Obesity Surgery Handbook
|
|
|
- Roderick Andrews
- 8 years ago
- Views:
Transcription
1 Obesity Surgery Handbook Obesity Surgery Handbook Produced by S.O.S. (Surgical Obesity Service) Hamilton Wellington NEW ZEALAND Mr David Schroeder MBChB FRACS Mr Rowan French MBChB FRACS Mr Atul Dhabuwala MBBS FRACS Mr Jon Morrow MBChB FRACS Consultant Surgeons Hamilton 2015
2 INTRODUCTION We want to acknowledge your courage in taking the first step in finding out about obesity surgery. Widely held misbeliefs about people with obesity have shrouded obesity surgery with an atmosphere of failure and desperation. Whilst obesity surgery should be seen as the last resort, it is also the most effective treatment for patients with morbid obesity. It is now firmly established in most countries in the world, and there is a vast amount of reliable information available about most of the surgical procedures. As with most operations, there have been many advances over the last 15 years, and obesity surgery is now very safe when performed by experienced surgeons in well-established centres. DEFINITION OF OBESITY To define the different levels of obesity, we use a formula called the Body Mass Index (BMI). The Body Mass Index is calculated by dividing your weight in kilograms by your height in metres squared. BMI = Weight (kg) Height (m) X Height (m) The normal body mass index is Overweight people have a body mass index of People with obesity have a BMI above 30. If the BMI is above 35 you are said to be severely obese, above 40 you are morbidly obese, over 50 you are super obese. Normal Weight Overweight Obese Severely Obese Morbidly Obese When your BMI is greater than 35, the likelihood of suffering major medical, physical or social problems is much greater because of your weight. It is for this reason, that you would qualify for surgery if your BMI is greater than 40 kg/m 2 or greater than 35 kg/m 2 but with one of the health problems caused by obesity. However we will consider patients with a BMI greater than 30 in specific situations. These we will mention later in this booklet. To determine your BMI, please go to our website and enter your values in the BMI calculator.
3 PROBLEMS ASSOCIATED WITH OBESITY Shorter Life Expectancy: - As your weight increases, so too does the risk of dying. If your BMI is greater than 35 you are in the high-risk group and by the time you reach a BMI of 40, the risk is more than twice that of people who have normal weight. This risk rises greatly as your weight goes above a body mass index of 40. Major Health Risks: - Obesity is associated with numerous medical conditions, some of which are caused by obesity or are just made worse by obesity. These include Diabetes (type II), joint problems (arthritis), high blood pressure, heart disease, asthma, sleep disturbances and even some cancers. People with obesity also have an increased risk for: - gallbladder problems, reflux disease, problems with fertility and psychological problems (i.e. depression) Difficulties with Day-to-day Living: - People with obesity often struggle to do the things that others can do. Movement is more difficult and they tend to tire more quickly, which generally excludes them from sporting and other physical activities. Sometimes housework or even employment is a challenge. It is also often difficult to maintain personal hygiene, along with difficulties associated with getting into and out of cars, bus/airplane seats, telephone booths and turnstiles. Social Isolation: - Most people with significant obesity feel embarrassed in social situations, and even in public and hence prefer to withdraw from these situations. Obesity often produces a negative self-image and a low self-esteem, which can then lead to depression. People with obesity are discriminated against. Their fear of embarrassment and their lower physical activity level deprives them of the chance to work, the chance to join the family in outside activities and to join friends socially. They also face the stigma of living in a world that expects people to be thin. THE CAUSE OF OBESITY Obesity develops when the energy taken in food and drink over a long period of time is greater than the energy that is used up in day-to-day activities. We are very interested in why this occurs. None of our patients intend to get big, and they don t enjoy it when they are big. There are a number of factors that work together to cause this. The main underlying cause is a genetic tendency, but this, together with hormonal, environmental, social and cultural factors, produces a situation where there is a very powerful and irresistible drive to eat. This is made up by two important factors that can be hard to draw apart, but must both be present in the patient with obesity: 1. Food addiction: Over time, the brain comes to depend on food as the solution to challenging situations, or as a way to make the good times better. This creates the habits that are so hard to beat. Trying to overcome the urge to eat is harder than resisting alcohol and cigarettes because we can t give food up completely. This is what makes dieting so difficult- we are deliberately depriving our brains of something it desperately wants and needs. Initially the joy of the weight loss counteracts this, but all diets reach
4 plateaus, and when the weight loss stops, it is very hard to continue the diet. The slightest stress becomes an excuse to break the diet, and often weight ends up higher than before the diet (yo-yo dieting). 2. Insulin resistance: The normal fat cell has a job to do: when we eat, it s meant to take up fat and sugar and store them. Two hours later, when we have finished digesting our meal and the blood levels of energy reduce, the fat cell is meant to release its stored energy for use by the brain and body. Patients with obesity have fat cells that don t release their energy properly, and so the brain thinks, two hours after eating, that there is insufficient fuel, and makes them hungry again. The most likely chemical to be causing this blockage is insulin. Insulin has the job of pushing sugar into fat cells to make fat, and prevents breakdown. It also makes us hungry. All people with obesity have higher than normal levels of insulin. The biggest stimulus to insulin secretion is sugar and simple carbohydrates. That is why these foods fail to satisfy, and make us crave something to eat again so soon after eating them. And yet, these are the very substances that our brain becomes addicted to! The combination of these two things can produce an overwhelming obsession with food that can take over life completely. For this reason, if we see someone who has a BMI of 30 who has no life because of this, and who can t solve the problem with a low carbohydrate diet, we will consider a weight loss surgical procedure to give them their life back. THE SOLUTION TO OBESITY The common non-surgical techniques that have been used for controlling weight (gain) include diet, exercise programmes, behaviour modification and drugs (appetite suppressants and/or those which reduce absorption of fat in the gut). These methods of treatment can help you lose a small amount of weight initially but prolonged substantial weight loss usually requires something more than this. Diets and drugs (such as Xenical, Reductil and Duromine) if used optimally and permanently can provide you with a 10 to 15 kg weight loss, but many people soon regain their weight, or even end up weighing more when the treatment is ceased. If however, you need to lose much more than 10-15kg in weight, the research shows that you are simply not going to achieve it by following the diet tablet exercise regime. Surgery is the only method of consistent and sustainable weight loss for the majority of large people. However, not everyone who has a weight problem should consider surgery. It depends on whether or not you are overweight, obese or morbidly obese. When your BMI is 30 or above, surgery is a very effective form of treatment for longterm weight loss. But, keep in mind; surgery can help you achieve your long-term goal only if you are ready for, and committed to losing weight and keeping it off.
