Patient Information And Rehabilitation Guidelines Following Microfracture Surgery
|
|
|
- Gervais Moore
- 9 years ago
- Views:
Transcription
1 Patient Information And Rehabilitation Guidelines Following Microfracture Surgery This booklet gives you information on articular cartilage damage, the procedure involved and the rehabilitation process. Anatomy The knee is a complicated joint between the femur (thigh bone) and tibia (shin bone). The ends of these two bones are covered with a layer of articular cartilage. This is similar to the cartilage that you will have seen at the end of a chicken bone. This smooth, shiny surface ensures that when two bone ends meet they glide and slide over each other without rubbing. This reduces wear and tear stresses across the joint surfaces. This layer of articular cartilage can wear away over time; commonly known as osteoarthritis. It can also be damaged through injury in a more localised area (known as a lesion or defect) and can give symptoms such as pain, swelling or giving way of the knee. If you have injured this cartilage layer you will have a roughened area in the normally smooth surface. This occurs most commonly on the ends of the femur (thigh bone) but can occur behind the patella (knee cap) and on the top surface of the tibia (shin bone) as these areas all have articular cartilage covering them.
2 Operation An arthroscopy is a keyhole operation, which allows your consultant to look inside your knee joint using a special camera. The procedure is usually carried out under general anaesthetic and involves inserting a fibre optic camera that is about the size of a pencil into the joint through incisions that are approximately 1cm in length. Fluid is then passed into the joint; allowing the structures in the joint to be seen. Occasionally it may be necessary to use a larger incision which will be closed with staples. Microfracture involves drilling multiple small holes in the bone at the bottom of the cartilage defect. This causes bleeding and a clot is formed in the hole. This clot enables new cells to form a repair cartilage (fibrocartilage) that fills the gap. Although this is not exactly like the original cartilage it provides a better surface than bare bone. It is normal to be very sore for a while after this surgery and this does not mean that it will not work. After surgery it is important to protect this clot so that new cells can form. This is done by limiting weight bearing. You are allowed to place your foot on the floor, but not to take much weight through the leg for 6-8 weeks. Return to function and sporting activities can vary between individuals but most people notice significant improvement 6 months after surgery, although full recovery can take up to 12 to 18 months. If this technique is used on the patella you will be put in a knee brace, which restricts your range of movement when walking. You will be able to take weight through the leg as long as it is comfortable. Benefits The following symptoms should be improved following your operation, but remember this will not happen immediately. Reduction of pain Your knee should stop giving way or locking It can take 2-6 weeks for the knee to become less swollen.
3 Risks of surgery The table below outlines the risks of the surgery and how likely they are. Complication Risk Portal Infection 1 in 100 Septic arthritis (infection deep within the knee) 1 in 500 Complex regional pain syndrome (an abnormal pain reaction to any surgery) 1 in 100 Deep vein thrombosis (clot in the calf) 3 in 100 Pulmonary embolism (clot in the lungs) Very rare but potentially life threatening Any surgical intervention can theoretically result in mortality (death), it is extremely rare for this to happen for this procedure but recent legal rulings have mandated this be mentioned. Day of the operation Things to bring: Toiletries and a towel Dressing gown and slippers if you have them Suitable clothes to go home in eg loose trousers/skirt Diversional activities eg book/magazines Walking aids if you use them Admission information You will be admitted to the ward usually the day case unit on the morning of your operation. Ensure you have followed the fasting instructions given in your letter. You will usually be seen by Professor McNicholas and the anaesthetist. You will sign the consent form unless done in clinic. When you are ready you will be take to the theatre room, either walking or in a chair.
4 After the operation You will wake up in the recovery area of the theatre. You may have 2 or 3 small wounds, which will be covered with a small dressing. You will have a compressive wool and crepe bandage on your knee. It is normal for your knee to be a little sore and swollen for the first 48 hours. You may need elbow crutches. You will probably be allowed to go home on the day of your operation and you will be given some painkillers on discharge from hospital. It is important that someone will be with you overnight after the operation; otherwise you will have to stay in hospital overnight. Depending on the area treated you may not be allowed to place all your weight on the leg for the first 6 weeks. Or your leg may be placed in a brace for the first 6 weeks. As a general rule, avoid activities that are painful and cause the knee to swell. A swollen knee is harder to bend and straighten. You may need to keep walking distances short to keep swelling at a minimum. For the first few days rest as much as possible with your leg elevated and move feet and ankles up and down to help your circulation. If at any times your knee becomes acutely painful, you can take pain-killing tablets and it may be worth using ice to reduce your symptoms. To do this, make sure the ice is in a sealed bag, and then wrapped in a damp towel. Alternatively a bag of frozen peas wrapped in a damp towel may be used. Apply the ice for no longer than 10 minutes at any one time. You can use ice every hour if necessary. Follow-up You will be seen at 2 weeks after the operation by Professor McNicholas or his team. Your staples/stitches will be removed now (if you have them) and an explanation of your operation given. You will also be seen 6, 12 and 26 months after the operation. The results of the surgery are monitored to provide information on our performance and how well you recover from the surgery. Before surgery you will receive a questionnaire to determine your knee function. This will be repeated after surgery in order to assess the success of the operation.
