THREE-DIMENSIONAL EVALUATION OF IMPLANT-SUPPORTED RAPID MAXILLARY EXPANSION VS. TRADITIONAL TOOTH-BORNE RAPID MAXILLARY EXPANSION USING CONE-BEAM
|
|
|
- Gladys Ramsey
- 10 years ago
- Views:
Transcription
1 THREE-DIMENSIONAL EVALUATION OF IMPLANT-SUPPORTED RAPID MAXILLARY EXPANSION VS. TRADITIONAL TOOTH-BORNE RAPID MAXILLARY EXPANSION USING CONE-BEAM COMPUTED TOMOGRAPHY Mary Ellen Helmkamp, D.D.S. An Abstract Presented to the Graduate Faculty of St. Louis University in Partial Fulfillment of the Requirements for the Degree of Master of Science in Dentistry (Research) 2012
2 Abstract Introduction: Transverse maxillary deficiency is a common problem among patients seeking orthodontic care and rapid maxillary expansion (RME) is one of the most frequent methods used by orthodontists to treat this problem. With the advent of orthodontic mini-screw implants, new appliances have been developed that use the palatal bone rather than the teeth as anchorage for the expansion appliance. Purpose: The purpose of this study is to evaluate the skeletal and dental effects of rapid maxillary expansion in the transverse plane using two different expansion appliances: a traditional tooth-supported Hyrax expander versus an implantsupported rapid maxillary expansion appliance. Materials and Methods: A sample of 11 patients who have been treated with an implant-supported RME and 18 patients who have been treated with a Hyrax RME were utilized for this study. CBCT scans were taken before treatment (T1) and immediately following full activation of the expansion appliances (T2). Defined landmarks were located on the pre- and post-treatment orientated images. Changes in pre- and post-treatment measurements were noted and differences between the two treatment groups were evaluated using the Mann-Whitney U test and independent samples t-test. Results: RME produced an increase in all the maxillary transverse dimensions at the skeletal, alveolar, and dental levels for both the implant-supported and tooth-borne Hyrax RME groups. Significant differences (p <0.05) in treatment changes were found at two parameters: maxillary base width at the level of the premolar and left premolar angulation. For both treatment groups, there was less expansion at the skeletal level than the dental level. Conclusions: Both groups showed similar results with greater expansion occurring at the dental level than skeletal level. Crown expansion was greatest followed by alveolar expansion and sutural expansion. Implant-supported RME may serve as a non-surgical alternative to traditional tooth-borne RME when anchorage to the teeth is 1
3 undesirable or unavailable. Further studies are needed to evaluate treatment differences between implant-supported expansion appliances and tooth-borne rapid maxillary expanders. 2
4 THREE DIMENSIONAL EVALUATION OF IMPLANT-SUPPORTED RAPID MAXILLARY EXPANSION VS. TRADITIONAL TOOTH-BORNE RAPID MAXILLARY EXPANSION USING CONE-BEAM COMPUTED TOMOGRAPHY Mary Ellen Helmkamp, D.D.S. A Thesis Presented to the Graduate Faculty of St. Louis University in Partial Fulfillment of the Requirements for the Degree of Master of Science in Dentistry (Research) 2012
5 COMMITTEE IN CHARGE OF CANDIDACY: Professor Rolf G. Behrents, Chairperson and Advisor Professor Eustaquio A. Araujo Professor Donald R. Oliver i
6 Dedication I dedicate this to my loving family, especially my parents. They have encouraged, supported and helped me every step of the way. They instilled in me the desire to dream big, work hard, and always give my very best in everything I do. I feel grateful to have such an amazing family. ii
7 Acknowledgements I would like to acknowledge a number of individuals for their contributions to this thesis. Dr. Kim for introducing me to the implant-supported rapid maxillary expander and all the advice and encouragement he gave to me along the way. Dr. Behrents for making me look at things from different and new perspectives and for helping me with organization. Dr. Araujo for his constant encouragement and advice through the entire process. Dr. Oliver for his analytical eye and attention to detail. Heidi Israel for her help in statistical analysis. iii
8 TABLE OF CONTENTS List of Tables... v List of Figures... vi CHAPTER 1: INTRODUCTION... 1 CHAPTER 2: REVIEW OF LITERATURE Growth and Development of the Maxilla... 4 Etiology of Transverse Maxillary Deficiency... 5 History of Rapid Maxillary Expansion... 7 Biomechanical Basis of Rapid Maxillary Expansion... 9 Expansion Appliances Skeletal and Dental Effects of Rapid Maxillary Expansion Bone-anchored Rapid Maxillary Expansion Summary and Statement of Thesis References CHAPTER 3: JOURNAL ARTICLE Abstract Introduction Materials and Methods Patient Selection Imaging Landmark Selection Statistics Results Discussion Conclusions References Vita Auctoris iv
9 List of Tables Table 3.1: Landmarks for transverse maxillary evaluation Table 3.2: Parameters measured for transverse maxillary evaluation Table 3.3: Comparison of maxillary transverse dimensions at T Table 3.4: Comparison of maxillary transverse dimensions at T Table 3.5: Comparison of the mean changes in maxillary transverse dimension from T1-T Table 3.6: Percentages of skeletal, alveolar, and dental expansion for both groups v
10 List of Figures Figure 3.1: Figure 3.2: Figure 3.3: Implant-supported RME design with four mini-screw implants and lingual wire extensions Implant-supported RME design with four mini-screw implants and no lingual wire extensions Implant-supported RME design with two mini-screw implants and lingual wire extensions Figure 3.4: Tooth-borne Hyrax RME Figure 3.5: Cone-beam computed tomography image orientation Figure 3.6: Figure 3.7: Cone-beam computed tomography coronal slice at the molar level with landmarks Cone-beam computed tomography coronal slice at the premolar level with landmarks vi
11 CHAPTER 1: INTRODUCTION Transverse maxillary deficiency is a common problem among patients seeking orthodontics care. It is characterized by a narrow maxilla in relation to the rest of the craniofacial structures, a narrow palatal vault, and often a posterior crossbite. According to a recent epidemiological study, the prevalence of some form of posterior crossbite in the primary dentition is 20.81%. 1 A long history of palatal expansion as a way to treat crossbites, anteroposterior discrepancies, dental crowding, and airway issues has made it a common treatment modality in most orthodontic practices today. The etiologies of transverse maxillary deficiency are numerous. It can be due to both genetic and environmental factors, soft tissue influences, cleft palate, low tongue position, CIII anteroposterior skeletal discrepancies, and habits. 2 Rapid maxillary expansion (RME) is one of the most frequent methods used by orthodontics to treat this problem. RME is based on the concept of widening the dental arch by means of opening the midpalatal suture. The concept dates back to 1860 when Angell described rapid expansion in a paper to the dental community. Since its origin, the concept of rapid maxillary expansion has been used to increase nasal permeability, correct posterior crossbites, and increase arch perimeter to relieve crowding and tooth size-arch length discrepancies. RME uses orthopedic forces to separate the two halves of the maxilla at the mid-palatal suture. 3 This is accomplished with an expansion screw that is anchored to the maxillary teeth and is typically activated 0.5 to 1 mm per day. Studies have reported various amounts of dental and skeletal expansion that occur with RME, but it is postulated that RME produces expansion that is 50% dental and 50% skeletal. 4 It is often the goal of orthodontists to maximize skeletal expansion and minimize dental expansion 1
12 in order to prevent unwanted negative side effects. Disadvantages that have been identified with traditional tooth-borne expansion appliances include limited skeletal movement, undesirable tooth movement and dental tipping, root resorption, dehiscence, and relapse. Because of these disadvantages alternative methods have been developed including implant-supported rapid maxillary expanders. These appliances anchor the expansion screw directly to the palatal bone rather than using the teeth as anchorage for the device. Skeletal anchorage devices have been successfully used in the past and include palatal distracters, implant-supported Hyrax screws, and bone anchors for maxillary protraction. 5 Only a limited number of studies have been published that test the differences between traditional tooth-borne expansion appliances versus bone-anchored expansion appliances though. Of the studies published, many have used distraction or surgically-assisted rapid maxillary expansion protocols which involve a more invasive surgical procedure for the patient. Studies using either a bone-anchored hyrax expansion screw with surgically-assisted expansion or palatal distraction have been done to compare the effects of these appliances with tooth-anchored expansion appliances. Cortese et al. found that after expansion with a palatal distractor device, there was minimal tipping of the teeth and that the main movement was of the maxillary segments themselves. 6 Likewise, studies evaluating the effects of surgically assisted expansion using bone-borne implant supported expansion appliances show minimal dental tipping, greater expansion at the level of the alveolar process than the tooth crown, suggesting greater skeletal expansion than dental expansion. 7-8 Harzer et al. found 10 degrees less molar tipping than toothsupported expansion in their study looking at the effects of direct fixation of the expansion screw to the palatal bone for RME. 9 All of these studies involved surgically-assisted expansion. 2
13 On the contrary, Lagravère et al. used cone-beam computed tomography to evaluate bone-anchored versus traditional rapid maxillary expansion in adolescents. Unlike the previous studies, Lagravère et al. concluded that the skeletal and dental changes for both groups were similar. 10 Recently, hybrid appliances using mini-implant and tooth-borne RME have been introduced as well. These appliances are cited as having the advantage of being less invasive than traditional bone-borne expansion devices that involve surgical involvement while providing the benefit of less buccal tooth tipping associated with tooth-borne expansion appliances Despite the varying conclusions that have been made in the literature regarding the differences between bone-anchored and tooth-borne rapid maxillary expansion, little research has been done evaluating implant-supported RME versus tooth-borne RME without the use of surgically assisted expansion or distraction. The purpose of this study is to use CBCT to evaluate and compare the skeletal and dental changes in the transverse dimension following rapid maxillary expansion with an implantsupported expansion appliance versus a tooth-born expansion appliance. Additionally, suture opening, alveolar expansion, tooth expansion and tooth angulation changes will be evaluated. 3
14 CHAPTER 2: REVIEW OF THE LITERATURE Growth and Development of the Maxilla In order to better understand the etiology of transverse maxillary deficiency, one should first understand the normal growth and development of the maxilla, particularly transverse growth and development. The bones of the maxilla develop entirely through intramembranous ossification. Growth occurs either by apposition of bone at the sutures or surface remodeling. 4 Growth of the soft tissues translates the maxillary complex downward and forward as bone fills in the space opened at the posterior and superior sutures. This downward and forward growth of the maxilla is accompanied by a corresponding resorption of the anterior surfaces of the maxilla by surface remodeling. 4 The midpalatal suture develops at about 12 weeks in utero and growth was originally thought to cease at around 3 years of age. 13 Latham s study of histological specimens ranging in age from 16 weeks in utero to 15 years of age, notes that although sutural growth stopped early, fusion had not occurred in any of his specimens. Growth rates in the transverse, vertical and horizontal planes vary depending on age. According to a study by Snodell et al., at the age of 6 the transverse dimension had a greater percentage of adult size than vertical measurement for males and females. 14 The transverse dimension is the first to reach adult size, followed by sagittal and vertical. Because of this fact, questions as to when the suture fuses and growth is complete becomes of importance in treatment planning. It is known that the midpalatal suture does not fuse until somewhere between the ages of years on average and even older in some cases. Bjork found that age 17 was the average age in which the median suture fused. 15 Melsen found growth of the suture of the maxilla to fuse at age 16 years in females and 18 years 4
15 in males, while Snodell et al. found that transverse growth was completed for the majority of females at age 15 and 17 years for males. 14 This is important in the timing of rapid maxillary expansion treatment, as it is expected to be successful in patients that have not reached the age in which their midpalatal suture has fused. Implant studies by Bjork and Skieller state that growth in the median suture is the most important factor in growth in the width of the maxilla. Their studies show that in general the two maxillae rotate in relation to each other in the traverse plane during development, while at the same time the maxilla shifts forward in the sagittal plane and rotates, forward or backward, in the vertical plane. From ages 10 to adulthood, the width of bilateral implants increased.9 mm in the anterior region and 3.0 mm in the posterior region. This indicates a greater amount of transverse growth posteriorly than anteriorly. 15 Similar findings were found by Korn and Baumrind in their implant study on transverse development of the human jaws between ages 8.5 and 15.5 years. They concluded that transverse widening was greater in the more posterior part of the palate and found annual growth rates that closely corresponded to the rates found by Bjork and Skieller. 16 Gandini and Buschang s study using metallic implants found maxillary width increases that were 0.1 mm/yr less than previous studies. The authors attributed this difference to the growth potential of their treatment groups which were 14 years of age at the initiation of treatment. 17 Etiology of Transverse Maxillary Deficiency Transverse maxillary deficiency is characterized by a narrow maxilla in relation to the rest of the craniofacial structures, a narrow palatal vault and often the presence of a unilateral or 5
