MEDICAL POLICY No R0 KNEE ARTHROSCOPY I. POLICY/CRITERIA
|
|
|
- Darleen McCoy
- 9 years ago
- Views:
Transcription
1 KNEE ARTHROSCOPY MEDICAL POLICY Effective Date: March 24, 2014 Review Dates: 4/11, 4/12, 4/13, 5/14, 5/15, 5/16 Date Of Origin: April 13, 2011 Status: Current I. POLICY/CRITERIA Knee arthroscopy is covered for the following indications when the stated criteria are met. 1. Diagnosis or treatment of intra-articular joint pathology. One or more of the following must be present: a. Fracture treatment b. Loose bodies or foreign body, demonstrated on imaging studies c. A true locked knee (knee that will flex but not fully extend) d. Failure of at least 8 weeks of conservative management, including: i. Anti-inflammatory medication (NSAIDs), unless contraindicated ii. At least one corticosteroid injection or one course of hyaluronate injections (HA), and iii. Physical therapy e. Suspected plica syndrome, when symptoms persist after 8 weeks of conservative management (anti-inflammatory medication and PT) 2. Repair of an osteochondral defect, including osteochondral dissecans. All of the following must be present: a. Osteochondral defect is demonstrated on imaging studies b. One of the following clinical conditions: i. Osteochondral lesion displacement or unstable lesion ii. Loose body or bodies are present iii. Nondisplaced osteochondral lesion in adult (defined as closed growth plates) iv. Nondisplaced osteochondral lesion in child (defined as open growth plate) and stable lesion < 2 cm 2 that does not respond to conservative care for greater than 3 months, such as physical therapy, immobilization and partial weight-bearing, progressing to gradual weight-bearing, as tolerated, with radiographic evidence of healing 3. Symptomatic acute meniscal tear on exam or MRI. One of the following must be present: a. Bucket handle tear, symptomatic horizontal cleavage tear, radial tear, posterior horn tear, complex tear, or a displaced/unstable meniscal fragment on MRI b. Symptomatic meniscal tear on exam with catching, locking or instability Page 1 of 9
2 c. Continued symptoms and/or disability following a failed 8 week course of conservative treatment (e.g. physical therapy and NSAIDs if not contraindicated) 4. Knee osteoarthritis with a concomitant meniscal tear when any of the following are present: a. Symptomatic bucket handle tear with catching or locking on exam or MRI b. Displaced or unstable symptomatic meniscal fragment on MRI c. Acute traumatic tear and failed 8-week non-operative program d. Age 45 and older, and all of the following: i. Kellgren-Lawrence Grade* 1 or 2 knee osteoarthritis ii. A minimum of eight (8) physical therapy visits iii. A minimum of three weeks of anti-inflammatory medications (unless contraindicated) iv. At least one corticosteroid injection or one course of hyaluronate injections 5. Reconstruction of anterior cruciate ligament (ACL). All of the following are required: a. Evidence of torn ACL on clinical exam or imaging, with one or more of the following: i. Anterior drawer sign is positive for ACL laxity ii. Positive pivot shift test iii. Positive Lachman test b. One of the following i. ACL tear occurred with other major ligamentous injury, such as the medial or posterior collateral ligament, the posterior cruciate ligament or a posterolateral corner ligamentous injury ii. Failure of at least 8 weeks of conservative management, such as immobilization, knee brace and physical therapy iii. Patient s occupation is highly physically demanding, such as law enforcement, firefighter or other safety personnel, construction, or high-performance athlete participating in cutting, jumping, and pivoting sports (skiing, tennis, basketball, football) 6. Debridement, drainage, or lavage for one or more of the following: a. Rheumatoid arthritis b. Septic joint or osteomyelitis c. Septic prosthetic joint d. Postoperative arthrofibrosis (occurring after ACL repair or total knee replacement) when there is a loss of range of motion and failure to respond to nonoperative care, such as physical therapy, or manipulation under anesthesia 7. Repair or reconstruction of posterior cruciate ligament (PCL). All of the following are required: a. Evidence of torn PCL on clinical exam, with one or more of the following: i. Posterior drawer sign is positive for laxity of the PCL Page 2 of 9
3 ii. Positive reversed pivot shift test iii. Positive posterior sag sign b. Diagnostic imaging demonstrates PCL tear c. PCL tear occurred with other injuries, such as injury to the posterolateral corner of the knee, medial collateral ligament tear, ACL tear, avulsion fracture of fibular head or avulsion of the tibia distal to the lateral plateau 8. Excision of popliteal (Baker) cyst. All of the following are required: a. Visible or palpable bulge in popliteal fossa on clinical exam, or diagnostic imaging demonstrating the presence of the cyst b. Failure of at least 8 weeks of conservative treatment, such as activity modification, anti-inflammatory medication or treatment of intra-articular pathology such as rheumatoid arthritis 9. Synovectomy. One or more of the following must be present: a. Rheumatoid arthritis b. Hemophiliac joint disease c. Localized pigmented villonodular synovitis d. Other chronic inflammatory conditions such as antibiotic-resistant Lyme arthritis 10. Lateral retinacular release for patellar pathology, with one or more of the following: a. Lateral patellar compression syndrome, when either a positive patella glide or tilt test is present b. Procedure concurrent with other patellar realignment procedures Knee arthroscopy is not covered for the following indications because they are not considered medically necessary. 1. Arthroscopic debridement or lavage for a primary diagnosis of symptomatic knee osteoarthritis without a meniscal tear. 2. Knee osteoarthritis Kellgren-Lawrence grade* 3 or 4 with a meniscal tear NOT meeting any of the criteria listed above. 3. Knee Osteoarthritis *Kellgren-Lawrence Grading Scale Grade 1: doubtful narrowing of joint space and possible osteophytic lipping Grade 2: definite osteophytes, definite narrowing of joint space Grade 3: moderate multiple osteophytes, definite narrowing of joint space, some sclerosis and possible deformity of bone contour Grade 4: large osteophytes, marked narrowing of joint space, severe sclerosis and definite deformity of bone contour II. MEDICAL NECESSITY REVIEW Required Not Required Not Applicable Page 3 of 9
