High Titre Anti-A/B Testing of Donors within NHS Blood and Transplant (NHSBT)
|
|
|
- Vivien Quinn
- 8 years ago
- Views:
Transcription
1 INFORMATION INF178/1.1 Effective: 10/08/11 Purpose To minimise the risk of causing clinically significant haemolysis due to the presence of high-titre anti-a or anti-b when plasma-rich blood components are transfused to patients of other blood groups. Method Review of the literature of cases of haemolytic episodes attributed to the transfusion of high-titre anti-a or anti-b, and of current practice in NHS Blood and Transplant (NHSBT). Recommendations made based on apparent critical titre levels from the literature and operational considerations. Recommendations were graded using Guidelines originating from the US Agency for Health Care Policy and Research (see Appendix). Status Original version (11) approved by the NBS Transfusion Medicine Clinical Policies Group on 18 th February Reviewed and revised November 2006 Reviewed and revised June 2011 Summary A recognised, though rare, complication of transfusion is acute haemolysis due to the passive transfusion of high titre anti-a or anti-b when plasma-rich components (almost always of Group O) are transfused to patients of Group A or B. No international consensus exists on the optimal testing method or titration that should be adopted to ensure that this complication does not occur. Review of the literature found 16 case reports in which significant haemolysis was attributed to hightitre anti-a or -B, one of which was fatal. In all cases, the titre of antibody exceeded 256 (Indirect Antiglobulin Test, IAT) or 128 (haemolysin titre) (Level of evidence III). Practice in the NBS prior to 2002 was for testing to be performed universally on the Olympus PK7200 automated blood grouper, but with varying dilutions and cut-off levels. Work in the Northern Zone (unpublished) had previously suggested that a 1/100 dilution is equivalent to a 1/128 saline titre, and approximately 5% of donations were found to be positive when this dilution was used as a cut-off level. Level of evidence III). A uniform testing strategy was adopted in 2002, which identified approximately 5% of donations as high-titre. (Grade B recommendation). This testing strategy has since been revised, and currently procedures now identify approximately 10% of donations as high titre. Clinicians should be aware of the risk of transfusing large volumes of Group O plasma (particularly in platelet components, and particularly to children) to non-group O patients. It is recommended that adverse haemolytic reactions thought to be due to high-titre ABO antibodies be reported to SABRE and SHOT. Author(s): Dr N Win Page 1 of 9
2 Introduction It has long been recognised that, although Group O red cells and platelets may be transfused to patients of any group, rarely the transfusion may be complicated by a haemolytic reaction due to the passive transfer of antibodies to A or B red cells 1,2 (particularly when platelets containing relatively large volumes of plasma are transfused). The majority of reports are of single cases, suggesting that this is a rare complication of transfusion 3-17 (Table 1). Five out of the twelve reported cases occurred in children, one of whom received a platelet transfusion from her mother with a fatal outcome 13. In all cases, there was a significant haemolytic reaction. In addition to published case reports, some indication of the relative frequency of problems due to passive antibody transfer is available from the Serious Hazards of Transfusion (SHOT) reporting scheme, which began in In the first 3 years of SHOT there were three reported cases of haemolysis suspected to be due to passive transfer of anti-a in platelet components, one in each annual report The first involved a group A patient and group O platelet transfusion, although subsequent investigation did not show that the platelet donor had high titre anti-a. In the second report, a group A patient was given 2 units of group O platelets prior to a haemolytic episode and anti- A was eluted from the red cells. No further information was available about the anti-a titre of the donors involved. In the third report, haemolysis occurred after transfusion of a unit of Group O platelets to a Group A patient. Although testing for haemolysins at saline 37 0 C had been performed and found negative, retrospective testing by IAT for IgG anti-a found a titre of 1 in 20, further cases have been reported up to ,22. An International Forum 23 asked experts from 16 countries what measures if any they took to prevent haemolysis following the transfusion of incompatible apheresis platelets. All countries responding recognised this to be a potential problem and had some measures in place to try to minimise the risk. Titration of anti-a/b In almost all of the case reports (see Table 1) further investigation of the donor s serum revealed a titre of at least 256 by IAT, and/or 128 haemolysin saline titre at room temperature. Mollison 24 reviews two early studies when group O plasma was deliberately transfused to group A volunteers. These studies found the lowest titres of anti-a to cause haemolysis were 512 and 640, and similar or greater levels than this were found in 40% and 23% of donors respectively. It is recognised that such haemolytic reactions may be prevented by screening to detect those donors who have high anti-a or anti-b titres, and ensuring that these components are not transfused to patients of other groups; however there has been very little consensus in the past on the method of screening or the effective cut-off level. The seventh edition of Guidelines for the Blood Transfusion Services in the United Kingdom 25 states that each Blood Establishment should have a testing and issuing policy to avoid the use of high-titre anti-a and / or anti-b in instances where a significant adverse clinical reaction is likely. It is recommended that a saline agglutination test should give a negative result at a dilution of 1/128 or an equivalent dilution by other techniques. Manual titration is well recognised to be an imprecise technique. Furthermore, the UK Transfusion Services now rely heavily on automated testing procedures, and it is no longer feasible to perform manual saline titration of IAT tests on all Group O donations. The challenge is to find an automated test (with electronic transmission of results) which can be performed routinely on all donations and which would reliably detect high titre antibodies at a level sensitive enough to prevent haemolysis in all recipients (including neonates), while at the same time not labelling more donors than necessary as high titre so that supply of components is compromised. Author(s): Dr Nay Win Page 2 of 9
3 In work performed at Leeds for the NHSBT Northern Zone Testing Managers Group (B. Keyworth - personal communication) it was shown that tests performed by saline against both A 1 B cells, and separate A 1 and B cells showed 31% of donors to be positive at a dilution of 1/32, and 6% at 1/128. Dilutions of 1/40 and 1/100 were then tested them on the Olympus PK7200, and 39% and 5% of donors were found to be positive respectively, i.e. very similar to the saline results. They concluded that the techniques were comparable and that testing using a 1/100 dilution on the Olympus was equivalent to a 1/128 titre. Current testing practice The NHSBT has now adopted a uniform test for haemolysins on the Olympus automated blood grouper, in which diluted A 2 B cells are tested against donor plasma. Using this test, approximately 90% of donations are designated negative for high-titre. All donations, irrespective of ABO group, are tested for the presence of high-titre anti-a and B. Labelling of components All components (red cells, platelets and frozen components), of all ABO groups, which are found to be negative for high-titre anti-a,b, are labelled as NEG: HT. This includes pooled platelets if all constituent donations are negative. The specification for neonatal components includes the requirement for donations to be high-titre anti- A,B negative. Components labelled as suitable for neonatal use are therefore negative for high-titre anti-a,b even though this may not be specifically stated on the label. Recommendations A national uniform approach to testing for high-titre anti-a and anti-b has been agreed and adopted. When deciding which cut-off dilution to adopt, the risk of losing a larger number of donations by using a lower titration has to be considered and balanced against any potential benefit. There have only been eight cases of possible haemolysis in the UK reported to SHOT during the past eight years. There may be some degree of under-reporting, but the risk does not appear to be excessive according to the available data, and is likely to be less than the risk of shortage of supply, particularly of platelets, if too many donations are excluded. Guidelines for the Blood Transfusion Services in the UK 25 recommend that There should be a procedure in place to collect and review testing and patient outcome data and to implement changes in policy in the light of continuing clinical experience with the plasma containing blood products issued. Data on acute transfusion reactions is collated by SHOT, and regular review of reports of haemolysis follwing platelet transfusion should be performed in order to provide feedback on the efficacy of the high titre testing procedure. A set of controls are under development, following recommendations for improving high titre testing in the UK made to the Joint Professional Advisory Committee of the UK Transfusion Services (JPAC) by the Standing Advisory Committees on Immunohaematology and Blood Components. These controls are designed to provide a positive and negative standard when tested on the Olympus Blood Grouper. If these controls are shown to work in practice, then use of them should help to standardise the procedure. Author(s): Dr Nay Win Page 3 of 9
