JAMA. 1998;280:
|
|
|
- Dennis Ferguson
- 8 years ago
- Views:
Transcription
1 Original Contributions Biochemical Outcome After Radical Prostatectomy, Radiation Therapy, or Interstitial for Clinically Localized Prostate Cancer Anthony V. D Amico, MD, PhD; Richard Whittington, MD; S. Bruce Malkowicz, MD; Delray Schultz, PhD; Kenneth Blank, MD; Gregory A. Broderick, MD; John E. Tomaszewski, MD; Andrew A. Renshaw, MD; Irving Kaplan, MD; Clair J. Beard, MD; Alan Wein, MD Context. Interstitial radiation (implant) therapy is used to treat clinically localized adenocarcinoma of the prostate, but how it compares with other treatments is not known. Objective. To estimate control of prostate-specific antigen (PSA) after radical prostatectomy (RP), external beam radiation (RT), or implant with or without neoadjuvant androgen deprivation therapy in patients with clinically localized prostate cancer. Design. Retrospective cohort study of outcome data compared using Cox regression multivariable analyses. Setting and Patients. A total of 87 men treated between January 989 and October 997 with an RP (n = 888) or implant with or without neoadjuvant androgen deprivation therapy (n = 8) at the Hospital of the University of Pennsylvania, Philadelphia, or RT (n = 766) at the Joint Center for, Boston, Mass, were enrolled. Main Outcome Measure. Actuarial freedom from PSA failure (defined as PSA outcome). Results. The relative risk (RR) of PSA failure in low-risk patients (stage Tc, Ta and PSA level ng/ml and Gleason score 6) treated using RT, implant plus androgen deprivation therapy, or implant therapy was. (95% confidence interval [CI],.5-.7),.5 (95% CI,.-.9), and. (95% CI,.-.6), respectively, compared with those patients treated with RP. The RRs of PSA failure in the intermediate-risk patients (stage Tb or Gleason score of 7 or PSA level and ng/ml) and high-risk patients (stage Tc or PSA level ng/ml or Gleason score 8) treated with implant compared with RP were. (95% CI,.5-6.) and. (95% CI,.8-5.), respectively. The addition of androgen deprivation to implant therapy did not improve PSA outcome in high-risk patients but resulted in a PSA outcome that was not statistically different compared with the results obtained using RP or RT in intermediate-risk patients. These results were unchanged when patients were stratified using the traditional rankings of biopsy Gleason scores of through vs 5 through 6 vs 7 vs 8 through. Conclusions. Low-risk patients had estimates of 5-year PSA outcome after treatment with RP, RT, or implant with or without neoadjuvant androgen deprivation that were not statistically different, whereas intermediate- and high-risk patients treated with RP or RT did better then those treated by implant. Prospective randomized trials are needed to verify these findings. JAMA. 998;8: From the Joint Center for, Harvard Medical School, Boston, Mass (Drs D Amico, Kaplan, and Beard); Departments of Radiation Oncology (Drs Whittington and Blank), Urology (Drs Malkowicz, Broderick, and Wein), and Pathology (Dr Tomaszewski), Hospital of the University of Pennsylvania, Philadelphia; Department of Mathematics, University of Millersville (Dr Schultz), Millersville, Pa; and Department of Pathology, Brigham and Women s Hospital (Dr Renshaw), Boston, Mass. Reprints: Anthony V. D Amico, MD, PhD, Joint Center for, Brookline Ave, Fifth Floor, Boston, MA 5 ( ADAMICO@jcrt.harvard.edu). THERE ARE no completed prospective randomized trials, to our knowledge, that compare definitive local treatment options for clinically localized adenocarcinoma of the prostate. Retrospective comparisons, stratified by the known prognostic factors and using actuarial analyses have been published comparing radical prostatectomy (RP) with external beam radiation therapy (RT). However, a direct comparison of the results of ultrasound-guided interstitial prostate radiation (implant) therapy withrporrtstratifiedbythepretreatment prognostic factors has not been previously reported. See also pp 975 and 8. The utility of the pretreatment prostate-specific antigen (PSA), biopsy Gleason score, and American Joint Commission on Cancer Staging (AJCC) T stage 5 in predicting postradiation 6- and postoperative -6 PSA outcome has been previously published by several investigators. The purpose of this study is to provide PSA outcome data stratified by the pretreatment PSA, biopsy Gleason score, and AJCC T stage in men treated with RP,RT,orimplanttherapywithorwithout the addition of neoadjuvant androgen deprivation for clinically localized prostate cancer. METHODS Patient Population Between January 989 and October 997, 87 men with clinically localized prostate cancer underwent definitive local therapy. Local therapy received was RP (n = 888) or implant with or without neoadjuvant androgen deprivation therapy (n = 8) at the Hospital of the JAMA, September 6, 998 Vol 8, No. PSA Control After Local Therapy for Prostate Cancer D Amico et al 969 Downloaded From: on 6/7/ 998 American Medical Association. All rights reserved.
2 University of Pennsylvania (HUP), Philadelphia, or conformal RT (n = 766) at the Joint Center for, Boston, Mass. Staging Inallcases, stagingevaluationincluded a history and physical examination including a digital rectal examination, serum PSA, computed tomographic scan of the pelvis or an endorectal and pelvic coil magnetic resonance imaging scan of the prostateandpelvis, bonescan, andatransrectal ultrasound-guided needle biopsy of the prostate with Gleason score histologic grading. A sextant biopsy was performed using a 8-gauge Tru-Cut needle (Travenol Laboratories, Deerfield, Ill) via a transrectal approach. The clinical stage was obtained from the digital rectal examination findings using the 99 AJCCstagingsystem. 5 Radiologicandbiopsy information was not used to determine clinical stage. The PSA level was obtained on an ambulatory basis prior to radiologic studies and the biopsy procedure.allpsameasurements weremade using the Hybritech (San Diego, Calif), Tosoh (Foster City, Calif), or Abbott assays (Chicago, Ill). Treatment Arefereegenitourinarypathologistreviewed the diagnostic biopsy specimens for all patients undergoing surgery or implant at the HUP (J.E.T.) and RT at the Joint Center for (A.A.R.). Surgical treatment consisted of a radical retropubic prostatectomy and bilateral pelvic lymph node sampling. All patients managed with definitive RT were treated using at least -MV photons and a conformal shaped -field technique. Those patients with AJCC clinical stage Tc, Ta disease who also had a PSA level of ng/ml or less and biopsy Gleason score of to 6 were treated to the prostate only with a.5- cm margin. The median prescription dose was 66 Gy (66-7 Gy) and was delivered using -Gy fractions. All other patients with clinically localized disease received a median prescription dose of 5 Gy (5-5. Gy) in.8-gy fractions to the prostate and seminal vesicles plus a.5-cm margin. This was followed by treatment to the prostate alone using a shrinking field technique with a.5-cm margin to a median prescription dose of Gy (8- Gy) in.8- to.-gy fractions. A 95% normalization was used. therapy was performed using palladium ( Pd) seeds, a perineal template-guided, peripheral-loading technique, and a Bruel & Kjaer 855 transrectal ultrasound unit (Naerum, Denmark). The minimum peripheral dose to the prostatic capsule was 5 Gy. A transrectal ultrasound probe was used to image the prostate at 5-mm intervals preoperatively to ascertain the optimal number and locationofseedsneededtodelivertheminimum peripheral dose to the entire prostate gland volume. Individual seed strength ranged from 58 to 6 MBq. The total amount implanted ranged from 6 to 789 MBq. Postimplant dosimetry was performed on all patients based on films obtained at weeks after the implant. For the first patients this consisted of orthogonal films, and for the latter 75 patients, computed tomography was used. Of the 8 patients who received implant therapy, 5 (7%) received neoadjuvant androgen deprivation for a median of months (- months). Hormonal therapy consisted of a luteinizing hormonereleasing hormone agonist that was preceded by the use of a nonsteroidal antiandrogen for 7 to days. Ninety-six (6%) of 5 patients received months of neoadjuvant androgen deprivation therapy. The remaining (.%), 5 (%), (9%), (%), (%), (.%), and (.