5 SURGICAL TREATMENT There are two types of surgical treatment available for obesity today, which work in a restrictive or malabsorptive fashion. Restrictive procedures physically reduce the size of the stomach, initially limiting the amount of food that can enter, resulting in weight loss (e.g. gastric banding, stomach stapling, gastric bypass and sleeve gastrectomy). Longer term, they work by decreasing the drive to eat and giving a feeling of fullness. Malabsorptive procedures (e.g. biliopancreatic diversion [BPD]), bypass the normal absorptive capacity of the gut. However as significant permanent symptoms generally exist, these are not performed in our centre, and won t be discussed further in this booklet. When researching obesity surgery, it is important to look at all the options available. We offer two different operations (gastric bypass and sleeve gastrectomy), each of which has advantages and disadvantages. We encourage you to read the information, but to come to your appointments with an open mind and all of your questions. Listen to the experiences of others, both positive and negative, but be aware that they may not apply to you or your situation. The important thing to bear in mind is that any surgery has risks, and we need to weigh up the risks versus the complications in each individual s situation. We are happy to share our knowledge with respect to what we have found to be best for each patient, and will support you fully in whichever decision you make. 1. LAPAROSCOPIC ROUX-EN-Y GASTRIC BYPASS (REYGB) The Roux-en-Y gastric bypass procedure is usually performed laparoscopically (i.e. keyhole surgery with a telescope) by our service; however, in some cases, it may be necessary to perform an open procedure through a large cut in the abdomen, usually if you have had an open operation before. This type of bypass operation has proven to be an effective, consistent way of losing weight and keeping it off, but to achieve these results it requires lifelong changes to lifestyle and eating. In this gastric bypass operation, the stomach is completely divided with a stapler to leave a pouch that initially measures only 15ml. The small bowel is divided and the divided end brought up to the small stomach pouch. The other small bowel end is joined back to the small bowel about a metre down from the stomach. Thus the whole stomach is bypassed apart from a tiny pouch. This operation works in two ways:
6 Initially the small pouch means that only a small amount of food can be taken in at any sitting, producing an initial rapid weight loss. Longer term, you can eat an entree at a restaurant, and the weight stays off because of the feeling of fullness and the same switching off of the intense need to eat. When undigested high sugar and/or high fat food passes into the small bowel, it causes significant symptoms, known as dumping (such as nausea, sweaty, clammy, dizzy feelings), putting people off eating the wrong sort of foods. If people don t dump, they can eat carbohydrates, and get back into the addiction cycle. Only about 30% of people continue to dump long term. This procedure has a higher complication rate than some of the other operations (i.e. gastric banding), however the weight loss is more consistent and patients can expect to lose more, quickly. The expected average weight loss is more like 80-85% of excess weight and will still be influenced long-term by exercise and diet. Patients will need to take daily supplements for the rest of their life. The complications that arise from dividing and stapling include bleeding, leaks from joins or staple lines, and bowel obstruction. 2. LAPAROSCOPIC SLEEVE GASTRECTOMY Sleeve Gastrectomy is a relatively new technique that was originally developed as the first stage of a two stage malabsorptive procedure in high-risk patients. Surgeons found that if they removed three-quarters of the stomach, left the patients to lose weight, then came back and finished the operation, the death rate was much lower. However, some patients did quite well even without the second procedure, although the majority did have some weight regain long term. It is an easier operation to perform than the REYGB as there are no joins, and so is being used more widely, despite the lack of long term follow up. The procedure is still performed laparoscopically; a stapler is used to completely divide the stomach, leaving a thin tube down to a normal outlet. The remaining stomach is removed through a slightly enlarged 12mm incision. Weight loss at one year averages 75% of excess weight. The first three months, though, can be plagued with reflux and nausea. The advantages are that there is less malabsorption, so there is possibly less need for supplements, and there is little risk of bowel obstruction or ulcers. The disadvantages are similar to the REYGB: bleeding and leaks from the staple line,
7 however these are often more difficult to resolve in a sleeve and will often require conversion to another procedure such as the gastric bypass. In our practice, we have had such a low complication rate with the REYGB that we are reluctant to try a new procedure with unproven outcomes, unless there are special circumstances e.g. previous surgery making it impossible to use the small bowel, or extreme distance for follow up. The sleeve gastrectomy is therefore used as a second choice operation. It costs $ more than a gastric bypass, as we need to use a special instrument to divide and seal all the blood vessels to the stomach that is removed. How surgery works- addiction versus habits Most patients assume that the reason they will lose weight after surgery is that their stomach will not be able to tolerate the large amount of food they used to eat. Whilst this is true in the short term, the main reason for the long-term weight loss is a poorly understood effect on the eating centres in the brain. After surgery, patients usually lose their overpowering drive to eat. They are no longer thinking about food all the time. They have been given back choice. With the bypass and sleeve, this loss is usually stable for the first 6 months. With a gastric band, the hunger switches back on after 1-2 weeks, and stays on until the first adjustment. Until this is done, people are reliant on won t-power again, which can be frustrating. However it is important for the band site to be well healed before starting inflations. By regaining greater control over the drive to eat, people can then choose the diet that suits their body. You still need to eat a high protein, moderate fat, low simplecarbohydrate diet afterwards, for life, as we haven t changed the abnormal fat cell metabolism. The surgery makes this possible. However, no operation will switch off the habits that are related to eating, and have been generated over many years. These are like short circuits in the brain- a button is pushed, and you have eaten something you didn t intend to before you realise it. Changing these sorts of behaviours takes brain work, and is what determines the final result that people get after the operation. Those that work with all the tools and strategies we give them can achieve whatever weight they like. They can choose, when the button is pushed, to either respond with the new strategy and win, or do what they always did, and get what they always got - no weight loss and subsequent weight regain. The most common reason for failure of any operation is that patients get back into eating carbohydrates again, either out of habit, addiction, or because it s easy. This restarts the cycle of hunger, cravings, and lack of satiety. Fortunately, if we become aware of this, we can help patients reclaim their operation with dietary and psychological tools. This explains one of the differences in weight loss at two years between bypass/sleeve and the gastric band- the bypass and sleeve operations helps throttle back the habits more effectively than does a band. Both of these procedures can be highly effective if you approach the surgery understanding that this is the first step of a long learning process, and with a willingness to be honest and seek whatever help you need to overcome the habits.
