Management of Genital Herpes in Pregnancy. October 2014
|
|
|
- Bethany Carroll
- 9 years ago
- Views:
Transcription
1 Management of Genital Herpes in Pregnancy October 2014
2 Foley E, larke E, Beckett VA, Harrison S, Pillai A, FitzGerald M, Owen P, Low-Beer N, Patel R. Guideline date: October 2014 Date of review: by 2018 Guideline development group: Elizabeth Foley MB BS BSc FRP FROG (lead author), onsultant in Genitourinary and HIV Medicine, Solent NHS Trust Emily larke BSc BM MSc MRP (UK), ST3 Genitourinary Medicine, Solent NHS Trust Virginia Beckett MB BS BSc FROG (lead author on behalf of ROG), onsultant Obstetrician and Gynaecologist, Bradford Teaching Hospitals NHS Foundation Trust, Honorary Senior Lecturer, University of Bradford Sam Harrison MROG, ST6 Obstetrics and Gynaecology, Bradford Teaching Hospitals NHS Foundation Trust Anil Pillai MRP, onsultant Neonatologist, Bradford Teaching Hospitals NHS Foundation Trust Mark FitzGerald FRP, Lead Editor, BASHH guideline on Management of Genital Herpes (2014), BASHH linical Effectiveness Group, onsultant Physician in Genitourinary Medicine, Musgrove Park Hospital, Taunton Philip Owen MD FROG, hair (to May 2014), ROG Guidelines ommittee, onsultant Obstetrician and Gynaecologist, Princess Royal Maternity, Glasgow Naomi Low-Beer MBBS MD MROG MEd, onsultant Gynaecologist, helsea and Westminster Hospital NHS Foundation Trust, Honorary Senior linical Lecturer, Imperial ollege London Rajul Patel FRP, Senior Lecturer, University of Southampton, onsultant in Genitourinary and HIV Medicine, Solent NHS Trust 2
3 ontents 1. Objective and scope 4 2. Search strategy 5 3. Background 6 4. Management of pregnant women with first episode genital herpes 8 5. Management of pregnant women with recurrent genital herpes Management of women with primary or recurrent genital lesions at the onset of labour Genital herpes in preterm prelabour rupture of membranes 13 (before weeks of gestation) 8. Management of HIV-positive women with HSV infection Management of the neonate Prevention of postnatal transmission Performance measures About this guideline 19 References 21 Appendix I 25 Appendix II 26 What s new in the 2014 Management of Genital Herpes in Pregnancy guideline? This guideline has been written as a consensus guideline between the British Association for Sexual Health and HIV (BASHH) and the Royal ollege of Obstetricians and Gynaecologists (ROG) where previously there were two separate guidelines which in part gave conflicting advice. Stronger recommendation to offer a vaginal delivery to women with recurrent genital herpes in pregnancy. New section on genital herpes in preterm prelabour rupture of membranes. New section on the management of HIV-positive women with genital herpes. Flow chart for management of herpes in mother and neonate (Appendix 1). 3
4 1. Objective and scope In 2007, the British Association for Sexual Health and HIV (BASHH) published its guidance on the management of genital herpes, including a section on management in pregnancy, and the Royal ollege of Obstetricians and Gynaecologists (ROG) published their Green-top Guideline on the management of genital herpes in pregnancy. 1,2 In 2010, a European guideline on the management of genital herpes was published, which included a section on management in pregnancy. 3 In order to achieve consensus, it was decided that a joint BASHH and ROG guideline on the management of herpes in pregnancy should be written to update the previous guidance from the two organisations. For more detailed information on the general management of genital herpes infection in nonpregnant patients, this guideline should be considered in conjunction with the 2014 BASHH guideline on the management of genital herpes (currently undergoing consultation). The scope of this guideline is the inpatient and outpatient management of genital herpes simplex virus infection in the antenatal, intrapartum and postnatal periods. For the prevention of genital herpes infection in uninfected mothers during pregnancy, please see the transmission prevention advice in the 2014 BASHH guideline on the management of genital herpes (currently undergoing consultation). The population covered by this guideline includes pregnant women with a suspected or confirmed diagnosis of genital herpes simplex infection in primary or secondary care. This guideline is aimed at healthcare professionals working in maternity units and departments offering level 3 care in the management of sexually transmitted infections within the UK. However, the principles of the recommendations should be adopted across all services, including community care. Stakeholder involvement linicians from the Herpes Special Interest Group of BASHH and the ROG Guidelines ommittee have been involved in writing this guideline. The draft guideline was sent for consultation to the Herpes Viruses Association (HVA) for patient involvement. The guideline was posted on the BASHH and ROG websites for 3 months for consultation, with a direct request to the Royal ollege of Paediatrics and hild Health (RPH) for external peer review. 4
5 2. Search strategy This document was produced in accordance with the guidance set out in the BASHH linical Effectiveness Group s (EG s) document Framework for guideline development and assessment (available from: A literature search was performed using PubMed/MEDLINE, EMBASE, Google, The ochrane Library and relevant guidelines from January 1981 to January A MEDLINE/PubMed and EMBASE search was carried out from January 1981 to January 2014 using the following search terms/medical Subject Headings (MeSH): HSV/herpes, genital ulcers, HSV/herpes pregnancy, neonatal HSV/herpes, HSV/herpes drugs, pregnancy complications: infectious, Herpes genitalis and Herpes simplex diagnosis. The search was limited to humans and the English language. For some specific recommendations, an additional MEDLINE/PubMed search was performed when necessary. A Google search was performed in January 2014 with the search term HSV guideline(s) and all relevant documents of the first 150 search results were reviewed. A search of The ochrane Library included the ochrane Database of Systematic Reviews, Database of Abstracts of Reviews of Effects and ochrane entral Register of ontrolled Trials. The following guidelines were reviewed in detail: 2010 European guideline for the management of genital herpes; 2007 BASHH guidance on the management of genital herpes; and the 2007 ROG Green-top Guideline on the management of genital herpes in pregnancy. The members of the guideline development group selected studies relevant to the scope of the guideline. Article titles and abstracts were reviewed and if relevant the full-text article obtained. Priority was given to randomised controlled trial and systematic review evidence and, where possible, recommendations were made and graded on the basis of the best available evidence (Appendix 2). In areas where evidence is lacking, recommendations based on consensus opinion within the writing group have been made. 5
6 3. Background Neonatal herpes is a very rare but serious viral infection with a high morbidity and mortality. 4 It is classified into three subgroups in the infant depending on the site of infection: disease localised to skin, eye and/or mouth local central nervous system (NS) disease (encephalitis alone) disseminated infection with multiple organ involvement. Disease localised to skin, eye and/or mouth Infants who present with symptoms localised to the skin, eye or mouth alone have the best prognosis and represent approximately 30% of neonatal herpes infections. 5 With appropriate antiviral treatment, neurological and/or ocular morbidity is less than 2%. 6 Local NS disease and disseminated infection 70% of infants with neonatal herpes have disseminated and/or NS infection and approximately 60% of infants with local NS and/or disseminated disease will present without skin, eye and/or mouth infection. 5 Infants with local NS disease often present late (generally between 10 days and 4 weeks of age). With antiviral treatment, mortality from local NS disease is around 6% and neurological morbidity (which may be lifelong) is 70%. Disseminated disease carries the worst prognosis; with appropriate antiviral treatment, mortality is around 30% and 17% have long-term neurological sequelae. The poor outcomes of disseminated and local NS disease have been attributed to delays between symptom onset and treatment. 6 Neonatal infection occurs as the result of an infection at the time of birth; in contrast, congenital herpes is extremely rare and occurs by transfer of infection in utero. Incidence Neonatal herpes is rare in the UK, in contrast to some other European countries and the USA. Active surveillance by the British Paediatric Surveillance Unit (BPSU) between 1986 and 1991 found 76 cases over the five-and-a-half-year surveillance period with an incidence of 1.65/ live births annually (95% I ). 7 Subsequent surveillance from 2004 to 2006 showed an approximate doubling of incidence with 86 cases seen over the three-year surveillance period. 5 This increase may reflect the rise in the prevalence of sexually transmitted infections, demographic and social changes within the general population and improvements in diagnostic techniques. 5 Further published incidence data are awaited. The incidence in the UK is around 50% of that reported from other European countries. 8 In the USA, the average reported incidence is 1 in , but there is considerable variation between populations and rates of up to 1 in 7500 have been reported in certain deprived inner-city populations. 6,9 6
7 Aetiology Neonatal herpes may be caused by herpes simplex virus type 1 (HSV-1) or herpes simplex virus type 2 (HSV-2) as either viral type can cause genital herpes in the mother. Approximately 50% of neonatal herpes is due to HSV-1 and 50% due to HSV-2. 5 Most cases of neonatal herpes occur as a result of direct contact with infected maternal secretions, although in 25% of cases a possible source of postnatal infection was identified, usually a close relative of the mother. 5,7 Postnatal infection may occur as a result of exposure to oro-labial herpes infection. Transmission Factors associated with transmission include the type of maternal infection (primary or recurrent), the presence of transplacental maternal neutralising antibodies, the duration of rupture of membranes before delivery, the use of fetal scalp electrodes and the mode of delivery. 6,9 The risks are greatest when a woman acquires a new infection (primary genital herpes) in the third trimester, particularly within 6 weeks of delivery, as viral shedding may persist and the baby is likely to be born before the development of protective maternal antibodies. 6,9 Rarely, congenital herpes may occur as a result of transplacental intrauterine infection. ase reports suggest that the skin, eyes and NS may be affected and there may be fetal growth restriction or fetal death Disseminated herpes is more common in preterm infants and occurs almost exclusively as a result of primary infection in the mother. Although recurrent genital herpes is associated with a very low risk of neonatal herpes, recurrent herpes at the time of delivery, which is commonly asymptomatic or unrecognised, may cause the localised forms of neonatal herpes: both local NS disease and skin, eye and mouth infection. Transplacentally acquired HSV antibodies do not prevent herpes virus spreading to the brain of the neonate. 13 Data from the USA suggest that around 2% of women acquire genital HSV infection in pregnancy 4 and most of these maternal infections are asymptomatic or unrecognised. 4,9 However, acquisition in the UK in pregnancy may vary markedly given differing rates of neonatal herpes between the UK and USA. It may be difficult to distinguish clinically between recurrent and primary genital HSV infections, as many first episode HSV infections are not true primary infections. 14 Disseminated herpes infection in the mother Disseminated herpes, which may present with encephalitis, hepatitis, disseminated skin lesions or a combination of these conditions, is rare in adults. However, it has been more commonly reported in pregnancy, particularly in the immunocompromised. The maternal mortality associated with this condition is high. 15 All immunocompromised women, such as those infected with the HIV virus, are at increased risk of more severe and frequent symptomatic recurrent episodes of genital herpes during pregnancy and of asymptomatic shedding of HSV at term. 16,17 As co-infection with HSV and HIV results in an increased replication of both viruses, 18 there are concerns that genital reactivation of HSV may increase the risk of perinatal transmission of both HIV and HSV, 16,17 although this has not been realised in practice in the UK. For more detailed information on the diagnosis and management of HSV infection in the mother, please refer to the 2014 BASHH guideline on the management of genital herpes. 7