16 bilateral posterior crossbite or dental crowding. Both posterior crossbite and dental crowding are some of the easily recognizable signs of maxillary deficiency. Estimates of the percentage of children and adolescents exhibiting a posterior crossbite vary in the literature. The Division of Health Statistics of the U.S. Public Health Service estimated the prevalence of various malocclusions in a large scale survey in Proffit notes that this survey (NHANES III) found the prevalence of posterior crossbite among all races, genders, and age to be 9.1% of the U.S. population. 4 This is similar to Helm s estimate of the prevalence of unilateral or bilateral crossbites in 9.4% of boys and 14.1% of girls. 18 Others have estimated anywhere from 1.0% to 23.5% of children as having a posterior crossbite in the primary dentition. 1 According to a more recent epidemiologic study by da Silva et al., 20.81% of children have some form of posterior crossbite in the primary dentition. 1 Despite the variation over the exact incidence of posterior crossbites, orthodontists are routinely confronted with the challenge of correcting a transverse maxillary deficiency and etiology is an important consideration in treatment planning. Posterior crossbites can be dental or skeletal in origin or a combination of both. Likewise, the discrepancy may originate in the maxilla or the mandible or a little of both. Haas makes an important point in distinguishing true maxillary deficiency from relative maxillary deficiency. Relative maxillary deficiency occurs when the maxilla is the correct size compared with the upper face, but the mandible is too large resulting in a posterior crossbite. On the other hand, true maxillary deficiency is characterized by a small maxilla and constriction of the buccal tooth segments, indicating a true undersized maxilla A narrow maxilla can be due to genetic or environmental factors or a combination of both. 2 Possible causes include cleft palate, soft tissue influences, true skeletal transverse discrepancy between the maxilla and mandible, non-nutritive sucking habits, open mouth 6
17 posture, low tongue position, Class III anteroposterior skeletal discrepancies, and abnormal function. 2 Treatment is individualized based on the nature of the discrepancy, etiology, and skeletal maturity of the patient. History of Rapid Maxillary Expansion The concept of widening the dental arch by means of opening the midpalatal suture dates back to 1860 when Angell described rapid expansion of the upper arch in a paper he presented to the dental community. In the first issue of Dental Cosmos in 1860, he wrote of an apparatus that at the end of two weeks, the jaw was so widened as to leave a space between the front incisors, showing conclusively that the maxillary bones had been separated. 21 This concept of splitting the suture to expand the maxilla flourished during the early 1900s. These years have been referred to as the maxillary expansion years by both orthodontists and rhinologists. It was during this time that rhinologist Brown, as well as many others, promoted maxillary expansion for the purpose of increasing nasal permeability and obtaining greater nasal width Pfaff supported this concept with the opinion that expansion of the dental arch lowered the palatal vault and induced straightening of the nasal septum. 24 Indications for RME are widespread in the literature. These include lateral discrepancies resulting in unilateral or bilateral crossbites, anteroposterior discrepancies, cleft lip and palate and to gain arch length. Rapid maxillary expansion as a means of increasing arch width and perimeter became a popular area of investigation resulting in numerous clinical and animal studies on the subject in the mid-1900s. Cleall et al. 25 published a paper indicating that strong expansion forces applied to the maxilla of a growing Macaca rhesus monkey resulted in the 7
18 breakdown of the midpalatal suture and eventual restoration of normal sutural morphology. Likewise, Haas pig study indicated that the midpalatal suture could indeed be opened to a degree sufficient to cause a widening of the dental arch and an increase in intranasal capacity. 23 In the same publication, Haas clinical study described the direction of opening of the suture, effect on the surrounding structures and the corresponding buccal inclination of the mandibular teeth. In the 1950s, following Bjork s protocol, Krebs implant studies showed an increase in dental arch width that was about half of the basal maxillary segments and noted rotation of the maxillary segments in the frontal plane. 26 Haas became one of the leaders in research regarding palatal expansion at that time and wrote numerous articles on the effects of palatal expansion. In an article in 1970, Haas noted the specific skeletal effects of rapid palatal including a triangular pattern of opening with the apex being in the nasal cavity. 27 He also noted that the procedure produced forward and downward movement of the maxilla and downward and backward rotation of the mandible. 27 Many other authors have verified the finding that rapid maxillary expansion causes the palatal shelves to rotate upon opening resulting in the rotation of the palatal processes, alveolar processes and teeth around the midpalatal suture. 28 Starnbach elaborated on this concept by looking at the effects of rapid maxillary expansion on the entire craniofacial skeleton and the dental changes that resulted, noting that not only do changes in the midpalatal suture occur but histologic changes are also seen in the zygomaticomaxillary suture and the zygomaticotemporal sutures as well. 28 Rapid maxillary expansion has also been used to alleviate tooth size-arch length discrepancies as an alternative to extractions, providing additional space in the arch to relieve crowding. With rapid maxillary expansion, studies show an increase in arch perimeter of 8
19 4-4.7 mm in maxilla and 2.5 mm in the mandible According to Adkins et al., RME with Hyrax appliances produce an increase in maxillary arch perimeter at the rate of approximately 0.7 times the change in first premolar width. 29 Biomechanical Basis of Rapid Maxillary Expansion Bell summed up the mechanics of rapid maxillary expansion simply when he reported, If the applied transverse forces are of sufficient magnitude to overcome the bioelastic strength of the sutural elements, orthopedic separation of the maxillary segments can occur. 31 This is the basis of rapid maxillary expansion. At the same time, expansion appliances compress the periodontal ligament, bend the alveolar processes, tip the anchor teeth, and gradually open the midpalatal suture when the forces exceed the limits needed for orthodontic tooth movement. 32 Typically, rapid maxillary expansion is done with a jackscrew at the rate of mm per day, while slow maxillary expansion is done at a rate of 1 mm per week. According to Isaacson, a single activation of the expansion screw produces 3-10 pounds of force, with a smaller load being produced per activation in younger patients as compared with more mature patients. 3 The midpalatal suture becomes more interdigitated with age and therefore heavier forces are needed to overcome the partially interlocked suture in older adolescents and adults. These forces decay rapidly following activation, but the rate of decay decreases within several minutes. 3 Active expansion usually takes place for 2-3 weeks followed by 3-6 months of the appliance being left in place as the suture reorganizes. According to Isaacson, the main resistance to rapid maxillary expansion is not just the midpalatal suture but the other maxillary articulations. 3 The maxilla articulates with ten other 9
20 bones in the face and cranium and resistance to midpalatal suture opening is partly due to this, especially the zygomatic and sphenoid bones. 32 In order to minimize dental tipping and get a more linear opening of the midpalatal suture, the rigidity of both the expansion screw and wires joining it to the teeth should be as high as possible. Braun discusses the fact that the moments induced by the dentomaxillary centers of resistance and the moment-to-force ratios at the centers of resistance are reduced as the rigidity of the appliance is increased. 33 For this reason Braun advises against using an acrylic interface with the teeth as this is less stiff than stainless steel wires. Expansion Appliances The rationale behind rapid maxillary expansion is that the orthopedic forces exerted by the expansion appliance can, up to a certain age, open the midpalatal suture and widen the palate. Although it has been documented that expansion appliances in some form or another have been used since the 1860s, regular use of the appliance did not become popular until Haas introduced his expansion appliance in the 1950s. The Haas expander consists of a metal framework with an expansion screw in the palatal vault, bands on the first molars and premolars, an acrylic pad on the palatal tissue and buccal soldered bars as well to maximize anchorage and promote suture opening. 27 According to Haas, the split acrylic palatal appliance is superior in that the orthopedic force is resisted by the inclined walls of the palatal vault, alveolar process, and teeth resulting in less tooth movement and a more orthopedic movement than other expansion appliances that do not have an acrylic pad on the palatal shelves
21 An alternative to the Haas appliance is the hygienic or Hyrax expander developed by Biederman. This appliance was developed in response to the soft tissue irritation often seen with the Haas appliance. 34 The Hygienic appliance consists of four orthodontic bands placed on the maxillary first molars and premolars with a expansion screw in the middle of the palate and a.040 buccal wire connecting the molar to the premolar bands on the buccal side of the teeth. Like the Haas appliance, activation is two turns per day and a retention period of 3 months. According to Biederman, the main advantages of the hygienic appliance are patient comfort, easier hygiene, and prevention of lesions to the palatal mucosa. The Haas and Hyrax expansion appliances are the most widely used and studied appliances. The main difference is simply the presence or absence of the acrylic pad which some say has a large effect of the amount of skeletal versus dental expansion that is achieved. Garib et al. performed a study evaluating the differences between the two appliances by means of computed tomography (CT). They concluded that both appliances produced significant increases in all transverse dimensions with a decreasing upward expanding effect. 35 It was determined that both appliances produced similar orthopedic effects, while the tooth-tissue borne expander produced a greater change in the axial inclination of the supporting teeth especially the premolars. 35 More recently, expansion appliances have been developed that use mini-screw implants to secure the expansion screw directly to the palate, reducing the forces being placed directly on the teeth. Obviously this form of RPE, has been developed in an effort to maximize skeletal expansion and minimize dental tipping. The idea of avoiding direct forces on the teeth in order to maximize the orthopedic effect is the basis of bone-anchored rapid maxillary expanders, although appliance designs can vary greatly. Palatal distractors have been developed as an 11
22 alternative to tooth-borne expansion appliances as well. 7-8, Some of the first appliances to utilize this concept were variations of palatal distracters to expand the palate in adult patients after surgical osteotomy. Cortese developed an appliance consisting of four 8 mm mini-screw implants that secure 2 titanium miniplates and a titanium jackscrew to the palate. 6 Likewise, Lagrevère used a bone-anchored maxillary expander that consisted of an expansion screw and 2 stainless steel onplants secured to the palate by 2 mini-screw implants. 10 Likewise, hybrid appliances utilizing mini-screw implants and tooth-borne RME have been developed as well These more recent alternatives to the traditional tooth-borne appliances could serve as possible future replacements for the Haas and Hyrax appliances if the orthopedic effects of these appliances prove to be superior. Skeletal and Dental Effects of Rapid Maxillary Expansion The exact dental and skeletal effects of rapid maxillary expansion have been studied extensively and, although skeletal expansion is the goal of treatment, a significant amount of dental expansion occurs as well. Because of the difficulty in comparing samples that have large variations in age, size, retention protocol, and the amount of expansion accomplished, clinical studies have reported varying amounts of skeletal versus dental expansion. Proffit notes that the expansion achieved with RME is 50% skeletal and 50% dental. This is supported by numerous studies including Podessor s evaluation of the effects of RME in growing children using computed tomography. This study found actual skeletal expansion to vary from 25% to 53% of the total expansion. 18 Chung and Font found that 9.7% of the first premolar expansion and 4.3% of the first molar expansion was due to buccal crown tipping. 38 In a study by Ghoneima et al 12
23 using CT to evaluate changes with RME, they concluded that although significant increases occur in most dental and skeletal measurements, dental tipping explained most of the expansion. 39 Skeletally, RME separates the midpalatal suture as the two halves of the palate rotate laterally forming a triangular or wedge shaped pattern of opening. The widest areas of expansion are located anteriorly from an occlusal view and apically from a frontal view ,27-28,33,40-41 Numerous studies have found the center of rotation for the maxilla in the area of the frontonasal suture. 22,27,33 It is thought that the two palatal halves rotate around a point located near the frontonasal suture. 22 With RME, the maxilla moves in a forward and downward direction and the mandible is thought to move downward and backward, opening the mandibular plane 22, 38,42 angle. Arch perimeter gains can be attributed to rapid maxillary expansion as well. Geran et al. notes a significant increase in arch perimeter in the maxilla and mandible compared to controls. 30 Dentally, there is buccal movement of the posterior teeth and alveolar processes. Because the appliance is anchored to the teeth, buccal tipping of the dentition is one of the most common and undesirable side effects of RME. Schiffman and Tuncay published a meta-analysis that summarized the long term changes documented in the maxillary expansion literature from The results of their metaanalysis gave an average immediate expansion of 6.0 mm which relapsed to 4.71 mm after short term retainer wear, then further reduced to 3.88 mm after the retention period. In the long term, expansion was only 2.4 mm. Their conclusion was that this amount was no greater than documented with normal growth and no useful expansion beyond normal growth is achieved in the long term