8 The final part of the operation that is entirely over to the patient, is to find a replacement for the joy of food. Food gave you a lift and comforted you. You need to find other things that do it for you that aren t illegal, immoral or that make you fat! For some people this is easy- they have very full lives that just expand into the previous areas occupied by food. However for those with a life limited by pain, social isolation or low self-esteem, it can be very difficult. Ask for help - we have the experience to help people through these difficult stages. If you don t find these things, your brain will automatically take you back to food, and you will not get the desired results. In summary, to get the results you want, we provide: 1. An operation to switch off the food addiction 2. Knowledge of the diet your body needs to get the best out of it (low in both sugar and simple carbohydrates) 3. Brain tools to deal with habits and to cope with stress in a healthy adult way 4. Goal setting tools to develop your plan forward and that support you to create different rewards in everyday life to replace the joy of food Foundations of Healthy Living Retreats As we know how difficult it is for patients to manage to sustain new habits and lifestyle choices without succumbing to their old ways, we have as part of our process a residential retreat program called Foundations of Healthy Living. The goal at our 4 day retreat is to help promote personal growth through group support and learn skills to help you maintain and restore increased awareness and self esteem. Our mind/body focus looks at physical activity, nutrition and overall wellness with the foundation being self-love and self-care. The structured program supports you to make comprehensive changes in the areas of behaviour, diet and exercise. We also help you to address the underlying emotional triggers that can prevent you from moving forward into a healthy fulfilling lifestyle. The retreat program is designed to help you learn to change the way you think, feel, act and live and subsequently we encourage all patients to make it an essential part of the program. Which operation is for me? As you can see, all the operations work by reducing the drive and capacity to eat, thereby allowing people to eat the diet their body needs. Usually people come to us with a clear idea of which operation they want usually based on what they have seen and heard from friends and acquaintances, or from blogs on the Internet. We will very rarely dissuade people from their choice unless there is good reason: If people have had any previous surgery around the top of the stomach that may have damaged the nerves in this area e.g. hiatus hernia repair, we will need to perform either a gastric bypass or sleeve gastrectomy procedure. People who have had previous surgery involving the colon and small bowel usually are not suitable for a bypass as there may not be enough small bowel free through previous scarring. We would recommend sleeve gastrectomy for these people, or they may need an open operation. Those with Type 2 diabetes who respond to surgery (90%) will get a more rapid reversal of their diabetes with a bypass. They may get improvement with a sleeve gastrectomy too, but as they need to lose the weight first, we will generally
9 recommend a gastric bypass. Because we are encompassing more and more understanding about the causes of obesity, and new drugs are always coming on the market, we may in some special circumstances ask the patient to consider using a non-surgical approach first. However we usually consider gastric bypass in most people, including mature teenagers. Please voice your questions at your initial assessment so that you are making your decision based on facts. No operation will work unless you work with it - there is no guaranteed weight loss procedure. Whichever operation people choose, we will support them as best we can! Effects, risks and complications What can we expect? Along with your weight loss, we also expect that there will be improvements in some of the medical problems that you may have. You usually have a much greater capacity for physical activity and you will be socially a lot more comfortable. Your self-esteem and self-confidence are likely to improve and there is likely to be an overall improvement in the quality of your life. We also hope that your life expectancy will improve. Primarily, substantial weight loss is our patient s focus. We expect that, on average, people who have the gastric bypass procedure will lose approximately 80% of their excess weight. For example, if your current weight is 120kg and your ideal weight is 60kg, then your total excess weight is 60kg. 80 per cent of this is 48kg. Therefore you could expect your weight would come down to around 72kg on average. These results may vary widely: some will lose very little weight and others will get down to their ideal body weight. Our aim is to achieve the weight loss without interfering unnecessarily with the quality of life, or by placing too severe a restriction on your normal living pattern. We are not just aiming to achieve some ideal weight, but also to solve the problems that obesity causes. Diseases such as diabetes, asthma, high blood pressure, joint pain and heartburn are greatly improved with the weight loss. What are the risks and complications? All surgery has risks, especially major surgery. Any stomach operation for obesity is considered major surgery, and therefore has significant risks associated with it. Risks during surgery: People have died from having operations for morbid obesity it happens rarely, but we can never take away the risk completely. If you are older and if you already have certain problems related to your obesity, your risk will rise. Heart attacks after the operation, clots that form in the leg veins and then pass to the lungs, or leakage of stomach joins can cause death in people with obesity.
10 Precautions are taken during surgery and your hospital stay in order to prevent these risks occurring. To try and prevent clots forming in the leg veins, patients are given blood-thinning injections prior to surgery, wear compression stockings whilst in hospital and have intermittent compression of their calves during the operation. We also mobilize you as soon as possible after surgery, and encourage you to walk as much as possible in the weeks after going home. As mentioned above, bleeding can occur after any surgery, but is greatest after stapling operations (0.1% of people will need a blood transfusion). Bleeding may come from damage to the spleen or liver, or from the staple lines. For this reason, we will not operate on people who refuse blood transfusions for religious reasons. Risks immediately after surgery: Leaks mean that fluids normally contained in the gut leak out into the abdominal cavity, causing pain and infection. This is a very serious situation and will always require another operation. Although we do our utmost to prevent this, it can occasionally happen, and may result in a very prolonged hospital stay. In the very few cases where this has happened, patients are admitted to the public hospital, so expense is less of an issue than health. However, if we do need to re-operate in the private hospital because of a rare complication, the hospital will charge for a small portion of the costs, usually to a maximum of $2000. Risks after you go home: Sleeve and Gastric bypass: After a bypass, too much healing can occur at the join between the stomach pouch and the small bowel, causing a narrowing that must be dilated. The patient presents with an inability to progress to solid food, usually around the 6-week mark. Correcting this is very safe and takes very little time to do, but does require a heavy sedation and passing a telescope down into the stomach to use a balloon to stretch the scar tissue. We will cover the cost of this procedure should it be required. Fortunately since we have been sending everyone home on anti ulcer medication, the rate of having to do this has dropped to less than 2%. Long-term risks: Sleeve and Gastric bypass: The bypass and sleeve risks can be associated with a failure of the stomach to produce factors that help absorb Vitamin B12. With either of these operations, B12 deficiency can occur even years after the operation, so regular blood tests are needed. The bypass can also cause iron, calcium and other vitamin malabsorption, and good quality supplements must be taken for life. Failure to do can lead to brain damage that may not be completely reversible with restarting the supplements. This is a rare but dangerous complication that can be completely avoided by simply following the rules. Multivitamins must be taken daily, for life, after all weight loss surgery procedures. With the bypass, re-routing of the small bowel does create potential spaces for the bowel to get twisted in, and can cause life threatening bowel death. This is rare and completely fixable by re-operating to untwist the bowel. Currently we close all potential spaces, so the risk of this should be minimal. The small bowel is not designed to receive acid. This doesn t matter when there is such a small stomach, but if we add drugs that cause ulcers in ordinary people, we can set people up to get ulcers. The drugs that classically do this are antiinflammatories such as Aspirin and Voltaren, as well as Prednisone. We have had people perforate ulcers after taking these medications. You can use these, but you do need to take anti-ulcer medication at the same time. Smoking has the same effect and for this reason we require you to give up smoking prior to surgery and do not restart.