4 Further precautions to reduce the risk of haemolysis Red cell transfusion British Committee for Standards in Haematology (BCSH) Guidelines for compatibility procedures in blood transfusion laboratories 26 state that red cells of the same ABO group as the patient should be selected wherever possible. This will remove the risk of haemolysis in addition to conserving Group O blood. If ABO identical is not available, group O blood may be used as long as it is negative for hightitre haemagglutinins. Group AB blood should be used for AB patients, but if it is not available then Group A or B, rather than group O red cells, should be used for blood conservation reasons. Platelet transfusion Even with uniform testing to prevent high-titre donations from being transfused to patients of blood groups other than O, there will still be a potential risk if large volumes of low titre plasma are transfused. This may be particularly likely in instances such as large volumes of double-dose HLA matched platelets being transfused daily to an individual, or where children are repeatedly transfused with adult doses of apheresis platelets. Pooled platelets theoretically pose a lesser risk; for a pool to be labelled high titre negative, all of the donations in that pool must have been found to be of low titre. Clinicians should be made aware of the potential for haemolysis in these circumstances. The Transfusion Medicine Clinical Policies Group document on ABO and RhD Compatibility in relation to Platelet Transfusions 27 provides the relevant information:- Platelet concentrates from donors of the same ABO group as the patient are the components of choice. Platelet recovery of both major and minor ABO incompatible platelet transfusions may be impaired to some extent, but this is not usually clinically significant. A more important consideration concerning donor ABO antibodies is the avoidance of acute haemolysis, which may occur after ABO-incompatible platelet transfusions, typically with transfusions of high titre anti-a to A 1 recipients. This problem has been particularly apparent in small children receiving apheresis platelet concentrates, which contain large volumes of plasma from single donors. It is preferable to use Group A platelets for Group B patients and vice versa rather than Group O if ABO identical platelets are not available. If these are also not available then Group O may be used, but in either case platelets should be selected which are labelled as hightitre negative as above. Plasma Transfusion Plasma components should preferably be ABO identical. If this is not possible, for example because of supply shortage when large volumes are required, they should always be ABO compatible i.e. group O plasma should only be given to group O recipients 28. It is even more critical that plasma for transfusion to neonates should be ABO compatible because of the increased risk of haemolysis due to their low plasma volume. Author(s): Dr Nay Win Page 4 of 9
5 Conclusion The risk of haemolysis due to passively transfused anti-a and anti-b is small but present, and should be considered in any situation in which relatively large volumes of incompatible plasma are transfused (including platelet components). It is important to recognise that, although testing for high titre ABO antibodies in blood donors may reduce the risk of HTR in out of group transfusion, it cannot be entirely eliminated through this route. Group O platelets can cause HTR even when tested and labelled negative for high-titre haemolysis. They should only be used for non-group O patients (particularly paediatric patients) as a last resort. Any suspected instance of haemolysis should be reported to the local Blood Centre, SABRE and SHOT so that further investigation can be performed and the effectiveness of the testing regime can be monitored. Author(s): Dr Nay Win Page 5 of 9
6 First author and Ref Table 1. Reported cases of haemolysis due to anti-a/b Year of public ation Recipi ent Group Don or Gro up Implicate d antibody Component transfused Keidan A O A Grp O whole blood Severe haemolytic leading to acute renal failure Zoes A int B O anti-a 1 10 units recovered platelets Inwood A O anti-a Almost whole unit of red cells (~ 95 ml plasma) McLeod A O anti-a 2 units recovered platelets Reaction ~ A/B titre Age of recipient Severe haemolytic. Free haemoglobin in serum & bilirubin Haemolytic with haemoglobulinaemia & haemoglobinuria Significant haemolytic Hb 14 8 Conway A O anti-a Apheresis platelets Haemolytic DIC (Donor was sister) Required haemodialysis Pierce A B O O anti-a anti-b Apheresis platelets 1 Gp O recovered platelet in pool with 5 Gp B Ferguson A O anti-a Recovered platelets x1 Severe haemolytic (Donor was mother) DIC & death Hb No acute reaction Hb in 7 days No haemoglobinaemia Acute haemolytic, red serum & urine, back pain. Hb 2.6 g/dl in 5 hrs. Reis B O anti-b Apheresis platelets Haemolytic. Hb Murphy A O anti-a HLA-matched platelets (448 ml) Boothe B O anti-b O cells resuspended in AB plasma Severe haemolysis, Hb g/dl, acute renal failure Severe haemolytic, temp, haemoglobinuria. (Neonatal exchange transfusion) Duguid A O anti-a Platelets Infant undergoing cardiac surgery. No acute reaction. Hb at 48 hrs Mair A O anti-a Apheresis platelets Severe haemolytic. Hb in 24 hrs. Barjas A O anti-a Red cells (approx. Castro ml plasma) Sapatnekar 17 Fever, back pain, haemoglobinaemia, Hb in 24 hours after 1 unit transfusion 2005 A O anti-a Apheresis platelets Shock, severe intravasc haemolysis Hb (after 2 units of O red cells) Sadani A O anti-a Apheresis platelets x 3 Haemoglobinuria and jaundice. Hb Renal failure H/L 128 agglut yrs 256 (pool of 44 yrs all donations) yrs Both donors (IAT) H/L titre (saline) (IAT) (Weak pos in saline at RT) 256 (IAT) > 4000 (IAT) 256 (RT) 45 yrs 15 yrs 2½ yrs 58 yrs 66 yrs 4096 (IAT) 56 yrs 256 (sal) 1024 (IAT) (sal) > 64,000 (IAT) 30 yrs 6 days 3200 (IAT) 5 weeks 128 (sal) 28 yrs 1024 (sal) 38 yrs 2048 (sal) (IAT) 640 (IAT) IgG alone yrs 65 yrs Author(s): Dr Nay Win Page 6 of 9
7 References (1) Gardner JM, Tovey GH. Potentially dangerous group-o blood: a screening test. Lancet. 1954;266: (2) Murphy S. ABO blood groups and platelet transfusion. Transfusion. 1988;28: (3) Boothe G, Brecher ME, Root M, Robinson J, Haley R. Acute hemolysis due to passively transfused high-titre anti B causing spontaneous in vitro agglutination. Immunohematology. 1995;11: (4) Duguid JK, Minards J, Bolton-Maggs PH. Lesson of the week: incompatible plasma transfusions and haemolysis in children. BMJ. 1999;318: (5) Conway LT, Scott EP. Acute hemolytic transfusion reaction due to ABO incompatible plasma in a plateletapheresis concentrate. Transfusion. 1984;24: (6) Ferguson DJ. Acute intravascular haemolysis after a platelet transfusion. Can Med Ass Journal. 1988;138: (7) Garratty G. Problems associated with passively transfused blood group alloantibodies. Am J Clin Pathol. 1998;109: (8) Inwood MJ, Zuliani B. Anti-A hemolytic transfusion with packed O cells. Ann Intern Med. 1978;89: (9) Keidan SE, Lohoar E, Mainwaring D. Acute anuria in a haemophiliac; due to transfusion of incompatible plasma. Lancet. 1966;1: (10) Mair B, Benson K. Evaluation of changes in hemoglobin levels associated with ABOincompatible plasma in apheresis platelets. Transfusion. 1998;38: (11) McLeod BC, Sassetti RJ, Weens JH, Vaithianathan T. Haemolytic transfusion reaction due to ABO incompatible plasma in a platelet concentrate. Scand J Haematol. 1982;28: (12) Murphy MF, Hook S, Waters AH et al. Acute haemolysis after ABO-incompatible platelet transfusions. Lancet. 1990;335: (13) Pierce RN, Reich LM, Mayer K. Hemolysis following platelet transfusions from ABOincompatible donors. Transfusion. 1985;25: (14) Zoes C, Dube VE, Miller HJ, Vye MV. Anti-A1 in the plasma of platelet concentrates causing a hemolytic reaction. Transfusion. 1977;17: (15) Sadani DT, Urbaniak SJ, Bruce M, Tighe JE. Repeat ABO-incompatible platelet transfusions leading to haemolytic transfusion reaction. Transfus Med. 2006;16: (16) Barjas-Castro ML, Locatelli MF, Carvalho MA, Gilli SO, Castro V. Severe immune haemolysis in a group A recipient of a group O red blood cell unit. Transfus Med. 2003;13: (17) Sapatnekar S, Sharma G, Downes KA et al. Acute hemolytic transfusion reaction in a pediatric patient following transfusion of apheresis platelets. J Clin Apher. 2005;20: Author(s): Dr Nay Win Page 7 of 9
8 (18) Williamson LM, Lowe S, Love E et al. Serious Hazards of Transfusion (SHOT) Annual Report Manchester: SHOT Office; (19) Williamson LM, Lowe S, Love E et al. Serious Hazards of Transfusion (SHOT) Annual Report Manchester: (20) Love EM, Williamson LM, Cohen H et al. Serious Hazards of Transfusion (SHOT) Annual Report Manchester: SHOT Office; (21) Stainsby D, Cohen H, Jones H et al. Serious Hazards of Transfusion (SHOT) Annual Report Manchester Blood Centre: Serious Hazards of Transfusion Office; (22) Stainsby D, Cohen H, Jones H et al. Serious Hazards of Transfusion (SHOT) Annual Report Manchester: SHOT Office; (23) Pietersz RNI, Engelfreit CP, Reesink HW. International Forum - Transfusion of apheresis platelets and ABO groups. Vox Sanguinis. 2005;88: (24) Klein HD, Anstee DJ. Red cell incompatibility in vivo. Blood Transfusion in Clinical Medicine. Oxford: Blackwell Publishing; 2005: (25) Joint UKBTS/NIBSC Professional Advisory Committee. Guidelines for the Blood Transfusion Services in the United Kingdom. 7 ed. Norwich: TSO; (26) Chapman JF, Elliott C, Knowles SM, Milkins CE, Poole GD. Guidelines for compatibility procedures in blood transfusion laboratories. Transfus Med. 2004;14: (27) Murphy MF. ABO and RhD compatibility in relation to platelet transfusions (28) O'Shaughnessy DF, Atterbury C, Bolton MP et al. Guidelines for the use of fresh-frozen plasma, cryoprecipitate and cryosupernatant. Br J Haematol. 2004;126: (29) Reis MD, Coovadia AS. Transfusion of ABO-incompatible platelets causing severe haemolytic reaction. Clin Lab Haematol. 1989;11: Author(s): Dr Nay Win Page 8 of 9
9 Appendix Key to evidence statements and grades of recommendations The definitions of the types of evidence and the grading of recommendations used in this guideline originate from the US Agency for Health Care Policy and Research and are set out in the following tables. STATEMENTS OF EVIDENCE Ia Ib IIa IIb III IV Evidence obtained from meta-analysis of randomised controlled trials. Evidence obtained from at least one randomised controlled trial. Evidence obtained from at least one well-designed controlled study without randomisation Evidence obtained from at least one other type of well-designed quasi-experimental study Evidence obtained from well-designed non-experimental descriptive studies, such as comparative studies, correlation studies and case studies. Evidence obtained from expert committee reports or opinions and/or clinical experiences of respected authorities. GRADES OF RECOMMENDATIONS A B C Requires at least one randomised controlled trial as part of a body of literature of overall good quality and consistency addressing the specific recommendation. (Evidence levels Ia, Ib) Requires the available of well conducted clinical studies but no randomised clinical trials on the topic of recommendation. (Evidence levels IIa, IIb, III) Requires evidence obtained from expert committee reports or opinions and/or clinical experiences of respected authorities. Indicates an absence of directly applicable clinical studies of good quality. (Evidence level IV) Author(s): Dr Nay Win Page 9 of 9
Selecting Appropriate Blood Products for Recipients of ABO/Rh Mismatched Stem Cell Transplants. Summary of Significant Changes. Purpose.