%) received,, 5, 6, 7, 9, or months of neoadjuvant androgen deprivation therapy, respectively. Follow-up The median follow-up of the 888 surgically managed patients at HUP was 8 months (8- months). The median follow-up for the 766 and 8 radiation-managed patients at the Joint Center for Radiation Therapy and HUP was 8 months (8-75 months) and months (-7 months), respectively. The patients were seen month postoperatively or after the end of radiation therapy, then at -month intervals for years, every 6 months for 5 years, and annually thereafter. At each follow-up a serum PSA was obtained prior to performing the digital rectal examination. All pretreatment PSA values were obtained within month of the date of surgery or start of radiation. No patient was lost to follow-up and all patients were alive at the time of this analysis. Statistical Analyses In order to have the multivariable analysis results of the Cox proportional Table. Clinical Pretreatment Characteristics of the 87 Patients Used in the Time to Prostate-Specific Antigen (PSA) Failure Analyses Are Shown Stratified by Type of Treatment Clinical Factor at the Hospital of the University of Pennsylvania (N = 888) No. (%) of Patients Receiving Treatment* Radiation Therapy at the Joint Center for (N = 766) Interstitial Radiation () (N = 66) Interstitial Radiation () Plus Neoadjuvant Androgen Deprivation Therapy (N = 5) PSA, ng/ml 85 () 77 () 5 (8) 6 (.5).- 5 (57) 9 () 7 (56) (7).- () 98 (6) 6 () (6) 8 (9)* 6 () 8 () (.5) Gleason score - 6 (9) 9 () 6 (9) (7) (58) 76 (9) 7 (7) (7) 7 (5) 9 (5) (5) 9 (9) 8-7 (8) 89 () (5) () American Joint Commission on Cancer Staging T stage Tc 56 (9) (9) 5 () 57 (7.5) Ta 88 () 6 () 5 (5) 68 (5) Tb 9 () (8) 5 (7) 7 (.5) Tc 5 (7) 57 () (7) () *PSA range of. to ng/ml and median of 9.8 ng/ml. PSA range of. to 56 ng/ml and median of.6 ng/ml. PSA range of. to 96.7 ng/ml and median of 6 ng/ml. PSA value of 6.9 ng/ml and median of 6.9 ng/ml. 97 JAMA, September 6, 998 Vol 8, No. PSA Control After Local Therapy for Prostate Cancer D Amico et al 998 American Medical Association. All rights reserved. Downloaded From: on 6/7/
3 Table. Detailed Description of the Clinical Pretreatment Characteristics of the 87 Patients Used in the Time to Prostate-Specific Antigen (PSA) Failure Analyses Stratified by Risk Group and the Type of Treatment No. (%) of Patients Receiving Treatment* Radiation Interstitial Interstitial Radiation () at the Hospital of the Therapy at the Joint Center Radiation Plus Neoadjuvant Androgen Level of Risk University of Pennsylvania for () Deprivation Therapy Low (n = ) (n = 5) (n = ) (n = 9) PSA - 68 (7) (9) () () PSA.- (8) 8 (8) 8 (87) 79 (87) Biopsy Gleason score - (6) 5 () () 7 (8) Biopsy Gleason score (7) 7 (76) 8 (88) 8 (9) American Joint Commission on () 5 () () 9 () Cancer Staging (AJCC) Tc, Ta Intermediate (n = 7) (n = ) (n = 5) (n = 8) PSA - 9 () () (7) () PSA.- () 8 (5) (7) 9 (5) PSA.- 8 (56) 7 (55) (66) 8 (7) Biopsy Gleason score - () () () (8) Biopsy Gleason score (5) 9 (9) 6 () () Biopsy Gleason score 7 9 (6) (8) 6 () (6) AJCC Tc, Ta 79 (7) 8 (59) (8) (8) AJCC Tb 68 (8) 9 () () 7 (8) High (n = 9) (n = 9) (n = 9) (n = ) PSA - 8 () () () () PSA.- 76 () 6 () 5 (6) (57) PSA.- 7 () 7 () 6 () 6 (6) PSA 8 (5) 6 (5) 8 () () Biopsy Gleason score - 9 () 5 (8) () () Biopsy Gleason score (9) (6) (6) (6) Biopsy Gleason score 7 (8) 8 (7) () 6 (6) Biopsy Gleason score 8-7 () 89 (9) (6) () AJCC Tc, Ta 6 (6) 5 () 6 () () AJCC Tb 5 () 7 (5) () () AJCC Tc 5 (6) 57 (5) (58) (87) *n indicates sample sizes stratified by risk and treatment. hazards regression model be applicable in the clinical setting for an individual patient, risk groups were defined. These risk groups were established from a review of the literature 6-9 and were based on the known prognostic factors: PSA level, biopsy Gleason score, and 99 AJCC T stage. Patients with AJCC clinical T stage Tc, Ta and PSA level of ng/ml or less and biopsy Gleason score of 6 or less have been identified to be at low risk ( 5% at 5 years) for posttherapy PSA failure. Conversely, patients with AJCC stage Tc disease or a PSA level of more than ng/ml or a biopsy Gleason score of 8 or more have a risk higher than 5% at 5 years of posttherapy PSA failure. The remaining patients with PSA levels higher than and ng/ml or lower, a biopsy Gleason score of 7, or AJCC clinical stage Tb have been found to have an intermediate risk (5%-5% at 5 years of posttherapy PSA failure). Patients with AJCC clinical stage Ta, Tb were not managed using implant therapy because of the significant rate or urinary incontinence noted 7 using this approach in patients with a history of a transurethralresectionoftheprostate. Therefore, patients with AJCC clinical stage Ta, Tb disease managed with RP or RT were excluded from the study to ensure statistically valid comparisons. A Cox regression multivariable analysis was used to compare PSA outcome among the therapies within each risk group. For each analysis the assumptions of the Cox model were tested and satisfied. Coefficients from the Cox regression model were used to calculate the overall relative risk of PSA failure for patients managed with RT or implant with or without neoadjuvant androgen suppression as compared with patients managed with RP. For the purposes of the multivariable analysis, the type of therapy was treated as a categorical variable indicating RP at HUP, RT, implant, or implant plus neoadjuvant androgen deprivation. Radical prostatectomy at HUP was defined as the baseline group for the purposes of the multivariable analyses. Patients were also stratified and analyzed with the traditional rankingsofabiopsygleasonscoreofthrough, 5 through 6, 7, and 8 through. Prostate-specific antigen failure was defined according to the American Society of Therapeutic Radiation and Oncology 996 consensus statement for all study patients. The definition required that a patient have consecutive rising PSA values each obtained at least months apart before PSA failure was scored. The time of PSA failure was defined as the midpoint between the time of the PSA nadir value and the time of the first rising PSA value. Time zero was defined as the date of diagnosis for all study patients. Pairwise comparisons were made using the log-rank test. In the case where a number of comparisons were made, the level of significance in order to be called statistically significant was lowered from the convention of.5 to.5 divided by the number of comparisons following the Bonferonni adjustment. For the purpose of illustration, estimates of PSA outcome were calculated using the Kaplan- Meier actuarial method and graphically displayed. In the low-, intermediate-, and high-risk patient groups the sample size and the number of events in this study was sufficient to detect a %, 7%, and 5% difference in PSA survival, respectively, with 8% power at a.5 level of significance. This was calculated for a baseline PSA survival of 85%, 6%, and % at 5 years in the low-, intermediate-, and high-risk patients, respectively. JAMA, September 6, 998 Vol 8, No. PSA Control After Local Therapy for Prostate Cancer D Amico et al American Medical Association. All rights reserved. Downloaded From: on 6/7/
4 Table. Pairwise P Values Comparing the Proportion of Patients With the Given Pretreatment Clinical Characteristic Shown in Table Across Treatment Modalities* Level of Risk Low Radical prostatectomy (RP) vs external beam radiation therapy (RT) RESULTS Risk Group Analysis The clinical pretreatment characteristics of the 87 patients used in the time to PSA-failure analyses are listed in Table and are stratified by the type of treatment. Table lists the clinical characteristics of the study patients within each risk group. The pairwise P values from the comparative analyses of the proportion of patients having a specific pretreatment clinical characteristic betweenthetreatmentgroupsareshown in Table. After adjustment for the multiple comparisons, no significant differences were noted in low-risk and intermediate-riskpatients. High-riskpatients managed with implant plus neoadjuvant androgen deprivation had an increased proportion of patients with PSA levels lower than ng/ml and decreased proportion of patients with a PSA level of more than ng/ml compared with patients managed with RP (P =.) or RT (P =.). Both of these differences Prostate-Specific Antigen Gleason Score Clinical Stage RP vs interstitial radiation (implant) RP vs implant and neoadjuvant androgen deprivation therapy (H) RT vs implant RT vs implant plus H...99 vs implant plus H Intermediate RP vs RT RP vs implant RP vs implant plus H.6.. RT vs implant RT vs implant plus H...9 vs implant plus H High RP vs RT..9. RP vs implant RP vs implant plus H...5 RT vs implant RT vs implant plus H vs implant plus H *Because of the multiple comparisons, the level of significance as per Bonferonni method was defined as.5 divided by 6 or.8. Table. P Values From the Cox Regression Analyses Evaluating the Ability of a Treatment Modality to Predict the Time to Posttherapy Prostate-Specific Antigen (PSA) Failure Stratified by Risk Group* RR (95% CI) [P Value] Treatment Low Risk Intermediate Risk High Risk External beam radiation therapy at. (.5-.7) [.79].8 (.5-.) [.6].9 (.7-.) [.6] the Joint Center for Interstitial radiation (implant). (.-.6) [.9]. (.5-6.) [.6]. (.8-5.) [.] plus neoadjuvant androgen.5 (.-.9) [.].6 (.8-.) [.]. (.