Principles of radiation therapy
|
|
|
- Ashlyn Barker
- 7 years ago
- Views:
Transcription
1 CHAPTER 2 Principles of radiation therapy Michael J. Gazda, MS, and Lawrence R. Coia, MD This chapter provides a brief overview of the principles of radiation therapy. The topics to be discussed include the physical aspects of how radiation works (ionization, radiation interactions) and how it is delivered (treatment machines, treatment planning, and brachytherapy). Recent relevant techniques of radiation oncology, such as conformal and stereotactic radiation, also will be presented. These topics are not covered in great technical detail, and no attempt is made to discuss the radiobiological effects of radiation therapy. It is hoped that a basic understanding of radiation treatment will benefit those practicing in other disciplines of cancer management. RADIATION THERAPY How radiation works IONIZING RADIATION Ionizing radiation is energy sufficiently strong to remove an orbital electron from an atom. This radiation can have an electromagnetic form, such as a high-energy photon, or a particulate form, such as an electron, proton, neutron, or alpha particle. High-energy photons By far, the most common form of radiation used in practice today is the high-energy photon. Photons that are released from the nucleus of a radioactive atom are known as gamma rays. When photons are created electronically, such as in a clinical linear accelerator, they are known as x-rays. Thus, the only difference between the two terms is the origin of the photon. Inverse square law The intensity of an x-ray beam is governed by the inverse square law. This law states that the radiation intensity from a point source is inversely proportional to the square of the distance away from the radiation source. In other words, the dose at 2 cm will be one-fourth of the dose at 1 cm. Electron volt Photon absorption in human tissue is determined by the energy of the radiation, as well as the atomic structure of the tissue in question. The basic unit of energy used in radiation oncology is the electron volt (ev); 10 3 ev = 1 kev, 10 6 ev = 1 MeV. PRINCIPLES OF RADIATION THERAPY 9
2 RADIATION THERAPY PHOTON-TISSUE INTERACTIONS Three interactions describe photon absorption in tissue: the photoelectric effect, Compton effect, and pair production. Photoelectric effect In this process, an incoming photon undergoes a collision with a tightly bound electron. The photon transfers practically all of its energy to the electron and ceases to exist. The electron departs with most of the energy from the photon and begins to ionize surrounding molecules. This interaction depends on the energy of the incoming photon, as well as the atomic number of the tissue; the lower the energy and the higher the atomic number, the more likely that a photoelectric effect will take place. An example of this interaction in practice can be seen on a diagnostic x-ray film. Since the atomic number of bone is 60% higher than that of soft tissue, bone is seen with much more contrast and detail than is soft tissue. The energy range in which the photoelectric effect predominates in tissue is about kev. Compton effect The Compton effect is the most important photon-tissue interaction for the treatment of cancer. In this case, a photon collides with a free electron, ie, one that is not tightly bound to the atom. Unlike the photoelectric effect, in the Compton interaction both the photon and electron are scattered. The photon can then continue to undergo additional interactions, albeit with a lower energy. The electron begins to ionize with the energy given to it by the photon. The probability of a Compton interaction is inversely proportional to the energy of the incoming photon and is independent of the atomic number of the material. When one takes an image of tissue using photons in the energy range in which the Compton effect dominates (~25 kev-25 MeV), bone and softtissue interfaces are barely distinguishable. This is a result of the atomic number independence. The Compton effect is the most common interaction occurring clinically, as most radiation treatments are performed at energy levels of about 6-20 MeV. Port films are films taken with such high-energy photons on the treatment machine and are used to check the precision and accuracy of the beam; because they do not distinguish tissue densities well, however, they are not equal to diagnostic films in terms of resolution. Pair production In this process, a photon interacts with the nucleus of an atom, not an orbital electron. The photon gives up its energy to the nucleus and, in the process, creates a pair of positively and negatively charged electrons. The positive electron (positron) ionizes until it combines with a free electron. This generates two photons that scatter in opposite directions. The probability of pair production is proportional to the logarithm of the energy of the incoming photon and is dependent on the atomic number of the material. The energy range in which pair production dominates is 25 MeV. This interaction does occur to some extent in routine radiation treatment with high-energy photon beams. 10 CANCER MANAGEMENT: A MULTIDISCIPLINARY APPROACH
3 ELECTRON BEAMS With the advent of high-energy linear accelerators, electrons have become a viable option in treating superficial tumors up to a depth of about 5 cm. Electron depth dose characteristics are unique in that they produce a high skin dose but exhibit a falloff after only a few centimeters. Electron absorption in human tissue is greatly influenced by the presence of air cavities and bone. The dose is increased when the electron beam passes through an air space and is reduced when the beam passes through bone. Common uses The most common clinical uses of electron beams include the treatment of skin lesions, such as basal cell carcinomas, and boosting of (giving further radiation to) areas that have previously received photon irradiation, such as the postoperative lumpectomy or mastectomy scar in breast cancer patients, as well as select nodal areas in the head and neck. MEASURING RADIATION ABSORPTION The dose of radiation absorbed correlates directly with the energy of the beam. An accurate measurement of absorbed dose is critical in radiation treatment. The deposition of energy in tissues results in damage to DNA and diminishes or eradicates the cell s ability to replicate indefinitely. Gray The basic unit of radiation absorbed dose is the amount of energy (joules) absorbed per unit mass (kg). This unit, known as the gray (Gy), has replaced the unit of rad used in the past (100 rads = 1 Gy; 1 rad = 1 cgy). Exposure In order to measure dose in a patient, one must first measure the ionization produced in air by a beam of radiation. This quantity is known as exposure. One can then correct for the presence of soft tissue in the air and calculate the absorbed dose in Gy. Percentage depth dose The dose absorbed by tissues due to these interactions can be measured and plotted to form a percentage depth dose curve. As energy increases, the penetrative ability of the beam increases and the skin dose decreases. How radiation is delivered TREATMENT MACHINES Linear accelerators High-energy radiation is delivered to tumors by means of a linear accelerator. A beam of electrons is generated and accelerated through a waveguide that increases their energy to the kev to MeV range. These electrons strike a tungsten target and produce x-rays. X-rays generated in the keV range are known as grenz rays, whereas the energy range for superficial units is about kev. Orthovoltage units generate x-rays from kev. PRINCIPLES OF RADIATION THERAPY 11
4 Orthovoltage units continue to be used today to treat superficial lesions; in fact, they were practically the only machines treating skin lesions before the recent emergence of electron therapy. The maximum dose from any of these low-energy units is found on the surface of patients; thus, skin becomes the dose-limiting structure when treating patients at these energies. The depth at which the dose is 50% of the maximum is about 7 cm. Table 1 lists the physical characteristics of several relevant x-ray energies. Megavoltage units The megavoltage linear accelerator has been the standard radiotherapy equipment for the past years. Its production of x-rays is identical to that of lower-energy machines. However, the energy range of megavoltage units is quite broad from 4 to 20 MeV. The depth of the maximum dose in this energy range is cm. The dose to the skin is about 30%-40% of the maximum dose. Most megavoltage units today also have electron-beam capabilities, usually in the energy range of about 5-20 MeV. In order to produce an electron beam, the tungsten target is moved away from the path of the beam. The original electron beam that was aimed at the tungsten target is now the electron beam used for treatment. Unlike that of photons, the electron skin dose is quite high, about 80%-95% of the maximum dose. A rule of thumb regarding the depth of penetration of electrons is that 80% of the dose is delivered at a depth (in cm) corresponding to one-third of the electron energy (in MeV). Thus, a 12-MeV beam will deliver 80% of the dose at a depth of 4 cm. Altering beam intensity and field size When measurements are made at the point just past the target, the beam is more intense in the center than at the edges. Optimal treatment planning is obtained with a relatively constant intensity across the width of the beam. This process is accomplished by placing a flattening filter below the target. In order for the radiation beam to conform to a certain size, high atomic number collimators are installed in the machine. They can vary the field size from 4 4 cm to cm at a distance of 100 cm from the target, which is the distance at which most treatments are performed. TABLE 1: Depth dose characteristics for clinical radiotherapy beams Nominal energy Depth of maximum dose (cm) Skin dose (%) 240 kv(p) Surface 100 Cobalt MeV MeV MeV kv(p) = kilovolt (peak) 12 CANCER MANAGEMENT: A MULTIDISCIPLINARY APPROACH