8 4. Management of pregnant women with first episode genital herpes First or second trimester acquisition (until weeks of gestation) A There is no evidence of an increased risk of spontaneous miscarriage with primary genital herpes in the first trimester. Women with suspected genital herpes should be referred to a genitourinary medicine physician who will confirm or refute the diagnosis by viral polymerase chain reaction (PR), advise on management of genital herpes and arrange a screen for other sexually transmitted infections. Treatment, however, should not be delayed. Management of the woman should be in line with her clinical condition and will usually involve the use of oral (or intravenous for disseminated HSV) aciclovir in standard doses (400 mg three times daily, usually for 5 days). The use of aciclovir is associated with a reduction in the duration and severity of symptoms and a decrease in the duration of viral shedding. Aciclovir is not licensed for use in pregnancy but is considered safe and has not been associated with an increased incidence of birth defects. Transient neonatal neutropenia has been reported but no clinically significant adverse maternal or neonatal effects have been reported. Aciclovir is well tolerated in pregnancy. For treatment courses no dose adjustment is necessary. 23,24 There is no evidence of an increased risk of birth defects with aciclovir, famciclovir or valaciclovir if used in the first trimester. 22 Safety data for aciclovir may be extrapolated to valaciclovir in late pregnancy, as it is the valine ester, but as there is less experience with the use of valaciclovir or famciclovir, they are not recommended as a firstline treatment. 22 The obstetrician should be informed Paracetamol and topical lidocaine 2% gel can be offered as symptomatic relief. There is no evidence that either is harmful in pregnancy in standard doses. Women with suspected genital herpes who are having midwifery-led care should be referred for review by an obstetrician, ideally after review by a genitourinary medicine physician. Providing that delivery does not ensue within the next 6 weeks, the pregnancy should be managed expectantly and vaginal delivery anticipated. There is no evidence that HSV acquired in pregnancy is associated with an increased incidence of congenital abnormalities. 25 Following first or second trimester acquisition, daily suppressive aciclovir 400 mg three times daily from 36 weeks of gestation reduces HSV lesions at term and hence the need for delivery by caesarean section It has also been shown to reduce asymptomatic viral shedding (similar results have been seen with valaciclovir, although valaciclovir is not recommended for use in pregnancy in view of lack of experience with its use). 27,32,33 III IV III III Ib 8
9 Third trimester acquisition (from 28 weeks of gestation) B B There is some evidence of increased perinatal morbidity (preterm labour and low birthweight), together with stillbirth, 4,34 however the data are conflicting 4 so no additional monitoring of such pregnancies is recommended. There is insufficient evidence to suggest an association between HSV and stillbirth as a cause of fetal death 35 with some studies demonstrating no association. 36 Treatment should not be delayed. Management of the woman should be in line with her clinical condition and will usually involve the use of oral (or intravenous for disseminated HSV) aciclovir in standard doses (400 mg three times daily, usually for 5 days). In the third trimester, treatment will usually continue with daily suppressive aciclovir 400 mg three times daily until delivery. aesarean section should be the recommended mode of delivery for all women developing first episode genital herpes in the third trimester, particularly those developing symptoms within 6 weeks of expected delivery, as the risk of neonatal transmission of HSV is very high at 41%. 4,37 39 It can be difficult to distinguish clinically between primary and recurrent genital HSV infections, as in up to 15% of cases where a woman presents with a first episode of clinical HSV infection, it will actually be a recurrent infection. 14 For women presenting with first episode genital herpes in the third trimester, particularly within 6 weeks of expected delivery, typespecific HSV antibody testing (immunoglobulin G [IgG] antibodies to HSV-1 and HSV-2) is advisable. For these women, characterising the infection will influence the advice given regarding mode of delivery and risk of neonatal herpes infection. The presence of antibodies of the same type as the HSV isolated from genital swabs would confirm this episode to be a recurrence rather than a primary infection and elective caesarean section would not be indicated to prevent neonatal transmission. However, it should be noted that it may take 2 3 weeks for the results of this test to become available. It is therefore recommended that an initial plan of delivery should be based on the assumption that all first episode lesions are primary genital herpes. This plan can then be modified if HSV antibody test results subsequently confirm a recurrent, rather than primary, infection. As interpretation of serology can be complicated, results should be discussed with a virologist or genitourinary medicine physician. III IIb IV 9
10 5. Management of pregnant women with recurrent genital herpes B B Women with recurrent genital herpes should be informed that the risk of neonatal herpes is low, even if lesions are present at the time of delivery (0 3% for vaginal delivery). Although there is no evidence that aciclovir is unsafe in early pregnancy, the majority of recurrent episodes of genital herpes are short-lasting and resolve within 7 10 days without antiviral treatment. Supportive treatment measures using saline bathing and analgesia with standard doses of paracetamol alone will usually suffice. Vaginal delivery should be anticipated in the absence of other obstetric indications for caesarean section. Daily suppressive aciclovir 400 mg three times daily should be considered from 36 weeks of gestation. There is insufficient evidence to determine whether this reduces the incidence of neonatal herpes; however, it reduces viral shedding and recurrences at delivery so may reduce the need for caesarean section. Limited information exists regarding the neonatal safety of prophylaxis. The risks, benefits and alternatives to daily suppressive therapy should be discussed with women who have a history and prophylaxis initiated for women who desire intervention. 33 This increase from the standard suppressive dose of 400 mg twice daily is recommended in view of the greater volume of distribution of the drug during pregnancy. 26,40 Sequential PR culture during late gestation to predict viral shedding at term, 17 or at delivery to identify women who are asymptomatically shedding HSV, is not indicated. There is no increased risk of preterm labour, preterm prelabour rupture of membranes or fetal growth restriction associated with women seropositive for HSV. The incidence of congenital abnormalities is not increased in the presence of recurrent genital herpes infection. 41 III Ia IIa 10
11 6. Management of women with primary or recurrent genital lesions at the onset of labour General management Management of a woman with genital herpes at the onset of labour will be based on clinical assessment as there will not be time for confirmatory laboratory testing. The clinician must take a history in order to ascertain whether this is a primary or recurrent episode. A viral swab from the lesion(s) should nonetheless be taken, since the result may influence management of the neonate. The neonatologist should be informed. Primary episode B aesarean section should be recommended to all women presenting with primary episode genital herpes lesions at the time of delivery, or within 6 weeks of the expected date of delivery, in order to reduce exposure of the fetus to HSV which may be present in maternal genital secretions. 9 There is some evidence to suggest that the benefit of caesarean section reduces if the membranes have been ruptured for greater than 4 hours. 42 However, there may be some benefit in performing a caesarean section even after this time interval. Intravenous aciclovir given intrapartum to the mother (5 mg/kg every 8 hours) and subsequently to the neonate (intravenous aciclovir 20 mg/kg every 8 hours) may be considered for those mothers opting for vaginal delivery. 13,25 It is unknown whether intrapartum aciclovir reduces the risk of neonatal HSV infection. Where primary episode genital herpes lesions are present at the time of delivery and the baby is delivered vaginally, the risk of neonatal herpes is estimated to be 41%. 4,37 39 The risk of perinatal transmission depends on the timing of maternal acquisition of HSV, with the highest risk in infants born to women who have not completed HSV seroconversion during pregnancy (most commonly in the third trimester, within 6 weeks of delivery). Although vaginal delivery should be avoided if possible, in women who deliver vaginally in the presence of primary genital herpes lesions, invasive procedures (application of fetal scalp electrodes, fetal blood sampling, artificial rupture of membranes and/or instrumental deliveries) should be avoided. 4,43 45 III IV III 11
12 Recurrent genital herpes B Women presenting with recurrent genital herpes lesions at the onset of labour should be advised that the risk to the baby of neonatal herpes is low (0 3% for vaginal delivery). 1,38 Evidence from the Netherlands shows that a conservative approach, allowing vaginal delivery in the presence of an anogenital lesion, has not been associated with a rise in the number of neonatal HSV cases. 46 Vaginal delivery should be offered to women with recurrent genital herpes lesions at the onset of labour. A caesarean section delivery can be considered but the risk to the mother and future pregnancies should be set against the small risk of neonatal transmission of HSV with recurrent disease (0 3% for vaginal delivery). The final choice of vaginal delivery versus caesarean section should be made by the mother, who should base her decision on the very low risk of transmission set against any other obstetric risk factors and the risks associated with caesarean section. It has been reported that invasive procedures (fetal blood sampling, application of fetal scalp electrodes, artificial rupture of membranes and/or instrumental deliveries) increase the risk of neonatal HSV infection. 47 However, given the small background risk (0 3%) of transmission in this group, the increased risk associated with invasive procedures is unlikely to be clinically significant so they may be used if required. Women should be managed in accordance with standard National Institute for Health and are Excellence (NIE) intrapartum guidelines. 45 There is no evidence to guide the management of women with spontaneous rupture of membranes at term, but many clinicians will advise expediting delivery in an attempt to minimise the duration of potential exposure of the fetus to HSV. III IV III IV 12
