD, McCormick WC, Teri L et al (1997) Head injury and risk of Alzheimer s disease by apolipoprotein E genotype. Am J Epidemiol 146: Omalu BI, DeKosky ST, Minster RL, Kamboh MI, Hamilton RL, Wecht CH (2005) Chronic traumatic encephalopathy in a National Football League player. Neurosurgery 57: ; discussion Omalu BI, DeKosky ST, Hamilton RL, Minster RL, Kamboh MI, Shakir AM, Wecht CH (2006) Chronic traumatic encephalopathy in a national football league player: part II. Neurosurgery 59: ; discussion Plassman BL, Havlik RJ, Steffens DC, Helms MJ, Newman TN, Drosdick D et al (2000) Documented head injury in early adulthood and risk of Alzheimer s disease and other dementias. Neurology 55: Price JL, Morris JC (1999) Tangles and plaques in nondemented aging and preclinical Alzheimer s Disease. Ann Neurol 45: Roberts GW, Allsop D, Bruton C (1990) The occult aftermath of boxing. J Neurol Neurosurg Psychiatry 53: Roberts GW, Gentleman SM, Lynch A, Graham DI (1991) beta A4 amyloid protein deposition in brain after head trauma. Lancet 338: Roberts GW, Gentleman SM, Lynch A, Murray L, Landon M, Graham DI (1994) Beta amyloid protein deposition in the brain after severe head injury: implications for the pathogenesis of Alzheimer s disease. J Neurol Neurosurg Psychiatry 57: Salib E, Hillier V (1997) Head injury and the risk of Alzheimer s disease: a case control study. Int J Geriatr Psychiatry 12: Schofield PW, Tang M, Marder K, Bell K, Dooneief G, Chun M et al (1997) Alzheimer s disease after remote head injury: an incidence study. J Neurol Neurosurg Psychiatry 62: Smith C, Graham DI, Murray LS, Nicoll JA (2003) Tau immunohistochemistry in acute brain injury. Neuropathol Appl Neurobiol 29: Smith DH, Chen XH, Iwata A, Graham DI (2003) Amyloid beta accumulation in axons after traumatic brain injury in humans. J Neurosurg 98: Sullivan P, Petitti D, Barbaccia J (1987) Head trauma and age of onset of dementia of the Alzheimer type. JAMA 257: Tokuda T, Ikeda S, Yanagisawa N, Ihara Y, Glenner GG (1991) Re-examination of ex-boxers brains using immunohistochemistry with antibodies to amyloid beta-protein and tau protein. Acta Neuropathol 82: Troncoso JC, Martin LJ, Dal Forno G, Kawas CH (1996) Neuropathology in controls and demented subjects from the Baltimore longditudinal study of aging. Neurobiol Aging 17: Uryu K, Chen XH, Martinez D, Browne KD, Johnson VE, Graham DI et al (2007) Multiple proteins implicated in neurodegenerative diseases accumulate in axons after brain trauma in humans. Exp Neurol 208: Brain Pathology 22 (2012)
Cholinesterase inhibitors and memantine use for Alzheimer s disease TOPIC REVIEW
 Cholinesterase inhibitors and memantine use for Alzheimer s disease TOPIC REVIEW Diagnosis of Dementia : DSM-IV criteria Loss of memory and one or more other cognitive abilities Aphasia Apraxia Agnosia
Cholinesterase inhibitors and memantine use for Alzheimer s disease TOPIC REVIEW Diagnosis of Dementia : DSM-IV criteria Loss of memory and one or more other cognitive abilities Aphasia Apraxia Agnosia
Linguistic Ability in Early Life and the Neuropathology of Alzheimer s Disease and Cerebrovascular Disease
 Linguistic Ability in Early Life and the Neuropathology of Alzheimer s Disease and Cerebrovascular Disease Findings from the Nun Study D.A. SNOWDON, a,b L.H. GREINER, a AND W.R. MARKESBERY a,c a Sanders-Brown
Linguistic Ability in Early Life and the Neuropathology of Alzheimer s Disease and Cerebrovascular Disease Findings from the Nun Study D.A. SNOWDON, a,b L.H. GREINER, a AND W.R. MARKESBERY a,c a Sanders-Brown
THEORIES OF NEUROLOGICAL AGING AND DEMENTIA
 THEORIES OF NEUROLOGICAL AGING AND DEMENTIA Aging Overview The primary care physician must advise middle-age and older patients about ways to age successfully. Dementia is a common disabling illness that
THEORIES OF NEUROLOGICAL AGING AND DEMENTIA Aging Overview The primary care physician must advise middle-age and older patients about ways to age successfully. Dementia is a common disabling illness that
2014 CAS Annual Meeting
 2014 CAS Annual Meeting C10: Claim Issues - Both Emerging and Perennial Traumatic Brain Injury Julianne Callaway, ACAS, ASA, MAAA Assistant Actuary, Global Research & Development RGA Reinsurance Company
2014 CAS Annual Meeting C10: Claim Issues - Both Emerging and Perennial Traumatic Brain Injury Julianne Callaway, ACAS, ASA, MAAA Assistant Actuary, Global Research & Development RGA Reinsurance Company
MCDB 4777/5777 Molecular Neurobiology Lecture 38 Alzheimer s Disease
 MCDB 4777/5777 Molecular Neurobiology Lecture 38 Alzheimer s Disease Outline of Today s Lecture Why is Alzheimer s disease a problem? What is Alzheimer s Disease? What causes Alzheimer s disease? How can
MCDB 4777/5777 Molecular Neurobiology Lecture 38 Alzheimer s Disease Outline of Today s Lecture Why is Alzheimer s disease a problem? What is Alzheimer s Disease? What causes Alzheimer s disease? How can
Traumatic brain injury (TBI) is a significant public health. Short Communications
 JOURNAL OF NEUROTRAUMA 30:1299 1304 ( July 15, 2013) ª Mary Ann Liebert, Inc. DOI: 10.1089/neu.2012.2690 Short Communications Profile of Self-Reported Problems with Executive Functioning in College and
JOURNAL OF NEUROTRAUMA 30:1299 1304 ( July 15, 2013) ª Mary Ann Liebert, Inc. DOI: 10.1089/neu.2012.2690 Short Communications Profile of Self-Reported Problems with Executive Functioning in College and