5 If it is decided that a beam should be more intense on one side than the other, high atomic number filters, known as wedges, are placed in the beam. These filters can shift the dose distribution surrounding the tumor by 15º-60º. Wedges can also be used to optimize the dose distribution if the treatment surface is curved or irregular. Shielding normal tissue Once the collimators have been opened to the desired field size that encompasses the tumor, the physician may decide to block out some normal tissue that remains in the treatment field. This is accomplished by placing blocks (or alloy), constructed of a combination of bismuth, tin, cadmium, and lead, in the path of the beam. In this way, normal tissues are shielded, and the dose can be delivered to the tumor at a higher level than if the normal structures were in the field. These individually constructed blocks are used in both x-ray and electron treatments. A more modern technique involves multileaf collimators mounted inside the gantry. They provide computerized, customized blocking instead of having to construct a new block for each field. (See Intensity-modulated radiation therapy. ) PRETREATMENT PROCEDURES Certain imaging procedures must be done before radiation therapy is begun: Pretreatment CT Before any treatment planning can begin, a pretreatment CT scan is often performed. This scan allows the radiation oncologist to identify both tumor and surrounding normal structures. Simulation The patient is then sent for a simulation. The patient is placed on a diagnostic x-ray unit that geometrically simulates an actual treatment machine. With use of the CT information, the patient s treatment position is simulated by means of fluoroscopy. A series of orthogonal films are taken, and block templates that will shield any normal structures are drawn on the films. These films are sent to the mold room, where technicians construct the blocks to be used for treatment. CT simulation is a modern alternative to conventional simulation and is described later in this chapter. Guides for treatment field placement Small skin marks, or tattoos, are placed on the patient following proper positioning in simulation. These tattoos will guide the placement of treatment fields and give the physician a permanent record of past fields should the patient need additional treatment in the future. It is imperative that the patient be treated in a reproducible manner each day. In order to facilitate this, Styrofoam casts that conform to the patient s contour and place the patient in the same position for each treatment are constructed. Lasers also help line up the patient during treatment. TREATMENT PLANNING AND DELIVERY Determining optimal dose distribution The medical physicist or dosimetrist uses the information from CT and simulation to plan the treatment on a computer. A complete collection of machine data, including depth dose and beam profile information, is stored in the computer. The physics staff aids the radia- PRINCIPLES OF RADIATION THERAPY 13
6 tion oncologist in deciding the number of beams (usually two to four) and angles of entry. The goal is to maximize the dose to the tumor while minimizing the dose to surrounding normal structures. Several treatment plans are generated, and the radiation oncologist chooses the optimal dose distribution. The beam-modifying devices discussed earlier, such as blocks and wedges, may be used to optimize the dose distribution around the tumor. Establishing the treatment plan The planning computer will calculate the amount of time each beam should be on during treatment. All pertinent data, such as beam-on time, beam angles, blocks, and wedges, are recorded in the patient s treatment chart and sent to the treatment machine. The radiation therapist will use this information, as well as any casts, tattoos, and lasers, to set up and treat the patient consistently and accurately each day. Port films As part of departmental quality assurance, weekly port films are taken for each beam. They ensure that the beams and blocks are consistently and correctly placed for each treatment. Port films are images generated by the linear accelerator at energies of 6-20 MeV. Because of the predominance of the Compton effect in this energy range, these images are not as detailed as those at diagnostic film energies (as mentioned earlier), but they still add important information on treatment accuracy and ensure the quality of setup and treatment. BRACHYTHERAPY Brachytherapy is the term used to describe radiation treatment in which the radiation source is in contact with the tumor. This therapy contrasts with externalbeam radiotherapy, in which the radiation source is cm away from the patient. In brachytherapy, dose distribution is almost totally dependent on the inverse square law because the source is usually within the tumor volume. Because of this inverse square dependence, proper placement of radiation sources is crucial. TABLE 2: Physical characteristics of commonly used radioisotopes Isotope Energy (MeV) Half-life Radium ,600 yr Cesium yr Cobalt yr Iridium d Iodine d Gold d 14 CANCER MANAGEMENT: A MULTIDISCIPLINARY APPROACH
7 Isotopes Table 2 lists commonly used isotopes and their properties. In the past, radium was the primary isotope used in brachytherapy. Recently, because of its long half-life and high energy output, radium has been replaced with cesium (Cs), gold (Au), and iridium (Ir). These isotopes have shorter half-lives than radium and can be shielded more easily because of their lower energies. Types of implants Brachytherapy procedures can be performed with either temporary or permanent implants. Temporary implants usually have long halflives and higher energies than permanent implants. These sources can be manufactured in several forms, such as needles, seeds, and ribbons. All temporary sources are inserted into catheters that are placed in the tumor during surgery. A few days after surgery, the patient is brought to the radiation clinic and undergoes pretreatment simulation. Wires with nonradioactive metal seeds are threaded into these catheters. Several films are taken, and the images of the seed placement can be digitized into a brachytherapy treatment planning computer. Once the treatment plan is complete and the physician has chosen the optimal dose rate (usually cgy/h), the sources can be implanted. The actual implantation takes place in the patient s private room. The duration of treatment is usually 1-3 days. The majority of temporary implants are loaded interstitially. Common uses Interstitial low-dose-rate (LDR) brachytherapy is commonly used for cancer of the oral cavity and oropharynx and sarcoma. Prostate cancer is probably the most common site for which LDR brachytherapy seeds are used today. Intracavitary LDR brachytherapy is frequently used in gynecologic applications. High-dose-rate (HDR) brachytherapy is used with remote afterloading techniques, as described below. Remote afterloading brachytherapy Because brachytherapy requires numerous safety precautions and entails unnecessary exposure of personnel and family members to radiation, remote afterloading of temporary implants has become popular in recent years. The two types of remote afterloading that can be used for treatment are LDR and HDR sources. The most popular LDR source used today is Cs-137, which has a dose rate of about 1 cgy/min. The most widely used HDR source is Ir-192. This isotope has a dose rate of about 100 cgy/min. General procedures The pretreatment brachytherapy procedures outlined above are also implemented in remote afterloading brachytherapy. Once the treatment plan has been approved by the physician, the patient is brought into the treatment room. The LDR cesium source or HDR iridium source is connected to the end of a cable inside its respective afterloading unit. This unit is programmed with the data from the planning computer. The cable is sent out from the unit into one of the patient s catheters. Several catheters can be connected to the unit. Each catheter is irradiated, one at a time, until the prescribed dose has been delivered. PRINCIPLES OF RADIATION THERAPY 15