13 7. Genital herpes in preterm prelabour rupture of membranes (before weeks of gestation) Primary genital herpes in preterm prelabour rupture of membranes (PPROM) There is limited evidence to inform best obstetric practice when PPROM is complicated by primary HSV infection. Management should be guided by multidisciplinary team discussion involving the obstetricians, neonatologists and genitourinary medicine physicians and will depend on the gestation that PPROM occurred. If the decision is made for immediate delivery then the anticipated benefits of caesarean section will remain. If there is initial conservative management, the mother should be recommended to receive intravenous aciclovir 5 mg/kg every 8 hours. Prophylactic corticosteroids should be considered to reduce the implications of preterm delivery upon the infant. 48 If delivery is indicated within 6 weeks of the primary infection, delivery by caesarean section may still offer some benefit despite the prolonged rupture of membranes IV Recurrent genital herpes in PPROM When PPROM is encountered in the presence of recurrent genital herpes lesions, the risk of neonatal transmission is very small and may be outweighed by the morbidity and mortality associated with premature delivery. In the case of PPROM before 34 weeks there is evidence to suggest that expectant management is appropriate, including oral aciclovir 400 mg three times daily for the mother. 49 After this gestation, it is recommended that management is undertaken in accordance with relevant ROG guidelines on PPROM 52 and antenatal corticosteroid administration 53 to reduce neonatal morbidity and mortality and is not materially influenced by the presence of recurrent genital herpes lesions. 49,54 IV 13
14 8. Management of HIV-positive women with HSV infection Primary HSV infection HIV-positive women with primary genital HSV infection in the last trimester of pregnancy should be managed according to the recommendations for all women with primary genital HSV infection. Recurrent HSV infection There is some evidence that HIV antibody positive women with genital HSV ulceration in pregnancy are more likely to transmit HIV infection independent of other factors. 17,55 However, this is not a consistent finding across all studies. 56 Women who are HIV antibody positive and have a history of genital herpes should be offered daily suppressive aciclovir 400 mg three times daily from 32 weeks of gestation to reduce the risk of transmission of HIV infection, especially in women where a vaginal delivery is planned. Starting therapy at this earlier gestation than usual should be considered in view of the increased possibility of preterm labour in HIV-positive women. The mode of delivery should be in line with the BHIVA HIV in pregnancy guideline recommendations according to obstetric factors and HIV parameters such as HIV viral load. 42,57 There is currently no evidence to recommend daily suppressive treatment of HSV for HIV antibody positive women who are HSV-1 or -2 seropositive but have no history of genital herpes. 56 III IV 14
15 9. Management of the neonate General management In all cases the neonatal team should be informed. Management of babies born by caesarean section in mothers with primary HSV infection in the third trimester These babies are at low risk of vertically transmitted HSV infection so conservative management is recommended. Liaise with the neonatal team. Swabs from the neonate are not indicated. No active treatment is required for the baby. Normal postnatal care of the baby is advised with a neonatal examination at 24 hours of age, after which the baby can be discharged from the hospital if well and feeding is established. Parents should be educated regarding good hand hygiene and due care to reduce risk of postnatal infection. Parents should be advised to seek medical help if they have concerns regarding their baby. In particular, they should be advised to look for: skin, eye and mucous membrane lesions, lethargy/irritability, poor feeding. Management of babies born by spontaneous vaginal delivery in mothers with a primary HSV infection within the previous 6 weeks These babies are at high risk of vertically transmitted HSV infection. Liaise with the neonatal team. If the baby is well: Swabs of the skin, conjunctiva, oropharynx and rectum should be sent for herpes simplex PR. A lumbar puncture is not necessary. Empirical treatment with intravenous aciclovir (20 mg/kg every 8 hours) should be initiated until evidence of active infection is ruled out. Strict infection control procedures should be put in place for both mother and baby. Breastfeeding is recommended unless the mother has herpetic lesions around the nipples. Parents should be warned to report any early signs of infection such as poor feeding, lethargy, fever or any suspicious lesions. If the baby is unwell or presents with skin lesions: Swabs of the skin, lesions, conjunctiva, oropharynx and rectum should be sent for herpes simplex PR. A lumbar puncture should be performed even if NS features are not present. 15
16 Intravenous aciclovir (20 mg/kg every 8 hours) should be initiated until evidence of active infection is ruled out. Management of babies born to mothers with recurrent HSV infection in pregnancy with or without active lesions at delivery B In the case of recurrent genital herpes infections in the mother, maternal IgG will be protective in the baby and hence the infection risk is low. onservative management of the neonate is advised. 55 Liaise with the neonatal team. Surface swabs from the neonate are not indicated. No active treatment is advised for the baby. Normal postnatal care of the baby is advised with a neonatal examination at 24 hours of age, after which the baby can be discharged from the hospital if well and feeding is established. Parents should be educated regarding good hand hygiene and due care to reduce risk of postnatal infection. Parents should be advised to seek medical help if they have concerns regarding their baby. In particular, they should be advised to look for: skin, eye and mucous membrane lesions, lethargy/irritability, poor feeding. III In cases where there are concerns regarding the neonate (clinical evidence of sepsis, poor feeding) Liaise with the neonatal team. In addition to considering bacterial sepsis, HSV infection should be considered. Surface swabs and blood for HSV culture and PR. Intravenous aciclovir (20 mg/kg every 8 hours) should be given while awaiting cultures. Further management by the neonatal team according to condition of the baby and test results. See Appendix 1 for flow chart of management. 16
17 10. Prevention of postnatal transmission In 25% of cases a possible source of postnatal infection is responsible, usually a close relative of the mother. 2 Efforts to prevent postnatal transmission of HSV are therefore important and advice should be given to the mother regarding this. The mother and all those with herpetic lesions who may be in contact with the neonate, including staff, should practice careful hand hygiene. Those with oral herpetic lesions (cold sores) should not kiss the neonate. IV 17
18 11. Performance measures 1. When a herpes antiviral drug is used against a previously undiagnosed genital herpes episode, a swab for herpes PR should be sent target 100%. 2. In order that a discussion on the mode of delivery is undertaken with an obstetrician, there must be documentation in the clinic notes that the obstetrician and/or GP have been advised of this need and that the patient has also been informed of this need target 100%. 3. For women with suspected primary genital herpes in pregnancy diagnosed in level 1/2 services, primary care or obstetric services, referral to a genitourinary medicine physician should be made (unless in labour) target 100%. 4. Where a first episode diagnosis of genital herpes is made in the third trimester, the woman s case should be discussed between the obstetrician and neonatologist with documentation of the agreed management target 100%. 5. Pregnant women with genital herpes should be provided with written information on genital herpes in pregnancy (e.g. the ROG patient information leaflet) target 90%. 18
19 12. About this guideline Qualifying statement The recommendations in this guideline may not be appropriate for use in all clinical situations. Decisions to follow these recommendations must be based on the professional judgement of the clinician and consideration of individual patient circumstances and available resources. All possible care has been undertaken to ensure the publication of the correct dosage of medication and route of administration. However, it remains the responsibility of the prescribing clinician to ensure the accuracy and appropriateness of the medication they prescribe. Editorial independence This guideline was commissioned, edited and endorsed by the BASHH EG and the ROG without external funding being sought or obtained. Declarations of interest All members of the guideline writing committee completed the BASHH conflict of interest declaration at the time that the guideline s final draft was submitted to the EG. Dr Rajul Patel has received honoraria for talks and fees for consultancy from Novatis, Becton Dickinson and Roche pharmaceutical and diagnostic companies. Resource implications The resource implications of this guideline will have little impact on current recommendations for management of herpes in pregnancy. There may be a cost saving if women with recurrent genital herpes simplex virus infection elect to have a vaginal delivery when herpetic lesions are present at term rather than undergoing a caesarean section. The cost of suppressive aciclovir (400 mg three times daily) for 1 month is 6.45*. Membership of the writing group EF and E drafted the initial document and redrafts, VAB and SH drafted the obstetric component and AP drafted the neonatal section. PO, NLB and RP commented on the drafts and redrafts of the document. Membership of the EG Dr Keith Radcliffe (hair), onsultant Physician in Genitourinary Medicine, Whittall Street linic Dr David Daniels, Sexual Health linic, West Middlesex University Hospital, West Middlesex University Hospital NHS Trust Dr Mark FitzGerald, onsultant Physician in Genitourinary Medicine, Musgrove Park Hospital 19
20 Dr Deepa Grover, onsultant in Genitourinary/HIV Medicine, Barnet Hospital/Royal Free Hospital Dr Stephen Higgins, onsultant Physician in Genitourinary Medicine, North Manchester General Hospital, Manchester Dr Margaret Kingston, onsultant Physician in Genitourinary Medicine, Manchester entre for Sexual Health Dr Neil Lazaro, Associate Specialist in Genitourinary Medicine, Royal Preston Hospital Dr Louise Melvin, Faculty of Sexual & Reproductive Healthcare representative, onsultant Sexual Health, Glasgow Dr Ann Sullivan, onsultant Physician in Genitourinary Medicine, helsea and Westminster Hospital NHS Foundation Trust. Timescale for next review: Acknowledgements BASHH National Audit Group for suggesting the performance measures. Dr Jolanta Bernatoniene and Dr atherine O Sullivan on behalf of the RPH for their expert review of the neonatal sections of the guideline. Marian Nicholson from the Herpes Viruses Association (HVA) for her invaluable input into this guideline. *Source of costing: British National Formulary September 2014 (different prices may be negotiated by NHS hospital trusts)
