Regional Perinatal Intensive Care Centers (RPICC) Annual Report. Fiscal Year
|
|
|
- Julia Kennedy
- 9 years ago
- Views:
Transcription
1 Regional Perinatal Intensive Care Centers (RPICC) Annual Report Fiscal Year Charlie Crist, Governor Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General December 1, 2009
2 Table of Contents Page i Executive Summary 1 Program Summary 2 Introduction 3 Transportation Education and Coordination RPICC Data System Obstetrical Component and Data 6 Chart 1: Medicaid Rates for Obstetrical Care Groups Table 1: FY Obstetrical Program Patients Served Graph 1: Obstetrical Program Caseload from to Present Obstetric Satellite Clinic Component and Data 12 Table 2: FY Obstetrical Satellite Program Patients Served Graph 2: Obstetrical Satellite Program Caseload from to Present Neonatal Component and Data 16 Chart 2: Medicaid Rates for Neonatal Care Groups Table 3: FY Neonatal Program Patients Served Graph 3: Neonatal Program Caseload from to Present Appendices Appendix A: Regional Perinatal Intensive Care Center Program Timeline 20 Appendix B: Definitions of Terms 21 Appendix C: Map of FY Florida RPICC Programs 23 Appendix D: Map of FY Florida RPICC Obstetrical Satellite Programs 24
3 EXECUTIVE SUMMARY This report, required by section , Florida Statutes, provides summary statistics and information about the Regional Perinatal Intensive Care Centers (RPICC) Program for fiscal year (FY) A brief overview of findings: Since the RPICC Neonatal Program began in 1974, more than 170,349 critically ill newborns have been served in RPICC-designated hospitals. Since 1977, when the RPICC Program expanded to include obstetrical services, prenatal and obstetrical intensive care services have been provided to more than 213,044 women with high-risk pregnancies. The High-Risk Obstetrical Satellite Clinic Program began in 1991 as a part of the Healthy Start Initiative, has served more than 23,205 high-risk obstetrical patients. In FY , an estimated cost avoidance of approximately $18,180,172 in hospital and physician reimbursements associated with neonatal intensive care unit services was realized by providing the RPICC Program prenatal care Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 1
4 PROGRAM SUMMARY Obstetrical Component There were 11,273 pregnant women enrolled in the RPICC program. The number of pregnant women who received services decreased slightly during FY There were 9,434 RPICC obstetrical patients who delivered 9,887 neonates. Of these neonates, 9,082 were born alive. There were 8,805 women, or 78.1 percent, who entered the program during the prenatal period. Women who received program-based prenatal care made an average of 7 Children s Medical Services (CMS) high-risk obstetrical visits. The average hospital stay for RPICC obstetrical patients was 4 days for antepartum, intrapartum, and postpartum periods. This remained stable during FY High-Risk OB Satellite Clinic Program There were 12 clinic sites operational during the year. There were 1,899 RPICC obstetrical satellite clinic patients seen at the 12 OB satellite clinic sites. These women made 2,444 clinic visits, or 1.29 visits per patient. Of the 1098 reported low-income women who received RPICC obstetrical satellite clinic services and subsequently delivered, only 24.1 percent required delivery at a RPICC facility. Of the 1099 neonates born alive to the RPICC obstetrical satellite clinic patients, 4.3 percent required level three neonatal intensive care unit services. Neonatal Component There were 3,220 RPICC Program neonates served in the RPICC neonatal intensive care units, a 5.6 percent increase from FY Of the neonates born in RPICC facilities, 90.4 percent of them survived through the neonatal period. The average length of stay for RPICC Program neonates discharged from the RPICCs was 35.5 days, a 16.6 percent decrease in the average length of stay for RPICC Program neonates served during FY Compared to a statewide incidence of 1.5 percent in calendar year 2008, 28 percent of the neonates admitted to the RPICCs had a birth weight of greater than 500 grams and less than 1,500 grams (3.5 pounds). The mortality rate for these neonates was 9.61 percent, a decrease of.43 percent over the rate Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 2
5 INTRODUCTION Statutory Authority This report, required by section , Florida Statutes, provides summary statistics and information about the Regional Perinatal Intensive Care Centers (RPICC) Program for Fiscal Year (FY) Program History The Regional Perinatal Intensive Care Centers Program is a comprehensive, statewide perinatal healthcare delivery system administered by Children s Medical Services (CMS) in the Department of Health. The RPICC Program provides obstetrical (OB) services to women identified as having highrisk pregnancies, and neonatal intensive care services to critically ill/low birth-weight newborns. The ultimate goal of the RPICC Program is to improve the immediate and long-term outcomes of pregnancy, and of infants born at risk. In 1974, the need to establish a statewide program for high-risk newborns was recognized, resulting in an initial appropriation by the Florida Legislature to fund five Regional Neonatal Intensive Care Centers. Sections through , Florida Statutes, enacted in 1976, provide the statutory basis for the Regional Neonatal Intensive Care Centers Program. The statute, amended in 1977 to include high-risk obstetrical services, changed the name to Regional Perinatal Intensive Care Centers Program, and provided for 10 designated centers. In 1982, the statute was amended to authorize the provision of step-down neonatal special care services to infants who had received care in a RPICC level three neonatal intensive care unit. In FY , with the enactment of section , Florida Statutes, step-down hospitals were no longer designated by, or included in, the RPICC Program. The RPICC statute, amended in 1994, allowed designation of 11 centers. See the Florida RPICC Programs map on page 23. Since the inception of the Regional Neonatal Intensive Care Centers Program in 1974, the impact of high-risk birth and neonatal intensive care on children has been measured. The Developmental Evaluation and Intervention Program (originally known as the Developmental Evaluation Follow-up Component of the RPICC Program) provided a mechanism for the early identification of infants with developmental and/or medical problems, and referrals for early intervention services for the infant and his or her family. In 1987, section , Florida Statutes, required establishment of developmental intervention, parent support, and training programs in conjunction with each RPICC. It also provided for expansion of the Developmental Evaluation and Intervention Program to provide in hospital and post-discharge intervention services. The focus shifted from the evaluation of care in a neonatal intensive care unit to determining the child and family s concerns and needs, assuring the provision of service coordination, referrals to services, and short-term provision of intervention services. The RPICC Developmental Evaluation and Intervention Program, one of several programs that have been incorporated under the umbrella program called the Children s Medical Services Early Steps Program, was transferred from the RPICC Program in In 1988, a high-risk obstetrical satellite clinic was established in Naples to provide community-based consultative services for high-risk indigent women within their local community. In 1991, the Legislature provided six months of funding to expand the High-Risk Obstetrical Satellite Clinic Program to 12 sites throughout Florida under Governor Chiles' Healthy Start Initiative. In 1992, the Legislature provided additional funding for the High-Risk Obstetrical Satellite Clinic Program for expansion throughout the state. In FY , the funding source for the RPICC Program hospital and professional services shifted to the Medicaid program. Because of the funding shift, Medicaid financial eligibility expanded to include pregnant women, and children less than one year old, with incomes up to 150 percent of Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 3
6 the federal, non-farm poverty level. In May 1992, Medicaid financial eligibility expanded to include women with incomes up to 185 percent of the federal, non-farm poverty level. In July 2000, the Medicaid financial eligibility expanded to include incomes up to 200 percent of the federal non-farm poverty level for children less than one year old. All RPICC obstetrical and neonatal program patients are potential Medicaid recipients. Since FY , Medicaid has used the Neonatal Care Group and Obstetrical Care Group methodology for reimbursement of RPICC obstetrical and neonatal professional providers. For the definition of terms, see Appendix B on page 21. RPICC hospitals that complied with statutory requirements received special RPICC disproportionate share funds when allocated by the legislature, in addition to any other disproportionate share funds they may receive from Medicaid. It should be noted that Lee Memorial Hospital did not receive RPICC disproportionate share funds, because its funding could not negatively impact the disproportionate share funds of the other centers. In 2004, due to Medicaid Reform, the disproportionate share (DSH) funds for each RPICC were shifted into the statewide DSH fund program. For a comprehensive RPICC Program timeline, see Appendix A on page 20. Each year, CMS contracts with hospitals and physicians to provide RPICC Program services to all medically and financially eligible patients. Obstetrical and neonatal services are funded by Medicaid. During FY , 12 hospitals participated in the RPICC Program as 11 designated centers. Bayfront Medical Center and All Children's Hospital together are considered one center. Throughout the history of the RPICC Program, faculty and staff of designated centers have made significant contributions to perinatal care in Florida. In addition to providing care and treatment for RPICC patients and their families, RPICC staff have been involved in the following: Participation in the National Perinatal Information Center study to assess the status of regionalized perinatal care in Florida. Involvement in the Florida Perinatal Association. Using neonatal morbidity and mortality data for quality assurance indicators. Participation in efforts to stop mandatory early maternal discharge after delivery. Involvement in family-centered care in the neonatal intensive care unit and in maternity units. Assessment of quality assurance and improvement activities to assure the provision of quality, state-of-the-art care for women with high-risk pregnancies and sick/low birth-weight infants. Analysis of data to determine the long-term impact of the care in neonatal intensive care unit on school performance. Participation in workgroups that ensure the continued provision of quality neonatal transport services. Participation in the Pregnancy-Associated Mortality Review workgroup in the Department of Health. Participation in Florida Perinatal Quality Improvement Initiative within the Department of Health partnering with the March of Dimes and other states. The provision of perinatal intensive care services continues to have a beneficial impact on the quality of life for residents of Florida. Since 1977, when the program expanded to include obstetrics, Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 4