PET Scanning of Brain Tau in Retired National Football League Players: Preliminary Findings
 PET Scanning of Brain Tau in Retired National Football League Players: Preliminary Findings Gary W. Small, M.D., Vladimir Kepe, Ph.D., Prabha Siddarth, Ph.D., Linda M. Ercoli, Ph.D., David A. Merrill,
PET Scanning of Brain Tau in Retired National Football League Players: Preliminary Findings Gary W. Small, M.D., Vladimir Kepe, Ph.D., Prabha Siddarth, Ph.D., Linda M. Ercoli, Ph.D., David A. Merrill,
League of Denial Video guide and questions I
 League of Denial Video guide and questions I Part I Mike Webster 0:00-21:37 minutes Vocabulary concussion - a stunning, damaging, or shattering effect from a hard blow; especially : a jarring injury of
League of Denial Video guide and questions I Part I Mike Webster 0:00-21:37 minutes Vocabulary concussion - a stunning, damaging, or shattering effect from a hard blow; especially : a jarring injury of
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Traumatic brain injury (TBI)
 Traumatic brain injury (TBI) A topic in the Alzheimer s Association series on understanding dementia. About dementia Dementia is a condition in which a person has significant difficulty with daily functioning
Traumatic brain injury (TBI) A topic in the Alzheimer s Association series on understanding dementia. About dementia Dementia is a condition in which a person has significant difficulty with daily functioning
SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY
 J Rehabil Med 2005; 37: 137 141 SPECIAL REPORT SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY Lena Holm, 1,2 J. David Cassidy, 3 Linda J. Carroll 4 and
J Rehabil Med 2005; 37: 137 141 SPECIAL REPORT SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY Lena Holm, 1,2 J. David Cassidy, 3 Linda J. Carroll 4 and
Integrated Neuropsychological Assessment
 Integrated Neuropsychological Assessment Dr. Diana Velikonja C.Psych Neuropsychology, Hamilton Health Sciences, ABI Program Assistant Professor, Psychiatry and Behavioural Neurosciences Faculty of Health
Integrated Neuropsychological Assessment Dr. Diana Velikonja C.Psych Neuropsychology, Hamilton Health Sciences, ABI Program Assistant Professor, Psychiatry and Behavioural Neurosciences Faculty of Health
Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi.
 Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi. Suresh Kumar, M.D. AUTHOR Director of: Neurology & Headaches Center Inc. Neurocognitve &TBI Rehabilitation Center
Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi. Suresh Kumar, M.D. AUTHOR Director of: Neurology & Headaches Center Inc. Neurocognitve &TBI Rehabilitation Center
Mary Case, MD Professor of Pathology St. Louis University USA. 2015 MO Juvenile Justice Association Conference Lake Ozark, MO
 Mary Case, MD Professor of Pathology St. Louis University USA 2015 MO Juvenile Justice Association Conference Lake Ozark, MO I have nothing to disclose 75 80% of child abuse deaths are due to head trauma
Mary Case, MD Professor of Pathology St. Louis University USA 2015 MO Juvenile Justice Association Conference Lake Ozark, MO I have nothing to disclose 75 80% of child abuse deaths are due to head trauma
Victims Compensation Claim Status of All Pending Claims and Claims Decided Within the Last Three Years
 Claim#:021914-174 Initials: J.T. Last4SSN: 6996 DOB: 5/3/1970 Crime Date: 4/30/2013 Status: Claim is currently under review. Decision expected within 7 days Claim#:041715-334 Initials: M.S. Last4SSN: 2957
Claim#:021914-174 Initials: J.T. Last4SSN: 6996 DOB: 5/3/1970 Crime Date: 4/30/2013 Status: Claim is currently under review. Decision expected within 7 days Claim#:041715-334 Initials: M.S. Last4SSN: 2957
John E. O Toole, Marjorie C. Wang, and Michael G. Kaiser
 Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Biomarkers and treatments for mild traumatic brain injury: from bench to fieldside
 Biomarkers and treatments for mild traumatic brain injury: from bench to fieldside Sandy R Shultz, PhD Department of Medicine The University of Melbourne Australian Rules Football Rugby Findings from
Biomarkers and treatments for mild traumatic brain injury: from bench to fieldside Sandy R Shultz, PhD Department of Medicine The University of Melbourne Australian Rules Football Rugby Findings from
The neuropathology of CJD
 The neuropathology of CJD Definitive diagnosis of a human prion disease requires neuropathological examination of the brain of the affected individual. In the laboratory investigation of human prion diseases
The neuropathology of CJD Definitive diagnosis of a human prion disease requires neuropathological examination of the brain of the affected individual. In the laboratory investigation of human prion diseases
CHILDHOOD CANCER SURVIVOR STUDY Analysis Concept Proposal
 CHILDHOOD CANCER SURVIVOR STUDY Analysis Concept Proposal 1. STUDY TITLE: Longitudinal Assessment of Chronic Health Conditions: The Aging of Childhood Cancer Survivors 2. WORKING GROUP AND INVESTIGATORS:
CHILDHOOD CANCER SURVIVOR STUDY Analysis Concept Proposal 1. STUDY TITLE: Longitudinal Assessment of Chronic Health Conditions: The Aging of Childhood Cancer Survivors 2. WORKING GROUP AND INVESTIGATORS:
Trends in Life Expectancy and Causes of Death Following Spinal Cord Injury. Michael J. DeVivo, Dr.P.H.
