Headaches and Facial Pain (updated 09/06)
|
|
|
- Joshua Newton
- 8 years ago
- Views:
Transcription
1 Headaches and Facial Pain (updated 09/06) 1. Review the sensory innervation to the ear and discuss pathways of referred pain. Medical Clin North Am 1991;75:677. SW 2. Discuss sinonasal innervation. Medical Clin North Am 1991;75:677. CB 3. Brain parenchyma is pain insensitive. Explain source of pain with migraines AL The parenchyma of the brain is insensitive to direct noxious stimuli. The trigeminal nerve is the largest of all the cranial nerves. It is a mixed nerve situated on the ventrolateral aspect of the pons. The sensory root conveys impulses from the face and scalp, parts of the external ear and acoustic meatus, the nasal and oral cavities, teeth, temporomandibular joint (TMJ), nasopharynx, and most of the meninges of the anterior and middle fossa. It passes outward and forward over the petrous temporal bone near the apex, extending into the trigeminal ganglion. These pseudounipolar cells pass peripherally to become the three major divisions: ophthalmic, maxillary, and mandibular. In the primary head and face pains, abnormal activation of peripheral neurons or central structures results in distinctive pain description, phenomenology, and associations (5). These may then refer to areas of the head, neck, or face at distance from the area of activation, making diagnosis more challenging (Table 18.1). The central connections of second-order sensory neurons of the trigeminal system project to the thalamus and thence to the primary sensory cortex of the parietal lobe. Descending inhibitory projections from periaqueductal gray and paracentral aminergic nuclei modify the pain experience and have become increasingly important in our understanding of the primary headaches. J Vestib Res. 2011;21(6): The science of migraine. Burstein R, Jakubowski M, Rauch SD. Departments of Anesthesia, Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA, USA. rburstei@bidmc.harvard.edu Abstract The cardinal symptom of migraine is headache pain. In this paper we review the neurobiology of this pain as it is currently understood. In recent years, we discovered that the network of neurons that sense pain signals from the dura changes rapidly during the course of a single migraine attack and that the treatment of an attack is a moving target. We found that if the pain is not stopped within minutes after it starts, the first set of neurons in the network, those located in the trigeminal ganglion, undergo molecular changes that make them hypersensitive to the changing pressure inside the head, which explains why migraine headache throbs and is worsened by bending over and sneezing. We found that if the pain is not stopped within minutes, the second group of neurons in the network, those located in the spinal trigeminal nucleus, undergoes molecular changes that convert them from being dependent on sensory signals they receive from the dura by the first set of neurons, into an independent state in which they themselves become the pain generator of the headache. When this happens, patients notice that brushing their hair, taking a shower, touching their periorbital skin, shaving, wearing earrings, etc become painful, a condition called cutaneous allodynia. Based on this scenario, we showed recently that the success rate of rendering migraine patients pain-free increased dramatically if medication was given before the establishment of cutaneous allodynia and central sensitization. The molecular shift from activity-dependent to activity-independent central sensitization together with our recent conclusion that triptans have the ability to disrupt communications between peripheral and central trigeminovascular neurons (rather than inhibiting directly peripheral or central neurons) explain their clinical effects. Both our clinical and pre-clinical findings of the last five years point to possible short- and long-term advantages in using an early-treatment approach in the treatment of acute migraine attacks.
2 4. What is Eagle s syndrome? Trotter s syndrome? SW 5. Differentiate temporamandibular joint disorder from myofascial pain-dysfunction syndrome. AL The TMJ and the muscles of mastication can be a source of pain that radiates to the head and the ear. The TMJ and its articulations are innervated by the auriculotemporal nerve as it passes behind the condyle and then upward in front of the ear. Pain can be reported as a diffuse temporal headache or as ipsilateral ear pain The temporomandibular disorders (TMDs) can occur as diffuse temporal headache, earache, and facial pain. True TMJ pain is characterized by tenderness to palpation over the condyle and by pain on jaw movement. Internal derangements are characterized by anterior and medial displacement of the articular disk when the teeth are interdigitated in occlusion. About 25 mm of space between the anterior teeth is the limit of rotational opening because further opening requires translation of the condyle. Degenerative joint disease (DJD) is characterized by crepitus and pain on jaw movement. It is usually selflimited and can be managed with NSAIDs. Most patients have combined muscle and joint pain with tenderness of the masticatory muscles and worsening with joint movement. A click on movement may be present. Mouth opening is limited. Management is similar to that for tension headache. NSAIDs and physical therapy form the mainstay of treatment. Other methods for muscle pain management such as biofeedback, trigger-point injection, and physical therapy are useful. Dental splints may be useful, and referral to dentistry is indicated. MPD syndrome is a muscular disease that is believed to be multifactorial in origin.43 It is generally accepted that centrally induced muscle tension from stress and anxiety combined with parafunctional habits such as clenching or grinding of the teeth results in abnormal muscle function and hyperactivity. This leads to fatigue and spasm of the muscles that ultimately produces pain and dysfunction. The pain stimulates muscle fibers to react, leading to further muscular dysfunction and spasm. Thus one can appreciate the cyclic nature of this disorder. Similar symptoms can also occasionally result from muscular overextension, muscle overcontraction, or trauma (Fig. 94-3). MPD syndrome most frequently affects females in the 20- to 40-year age group. Men are much less affected, with a ratio of approximately 1 : 4. Children are rarely affected. MPD syndrome is characterized by diffuse, poorly localized pain that ranges from complaint of preauricular pain to generalized pain throughout the muscles of mastication. The pain is often described as dull, aching, radiating pain that may be more severe in the morning. Patients also complain of pain and limitation of opening during function. The condition generally involves only one side of the face, and on examination, tenderness can usually be elicited in one or more of the muscles of mastication or their tendinous attachments.44 Headache is frequently mentioned as a symptom. Ciancaglini and Radaelli45 report a significant increase in headache in patients with TMD symptoms (27.4% vs. 15.2%). The