-.) [.] deprivation therapy *Radical prostatectomy at the Hospital of the University of Pennsylvania is the baseline group. RR indicates relative risk; CI, confidence interval. RR is defined as the proportional increase in PSAfailure expected with a given treatment modality when compared with radical prostatectomy. could bias the comparisons of PSA survival in favor of the implant plus neoadjuvant androgen suppression patient cohort. The use of multiple comparisons between treatment modalities (n = 6) required that the level of statistical significance as per Bonferonni adjustment be redefined as lower than.8. Time to PSA Failure Analyses Table lists the P values from the Cox regression multivariable analyses evaluating the effect of the treatment type on time to posttherapy PSA failure stratified by risk group. The relative risks of PSA failure with a 95% confidence interval are also listed. No significant difference(p.5)inoutcomewasnotedinlowriskpatients(tc,taandpsalevel ng/ml and Gleason score 6) across all treatment modalities. The 95% confidence intervals for the relative risk of PSA failure relative to RP for all patients included.. High-risk patients (Tc, PSA level ng/ml, or Gleason score 8), however, treated using a RP or RT did significantly better (P.) then thosemanagedwithimplantwithorwithout neoadjuvant androgen deprivation. Specifically, high-risk patients managed with implant therapy had at least a.- fold increased risk of PSA failure compared with those treated with RP even if neoadjuvant androgen deprivation therapy was used. Intermediate-risk patients (Tb, Gleason score of 7, or PSA level and ng/ml) did significantly worse (P.) if managed by implant alone, but fared equivalently (P =.8) to those patients managed with RP if androgen deprivation was also administered. Intermediate-risk patients managed with implant therapy alone had a.-fold increased risk of PSA failure compared with those patients managed with RP. These results remained unchanged when patients were stratified using the traditional groups of biopsy Gleason score. Specifically, patients with biopsy Gleason score of through 6 had nostatisticaldifferenceintheirestimates of PSA failure-free survival across all the treatment modalities evaluated in this study. However, patients with biopsy Gleason scores of 8 through who were managed with implant with or without neoadjuvant androgen deprivation therapyhadalowerpsafailure-freesurvival that approached statistical significance(p.7)whencomparedwiththose patients managed with RP or RT. Patients with biopsy Gleason scores of 7 did not have statistically different PSA failure-free survival when managed with RP, RT, or implant plus neoadjuvant androgen deprivation therapy (P.59). However these patients did statistically worse (P.) if managed by implant alone. This analysis was repeated using the traditional Gleason score groupings for patients with PSA levels lower than ng/ml and the results remained unchanged. For the purpose of illustration, estimates of PSA outcome with pairwise P values evaluating the comparisons between treatment types were calculated using the Kaplan-Meier actuarial method and are graphically displayed by risk group in Figures through and by biopsy Gleason score in Figures through 7. COMMENT Several studies from the urologic -6 and oncologic 6-,7-9 literature support that the combination of the AJCC clinical T stage, pretreatment PSA, and biopsy Gleason score can predict the pathologic organ confinement rate, biochemical failure rate, and subsequent metastatic rates in patients managed with definitive local therapy for clinically localized prostate 97 JAMA, September 6, 998 Vol 8, No. PSA Control After Local Therapy for Prostate Cancer D Amico et al Downloaded From: on 6/7/ 998 American Medical Association. All rights reserved.
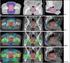
5 and Neoadjuvant Figure. Estimated prostate-specific antigen outcome for low-risk patients stratified by treatment modality. All pairwise P values are more than and Neoadjuvant Figure. Estimated prostate-specific antigen outcome for intermediate-risk patients. Pairwise P values are as follows: radical prostatectomy (RP) vs external beam radiation therapy (RT),.6; RP vs implant plus androgen ablation,.8; RP vs implant,.; RT vs implant plus androgen ablation,.9; RT vs implant,.; and implant plus androgen ablation vs implant, and Neoadjuvant Figure. Estimated prostate-specific antigen outcome for high-risk patients. Pairwise P values are as follows: radical prostatectomy (RP) vs external beam radiation therapy (RT),.5; RP vs implant plus androgen ablation,.; RP vs implant,.5; RT vs implant plus androgen ablation,.7; RT vs implant, less than.; and implant plus androgen ablation vs implant, and Neoadjuvant 8 7 cancer. Therefore, when attempting to compare PSA outcome across different treatment modalities, it is important to control for the values of these prognostic factors. Using the results of the published literature, 6-9 the risk of postradiation and postoperative PSA failure was classified into groups based on the pretreatment prognostic factors. Using a multivariable time-to-psafailure analysis to compare PSA outcome after RP, RT, or implant with or without neoadjuvant androgen deprivation therapy for patients stratified by the defined pretreatment risk groups, several observations were noted. First, the group of patients defined to be at low risk for posttherapy PSA failure were estimated to derive equal benefit from treatment with RP, RT, or implant (Figure ) at 5 years. Moreover, the addition of neoadjuvant androgen deprivation to implant therapy in low-risk patients provided no further benefit in the estimated 5-year PSA outcome. Second, patients at high risk for posttherapy PSA failure did significantly worse with implant therapy despite the addition of neoadjuvant hormonal deprivation when compared with patients treated with RP or RT (Figure ). A statistically significant increase in favorable prognostic factors was present in the high-risk patients managed with implant plus neoadjuvant androgen suppression (ie, PSA level ng/ml) compared with patients managed with RP or 55 5 Figure. Estimated prostate-specific antigen outcome for patients with biopsy Gleason score through. All pairwise P values are more than.6. 6 RT (Tables and ). Despite this potential bias in favor of the patients managed with implant plus neoadjuvant androgen suppression, the PSA outcome of these patients was still inferior to those patients managed with RP or RT. Finally, patients in the intermediate category for posttherapy PSA failure did significantly worse when managed with implant alone as compared with patients managed with RP, RT, or implant plus neoadjuvant androgen deprivation (Figure ). While a statistical difference may exist for intermediate-risk patients managed with implant plus neoadjuvant androgen deprivation therapy vs RP or RT, this study was not adequately powered to detect this difference. Further follow-up is needed to ascertain if these results are maintained. In particular, low-risk patients can sustain late PSA failures (ie, beyond 5 years). Moreover, men with low-grade or lowrisk disease have a relatively low rate of PSA progression requiring numbers of patients much larger than presented in this study in order to prove a statistical difference. Therefore, while small differences may exist, they are unlikely to reach statistical significance. In addition, the intermediate-risk patients managed with a median of months of neoadjuvant androgen deprivation and implant therapy may be experiencing a hormone-induced delay in PSA failure and not a true therapeutic gain. With only 9 patients at risk after years in the implant plus androgen deprivation group compared with 6 and 77 in the RP and RT managed groups, respectively, it is too soon to make conclusions regarding the relative efficacy of these treatments. Therefore, because of the small numbers and relatively short follow-up, particularly in the patients receiving neoadjuvant androgen deprivation, the results must be viewed as preliminary. However, these early data suggest that in high-risk patients, who are in greater need of treatment and who have the most to lose by ineffective therapy, implant therapy with or without the addition of a median of months of neoadjuvant androgen deprivation was less effective than RP or RT at maintaining PSAbased survival. When examining the PSA failure-free survival using the traditional groupings of biopsy Gleason score, the exact results were found as those noted when the data were analyzed according to the risk groups lending further support to this study s findings. Several issues remain that are not addressed by the data in this study. First, the comparison of PSA outcome for expectant management vs treatment is lacking. This comparison would be particularly relevant in the low-risk patients JAMA, September 6, 998 Vol 8, No. PSA Control After Local Therapy for Prostate Cancer D Amico et al 97 Downloaded From: on 6/7/ 998 American Medical Association. All rights reserved.