11 What are the side effects? Hair Loss Due to rapid weight reduction, it is common to notice that some of your hair may thin out. This is due to the body prioritizing the usage of the reduced amount of protein for more important processes in the body during this time. It usually is temporary and stops when the weight loss slows (about six to eight months after the operation) and then will grow back again. Loose skin Some people are left with excessive loose skin after losing their weight. You may need to have further surgery at a later stage if this continues to be a problem. We recommend you wait 2 years before you go ahead with this. Dietary issues During the initial phase of new eating patterns, you may have occasional episodes of vomiting if you eat the wrong type of food or if you eat too quickly. With time, you will learn to identify those foods that cause you problems, however if you eat slowly, eat small amounts, chew really well and take your time; you can avoid some of these difficulties. Your eating pattern will steadily improve and 9-12 months after your operation, you will be eating a wide range of high protein, moderate fat, low carbohydrate foods, in socially adequate amounts. As your food intake will be restricted by your operation, it is important to eat wisely. The success of any obesity operation requires you to take responsibility for your eating and exercise patterns. Therefore, we hope that you will follow the guidelines provided by our nutritionist/dietitian:! Eat three regular nutritious meals each day, with preferably no snacks in between! Take your time and chew food really well. Stop when you are comfortable! Eat only good foods that help meet all of your nutritional requirements Your exercise guide Exercise regularly and be active. Exercise promotes weight loss and improves your general health as well. We recommend 30 minutes a day, 5 times per week, starting 1 week after leaving hospital. This will be difficult at first, but as you lose weight it becomes easier. Start with small achievable exercise goals, choosing activities that you enjoy and will be able to continue with. Walking is ideal to begin with. Take the stairs instead of the elevator, park a few rows further back at the supermarket, walk the dog or play with the kids. These are all activities that can help you increase your daily exercise. When possible, commit to exercise with another person and make it a social, fun experience. Involve a personal trainer, fitness consultant or exercise group if you need extra motivation. Wear loose comfortable clothing and appropriate footwear for the exercise that you are undertaking. Exercise requires commitment, so make it a priority and set-aside time in your daily schedule. The more active you are, the fitter and healthier you will feel, and the greater your weight loss will be.
12 Hospital stay The operation You will come into hospital on the day of the procedure, having not had anything to eat or drink from the times given to you on the admission form. The anaesthetist and the surgeon will visit you in the hospital before you have your surgery. The operation is performed under a General Anaesthetic and takes about min for a sleeve gastrectomy or gastric bypass. It is almost always done laparoscopically (i.e. with a telescope through small cuts) so the recovery is quicker, the complications of wound infections and hernias are less severe, and the cosmetic result is excellent. After surgery, people usually become aware in the Recovery room, but sometimes back in their hospital room. Any pain and nausea should be reported to the nurses immediately, so you will receive whatever medication you need at this stage. On return to your ward, the nursing staff will have been instructed to get you up and moving. On the day of the operation you can have crushed ice. Over the next 2 days, you will be gradually increasing your oral intake, starting with water and progressing to low calorie fluids/yoghurt by the time you leave hospital. You are expected to be in hospital for 2 nights. We would expect you to resume your normal activities within 2 weeks after any of the surgical procedures. If however, the surgeon found it necessary to convert to an open operation, you will generally have more discomfort after the procedure and you may need to stay in hospital longer. Return to your normal activities will take longer also. Post-operative course and follow up Post Operative You will be given a diet sheet to follow for the four weeks following the operation. The amount of exercise you should do will also be explained. The first 3 months are a difficult time with eating, as you learn to live with your new stomach. With all operations, this is the time to learn to eat slowly and chew well. Failure to do so will result in painful blockages and eventually vomiting! This should happen infrequently as you learn how to eat. Follow Up Regular follow up with members of our team is an essential part of this operation. Our nurse will call you the week after the operation to check that things are progressing normally. The initial post op visit is 4-6 weeks after the operation; the next is 10 weeks later (4 months) and after this at 8 months, 1 year, 18 months and 2 years. From then on we need to see you annuallu and check that there are no nutritional problems. Regular blood tests are done to check that enough of the right nutrition is being consumed, and to see if other supplementation is needed. Everyone who has had a bypass must take good quality multi-vitamin tablets daily plus iron/folic acid, calcium
13 and B12 for the rest of their life (men and women may differ slightly). Alternatively, Vitamin B12 injections can be done 3 monthly instead. At each follow-up appointment a further dietary assessment is done to ensure adequate nutrition. You need to eat sensibly for the rest of your life. We have put a lot of effort and commitment into achieving the best possible result for you and it is absolutely essential for you to also put in that effort and attend the follow-ups as requested. The brain work As mentioned at the beginning of this information booklet, whilst the operation will give you the ability to choose your food because for the first time you will feel full, and won t have food niggling at your brain the whole time, it doesn t make this happen. We now understand that people with obesity develop a bunch of habits because food does it for them. These habits don t automatically go away after the operation- they are the default pathway still for people in many situations. We know that those who do well after the surgery are the ones who work with us to retrain the brain. This is achieved through a combination of strategies, skills and awareness that all members of the team will bring to you. Attendance at the Foundations of Healthy Living retreat emphasizes this. We believe that good results with any operation are 50% surgery, 50% brain work. It is easier for people to have something done to them, than to change the way they think. This is why the follow up is so essential: we are constantly trying to help you achieve the goals you had decided on when you embarked on this process. Weight Loss Surgery and Smoking: A Dangerous Combination Illness resulting from tobacco usage is the single greatest cause of disease and premature death in New Zealand. It is also the most preventable. We are committed to helping our patients improve their overall health, so we make a thorough effort to not only address your weight loss needs but also to encourage and assist you in quitting smoking. Additionally, when smoking and weight loss surgery are combined, there is an increased risk of complications during surgery, often affecting the ability to heal. Here s why: tobacco smoke causes the blood vessels to constrict (shrink) which decreases blood flow to the stomach. Carbon monoxide (a substance produced during cigarette smoking) reduces the ability of red blood cells to carry oxygen. These combined factors can cause healing following weight loss surgery to slow considerably. Prior to Roux-En-Y Gastric Bypass surgery, there are five blood vessels that supply blood to the stomach. After the surgery, the number of blood vessels to the stomach is reduced. For patient s who smoke prior to weight loss surgery, you put yourself at risk of complications during or immediately after surgery. These may include: Heart attack or stroke during surgery Breathing difficulties causing pneumonia or bronchitis By continuing to smoke following surgery, a patient can experience a host of other complications, including: Stricture (narrowing) at top join a four fold greater risk