only type of headache that is functionally related to MPD syndrome, however, is the tension-type headache, with other types being coincidental findings. The same is true for multiple complaints noted by MPD patients such as decreased hearing, tinnitus, burning tongue, and neuralgic pains. MPD syndrome that is left untreated can ultimately lead to organic changes in the TMJ and the masticatory muscles and may even cause alterations in the dentition. The cardinal signs and symptoms of MPD syndrome are similar to those produced by intracapsular disorders, as well as by a variety nonarticular conditions (Tables 94-2 and 94-3). A careful history and thorough clinical evaluation should be performed to rule out these other clinical entities. Screening radiographs, particularly intraoral periapical films and a panoramic film delineating the structures of the jaws and the TMJ, can be helpful. If the screening views of the TMJ show some abnormality, tomographic views or CT scans are useful in further evaluating bony abnormalities. Magnetic resonance imaging is valuable in evaluating soft tissue structures particularly
3 when an internal derangement of the TMJ is suspected. In addition, certain laboratory tests may be helpful in some patients. These tests include a complete blood cell count if an infection is suspected; serum calcium, phosphorus, and alkaline phosphatase measurements for possible bone disease; serum uric acid determination for gout; serum creatinine and creatine phosphokinase levels as indicators of muscle disease; and erythrocyte sedimentation rate, rheumatoid factor, latex fixation, and antinuclear antibody tests for suspected rheumatoid arthritis. In patients suspected primarily of MPD syndrome, muscular function may be evaluated through electromyography. Many clinicians recommend psychologic evaluation, primarily to help determine patient compliance and to predict anticipated treatment outcomes. 6. Characterize migraines. Discuss the treatment to include drugs, behavior modification, etc. How do migraines differ from cluster headaches? Otolaryngol Head Neck Surg 2000;123:66. AL Migraine with and without aura 1.1 Migraine without aura A. Headache attacks lasting 4 72 h (untreated or successfully treated) B. Headache has at least two of the following characteristics 1. Unilateral location
4 2. Pulsating quality 3. Moderate or severe intensity 4. Aggravation by or causing avoidance of routine physical activity (e.g., walking or climbing stairs) C. During headache, at least one of the following: 1. Nausea or vomiting 2. Photophobia and phonophobia D. Not attributed to another disorder C. At least two of the following: 1. Homonymous visual symptoms and/or unilateral sensory symptoms 2. At least one aura symptom develops gradually over Ñ 5 min, and/or different aura symptoms occur in succession over Ñ 5 min D. Headache fulfilling criteria B D for 1.1 Migraine without aura begins during the aura or follows within 60 min E. Not attributed to another disorder 1.2 Migraine with typical aura A. At least two attacks B. Aura consisting of at least one of the following but no motor weakness: 1. Fully reversible visual symptoms including positive features (e.g., flickering lights, spots, or lines) and/or negative features (i.e., loss of vision) 2. Fully reversible sensory symptoms including positive features (i.e., pins-and-needles) and/or negative features (i.e., numbness) 3. Fully reversible dysphasic speech disturbance Treatment: ACUTE Therapies: Triptans/5-HT1B/D agonists CGRP antagonists (calcitonin gene related peptide receptor) or Gepants onset of action is slower than triptans but no adverse effects Telcagepant Newer Promising Drugs: Lasmiditan highly selective 5-HT1F agonists, but lacks vasoconstricting effect. Side effects: dizziness, paresthesias, sensation of limb heaviness NXN-188: inhibition of neuronal nitric oxide synthase AND bidning to 5HT1B/D receptors, mild side effects (dizziness) Neuromodulation: Transcranial magnetic stimulation Nonspecific: butorphanol, ibuprofen, naproxen, prochlorperazine, ASA, APAP/ASA/Caffeine, APAP, isometheptine, opioids Triptans: almotriptan, eletriptan, frovatriptan, naratriptan, rizatriptan, sumatriptan, zolmitriptan, dihydroergotamine Comment: There is a triptan class effect for side effects, the majority of which are minor and not dangerous. Chest tightness, throat or head pressure, tingling, nausea, and flushing usually improve with patient education and repeated use. Daily maximums vary, although no more than two doses in 24 hours is the rule. They are contraindicated in patients with uncontrolled hypertension or a history of cerebral or coronary artery disease but are generally extremely safe and effective. Preventive Therapy: Anticonvulsants: Divalproex, topiramate, gabapentin Antidepressants: Tricyclics, SSRI, B blockers Calcium Channel Blockers: verapamil NSAIDS: naproxen Other: Riboflavin, magnesium, feverfew Alternative Nonpharmacological Procedures; Biofeedback and basic relaxation techniques did not significantly increase the outcome of relaxation alone Combination of B blocker and behavioural migraine management is significantly superior to either treatment alone Endovascular patent forament ovale closure: reported improvement in migraine Chronic Migraine Management: most disabling form of migraine, highly drug resistant
5 Occipital nerve stimulation: prelim data is encouraging Botox: failed in chronic tension HA, episodic MA, or chronic daily HA. Only small studies so far Cluster Headache CH is an uncommon disorder. Abrupt onset of strictly unilateral, blinding, and shortduration attacks raise questions about potentially devastating consequences including subarachnoid hemorrhage. Among the primary headaches, CH pain is assumed to be the most severe pain, and the accompanying autonomic features may confuse the diagnosis with pathology in orbital or periorbital areas or sinuses. Awakening the patient from sleep at a time when dreaming is presumed to occur leads to sleep evaluations, and CH's seasonal or circannual occurrence implies botanical allergy. Secondary causes of CH can include cranial, cervical, or vascular disorders. The carotid artery, cavernous sinus, and various brain structures, including the periaqueductal gray matter, appear to participate in pain generation and modulation associated with this disease (21). CH occurs in 0.2% to 0.6% of the population, with a male-to -female ratio of 4:1 to 12:1. Recent studies have suggested that although the gender ratio of CH may be changing, the overall prevalence has remained stable for the last 2 to 3 decades. Genetic studies suggest autosomal dominant transmission with a low frequency of the susceptibility allele. CH has been recognized as a distinctive clinical entity since as early as the 1700s. During active periods, most commonly in the spring and autumn, clusters of individual headaches lasting between 30 and 180 minutes occur daily, with episodes lasting weeks or months. The majority of patients have episodic, recurrent attacks of unilateral, temporal, or periorbital pain associated with autonomic features including ptosis, miosis, lacrimation, rhinorrhea, and