8 The motor that drives the source out of the treatment unit is connected electronically to the door of the treatment room. If the treatment must be stopped for any reason, simply opening the door triggers an interlock that draws the source back into the unit. Because of this device, oncology personnel will not be exposed to any radiation should they need to see the patient during treatment. This interlock is the main safety advantage of remote afterloading over manual afterloading. LDR treatment Uterine cancer is the most popular site for intracavitary treatment with LDR remote afterloading brachytherapy. These procedures are performed in the patient s room. The interlock is connected to the patient s door so that nurses can take vital signs and give medication and family members can visit the patient without risk of radiation exposure. HDR treatment The most common applications of HDR brachytherapy are for tumors of the vaginal apex, esophagus, lungs, and, most recently, breast and prostate. Most HDR treatments are performed on an outpatient basis. Allowing the patient to return home the same day after therapy is one advantage of HDR afterloading brachytherapy. Patients with prostate cancer are the exception. They may remain in the hospital for 2-3 days during the treatment. Recent advances in planning and treatment CT SIMULATION Until recently, CT and simulation were separate pretreatment procedures. Within the past decade, many cancer centers have combined CT and simulation into a single diagnostic-treatment planning unit, known as a CT-simulator. The major advantage of this combination is that both procedures can be performed by one unit and, thus, the patient does not have to make two separate visits to the clinic. Also, CT simulation is bringing the radiation clinic into the digital age, with hospitals reporting an increase in speed, efficiency, and accuracy of treatment planning and delivery. Procedure In brief, in the first step of this new procedure, the patient is placed on the CT-simulator table and undergoes a normal CT study. The physician has the capability of outlining the tumor and any normal structures on each CT slice. A computer performs a three-dimensional (3D) transformation of the CT slices and creates a digitally reconstructed radiograph (DRR). The DRR resembles a normal diagnostic film, except that it is digital and can be manipulated to achieve better contrast and detail than regular film. The outlines of the tumor and organs are displayed on the DRRs for any viewing angle. The physician can then draw blocks on the DRRs with a more accurate idea of where the tumor and normal tissues actually lie. The DRRs are digitized into the treatment planning computer, and any CT slices and their contours drawn by the physician are transferred as well. These DRRs are either sent to the mold room for block construction or are trans- 16 CANCER MANAGEMENT: A MULTIDISCIPLINARY APPROACH
9 ferred to the treatment planning software for multileaf collimator optimization. Treatment plans are generated as discussed earlier. At the time of the patient s first treatment, DRRs and port films are digitized and saved on a local area network (LAN). Physicians can then call up these images on their desktop computers for weekly patient quality assurance. CONFORMAL RADIATION THERAPY Conformal radiation therapy is a geometric shaping of the radiation beam that conforms with the beam s eye view of the tumor. Conformal therapy utilizes the outlining capabilities of the CT-simulator. The physician outlines the tumor volume, generates DRRs, and draws an appropriate margin from 1-2 cm around the tumor. These fields conform closely to the shape of the tumor and, thus, shield more critical structures than do normal blocks. The margin allows for setup errors of a few millimeters each day. Appropriate immobilization of the target volume must be achieved in each patient through the use of devices that constrain movement ( casts ) so that the target is accurately localized. These films are sent to the mold room for block construction. Since the fields are tighter around the tumor, the prescribed dose can be increased. Clinicians believe that by increasing the dose to the tumor, local control will be improved. Intensity-modulated radiation therapy (IMRT), an extension of conformal therapy, allows for shaping of the intensity of the radiation beam. This is an important improvement, especially when the target is not well separated from normal tissues. A uniform dose distribution can be created around the tumor by either modulating the intensity of the beam during its journey through the linear accelerator or by the use of multileaf collimators. Multileaf collimators consist of 80 or more individual collimators, or leaves, located at the head of the linear accelerator, which can be adjusted to the shape of the tumor. (For a technical description, the reader is referred to the text by Khan; see Suggested Reading. ) Both of these methods alter the fluence of radiation exiting the accelerator. The final result is a uniform dose distribution around the tumor and minimal dose to the surrounding normal tissues, often below tolerance levels. This improves the risk-benefit ratio. The clinical use of IMRT has grown as computer power increases and costs decline. Preliminary clinical data have shown that prostate doses can be increased significantly without increasing the complication rate. IMRT must be administered within a closely monitored program with rigorous quality assurance since it can potentially cause significant injury if not appropriately applied. Several types of IMRT delivery are now becoming standard in radiation oncology clinics. Dynamic conformal therapy with multileaf collimators is being used routinely in hospitals around the country. With this approach, collimators conform to the tumor volume with the beam on while the treatment unit is PRINCIPLES OF RADIATION THERAPY 17
10 rotating around the patient. This is an example of totally computer-controlled radiation delivery. Another method of IMRT delivery serial tomotherapy is an enhancement of the method described above. An accelerator is equipped with mini-multileaf collimators that form a slit of radiation (normally 2 20 cm). The gantry is rotated through an entire arc around the patient while the mini-multileaf collimators are driven in and out of the field, thus modulating the intensity of the beam. The treatment couch is advanced by a few millimeters and the next arc is treated. An entire treatment is given once all the adjoining arcs have been delivered. Instead of treating the patient on a normal linear accelerator, with helical tomotherapy the patient travels continuously through a modified CT ring. This CT ring has the capability of administering 6-mV x-rays, as in a standard linear accelerator, while at the same time performing a conventional diagnostic CT scan. Any anatomic or position changes that might require replanning can be performed before that day s treatment. Following treatment, a daily, real-time image of the dose distribution can be obtained. PROTON THERAPY Protons, a form of particulate radiation, have been investigated recently as a means to improve tumor control. A proton has a charge of +1, is a stable particle, and, together with the neutron, makes up the atomic nucleus. Protons are delivered to the tumor in the same manner as are photons and electrons. The dose deposited by protons remains relatively constant as they travel through the normal tissues proximal to the target. The kinetic energy of the protons is transferred to the tumors by electrons knocked out of atoms. These electrons ionize DNA, and their biological effectiveness resembles that of megavoltage photons. Bragg peak At the end of the path, biological effectiveness increases sharply as the protons slow down and eventually stop. This increase in dose is called the Bragg peak. The size of the Bragg peak is usually smaller than the tumor, however. This problem can be resolved by scanning the Bragg peak through the tumor volume by sequentially irradiating the target with lower energies. The dose falloff of the Bragg peak is sharp enough that the normal tissues distal to the tumor receive a negligible radiation dose. Current clinical applications Uveal melanomas and skull-base sarcomas adjacent to CNS tissues are two areas that have been under clinical study with promising results. Clinical studies have also begun recently in treating non small-cell lung, hepatocellular, and paranasal sinus carcinomas. STEREOTACTIC RADIOSURGERY Stereotactic radiosurgery is a 3D technique that delivers the radiation dose in one fraction. Specially designed collimators are attached to a linear accelerator, which delivers a high dose of radiation to a small volume, usually about 18 CANCER MANAGEMENT: A MULTIDISCIPLINARY APPROACH
11 3 cm in diameter. Several stationary beams or multiple arc rotations concentrate the radiation dose to the lesion while sparing surrounding normal tissue. Use in treating arteriovenous malformations Stereotactic radiosurgery is used to treat certain patients with arteriovenous malformations. These intracranial lesions arise from the abnormal development of arteries and venous sinuses. Surgical excision is the standard treatment of choice for operable lesions, but stereotactic radiosurgery has become a viable option for inoperable malformations. Use in treating brain tumors As with conformal radiotherapy, clinical trials involving stereotactic radiosurgery for brain tumors are being conducted at major cancer centers. However, based on positive early results, many community centers have begun instituting a stereotactic radiosurgery program, either with a dedicated cobalt unit (gamma knife) or a linear accelerator based system. Small (< 4 cm) tumors of the brain, whether primary, metastatic, or recurrent, may benefit from this treatment technique. SUGGESTED READING Coia LR, Schultheiss TE, Hanks GE: A Practical Guide to CT Simulation. Madison, Wisconsin, Advanced Medical Publishing, IMRT CWG: Intensity modulated radiotherapy: Current status and issues of interest. Int J Radiat Biol Phys 51: , Khan FM: Treatment Planning in Radiation Oncology. Baltimore, Maryland, Williams & Wilkins, Perez CA, Brady LW: Principles and Practice of Radiation Oncology. Philadelphia, Lippincott-Raven, Suit H: The Gray Lecture: Coming technical advances in radiation oncology. Int J Radiat Biol Phys 53: , Van Dyk J: The Modern Technology of Radiation Oncology. Madison, Wisconsin, Medical Physics Publishing, PRINCIPLES OF RADIATION THERAPY 19
Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment.
 Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Basic Radiation Therapy Terms
 Basic Radiation Therapy Terms accelerated radiation: radiation schedule in which the total dose is given over a shorter period of time. (Compare to hyperfractionated radiation.) adjuvant therapy (add-joo-vunt):
Basic Radiation Therapy Terms accelerated radiation: radiation schedule in which the total dose is given over a shorter period of time. (Compare to hyperfractionated radiation.) adjuvant therapy (add-joo-vunt):
NIA RADIATION ONCOLOGY CODING STANDARD. Dosimetry Planning
 NIA RADIATION ONCOLOGY CODING STANDARD Dosimetry Planning CPT Codes: 77295, 77300, 77301, 77306, 77307, 77321, 77316, 77317, 77318, 77331, 77399 Original Date: April, 2011 Last Reviewed Date: November,
NIA RADIATION ONCOLOGY CODING STANDARD Dosimetry Planning CPT Codes: 77295, 77300, 77301, 77306, 77307, 77321, 77316, 77317, 77318, 77331, 77399 Original Date: April, 2011 Last Reviewed Date: November,
1. Orthovoltage vs. megavoltage x-rays. (AL) External beam radiation sources: Orthovoltage radiotherapy: 200-500 kv range
 1. Orthovoltage vs. megavoltage x-rays. (AL) External beam radiation sources: Orthovoltage radiotherapy: 200-500 kv range The radiation from orthovoltage units is referred to as x-rays, generated by bombarding
1. Orthovoltage vs. megavoltage x-rays. (AL) External beam radiation sources: Orthovoltage radiotherapy: 200-500 kv range The radiation from orthovoltage units is referred to as x-rays, generated by bombarding
INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS
 INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS HOW DOES RADIATION THERAPY WORK? Cancer is the unrestrained growth of abnormal cells within the body. Radiation therapy kills both
INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS HOW DOES RADIATION THERAPY WORK? Cancer is the unrestrained growth of abnormal cells within the body. Radiation therapy kills both
HADRON THERAPY FOR CANCER TREATMENT
 HADRON THERAPY FOR CANCER TREATMENT Seminar presented by Arlene Lennox at Fermilab on Nov 21, 2003 CANCER STAGES LOCAL TUMOR REGIONAL METASTASIS SYSTEMIC DISEASE CANCER TREATMENT SURGERY RADIATION THERAPY
HADRON THERAPY FOR CANCER TREATMENT Seminar presented by Arlene Lennox at Fermilab on Nov 21, 2003 CANCER STAGES LOCAL TUMOR REGIONAL METASTASIS SYSTEMIC DISEASE CANCER TREATMENT SURGERY RADIATION THERAPY
Understanding brachytherapy
 Understanding brachytherapy Brachytherapy Cancer Treatment Legacy Cancer Institute Your health care provider has requested that you receive a type of radiation treatment called brachytherapy as part of
Understanding brachytherapy Brachytherapy Cancer Treatment Legacy Cancer Institute Your health care provider has requested that you receive a type of radiation treatment called brachytherapy as part of
RADIATION THERAPY IN THE MANAGEMENT OF CANCER
 RADIATION THERAPY IN THE MANAGEMENT OF CANCER G K Rath Introduction Radiotherapy or radiation treatment is defined as the treatment of diseases (mostly malignant) with ionizing radiation. The various types
RADIATION THERAPY IN THE MANAGEMENT OF CANCER G K Rath Introduction Radiotherapy or radiation treatment is defined as the treatment of diseases (mostly malignant) with ionizing radiation. The various types
Proton Therapy: Cutting Edge Treatment for Cancerous Tumors. By: Cherilyn G. Murer, JD, CRA
 Proton Therapy: Cutting Edge Treatment for Cancerous Tumors By: Cherilyn G. Murer, JD, CRA Introduction Put simply, proton therapy is a new cutting edge cancer treatment that promises better outcomes for
Proton Therapy: Cutting Edge Treatment for Cancerous Tumors By: Cherilyn G. Murer, JD, CRA Introduction Put simply, proton therapy is a new cutting edge cancer treatment that promises better outcomes for
Intensity-Modulated Radiation Therapy (IMRT)
 Scan for mobile link. Intensity-Modulated Radiation Therapy (IMRT) Intensity-modulated radiotherapy (IMRT) uses linear accelerators to safely and painlessly deliver precise radiation doses to a tumor while
Scan for mobile link. Intensity-Modulated Radiation Therapy (IMRT) Intensity-modulated radiotherapy (IMRT) uses linear accelerators to safely and painlessly deliver precise radiation doses to a tumor while
MVP/Care Core National 2015 Radiation Therapy Prior Authorization List (Effective January 1, 2015)
 MVP/Care Core National 2015 Radiation Therapy Prior Authorization List (Effective January 1, 2015) CODE CODE TYPE Description 0330 REVCODE RADIOLOGY/THERAPEUTIC - GENERAL CLASSIFICATION 0333 REVCODE RADIOLOGY/THERAPEUTIC
MVP/Care Core National 2015 Radiation Therapy Prior Authorization List (Effective January 1, 2015) CODE CODE TYPE Description 0330 REVCODE RADIOLOGY/THERAPEUTIC - GENERAL CLASSIFICATION 0333 REVCODE RADIOLOGY/THERAPEUTIC
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
Proton Therapy. What is proton therapy and how is it used?
 Scan for mobile link. Proton Therapy Proton therapy delivers radiation to tumor tissue in a much more confined way than conventional photon therapy thus allowing the radiation oncologist to use a greater
Scan for mobile link. Proton Therapy Proton therapy delivers radiation to tumor tissue in a much more confined way than conventional photon therapy thus allowing the radiation oncologist to use a greater
Corporate Medical Policy
 Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of Head and Neck File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_head_and_neck
Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of Head and Neck File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_head_and_neck
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
PRINIPLES OF RADIATION THERAPY Adarsh Kumar. The basis of radiation therapy revolve around the principle that ionizing radiations kill cells
 PRINIPLES OF RADIATION THERAPY Adarsh Kumar The basis of radiation therapy revolve around the principle that ionizing radiations kill cells Radiotherapy terminology: a. Radiosensitivity: refers to susceptibility
PRINIPLES OF RADIATION THERAPY Adarsh Kumar The basis of radiation therapy revolve around the principle that ionizing radiations kill cells Radiotherapy terminology: a. Radiosensitivity: refers to susceptibility
Department of Radiation Oncology
 Department of Radiation Oncology Welcome to Radiation Oncology at Emory Clinic Every member of Emory Clinic Department of Radiation Oncology strives to provide the highest quality of care for you as our
Department of Radiation Oncology Welcome to Radiation Oncology at Emory Clinic Every member of Emory Clinic Department of Radiation Oncology strives to provide the highest quality of care for you as our
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate
 Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
IGRT. IGRT can increase the accuracy by locating the target volume before and during the treatment.
 DERYA ÇÖNE RADIOTHERAPY THERAPIST ACIBADEM KOZYATAGI HOSPITAL RADIATION ONCOLOGY DEPARTMENT IGRT IGRT (image-guided radiation therapy) is a technique that reduces geometric uncertainties by considering
DERYA ÇÖNE RADIOTHERAPY THERAPIST ACIBADEM KOZYATAGI HOSPITAL RADIATION ONCOLOGY DEPARTMENT IGRT IGRT (image-guided radiation therapy) is a technique that reduces geometric uncertainties by considering
First Three Years After Project Proton Therapy Facility:
 39. Project Related Utilization and Financial Information. Proton Therapy Facility: Unit of Service Delivery Projected Utilization FY2017 FY2018 FY2019 Estimated Patients 448 670 808 Average Revenue Per
39. Project Related Utilization and Financial Information. Proton Therapy Facility: Unit of Service Delivery Projected Utilization FY2017 FY2018 FY2019 Estimated Patients 448 670 808 Average Revenue Per
Radiation Therapy for Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Radiation Therapy for
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Radiation Therapy for
ACCELERATORS AND MEDICAL PHYSICS 2
 ACCELERATORS AND MEDICAL PHYSICS 2 Ugo Amaldi University of Milano Bicocca and TERA Foundation EPFL 2-28.10.10 - U. Amaldi 1 The icone of radiation therapy Radiation beam in matter EPFL 2-28.10.10 - U.
ACCELERATORS AND MEDICAL PHYSICS 2 Ugo Amaldi University of Milano Bicocca and TERA Foundation EPFL 2-28.10.10 - U. Amaldi 1 The icone of radiation therapy Radiation beam in matter EPFL 2-28.10.10 - U.