5 We would be grateful for your co-operation to enable us to achieve our longterm follow-up plans, which will help to further improve our knee service. If you change address in the future could you please inform us in order to continue the follow-up. Exercises The following exercises should be started immediately and continued at home. These should be performed 4 times each day. 1. Sitting on the bed, place a sock on your foot. Place a slippery board/tray under your foot and a band around it. Bend your knee as far as possible. Gently pull the band to bend a little more. Hold 5 seconds. Repeat 10 times. 2. Sit on a chair with the heel of your operated leg on a stool. Allow your knee to straighten as much as possible for 10 seconds. Repeat 10 times. You can gently press down on your knee with your hands to stretch a little further. 3. Lying on your back. Lift your leg 6 inches, keeping your knee straight. Hold 5 seconds. Repeat 10 times. 4. Sit on the edge of a firm bench so your feet are not supported. Your back should be straight and your hands in the small of the back to stop any slumping. Slowly straighten out your right leg. Hold the stretch for 20 seconds. Repeat 5 times. 5. Stand with the leg to be stretched straight behind you and the other leg bent in front of you. Take support from a wall or chair. Lean your body forwards until you feel the stretching in the calf of the straight leg. Hold the stretch for 20 seconds. Repeat 5 times.
6 General Advice Crutch walking: Crutches and operated leg move first, and then follow through with your good leg. Stick walking: Use the stick in the hand opposite to your operated leg. Stick and operated leg move first, and then follow through with your good leg. Stairs: Keep both crutches or stick in one hand, hold the banister with your other hand. Going up stairs lead with your non- operated leg, when going down stairs lead with your operated leg. Always keep the walking aid on the same step as the operated leg. Showering: You may shower provided that you keep the affected area water tight, i.e. with a plastic bag or cling film around your leg and sealed. If the dressing becomes wet or soiled, please replace it with a clean dry one. Return to work: For desk jobs this could be 5-7 days depending on pain and swelling. For manual jobs it may take 2-6 weeks depending on activities involved and how your knee feels. Driving: Return to driving can vary considerably from person to person. Most people are able to drive 1 to 4 weeks after surgery. However, it is advisable that the following are achieved before trying to drive. You should be walking without crutches with a minimal limp You should be able to safely perform an emergency stop You should feel confident that you are in full control of your car. If you drive an automatic car and your left knee was operated on you can drive once the small wounds are healed. You should notify your insurance company of the procedure that has been undertaken to ensure that your cover is valid. For further information follow this web link: Flying: Flying is not permitted for 8 weeks following surgery due to a higher risk of developing a blood clot. For further information follow the web link below:
7 VTE (blood clots) VTE is a collective term for two conditions: DVT (deep vein thrombosis) this is a blood clot most commonly found in a deep vein that blocks the flow of blood. PE (pulmonary embolism) a potential fatal complication where a blood clot breaks free and travels to the lungs. Whilst you are less mobile, especially during the first few weeks following your procedure, the risk of VTE is higher because of your immobility. Professor McNicholas may prescribe you a daily injection of Clexane to help thin your blood and these should last approximately 14 days. If this is needed, you will be shown how to inject this drug yourself. Symptoms: Swelling you will have some swelling due to your surgery but if you have any concerns please call for advice Pain any new pain we want to know about Calf tenderness Heat and redness compared with the other leg Shortness of breath Chest pain when breathing in Things you can do to prevent VTE Move around as much as possible. Be sensible though, short and regular movement is best Drink plenty of water to keep yourself hydrated We strongly advise you not to smoke this will have been discussed in pre op but we can also refer you to our smoking cessation team within the Hospital. Move your ankle around as much as possible to keep your calf muscle pumping Small preventative measures can have a huge impact on your recovery. Written by: Edited by: Mrs A Hatcher, Orthopaedic Physiotherapist Specialist Mr P Ellison, Orthopaedic Physiotherapist Specialist Richard Norris, Orthopaedic Physiotherapist Specialist Professor MJ McNicholas, Consultant Orthopaedic Surgeon Miss F Rashid, Orthopaedic Registrar Date last reviewed: April 2016
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Tibial Intramedullary Nailing
 Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Broström Lateral Ligament Reconstruction of Ankle
 Broström Lateral Ligament Reconstruction of Ankle This leaflet aims to answer your questions about having a broström lateral ligament reconstruction of ankle under the care of Mr Sam Singh. It explains
Broström Lateral Ligament Reconstruction of Ankle This leaflet aims to answer your questions about having a broström lateral ligament reconstruction of ankle under the care of Mr Sam Singh. It explains