24 In a separate meta-analysis by Lagravère et al. in 2006, the immediate changes with rapid maxillary expansion were looked at. Immediate dental changes in the transverse dimension included an increase of mm in maxillary intermolar width, 5.35 mm increase in intercanine width, and a 3.1 degree increase in intermolar angulation. 44 The mandibular intermolar width increase was only.49 mm and was not statistically significant. Skeletally, the nasal cavity width increased 2.14 mm and the left and right jugale width increased 2.73 mm. Overall, the greatest dental and skeletal changes occurred in the transverse dimension. On average, 6.7 mm of expansion was noted as measured between the maxillary molar crowns, while 4.5 mm of expansion was noted at the maxillary molar root apexes supporting the claim that RME using tooth-anchored appliances will cause tipping of the teeth. The average tipping of the teeth was 3 degrees. 44 Additionally, significant skeletal increases for maxillary interalveolar width measured from the buccal plates increased 2-3 mm, showing a large portion of the true expansion must be dental rather than skeletal. In a systematic review published by Lagravère et al. in 2005, the long-term dental arch effects of rapid maxillary expansion were evaluated and the following conclusions were made. Rapid maxillary expansion resulted in a significant long-term maxillary molar width increase as well as consistent maxillary cuspid arch width expansion of mm. Less mandibular molar and cuspid expansion was attained in adults compared to children and significant gains in arch perimeter of 6mm in the maxilla and 4.5 mm in the mandible were attained in adolescents, and no anteroposterior or vertical changes were associated with RME. 45 Recently, studies utilizing cone-beam computed tomography (CBCT) rather than two dimensional radiographs to evaluate the skeletal and dental effects of RME have become more abundant. Garrett et al evaluated the skeletal and dental effects of the maxilla after RME using 14
25 CBCT. These authors found that orthopedic or skeletal expansion accounted for 55% of the total expansion at the first premolar, 45% at the second premolar, and 38% at the first molar. Alveolar tipping accounted for 6% at the first premolar, 9% at the second premolar, and 13% at the first molar. Dental tipping accounted for 39% of the expansion at the first premolar, 46% at the second premolar, and 49% at the first molar. Alveolar and dental tipping were greater posteriorly than anteriorly. 40 On the contrary, Kartalian et al. used CBCT and found no statistically significant amount of relative dental tipping, but did find significant alveolar tipping as compared to controls. 46 The angle of the alveolus significantly increased on average by approximately 5 degrees in the RME group, while the alveolar angulation of the control groups decreased by an average of 2.84 degrees. This study found no changes in relative dental tipping as the teeth remained relatively constant in their angulation, while previous studies found dental tipping changes anywhere from 2.5 to 6 degrees. 44,47 Furthermore, the author notes that the posterior teeth actually moved in a slightly lingual direction due to denture uprighting after the expansion. While there is significant literature on the skeletal and dental effects of RME, the exact values and percentages of skeletal and dental changes vary greatly. This is due to a number of factors that make comparing samples and studies difficult, including variations in expansion appliance design, activation protocol and methods of assessing the expansion. Bone-anchored Rapid Maxillary Expansion Traditional tooth-borne expansion appliances have been effectively used for decades to correct transverse maxillary deficiencies, yet this treatment is not without negative side effects. 15
26 Disadvantages have been identified with traditional tooth-borne expansion appliances including limited skeletal movement, undesirable tooth movement, root resorption, dehiscence, a decrease 5,10, in the thickness of the buccal cortical plate and relapse. Because of these disadvantages, alternative methods have been developed including the implant-supported rapid maxillary expander. These appliances anchor the expansion screw directly to the palatal bone, avoiding direct tooth contact. Likewise, bone-anchored expansion appliances may be indicated when a patient has missing or compromised posterior permanent teeth and periodontal concerns, providing an alternative when traditional RME cannot be used. Skeletal anchorage devices have been successfully applied in patients in the past. These include palatal distracters for rapid palatal expansion, implant-supported Hyrax screw for RME and bone anchors for maxillary protraction. 5 To date, only a limited number of studies have been published that test the differences between traditional tooth-borne expansion appliances versus bone-anchored expansion appliances. Many of these studies used distraction or surgically assisted expansion protocols involving slightly more invasive surgical procedures. Cortese et al. used a palatal distractor device to treat severe maxillary constriction in adult patients who were to undergo surgically assisted rapid maxillary expansion. 6 The palatal distractor device was made of a titanium expansion, 2 titanium miniplates and four mini-screw implants. The procedure involved general anesthesia for a Le Fort I-type osteotomy and separation of the palate at the median line and results were evaluated using computed tomography (CT). Expansion averaged 5.1 mm at the canines, 4.5 mm at the first premolars, and 3.7 mm at the molars. The authors noted that the angular changes in the frontal plane were minimal with a maximum change of 0.8 or less at the palatal molar cusp level, suggesting that the main movement involved rotation of the maxillary segments and not the teeth themselves. 16
27 Lagravère et al. used CBCT to evaluate the transverse, vertical, and anteroposterior changes associated with bone-anchored and traditional rapid maxillary expansion in adolescents. 10 The experimental group (bone-anchored maxillary expander) consisted of an appliance with two custom-milled onplants and 2 mini-screw implants (12 x 1.5 mm) to secure the expansion appliance directly to the palatal bone. This required the reflection of the periosteum and a second surgery to remove the appliance after treatment. Long term and short term changes were evaluated and the authors found that immediately after completion of appliance activation, the skeletal and dental changes for both treatment groups were similar. The primary difference was the there was greater expansion at the maxillary first premolars in the tooth-anchored maxillary expander group. Furthermore, root apex expansion was less than crown expansion for both the bone-anchored maxillary expander group and the tooth-anchored maxillary expander subjects, resulting in significant buccal crown inclination. 10 The results of this study indicate that tooth-anchored expansion appliances and bone-anchored expansion appliances produce similar results. Tausche et al. evaluated three-dimensional changes in dental, alveolar, and skeletal structures caused by a bone-borne implant supported rapid maxillary expander device (Dresden distractor) using CT. The authors found an average increase in the transverse dimension at the alveolar bone to be 7.52 mm in the premolar region and 7.17 mm in the molar region, noting that these were greater skeletal increases than previous studies using tooth-borne expanders. 7 There was.8 mm more expansion in the premolar region and.73 mm more in the molar region as measured at the alveolar bone than at the teeth. Stated more simply, the teeth tipped 6 degrees to 9 degrees less than the alveolar process. This suggests that the tooth crowns expanded less than 17
28 the alveolar bone, most likely due to application of direct force to the bone and the torque effect of the brackets. 7 Hansen et al. conducted a similar study with the aim of carrying out a three-dimensional analysis of the teeth, alveolar, and skeletal structures during bone-borne, surgically-assisted rapid maxillary expansion. CT showed a transverse expansion of 5.55 mm in the alveolar process of the premolar region and 4.87 mm in the molar region. Width increases were 6.07 mm in the premolar region and 5.71 mm in the molar region. Buccal tipping of the teeth was minimal, only degrees in the premolars and degrees in the molar region. Like Tausche et al. concluded, this is most likely due to the direct transfer of expansion forces to the bone and the torque of the brackets. 8 Harzer et al. published a pilot study of two females treated hyrax expansion screws with palatal anchorage. Bilateral osteotomy and splitting of the midpalatal suture was performed under general anesthesia and the hyrax expansions screw was directly fixed on one side with a titanium implant and on the other side with an osteosynthesis screw. The authors concluded that direct fixation of the hyrax expansion screw at the palatal bone for RME was an effective alternative to tooth-supported appliances and had 10 degrees less molar tipping than toothsupported expansion. 9 Advantages of implant-supported rapid maxillary expansion appear to be less dental tipping and more skeletal expansion, shorter treatment times, increased anchorage for expansion, and less periodontal effects. Varying conclusions have been made regarding the claim of the superiority of implant-supported RME versus traditional tooth-borne RME though and future 18
29 studies on the subject are indicated, especially with regard to bone-borne non-surgically assisted RME. Summary and Statement of Thesis Rapid maxillary expansion has been successfully used to treat transverse maxillary deficiencies by orthodontists for many years and researchers have been trying to quantify the exact dental and skeletal effects of this treatment. Although effective in correcting posterior crossbites and relieving dental crowding due to arch length discrepancies, undesirable side effects have been noted with both tooth and tissue-borne RME treatments. These include limited skeletal expansion, buccal crown tipping, undesirable tooth movements, and root resorption. Because of these side effects, alternatives to the traditional Haas or Hyrax tooth-borne appliances have been introduced, particularly the implant-supported RME. Implant-supported rapid maxillary expanders differ from the Hyrax expander in that the appliance does not have anchorage on the teeth. The goal is to decrease dental and alveolar tipping, root resorption, and dehiscence while increasing the orthopedic effect. Little research has been done comparing the effects of these two appliances without the use of surgical intervention. The purpose of this study is to use CBCT images to compare and contrast the skeletal and dental changes that occur in the transverse dimension following rapid maxillary expansion with these two appliances. Additionally, suture opening, alveolar bending, and molar and premolar angulation changes will be evaluated. 19
30 References 1. da Silva Filho OG, Santamaria M Jr, Capelozza Filho L. Epidemiology of posterior crossbite in the primary dentition. J Clin Pediatr Dent. 2007;32(1): Malandris M, Mahoney EK. Aetiology, diagnosis and treatment of posterior cross-bites in the primary dentition. Int J Paediatr Dent May;14(3): Isaacson RJ, Ingram A. Forces produced by rapid maxillary expansion II. Forces present during treatment. Angle Orthod Oct;34(4): Proffit WR, Henry W. Fields, Jr. Contemporary Orthodontics. Third. Mosby, Inc Wehrbein H, Göllner P. Skeletal anchorage in orthodontics--basics and clinical application. J Orofac Orthop Nov;68(6): Cortese A, Savastano M, Savastano G, Papa F, Howard CM, Claudio PP. Maxillary constriction treated by a new palatal distractor device: surgical and occlusal evaluations of 10 patients. J Craniofac Surg Mar;21(2): Tausche E, Hansen L, Hietschold V, Lagravère MO, Harzer W. Three-dimensional evaluation of surgically assisted implant bone-borne rapid maxillary expansion: a pilot study. Am J Orthod Dentofacial Orthop Apr;131(4 Suppl):S Hansen L, Tausche E, Hietschold V, Hotan T, Lagravère M, Harzer W. Skeletally-anchored rapid maxillary expansion using the Dresden Distractor. J Orofac Orthop Mar;68(2): Harzer W, Schneider M, Gedrange T. Rapid maxillary expansion with palatal anchorage of the hyrax expansion screw--pilot study with case presentation. J Orofac Orthop Sep;65(5): Lagravère MO, Carey J, Heo G, Toogood RW, Major PW. Transverse, vertical, and anteroposterior changes from bone-anchored maxillary expansion vs traditional rapid maxillary expansion: a randomized clinical trial. Am J Orthod Dentofacial Orthop Mar;137(3):304.e1 12; discussion Wilmes B, Nienkemper M, Drescher D. Application and effectiveness of a mini-implant- and tooth-borne rapid palatal expansion device: the hybrid hyrax. World J Orthod. 2010;11(4): Lee K-J, Park Y-C, Park J-Y, Hwang W-S. Miniscrew-assisted nonsurgical palatal expansion before orthognathic surgery for a patient with severe mandibular prognathism. Am J Orthod Dentofacial Orthop Jun;137(6): Latham RA. The development, structure and growth pattern of the human mid-palatal suture. J. Anat Jan;108(Pt 1):