 Trends in Life Expectancy and Causes of Death Following Spinal Cord Injury Michael J. DeVivo, Dr.P.H. Disclosure of PI-RRTC Grant James S. Krause, PhD, Holly Wise, PhD; PT, and Emily Johnson, MHA have
Trends in Life Expectancy and Causes of Death Following Spinal Cord Injury Michael J. DeVivo, Dr.P.H. Disclosure of PI-RRTC Grant James S. Krause, PhD, Holly Wise, PhD; PT, and Emily Johnson, MHA have
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. The answers will refer you back to
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. The answers will refer you back to
Does referral from an emergency department to an. alcohol treatment center reduce subsequent. emergency room visits in patients with alcohol
 Does referral from an emergency department to an alcohol treatment center reduce subsequent emergency room visits in patients with alcohol intoxication? Robert Sapien, MD Department of Emergency Medicine
Does referral from an emergency department to an alcohol treatment center reduce subsequent emergency room visits in patients with alcohol intoxication? Robert Sapien, MD Department of Emergency Medicine
Falls are the most common cause of traumatic
 THE INSURANCE IMPLICATIONS OF TRAUMATIC BRAIN INJURY 72 Julianne Callaway, ASA, ACAS, MAAA Assistant Actuary RGA Reinsurance Company Chesterfield, MO jcallaway@rgare.com Causes of Traumatic Brain Injury
THE INSURANCE IMPLICATIONS OF TRAUMATIC BRAIN INJURY 72 Julianne Callaway, ASA, ACAS, MAAA Assistant Actuary RGA Reinsurance Company Chesterfield, MO jcallaway@rgare.com Causes of Traumatic Brain Injury
TYPE OF INJURY and CURRENT SABS Paraplegia/ Tetraplegia
 Paraplegia/ Tetraplegia (a) paraplegia or quadriplegia; (a) paraplegia or tetraplegia that meets the following criteria i and ii, and either iii or iv: i. ii. iii i. The Insured Person is currently participating
Paraplegia/ Tetraplegia (a) paraplegia or quadriplegia; (a) paraplegia or tetraplegia that meets the following criteria i and ii, and either iii or iv: i. ii. iii i. The Insured Person is currently participating
Spine Vol. 30 No. 16; August 15, 2005, pp 1799-1807
 A Randomized Controlled Trial of an Educational Intervention to Prevent the Chronic Pain of Whiplash Associated Disorders Following Rear-End Motor Vehicle Collisions 1 Spine Vol. 30 No. 16; August 15,
A Randomized Controlled Trial of an Educational Intervention to Prevent the Chronic Pain of Whiplash Associated Disorders Following Rear-End Motor Vehicle Collisions 1 Spine Vol. 30 No. 16; August 15,
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
2.1 Who first described NMO?
 History & Discovery 54 2 History & Discovery 2.1 Who first described NMO? 2.2 What is the difference between NMO and Multiple Sclerosis? 2.3 How common is NMO? 2.4 Who is affected by NMO? 2.1 Who first
History & Discovery 54 2 History & Discovery 2.1 Who first described NMO? 2.2 What is the difference between NMO and Multiple Sclerosis? 2.3 How common is NMO? 2.4 Who is affected by NMO? 2.1 Who first
Several professional players of the National CHRONIC TRAUMATIC ENCEPHALOPATHY IN A NATIONAL FOOTBALL LEAGUE PLAYER SPECIAL REPORT
 SPECIAL REPORT CHRONIC TRAUMATIC ENCEPHALOPATHY IN A NATIONAL FOOTBALL LEAGUE PLAYER Bennet I. Omalu, M.D., M.P.H. Departments of Pathology and Epidemiology, Steven T. DeKosky, M.D. Departments of Human
SPECIAL REPORT CHRONIC TRAUMATIC ENCEPHALOPATHY IN A NATIONAL FOOTBALL LEAGUE PLAYER Bennet I. Omalu, M.D., M.P.H. Departments of Pathology and Epidemiology, Steven T. DeKosky, M.D. Departments of Human
The Concept of Cognitive Reserve: A Catalyst for Research
 Journal of Clinical and Experimental Neuropsychology 1380-3395/03/2505-589$16.00 2003, Vol. 25, No. 5, pp. 589 593 # Swets & Zeitlinger The Concept of Cognitive Reserve: A Catalyst for Research Yaakov
Journal of Clinical and Experimental Neuropsychology 1380-3395/03/2505-589$16.00 2003, Vol. 25, No. 5, pp. 589 593 # Swets & Zeitlinger The Concept of Cognitive Reserve: A Catalyst for Research Yaakov
Early Changes in the Brain Proteome Associated with Alzheimer's Disease Risk
 Early Changes in the Brain Proteome Associated with Alzheimer's Disease Risk Nicholas T. Seyfried Assistant Professor Departments of Biochemistry and Neurology Alzheimer s Disease Research Center Emory
Early Changes in the Brain Proteome Associated with Alzheimer's Disease Risk Nicholas T. Seyfried Assistant Professor Departments of Biochemistry and Neurology Alzheimer s Disease Research Center Emory
acbis Chapter 1: Overview of Brain Injury
 acbis Academy for the Certification of Brain Injury Specialists Certification Exam Preparation Course Chapter 1: Overview of Brain Injury Module Objectives Describe the incidence, prevalence and epidemiology
acbis Academy for the Certification of Brain Injury Specialists Certification Exam Preparation Course Chapter 1: Overview of Brain Injury Module Objectives Describe the incidence, prevalence and epidemiology
Woods Traumatic Brain Injury Symposium
 Woods Traumatic Brain Injury Symposium Veterans Health Affairs (VHA) Polytrauma/Traumatic Brain Injury (TBI) System of Care Philadelphia, PA September 28, 2013 VHA/Polytrauma/TBI Program: Presenters Keith
Woods Traumatic Brain Injury Symposium Veterans Health Affairs (VHA) Polytrauma/Traumatic Brain Injury (TBI) System of Care Philadelphia, PA September 28, 2013 VHA/Polytrauma/TBI Program: Presenters Keith
Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD
 Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD Definition and Criteria PTSD is unlike any other anxiety disorder. It requires that
Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD Definition and Criteria PTSD is unlike any other anxiety disorder. It requires that
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is an author's version which may differ from the publisher's version. For additional information about this
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is an author's version which may differ from the publisher's version. For additional information about this
Epilepsy 101: Getting Started
 American Epilepsy Society 1 Epilepsy 101 for nurses has been developed by the American Epilepsy Society to prepare professional nurses to understand the general issues, concerns and needs of people with
American Epilepsy Society 1 Epilepsy 101 for nurses has been developed by the American Epilepsy Society to prepare professional nurses to understand the general issues, concerns and needs of people with
Crash Outcome Data Evaluation System
 Crash Outcome Data Evaluation System HEALTH AND COST OUTCOMES RESULTING FROM TRAUMATIC BRAIN INJURY CAUSED BY NOT WEARING A HELMET, FOR MOTORCYCLE CRASHES IN WISCONSIN, 2011 Wayne Bigelow Center for Health
Crash Outcome Data Evaluation System HEALTH AND COST OUTCOMES RESULTING FROM TRAUMATIC BRAIN INJURY CAUSED BY NOT WEARING A HELMET, FOR MOTORCYCLE CRASHES IN WISCONSIN, 2011 Wayne Bigelow Center for Health
Neurobiology of Depression in Relation to ECT. PJ Cowen Department of Psychiatry, University of Oxford
 Neurobiology of Depression in Relation to ECT PJ Cowen Department of Psychiatry, University of Oxford Causes of Depression Genetic Childhood experience Life Events (particularly losses) Life Difficulties
Neurobiology of Depression in Relation to ECT PJ Cowen Department of Psychiatry, University of Oxford Causes of Depression Genetic Childhood experience Life Events (particularly losses) Life Difficulties
Memory Development and Frontal Lobe Insult
 University Press Scholarship Online You are looking at 1-10 of 11 items for: keywords : traumatic brain injury Memory Development and Frontal Lobe Insult Gerri Hanten and Harvey S. Levin in Origins and
University Press Scholarship Online You are looking at 1-10 of 11 items for: keywords : traumatic brain injury Memory Development and Frontal Lobe Insult Gerri Hanten and Harvey S. Levin in Origins and
Is there a Distinct Phenotype to Memory Loss in Alzheimer's Disease?