4 III. APPLICATION TO PRODUCTS Coverage is subject to member s specific benefits. Group specific policy will supersede this policy when applicable. HMO/EPO: This policy applies to insured HMO/EPO plans. POS: This policy applies to insured POS plans. PPO: This policy applies to insured PPO plans. Consult individual plan documents as state mandated benefits may apply. If there is a conflict between this policy and a plan document, the provisions of the plan document will govern. ASO: For self-funded plans, consult individual plan documents. If there is a conflict between this policy and a self-funded plan document, the provisions of the plan document will govern. INDIVIDUAL: For individual policies, consult the individual insurance policy. If there is a conflict between this medical policy and the individual insurance policy document, the provisions of the individual insurance policy will govern. MEDICARE: Coverage is determined by the Centers for Medicare and Medicaid Services (CMS); if a coverage determination has not been adopted by CMS, this policy applies. MEDICAID/HEALTHY MICHIGAN PLAN: For Medicaid/Healthy Michigan Plan members, this policy will apply. Coverage is based on medical necessity criteria being met and the appropriate code(s) from the coding section of this policy being included on the Michigan Medicaid Fee Schedule located at: If there is a discrepancy between this policy and the Michigan Medicaid Provider Manual located at: the Michigan Medicaid Provider Manual will govern. For Medical Supplies/DME/Prosthetics and Orthotics, please refer to the Michigan Medicaid Fee Schedule to verify coverage. IV. DESCRIPTION An arthroscope is a small fiberoptic telescope, used to visualize the inside of a joint for damaged tissue. The most common types of knee arthroscopic surgery include repair of a torn meniscus, ligament reconstruction, removal of loose debris and trimming damaged cartilage. Arthroscopy is less traumatic than an open surgical procedure. The smaller incisions promote faster healing and a more rapid recovery. V. CODING INFORMATION ICD-10 Codes that may apply: A18.02 Tuberculous arthritis of other joints K68.11 Postprocedural retroperitoneal abscess M M Staphylococcal arthritis, knee M M Pneumococcal arthritis, knee M M Other streptococcal arthritis, knee M M Arthritis due to other bacteria, knee M01.x61 - M01.x69 Direct infection of knee in infectious and parasitic diseases classified elsewhere Page 4 of 9
5 M M Other reactive arthropathies, knee M M Felty s syndrome, knee M M Rheumatoid arthritis of knee with involvement of other organs and systems M M Rheumatoid arthritis with rheumatoid factor of knee without organ or systems involvement M M Other rheumatoid arthritis with rheumatoid factor of knee M M Rheumatoid arthritis without rheumatoid factor, knee M06.1 Adult-onset Still's disease M M Rheumatoid nodule, knee M M Other specified rheumatoid arthritis, knee M08.3 Juvenile rheumatoid polyarthritis (seronegative) M M Pauciarticular juvenile rheumatoid arthritis, knee M Other specified crystal arthropathies, unspecified knee M M Villonodular synovitis (pigmented), knee M M22.02 Recurrent dislocation of patella, knee M M22.12 Recurrent subluxation of patella, knee M22.2x1 - M22.2x9 Patellofemoral disorders, knee M22.3x1 - M22.3x9 Other derangements of patella, knee M M22.42 Chondromalacia patellae, knee M22.8x1 - M22.8x9 Other disorders of patella, right knee M M22.92 Unspecified disorder of patella, knee M M Cystic M M Derangement of l meniscus M M Other meniscus derangements M M23.52 Chronic instability of knee M M Other spontaneous disruption of ligament of knee M23.8x1 - M23.8x9 Other internal derangements of knee M M23.92 Unspecified internal derangement of knee M M Pathological dislocation of knee M M Recurrent dislocation, knee M M Contracture, knee M M Ankylosis, knee M24.80 Other specific joint derangements of unspecified joint, not elsewhere classified M M Fistula, knee M M Flail joint, knee M M Other instability, knee M36.2 Hemophilic arthropathy M36.3 Arthropathy in other blood disorders M42.9 Spinal osteochondrosis, unspecified M M Abscess of tendon sheath, lower leg M M Other infective (teno)synovitis, knee M M Other synovitis and tenosynovitis, lower leg M M Other synovitis and tenosynovitis, lower leg M66.0 Rupture of popliteal cyst M M Synovial hypertrophy, not elsewhere classified, lower leg M M Transient synovitis, knee M M67.52 Plica syndrome, knee Page 5 of 9
6 M M Other specified disorders of synovium, knee M M Other specified disorders of tendon, knee M Other specified disorders of tendon, knee M Other specified disorders of synovium and tendon, unspecified knee M M Abscess of bursa, knee M M71.22 Synovial cyst of popliteal space [Baker], knee M M Other specified bursopathies, knee M85.9 Disorder of bone density and structure, unspecified M86.8x6 Other osteomyelitis, lower leg M86.9 Osteomyelitis, unspecified M89.9 Disorder of bone, unspecified M M Osteopathy in diseases classified elsewhere, lower leg M M Osteochondritis dissecans, knee M M Osteochondropathy, unspecified, lower leg M99.86 Other biomechanical lesions of lower extremity Q68.2 Congenital deformity of knee Q74.1 Congenital malformation of knee S72.411A - S72.416S Displaced unspecified condyle fracture of lower end of femur, for fracture S72.421A - S72.426S Displaced fracture of lateral condyle of femur, for fracture S72.431A - S72.431S Displaced fracture of medial condyle of femur, for fracture S72.433A - S72.433S Displaced fracture of medial condyle of unspecified femur, for fracture S72.434A - S72.436S Nondisplaced fracture of medial condyle of femur, for fracture S81.009A - S81.009S Unspecified open wound, unspecified knee S82.001A S82.099S Patella fracture S82.101A - S82.199S Fracture of upper end of tibia S82.831A - S82.832S Fracture of upper and lower end of fibula S83.001A - S83.096S Subluxation\dislocation of patella, initial encounter S83.004A - S83.096S Unspecified dislocation of patella S83.106A - S83.146S Dislocation\subluxation of proximal