6 and Neoadjuvant Figure 5. Estimated prostate-specific antigen outcome for patients with biopsy Gleason score 5 through 6. All pairwise P values are more than and Neoadjuvant Figure 6. Estimated prostate-specific antigen outcome for patients with biopsy Gleason score 7. Pairwise P values are as follows: radical prostatectomy (RP) vs external beam radiation therapy (RT),.59; RP vs implant plus androgen ablation,.95; RP vs implant,.; RT vs implant plus androgen ablation,.79; RT vs implant,.; and implant plus androgen ablation vs implant, and Neoadjuvant where 5-year PSA-progression rates numericallyapproximatethe-yearclinicalprogression rates noted from expectant management series.,5 Second, the PSA outcomes of the now widely practiced combination therapies of RT plus implant with or without neoadjuvant androgen deprivation therapy need to be prospectively compared with the PSA outcomes achieved after RP, RT, or implant. These comparisons would be particularly relevant in the high-risk and intermediaterisk groups where implant therapy alone may be insufficient. A final unanswered question remains. That is whether the use of Pd as opposed to the conventional iodine 5 ( 5 I) affected the PSA outcome data reported in this study. The physical characteristics of these radionuclides differ in that the half life and mean photon energy are 6 days, 7 kev and 7 days, kev for 5 I and Pd, respectively. These differences result in an initial dose rate of.77 Gy/h and.97 Gy/h for 5 I and Pd, respectively. It is therefore conceivable that the higher dose rate of palladium could have affected the results. Further investigations of these issues are needed. Nevertheless, considering the widespread increase in the use of implant therapy throughout the United States, these data serve to heighten awareness to the possibility that this form of prostate cancer therapy may only be clinically efficacious in a select subgroup of patients and possibly inadequate in others. While no definitive conclusions can be reached using nonrandomized retrospective data, these analyses can provide the basis on which to design prospective randomized clinical trials that could definitively compare PSA, causespecific, and overall survival outcomes among treatment modalities. References. Kupelian P, Katcher J, Levin HS, Klein EA. Stage T- prostate cancer. Int J Radiat Oncol Biol Phys. 997;7:-5.. D Amico AV, Whittington R, Kaplan I, et al. Equivalent biochemical failure free survival after external beam radiation therapy or radical prostatectomy in patients with a pretreatment prostate specific antigen of - ng/ml. Int J Radiat Oncol Biol Phys. 997;7: Oesterling JE, Jacobsen SJ, Klee GG, et al. Free, complexed and total serum prostate specific antigen. J Urol. 995;5: GleasonDFandtheVeteransAdministrationCooperative Urological Research Group. Histologic grading and staging of prostatic carcinoma. In: Tannenbaum M, ed. Urologic Pathology. Philadelphia, Pa: Lea & Febiger; 977: Figure 7. Estimated prostate-specific antigen outcome for patients with biopsy Gleason score 8 through. Pairwise P values are as follows: radical prostatectomy (RP) vs external beam radiation therapy (RT),.7; RP vs implant plus androgen ablation,.7; RP vs implant,.6; RT vs implant plus androgen ablation,.6; RT vs implant,.5; and implant plus androgen ablation vs implant, Beahrs OH, Henson DE, Hutter RVP. American Joint Committee on Cancer: Manual for Staging Cancer. th ed. Philadelphia, Pa: JB Lippincott; Zagars GK, Pollack A, Kavadi VS, von Eschenbach AC. Prostate specific antigen and radiation therapy for clinically localized prostate cancer. Int J Radiat Oncol Biol Phys. 995;: Pisansky TM, Kahn MJ, Rasp GM, Cha SS, Haddock MG, Bostwick DG. A multiple prognostic index predictive of disease outcome after irradiation for clinically localized prostate cancer. Cancer. 997;79: Lee WR, Hanks GE, Schultheiss TE, Corn BW, Hunt MA. Localized prostate cancer treated by externalbeamradiotherapyalone:serumprostatespecific antigen driven outcome analysis. J Clin Oncol. 995;: Pisansky TM, Cha SS, Earle JD, Durr ED, Kozelsky TF, Wie HS. Prostate specific antigen as a pretherapy prognostic factor in patients treated with radiation therapy for clinically localized prostate cancer. J Clin Oncol. 99;: Zietman AL, Coen JJ, Shipley WU, Willett CG, Efird JT. Radical radiation therapy in the management of prostatic adenocarcinoma. J Urol. 99; 5: Hanks GE, Lee WR, Schultheiss TE. Clinical and biochemical evidence of control of prostate cancer at 5 years after external beam radiation. J Urol. 995;5: Partin AW, Piantadosi S, Sanda MG, Epstein JI, Marshall FF, Mohler JL. Selection of men at high risk for disease recurrence for experimental adjuvanttherapyfollowingradicalprostatectomy.urology. 995;5: Lerner SE, Blute ML, Bergstralh EJ, Bostwick DG, Eickholt JT, Zincke H. Analysis of risk factors for progression in patients with pathologically organ confined prostate cancers after radical retropubic prostatectomy. J Urol. 996;56:7-.. Zietman AL, Edelstein RA, Coen JJ, Babayan RK, Krane RJ. Radical prostatectomy for adenocarcinomaoftheprostate. Urology. 99;: D Amico AV, Whittington R, Malkowicz SB, Schultz D, Tomaszewski JE, Wein A. PSA failure despite pathologically organ confined and margin negative disease. J Clin Oncol. 997;5: D AmicoAV, WhittingtonR, MalkowiczSB, Tomaszewski JE, Schultz D, Wein A. Outcome based stagingforclinicallylocalizedadenocarcinomaofthe prostate. J Urol. 997;58: Ragde H, Blasko JC, Grimm PD, et al. Interstitial iodine 5 radiation without adjuvant therapy in the treatment of clinically localized prostate carcinoma. Cancer. 997;8: Blasko JC, Wallner K, Grimm PD, Ragde H. Prostate specific antigen based disease control following ultrasound guided I 5 implantation for stage T /T prostatic carcinoma. J Urol. 995;5: Wallner K, Roy J, Harrison L. Tumor control andmorbidityfollowingtransperinealiodine5implantation for stage T /T prostatic carcinoma. J Clin Oncol. 996;:9-5.. Cox DR. Regression models and life tables. J R Stat Soc B. 97;: Cox JD for the American Society for Therapeutic Radiology and Oncology Consensus Panel. Consensus statement: guidelines for PSA following radiation therapy. Int J Radiat Oncol Biol Phys. 997; 7:5-.. Neter J, Wasserman W, Kutner M, eds. Simultaneous inferences and other topics in regression analysis-. In: Applied Linear Regression Models. Homewood, Ill: Richard D Irwin Inc; 98:5-5.. Kaplan EL, Meier P. Non-parametric estimation from incomplete observations. J Am Stat Assoc. 958;5: Chodak GW, Thisted RA, Gerber GS, et al. Results of conservative management of clinically localized prostate cancer. N Engl J Med. 99;: Adolfsson J, Steineck G, Hedlund PO. Deferred treatment of clinically localized prostate cancer. Urology. 997;5: JAMA, September 6, 998 Vol 8, No. PSA Control After Local Therapy for Prostate Cancer D Amico et al Downloaded From: on 6/7/ 998 American Medical Association. All rights reserved.