 Is there a Distinct Phenotype to Memory Loss in Alzheimer's Disease? David A. Wolk, M.D. Assistant Director Penn Memory Center Assistant Professor of Neurology University of Pennsylvania 5 Million Clinical
Is there a Distinct Phenotype to Memory Loss in Alzheimer's Disease? David A. Wolk, M.D. Assistant Director Penn Memory Center Assistant Professor of Neurology University of Pennsylvania 5 Million Clinical
Brain Injury Litigation. Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com
 Brain Injury Litigation Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com Some General Facts About Traumatic Brain Injury TBIs contribute to a substantial number of deaths and
Brain Injury Litigation Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com Some General Facts About Traumatic Brain Injury TBIs contribute to a substantial number of deaths and
Alzheimer s disease. What is Alzheimer s disease?
 Alzheimer s disease What is Alzheimer s disease? What we know about dementia and Alzheimer s disease Alzheimer s disease is the most common of a large group of disorders known as dementias. It is an irreversible
Alzheimer s disease What is Alzheimer s disease? What we know about dementia and Alzheimer s disease Alzheimer s disease is the most common of a large group of disorders known as dementias. It is an irreversible
How To Map Language With Magnetic Source Imaging
 MAGNETIC SOURCE IMAGING VS. THE WADA TEST IN LANGUAGE LATERALIZATION Robert C. Doss, PsyD Wenbo Zhang, MD, PhD Gail L. Risse, PhD Deanna L. Dickens, MD This paper has been prepared specifically for: American
MAGNETIC SOURCE IMAGING VS. THE WADA TEST IN LANGUAGE LATERALIZATION Robert C. Doss, PsyD Wenbo Zhang, MD, PhD Gail L. Risse, PhD Deanna L. Dickens, MD This paper has been prepared specifically for: American
Examination of the Clinicopathologic Continuum of Alzheimer Disease in the Autopsy Cohort of the National Alzheimer Coordinating Center
 J Neuropathol Exp Neurol Copyright Ó 2013 by the American Association of Neuropathologists, Inc. Vol. 72, No. 12 December 2013 pp. 1182Y1192 ORIGINAL ARTICLE Examination of the Clinicopathologic Continuum
J Neuropathol Exp Neurol Copyright Ó 2013 by the American Association of Neuropathologists, Inc. Vol. 72, No. 12 December 2013 pp. 1182Y1192 ORIGINAL ARTICLE Examination of the Clinicopathologic Continuum
Cerebral Palsy An Expensive Enigma
 Cerebral Palsy An Expensive Enigma Rhona Mahony National Maternity Hospital A group of permanent disorders of the development of movement and posture, causing activity limitation that are not attributed
Cerebral Palsy An Expensive Enigma Rhona Mahony National Maternity Hospital A group of permanent disorders of the development of movement and posture, causing activity limitation that are not attributed
Disease Surveillance in New Jersey Spring 2006
 Creutzfeldt-Jakob Disease Surveillance in New Jersey Spring 2006 Shereen Brynildsen, MS Epidemiologist, Infectious & Zoonotic Disease Program New Jersey Department of Health & Senior Services Phone: 609-588
Creutzfeldt-Jakob Disease Surveillance in New Jersey Spring 2006 Shereen Brynildsen, MS Epidemiologist, Infectious & Zoonotic Disease Program New Jersey Department of Health & Senior Services Phone: 609-588
Pragmatic Evidence Based Review Substance Abuse in moderate to severe TBI
 Pragmatic Evidence Based Review Substance Abuse in moderate to severe TBI Reviewer Emma Scheib Date Report Completed November 2011 Important Note: This report is not intended to replace clinical judgement,
Pragmatic Evidence Based Review Substance Abuse in moderate to severe TBI Reviewer Emma Scheib Date Report Completed November 2011 Important Note: This report is not intended to replace clinical judgement,
BINSA Information on Brain Injury
 Acquired Brain Injury (ABI) There are a number of ways an individual can suffer an acquired brain injury (ABI) Figure one - ABI causes Significant causes of ABI Traumatic Brain Injury (TBI) Traumatic Brain
Acquired Brain Injury (ABI) There are a number of ways an individual can suffer an acquired brain injury (ABI) Figure one - ABI causes Significant causes of ABI Traumatic Brain Injury (TBI) Traumatic Brain
Natalizumab (Tysabri) and PMLthe current figures. Paul-Ehrlich-Institut Brigitte Keller Stanislawski Paul-Ehrlich-Str. 51-59 63225 Langen GERMANY
 Natalizumab (Tysabri) and PMLthe current figures Paul-Ehrlich-Institut Brigitte Keller Stanislawski Paul-Ehrlich-Str. 51-59 63225 Langen GERMANY Humanised MAB Natalizumab Specific binding to a4-integrin
Natalizumab (Tysabri) and PMLthe current figures Paul-Ehrlich-Institut Brigitte Keller Stanislawski Paul-Ehrlich-Str. 51-59 63225 Langen GERMANY Humanised MAB Natalizumab Specific binding to a4-integrin
Alcohol and Brain Damage
 Alcohol and Brain Damage By: James L. Holly, MD O God, that men should put an enemy in their mouths to steal away their brains! That we should, with joy, pleasance, revel, and applause, transform ourselves
Alcohol and Brain Damage By: James L. Holly, MD O God, that men should put an enemy in their mouths to steal away their brains! That we should, with joy, pleasance, revel, and applause, transform ourselves
Albumin and All-Cause Mortality Risk in Insurance Applicants
 Copyright E 2010 Journal of Insurance Medicine J Insur Med 2010;42:11 17 MORTALITY Albumin and All-Cause Mortality Risk in Insurance Applicants Michael Fulks, MD; Robert L. Stout, PhD; Vera F. Dolan, MSPH
Copyright E 2010 Journal of Insurance Medicine J Insur Med 2010;42:11 17 MORTALITY Albumin and All-Cause Mortality Risk in Insurance Applicants Michael Fulks, MD; Robert L. Stout, PhD; Vera F. Dolan, MSPH
GE Global Research. The Future of Brain Health
 GE Global Research The Future of Brain Health mission statement We will know the brain as well as we know the body. Future generations won t have to face Alzheimer s, TBI and other neurological diseases.