 This Specification replaces SPN/DDR/RC/023/05 (SPN215/1) Copy Number Summary of Significant Changes Change to new document reference numbers. Effective 18/10/11 Removal of ABO titres from sections 3.1
This Specification replaces SPN/DDR/RC/023/05 (SPN215/1) Copy Number Summary of Significant Changes Change to new document reference numbers. Effective 18/10/11 Removal of ABO titres from sections 3.1
CORD BLOOD EVALUATION
 CORD BLOOD EVALUATION Principle: When there is incompatibility between a mother s antibodies and an infant s red blood cell antigens, the infant is at risk of developing Hemolytic Disease of the Fetus
CORD BLOOD EVALUATION Principle: When there is incompatibility between a mother s antibodies and an infant s red blood cell antigens, the infant is at risk of developing Hemolytic Disease of the Fetus
1. BLOOD GROUP SYSTEMS. Page 1. Haematology LECTURE 10. BLOOD GROUPS AND TRANSFUSIONS OVERVIEW. 1. Blood Group Systems
 Undergraduate Course in Veterinary Clinical PathologySocrates Programme Haematology LECTURE 10. BLOOD GROUPS AND TRANSFUSIONS 10-1 OVERVIEW 1. Blood Group Systems 2. Blood group testing and cross-matching
Undergraduate Course in Veterinary Clinical PathologySocrates Programme Haematology LECTURE 10. BLOOD GROUPS AND TRANSFUSIONS 10-1 OVERVIEW 1. Blood Group Systems 2. Blood group testing and cross-matching
Introduction. Laboratory Procedure Manual
 Exercise 9 Elution Study Objectives: 1. State when an elution procedure may be performed. 2. List four situations in which the performance of an elution may provide helpful information. 3. List three types
Exercise 9 Elution Study Objectives: 1. State when an elution procedure may be performed. 2. List four situations in which the performance of an elution may provide helpful information. 3. List three types
Direct Antiglobulin Test (DAT)
 Exercise 8 Exercise 9 Direct Antiglobulin Test (DAT) Elution Study Task Aim Introduction To perform the DAT and elution procedure with correct interpretation of results. To perform with 100% accuracy the
Exercise 8 Exercise 9 Direct Antiglobulin Test (DAT) Elution Study Task Aim Introduction To perform the DAT and elution procedure with correct interpretation of results. To perform with 100% accuracy the
Direct Antiglobulin Test (DAT)
 Exercise 8 Direct Antiglobulin Test (DAT) Objectives: 1. State the purpose for performing the DAT. 2. State what a positive DAT indicates. 3. List the reagents which are used for performing the DAT. 4.
Exercise 8 Direct Antiglobulin Test (DAT) Objectives: 1. State the purpose for performing the DAT. 2. State what a positive DAT indicates. 3. List the reagents which are used for performing the DAT. 4.
BLOOD GROUP ANTIGENS AND ANTIBODIES
 BLOOD GROUP ANTIGENS AND ANTIBODIES Over 20 blood group systems having approximately 400 blood group antigens are currently recognised. The ABO and Rhesus (Rh) blood group systems are of major clinical
BLOOD GROUP ANTIGENS AND ANTIBODIES Over 20 blood group systems having approximately 400 blood group antigens are currently recognised. The ABO and Rhesus (Rh) blood group systems are of major clinical
Validation of column agglutination technology for blood group alloantibody titration
 Validation of column agglutination technology for blood group alloantibody titration Melanie J Adriaansen and Holly E Perry Abstract Objective: To compare the performance of column agglutination technology
Validation of column agglutination technology for blood group alloantibody titration Melanie J Adriaansen and Holly E Perry Abstract Objective: To compare the performance of column agglutination technology
EDUCATIONAL COMMENTARY ANTIBODY TITRATIONS
 EDUCATIONAL COMMENTARY ANTIBODY TITRATIONS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn
EDUCATIONAL COMMENTARY ANTIBODY TITRATIONS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn
How to effectively report to SABRE and SHOT. Richard Haggas Transfusion Quality Manager Richard.haggas@leedsth.nhs.uk
 How to effectively report to SABRE and SHOT Richard Haggas Transfusion Quality Manager Richard.haggas@leedsth.nhs.uk Remit To explain how to successfully report to both MHRA and SHOT through the SABRE
How to effectively report to SABRE and SHOT Richard Haggas Transfusion Quality Manager Richard.haggas@leedsth.nhs.uk Remit To explain how to successfully report to both MHRA and SHOT through the SABRE
Blood Physiology. Practical 4. Contents. Practical tasks. Erythrocytes The blood types
 Blood Physiology Practical 4 Contents Erythrocytes The blood types Practical tasks Determination of blood groups of the ABO system Determination of the Rhesus system (Rh factor) The cross matching test
Blood Physiology Practical 4 Contents Erythrocytes The blood types Practical tasks Determination of blood groups of the ABO system Determination of the Rhesus system (Rh factor) The cross matching test
TRANSFUSION MEDICINE
 TRANSFUSION MEDICINE Transfusion medicine is a one-month per year rotation for a total of three months. During each rotation the resident is exposed to the basic concepts of transfusion medicine. Specific
TRANSFUSION MEDICINE Transfusion medicine is a one-month per year rotation for a total of three months. During each rotation the resident is exposed to the basic concepts of transfusion medicine. Specific
QUICK REFERENCE TO BLOOD BANK TESTING
 QUICK REFERENCE TO BLOOD BANK TESTING All Blood bank Tests are performed on demand 24 hours a day, 7 days a week. Feto/Maternal Bleed Quantitation estimates will be available within 4 hours of blood bank
QUICK REFERENCE TO BLOOD BANK TESTING All Blood bank Tests are performed on demand 24 hours a day, 7 days a week. Feto/Maternal Bleed Quantitation estimates will be available within 4 hours of blood bank
REQUEST FOR TESTING TRANSFUSION SERVICES
 REQUEST FOR TESTING TRANSFUSION SERVICES 921 Terry Avenue Seattle, WA 98104-1256 TO REORDER FORMS CALL 425-656-3019 PSBC Tech PSBC ID / CL # Time Received See the back of this order form for sample requirements.
REQUEST FOR TESTING TRANSFUSION SERVICES 921 Terry Avenue Seattle, WA 98104-1256 TO REORDER FORMS CALL 425-656-3019 PSBC Tech PSBC ID / CL # Time Received See the back of this order form for sample requirements.