end of tibia, knee S83.200A - S83.202S Bucket-handle tear of unspecified meniscus, current injury, knee S83.203A - S83.205S Other tear of unspecified meniscus, current injury, knee S83.206A - S83.209S Unspecified tear of unspecified meniscus, current injury, knee S83.211A - S83.219S Bucket-handle tear of medial meniscus, current injury, knee S83.221A - S83.229S Peripheral tear of medial meniscus, current injury, knee S83.231A - S83.239S Complex tear of medial meniscus, current injury, knee S83.241A - S83.249S Other tear of medial meniscus, current injury, knee S83.251A - S83.259S Bucket-handle tear of lateral meniscus, current injury, knee S83.261A - S83.269S Peripheral tear of lateral meniscus, current injury, knee S83.271A - S83.279S Complex tear of lateral meniscus, current injury, knee S83.281A - S83.289S Other tear of lateral meniscus, current injury, knee S83.30xA - S83.32xS S89.001A - S89.009S Tear of articular cartilage of unspecified knee Unspecified physeal fracture of upper end of t tibia, for closed fracture Page 6 of 9
7 S89.011A - S89.049S S89.091A - S89.099S S89.80xA - S89.92xS T81.4xxA - T81.4xxS T84.50xA - T84.50xS T84.53xA - T84.54xS T84.7xxA - T84.7xxA Salter-Harris physeal fracture of upper end of tibia, for fracture Other physeal fracture of upper end of right tibia, initial encounter for closed fracture Other specified injuries of lower leg Infection following a procedure, initial encounter Infection and inflammatory reaction due to unspecified internal joint prosthesis Infection and inflammatory reaction due to internal knee prosthesis Infection and inflammatory reaction due to other internal orthopedic prosthetic devices, implants and grafts, CPT/HCPCS Codes Arthroscopically aided treatment of intercondylar spine(s) and/or tuberosity fracture(s) of the knee, with or without manipulation; without internal or external fixation (includes arthroscopy) Arthroscopically aided treatment of intercondylar spine(s) and/or tuberosity fracture(s) of the knee, with or without manipulation; with internal or external fixation (includes arthroscopy) Arthroscopically aided treatment of tibial fracture, proximal (plateau); unicondylar, includes internal fixation, when performed (includes arthroscopy) Arthroscopically aided treatment of tibial fracture, proximal (plateau); bicondylar, includes internal fixation, when performed (includes arthroscopy) Arthroscopy, knee, diagnostic, with or without synovial biopsy (separate procedure) Arthroscopy, knee, surgical; for infection, lavage and drainage Arthroscopy, knee, surgical; with lateral release Arthroscopy, knee, surgical; for removal of loose body or foreign body (eg, osteochondritis dissecans fragmentation, chondral fragmentation) Arthroscopy, knee, surgical; synovectomy, limited (eg, plica or shelf resection) (separate procedure) Arthroscopy, knee, surgical; synovectomy, major, 2 or more compartments (eg, medial or lateral) Arthroscopy, knee, surgical; debridement / shaving or articular cartilage (chondroplasty) Arthroscopy, knee, surgical; abrasion arthroplasty (includes chondroplasty where necessary) or multiple drilling or microfracture Arthroscopy, knee, surgical; with meniscectomy (medial AND lateral, including any meniscal shaving) Arthroscopy, knee, surgical; with meniscectomy (medial OR lateral, including any meniscal shaving) Arthroscopy, knee, surgical; with meniscus repair (medial OR lateral) Arthroscopy, knee, surgical; with meniscus repair (medial AND lateral) Arthroscopy, knee, surgical; with lysis of adhesions, with or without manipulation (separate procedure) Page 7 of 9
8 29885 Arthroscopy, knee, surgical; drilling for osteochondritis dissecans with bone grafting, with or without internal fixation (including debridement of base of lesion) Arthroscopy, knee, surgical; drilling for intact osteochondritis dissecans lesion Arthroscopy, knee, surgical; drilling for intact osteochondritis dissecans lesion with internal fixation Arthroscopically aided anterior cruciate ligament repair/augmentation or reconstruction Arthroscopically aided posterior cruciate ligament repair/augmentation or reconstruction G0289 Arthroscopy, knee, surgical, for removal of loose body, foreign body, debridement/shaving of articular cartilage (chondroplasty) at the time of other surgical knee arthroscopy in a different compartment of the same knee See medical policy Autologous Chondrocyte Implant/Meniscal Allograft/Osteochondral Replacement for criteria for the following codes: Arthroscopy, knee, surgical; osteochondral autograft(s) (eg, mosaicplasty) (includes harvesting of the autograft[s]) Arthroscopy, knee, surgical; osteochondral allograft (eg, mosaicplasty) Arthroscopy, knee, surgical; meniscal transplantation (includes arthrotomy for meniscal insertion), medial or lateral ICD-10 Codes: Non-covered indications for the procedures listed below. M17.0 M17.9 Osteoarthritis of knee M M Pain in knee M M Stiffness of knee CPT/HCPCS Codes: These procedures are not covered for the above diagnoses Arthroscopy, knee, diagnostic, with or without synovial biopsy (separate procedure) Arthroscopy, knee, surgical; debridement/shaving of articular cartilage chondroplasty) VI. REFERENCES 1. Milliman Care Guidelines. Inpatient and Surgical Care. 14th Edition. Knee Arthroscopy. ORG: S-705(ISC). Last update: Nutton RW., Is arthroscopic surgery a beneficial treatment for knee osteoarthritis? Nat Clin Pract Rheumatol Mar;5(3): Brunner F., [zur Studie von Kirkley et a1. "A randomized trial of arthroscopic surgery for osteoarthritis of the knee"], Praxis(Bern1994).2008 Dec17;97(25):1347. Gennan. Page 8 of 9