7 more than 213,044 women with high-risk pregnancies have been provided prenatal and obstetrical intensive care services. The neonatal mortality rate in Florida has decreased from 13.6 deaths per 1000 live births in 1974, to 4.6 deaths per 1000 live births in Since the RPICC Program began in 1974, more than 170,349 critically ill newborns have been served in the RPICC-designated hospitals. TRANSPORTATION The provision of a transport system to bring low birth-weight or sick newborns and high-risk pregnant women to the 11 centers is contractually required. Each center has a ground transport system for the inter-hospital transfer of patients within the center's general catchment area. Six of the 11 centers have developed the capability to provide air transports from referring hospitals over a distance of 75 miles from the center. These center-based transport systems focus on neonatal rather than maternal transports. The referring physician, who uses the emergency medical services providers available within their geographic area, arranges obstetrical patient transports. This applies to the majority of the centers, which require transport services. However, two centers have specialized obstetrical transport systems to move high-risk patients directly to the center. The statewide aspect of the RPICC Program often means that patients must be transported long distances to access the nearest available intensive care bed. During FY , Children s Medical Services continued to contract with Shands Teaching Hospital to provide long distance, (greater than 75 miles), and inter-hospital air transports. Transports are required when the receiving center cannot conduct the transport to move the patient to critically needed perinatal intensive care services. EDUCATION AND COORDINATION The education and coordination component is an important aspect of the RPICC Program. This component enhances the education and training of healthcare professionals who participate in the delivery of high-risk neonatal and obstetrical care. In addition, healthcare professionals in the local communities target educational enhancements to expand knowledge and experience in service delivery to high-risk pregnant women and neonates in community-based settings. During the year, each center provides staff development programs for its own staff. RPICC personnel provide educational outreach programs to community hospital and county public health unit personnel. These outreach programs for staff at community hospitals are held at either the local hospitals or the centers. The knowledge and skills acquired by community hospital personnel enhance their ability to deal with maternal and neonatal emergencies when they arise in their facilities. The educational outreach activities have resulted in an increase in the number and the appropriateness of both maternal and neonatal referrals to the RPICCs. In FY , the centers provided more than 400 educational programs. Approximately 25 percent of the programs were outreach education programs. RPICC DATA SYSTEM The need to collect data to assess the impact of the RPICC Program on perinatal mortality and morbidity was recognized when the program began in From 1974 until 1979, Sacred Heart Hospital collected data about neonates receiving neonatal intensive care services in the centers. In 1977, Shands Teaching Hospital at the University of Florida began to collect and analyze data about infants and children receiving developmental evaluation component services. An integrated, comprehensive, online, computerized data system was implemented in The RPICC data system expanded in 1992 to collect patient information for the High-Risk Obstetrical Satellite Clinic Program. In FY , the cumulative database of the RPICC Data System contained demographic and medical information for more than 170,349 newborns who received neonatal intensive care services in a RPICC neonatal intensive care center. Data for more than 213,044 women with high-risk pregnancies have been collected since Data for approximately 23,205 women who were served in the high-risk obstetrical satellite clinics have been collected. This extensive database provides the foundation for analysis of the Florida RPICC Program service delivery system Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 5
8 OBSTETRICAL COMPONENT AND DATA The obstetrical component of the RPICC Program is designed to provide comprehensive obstetrical services to pregnant women with a medical condition that would adversely affect the normal pattern of pregnancy, labor, and/or delivery. The overall objective of the obstetrical component is to provide specialized prenatal care, either on an episodic or continuous basis, to protect the lives and health of high-risk pregnant women and their unborn babies. It is preferred that pregnant women, for whom a high-risk delivery or delivery of an infant requiring neonatal intensive care is anticipated, deliver their infants at a RPICC facility where a high level of expertise in both obstetrics and neonatology is available. This ensures the most favorable outcome possible for mother and newborn. All of the 11 RPICCs provide high-risk obstetrical services to eligible pregnant women. However, access to these regional centers for high-risk prenatal care and delivery is often limited due to the distance between the woman s residence and the nearest RPICC. In response to this barrier of care, the RPICC High-Risk Obstetrical Satellite Clinic Program was initiated in For more information about the Obstetrical Satellite Clinic Program, see page 12. The only valid grounds for refusal to admit a high-risk pregnant woman to a RPICC are the lack of functional bed space for the woman and/or expected neonate, or the lack of available transportation for the woman to the center. A woman must meet medical and financial eligibility criteria to become a CMS RPICC Program patient. The Obstetrical Care Group is a prospective pricing system implemented for the obstetrical component of the RPICC Program on July 1, This system is a modification of the federal diagnosis-related groups prospective payment system. It places patients into homogeneous groups based on clinical factors that include delivery type, complications, and antepartum and postpartum hospitalizations. The Medicaid program adopted the Obstetrical Care Group reimbursement methodology for RPICC Program patients in FY Medicaid provides all funding for center-based services for RPICC Program obstetrical patients. Therefore, all RPICC patients must meet financial eligibility criteria to be potential Medicaid recipients. RPICC consultant obstetricians receive Medicaid reimbursements based on the Obstetrical Care Group rates established by the Department of Health for RPICC-eligible patients who have Medicaid coverage. RPICC hospital services, reimbursed by Medicaid, are based on the hospital per diem rate for RPICC-eligible patients who have Medicaid coverage. Because cesarean rates more than quadrupled from 1970 to 1990, the Florida Legislature responded to concerns about inappropriate utilization of cesarean delivery and the rapidly increasing cost of health care by mandating the Agency for Health Care Administration (AHCA) annually assess the cesarean rate in Florida hospitals. The average cesarean rate for 2008 was 37.7 percent for RPICC hospitals while the average for all of the hospitals in Florida was 38.2 percent. During FY , RPICC Program services were provided for 11,273 women with high-risk pregnancies. This represents a slight decrease in the number of pregnant women served during FY compared to the number served in FY The RPICC obstetrical caseload initially declined after FY , when Medicaid s reimbursement rate for prenatal care and delivery was increased. However, referrals for RPICC Program services have increased 48 percent since FY Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 6
9 There are two points of entry into the RPICC high-risk obstetrical program: 1) Referral into the clinic for consultation or ongoing prenatal care (78.1 percent entered the program via referral to the high-risk clinic). 2) Entry into the program during hospitalization either at delivery or during an antepartum inpatient stay, (21.9 percent of the patients served during the past fiscal year entered the RPICC Program during hospitalization). Entry into the RPICC Program during hospitalization has been less than 25 percent over the past three years. Of those patients referred into the clinic: 29.2 percent came from county health departments percent were referred from a low-risk center clinic percent were referred from hospital-based clinics or other sources percent were received from private providers. During FY , 9,434 program patients were hospitalized, delivered, and discharged. Of these patients served, there were 9,887 live births. During FY , there were 5,707 infants born to obstetrical patients who entered the program at delivery. Of the 5,603 live births: 3,852, or 67.5 percent, went to regular newborn care. 1,309, or 22.9 percent, went to neonatal intensive care unit care. 530, or 9.3 percent, went to intermediate care. 16, or 0.28 percent, expired after delivery. Of the remaining 104 births: 65 expired prior to delivery. 11 expired at an unknown time. 28 had unknown outcomes, other dispositions, and invalid codes. There were 3,577 births to women who received RPICC Program prenatal care. Of the 3,517 live births: 2,646, or 75.2 percent, went to regular newborn care. 549, or 15.6 percent, went to level three neonatal intensive care unit care. 305, or 8.7 percent, went to level two neonatal intensive care. 16, or 0.45 percent, expired after delivery. Of the remaining births, 37 expired prior to delivery. There is a large difference in the neonatal intensive care unit utilization for infants from the two groups of high-risk RPICC Program obstetrical patients for FY Based on the experience of the high-risk patients who received no RPICC prenatal care, it would have been expected that 1,309 or 23 percent of the infants born to high-risk obstetrical patients with prenatal care would have required care in the neonatal intensive care unit. However, only 549 infants, or 15.6 percent, required level three neonatal intensive care services Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 7
10 The provision of RPICC Program prenatal care contributed to 273 newborns that did not require care in the neonatal intensive care unit. The neonatal cost avoidance of providing RPICC Program prenatal care to pregnant women can be estimated by multiplying the average total cost per day for neonatal intensive care ($1,873.25) by the number of bed days for the infants that did not require care in the neonatal intensive care unit (9, bed days). This estimation does not include the cost of prenatal care or normal newborn care. However, a cost avoidance of approximately $18,180,172 in FY hospital and physician reimbursements associated with neonatal intensive care unit services may have been realized by providing RPICC Program prenatal care. The average age of the RPICC Program obstetrical patients at delivery was 28.1 years for FY The Office of Vital Statistics reported the average age of all women delivering during 2008 was approximately 27.7 years. There were 1.4 percent of the RPICC obstetrical patients 16 years old or younger compared to 1.5 percent of the general population for this age group in In addition, 20.9 percent of the RPICC obstetrical population were age 35 or older, as opposed to 14.6 percent of the general population. The breakdown of RPICC Obstetrical Program patients by age is: 136, or 1.4 percent, were younger than 17 years old. 769, or 7.8 percent, were 17 to 19 years old. 2,517, or 25.7 percent, were 20 to 24 years old. 2,431, or 24.8 percent, were 25 to 29 years old. 1,896, or 19.4 percent, were 30 to 34 years old. 2,044, or 20.9 percent, were 35 years old or older. The racial make-up of RPICC Program women discharged during FY was: 4,968, or 48.5 percent, White. 4,172, or 40.7 percent, Black. 113, or 1.1 percent, Asian, Haitian, Hispanic, and Native American. 990, or 9.6 percent, listed as Other. The average number of pregnancies for each patient was A total of 433 RPICC Program patients had 416 sets of twins and 14 sets of triplets and 3 sets of quadruplets. The RPICC Program obstetrical patients had an average educational level of 11.2 years. The average family size for each patient was 3.6 members. Of the program obstetrical patients: 44.0 percent were never married percent were married. 4.2 percent were divorced or separated percent were living together. 0.2 percent were widowed. RPICC hospitals are located in the larger cities in Florida and have a large number of deliveries every year. Because high-risk patients deliver there, it is expected that a significant number of the recorded maternal deaths would occur at one of the RPICCs. Between 1985 and 2006 between 2 and 34 percent of the maternal deaths each year did occur at a RPICC. In 2008, 4 of the 32 maternal deaths recorded with the Office of Vital Statistics was a patient of the Regional Perinatal Intensive Care Center Program Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 8
11 A total of 3,516 women who delivered while in the program, or 35.6 percent, entered the program during the prenatal period in FY A total of 4,113 program patients, many of whom had not delivered by the end of the fiscal year, received prenatal services through 29,753 high-risk obstetrical clinic visits. Each program patient averaged 7 RPICC high-risk obstetrical clinic prenatal visits during the fiscal year. In FY , the average number of hospitalization days for RPICC Program obstetrical patients discharged was 4.1 days, which represents an increase of 2.5 percent from the average length of stay during FY An average stay of 4.1 days includes hospital days during the antepartum, delivery, and postpartum periods. The investment in high-risk prenatal care includes RPICC-based prenatal care, as well as outreach education, Women, Infants and Children (WIC) Nutrition Services, and other programs. The results of these investments are a: Reduced risk of neonatal disabilities/developmental delays. Reduced neonatal morbidity and mortality rates. Reduced maternal morbidity and mortality rates. Medicaid has reimbursed RPICC physician providers $10,477, for Obstetrical Care Groups. These reimbursements are for patients whose dates of service occurred during FY and whose claims were adjudicated through August It should be noted that providers have one year from the date of service to bill Medicaid for reimbursements. Therefore, not all claims have been submitted for patients whose dates of service occurred during FY The FY RPICC Program obstetrical caseload by center provided in Table 1 on page 11, and the obstetrical caseloads by year between FY and FY depicted in Graph 1 on page 11. Medicaid rates for obstetrical care groups reimbursement to RPICC physicians is provided in Chart 1 on page Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 9