ipsilateral stuffiness. In a chronic form of this disorder, unrelenting and daily attacks of typical CHs persist without interruption. Episodic cluster is defined by gaps in time between painful periods. Chronic cluster is unremitting. Episodes occur once or twice per year in 75% of patients, with a typical episode lasting approximately 2 months. Attacks typically last between 72 and 159 minutes, with attack frequency between two per week and five per day (Table 18.8), and 73% of patients have a predictable onset of attacks at night. Of episodic patients, 43% describe a seasonal onset, and chronic sufferers also describe seasonal exacerbations. CH is a strictly unilateral headache in 100% of attacks occurring during a symptomatic cluster episode. Autonomic features including ipsilateral facial flushing, lacrimation, nasal stuffiness, ptosis, or miosis occur in 70% to 90% of patients. Previous head trauma appears to be associated with CH, although duration from time of trauma is extremely variable. Differentiating CH from migraine is not clinically difficult. CH is of shorter duration and male preponderant. Photophobia, nausea, or other features classically associated with migraine may occur. The defining clinical feature is the tendency for patients to describe attack-associated behavioral agitation. During attacks, up to 93% of patients experience restlessness (22) during which they rock, pace, and rub or beat their heads. 3.1 Cluster headache A. At least five attacks fulfilling criteria B D B. Severe or very severe unilateral orbital, supraorbital, and/or temporal pain lasting min if untreated C. Headache accompanied by at least one of the following: 1. Ipsilateral conjunctival injection and/or lacrimation 2. Ipsilateral nasal congestion and/or rhinorrhea 3. Ipsilateral eyelid edema 4. Ipsilateral forehead and facial sweating 5. Ipsilateral miosis and/or ptosis 6. A sense of restlessness or agitation D. Attacks have a frequency of from one every other day to eight per day E. Not attributed to another disorder 7. Discuss the classic presentation of temporal arteritis? Why is this a headache emergency? SW 8. Differentiate trigemenal neuralgia from atypical facial pain. How would you treat each? CB
6 9. Is sinus surgery effective in the management of patients with headaches? Laryngoscope 1998;108:696 and Arch Otolaryngol Head Neck Surg 2000;126:1274. TT 10. What is the anterior ethmoid nerve syndrome? TT
HEADACHE. as. MUDr. Rudolf Černý, CSc. doc. MUDr. Petr Marusič, Ph.D.
 HEADACHE as. MUDr. Rudolf Černý, CSc. doc. MUDr. Petr Marusič, Ph.D. Dpt. of Neurology Charles University in Prague, 2nd Faculty of Medicine Motol University Hospital History of headache 1200 years B.C.
HEADACHE as. MUDr. Rudolf Černý, CSc. doc. MUDr. Petr Marusič, Ph.D. Dpt. of Neurology Charles University in Prague, 2nd Faculty of Medicine Motol University Hospital History of headache 1200 years B.C.
Post Traumatic and other Headache Syndromes. Danielle L. Erb, MD Brain Rehabilitation Medicine, LLC Brain Injury Rehab Center, PRA
 Post Traumatic and other Headache Syndromes Danielle L. Erb, MD Brain Rehabilitation Medicine, LLC Brain Injury Rehab Center, PRA Over 45 million Americans have chronic, recurring headaches 62% of these
Post Traumatic and other Headache Syndromes Danielle L. Erb, MD Brain Rehabilitation Medicine, LLC Brain Injury Rehab Center, PRA Over 45 million Americans have chronic, recurring headaches 62% of these
Headaches + Facial pain
 Headaches + Facial pain Introduction: Each of us experienced sporadically/ chronically headache 40% worldwide population suffers with severe, disabling headache at least annually Common ailment Presenting
Headaches + Facial pain Introduction: Each of us experienced sporadically/ chronically headache 40% worldwide population suffers with severe, disabling headache at least annually Common ailment Presenting
Sinus Headache vs. Migraine
 Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Differential diagnosis of Orofacial Pain. Prof. Yair Sharav School of Dental Medicine Hebrew University-Hadassah, Jerusalem
 Differential diagnosis of Orofacial Pain Prof. Yair Sharav School of Dental Medicine Hebrew University-Hadassah, Jerusalem Orofacial Pain & Headache Yair Sharav & Rafael Benoliel 2008, MOSBY, Elsevir Special
Differential diagnosis of Orofacial Pain Prof. Yair Sharav School of Dental Medicine Hebrew University-Hadassah, Jerusalem Orofacial Pain & Headache Yair Sharav & Rafael Benoliel 2008, MOSBY, Elsevir Special
HEADACHES AND THE THIRD OCCIPITAL NERVE
 HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
Headaches in Children How to Manage Difficult Headaches
 Headaches in Children How to Manage Difficult Headaches Peter Procopis Childhood headaches Differential diagnosis Migraine Psychological Raised Pressure Childhood headaches Other causes: Constitutional
Headaches in Children How to Manage Difficult Headaches Peter Procopis Childhood headaches Differential diagnosis Migraine Psychological Raised Pressure Childhood headaches Other causes: Constitutional
Headaches. This chapter will discuss:
 C H A P T E R Headaches 1 1 Almost everyone gets an occasional headache at some time or another. Some people get frequent headaches. Most people do not worry about headaches and learn to live with them
C H A P T E R Headaches 1 1 Almost everyone gets an occasional headache at some time or another. Some people get frequent headaches. Most people do not worry about headaches and learn to live with them
Neurovascular Orofacial Pain. Orofacial pain of potential neurovascular origin may mimic odontogenic pain to the extent that
 Neurovascular Orofacial Pain Introduction Orofacial pain of potential neurovascular origin may mimic odontogenic pain to the extent that a large population of patients with migraine and trigeminal autonomic
Neurovascular Orofacial Pain Introduction Orofacial pain of potential neurovascular origin may mimic odontogenic pain to the extent that a large population of patients with migraine and trigeminal autonomic
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE
 TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
BOTOX Treatment. for Chronic Migraine. Information for patients and their families. Botulinum Toxin Type A
 BOTOX Treatment Botulinum Toxin Type A for Chronic Migraine Information for patients and their families. Is Chronic Migraine the same as Migraine? Chronic Migraine is similar to migraine as sufferers experience
BOTOX Treatment Botulinum Toxin Type A for Chronic Migraine Information for patients and their families. Is Chronic Migraine the same as Migraine? Chronic Migraine is similar to migraine as sufferers experience
Classification of Chronic Headache
 Chronic Headache Classification of Chronic Headache JMAJ 47(3): 112 117, 2004 Mitsunori MORIMATSU Professor, Department of Neurology and Clinical Neuroscience, Yamaguchi University School of Medicine Abstract:
Chronic Headache Classification of Chronic Headache JMAJ 47(3): 112 117, 2004 Mitsunori MORIMATSU Professor, Department of Neurology and Clinical Neuroscience, Yamaguchi University School of Medicine Abstract:
HEADACHES IN CHILDREN AND ADOLESCENTS. Brian D. Ryals, M.D.
 HEADACHES IN CHILDREN AND ADOLESCENTS Brian D. Ryals, M.D. Frequency and Type of Headaches in Schoolchildren 8993 children age 7-15 in Sweden Migraine in 4% Frequent Nonmigrainous in 7% Infrequent Nonmigrainous
HEADACHES IN CHILDREN AND ADOLESCENTS Brian D. Ryals, M.D. Frequency and Type of Headaches in Schoolchildren 8993 children age 7-15 in Sweden Migraine in 4% Frequent Nonmigrainous in 7% Infrequent Nonmigrainous
X-Plain Temporomandibular Joint Disorders Reference Summary
 X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
None related to the presentation Grants to conduct clinical trials from:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Evaluation of Headache Syndromes and Migraine
 Evaluation of Headache Syndromes and Migraine Sonja Potrebic MD PhD Department of Neurology Los Angeles Kaiser Objectives 1) Identify the diagnostic features of migraine Differentiate from sinusitis 2)
Evaluation of Headache Syndromes and Migraine Sonja Potrebic MD PhD Department of Neurology Los Angeles Kaiser Objectives 1) Identify the diagnostic features of migraine Differentiate from sinusitis 2)
HEADACHE: CLINICAL SYNDROMES, PATHOPHYSIOLOGY AND MANAGEMENT Joanna G Katzman, M.D., MSPH Assistant Professor UNM Pain Center and ECHO Pain
 HEADACHE: CLINICAL SYNDROMES, PATHOPHYSIOLOGY AND MANAGEMENT Joanna G Katzman, M.D., MSPH Assistant Professor UNM Pain Center and ECHO Pain University of New Mexico Health Sciences Center 11/14/13 After
HEADACHE: CLINICAL SYNDROMES, PATHOPHYSIOLOGY AND MANAGEMENT Joanna G Katzman, M.D., MSPH Assistant Professor UNM Pain Center and ECHO Pain University of New Mexico Health Sciences Center 11/14/13 After
8/23/2015 A PRACTICAL OPTOMETRIC HEADACHE APPROACH A PRACTICAL OPTOMETRIC HEADACHE APPROACH A PRACTICAL OPTOMETRIC HEADACHE APPROACH
 8/23/2015 A Practical Optometric Approach To Headaches Leonid Skorin, Jr., OD, DO, MS, FAAO, FAOCO Consultant, Department of Surgery Community Division of Ophthalmology Mayo Clinic Health System in Albert
8/23/2015 A Practical Optometric Approach To Headaches Leonid Skorin, Jr., OD, DO, MS, FAAO, FAOCO Consultant, Department of Surgery Community Division of Ophthalmology Mayo Clinic Health System in Albert
Toothaches of Non-dental Origin
 Toothaches of Non-dental Origin This brochure is produced by the American Academy of Orofacial Pain The American Academy of Orofacial Pain is an organization of health care professionals dedicated to alleviating
Toothaches of Non-dental Origin This brochure is produced by the American Academy of Orofacial Pain The American Academy of Orofacial Pain is an organization of health care professionals dedicated to alleviating
SIGN. Diagnosis and management of headache in adults. Quick Reference Guide. Scottish Intercollegiate Guidelines Network
 SIGN Scottish Intercollegiate Guidelines Network 107 iagnosis and management of headache in adults Quick Reference Guide November 2008 opies of all SIGN guidelines are available online at www.sign.ac.uk
SIGN Scottish Intercollegiate Guidelines Network 107 iagnosis and management of headache in adults Quick Reference Guide November 2008 opies of all SIGN guidelines are available online at www.sign.ac.uk
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies
 Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
MIGRAINE. Denise Cambier M.D. Delaware Neurology, Ohio Health March 2013
 MIGRAINE Denise Cambier M.D. Delaware Neurology, Ohio Health March 2013 HISTORY: Graham and Wolff 1938: decreased amplitude of arterial pulsations coincided with reduction of headache with IV ergotamine.
MIGRAINE Denise Cambier M.D. Delaware Neurology, Ohio Health March 2013 HISTORY: Graham and Wolff 1938: decreased amplitude of arterial pulsations coincided with reduction of headache with IV ergotamine.
Headaches and Kids. Jennifer Bickel, MD Assistant Professor of Neurology Co-Director of Headache Clinic Children s Mercy Hospital
 Headaches and Kids Jennifer Bickel, MD Assistant Professor of Neurology Co-Director of Headache Clinic Children s Mercy Hospital Overview Headache classifications and diagnosis Address common headache
Headaches and Kids Jennifer Bickel, MD Assistant Professor of Neurology Co-Director of Headache Clinic Children s Mercy Hospital Overview Headache classifications and diagnosis Address common headache
National Hospital for Neurology and Neurosurgery. Migraine associated dizziness Department of Neuro-otology
 National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
TMJ. Problems. Certain headaches and pain in. the ear, jaw, neck, tooth, and. sinus can be the result of a. temporomandibular joint (TMJ)
 DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
Oh, 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8
 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
Eastman Dental Hospital. Temporomandibular disorder. Facial Pain Team
 Eastman Dental Hospital Temporomandibular disorder Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on 020 3456
Eastman Dental Hospital Temporomandibular disorder Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on 020 3456
Careful Coding: Headaches
 Dynamic Chiropractic March 26, 2012, Vol. 30, Issue 07 Careful Coding: Headaches By K. Jeffrey Miller, DC, DABCO and Ray Tuck, DC Because s are among the most common reasons for seeking chiropractic care,
Dynamic Chiropractic March 26, 2012, Vol. 30, Issue 07 Careful Coding: Headaches By K. Jeffrey Miller, DC, DABCO and Ray Tuck, DC Because s are among the most common reasons for seeking chiropractic care,
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the UBC Headache Clinic Rotation
 UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the UBC Headache Clinic Rotation Overview: The UBC Headache Clinic is located in located in rm. 267, on the 2nd floor of UBC Hospital.
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the UBC Headache Clinic Rotation Overview: The UBC Headache Clinic is located in located in rm. 267, on the 2nd floor of UBC Hospital.
Migraine The Problem: Common Symptoms:
 Migraine The Problem: A combination of genetic and environmental factors alter pain mechanisms in your brain Transient changes in brain chemicals such as serotonin and neuropeptides affect the membranes
Migraine The Problem: A combination of genetic and environmental factors alter pain mechanisms in your brain Transient changes in brain chemicals such as serotonin and neuropeptides affect the membranes
Adult with headache. Problem-specific video guides to diagnosing patients and helping them with management and prevention
 Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Sporadic attacks of severe tension-type headaches may respond to analgesics.
 MEDICATIONS While we are big advocates of non-drug treatments, many people do require the use of medications to control headaches. Headache medications are divided into two categories. Abortive drugs are
MEDICATIONS While we are big advocates of non-drug treatments, many people do require the use of medications to control headaches. Headache medications are divided into two categories. Abortive drugs are
Akuter Kopfschmerz. Till Sprenger, MD Neurologie USB
 Akuter Kopfschmerz Till Sprenger, MD Neurologie USB Disclosure I have consulted for Biogen Idec, Novartis, Mitsubishi Pharmaceuticals, Eli Lilly, Genzyme and Allergan. I have received compensation for
Akuter Kopfschmerz Till Sprenger, MD Neurologie USB Disclosure I have consulted for Biogen Idec, Novartis, Mitsubishi Pharmaceuticals, Eli Lilly, Genzyme and Allergan. I have received compensation for
Differential Diagnosis of Craniofacial Pain
 1. Differential Diagnosis of Craniofacial Pain 2. Headache Page - 1 3. International Headache Society International Classification... 4. The Primary Headaches (1-4) Page - 2 5. The Secondary Headaches
1. Differential Diagnosis of Craniofacial Pain 2. Headache Page - 1 3. International Headache Society International Classification... 4. The Primary Headaches (1-4) Page - 2 5. The Secondary Headaches
Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries
 1 Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries J Bone Joint Surg (Br) 2001 Mar;83(2):226-9 Ide M, Ide J, Yamaga M, Takagi K Department of Orthopaedic Surgery, Kumamoto University
1 Symptoms and Signs of Irritation of the Brachial Plexus in Whiplash Injuries J Bone Joint Surg (Br) 2001 Mar;83(2):226-9 Ide M, Ide J, Yamaga M, Takagi K Department of Orthopaedic Surgery, Kumamoto University
Lateral pterygoid muscle Medial pterygoid muscle
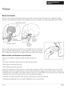 PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
Polymyalgia Rheumatica www.arthritis.org.nz
 Polymyalgia Rheumatica www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Polymyalgia rheumatica is a common rheumatic condition. It affects more women
Polymyalgia Rheumatica www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Polymyalgia rheumatica is a common rheumatic condition. It affects more women
Cervical Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education
 Cervical Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for headache
Cervical Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for headache
Medical Massage Client Intake Form Medical Massage Client Intake Form
 Medical Massage Client Intake Form Medical Massage Client Intake Form Client Name: Date: Please note: The more information you are able to provide, the better equipped our therapists will be to help you.
Medical Massage Client Intake Form Medical Massage Client Intake Form Client Name: Date: Please note: The more information you are able to provide, the better equipped our therapists will be to help you.
Headaches in Children
 Children s s Hospital Headaches in Children Manikum Moodley, MD, FRCP Section of Pediatric Neurology The Cleveland Clinic Foundation Introduction Headaches are common in children Most headaches are benign
Children s s Hospital Headaches in Children Manikum Moodley, MD, FRCP Section of Pediatric Neurology The Cleveland Clinic Foundation Introduction Headaches are common in children Most headaches are benign
What is chronic daily headache? Information for patients Neurology
 What is chronic daily headache? Information for patients Neurology What is chronic daily headache (CDH)? Chronic daily headache (CDH) is the term used when a person has a headache on 15 days a month or
What is chronic daily headache? Information for patients Neurology What is chronic daily headache (CDH)? Chronic daily headache (CDH) is the term used when a person has a headache on 15 days a month or
Addendum. 1 Headache
 Addendum 1 Headache Headache Addendum Levittown Health Center Headache Working Group Introduction Headache is a common complaint in primary care practice, and is the third most common patient complaint
Addendum 1 Headache Headache Addendum Levittown Health Center Headache Working Group Introduction Headache is a common complaint in primary care practice, and is the third most common patient complaint
Whiplash and Whiplash- Associated Disorders
 Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
MISCP MCSP MMACP. Chartered Physiotherapist specialising in treating Sports & Musculoskeletal Disorders
 MISCP MCSP MMACP Chartered Physiotherapist specialising in treating Sports & Musculoskeletal Disorders Physiotherapy Treatment of Migraine Classification of headaches Primary Pain felt in the head from
MISCP MCSP MMACP Chartered Physiotherapist specialising in treating Sports & Musculoskeletal Disorders Physiotherapy Treatment of Migraine Classification of headaches Primary Pain felt in the head from
HEADACHES IN CHILDREN : A CLINICAL APPROACH
 HEADACHES IN CHILDREN : A CLINICAL APPROACH Chong Shang Chee A physician is commonly faced with a child presenting with headaches. The assessment of a child s headache is challenging, but an accurate assessment
HEADACHES IN CHILDREN : A CLINICAL APPROACH Chong Shang Chee A physician is commonly faced with a child presenting with headaches. The assessment of a child s headache is challenging, but an accurate assessment
Differential Diagnosis of Chronic Headache
 Chronic Headache Differential Diagnosis of Chronic Headache JMAJ 47(3): 118 123, 2004 Koichi HIRATA Professor, Department of Neurology, Dokkyo University School of Medicine Abstract: Headache is one of
Chronic Headache Differential Diagnosis of Chronic Headache JMAJ 47(3): 118 123, 2004 Koichi HIRATA Professor, Department of Neurology, Dokkyo University School of Medicine Abstract: Headache is one of
Migraine Treatment - What You Should Know
 What kind of headache do you have? Less than 2% of the population have never had a headache. Most of us get them from time to time and they are usually resolved with a couple of painkillers, a rest or
What kind of headache do you have? Less than 2% of the population have never had a headache. Most of us get them from time to time and they are usually resolved with a couple of painkillers, a rest or
CHPN Review Course Pain Management Part 1 Hospice and Palliative Nurses Association
 CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY
 Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY Neuroophthalmology focuses on conditions caused by brain or systemic abnormalities that result in visual disturbances, among other symptoms.
Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY Neuroophthalmology focuses on conditions caused by brain or systemic abnormalities that result in visual disturbances, among other symptoms.
THE TMJ TREATMENT CENTER
 THE TMJ TREATMENT CENTER TEMPOROMANDIBULAR JOINT DISORDERS, CRANIOFACIAL DISORDERS, CERVICOCRANIAL INSTABILITY & EHLERS-DANLOS SYNDROME ABOUT DR. MITAKIDES & THE TMJ TREATMENT CENTER Dedicated to the diagnosis
THE TMJ TREATMENT CENTER TEMPOROMANDIBULAR JOINT DISORDERS, CRANIOFACIAL DISORDERS, CERVICOCRANIAL INSTABILITY & EHLERS-DANLOS SYNDROME ABOUT DR. MITAKIDES & THE TMJ TREATMENT CENTER Dedicated to the diagnosis
From Elizabeth To my father, Thomas Wentz From Paul To my father, Hugo; my uncle, Lewis; and my aunt, Lilia From Liz To my brother Mark and his
 From Elizabeth To my father, Thomas Wentz From Paul To my father, Hugo; my uncle, Lewis; and my aunt, Lilia From Liz To my brother Mark and his family contents Title Page Dedication Chapter 1 What Are
From Elizabeth To my father, Thomas Wentz From Paul To my father, Hugo; my uncle, Lewis; and my aunt, Lilia From Liz To my brother Mark and his family contents Title Page Dedication Chapter 1 What Are
Patient Information ONZETRA TM (On ze' trah) Xsail TM (Eks'-seil) (sumatriptan nasal powder) 11 mg
 Patient Information ONZETRA TM (On ze' trah) Xsail TM (Eks'-seil) (sumatriptan nasal powder) 11 mg Read this Patient Information before you start using ONZETRA Xsail and each time you get a refill. There
Patient Information ONZETRA TM (On ze' trah) Xsail TM (Eks'-seil) (sumatriptan nasal powder) 11 mg Read this Patient Information before you start using ONZETRA Xsail and each time you get a refill. There
Cervicogenic Headaches
 Cervicogenic Headaches Definition/Description Cervicogenic headaches refer to headache type sensations felt in the head and/face that originates from the neck, most commonly the upper cervical zygapophyseal
Cervicogenic Headaches Definition/Description Cervicogenic headaches refer to headache type sensations felt in the head and/face that originates from the neck, most commonly the upper cervical zygapophyseal
When the Pain Won t Stop: Managing Chronic Daily Headache
 When the Pain Won t Stop: Managing Chronic Daily Headache Arnolda Eloff, MB, ChB, Mmed Presented at the University of Calgary s Wednesday Evening Course Program, Calgary, Alberta. Copyright Chronic daily
When the Pain Won t Stop: Managing Chronic Daily Headache Arnolda Eloff, MB, ChB, Mmed Presented at the University of Calgary s Wednesday Evening Course Program, Calgary, Alberta. Copyright Chronic daily
Post-Concussive Headaches and Dizziness Louise M. Klebanoff, MD
 Post-Concussive Headaches and Dizziness Louise M. Klebanoff, MD Associate Professor and Vice Chairman for Operations Chief, General Neurology Department of Neurology Disclosures: None Introduction: Headaches
Post-Concussive Headaches and Dizziness Louise M. Klebanoff, MD Associate Professor and Vice Chairman for Operations Chief, General Neurology Department of Neurology Disclosures: None Introduction: Headaches
BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required]
![BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required] BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required]](/thumbs/29/13417512.jpg) BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required] Medical Policy: MP-RX-01-11 Original Effective Date: March 24, 2011 Reviewed: Revised: This policy applies to products
BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required] Medical Policy: MP-RX-01-11 Original Effective Date: March 24, 2011 Reviewed: Revised: This policy applies to products
Trigeminal Neuralgia. U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health
 Trigeminal Neuralgia U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Trigeminal Neuralgia What is trigeminal neuralgia? Trigeminal neuralgia (TN), also
Trigeminal Neuralgia U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Trigeminal Neuralgia What is trigeminal neuralgia? Trigeminal neuralgia (TN), also
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
New Patient Evaluation
 What area hurts you the most? (Please choose one) When did this pain start? Neck Other: Back How did this pain start? How often do you experience this pain? Describe what this pain feels like. What makes
What area hurts you the most? (Please choose one) When did this pain start? Neck Other: Back How did this pain start? How often do you experience this pain? Describe what this pain feels like. What makes
Sleep Difficulties. Insomnia. By Thomas Freedom, MD and Johan Samanta, MD
 Sleep Difficulties By Thomas Freedom, MD and Johan Samanta, MD For most people, night is a time of rest and renewal; however, for many people with Parkinson s disease nighttime is a struggle to get the
Sleep Difficulties By Thomas Freedom, MD and Johan Samanta, MD For most people, night is a time of rest and renewal; however, for many people with Parkinson s disease nighttime is a struggle to get the
*A discrete, hypersensitive nodule within tight band of muscle or fascia that present with classic pattern of pain referral that does not follow
 A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
A fresh, new, effective holistic approach to the age-old problem of treating headaches. Dr Prue King
 A fresh, new, effective holistic approach to the age-old problem of treating headaches Dr Prue King Just how big a problem are headaches? Headache disorders are among the most common disorders of the nervous
A fresh, new, effective holistic approach to the age-old problem of treating headaches Dr Prue King Just how big a problem are headaches? Headache disorders are among the most common disorders of the nervous
X-Plain Trigeminal Neuralgia Reference Summary
 X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
Natural Modality in the Treatment of Primary Headaches. William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P.
 Natural Modality in the Treatment of Primary Headaches William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P. Abstract Headaches are both a prevalent and disabling condition.
Natural Modality in the Treatment of Primary Headaches William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P. Abstract Headaches are both a prevalent and disabling condition.
Chronic Low Back Pain
 Chronic Low Back Pain North American Spine Society Public Education Series What is Chronic Pain? Low back pain is considered to be chronic if it has been present for longer than three months. Chronic low
Chronic Low Back Pain North American Spine Society Public Education Series What is Chronic Pain? Low back pain is considered to be chronic if it has been present for longer than three months. Chronic low
Neck Pain Overview Causes, Diagnosis and Treatment Options
 Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Fibromyalgia Syndrome
 Fibromyalgia Syndrome Fibro (fibre) Myo (muscle) Algia (pain) Syndrome (group of symptoms). Fibromyalgia, also known as Fibrositis, is not necessarily known as a disease; it may be better described as
Fibromyalgia Syndrome Fibro (fibre) Myo (muscle) Algia (pain) Syndrome (group of symptoms). Fibromyalgia, also known as Fibrositis, is not necessarily known as a disease; it may be better described as
Please fill out (in medium blue or black pen) as completely as possible and bring to your first visit.
 PATIENT S NAME MED. REC. # PATIENT QUESTIONNAIRE HEADACHE DOB Patient Identification Please fill out (in medium blue or black pen) as completely as possible and bring to your first visit. Patient Name:
PATIENT S NAME MED. REC. # PATIENT QUESTIONNAIRE HEADACHE DOB Patient Identification Please fill out (in medium blue or black pen) as completely as possible and bring to your first visit. Patient Name:
A Manic Episode is defined by a distinct period during which there is an abnormally and persistently elevated, expansive, or irritable mood.
 Bipolar disorder Bipolar (manic-depressive illness) is a recurrent mode disorder. The patient may feel stable at baseline level but experience recurrent shifts to an emotional high (mania or hypomania)
Bipolar disorder Bipolar (manic-depressive illness) is a recurrent mode disorder. The patient may feel stable at baseline level but experience recurrent shifts to an emotional high (mania or hypomania)
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Pain Syndromes Acute Neck and Back Pain with or without arm or leg pain Chronic Neck and Back Pain with or without arm or leg pain
 Pain Syndromes The most common and best understood type of pain is acute pain. Acute pain will result when tissue is injured by trauma, surgery, illness, or infection. This type of pain is generally understood
Pain Syndromes The most common and best understood type of pain is acute pain. Acute pain will result when tissue is injured by trauma, surgery, illness, or infection. This type of pain is generally understood
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
TMJ Exercises Information for patients
 Oxford University Hospitals NHS Trust Specialist Surgery TMJ Exercises Information for patients What is the Temporomandibular Joint? The temporomandibular joint (TMJ) is located in front of the ear where
Oxford University Hospitals NHS Trust Specialist Surgery TMJ Exercises Information for patients What is the Temporomandibular Joint? The temporomandibular joint (TMJ) is located in front of the ear where
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Emergency and inpatient treatment of migraine: An American Headache Society
 Emergency and inpatient treatment of migraine: An American Headache Society survey. The objective of this study was to determine the practice preferences of AHS members for acute migraine treatment in
Emergency and inpatient treatment of migraine: An American Headache Society survey. The objective of this study was to determine the practice preferences of AHS members for acute migraine treatment in
Diagnosis of TMD and Associated Head Pain. Cortex Thalamus C 1 C 2 C 3. A Peer-Reviewed Publication Written by Steven R.
 Cortex Thalamus Earn 3 CE credits This course was written for dentists, dental hygienists, and assistants. C 1 C 2 C 3 Diagnosis of TMD and Associated Head Pain A Peer-Reviewed Publication Written by Steven
Cortex Thalamus Earn 3 CE credits This course was written for dentists, dental hygienists, and assistants. C 1 C 2 C 3 Diagnosis of TMD and Associated Head Pain A Peer-Reviewed Publication Written by Steven
6245.02: Headache 6245.02 HEADACHE
 INTRODUCTION Headache is among the most common complaints encountered by emergency healthcare clinicians. The goal of managing a patient with headache involves identifying emergent versus non-emergent
INTRODUCTION Headache is among the most common complaints encountered by emergency healthcare clinicians. The goal of managing a patient with headache involves identifying emergent versus non-emergent
Spine University s Guide to Neuroplasticity and Chronic Pain
 Spine University s Guide to Neuroplasticity and Chronic Pain 2 Introduction Neuroplasticity is also called Brain Plasticity. Neuroplasticity is the ability of your brain to reorganize neural (nerve) pathways
Spine University s Guide to Neuroplasticity and Chronic Pain 2 Introduction Neuroplasticity is also called Brain Plasticity. Neuroplasticity is the ability of your brain to reorganize neural (nerve) pathways
Recognition and Management of Headache
 Clinical P r a c t i c e Recognition and Management of Headache Sujay A. Mehta, DMD; Joel B. Epstein, DMD, MSD, FRCD(C); Charles Greene, DDS ABSTRACT Contact uthor Dr. Mehta Email: mehta@ interchange.ubc.ca
Clinical P r a c t i c e Recognition and Management of Headache Sujay A. Mehta, DMD; Joel B. Epstein, DMD, MSD, FRCD(C); Charles Greene, DDS ABSTRACT Contact uthor Dr. Mehta Email: mehta@ interchange.ubc.ca
Angela Wilkin May 2013
 Angela Wilkin May 2013 Upper Motor Neuron v Lower Motor Neuron Lesions UMN Lesion LMN Lesion Forehead usually unaffected (bilateral innervation) Forehead affected Contralateral side Ipsilateral side Often
Angela Wilkin May 2013 Upper Motor Neuron v Lower Motor Neuron Lesions UMN Lesion LMN Lesion Forehead usually unaffected (bilateral innervation) Forehead affected Contralateral side Ipsilateral side Often
Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury. Canadian Family Physician
 Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury 1 Canadian Family Physician Volume 32, September 1986 Arthur Ameis, MD Dr. Ames practices physical medicine and rehabilitation,
Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury 1 Canadian Family Physician Volume 32, September 1986 Arthur Ameis, MD Dr. Ames practices physical medicine and rehabilitation,
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
What Is an Arteriovenous Malformation (AVM)?