31 14. Snodell SF, Nanda RS, Currier GF. A longitudinal cephalometric study of transverse and vertical craniofacial growth. Am J Orthod Dentofacial Orthop Nov;104(5): Björk A, Skieller V. Growth of the maxilla in three dimensions as revealed radiographically by the implant method. Br J Orthod Apr;4(2): Korn EL, Baumrind S. Transverse development of the human jaws between the ages of 8.5 and 15.5 years, studied longitudinally with use of implants. J. Dent. Res Jun;69(6): Gandini LG Jr, Buschang PH. Maxillary and mandibular width changes studied using metallic implants. Am J Orthod Dentofacial Orthop Jan;117(1): Podesser B, Williams S, Crismani AG, Bantleon H-P. Evaluation of the effects of rapid maxillary expansion in growing children using computer tomography scanning: a pilot study. Eur J Orthod Feb;29(1): Haas AJ. Long-term posttreatment evaluation of rapid palatal expansion. Angle Orthod Jul;50(3): Haas AJ. The treatment of maxillary deficiency by opening the midpalatal suture. Angle Orthod Jul;35: Angell EH. Treatment irregularities of the permanent or adult dentition. Dental Cosmos. 1860;1: Wertz RA. Skeletal and dental changes accompanying rapid midpalatal suture opening. Am J Orthod Jul;58(1): Haas AJ. Rapid expansion of the maxillary dental arch and nasal cavity by opening of the midpalatal suture. Angle Orthod. 1961;31: Pfaff W. Stenosis of the nasal cavity caused by contraction of the palatal arch and abnormal position of the teeth: Treatment by expansion of the maxilla. Dental Cosmos. 1905;47: Cleall JF, Bayne DI, Posen JM, Subtelny JD. Expansion of the midpalatal suture in the monkey. Angle Orthod Jan;35: Krebs A. Expansion of the midpalatal suture studied by means of metallic implants. European Orthodontic Society Rep. 1958;34: Haas AJ. Palatal expansion: just the beginning of dentofacial orthopedics. Am J Orthod Mar;57(3): Starnbach H, Bayne D, Cleall J, Subtelny JD. Facioskeletal and dental changes resulting from rapid maxillary expansion. Angle Orthod Apr;36(2):
32 29. Adkins MD, Nanda RS, Currier GF. Arch perimeter changes on rapid palatal expansion. Am J Orthod Dentofacial Orthop Mar;97(3): Geran RG, McNamara JA Jr, Baccetti T, Franchi L, Shapiro LM. A prospective long-term study on the effects of rapid maxillary expansion in the early mixed dentition. Am J Orthod Dentofacial Orthop May;129(5): Bell RA. A review of maxillary expansion in relation to rate of expansion and patient s age. Am J Orthod Jan;81(1): Bishara SE, Staley RN. Maxillary expansion: clinical implications. Am J Orthod Dentofacial Orthop Jan;91(1): Braun S, Bottrel JA, Lee KG, Lunazzi JJ, Legan HL. The biomechanics of rapid maxillary sutural expansion. Am J Orthod Dentofacial Orthop Sep;118(3): Biederman W. A hygienic appliance for rapid expansion. J Pract Orthod Feb;2(2): Garib DG, Henriques JFC, Janson G, Freitas MR, Coelho RA. Rapid maxillary expansion-- tooth tissue-borne versus tooth-borne expanders: a computed tomography evaluation of dentoskeletal effects. Angle Orthod Jul;75(4): Ramieri GA, Spada MC, Austa M, Bianchi SD, Berrone S. Transverse maxillary distraction with a bone-anchored appliance: dento-periodontal effects and clinical and radiological results. Int J Oral Maxillofac Surg Jun;34(4): Gerlach KL, Zahl C. Transversal palatal expansion using a palatal distractor. J Orofac Orthop Nov;64(6): Chung C-H, Font B. Skeletal and dental changes in the sagittal, vertical, and transverse dimensions after rapid palatal expansion. Am J Orthod Dentofacial Orthop Nov;126(5): Ghoneima A, Abdel-Fattah E, Eraso F, Fardo D, Kula K, Hartsfield J. Skeletal and dental changes after rapid maxillary expansion: a computed tomography study. Aust Orthod J Nov;26(2): Garrett BJ, Caruso JM, Rungcharassaeng K, Farrage JR, Kim JS, Taylor GD. Skeletal effects to the maxilla after rapid maxillary expansion assessed with cone-beam computed tomography. Am J Orthod Dentofacial Orthop Jul;134(1): da Silva Filho OG, Montes LA, Torelly LF. Rapid maxillary expansion in the deciduous and mixed dentition evaluated through posteroanterior cephalometric analysis. Am J Orthod Dentofacial Orthop Mar;107(3): Davis WM, Kronman JH. Anatomical changes induced by splitting of the midpalatal suture. Angle Orthod Apr;39(2):
33 43. Schiffman PH, Tuncay OC. Maxillary expansion: a meta analysis. Clin Orthod Res May;4(2): Lagravère MO, Heo G, Major PW, Flores-Mir C. Meta-analysis of immediate changes with rapid maxillary expansion treatment. J Am Dent Assoc Jan;137(1): Lagravere MO, Major PW, Flores-Mir C. Long-term dental arch changes after rapid maxillary expansion treatment: a systematic review. Angle Orthod Mar;75(2): Kartalian A, Gohl E, Adamian M, Enciso R. Cone-beam computerized tomography evaluation of the maxillary dentoskeletal complex after rapid palatal expansion. Am J Orthod Dentofacial Orthop Oct;138(4): Handelman CS. Nonsurgical rapid maxillary alveolar expansion in adults: a clinical evaluation. Angle Orthod. 1997;67(4): ; discussion Baysal A, Karadede I, Hekimoglu S, Ucar F, Ozer T, Veli I, et al. Evaluation of root resorption following rapid maxillary expansion using cone-beam computed tomography. Angle Orthod [Internet] Aug 15 [cited 2011 Nov 10];Available from: Garib DG, Henriques JFC, Janson G, de Freitas MR, Fernandes AY. Periodontal effects of rapid maxillary expansion with tooth-tissue-borne and tooth-borne expanders: a computed tomography evaluation. Am J Orthod Dentofacial Orthop Jun;129(6):
34 CHAPTER 3: JOURNAL ARTICLE Abstract Introduction: Transverse maxillary deficiency is a common problem among patients seeking orthodontic care and rapid maxillary expansion (RME) is one of the most frequent methods used by orthodontists to treat this problem. With the advent of orthodontic mini-screw implants, new appliances have been developed that use the palatal bone rather than the teeth as anchorage for the expansion appliance. Purpose: The purpose of this study is to evaluate the skeletal and dental effects of rapid maxillary expansion in the transverse plane using two different expansion appliances: a traditional tooth-supported Hyrax expander versus an implantsupported rapid maxillary expansion appliance. Materials and Methods: A sample of 11 patients who have been treated with an implant-supported RME and 18 patients who have been treated with a Hyrax RME were utilized for this study. CBCT scans were taken before treatment (T1) and immediately following full activation of the expansion appliances (T2). Defined landmarks were located on the pre- and post-treatment orientated images. Changes in pre- and post-treatment measurements were noted and differences between the two treatment groups were evaluated using the Mann-Whitney U test and independent samples t test. Results: RME produced an increase in all the maxillary transverse dimensions at the skeletal, alveolar, and dental levels for both the implant-supported and tooth-borne Hyrax RME groups. Significant differences (p <0.05) in treatment changes were found at two parameters: maxillary base width at the level of the premolar and left premolar angulation. For both treatment groups, there was less expansion at the skeletal level than the dental level. Crown expansion was greatest followed by alveolar expansion and sutural expansion. Conclusions: Both groups showed similar results with greater expansion occurring at the dental level than skeletal level. Implant-supported RME may 24
35 serve as a non-surgical alternative to traditional tooth-borne RME when anchorage to the teeth is undesirable or unavailable. Further studies are needed to evaluate treatment differences between implant-supported expansion appliances and tooth-borne rapid maxillary expanders. 25
36 Introduction Expansion of the maxillary arch through separation of the midpalatal suture has been used as a means of correcting transverse discrepancies for decades. Rapid maxillary expansion (RME) first appeared in the dental literature when Angell introduced it to the dental community in In the early 1900s, rapid maxillary expansion was also promoted for the purpose of increasing nasal permeability, increasing nasal width and straightening the nasal septum. 2,3,4 In addition, numerous studies cite RME as a means of increasing arch perimeter and width to relieve dental crowding and tooth-size arch length discrepancies. 5-6 A long history of palatal expansion as a way to treat crossbites, anteroposterior discrepancies, dental crowding, and airway issues has made it a common treatment modality in most orthodontic practices today and the need for maxillary expansion is common among patients seeking orthodontic care. According to a recent epidemiologic study by da Silva et al., 20.81% of children have some form of posterior crossbite in the primary dentition. 7 Others have estimated that anywhere from 1.0% to 23.5% of children have a posterior crossbite in the primary dentition. 7 Helm estimates the prevalence of unilateral or bilateral crossbites to be present in 9.4% of boys and 14.1% of girls, similar to the NHANES III finding of 9.1% of the U.S. population across all genders, races, and age groups. 8,9 While estimates of the prevalence of posterior crossbites vary, it is clear that orthodontists are faced with the challenge of correcting this malocclusion frequently in practice and understanding the origin of the malocclusion is an important aspect of treatment planning. Posterior crossbites can be dental or skeletal in origin or a combination of both. Likewise, the discrepancy may originate in the maxilla or the mandible or a little of both. Haas makes an 26
37 important point in distinguishing true maxillary deficiency from relative maxillary deficiency. Relative maxillary deficiency occurs when the maxilla is the correct size compared with the upper face, but the mandible is too large resulting in a posterior crossbite. On the other hand, true maxillary deficiency is characterized by a small maxilla and constriction of the buccal tooth segments, indicating a true undersized maxilla. 10,11 Haas popularized RME with the introduction of his expansion appliance in the 1950s. The Haas expander consists of a metal framework with an expansion screw in the palatal vault, bands on the first molars and premolars, an acrylic pad on the palatal tissue and buccal soldered bars as well to maximize anchorage and promote suture opening. 12 An alternative to the Haas expander is hygienic or Hyrax expander developed by Biederman. 13 This appliance was developed in response to the soft issue irritation seen with the Haas appliance. The Hygienic appliance consists of four orthodontic bands placed on the maxillary first molars and premolars with a expansion screw in the middle of the palate and a.040 buccal wire connecting the molar to the premolar bands on the buccal side of the teeth. The main difference between the two appliances is the presence or absence of the acrylic pad. Studies have attempted to evaluate the differences between the two appliances with varying results Rapid maxillary expansion is based on the concept that if a transverse force large enough to overcome the strength of the suture is applied, orthopedic separation of the maxillary segments will occur. 16 The amount of force necessary to separate the midpalatal suture is largely dependent on the age of the patient. It is known that the midpalatal suture does not fuse until somewhere between the ages of years on average and even older in some cases As long as the midpalatal suture has not fused, separation of the suture is expected to occur. While separation of the maxillary halves occurs, rapid maxillary expansion also causes compression of 27
38 the periodontal ligament, bending of the alveolar process, and tipping of the anchor teeth. 19 Because of the forces on the anchor teeth, compression of the periodontal ligament, alveolar bone resorption and tooth movement can occur as well. 20 This can result in root resorption, bony dehiscence and decreases in the thickness of the buccal cortical plate with RME Resistance to separation is due to both the interdigitation of the midpalatal suture with age and other maxillary articulations. 23 Numerous studies have attempted to quantify the exact skeletal and dental effects of rapid maxillary expansion. Skeletally, RME separates the midpalatal suture as the two halves of the palate rotate laterally forming a triangular or wedge-shaped pattern of opening. It is suggested that the two palatal have rotate around a point located near the frontonasal suture with the widest areas of expansion located anteriorly from an occlusal view and apically from a frontal view. 2,4,12,20,24-25 Similarly, rapid maxillary expansion has an effect on much of the maxillo-facial skeleton including the zygomaticomaxillary and zygomaticotemporal sutures. 20,26 Although changes are seen in the entire maxillo-facial skeleton, the greatest effects are seen in the anterior sutures. 27 Proffit notes that the expansion achieved with RME is 50% skeletal and 50% dental. 8 Another study found actual skeletal expansion to vary between 25% to 53% of the total expansion. 9 Garrett et al., found skeletal expansion to account for 55% of the total expansion at the first premolar, 45% at the second premolar, and 38% at the first molar, while dental tipping accounted for 39% of the expansion at the first premolar, 46% at the second premolar and 49% at the first molar. 28 Others have found significant amounts of alveolar tipping, but no statistically significant dental tipping. 29 More recently, expansion appliances have been developed that use mini-screw implants to secure the expansion screw directly to the palate, reducing the forces being placed directly on 28
39 the teeth. This form of RME has been developed in an effort to maximize skeletal expansion and minimize dental tipping while attempting to overcome the disadvantages of the traditional toothsupported RME. Such complications might include root resorption, undesirable tooth movements, relapse, loss of buccal cortical bone at the anchorage teeth and limited skeletal movement. Anchoring the expansion screw directly to the palate also allows for active orthodontics to be started immediately because the crowns of the teeth are not connected to the RME device. 30 Similarly, expansion can be accomplished on patients missing multiple posterior teeth or with periodontal concerns. 31 The idea of avoiding direct forces on the teeth in order to maximize the orthopedic effect is the basis of bone-anchored rapid maxillary expanders, although appliance designs can vary greatly. Successful use of skeletal anchorage devices in the past include the use of palatal distracters, implant-supported Hyrax screws, and bone anchors for maxillary protraction. 32 Some of the first appliances to utilize this concept were variations of palatal distracters designed to expand the palate in adult patients after surgical osteotomy. Only a limited number of studies have been published that test the differences between traditional tooth-borne expansion appliances versus bone-anchored expansion appliances though. Of the studies published, many have used distraction or surgically-assisted rapid maxillary expansion protocols which involve a more invasive surgical procedure for the patient. Cortese et al. found that after expansion with a palatal distractor device, there was minimal buccal tipping of the teeth and that the main movement was of the maxillary segments themselves. 30 Likewise, studies evaluating the effects of surgically assisted expansion using bone-borne implant supported expansion appliances show minimal dental tipping, greater expansion at the level of the alveolar process than the tooth crown, suggesting greater skeletal expansion than dental expansion. 31,33 Harzer et al. found 10 29