12 Chart 1: Medicaid Rates For Obstetrical Care Groups* OBCG 370A 370B 370C 470A 470B 470C 372A 372B 372C 472A 472B 472C 376A 476A 383A 383B 383C Description C-section, no complications C-section, 1 complication C-section, 2 complications C-section with tubal ligation C-section with hysterectomy and 1or more complication C-section with tubal ligation and 1 or more complications Vaginal delivery, no complications Vaginal delivery, 1 complication Vaginal delivery, 2 or more complications Vaginal delivery with tubal ligation Vaginal delivery with hysterectomy and 1 or more complications Vaginal delivery with tubal ligation and 1 or more complications Postpartum hospitalization Postpartum hospitalization with hysterectomy Antepartum hospital, no complications Antepartum hospital, 1 complication Antepartum hospital, 2 or more complications Payment amount Age 0-20 Payment amount Age 20+ LOS Days Through Begin Date Outlier #1 Per Diem Age Outlier #1 Per Diem Age 20+ 1,568 1, ,676 1, ,785 1, ,676 1, ,785 1, ,785 1, ,568 1, ,676 1, ,785 1, ,676 1, ,785 1, ,785 1, ,244 1, Rates listed were effective through January 1, Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 10
13 Table 1: Center # Graph 1: Regional Perinatal Intensive Care Center Obstetrical Program RPICC Tampa General Hospital (TGH) Tampa Shands Teaching Hospital (STH) Gainesville Shands-Jacksonville (S-Jax) Jacksonville Jackson Memorial Medical Center (JMMC) Miami Sacred Heart Hospital (SHH) Pensacola Arnold Palmer Hospital (APH), Orlando Bayfront Medical Center (BMC) Saint Petersburg Saint Mary s Hospital (STM) West Palm Beach Broward General Medical Center (BGMC) Fort Lauderdale Memorial Regional Hospital (MHH) Hollywood Lee Memorial HealthPark (LMH) Fort Myers # of RPICC obstetrical patients # of deliveries FY % of RPICC deliveries 1,261 5, % 722 2, % 976 3, % 3,238 5, % 319 3, % 1,879 13, % 834 3, % 1,139 3, % 590 3, % 280 4, % 85 3, % Statewide Total 11,273 52, % Regional Perinatal Care Center Obstetrical Program Patients Served Since Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 11
14 OBSTETRICAL SATELLITE CLINIC PROGRAM COMPONENT AND DATA The RPICC Program provides medical services to women with high-risk pregnancies at 12 designated hospitals throughout Florida. However, inadequate transportation resources and geographic distances of more than 100 miles sometimes limit access to RPICC services for women living in rural areas. In an effort to address these problems, Children s Medical Services established a model High-Risk Obstetrical Satellite Clinic Program in Naples, Florida, in Based on the experience in the Naples Obstetrical Satellite Clinic, the Florida Legislature in 1991 provided funding to expand the program to 12 sites as a part of the Healthy Start Initiative. In FY , the Legislature increased funding to expand the services to additional sites statewide. The prenatal care picture in Florida is constantly changing, with perinatologists moving into and out of areas, an increase in managed care, and county health departments discontinuing the provision of prenatal care. During FY , two clinics closed (Bartow, Lakeland) and one clinic was initiated (Crestview), making 15 clinics operational in FY The Bartow clinic closed as a result of the local hospital closing. An additional change in FY was the relocation of the satellite clinic in Citrus County from Inverness to Lecanto. In April 1998, the clinic in Brooksville closed and the clinic in Ruskin opened. In July 1998, the clinic in Lake City closed, and in May 1999, the clinic in Fort Pierce closed. In December 1999, the clinic in Palatka closed. In FY , the Crestview clinic moved to Fort Walton and the Daytona Beach clinic moved to Deland. In , the clinic at Umatilla relocated to Leesburg. In , Bayfront Hospital discontinued services at the OB Satellite clinic at New Port Richey and Tampa General agreed to start providing services to the clinic. Due to a shortage of qualified Maternal Fetal Medicine specialists, in Sacred Heart closed the clinics in Panama City and Fort Walton. Later, in 2006 Sacred Heart opened an OB Satellite clinic at Miramar Beach. In , Jackson Memorial opened an OB Satellite clinic in North Miami Beach. As of June 30, 2009 there were 12 RPICC high-risk obstetrical satellite clinics operational in the following locations: Ocala, Lecanto, Leesburg, Ruskin, Bartow, Dade City, New Port Richey, Deland, Rockledge, Sebring, Miramar Beach and North Miami Beach. The clinics provide tertiary-level consultative services by a Children s Medical Services maternalfetal specialist and the multidisciplinary team services of an obstetrical nurse, an ultrasound technician, and in some locations, a genetic counselor. This team works with the local prenatal care provider, either periodically or on an ongoing basis, to provide comprehensive, appropriate prenatal care in the woman's local community. While the clinics serve high-risk pregnant women with low incomes, private patients are served in most of the clinics on a fee-for-service basis. In this way, the expertise of the high-risk perinatal staff is available to the entire community. The majority of these clinics are conducted in county health departments; however, several are located in community health centers or in local hospitals. In-service educational programs are provided to community physicians and other healthcare providers on topics related to high-risk obstetrical care. During FY , approximately 20 inservice education programs were provided. The primary goals of the obstetrical satellite clinics are: To increase the number of high-risk pregnant women receiving prenatal care and delivery in their local community. To decrease the number of sick/low birth-weight newborns that require neonatal intensive care services that are born to these women. During FY , 1,899 low-income pregnant women were provided services in the obstetrical satellite clinics (or were served during the previous fiscal year and delivered during this fiscal year) Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 12
15 This represents a 1.8 percent decrease in the number of women served this fiscal year compared to those served in FY During this time, private patients were provided services in the clinic. Since no data was collected for the private patients, all data presented in this report represent only the low-income patients served in the satellite clinics. There were 2,444 clinic visits made by the women served in FY , or 1.29 visits per patient. This is a slight increase in the number of per-patient visits recorded in FY There were 2,193 ultrasound examinations and 55 amniocenteses performed on these patients. The number of clinic visits per patient continues to support the goal of providing consultative services, with the ongoing prenatal care provided by the community physician. Some patients medical condition requires transfer to a RPICC hospital for ongoing care after one or two visits to the obstetrical satellite clinic. Performance indicators, against which program effectiveness is measured, include the following: At least 70 percent of the high-risk pregnant women enrolled in the satellite clinic program will be delivered in community-based hospital facilities. No more than 9 percent of the infants born to women enrolled in the satellite clinic program will require neonatal intensive care services. Of the 1,098 women who received RPICC obstetrical satellite clinic services and for whom the subsequent delivery hospital is known, 24.1 percent delivered in a RPICC facility. This number represents 1.6 percent more women delivering in a RPICC than during the previous fiscal year. This outcome meets the first performance indicator stated above. In addition, of the 1,099 live-born neonates born to these women, only 47, or 4.3 percent, required level three neonatal intensive care. This outcome meets the second performance indicator stated above. The outcomes of all live-born neonates were as follows: 1,054 or 91.1 percent, went to the newborn nursery. 49, or 4.6 percent, went to a level two neonatal unit. 47, or 4.3 percent, required level three neonatal intensive care. 7, or.6 percent, expired after delivery. Of the 1,631 patients for whom educational level is known: 602, or 36.9 percent, had less than a high school education. 716, or 43.9 percent, completed 12 years of school. 305, or 18.7 percent, completed some or all of college. 9 or 0.5 percent, completed some post-graduate coursework. The average age of the obstetrical satellite clinic patients was 28.5 years with a median age of 29 years. Of the 1,882 patients for whom age is known: 19, or 1.0 percent, were younger than age 17-years old. 137, or 7.3 percent, were 17 to 19 years old. 451, or 24.0 percent, were 20 to 24 years old. 450, or 23.9 percent, were 25 to 29 years old. 282, or 15.0 percent, were 30 to 34 years old. 543, or 28.8 percent, were older than 34 years old Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 13
16 Of the 1,781 patients for whom marital status is known: 669, or 37.6 percent, were married. 142, or 8.0 percent, were divorced or separated. 841, or 47.2 percent, were never married. 119, or 6.7 percent, were living together. 9, or 0.5 percent, were widowed. Of the 1,884 patients for whom race was recorded: 1,332, or 70.7 percent, were White. 269, or 14.3 percent, were Black. 237, or 12.6 percent, were listed as Other. 44, or 2.3 percent, were listed as Hispanic (2) and Asian (42) Of the 1,117 infants born to mothers enrolled in the satellite clinic program for which birth weights are known: 33, or 2.9 percent, weighed less than 1,500 grams (3 pounds, 8 ounces). 121, or 10.8 percent, weighed between 1,500 and 2,499 grams. 963, or 86.2 percent, weighed 2,500 grams (5 pounds, 8 ounces.) or more. The most common reasons for referral into this program were: Advanced maternal age. Abruption. Possible congenital fetal anomaly. Gestational diabetes. Prior cesarean section. Multiple gestation. Past history of anomaly. Previous low birth weight premie The FY RPICC Program obstetrical satellite clinic caseload by center is provided in Table 2 on page 15, and the caseloads by year between FY to the present are depicted in Graph 2 on page Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 14
17 Table 2: Obstetrical Satellite Clinic Program Non-Private Patients Served in FY Associated RPICC Center Tampa General Hospital Tampa General Hospital Tampa General Hospital Tampa General Hospital Clinic # Clinic Site Number of Obstetrical Satellite Patients FY Polk County Bartow Pasco County Dade City Hillsborough Ruskin 58 8 Pasco County New Port Richey 113 Shands Hospital 2 Marion County Ocala 145 Shands Hospital 4 Lake County Leesburg 182 Shands Hospital 18 Citrus County Lecanto 373 Sacred Heart Hospital 23 Miramar-Okaloosa County 92 Arnold Palmer Hospital 15 Brevard County Rockledge 310 Arnold Palmer Hospital 16 Volusia County Deland 142 Arnold Palmer Hospital 17 Highlands County Sebring 113 Jackson Memorial Medical Center Graph 2: 23 Dade County North Miami Beach 67 Statewide Total 1,899 2,000 1,800 1,600 1,400 1,200 1, RPICC Obstetrical Satellite Clinic Patients Served Since ,262 1,4031,480 1,404 1,218 1,141 1,055 1,050 1,202 1,253 1,473 1,478 1,499 1,705 1,933 1, Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 15