GE Global Research The Future of Brain Health mission statement We will know the brain as well as we know the body. Future generations won t have to face Alzheimer s, TBI and other neurological diseases.
Hospitalizations and Medical Care Costs of Serious Traumatic Brain Injuries, Spinal Cord Injuries and Traumatic Amputations
 Hospitalizations and Medical Care Costs of Serious Traumatic Brain Injuries, Spinal Cord Injuries and Traumatic Amputations FINAL REPORT JUNE 2013 J. Mick Tilford, PhD Professor and Chair Department of
Hospitalizations and Medical Care Costs of Serious Traumatic Brain Injuries, Spinal Cord Injuries and Traumatic Amputations FINAL REPORT JUNE 2013 J. Mick Tilford, PhD Professor and Chair Department of
Environmental enrichment mitigates cognitive deficits in a mouse model for Alzheimer s disease
 Environmental enrichment mitigates cognitive deficits in a mouse model for Alzheimer s disease Joanna L. Jankowsky California Institute of Technology Tatiana Melnikova, Daniel Fadale, Guilian Xu, Hilda
Environmental enrichment mitigates cognitive deficits in a mouse model for Alzheimer s disease Joanna L. Jankowsky California Institute of Technology Tatiana Melnikova, Daniel Fadale, Guilian Xu, Hilda
Jordan Chamberlain Brooks
 Jordan Chamberlain Brooks CURRICULUM VITAE February 2015 CONTACT Life Expectancy Project 1439-17th Avenue San Francisco, CA 94122-3402 Phone: (415) 731-0276 Fax: (415) 731-0290 Cell: (510) 507-1418 Brooks@LifeExpectancy.org
Jordan Chamberlain Brooks CURRICULUM VITAE February 2015 CONTACT Life Expectancy Project 1439-17th Avenue San Francisco, CA 94122-3402 Phone: (415) 731-0276 Fax: (415) 731-0290 Cell: (510) 507-1418 Brooks@LifeExpectancy.org
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
 CAMBRIDGE UNIVERSITY CENTRE FOR BRAIN REPAIR A layman's account of our scientific objectives What is Brain Damage? Many forms of trauma and disease affect the nervous system to produce permanent neurological
CAMBRIDGE UNIVERSITY CENTRE FOR BRAIN REPAIR A layman's account of our scientific objectives What is Brain Damage? Many forms of trauma and disease affect the nervous system to produce permanent neurological
Biomarkers for Alzheimer's Disease in Down Syndrome
 Biomarkers for Alzheimer's Disease in Down Syndrome Brad Christian, Ph.D. Waisman Laboratory for Brain Imaging Outline Rationale for Studying AD in Down Syndrome Background of Alzheimer s Disease Biomarkers
Biomarkers for Alzheimer's Disease in Down Syndrome Brad Christian, Ph.D. Waisman Laboratory for Brain Imaging Outline Rationale for Studying AD in Down Syndrome Background of Alzheimer s Disease Biomarkers
REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD
 REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD What is Rehabilitation Medicine? Rehabilitation Medicine (RM) is the medical specialty with rehabilitation as its primary strategy. It provides services
REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD What is Rehabilitation Medicine? Rehabilitation Medicine (RM) is the medical specialty with rehabilitation as its primary strategy. It provides services
Safety of artificial turf and natural grass sports surfaces
 Safety of artificial turf and natural grass sports surfaces Executive Summary This paper briefly summarizes some of the research related to traumatic head injuries in the context of sports. We also introduce
Safety of artificial turf and natural grass sports surfaces Executive Summary This paper briefly summarizes some of the research related to traumatic head injuries in the context of sports. We also introduce
Retinal Imaging Biomarkers for Early Diagnosis of Alzheimer s Disease
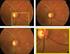 Retinal Imaging Biomarkers for Early Diagnosis of Alzheimer s Disease Eleonora (Nora) Lad, MD, PhD Assistant Professor of Ophthalmology, Vitreoretinal diseases Duke Center for Macular Diseases Duke University
Retinal Imaging Biomarkers for Early Diagnosis of Alzheimer s Disease Eleonora (Nora) Lad, MD, PhD Assistant Professor of Ophthalmology, Vitreoretinal diseases Duke Center for Macular Diseases Duke University
Screening Mammography for Breast Cancer: American College of Preventive Medicine Practice Policy Statement
 Screening Mammography for Breast Cancer: American College of Preventive Medicine Practice Policy Statement Rebecca Ferrini, MD, Elizabeth Mannino, MD, Edith Ramsdell, MD and Linda Hill, MD, MPH Burden
Screening Mammography for Breast Cancer: American College of Preventive Medicine Practice Policy Statement Rebecca Ferrini, MD, Elizabeth Mannino, MD, Edith Ramsdell, MD and Linda Hill, MD, MPH Burden
The Effect of Age and Education Transformations on Neuropsychological Test Scores of Persons With Diffuse or Bilateral Brain Damage 1
 THE EFFECT OF AGE AND EDUCATION TRANSFORMATIONS REITAN & WOLFSON Applied Neuropsychology 2005, Vol. 12, No. 4, 181 189 Copyright 2005 by Lawrence Erlbaum Associates, Inc. The Effect of Age and Education
THE EFFECT OF AGE AND EDUCATION TRANSFORMATIONS REITAN & WOLFSON Applied Neuropsychology 2005, Vol. 12, No. 4, 181 189 Copyright 2005 by Lawrence Erlbaum Associates, Inc. The Effect of Age and Education
Surgery in Individuals Age 65+ Possible Risks. Possible Benefits. Potential Causes of POCD 11/24/2014. What is POCD?