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
NATURAL HISTORY OF CLINICALLY STAGED LOW- AND INTERMEDIATE-RISK PROSTATE CANCER TREATED WITH MONOTHERAPEUTIC PERMANENT INTERSTITIAL BRACHYTHERAPY
 doi:1.116/j.ijrobp.9..1 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No., pp. 349 354, 1 Copyright Ó 1 Elsevier Inc. Printed in the USA. All rights reserved 36-316/1/$ see front matter CLINICAL INVESTIGATION
doi:1.116/j.ijrobp.9..1 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No., pp. 349 354, 1 Copyright Ó 1 Elsevier Inc. Printed in the USA. All rights reserved 36-316/1/$ see front matter CLINICAL INVESTIGATION
PROTON THERAPY FOR PROSTATE CANCER: THE INITIAL LOMA LINDA UNIVERSITY EXPERIENCE
 doi:10.1016/j.ijrobp.2003.10.011 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 2, pp. 348 352, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
doi:10.1016/j.ijrobp.2003.10.011 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 2, pp. 348 352, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
doi:10.1016/j.ijrobp.2006.07.1382 CLINICAL INVESTIGATION
 doi:10.1016/j.ijrobp.2006.07.1382 Int. J. Radiation Oncology Biol. Phys., Vol. 67, No. 1, pp. 57 64, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front matter
doi:10.1016/j.ijrobp.2006.07.1382 Int. J. Radiation Oncology Biol. Phys., Vol. 67, No. 1, pp. 57 64, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front matter
FIVE-YEAR BIOCHEMICAL OUTCOME FOLLOWING PERMANENT INTERSTITIAL BRACHYTHERAPY FOR CLINICAL T1 T3 PROSTATE CANCER
 PII S0360-3016(01)01594-2 Int. J. Radiation Oncology Biol. Phys., Vol. 51, No. 1, pp. 41 48, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/01/$ see front matter
PII S0360-3016(01)01594-2 Int. J. Radiation Oncology Biol. Phys., Vol. 51, No. 1, pp. 41 48, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/01/$ see front matter
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Historical Basis for Concern
 Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
Surrogate End Point for Prostate Cancer Specific Mortality After Radical Prostatectomy or Radiation Therapy
 Surrogate End Point for Prostate Cancer Specific Mortality After Radical Prostatectomy or Radiation Therapy Anthony V. D Amico, Judd W. Moul, Peter R. Carroll, Leon Sun, Deborah Lubeck, Ming-Hui Chen Background:
Surrogate End Point for Prostate Cancer Specific Mortality After Radical Prostatectomy or Radiation Therapy Anthony V. D Amico, Judd W. Moul, Peter R. Carroll, Leon Sun, Deborah Lubeck, Ming-Hui Chen Background:
J Clin Oncol 23:6992-6998. 2005 by American Society of Clinical Oncology INTRODUCTION
 VOLUME 23 NUMBER 28 OCTOBER 1 2005 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Predictors of Prostate Cancer Specific Mortality After Radical Prostatectomy or Radiation Therapy Ping Zhou,
VOLUME 23 NUMBER 28 OCTOBER 1 2005 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Predictors of Prostate Cancer Specific Mortality After Radical Prostatectomy or Radiation Therapy Ping Zhou,
PROSTATE CANCER WITH LARGE GLANDS TREATED WITH 3- DIMENSIONAL COMPUTERIZED TOMOGRAPHY GUIDED PARARECTAL BRACHYTHERAPY: UP TO 8 YEARS OF FOLLOWUP
 0022-5347/03/1694-1331/0 Vol. 169, 1331 1336, April 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000055773.91290.e8 PROSTATE CANCER
0022-5347/03/1694-1331/0 Vol. 169, 1331 1336, April 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000055773.91290.e8 PROSTATE CANCER
the risk of developing skeletal metastases or local recurrence.
 Original Article SERUM PSA AND CLINICAL RECURRENCE AFTER RRP FOR LOCALIZED PROSTATE CANCER HAUKAAS et al. Is preoperative serum prostate-specific antigen level significantly related to clinical recurrence
Original Article SERUM PSA AND CLINICAL RECURRENCE AFTER RRP FOR LOCALIZED PROSTATE CANCER HAUKAAS et al. Is preoperative serum prostate-specific antigen level significantly related to clinical recurrence
Prostate Cancer What Are the Outcomes of Radical Prostatectomy for High-risk Prostate Cancer?
 Prostate Cancer What Are the Outcomes of Radical Prostatectomy for High-risk Prostate Cancer? Stacy Loeb, Edward M. Schaeffer, Bruce J. Trock, Jonathan I. Epstein, Elizabeth B. Humphreys, and Patrick C.
Prostate Cancer What Are the Outcomes of Radical Prostatectomy for High-risk Prostate Cancer? Stacy Loeb, Edward M. Schaeffer, Bruce J. Trock, Jonathan I. Epstein, Elizabeth B. Humphreys, and Patrick C.
PSA After Radiation for Prostate Cancer
 Review Article [1] May 01, 2004 By Deborah A. Kuban, MD [2], Howard D. Thames, PhD [3], and Larry B. Levy, MS [4] The introduction of prostate-specific antigen (PSA) as a reliable tumor marker for prostate
Review Article [1] May 01, 2004 By Deborah A. Kuban, MD [2], Howard D. Thames, PhD [3], and Larry B. Levy, MS [4] The introduction of prostate-specific antigen (PSA) as a reliable tumor marker for prostate
Prostatectomy, pelvic lymphadenect. Med age 63 years Mean followup 53 months No other cancer related therapy before recurrence. Negative.
 Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引
 馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
Adjuvant radiation therapy for recurrent PSA after radical prostatectomy in T1±T2 prostate cancer
 Adjuvant radiation therapy for recurrent after radical prostatectomy in T1±T2 prostate cancer Prostate Cancer and Prostatic Diseases (1998) 1, 321±325 ß 1998 Stockton Press All rights reserved 1365±7852/98
Adjuvant radiation therapy for recurrent after radical prostatectomy in T1±T2 prostate cancer Prostate Cancer and Prostatic Diseases (1998) 1, 321±325 ß 1998 Stockton Press All rights reserved 1365±7852/98
Does my patient need more therapy after prostate cancer surgery?
 Does my patient need more therapy after prostate cancer surgery? Contact the GenomeDx Patient Care Team at: 1.888.792.1601 (toll-free) or e-mail: client.service@genomedx.com Prostate Cancer Classifier
Does my patient need more therapy after prostate cancer surgery? Contact the GenomeDx Patient Care Team at: 1.888.792.1601 (toll-free) or e-mail: client.service@genomedx.com Prostate Cancer Classifier
Implementation Date: April 2015 Clinical Operations
 National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
Brachytherapy for prostate cancer
 Brachytherapy for prostate cancer Findings by SBU Alert Published Jun 7, 2000 Version 1 Brachytherapy is not widely used in Sweden to treat localized prostate cancer. This treatment method has been available
Brachytherapy for prostate cancer Findings by SBU Alert Published Jun 7, 2000 Version 1 Brachytherapy is not widely used in Sweden to treat localized prostate cancer. This treatment method has been available
A new score predicting the survival of patients with spinal cord compression from myeloma
 A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
PROSTATE CANCER. Get the facts, know your options. Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology
 PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
LONG-TERM URINARY TOXICITY AFTER 3-DIMENSIONAL CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER IN PATIENTS WITH PRIOR HISTORY OF TRANSURETHRAL RESECTION
 PII S0360-3016(00)00714-8 Int. J. Radiation Oncology Biol. Phys., Vol. 48, No. 3, pp. 643 647, 2000 Copyright 2000 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/00/$ see front
PII S0360-3016(00)00714-8 Int. J. Radiation Oncology Biol. Phys., Vol. 48, No. 3, pp. 643 647, 2000 Copyright 2000 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/00/$ see front
How To Know If You Should Get A Brachytherapy Or Radioactive Seed Implantation
 MEDICAL POLICY SUBJECT: BRACHYTHERAPY OR PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy
MEDICAL POLICY SUBJECT: BRACHYTHERAPY OR PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy
LATE MORBIDITY PROFILES IN PROSTATE CANCER PATIENTS TREATED TO 79 84 GY BY A SIMPLE FOUR-FIELD COPLANAR BEAM ARRANGEMENT
 PII S0360-3016(02)03822-1 Int. J. Radiation Oncology Biol. Phys., Vol. 55, No. 1, pp. 71 77, 2003 Copyright 2003 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/03/$ see front matter
PII S0360-3016(02)03822-1 Int. J. Radiation Oncology Biol. Phys., Vol. 55, No. 1, pp. 71 77, 2003 Copyright 2003 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/03/$ see front matter
Prostate cancer volume at biopsy vs. findings at Prostatectomy
 Prostate cancer volume at biopsy vs. findings at Prostatectomy May 2005 By Shelly Smits, RHIT, CCS, CTR Ian Thompson, MD Data Source: Cancer registry data of prostate cancer treated with prostatectomy
Prostate cancer volume at biopsy vs. findings at Prostatectomy May 2005 By Shelly Smits, RHIT, CCS, CTR Ian Thompson, MD Data Source: Cancer registry data of prostate cancer treated with prostatectomy
In 2006 approximately 234,000 men were diagnosed with
 Long-Term Survival in Men With High Grade Prostate Cancer: A Comparison Between Conservative Treatment, Radiation Therapy and Radical Prostatectomy A Propensity Scoring Approach Ashutosh Tewari,*, George
Long-Term Survival in Men With High Grade Prostate Cancer: A Comparison Between Conservative Treatment, Radiation Therapy and Radical Prostatectomy A Propensity Scoring Approach Ashutosh Tewari,*, George
Saturation Biopsy for Diagnosis and Staging of Prostate Cancer. Original Policy Date
 MP 7.01.101 Saturation Biopsy for Diagnosis and Staging of Prostate Cancer Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date /12/2013 Return to Medical Policy
MP 7.01.101 Saturation Biopsy for Diagnosis and Staging of Prostate Cancer Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date /12/2013 Return to Medical Policy
Early stage prostate cancer: biochemical recurrence after treatment
 REVIEW ARTICLE Vol. 40 (2): 137-145, March - April, 2014 doi: 10.1590/S1677-5538.IBJU.2014.02.02 Early stage prostate cancer: biochemical recurrence after treatment Danielle A. Zanatta, Reginaldo J. Andrade,
REVIEW ARTICLE Vol. 40 (2): 137-145, March - April, 2014 doi: 10.1590/S1677-5538.IBJU.2014.02.02 Early stage prostate cancer: biochemical recurrence after treatment Danielle A. Zanatta, Reginaldo J. Andrade,
The optimal treatment for clinically localized
 REVIEW COMBINING EXTERNAL BEAM RADIOTHERAPY WITH PROSTATE BRACHYTHERAPY: ISSUES AND RATIONALE CLARISSA FEBLES AND RICHARD K. VALICENTI The optimal treatment for clinically localized prostate cancer remains
REVIEW COMBINING EXTERNAL BEAM RADIOTHERAPY WITH PROSTATE BRACHYTHERAPY: ISSUES AND RATIONALE CLARISSA FEBLES AND RICHARD K. VALICENTI The optimal treatment for clinically localized prostate cancer remains
Beyond the PSA: Genomic Testing in Localized Prostate Cancer
 Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
A new score predicting the survival of patients with spinal cord compression from myeloma
 A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
A918: Prostate: adenocarcinoma
 A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
Neoadjuvant and Adjuvant Hormone Therapy: How and When?