40 degrees less molar tipping than tooth-supported expansion in their study looking at the effects of direct fixation of the expansion screw to the palatal bone for RME. 34 Lagravère et al. used conebeam computed tomography to evaluate bone-anchored versus traditional rapid maxillary expansion in adolescents and, contrary to previous studies, found that the skeletal and dental changes for both groups were similar. 35 Little research has been done evaluating implant-supported RME versus tooth-borne RME without the use of surgically assisted expansion or distraction. Among the studies involving distraction or surgically assisted expansion that have been published, varying conclusions have been made regarding the differences between bone-anchored and tooth-borne rapid maxillary expansion. The purpose of this study is to use CBCT to evaluate and compare the skeletal and dental changes in the transverse dimension following rapid maxillary expansion with an implant-supported expansion appliance versus a tooth-born expansion appliance. Additionally, suture opening, alveolar expansion, tooth expansion and tooth angulation changes will be evaluated. Materials and Methods Patient Selection Twenty-nine patients were used for this retrospective study. The records of 11 patients were collected from Saint Louis University to be included in the implant-supported RME group. The records of 18 patients were selected from a private orthodontic practice to be included in the tooth-borne RME group. 30
41 Patients were chosen based on the following inclusion criteria: 1. A treatment plan indicating the use of rapid maxillary expansion to correct a transverse maxillary deficiency or a tooth-arch length discrepancy. 2. Two CBCT scans available including one immediately prior to RME and one immediately following appliance activation before fixed appliances. The implant-supported RME treatment group consisted of 11 patients with a mean chronological age of 17.0 years and a median age years (range, years) at the time of the first CBCT. The implant-supported RME appliances consisted of 2-4 miniscrew implants that secured the expansion screw directly to the palate with no direct anchorage on the teeth. Eight patients had the expansion screw secured to the palate with four 1.6 x 8 mm mini-screws and stainless steel supporting wires extending on the lingual side of the dentition from the expansion screw to the molars then anteriorly to the canines (Figure 3.1). One patient had four 1.6 x 8 mm mini-screw implants securing the expansion screw to the palate with no metal supporting wires extending to the teeth (Figure 3.2). Two patients had the expansion screw secured to the palate with two 1.6 x 8mm mini-screws and stainless steel supporting wires extending from the expansion screw to the lingual of first or second molars and then extended anteriorly to the canines (Figure 3.3). All the appliances were activated at a rate of 1-2 turns/day until adequate expansion was achieved as judged by the orthodontists. The tooth-borne RME treatment group consisted of 18 patients treated with a toothborne (Hyrax) maxillary expander. The 18 patients treated with the tooth-borne (Hyrax) RME were taken from a group of 23 patients with a mean chronological age of 12.3 years (range,
42 17.8 years). The 5 patients excluded from this group were not included in the study because their premolars were not erupted fully. The appliance consisted of a 7 mm expansion screw with stainless steel arms soldered to orthodontics bands on the maxillary first molars and supporting stainless steel wires extending anteriorly on the lingual side of the dentition to the canines (Figure 3.4). The expansion screw was activated with 2 turns at the time of delivery and then activated at a rate of 2 turns per day until overcorrection to the point where the palatal cusps of the maxillary molars were edge-to-edge with the buccal cusps of the mandibular molars. Figure 3.1: Implant-supported RME design with four mini-screw implants and lingual wire extensions 32
43 Figure 3.2: Implant-supported RME design with four mini-screw implants and no lingual wire extensions Figure 3.3: Implant-supported RME design with two mini-screw implants and lingual wire extensions 33
44 Figure 3.4: Tooth-borne Hyrax RME design Imaging Each patient received two CBCT scans using the Classic i-cat (Imaging Sciences International, Inc., Hatfield, PA) cone-beam CT scanner. One scan was taken prior to the start of expansion (T1) and one was taken immediately following what was judged as adequate activation of the appliance (T2). CBCT scans were taken with the patients head stabilized to prevent unwanted movement, teeth in centric occlusion, and Frankfort Horizontal Plane parallel to the floor, as determined by the external auditory meatus and soft-tissue orbitale. All scans were taken with the voxel size set at 0.25 to 0.4 mm and either a 20 second or 26.9 second scan. Each scan was assigned a number to eliminate the possibility of patient identification and was imported to Dolphin Imaging 10.5 software (Dolphin Imaging and Management Solution, Chatsworth, CA). Each scan was oriented along the mid-sagittal plane (z plane), Frankfort Horizontal ( x plane) and the coronal plane (y plane). See Figure 3.5. The image was first 34
45 oriented in the horizontal plane as determined by Frankfort Horizontal (defined as the superiorlateral border of the external auditory meatus on both the right and left sides and left orbitale). Next, the scan was oriented long the mid-sagittal plane (determined by nasion and a point between the nasal bones). Lastly, the scan was oriented in the coronal plane (determined by the most anterior wall of the right and left external auditory meatus). Figure 3.5 Cone-beam computed tomography image orientation Landmark Selection Placement of landmarks was accomplished on the Dolphin Imaging software. After orientation of the CBCT scans, the scans were visualized in all three planes of space in order to obtain two coronal slices that would be used to locate the landmarks used in the evaluation. To obtain standardized coronal slices and thus allow comparison between T1 and T2, the following 35
46 references were used. The molar slice was defined as the first slice moving from anterior to posterior in which the palatal root and the crown of the maxillary first molar were visible. The premolar slice was defined as the first anterior slice in which the crown and buccal root of the first premolar were visible. To aid in standardizing the coronal slices, axial slices of the images were used to identify the root apexes of the molars and premolars in order to better determine the correct location of the coronal slices. Additionally, screen-shots of the coronal slices were taken on the T1 scans and used as reference when creating the coronal slices on the T2 scans. Anatomical features such as nasal cavity curvature, maxillary sinus shape, root shape and root curvature were used to verify standardized coronal slices on the pre- and post-treatment CBCT scans. The landmarks used for evaluation of the transverse maxillary changes are shown in Figures 3.6 and 3.7. Table 3.1 defines each landmark. Once the landmarks were defined on the molar and premolar coronal slices, the parameters listed in Table 3.2 were measured and calculated. The differences between the values at T1 and T2 were then calculated for each measurement so the treatment effects could be determined and any differences between the groups could be evaluated. Comparisons were then made between the two treatment groups at T1, T2 and T2-T1. 36
47 Figure 3.6 Cone-beam computed tomography coronal slice at the molar level with landmarks Figure 3.7 Cone-beam computed tomography coronal slice at the premolar level with landmarks 37
48 Table 3.1 Landmarks for transverse maxillary evaluation 1-2 Right and left inner lower surface of the nasal cavity defined by a tangent to the base of the nose, termed molar baseline. 3-4 Most coronal points of the maxillary alveolar process on the molar slice, right and left, respectively 5-6 Established as points at which the molar baseline intersects the buccal alveolar contour on the right and left sides. 7-8 Buccal cusp tips (mesial-buccal or distal-buccal) of the maxillary first molars, right and left, respectively 9-10 Apices of the palatal roots of the maxillary first molars, right and left, respectively Inner lateral limits of the nose, right and left, respectively. The points are joined by a line parallel to the molar baseline to determine the maximum width of the nasal cavity Medial limits of the palatine process at the molar level, right and left, respectively Right and left inner lower surface of the nasal cavity defined by a tangent to the base of the nose, termed premolar baseline Most coronal points of the maxillary alveolar process on the premolar slice, right and left, respectively Established as points at which the premolar baseline intersects the buccal alveolar contour on the right and left sides Buccal cusp tips of the maxillary first premolars, right and left, respectively Apices of the buccal roots of the maxillary first premolars, right and left, respectively Inner lateral limits of the nose, right and left, respectively. The points are joined by a line parallel to the premolar baseline to determine the maximum width of the nasal cavity Medial limits of the palatine process the premolar level, right and left, respectively 38
49 Table 3.2 Parameters measured for transverse maxillary evaluation Line 1 Distance between landmarks 3-4 Maxillary alveolar width at the level of the first molar Line 2 Distance between landmarks 5-6 Maxillary base width at the level of the first molar Line 3 Distance between landmarks 7-8 Inter-molar crown width Line 4 Distance between landmarks 9-10 Inter-molar apex width Line 5 Distance between landmarks Nasal width at the molar Line 6 Distance between landmarks Suture opening at the level of the molar Line 7 Distance between landmarks Maxillary alveolar width at the level of the first premolar Line 8 Distance between landmarks Maxillary base width at the level of the first premolar Line 9 Distance between landmarks Inter-premolar crown width Line 10 Distance between landmarks Inter-premolar apex width Line 11 Distance between landmarks Nasal width at the level of the premolar Line 12 Distance between landmarks Suture opening at the level of the premolar Angle 1 Line 7-9 to molar baseline Right molar angulation Angle 2 Line 8-10 to molar baseline Left molar angulation Angle 3 Line to premolar baseline Right premolar angulation Angle 4 Line to premolar baseline Left premolar angulation 39
50 Statistics All statistics were calculated using SPSS 18.0 Statistical Software (SPSS, Inc., Chicago, IL). For each parameter, the difference between T1 and T2 was calculated to determine change with expansion treatment. To determine differences between the two treatment groups for each parameter, independent sample Mann-Whitney U tests were calculated because of the small sample size in addition to independent sample t-tests. The level of significance was defined as P < Additionally, each parameter was compared between the two groups at T1 and T2 to determine any differences that existed before treatment and after treatment in addition to comparing the differences in treatment changes. In order to calculate the relative skeletal and dentoalveolar changes, the ratio between sutural opening and intermolar/interpremolar crown width was expressed as a percentage. To calculate intra-examiner reliability, four of the twenty-eight patients were randomly selected and all landmarks and measurements were re-measured to test for reliability with an intraclass correlation coefficient. A Cronbach s Alpha test was executed on repeated measures. A Cronbach s alpha greater than 0.80 is considered an indicator for reliable technique. Results The intraclass correlation coefficient showed all the landmarks to be highly reliable. All of the landmarks had a Cronbach s alpha above 0.975, ranging from to This shows there is no significant difference between the original measurements and the repeated measurements made on all the parameters for four of the 28 patients. 40
51 There was an increase in the transverse plane at the skeletal, alveolar, and dental levels for both the implant-supported and tooth-borne RME groups. A comparison of the two treatment groups at T1 is shown in Table 3.3. The following parameters were significantly different between the groups at T1: Maxillary base width at the level of the premolar, intermolar crown width, nasal width at the molar level, suture opening at the molar level and right molar angulation. A comparison of the two treatment groups at T2 is shown in Table 3.4. The following parameters were significantly different between the groups at T2: Maxillary base width at the level of the premolar, Intermolar crown width, nasal width at the molar level, right molar angulation and left molar angulation. A comparison of the mean values for changes resulting from the RME between the two groups is shown in Table 3.5. Significant differences in treatment changes were found at two parameters: maxillary base width at the level of the premolar and left premolar angulation. For both treatment groups, there was less expansion at the skeletal level than the dental level. In general, expansion at the crown was greater than that measured at the alveolus and suture, indicating the clinical effect is a result of both dental and skeletal expansion. Nasal width changes were fairly consistent anteriorly and posteriorly and between treatment groups. The average nasal width increase at the level of the molar was 1.69 mm (Implant-group) and 1.65 mm (hyrax-group), while at the premolar level both groups had an average increase of 1.65 mm. 41