14 Ulceration of the pouch three times the risk Inflammation (Gastritis) Wound infection Lung dysfunction Increased shortness of breath Reduced ability to absorb vitamins and minerals We are genuinely concerned about these potential complications and strive to ensure our patients have minimal on-going problems after surgery therefore we will encourage smokers to partake in a comprehensive smoking-cessation program. Completion of such a program is mandatory for weight loss surgery candidates who smoke, a minimum of two weeks prior to surgery, but preferably prior to your initial consultations. Your surgery will be postponed, or you could be released from consideration for surgery altogether if you continue to smoke. You will not be rescheduled for surgery until you have been tobacco-free for two weeks. In the event of any complications that occur as a result of smoking, the subsequent treatment involved in this will be at the patient s expense. Smoking cessation options we recommend nicotine replacement therapy - these products provide you with small doses of nicotine without the toxins found in cigarette smoke. By receiving graduallydecreasing doses, you will be weaned off the nicotine with less severe withdrawal symptoms. Nicotine replacement is available in three over-thecounter delivery methods: chewing gum, lozenges and skin patches. Two prescription options nasal sprays and inhalers are also available. However, these products can't be used immediately prior to or during surgery, as they can cause some of the same problems with healing as cigarettes. You need to let us know if you are using a nicotine replacement. Non-nicotine prescription oral medications can also be used to help you quit smoking. Buproprion (brand name Zyban), also sold as the antidepressant Wellbutrin, reduces the craving for nicotine. Varenicline tartrate (brand name Champix) targets the part of the brain that is affected by nicotine. In addition to reducing withdrawal symptoms, it dampens the pleasure a smoker gets if he or she relapses and lights up, thereby reducing the temptation to resume smoking. Other resources are also available to help you quit, including hypnotherapy, acupuncture and support groups (both online and in the community). QUITLINE ( offers many tools to help you quit smoking. These include a Quit Coach, Quit blogs (community support), Quitline (free advice), Txt2Quit and advice regarding nicotine, patches and lozenges We also know that patients have a fear that smoking cessation is often associated with weight gain, and many patients are afraid that if they stop smoking they will regain the weight they lost after surgery. Whilst we know that nicotine is an appetite suppressant and smoking slightly increases your metabolism, these effects are very slight and it is more likely that weight is gained due to emotional reasons or habit.
15 You may also find that when you are quitting you replace the hand-to-mouth habit of smoking with the hand-to-mouth eating behaviour. Part of quitting is to change some of your habits and routines. If you used to smoke after a meal, choose something else to do instead. Here are some examples: Clean your teeth Phone a friend Eat a piece of fruit Go for a walk Drink water Do the dishes It can be hard for your body to recognise the difference between hunger and a craving when you first stop smoking, so when you feel hungry at a time that you don't usually eat it's probably because you're craving a cigarette.! Change of Address To enable us to contact you and monitor your progress, it is important that we are informed of any changes in your details (address or phone number). Please help us to keep our records up to date. If at any time after your operation, you have problems that may be related to your surgery, or start regaining weight, please request a follow up visit. SURGICAL OBESITY SERVICE Hamilton SURGICAL OBESITY SERVICE Wellington 36 Grey St, Hamilton 3216 Southern Cross Specialist Centre Hanson Street Newtown
Bariatric Surgery a guide for patients 1
 Bariatric Surgery a guide for patients 1 Contents 1. Is obesity surgery effective? 2. Surgical procedures for obesity 3. Risks of obesity surgery 4. Before the operation 5. After the operation; It all
Bariatric Surgery a guide for patients 1 Contents 1. Is obesity surgery effective? 2. Surgical procedures for obesity 3. Risks of obesity surgery 4. Before the operation 5. After the operation; It all
What is the Sleeve Gastrectomy?
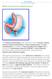 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY
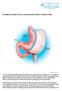 INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Introduction to obesity surgery
 Introduction to obesity surgery Auckland weight loss Surgery Surgery ADDRESS Mercy Specialist Centre PHONE FAX EMAIL WEB 100 Mountain Road, Epsom, Auckland 09 623 2409 09 630 8589 info@awls.co.nz www.aucklandweightlosssurgery.co.nz
Introduction to obesity surgery Auckland weight loss Surgery Surgery ADDRESS Mercy Specialist Centre PHONE FAX EMAIL WEB 100 Mountain Road, Epsom, Auckland 09 623 2409 09 630 8589 info@awls.co.nz www.aucklandweightlosssurgery.co.nz
Section 2. Overview of Obesity, Weight Loss, and Bariatric Surgery
 Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity
 Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
University College Hospital. Laparoscopic gastric bypass. Centre for Weight Loss, Metabolic and Endocrine Surgery
 University College Hospital Laparoscopic gastric bypass Centre for Weight Loss, Metabolic and Endocrine Surgery 2 3 If you need a large print, audio or translated copy of the document, please contact us
University College Hospital Laparoscopic gastric bypass Centre for Weight Loss, Metabolic and Endocrine Surgery 2 3 If you need a large print, audio or translated copy of the document, please contact us
Laparoscopic Gastric Bypass. Patient information leaflet. www.londonbariatricgroup.co.uk
 Laparoscopic Gastric Bypass Patient information leaflet www.londonbariatricgroup.co.uk The London Bariatric Group was formed to provide private patients with the highest quality Bariatric Surgery available
Laparoscopic Gastric Bypass Patient information leaflet www.londonbariatricgroup.co.uk The London Bariatric Group was formed to provide private patients with the highest quality Bariatric Surgery available
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. 201-795-8175 CarePointHealth.
 www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS
 GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
~ An Introduction to Weight Loss Surgery and the Southern DHB Bariatric Program
 ~ An Introduction to Weight Loss Surgery and the Southern DHB Bariatric Program Mark Smith MBChB MMedSci FRACS Renee Ladbrook PGDipDiet BSc Table of Contents Morbid Obesity... 1 What are we talking about?...