Immunohematology. Immunohematology. Blood Group Antigens
 Immunohematology Immunohematology Jeffrey S. Jhang, MD Assistant Director, Transfusion Medicine Demonstration of red cell antigen-red cell antibody reactions is the key to immunohematology Combination
Immunohematology Immunohematology Jeffrey S. Jhang, MD Assistant Director, Transfusion Medicine Demonstration of red cell antigen-red cell antibody reactions is the key to immunohematology Combination
Serotyping Techniques
 Serotyping Techniques Thomas A. Kruzel, M.T., N. D. Southwest College of Naturopathic Medicine & Health Sciences ABO Blood Groups Blood Group RBC Antigens Serum Antibodies Percentage O none Anti A & B
Serotyping Techniques Thomas A. Kruzel, M.T., N. D. Southwest College of Naturopathic Medicine & Health Sciences ABO Blood Groups Blood Group RBC Antigens Serum Antibodies Percentage O none Anti A & B
Wrong Blood In Tube The Tip of the Iceberg
 Wrong Blood In Tube The Tip of the Iceberg Dr Paula Bolton-Maggs SHOT Medical Director 14 th IHS Montréal SHOT Mission Statement (Serious Hazards of Transfusion) To improve patient safety in blood transfusion
Wrong Blood In Tube The Tip of the Iceberg Dr Paula Bolton-Maggs SHOT Medical Director 14 th IHS Montréal SHOT Mission Statement (Serious Hazards of Transfusion) To improve patient safety in blood transfusion
Comparing the Tube and Gel Techniques for ABO Antibody Titration, as Performed in Three European Centers 林 良 豐 100.07.18
 Comparing the Tube and Gel Techniques for ABO Antibody Titration, as Performed in Three European Centers 林 良 豐 100.07.18 Introduction Data from 60 consecutive ABO-incompatible kidney transplantations performed
Comparing the Tube and Gel Techniques for ABO Antibody Titration, as Performed in Three European Centers 林 良 豐 100.07.18 Introduction Data from 60 consecutive ABO-incompatible kidney transplantations performed
Guidelines for pre-transfusion compatibility procedures in blood transfusion laboratories.
 Guidelines for pre-transfusion compatibility procedures in blood transfusion laboratories. British Committee for Standards in Haematology Address for correspondence: BCSH Secretary British Society for
Guidelines for pre-transfusion compatibility procedures in blood transfusion laboratories. British Committee for Standards in Haematology Address for correspondence: BCSH Secretary British Society for
Chapter 18. Blood Types
 Chapter 18 Blood Types Blood Types blood types and transfusion compatibility are a matter of interactions between plasma proteins and erythrocytes Karl Landsteiner discovered blood types A, B and O in
Chapter 18 Blood Types Blood Types blood types and transfusion compatibility are a matter of interactions between plasma proteins and erythrocytes Karl Landsteiner discovered blood types A, B and O in
Validation. Richard Haggas Quality Manager, Blood Transfusion Department Leeds and Bradford Teaching Hospitals
 Validation. Richard Haggas Quality Manager, Blood Transfusion Department Leeds and Bradford Teaching Hospitals What do we mean by validation? The establishment of documented and objective evidence that
Validation. Richard Haggas Quality Manager, Blood Transfusion Department Leeds and Bradford Teaching Hospitals What do we mean by validation? The establishment of documented and objective evidence that
Haemolytic disease of the newborn. 09.06.2016 Burak Salgin
 Haemolytic disease of the newborn 09.06.2016 Burak Salgin Innovation and excellence in health and care Addenbrooke s Hospital I Rosie Hospital Haemolytic disease of the newborn......used to be synonymous
Haemolytic disease of the newborn 09.06.2016 Burak Salgin Innovation and excellence in health and care Addenbrooke s Hospital I Rosie Hospital Haemolytic disease of the newborn......used to be synonymous
Blood Type Testing Lab Report Section 1101 Nattanit Trakullapphan (Nam) Chawalnrath Wongdeshanan (Kat)
 Blood Type Testing Lab Report Section 1101 Nattanit Trakullapphan (Nam) Chawalnrath Wongdeshanan (Kat) Introduction: figure 1.1 (Blood type n.d.) figure 1.2 (Blood type, Antigens-Antibodies n.d.) Multiple
Blood Type Testing Lab Report Section 1101 Nattanit Trakullapphan (Nam) Chawalnrath Wongdeshanan (Kat) Introduction: figure 1.1 (Blood type n.d.) figure 1.2 (Blood type, Antigens-Antibodies n.d.) Multiple
Mother s blood test to check her unborn baby s blood group
 Mother s blood test to check her unborn baby s blood group This leaflet explains why it is important to have a blood test to check the baby s blood group, so that only those who need it, receive anti-d
Mother s blood test to check her unborn baby s blood group This leaflet explains why it is important to have a blood test to check the baby s blood group, so that only those who need it, receive anti-d
STANDARD OPERATING PROCEDURE FOR RESOLVING ABO & Rh BLOOD GROUP DISCREPANCIES
 STANDARD OPERATING PROCEDURE FOR RESOLVING ABO & Rh BLOOD GROUP DISCREPANCIES TITLE: STANDARD OPERATING PROCEDURE FOR RESOLVING ABO & RH BLOOD GROUP DISCREPANCIES 1.0 Principle 1.1 To resolve ABO and Rh
STANDARD OPERATING PROCEDURE FOR RESOLVING ABO & Rh BLOOD GROUP DISCREPANCIES TITLE: STANDARD OPERATING PROCEDURE FOR RESOLVING ABO & RH BLOOD GROUP DISCREPANCIES 1.0 Principle 1.1 To resolve ABO and Rh
Role of the Medical Director
 Role of the Medical Director Beth Shaz, MD Assistant Professor, Emory University School of Medicine Director, Transfusion Services, Grady Memorial Hospital Atlanta, GA 1.1.1 Medical Director Responsibilities
Role of the Medical Director Beth Shaz, MD Assistant Professor, Emory University School of Medicine Director, Transfusion Services, Grady Memorial Hospital Atlanta, GA 1.1.1 Medical Director Responsibilities
Suggestions for Optimizing Use of Plasma in the Era of TRALI Risk Reduction
 Suggestions for Optimizing Use of Plasma in the Era of TRALI Risk Reduction March 27, 2014 Steve Kleinman, MD TRALI: A brief history Identified as a non-infectious serious hazard of transfusion in the
Suggestions for Optimizing Use of Plasma in the Era of TRALI Risk Reduction March 27, 2014 Steve Kleinman, MD TRALI: A brief history Identified as a non-infectious serious hazard of transfusion in the
Time Frame 15 minutes. Student should strive to be able to perform multiple procedures simultaneously.
 Name Direct Antiglobulin Test (DAT) (Direct Coombs) Principle The DAT detects the in vivo sensitization of RBC with IgG incomplete or non-agglutinating antibodies. After thorough washing of RBC with saline
Name Direct Antiglobulin Test (DAT) (Direct Coombs) Principle The DAT detects the in vivo sensitization of RBC with IgG incomplete or non-agglutinating antibodies. After thorough washing of RBC with saline
Can receive blood from: * I A I A and I A i o Type A Yes No A or AB A or O I B I B and I B i o Type B No Yes B or AB B or O
 Genetics of the ABO Blood Groups written by J. D. Hendrix Learning Objectives Upon completing the exercise, each student should be able: to explain the concept of blood group antigens; to list the genotypes
Genetics of the ABO Blood Groups written by J. D. Hendrix Learning Objectives Upon completing the exercise, each student should be able: to explain the concept of blood group antigens; to list the genotypes
ABO-Rh Blood Typing Using Neo/BLOOD
 ABO-Rh Blood Typing Using Neo/BLOOD Objectives Determine the ABO and Rh blood type of unknown simulated blood samples. Prepare a simulated blood smear. Examine a prepared blood smear under the microscope
ABO-Rh Blood Typing Using Neo/BLOOD Objectives Determine the ABO and Rh blood type of unknown simulated blood samples. Prepare a simulated blood smear. Examine a prepared blood smear under the microscope
MANAGEMENT OF DIRECT ANTIGLOBULIN TEST (DAT) POSITIVE INFANTS NEONATAL CLINICAL GUIDELINE
 MANAGEMENT OF DIRECT ANTIGLOBULIN TEST (DAT) POSITIVE INFANTS NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1. To provide monitoring and treatment guidance for medical and nursing staff
MANAGEMENT OF DIRECT ANTIGLOBULIN TEST (DAT) POSITIVE INFANTS NEONATAL CLINICAL GUIDELINE 1. Aim/Purpose of this Guideline 1.1. To provide monitoring and treatment guidance for medical and nursing staff
Blood Group Incompatibility
 Joyce Poole, International Blood Group Reference Laboratory, Bristol, UK Blood group antibodies present in plasma can bind with blood group antigens on red cells and cause a reaction (blood group incompatibility).