Baylor Radiosurgery Center
 Radiosurgery Center Baylor Radiosurgery Center Sophisticated Radiosurgery for both Brain and Body University Medical Center at Dallas Radiosurgery Center 3500 Gaston Avenue Hoblitzelle Hospital, First
Radiosurgery Center Baylor Radiosurgery Center Sophisticated Radiosurgery for both Brain and Body University Medical Center at Dallas Radiosurgery Center 3500 Gaston Avenue Hoblitzelle Hospital, First
Production of X-rays. Radiation Safety Training for Analytical X-Ray Devices Module 9
 Module 9 This module presents information on what X-rays are and how they are produced. Introduction Module 9, Page 2 X-rays are a type of electromagnetic radiation. Other types of electromagnetic radiation
Module 9 This module presents information on what X-rays are and how they are produced. Introduction Module 9, Page 2 X-rays are a type of electromagnetic radiation. Other types of electromagnetic radiation
HDR Brachytherapy 1: Overview of QA. Disclosures: Learning Objectives 7/23/2014
 HDR Brachytherapy 1: Overview of QA Bruce Libby Department of Radiation Oncology University of Virginia Health System Disclosures: Nondisclosure agreement with Varian Brachytherapy Shareholder- Varian,
HDR Brachytherapy 1: Overview of QA Bruce Libby Department of Radiation Oncology University of Virginia Health System Disclosures: Nondisclosure agreement with Varian Brachytherapy Shareholder- Varian,
Production of X-rays and Interactions of X-rays with Matter
 Production of X-rays and Interactions of X-rays with Matter Goaz and Pharoah. Pages 11-20. Neill Serman Electrons traveling from the filament ( cathode) to the target (anode) convert a small percentage
Production of X-rays and Interactions of X-rays with Matter Goaz and Pharoah. Pages 11-20. Neill Serman Electrons traveling from the filament ( cathode) to the target (anode) convert a small percentage
Radiation Oncology Centers Participating in MassHealth. Daniel Tsai, Assistant Secretary and Director of MassHealth
 Executive Office of Health and Human s Office of Medicaid www.mass.gov/masshealth May 2015 TO: FROM: RE: Radiation Oncology Centers Participating in Daniel Tsai, Assistant Secretary and Director of (2015
Executive Office of Health and Human s Office of Medicaid www.mass.gov/masshealth May 2015 TO: FROM: RE: Radiation Oncology Centers Participating in Daniel Tsai, Assistant Secretary and Director of (2015
Horizon Blue Cross Blue Shield of New Jersey 2012 Radiation Therapy Payment Rules
 55875 55876 55876 Description Transperineal placement of needles or catheters into prostate for interstitial radioelement application, with or wout cytosocopy 55920 Placement of interstitial device(s)
55875 55876 55876 Description Transperineal placement of needles or catheters into prostate for interstitial radioelement application, with or wout cytosocopy 55920 Placement of interstitial device(s)
1. Provide clinical training in radiation oncology physics within a structured clinical environment.
 Medical Physics Residency Program Overview Our Physics Residency Training is a 2 year program typically beginning July 1 each year. The first year resident will work closely with medical physicists responsible
Medical Physics Residency Program Overview Our Physics Residency Training is a 2 year program typically beginning July 1 each year. The first year resident will work closely with medical physicists responsible
MEDICAL DOSIMETRY. COLLEGE OF APPLIED SCIENCES AND ARTS Graduate Faculty: therapy.
 Graduate Catalog 2012-2013 Medical Dosimetry / 339 MEDICAL DOSIMETRY COLLEGE OF APPLIED SCIENCES AND ARTS Graduate Faculty: Collins, Kevin Scott, Associate Professor, Ph.D., Jensen, Steve, Emeritus Professor,
Graduate Catalog 2012-2013 Medical Dosimetry / 339 MEDICAL DOSIMETRY COLLEGE OF APPLIED SCIENCES AND ARTS Graduate Faculty: Collins, Kevin Scott, Associate Professor, Ph.D., Jensen, Steve, Emeritus Professor,
Clinical Physics. Dr/Aida Radwan Assistant Professor of Medical Physics Umm El-Qura University
 Clinical Physics Dr/Aida Radwan Assistant Professor of Medical Physics Umm El-Qura University Physics of Radiotherapy using External Beam Dose distribution PHANTOMS Basic dose distribution data are usually
Clinical Physics Dr/Aida Radwan Assistant Professor of Medical Physics Umm El-Qura University Physics of Radiotherapy using External Beam Dose distribution PHANTOMS Basic dose distribution data are usually
Chapter 7: Clinical Treatment Planning in External Photon Beam Radiotherapy
 Chapter 7: Clinical Treatment Planning in External Photon Beam Radiotherapy Set of 232 slides based on the chapter authored by W. Parker, H. Patrocinio of the IAEA publication (ISBN 92-0-107304-6): Review
Chapter 7: Clinical Treatment Planning in External Photon Beam Radiotherapy Set of 232 slides based on the chapter authored by W. Parker, H. Patrocinio of the IAEA publication (ISBN 92-0-107304-6): Review
Seminar 7. Medical application of radioisotopes - radiotherapy
 Seminar 7 Medical application of radioisotopes - radiotherapy Radioisotopes in medical diagnosis. Gamma camera. Radionuclide imaging (PET, SPECT). Radiotherapy. Sources of radiation. Treatment planning.
Seminar 7 Medical application of radioisotopes - radiotherapy Radioisotopes in medical diagnosis. Gamma camera. Radionuclide imaging (PET, SPECT). Radiotherapy. Sources of radiation. Treatment planning.
A Patient s Guide to the Calypso System for Breast Cancer Treatment
 A Patient s Guide to the Calypso System for Breast Cancer Treatment Contents Introduction How Radiation Works To Treat Cancer Radiation Treatment for Breast Cancer Special Concerns for Treating the Left
A Patient s Guide to the Calypso System for Breast Cancer Treatment Contents Introduction How Radiation Works To Treat Cancer Radiation Treatment for Breast Cancer Special Concerns for Treating the Left
at a critical moment Physician Suggestion Line...
 Radiation Oncology Exceptional care at a critical moment When your patients require radiation therapy, they deserve the very best care available to them. The Department of Radiation Oncology provides exceptional
Radiation Oncology Exceptional care at a critical moment When your patients require radiation therapy, they deserve the very best care available to them. The Department of Radiation Oncology provides exceptional
There must be an appropriate administrative structure for each residency program.
 Specific Standards of Accreditation for Residency Programs in Radiation Oncology 2015 VERSION 3.0 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation
Specific Standards of Accreditation for Residency Programs in Radiation Oncology 2015 VERSION 3.0 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
What is the CyberKnife System?
 CYBERKNIFE Robotic Radiosurgery System PATIENT BROChURE 1 What is the CyberKnife System? have stabilizing frames bolted to their head or limit their breathing during treatment to minimize movement of the
CYBERKNIFE Robotic Radiosurgery System PATIENT BROChURE 1 What is the CyberKnife System? have stabilizing frames bolted to their head or limit their breathing during treatment to minimize movement of the
RADIATION THERAPY guide. Guiding you through your treatment
 RADIATION THERAPY guide Guiding you through your treatment 2013_RADIATION_GUIDE_6PG.indd 1 Before Treatment Consultation with the Radiation Oncologist During your first visit with the radiation oncologist,
RADIATION THERAPY guide Guiding you through your treatment 2013_RADIATION_GUIDE_6PG.indd 1 Before Treatment Consultation with the Radiation Oncologist During your first visit with the radiation oncologist,
The effects of radiation on the body can be divided into Stochastic (random) effects and deterministic or Non-stochastic effects.