~ An Introduction to Weight Loss Surgery and the Southern DHB Bariatric Program Mark Smith MBChB MMedSci FRACS Renee Ladbrook PGDipDiet BSc Table of Contents Morbid Obesity... 1 What are we talking about?...
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Laparoscopic Sleeve Gastrectomy. Patient information leaflet. www.londonbariatricgroup.co.uk
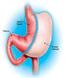 Laparoscopic Sleeve Gastrectomy Patient information leaflet www.londonbariatricgroup.co.uk The London Bariatric Group was formed to provide private patients with the highest quality Bariatric Surgery available
Laparoscopic Sleeve Gastrectomy Patient information leaflet www.londonbariatricgroup.co.uk The London Bariatric Group was formed to provide private patients with the highest quality Bariatric Surgery available
Weight Loss before Hernia Repair Surgery
 Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Understanding Obesity
 Your Guide to Understanding Obesity As your partner in health for your life s journey, we want you to be as informed and confident as possible regarding the disease or medical issue you may be facing.
Your Guide to Understanding Obesity As your partner in health for your life s journey, we want you to be as informed and confident as possible regarding the disease or medical issue you may be facing.
SlEEvE GASTRECTomY SURGERY What is a sleeve gastrectomy operation? BARIATRIC SURGERY
 Sleeve gastrectomy surgery This leaflet gives you general information about your surgery. Please read carefully. Share the information with your partner and family (if you wish) so that they are able to
Sleeve gastrectomy surgery This leaflet gives you general information about your surgery. Please read carefully. Share the information with your partner and family (if you wish) so that they are able to
ORMISTON HOSPITAL WEIGHT LOSS SERVICE
 ORMISTON HOSPITAL WEIGHT LOSS SERVICE Most patients achieve good to excellent weight loss results following gastric sleeve surgery, typically this is 50-60% of excess weight. A new beginning Welcome to
ORMISTON HOSPITAL WEIGHT LOSS SERVICE Most patients achieve good to excellent weight loss results following gastric sleeve surgery, typically this is 50-60% of excess weight. A new beginning Welcome to
Gastric Sleeve Surgery
 Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
If you are morbidly obese, you should remember these important points:
 What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
INFORMATION SHEET FOR A LAPAROSCOPIC GASTRIC BAND
 INFORMATION SHEET FOR A LAPAROSCOPIC GASTRIC BAND You are considering undergoing a laparoscopic gastric band for weight loss. The purpose of this information sheet is to provide you with the necessary
INFORMATION SHEET FOR A LAPAROSCOPIC GASTRIC BAND You are considering undergoing a laparoscopic gastric band for weight loss. The purpose of this information sheet is to provide you with the necessary
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
Weight Loss Surgery. Malabsorptive: Your intestines are rearranged to reduce the amount of food absorbed into the system
 The Region s Leader Weight Loss Surgery Table of Contents About Weight Loss Surgery 1 Laparoscopic Procedures 2 Adjustable Gastric Band 2 Biliopancreatic Diversion With Duodenal Switch 3 Rou-en-Y (RNY)
The Region s Leader Weight Loss Surgery Table of Contents About Weight Loss Surgery 1 Laparoscopic Procedures 2 Adjustable Gastric Band 2 Biliopancreatic Diversion With Duodenal Switch 3 Rou-en-Y (RNY)
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
GASTRIC BYPASS SURGERY
 GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
GASTRIC BYPASS SURGERY This leaflet gives you general information about your surgery. Please read it carefully. Share the information with your partner and family (if you wish) so that they are able to
really help your physical, social and emotional wellbeing helping you do more of the things you want and feel more confident and relaxed.
 Weight loss surgery If you are seriously overweight, losing excess weight can transform your life. Find out how you can make that change with the help of Spire Healthcare. If you One are off seriously
Weight loss surgery If you are seriously overweight, losing excess weight can transform your life. Find out how you can make that change with the help of Spire Healthcare. If you One are off seriously
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy
 Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Hypnotic. Gastric Band. Paul McKenna
 Hypnotic Gastric Band Paul McKenna Hypnotic Gastric Band The Amazing Truth About A Hypnotic Gastric Band A Gastric Band is a radical, surgical operation that reduces the available space in your stomach
Hypnotic Gastric Band Paul McKenna Hypnotic Gastric Band The Amazing Truth About A Hypnotic Gastric Band A Gastric Band is a radical, surgical operation that reduces the available space in your stomach
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
UW MEDICINE PATIENT EDUCATION. Weight Loss Surgery. What is bariatric surgery?
 UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
The first 6 weeks after gastric band/bypass surgery
 Patient information The first 6 weeks after gastric band/bypass surgery Eating and drinking In the first 4-6 weeks after the operation it is vital that you keep to the diet that we have advised in order
Patient information The first 6 weeks after gastric band/bypass surgery Eating and drinking In the first 4-6 weeks after the operation it is vital that you keep to the diet that we have advised in order
Surgical Associates of Ithaca Guide to Weight-loss Surgery
 Surgical Associates of Ithaca Guide to Weight-loss Surgery Please read through this entire guide. Weight loss surgeons Dr. John Mecenas and Dr. Brian Bollo are bariatric trained surgeons affiliated with
Surgical Associates of Ithaca Guide to Weight-loss Surgery Please read through this entire guide. Weight loss surgeons Dr. John Mecenas and Dr. Brian Bollo are bariatric trained surgeons affiliated with
INFORMATION SHEET FOR LAPAROSCOPIC ROUX-EN-Y GASTRIC BYPASS
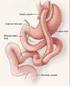 INFORMATION SHEET FOR LAPAROSCOPIC ROUX-EN-Y GASTRIC BYPASS You are considering undergoing a laparoscopic Roux-en-Y gastric bypass for weight loss. The purpose of this information sheet is to provide you
INFORMATION SHEET FOR LAPAROSCOPIC ROUX-EN-Y GASTRIC BYPASS You are considering undergoing a laparoscopic Roux-en-Y gastric bypass for weight loss. The purpose of this information sheet is to provide you
Bariatric Surgery Guide Dr. Stewart s Weight Loss Specialists of North Texas
 Welcome. This resource is created for you by Dr. Stewart and our bariatric surgery team with input from people who have found success through weight loss surgery. It is not intended to replace consultation
Welcome. This resource is created for you by Dr. Stewart and our bariatric surgery team with input from people who have found success through weight loss surgery. It is not intended to replace consultation
Weight Loss Surgery Information Session. WFBH Bariatric Surgery Program
 Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
University College Hospital. Laparoscopic sleeve gastrectomy. Centre for Weight Loss, Metabolic and Endocrine Surgery
 University College Hospital Laparoscopic sleeve gastrectomy Centre for Weight Loss, Metabolic and Endocrine Surgery 2 3 If you need a large print, audio or translated copy of the document, please contact
University College Hospital Laparoscopic sleeve gastrectomy Centre for Weight Loss, Metabolic and Endocrine Surgery 2 3 If you need a large print, audio or translated copy of the document, please contact
GASTRIC SLEEVE INSTRUCTIONS
 GASTRIC SLEEVE INSTRUCTIONS 3-6 months after surgery What you are likely to be experiencing Appetite you are probably getting hungry on most days, though not necessarily for 3 regular meals every day.
GASTRIC SLEEVE INSTRUCTIONS 3-6 months after surgery What you are likely to be experiencing Appetite you are probably getting hungry on most days, though not necessarily for 3 regular meals every day.
LAPAROSCOPIC GASTRIC BANDING
 LAPAROSCOPIC GASTRIC BANDING This information leaflet gives you general information about your surgery. Please read the information leaflet carefully. Share the information with your partner and family
LAPAROSCOPIC GASTRIC BANDING This information leaflet gives you general information about your surgery. Please read the information leaflet carefully. Share the information with your partner and family
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Bulimia Nervosa. This reference summary explains bulimia. It covers symptoms and causes of the condition, as well as treatment options.
 Bulimia Nervosa Introduction Bulimia nervosa, or bulimia, is an eating disorder. A person with bulimia eats a large amount of food in a short amount of time. To prevent weight gain, the person then purges.
Bulimia Nervosa Introduction Bulimia nervosa, or bulimia, is an eating disorder. A person with bulimia eats a large amount of food in a short amount of time. To prevent weight gain, the person then purges.
Quit plan. Your free guide on how to stop smoking. www.want2stop.info
 Quit plan Your free guide on how to stop smoking www.want2stop.info Thinking? about stopping Around three quarters of those people in Northern Ireland who smoke say they would like to stop. If you are
Quit plan Your free guide on how to stop smoking www.want2stop.info Thinking? about stopping Around three quarters of those people in Northern Ireland who smoke say they would like to stop. If you are
Your guide to stopping smoking for good
 Your guide to stopping smoking for good Reading this is your first step to stopping smoking for good Help2Quit gives you advice and support to help stop smoking for good. Nicotine replacement therapy and
Your guide to stopping smoking for good Reading this is your first step to stopping smoking for good Help2Quit gives you advice and support to help stop smoking for good. Nicotine replacement therapy and
Patient information. How to Stop Smoking Before your Operation PIF 734 V5
 Patient information How to Stop Smoking Before your Operation PIF 734 V5 Fag Ends can help you stop smoking before your operation. To contact Fag Ends for help to stop smoking please call Freephone: 0800
Patient information How to Stop Smoking Before your Operation PIF 734 V5 Fag Ends can help you stop smoking before your operation. To contact Fag Ends for help to stop smoking please call Freephone: 0800
Bariatric Weight Loss Surgery
 BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
About one-half of all smokers die of a disease caused by smoking.the most common ones are lung cancer, heart disease, and strokes
 Patient information from the BMJ Group Stopping smoking Smoking harms your health, but it's difficult to stop. That s because most people who smoke have become addicted to nicotine, a chemical in tobacco.
Patient information from the BMJ Group Stopping smoking Smoking harms your health, but it's difficult to stop. That s because most people who smoke have become addicted to nicotine, a chemical in tobacco.
INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types:
 INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types: Obesity associated health risks: Psychosocial Cardiovascular
INFORMATION FOR PATIENTS CONSIDERING BARIATRIC SURGERY: Obesity can lead to many health problems - these are mainly of the following types: Obesity associated health risks: Psychosocial Cardiovascular
Dr James Askew General Surgeon
 Dr James Askew General Surgeon Suite 19, Sunshine Coast University Private Hospital, 3 Doherty St Birtinya, Queensland 4575 Write questions or notes here: Document Title: Laparoscopic Sleeve Gastrectomy
Dr James Askew General Surgeon Suite 19, Sunshine Coast University Private Hospital, 3 Doherty St Birtinya, Queensland 4575 Write questions or notes here: Document Title: Laparoscopic Sleeve Gastrectomy
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Medications to help you quit smoking
 Medications to help you quit smoking How can medication help me quit smoking? Using medications can increase your chances of quitting smoking 2 to 3 times more than quitting without using medications.
Medications to help you quit smoking How can medication help me quit smoking? Using medications can increase your chances of quitting smoking 2 to 3 times more than quitting without using medications.
Recovery plan: radical cystectomy Information for patients
 Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Weight Loss Surgery. Our Surgeons. A Patient s Guide
 Our Surgeons Our bariatric surgeons and support staff provide the information and support necessary to achieve substantial and sustainable weight loss. Our surgeons: Weight Loss Surgery A Patient s Guide
Our Surgeons Our bariatric surgeons and support staff provide the information and support necessary to achieve substantial and sustainable weight loss. Our surgeons: Weight Loss Surgery A Patient s Guide
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Technical Aspects of Bariatric Surgical Procedures. Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital
 Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Dr Candice Silverman
 Dr Candice Silverman Suite 3 / 3 McLean Street Coolangatta, QLD 4225 Tel: 07 5536 8855 Write questions or notes here: Document Title: Laparoscopic Gastric Bypass Further Information and Feedback: Tell
Dr Candice Silverman Suite 3 / 3 McLean Street Coolangatta, QLD 4225 Tel: 07 5536 8855 Write questions or notes here: Document Title: Laparoscopic Gastric Bypass Further Information and Feedback: Tell
Laparoscopic Antireflux Surgery Information Sheet
 Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
Weight Loss Surgery Program
 Weight loss surgery helped me lose 112 pounds. Jennifer Weaver Weight Loss Surgery Program baylor university medical center at dallas Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When
Weight loss surgery helped me lose 112 pounds. Jennifer Weaver Weight Loss Surgery Program baylor university medical center at dallas Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When
Sleeve gastrectomy surgery
 Sleeve gastrectomy surgery Surgery is a serious step forward and should only be contemplated after you have undertaken considerable research into the various options. You should have discussed other options
Sleeve gastrectomy surgery Surgery is a serious step forward and should only be contemplated after you have undertaken considerable research into the various options. You should have discussed other options
Weight Loss Surgery Advisory
 PATIENT NAME: D.O.B.: / / INSTRUCTIONS: As you consider surgical treatment for morbid obesity, it is very important that you fully understand (1) the nature of your condition, (2) the types of surgical
PATIENT NAME: D.O.B.: / / INSTRUCTIONS: As you consider surgical treatment for morbid obesity, it is very important that you fully understand (1) the nature of your condition, (2) the types of surgical
Having a Gastric Band
 Having a Gastric Band Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2014. Document for issue as handout. This booklet aims to describe: l What is a gastric band page 2 l How is
Having a Gastric Band Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2014. Document for issue as handout. This booklet aims to describe: l What is a gastric band page 2 l How is
Tobacco Addiction. Why does it seem so hard to stop smoking? What's in cigarettes? What if I smoke just a few cigarettes a day?