21 References 1. Royal ollege of Obstetricians and Gynaecologists. Management of Genital Herpes in Pregnancy. Green-top Guideline No. 30. London: ROG; linical Effectiveness Group (British Association for Sexual Health and HIV) National Guideline for the Management of Genital Herpes. Macclesfield: BASHH; Patel R, Alderson S, Geretti A, Nilsen A, Foley E, Lautenschlager S, et al European guideline for the management of genital herpes. [place unknown]; International Union against Sexually Transmitted Infections; Brown ZA, Selke S, Zeh J, Kopelman J, Maslow A, Ashley RL, et al. The acquisition of herpes simplex virus during pregnancy. N Engl J Med 1997;337: British Paediatric Surveillance Unit. BPSU 21st Annual Report London: British Paediatric Surveillance Unit/Royal ollege of Paediatrics and hild Health; Brown Z. Preventing herpes simplex virus transmission to the neonate. Herpes 2004;11 Suppl 3:175A 186A. 7. Tookey P, Peckham S. Neonatal herpes simplex virus infection in the British Isles. Paediatr Perinat Epidemiol 1996;10: Hemelaar SJ, Poeran J, Steegers EA, van der Meijden WI. Neonatal herpes infections in The Netherlands in the period J Matern Fetal Neonatal Med 2014 Jul 11 [Epub ahead of print]. 9. Brown ZA, Wald A, Morrow RA, Selke S, Zeh J, orey L. Effect of serologic status and cesarean delivery on transmission rates of herpes simplex virus from mother to infant. JAMA 2003;289: Diguet A, Patrier S, Eurin D, houchene S, Marpeau L, Laquerrière A, et al. Prenatal diagnosis of an exceptional intrauterine herpes simplex type 1 infection. Prenat Diagn 2006;26: Vasileiadis GT, Roukema HW, Romano W, Walton J, Gagnon R. Intrauterine herpes simplex infection. Am J Perinatol 2003;20: Lee A, Bar-Zeev N, Walker SP, Permezel M. In utero herpes simplex encephalitis. Obstet Gynecol 2003;102: Nahmias AJ. Neonatal HSV infection Part 1: continuing challenges. Herpes 2004;11: Hensleigh PA, Andrews WW, Brown Z, Greenspoon J, Yasukawa L, Prober G. Genital herpes during pregnancy: inability to distinguish primary and recurrent infections clinically. Obstet Gynecol 1997;89: Young EJ, hafizadeh E, Oliveira VL, Genta RM. Disseminated herpesvirus infection during pregnancy. lin Infect Dis 1996;22: Hitti J, Watts DH, Burchett SK, Schacker T, Selke S, Brown ZA, et al. Herpes simplex virus seropositivity and reactivation at delivery among pregnant women infected with human immunodeficiency virus-1. Am J Obstet Gynecol 1997;177: hen KT, Segú M, Lumey LH, Kuhn L, arter RJ, Bulterys M, et al.; New York ity Perinatal AIDS ollaborative Transmission Study (PATS) Group. Genital herpes simplex virus infection and perinatal transmission of human immunodeficiency virus. Obstet Gynecol 2005;106: Heng M, Heng SY, Allen SG. o-infection and synergy of human immunodeficiency virus-1 and herpes simplex virus-1. Lancet 1994;i: Andrews WW, Kimberlin DF, Whitley R, liver S, Ramsey PS, Deeter R. Valacyclovir therapy to reduce recurrent genital herpes in pregnant women. Am J Obstet Gynecol 2006;194:
22 20. Stone KM, Reiff-Eldridge R, White AD, ordero JF, Brown Z, Alexander ER, et al. Pregnancy outcomes following systemic prenatal acyclovir exposure: onclusions from the international acyclovir pregnancy registry, Birth Defects Res A lin Mol Teratol 2004;70: Ratanajamit, Vinther Skriver M, Jepsen P, hongsuvivatwong V, Olsen J, Sørensen HT. Adverse pregnancy outcome in women exposed to acyclovir during pregnancy: a population-based observational study. Scand J Infect Dis 2003;35: Pasternak B, Hviid A. Use of acyclovir, valacyclovir, and famciclovir in the first trimester of pregnancy and the risk of birth defects. JAMA 2010;304: Frenkel LM, Brown ZA, Bryson YJ, orey L, Unadkat JD, Hensleigh PA, et al. Pharmacokinetics of acyclovir in the term human pregnancy and neonate. Am J Obstet Gynecol 1991;164: Kimberlin DF, Weller S, Whitley RJ, Andrews WW, Hauth J, Lakeman F, et al. Pharmacokinetics of oral valacyclovir and acyclovir in late pregnancy. Am J Obstet Gynecol 1998;179: Ács N, Bánhidy F, Puhó E, zeizel AE. No association between maternal recurrent genital herpes in pregnancy and higher risk for congenital abnormalities. Acta Obstet Gynecol Scand 2008;87: Sheffield JS, Hollier LM, Hill JB, Stuart GS, Wendel GD Jr. Acyclovir prophylaxis to prevent herpes simplex virus recurrence at delivery: a systematic review. Obstet Gynecol 2003;102: Watts DH, Brown ZA, Money D, Selke S, Huang ML, Sacks SL, et al. A double-blind, randomized, placebo-controlled trial of acyclovir in late pregnancy for the reduction of herpes simplex virus shedding and cesarean delivery. Am J Obstet Gynecol 2003;188: Scott LL, Hollier LM, McIntire D, Sanchez PJ, Jackson GL, Wendel GD Jr. Acyclovir suppression to prevent recurrent genital herpes at delivery. Infect Dis Obstet Gynecol 2002;10: Brocklehurst P, Kinghorn G, arney O, Helsen K, Ross E, Ellis E, et al. A randomised placebo controlled trial of suppressive acyclovir in late pregnancy in women with recurrent genital herpes infection. Br J Obstet Gynaecol 1998;105: Scott LL, Sanchez PJ, Jackson GL, Zeray F, Wendel GD Jr. Acyclovir suppression to prevent cesarean delivery after first-episode genital herpes. Obstet Gynecol 1996;87: Braig S, Luton D, Sibony O, Edlinger, Boissinot, Blot P, et al. Acyclovir prophylaxis in late pregnancy prevents recurrent genital herpes and viral shedding. Eur J Obstet Gynecol Reprod Biol 2001;96: Sheffield JS, Hill JB, Hollier LM, Laibl VR, Roberts SW, Sanchez PJ, et al. Valacyclovir prophylaxis to prevent recurrent herpes at delivery: a randomized clinical trial. Obstet Gynecol 2006;108: Hollier LM, Wendel GD. Third trimester antiviral prophylaxis for preventing maternal genital herpes simplex virus (HSV) recurrences and neonatal infection. ochrane Database Syst Rev 2008;(1):D Brown ZA, Benedetti J, Selke S, Ashley R, Watts DH, orey L. Asymptomatic maternal shedding of herpes simplex virus at the onset of labor: relationship to preterm labor. Obstet Gynecol 1996;87: Syridou G, Spanakis N, Konstantinidou A, Piperaki ET, Kafetzis D, Patsouris E, et al. Detection of cytomegalovirus, parvovirus B19 and herpes simplex viruses in cases of intrauterine fetal death: association with pathological findings. J Med Virol 2008;80: Eskild A, Jeansson S, Stray-Pedersen B, Jenum PA. Herpes simplex virus type-2 infection in pregnancy: no risk of fetal death: results from a nested case control study within 35,940 women. BJOG 2002;109:
23 37. Brown ZA, Vontver LA, Benedetti J, ritchlow W, Sells J, Berry S, et al. Effects on infants of a first episode of genital herpes during pregnancy. N Engl J Med 1987;317: Prober G, Sullender WM, Yasukawa LL, Au DS, Yeager AS, Arvin AM. Low risk of herpes simplex virus infections in neonates exposed to the virus at the time of vaginal delivery to mothers with recurrent genital herpes simplex virus infections. N Engl J Med 1987;316: Brown ZA, Benedetti J, Ashley R, Burchett S, Selke S, Berry S, et al. Neonatal herpes simplex virus infection in relation to asymptomatic maternal infection at the time of labor. N Engl J Med 1991;324: Gardella, Brown ZA, Wald A, Morrow RA, Selke S, Krantz E, et al. Poor correlation between genital lesions and detection of herpes simplex virus in women in labor. Obstet Gynecol 2005;106: Kim ID, hang HS, Hwang KJ. Herpes simplex virus 2 infection rate and necessity of screening during pregnancy: a clinical and seroepidemiologic study. Yonsei Med J 2012;53: Nahmias AJ, Josey WE, Naib ZM, Freeman MG, Fernandez RJ, Wheeler JH. Perinatal risk associated with maternal genital herpes simplex virus infection. Am J Obstet Gynecol 1971;110: Kohelet D, Katz N, Sadan O, Somekh E. Herpes simplex virus infection after vacuum-assisted vaginally delivered infants of asymptomatic mothers. J Perinatol 2004;24: Amann ST, Fagnant RJ, hartrand SA, Monif GR. Herpes simplex infection associated with short-term use of a fetal scalp electrode. A case report. J Reprod Med 1992;37: National Institute for Health and linical Excellence. Intrapartum care: are of healthy women and their babies during childbirth. NIE clinical guideline 55. Manchester: NIE; Singhal P, Naswa S, Marfatia YS. Pregnancy and sexually transmitted viral infections. Indian J Sex Transm Dis 2009;30: Parvey LS, h ien LT. Neonatal herpes simplex virus infection introduced by fetal-monitor scalp electrodes. Pediatrics 1980;65: Kimberlin DW, Baley J; ommittee on Infectious Diseases; ommittee on Fetus and Newborn. Guidance on management of asymptomatic neonates born to women with active genital herpes lesions. Pediatrics 2013;131:e Major A, Towers V, Lewis DF, Garite TJ. Expectant management of preterm premature rupture of membranes complicated by active recurrent genital herpes. Am J Obstet Gynecol 2003;188:1551 4; discussion Utley K, Bromberger P, Wagner L, Schneider H. Management of primary herpes in pregnancy complicated by ruptured membranes and extreme prematurity: case report. Obstet Gynecol 1987;69(3 Pt 2): Dietrich YM, Napolitano PG. Acyclovir treatment of primary herpes in pregnancy complicated by second trimester preterm premature rupture of membranes with term delivery: case report. Am J Perinatol 2002;19: Pinninti SG, Kimberlin DW. Management of neonatal herpes simplex virus infection and exposure. Arch Dis hild Fetal Neonatal Ed 2014;99:F Royal ollege of Obstetricians and Gynaecologists. Antenatal orticosteroids to Reduce Neonatal Morbidity and Mortality. Green-top Guideline No. 7. London: ROG; Ehsanipoor RM, Major A. Herpes simplex and HIV infections and preterm PROM. lin Obstet Gynecol 2011;54: Drake AL, John-Stewart G, Wald A, Mbori-Ngacha DA, Bosire R, Wamalwa D, et al. Herpes simplex virus type 2 and risk of intrapartum human immunodeficiency virus transmission. Obstet Gynecol 2007;109:
24 56. hen KT, Tuomala RE, hu, Huang ML, Watts DH, Zorrilla D, et al. No association between antepartum serologic and genital tract evidence of herpes simplex virus-2 coinfection and perinatal HIV-1 transmission. Am J Obstet Gynecol 2008;198:399.e British HIV Association. British HIV Association guidelines for the management of HIV infection in pregnant women 2012 (2014 interim review). London: BHIVA; NIE Evidence Services. British National Formulary September Aciclovir (Acyclovir) [ herpesvirus-infections/5321-herpes-simplex-and-varicellazoster-infection/aciclovir?q= AILOVIR] Accessed 2014 Sep
25 Appendix I Algorithm for the management of herpes in pregnancy and care of neonate Recurrent genital herpes Primary acquisition of genital herpes in first or second trimester Primary acquisition of genital herpes in third trimester Treat episodes with standard doses of aciclovir if necessary Treat primary episode with standard doses of aciclovir Treat primary episode with standard doses of aciclovir onsider aciclovir 400 mg tds from 36/40 gestation onsider aciclovir 400 mg tds until delivery Recommend planned S especially if within 6 weeks of delivery Offer vaginal delivery If vaginal delivery ensues inform neonatologist Inform neonatologist Normal postnatal care Discharge home if baby well at 24 hours Advise parents regarding later management if any concerns Normal postnatal care Genital HSV lesions at delivery Baby well Baby unwell Normal postnatal care Discharge home if baby well at 24 hours Advise parents regarding later management if any concerns Perform lumbar puncture for HSV PR Start aciclovir 20 mg/kg tds for 10 days while awaiting results Abbreviations S caesarean section; HSV herpes simplex virus; PR polymerase chain reaction; Abbreviations tds three times daily 25
26 Appendix II Levels of evidence and grading of recommendations Levels of evidence Ia Meta-analysis of randomised controlled trials Ib At least one randomised controlled trial IIa At least one well-designed controlled study without randomisation IIb At least one other type of well-designed quasi-experimental study III Well-designed non-experimental descriptive studies IV Expert committee reports or opinions of respected authorities Grading of recommendations A Evidence at level Ia or Ib B Evidence at level IIa, IIb or III Evidence at level IV 26
How can herpes simplex spread to an infant?