 Surgery in Individuals Age 65+ Postoperative Cognitive Dysfunction in Older Adults Ryan W. Schroeder, Psy.D., LP, ABPP-CN Neuropsychologist & Assistant Professor University of Kansas School of Medicine
Surgery in Individuals Age 65+ Postoperative Cognitive Dysfunction in Older Adults Ryan W. Schroeder, Psy.D., LP, ABPP-CN Neuropsychologist & Assistant Professor University of Kansas School of Medicine
Cycling-related Traumatic Brain Injury 2011
 Cycling-related Traumatic Brain Injury 2011 The Chinese University of Hong Kong Division of Neurosurgery, Department of Surgery Accident & Emergency Medicine Academic Unit Jockey Club School of Public
Cycling-related Traumatic Brain Injury 2011 The Chinese University of Hong Kong Division of Neurosurgery, Department of Surgery Accident & Emergency Medicine Academic Unit Jockey Club School of Public
Case: 1:13-cv-09116 Document #: 70 Filed: 07/29/14 Page 1 of 164 PageID #:1002
 Case: 1:13-cv-09116 Document #: 70 Filed: 07/29/14 Page 1 of 164 PageID #:1002 In re National Collegiate Athletic Association Student-Athlete Concussion Injury Litigation Expert Report of Bruce Deal Regarding
Case: 1:13-cv-09116 Document #: 70 Filed: 07/29/14 Page 1 of 164 PageID #:1002 In re National Collegiate Athletic Association Student-Athlete Concussion Injury Litigation Expert Report of Bruce Deal Regarding
Guidance for Industry Alzheimer s Disease: Developing Drugs for the Treatment of Early Stage Disease
 Guidance for Industry Alzheimer s Disease: Developing Drugs for the Treatment of Early Stage Disease DRAFT GUIDANCE This guidance document is being distributed for comment purposes only. Comments and suggestions
Guidance for Industry Alzheimer s Disease: Developing Drugs for the Treatment of Early Stage Disease DRAFT GUIDANCE This guidance document is being distributed for comment purposes only. Comments and suggestions
1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136. Days and Hours: Monday Friday 8:30a.m. 6:00p.m. (305) 355 9028 (JMH, Downtown)
 UNIVERSITY OF MIAMI, LEONARD M. MILLER SCHOOL OF MEDICINE CLINICAL NEUROPSYCHOLOGY UHEALTH PSYCHIATRY AT MENTAL HEALTH HOSPITAL CENTER 1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136 Days and Hours:
UNIVERSITY OF MIAMI, LEONARD M. MILLER SCHOOL OF MEDICINE CLINICAL NEUROPSYCHOLOGY UHEALTH PSYCHIATRY AT MENTAL HEALTH HOSPITAL CENTER 1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136 Days and Hours:
2015 Alzheimer s Disease Facts and Figures
 2015 Alzheimer s Disease Facts and Figures Includes a Special Report on Disclosing a Diagnosis of Alzheimer s Disease Alzheimer s Disease is the sixth-leading cause of death in the United States. more
2015 Alzheimer s Disease Facts and Figures Includes a Special Report on Disclosing a Diagnosis of Alzheimer s Disease Alzheimer s Disease is the sixth-leading cause of death in the United States. more
Traumatic Brain Injury in Young Athletes. Andrea Halliday, M.D. Oregon Neurosurgery Specialists
 Traumatic Brain Injury in Young Athletes Andrea Halliday, M.D. Oregon Neurosurgery Specialists Variability in defining concussion Lack of reliable biomarkers for concussions Reliance on subjective system
Traumatic Brain Injury in Young Athletes Andrea Halliday, M.D. Oregon Neurosurgery Specialists Variability in defining concussion Lack of reliable biomarkers for concussions Reliance on subjective system
Traumatic Brain Injury and Incarceration. Objectives. Traumatic Brain Injury. Which came first, the injury or the behavior?