9 4. Koch P., [zur Studie von Kirkley et a1. "A randomized trial of arthroscopic surgery for osteoarthritis of the knee"], Praxis (Benl 1994) Dec 17;97(25):1346. Gennan. 5. Richmond JC., Surgery for osteoarthritis of the knee. Med Clin North Am Jan;93(1):213-22, xii. 6. Jager A., [Gonarthrosis. Is the arthroscopic therapy meaningless?], MMW Fortschr Med Nov 6;150(45):19. Gennan. 7. Roos H, Karlsson J, Svensson 0, Engebretsen L, Renstrom P, Dahlberg L., [Arthroscopy in knee osteoarthritis is one thing--surgery of the menisci another], Lakartidningen Oct 15-21;105(42): Swedish. 8. Bruun N., [Arthroscopic treatment of knee osteoarthritis is not better than conservative treatment], Ugeskr Laeger Oct 20;170(43):3446. Danish. No abstract available. 9. Hawker G, Guan J, Judge A, Dieppe P., Knee arthroscopy in England and Ontario: patterns of use, changes over time, and relationship to Joint Surg Am Nov;90(11): Osteoarthritis of the Knee: Selected Treatments, Aetna Clinical Policy (Retrieved March 27, 2014 & March 30, 2016). AMA CPT Copyright Statement: All Current Procedure Terminology (CPT) codes, descriptions, and other data are copyrighted by the American Medical Association. This document is for informational purposes only. It is not an authorization, certification, explanation of benefits, or contract. Receipt of benefits is subject to satisfaction of all terms and conditions of coverage. Eligibility and benefit coverage are determined in accordance with the terms of the member s plan in effect as of the date services are rendered. Priority Health s medical policies are developed with the assistance of medical professionals and are based upon a review of published and unpublished information including, but not limited to, current medical literature, guidelines published by public health and health research agencies, and community medical practices in the treatment and diagnosis of disease. Because medical practice, information, and technology are constantly changing, Priority Health reserves the right to review and update its medical policies at its discretion. Priority Health s medical policies are intended to serve as a resource to the plan. They are not intended to limit the plan s ability to interpret plan language as deemed appropriate. Physicians and other providers are solely responsible for all aspects of medical care and treatment, including the type, quality, and levels of care and treatment they choose to provide. The name Priority Health and the term plan mean Priority Health, Priority Health Managed Benefits, Inc., Priority Health Insurance Company and Priority Health Government Programs, Inc. Page 9 of 9
KNEE ARTHROSCOPY. Effective Date: March 24, 2014 Review Dates: 4/11, 4/12, 4/13, 5/14, 5/15
 KNEE ARTHROSCOPY MEDICAL POLICY Effective Date: March 24, 2014 Review Dates: 4/11, 4/12, 4/13, 5/14, 5/15 Date Of Origin: April 13, 2011 Status: Current I. POLICY/CRITERIA Knee arthroscopy is covered for
KNEE ARTHROSCOPY MEDICAL POLICY Effective Date: March 24, 2014 Review Dates: 4/11, 4/12, 4/13, 5/14, 5/15 Date Of Origin: April 13, 2011 Status: Current I. POLICY/CRITERIA Knee arthroscopy is covered for
ELBOW REPLACEMENT SURGERY (ARTHROPLASTY)
 Protocol: ORT014 Effective Date: August 1, 2015 ELBOW REPLACEMENT SURGERY (ARTHROPLASTY) Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE... 1 U.S. FOOD AND DRUG ADMINISTRATION
Protocol: ORT014 Effective Date: August 1, 2015 ELBOW REPLACEMENT SURGERY (ARTHROPLASTY) Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE... 1 U.S. FOOD AND DRUG ADMINISTRATION
Anatomy and Physiology 101 for Attorneys
 Knee Injuries Anatomy and Physiology 101 for Attorneys Phil Davidson, MD Heiden-Davidson Orthopedics Salt Lake City, UT May 2011 Introduction Dr. Phil Davidson Park City and SLC clinics Education: Harvard,
Knee Injuries Anatomy and Physiology 101 for Attorneys Phil Davidson, MD Heiden-Davidson Orthopedics Salt Lake City, UT May 2011 Introduction Dr. Phil Davidson Park City and SLC clinics Education: Harvard,
MEDICAL POLICY No. 91503-R4 BLOOD PRESSURE MONITORS & AMBULATORY BLOOD PRESSURE MONITORING
 BLOOD PRESSURE MONITORS & Effective Date: December 21, 2015 Review Dates: 01/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14, 11/15 Date Of Origin: January 19, 2005 Status: Current
BLOOD PRESSURE MONITORS & Effective Date: December 21, 2015 Review Dates: 01/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14, 11/15 Date Of Origin: January 19, 2005 Status: Current
Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine
 Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine Anterior Cruciate Ligament Injury Injury to the anterior cruciate ligament (ACL) is common, especially in athletic
Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine Anterior Cruciate Ligament Injury Injury to the anterior cruciate ligament (ACL) is common, especially in athletic
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
Patellofemoral Chondrosis
 Patellofemoral Chondrosis What is PF chondrosis? PF chondrosis (cartilage deterioration) is the softening or loss of smooth cartilage, most frequently that which covers the back of the kneecap, but the
Patellofemoral Chondrosis What is PF chondrosis? PF chondrosis (cartilage deterioration) is the softening or loss of smooth cartilage, most frequently that which covers the back of the kneecap, but the
Goals. Our Real Goals. Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas. Perform a basic, logical, history and physical exam
 Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas Goals Our Real Goals Perform a basic, logical, history and physical exam on a patient with knee pain Learn through cases, some common
Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas Goals Our Real Goals Perform a basic, logical, history and physical exam on a patient with knee pain Learn through cases, some common
ORTHOPAEDIC KNEE CONDITIONS AND INJURIES
 11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
AAOS Guideline of The Diagnosis and Treatment of Osteochondritis Dissecans
 AAOS Guideline of The Diagnosis and Treatment of Osteochondritis Dissecans Summary of Recommendations The following is a summary of the recommendations in the AAOS clinical practice guideline, The Diagnosis
AAOS Guideline of The Diagnosis and Treatment of Osteochondritis Dissecans Summary of Recommendations The following is a summary of the recommendations in the AAOS clinical practice guideline, The Diagnosis
Arthroscopy of the Hand and Wrist
 Arthroscopy of the Hand and Wrist Arthroscopy is a minimally invasive procedure whereby a small camera is inserted through small incisions of a few millimeters each around a joint to view the joint directly.
Arthroscopy of the Hand and Wrist Arthroscopy is a minimally invasive procedure whereby a small camera is inserted through small incisions of a few millimeters each around a joint to view the joint directly.