Joyce Poole, International Blood Group Reference Laboratory, Bristol, UK Blood group antibodies present in plasma can bind with blood group antigens on red cells and cause a reaction (blood group incompatibility).
Blood Typing Laboratory Exercise 40
 Blood Typing Laboratory Exercise 40 Background Blood typing involves identifying protein substances called antigens that are present in red blood cell membranes. Although there are many different antigens
Blood Typing Laboratory Exercise 40 Background Blood typing involves identifying protein substances called antigens that are present in red blood cell membranes. Although there are many different antigens
MLT 118L Clinical Immunology/Immunohematology Lab
 Page 1 of 5 MLT 118L Clinical Immunology/Immunohematology Lab Approval Date: Effective Term: Department: MEDICAL LABORATORY TECHNICIAN Division: Allied Health/Public Safety Units: 1.00 Grading Option:
Page 1 of 5 MLT 118L Clinical Immunology/Immunohematology Lab Approval Date: Effective Term: Department: MEDICAL LABORATORY TECHNICIAN Division: Allied Health/Public Safety Units: 1.00 Grading Option:
Blood Stains at the Crime Scene Forensic Investigation
 Blood Stains at the Crime Scene Forensic Investigation Introduction Blood stains at a crime scene can be crucial in solving the crime. Numerous analytical techniques can be used to study blood stains.
Blood Stains at the Crime Scene Forensic Investigation Introduction Blood stains at a crime scene can be crucial in solving the crime. Numerous analytical techniques can be used to study blood stains.
Information for patients needing irradiated blood
 Information for patients needing irradiated blood Patient information I am at risk of transfusion-associated graft-versus-host disease If I need to have a blood transfusion, cellular blood components (Red
Information for patients needing irradiated blood Patient information I am at risk of transfusion-associated graft-versus-host disease If I need to have a blood transfusion, cellular blood components (Red
CHAPTER 10 BLOOD GROUPS: ABO AND Rh
 CHAPTER 10 BLOOD GROUPS: ABO AND Rh The success of human blood transfusions requires compatibility for the two major blood group antigen systems, namely ABO and Rh. The ABO system is defined by two red
CHAPTER 10 BLOOD GROUPS: ABO AND Rh The success of human blood transfusions requires compatibility for the two major blood group antigen systems, namely ABO and Rh. The ABO system is defined by two red
Guidance for Industry and FDA Review Staff on Collection of Platelets by Automated Methods
 Guidance for Industry and FDA Review Staff on Collection of Platelets by Automated Methods Blood Products Advisory Committee, March 9, 2006 Steven Kleinman, MD Senior Medical Advisor, AABB Co-chair, AABB
Guidance for Industry and FDA Review Staff on Collection of Platelets by Automated Methods Blood Products Advisory Committee, March 9, 2006 Steven Kleinman, MD Senior Medical Advisor, AABB Co-chair, AABB
ASPIRATION ASPIRATIO 09 HSA ANNUAL REPORT 10
 ASPIRATION ASPIRATIO ASPIRATION 09 HSA ANNUAL REPORT 10 NBLOOD SERVICES GROUP The Blood Services Group is dedicated to securing the safety and stability of Singapore s blood supply. Our stringent quality
ASPIRATION ASPIRATIO ASPIRATION 09 HSA ANNUAL REPORT 10 NBLOOD SERVICES GROUP The Blood Services Group is dedicated to securing the safety and stability of Singapore s blood supply. Our stringent quality
Indications 18 : PLATELET TRANSFUSION, ALLOIMMUNIZATION AND MANAGEMENT OF PLATELET REFRACTORINESS
 18 : PLATELET TRANSFUSION, ALLOIMMUNIZATION AND MANAGEMENT OF PLATELET REFRACTORINESS Alan Tinmouth Platelets are the smallest of the blood cells, with a diameter of 2 3 µm and no nucleus. Their function
18 : PLATELET TRANSFUSION, ALLOIMMUNIZATION AND MANAGEMENT OF PLATELET REFRACTORINESS Alan Tinmouth Platelets are the smallest of the blood cells, with a diameter of 2 3 µm and no nucleus. Their function
Mark Yazer, MD FRCPC. The Institute For Transfusion Medicine Department of Pathology, University of Pittsburgh
 Medical Aspects of the Pittsburgh Centralized Transfusion Service Mark Yazer, MD FRCPC The Institute For Transfusion Medicine Department of Pathology, University of Pittsburgh Pittsburgh ITXM is the parent
Medical Aspects of the Pittsburgh Centralized Transfusion Service Mark Yazer, MD FRCPC The Institute For Transfusion Medicine Department of Pathology, University of Pittsburgh Pittsburgh ITXM is the parent
Health Service Circular
 Health Service Circular Series Number: HSC 2002/009 Issue Date: 04 July 2002 Review Date: 04 July 2005 Category: Public Health Status: Action sets out a specific action on the part of the recipient with
Health Service Circular Series Number: HSC 2002/009 Issue Date: 04 July 2002 Review Date: 04 July 2005 Category: Public Health Status: Action sets out a specific action on the part of the recipient with
Comparison of test tube, gel column agglutination and solid phase red cell adherence methods
 Comparison of test tube, gel column agglutination and solid phase red cell adherence methods with and without drug added for detection of drug-dependent antibodies Phyllis Kirchner, MT(ASCP)SH, SBB ABSTRACT
Comparison of test tube, gel column agglutination and solid phase red cell adherence methods with and without drug added for detection of drug-dependent antibodies Phyllis Kirchner, MT(ASCP)SH, SBB ABSTRACT
Unit 8 Pretransfusion Compatibility Testing
 Unit 8 Pretransfusion Compatibility Testing A. The purpose of pretransfusion testing is to select, for each recipient, blood components that, when transfused, will have acceptable survival and will not
Unit 8 Pretransfusion Compatibility Testing A. The purpose of pretransfusion testing is to select, for each recipient, blood components that, when transfused, will have acceptable survival and will not
- Lessons from SHOT Haemorrhage cases
 - Lessons from SHOT Haemorrhage cases Tony Davies Patient Blood Management Practitioner SHOT / NHSBT Patient Blood Management Team SHOT Annual Symposium 2013 For action by Trusts by April 2011 Decision
- Lessons from SHOT Haemorrhage cases Tony Davies Patient Blood Management Practitioner SHOT / NHSBT Patient Blood Management Team SHOT Annual Symposium 2013 For action by Trusts by April 2011 Decision
BLOOD BANK Department
 BLOOD BANK Department INTRODUCTION Blood products used at Saint Michael s Hospital are obtained from the BloodCenter of Wisconsin. There is no charge for the blood, but there is a fee for testing and processing
BLOOD BANK Department INTRODUCTION Blood products used at Saint Michael s Hospital are obtained from the BloodCenter of Wisconsin. There is no charge for the blood, but there is a fee for testing and processing
Hemolysis. Intravascular vs. Extravascular. Classification. Warm vs. Cold Auto. Warm Auto. WAIHA Serologic Investigation
 Positive Direct Antiglobulin Test and Autoimmune Hemolytic Anemias Jeffrey S. Jhang, M.D. Assistant Professor of Clinical Pathology College of Physicians and Surgeons of Columbia University Direct Antiglobulin
Positive Direct Antiglobulin Test and Autoimmune Hemolytic Anemias Jeffrey S. Jhang, M.D. Assistant Professor of Clinical Pathology College of Physicians and Surgeons of Columbia University Direct Antiglobulin
Donor Adverse Events
 Donor Adverse Events Common terminology Frequency Risk factors Hold still, Mrs. Brown, while I draw your blood Mindy Goldman, MD Canadian Blood Services IHN Seminar, Paris March 11, 2016 Outline Donor
Donor Adverse Events Common terminology Frequency Risk factors Hold still, Mrs. Brown, while I draw your blood Mindy Goldman, MD Canadian Blood Services IHN Seminar, Paris March 11, 2016 Outline Donor
RhD typing. Practice for IV year medical students. Zita Csernus MD. National Blood Transfusion Service Blood Transfusion Centre Pécs
 immunisation Bed side test Antibody tests RhD typing Practice for IV year medical students Zita Csernus MD National Blood Transfusion Service Blood Transfusion Centre Pécs Rh Blood Group System Discovery:
immunisation Bed side test Antibody tests RhD typing Practice for IV year medical students Zita Csernus MD National Blood Transfusion Service Blood Transfusion Centre Pécs Rh Blood Group System Discovery:
Standardization and Evaluation of IgA and IgM Gel Column Agglutination for Direct Antiglobulin Testing
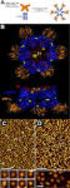 Standardization and Evaluation of IgA and IgM Gel Column Agglutination for Direct Antiglobulin Testing ABSTRACT BACKGROUND: Diagnosis of autoimmune hemolytic anemia is commonly confirmed with a positive
Standardization and Evaluation of IgA and IgM Gel Column Agglutination for Direct Antiglobulin Testing ABSTRACT BACKGROUND: Diagnosis of autoimmune hemolytic anemia is commonly confirmed with a positive
Transfusion Medicine GUIDELINES SUMMARY BACKGROUND
 Transfusion Medicine GUIDELINES UK Transfusion Laboratory Collaborative: minimum standards for staff qualifications, training, competency and the use of information technology in hospital transfusion laboratories
Transfusion Medicine GUIDELINES UK Transfusion Laboratory Collaborative: minimum standards for staff qualifications, training, competency and the use of information technology in hospital transfusion laboratories
JOINT COMMISSION INTERNATIONAL ACCREDITATION STANDARDS FOR. 2nd Edition
 JOINT COMMISSION INTERNATIONAL ACCREDITATION STANDARDS FOR CliniCAl laboratories 2nd Edition Effective 1 April 2010 International Patient Safety Goals (IPSG) Goals The following is a list of all goals.