 Traumatic Brain Injury and Incarceration Which came first, the injury or the behavior? Barbara Burchell Curtis RN, MSN Objectives Upon completion of discussion, participants should be able to Describe
Traumatic Brain Injury and Incarceration Which came first, the injury or the behavior? Barbara Burchell Curtis RN, MSN Objectives Upon completion of discussion, participants should be able to Describe
Stem cells for brain cures
 13-14/11/2006, Istituto Superiore di Sanità Rome, Italy Frontiers in Imaging Science: High Performance Nuclear Medicine Imagers for Vascular Disease Imaging (Brain and Heart) Stem cells for brain cures
13-14/11/2006, Istituto Superiore di Sanità Rome, Italy Frontiers in Imaging Science: High Performance Nuclear Medicine Imagers for Vascular Disease Imaging (Brain and Heart) Stem cells for brain cures
2014 Alzheimer s Disease Facts and Figures
 2014 Alzheimer s Disease Facts and Figures Includes a Special Report on Women and Alzheimer s Disease Almost two-thirds of Americans with Alzheimer s disease are women. Alzheimer s Disease is the six eading
2014 Alzheimer s Disease Facts and Figures Includes a Special Report on Women and Alzheimer s Disease Almost two-thirds of Americans with Alzheimer s disease are women. Alzheimer s Disease is the six eading
Comparison of traumatic brain injury (TBI) between Aboriginal communities of Northern Quebec and the general Quebec population
 Comparison of traumatic brain injury (TBI) between Aboriginal communities of Northern Quebec and the general Quebec population www.bonjourquebec.com/qc en/baiejames0.html Roy Dudley, Mitra Feyz, Mohammed
Comparison of traumatic brain injury (TBI) between Aboriginal communities of Northern Quebec and the general Quebec population www.bonjourquebec.com/qc en/baiejames0.html Roy Dudley, Mitra Feyz, Mohammed
ALCOHOL RELATED DISORDERS Includes Alcohol Abuse and Alcohol Dependence; Does Not Include Alcohol Use Disorders
 1 MH 12 ALCOHOL RELATED DISORDERS Includes Alcohol Abuse and Alcohol Dependence; Does Not Include Alcohol Use Disorders Background This case definition was developed by the Armed Forces Health Surveillance
1 MH 12 ALCOHOL RELATED DISORDERS Includes Alcohol Abuse and Alcohol Dependence; Does Not Include Alcohol Use Disorders Background This case definition was developed by the Armed Forces Health Surveillance
Identification of Novel Biomarkers of Brain Injury by Integrating Bioinformatics and Mass Spectrometry-based Proteomics
 Identification of Novel Biomarkers of Brain Injury by Integrating Bioinformatics and Mass Spectrometry-based Proteomics Collaborative Study 2 Introduction Brain injury: 1. Non-traumatic Infection Stroke
Identification of Novel Biomarkers of Brain Injury by Integrating Bioinformatics and Mass Spectrometry-based Proteomics Collaborative Study 2 Introduction Brain injury: 1. Non-traumatic Infection Stroke
1 in 3 seniors dies with Alzheimer s or another dementia.
 2013 Alzheimer s disease facts and figures Includes a Special Report on long-distance caregivers 1 in 3 seniors dies with Alzheimer s or another dementia. Out-of-pocket expenses for long-distance caregivers
2013 Alzheimer s disease facts and figures Includes a Special Report on long-distance caregivers 1 in 3 seniors dies with Alzheimer s or another dementia. Out-of-pocket expenses for long-distance caregivers
Health on the Homefront:
 Health on the Homefront: TRAUMATIC BRAIN INJURY SURVEILLANCE, DEPARTMENT OF THE NAVY, SAILORS AND MARINES IN VIRGINIA, 2008-2018 Jean Slosek, MS, Epidemiologist Deployment Health Division, Epidemiology
Health on the Homefront: TRAUMATIC BRAIN INJURY SURVEILLANCE, DEPARTMENT OF THE NAVY, SAILORS AND MARINES IN VIRGINIA, 2008-2018 Jean Slosek, MS, Epidemiologist Deployment Health Division, Epidemiology
chronic leukemia lymphoma myeloma differentiated 14 September 1999 Pre- Transformed Ig Surface Surface Secreted Myeloma Major malignant counterpart
 Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Curriculum Vitae. Board Certification: American Board of Professional Psychology Clinical Neuropsychology and Pediatric Neuropsychology
 Place of Birth: Washington, DC Curriculum Vitae Karen Spangenberg Postal, Ph.D., ABPP-CN 166 North Main Street Suite 3B Andover, MA 01810 (978) 475-2025 E-mail: karenpostal@comcast.net Board Certification:
Place of Birth: Washington, DC Curriculum Vitae Karen Spangenberg Postal, Ph.D., ABPP-CN 166 North Main Street Suite 3B Andover, MA 01810 (978) 475-2025 E-mail: karenpostal@comcast.net Board Certification:
PREDICTORS OF DEPRESSION WITHIN THE CAREGIVERS
 PREDICTORS OF DEPRESSION WITHIN THE CAREGIVERS OF DEMENTIA PATIENTS Melissa G. Sneed Faculty Co-Authors and Sponsors: Nancy H. Wrobel and Robert W. Hymes Department of Behavioral Sciences, University of
PREDICTORS OF DEPRESSION WITHIN THE CAREGIVERS OF DEMENTIA PATIENTS Melissa G. Sneed Faculty Co-Authors and Sponsors: Nancy H. Wrobel and Robert W. Hymes Department of Behavioral Sciences, University of
PE finding: Left side extremities mild weakness No traumatic wound No bloody otorrhea, nor rhinorrhea
 Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA
 KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
Alzheimer s & Dementia 7 (2011) 280 292
 Alzheimer s & Dementia 7 (2011) 280 292 Toward defining the preclinical stages of Alzheimer s disease: Recommendations from the National Institute on Aging-Alzheimer s Association workgroups on diagnostic
Alzheimer s & Dementia 7 (2011) 280 292 Toward defining the preclinical stages of Alzheimer s disease: Recommendations from the National Institute on Aging-Alzheimer s Association workgroups on diagnostic
Glioblastoma (cancer affecting the brain) A guide for journalists on glioblastoma and its treatment
 Glioblastoma (cancer affecting the brain) A guide for journalists on glioblastoma and its treatment Section 1 Glioblastoma Section 2 Epidemiology and prognosis Section 3 Treatment Contents Contents 2 3
Glioblastoma (cancer affecting the brain) A guide for journalists on glioblastoma and its treatment Section 1 Glioblastoma Section 2 Epidemiology and prognosis Section 3 Treatment Contents Contents 2 3
Karen R. Waters. Advanced Nurse Practitioner and Professor Martin Johnson, University of Salford
 Dying with dementia: A retrospective case note analysis of nursing and care home residents who died in hospital. Karen R. Waters. Advanced Nurse Practitioner and Professor Martin Johnson, University of
Dying with dementia: A retrospective case note analysis of nursing and care home residents who died in hospital. Karen R. Waters. Advanced Nurse Practitioner and Professor Martin Johnson, University of
Diseases of the Nervous System. Neal G. Simon, Ph.D. Professor, Dept of Biological Sciences Lehigh University
 Diseases of the Nervous System Neal G. Simon, Ph.D. Professor, Dept of Biological Sciences Lehigh University Outline A. Stress-related Disorders 1. Emotional Circuitry: Key Components 2. The Hypothalamic
Diseases of the Nervous System Neal G. Simon, Ph.D. Professor, Dept of Biological Sciences Lehigh University Outline A. Stress-related Disorders 1. Emotional Circuitry: Key Components 2. The Hypothalamic
Why study clinical neuropsychology?