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Elbow arthroscopy. Key points
 Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle
 A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
Biceps Tenodesis. An information guide for patients. Delivering the best in care. UHB is a no smoking Trust
 Biceps Tenodesis An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Biceps Tenodesis An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
LASER TREATMENT FOR VARICOSE VEINS
 LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
LASER TREATMENT FOR VARICOSE VEINS How can varicose veins be treated by laser? Laser treatment of varicose veins, Endovascular Laser Ablation (known as EVLA), is a minimally invasive procedure for treating
Total Knee Replacement
 Manchester Royal Infirmary Total Knee Replacement Department of Orthopaedic Surgery 2 What is a Total Knee Replacement? Total knee replacement is one of the most commonly performed orthopaedic operations
Manchester Royal Infirmary Total Knee Replacement Department of Orthopaedic Surgery 2 What is a Total Knee Replacement? Total knee replacement is one of the most commonly performed orthopaedic operations
KNEE ARTHROSCOPY HANDBOOK
 KNEE ARTHROSCOPY HANDBOOK 1450 Ellis Street Suite 201 Bozeman, Montana 59715 (406) 587-0122 FAX (406) 587-5548 www.bridgerorthopedic.com Your Arthroscopy Handbook Contemplating surgery of any kind leads
KNEE ARTHROSCOPY HANDBOOK 1450 Ellis Street Suite 201 Bozeman, Montana 59715 (406) 587-0122 FAX (406) 587-5548 www.bridgerorthopedic.com Your Arthroscopy Handbook Contemplating surgery of any kind leads
Delivering Excellence. Nuffield Orthopaedic Centre NHS Trust. Information for Patients. Hip and Knee service. Total Knee Replacement NHS
 www.noc.nhs.uk/hipandknee/default.aspx Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Total Knee Replacement Information for Patients Hip and Knee service Delivering Excellence Contents Page
www.noc.nhs.uk/hipandknee/default.aspx Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Total Knee Replacement Information for Patients Hip and Knee service Delivering Excellence Contents Page
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Elective Laparoscopic Cholecystectomy
 General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
General Surgery Elective Laparoscopic Cholecystectomy This information aims to explain what will happen before, during and after your surgery to remove your gallbladder. It includes information about the
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Deep Vein Thrombosis (DVT) in pregnancy
 Deep Vein Thrombosis (DVT) in pregnancy Information and advice for women and families Maternity What is a deep vein thrombosis (DVT)? A deep vein thrombosis (DVT) is a blood clot that forms in a deep leg
Deep Vein Thrombosis (DVT) in pregnancy Information and advice for women and families Maternity What is a deep vein thrombosis (DVT)? A deep vein thrombosis (DVT) is a blood clot that forms in a deep leg
Rehabilitation guidelines for patients undergoing knee arthroscopy
 Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
SLAP repair. An information guide for patients. Delivering the best in care. UHB is a no smoking Trust
 SLAP repair An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
SLAP repair An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY
 PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction This leaflet has been compiled by the Physiotherapy Team to help you understand the hip
PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction This leaflet has been compiled by the Physiotherapy Team to help you understand the hip
Arthroscopic Ankle Fusion (Arthrodesis)
 Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME
 KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
KNEE ARTHROSCOPIC SURGERY IN INJURY AND DISEASE
 KNEE ARTHROSCOPIC SURGERY IN INJURY AND DISEASE INFORMATION FOR PATIENTS and peri-oerative health WORKERS IN GHANA AND SUB-SAHARAN AFRICA RACHEL GEVEL (chartered physiotherapist) & P OFORI-ATTA (orthopaedic
KNEE ARTHROSCOPIC SURGERY IN INJURY AND DISEASE INFORMATION FOR PATIENTS and peri-oerative health WORKERS IN GHANA AND SUB-SAHARAN AFRICA RACHEL GEVEL (chartered physiotherapist) & P OFORI-ATTA (orthopaedic
Further information You can get more information and share your experience at www.aboutmyhealth.org
 OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST
 PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Reverse Shoulder Replacement
 Reverse Shoulder Replacement An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Reverse Shoulder Replacement An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Subtotal Colectomy. Delivering the best in care. UHB is a no smoking Trust
 Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Arthroscopic subacromial decompression and rotator cuff repair
 Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Patella Realignment Tibial Tuberosity Transfer with Lateral Release
 Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Rivaroxaban to prevent blood clots for patients who have a lower limb plaster cast. Information for patients Pharmacy
 Rivaroxaban to prevent blood clots for patients who have a lower limb plaster cast Information for patients Pharmacy Your doctor has prescribed a tablet called rivaroxaban. This leaflet tells you about