 What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Cluster headache: Epidemiology, clinical features,
 Página 1 de 14 Official reprint from UpToDate www.uptodate.com Print Back Cluster headache: Epidemiology, clinical features, and diagnosis Author Arne May, MD Section Editor Jerry W Swanson, MD Deputy
Página 1 de 14 Official reprint from UpToDate www.uptodate.com Print Back Cluster headache: Epidemiology, clinical features, and diagnosis Author Arne May, MD Section Editor Jerry W Swanson, MD Deputy
Botulinum toxin in the treatment of chronic migraine. Gregory P. Hanes, MD Neuroscience Summit 5/14/15
 Botulinum toxin in the treatment of chronic migraine Gregory P. Hanes, MD Neuroscience Summit 5/14/15 Primary Headache Disorders: Frequency Classification After Secondary Causes Are Ruled Out Short-Duration
Botulinum toxin in the treatment of chronic migraine Gregory P. Hanes, MD Neuroscience Summit 5/14/15 Primary Headache Disorders: Frequency Classification After Secondary Causes Are Ruled Out Short-Duration
Role of Electrodiagnostic Tests in Neuromuscular Disease
 Role of Electrodiagnostic Tests in Neuromuscular Disease Electrodiagnostic tests Electroencephalogram (EEG) Electromyography (NCV, EMG) Cerebral evoked potentials (CEP) Motor evoked potentials (MEP) Electronystagmogram
Role of Electrodiagnostic Tests in Neuromuscular Disease Electrodiagnostic tests Electroencephalogram (EEG) Electromyography (NCV, EMG) Cerebral evoked potentials (CEP) Motor evoked potentials (MEP) Electronystagmogram
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Headache Medicine Core Curriculum
 Headache Medicine Core Curriculum Adopted by the United Council for Neurologic Subspecialties (UCNS) Board of Directors December 2005 2005 Table of Contents 1. Traditional Curriculum Components 3 A. Definition
Headache Medicine Core Curriculum Adopted by the United Council for Neurologic Subspecialties (UCNS) Board of Directors December 2005 2005 Table of Contents 1. Traditional Curriculum Components 3 A. Definition
There are two different types of migraines: migraines without aura and migraines with aura.
 What is migraine? A migraine is a relatively common medical condition that can severely affect the quality of life of the sufferer and his or her family and friends. 1 Almost 8% of Canadians over the age
What is migraine? A migraine is a relatively common medical condition that can severely affect the quality of life of the sufferer and his or her family and friends. 1 Almost 8% of Canadians over the age
Medications for chronic pain
 Medications for chronic pain When it comes to treating chronic pain with medications, there are many to choose from. Different types of pain medications are used for different pain conditions. You may
Medications for chronic pain When it comes to treating chronic pain with medications, there are many to choose from. Different types of pain medications are used for different pain conditions. You may
Colossus Important Diagnoses. Instructions for How to List Diagnoses
 1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
Headache Types. Behavioral Treatments of. Tension Headache. Migraine Headache. Mixed Headaches. TMJ Disorder. Tension Migraine.
 Headache Types Behavioral Treatments of Migraine Headaches Jonathan D. Cole, Ph.D. Clinical and Health Psychologist Bluegrass Health Psychology Lexington, KY Tension Migraine Mixed Cluster TMJ Tension
Headache Types Behavioral Treatments of Migraine Headaches Jonathan D. Cole, Ph.D. Clinical and Health Psychologist Bluegrass Health Psychology Lexington, KY Tension Migraine Mixed Cluster TMJ Tension
Botulinum Toxin in the Treatment of Chronic Migraine
 Botulinum Toin in the Treatment of Chronic Migraine ERIC L. FRY, MD ASSOCIATE PROFESSOR OF OPHTHALMOLOGY UNIVERSITY OF KANSAS FRY EYE ASSOCIATES, GARDEN CITY, KS History of Botulinum Toin Justinus Kerner,
Botulinum Toin in the Treatment of Chronic Migraine ERIC L. FRY, MD ASSOCIATE PROFESSOR OF OPHTHALMOLOGY UNIVERSITY OF KANSAS FRY EYE ASSOCIATES, GARDEN CITY, KS History of Botulinum Toin Justinus Kerner,
Name Date of Birth Social Security # XXX-XX- Address Apt. # City State Zip. Home Ph# Cell Ph# Driver s License #
 PATIENT INFORMATION Name Date of Birth Social Security # XXX-XX- Address Apt. # City State Zip Home Ph# Cell Ph# Driver s License # E-mail address: Race: Afro-American Am-Indian American Asian Black Caucasian
PATIENT INFORMATION Name Date of Birth Social Security # XXX-XX- Address Apt. # City State Zip Home Ph# Cell Ph# Driver s License # E-mail address: Race: Afro-American Am-Indian American Asian Black Caucasian
Anatomy: The sella is a depression in the sphenoid bone that makes up part of the skull base located behind the eye sockets.
 Pituitary Tumor Your doctor thinks you may have a pituitary tumor. Pituitary tumors are benign (non-cancerous) overgrowth of cells that make up the pituitary gland (the master gland that regulates other
Pituitary Tumor Your doctor thinks you may have a pituitary tumor. Pituitary tumors are benign (non-cancerous) overgrowth of cells that make up the pituitary gland (the master gland that regulates other

![Bell s Palsy ]]> <![CDATA[Bell's Palsy]]> Bell s Palsy ]]> <![CDATA[Bell's Palsy]]>](/thumbs/27/10105461.jpg)