 University Leiden, The Netherlands Master (MSc) in Clinical Neuropsychology H.A.M.Middelkoop@lumc.nl www.neuropsychologie.leidenuniv.nl Why study clinical neuropsychology? You are interested in: brain/behavior
University Leiden, The Netherlands Master (MSc) in Clinical Neuropsychology H.A.M.Middelkoop@lumc.nl www.neuropsychologie.leidenuniv.nl Why study clinical neuropsychology? You are interested in: brain/behavior
HLA-Cw*0602 associates with a twofold higher prevalence. of positive streptococcal throat swab at the onset of
 1 HLA-Cw*0602 associates with a twofold higher prevalence of positive streptococcal throat swab at the onset of psoriasis: a case control study Lotus Mallbris, MD, PhD, Katarina Wolk, MD, Fabio Sánchez
1 HLA-Cw*0602 associates with a twofold higher prevalence of positive streptococcal throat swab at the onset of psoriasis: a case control study Lotus Mallbris, MD, PhD, Katarina Wolk, MD, Fabio Sánchez
Wolfram Hell *, Matthias Graw. Ludwig Maximilians University, Forensic Medicine, Munich, Germany
 Elderly people in fatal traffic accidents. Analysis of the LMU Safety Accident Database with results from Accident reconstruction, autopsy and ideas of countermeasures from the technical and medical perspective.
Elderly people in fatal traffic accidents. Analysis of the LMU Safety Accident Database with results from Accident reconstruction, autopsy and ideas of countermeasures from the technical and medical perspective.
Compassionate Allowance Outreach Hearing on Brain Injuries. Social Security Administration. November 18, 2008. Statement of
 Compassionate Allowance Outreach Hearing on Brain Injuries Social Security Administration November 18, 2008 Statement of Jerome E. Herbers, Jr., M.D. Office of Healthcare Inspections Office of Inspector
Compassionate Allowance Outreach Hearing on Brain Injuries Social Security Administration November 18, 2008 Statement of Jerome E. Herbers, Jr., M.D. Office of Healthcare Inspections Office of Inspector
Elevated Serum Lactate Dehydrogenase Values in Children with Multiorgan Involvements and Severe Febrile Illness
 Iranian Journal of Pediatrics Society Volume 1, Number 1, 2007: 31-35 Original Article Elevated Serum Lactate Dehydrogenase Values in Children with Multiorgan Involvements and Severe Febrile Illness Farah
Iranian Journal of Pediatrics Society Volume 1, Number 1, 2007: 31-35 Original Article Elevated Serum Lactate Dehydrogenase Values in Children with Multiorgan Involvements and Severe Febrile Illness Farah
Outcome Prediction after Moderate and Severe Head Injury Using an Artificial Neural Network
 241 Outcome Prediction after Moderate and Severe Head Injury Using an Artificial Neural Network Min-Huei Hsu a,b, Yu-Chuan Li c, Wen-Ta Chiu d, Ju-Chuan Yen e a Department of Neurosurgery, e Department
241 Outcome Prediction after Moderate and Severe Head Injury Using an Artificial Neural Network Min-Huei Hsu a,b, Yu-Chuan Li c, Wen-Ta Chiu d, Ju-Chuan Yen e a Department of Neurosurgery, e Department
High Risk Emergency Medicine
 High Risk Emergency Medicine Minor Head Injuries in Patients on Oral Anticoagulants David Thompson, MD, MPH Assistant Professor Department of Emergency Medicine No relevant financial relationships to disclose
High Risk Emergency Medicine Minor Head Injuries in Patients on Oral Anticoagulants David Thompson, MD, MPH Assistant Professor Department of Emergency Medicine No relevant financial relationships to disclose
Stroke & Alzheimer s Disease: An Inflammatory Duo
 Stroke & Alzheimer s Disease: An Inflammatory Duo Stroke and Dementia One in 3 will experience a stroke, dementia or both 64% of persons with a stroke have some degree of cognitive impairment and up to
Stroke & Alzheimer s Disease: An Inflammatory Duo Stroke and Dementia One in 3 will experience a stroke, dementia or both 64% of persons with a stroke have some degree of cognitive impairment and up to
Preventing Dementia: The Depression-Diabetes Nexus
 Preventing Dementia: The Depression-Diabetes Nexus Roger S McIntyre Assoc. Professor of Psychiatry and Pharmacology, University of Toronto Head, Mood Disorders Psychopharmacology Unit, University Health
Preventing Dementia: The Depression-Diabetes Nexus Roger S McIntyre Assoc. Professor of Psychiatry and Pharmacology, University of Toronto Head, Mood Disorders Psychopharmacology Unit, University Health
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Primary Endpoints in Alzheimer s Dementia
 Primary Endpoints in Alzheimer s Dementia Dr. Karl Broich Federal Institute for Drugs and Medical Devices (BfArM) Kurt-Georg-Kiesinger-Allee 38, D-53175 Bonn Germany Critique on Regulatory Decisions in
Primary Endpoints in Alzheimer s Dementia Dr. Karl Broich Federal Institute for Drugs and Medical Devices (BfArM) Kurt-Georg-Kiesinger-Allee 38, D-53175 Bonn Germany Critique on Regulatory Decisions in
Clinical Medical Policy Cognitive Rehabilitation
 Benefit Coverage Outpatient cognitive rehabilitation is considered to be the most appropriate setting for members who have sustained a traumatic brain injury or an acute brain insult. Cognitive rehabilitation
Benefit Coverage Outpatient cognitive rehabilitation is considered to be the most appropriate setting for members who have sustained a traumatic brain injury or an acute brain insult. Cognitive rehabilitation
Hospital-based SNF Coding Tip Sheet: Top 25 codes and ICD-10 Chapter Overview
 Hospital-based SNF Coding Tip Sheet: Top 25 codes and Chapter Overview Chapter 5 - Mental, Behavioral and Neurodevelopmental Disorders (F00-F99) Classification improvements (different categories) expansions:
Hospital-based SNF Coding Tip Sheet: Top 25 codes and Chapter Overview Chapter 5 - Mental, Behavioral and Neurodevelopmental Disorders (F00-F99) Classification improvements (different categories) expansions:
