The Present On Admission Indicator. James S. Kennedy MD, CCS, CDIP
|
|
|
- Wendy Ramsey
- 10 years ago
- Views:
Transcription
1 The Present On Admission Indicator James S. Kennedy MD, CCS, CDIP
2 James S. Kennedy MD, CCS, CDIP President, CDIMD.COM Engaged in Clinical Documentation Integrity Physician Champion Services Physician/CDS/coder education, training, and process development Interim Physician Advisor services Education and Certifications Medical School University of Tennessee, Memphis, 1979 Board Certified Internal Medicine, 1983 AHIMA CCS Certification 2001 Publications 2007 AHIMA Severity Adjusted DRGs, an MS DRG Primer 2009 ACDIS Physician Query Handbook 2014 HcPRO Physician Advisory Handbook Ongoing Minute for the Medical Staff in HcPRO s Medical Records Briefings Multiple lectures at client hospitals Contact 200 Spirit Hill Circle, Suite A 1 Smyrna, Tennessee (615) Office (615) Cellular [email protected] 2
3 Goals Describe the ICD 9 CM and ICD 10 Present On Admission and its role in measuring quality Explores different applications of the POA Indicator, such as: Hospital acquired conditions (HACs) AHRQ s Patient Safety Indicators (PSIs) Others, such as the 3M Potentially Preventable Complications Develop compliant concurrent and retrospective documentation and query strategies conducive to accurate PSI assignment 3
4 The Present On Admission Indicator What Is It? The Present On Admission (POA) indicator is a data element on the inpatient UB 04 (paper) or the ASC X12N 837, version 5010, (electronic) formats reporting if condition reported using ICD 9 CM was present at the time that the inpatient order was written. 4
5 POA Indicator Requirement to Report Since January 1, 2008, all hospitals receiving Medicare IPPS payments and all hospitals in the state of Maryland (including critical access) While Medicare exempts certain facilities (such as critical access hospitals), POA submission is required for all facilities (including critical access hospitals) by BCBSND North Dakota Medicaid (including Indian Health Service) Wellmark BCBS (South Dakota) Minnesota Medicaid 5
6 What ICD 9 CM or ICD 10 CM Codes require the POA Indicator? All ICD 9 CM or ICD 10 CM codes (including ICD 9 CM E codes ) require the POA Indicator unless they are on the exempt list. A list of these are available in the ICD 9 CM or ICD 10 CM Official Guidelines for Coding and Reporting 6
7 Examples of Exempt ICD 10 CM Codes B90 B94, Sequelae of infectious and parasitic diseases E64, Sequelae of malnutrition and other nutritional deficiencies I25.2, Old myocardial infarction I69, Sequelae of cerebrovascular disease O09, Supervision of high risk pregnancy O66.5, Attempted application of vacuum extractor and forceps O80, Encounter for full term uncomplicated delivery O94, Sequelae of complication of pregnancy, childbirth, and the puerperium P00, Newborn (suspected to be) affected by maternal conditions that may be unrelated to present pregnancy Q00 Q99, Congenital malformations, deformations and chromosomal abnormalities S00 T88.9, Injury, poisoning and certain other consequences of external causes with 7th character representing subsequent encounter or sequela Obtain a complete list from the ICD 9 CM or ICD 10 CM Official Guidelines 7
8 Examples of Exempt ICD 10 CM Codes V00 V09, Pedestrian injured in transport accident Except V00.81, Accident with wheelchair (powered) V00.83, Accident with motorized mobility scooter V10 V19, Pedal cycle rider injured in transport accident V20 V29, Motorcycle rider injured in transport accident V30 V39, Occupant of threewheeled motor vehicle injured in transport accident V40 V49, Car occupant injured in transport accident V50 V59, Occupant of pick up truck or van injured in transport accident V60 V69, Occupant of heavy transport vehicle injured in transport accident V70 V79, Bus occupant injured in transport accident V80 V89, Other land transport accidents Obtain a complete list from the ICD 9 CM or ICD 10 CM Official Guidelines 8
9 Special Caution About E Codes CMS Statement Similar to ICD 9 CM, there is no national requirement for mandatory ICD 10 CM external cause code reporting. Unless you are subject to a State based external cause code reporting mandate or these codes are required by a particular payer, you are not required to report ICD 10 CM codes found in Chapter 20 of the ICD 10 CM, External Causes of Morbidity. If you have not been reporting ICD 9 CM external cause codes, you will not be required to report ICD 10 CM codes found in Chapter 20 unless a new State or payer based requirement about the reporting of these codes is instituted. If such a requirement is instituted, it would be independent of ICD 10 CM implementation. In the absence of a mandatory reporting requirement, you are encouraged to voluntarily report external cause codes, as they provide valuable data for injury research and evaluation of injury prevention strategies. 10QuickRefer.pdf 9
10 Provider Preventable Procedures CMS and ND Medicaid identifies the following provider preventable procedures for nonpayment: E876.5 Performance of wrong operation (procedure) on correct patient (existing code) E876.6 Performance of operation (procedure) on patient not scheduled for surgery E876.7 Performance of correct operation As we will see later, other E codes for which the POA indicator is applied can affect quality measures (procedure) on wrong side/body part While E codes are not mandatory, failure to report these codes and their POA indicator is reckless disregard of CMS and ND payer rules 10
11 POA Options Y Diagnosis was present at time of IP admission N Diagnosis was not present at time of IP admission. U Documentation insufficient to determine if condition was present at the time of IP admission Interpreted for payment purposes as a No by CMS W Clinically undetermined. Provider unable to clinically determine whether the condition was present at the time of inpatient admission. Interpreted for payment purposes as a Yes by CMS If the code is POA Exempt, the field is left blank Do NOT use a 1 as was used with the
12 Timing of the Inpatient Admission The Inpatient Order Uniform Hospital Discharge Data Set Admission date Month, day, and year. Clarification is added to this data item to note that for emergency and observation type patients, the time of admission is guided by the time that the physician gives the order to admit the patient as an inpatient. 12
13 Why the POA Indicator is Critical CMS Hospital Acquired Conditions On February 8, 2006, the President signed the Deficit Reduction Act (DRA) of Section 5001(c) of DRA requires the identification of conditions that are: High cost or high volume or both; Result in the assignment of a case to a Diagnosis Related Group (DRG) that has a higher payment when present as a secondary diagnosis; and Could reasonably have been prevented through the application of evidence based guidelines. Section 5001(c) provides that CMS can revise the list of conditions from time to time, as long as it contains at least two conditions. For discharges occurring on or after October 1, 2008, hospitals will not receive additional payment for cases in which one of the selected conditions was not present on admission. That is, the case would be paid as though the secondary diagnosis were not present. 13
14 MS DRG Options CCs and MCCs MS DRG MDC TYPE MS DRG Title Weight RESPIRATORY INFECTIONS & INFLAMMATIONS MED W MCC RESPIRATORY INFECTIONS & INFLAMMATIONS MED W CC RESPIRATORY INFECTIONS & INFLAMMATIONS MED W/O CC/MCC Payment Base = $7000 Geometric Mean LOS $13, $9, $6, MED SIMPLE PNEUMONIA & PLEURISY W MCC $10, MED SIMPLE PNEUMONIA & PLEURISY W CC $6, MED SIMPLE PNEUMONIA & PLEURISY W/O CC/MCC $4, Diagnosis Related Group methodology CC = Comorbidity/Complication; MCC = Major CC Relative weight x base rate = Payment If a CMS designated condition qualifies as a HAC and the POA status is N or U, then it does not qualify as a CC or MCC
15 CMS Hospital Acquired Conditions ICD 10 Diagnosis Code & POA Based Foreign object retained after surgery Air embolism Blood incompatibility Stage III and IV pressure ulcers Falls and trauma Fractures Dislocations Intracranial injuries Crushing injuries Burns Other injuries Manifestations of poor glycemic control Diabetic ketoacidosis Nonketotic hyperosmolar coma Hypoglycemic coma Secondary diabetes with ketoacidosis Secondary diabetes with hyperosmolarity Iatrogenic pneumothorax w/venous catheterization Catheter associated urinary tract infection (UTI) Vascular catheter associated infection Surgical site infection, mediastinitis, following CABG Surgical site infection following bariatric surgery for obesity Laparoscopic gastric bypass Gastroenterostomy Laparoscopic gastric restrictive surgery Surgical site infection following certain orthopedic procedures: Spine Neck Shoulder Elbow Surgical site infection following cardiac implantable electronic device (CIED) DVT or PE following certain orthopedic procedures: Total knee replacement Hip replacement
16 North Dakota Medicaid HACs Effective March 1, 2012, North Dakota Medicaid will be implementing HAC standards that mirror Medicare guidelines and will required all IPPS hospitals to submit claims with the POA indicator. The ten hospital acquired conditions include: foreign object retained after surgery, air embolism, blood incompatibility, pressure ulcer stages III and IV, falls and trauma, catheter associated urinary tract infection (UTI), vascular catheter associated infection, manifestations of poor glycemic control, deep vein thrombosis/pulmonary embolism, and surgical site infections. When a HAC is not present on admission, but is reported as a diagnosis associated with the hospitalization, the Medicaid payment under the IPPS to the hospital may be reduced to reflect that the condition was hospital acquired. If the HAC was present on admission, the Medicaid payment under IPPS to the hospital would not be reduced. If applicable, North Dakota Medical Services will be changing the payment based on the POA indicator during a retro review of claims. If you have questions on the above mentioned matter, please contact North Dakota Medical Services to speak with a Medical Coding Specialist at
17 POA Options Y Diagnosis was present at time of IP admission N Diagnosis was not present at time of IP admission. U Documentation insufficient to determine if condition was present at the time of IP admission Interpreted for payment purposes as a No by CMS W Clinically undetermined. Provider unable to clinically determine whether the condition was present at the time of inpatient admission. Interpreted for payment purposes as a Yes by CMS If the code is POA Exempt, the field is left blank Do NOT use a 1 as was used with the
18 Timing of the Inpatient Admission The Inpatient Order Uniform Hospital Discharge Data Set Admission date Month, day, and year. Clarification is added to this data item to note that for emergency and observation type patients, the time of admission is guided by the time that the physician gives the order to admit the patient as an inpatient. 18
19 Caveats in POA Reporting ICD 9 CM Pressure Ulcers Coding Clinic, 4 th Quarter, 2008, page 19. Question: A patient is admitted to the hospital with a stage II pressure ulcer of the heel. During the hospitalization, the pressure ulcer worsens and becomes a stage III. Based on the new Official Coding Guidelines, we would be assigning the code for the highest stage for that site. What would be the correct POA indicator assignment for the stage III code? Answer: Assign "Y" to the pressure ulcer stage III code since this code is referring to a pressure ulcer that was present on admission rather than a new ulcer. 19
20 Caveats in POA Reporting ICD 9 CM Pressure Ulcers Question: A patient on admission has a pressure ulcer of her ankle due to a previously placed internal fixation device. Over several days, it was noted that the ulcer further deteriorated to stage 4. Later in the stay the patient developed another pressure ulcer in the sacrum, Because of the patient s debilitated state, the sacral ulcer progressed to stage 4. The POA indicators for the sacral decubitus and stage 4 are N. However, the POA indicators for the stage 4 ankle ulcer are both Y. How is the POA indicator captured for stage 4 pressure ulcers of different sites? Answer: Report the POA indicator N for the ulcer stage. There is no ideal answer for this situation; however, due to the constraints of the classification, this is the most appropriate approach. The Official Guidelines for Coding and Reporting indicate that ICD 9 CM diagnosis codes may not be reported twice on the same admission. This problem will be addressed with ICD 10 CM, since information about the site and stage is included in a single code. Coding Clinic, Second Quarter 2010 Pages:
21 Diagnostic Criteria For DKA and Hyperosmolar State Mild (plasma glucose >250 mg/dl) DKA Moderate (plasma glucose >250 mg/dl) Severe (plasma glucose >250 mg/dl) HHS Plasma glucose >600 mg/dl Arterial ph to <7.24 <7.00 >7.30 Serum bicarbonate to <15 <10 >18 (meq/l) Urine ketone * Positive Positive Positive Small Serum ketone * Positive Positive Positive Small Effective serum osmolality Variable Variable Variable >320 mosm/kg Anion gap >10 >12 >12 Variable Mental status Alert Alert/drowsy Stupor/coma Stupor/coma Diabetes Care July 2009, vol. 32 no. 7,
22 Iatrogenic Pneumothorax with Venous Catheterization Qualifying Diagnoses and Procedure Iatrogenic pneumothorax (CC) Venous catheterization NEC Caveats Coding Clinic, First Quarter 2011 Page: 14 If a physician documents iatrogenic pneumothorax or the pneumothorax was due to a procedure, the coder must code Coding Clinic, Third Quarter 2003 Page: 19 Since pneumothorax is a known risk associated with most thoracic surgeries, it would be inappropriate to assign an additional code for the iatrogenic pneumothorax, based on an x ray finding alone, without physician concurrence. 22
23 Definition of a Complication in Coding Clinic It is important to note that not all conditions that occur during or following surgery are classified as complications. First, there must be more than a routinely expected condition or occurrence, and There must be a cause and effect relationship between the care provided and the condition, and Differentiation between surgical/pharmaceutical care and diseases There is indication in the documentation that it is a complication. The coder cannot make the determination whether something that occurred during surgery is a complication or an expected outcome. Only a physician can diagnose a condition, and the physician must explicitly document whether the condition is a complication. If it is not clearly documented, the coder should query the physician for clarification. Source: Coding Clinic, First Quarter 2011 Pages:
24 ICD 9 CM ICD 10 CM 24
25 Medicare Public Reporting Hospital_Name AHRQ_PSI_90_Score Total_HAC_Score ST ALEXIUS MEDICAL CENTER TRINITY HOSPITALS SANFORD HEALTH SYSTEM SANFORD MEDICAL CENTER BISMARCK ALTRU HOSPITAL P H S INDIAN HOSP AT BELCOURT QUENTIN N BURDICK 7 7 STANDING ROCK INDIAN HEALTH SERVICE HOSPITAL Not Available Not Available ESSENTIA HEALTH compare Accessed 2/25/
26 PSI 12 and PSI 15 Hospital Name ST ALEXIUS MEDICAL CENTER TRINITY HOSPITALS SANFORD MEDICAL CENTER FARGO SANFORD MEDICAL CENTER BISMARCK ALTRU HOSPITAL P H S INDIAN HOSP AT BELCOURT QUENTIN N BURDICK ESSENTIA HEALTH FARGO PSI_12_POSTOP_ PULMEMB_DVT No Different than the National Rate No Different than the National Rate Better than the National Rate No Different than the National Rate Better than the National Rate NA Better than the National Rate PSI_15_ACC_LAC No Different than the National Rate Worse than the National Rate No Different than the National Rate No Different than the National Rate Worse than the National Rate No Different than the National Rate Worse than the National Rate 26
27 What are AHRQ PSIs? The Patient Safety Indicators (PSIs) are a set of indicators providing information on potential in hospital complications and adverse events following surgeries, procedures, and childbirth. The PSIs were developed after a comprehensive literature review, analysis of ICD 9 CM codes, review by a clinician panel, implementation of risk adjustment, and empirical analyses. Pediatric measures are also in place 27
28 NQF approved PSI 90 Composite PSIs 28
29 PSI Intended Uses Help hospitals identify potential adverse events that might need further study; Provide the opportunity to assess the incidence of adverse events and in hospital complications using administrative data found in the typical discharge record; Include indicators for complications occurring in hospital that may represent patient safety events Includes area level analogs designed to detect patient safety events on a regional level 29
30 PSI Methodology PSIs are based ONLY on ICD 9 CM codes and other elements of the UB 04 (e.g. procedure dates, patient age) No clinical abstraction is performed like on does for the NCDR, STS, or other clinical databases The key to getting PSIs right is to know how there are constructed, ascertain that provider documentation is congruent with the patient s clinical circumstances and follows ICD 9 CM rules, guidelines, and official advice 30
31 31
32 When all else fails, read the directions 32
33 Accidental Lacerations 33
34 PSI 15 Criteria 34
35 PSI 15 Criteria Exclusions 35
36 Coding Clinic for ICD 9 CM 2 nd Quarter, 2013, pages Clarification on the use of external cause and unspecified codes in ICD 10 CM The following statement was approved and posted by the four Cooperating Parties in May 2013 and is now reproduced in its entirety. External Cause Codes Just as with ICD 9 CM, there is no national requirement for mandatory ICD 10 CM external cause code reporting. Unless a provider is subject to a state based external cause code reporting mandate or these codes are required by a particular payer, reporting of ICD 10 CM codes in Chapter 20, External Causes of Morbidity, is not required. If a provider has not been reporting ICD 9 CM external cause codes, the provider will not be required to report ICD 10 CM codes in Chapter 20, unless a new state or payer based requirement regarding the reporting of these codes is instituted. Such a requirement would be independent of ICD 10 CM implementation. In the absence of a mandatory reporting requirement, providers are encouraged to voluntarily report external cause codes, as they provide valuable data for injury research and evaluation of injury prevention strategies. 36
37 37
38 E code use In the course of a gastroscopy, the physician s scope causes a esophageal varices to significantly bleed resulting in an acute blood loss anemia, which the physician stated was a complication of the procedure 38
39 998.2 Index to Diseases Examples Complications accidental puncture or laceration during a procedure mechanical catheter NEC during a procedure Perforation, perforative (nontraumatic) by instrument (any) during a procedure, accidental Injury blood vessel NEC due to accidental puncture or laceration during procedure instrumental (during surgery) Paralysis, paralytic (complete) (incomplete) diaphragm (flaccid) due to accidental section of phrenic nerve during procedure
40
41 Accidental Lacerations During Surgery Coding Clinic, 2nd Quarter 2007, pp Question: During an procedure, the surgeon noted, a small capsular injury of the spleen, which was hemostatic. This injury did not require repair. An esophagogastroduodenscopy (EGD) was then performed for evaluation of the distal esophagus since the mass had adhered at the gastroesophageal junction. The EGD revealed a serosal injury to the stomach, which was repaired with interrupted Lembert sutures. The surgeon did not include the intraoperative tears in the diagnostic statement. What are the appropriate code assignments? 41
42 Coding Clinic Answer Answer: Query the provider, and if the provider states the tear is not clinically significant, omit codes for both the diagnosis and procedure. When a tear is documented in the operative report, such as a small serosal tear of the stomach, the surgeon should be queried as to whether the small tear was an incidental occurrence inherent in the surgical procedure or whether the tear should be considered by the physician to be a complication of the procedure. If the provider documents that the seromuscular tear is a complication of the surgery, assign code 998.2, Accidental puncture or laceration during a procedure, as an additional diagnosis. This advice is consistent with that previously published in Coding Clinic, 3 rd Quarter 1990, p
43 A Compliant Complications Query 2013 ACDIS AHIMA Practice Brief Clinical scenario: During the removal of an abdominal mass, the surgeon documents, in the description of the operative procedure, a serosal injury to the stomach was repaired with interrupted sutures. Query: In the description of the operative procedure a serosal injury to the stomach was noted and repaired with interrupted sutures. Was this serosal injury and repair: A complication of the procedure Integral to the above procedure Not clinically significant Other Clinically Undetermined Please document your response in the health record or below accompanied by clinical substantiation. Rationale: This is an example of a query necessary to determine the clinical significance of a condition resulting from a procedure. 43
44 Review of the ICD 10 CM Guidelines For POA Reporting POA indicator is assigned to principal and secondary diagnoses (as defined in Section II of the Official Guidelines for Coding and Reporting) and the external cause of injury codes. Issues related to inconsistent, missing, conflicting or unclear documentation must still be resolved by the provider. If a condition would not be coded and reported based on UHDDS definitions and current official coding guidelines, then the POA indicator would not be reported. 44
45 Timeframes For Reporting There is no required timeframe as to when a provider (per the definition of provider used in these guidelines) must identify or document a condition to be present on admission. In some clinical situations, it may not be possible for a provider to make a definitive diagnosis (or a condition may not be recognized or reported by the patient) for a period of time after admission. In some cases it may be several days before the provider arrives at a definitive diagnosis. This does not mean that the condition was not present on admission. Determination of whether the condition was present on admission or not will be based on the applicable POA guideline as identified in this document, or on the provider s best clinical judgment. 45
46 ICD 10 CM Official Guidelines Assigning Y to the POA Status Any condition the provider explicitly documents as being present on admission. Assign N for any condition the provider explicitly documents as not present at the time of admission. Conditions that were diagnosed prior to admission (example: hypertension, diabetes mellitus, asthma) 46
47 ICD 10 CM Official Guidelines Assigning Y to the POA Status Conditions diagnosed during the admission that were clearly present but not diagnosed until after admission occurred. Diagnoses subsequently confirmed after admission are considered present on admission if at the time of admission they are documented as suspected, possible, rule out, differential diagnosis, or Diagnoses that constitute an underlying cause of a symptom that is present at the time of admission. A condition that develops during an outpatient encounter prior to a written order for inpatient admission. 47
48 ICD 10 CM Official Guidelines Assigning Y to the POA Status Congenital conditions and anomalies Assign Y for congenital conditions and anomalies except for categories Q00 Q99, Congenital anomalies, which are on the exempt list. Congenital conditions are always considered present on admission. 48
49 ICD 10 CM Official Guidelines Acute and Chronic Conditions Assign Y for acute conditions that are present at time of admission and N for acute conditions that are not present at time of admission. Assign Y for chronic conditions, even though the condition may not be diagnosed until after admission. If a single code identifies both an acute and chronic condition, see the POA guidelines for combination codes. 49
50 Coding Clinic For ICD 10 CM Progression of A Disease Question: The patient was admitted with acute respiratory failure, acute kidney injury due to acute tubular necrosis and chronic kidney disease, stage 3. The patient had a prolonged hospitalization and during the hospital course, he advanced to end stage renal disease (ESRD) and was started on hemodialysis. The provider stated, Concerning possible renal recovery, it appears unlikely he will ever be dialysis independent given his history of CKD prior to his acute on chronic kidney injury and also because he is almost three months from his initial renal insult with no signs of renal recovery. Since the chronic kidney disease, stage 3 had progressed to ESRD, requiring dialysis, what is the appropriate present on admission (POA) indicator for the ESRD? Answer: Assign POA indicator Y, for the ESRD. The patient experienced deterioration or worsening of the same condition. Even though chronic kidney disease stage 3 and ESRD are assigned different codes, only one code is reported for the highest or most severe stage. This advice is similar to that previously published in Coding Clinic, First Quarter 2009, page 19, regarding a deteriorating pressure ulcer Coding Clinic, First Quarter 2013 Page: 18 50
51 ICD 10 CM Official Guidelines Uncertain Diagnoses Conditions documented as possible, probable, suspected, or rule out at the time of discharge If the final diagnosis contains a possible, probable, suspected, or rule out diagnosis, and this diagnosis was based on signs, symptoms or clinical findings suspected at the time of inpatient admission, assign Y. If the final diagnosis contains a possible, probable, suspected, or rule out diagnosis, and this diagnosis was based on signs, symptoms or clinical findings that were not present on admission, assign N. 51
52 ICD 10 CM Official Guidelines Impending or Threatened Conditions Conditions documented as impending or threatened at the time of discharge If the final diagnosis contains an impending or threatened diagnosis, and this diagnosis is based on symptoms or clinical findings that were present on admission, assign Y. If the final diagnosis contains an impending or threatened diagnosis, and this diagnosis is based on symptoms or clinical findings that were not present on admission, assign N. 52
53 ICD 10 CM Official Guidelines External Cause of Injury Codes Assign Y for any external cause code representing an external cause of morbidity that occurred prior to inpatient admission (e.g., patient fell out of bed at home, patient fell out of bed in emergency room prior to admission) Assign N for any external cause code representing an external cause of morbidity that occurred during inpatient hospitalization (e.g., patient fell out of hospital bed during hospital stay, patient experienced an adverse reaction to a medication administered after inpatient admission) 53
54 ICD 10 CM Official Guidelines Combination Codes Assign N if any part of the combination code was not present on admission (e.g., COPD with acute exacerbation and the exacerbation was not present on admission; gastric ulcer that does not start bleeding until after admission; asthma patient develops status asthmaticus after admission) Assign Y if all parts of the combination code were present on admission (e.g., patient with acute prostatitis admitted with hematuria ) 54
55 ICD 10 CM Official Guidelines Same Diagnosis 2 or More Conditions When the same ICD 10 CM diagnosis code applies to two or more conditions during the same encounter (e.g. two separate conditions classified to the same ICD 10 CM diagnosis code): Assign Y if all conditions represented by the single ICD 10 CM code were present on admission (e.g. bilateral unspecified age related cataracts). Assign N if any of the conditions represented by the single ICD 10 CM code was not present on admission (e.g. traumatic secondary and recurrent hemorrhage and seroma is assigned to a single code T79.2, but only one of the conditions was present on admission). 55
56 ICD 10 CM Official Guidelines Obstetrics Whether or not the patient delivers during the current hospitalization does not affect assignment of the POA indicator. The determining factor for POA assignment is whether the pregnancy complication or obstetrical condition described by the code was present at the time of admission or not. If the pregnancy complication or obstetrical condition was present on admission (e.g., patient admitted in preterm labor), assign Y. If the pregnancy complication or obstetrical condition was not present on admission (e.g., 2nd degree laceration during delivery, postpartum hemorrhage that occurred during current hospitalization, fetal distress develops after admission), assign N. If the obstetrical code includes more than one diagnosis and any of the diagnoses identified by the code were not present on admission assign N. (e.g., Category O11, Pre existing hypertension with preeclampsia) 56
57 ICD 10 CM Official Guidelines Perinatal Conditions Newborns are not considered to be admitted until after birth. Therefore, any condition present at birth or that developed in utero is considered present at admission and should be assigned Y. This includes conditions that occur during delivery (e.g., injury during delivery, meconium aspiration, exposure to streptococcus B in the vaginal canal). 57
58 ICD 10 CM Official Guidelines Uncertain vs. Clinically Undetermined Documentation does not indicate whether condition was present on admission Assign U when the medical record documentation is unclear as to whether the condition was present on admission. U should not be routinely assigned and used only in very limited circumstances. Coders are encouraged to query the providers when the documentation is unclear. Documentation states that it cannot be determined whether the condition was or was not present on admission Assign W when the medical record documentation indicates that it cannot be clinically determined whether or not the condition was present on admission. 58
59 CDI Foundations Responsibilities Physician/provider Definition of diagnostic or therapeutic terminology Diagnosis/Description of patient conditions or description of treatments Documentation in the medical record Everyone Defense when held accountable by outside entities Clinical documentation, ancillary, and coding staff (Facility) Deciphering inconsistent, incomplete, imprecise, unreliable, conflicting, or illegible documentation and clarifying it prior to claim submission Delineation of documented diagnoses or treatments in the context of the patient s conditions and treatments within the limitations of HIPAAassociated transaction sets Deployment of ICD 9 CM and CPT/HCPCS (outpatient) codes based upon physician/provider documentation 59
60 2008 Version 60
61 2008 AHIMA Query Practice Brief In general, query forms should not be designed to ask questions about a diagnosis or procedure that can be responded to in a yes/no fashion. The exception is present on admission (POA) queries when the diagnosis has already been documented. The problem with this is that a No answer does not allow for the option of Clinically Undetermined 61
62 2008 AHIMA Query Practice Brief Multiple choice formats that employ checkboxes may be used as long as all clinically reasonable choices are listed, regardless of the impact on reimbursement or quality reporting. The choices should also include an other option, with a line that allows the provider to add free text. Providers should also be given the choice of unable to determine. This format is designed to make multiple choice questions as open ended as possible. 62
63 Sample POA Query 63
64 Summary POA status is important POA status is required POA status reflects the quality of our care POA status is ultimately the responsibility of the physician and coder with support by the CDI process POA status is something we can do 64
65 65
66 66
67 Thank You! Contact information James S. Kennedy MD CCS (615) or (615)
Present on Admission Reporting Guidelines
 Introduction Present on Admission Reporting Guidelines These guidelines are to be used as a supplement to the ICD-9-CM Official Guidelines for Coding and Reporting to facilitate the assignment of the Present
Introduction Present on Admission Reporting Guidelines These guidelines are to be used as a supplement to the ICD-9-CM Official Guidelines for Coding and Reporting to facilitate the assignment of the Present
CMS Progress Toward Implementing Value-Based Purchasing
 Centers for Medicare & Medicaid Services CMS Progress Toward Implementing Value-Based Purchasing Thomas B. Valuck, MD, JD Medical Officer & Senior Adviser Center for Medicare Management Presentation Overview
Centers for Medicare & Medicaid Services CMS Progress Toward Implementing Value-Based Purchasing Thomas B. Valuck, MD, JD Medical Officer & Senior Adviser Center for Medicare Management Presentation Overview
CMS Progress Toward Implementing Value-Based Purchasing
 Centers for Medicare & Medicaid Services CMS Progress Toward Implementing Value-Based Purchasing Lisa Grabert, MPH Health Insurance Specialist Hospital & Ambulatory Policy Group Presentation Overview CMS
Centers for Medicare & Medicaid Services CMS Progress Toward Implementing Value-Based Purchasing Lisa Grabert, MPH Health Insurance Specialist Hospital & Ambulatory Policy Group Presentation Overview CMS
HOSPITAL-ACQUIRED CONDITION PAYMENT POLICY
 Health Care Purchaser Toolkit: HOSPITAL-ACQUIRED CONDITION PAYMENT POLICY August 2009 Developed for NBCH by: Developed with support from: www.discernconsulting.com 410-542-4470 Health Care Purchaser Toolkit:
Health Care Purchaser Toolkit: HOSPITAL-ACQUIRED CONDITION PAYMENT POLICY August 2009 Developed for NBCH by: Developed with support from: www.discernconsulting.com 410-542-4470 Health Care Purchaser Toolkit:
Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium
 Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium October 30, 2008 Barry Libman, RHIA, CCS, CCS-P President, Barry Libman Inc. Stroke Coding Issues Outline Medical record documentation
Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium October 30, 2008 Barry Libman, RHIA, CCS, CCS-P President, Barry Libman Inc. Stroke Coding Issues Outline Medical record documentation
Creating a Hybrid Database by Adding a POA Modifier and Numerical Laboratory Results to Administrative Claims Data
 Creating a Hybrid Database by Adding a POA Modifier and Numerical Laboratory Results to Administrative Claims Data Michael Pine, M.D., M.B.A. Michael Pine and Associates, Inc. [email protected] Overview
Creating a Hybrid Database by Adding a POA Modifier and Numerical Laboratory Results to Administrative Claims Data Michael Pine, M.D., M.B.A. Michael Pine and Associates, Inc. [email protected] Overview
Certified Clinical Documentation Specialist Examination Content Outline - 2016
 Certified Clinical Documentation Specialist Examination Content Outline - 2016 1. Healthcare Regulations, Reimbursement, and Documentation Requirements Related to the Inpatient Prospective Payment System
Certified Clinical Documentation Specialist Examination Content Outline - 2016 1. Healthcare Regulations, Reimbursement, and Documentation Requirements Related to the Inpatient Prospective Payment System
Cognos Web-based Analytic Tool Overview
 Cognos Web-based Analytic Tool Overview Market, Quality and Physician Data Analysis with Drill-thru Feature Mari Tietze, PhD, RN-BC Director, Nursing Research and Informatics DFWHC ERF 2009 1 UB-04 Source
Cognos Web-based Analytic Tool Overview Market, Quality and Physician Data Analysis with Drill-thru Feature Mari Tietze, PhD, RN-BC Director, Nursing Research and Informatics DFWHC ERF 2009 1 UB-04 Source
The ICD-9-CM uses an indented format for ease in reference I10 I10 I10 I10. All information subject to change. 2013 1
 Section I. Conventions, general coding guidelines and chapter specific guidelines The conventions, general guidelines and chapter-specific guidelines are applicable to all health care settings unless otherwise
Section I. Conventions, general coding guidelines and chapter specific guidelines The conventions, general guidelines and chapter-specific guidelines are applicable to all health care settings unless otherwise
The Official Guidelines for coding and reporting using ICD-9-CM
 Reporting Accurate Codes In the Era of Recovery Audit Contractor Reviews Sue Roehl, RHIT, CCS The Official Guidelines for coding and reporting using ICD-9-CM A set of rules that have been developed to
Reporting Accurate Codes In the Era of Recovery Audit Contractor Reviews Sue Roehl, RHIT, CCS The Official Guidelines for coding and reporting using ICD-9-CM A set of rules that have been developed to
FAQ for Coding Encounters in ICD 10 CM
 FAQ for Coding Encounters in ICD 10 CM Topics: Encounter for Routine Health Exams Encounter for Vaccines Follow Up Encounters Coding for Injuries Encounter for Suture Removal External Cause Codes Tobacco
FAQ for Coding Encounters in ICD 10 CM Topics: Encounter for Routine Health Exams Encounter for Vaccines Follow Up Encounters Coding for Injuries Encounter for Suture Removal External Cause Codes Tobacco
ICD-10... What Are You Waiting For?
 ICD-10... What Are You Waiting For? What is it? International classification for all general epidemiological, many health management purposes, and clinical use Published by the World Health Organization
ICD-10... What Are You Waiting For? What is it? International classification for all general epidemiological, many health management purposes, and clinical use Published by the World Health Organization
How To Improve A Hospital'S Performance
 FY 16 MHAC Methodology Redesign HSCRC Performance Measurement Work Group February 20, 2014 1 Presentation Contents Background: Reason to change, guiding principles, timing Measurement Methodology Payment
FY 16 MHAC Methodology Redesign HSCRC Performance Measurement Work Group February 20, 2014 1 Presentation Contents Background: Reason to change, guiding principles, timing Measurement Methodology Payment
ICD-10-CM Official Guidelines for Coding and Reporting
 2013 Narrative changes appear in bold text Items underlined have been moved within the guidelines since the 2012 version Italics are used to indicate revisions to heading changes The Centers for Medicare
2013 Narrative changes appear in bold text Items underlined have been moved within the guidelines since the 2012 version Italics are used to indicate revisions to heading changes The Centers for Medicare
HCIM ICD-10 Training Online Course Catalog August 2015
 HCIM ICD-10 Training Online Course Catalog August 2015 Course/Content Duration Quiz Duration CME Credits Assessments: Assessment: Provider - Baseline - E/M Emergency Department 45 5/1/2015 Assessment:
HCIM ICD-10 Training Online Course Catalog August 2015 Course/Content Duration Quiz Duration CME Credits Assessments: Assessment: Provider - Baseline - E/M Emergency Department 45 5/1/2015 Assessment:
Breaking the Code: ICD-9-CM Coding in Details
 Breaking the Code: ICD-9-CM Coding in Details ICD-9-CM diagnosis codes are 3- to 5-digit codes used to describe the clinical reason for a patient s treatment. They do not describe the service performed,
Breaking the Code: ICD-9-CM Coding in Details ICD-9-CM diagnosis codes are 3- to 5-digit codes used to describe the clinical reason for a patient s treatment. They do not describe the service performed,
Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008
 Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008 Please refer to the complete ICD-9-CM Official Guidelines for Coding and Reporting posted on this
Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008 Please refer to the complete ICD-9-CM Official Guidelines for Coding and Reporting posted on this
Present on Admission Reporting
 Present on Admission Reporting Audio Seminar/Webinar February 21, 2008 Practical Tools for Seminar Learning Copyright 2008 American Health Information Management Association. All rights reserved. Disclaimer
Present on Admission Reporting Audio Seminar/Webinar February 21, 2008 Practical Tools for Seminar Learning Copyright 2008 American Health Information Management Association. All rights reserved. Disclaimer
Best of AHA Coding Clinic for ICD 10 CM. Disclaimer
 Best of AHA Coding Clinic for ICD 10 CM Wednesday, June 18, 2014 12:00 1:00pm CST Nelly Leon Chisen, RHIA, Director of Coding and Classification, AHA Anita Rapier, RHIT, CCS, Senior Coding Consultant,
Best of AHA Coding Clinic for ICD 10 CM Wednesday, June 18, 2014 12:00 1:00pm CST Nelly Leon Chisen, RHIA, Director of Coding and Classification, AHA Anita Rapier, RHIT, CCS, Senior Coding Consultant,
Description of the OECD Health Care Quality Indicators as well as indicator-specific information
 Appendix 1. Description of the OECD Health Care Quality Indicators as well as indicator-specific information The numbers after the indicator name refer to the report(s) by OECD and/or THL where the data
Appendix 1. Description of the OECD Health Care Quality Indicators as well as indicator-specific information The numbers after the indicator name refer to the report(s) by OECD and/or THL where the data
Guidelines Most Significantly Affected Under ICD-10-CM. May 29, 2013
 Guidelines Most Significantly Affected Under ICD-10-CM May 29, 2013 Guidelines Most Significantly Affected Under ICD-10-CM A look at the new system and how it compares to ICD-9-CM Presented by Therese
Guidelines Most Significantly Affected Under ICD-10-CM May 29, 2013 Guidelines Most Significantly Affected Under ICD-10-CM A look at the new system and how it compares to ICD-9-CM Presented by Therese
How Regulations Affect Coding and Documentation
 How Regulations Affect Coding and Documentation Byline Deborah Neville, RHIA, CCS-P Director Revenue Cycle, Coding and Compliance for Elsevier, Inc. INTRODUCTION Regulations, laws, mandates, and guidelines
How Regulations Affect Coding and Documentation Byline Deborah Neville, RHIA, CCS-P Director Revenue Cycle, Coding and Compliance for Elsevier, Inc. INTRODUCTION Regulations, laws, mandates, and guidelines
CMS Office of Public Affairs 202-690-6145 MEDICARE PROPOSES NEW HOSPITAL VALUE-BASED PURCHASING PROGRAM
 For Immediate Release: Friday, January 07, 2011 Contact: CMS Office of Public Affairs 202-690-6145 MEDICARE PROPOSES NEW HOSPITAL VALUE-BASED PURCHASING PROGRAM OVERVIEW: Today the Centers for Medicare
For Immediate Release: Friday, January 07, 2011 Contact: CMS Office of Public Affairs 202-690-6145 MEDICARE PROPOSES NEW HOSPITAL VALUE-BASED PURCHASING PROGRAM OVERVIEW: Today the Centers for Medicare
The Why and How of a CDI Program. Deb Neville, RHIA, CCS-P, Elsevier/MC Strategies Donna Bonno, CPC- CPC-I, QuadraMed September 12, 2012
 The Why and How of a CDI Program Deb Neville, RHIA, CCS-P, Elsevier/MC Strategies Donna Bonno, CPC- CPC-I, QuadraMed September 12, 2012 Objectives Understand the reasons behind a Clinical Documentation
The Why and How of a CDI Program Deb Neville, RHIA, CCS-P, Elsevier/MC Strategies Donna Bonno, CPC- CPC-I, QuadraMed September 12, 2012 Objectives Understand the reasons behind a Clinical Documentation
The Top 20 ICD-10 Documentation Issues That Cause DRG Changes
 7th Annual Association for Clinical Documentation Improvement Specialists Conference The Top 20 ICD-10 Documentation Issues That Cause DRG Changes Donna Smith, RHIA Project Manager, Consulting Services
7th Annual Association for Clinical Documentation Improvement Specialists Conference The Top 20 ICD-10 Documentation Issues That Cause DRG Changes Donna Smith, RHIA Project Manager, Consulting Services
ICD-9 Basics Study Guide
 Board of Medical Specialty Coding ICD-9 Basics Study Guide for the Home Health ICD-9 Basic Competencies Examination Two Washingtonian Center 9737 Washingtonian Blvd., Ste. 100 Gaithersburg, MD 20878-7364
Board of Medical Specialty Coding ICD-9 Basics Study Guide for the Home Health ICD-9 Basic Competencies Examination Two Washingtonian Center 9737 Washingtonian Blvd., Ste. 100 Gaithersburg, MD 20878-7364
Regulatory Compliance Policy No. COMP.RCC 4.71 Title:
 I. SCOPE: Regulatory Compliance Policy No. COMP.RCC 4.71 Page: 1 of 12 This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); (2)
I. SCOPE: Regulatory Compliance Policy No. COMP.RCC 4.71 Page: 1 of 12 This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); (2)
Rehabilitation Best Practice Documentation
 Rehabilitation Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Reason for Admission to Inpatient Rehab CVA Deficits Fractures Secondary
Rehabilitation Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Reason for Admission to Inpatient Rehab CVA Deficits Fractures Secondary
ICD-10 in the Provider Newsletter
 ICD-10 in the Provider Newsletter ICD-10 CM Code Structure, July 2013 ICD-10 Implementation, April 2013 ICD-10 Manual, January 2013 ICD-10 Back on Track, October 2012 ICD-10 Training, July 2012 ICD-10
ICD-10 in the Provider Newsletter ICD-10 CM Code Structure, July 2013 ICD-10 Implementation, April 2013 ICD-10 Manual, January 2013 ICD-10 Back on Track, October 2012 ICD-10 Training, July 2012 ICD-10
In the second of a quarterly series of articles available to ACDIS members,
 Coding Clinic update Conditions documented at the time of discharge, diabetes opportunities highlight important updates for CDI specialists W h i t e p a p e r Editor s note: The following article is provided
Coding Clinic update Conditions documented at the time of discharge, diabetes opportunities highlight important updates for CDI specialists W h i t e p a p e r Editor s note: The following article is provided
Healthcare Financial Management Association Southern California. Implementation of MS-DRGs. November 20, 2008
 Healthcare Financial Management Association Southern California Implementation of MS-DRGs November 20, 2008 John Valenta, CPA, MBA, Director Health Sciences Regulatory Practice Deloitte & Touche LLP Agenda
Healthcare Financial Management Association Southern California Implementation of MS-DRGs November 20, 2008 John Valenta, CPA, MBA, Director Health Sciences Regulatory Practice Deloitte & Touche LLP Agenda
CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014
 CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014 e 55 0495 2 Emergency Department (ED)- 1 Emergency Department Throughput Median time from
CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014 e 55 0495 2 Emergency Department (ED)- 1 Emergency Department Throughput Median time from
Kathryn DeVault, RHIA, CCS, CCS-P Director, HIM Solutions, AHIMA
 ICD-10-CM: Let s Code, Part II Kathryn DeVault, RHIA, CCS, CCS-P Director, HIM Solutions, AHIMA Agenda Coding questions answered Review of ICD-10-CM coding scenarios ICD-10-CM Coding Questions Coding Questions...
ICD-10-CM: Let s Code, Part II Kathryn DeVault, RHIA, CCS, CCS-P Director, HIM Solutions, AHIMA Agenda Coding questions answered Review of ICD-10-CM coding scenarios ICD-10-CM Coding Questions Coding Questions...
ICD 10 ICD 9. 14, 000 codes No laterality Limited severity parameters No placeholders 3-5 digits
 ICD 10 Conversion 1 Why Change? ICD 9 14, 000 codes No laterality Limited severity parameters No placeholders 3-5 digits 1 2 3 4 5 ICD 10 69,000+ codes Indicates Rt or Lt Extensive severity parameters
ICD 10 Conversion 1 Why Change? ICD 9 14, 000 codes No laterality Limited severity parameters No placeholders 3-5 digits 1 2 3 4 5 ICD 10 69,000+ codes Indicates Rt or Lt Extensive severity parameters
Getting Ready for ICD-10. Part 2: ICD-10 Coding
 Getting Ready for ICD-10 Part 2: ICD-10 Coding Introduction In the United States, on October 1, 2015 the ICD 9 code set used to report medical diagnoses and inpatient procedures will be replaced by International
Getting Ready for ICD-10 Part 2: ICD-10 Coding Introduction In the United States, on October 1, 2015 the ICD 9 code set used to report medical diagnoses and inpatient procedures will be replaced by International
Long term care coding issues for ICD-10-CM
 Long term care coding issues for ICD-10-CM Coding Clinic, Fourth Quarter 2012 Pages: 90-98 Effective with discharges: October 1, 2012 Related Information Long Term Care Coding Issues for ICD-10-CM Coding
Long term care coding issues for ICD-10-CM Coding Clinic, Fourth Quarter 2012 Pages: 90-98 Effective with discharges: October 1, 2012 Related Information Long Term Care Coding Issues for ICD-10-CM Coding
Using the ICD-10-CM. The Alphabetic Index helps you determine which section to refer to in the Tabular List. It does not always provide the full code.
 Using the ICD-10-CM Selecting the Correct Code To determine the correct International Classification of Diseases, 10 Edition, Clinical Modification (ICD-10-CM) code, follow these two steps: Step 1: Look
Using the ICD-10-CM Selecting the Correct Code To determine the correct International Classification of Diseases, 10 Edition, Clinical Modification (ICD-10-CM) code, follow these two steps: Step 1: Look
Importance of Revenue Cycle Continuous. Presentation Outline
 Importance of Revenue Cycle Continuous Education EHR EMR ICD-10 Presented by: Gloria Doehling, Consultant, ICD-10 SME Encore Health Resources 21 September 2012 1 Presentation Outline Definitions Best Practice
Importance of Revenue Cycle Continuous Education EHR EMR ICD-10 Presented by: Gloria Doehling, Consultant, ICD-10 SME Encore Health Resources 21 September 2012 1 Presentation Outline Definitions Best Practice
ICD-10: Navigating the Change. Presented by: Shelley Garrett, CPC, CMC, CMOM, CMIS
 ICD-10: Navigating the Change Presented by: Shelley Garrett, CPC, CMC, CMOM, CMIS A journey of a thousand miles begins with a single step -Confucius 5010 Conversion January 1, 2012 5010 Conversion Version
ICD-10: Navigating the Change Presented by: Shelley Garrett, CPC, CMC, CMOM, CMIS A journey of a thousand miles begins with a single step -Confucius 5010 Conversion January 1, 2012 5010 Conversion Version
CODE AUDITING RULES. SAMPLE Medical Policy Rationale
 CODE AUDITING RULES As part of Coventry Health Care of Missouri, Inc s commitment to improve business processes, we are implemented a new payment policy program that applies to claims processed on August
CODE AUDITING RULES As part of Coventry Health Care of Missouri, Inc s commitment to improve business processes, we are implemented a new payment policy program that applies to claims processed on August
Module 9: Diseases of the Endocrine System and Nutritional Disorders Exercises
 Module 9: Diseases of the Endocrine System and Nutritional Disorders Exercises 1. An 86 year old male with brittle Type I DM is admitted for orthopedic surgery. The physician documents in the operative
Module 9: Diseases of the Endocrine System and Nutritional Disorders Exercises 1. An 86 year old male with brittle Type I DM is admitted for orthopedic surgery. The physician documents in the operative
Billing and Coding Guidance Co-morbidities associated with morbid obesity
 Billing and Coding Guidance Co-morbidities associated with morbid obesity AMA CPT / ADA CDT / AHA NUBC Copyright Statement CPT only copyright 2002-2014 American Medical Association. All Rights Reserved.
Billing and Coding Guidance Co-morbidities associated with morbid obesity AMA CPT / ADA CDT / AHA NUBC Copyright Statement CPT only copyright 2002-2014 American Medical Association. All Rights Reserved.
Florida Center for Health Information and Policy Analysis
 Florida Center for Health Information and Policy Analysis Data Overview for the Commission on Healthcare and Hospital Funding May 20, 2015 1 Office of Data Collection and Quality Assurance Collection of
Florida Center for Health Information and Policy Analysis Data Overview for the Commission on Healthcare and Hospital Funding May 20, 2015 1 Office of Data Collection and Quality Assurance Collection of
Home Health Care ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Home Health Care and Top 20 codes
 Home Health Care ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Home Health Care and Top 20 codes Chapter 4: Endocrine, Nutritional and Metabolic Diseases (E00-E99) ICD-10-CM diabetes mellitus
Home Health Care ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Home Health Care and Top 20 codes Chapter 4: Endocrine, Nutritional and Metabolic Diseases (E00-E99) ICD-10-CM diabetes mellitus
All Patient Refined DRGs (APR-DRGs) An Overview. Presented by Treo Solutions
 All Patient Refined DRGs (APR-DRGs) An Overview Presented by Treo Solutions Presentation Highlights History of inpatient classification systems APR-DRGs: what they are, how they work, and why they are
All Patient Refined DRGs (APR-DRGs) An Overview Presented by Treo Solutions Presentation Highlights History of inpatient classification systems APR-DRGs: what they are, how they work, and why they are
PHC4 35 Diseases, Procedures, and Medical Conditions for which Laboratory Data is Required Effective 10/1/2015
 PHC4 35 Diseases, Procedures, and Medical Conditions for which Laboratory Data is Required Effective 10/1/2015 Laboratory data is to be submitted for discharges in the following conditions: 1. Heart Attack
PHC4 35 Diseases, Procedures, and Medical Conditions for which Laboratory Data is Required Effective 10/1/2015 Laboratory data is to be submitted for discharges in the following conditions: 1. Heart Attack
Hospital Inpatient Quality Reporting (IQR) Program
 Clinical Process Measures Program Changes for Fiscal Year 2014 Beginning with January 1, 2012 discharges; hospitals will begin data collection and submission for 4 new measures. Hospitals will not be required
Clinical Process Measures Program Changes for Fiscal Year 2014 Beginning with January 1, 2012 discharges; hospitals will begin data collection and submission for 4 new measures. Hospitals will not be required
ICD-10-CM Official Guidelines for Coding and Reporting FY 2016 Page 2 of 115
 Narrative changes appear in bold text Items underlined have been moved within the guidelines since the FY 2014 version Italics are used to indicate revisions to heading changes The Centers for Medicare
Narrative changes appear in bold text Items underlined have been moved within the guidelines since the FY 2014 version Italics are used to indicate revisions to heading changes The Centers for Medicare
Tony Matejicka, DO, MPH, FACP Medical Director Coding and Utilization August 20, 2012
 Tony Matejicka, DO, MPH, FACP Medical Director Coding and Utilization August 20, 2012 Understand the history of CMS to appreciate our clinical disconnect from Medicare reimbursement. Recognize terms from
Tony Matejicka, DO, MPH, FACP Medical Director Coding and Utilization August 20, 2012 Understand the history of CMS to appreciate our clinical disconnect from Medicare reimbursement. Recognize terms from
South Dakota Medicaid ICD-10 Provider Education Series
 South Dakota Medicaid ICD-10 Provider Education Series Lori Lawson, Deputy Medicaid Director, DSS Jane Beth Turner, RHIA, AHIMA ICD-10 Approved Trainer, Cognosante 1 Agenda Brief overview of transition
South Dakota Medicaid ICD-10 Provider Education Series Lori Lawson, Deputy Medicaid Director, DSS Jane Beth Turner, RHIA, AHIMA ICD-10 Approved Trainer, Cognosante 1 Agenda Brief overview of transition
Data Analysis Project Summary
 of Introduction The notion that adverse patient safety events result in excess costs is not a new concept. However, more research is needed on the actual costs of different types of adverse events at an
of Introduction The notion that adverse patient safety events result in excess costs is not a new concept. However, more research is needed on the actual costs of different types of adverse events at an
How To Report A Serious Medical Event
 SERIOUS REPORTABLE EVENTS & PROVIDER PREVENTABLE CONDITIONS Effective October 1, 2015 Policy: NHP does not reimburse services associated with serious reportable events (SRE), never events and/or Provider
SERIOUS REPORTABLE EVENTS & PROVIDER PREVENTABLE CONDITIONS Effective October 1, 2015 Policy: NHP does not reimburse services associated with serious reportable events (SRE), never events and/or Provider
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services ICD-10-CM/PCS THE NEXT GENERATION OF CODING
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services ICD-10-CM/PCS THE NEXT GENERATION OF CODING ICN 901044 April 2013 This publication provides the following information on
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services ICD-10-CM/PCS THE NEXT GENERATION OF CODING ICN 901044 April 2013 This publication provides the following information on
Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures
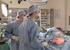 Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures Table 1: Surgeon Billing for Laparoscopic Adjustable Gastric Band Procedures 2012 Medicare Payment 2 43770
Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures Table 1: Surgeon Billing for Laparoscopic Adjustable Gastric Band Procedures 2012 Medicare Payment 2 43770
National Provider Call: Hospital Value-Based Purchasing (VBP) Program
 National Provider Call: Hospital Value-Based Purchasing (VBP) Program Fiscal Year 2016 Overview for Beneficiaries, Providers and Stakeholders Cindy Tourison, MSHI Lead, Hospital Inpatient Quality Reporting
National Provider Call: Hospital Value-Based Purchasing (VBP) Program Fiscal Year 2016 Overview for Beneficiaries, Providers and Stakeholders Cindy Tourison, MSHI Lead, Hospital Inpatient Quality Reporting
Clinical Governance Development Committee October 2007 Dr Foster RTM Alerts Progress Report
 Clinical Governance Development Committee October 2007 Dr Foster RTM Alerts Progress Report 1. Background Information 1.1. Initial review of the tool in November 2006, and subsequent queries in January
Clinical Governance Development Committee October 2007 Dr Foster RTM Alerts Progress Report 1. Background Information 1.1. Initial review of the tool in November 2006, and subsequent queries in January
ICD-10 Provider Preparation
 ICD-10 Provider Preparation After browsing this slide deck, the viewer will become more familiar with the following information: What are the origins of ICD-10? Why transition to ICD-10? Why ICD-10 matters.