 CHAPTER 3 HERPES AND PREGNANCY As an expectant parent eagerly awaiting the birth of your new baby, you are probably taking a number of steps to ensure your baby s health. One step many experts recommend
CHAPTER 3 HERPES AND PREGNANCY As an expectant parent eagerly awaiting the birth of your new baby, you are probably taking a number of steps to ensure your baby s health. One step many experts recommend
Neonatal herpes simplex virus (HSV) infections
 Neonatal Herpes Simplex Virus Infections CAROLINE M. RUDNICK, M.D., PH.D., St. Anthony s Medical Center, St. Louis, Missouri GRANT S. HOEKZEMA, M.D., St. John s Mercy Medical Center, St. Louis, Missouri
Neonatal Herpes Simplex Virus Infections CAROLINE M. RUDNICK, M.D., PH.D., St. Anthony s Medical Center, St. Louis, Missouri GRANT S. HOEKZEMA, M.D., St. John s Mercy Medical Center, St. Louis, Missouri
Yes, I know I have genital herpes:
 Counseling Messages for Herpes Simplex Type II (HSV-II) Genital herpes Always take the time to attend to the participant s feelings and emotional state; for some people, this is the most devastating news
Counseling Messages for Herpes Simplex Type II (HSV-II) Genital herpes Always take the time to attend to the participant s feelings and emotional state; for some people, this is the most devastating news
A guide for people with genital herpes
 A guide for people with genital herpes Contents Getting the facts 4 The key facts 6 What is genital herpes? 8 Genital herpes symptoms 10 Getting tested 12 The first outbreak 14 Recurrent outbreaks 16 Common
A guide for people with genital herpes Contents Getting the facts 4 The key facts 6 What is genital herpes? 8 Genital herpes symptoms 10 Getting tested 12 The first outbreak 14 Recurrent outbreaks 16 Common
Accent on Health Obgyn, PC HERPES Frequently Asked Questions
 1. What is herpes? 2. How common is herpes? 3. Is there a cure for herpes? 4. What is oral herpes (cold sores)? 5. How is oral herpes spread? 6. What is genital herpes? 7. How is genital herpes spread?
1. What is herpes? 2. How common is herpes? 3. Is there a cure for herpes? 4. What is oral herpes (cold sores)? 5. How is oral herpes spread? 6. What is genital herpes? 7. How is genital herpes spread?
ROYAL HOSPITAL FOR WOMEN
 HEPATITIS B POSITIVE MOTHERS AND THEIR BABIES This LOP is developed to guide clinical practice at the Royal Hospital for Women. Individual patient circumstances may mean that practice diverges from this
HEPATITIS B POSITIVE MOTHERS AND THEIR BABIES This LOP is developed to guide clinical practice at the Royal Hospital for Women. Individual patient circumstances may mean that practice diverges from this
Parvovirus B19 Infection in Pregnancy
 Parvovirus B19 Infection in Pregnancy Information Pack Parvovirus B19 Infection in Pregnancy Information Booklet CONTENTS: THE VIRUS page 3 CLINICAL MANIFESTATIONS page 6 DIAGNOSIS page 8 PATIENT MANAGEMENT
Parvovirus B19 Infection in Pregnancy Information Pack Parvovirus B19 Infection in Pregnancy Information Booklet CONTENTS: THE VIRUS page 3 CLINICAL MANIFESTATIONS page 6 DIAGNOSIS page 8 PATIENT MANAGEMENT
Zika Virus. Fred A. Lopez, MD, MACP Richard Vial Professor Department of Medicine Section of Infectious Diseases
 Zika Virus Fred A. Lopez, MD, MACP Richard Vial Professor Department of Medicine Section of Infectious Diseases What is the incubation period for Zika virus infection? Unknown but likely to be several
Zika Virus Fred A. Lopez, MD, MACP Richard Vial Professor Department of Medicine Section of Infectious Diseases What is the incubation period for Zika virus infection? Unknown but likely to be several
ZOVIRAX Cold Sore Cream
 Data Sheet ZOVIRAX Cold Sore Cream Aciclovir 5% w/w Presentation Topical cream Indications ZOVIRAX Cold Sore Cream is indicated for the treatment of Herpes simplex virus infections of the lips and face
Data Sheet ZOVIRAX Cold Sore Cream Aciclovir 5% w/w Presentation Topical cream Indications ZOVIRAX Cold Sore Cream is indicated for the treatment of Herpes simplex virus infections of the lips and face
Chickenpox in pregnancy: what you need to know
 Chickenpox in pregnancy: what you need to know First published December 2003 Revised edition published November 2008 What is chickenpox? Chickenpox is a very infectious illness caused by a virus called
Chickenpox in pregnancy: what you need to know First published December 2003 Revised edition published November 2008 What is chickenpox? Chickenpox is a very infectious illness caused by a virus called
Treatment of Neonates Exposed to and Infected with HSV
 Treatment of Neonates Exposed to and Infected with HSV Michael T. Brady, MD Pediatric Professor The Ohio State University Associate Medical Director Nationwide Children s Hostile Faculty Disclosure Michael
Treatment of Neonates Exposed to and Infected with HSV Michael T. Brady, MD Pediatric Professor The Ohio State University Associate Medical Director Nationwide Children s Hostile Faculty Disclosure Michael
Obtaining Valid Consent to Participate in Perinatal Research Where Consent is Time Critical
 Obtaining Valid Consent to Participate in Perinatal Research Where Consent is Time Critical February 2016 Obtaining Valid Consent to Participate in Perinatal Research Where Consent is Time Critical This
Obtaining Valid Consent to Participate in Perinatal Research Where Consent is Time Critical February 2016 Obtaining Valid Consent to Participate in Perinatal Research Where Consent is Time Critical This
William Atkinson, MD, MPH Hepatitis B Vaccine Issues June 16, 2016
 William Atkinson, MD, MPH Hepatitis B Vaccine Issues June 16, 2016 Advisory Committee on Immunization Practices (ACIP) The recommendations to be discussed are primarily those of the ACIP composed of 15
William Atkinson, MD, MPH Hepatitis B Vaccine Issues June 16, 2016 Advisory Committee on Immunization Practices (ACIP) The recommendations to be discussed are primarily those of the ACIP composed of 15
The challenge of herpes
 The challenge of herpes Herpes is a common and personally challenging disease Herpes is very common. One out of four adults has genital herpes. When people first hear that they are infected, many become
The challenge of herpes Herpes is a common and personally challenging disease Herpes is very common. One out of four adults has genital herpes. When people first hear that they are infected, many become
35-40% of GBS disease occurs in the elderly or in adults with chronic medical conditions.
 What is Group B Strep (GBS)? Group B Streptococcus (GBS) is a type of bacteria that is found in the lower intestine of 10-35% of all healthy adults and in the vagina and/or lower intestine of 10-35% of
What is Group B Strep (GBS)? Group B Streptococcus (GBS) is a type of bacteria that is found in the lower intestine of 10-35% of all healthy adults and in the vagina and/or lower intestine of 10-35% of
SOGC recommendation on ZIKA virus exposure for clinicians caring for pregnant women and those who intend to get pregnant
 SOGC recommendation on ZIKA virus exposure for clinicians caring for pregnant women and those who intend to get pregnant Foreword The rapid emergence of Zika virus as a potential causative agent for fetal
SOGC recommendation on ZIKA virus exposure for clinicians caring for pregnant women and those who intend to get pregnant Foreword The rapid emergence of Zika virus as a potential causative agent for fetal
VARICELLA ZOSTER (VZ) VIRUS, CHICKENPOX & SHINGLES GUIDANCE
 VARICELLA ZOSTER (VZ) VIRUS, CHICKENPOX & SHINGLES GUIDANCE Summary This guidance provides background information on varicella zoster (VZ), chickenpox and shingles and sets out the infection control measures
VARICELLA ZOSTER (VZ) VIRUS, CHICKENPOX & SHINGLES GUIDANCE Summary This guidance provides background information on varicella zoster (VZ), chickenpox and shingles and sets out the infection control measures
41 Viral rashes and skin infections
 41 Viral rashes and skin infections Clinical There are several kinds of skin infections caused by viruses, and these are best considered in the four categories that group together similar symptoms for
41 Viral rashes and skin infections Clinical There are several kinds of skin infections caused by viruses, and these are best considered in the four categories that group together similar symptoms for
Laboratory confirmation requires isolation of Bordetella pertussis or detection of B. pertussis nucleic acid, preferably from a nasopharyngeal swab.
 Pertussis Epidemiology in New Zealand New Zealand has continued to experience outbreaks of pertussis in recent decades. This is in part due to historically low immunisation rates and in part because immunity
Pertussis Epidemiology in New Zealand New Zealand has continued to experience outbreaks of pertussis in recent decades. This is in part due to historically low immunisation rates and in part because immunity
NHS FORTH VALLEY Guidelines for Hepatitis B Vaccination in High Risk Groups
 NHS FORTH VALLEY Guidelines for Hepatitis B Vaccination in High Risk Groups Approved 01/04/2012 Version 1.0 Date of First Issue 01/04/2012 Review Date 01/02/2014 Date of Issue 01/04/2012 EQIA Yes Author
NHS FORTH VALLEY Guidelines for Hepatitis B Vaccination in High Risk Groups Approved 01/04/2012 Version 1.0 Date of First Issue 01/04/2012 Review Date 01/02/2014 Date of Issue 01/04/2012 EQIA Yes Author
MANAGEMENT OF INFANTS BORN TO HIV POSITIVE MOTHERS
 MANAGEMENT OF INFANTS BORN TO HIV POSITIVE MOTHERS Introduction Perinatal management of infants born to HIV-infected mothers requires a coordinated multidisciplinary team approach. The consultant leads
MANAGEMENT OF INFANTS BORN TO HIV POSITIVE MOTHERS Introduction Perinatal management of infants born to HIV-infected mothers requires a coordinated multidisciplinary team approach. The consultant leads
OET: Listening Part A: Influenza
 Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Crohn's disease and pregnancy.
 Gut, 1984, 25, 52-56 Crohn's disease and pregnancy. R KHOSLA, C P WILLOUGHBY, AND D P JEWELL From the Gastroenterology Unit, Radcliffe Infirmary, Oxford SUMMARY Infertility and the outcome of pregnancy
Gut, 1984, 25, 52-56 Crohn's disease and pregnancy. R KHOSLA, C P WILLOUGHBY, AND D P JEWELL From the Gastroenterology Unit, Radcliffe Infirmary, Oxford SUMMARY Infertility and the outcome of pregnancy
California Guidelines for STD Screening and Treatment in Pregnancy
 California Guidelines for STD Screening and Treatment in Pregnancy These guidelines were developed by the California Department of Public Health (CDPH) Sexually Transmitted Diseases (STD) Control Branch
California Guidelines for STD Screening and Treatment in Pregnancy These guidelines were developed by the California Department of Public Health (CDPH) Sexually Transmitted Diseases (STD) Control Branch
PROTOCOL FOR THE MANAGEMENT OF CLOSE CONTACTS OF PERTUSSIS INFECTION
 PROTOCOL FOR THE MANAGEMENT OF CLOSE CONTACTS OF PERTUSSIS INFECTION Printed copies must not be considered the definitive version DOCUMENT CONTROL PROTOCOL NO. 1.03 Policy Group Infection Control Committee
PROTOCOL FOR THE MANAGEMENT OF CLOSE CONTACTS OF PERTUSSIS INFECTION Printed copies must not be considered the definitive version DOCUMENT CONTROL PROTOCOL NO. 1.03 Policy Group Infection Control Committee
Lyme Disease in Pregnancy. Dr Sarah Chissell Consultant Obstetrician William Harvey Hospital, Kent
 Lyme Disease in Pregnancy Dr Sarah Chissell Consultant Obstetrician William Harvey Hospital, Kent Conflict of interest My son has chronic Lyme disease Infections in pregnancy Transplacental infection Perinatal
Lyme Disease in Pregnancy Dr Sarah Chissell Consultant Obstetrician William Harvey Hospital, Kent Conflict of interest My son has chronic Lyme disease Infections in pregnancy Transplacental infection Perinatal
Mother s blood test to check her unborn baby s blood group
 Mother s blood test to check her unborn baby s blood group This leaflet explains why it is important to have a blood test to check the baby s blood group, so that only those who need it, receive anti-d
Mother s blood test to check her unborn baby s blood group This leaflet explains why it is important to have a blood test to check the baby s blood group, so that only those who need it, receive anti-d
Assessment of Fetal Growth
 Assessment of Fetal Growth Unit / Trust: 1. INTRODUCTION The aim of this guideline template is to outline the methods used to assess fetal growth and the referral pathways utilising customised antenatal
Assessment of Fetal Growth Unit / Trust: 1. INTRODUCTION The aim of this guideline template is to outline the methods used to assess fetal growth and the referral pathways utilising customised antenatal
Pregnancy and Tuberculosis. Information for clinicians
 Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
Childhood Diseases and potential risks during pregnancy: (All information available on the March of Dimes Web Site.) http://www.modimes.
 Childhood Diseases and potential risks during pregnancy: (All information available on the March of Dimes Web Site.) http://www.modimes.org/ Fifth disease (erythema infectiosum) is a common, mild, childhood
Childhood Diseases and potential risks during pregnancy: (All information available on the March of Dimes Web Site.) http://www.modimes.org/ Fifth disease (erythema infectiosum) is a common, mild, childhood
GLOBAL CONCERNS ABOUT HPV VACCINES FACT SHEET
 GLOBAL CONCERNS ABOUT HPV VACCINES FACT SHEET When detected, HPV infection is easily managed and rarely proceeds to cancer Very few women with HPV develop cervical cancer HPV infections are only one of
GLOBAL CONCERNS ABOUT HPV VACCINES FACT SHEET When detected, HPV infection is easily managed and rarely proceeds to cancer Very few women with HPV develop cervical cancer HPV infections are only one of
Neural tube defects: open spina bifida (also called spina bifida cystica)
 Screening Programmes Fetal Anomaly Neural tube defects: open spina bifida (also called spina bifida cystica) Information for health professionals Publication date: April 2012 Review date: April 2013 Version
Screening Programmes Fetal Anomaly Neural tube defects: open spina bifida (also called spina bifida cystica) Information for health professionals Publication date: April 2012 Review date: April 2013 Version
Management of HIV in Pregnancy
 Green-top Guideline No. 39 June 2010 Management of HIV in Pregnancy Management of HIV in Pregnancy This is the second edition of this guideline, which was originally published in 2004 under the same title.
Green-top Guideline No. 39 June 2010 Management of HIV in Pregnancy Management of HIV in Pregnancy This is the second edition of this guideline, which was originally published in 2004 under the same title.
MANAGING HERPES. Living and loving with hsv. American Social Health association. by Charles Ebel & Anna Wald, M.D., M.P.H.
 MANAGING HERPES Living and loving with hsv by Charles Ebel & Anna Wald, M.D., M.P.H. American Social Health association RESEARCH TRIANGLE PARK, NORTH CAROLINA contents contents Preface xi Acknowledgments
MANAGING HERPES Living and loving with hsv by Charles Ebel & Anna Wald, M.D., M.P.H. American Social Health association RESEARCH TRIANGLE PARK, NORTH CAROLINA contents contents Preface xi Acknowledgments
Women, Children and Sexual Health Division Maternity Services. Guideline: Anti D- Prophylaxis
 Women, Children and Sexual Health Division Maternity Services Guideline: Anti D- Prophylaxis 1. Introduction The National Institute for Clinical Excellence recommend routine antenatal anti-d prophylaxis
Women, Children and Sexual Health Division Maternity Services Guideline: Anti D- Prophylaxis 1. Introduction The National Institute for Clinical Excellence recommend routine antenatal anti-d prophylaxis
Cytomegalovirus (HHV5/CMV) Roseolovirus (HHV6 & 7)
 Betaherpesvirinae Cytomegalovirus (HHV5/CMV) Roseolovirus (HHV6 & 7) CYTOMEGALOVIRUS CMV is thought to be amongst the oldest type of herpesvirus in evolutionary terms. CMV is the prototype of beta-herpesviruses
Betaherpesvirinae Cytomegalovirus (HHV5/CMV) Roseolovirus (HHV6 & 7) CYTOMEGALOVIRUS CMV is thought to be amongst the oldest type of herpesvirus in evolutionary terms. CMV is the prototype of beta-herpesviruses
Vaccines in Pregnancy MARK H. SAWYER, MD UCSD SCHOOL OF MEDICINE RADY CHILDREN S HOSPITAL SAN DIEGO
 Vaccines in Pregnancy MARK H. SAWYER, MD UCSD SCHOOL OF MEDICINE RADY CHILDREN S HOSPITAL SAN DIEGO 1 Objectives List vaccines that should be given either during pregnancy or immediately post-partum in
Vaccines in Pregnancy MARK H. SAWYER, MD UCSD SCHOOL OF MEDICINE RADY CHILDREN S HOSPITAL SAN DIEGO 1 Objectives List vaccines that should be given either during pregnancy or immediately post-partum in
AUSTRALIA AND NEW ZEALAND FACTSHEET
 AUSTRALIA AND NEW ZEALAND FACTSHEET What is Stillbirth? In Australia and New Zealand, stillbirth is the death of a baby before or during birth, from the 20 th week of pregnancy onwards, or 400 grams birthweight.
AUSTRALIA AND NEW ZEALAND FACTSHEET What is Stillbirth? In Australia and New Zealand, stillbirth is the death of a baby before or during birth, from the 20 th week of pregnancy onwards, or 400 grams birthweight.
3/25/2014. April 3, 2014. Dennison MM, et al. Ann Intern Med. 2014;160:293 300.
 April 3, 2014 3.6 million persons ever infected; 2.7 million chronic infections 1 Up to 75% unaware of status Transmitted through percutaneous exposure to infected blood Injection drug use (IDU) is the
April 3, 2014 3.6 million persons ever infected; 2.7 million chronic infections 1 Up to 75% unaware of status Transmitted through percutaneous exposure to infected blood Injection drug use (IDU) is the
Clinical Policy Title: Home uterine activity monitoring
 Clinical Policy Title: Home uterine activity monitoring Clinical Policy Number: 12.01.01 Effective Date: August 19, 2015 Initial Review Date: July 17, 2013 Most Recent Review Date: July 15, 2015 Next Review
Clinical Policy Title: Home uterine activity monitoring Clinical Policy Number: 12.01.01 Effective Date: August 19, 2015 Initial Review Date: July 17, 2013 Most Recent Review Date: July 15, 2015 Next Review
CMV: Your questions answered
 The basics about the virus CMV: Your questions answered What is CMV? CMV, or Cytomegalovirus, is a common virus that can infect people of all ages. Once CMV is in a person s body, it stays there for life.
The basics about the virus CMV: Your questions answered What is CMV? CMV, or Cytomegalovirus, is a common virus that can infect people of all ages. Once CMV is in a person s body, it stays there for life.
Caesarean section and quality of obstetric care
 Caesarean section and quality of obstetric care Gjennombruddsprosjekt for keisersnitt September 2014 Michael Robson The National Maternity Hospital Dublin, Ireland [email protected] Gjennombruddsprosjekt
Caesarean section and quality of obstetric care Gjennombruddsprosjekt for keisersnitt September 2014 Michael Robson The National Maternity Hospital Dublin, Ireland [email protected] Gjennombruddsprosjekt
The timing of vaccination with respect to anaesthesia and surgery. 1. Surgery following immunisation with inactivated vaccines
 The timing of vaccination with respect to anaesthesia and surgery Main recommendations: 1. Surgery following immunisation with inactivated vaccines Delay surgery 48 hours post vaccination to avoid postvaccination
The timing of vaccination with respect to anaesthesia and surgery Main recommendations: 1. Surgery following immunisation with inactivated vaccines Delay surgery 48 hours post vaccination to avoid postvaccination
Aciclovir 200mg Tablets Aciclovir 400mg Tablets Aciclovir 800mg Tablets PL 29831/0517 PL 29831/0518 PL 29831/0519 UKPAR
 Aciclovir 200mg Tablets Aciclovir 400mg Tablets Aciclovir 800mg Tablets PL 29831/0517 PL 29831/0518 PL 29831/0519 UKPAR TABLE OF CONTENTS Lay Summary Page 2 Scientific discussion Page 3 Steps taken for
Aciclovir 200mg Tablets Aciclovir 400mg Tablets Aciclovir 800mg Tablets PL 29831/0517 PL 29831/0518 PL 29831/0519 UKPAR TABLE OF CONTENTS Lay Summary Page 2 Scientific discussion Page 3 Steps taken for
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME standard topic: Specialist neonatal care Output: standard advice to the Secretary of State
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME standard topic: Specialist neonatal care Output: standard advice to the Secretary of State
Vaccination against pertussis (whooping cough) - the replacement of Repevax with Boostrix -IPV an update for registered healthcare practitioners
 Vaccination against pertussis (whooping cough) - the replacement of Repevax with Boostrix -IPV an update for registered healthcare practitioners Questions and Answers May 2014 Health Protection Scotland
Vaccination against pertussis (whooping cough) - the replacement of Repevax with Boostrix -IPV an update for registered healthcare practitioners Questions and Answers May 2014 Health Protection Scotland
FAQs HIV & AIDS. What is HIV? A virus that reduces the effectiveness of your immune system, meaning you are less protected against disease.
 HIV & AIDS What is HIV? A virus that reduces the effectiveness of your immune system, meaning you are less protected against disease. What does HIV stand for? Human Immunodeficiency Virus Where did HIV
HIV & AIDS What is HIV? A virus that reduces the effectiveness of your immune system, meaning you are less protected against disease. What does HIV stand for? Human Immunodeficiency Virus Where did HIV
Expedited Partner Therapy (EPT) for Sexually Transmitted Diseases Protocol for Health Care Providers in Oregon
 Expedited Partner Therapy (EPT) for Sexually Transmitted Diseases Protocol for Health Care Providers in Oregon Oregon Health Authority Center for Public Health Practice HIV/STD/TB Section Principles of
Expedited Partner Therapy (EPT) for Sexually Transmitted Diseases Protocol for Health Care Providers in Oregon Oregon Health Authority Center for Public Health Practice HIV/STD/TB Section Principles of
THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives
 THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives Ellen Blix Doctoral thesis at the Nordic School of Public
THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives Ellen Blix Doctoral thesis at the Nordic School of Public
Fact Sheet for Health Care Providers: Interpreting Results from the Aptima Zika Virus Assay. June 17, 2016
 Dear Health Care Provider: Fact Sheet for Health Care Providers: Interpreting Results from the Aptima Zika Virus Assay June 17, 2016 The U.S. Food and Drug Administration (FDA) has issued an Emergency
Dear Health Care Provider: Fact Sheet for Health Care Providers: Interpreting Results from the Aptima Zika Virus Assay June 17, 2016 The U.S. Food and Drug Administration (FDA) has issued an Emergency
hiv/aids Programme Use of Antiretroviral Drugs for Treating Pregnant Women and Preventing HIV Infection in Infants
 hiv/aids Programme Programmatic update Use of Antiretroviral Drugs for Treating Pregnant Women and Preventing HIV Infection in Infants EXECUTIVE SUMMARY April 2012 EXECUTIVE SUMMARY Recent developments
hiv/aids Programme Programmatic update Use of Antiretroviral Drugs for Treating Pregnant Women and Preventing HIV Infection in Infants EXECUTIVE SUMMARY April 2012 EXECUTIVE SUMMARY Recent developments
How To Test For Fetal Blood
 Fetal (FBS) / paired cord blood sampling guideline (GL839) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Mr Mark Selinger, Consultant
Fetal (FBS) / paired cord blood sampling guideline (GL839) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Mr Mark Selinger, Consultant
THE QUALITY OF MATERNITY SERVICES IN LONDON: A SUMMARY OF THE HEALTHCARE COMMISSION SURVEYS KEY MESSAGES FOR LONDON:
 THE QUALITY OF MATERNITY SERVICES IN LONDON: A SUMMARY OF THE HEALTHCARE COMMISSION SURVEYS KEY MESSAGES FOR LONDON: London is different: the mobility and diversity of London s pregnant mothers together
THE QUALITY OF MATERNITY SERVICES IN LONDON: A SUMMARY OF THE HEALTHCARE COMMISSION SURVEYS KEY MESSAGES FOR LONDON: London is different: the mobility and diversity of London s pregnant mothers together
PERINATAL HIV. AIIMS- NICU protocols 2008. Sunil Saharan 1, Rakesh Lodha 2, Ramesh Agarwal 2, Ashok Deorari 3, Vinod Paul 3 1
 PERINATAL HIV Sunil Saharan 1, Rakesh Lodha 2, Ramesh Agarwal 2, Ashok Deorari 3, Vinod Paul 3 1 Senior resident, 2 Assistant Professor, 3 Professor Division of Neonatology, Department of Pediatrics All
PERINATAL HIV Sunil Saharan 1, Rakesh Lodha 2, Ramesh Agarwal 2, Ashok Deorari 3, Vinod Paul 3 1 Senior resident, 2 Assistant Professor, 3 Professor Division of Neonatology, Department of Pediatrics All
Bachelor s degree in Nursing (Midwifery)
 Tbilisi State Medical University Faculty of Physical Medicine and Rehabilitation The first level of academic higher education Bachelor s degree in Nursing (Midwifery) TBILISI 2012 Name of qualification
Tbilisi State Medical University Faculty of Physical Medicine and Rehabilitation The first level of academic higher education Bachelor s degree in Nursing (Midwifery) TBILISI 2012 Name of qualification
Obstetric Cholestasis (itching liver disorder) Information for parents-to-be
 Oxford University Hospitals NHS Trust Obstetric Cholestasis (itching liver disorder) Information for parents-to-be page 2 You have been given this leaflet because you have been diagnosed with (or are suspected
Oxford University Hospitals NHS Trust Obstetric Cholestasis (itching liver disorder) Information for parents-to-be page 2 You have been given this leaflet because you have been diagnosed with (or are suspected
ABSTRACT LABOR AND DELIVERY
 ABSTRACT POLICY Prior to fetal viability, intentionally undertaking delivery of a fetus is the equivalent of abortion and is not permissible. After fetal viability has been reached, intentionally undertaking
ABSTRACT POLICY Prior to fetal viability, intentionally undertaking delivery of a fetus is the equivalent of abortion and is not permissible. After fetal viability has been reached, intentionally undertaking
Rural Health Advisory Committee s Rural Obstetric Services Work Group
 Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
HIV/AIDS: General Information & Testing in the Emergency Department
 What Is HIV? HIV/AIDS: General Information & Testing in the Emergency Department HIV is the common name for the Human Immunodeficiency Virus. HIV is a retrovirus. This means it can enter the body s own
What Is HIV? HIV/AIDS: General Information & Testing in the Emergency Department HIV is the common name for the Human Immunodeficiency Virus. HIV is a retrovirus. This means it can enter the body s own
Tdap booster vaccine for Health Care Workers Frequently Asked Questions for Health Professionals
 Tdap booster vaccine for Health Care Workers Frequently Asked Questions for Health Professionals NEW items in 2013 Immunisation Guidelines for Ireland are in RED What is Tdap booster vaccine? Tdap is a
Tdap booster vaccine for Health Care Workers Frequently Asked Questions for Health Professionals NEW items in 2013 Immunisation Guidelines for Ireland are in RED What is Tdap booster vaccine? Tdap is a
SWISS SOCIETY OF NEONATOLOGY. Umbilical cord complications in two subsequent pregnancies
 SWISS SOCIETY OF NEONATOLOGY Umbilical cord complications in two subsequent pregnancies June 2006 2 Hetzel PG, Godi E, Bührer C, Department of Neonatology (HPG, BC), University Children s Hospital, Basel,
SWISS SOCIETY OF NEONATOLOGY Umbilical cord complications in two subsequent pregnancies June 2006 2 Hetzel PG, Godi E, Bührer C, Department of Neonatology (HPG, BC), University Children s Hospital, Basel,
Oregon Birth Outcomes, by Planned Birth Place and Attendant Pursuant to: HB 2380 (2011)
 Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Chapter 3: Healthy Start Risk Screening
 Introduction Healthy Start legislation requires that all pregnant women and infants be offered screening for risk factors that may affect their pregnancy, health, or development. The prenatal and infant
Introduction Healthy Start legislation requires that all pregnant women and infants be offered screening for risk factors that may affect their pregnancy, health, or development. The prenatal and infant
When an occupational exposure occurs, the source patient should be evaluated for both hepatitis B and hepatitis C. (AII)
 XI. OCCUPATIONAL EXPOSURES TO HEPATITIS B AND C RECOMMENDATION: When an occupational exposure occurs, the source patient should be evaluated for both hepatitis B and hepatitis C. (AII) The risk of transmission
XI. OCCUPATIONAL EXPOSURES TO HEPATITIS B AND C RECOMMENDATION: When an occupational exposure occurs, the source patient should be evaluated for both hepatitis B and hepatitis C. (AII) The risk of transmission
Transient Hypogammaglobulinemia of Infancy. Chapter 7
 Transient Hypogammaglobulinemia of Infancy Chapter 7 An unborn baby makes no IgG (antibody) and only slowly starts producing it after birth. However, starting at about the sixth month of pregnancy, the
Transient Hypogammaglobulinemia of Infancy Chapter 7 An unborn baby makes no IgG (antibody) and only slowly starts producing it after birth. However, starting at about the sixth month of pregnancy, the
Guideline. Treatment of tuberculosis in pregnant women and newborn infants. Version 3.0
 Guideline Treatment of tuberculosis in pregnant women and newborn infants Version 3.0 Key critical points The decision to treat tuberculosis (TB) in pregnancy must consider the potential risks to mother
Guideline Treatment of tuberculosis in pregnant women and newborn infants Version 3.0 Key critical points The decision to treat tuberculosis (TB) in pregnancy must consider the potential risks to mother
Substance Use Guideline 4B PERINATAL OPIOID EXPOSURE, CARE OF THE NEWBORN
 British Columbia Reproductive Care Program Substance Use Guideline 4B PERINATAL OPIOID EXPOSURE, CARE OF THE NEWBORN INTRODUCTION During the antenatal period, the opportunity exists for the primary care
British Columbia Reproductive Care Program Substance Use Guideline 4B PERINATAL OPIOID EXPOSURE, CARE OF THE NEWBORN INTRODUCTION During the antenatal period, the opportunity exists for the primary care
Management of Pregnancy. Opioid Addiction Treatment
 Management of Pregnancy Opioid Addiction Treatment Perinatal Opioid Addiction Pharmacotherapy and co-ordination of care are essential elements in the comprehensive care of pregnant patients with opioid
Management of Pregnancy Opioid Addiction Treatment Perinatal Opioid Addiction Pharmacotherapy and co-ordination of care are essential elements in the comprehensive care of pregnant patients with opioid
EPIDEMIOLOGY OF HEPATITIS B IN IRELAND
 EPIDEMIOLOGY OF HEPATITIS B IN IRELAND Table of Contents Acknowledgements 3 Summary 4 Introduction 5 Case Definitions 6 Materials and Methods 7 Results 8 Discussion 11 References 12 Epidemiology of Hepatitis
EPIDEMIOLOGY OF HEPATITIS B IN IRELAND Table of Contents Acknowledgements 3 Summary 4 Introduction 5 Case Definitions 6 Materials and Methods 7 Results 8 Discussion 11 References 12 Epidemiology of Hepatitis
CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE
 CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Obstetric Early Warning Score Guideline Implementation
CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Obstetric Early Warning Score Guideline Implementation
Evaluation and Follow-up of Fetal Hydronephrosis
 Evaluation and Follow-up of Fetal Hydronephrosis Deborah M. Feldman, MD, Marvalyn DeCambre, MD, Erin Kong, Adam Borgida, MD, Mujgan Jamil, MBBS, Patrick McKenna, MD, James F. X. Egan, MD Objective. To
Evaluation and Follow-up of Fetal Hydronephrosis Deborah M. Feldman, MD, Marvalyn DeCambre, MD, Erin Kong, Adam Borgida, MD, Mujgan Jamil, MBBS, Patrick McKenna, MD, James F. X. Egan, MD Objective. To
150 7,114,974 75.8 -53-3.2 -3.6 -2.9. making progress
 Per 1 LB African Region Maternal and Perinatal Health Profile Department of Maternal, Newborn, Child and Adolescent Health (MCA/WHO) Demographics and Information System Health status indicators - Maternal