 european urology supplements 7 (2008) 747 751 available at www.sciencedirect.com journal homepage: www.europeanurology.com Neoadjuvant and Adjuvant Hormone Therapy: How and When? Hein Van Poppel * Department
european urology supplements 7 (2008) 747 751 available at www.sciencedirect.com journal homepage: www.europeanurology.com Neoadjuvant and Adjuvant Hormone Therapy: How and When? Hein Van Poppel * Department
Role of Radiation after Radical Prostatectomy Review of Literature
 Vol. 9, No: 1 Jan - Jun 2013. Page 1-44 Role of Radiation after Radical Prostatectomy Review of Literature S.K. Raghunath, N. Srivatsa Abstract Biochemical relapse after radical prostatectomy occurs in
Vol. 9, No: 1 Jan - Jun 2013. Page 1-44 Role of Radiation after Radical Prostatectomy Review of Literature S.K. Raghunath, N. Srivatsa Abstract Biochemical relapse after radical prostatectomy occurs in
Neoadjuvant hormonal therapy in prostate cancer impact of PSA level before radiotherapy
 JBUON 2013; 18(4): 949-953 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Neoadjuvant hormonal therapy in prostate cancer impact of PSA level
JBUON 2013; 18(4): 949-953 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Neoadjuvant hormonal therapy in prostate cancer impact of PSA level
Prognostic factors in locally advanced prostate cancer as determined by biochemistry, imaging studies and pathology
 Prognostic factors in locally advanced prostate cancer as determined by biochemistry, imaging studies and pathology Authors Key words C.Y. Hsu, S. Joniau, R. Oyen, T. Roskams, H. Van Poppel Prognostic
Prognostic factors in locally advanced prostate cancer as determined by biochemistry, imaging studies and pathology Authors Key words C.Y. Hsu, S. Joniau, R. Oyen, T. Roskams, H. Van Poppel Prognostic
Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD
 MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD Division of Urology, MCP Hahnemann University, Philadelphia, PA
MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD Division of Urology, MCP Hahnemann University, Philadelphia, PA
DIAGNOSIS OF PROSTATE CANCER
 DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
THE PROSTATE gland is the most common cancer site in
 Prognostic Significance of Visible Lesions on Transrectal Ultrasound in Impalpable Prostate Cancers: Implications for Staging By Herbert Augustin, Markus Graefen, Jüri Palisaar, Jakob Blonski, Andreas
Prognostic Significance of Visible Lesions on Transrectal Ultrasound in Impalpable Prostate Cancers: Implications for Staging By Herbert Augustin, Markus Graefen, Jüri Palisaar, Jakob Blonski, Andreas
Locally Recurrent Prostate Cancer After Initial Radiation Therapy: A Comparison of Salvage Radical Prostatectomy Versus Cryotherapy
 Locally Recurrent Prostate Cancer After Initial Radiation Therapy: A Comparison of Salvage Radical Prostatectomy Versus Cryotherapy Louis L. Pisters,*, Dan Leibovici, Michael Blute, Horst Zincke, Thomas
Locally Recurrent Prostate Cancer After Initial Radiation Therapy: A Comparison of Salvage Radical Prostatectomy Versus Cryotherapy Louis L. Pisters,*, Dan Leibovici, Michael Blute, Horst Zincke, Thomas
External-Beam Radiotherapy in the Management of Carcinoma of the Prostate
 Technological advances in external-beam radiation therapy and the developments in equipment and computers allow for safer delivery of higher radiation doses to the prostate. Tina Sotis. The Tropic of Capricorn
Technological advances in external-beam radiation therapy and the developments in equipment and computers allow for safer delivery of higher radiation doses to the prostate. Tina Sotis. The Tropic of Capricorn
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Oncology Annual Report: Prostate Cancer 2005 Update By: John Konefal, MD, Radiation Oncology
 Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
CMScript. Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014
 Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Prostate cancer is the most common cause of death from cancer in men over age 75. Prostate cancer is rarely found in men younger than 40.
 A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer
 Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer Adam R. Kuykendal, MD; Laura H. Hendrix, MS; Ramzi G. Salloum, PhD; Paul A. Godley, MD, PhD; Ronald C. Chen, MD, MPH No conflicts
Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer Adam R. Kuykendal, MD; Laura H. Hendrix, MS; Ramzi G. Salloum, PhD; Paul A. Godley, MD, PhD; Ronald C. Chen, MD, MPH No conflicts
Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy
 Brachytherapy - (2012) - Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy Carlos Vargas 1, *, Douglas Swartz 2, Apoorva Vashi 2, Mark Blasser
Brachytherapy - (2012) - Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy Carlos Vargas 1, *, Douglas Swartz 2, Apoorva Vashi 2, Mark Blasser
Jurisdiction Virginia
 PROPOSED/DRAFT Local Coverage Determination (LCD): MolDX: Prolaris Prostate Cancer Genomic Assay (DL35629) Please note: This is a Proposed/Draft policy. Proposed/Draft LCDs are works in progress that are
PROPOSED/DRAFT Local Coverage Determination (LCD): MolDX: Prolaris Prostate Cancer Genomic Assay (DL35629) Please note: This is a Proposed/Draft policy. Proposed/Draft LCDs are works in progress that are
PCa Commentary. Volume 73 January-February 2012 PSA AND TREATMENT DECISIONS:
 1101 Madison Street Suite 1101 Seattle, WA 98104 P 206-215-2480 www.seattleprostate.com PCa Commentary Volume 73 January-February 2012 CONTENTS PSA SCREENING & BASIC SCIENCE PSA AND TREATMENT 1 DECISIONS
1101 Madison Street Suite 1101 Seattle, WA 98104 P 206-215-2480 www.seattleprostate.com PCa Commentary Volume 73 January-February 2012 CONTENTS PSA SCREENING & BASIC SCIENCE PSA AND TREATMENT 1 DECISIONS
Understanding the. Controversies of. testosterone replacement. therapy in hypogonadal men with prostate cancer. controversies surrounding
 Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds
 Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy:
Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy:
CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results. Alan Katz MD JD Flushing, NY USA
 CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results Alan Katz MD JD Flushing, NY USA Prostate Ablative Therapy Over the last 10 years our therapy has improved bned rates for LDR/HDR
CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results Alan Katz MD JD Flushing, NY USA Prostate Ablative Therapy Over the last 10 years our therapy has improved bned rates for LDR/HDR
Erectile function and quality of life after interstitial radiation therapy for prostate cancer
 (2000) 12, Suppl 3, S18±S24 ß 2000 Macmillan Publishers Ltd All rights reserved 0955-9930/00 $15.00 www.nature.com/ijir Erectile function and quality of life after interstitial radiation therapy for prostate
(2000) 12, Suppl 3, S18±S24 ß 2000 Macmillan Publishers Ltd All rights reserved 0955-9930/00 $15.00 www.nature.com/ijir Erectile function and quality of life after interstitial radiation therapy for prostate
Local Coverage Determination (LCD): MolDX: Genomic Health Oncotype DX Prostate Cancer Assay (L36153)
 Local Coverage Determination (LCD): MolDX: Genomic Health Oncotype DX Prostate Cancer Assay (L36153) Contractor Information Contractor Name Palmetto GBA LCD Information Document Information LCD ID L36153
Local Coverage Determination (LCD): MolDX: Genomic Health Oncotype DX Prostate Cancer Assay (L36153) Contractor Information Contractor Name Palmetto GBA LCD Information Document Information LCD ID L36153
Local Salvage Therapies After Failed Radiation for Prostate Cancer. Biochemical Failure after Radiation
 Local Salvage Therapies After Failed Radiation for Prostate Cancer James Eastham, MD Memorial Sloan-Kettering Cancer Center New York, New York Biochemical Failure after Radiation ASTRO criteria 3 consecutive