52 Table 3.3 Comparison of maxillary transverse dimensions at T1 Parameter Implant-supported RME T1 (mean ± SD) Hyrax tooth-borne RME T1 (mean ± SD) P (t-test) Sig. (Mann- WhitneyU) Maxillary alveolar width at the level of the molar (mm) Maxillary base width at the level of the molar (mm) Inter-molar crown width (mm) ± ± ± ± * 0.013* ± ± * 0.051* Intermolar apex width (mm) ± ± * Nasal width at the molar (mm) Suture opening at the level of the molar (mm) Maxillary alveolar width at the level of the premolar (mm) Maxillary base width at the level of the premolar (mm) Inter-premolar crown width (mm) Inter-premolar apex width (mm) Nasal width at the level of the premolar (mm) Suture opening at the level of the premolar (mm) Right molar angulation (degrees) Left molar angulation (degrees) Right premolar angulation (degrees) ± ± * 0.017* 0.29 ± ± * 0.016* ± ± ± ± ± ± ± ± ± ± ± ± ± ± * 0.007* ± ± * 0.000* ± ± Left premolar angulation (degrees) *Indicates statistically significant (<0.05) ± ±
53 Table 3.4 Comparison of maxillary transverse dimensions at T2 Parameter Implant-supported RME T2 (mean ± SD) Hyrax tooth-borne RME T2 (mean ± SD) P (t-test) Sig. (Mann- WhitneyU) Maxillary alveolar width at the level of the molar (mm) Maxillary base width at the level of the molar (mm) Inter-molar crown width (mm) ± ± ± ± * 0.051* ± ± * 0.045* Intermolar apex width (mm) ± ± Nasal width at the molar (mm) Suture opening at the level of the molar (mm) Maxillary alveolar width at the level of the premolar (mm) Maxillary base width at the level of the premolar (mm) Inter-premolar crown width (mm) Inter-premolar apex width (mm) Nasal width at the level of the premolar (mm) Suture opening at the level of the premolar (mm) Right molar angulation (degrees) Left molar angulation (degrees) Right premolar angulation (degrees) ± ± * 0.014* 2.59 ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± * 0.005* ± ± * 0.000* ± ± Left premolar angulation (degrees) * Indicates statistically significant (< 0.05) ± ±
54 Table 3.5 Comparison of the mean changes in the maxillary transverse dimension: T1-T2 Parameter Maxillary alveolar width at the level of the molar (mm) Maxillary base width at the level of the molar (mm) Inter-molar crown width (mm) Implant-supported RME T2-T1 (mean ± SD) Hyrax tooth-borne RME T2-T1 (mean ± SD) P (T-test) Sig.(Mann- WhitneyU) 3.08 ± ± ± ± ± ± Intermolar apex width (mm) 1.90 ± ± Nasal width at the molar (mm) Suture opening at the level of the molar (mm) Maxillary alveolar width at the level of the premolar (mm) Maxillary base width at the level of the premolar (mm) Inter-premolar crown width (mm) Inter-premolar apex width (mm) Nasal width at the level of the premolar (mm) Suture opening at the level of the premolar (mm) Right molar angulation (degrees) Left molar angulation (degrees) Right premolar angulation (degrees) 1.69 ± ± ± ± ± ± ± ± * 0.006* 3.98 ± ± ± ± ± ± ± ± ± ± ± ± ± ± Left premolar angulation (degrees) *Indicates statistically significant (<0.05) 2.11 ± ± * 0.004* 44
55 Actual screw expansion varied between the groups. The implant-supported RME group showed an actual screw expansion of 8.15 mm while the tooth-borne RME group showed a screw expansion of 6.01 mm. The average total expansion at the molar crown was 3.48 mm (Implant-group) and 4.18 (Hyrax-group) while average expansion at the molar apex was 1.90 mm (Implant-group) and 2.62 mm (Hyrax-group). At the premolar crown, expansion was 3.98 mm (Implant-group) and 4.65 mm (Hyrax-group) while expansion at the apex was 2.20 mm (Implant-group) and 1.57 mm (Hyrax-group). The alveolar width at the level of the molar increased by 3.08 mm (Implant-group) and 3.45 mm (Hyrax-group). The alveolar width at the level of the premolar increased by 2.77 mm (Implant-group) and 3.16mm (Hyrax-group). This was greater than expansion of the maxillary base which increased only 0.53 mm (Implant-group) and 1.58 mm (Hyrax group) at the level of the molar and 2.37 mm (Implant-group) and 0.26 mm (Hyrax-group) at the level of the premolar. No significant differences were found between the groups among these measurements. Sutural opening for the implant-supported RME group was on average 2.30 mm at the molar and 1.93 mm at the premolar. For the tooth-borne Hyrax RME group, sutural opening averaged 2.07 mm at the molar and 2.56 mm at the premolar. Expansion was accompanied by molar and premolar tipping. Angulation changes with RME treatment were not identical for the right and left sides. In the implant-supported group, the right molar and left molars tipped 2.55 and 1.36 respectively, while the right and left premolars tipped 3.55 and 2.11 respectively. In the tooth-borne Hyrax group, the right and left molars tipped 2.28 and 0.83 respectively. The right and left premolars tipped 4.43 and 6.09 respectively. The only statistically significant differences between the groups was the left premolar angulation change. 45
56 The relationship between skeletal and dentoalveolar changes can be expressed as a proportion by dividing sutural expansion by the total increase in crown width to get the percentage of total expansion that is due to skeletal expansion. Likewise, actual dental expansion can be calculated by subtracting sutural and alveolar expansion from the expansion at the dental level. These results were converted to percentages and listed in Table 3.6. Table 3.6 Percentages of skeletal, alveolar, and dental expansion for both treatment groups Parameter Sutural expansion Molar: mm (% of total expansion) Premolar: mm (% of total expansion) Alveolar expansion Molar: mm (% of total expansion) Premolar: mm (% of total expansion) Dental expansion Molar: mm (% of total expansion) Premolar: mm (% of total expansion) Total expansion Molar: mm (% of total expansion) Premolar: mm (% of total expansion) Implant-supported RME (mean) 2.30 (66.09%) 1.93 ( 48.49%) 0.78 (22.41%) 0.84 (21.10%) 0.40 (11.49%) 1.21 (30.40%) 3.48 (100%) 3.98 (100%) Hyrax tooth-borne RME (mean) 2.07 (49.52) 2.56 (55.05%) 1.38 (33.01%) 0.60 (12.90%) 0.73 (17.46%) 1.49 (32.04%) 4.18 (100%) 4.65 (100%) Discussion Few studies exist that compare bone-anchored RME to traditional tooth-supported RME without the use of distraction, lateral osteotomy or surgical assistance. Because of this, comparisons between this study and previous studies becomes difficult although some parallelisms can be made. This study adds to the literature in that it evaluates the effects of 46
57 implant-supported versus tooth-borne RME with no surgical intervention. Lagravère et al. conducted a randomized clinical trial looking at non-surgical bone-anchored maxillary expansion versus traditional rapid maxillary expansion using CBCT as well, although their studied differed from the current study in that the placement of the appliance involved a slightly more invasive procedure where reflection of the periosteum for direct bone-to-onplant contact was performed. Results from this study show that there were similar changes in the transverse plane with RME at the skeletal, alveolar, and dental levels for both the implant-supported RME group and the tooth-borne Hyrax RME group. In general, the greatest transverse changes were seen at the dental level when compared to sutural and alveolar width increases, indicating that the expansion was the result of both dentoalveolar and skeletal movements. Crown width increases were greater than alveolar width increases which were greater than sutural width increases for both groups. This implies the total expansion was the result of a combination of sutural, alveolar, and dental expansion. The two groups varied in the amount of actual screw expansion as measured on the CBCT. The implant-supported RME group showed greater actual screw expansion with 8.15 mm of screw activation while the tooth-borne RME group showed a screw expansion of 6.01mm. Interestingly, although the total amount of screw activation for both groups varied, no significant differences were found in sutural, alveolar, or crown expansion between the groups showing that despite the increased screw activation in the implant-supported RME group no significant differences were found at sutural, alveolar or dental levels between the groups. The implant-supported RME group produced greater skeletal expansion at the first molar than the first premolar with 2.30mm and 1.93mm of sutural expansion at the molar and premolar respectively. The skeletal gain in the implant-supported RME group accounted for 66.09% (at the molar level) and 48.49% (at the premolar level) of the total expansion. In the tooth-borne 47
58 RME group, skeletal expansion accounted for % of the expansion at the molar and 55.05% of the expansion at the premolar. This greater skeletal expansion anteriorly is the opposite of what was found in the implant-supported RME group and is in agreement with previous studies on RME. 15,28,33,35 In the tooth-borne Hyrax RME group, skeletal expansion ranged from 49.52% % of the total expansion, while sutural expansion ranged from 48.49% % for the implant-supported RME group. It has been reported that 50% of the total expansion with RME is 8, 36 skeletal while 50% is dental. In a study using CBCT by Kartalian et al., expansion was found to be 40% skeletal. 29 Likewise, in a study by Garrett et al., 55% of the total expansion at the first premolar was found to be skeletal expansion while 38% of the expansion at the molar was skeletal as well. 28 On the other hand, Hansen et al. used CT to evaluate the effects of surgicallyassisted rapid maxillary expansion using a palatal distractor. Their study found 85-91% of the total expansion that was measured at the crowns in the molar and premolar region to be due to skeletal expansion. This number is much greater than the values obtained in this study. The lower percentages of skeletal expansion in this study may be due to the fact that no surgicalassistance or distraction was used in this study as compared with the study by Hansen et al. Alveolar width increases were not significantly different between the two treatment groups. The greater amounts of expansion at the alveolar level than sutural level show that bending of the alveolar processes occurred in both treatment groups. Alveolar expansion accounted for 24.41% of the total molar expansion in the implant-supported RME group and 33.01% of the total molar expansion in the traditional tooth-borne RME group. At the level of the premolar, alveolar expansion accounted for 21.10% and 12.90% of the total expansion in the implant-supported RME and tooth-borne Hyrax RME groups, respectively. 48
59 Increases at the dental level were the greatest transverse changes seen in both groups. In the implant-supported RME group, intermolar crown width increased on average by 3.48 mm while interpremolar crown width increased by 3.98 mm. In the tooth-borne Hyrax group, intermolar and interpremolar crown width increased on average by 4.18 mm and 4.65 mm, respectively. The actual dental expansion can be found by subtracting sutural and alveolar expansion from the total crown expansion to give the actual amount of dental expansion that contributed to the total expansion. In the implant-supported RME groups, this was 0.40 mm and 1.21 mm at the molar and premolar respectively, while the tooth-borne RME group has 0.73 mm and 1.49 mm of dental expansion at the molar and premolar, respectively. This accounted for 11.49% and 30.40% of the total expansion in the implant-supported RME group and 17.46% and 32.04% in the tooth-borne Hyrax RME group. Both groups showed greater dental expansion at the level of the premolar compared to the molar and there were no statistically significant differences between the groups concerning molar or premolar crown expansion. Contrary to this study s results, Tausche et al. found greater expansion at the alveolar bone than the teeth. 33 Similarly, Hansent et al. found greater tipping of the alveolar process than the teeth as well. Both of these studies had fixed appliances in place during the expansion. The authors attribute their results to the direct transfer of expansion forces to the bone on the one hand, and on the other to the torque effect of the rectangular wires within the bracket slot. 31 This could be explained by the fact that the implant-supported RME group had stainless steel supporting wire extensions on the lingual side of the dentition, possibly may preventing the lingual tipping of the teeth as the alveolus expanded. Similarly, molar and premolar crown expansion was greater than expansion at the apex indicating tipping of the teeth in both groups. In the implant-supported RME group, molar crown 49
60 expansion was 3.48 mm while the apex expanded 1.90 mm. Similarly, in the tooth-born Hyrax RME group, crown expansion was 4.18 mm and molar apex expansion was 2.62 mm. The same pattern existed at the premolars. Previous studies confirm this buccal crown tipping with both tooth-borne and skeletally-anchored expansion appliances. 31,33,35 In a systematic review of the effects of bone-borne surgical assisted maxillary expansion, only weak evidence was found for less buccal tipping of the teeth in the bone-borne surgically assisted RME group when compared to tooth-borne surgically assisted RME. 37 This is supported by the results of this study. While no statistically significant differences were found between the groups with regards to the linear measurements of apex and crown expansion, left premolar angulation was found to be statistically different between the two groups with the tooth-borne Hyrax RME group showing greater left premolar angulation changes with treatment than the implant-supported RME group. This was somewhat surprising in that no bands or direct anchorage was placed on the premolars in either group. If anything, one would have expected the molars in the toothborne Hyrax RME group to exhibit greater angulation changes and tipping because of their direct attachment to the expansion screw. Molar angulation changes ranged from 0.83 to Premolar angulation changes were greater and more variable ranging from This greater dental tipping at the premolar than the molar confirms results obtained by others. 31,38 In a study by Hansen et al. evaluating bone-bone surgically assisted expansion, of buccal tipping of the premolars and of buccal tipping of the molars was found with a bone-bone expansion appliance, this was 4-8 less than the tipping at the alveolar process. Similarly, Tausche et al. found 2.5 to 3.9 of dental tipping with surgically-assisted implant bone-borne RME, although this was less than the tipping of the alveolar process. 33 Harzer et al. reports 10 more dental tipping in cases where 50