18 NEONATAL COMPONENT AND DATA The neonatal component of the RPICC Program was designed to provide level three neonatal intensive care services to sick/low birth-weight neonates and level two neonatal intensive care services for the RPICC level three graduates who continue to require special care. A major goal of the neonatal component is to decrease neonatal mortality and morbidity rates through the provision of optimal medical care to sick/low birth-weight neonates, and through the early identification of infants at risk for disease, death, or disabling conditions. Neonatal intensive care services are provided at the RPICC hospitals in specialized intensive care units. With advances in technology, the very sick and/or extremely small neonates may receive total life support through special equipment and expert medical care from professionals trained in neonatal care in these centers. Level two neonatal intensive care services are a less intensive continuum of highly specialized neonatal services for infants who have received care in a RPICC level three neonatal intensive care unit. Generally, they no longer require total support to maintain life, but still require the services of a neonatologist, close observation, and partial life support. The centers also have transport systems to bring sick neonates to the centers for care. All neonates who are born in Florida and require neonatal intensive care are eligible to access services at a RPICC neonatal intensive care center. The only valid grounds for a RPICC to refuse admission of a neonate are the lack of functional bed space or unavailability of transportation for the neonate to a center. All neonates are screened for RPICC Program eligibility upon admission to a RPICC neonatal intensive care center. Eligibility for the RPICC Program is limited to neonates who meet certain medical criteria that focus on severe medical problems and/or low birth weight. The neonate's family must also meet financial eligibility criteria for the neonate to be eligible for the RPICC Program. However, RPICC Program eligibility does not impact an individual neonate's ability to access RPICC neonatal intensive care center services. Every neonate born in Florida, regardless of the family's financial status, is afforded the same access to needed services. The Neonatal Care Group is a prospective pricing system that was implemented for the neonatal component of the RPICC Program on July 1, This system is a modification of the federal diagnosis-related groups prospective payment system. It places neonates into homogeneous groups based on clinical factors that include birth weight, ventilation, surgery, and survival status. The Medicaid program adopted the Neonatal Care Group reimbursement methodology for RPICC Program patients in FY Medicaid provides funding for center-based services for RPICC Program patients. Therefore, all RPICC patients must meet financial eligibility criteria to be Medicaid recipients. RPICC consultant neonatologists receive Medicaid reimbursements based on the Neonatal Care Group rates established by the department for RPICC eligible patients who have Medicaid coverage. Medicaid reimbursed the RPICC hospital services based on the hospital per diem rate for RPICC-eligible patients who have Medicaid coverage. There were 9,881 neonates admitted into a RPICC level three neonatal intensive care center during FY National statistics indicate that approximately 4 percent to 8 percent of all live births require intensive care services. Using the 6 percent mean, the target population for FY would have been 13,885 neonates (231,417 live births in Florida during 2008 multiplied by.06). Therefore, the 11 designated RPICCs served 71.2 percent of the projected need this fiscal year. This represents a.9 percent decrease as compared to need served for FY Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 16
19 The RPICC neonatal intensive care centers served 9,881 neonates in FY , which represents a 4.5 percent decrease caseload from FY Of the 9,881 neonates served by the RPICC neonatal intensive care centers during FY , 3,220 or 32.5 percent, were RPICC Program patients. The number of RPICC Program patients increased slightly FY With the RPICC Program changes that occurred in FY , all RPICC patients are potentially eligible for Medicaid. The percentage of unfunded neonatal patients is 1.6 percent. This is an increase of 1.2 percent over last fiscal year. The percentage of eligible neonatal patients with major medical insurance was 7.5 percent. The percentage of eligible neonatal patients with Medicaid coverage (including Medicaid health maintenance organizations) was 89.5 percent. Of those RPICC neonates discharged from the RPICC neonatal intensive care centers during FY , the racial distribution was: 50.1 percent White, including Hispanic percent Black percent Asian. 6.3 percent listed as Other. Of all RPICC discharged neonates, 1,657, or 54.7 percent, were male and 1,369, or 45.2 percent, were female. The average gestational age was 32.2 weeks. Those neonates admitted into the level three neonatal intensive care centers in the RPICCs, whose birth weight was greater than 500 grams and less than 1,500 grams, accounted for 28 percent of all admissions, while 56.7 percent had birth weights of 2,500 grams or greater. For FY , the average length of stay for program neonates discharged from the RPICC was 35.5 days, which was a decrease of 16.6 percent in the average length of stay in FY Of all neonates born in the RPICCs and admitted to the level three neonatal intensive care units, 90.4 percent survived through the neonatal period. It should be noted that infants with a birth weight between 750 and 1,000 grams now have a better than 87 percent chance of survival if admitted to a level three RPICC. The survival curve is essentially flat after that weight, approaching a 100 percent survival rate for the inborn population. Survival by weight class for all neonates born at a RPICC and admitted to a level-three neonatal intensive care unit was: 39.2 percent for grams percent for grams percent for 751-1,000 grams percent for 1,001-1,500 grams percent for 1,501-2,000 grams percent for 2,001-2,500 grams 99.9 percent for neonates that weighed more than 2,500 grams. Medicaid has reimbursed RPICC physician providers for Neonatal Care Groups a total of $12,040, These reimbursements are for patients who received RPICC services and were discharged during FY , and for whom claims were adjudicated through August It should be noted that providers have one year from the date of service to bill Medicaid for reimbursements. Therefore, not all claims for patients, whose dates of service occurred during FY , have been submitted. The FY RPICC Program neonatal caseload by center is provided in Table 3 on page 19, and the neonatal caseloads by year between FY and is depicted in Graph 3 on page 19. Medicaid rates for neonatal care groups reimbursement to RPICC physicians is shown in Chart 2 on page Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 17
20 Chart 2: Medicaid Rates For Neonatal Care Groups* NCG Description Payment Amount LOS through Outlier #1 Begin date Outlier #1 Per diem Outlier #2 Begin date Outlier #2 Per diem 385A Died 0 to 5 days 1, B Died 6 to 10 days 3, C Died 11 to 15 days 5, D Died 16 plus days 16, A 386B 386V 387L 388L 387H 388H S 389E Extreme prematurity less than 750 g Premature g w/o ventilation Premature g w/ ventilation Premature 1,000-1,499g w/ ventilation Premature 1,000-1,499g w/o ventilation Premature 1,500-2,499g w/ ventilation Premature 1,500-2,499g w/o ventilation Full term more than 2,500g w/ ventilation Full term more than 2,500 g w/o ventilation Complex surgery more than 1,500 g Extracorporeal oxygenation Rates listed were effective January 1, g = grams; w/ = with; w/o = without 24, , , , , , , , , , , Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 18
21 Table 3: Center # Graph 3: Regional Perinatal Intensive Care Center Neonatal Program Patients Served for FY % Of RPICC patients/nicu admissions # Of RPICC RPICC patients served # Of NICU admissions Tampa General Hospital (TGH) Tampa % Shands Teaching Hospital (STH) Gainesville % Shands-Jacksonville (S-Jax) Jacksonville % Jackson Memorial Medical Center(JMMH) Miami 449 2, % Sacred Heart Hospital (SHH) Pensacola % Arnold Palmer Hospital (APH), Orlando 405 1, % All Children s Hospital (ACH) Saint Petersburg % Saint Mary s Hospital (STM) West Palm Beach % Broward General Medical Center(BGMC) Fort Lauderdale % Memorial Regional Hospital (MRH) Hollywood % Lee Memorial Healthpark(LMH) Fort Myers % Statewide Total 3,220 9, % 4,000 3,500 3,000 2,500 3,030 3,436 RPICC Neonatal Patients Served Since ,124 3,935 3,877 3,978 2,895 2,358 2,327 2,6132,842 3,037 3,315 3,054 3,050 3,220 2,000 1,500 1, Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 19
22 Appendix A: Regional Perinatal Intensive Care Center Program Timeline Initial funding for five Regional Neonatal Intensive Care Centers located in Alachua, Escambia, Duval, Hillsborough, and Dade Counties. The centers were located at Tampa General, Shands Teaching Hospital, University Medical Center, Jackson Memorial Hospital, Sacred Heart Hospital Funding expanded to include a sixth Regional Neonatal Intensive Care Center located in Orange County. (Arnold Palmer Hospital) Funding expanded to include a seventh Regional Neonatal Intensive Care Center located in Pinellas County. (All Children s Hospital) Section , Florida Statutes, enacted to give statutory authority for program Program expanded to serve high-risk pregnant women and renamed Regional Perinatal Intensive Care Centers (RPICC) Program. Funding expanded to designate three additional centers located in Broward and Palm Beach counties, and a second center in Dade County. (Saint Mary s Hospital, Broward General Hospital) Statewide Communication and Referral Line established to assist with the placement of infants in need of neonatal intensive care Online, computerized data system implemented Program expanded to include step-down neonatal special care centers and provide limited inter-hospital, air transportation services to facilitate patient access to needed intensive care services The Neonatal Care Group system, a prospective pricing system, was implemented for neonatal hospital services First high-risk obstetrical satellite clinic established in Key West. Obstetrical Care Group system, a prospective pricing system, was implemented for both inpatient and outpatient obstetrical hospital services Second high-risk obstetrical satellite clinic established in Naples. Neonatal Care Group and Obstetrical Care Group systems implemented Section , Florida Statutes, authorizing the Perinatal Advisory Council, was repealed by the Legislature The RPICC Program no longer includes step-down neonatal special care centers. Physician charges are reimbursed through Medicaid on the Obstetrical Care Group and Neonatal Care Group methodology. Hospital charges are reimbursed through Medicaid at the current Medicaid per diem rate Memorial Hospital of Hollywood became the tenth RPICC. Governor Chiles Healthy Start Initiative provided for the expansion of 12 obstetrical satellite clinics Legislative funding received to expand the obstetrical satellite clinic program to 18 sites Section , Florida Statutes, revised to increase the number of RPICCs to 11 and renumber the Early Intervention Program section as a separate statute Lee Memorial Hospital became the eleventh RPICC Obstetrical Satellite Clinic online data moved from DOS-based to web-based program RPICC neonatal and obstetrical components online data moved to web-based program Bayfront Hospital discontinued OB Satellite clinic services at New port Richey and Tampa General Hospital providers agreed to add this OBSAT Clinic to their contract Sacred Heart Hospital discontinued OB Satellite clinic services in Ft. Walton Beach and Panama City. In 2006, Sacred Heart began OB Satellite clinic in Miramar Beach Jackson Memorial Hospital began OB Satellite clinic in Opa-Locka Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 20