Local Salvage Therapies After Failed Radiation for Prostate Cancer James Eastham, MD Memorial Sloan-Kettering Cancer Center New York, New York Biochemical Failure after Radiation ASTRO criteria 3 consecutive
Salvage Conformal Radiotherapy for Biochemical Recurrent Prostate Cancer after Radical Prostatectomy
 Clinical Urology Salvage Conformal Radiotherapy for Prostate Cancer International Braz J Urol Vol. 32 (4): 46-427, July - August, 2006 Salvage Conformal Radiotherapy for Biochemical Recurrent Prostate
Clinical Urology Salvage Conformal Radiotherapy for Prostate Cancer International Braz J Urol Vol. 32 (4): 46-427, July - August, 2006 Salvage Conformal Radiotherapy for Biochemical Recurrent Prostate
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Newly Diagnosed Prostate Cancer: Understanding Your Risk
 Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Prostate Cancer. Treatments as unique as you are
 Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Gleason Score. Oncotype DX GPS. identified for. about surveillance. time to get sophisticated
 patient: MARK SMITH PSA 6.2 Gleason Score 6 Oncotype DX GPS 8 identified for active surveillance time to get sophisticated about surveillance Accurate prediction of prostate cancer risk is needed at the
patient: MARK SMITH PSA 6.2 Gleason Score 6 Oncotype DX GPS 8 identified for active surveillance time to get sophisticated about surveillance Accurate prediction of prostate cancer risk is needed at the
Protons vs. CyberKnife. Protons vs. CyberKnife. Page 1 UC SF. What are. Alexander R. Gottschalk, M.D., Ph.D.
 Protons vs. CyberKnife UC SF Protons vs. CyberKnife UC SF Alexander R. Gottschalk, M.D., Ph.D. Associate Professor and Director of the CyberKnife Radiosurgery Program Department of Radiation Oncology University
Protons vs. CyberKnife UC SF Protons vs. CyberKnife UC SF Alexander R. Gottschalk, M.D., Ph.D. Associate Professor and Director of the CyberKnife Radiosurgery Program Department of Radiation Oncology University
The Evolving Role of Prostate Brachytherapy
 Brachytherapy is rapidly becoming a preferred choice by patients for the management of their localized prostate cancer. Faith Krucina. Power of Sound. 36 24. Acrylic on canvas, Courtesy of Artistic Images
Brachytherapy is rapidly becoming a preferred choice by patients for the management of their localized prostate cancer. Faith Krucina. Power of Sound. 36 24. Acrylic on canvas, Courtesy of Artistic Images
Original Article. Cancer March 1, 2009 981
 Time to Prostate-Specific Antigen Nadir Independently Predicts Overall Survival in Patients Who Have Metastatic Hormone-Sensitive Prostate Cancer Treated With Androgen-Deprivation Therapy Toni K. Choueiri,
Time to Prostate-Specific Antigen Nadir Independently Predicts Overall Survival in Patients Who Have Metastatic Hormone-Sensitive Prostate Cancer Treated With Androgen-Deprivation Therapy Toni K. Choueiri,
Radiation Therapy for Prostate Cancer: Treatment options and future directions
 Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
Current and Future Trends in Proton Treatment of Prostate Cancer
 Current and Future Trends in Proton Treatment of Prostate Cancer Reinhard W. Schulte Assistant Professor Department of Radiation Medicine Loma Linda University Medical Center Loma Linda, CA, USA Outline
Current and Future Trends in Proton Treatment of Prostate Cancer Reinhard W. Schulte Assistant Professor Department of Radiation Medicine Loma Linda University Medical Center Loma Linda, CA, USA Outline
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
A STATISTICAL EVALUATION OF RULES FOR BIOCHEMICAL FAILURE AFTER RADIOTHERAPY IN MEN TREATED FOR PROSTATE CANCER
 doi:10.1016/j.ijrobp.2009.01.013 Int. J. Radiation Oncology Biol. Phys., Vol. 75, No. 5, pp. 1357 1363, 2009 Copyright Ó 2009 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/09/$ see front
doi:10.1016/j.ijrobp.2009.01.013 Int. J. Radiation Oncology Biol. Phys., Vol. 75, No. 5, pp. 1357 1363, 2009 Copyright Ó 2009 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/09/$ see front
Prostate Cancer In-Depth
 Prostate Cancer In-Depth Introduction Prostate cancer is the most common visceral malignancy among American men. In the year 2003, there are expected to be 220,000 new cases and nearly 29,000 deaths in
Prostate Cancer In-Depth Introduction Prostate cancer is the most common visceral malignancy among American men. In the year 2003, there are expected to be 220,000 new cases and nearly 29,000 deaths in
STATE OF MICHIGAN DEPARTMENT OF INSURANCE AND FINANCIAL SERVICES Before the Director of Insurance and Financial Services
 STATE OF MICHIGAN DEPARTMENT OF INSURANCE AND FINANCIAL SERVICES Before the Director of Insurance and Financial Services In the matter of: Petitioner, v Blue Care Network of Michigan, Respondent. File
STATE OF MICHIGAN DEPARTMENT OF INSURANCE AND FINANCIAL SERVICES Before the Director of Insurance and Financial Services In the matter of: Petitioner, v Blue Care Network of Michigan, Respondent. File
Prostate Cancer Screening in Taiwan: a must
 Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
Individual Prediction
 Individual Prediction Michael W. Kattan, Ph.D. Professor of Medicine, Epidemiology and Biostatistics, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University Chairman, Department
Individual Prediction Michael W. Kattan, Ph.D. Professor of Medicine, Epidemiology and Biostatistics, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University Chairman, Department
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH
 9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
Department of Urology, Erasmus MC, 3015 CE Rotterdam, The Netherlands
 Advances in Urology Volume 2012, Article ID 612707, 6 pages doi:10.1155/2012/612707 Research Article The Role of Adjuvant Hormonal Treatment after Surgery for Localized High-Risk Prostate Cancer: Results
Advances in Urology Volume 2012, Article ID 612707, 6 pages doi:10.1155/2012/612707 Research Article The Role of Adjuvant Hormonal Treatment after Surgery for Localized High-Risk Prostate Cancer: Results
Prostate Cancer. Patient Information
 Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
TARGETED CRYOABLATION OF THE PROSTATE: 7-YEAR OUTCOMES IN THE PRIMARY TREATMENT OF PROSTATE CANCER
 TARGETED CRYOABLATION OF THE PROSTATE: 7-YEAR OUTCOMES IN THE PRIMARY TREATMENT OF PROSTATE CANCER DUKE K. BAHN, FRED LEE, ROBERT BADALAMENT, ANIL KUMAR, JEFFREY GRESKI, AND MICHAEL CHERNICK ABSTRACT The
TARGETED CRYOABLATION OF THE PROSTATE: 7-YEAR OUTCOMES IN THE PRIMARY TREATMENT OF PROSTATE CANCER DUKE K. BAHN, FRED LEE, ROBERT BADALAMENT, ANIL KUMAR, JEFFREY GRESKI, AND MICHAEL CHERNICK ABSTRACT The
Cyberknife Information Guide. Prostate Cancer Treatment
 Cyberknife Information Guide Prostate Cancer Treatment CYBERKNIFE INFORMATION GUIDE PROSTATE CANCER TREATMENT As a patient recently diagnosed with localized prostate cancer, it is important that you familiarize
Cyberknife Information Guide Prostate Cancer Treatment CYBERKNIFE INFORMATION GUIDE PROSTATE CANCER TREATMENT As a patient recently diagnosed with localized prostate cancer, it is important that you familiarize
American College Of Radiology ACR Appropriateness Criteria PERMANENT SOURCE BRACHYTHERAPY FOR PROSTATE CANCER
 American College Of Radiology ACR Appropriateness Criteria PERMANENT SOURCE BRACHYTHERAPY FOR PROSTATE CANCER Expert Panel on Radiation Oncology Prostate Work Group: Louis Potters, MD 1 ; Carlos A. Perez,
American College Of Radiology ACR Appropriateness Criteria PERMANENT SOURCE BRACHYTHERAPY FOR PROSTATE CANCER Expert Panel on Radiation Oncology Prostate Work Group: Louis Potters, MD 1 ; Carlos A. Perez,
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
Prostate Cancer Treatment: What s Best for You?
 Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Treatment strategies for high-risk locally advanced prostate cancer
 REVIEwS Treatment strategies for high-risk locally advanced prostate cancer Seth A. Rosenthal and Howard M. Sandler Abstract High-risk prostate cancer can be defined by the assessment of pretreatment prognostic
REVIEwS Treatment strategies for high-risk locally advanced prostate cancer Seth A. Rosenthal and Howard M. Sandler Abstract High-risk prostate cancer can be defined by the assessment of pretreatment prognostic
LOW LEVELS OF PROSTATE-SPECIFIC ANTIGEN PREDICT LONG-TERM RISK OF PROSTATE CANCER: RESULTS FROM THE BALTIMORE LONGITUDINAL STUDY OF AGING
 ADULT UROLOGY CME ARTICLE LOW LEVELS OF PROSTATE-SPECIFIC ANTIGEN PREDICT LONG-TERM RISK OF PROSTATE CANCER: RESULTS FROM THE BALTIMORE LONGITUDINAL STUDY OF AGING JUNYONG FANG, E. JEFFREY METTER, PATRICIA
ADULT UROLOGY CME ARTICLE LOW LEVELS OF PROSTATE-SPECIFIC ANTIGEN PREDICT LONG-TERM RISK OF PROSTATE CANCER: RESULTS FROM THE BALTIMORE LONGITUDINAL STUDY OF AGING JUNYONG FANG, E. JEFFREY METTER, PATRICIA
Proton Therapy for Prostate Cancer
 Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director, Proton Therapy Center Associate Professor Department of Radiation Oncology M.D. Anderson Cancer Center Randomized studies showing benefit
Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director, Proton Therapy Center Associate Professor Department of Radiation Oncology M.D. Anderson Cancer Center Randomized studies showing benefit
Prostate cancer. Christopher Eden. The Royal Surrey County Hospital, Guildford & The Hampshire Clinic, Old Basing.
 Prostate cancer Christopher Eden The Royal Surrey County Hospital, Guildford & The Hampshire Clinic, Old Basing. Screening Screening men for PCa (prostate cancer) using PSA (Prostate Specific Antigen blood
Prostate cancer Christopher Eden The Royal Surrey County Hospital, Guildford & The Hampshire Clinic, Old Basing. Screening Screening men for PCa (prostate cancer) using PSA (Prostate Specific Antigen blood
Clinical Trials and Radiation Treatment. Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto
 Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT
 MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
Prostate Cancer Results Study Group 2014 Results Comparing Treatment of. About This Review Study
 Prostate Cancer Results Study Group Results Comparing Treatment of Prostate Cancer Peter Grimm, DO Seattle, WA About This Review Study,000+ prostate studies were published between 00 and June 3, of those
Prostate Cancer Results Study Group Results Comparing Treatment of Prostate Cancer Peter Grimm, DO Seattle, WA About This Review Study,000+ prostate studies were published between 00 and June 3, of those
SRO Tutorial: Prostate Cancer Treatment Options
 SRO Tutorial: Prostate Cancer Treatment Options May 7th, 2010 Daniel M. Aebersold Klinik und Poliklinik für Radio-Onkologie Universität Bern, Inselspital Is cure necessary in those in whom it may be possible,
SRO Tutorial: Prostate Cancer Treatment Options May 7th, 2010 Daniel M. Aebersold Klinik und Poliklinik für Radio-Onkologie Universität Bern, Inselspital Is cure necessary in those in whom it may be possible,
A New Biomarker in Prostate Cancer Care: Oncotype Dx. David M Albala, MD Chief of Urology Crouse Hospital Syracuse, NY
 A New Biomarker in Prostate Cancer Care: Oncotype Dx David M Albala, MD Chief of Urology Crouse Hospital Syracuse, NY Learning Objectives Review the current challenges in the prediction and prognosis of
A New Biomarker in Prostate Cancer Care: Oncotype Dx David M Albala, MD Chief of Urology Crouse Hospital Syracuse, NY Learning Objectives Review the current challenges in the prediction and prognosis of
Transrectal high-intensity focused ultrasound for the treatment of localized prostate cancer: Eight-year experience
 International Journal of Urology (2009) 16, 881 886 doi: 10.1111/j.1442-2042.2009.02389.x Original Article: Clinical Investigationiju_2389 881..886 Transrectal high-intensity focused ultrasound for the
International Journal of Urology (2009) 16, 881 886 doi: 10.1111/j.1442-2042.2009.02389.x Original Article: Clinical Investigationiju_2389 881..886 Transrectal high-intensity focused ultrasound for the
Saturation Biopsy vs. 3D Spatial Biopsy vs. Free Hand Ultrasound biopsy for Targeted Prostate Cancer Therapies
 Saturation Biopsy vs. 3D Spatial Biopsy vs. Free Hand Ultrasound biopsy for Targeted Prostate Cancer Therapies John F. Ward, MD Assistant Professor University of Texas M. D. Anderson Cancer Center Ablation
Saturation Biopsy vs. 3D Spatial Biopsy vs. Free Hand Ultrasound biopsy for Targeted Prostate Cancer Therapies John F. Ward, MD Assistant Professor University of Texas M. D. Anderson Cancer Center Ablation
Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward
 Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward 33 rd Annual Internal Medicine Update December 5, 2015 Ryan C. Hedgepeth, MD, MS Chief of
Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward 33 rd Annual Internal Medicine Update December 5, 2015 Ryan C. Hedgepeth, MD, MS Chief of
Prostate Cancer. Guideline for the Management of Clinically Localized Prostate Cancer: 2007 Update
 Prostate Cancer Members, (specialty): Ian Thompson, M.D., Chair, (Urology) James Brantley Thrasher, M.D., Co-Chair, (Urology) Gunnar Aus, M.D., (Urology) Arthur L. Burnett, M.D., (Sexual Medicine) Edith
Prostate Cancer Members, (specialty): Ian Thompson, M.D., Chair, (Urology) James Brantley Thrasher, M.D., Co-Chair, (Urology) Gunnar Aus, M.D., (Urology) Arthur L. Burnett, M.D., (Sexual Medicine) Edith
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA
 KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
Advances In Chemotherapy For Hormone Refractory Prostate Cancer. TAX 327 study results & SWOG 99-16 study results presented at ASCO 2004
 Ronald de Wit Rotterdam Cancer Institute The Netherlands Advances In Chemotherapy For Hormone Refractory Prostate Cancer TAX 327 study results & SWOG 99-16 study results presented at Slide 1 Prostate Cancer
Ronald de Wit Rotterdam Cancer Institute The Netherlands Advances In Chemotherapy For Hormone Refractory Prostate Cancer TAX 327 study results & SWOG 99-16 study results presented at Slide 1 Prostate Cancer
Patient Selection for Prostate Brachytherapy
 Patient Selection for Prostate Brachytherapy a report by Gregory S Merrick, MD 1, Wayne M Butler, PhD 1 and K ent E Wallner, MD 2 1. Schiffler Cancer Center and Wheeling Jesuit University, 2. Puget Sound
Patient Selection for Prostate Brachytherapy a report by Gregory S Merrick, MD 1, Wayne M Butler, PhD 1 and K ent E Wallner, MD 2 1. Schiffler Cancer Center and Wheeling Jesuit University, 2. Puget Sound
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTATION CANCER OF THE PROSTATE
 BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTATION CANCER OF THE PROSTATE Prostate cancer, like other cancers, is a disease of the body's cells. Normal cells reproduce themselves by dividing--facilitating
BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTATION CANCER OF THE PROSTATE Prostate cancer, like other cancers, is a disease of the body's cells. Normal cells reproduce themselves by dividing--facilitating