ICD-10 Provider Preparation After browsing this slide deck, the viewer will become more familiar with the following information: What are the origins of ICD-10? Why transition to ICD-10? Why ICD-10 matters.
See page 331 of HEDIS 2013 Tech Specs Vol 2. HEDIS specs apply to plans. RARE applies to hospitals. Plan All-Cause Readmissions (PCR) *++
 Hospitalizations Inpatient Utilization General Hospital/Acute Care (IPU) * This measure summarizes utilization of acute inpatient care and services in the following categories: Total inpatient. Medicine.
Hospitalizations Inpatient Utilization General Hospital/Acute Care (IPU) * This measure summarizes utilization of acute inpatient care and services in the following categories: Total inpatient. Medicine.
Abu Dhabi Clinical Coding Audit
 Abu Dhabi Clinical Coding Audit 1 st January, 2014 Clinical Coding Steering Committee v4 1 Contents Section or Table 1. Objective 3 2. Who May Ask for an Audit? 3 3. Who May Conduct the Audits? 3 4. Payers
Abu Dhabi Clinical Coding Audit 1 st January, 2014 Clinical Coding Steering Committee v4 1 Contents Section or Table 1. Objective 3 2. Who May Ask for an Audit? 3 3. Who May Conduct the Audits? 3 4. Payers
6/30/2015. Physician Revenue Cycle: Basics and Beginnings. Today s Agenda. Codes by Setting
 Revenue Cycle: Basics and Beginnings Leigh Williams CPC, CPHIMS AHIMA Approved ICD-10-CM/PCS Trainer Director, Revenue Cycle/HIM Today s Agenda Terminology for code sets ICD Modifier RVU What about ICD-10?
Revenue Cycle: Basics and Beginnings Leigh Williams CPC, CPHIMS AHIMA Approved ICD-10-CM/PCS Trainer Director, Revenue Cycle/HIM Today s Agenda Terminology for code sets ICD Modifier RVU What about ICD-10?
The American Hospital Association s Coding Clinic for ICD-9-CM is one
 Coding Clinic update Complications of surgery, uncertain diagnoses and more high light important updates for CDI specialists in third quarter 2009 W h i t e p a p e r Editor s note: The following article
Coding Clinic update Complications of surgery, uncertain diagnoses and more high light important updates for CDI specialists in third quarter 2009 W h i t e p a p e r Editor s note: The following article
Modifier -25 Significant, Separately Identifiable E/M Service
 Manual: Policy Title: Reimbursement Policy Modifier -25 Significant, Separately Identifiable E/M Service Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM028 Last Updated:
Manual: Policy Title: Reimbursement Policy Modifier -25 Significant, Separately Identifiable E/M Service Section: Modifiers Subsection: None Date of Origin: 1/1/2000 Policy Number: RPM028 Last Updated:
Oral Health Coding Fact Sheet for Primary Care Physicians
 2015 Oral Health Coding Fact Sheet for Primary Care Physicians CPT Codes: Current Procedural Terminology (CPT) codes are developed and maintained by the American Medical Association. The codes consist
2015 Oral Health Coding Fact Sheet for Primary Care Physicians CPT Codes: Current Procedural Terminology (CPT) codes are developed and maintained by the American Medical Association. The codes consist
HFMA s Revenue Cycle Forum
 A peer-to-peer online discussion community REPRINT July/August 2013 HFMA s Revenue Cycle Forum www.hfma.org/forums Understanding a Declining CMI: A Step-by-Step Analysis By Garri Garrison The first step
A peer-to-peer online discussion community REPRINT July/August 2013 HFMA s Revenue Cycle Forum www.hfma.org/forums Understanding a Declining CMI: A Step-by-Step Analysis By Garri Garrison The first step
Preparing for ICD-10 WellStar Medical Group Toolkit
 Preparing for ICD-10 WellStar Medical Group Toolkit Preparing for ICD-10 On Oct. 1, 2015, WellStar will transition from ICD-9 to ICD-10 coding for all medical diagnoses and hospital procedures Systemwide.
Preparing for ICD-10 WellStar Medical Group Toolkit Preparing for ICD-10 On Oct. 1, 2015, WellStar will transition from ICD-9 to ICD-10 coding for all medical diagnoses and hospital procedures Systemwide.
TRANSITIONING FROM ICD-9 TO ICD-10 CODES PRESENTED OCTOBER 8, 2015 NATALIE RIVERA, RN, MS, BSN, CCM, CNLCP
 TRANSITIONING FROM ICD-9 TO ICD-10 CODES PRESENTED OCTOBER 8, 2015 NATALIE RIVERA, RN, MS, BSN, CCM, CNLCP ICD-10: INTERNATIONAL CLASSIFICATION OF DISEASES 10 TH REVISION International Classification of
TRANSITIONING FROM ICD-9 TO ICD-10 CODES PRESENTED OCTOBER 8, 2015 NATALIE RIVERA, RN, MS, BSN, CCM, CNLCP ICD-10: INTERNATIONAL CLASSIFICATION OF DISEASES 10 TH REVISION International Classification of
Introduction to ICD-10. Frederic F. Little, MD Department of Medicine ICD-10 Physician Champion Boston Medical Center
 Introduction to ICD-10 Frederic F. Little, MD Department of Medicine ICD-10 Physician Champion Boston Medical Center Outline ICD-10 and BMC History and Background Physician Impact ICD-10 transition: General
Introduction to ICD-10 Frederic F. Little, MD Department of Medicine ICD-10 Physician Champion Boston Medical Center Outline ICD-10 and BMC History and Background Physician Impact ICD-10 transition: General
ICD-10-CM Coding Overview AHCA Spring Convention & Trade Show April 21-23, 2015
 ICD-10-CM Coding Overview AHCA Spring Convention & Trade Show April 21-23, 2015 1 Why the Conversion to ICD-10-CM? ICD-10-CM provides more specific data than ICD-9-CM Better reflection of current medical
ICD-10-CM Coding Overview AHCA Spring Convention & Trade Show April 21-23, 2015 1 Why the Conversion to ICD-10-CM? ICD-10-CM provides more specific data than ICD-9-CM Better reflection of current medical
ICD 10: Final Steps for Successful Implementation
 ICD 10: Final Steps for Successful Implementation Gayle R. Lee, JD Matt Elrod, PT, DPT, MEd, NCS Presenters Gayle Lee, JD, has more than 15 years of experience working on health care issues impacting the
ICD 10: Final Steps for Successful Implementation Gayle R. Lee, JD Matt Elrod, PT, DPT, MEd, NCS Presenters Gayle Lee, JD, has more than 15 years of experience working on health care issues impacting the
Regulatory Compliance Policy No. COMP.RCC 4.70 Title:
 I. SCOPE: Regulatory Compliance Policy No. COMP.RCC 4.70 Page: 1 of 9 This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); (2)
I. SCOPE: Regulatory Compliance Policy No. COMP.RCC 4.70 Page: 1 of 9 This policy applies to (1) Tenet Healthcare Corporation and its wholly-owned subsidiaries and affiliates (each, an Affiliate ); (2)
Using Medicare Hospitalization Information and the MedPAR. Beth Virnig, Ph.D. Associate Dean for Research and Professor University of Minnesota
 Using Medicare Hospitalization Information and the MedPAR Beth Virnig, Ph.D. Associate Dean for Research and Professor University of Minnesota MedPAR Medicare Provider Analysis and Review Includes information
Using Medicare Hospitalization Information and the MedPAR Beth Virnig, Ph.D. Associate Dean for Research and Professor University of Minnesota MedPAR Medicare Provider Analysis and Review Includes information
CCS Prep CTHIMA September 23, 2013. Speakers: Phyllis Hilt, MBA, RHIA Rachael D Andrea, MS, RHIA, CPHQ
 CCS Prep CTHIMA September 23, 2013 Speakers: Phyllis Hilt, MBA, RHIA Rachael D Andrea, MS, RHIA, CPHQ CCS Prep Certified Coding Specialist (CCS ) The CCS credential denotes a high standard of competence
CCS Prep CTHIMA September 23, 2013 Speakers: Phyllis Hilt, MBA, RHIA Rachael D Andrea, MS, RHIA, CPHQ CCS Prep Certified Coding Specialist (CCS ) The CCS credential denotes a high standard of competence
2/28/2013 ICD-10 AS MANDATED BY ACCME SPEAKERS ARE ASKED TO DISCLOSE ANY REAL OR APPARENT CONFLICT RELATED TO THE CONTENT OF THEIR PRESENTATION
 ICD-10 An Overview of the Code Sets with Emphasis on Documentation Requirements & Practice Readiness UMMC Family Medicine Update March 5-8, 2013 Flowood, Mississippi Patty Harper, RHIA AHIMA Approved ICD-CM/PCS