Anterior Cruciate Ligament Reconstruction
 1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
Model Coverage Determination: Total Joint Arthroplasty
 Model Coverage Determination: Total Joint Arthroplasty LCD ID Number LCD Title Major Joint Replacement (Hip and Knee) Indications and Limitations of Coverage and/or Medical Necessity Joint replacement
Model Coverage Determination: Total Joint Arthroplasty LCD ID Number LCD Title Major Joint Replacement (Hip and Knee) Indications and Limitations of Coverage and/or Medical Necessity Joint replacement
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Corporate Medical Policy Continuous Passive Motion in the Home Setting
 Corporate Medical Policy Continuous Passive Motion in the Home Setting File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_passive_motion_in_the_home_setting 9/1993 6/2016
Corporate Medical Policy Continuous Passive Motion in the Home Setting File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_passive_motion_in_the_home_setting 9/1993 6/2016
Evaluating Knee Pain
 Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Rehabilitation of Revision ACL Reconstruction
 Chapter 1 Rehabilitation of Revision ACL Reconstruction Michael B. Ellman, MD Rush University Medical Center, Chicago, Illinois Michael D. Rosenthal, PT, DSc, SCS, ECS, ATC, CSCS Naval Medical Center,
Chapter 1 Rehabilitation of Revision ACL Reconstruction Michael B. Ellman, MD Rush University Medical Center, Chicago, Illinois Michael D. Rosenthal, PT, DSc, SCS, ECS, ATC, CSCS Naval Medical Center,
Name of Policy: Arthroscopic Debridement and Lavage as Treatment for Osteoarthritis of the Knee
 Name of Policy: Arthroscopic Debridement and Lavage as Treatment for Osteoarthritis of the Knee Policy #: 391 Latest Review Date: December 2014 Category: Surgery Policy Grade: B Background/Definitions:
Name of Policy: Arthroscopic Debridement and Lavage as Treatment for Osteoarthritis of the Knee Policy #: 391 Latest Review Date: December 2014 Category: Surgery Policy Grade: B Background/Definitions:
Acceptable CPT Codes for the ABOS Sports Subspecialty Case List
 20520 Removal of foreign body in muscle or tendon sheath; simple 20525 Removal of foreign body in muscle or tendon sheath; deep or complicated 20670 Removal of implant; superficial, (eg, buried wire, pin
20520 Removal of foreign body in muscle or tendon sheath; simple 20525 Removal of foreign body in muscle or tendon sheath; deep or complicated 20670 Removal of implant; superficial, (eg, buried wire, pin
Synopsis of Causation
 Ministry of Defence Synopsis of Causation Internal Derangement of the Knee Author: Dr Tony Fisher, Medical Author, Medical Text, Edinburgh Validator: Mr Malcolm Glasgow, Norfolk and Norwich University
Ministry of Defence Synopsis of Causation Internal Derangement of the Knee Author: Dr Tony Fisher, Medical Author, Medical Text, Edinburgh Validator: Mr Malcolm Glasgow, Norfolk and Norwich University
A Simplified Approach to Common Shoulder Problems
 A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
Treatment Guide Knee Pain
 Treatment Guide Knee Pain Choosing Your Care Approximately 18 million patients visit a doctor or a hospital because of knee pain each year. Fortunately, there are many ways to successfully treat knee pain
Treatment Guide Knee Pain Choosing Your Care Approximately 18 million patients visit a doctor or a hospital because of knee pain each year. Fortunately, there are many ways to successfully treat knee pain
Musculoskeletal: Acute Lower Back Pain
 Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
Is Your Horse Off Behind?? Hindlimb Facts. Common Hindlimb Lameness. Diagnostic Techniques. Gait Analysis 3/21/2012
 Is Your Horse Off Behind?? Nathaniel A. White II DVM MS DACVS Jean Ellen Shehan Professor and Director Common Hindlimb Lameness Sacroiliac joint pain Hip Lameness Stifle Lameness Stress Fractures Hock
Is Your Horse Off Behind?? Nathaniel A. White II DVM MS DACVS Jean Ellen Shehan Professor and Director Common Hindlimb Lameness Sacroiliac joint pain Hip Lameness Stifle Lameness Stress Fractures Hock
Sports Injuries of the Foot and Ankle. Dr. Travis Kieckbusch August 7, 2014
 Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Systemic condition affecting synovial tissue Hypertrohied synovium destroys. Synovectomy. Tenosynovectomy Tendon Surgery Arthroplasty Arthrodesis
 Surgical Options for Rheumatoid Arthritis of the Wrist Raj Bhatia Consultant Hand & Orthopaedic Surgeon Bristol Royal Infirmary & Avon Orthopaedic Centre Rheumatoid Arthritis Systemic condition affecting
Surgical Options for Rheumatoid Arthritis of the Wrist Raj Bhatia Consultant Hand & Orthopaedic Surgeon Bristol Royal Infirmary & Avon Orthopaedic Centre Rheumatoid Arthritis Systemic condition affecting
MEDICAL POLICY No. 91104-R7 DETOXIFICATION I. POLICY/CRITERIA
 DETOXIFICATION MEDICAL POLICY Effective Date: January 7, 2013 Review Dates: 1/93, 2/97, 4/99, 2/01, 12/01, 2/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14 Date
DETOXIFICATION MEDICAL POLICY Effective Date: January 7, 2013 Review Dates: 1/93, 2/97, 4/99, 2/01, 12/01, 2/02, 2/03, 1/04, 1/05, 12/05, 12/06, 12/07, 12/08, 12/09, 12/10, 12/11, 12/12, 12/13, 11/14 Date
The Knee Internal derangement of the knee (IDK) The Knee. The Knee Anatomy of the anteromedial aspect. The Knee
 Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
CHART 4 - NEW FEE CODES - EFFECTIVE OCTOBER 1, 2010
 Bulletin 4520 Implementation of the 2008 Physician Services Agreement Changes Effective, Chart 4 REVISED CHART 4 - NEW FEE CODES - EFFECTIVE OCTOBER A190 Special psychiatric consultation A $285.00 A231
Bulletin 4520 Implementation of the 2008 Physician Services Agreement Changes Effective, Chart 4 REVISED CHART 4 - NEW FEE CODES - EFFECTIVE OCTOBER A190 Special psychiatric consultation A $285.00 A231
Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria
 Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria MAY 2013 When paying the reasonable costs of medical services, the TAC and WorkSafe pay in
Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria MAY 2013 When paying the reasonable costs of medical services, the TAC and WorkSafe pay in
MANAGEMENT OF ANTERIOR CRUCIATE LIGAMENT INJURIES SUMMARY. This Guideline has been endorsed by the following organizations:
 MANAGEMENT OF ANTERIOR CRUCIATE LIGAMENT INJURIES SUMMARY This Guideline has been endorsed by the following organizations: Disclaimer This Clinical Practice Guideline was developed by an AAOS multidisciplinary
MANAGEMENT OF ANTERIOR CRUCIATE LIGAMENT INJURIES SUMMARY This Guideline has been endorsed by the following organizations: Disclaimer This Clinical Practice Guideline was developed by an AAOS multidisciplinary
Notice of Independent Review Decision DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE:
 Notice of Independent Review Decision DATE OF REVIEW: 12/10/10 IRO CASE #: NAME: DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE: Determine the appropriateness of the previously denied request for right
Notice of Independent Review Decision DATE OF REVIEW: 12/10/10 IRO CASE #: NAME: DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE: Determine the appropriateness of the previously denied request for right
Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013
 Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013 Jeffrey R. Baker, DPM, FACFAS Weil Foot and Ankle Institute Des Plaines, IL Ankle Injury/Sprains
Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013 Jeffrey R. Baker, DPM, FACFAS Weil Foot and Ankle Institute Des Plaines, IL Ankle Injury/Sprains
ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015
 Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1
 Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
I. Ankle and Foot Orthotics: (AFO) are considered medical necessary when One or more of the following are met:
 Moda Health Plan, Inc. Medical Necessity Criteria Subject: Origination Date: 05/2015 Revision Date(s): Developed By: Medical Criteria Committee Effective 07/01/2015 Ankle-Foot Orthotics (AFO) Page 1 of
Moda Health Plan, Inc. Medical Necessity Criteria Subject: Origination Date: 05/2015 Revision Date(s): Developed By: Medical Criteria Committee Effective 07/01/2015 Ankle-Foot Orthotics (AFO) Page 1 of
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA
 Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Rehabilitation Guidelines for Autologous Chondrocyte Implantation. Ashley Conlin, PT, DPT, SCS, CSCS
 Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY
 George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
Good morning, everyone! I m Sue Banta, a coding consultant for Amphion Medical. ambulatory knee and shoulder procedures.