23 Appendix B: Definitions of Terms Children's Medical Services (CMS) Program Office: The organizational unit within the Department of Health that is responsible for general, statewide supervision of the administration of the RPICC Program and for the RPICC data system. High-Risk Infant (neonate): An infant of a complicated pregnancy or delivery, which puts the infant at risk for disease, death, or disability; or a newborn infant whose prematurity, congenital anomaly, or illness places that infant at high risk for disease, death, or disability immediately after birth. High-Risk Pregnancy: Major medical condition(s) in a pregnant woman that can significantly alter the usual management of the pregnancy and/or the infant. Low Birth Weight: Less than 2,500 grams (5 pounds, 8 ounces) at birth. Neonate: An infant less than 29 days old, or for the purpose of the RPICC Program, a RPICC Program infant past the age of 28 days who requires continuance of neonatal intensive care services. Neonatal Care Group (NCG) Payment System: A payment system developed by CMS, which classifies neonatal illness into groups expected to present similar medical needs and will result in approximately equal use of resources. Non-Eligible Patient (NN) (Private Patients): Neonates admitted to a RPICC neonatal intensive care unit that do not meet the medical and/or financial eligibility criteria for the RPICC Program, and pregnant women, seen in a RPICC high-risk obstetrical clinic to determine medical eligibility for the RPICC Program, who are determined to be ineligible for the program. Obstetrical Care Group (OBCG) Payment System: A payment system developed by CMS, which classifies obstetrical illness into groups expected to present similar needs and will result in approximately equal use of resources. Perinatal Period: For the purpose of this program, it is that period from medical diagnosis of pregnancy through 28 days after birth. Preterm birth: A delivery before 37 weeks gestation. Regional Perinatal Intensive Care Centers (RPICC or centers): Specialized units within hospitals specifically designed to provide a full range of health services to women with high-risk pregnancies and a full range of newborn intensive care services, which have been designated by the Department of Health and meet certain standards for facilities, staffing, and services, or committed to meet and maintain these standards within three years of designation as centers. RPICC Data System: A comprehensive, automated microcomputer-based system that collects and correlates data from all components of the RPICC Program, and provides periodic analysis of RPICC Program data. RPICC High-Risk Obstetrical Satellite Clinic: A facility located outside the RPICC that provides comprehensive, high-risk, outpatient obstetrical services that are staffed by RPICC perinatal teams per contractual agreements in areas distant to the RPICC, where there is limited access to public transportation or the unavailability of medical expertise in high-risk obstetrics for indigent women Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 21
24 RPICC Insurance-Eligible Patients (IE): All patients who meet medical and financial eligibility criteria as outlined in the RPICC Neonatal and Obstetrical standards in Chapter 64C-6, Florida Administrative Code, and who have been determined by the center to have adequate major medical insurance coverage. RPICC Level Two Neonatal Intensive Care Unit: A designated level two patient care area in a RPICC with the capability of delivering specialized care to newborns who have received care in a CMS RPICC Program level three neonatal intensive care unit and may require specialized nutritional support, or whose oxygen requirement does not exceed 40 percent at ambient pressure, and/or whose weight or medical/surgical diagnosis precludes discharge to recovery care. Such care requires a minimum of a 1:4 ratio of nurses to patients. RPICC Level Three Neonatal Intensive Care Unit: A designated level three patient care area within a RPICC having patient care stations with the capability of delivering total intensive care to newborns including, but not limited to, total respiratory support, supplemental parenteral alimentation, constant mechanical monitoring of vital signs, and long-term arterial catheterization. Such care requires a minimum of a 1:2 ratio of nurses to patients. RPICC Medicaid-Eligible Patients (EL): All patients who meet medical and financial eligibility criteria as outlined in the RPICC Neonatal and Obstetrical standards in Chapter 64C-6, Florida Administrative Code, and who are eligible for Medicaid funding. RPICC Medicaid Health Maintenance Organization Patients (HM): All neonates and pregnant women who meet both medical and financial criteria, as outlined in Chapter 64C-6, Florida Administrative Code, and in the RPICC Handbook, who have been determined by the center to have medical coverage through a Medicaid health maintenance organization. RPICC Program Patients: All neonatal and obstetrical patients who meet medical and financial eligibility criteria as outlined in the RPICC standards in Chapter 64C-6, Florida Administrative Code. This phrase does not indicate any specific RPICC Program status (for example, IE, EL, UF, HM). RPICC Unfunded Patients (UF): All patients who meet medical and financial eligibility criteria as outlined in the RPICC neonatal and obstetrical standards in Chapter 64C-6, Florida Administrative Code, who have no third party resources. Two-Point Transports: Those transports provided by a RPICC transport team for patients from a referring hospital to the receiving RPICC, or from the RPICC back to the referring hospital or another appropriate facility. Three-Point Transports: Those transports provided by a RPICC transport team originating from one RPICC and transporting patients from a referring hospital to another RPICC or designated facility, or from another RPICC back to the referring hospital or another appropriate facility (other than the RPICC doing the transport). Very Low Birth Weight: Less than 1,500 grams (3 pounds, 8 ounces) at birth Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 22
25 Appendix C: FY Florida Regional Perinatal Intensive Care Centers Program Regional Perinatal Intensive Care Centers Pensacola - Sacred Heart Hospital Gainesville - Shands Teaching Hospital Jacksonville - Shands Jacksonville Tampa - Tampa General Hospital Orlando - Arnold Palmer Hospital Saint Petersburg - All Children's Hospital (Neonatal) Bayfront Medical Center (Obstetrical) West Palm Beach - Saint Mary's Hospital Fort Lauderdale - Broward General Medical Center Hollywood - Memorial Regional Hospital Fort Myers - Lee Memorial HealthPark Miami - Jackson Memorial Medical Center Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 23
26 Appendix D: FY Florida High-Risk Obstetrical (OB) Satellite Clinic Program Regional Perinatal Intensive Care Centers OB Satellite Clinics Miramar Beach - Emerald Coast Hospital North Miami - Jackson North Medical Center New Port Richey - Pasco CHD* Dade City - Premier Community Health Care Rockledge - Wuesthoff Hospital Deland - Volusia CHD* Ocala - Marion CHD* Leesburg - Women s Wellness Center alecanto - Citrus CHD* Ruskin - Hillsborough CHD* Bartow - Polk CHD* Sebring - Highlands CHD* * CHD - County Health Department Florida Regional Perinatal Intensive Care Centers Program Annual Report Page 24
Regional Perinatal Intensive Care Centers (RPICC) Annual Report. Fiscal Year 2006-2007
 Regional Perinatal Intensive Care Centers (RPICC) Annual Report Fiscal Year 2006-2007 Charlie Crist, Governor Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General December 1, 2007 Table of Contents
Regional Perinatal Intensive Care Centers (RPICC) Annual Report Fiscal Year 2006-2007 Charlie Crist, Governor Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General December 1, 2007 Table of Contents
Regional Perinatal Intensive Care Centers Handbook
 Regional Perinatal Intensive Care Centers Handbook AUGUST 2010 TABLE OF CONTENTS 1 INTRODUCTION..4 1.1 Purpose...4 1.2 History...5 1.3 Range of Services...6 1.4 Civil Rights...7 1.5 Transportation...7
Regional Perinatal Intensive Care Centers Handbook AUGUST 2010 TABLE OF CONTENTS 1 INTRODUCTION..4 1.1 Purpose...4 1.2 History...5 1.3 Range of Services...6 1.4 Civil Rights...7 1.5 Transportation...7
Rural Health Advisory Committee s Rural Obstetric Services Work Group
 Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Chapter 3: Healthy Start Risk Screening
 Introduction Healthy Start legislation requires that all pregnant women and infants be offered screening for risk factors that may affect their pregnancy, health, or development. The prenatal and infant
Introduction Healthy Start legislation requires that all pregnant women and infants be offered screening for risk factors that may affect their pregnancy, health, or development. The prenatal and infant
Children s Medical Services Program Overview
 Children s Medical Services Program Overview 1 Children s Medical Services Family-centered, comprehensive, coordinated statewide managed system of care that links community-based health care with multidisciplinary,
Children s Medical Services Program Overview 1 Children s Medical Services Family-centered, comprehensive, coordinated statewide managed system of care that links community-based health care with multidisciplinary,
Who Is Involved in Your Care?
 Patient Education Page 3 Pregnancy and Giving Birth Who Is Involved in Your Care? Our goal is to surround you and your family with a safe environment for the birth of your baby. We look forward to providing
Patient Education Page 3 Pregnancy and Giving Birth Who Is Involved in Your Care? Our goal is to surround you and your family with a safe environment for the birth of your baby. We look forward to providing
Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General
 Florida Department of Health Division of Disease Control Bureau of Epidemiology Chronic Disease Epidemiology Section Charlie Crist Governor Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General Florida
Florida Department of Health Division of Disease Control Bureau of Epidemiology Chronic Disease Epidemiology Section Charlie Crist Governor Ana M. Viamonte Ros, M.D., M.P.H. State Surgeon General Florida
Maternity Care Primary C-Section Rate Specifications 2014 (07/01/2013 to 06/30/2014 Dates of Service)
 Summary of Changes Denominator Changes: Two additions were made to the denominator criteria. The denominator was changed to include patients who had: a vertex position delivery AND a term pregnancy of
Summary of Changes Denominator Changes: Two additions were made to the denominator criteria. The denominator was changed to include patients who had: a vertex position delivery AND a term pregnancy of
Pregnant and Parenting Youth in Foster Care in Washington State: Comparison to Other Teens and Young Women who Gave Birth
 January 2014 RDA Report 11.202 Olympia, Washington Pregnant and Parenting in Care in Washington State: Comparison to Other and Women who Gave Birth Laurie Cawthon, MD, MPH Barbara Lucenko, PhD Peter Woodcox,
January 2014 RDA Report 11.202 Olympia, Washington Pregnant and Parenting in Care in Washington State: Comparison to Other and Women who Gave Birth Laurie Cawthon, MD, MPH Barbara Lucenko, PhD Peter Woodcox,
Chapter 13: Transition and Interagency Agreements
 Healthy Start Standards & Guidelines 2007 Chapter 13: Transition and Interagency Agreements Introduction Transition is movement or change from one environment to another. Transition activities are a critical
Healthy Start Standards & Guidelines 2007 Chapter 13: Transition and Interagency Agreements Introduction Transition is movement or change from one environment to another. Transition activities are a critical
MED145 Deliverable 1.4 Interim Report. Presented to
 MED145 Deliverable 1.4 DY14 Interim Report MED145 Deliverable 1.4 Interim Report Presented to by April 7, 2014 Family Data Center College of Medicine University of Florida i Table of Contents Introduction...
MED145 Deliverable 1.4 DY14 Interim Report MED145 Deliverable 1.4 Interim Report Presented to by April 7, 2014 Family Data Center College of Medicine University of Florida i Table of Contents Introduction...
Provider Notification Obstetrical Billing
 Provider Notification Obstetrical Billing Date of Notification September 1, 20 Revision Date September 17, 2015 Plans Affected Mercy Care Plan and Mercy Care Long Term Care Plan Referrals As outlined in
Provider Notification Obstetrical Billing Date of Notification September 1, 20 Revision Date September 17, 2015 Plans Affected Mercy Care Plan and Mercy Care Long Term Care Plan Referrals As outlined in
AHE 232 Introduction to Clinical Software. Week ten:
 AHE 232 Introduction to Clinical Software Week ten: Note: I have set up the entire curriculum for this class with weekly lesson plans. This will allow the Instructor to determine how to incorporate the
AHE 232 Introduction to Clinical Software Week ten: Note: I have set up the entire curriculum for this class with weekly lesson plans. This will allow the Instructor to determine how to incorporate the
Chapter 16: Performance Based Contracts and Memoranda of Agreement
 Chapter 16: Performance Based Contracts and Memoranda of Agreement Introduction The following standards support activities that are: designated in statute and rule, necessary to accomplish implementation
Chapter 16: Performance Based Contracts and Memoranda of Agreement Introduction The following standards support activities that are: designated in statute and rule, necessary to accomplish implementation
Section IX Special Needs & Case Management
 Section IX Special Needs & Case Management Special Needs and Case Management 179 Integrated Care Management/Complex Case Management The Case Management/Care Coordination (CM/CC) program is a population-based
Section IX Special Needs & Case Management Special Needs and Case Management 179 Integrated Care Management/Complex Case Management The Case Management/Care Coordination (CM/CC) program is a population-based
OBGYN Orientation & Billing Guide 9/22/2014
 OBGYN Orientation & Billing Guide 2014 Welcome to Magnolia Health! We thank you for being part of or considering Magnolia s network of participating providers, hospitals, and other healthcare professionals.