 Tobacco Addiction Why does it seem so hard to stop smoking? Smoking causes changes in your body and in the way you act. The changes in your body are caused by an addiction to nicotine. The changes in the
Tobacco Addiction Why does it seem so hard to stop smoking? Smoking causes changes in your body and in the way you act. The changes in your body are caused by an addiction to nicotine. The changes in the
Nutrition After Weight Loss Surgery
 Nutrition After Weight Loss Surgery Gastric Bypass Sleeve Gastrectomy Gastric Banding HOW YOU WILL USE YOUR NEW TOOL SUCCESSFULLY TEXAS CENTER FOR MEDICAL & SURGICAL WEIGHT LOSS What We ll Cover Today
Nutrition After Weight Loss Surgery Gastric Bypass Sleeve Gastrectomy Gastric Banding HOW YOU WILL USE YOUR NEW TOOL SUCCESSFULLY TEXAS CENTER FOR MEDICAL & SURGICAL WEIGHT LOSS What We ll Cover Today
HOUSTON METHODIST SURGICAL WEIGHT LOSS
 HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Bariatric Surgery Guide
 One Bariatric Surgery Guide Get back to enjoying the everyday moments. Obesity is one of the nation s leading health issues. More than half of Americans are overweight and roughly 12 million Americans
One Bariatric Surgery Guide Get back to enjoying the everyday moments. Obesity is one of the nation s leading health issues. More than half of Americans are overweight and roughly 12 million Americans
Informed Consent for Laparoscopic Roux en Y Gastric Bypass. Patient Name
 Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Weight Loss Surgery A Patient s Guide
 Our Surgeons Ibrahim M. Ibrahim, MD, FACS, BSCOE Medical Director of Bariatric Surgery at Englewood Hospital Weight Loss Surgery A Patient s Guide Jeffrey W. Strain, MD, FACS, BSCOE Celinés Morales-Ribeiro,
Our Surgeons Ibrahim M. Ibrahim, MD, FACS, BSCOE Medical Director of Bariatric Surgery at Englewood Hospital Weight Loss Surgery A Patient s Guide Jeffrey W. Strain, MD, FACS, BSCOE Celinés Morales-Ribeiro,
Weight Loss Surgery and Bariatric Nutrition. Jeanine Giordano, MS, RD, CDN
 Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Eating Disorders. 1995-2012, The Patient Education Institute, Inc. www.x-plain.com mhf70101 Last reviewed: 06/29/2012 1
 Eating Disorders Introduction Eating disorders are illnesses that cause serious changes in a person s daily diet. This can include not eating enough food or overeating. Eating disorders affect about 70
Eating Disorders Introduction Eating disorders are illnesses that cause serious changes in a person s daily diet. This can include not eating enough food or overeating. Eating disorders affect about 70
Living and succeeding with a gastric band. Practical advice for patients
 Living and succeeding with a gastric band Practical advice for patients page 2 Living and succeeding with a gastric band Bariatric surgery (weight loss surgery) is currently the most effective treatment
Living and succeeding with a gastric band Practical advice for patients page 2 Living and succeeding with a gastric band Bariatric surgery (weight loss surgery) is currently the most effective treatment
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
Am I at Risk for type 2 Diabetes? Taking Steps to Lower the Risk of Getting Diabetes NATIONAL DIABETES INFORMATION CLEARINGHOUSE
 NATIONAL DIABETES INFORMATION CLEARINGHOUSE Am I at Risk for type 2 Diabetes? Taking Steps to Lower the Risk of Getting Diabetes U.S. Department of Health and Human Services National Institutes of Health
NATIONAL DIABETES INFORMATION CLEARINGHOUSE Am I at Risk for type 2 Diabetes? Taking Steps to Lower the Risk of Getting Diabetes U.S. Department of Health and Human Services National Institutes of Health
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
If you have any questions or concerns about your illness or your treatment, please contact your medical team.
 This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery
 Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Obesity Obesity is defined as having a body mass index (BMI) of 30 or greater. Obesity is a serious medical
Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Obesity Obesity is defined as having a body mass index (BMI) of 30 or greater. Obesity is a serious medical
If you have any questions or concerns about your illness or your treatment, please contact your medical team.
 This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
This booklet is designed to give you information about your operation. We hope it will answer some of the questions that you or those who care for you may have at this time. This booklet is not meant to
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Smoking and the risk of stroke
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Smoking and the risk of stroke Smoking greatly increases your chances of developing serious health conditions like stroke. Stopping smoking can significantly
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Smoking and the risk of stroke Smoking greatly increases your chances of developing serious health conditions like stroke. Stopping smoking can significantly
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
THE LAP BAND: IS IT THE BEST OPTION FOR YOU?
 Prof. Paul O Brien 2006. All rights reserved. THE LAP BAND: IS IT THE BEST OPTION FOR YOU? Key Points: The LAP BAND works primarily by inducing a sense of satiety Its best features are the adjustability,
Prof. Paul O Brien 2006. All rights reserved. THE LAP BAND: IS IT THE BEST OPTION FOR YOU? Key Points: The LAP BAND works primarily by inducing a sense of satiety Its best features are the adjustability,
Surgical Weight Loss Program for Teens
 Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Frequently Asked Questions: Gastric Bypass Surgery at CMC
 Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Bariatric Surgery 101
 Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Diabetes and Weight-Loss Surgery
 WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
Gastric Bypass Surgery
 Gastric Bypass Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Bypass Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Laparoscopic gastric banding
 Laparoscopic gastric banding What is laparoscopic gastric banding? Laparoscopic gastric banding is one of 3 main bariatric procedures offered here at Derby. It has a restrictive component which helps
Laparoscopic gastric banding What is laparoscopic gastric banding? Laparoscopic gastric banding is one of 3 main bariatric procedures offered here at Derby. It has a restrictive component which helps