 Copyright 2013 by the American Health Information Management Association. All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted in any form or
Copyright 2013 by the American Health Information Management Association. All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted in any form or
How To Know If You Can Recover From A Knee Injury
 David R. Cooper, M.D. www.thekneecenter.com Wilkes-Barre, Pa. Knee Joint- Anatomy Is not a pure hinge Ligaments are balanced Mechanism of injury determines what structures get damaged Medial meniscus tears
David R. Cooper, M.D. www.thekneecenter.com Wilkes-Barre, Pa. Knee Joint- Anatomy Is not a pure hinge Ligaments are balanced Mechanism of injury determines what structures get damaged Medial meniscus tears
Scope it Out! Arthroscopic Procedures. Disclaimer
 Scope it Out! Arthroscopic Procedures Julie A. Leu, eu,cpc, C,CPCO, CO,C CPMA, CPC-I 2009-2011 NAB Member, Region 7 Disclaimer Every reasonable effort has been made to ensure that the educational material
Scope it Out! Arthroscopic Procedures Julie A. Leu, eu,cpc, C,CPCO, CO,C CPMA, CPC-I 2009-2011 NAB Member, Region 7 Disclaimer Every reasonable effort has been made to ensure that the educational material
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Structure & Function of the Knee. One of the most complex simple structures in the human body. The middle child of the lower extremity.
 Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Acute Ankle Injuries, Part 1: Office Evaluation and Management
 t June 08, 2009 Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the injury, and
t June 08, 2009 Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the injury, and
Anterior Knee Pain: Patellofemoral Pain a review
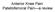 Anterior Knee Pain: Patellofemoral Pain a review Overview Anatomy review A brief understanding of biomechanics The differential for anterior knee pain Pertinent history and physical Imaging which one and
Anterior Knee Pain: Patellofemoral Pain a review Overview Anatomy review A brief understanding of biomechanics The differential for anterior knee pain Pertinent history and physical Imaging which one and
Why knees hurt, and what you can do about it.
 Why knees hurt, and what you can do about it. Table of Contents How Knees Work Common Conditions and Treatment Options Surgical Procedures START Start the Journey to Pain-Free Knees START What Sets Us
Why knees hurt, and what you can do about it. Table of Contents How Knees Work Common Conditions and Treatment Options Surgical Procedures START Start the Journey to Pain-Free Knees START What Sets Us
When is Hip Arthroscopy recommended?
 HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
Treatment Guide Understanding Elbow Pain. Using this Guide. Choosing Your Care. Table of Contents:
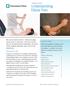 Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Fracture Care Coding September 28, 2011
 Fracture Care Coding September 28, 2011 Julie Edens Leu, CPC, CPCO, CPMA, CPC-I 1 Disclaimer Every reasonable effort has been made to ensure that the educational material provided today is accurate and
Fracture Care Coding September 28, 2011 Julie Edens Leu, CPC, CPCO, CPMA, CPC-I 1 Disclaimer Every reasonable effort has been made to ensure that the educational material provided today is accurate and
Procedure. 2 29827 $ 3,560 $ 1,476 Arthroscopy, shoulder, surgical; with rotator cuff repair 5.5% 241.1%
 Exhibit 1 Top 50% of Payments for Surgical s (Physician costs) On average, Workers' payments for Surgical s in are 256% the average allowed claim costs for Healthcare in. $6,000 $5,000 $4,000 Allowed Claim
Exhibit 1 Top 50% of Payments for Surgical s (Physician costs) On average, Workers' payments for Surgical s in are 256% the average allowed claim costs for Healthcare in. $6,000 $5,000 $4,000 Allowed Claim
The Petrylaw Lawsuits Settlements and Injury Settlement Report
 The Petrylaw Lawsuits Settlements and Injury Settlement Report KNEE INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Knee Injury Cases The Petrylaw Lawsuits Settlements and Injury
The Petrylaw Lawsuits Settlements and Injury Settlement Report KNEE INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Knee Injury Cases The Petrylaw Lawsuits Settlements and Injury
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
The Ankle Sprain That Won t Get Better. By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the
 The Ankle Sprain That Won t Get Better By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the orthopaedist alike can expect to see more than his or her
The Ankle Sprain That Won t Get Better By: George E. Quill, Jr., M.D. With springtime in Louisville upon us, the primary care physician and the orthopaedist alike can expect to see more than his or her
Ankle Sports injuries. Ben Yates
 Ankle Sports injuries Ben Yates Common Extra-articular Conditions Lateral collateral ligament sprains (grades 1,2,3) Functional instability Mechanical instability Achilles tendonopathy (Achillodynia) superficial
Ankle Sports injuries Ben Yates Common Extra-articular Conditions Lateral collateral ligament sprains (grades 1,2,3) Functional instability Mechanical instability Achilles tendonopathy (Achillodynia) superficial
Knee injuries are a common concern resulting in
 F A N T A S T I C F I N D I N G S The Case for Utilizing Prolotherapy as First-Line Treatment for Meniscal Pathology: A Retrospective Study Shows Prolotherapy is Effective in the Treatment of MRI-Documented
F A N T A S T I C F I N D I N G S The Case for Utilizing Prolotherapy as First-Line Treatment for Meniscal Pathology: A Retrospective Study Shows Prolotherapy is Effective in the Treatment of MRI-Documented
LATERAL PAIN SYNDROMES OF THE FOOT AND ANKLE
 C H A P T E R 3 LATERAL PAIN SYNDROMES OF THE FOOT AND ANKLE William D. Fishco, DPM The majority of patient encounters with the podiatrist are secondary to pain in the foot and/or ankle. If we draw an
C H A P T E R 3 LATERAL PAIN SYNDROMES OF THE FOOT AND ANKLE William D. Fishco, DPM The majority of patient encounters with the podiatrist are secondary to pain in the foot and/or ankle. If we draw an
Local Coverage Determination (LCD): Non-Vascular Extremity Ultrasound (L34716)
 Local Coverage Determination (LCD): Non-Vascular Extremity Ultrasound (L34716) Contractor Information Contractor Name Novitas Solutions, Inc. LCD Information Document Information LCD ID L34716 LCD Title
Local Coverage Determination (LCD): Non-Vascular Extremity Ultrasound (L34716) Contractor Information Contractor Name Novitas Solutions, Inc. LCD Information Document Information LCD ID L34716 LCD Title
Hand and Upper Extremity Injuries in Outdoor Activities. John A. Schneider, M.D.
 Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Patellofemoral Joint: Superior Glide of the Patella
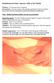 Patellofemoral Joint: Superior Glide of the Patella Purpose: To increase knee extension. Precautions: Do not compress the patella against the femoral condyles. Do not force the knee into hyperextension
Patellofemoral Joint: Superior Glide of the Patella Purpose: To increase knee extension. Precautions: Do not compress the patella against the femoral condyles. Do not force the knee into hyperextension
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
Rheumatoid Arthritis. Nicole Klett,, M.D.
 Rheumatoid Arthritis Nicole Klett,, M.D. Rheumatoid Arthritis Systemic Chronic Inflammatory Primarily targets the synovium of diarthrodial joints Etiology likely combination genetic and environmental Diarthrodial
Rheumatoid Arthritis Nicole Klett,, M.D. Rheumatoid Arthritis Systemic Chronic Inflammatory Primarily targets the synovium of diarthrodial joints Etiology likely combination genetic and environmental Diarthrodial
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Semmelweis University Department of Traumatology Dr. Gál Tamás
 Semmelweis University Department of Traumatology Dr. Gál Tamás Anatomy Ankle injuries DIRECT INDIRECT Vertical Compression (Tibia plafond Pilon) AO 43-A,B,C Suppination (adduction + inversion) AO 44-A
Semmelweis University Department of Traumatology Dr. Gál Tamás Anatomy Ankle injuries DIRECT INDIRECT Vertical Compression (Tibia plafond Pilon) AO 43-A,B,C Suppination (adduction + inversion) AO 44-A
MEDICAL POLICY No. 91607-R1 MENTAL HEALTH RESIDENTIAL TREATMENT: CHILD AND ADOLESCENT
 Summary of Changes MEDICAL POLICY MENTAL HEALTH RESIDENTIAL TREATMENT: CHILD ADOLESCENT Effective Date: June 4, 2015 Review Dates: 5/14, 5/15 Date Of Origin: May 14, 2014 Status: Current Clarifications:
Summary of Changes MEDICAL POLICY MENTAL HEALTH RESIDENTIAL TREATMENT: CHILD ADOLESCENT Effective Date: June 4, 2015 Review Dates: 5/14, 5/15 Date Of Origin: May 14, 2014 Status: Current Clarifications:
ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Introduction
 ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or
ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
5/7/2009 SHOULDER) CONDITIONS OF THE SHOULDER NOW IT TIME TO TEST YOU ICD-9 SKILLS: PLEASE APPEND THE APPROPRIATE DIAGNOSIS CODE FOR EACH:
 SHOULDER CONDITIONS OF THE SHOULDER AND THEIR TREATMENT Presented by Kevin Solinsky, CPC,CPC-I,CEDC, CEMC The is a major joint and plays a large part in daily life, particularly for athletes and those
SHOULDER CONDITIONS OF THE SHOULDER AND THEIR TREATMENT Presented by Kevin Solinsky, CPC,CPC-I,CEDC, CEMC The is a major joint and plays a large part in daily life, particularly for athletes and those
Standard of Care: Tibial Plateau Fracture
 Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: ICD-9: 823.00 - fracture of proximal tibia Tibial plateau fractures can occur as a result of high-energy trauma or in low-energy
Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: ICD-9: 823.00 - fracture of proximal tibia Tibial plateau fractures can occur as a result of high-energy trauma or in low-energy
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
At the completion of the rotation, the resident will have acquired the following competencies and will function effectively as:
 Goals and Objectives Orthopedic Surgery Residency Program - Memorial University Plastic Surgery DEFINITION Traumatic or acquired problems of the musculoskeletal system frequently have a soft tissue component
Goals and Objectives Orthopedic Surgery Residency Program - Memorial University Plastic Surgery DEFINITION Traumatic or acquired problems of the musculoskeletal system frequently have a soft tissue component
5/24/2010. The 10 Ways to Improve Coding
 10 WAYS TO IMPROVE an ASCs ORTHO & SPINE CODING Orthopedic, Spine & PM ASC Conference asc Communications/the ASC Assoc. Conference Speaker: Stephanie Ellis, R.N., CPC Ellis Medical Consulting, Inc. (615)
10 WAYS TO IMPROVE an ASCs ORTHO & SPINE CODING Orthopedic, Spine & PM ASC Conference asc Communications/the ASC Assoc. Conference Speaker: Stephanie Ellis, R.N., CPC Ellis Medical Consulting, Inc. (615)
MEDICAL POLICY No. 91608-R1 MENTAL HEALTH RESIDENTIAL TREATMENT: ADULT
 MENTAL HEALTH RESIDENTIAL TREATMENT: ADULT Effective Date: June 4, 2015 Review Dates: 5/14, 5/15 Date Of Origin: May 12, 2014 Status: Current Summary of Changes Clarifications: Pg 4, Description, updated
MENTAL HEALTH RESIDENTIAL TREATMENT: ADULT Effective Date: June 4, 2015 Review Dates: 5/14, 5/15 Date Of Origin: May 12, 2014 Status: Current Summary of Changes Clarifications: Pg 4, Description, updated
Fast Forward. ICD-9-CM Code ICD-10-CM Code(s) ICD-9-CM Code ICD-10-CM Code(s) Codes. (cont.) 719.41 Pain in joint, shoulder region.