ICD-10 An Overview of the Code Sets with Emphasis on Documentation Requirements & Practice Readiness UMMC Family Medicine Update March 5-8, 2013 Flowood, Mississippi Patty Harper, RHIA AHIMA Approved ICD-CM/PCS
ICD-10 Preparation for Non- Coders in the Revenue Cycle
 ICD-10 Preparation for Non- Coders in the Revenue Cycle September 24, 2015 Arkansas HFMA Revenue Cycle Seminar Susan Wallace, MEd, RHIA, CCS, CCDS, CDIP, FAHIMA Program Objectives Explain the impact of
ICD-10 Preparation for Non- Coders in the Revenue Cycle September 24, 2015 Arkansas HFMA Revenue Cycle Seminar Susan Wallace, MEd, RHIA, CCS, CCDS, CDIP, FAHIMA Program Objectives Explain the impact of
STATISTICAL BRIEF #8. Conditions Related to Uninsured Hospitalizations, 2003. Highlights. Introduction. Findings. May 2006
 HEALTHCARE COST AND UTILIZATION PROJECT STATISTICAL BRIEF #8 Agency for Healthcare Research and Quality May 2006 Conditions Related to Uninsured Hospitalizations, 2003 Anne Elixhauser, Ph.D. and C. Allison
HEALTHCARE COST AND UTILIZATION PROJECT STATISTICAL BRIEF #8 Agency for Healthcare Research and Quality May 2006 Conditions Related to Uninsured Hospitalizations, 2003 Anne Elixhauser, Ph.D. and C. Allison
Preventing Readmissions
 Emerging Topics in Healthcare Reform Preventing Readmissions Janssen Pharmaceuticals, Inc. Preventing Readmissions The Patient Protection and Affordable Care Act (ACA) contains several provisions intended
Emerging Topics in Healthcare Reform Preventing Readmissions Janssen Pharmaceuticals, Inc. Preventing Readmissions The Patient Protection and Affordable Care Act (ACA) contains several provisions intended
A review of the Condition Present on Admission (CPoA) variable
 A review of the Condition Present on Admission (C) variable Miles Utz, Rachael Wills, Stephanie Callaghan, Taku Endo, Lachlan Mortimer, Sandra Martyn, Trisha Johnston, Corrie Martin Health Statistics Centre,
A review of the Condition Present on Admission (C) variable Miles Utz, Rachael Wills, Stephanie Callaghan, Taku Endo, Lachlan Mortimer, Sandra Martyn, Trisha Johnston, Corrie Martin Health Statistics Centre,
MASSACHUSETTS RESIDENTS CENTRAL MA. Acute Care Hospital Utilization Trends in Massachusetts FY2009-2012
 ACUTE CARE HOSPITAL UTILIZATION TRENDS I N MASSACHUSETTS FY2009-2012 MASSACHUSETTS RESIDENTS CENTRAL MA Introduction The Center for Health Information and Analysis (CHIA) is publishing these inpatient,
ACUTE CARE HOSPITAL UTILIZATION TRENDS I N MASSACHUSETTS FY2009-2012 MASSACHUSETTS RESIDENTS CENTRAL MA Introduction The Center for Health Information and Analysis (CHIA) is publishing these inpatient,
ICD-10-CM KEVIN SOLINSKY, CPC, CPC-I, CEDC, CEMC PRESIDENT HEALTHCARE CODING CONSULTANTS, LLC 480-200-4590
 ICD-10-CM KEVIN SOLINSKY, CPC, CPC-I, CEDC, CEMC PRESIDENT HEALTHCARE CODING CONSULTANTS, LLC 480-200-4590 ICD-10 FINAL RULE Implementation date October 1, 2014. ICD-9-CM codes will not be accepted by
ICD-10-CM KEVIN SOLINSKY, CPC, CPC-I, CEDC, CEMC PRESIDENT HEALTHCARE CODING CONSULTANTS, LLC 480-200-4590 ICD-10 FINAL RULE Implementation date October 1, 2014. ICD-9-CM codes will not be accepted by
It s Time to Transition to ICD-10
 July 22, 2015 It s Time to Transition to ICD-10 What do the changes mean to your SNF? Presented by: Linda S. Little, RN-BSN Clinical Consultant HMM Consulting Office: (631) 265-6289 E-Mail: [email protected]
July 22, 2015 It s Time to Transition to ICD-10 What do the changes mean to your SNF? Presented by: Linda S. Little, RN-BSN Clinical Consultant HMM Consulting Office: (631) 265-6289 E-Mail: [email protected]
Evidence Based Practice to. Value Based Purchasing. Barb Rogness BSN MS Building Bridges May 2013
 Evidence Based Practice to Value Based Purchasing Barb Rogness BSN MS Building Bridges May 2013 Why this topic? Value based Purchasing is here and not going away. It will grow by leaps and bounds. The
Evidence Based Practice to Value Based Purchasing Barb Rogness BSN MS Building Bridges May 2013 Why this topic? Value based Purchasing is here and not going away. It will grow by leaps and bounds. The
ICD-9-CM Official Guidelines For Coding and Reporting Effective October 1, 2002 Narrative changes appear in bold text
 ICD-9-CM Official Guidelines For Coding and Reporting Effective October 1, 2002 Narrative changes appear in bold text The Centers for Medicare and Medicaid Services (CMS) formerly the Health Care Financing
ICD-9-CM Official Guidelines For Coding and Reporting Effective October 1, 2002 Narrative changes appear in bold text The Centers for Medicare and Medicaid Services (CMS) formerly the Health Care Financing
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
ICD-10 for Ophthalmology
 June 2015 ICD-10 for Ophthalmology UConn Health Introduction Dr. Frank Turner ICD-10 Implementation Physician Advisor 2 Agenda After attending this session, participants will be able to: Describe the challenges
June 2015 ICD-10 for Ophthalmology UConn Health Introduction Dr. Frank Turner ICD-10 Implementation Physician Advisor 2 Agenda After attending this session, participants will be able to: Describe the challenges
ICD-10 Transition & Implementation Information
 ICD-10 Transition & Implementation Information I ICD-10 Implementation Compliance Date: October 1, 2015 ICD-10-CM diagnoses codes will be used by all providers in every health care setting. ICD-10-PCS
ICD-10 Transition & Implementation Information I ICD-10 Implementation Compliance Date: October 1, 2015 ICD-10-CM diagnoses codes will be used by all providers in every health care setting. ICD-10-PCS
The electronic health record (EHR) has been a game-changer for CDI specialists.
 Physician queries and the use of prior information: Reevaluating the role of the CDI specialist WHITE PAPER Summary: The following white paper examines the issue of whether to use information from a prior
Physician queries and the use of prior information: Reevaluating the role of the CDI specialist WHITE PAPER Summary: The following white paper examines the issue of whether to use information from a prior
Billing an NP's Service Under a Physician's Provider Number
 660 N Central Expressway, Ste 240 Plano, TX 75074 469-246-4500 (Local) 800-880-7900 (Toll-free) FAX: 972-233-1215 [email protected] Selection from: Billing For Nurse Practitioner Services -- Update
660 N Central Expressway, Ste 240 Plano, TX 75074 469-246-4500 (Local) 800-880-7900 (Toll-free) FAX: 972-233-1215 [email protected] Selection from: Billing For Nurse Practitioner Services -- Update
Common Pathology Diagnoses: ICD-9 to ICD-10 Mapping
 PERFORMANCE THAT MATTERS NUMBER OF CODES 14,000 69,000 ICD-9 DIAGNOSIS CODES ICD-10 DIAGNOSIS CODES CODE STRUCTURE ICD-9-CM CODE FORMAT ICD-10-CM CODE FORMAT X X X X X X X X X X X X CATEGORY ETIOLOGY,
PERFORMANCE THAT MATTERS NUMBER OF CODES 14,000 69,000 ICD-9 DIAGNOSIS CODES ICD-10 DIAGNOSIS CODES CODE STRUCTURE ICD-9-CM CODE FORMAT ICD-10-CM CODE FORMAT X X X X X X X X X X X X CATEGORY ETIOLOGY,
Alameda Alliance for Heath ICD-9 to ICD-10 TRANSLATION CODES E10.10
 DIABETES ICD-9 CM ICD-9 CM Volume 1 - Diagnosis Description ICD-10 CM - Diagnosis Code ICD-10 CM - Diagnosis Description 250.00 Diabetes mellitus without mention of complication, type II or unspecified
DIABETES ICD-9 CM ICD-9 CM Volume 1 - Diagnosis Description ICD-10 CM - Diagnosis Code ICD-10 CM - Diagnosis Description 250.00 Diabetes mellitus without mention of complication, type II or unspecified
AGENDA WHAT IS COMPUTER-ASSISTED CODING, REALLY? J03.0 F43.0 I10 A78 R52
 R06.2 F43.0 I10 06BY3ZC J03.0 A78 03HK0MZ R52 0SG1430 COMPUTER-ASSISTED CODING AGENDA Evaluating and Understanding the Technology Review of Lessons Learned from Early Adopters Workflow and Analytics with
R06.2 F43.0 I10 06BY3ZC J03.0 A78 03HK0MZ R52 0SG1430 COMPUTER-ASSISTED CODING AGENDA Evaluating and Understanding the Technology Review of Lessons Learned from Early Adopters Workflow and Analytics with