OBGYN Orientation & Billing Guide 2014 Welcome to Magnolia Health! We thank you for being part of or considering Magnolia s network of participating providers, hospitals, and other healthcare professionals.
Table of Contents. Why Are Changes Being Made to Florida s Medicaid Program?... 3. What Is Managed Care?... 3
 Table of Contents Why Are Changes Being Made to Florida s Medicaid Program?... 3 What Is Managed Care?... 3 When Will These Changes to Florida Medicaid Occur?... 3 What Is the Goal of the Florida Managed
Table of Contents Why Are Changes Being Made to Florida s Medicaid Program?... 3 What Is Managed Care?... 3 When Will These Changes to Florida Medicaid Occur?... 3 What Is the Goal of the Florida Managed
Health Care Access to Vulnerable Populations
 Health Care Access to Vulnerable Populations Closing the Gap: Reducing Racial and Ethnic Disparities in Florida Rosebud L. Foster, ED.D. Access to Health Care The timely use of personal health services
Health Care Access to Vulnerable Populations Closing the Gap: Reducing Racial and Ethnic Disparities in Florida Rosebud L. Foster, ED.D. Access to Health Care The timely use of personal health services
On behalf of the Association of Maternal and Child Health Programs (AMCHP), I am
 Christopher Kus, M.D., M.P.H. Association of Maternal and Child Health Programs, Public Witness Testimony House Labor, Health and Human Services and Education Appropriations Subcommittee March 13, 2013
Christopher Kus, M.D., M.P.H. Association of Maternal and Child Health Programs, Public Witness Testimony House Labor, Health and Human Services and Education Appropriations Subcommittee March 13, 2013
How To Bill For A Pregnancy
 Maternity Billing The Maternity Period - For billing purposes, the obstetrical period begins on the date of the initial visit in which pregnancy was confirmed and extends through the end of the postpartum
Maternity Billing The Maternity Period - For billing purposes, the obstetrical period begins on the date of the initial visit in which pregnancy was confirmed and extends through the end of the postpartum
A Descriptive Study of Depression, Substance Abuse, and Intimate Partner Violence Among Pregnant Women
 A Descriptive Study of Depression, Substance Abuse, and Intimate Partner Violence Among Pregnant Women 1 OVERVIEW This presentation is based on the study of pregnant women enrolled in the Augusta Partnership
A Descriptive Study of Depression, Substance Abuse, and Intimate Partner Violence Among Pregnant Women 1 OVERVIEW This presentation is based on the study of pregnant women enrolled in the Augusta Partnership
Total Number of Foreign Students: 26,264. Part 1: Net Contribution to State Economy by Foreign Students (2004-05)
 Florida Total Number of Foreign Students: 26,264 Part 1: Net Contribution to State Economy by Foreign Students (2004-05) Contribution from Tuition and Fees to State Economy: $426,977,000 Contribution from
Florida Total Number of Foreign Students: 26,264 Part 1: Net Contribution to State Economy by Foreign Students (2004-05) Contribution from Tuition and Fees to State Economy: $426,977,000 Contribution from
Substance-Exposed Newborns
 Substance-Exposed Newborns State of Oklahoma 2013 Substance-Exposed Newborns State of Oklahoma 2013 Legal Background Federal guidelines in the Child Abuse Prevention and Treatment Act (CAPTA) require states
Substance-Exposed Newborns State of Oklahoma 2013 Substance-Exposed Newborns State of Oklahoma 2013 Legal Background Federal guidelines in the Child Abuse Prevention and Treatment Act (CAPTA) require states
Access to Appropriate Services for High Risk. in New York State. New York State Department of Health
 Access to Appropriate Services for High Risk Neonates in New York State Di i i f F il H l h Division of Family Health New York State Department of Health Perinatal Regionalization in New York State Perinatal
Access to Appropriate Services for High Risk Neonates in New York State Di i i f F il H l h Division of Family Health New York State Department of Health Perinatal Regionalization in New York State Perinatal
Oregon Birth Outcomes, by Planned Birth Place and Attendant Pursuant to: HB 2380 (2011)
 Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
in children less than one year old. It is commonly divided into two categories, neonatal
 INTRODUCTION Infant Mortality Rate is one of the most important indicators of the general level of health or well being of a given community. It is a measure of the yearly rate of deaths in children less
INTRODUCTION Infant Mortality Rate is one of the most important indicators of the general level of health or well being of a given community. It is a measure of the yearly rate of deaths in children less
May 18, 2015. The Honorable Rick Scott Office of the Governor 400 S. Monroe St. Tallahassee, FL 32399. Dear Governor Scott,
 May 1, 01 The Honorable Rick Scott Office of the Governor 00 S. Monroe St. Tallahassee, FL Dear Governor Scott, We appreciate the opportunity to respond to your May 1, 01 data request. As you may know,
May 1, 01 The Honorable Rick Scott Office of the Governor 00 S. Monroe St. Tallahassee, FL Dear Governor Scott, We appreciate the opportunity to respond to your May 1, 01 data request. As you may know,
Wendy Martinez, MPH, CPH County of San Diego, Maternal, Child & Adolescent Health
 Wendy Martinez, MPH, CPH County of San Diego, Maternal, Child & Adolescent Health Describe local trends in birth Identify 3 perinatal health problems Identify 3 leading causes of infant death Age Class
Wendy Martinez, MPH, CPH County of San Diego, Maternal, Child & Adolescent Health Describe local trends in birth Identify 3 perinatal health problems Identify 3 leading causes of infant death Age Class
University Hospital Community Health Needs Assessment FY 2014
 FY 2014 Prepared by Kathy Opromollo Executive Director of Ambulatory Care Services Newark New Jersey is the State s largest city. In striving to identify and address Newark s most pressing health care
FY 2014 Prepared by Kathy Opromollo Executive Director of Ambulatory Care Services Newark New Jersey is the State s largest city. In striving to identify and address Newark s most pressing health care
How Medicaid Is Changing in Florida for Those Needing Nursing Home, Assisted Living Facility, and At-Home Care
 Q &A for Advocates: How Medicaid Is Changing in Florida for Those Needing Nursing Home, Assisted Living Facility, and At-Home Care What Is Managed Care? In traditional Medicaid, a consumer can seek care
Q &A for Advocates: How Medicaid Is Changing in Florida for Those Needing Nursing Home, Assisted Living Facility, and At-Home Care What Is Managed Care? In traditional Medicaid, a consumer can seek care
8.2000: HOSPITAL PROVIDER FEE COLLECTION AND DISBURSEMENT
 DEPARTMENT OF HEALTH CARE POLICY AND FINANCING MEDICAL ASSISTANCE SECTION 8.2000 [Editor s Notes follow the text of the rules at the end of this CCR Document.] 8.2000: HOSPITAL PROVIDER FEE COLLECTION
DEPARTMENT OF HEALTH CARE POLICY AND FINANCING MEDICAL ASSISTANCE SECTION 8.2000 [Editor s Notes follow the text of the rules at the end of this CCR Document.] 8.2000: HOSPITAL PROVIDER FEE COLLECTION
Logic Model for SECCS Grant Program: Florida Early Childhood Comprehensive Systems (ECCS) Statewide Plan INTERVENTION
 TOTAL FUNDS REQUESTED (for GRANTEE/ PROJECT CHARACTERISTICS (i.e., the first year of the project): goals and description of the project, $155,496 Infant Mental Health Association Updated Florida's statewide
TOTAL FUNDS REQUESTED (for GRANTEE/ PROJECT CHARACTERISTICS (i.e., the first year of the project): goals and description of the project, $155,496 Infant Mental Health Association Updated Florida's statewide
MANA Home Birth Data 2004-2009: Consumer Considerations
 MANA Home Birth Data 2004-2009: Consumer Considerations By: Lauren Korfine, PhD U.S. maternity care costs continue to rise without evidence of improving outcomes for women or babies. The cesarean section
MANA Home Birth Data 2004-2009: Consumer Considerations By: Lauren Korfine, PhD U.S. maternity care costs continue to rise without evidence of improving outcomes for women or babies. The cesarean section
Connecticut s Medical Assistance Program
 Connecticut s Medical Assistance Program Olivia Puckett Council on Medical Assistance Program Oversight CSG-ERC Health Committee Meeting August 4, 2014 1 Agenda Council on Medical Assistance Program Oversight
Connecticut s Medical Assistance Program Olivia Puckett Council on Medical Assistance Program Oversight CSG-ERC Health Committee Meeting August 4, 2014 1 Agenda Council on Medical Assistance Program Oversight
Mississippi State Department of Health. Fiscal Years 2012-2016. Strategic Plan
 Mississippi State Department of Health Fiscal Years 2012-2016 Strategic Plan Prepared in Accordance with the Mississippi Performance Budget and Strategic Planning Act of 1994 Office of Health Administration
Mississippi State Department of Health Fiscal Years 2012-2016 Strategic Plan Prepared in Accordance with the Mississippi Performance Budget and Strategic Planning Act of 1994 Office of Health Administration
Quality Maternity Care: the Role of the Public Health Nurse
 Quality Maternity Care: the Role of the Public Health Nurse Lori Webel-Edgar RN, MN Program Manager-Reproductive Health Simcoe Muskoka District Health Unit Barrie, Ontario session overview quality maternity
Quality Maternity Care: the Role of the Public Health Nurse Lori Webel-Edgar RN, MN Program Manager-Reproductive Health Simcoe Muskoka District Health Unit Barrie, Ontario session overview quality maternity
PUBLIC HEALTH IMPROVEMENT PARTNERSHIP
 PUBLIC HEALTH IMPROVEMENT PARTNERSHIP PUBLIC HEALTH ACTIVITIES & SERVICES INVENTORY TECHNICAL NOTES HEALTHY FAMILY DEVELOPMENT Nurse-Family Partnership Nurse-Family Partnership is a voluntary program of
PUBLIC HEALTH IMPROVEMENT PARTNERSHIP PUBLIC HEALTH ACTIVITIES & SERVICES INVENTORY TECHNICAL NOTES HEALTHY FAMILY DEVELOPMENT Nurse-Family Partnership Nurse-Family Partnership is a voluntary program of
Why Accept Medicaid Dollars: The Facts
 Why Accept Medicaid Dollars: The Facts If we accept federal Medicaid dollars, nearly 500,000 North Carolinians will gain access to health insurance. As many as 1,100 medically unnecessary deaths per year
Why Accept Medicaid Dollars: The Facts If we accept federal Medicaid dollars, nearly 500,000 North Carolinians will gain access to health insurance. As many as 1,100 medically unnecessary deaths per year
Florida Center for Health Information and Policy Analysis
 Florida Center for Health Information and Policy Analysis Data Overview for the Commission on Healthcare and Hospital Funding May 20, 2015 1 Office of Data Collection and Quality Assurance Collection of
Florida Center for Health Information and Policy Analysis Data Overview for the Commission on Healthcare and Hospital Funding May 20, 2015 1 Office of Data Collection and Quality Assurance Collection of
Report of Results and Analysis of Parent Survey Data Collected in Southern West Virginia
 Partners in Community Outreach Education Begins at Home Partners in Community Outreach In-Home Family Education Programs Report of Results and Analysis of Parent Survey Data Collected in Southern West
Partners in Community Outreach Education Begins at Home Partners in Community Outreach In-Home Family Education Programs Report of Results and Analysis of Parent Survey Data Collected in Southern West
FCS Baccalaureate Programs. December 2014
 FCS Baccalaureate Programs December 2014 Questions 1. What is the purpose of offering Bachelor degrees in certain Florida College? 2. Are these programs replicating already accessible programs in their
FCS Baccalaureate Programs December 2014 Questions 1. What is the purpose of offering Bachelor degrees in certain Florida College? 2. Are these programs replicating already accessible programs in their
DEPARTMENT OF HEALTH & HUMAN SERVICES MEDICAID PROGRAM OVERVIEW
 DEPARTMENT OF HEALTH & HUMAN SERVICES MEDICAID PROGRAM OVERVIEW North Carolina General Assembly Fiscal Research Division February 2005 Overview Purpose of Medicaid Impact of Medicaid - On the State Economy
DEPARTMENT OF HEALTH & HUMAN SERVICES MEDICAID PROGRAM OVERVIEW North Carolina General Assembly Fiscal Research Division February 2005 Overview Purpose of Medicaid Impact of Medicaid - On the State Economy
By: Latarsha Chisholm, MSW, Ph.D. Department of Health Management & Informatics University of Central Florida
 By: Latarsha Chisholm, MSW, Ph.D. Department of Health Management & Informatics University of Central Florida Health Disparities Health disparities refers to population-specific differences in the presence
By: Latarsha Chisholm, MSW, Ph.D. Department of Health Management & Informatics University of Central Florida Health Disparities Health disparities refers to population-specific differences in the presence
Testimony of the American College of Nurse-Midwives. at a Hearing of the House Committee on Energy and Commerce Subcommittee on Health.