 RADIATION SAFETY: HOW TO EDUCATE AND PROTECT YOURSELF AND YOUR STAFF John Farrelly, DVM, MS, ACVIM (Oncology), ACVR (Radiation Oncology) Cornell University Veterinary Specialists The Veterinary Cancer
RADIATION SAFETY: HOW TO EDUCATE AND PROTECT YOURSELF AND YOUR STAFF John Farrelly, DVM, MS, ACVIM (Oncology), ACVR (Radiation Oncology) Cornell University Veterinary Specialists The Veterinary Cancer
Radiation Therapy Coverage, Coding, and Reimbursement for New Technologies
 Radiation Therapy Coverage, Coding, and Reimbursement for New Technologies Presented by Susan Granucci, Healthcare Reimbursement Specialist Topics 1. Intensity Modulated Radiation Therapy (IMRT) 2. Tomotherapy
Radiation Therapy Coverage, Coding, and Reimbursement for New Technologies Presented by Susan Granucci, Healthcare Reimbursement Specialist Topics 1. Intensity Modulated Radiation Therapy (IMRT) 2. Tomotherapy
Analysis of Set-up Errors during CT-scan, Simulation, and Treatment Process in Breast Cancer Patients
 대한방사선종양학회지 2005;23(3):169~175 Analysis of Set-up Errors during CT-scan, Simulation, and Treatment Process in Breast Cancer Patients Department of Radiation Oncology, College of Medicine, Ewha Womans University
대한방사선종양학회지 2005;23(3):169~175 Analysis of Set-up Errors during CT-scan, Simulation, and Treatment Process in Breast Cancer Patients Department of Radiation Oncology, College of Medicine, Ewha Womans University
Introduction to Radiation Oncology
 Editors: Abigail T. Berman, MD, University of Pennsylvania Jordan Kharofa, MD, Medical College of Wisconsin Introduction to Radiation Oncology What Every Medical Student Needs to Know Objectives Introduction
Editors: Abigail T. Berman, MD, University of Pennsylvania Jordan Kharofa, MD, Medical College of Wisconsin Introduction to Radiation Oncology What Every Medical Student Needs to Know Objectives Introduction
Atomic and Nuclear Physics Laboratory (Physics 4780)
 Gamma Ray Spectroscopy Week of September 27, 2010 Atomic and Nuclear Physics Laboratory (Physics 4780) The University of Toledo Instructor: Randy Ellingson Gamma Ray Production: Co 60 60 60 27Co28Ni *
Gamma Ray Spectroscopy Week of September 27, 2010 Atomic and Nuclear Physics Laboratory (Physics 4780) The University of Toledo Instructor: Randy Ellingson Gamma Ray Production: Co 60 60 60 27Co28Ni *
The Canadian National System for Incident Reporting in Radiation Treatment (NSIR-RT) Taxonomy March 2, 2015 V2
 The Canadian National System for Incident Reporting in Radiation Treatment (NSIR-RT) Taxonomy March 2, 2015 V2 Taxonomy Data Category Number Description Data Fields and Menu Choices 1. Impact 1.1 Incident
The Canadian National System for Incident Reporting in Radiation Treatment (NSIR-RT) Taxonomy March 2, 2015 V2 Taxonomy Data Category Number Description Data Fields and Menu Choices 1. Impact 1.1 Incident
GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision
 RADIATION THERAPY FOR GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT GYNECOLOGIC CANCERS Gynecologic cancers
RADIATION THERAPY FOR GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT GYNECOLOGIC CANCERS Gynecologic cancers
Feasibility Study of Neutron Dose for Real Time Image Guided. Proton Therapy: A Monte Carlo Study
 Feasibility Study of Neutron Dose for Real Time Image Guided Proton Therapy: A Monte Carlo Study Jin Sung Kim, Jung Suk Shin, Daehyun Kim, EunHyuk Shin, Kwangzoo Chung, Sungkoo Cho, Sung Hwan Ahn, Sanggyu
Feasibility Study of Neutron Dose for Real Time Image Guided Proton Therapy: A Monte Carlo Study Jin Sung Kim, Jung Suk Shin, Daehyun Kim, EunHyuk Shin, Kwangzoo Chung, Sungkoo Cho, Sung Hwan Ahn, Sanggyu
Goals and Objectives: Breast Cancer Service Department of Radiation Oncology
 Goals and Objectives: Breast Cancer Service Department of Radiation Oncology The breast cancer service provides training in the diagnosis, management, treatment, and follow-up of breast malignancies, including
Goals and Objectives: Breast Cancer Service Department of Radiation Oncology The breast cancer service provides training in the diagnosis, management, treatment, and follow-up of breast malignancies, including
Prostate Cancer Treatment
 Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Our Facility. Advanced clinical center with the newest and highly exact technology for treatment of patients with cancer pencil beam
 PTC Czech The main goal of radiotherapy is to irreversibly damage tumor cells, whereas the cells of healthy tissue are damaged only reversibly or not at all. Proton therapy currently comes closest to this
PTC Czech The main goal of radiotherapy is to irreversibly damage tumor cells, whereas the cells of healthy tissue are damaged only reversibly or not at all. Proton therapy currently comes closest to this
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER
 BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
Comparison of Medical and DOE Health Physics Programs. Kevin Lee Radiation Safety Officer Palmetto Health
 Comparison of Medical and DOE Health Physics Programs Kevin Lee Radiation Safety Officer Palmetto Health Objectives To understand basic medical use of radiation producing equipment and radioactive materials.
Comparison of Medical and DOE Health Physics Programs Kevin Lee Radiation Safety Officer Palmetto Health Objectives To understand basic medical use of radiation producing equipment and radioactive materials.
Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required]
![Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required] Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required]](/thumbs/33/16383859.jpg) Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required] Medical Policy: MP-SU-01-11 Original Effective Date: February 24, 2011 Reviewed: February 24, 2012 Revised:
Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required] Medical Policy: MP-SU-01-11 Original Effective Date: February 24, 2011 Reviewed: February 24, 2012 Revised:
PROTON THERAPY FREQUENTLY ASKED QUESTIONS
 PROTON THERAPY FREQUENTLY ASKED QUESTIONS Table of contents 1. What is cancer?... 2 2. How is cancer treated?... 3 3. What is proton therapy?... 4 4. What are the clinical benefits of proton therapy?...
PROTON THERAPY FREQUENTLY ASKED QUESTIONS Table of contents 1. What is cancer?... 2 2. How is cancer treated?... 3 3. What is proton therapy?... 4 4. What are the clinical benefits of proton therapy?...
Current Status and Future Direction of Proton Beam Therapy
 Current Status and Future Direction of Proton Beam Therapy National Cancer Center Hospital East Division of Radiation Oncology and Particle Therapy Tetsuo Akimoto Comparison of status of particle therapy
Current Status and Future Direction of Proton Beam Therapy National Cancer Center Hospital East Division of Radiation Oncology and Particle Therapy Tetsuo Akimoto Comparison of status of particle therapy
Basics of Nuclear Physics and Fission
 Basics of Nuclear Physics and Fission A basic background in nuclear physics for those who want to start at the beginning. Some of the terms used in this factsheet can be found in IEER s on-line glossary.
Basics of Nuclear Physics and Fission A basic background in nuclear physics for those who want to start at the beginning. Some of the terms used in this factsheet can be found in IEER s on-line glossary.
Accelerated Partial Breast Irradiation (APBI) for Breast Cancer
 Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [For the list of services and procedures that need preauthorization, please refer to www.mcs.pr Go to Comunicados a Proveedores, and click
Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [For the list of services and procedures that need preauthorization, please refer to www.mcs.pr Go to Comunicados a Proveedores, and click
Corporate Medical Policy
 Corporate Medical Policy Intensity Modulated Radiation Therapy for Tumors of the Central File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_for_tumors
Corporate Medical Policy Intensity Modulated Radiation Therapy for Tumors of the Central File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_for_tumors
WELCOME. Massachusetts General Hospital Cancer Center
 Massachusetts General Hospital Cancer Center Department of Radiation Oncology 55 Fruit Street Boston, MA 02114 (617) 726-8650 www.massgeneral.org/cancer PROTON RADIOSURGERY Teresa M. McCue August Morning
Massachusetts General Hospital Cancer Center Department of Radiation Oncology 55 Fruit Street Boston, MA 02114 (617) 726-8650 www.massgeneral.org/cancer PROTON RADIOSURGERY Teresa M. McCue August Morning
intensity_modulated_radiation_therapy_imrt_of_abdomen_and_pelvis 11/2009 5/2016 5/2017 5/2016
 Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of Abdomen File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_abdomen_and_pelvis
Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of Abdomen File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_abdomen_and_pelvis
A SAFE, NON-INVASIVE TREATMENT OPTION: GAMMA KNIFE PERFEXION
 A SAFE, NON-INVASIVE TREATMENT OPTION: GAMMA KNIFE PERFEXION Not actually a knife, the Gamma Knife Perfexion is an advanced radiosurgery device which uses extremely precise beams of radiation to treat
A SAFE, NON-INVASIVE TREATMENT OPTION: GAMMA KNIFE PERFEXION Not actually a knife, the Gamma Knife Perfexion is an advanced radiosurgery device which uses extremely precise beams of radiation to treat
TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software.
 SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
Total Solutions. Best NOMOS One Best Drive, Pittsburgh, PA 15202 USA phone 412 312 6700 800 70 NOMOS www.nomos.com
 Serial Tomotherapy IGRT Total Solutions Treatment Planning Brachytherapy Imaging Best NOMOS One Best Drive, Pittsburgh, PA 15202 USA BMI.v.08.2010 Best NOMOS Your Single Source Oncology Solutions Provider
Serial Tomotherapy IGRT Total Solutions Treatment Planning Brachytherapy Imaging Best NOMOS One Best Drive, Pittsburgh, PA 15202 USA BMI.v.08.2010 Best NOMOS Your Single Source Oncology Solutions Provider
Quality Assurance of Radiotherapy Equipment
 Clinical Implementation of Technology & Quality Assurance in Radiation Oncology For the course: Survey of Clinical Radiation Oncology 1 Quality Assurance of Radiotherapy Equipment Outline: A. Criteria
Clinical Implementation of Technology & Quality Assurance in Radiation Oncology For the course: Survey of Clinical Radiation Oncology 1 Quality Assurance of Radiotherapy Equipment Outline: A. Criteria
Patient Guide. Brachytherapy: The precise answer for tackling breast cancer. Because life is for living
 Patient Guide Brachytherapy: The precise answer for tackling breast cancer Because life is for living This booklet is designed to provide information that helps women who have been diagnosed with early
Patient Guide Brachytherapy: The precise answer for tackling breast cancer Because life is for living This booklet is designed to provide information that helps women who have been diagnosed with early
X-ray Production. Target Interactions. Principles of Imaging Science I (RAD119) X-ray Production & Emission
 Principles of Imaging Science I (RAD119) X-ray Production & Emission X-ray Production X-rays are produced inside the x-ray tube when high energy projectile electrons from the filament interact with the
Principles of Imaging Science I (RAD119) X-ray Production & Emission X-ray Production X-rays are produced inside the x-ray tube when high energy projectile electrons from the filament interact with the
An Overview of Radiation Therapy
 An Overview of Radiation Therapy Guest Expert: Lynn, MD, MPH Professor and Vice Chairman, Department of Therapeutic Radiology, Yale School of Medicine www.wnpr.org www.yalecancercenter.org Welcome to Yale
An Overview of Radiation Therapy Guest Expert: Lynn, MD, MPH Professor and Vice Chairman, Department of Therapeutic Radiology, Yale School of Medicine www.wnpr.org www.yalecancercenter.org Welcome to Yale
Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Preauthorization Required]
![Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Preauthorization Required] Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Preauthorization Required]](/thumbs/33/16383903.jpg) Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Preauthorization Required] Medical Policy: MP-SU-01-11 Original Effective Date: February 24, 2011 Reviewed: Revised: This policy applies
Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Preauthorization Required] Medical Policy: MP-SU-01-11 Original Effective Date: February 24, 2011 Reviewed: Revised: This policy applies
AMERICAN BRAIN TUMOR ASSOCIATION. Proton Therapy
 AMERICAN BRAIN TUMOR ASSOCIATION Proton Therapy Acknowledgements About the American Brain Tumor Association Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit
AMERICAN BRAIN TUMOR ASSOCIATION Proton Therapy Acknowledgements About the American Brain Tumor Association Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit
RADIATION THERAPY FOR BRAIN METASTASES. Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY
 RADIATION THERAPY FOR BRAIN METASTASES Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT BRAIN METASTASIS Brain metastases are clusters
RADIATION THERAPY FOR BRAIN METASTASES Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT BRAIN METASTASIS Brain metastases are clusters
The Science behind Proton Beam Therapy
 The Science behind Proton Beam Therapy Anthony Zietman MD Shipley Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School Principles underlying Radiotherapy Radiation related
The Science behind Proton Beam Therapy Anthony Zietman MD Shipley Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School Principles underlying Radiotherapy Radiation related
Brachytherapy of the Uterine Corpus: Some Physical Considerations. Bruce Thomadsen. University of Wisconsin -Madison
 Brachytherapy of the Uterine Corpus: Some Physical Considerations Bruce Thomadsen University of Wisconsin -Madison Conflicts of Interest The author has no known conflicts involving this presentation Learning
Brachytherapy of the Uterine Corpus: Some Physical Considerations Bruce Thomadsen University of Wisconsin -Madison Conflicts of Interest The author has no known conflicts involving this presentation Learning
Radiographic Grid. Principles of Imaging Science II (RAD 120) Image-Forming X-Rays. Radiographic Grids
 Principles of Imaging Science II (RAD 120) Radiographic Grids 1 Image-Forming X-Rays Four X-ray paths a. X-rays interact with patient and scatter away from the receptor b. X-rays interact and are absorbed
Principles of Imaging Science II (RAD 120) Radiographic Grids 1 Image-Forming X-Rays Four X-ray paths a. X-rays interact with patient and scatter away from the receptor b. X-rays interact and are absorbed
Prostate Cancer. What is prostate cancer?
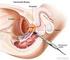 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
RADIATION THERAPY FOR BLADDER CANCER. Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY
 RADIATION THERAPY FOR Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT The bladder is located in the pelvis. It collects and stores
RADIATION THERAPY FOR Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT The bladder is located in the pelvis. It collects and stores
World-first Proton Pencil Beam Scanning System with FDA Clearance
 Hitachi Review Vol. 58 (29), No.5 225 World-first Proton Pencil Beam Scanning System with FDA Clearance Completion of Proton Therapy System for MDACC Koji Matsuda Hiroyuki Itami Daishun Chiba Kazuyoshi
Hitachi Review Vol. 58 (29), No.5 225 World-first Proton Pencil Beam Scanning System with FDA Clearance Completion of Proton Therapy System for MDACC Koji Matsuda Hiroyuki Itami Daishun Chiba Kazuyoshi
Accreditation a tool to help reduce medical errors. Professor Arthur T Porter PC MD FACR FRCPC FACRO
 Accreditation a tool to help reduce medical errors Professor Arthur T Porter PC MD FACR FRCPC FACRO Errors in Radiotherapy Radiation therapy is a highly regulated medical practice with historically low
Accreditation a tool to help reduce medical errors Professor Arthur T Porter PC MD FACR FRCPC FACRO Errors in Radiotherapy Radiation therapy is a highly regulated medical practice with historically low
Janusz Skowronek MD, PhD
 Janusz Skowronek MD, PhD Greatpoland Cancer Center Pozna, January 2004 1 1. About Brachytherapy Derived from ancient Greek words for short distance (brachios) and treatment (therapy) and refers to the
Janusz Skowronek MD, PhD Greatpoland Cancer Center Pozna, January 2004 1 1. About Brachytherapy Derived from ancient Greek words for short distance (brachios) and treatment (therapy) and refers to the
Radiation Therapy for Prostate Cancer: Treatment options and future directions
 Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
............... [2] At the time of purchase of a Strontium-90 source, the activity is 3.7 10 6 Bq.