Rivaroxaban to prevent blood clots for patients who have a lower limb plaster cast Information for patients Pharmacy Your doctor has prescribed a tablet called rivaroxaban. This leaflet tells you about
ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION. Under the Care of Mr M Paterson - 11 -
 ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION Under the Care of Mr M Paterson Acknowledgement: Drawings by Jean Paterson Perth Australia 2006 Brochure: R. Grubb Amended:
ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION Under the Care of Mr M Paterson Acknowledgement: Drawings by Jean Paterson Perth Australia 2006 Brochure: R. Grubb Amended:
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Ankle Sprain. Information and Rehabilitation. Grade II. Grade I. Grade III
 514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
AFTER TOTAL KNEE REPLACEMENT. Living with Your New Knee
 AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
.org. Knee Arthroscopy. Description. Preparing for Surgery. Surgery
 Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Venefit treatment for varicose veins
 Oxford University Hospitals NHS Trust Venefit treatment for varicose veins Information for patients Your consultant has recommended that we treat your varicose veins with a procedure known as Venefit radio
Oxford University Hospitals NHS Trust Venefit treatment for varicose veins Information for patients Your consultant has recommended that we treat your varicose veins with a procedure known as Venefit radio
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Cheilectomy. For more information please go to Mr Singh s Website: http://www.footandanklesurgeon.co.uk
 Cheilectomy This leaflet aims to answer your questions about having surgery for a cheilectomy procedure under the care of Mr Sam Singh. It explains the benefits, risks and alternatives, as well as what
Cheilectomy This leaflet aims to answer your questions about having surgery for a cheilectomy procedure under the care of Mr Sam Singh. It explains the benefits, risks and alternatives, as well as what
Frequently Asked Questions about Foot and Ankle Surgery. Foot & Ankle Clinic. Cambridge. A patient s guide. Fred Robinson
 Frequently Asked Questions about Foot and Ankle Surgery A patient s guide Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon www.cambridgefootandankle.com Frequently Asked Questions
Frequently Asked Questions about Foot and Ankle Surgery A patient s guide Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon www.cambridgefootandankle.com Frequently Asked Questions
Adult Advisor: Plantar Fasciitis. Plantar Fasciitis
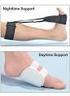 Adult Advisor: Plantar Fasciitis Page 1 of 3 Plantar Fasciitis What is plantar fasciitis? Plantar fasciitis is a painful inflammation of the bottom of the foot between the ball of the foot and the heel.
Adult Advisor: Plantar Fasciitis Page 1 of 3 Plantar Fasciitis What is plantar fasciitis? Plantar fasciitis is a painful inflammation of the bottom of the foot between the ball of the foot and the heel.
Hand & Plastics Physiotherapy Department Cubital Tunnel Syndrome Information for patients
 Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Cubital Tunnel Syndrome Information for patients This leaflet has been developed to answer any questions you may have regarding
Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Cubital Tunnel Syndrome Information for patients This leaflet has been developed to answer any questions you may have regarding
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
PLANTAR FASCITIS (Heel Spur Syndrome)
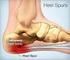 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Ankle Stabilisation Procedure
 Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Forefoot deformity correction
 Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
VARICOSE VEIN ADVICE SHEET PRIVATE DAY CASE Mr Paul O Byrne
 VARICOSE VEIN ADVICE SHEET PRIVATE DAY CASE Mr Paul O Byrne What are Varicose Veins Varicose veins are enlarged swollen veins. Most varicose veins are found in the legs. They are generally caused by a
VARICOSE VEIN ADVICE SHEET PRIVATE DAY CASE Mr Paul O Byrne What are Varicose Veins Varicose veins are enlarged swollen veins. Most varicose veins are found in the legs. They are generally caused by a
Coccydynia. (Coccyx Pain) Information for patients. Outpatients Physiotherapy Tel: 01473 703312
 Information for patients Coccydynia (Coccyx Pain) Outpatients Physiotherapy Tel: 01473 703312 DPS ref: 4508-12(RP) Issue 1: February 2013 Review date: January 2016 The Ipswich Hospital NHS Trust, 2013.
Information for patients Coccydynia (Coccyx Pain) Outpatients Physiotherapy Tel: 01473 703312 DPS ref: 4508-12(RP) Issue 1: February 2013 Review date: January 2016 The Ipswich Hospital NHS Trust, 2013.
Contents. Overview. Removing the womb (hysterectomy) Overview
 This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
Exercises for older people
 Exercise for older people Exercises for older people Sitting Getting started If you ve not done much physical activity for a while, you may want to get the all-clear from a GP before starting. For the
Exercise for older people Exercises for older people Sitting Getting started If you ve not done much physical activity for a while, you may want to get the all-clear from a GP before starting. For the