Per 1 LB African Region Maternal and Perinatal Health Profile Department of Maternal, Newborn, Child and Adolescent Health (MCA/WHO) Demographics and Information System Health status indicators - Maternal
Case Finding for Hepatitis B and Hepatitis C
 Case Finding for Hepatitis B and Hepatitis C John W. Ward, M.D. Division of Viral Hepatitis Centers for Disease Control and Prevention Atlanta, Georgia, USA Division of Viral Hepatitis National Center
Case Finding for Hepatitis B and Hepatitis C John W. Ward, M.D. Division of Viral Hepatitis Centers for Disease Control and Prevention Atlanta, Georgia, USA Division of Viral Hepatitis National Center
Prevention of Pertussis Among Pregnant & Post Partum Women and Their Infants. Marilyn Michels RN MSN CIC Kathleen Curtis MS RN
 Prevention of Pertussis Among Pregnant & Post Partum Women and Their Infants Marilyn Michels RN MSN CIC Kathleen Curtis MS RN Pertussis and Adults Pertussis (whooping cough) a poorly controlled vaccine-preventable
Prevention of Pertussis Among Pregnant & Post Partum Women and Their Infants Marilyn Michels RN MSN CIC Kathleen Curtis MS RN Pertussis and Adults Pertussis (whooping cough) a poorly controlled vaccine-preventable
Guidelines for Vaccinating Pregnant Women
 Guidelines for Vaccinating Pregnant Women U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Disease Control & Prevention Guidelines for Vaccinating Pregnant Women from Recommendations of the Advisory
Guidelines for Vaccinating Pregnant Women U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Disease Control & Prevention Guidelines for Vaccinating Pregnant Women from Recommendations of the Advisory
Policy Clinical Guideline South Australian Perinatal Practice Guidelines neonatal sepsis (including maternal group B streptococcal colonisation)
 Policy Clinical Guideline South Australian Perinatal Practice Guidelines neonatal sepsis (including maternal group B streptococcal colonisation) Policy developed by: SA Maternal & Neonatal Clinical Network
Policy Clinical Guideline South Australian Perinatal Practice Guidelines neonatal sepsis (including maternal group B streptococcal colonisation) Policy developed by: SA Maternal & Neonatal Clinical Network
Zika virus infection: guidance for primary care
 Introduction There is an ongoing outbreak of Zika virus infection, mostly focussed in South and Central America and the Caribbean. Based on a growing body of research, there is scientific consensus that
Introduction There is an ongoing outbreak of Zika virus infection, mostly focussed in South and Central America and the Caribbean. Based on a growing body of research, there is scientific consensus that
Health Professionals Advice: Azithromycin now fully funded 3 December 2012
 Health Professionals Advice: Azithromycin now fully funded 3 December 2012 SITUATION UPDATE The Pertussis epidemic has continued all year, and is expected to continue throughout 2013. Between 1 January
Health Professionals Advice: Azithromycin now fully funded 3 December 2012 SITUATION UPDATE The Pertussis epidemic has continued all year, and is expected to continue throughout 2013. Between 1 January
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
PENNSYLVANIA DEPARTMENT OF HEALTH 2015 PAHAN 307 04-02-ADV Pertussis in Centre County
 PENNSYLVANIA DEPARTMENT OF HEALTH 2015 PAHAN 307 04-02-ADV Pertussis in Centre County DATE: 04/02/2015 TO: Health Alert Network FROM: Karen M. Murphy, PhD, RN, Acting Secretary of Health SUBJECT: DISTRIBUTION:
PENNSYLVANIA DEPARTMENT OF HEALTH 2015 PAHAN 307 04-02-ADV Pertussis in Centre County DATE: 04/02/2015 TO: Health Alert Network FROM: Karen M. Murphy, PhD, RN, Acting Secretary of Health SUBJECT: DISTRIBUTION:
Dual elimination of mother-to-child transmission (MTCT) of HIV and syphilis
 Training Course in Sexual and Reproductive Health Research 2014 Module: Principles and Practice of Sexually Transmitted Infections Prevention and Care Dual elimination of mother-to-child transmission (MTCT)
Training Course in Sexual and Reproductive Health Research 2014 Module: Principles and Practice of Sexually Transmitted Infections Prevention and Care Dual elimination of mother-to-child transmission (MTCT)
Alzheimer s and Herpes Zoster
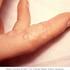 The relationship between Alzheimer's and herpes zoster should be studied. A solid link between herpes simplex virus-1 (HSV1) and Alzheimer's has been found. See: "Cold Sore Virus Linked To Alzheimer's
The relationship between Alzheimer's and herpes zoster should be studied. A solid link between herpes simplex virus-1 (HSV1) and Alzheimer's has been found. See: "Cold Sore Virus Linked To Alzheimer's
A Guide for Hospitals and Health Care Providers Perinatal Substance Use: Promoting Healthy Outcomes
 A Guide for Hospitals and Health Care Providers Perinatal Substance Use: Promoting Healthy Outcomes Virginia Legal Requirements and Health Care Practice Implications Perinatal Care To promote healthy maternal
A Guide for Hospitals and Health Care Providers Perinatal Substance Use: Promoting Healthy Outcomes Virginia Legal Requirements and Health Care Practice Implications Perinatal Care To promote healthy maternal
Maternity Care Primary C-Section Rate Specifications 2014 (07/01/2013 to 06/30/2014 Dates of Service)
 Summary of Changes Denominator Changes: Two additions were made to the denominator criteria. The denominator was changed to include patients who had: a vertex position delivery AND a term pregnancy of
Summary of Changes Denominator Changes: Two additions were made to the denominator criteria. The denominator was changed to include patients who had: a vertex position delivery AND a term pregnancy of
Viral hepatitis. Report by the Secretariat
 SIXTY-THIRD WORLD HEALTH ASSEMBLY A63/15 Provisional agenda item 11.12 25 March 2010 Viral hepatitis Report by the Secretariat THE DISEASES AND BURDEN 1. The group of viruses (hepatitis A, B, C, D and
SIXTY-THIRD WORLD HEALTH ASSEMBLY A63/15 Provisional agenda item 11.12 25 March 2010 Viral hepatitis Report by the Secretariat THE DISEASES AND BURDEN 1. The group of viruses (hepatitis A, B, C, D and
Certified Nurse-Midwife and Women s Health Care Nurse Practitioner
 Certified Nurse-Midwife and Women s Health Care Nurse Practitioner Practice Agreements at Chicago Revised March 2007 TABLE OF CONTENTS SIGNATURES OF AGREEMENT 3 ORGANIZATION RELATIONSHIPS AND MEMBERSHIP
Certified Nurse-Midwife and Women s Health Care Nurse Practitioner Practice Agreements at Chicago Revised March 2007 TABLE OF CONTENTS SIGNATURES OF AGREEMENT 3 ORGANIZATION RELATIONSHIPS AND MEMBERSHIP
Caring for Vulnerable Babies: The reorganisation of neonatal services in England
 Caring for Vulnerable Babies: The reorganisation of neonatal services in England LONDON: The Stationery Office 13.90 Ordered by the House of Commons to be printed on 17 December 2007 REPORT BY THE COMPTROLLER
Caring for Vulnerable Babies: The reorganisation of neonatal services in England LONDON: The Stationery Office 13.90 Ordered by the House of Commons to be printed on 17 December 2007 REPORT BY THE COMPTROLLER
117 4,904,773 -67-4.7 -5.5 -3.9. making progress
 Per 1 LB Eastern Mediterranean Region Maternal and Perinatal Health Profile Department of Maternal, Newborn, Child and Adolescent Health (MCA/WHO) Demographics and Information System Health status indicators
Per 1 LB Eastern Mediterranean Region Maternal and Perinatal Health Profile Department of Maternal, Newborn, Child and Adolescent Health (MCA/WHO) Demographics and Information System Health status indicators
NSW Pertussis Control Program 2015
 NSW Pertussis Control Program 2015 Pertussis Disease Pertussis ( whooping cough ) is a bacterial infection affecting the respiratory system, caused by the organism Bordetella pertussis It affects individuals
NSW Pertussis Control Program 2015 Pertussis Disease Pertussis ( whooping cough ) is a bacterial infection affecting the respiratory system, caused by the organism Bordetella pertussis It affects individuals
Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General
 Florida Department of Health Division of Disease Control Bureau of Epidemiology Chronic Disease Epidemiology Section Charlie Crist Governor Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General Florida
Florida Department of Health Division of Disease Control Bureau of Epidemiology Chronic Disease Epidemiology Section Charlie Crist Governor Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General Florida
68 3,676,893 86.7 -49-2.9 -3.2 -2.5. making progress
 Per 1 LB African Region Maternal and Perinatal Health Profile Department of Maternal, Newborn, Child and Adolescent Health (MCA/WHO) Demographics and Information System Health status indicators Maternal
Per 1 LB African Region Maternal and Perinatal Health Profile Department of Maternal, Newborn, Child and Adolescent Health (MCA/WHO) Demographics and Information System Health status indicators Maternal
Bloodborne Pathogens (HIV, HBV, and HCV) Exposure Management
 Bloodborne Pathogens Exposure Policy and Procedures Employees of the State of South Dakota Department of Health Bloodborne Pathogens (HIV, HBV, and HCV) Exposure Management PEP Hotline 1-888-448-4911 DOH
Bloodborne Pathogens Exposure Policy and Procedures Employees of the State of South Dakota Department of Health Bloodborne Pathogens (HIV, HBV, and HCV) Exposure Management PEP Hotline 1-888-448-4911 DOH
Perinatal Substance Use: Promoting Healthy Outcomes
 A Guide for Hospitals and Health Care Providers Perinatal Substance Use: Promoting Healthy Outcomes Virginia Legal Requirements and Health Care Practice Implications Perinatal Care To promote healthy maternal
A Guide for Hospitals and Health Care Providers Perinatal Substance Use: Promoting Healthy Outcomes Virginia Legal Requirements and Health Care Practice Implications Perinatal Care To promote healthy maternal
Epidemiology 521. Epidemiology of Maternal and Child Health Problems. Winter / Spring, 2010
 Extended MPH Degree Program School of Public Health Department of Epidemiology University of Washington Epidemiology 521 Epidemiology of Maternal and Child Health Problems Winter / Spring, 2010 Instructor:
Extended MPH Degree Program School of Public Health Department of Epidemiology University of Washington Epidemiology 521 Epidemiology of Maternal and Child Health Problems Winter / Spring, 2010 Instructor:
Evaluation of cardiotocographic and cord blood changes in induced labor with dinoprostone and misoprostol
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Pandey K et al. Int J Reprod Contracept Obstet Gynecol. 2014 Mar;3(1):199-203 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Pandey K et al. Int J Reprod Contracept Obstet Gynecol. 2014 Mar;3(1):199-203 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC)
 CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC) 1. Aim/Purpose of this Guideline 1.1. Due to a rise in the caesarean section rate there are increasing numbers of pregnant women who
CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC) 1. Aim/Purpose of this Guideline 1.1. Due to a rise in the caesarean section rate there are increasing numbers of pregnant women who