![............... [2] At the time of purchase of a Strontium-90 source, the activity is 3.7 10 6 Bq. ............... [2] At the time of purchase of a Strontium-90 source, the activity is 3.7 10 6 Bq.](/thumbs/40/21837699.jpg) 1 Strontium-90 decays with the emission of a β-particle to form Yttrium-90. The reaction is represented by the equation 90 38 The decay constant is 0.025 year 1. 90 39 0 1 Sr Y + e + 0.55 MeV. (a) Suggest,
1 Strontium-90 decays with the emission of a β-particle to form Yttrium-90. The reaction is represented by the equation 90 38 The decay constant is 0.025 year 1. 90 39 0 1 Sr Y + e + 0.55 MeV. (a) Suggest,
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
RADIATION THERAPY & CANCER
 CANCERCARE MANITOBA Mission Statement CancerCare Manitoba, by an act of the legislature, is responsible for cancer prevention, detection, care, research and education throughout Manitoba. RADIATION THERAPY
CANCERCARE MANITOBA Mission Statement CancerCare Manitoba, by an act of the legislature, is responsible for cancer prevention, detection, care, research and education throughout Manitoba. RADIATION THERAPY
Non-coronary Brachytherapy
 Non-coronary Brachytherapy I. Policy University Health Alliance (UHA) will reimburse for non-coronary brachytherapy when it is determined to be medically necessary and when it meets the medical criteria
Non-coronary Brachytherapy I. Policy University Health Alliance (UHA) will reimburse for non-coronary brachytherapy when it is determined to be medically necessary and when it meets the medical criteria
Chapter 7 CLINICAL TREATMENT PLANNING IN EXTERNAL PHOTON BEAM RADIOTHERAPY
 Chapter 7 CLINICAL TREATMENT PLANNING IN EXTERNAL PHOTON BEAM RADIOTHERAPY W. PARKER, H. PATROCINIO Department of Medical Physics, McGill University Health Centre, Montreal, Quebec, Canada 7.1. INTRODUCTION
Chapter 7 CLINICAL TREATMENT PLANNING IN EXTERNAL PHOTON BEAM RADIOTHERAPY W. PARKER, H. PATROCINIO Department of Medical Physics, McGill University Health Centre, Montreal, Quebec, Canada 7.1. INTRODUCTION
Gamma Knife and Axesse Radiosurgery
 Gamma Knife and Axesse Radiosurgery John C Flickinger MD Departments of Radiation Oncology & Neurological Surgery University of Pittsburgh School of Medicine Pittsburgh, Pennsylvania Origin of Radiosurgery
Gamma Knife and Axesse Radiosurgery John C Flickinger MD Departments of Radiation Oncology & Neurological Surgery University of Pittsburgh School of Medicine Pittsburgh, Pennsylvania Origin of Radiosurgery
In 1946 Harvard physicist Robert Wilson (1914-2000) suggested:
 In 1946 Harvard physicist Robert Wilson (1914-2000) suggested: Protons can be used clinically Accelerators are available Maximum radiation dose can be placed into the tumor Proton therapy provides sparing
In 1946 Harvard physicist Robert Wilson (1914-2000) suggested: Protons can be used clinically Accelerators are available Maximum radiation dose can be placed into the tumor Proton therapy provides sparing
FEATURE ARTICLE. One precise dose
 FEATURE ARTICLE Medical Physics Team at UNM Cancer Center Expands Treatment Choices From stereotactic radiosurgery to hippocampal-sparing treatment, the medical physics team provides new radiation therapy
FEATURE ARTICLE Medical Physics Team at UNM Cancer Center Expands Treatment Choices From stereotactic radiosurgery to hippocampal-sparing treatment, the medical physics team provides new radiation therapy
Proton Therapy for Prostate Cancer: Your Questions, Our Answers.
 Proton Therapy for Prostate Cancer: Your Questions, Our Answers. When you re looking for the right treatment for your prostate cancer, nothing s more important than accurate information. Read on, and learn
Proton Therapy for Prostate Cancer: Your Questions, Our Answers. When you re looking for the right treatment for your prostate cancer, nothing s more important than accurate information. Read on, and learn
Important Information for Women with Breast Cancer. what lumpectomy
 Important Information for Women with Breast Cancer what lumpectomy begins Your most important decisions MammoSite completes Today, more and more women with early-stage breast cancer are able to treat their
Important Information for Women with Breast Cancer what lumpectomy begins Your most important decisions MammoSite completes Today, more and more women with early-stage breast cancer are able to treat their
Radiation Oncology Nursing Care. Helen Lusby Radiation Oncology Nurse BAROC 2012
 Radiation Oncology Nursing Care Helen Lusby Radiation Oncology Nurse BAROC 2012 Definitions Radiation Therapy: Treatment of cancer using x- ray particles that cause ionisation within the cells. External
Radiation Oncology Nursing Care Helen Lusby Radiation Oncology Nurse BAROC 2012 Definitions Radiation Therapy: Treatment of cancer using x- ray particles that cause ionisation within the cells. External
Radioactivity III: Measurement of Half Life.
 PHY 192 Half Life 1 Radioactivity III: Measurement of Half Life. Introduction This experiment will once again use the apparatus of the first experiment, this time to measure radiation intensity as a function
PHY 192 Half Life 1 Radioactivity III: Measurement of Half Life. Introduction This experiment will once again use the apparatus of the first experiment, this time to measure radiation intensity as a function
Inova. Breast Care Institute
 Inova Breast Care Institute At the Inova Breast Care Institute, our commitment is to provide expert care for you, every step of the way. Our multidisciplinary team of more than 80 experts provides a full
Inova Breast Care Institute At the Inova Breast Care Institute, our commitment is to provide expert care for you, every step of the way. Our multidisciplinary team of more than 80 experts provides a full
THE DOSIMETRIC EFFECTS OF
 THE DOSIMETRIC EFFECTS OF OPTIMIZATION TECHNIQUES IN IMRT/IGRT PLANNING 1 Multiple PTV Head and Neck Treatment Planning, Contouring, Data, Tips, Optimization Techniques, and algorithms AAMD 2013, San Antonio,
THE DOSIMETRIC EFFECTS OF OPTIMIZATION TECHNIQUES IN IMRT/IGRT PLANNING 1 Multiple PTV Head and Neck Treatment Planning, Contouring, Data, Tips, Optimization Techniques, and algorithms AAMD 2013, San Antonio,
Nursing Care of the Patient Receiving Brachytherapy for Gynecologic Cancer
 Nursing Care of the Patient Receiving Brachytherapy for Gynecologic Cancer Una Randall, RN, BSN, OCN Dana Farber / Brigham and Women s Cancer Center Department of Radiation Oncology Una Randall is not
Nursing Care of the Patient Receiving Brachytherapy for Gynecologic Cancer Una Randall, RN, BSN, OCN Dana Farber / Brigham and Women s Cancer Center Department of Radiation Oncology Una Randall is not
Understanding INTRABEAM Intraoperative Radiation Therapy for Breast Cancer A patient guide
 Understanding INTRABEAM Intraoperative Radiation Therapy for Breast Cancer A patient guide A diagnosis of breast cancer is never easy, but today there are more treatment options than ever before. A breast
Understanding INTRABEAM Intraoperative Radiation Therapy for Breast Cancer A patient guide A diagnosis of breast cancer is never easy, but today there are more treatment options than ever before. A breast
Clinical Trials and Radiation Treatment. Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto
 Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
METASTASES TO THE BONE
 RADIATION THERAPY FOR METASTASES TO THE BONE Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY WHAT ARE BONE METASTASES? Cancer that starts
RADIATION THERAPY FOR METASTASES TO THE BONE Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY WHAT ARE BONE METASTASES? Cancer that starts
Proton Therapy for Cancer: A New Technology Brief
 September 8, 2009 Volume 6 / Number 17 A Closer Look This is the second article in a series of stories related to cancer technology. Look for the symbol on the left in an upcoming issue for the next article
September 8, 2009 Volume 6 / Number 17 A Closer Look This is the second article in a series of stories related to cancer technology. Look for the symbol on the left in an upcoming issue for the next article
Proton beam. Medical Technical Complex Joint Institute for Nuclear Research, Dubna, Russia
 Proton beam Medical Technical Complex Joint Institute for Nuclear Research, Dubna, Russia Egyptian Candidates Proton therapy It can do more!!! Effectiveness of the proton therapy in targeting and curing
Proton beam Medical Technical Complex Joint Institute for Nuclear Research, Dubna, Russia Egyptian Candidates Proton therapy It can do more!!! Effectiveness of the proton therapy in targeting and curing