 Testimony of the American College of Nurse-Midwives at a Hearing of the House Committee on Energy and Commerce Subcommittee on Health on the Improving Access to Maternity Care Act (H.R.1209) Wednesday,
Testimony of the American College of Nurse-Midwives at a Hearing of the House Committee on Energy and Commerce Subcommittee on Health on the Improving Access to Maternity Care Act (H.R.1209) Wednesday,
Overview. Key Flu Vaccine Coverage Findings. Summary
 2013-14 Season Flu Vaccine Coverage and Hospital Quality Data Centers for Disease Control and Prevention Highlights and Data Summary September 18, 2014 Overview Flu is unpredictable. Even healthy children
2013-14 Season Flu Vaccine Coverage and Hospital Quality Data Centers for Disease Control and Prevention Highlights and Data Summary September 18, 2014 Overview Flu is unpredictable. Even healthy children
Mississippi State Department of Health. Fiscal Years 2014-2018. Strategic Plan
 Mississippi State Department of Health Fiscal Years 2014-2018 Strategic Plan Prepared in Accordance with the Mississippi Performance Budget and Strategic Planning Act of 1994 Office of Health Administration
Mississippi State Department of Health Fiscal Years 2014-2018 Strategic Plan Prepared in Accordance with the Mississippi Performance Budget and Strategic Planning Act of 1994 Office of Health Administration
Genworth 2015 Cost of Care Survey Florida
 Cost of Care Survey 2015 Genworth 2015 Cost of Care Survey State-Specific Data 118928FL 04/01/15 Homemaker Services Hourly Rates USA $8 $20 $40 $44,616 2% Whole State $10 $18 $29 $41,184 2% Cape Coral
Cost of Care Survey 2015 Genworth 2015 Cost of Care Survey State-Specific Data 118928FL 04/01/15 Homemaker Services Hourly Rates USA $8 $20 $40 $44,616 2% Whole State $10 $18 $29 $41,184 2% Cape Coral
VIRGINIA S 2015 MATERNAL AND CHILD HEALTH BLOCK GRANT (Title V) Virginia Department of Health Executive Summary
 VIRGINIA S 2015 MATERNAL AND CHILD HEALTH BLOCK GRANT (Title V) Virginia Department of Health Executive Summary May 2014 1 VIRGINIA S 2015 MATERNAL AND CHILD HEALTH BLOCK GRANT (Title V) Virginia Department
VIRGINIA S 2015 MATERNAL AND CHILD HEALTH BLOCK GRANT (Title V) Virginia Department of Health Executive Summary May 2014 1 VIRGINIA S 2015 MATERNAL AND CHILD HEALTH BLOCK GRANT (Title V) Virginia Department
KANSAS DEPARTMENT OF HEALTH AND ENVIRONMENT DIVISION OF PUBLIC HEALTH BUREAU OF FAMILY HEALTH
 KANSAS DEPARTMENT OF HEALTH AND ENVIRONMENT DIVISION OF PUBLIC HEALTH BUREAU OF FAMILY HEALTH Teen Pregnancy Targeted Case Management Manual January 2016 1 TEEN PREGNANCY TARGETED CASE MANAGEMENT MANUAL
KANSAS DEPARTMENT OF HEALTH AND ENVIRONMENT DIVISION OF PUBLIC HEALTH BUREAU OF FAMILY HEALTH Teen Pregnancy Targeted Case Management Manual January 2016 1 TEEN PREGNANCY TARGETED CASE MANAGEMENT MANUAL
Community Health Needs Assessment Implementation Plan FY 14-16
 Community Health Needs Assessment Implementation Plan FY 14-16 South Miami Hospital conducted a community health needs assessment in 2013 to better understand the healthcare needs of the community it serves
Community Health Needs Assessment Implementation Plan FY 14-16 South Miami Hospital conducted a community health needs assessment in 2013 to better understand the healthcare needs of the community it serves
Chapter 6 Case Ascertainment Methods
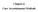 Chapter 6 Case Ascertainment Methods Table of Contents 6.1 Introduction...6-1 6.2 Terminology...6-2 6.3 General Surveillance Development...6-4 6.3.1 Plan and Document... 6-4 6.3.2 Identify Data Sources...
Chapter 6 Case Ascertainment Methods Table of Contents 6.1 Introduction...6-1 6.2 Terminology...6-2 6.3 General Surveillance Development...6-4 6.3.1 Plan and Document... 6-4 6.3.2 Identify Data Sources...
Innovative use of Neonatal Nurse Practitioners in Rural Hawaii
 Innovative use of Neonatal Nurse Practitioners in Rural Hawaii Petri Pate Pieron, MSN, MPH, APRN Rx, CPNP, NNP Presentation was supported by NIH 1 R25 RR019321 Clinical Research Education and Career Development
Innovative use of Neonatal Nurse Practitioners in Rural Hawaii Petri Pate Pieron, MSN, MPH, APRN Rx, CPNP, NNP Presentation was supported by NIH 1 R25 RR019321 Clinical Research Education and Career Development
UF Health Jacksonville CHNA Implementation Strategy
 UF Health Jacksonville CHA Implementation Strategy Adopted by the UF Health Jacksonville Governing Board on: December 7, 2015 This document describes how UF Health Jacksonville (the hospital) plans to
UF Health Jacksonville CHA Implementation Strategy Adopted by the UF Health Jacksonville Governing Board on: December 7, 2015 This document describes how UF Health Jacksonville (the hospital) plans to
New Jersey Home Visiting Initiative
 National Health Policy Forum Promoting Evidence-Based Interventions: Maternal, Infant & Early Childhood Home Visiting (MIECHV) A State Perspective on Home Visiting New Jersey Home Visiting Initiative Contact
National Health Policy Forum Promoting Evidence-Based Interventions: Maternal, Infant & Early Childhood Home Visiting (MIECHV) A State Perspective on Home Visiting New Jersey Home Visiting Initiative Contact
Facilities contract with Medicare to furnish
 Facilities contract with Medicare to furnish acute inpatient care and agree to accept predetermined acute Inpatient Prospective Payment System (IPPS) rates as payment in full. The inpatient hospital benefit
Facilities contract with Medicare to furnish acute inpatient care and agree to accept predetermined acute Inpatient Prospective Payment System (IPPS) rates as payment in full. The inpatient hospital benefit
Florida s Oral Anticancer Treatment Access Law: What Clinicians Need to Know
 Outdated coverage policies in Florida USED TO limit cancer patients access to lifesaving drugs! Traditionally, IV chemotherapy treatments are covered under a health plan s medical benefit where the patient
Outdated coverage policies in Florida USED TO limit cancer patients access to lifesaving drugs! Traditionally, IV chemotherapy treatments are covered under a health plan s medical benefit where the patient
JUST THE FACTS A Monthly Public Assistance Update from the Illinois Department of Human Services
 A Monthly Public Assistance Update from the Illinois Department of Human Services January 2014 Summary Total cases receiving Public Assistance in Illinois decreased by 10,008 (20,138 persons) in January
A Monthly Public Assistance Update from the Illinois Department of Human Services January 2014 Summary Total cases receiving Public Assistance in Illinois decreased by 10,008 (20,138 persons) in January
Amish Midwifery Care Program
 April 2012 Page 1 of 5 Grant Outcomes Report An Amish Midwifery Care Program in Chautauqua County The Problem: KEY INFORMATION: GRantEe Westfield Memorial Hospital, Inc. grant title Amish Midwifery Care
April 2012 Page 1 of 5 Grant Outcomes Report An Amish Midwifery Care Program in Chautauqua County The Problem: KEY INFORMATION: GRantEe Westfield Memorial Hospital, Inc. grant title Amish Midwifery Care
Pregnancy Care Management Standardized Plan Working together to improve the health of mothers and babies.