JOINT COMMISSION INTERNATIONAL ACCREDITATION STANDARDS FOR CliniCAl laboratories 2nd Edition Effective 1 April 2010 International Patient Safety Goals (IPSG) Goals The following is a list of all goals.
Women, Children and Sexual Health Division Maternity Services. Guideline: Anti D- Prophylaxis
 Women, Children and Sexual Health Division Maternity Services Guideline: Anti D- Prophylaxis 1. Introduction The National Institute for Clinical Excellence recommend routine antenatal anti-d prophylaxis
Women, Children and Sexual Health Division Maternity Services Guideline: Anti D- Prophylaxis 1. Introduction The National Institute for Clinical Excellence recommend routine antenatal anti-d prophylaxis
STANDARD OPERATING PROCEDURE FOR THE DIRECT ANTIGLOBULIN TEST
 STANDARD OPERATING PROCEDURE FOR THE DIRECT ANTIGLOBULIN TEST TITLE: Standard Operating Procedure for Performing the Direct Antiglobulin Test 1.0 Principle To detect in vivo sensitization of red blood
STANDARD OPERATING PROCEDURE FOR THE DIRECT ANTIGLOBULIN TEST TITLE: Standard Operating Procedure for Performing the Direct Antiglobulin Test 1.0 Principle To detect in vivo sensitization of red blood
Blood Transfusion. There are three types of blood cells: Red blood cells. White blood cells. Platelets.
 Blood Transfusion Introduction Blood transfusions can save lives. Every second, someone in the world needs a blood transfusion. Blood transfusions can replace the blood lost from a serious injury or surgery.
Blood Transfusion Introduction Blood transfusions can save lives. Every second, someone in the world needs a blood transfusion. Blood transfusions can replace the blood lost from a serious injury or surgery.
Antibody Identification. Part 1. Prerequisites. When Do We I.D.? Part 1: The Basics. A Blood Bank Guy Video Podcast
 Antibody Identification Part : The Basics A Blood Bank Guy Video Podcast D. Joe Chaffin, MD March Part Prerequisites Geography of a panel Antibody ID method Case examples Prerequisites When Do We I.D.?
Antibody Identification Part : The Basics A Blood Bank Guy Video Podcast D. Joe Chaffin, MD March Part Prerequisites Geography of a panel Antibody ID method Case examples Prerequisites When Do We I.D.?
Red blood cell transfusions in the Netherlands Towards (very) low use
 Red blood cell transfusions in the Netherlands Towards (very) low use Marian G.J. van Kraaij, MD PhD hematologist/ transfusion medicine specialist Director Dept Transfusion Medicine Sanquin Blood Supply,
Red blood cell transfusions in the Netherlands Towards (very) low use Marian G.J. van Kraaij, MD PhD hematologist/ transfusion medicine specialist Director Dept Transfusion Medicine Sanquin Blood Supply,
INSTRUCTIONS FOR USE
 Blood Grouping Reagent A/B/D Monoclonal and Reverse Grouping Card MTS080515 Intended Use For the performance of a forward and reverse ABO and D antigen grouping on a single Gel Card For use with the ID-Micro
Blood Grouping Reagent A/B/D Monoclonal and Reverse Grouping Card MTS080515 Intended Use For the performance of a forward and reverse ABO and D antigen grouping on a single Gel Card For use with the ID-Micro
1. To permit the resident to attain expertise in the methodological, diagnostic and scientific aspects of transfusion medicine and coagulation.
 BLOOD BANK CORE ROTATION Introduction The core rotation in blood banking is designed to expose the resident to a wide range of transfusion medicine and coagulation problems and provide training in solving
BLOOD BANK CORE ROTATION Introduction The core rotation in blood banking is designed to expose the resident to a wide range of transfusion medicine and coagulation problems and provide training in solving
INDICATIONS FOR BLOOD PRODUCT TRANSFUSIONS
 INDICATIONS FOR BLOOD PRODUCT TRANSFUSIONS Sarah Perry, LVT, BS, VTS (ECC) Licensed Veterinary Technician Animal Neurology, Rehabilitation and Emergency Center 1120 Welch Rd. Commerce, MI 48390 A very
INDICATIONS FOR BLOOD PRODUCT TRANSFUSIONS Sarah Perry, LVT, BS, VTS (ECC) Licensed Veterinary Technician Animal Neurology, Rehabilitation and Emergency Center 1120 Welch Rd. Commerce, MI 48390 A very
2nd Ed. 2004. Prepared by. Scientific Subcommittee of the Australian & New Zealand Society of Blood Transfusion Inc
 G u i d e l i n e s f o r B l o o d G r o u p i n g & A n t i b o d y S c r e e n i n g i n t h e A n t e n a t a l & P e r i n a t a l S e t t i n g 2nd Ed. 2004 Prepared by Scientific Subcommittee of
G u i d e l i n e s f o r B l o o d G r o u p i n g & A n t i b o d y S c r e e n i n g i n t h e A n t e n a t a l & P e r i n a t a l S e t t i n g 2nd Ed. 2004 Prepared by Scientific Subcommittee of
LAB 1 - Direct agglutination. Serology-the study of the in vitro reactions between antibody and antigen
 LAB 1 - Direct agglutination Serology-the study of the in vitro reactions between antibody and antigen Serological reaction: - quantitative (weight/volume) - qualitative Agglutination - the aggregation
LAB 1 - Direct agglutination Serology-the study of the in vitro reactions between antibody and antigen Serological reaction: - quantitative (weight/volume) - qualitative Agglutination - the aggregation
Evaluation of the Patient with Suspected Platelet Refractory State
 Evaluation of the Patient with Suspected Platelet Refractory State NOTE: While evaluating the patient for suspected immune refractory state provide ABO matched platelets if available. 1. Determine if the
Evaluation of the Patient with Suspected Platelet Refractory State NOTE: While evaluating the patient for suspected immune refractory state provide ABO matched platelets if available. 1. Determine if the
ABO-Rh Blood Typing With Synthetic Blood
 70-0101 ABO-Rh Blood Typing With Synthetic Blood Teacher s Manual World-Class Support for Science & Math The ability to type blood is an invaluable tool in the fields of medicine and criminology. Using
70-0101 ABO-Rh Blood Typing With Synthetic Blood Teacher s Manual World-Class Support for Science & Math The ability to type blood is an invaluable tool in the fields of medicine and criminology. Using
HUMAN BLOOD TYPE: TESTING FOR ABO AND Rh FACTORS STANDARDS 3.3.7.B, 3.3.7.C 3.3.10.B, 3.3.10.C
 HUMN LOOD TYPE: TESTING FOR O ND FCTORS STNDRDS 3.3.7., 3.3.7.C 3.3.10., 3.3.10.C Westminster College INTRODUCTION lood is a living tissue which circulates through the human body providing oxygen and nutrients
HUMN LOOD TYPE: TESTING FOR O ND FCTORS STNDRDS 3.3.7., 3.3.7.C 3.3.10., 3.3.10.C Westminster College INTRODUCTION lood is a living tissue which circulates through the human body providing oxygen and nutrients
HiPer Blood Grouping Teaching Kit
 HiPer Blood Grouping Teaching Kit Product Code: HTI008 Number of experiments that can be performed: 100 Duration of Experiment: Protocol: 15 minutes Storage Instructions: The kit is stable for 6 months
HiPer Blood Grouping Teaching Kit Product Code: HTI008 Number of experiments that can be performed: 100 Duration of Experiment: Protocol: 15 minutes Storage Instructions: The kit is stable for 6 months
Guidelines for the Blood Transfusion Services in the United Kingdom
 Guidelines for the Blood Transfusion Services in the United Kingdom 7 th Edition 2005 London: TSO Published by TSO (The Stationery Office) and available from: Online www.tsoshop.co.uk Mail,Telephone, Fax
Guidelines for the Blood Transfusion Services in the United Kingdom 7 th Edition 2005 London: TSO Published by TSO (The Stationery Office) and available from: Online www.tsoshop.co.uk Mail,Telephone, Fax
NHSBT Portfolio of Blood Components and Guidance for their Clinical Use. Summary of Significant Changes. Purpose. Definitions. Applicable Documents
 This replaces SPN223/6.1 Copy Number Summary of Significant Changes Effective: 22/09/2014 Correction of pooled platelet pathogen inactivated description against the component barcode. Also clarification
This replaces SPN223/6.1 Copy Number Summary of Significant Changes Effective: 22/09/2014 Correction of pooled platelet pathogen inactivated description against the component barcode. Also clarification
BLOOD BANK SPECIMEN COLLECTION PROCEDURE
 BLOOD BANK SPECIMEN COLLECTION PROCEDURE INTRODUCTION Scientific and technical advances in blood group serology have made the transfusion of blood a relatively safe procedure, but serious adverse effects
BLOOD BANK SPECIMEN COLLECTION PROCEDURE INTRODUCTION Scientific and technical advances in blood group serology have made the transfusion of blood a relatively safe procedure, but serious adverse effects
The Blood Budget: how can we reduce costs and influence best practice? Sue Redfearn Blood Transfusion Manager Poole Hospital NHS Foundation Trust
 The Blood Budget: how can we reduce costs and influence best practice? Sue Redfearn Blood Transfusion Manager Poole Hospital NHS Foundation Trust Poole Hospital vital statistics 680 beds 2011 (reduced
The Blood Budget: how can we reduce costs and influence best practice? Sue Redfearn Blood Transfusion Manager Poole Hospital NHS Foundation Trust Poole Hospital vital statistics 680 beds 2011 (reduced
Guideline on the Administration of Blood Components
 Guideline on the Administration of Blood Components British Committee for Standards in Haematology Address for correspondence: BCSH Secretary British Society for Haematology 100 White Lion Street London
Guideline on the Administration of Blood Components British Committee for Standards in Haematology Address for correspondence: BCSH Secretary British Society for Haematology 100 White Lion Street London
Administering blood transfusion
 Administering blood transfusion 1 Cherry Buckwell, CETL Interprofessional Clinical Skills Facilitator Is it safe? Approximately 3.34 million blood products are transfused each year in the UK. Blood transfusions
Administering blood transfusion 1 Cherry Buckwell, CETL Interprofessional Clinical Skills Facilitator Is it safe? Approximately 3.34 million blood products are transfused each year in the UK. Blood transfusions
FDA Considerations Regarding Frequent Plasma Collection Procedures
 FDA Considerations Regarding Frequent Plasma Collection Procedures Alan E. Williams, Ph.D. Office of Blood Research and Review Center for Biologics Evaluation and Research US Food and Drug Administration
FDA Considerations Regarding Frequent Plasma Collection Procedures Alan E. Williams, Ph.D. Office of Blood Research and Review Center for Biologics Evaluation and Research US Food and Drug Administration
Department of Transfusion Medicine and Immunohematology
 Department of Transfusion Medicine and Immunohematology Activities Transfusion medicine is a multidisciplinary area concerned with the proper use of blood and blood components in the treatment of human
Department of Transfusion Medicine and Immunohematology Activities Transfusion medicine is a multidisciplinary area concerned with the proper use of blood and blood components in the treatment of human
Recommendations to Transplant Centres Performing Cord Blood Transplants. Why Choosing the Right Thaw Method Could Save a Patient s Life
 Recommendations to Transplant Centres Performing Cord Blood Transplants Vicki Antonenas Why Choosing the Right Thaw Method Could Save a Patient s Life Lynn O Donnell (USA) 1 The process of receiving, testing
Recommendations to Transplant Centres Performing Cord Blood Transplants Vicki Antonenas Why Choosing the Right Thaw Method Could Save a Patient s Life Lynn O Donnell (USA) 1 The process of receiving, testing
Safe Blood Sampling Training Package
 Better Blood Transfusion - Education Programme Safe Blood Sampling Training Package SBS Training Package version 2010 to SNBTS www.learnbloodtransfusion.org.uk Learning Outcomes Following this session
Better Blood Transfusion - Education Programme Safe Blood Sampling Training Package SBS Training Package version 2010 to SNBTS www.learnbloodtransfusion.org.uk Learning Outcomes Following this session
THE PREPARATION OF SINGLE DONOR CRYOPRECIPITATE
 FACTS AND FIGURES JUNE 2004 NO 2 THE PREPARATION OF SINGLE DONOR CRYOPRECIPITATE Revised Edition Shân Lloyd National Blood Transfusion Service Zimbabwe Published by the World Federation of Hemophilia (WFH);
FACTS AND FIGURES JUNE 2004 NO 2 THE PREPARATION OF SINGLE DONOR CRYOPRECIPITATE Revised Edition Shân Lloyd National Blood Transfusion Service Zimbabwe Published by the World Federation of Hemophilia (WFH);
Northern Ireland Blood Transfusion Service
 DD:836:03:NIBT Page 1 of 7 Northern Ireland Blood Transfusion Service Job Ref: Title of Post: Location: Department: Band: 6 Hours: Job Description Biomedical Scientist Rotational Laboratories 37.5 hours
DD:836:03:NIBT Page 1 of 7 Northern Ireland Blood Transfusion Service Job Ref: Title of Post: Location: Department: Band: 6 Hours: Job Description Biomedical Scientist Rotational Laboratories 37.5 hours
Transplant Options When You Don t Have a Good Match
 Transplant Options When You Don t Have a Good Match 1 Transplant Options When You Don t Have a Good Match Being told you need a transplant may bring about many feelings, including anxiety and uncertainty.
Transplant Options When You Don t Have a Good Match 1 Transplant Options When You Don t Have a Good Match Being told you need a transplant may bring about many feelings, including anxiety and uncertainty.
PROTOCOL FOR THE MANAGEMENT OF CLOSE CONTACTS OF PERTUSSIS INFECTION
 PROTOCOL FOR THE MANAGEMENT OF CLOSE CONTACTS OF PERTUSSIS INFECTION Printed copies must not be considered the definitive version DOCUMENT CONTROL PROTOCOL NO. 1.03 Policy Group Infection Control Committee
PROTOCOL FOR THE MANAGEMENT OF CLOSE CONTACTS OF PERTUSSIS INFECTION Printed copies must not be considered the definitive version DOCUMENT CONTROL PROTOCOL NO. 1.03 Policy Group Infection Control Committee
Platelet antigens and antibodies in pregnancy. Patient information
 Platelet antigens and antibodies in pregnancy Patient information This leaflet explains the blood test results that you have been given and what this means to you and your baby. It contains information
Platelet antigens and antibodies in pregnancy Patient information This leaflet explains the blood test results that you have been given and what this means to you and your baby. It contains information
The Monocyte Monolayer Assay (MMA): An Adjunct to Compatibility Testing
 The Monocyte Monolayer Assay (MMA): An Adjunct to Compatibility Testing Ghislain Noumsi MD,SBB(ASCP) CM Molecular ImmunoHematologist Scientific Support Services LifeShare Blood Centers Shreveport, LA Objectives
The Monocyte Monolayer Assay (MMA): An Adjunct to Compatibility Testing Ghislain Noumsi MD,SBB(ASCP) CM Molecular ImmunoHematologist Scientific Support Services LifeShare Blood Centers Shreveport, LA Objectives
Characteristics and Serologic Determination of Antibodies to High Frequency Antigens
 Characteristics and Serologic Determination of Antibodies to High Frequency Antigens Nicole Thornton The International Blood Group Reference Laboratory Bristol, United Kingdom. 23 rd Regional Congress
Characteristics and Serologic Determination of Antibodies to High Frequency Antigens Nicole Thornton The International Blood Group Reference Laboratory Bristol, United Kingdom. 23 rd Regional Congress
WEST OF SCOTLAND BLOOD TRANSFUSION CENTRE GARTNAVEL GENERAL HOSPITAL 25 SHELLEY ROAD GLASGOW G12 0XB
 WEST OF SCOTLAND BLOOD TRANSFUSION CENTRE GARTNAVEL GENERAL HOSPITAL 25 SHELLEY ROAD GLASGOW G12 0XB SERVICE USERS HANDBOOK Date of Issue: 14 May 2012 Review date: 01 June 2014 CONTENTS Section Title Page
WEST OF SCOTLAND BLOOD TRANSFUSION CENTRE GARTNAVEL GENERAL HOSPITAL 25 SHELLEY ROAD GLASGOW G12 0XB SERVICE USERS HANDBOOK Date of Issue: 14 May 2012 Review date: 01 June 2014 CONTENTS Section Title Page
Laboratory Procedure Manual. Rh Phenotyping
 Exercise 4 Textbook: Quinley, Chapter 8 Skills: 20 Points Objectives:. State the antigens of the Rh blood group system. 2. Define the terms dominant, codominant, heterozygous, and homozygous as they relate
Exercise 4 Textbook: Quinley, Chapter 8 Skills: 20 Points Objectives:. State the antigens of the Rh blood group system. 2. Define the terms dominant, codominant, heterozygous, and homozygous as they relate
1) Siderophores are bacterial proteins that compete with animal A) Antibodies. B) Red blood cells. C) Transferrin. D) White blood cells. E) Receptors.
 Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Directed, Autologous and Therapeutic Donations
 Directed, Autologous and Therapeutic Donations Directed Donations: What is a directed donation? A directed donation is when a specific donor makes a blood donation at the request of a patient and the patient
Directed, Autologous and Therapeutic Donations Directed Donations: What is a directed donation? A directed donation is when a specific donor makes a blood donation at the request of a patient and the patient
Safe Blood and Blood Products
 Safe Blood and Blood Products Module 3 Blood Group Serology Safe Blood and Blood Products Module 3 Blood Group Serology Conversion of electronic files for the website edition was supported by Cooperative
Safe Blood and Blood Products Module 3 Blood Group Serology Safe Blood and Blood Products Module 3 Blood Group Serology Conversion of electronic files for the website edition was supported by Cooperative
BLOOD BANK ANNUAL STATISTICS (HOSPITALS)
 New Jersey Department of Health Clinical Laboratory Improvement Services PO Box 361 Trenton, NJ 08625-0361 BLOOD BANK ANNUAL STATISTICS (HOSPITALS) County Code Number Address Name of Individual Completing
New Jersey Department of Health Clinical Laboratory Improvement Services PO Box 361 Trenton, NJ 08625-0361 BLOOD BANK ANNUAL STATISTICS (HOSPITALS) County Code Number Address Name of Individual Completing
Using Blood-Typing to Determine Causes of Death in Surgery Patients Kim Williamson, East Clinton High School, Lees Creek, OH
 INTRODUCTION To close the yellow note, click once to select it and then click the box in the upper left corner. To open the note, double click (Mac OS) or right click (Windows) on the note icon. Using
INTRODUCTION To close the yellow note, click once to select it and then click the box in the upper left corner. To open the note, double click (Mac OS) or right click (Windows) on the note icon. Using
TESTING BLOOD PRE-TRANSFUSION COMPATIBILITY IN A GROUP OF CATS Meda Moldovan, L. Ognean, Alexandra Arion, I. Morar
 TESTING BLOOD PRE-TRANSFUSION COMPATIBILITY IN A GROUP OF CATS Meda Moldovan, L. Ognean, Alexandra Arion, I. Morar UNIVERSITY OF AGRICULTURAL SCIENCE AND VETERINARY MEDICINE, FACULTY OF VETERINARY MEDICINE,
TESTING BLOOD PRE-TRANSFUSION COMPATIBILITY IN A GROUP OF CATS Meda Moldovan, L. Ognean, Alexandra Arion, I. Morar UNIVERSITY OF AGRICULTURAL SCIENCE AND VETERINARY MEDICINE, FACULTY OF VETERINARY MEDICINE,
SAMPLE COLLECTION MANUAL. NZBS Blood Banks and NZBS Reference Laboratory
 SAMPLE COLLECTION MANUAL NZBS Blood Banks and NZBS Reference July 2012 SECTION 1. INTRODUCTION 3 SECTION 2. PRETRANSFUSION TESTING 3 2.1 COMPLETION OF REQUEST FORM... 3 2.2 SAMPLE COLLECTION... 4 2.3 SAMPLE
SAMPLE COLLECTION MANUAL NZBS Blood Banks and NZBS Reference July 2012 SECTION 1. INTRODUCTION 3 SECTION 2. PRETRANSFUSION TESTING 3 2.1 COMPLETION OF REQUEST FORM... 3 2.2 SAMPLE COLLECTION... 4 2.3 SAMPLE
POLICY FOR BLOOD COMPONENT AND BLOOD PRODUCT ADMINISTRATION
 TABLE OF CONTENTS Section I. POLICY STATEMENT... 3 Section II. DEFINITIONS... 3 Section III. GENERAL... 3 Section IV. ORDERING BLOOD COMPONENTS AND BLOOD PRODUCTS... 4 Section V. IDENTIFICATION... 4 Section
TABLE OF CONTENTS Section I. POLICY STATEMENT... 3 Section II. DEFINITIONS... 3 Section III. GENERAL... 3 Section IV. ORDERING BLOOD COMPONENTS AND BLOOD PRODUCTS... 4 Section V. IDENTIFICATION... 4 Section
Global Database on Blood Safety
 Global Database on Blood Safety Summary Report 2011 1 Key facts Global Blood Collection: Around 92 million blood donations are collected annually from all types of blood donors (voluntary unpaid, family/replacement
Global Database on Blood Safety Summary Report 2011 1 Key facts Global Blood Collection: Around 92 million blood donations are collected annually from all types of blood donors (voluntary unpaid, family/replacement
Lab 02: Blood Cytology (20 points)
 Pierce College Putman/Biol 242 Name: Lab 02: Blood Cytology (20 points) Reference: Marieb & Mitchell 9 th Ed: 29A (Activities 1, 2, 3, 4, 7); 10 th Ed: Exercise 29 (Activities 1, 2, 3, 4, 7). Pierce College
Pierce College Putman/Biol 242 Name: Lab 02: Blood Cytology (20 points) Reference: Marieb & Mitchell 9 th Ed: 29A (Activities 1, 2, 3, 4, 7); 10 th Ed: Exercise 29 (Activities 1, 2, 3, 4, 7). Pierce College
SARASOTA MEMORIAL HOSPITAL BLOOD COMPONENT CRITERIA AND INDICATIONS SCREENING GUIDELINES
 SARASOTA MEMORIAL HOSPITAL BLOOD COMPONENT CRITERIA AND INDICATIONS SCREENING GUIDELINES TABLE OF CONTENTS SUBJECT PAGE ADULT CRITERIA Red Blood Cells/Autologous 2 Washed Red Blood Cells 2 Cryoprecipitate
SARASOTA MEMORIAL HOSPITAL BLOOD COMPONENT CRITERIA AND INDICATIONS SCREENING GUIDELINES TABLE OF CONTENTS SUBJECT PAGE ADULT CRITERIA Red Blood Cells/Autologous 2 Washed Red Blood Cells 2 Cryoprecipitate
GUIDELINE FOR BLOOD GROUPING AND RED CELL ANTIBODY TESTING IN PREGNANCY
 GUIDELINE FOR BLOOD GROUPING AND RED CELL ANTIBODY TESTING IN PREGNANCY British Committee for Standards in Haematology Address for correspondence: BCSH Secretary British Society for Haematology 100 White
GUIDELINE FOR BLOOD GROUPING AND RED CELL ANTIBODY TESTING IN PREGNANCY British Committee for Standards in Haematology Address for correspondence: BCSH Secretary British Society for Haematology 100 White
Blood Transfusion. Red Blood Cells White Blood Cells Platelets
 Blood Transfusion Introduction Blood transfusions are very common. Each year, almost 5 million Americans need a blood transfusion. Blood transfusions are given to replace blood lost during surgery or serious
Blood Transfusion Introduction Blood transfusions are very common. Each year, almost 5 million Americans need a blood transfusion. Blood transfusions are given to replace blood lost during surgery or serious
Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI
 Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI Overview of Hematology, http://www.nu.edu.sa/userfiles/mhmorsy/h
Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI Overview of Hematology, http://www.nu.edu.sa/userfiles/mhmorsy/h
WEST OF SCOTLAND BLOOD TRANSFUSION CENTRE GARTNAVEL GENERAL HOSPITAL 25 SHELLEY ROAD GLASGOW G12 0XB
 WEST OF SCOTLAND BLOOD TRANSFUSION CENTRE GARTNAVEL GENERAL HOSPITAL 25 SHELLEY ROAD GLASGOW G12 0XB SERVICE USERS HANDBOOK Date of Issue: 14 October 2014 Review date: 01 November 2016 CONTENTS Section
WEST OF SCOTLAND BLOOD TRANSFUSION CENTRE GARTNAVEL GENERAL HOSPITAL 25 SHELLEY ROAD GLASGOW G12 0XB SERVICE USERS HANDBOOK Date of Issue: 14 October 2014 Review date: 01 November 2016 CONTENTS Section