 Top 50 Orthopaedics IC-9-CM Code Code(s) IC-9-CM Code Code(s) 724.2 Lumbago M54.5 Low back pain (Lumbago, NO) M54.40 Lumbago with sciatica, unspecified site M54.41 Lumbago with sciatica, right side M54.42
Top 50 Orthopaedics IC-9-CM Code Code(s) IC-9-CM Code Code(s) 724.2 Lumbago M54.5 Low back pain (Lumbago, NO) M54.40 Lumbago with sciatica, unspecified site M54.41 Lumbago with sciatica, right side M54.42
NIA Magellan 1 Hip, Knee & Spine Surgery Frequently Asked Questions (FAQs) for Florida Blue Medicare Advantage BlueMedicare SM HMO and PPO Plans
 NIA Magellan 1 Hip, Knee & Spine Surgery Frequently Asked Questions (FAQs) for Florida Blue Medicare Advantage BlueMedicare SM HMO and PPO Plans Question GENERAL Why is Florida Blue implementing a Musculoskeletal
NIA Magellan 1 Hip, Knee & Spine Surgery Frequently Asked Questions (FAQs) for Florida Blue Medicare Advantage BlueMedicare SM HMO and PPO Plans Question GENERAL Why is Florida Blue implementing a Musculoskeletal
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
RADIOGRAPHIC EVALUATION
 Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
Clients w/ Orthopedic, Injury and Rehabilitation Concerns. Chapter 21
 Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
US Reimbursement Guide
 US Reimbursement Guide The information with this notice is general reimbursement information only. It is not legal advice, nor is it about how to code, complete or submit any particular claim for payment.
US Reimbursement Guide The information with this notice is general reimbursement information only. It is not legal advice, nor is it about how to code, complete or submit any particular claim for payment.
ICD-10 and Sports Medicine
 ICD-10 and Sports Medicine Steven M. Verno, CMBS, CEMCS, CMSCS, CPM-MCS Page 1 of 15 ICD-10 and Sports Medicine Copyright 2011 Steven M. Verno, CMBS, CEMCS, CMSCS, CPm-MCS November 1, 2011 Note: and ICD-10
ICD-10 and Sports Medicine Steven M. Verno, CMBS, CEMCS, CMSCS, CPM-MCS Page 1 of 15 ICD-10 and Sports Medicine Copyright 2011 Steven M. Verno, CMBS, CEMCS, CMSCS, CPm-MCS November 1, 2011 Note: and ICD-10
DISEASES OF THE MUSKULOSKELETAL SYSTEM AND CONNECTIVE TISSUE
 DISEASES OF THE MUSKULOSKELETAL SYSTEM AND CONNECTIVE TISSUE ARTHROPATHIES AND RELATED DISORDERS (710 719.9) 710 DIFFUSE DISEASES OF CONNECTIVE TISSUE 710.0 SYSTEMIC LUPUS ERYTHEMATOSUS 710.1 SYSTEMIC
DISEASES OF THE MUSKULOSKELETAL SYSTEM AND CONNECTIVE TISSUE ARTHROPATHIES AND RELATED DISORDERS (710 719.9) 710 DIFFUSE DISEASES OF CONNECTIVE TISSUE 710.0 SYSTEMIC LUPUS ERYTHEMATOSUS 710.1 SYSTEMIC
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
The Knee: Problems and Solutions
 The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
MEDICAL POLICY No. 91332-R3 NON-ACUTE INPATIENT SERVICES
 NON-ACUTE INPATIENT SERVICES Effective Date: November 16, 2007 Review Dates: 1/93, 12/99, 12/01, 12/02, 11/03, 11/04, 10/05, 10/06, 10/07, 10/08, 10/09, 10/10, 10/11, 10/12, 10/13, 11/14 Date of Origin:
NON-ACUTE INPATIENT SERVICES Effective Date: November 16, 2007 Review Dates: 1/93, 12/99, 12/01, 12/02, 11/03, 11/04, 10/05, 10/06, 10/07, 10/08, 10/09, 10/10, 10/11, 10/12, 10/13, 11/14 Date of Origin:
Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the
 Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the JF Rick Hammesfahr, MD Editor s Note: Part Three consists of ankle injury evaluation and taping. Part Two
Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the JF Rick Hammesfahr, MD Editor s Note: Part Three consists of ankle injury evaluation and taping. Part Two
Posttraumatic medial ankle instability
 Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Standard of Care: Meniscal Tears
 Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: (diagnosis specific, impairment/ dysfunction specific) The menisci are semi lunar shaped regions of cartilage on the medial
Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: (diagnosis specific, impairment/ dysfunction specific) The menisci are semi lunar shaped regions of cartilage on the medial
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL
 REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL Michael M. Reinold, PT, ATC Kevin E. Wilk, PT Jeffrey R. Dugas, MD E. Lyle Cain, MD Scott D. Gillogly, MD The following has
REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL Michael M. Reinold, PT, ATC Kevin E. Wilk, PT Jeffrey R. Dugas, MD E. Lyle Cain, MD Scott D. Gillogly, MD The following has
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
A STUDY OF ARTHROSCOPIC MANAGEMENT OF MENISCAL INJURIES G. Ramesh 1, J. Ashok Vardhan Reddy 2, Manne Vishnu Vardhan 3
 A STUDY OF ARTHROSCOPIC MANAGEMENT OF MENISCAL INJURIES G. Ramesh 1, J. Ashok Vardhan Reddy 2, Manne Vishnu Vardhan 3 HOW TO CITE THIS ARTICLE: G. Ramesh, J. Ashok Vardhan Reddy, Manne Vishnu Vardhan.
A STUDY OF ARTHROSCOPIC MANAGEMENT OF MENISCAL INJURIES G. Ramesh 1, J. Ashok Vardhan Reddy 2, Manne Vishnu Vardhan 3 HOW TO CITE THIS ARTICLE: G. Ramesh, J. Ashok Vardhan Reddy, Manne Vishnu Vardhan.