 Working together to improve the health of mothers and babies. The Pregnancy Care Management outlines methods and standards for pregnancy care managers to follow, working together with Pregnancy Medical
Working together to improve the health of mothers and babies. The Pregnancy Care Management outlines methods and standards for pregnancy care managers to follow, working together with Pregnancy Medical
CDC National Survey of Maternity Practices in Infant Nutrition and Care (mpinc)
 OMB #0920-0743 EXP. DATE: 10/31/2010 CDC National Survey of Maternity Practices in Infant Nutrition and Care (mpinc) Hospital Survey Conducted for Centers for Disease Control and Prevention National Center
OMB #0920-0743 EXP. DATE: 10/31/2010 CDC National Survey of Maternity Practices in Infant Nutrition and Care (mpinc) Hospital Survey Conducted for Centers for Disease Control and Prevention National Center
Early Childhood Indicators Report
 2015 Early Childhood Indicators Report Carol Prentice, Prentice Consulting, 2012 Updated by Alaska Department of Health & Social Services, September 2013 Updated by Prentice Consulting, July 2015 Early
2015 Early Childhood Indicators Report Carol Prentice, Prentice Consulting, 2012 Updated by Alaska Department of Health & Social Services, September 2013 Updated by Prentice Consulting, July 2015 Early
State of Illinois Department of Human Services
 State of Illinois Department of Human Services Bruce Rauner, Governor James T. Dimas, Secretary 100 South Grand Avenue, East Springfield, Illinois 62762 401 South Clinton Street Chicago, Illinois 60607
State of Illinois Department of Human Services Bruce Rauner, Governor James T. Dimas, Secretary 100 South Grand Avenue, East Springfield, Illinois 62762 401 South Clinton Street Chicago, Illinois 60607
Public Health Services
 Public Health Services FUNCTION The functions of the Public Health Services programs are to protect and promote the health and safety of County residents. This is accomplished by monitoring health status
Public Health Services FUNCTION The functions of the Public Health Services programs are to protect and promote the health and safety of County residents. This is accomplished by monitoring health status
Iowa s Maternal Health, Child Health and Family Planning Business Plan
 Iowa s Maternal Health, Child Health and Family Planning Business Plan CHILD HEALTH Who we are... A public-private partnership that... Promotes access to regular preventive health care services for children
Iowa s Maternal Health, Child Health and Family Planning Business Plan CHILD HEALTH Who we are... A public-private partnership that... Promotes access to regular preventive health care services for children
Growth Management Requirements and Florida s Community Colleges
 Growth Management Requirements and Florida s Community Colleges Prepared for the Board of Governor s Master Plan 6C-21 Regulation Work Group by the Florida Department of Community Affairs June 11, 2008
Growth Management Requirements and Florida s Community Colleges Prepared for the Board of Governor s Master Plan 6C-21 Regulation Work Group by the Florida Department of Community Affairs June 11, 2008
Essential Hospitals VITAL DATA. Results of America s Essential Hospitals Annual Hospital Characteristics Survey, FY 2012
 Essential Hospitals VITAL DATA Results of America s Essential Hospitals Annual Hospital Characteristics Survey, FY 2012 Published: July 2014 1 ABOUT AMERICA S ESSENTIAL HOSPITALS METHODOLOGY America s
Essential Hospitals VITAL DATA Results of America s Essential Hospitals Annual Hospital Characteristics Survey, FY 2012 Published: July 2014 1 ABOUT AMERICA S ESSENTIAL HOSPITALS METHODOLOGY America s
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Save today for their tomorrow. ENROLLMENT KIT 2012 2013
 Save today for their tomorrow. ENROLLMENT KIT 2012 2013 THERE S NO TIME LIKE THE PRESENT TO GIVE THEM A PROMISING FUTURE. In today s challenging world, having a college degree is more important than ever.
Save today for their tomorrow. ENROLLMENT KIT 2012 2013 THERE S NO TIME LIKE THE PRESENT TO GIVE THEM A PROMISING FUTURE. In today s challenging world, having a college degree is more important than ever.
Chapter 7 Acute Care Inpatient/Outpatient Hospital Services
 Chapter 7: Acute Care Inpatient/ Outpatient Hospital Services Executive Summary Description Acute care hospitals are the largest group of enrolled hospital providers. Kansas Medicaid has 144 acute care
Chapter 7: Acute Care Inpatient/ Outpatient Hospital Services Executive Summary Description Acute care hospitals are the largest group of enrolled hospital providers. Kansas Medicaid has 144 acute care
Want to know. more. about. midwives? Promoting social change through policy-based research in women s health
 Want to know more midwives? about Promoting social change through policy-based research in women s health What is a midwife? A midwife is a health care professional who provides care to women throughout
Want to know more midwives? about Promoting social change through policy-based research in women s health What is a midwife? A midwife is a health care professional who provides care to women throughout
Prenatal Stress and Complications
 What moms had to say: Prenatal Stress and Complications I think doctors or nurses or whoever should help other pregnant women understand and deal with post-partum blues, cause I'm am still struggling with
What moms had to say: Prenatal Stress and Complications I think doctors or nurses or whoever should help other pregnant women understand and deal with post-partum blues, cause I'm am still struggling with
Medicaid Presumptive Eligibility Instructions for Providers September 2015
 Medicaid Presumptive Eligibility Instructions for Providers September 2015 KC 3767 (R-7-15) 0 MEDICAID PRESUMPTIVE ELIGIBILITY PROGRAM OVERVIEW The Medicaid Presumptive Eligibility (MPE) program is one
Medicaid Presumptive Eligibility Instructions for Providers September 2015 KC 3767 (R-7-15) 0 MEDICAID PRESUMPTIVE ELIGIBILITY PROGRAM OVERVIEW The Medicaid Presumptive Eligibility (MPE) program is one
Quality Health Plans. for Individuals and Families
 Quality Health Plans for Individuals and Families It s All About You! AvMed Individual Health offers individual and family health coverage at prices you can afford. You can control the cost based on the
Quality Health Plans for Individuals and Families It s All About You! AvMed Individual Health offers individual and family health coverage at prices you can afford. You can control the cost based on the
WATCH OWCH Office of Women s and Children s Health
 WATCH OWCH Office of Women s and Children s Health 150 N. 18th Avenue, Suite 320 Phoenix, AZ 85007-3242 Telephone: (602) 364-1400 Fall 2006 COMMUNITY HEALTH GRANTS The Office of Women s and Children s
WATCH OWCH Office of Women s and Children s Health 150 N. 18th Avenue, Suite 320 Phoenix, AZ 85007-3242 Telephone: (602) 364-1400 Fall 2006 COMMUNITY HEALTH GRANTS The Office of Women s and Children s
Florida Prepaid College Plans
 Florida Prepaid College Plans Enrollment Guide 2013-2014 Save today for their tomorrow. No matter where life takes your child in the future, or what career he/she may choose, a college education is the
Florida Prepaid College Plans Enrollment Guide 2013-2014 Save today for their tomorrow. No matter where life takes your child in the future, or what career he/she may choose, a college education is the
cambodia Maternal, Newborn AND Child Health and Nutrition
 cambodia Maternal, Newborn AND Child Health and Nutrition situation Between 2000 and 2010, Cambodia has made significant progress in improving the health of its children. The infant mortality rate has
cambodia Maternal, Newborn AND Child Health and Nutrition situation Between 2000 and 2010, Cambodia has made significant progress in improving the health of its children. The infant mortality rate has
USA MEDIGAP CPR a product of State of FLORIDA Accountable Alliance/USA Senior Care Network Sorted by County/Specialty
 ALACHUA BREVARD SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA WUESTHOFF HOSPITAL 1600 SW ARCHER RD 110 LONGWOOD AVE GAINESVILLE, FL 32610 (352) 265-0111 ROCKLEDGE, FL 32955 (321) 636-2211 WUESTHOFF MEDICAL
ALACHUA BREVARD SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA WUESTHOFF HOSPITAL 1600 SW ARCHER RD 110 LONGWOOD AVE GAINESVILLE, FL 32610 (352) 265-0111 ROCKLEDGE, FL 32955 (321) 636-2211 WUESTHOFF MEDICAL
A Plan to Include Detoxification Services as a Covered Medical Assistance Benefit
 A Plan to Include Detoxification Services as a Covered Medical Assistance Benefit Alcohol and Drug Abuse Division Minnesota Department of Human Services December 2014 For more information contact: Minnesota
A Plan to Include Detoxification Services as a Covered Medical Assistance Benefit Alcohol and Drug Abuse Division Minnesota Department of Human Services December 2014 For more information contact: Minnesota
Eligibility, Enrollment, Disenrollment & Grace Period
 Section 2. Eligibility, Enrollment, Disenrollment & Grace Period Enrollment Enrollment in Ohio s Marketplace Program The Centers for Medicare and Medicaid Services (CMS) is the program which implements
Section 2. Eligibility, Enrollment, Disenrollment & Grace Period Enrollment Enrollment in Ohio s Marketplace Program The Centers for Medicare and Medicaid Services (CMS) is the program which implements
USA MEDIGAP CPR a product of State of FLORIDA Accountable Alliance/USA Senior Care Network Sorted by County/Specialty
 ALACHUA BREVARD SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA WUESTHOFF HOSPITAL 1600 SW ARCHER RD 110 LONGWOOD AVE GAINESVILLE, FL 32610 (352) 265-0111 ROCKLEDGE, FL 32955 (321) 636-2211 WUESTHOFF MEDICAL
ALACHUA BREVARD SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA WUESTHOFF HOSPITAL 1600 SW ARCHER RD 110 LONGWOOD AVE GAINESVILLE, FL 32610 (352) 265-0111 ROCKLEDGE, FL 32955 (321) 636-2211 WUESTHOFF MEDICAL
Florida Medicaid Inpatient Prospective Payment System
 Florida Medicaid Inpatient Prospective Payment System Justin Senior Deputy Secretary for Medicaid, Agency for Health Care Administration Malcolm Ferguson Associate Director, Navigant Healthcare Senate
Florida Medicaid Inpatient Prospective Payment System Justin Senior Deputy Secretary for Medicaid, Agency for Health Care Administration Malcolm Ferguson Associate Director, Navigant Healthcare Senate
Hospice Demographic and Outcome Measures
 RICK SCOTT GOVERNOR CHARLES T. CORLEY SECRETARY 2012 REPORT Hospice Demographic and Outcome Measures elderaffairs.state.fl.us 1 Bureau of Planning & Evaluation, September 2012 Revised February 2013 Table
RICK SCOTT GOVERNOR CHARLES T. CORLEY SECRETARY 2012 REPORT Hospice Demographic and Outcome Measures elderaffairs.state.fl.us 1 Bureau of Planning & Evaluation, September 2012 Revised February 2013 Table
What s In The Proposed FY 2017 Budget For Health Care?
 An Affiliate of the Center on Budget and Policy Priorities 820 First Street NE, Suite 460 Washington, DC 20002 (202) 408-1080 Fax (202) 408-1073 www.dcfpi.org What s In The Proposed FY 2017 Budget For
An Affiliate of the Center on Budget and Policy Priorities 820 First Street NE, Suite 460 Washington, DC 20002 (202) 408-1080 Fax (202) 408-1073 www.dcfpi.org What s In The Proposed FY 2017 Budget For