61 tooth-supported RME is used although this study only had two subjects and differed from this study in that it involved surgical osteotomy with the RME and tipping was measured on dental casts. 34 Cortese et al. found a maximum change of 0.8 in premolar or molar angulation changes with palatal distraction. 30 The fact that distraction or surgically-assisted RME were used in all of these studies may account for the differences in treatment results compared with the implantsupported RME group in this study. As previously pointed out, in 10 of the 11 patients in the implant-supported RME group, lingual wire extensions were present helping to prevent palatal tipping of the teeth with expansion. Maxillary base width at the level of the premolar only increased on average 0.26mm in the Hyrax tooth-borne RME group, showing statistically significant less expansion than the implant-supported RME group. The Hyrax tooth-borne RME group also, showed a statistically significant greater increase in left premolar angulation with treatment, perhaps compensating for the reduced maxillary base width increase at the premolar level. In general, maxillary base width increases were less than sutural expansion, alveolar expansion, and dental expansion. The one exception to this was the maxillary base width increase in the implant-supported RME group was greater than sutural opening at the level of the premolar. Because of the fact that implant-supported RME is a fairly new treatment, the sample size in this study was small and may have been a factor in the lack of statistical significance among the parameters tested. This relatively small sample size is comparable to other published studies involving bone-anchored expansion appliances though ,33-34 As this treatment method becomes more common, further studies using larger samples would be beneficial. 51
62 At T1, the two treatment groups had a number of parameters that were statistically different from each other indicating some group differences at the start of treatment. All of the parameters that were statistically different between the two groups at T1, remained statistically different at T2 except intermolar apex width and suture opening at the level of the molar. This suggests that although the groups had some differences at the start of treatment, the majority of the differences were consistent before and after treatment suggesting equivalent changes with treatment. Suture opening at the level of the molar which was measured to be larger at T1 for the implant-supported but not at T2 suggests a lesser amount of sutural expansion in that group, although the change in suture opening from T2-T1 between groups was not statistically significant. The difference in the average age of the patients between the two groups may have influenced the results as well. One would expect skeletal expansion in younger patients to be more successful as there is less resistance at the suture. Baccetti et al. showed that significantly more favorable skeletal changes are obtained when RME is initiated before the pubertal peak in skeletal growth. Interestingly, the oldest patient in the implant-supported RME group was 34 years of age. This patient was included in the study because despite her age, a diastema was present and separation of the suture on the CBCT was evident. Handelman argues that nonsurgical skeletal expansion in adults is a necessary and safe practice resulting from displacement of the alveolar process. 39 This bending of the alveolar process was evident in both groups, accounting for anywhere from 12.90% to 33.01% of the total expansion. Because of the age differences between the two groups, it would be understandable to expect that alveolar expansion would contribute more to the expansion in the implant-supported RME group where the average age was greater, but this was not the case. Alveolar expansion between the two groups was not 52
63 statistically different, both showing greater expansion at the alveolus than the suture. This indicates some alveolar bending along with the sutural expansion in both groups. Only two mini-screw implant failures (out of 40 total miniscrews) were noted in this study. The two mini-screw implant failures were in separate patients that each had the RME screw secured with four mini-screw implants. Removal of the loosened screws in these two patients did not affect the stability of the expansion appliances as each were still secured by three mini-screw implants in both cases. The idea of using implant-supported expansion appliances for RME to eliminate some of the negative side effects of traditional RME, particularly dental tipping, does not seem to be supported by this study. The two treatment groups produced similar results in most of the parameters measured. Further studies with a larger sample size and matched ages are indicated. Conclusions Based on this study evaluating the immediate treatment effects of rapid maxillary expansion in the transverse plane using an implant-supported RME and a tooth-borne RME appliance, the following conclusions can be made: 1. RME produced increases in all the maxillary transverse dimensions measured with greater increases at the dental than skeletal level for both groups. 2. Both groups showed similar results in most parameters. The two exceptions were as follows: maxillary base width changes at the level of the premolar were greater for the implant- 53
64 supported RME group and left premolar angulation changes were greater for the tooth-borne RME group. Skeletal, alveolar, and dental changes with RME were similar for both groups. 3. Further studies with a larger sample size and matched ages are needed in the future. The implant-supported RME appliance can be used as a non-surgical alternative to the toothborne Hyrax RME appliance in patients missing multiple posterior teeth or when full active orthodontic therapy is to be started immediately. 54
65 References 1. Angell EH. Treatment irregularities of the permanent or adult dentition. Dental Cosmos. 1860;1: Wertz RA. Skeletal and dental changes accompanying rapid midpalatal suture opening. Am J Orthod Jul;58(1): Pfaff W. Stenosis of the nasal cavity caused by contraction of the palatal arch and abnormal position of the teeth: Treatment by expansion of the maxilla. Dental Cosmos. 1905;47: Haas AJ. Rapid expansion of the maxillary dental arch and nasal cavity by opening of the midpalatal suture. Angle Orthod. 1961;31: Adkins MD, Nanda RS, Currier GF. Arch perimeter changes on rapid palatal expansion. Am J Orthod Dentofacial Orthop Mar;97(3): Geran RG, McNamara JA Jr, Baccetti T, Franchi L, Shapiro LM. A prospective long-term study on the effects of rapid maxillary expansion in the early mixed dentition. Am J Orthod Dentofacial Orthop May;129(5): da Silva Filho OG, Santamaria M Jr, Capelozza Filho L. Epidemiology of posterior crossbite in the primary dentition. J Clin Pediatr Dent. 2007;32(1): Proffit WR, Henry W. Fields, Jr. Contemporary Orthodontics. Third Ed. Mosby, Inc Podesser B, Williams S, Crismani AG, Bantleon H-P. Evaluation of the effects of rapid maxillary expansion in growing children using computer tomography scanning: a pilot study. Eur J Orthod Feb;29(1): Haas AJ. Long-term posttreatment evaluation of rapid palatal expansion. Angle Orthod Jul;50(3): Haas AJ. The treatment of maxillary deficiency by opening the midpalatal suture. Angle Orthod Jul;35: Haas AJ. Palatal expansion: just the beginning of dentofacial orthopedics. Am J Orthod Mar;57(3): Biederman W. A hygienic appliance for rapid expansion. JPO J Pract Orthod Feb;2(2): Garib DG, Henriques JFC, Janson G, Freitas MR, Coelho RA. Rapid maxillary expansion-- tooth tissue-borne versus tooth-borne expanders: a computed tomography evaluation of dentoskeletal effects. Angle Orthod Jul;75(4):
66 15. Weissheimer A, de Menezes LM, Mezomo M, Dias DM, de Lima EMS, Rizzatto SMD. Immediate effects of rapid maxillary expansion with Haas-type and hyrax-type expanders: a randomized clinical trial. Am J Orthod Dentofacial Orthop Sep;140(3): Bell RA. A review of maxillary expansion in relation to rate of expansion and patient s age. Am J Orthod Jan;81(1): Björk A, Skieller V. Growth of the maxilla in three dimensions as revealed radiographically by the implant method. Br J Orthod Apr;4(2): Snodell SF, Nanda RS, Currier GF. A longitudinal cephalometric study of transverse and vertical craniofacial growth. Am J Orthod Dentofacial Orthop Nov;104(5): Bishara SE, Staley RN. Maxillary expansion: clinical implications. Am J Orthod Dentofacial Orthop Jan;91(1): Starnbach H, Bayne D, Cleall J, Subtelny JD. Facioskeletal and dental changes resulting from rapid maxillary expansion. Angle Orthod Apr;36(2): Garib DG, Henriques JFC, Janson G, de Freitas MR, Fernandes AY. Periodontal effects of rapid maxillary expansion with tooth-tissue-borne and tooth-borne expanders: a computed tomography evaluation. Am J Orthod Dentofacial Orthop Jun;129(6): Baysal A, Karadede I, Hekimoglu S, Ucar F, Ozer T, Veli I, et al. Evaluation of root resorption following rapid maxillary expansion using cone-beam computed tomography. Angle Orthod [Internet] Aug 15 [cited 2011 Nov 10];Available from: Isaacson RJ, Ingram A. Forces produced by rapid maxillary expansion II. Forces present during treatment. Angle Orthod Oct;34(4): Braun S, Bottrel JA, Lee KG, Lunazzi JJ, Legan HL. The biomechanics of rapid maxillary sutural expansion. Am J Orthod Dentofacial Orthop Sep;118(3): da Silva Filho OG, Montes LA, Torelly LF. Rapid maxillary expansion in the deciduous and mixed dentition evaluated through posteroanterior cephalometric analysis. Am J Orthod Dentofacial Orthop Mar;107(3): Woller J. An Assessment of the Maxilla after Rapid Maxillary Expansion Using Cone Beam Computed Tomography in Growing Children. [A Master's Thesis] St. Louis; Saint Louis University. 2009: Ghoneima A, Abdel-Fattah E, Hartsfield J, El-Bedwehi A, Kamel A, Kula K. Effects of rapid maxillary expansion on the cranial and circummaxillary sutures. Am J Orthod Dentofacial Orthop Oct;140(4):
67 28. Garrett BJ, Caruso JM, Rungcharassaeng K, Farrage JR, Kim JS, Taylor GD. Skeletal effects to the maxilla after rapid maxillary expansion assessed with cone-beam computed tomography. Am J Orthod Dentofacial Orthop Jul;134(1): Kartalian A, Gohl E, Adamian M, Enciso R. Cone-beam computerized tomography evaluation of the maxillary dentoskeletal complex after rapid palatal expansion. Am J Orthod Dentofacial Orthop Oct;138(4): Cortese A, Savastano M, Savastano G, Papa F, Howard CM, Claudio PP. Maxillary constriction treated by a new palatal distractor device: surgical and occlusal evaluations of 10 patients. J Craniofac Surg Mar;21(2): Hansen L, Tausche E, Hietschold V, Hotan T, Lagravère M, Harzer W. Skeletally-anchored rapid maxillary expansion using the Dresden Distractor. J Orofac Orthop Mar;68(2): Wehrbein H, Göllner P. Skeletal anchorage in orthodontics--basics and clinical application. J Orofac Orthop Nov;68(6): Tausche E, Hansen L, Hietschold V, Lagravère MO, Harzer W. Three-dimensional evaluation of surgically assisted implant bone-borne rapid maxillary expansion: a pilot study. Am J Orthod Dentofacial Orthop Apr;131(4 Suppl):S Harzer W, Schneider M, Gedrange T. Rapid maxillary expansion with palatal anchorage of the hyrax expansion screw--pilot study with case presentation. J Orofac Orthop Sep;65(5): Lagravère MO, Carey J, Heo G, Toogood RW, Major PW. Transverse, vertical, and anteroposterior changes from bone-anchored maxillary expansion vs traditional rapid maxillary expansion: a randomized clinical trial. Am J Orthod Dentofacial Orthop Mar;137(3):304.e1 12; discussion Krebs A. Expansion of the midpalatal suture studied by means of metallic implants. European Orthodontic Society Rep. 1958;34: Verstraaten J, Kuijpers-Jagtman AM, Mommaerts MY, Bergé SJ, Nada RM, Schols JGJH. A systematic review of the effects of bone-borne surgical assisted rapid maxillary expansion. J Craniomaxillofac Surg Apr;38(3): Domann CE, Kau CH, English JD, Xia JJ, Souccar NM, Lee RP. Cone beam computed tomography analysis of dentoalveolar changes immediately after maxillary expansion. Orthodontics (Chic.). 2011;12(3): Handelman C. Palatal expansion in adults: The nonsurgical approach. Am J Orthod Dentofacial Orthop Oct;140(4):
68 VITA AUCTORIS Mary Ellen Helmkamp was born on July 11, 1981 in Akron, Ohio. She grew up in Akron, Ohio where she attended St. Vincent- St. Mary High School. In 2000, she moved to Chicago, Illinois to attend DePaul University. In 2004, she graduated from DePaul University s Honor s Program with a B.S. in Biology. After graduating from college she spent a year working as a nanny in Chicago until she started dental school at the Ohio State University in Mary Ellen received her D.D.S. from the Ohio State University in In that same year, she began her residency in orthodontics at Saint Louis University and is planning on receiving her Master of Science in Dentistry (Research) in orthodontics from Saint Louis University in January of Mary Ellen is planning to stay in the St. Louis area after graduation where she will enter into private practice. 58
U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria
 U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria Alcune pubblicazioni della Scuola: Impacted maxillary incisors: diagnosis and predictive measurements. Pavoni C, Mucedero M, Laganà G, Paoloni
U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria Alcune pubblicazioni della Scuola: Impacted maxillary incisors: diagnosis and predictive measurements. Pavoni C, Mucedero M, Laganà G, Paoloni
Headgear Appliances. Dentofacial Orthopedics and Orthodontics. A Common Misconception. What is Headgear? Ideal Orthodontic Treatment Sequence
 Ideal Orthodontic Treatment Sequence Headgear Appliances Natalie A. Capan, D.M.D. 580 Sylvan Avenue, Suite 1M Englewood Cliffs, New Jersey 07632 (201)569-9055 www.capanorthodontics.com [email protected]
Ideal Orthodontic Treatment Sequence Headgear Appliances Natalie A. Capan, D.M.D. 580 Sylvan Avenue, Suite 1M Englewood Cliffs, New Jersey 07632 (201)569-9055 www.capanorthodontics.com [email protected]
Control of mandibular incisors with the combined Herbst and completely customized lingual appliance - a pilot study
 Control of mandibular incisors with the combined Herbst and completely customized lingual appliance - a pilot study Dirk Wiechmann 1 *, Rainer Schwestka-Polly 2 *, Hans Pancherz 3 *, Ariane Hohoff 4 *
Control of mandibular incisors with the combined Herbst and completely customized lingual appliance - a pilot study Dirk Wiechmann 1 *, Rainer Schwestka-Polly 2 *, Hans Pancherz 3 *, Ariane Hohoff 4 *
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery. Consequences of tooth loss.
 Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Classification of Malocclusion
 Classification of Malocclusion What s going on here? How would you describe this? Dr. Robert Gallois REFERENCE: Where Do We Begin? ESSENTIALS FOR ORTHODONTIC PRACTICE By Riolo and Avery Chapter 6 pages
Classification of Malocclusion What s going on here? How would you describe this? Dr. Robert Gallois REFERENCE: Where Do We Begin? ESSENTIALS FOR ORTHODONTIC PRACTICE By Riolo and Avery Chapter 6 pages
Dr. Park's Publications
 Dr. Park's Publications Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D. Diplomate, American Board of Orthodontics Editor-in-Chief, Pacific Coast Society of Orthodontists Chief Editor, Computed Tomography: New
Dr. Park's Publications Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D. Diplomate, American Board of Orthodontics Editor-in-Chief, Pacific Coast Society of Orthodontists Chief Editor, Computed Tomography: New
Removable appliances II. Functional jaw orthopedics
 Removable appliances II. Functional jaw orthopedics Melinda Madléna DMD, PhD Associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification
Removable appliances II. Functional jaw orthopedics Melinda Madléna DMD, PhD Associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification
Rapid Maxillary Expansion Followed by Fixed Appliances: A Long-term Evaluation of Changes in Arch Dimensions
 Original Article Rapid Maxillary Expaion Followed by Fixed Appliances: A Long-term Evaluation of Changes in Arch Dimeio James A. McNamara Jr, DDS, PhD a ; Tiziano Baccetti, DDS, PhD b ; Lorenzo Franchi,
Original Article Rapid Maxillary Expaion Followed by Fixed Appliances: A Long-term Evaluation of Changes in Arch Dimeio James A. McNamara Jr, DDS, PhD a ; Tiziano Baccetti, DDS, PhD b ; Lorenzo Franchi,
Clinical Practice Guideline For Orthodontics
 Clinical Practice Guideline For Orthodontics MOH- Oral Health CSN -Orthodontics -2010 Page 1 of 15 Orthodontic Management Guidelines 1. Definitions: Orthodontics is the branch of dentistry concerned with
Clinical Practice Guideline For Orthodontics MOH- Oral Health CSN -Orthodontics -2010 Page 1 of 15 Orthodontic Management Guidelines 1. Definitions: Orthodontics is the branch of dentistry concerned with
Orthodontic Treatment of an Ankylosed Maxillary Central Incisor through Osteogenic Distraction
 Case Report Orthodontic Treatment of an Ankylosed Maxillary Central Incisor through Osteogenic Distraction Doğan Dolanmaz a ; Ali Ihya Karaman b ; A.Alper Pampu c ; Ahu Topkara d ABSTRACT Tooth ankylosis
Case Report Orthodontic Treatment of an Ankylosed Maxillary Central Incisor through Osteogenic Distraction Doğan Dolanmaz a ; Ali Ihya Karaman b ; A.Alper Pampu c ; Ahu Topkara d ABSTRACT Tooth ankylosis
Expansion Screws. 600-400-10 1 piece 600-400-30 10 pieces. 600-300-30 10 pieces 600-300-60 100 pieces. 600-301-30 10 pieces 600-301-60 100 pieces
 Standard Expansion Screws Expansion Screws 600-400-10 1 piece 600-400-30 10 pieces rematitan -Expansion Screw, Medium Made of pure titanium. Skeleton design For transversal expansion and distalization
Standard Expansion Screws Expansion Screws 600-400-10 1 piece 600-400-30 10 pieces rematitan -Expansion Screw, Medium Made of pure titanium. Skeleton design For transversal expansion and distalization
The American Board of Orthodontics (ABO) Digital Model Requirements Original Release 04.23.2013 Last Update 03.26.2015
 Page 1 of 7 The American Board of Orthodontics (ABO) Digital Model Requirements Original Release 04.23.2013 Last Update 03.26.2015 Introduction In order to provide access to board certification for all
Page 1 of 7 The American Board of Orthodontics (ABO) Digital Model Requirements Original Release 04.23.2013 Last Update 03.26.2015 Introduction In order to provide access to board certification for all
Congenital absence of mandibular second premolars
 CLINICIAN S CORNER Congenitally missing mandibular second premolars: Clinical options Vincent G. Kokich a and Vincent O. Kokich b Seattle, Wash Introduction: Congenital absence of mandibular second premolars
CLINICIAN S CORNER Congenitally missing mandibular second premolars: Clinical options Vincent G. Kokich a and Vincent O. Kokich b Seattle, Wash Introduction: Congenital absence of mandibular second premolars
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
Anchorage onto deciduous teeth: effectiveness of early rapid maxillary expansion in increasing dental arch dimension and improving anterior crowding
 Mutinelli et al. Progress in Orthodontics (2015) 16:22 DOI 10.1186/s40510-015-0093-x RESEARCH Open Access Anchorage onto deciduous teeth: effectiveness of early rapid maxillary expansion in increasing
Mutinelli et al. Progress in Orthodontics (2015) 16:22 DOI 10.1186/s40510-015-0093-x RESEARCH Open Access Anchorage onto deciduous teeth: effectiveness of early rapid maxillary expansion in increasing
SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656
 SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656 ORTHODONTIC CLASSIFICATION / DIAGNOSIS Goal of diagnosis: An orderly reduction of the data base to a useful list of the patient s problems Useful??
SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656 ORTHODONTIC CLASSIFICATION / DIAGNOSIS Goal of diagnosis: An orderly reduction of the data base to a useful list of the patient s problems Useful??
Pitch, roll, and yaw: Describing the spatial orientation of dentofacial traits
 SPECIAL ARTICLE Pitch, roll, and yaw: Describing the spatial orientation of dentofacial traits James L. Ackerman, a William R. Proffit, b David M. Sarver, a Marc B. Ackerman, c and Martin R. Kean d Chapel
SPECIAL ARTICLE Pitch, roll, and yaw: Describing the spatial orientation of dentofacial traits James L. Ackerman, a William R. Proffit, b David M. Sarver, a Marc B. Ackerman, c and Martin R. Kean d Chapel
The etiology of orthodontic problems Fifth session
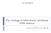 بنام خداوند جان و خرد The etiology of orthodontic problems Fifth session دکتر مھتاب نوری دانشيار گروه ارتدنسی Course Outline( 5 sessions) Specific causes of malocclusion Genetic Influences Environmental
بنام خداوند جان و خرد The etiology of orthodontic problems Fifth session دکتر مھتاب نوری دانشيار گروه ارتدنسی Course Outline( 5 sessions) Specific causes of malocclusion Genetic Influences Environmental
About the Doctor. Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D.
 About the Doctor Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D. Dr. Jae Hyun Park is a highly regarded, Board Certified Orthodontist with a strong commitment to clinical education, patient care and research.
About the Doctor Jae Hyun Park, D.M.D., M.S.D., M.S., Ph.D. Dr. Jae Hyun Park is a highly regarded, Board Certified Orthodontist with a strong commitment to clinical education, patient care and research.
Retrospective analysis of factors influencing the eruption of delayed permanent incisors after supernumerary tooth removal
 Retrospective analysis of factors influencing the eruption of delayed permanent incisors after supernumerary tooth removal R.A.E. BRYAN*, B.O.I. COLE**, R.R. WELBURY* ABSTRACT. Aim This was to assess the
Retrospective analysis of factors influencing the eruption of delayed permanent incisors after supernumerary tooth removal R.A.E. BRYAN*, B.O.I. COLE**, R.R. WELBURY* ABSTRACT. Aim This was to assess the
Universal Screw Removal System (USR)
 Craniomaxillofacial Surgery 3 Universal Screw Removal System (USR) Craniomaxillofacial rigid fixation systems are available from a variety of manufacturers. The USR system is a complete screwdriver array
Craniomaxillofacial Surgery 3 Universal Screw Removal System (USR) Craniomaxillofacial rigid fixation systems are available from a variety of manufacturers. The USR system is a complete screwdriver array
Case Report Case studies on local orthodontic traction by minis-implants before implant rehabilitation
 Int J Clin Exp Med 2015;8(5):8178-8184 www.ijcem.com /ISSN:1940-5901/IJCEM0006299 Case Report Case studies on local orthodontic traction by minis-implants before implant rehabilitation Pei Shen *, Wei-Feng
Int J Clin Exp Med 2015;8(5):8178-8184 www.ijcem.com /ISSN:1940-5901/IJCEM0006299 Case Report Case studies on local orthodontic traction by minis-implants before implant rehabilitation Pei Shen *, Wei-Feng
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
Condylar position in children with functional posterior crossbites: before and after crossbite correction*
 PEDIATRIC DENTISTRY/Copyright 1980 by The American Academy of Pedodontics/Vol. 2, No. 3 Condylar position in children with functional posterior crossbites: before and after crossbite correction* David
PEDIATRIC DENTISTRY/Copyright 1980 by The American Academy of Pedodontics/Vol. 2, No. 3 Condylar position in children with functional posterior crossbites: before and after crossbite correction* David
ABSTRACT INTRODUCTION. Facial Esthetics. Dental Esthetics
 ABSTRACT The FACE philosophy is characterized by clearly defined treatment goals. This increases diagnostic ability and improves the quality and stability of the end result. The objective is to establish
ABSTRACT The FACE philosophy is characterized by clearly defined treatment goals. This increases diagnostic ability and improves the quality and stability of the end result. The objective is to establish
Topics for the Orthodontics Board Exam
 Topics for the Orthodontics Board Exam I. Diagnostics, relations to paediatric dentistry, prevention 1. Etiology of dental anomalies. 2. Orthodontic anomalies, relationship between orthodontic treatment
Topics for the Orthodontics Board Exam I. Diagnostics, relations to paediatric dentistry, prevention 1. Etiology of dental anomalies. 2. Orthodontic anomalies, relationship between orthodontic treatment
Orthodontic treatment of gummy smile by using mini-implants (Part I): Treatment of vertical growth of upper anterior dentoalveolar complex
 O n l i n e O n l y Orthodontic treatment of gummy smile by using mini-implants (Part I): Treatment of vertical growth of upper anterior dentoalveolar complex Tae-Woo Kim*, Benedito Viana Freitas** Abstract
O n l i n e O n l y Orthodontic treatment of gummy smile by using mini-implants (Part I): Treatment of vertical growth of upper anterior dentoalveolar complex Tae-Woo Kim*, Benedito Viana Freitas** Abstract
Semirapid Maxillary Expansion A Study of Long-Term Transverse Effects in Older Adolescents and Adults
 Original Article Semirapid Maxillary ExpansionA Study of Long-Term Transverse Effects in Older Adolescents and Adults Haluk İşeri, DDS, PhD a ; Serhat Özsoy, DDS, PhD b Abstract: A new approach, namely,
Original Article Semirapid Maxillary ExpansionA Study of Long-Term Transverse Effects in Older Adolescents and Adults Haluk İşeri, DDS, PhD a ; Serhat Özsoy, DDS, PhD b Abstract: A new approach, namely,
Orthodontic miniscrews have become increasingly
 2008 JCO, Inc. May not be distributed without permission. www.jco-online.com Miniscrew System with Interchangeable butments ENEDICT WILMES, DDS, MSC DIETER DRESCHER, DDS, PHD Orthodontic miniscrews have
2008 JCO, Inc. May not be distributed without permission. www.jco-online.com Miniscrew System with Interchangeable butments ENEDICT WILMES, DDS, MSC DIETER DRESCHER, DDS, PHD Orthodontic miniscrews have
Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation
 Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Ahmed Abdel Moneim El Sayed Beirut Arab University (961) 1 300110 Ext: 2263 [email protected] [email protected]
 PERSONAL INFORMATION Ahmed Abdel Moneim El Sayed Beirut Arab University (961) 1 300110 Ext: 2263 [email protected] [email protected] Gender Male Date of birth 19/10/1952 Nationality Egyptian
PERSONAL INFORMATION Ahmed Abdel Moneim El Sayed Beirut Arab University (961) 1 300110 Ext: 2263 [email protected] [email protected] Gender Male Date of birth 19/10/1952 Nationality Egyptian
Efficiency of Three Mandibular Anchorage Forms in Herbst Treatment: A Cephalometric Investigation
 Original Article Efficiency of Three Mandibular Anchorage Forms in Herbst Treatment: A Cephalometric Investigation Dominique Weschler, DDS, Dr Med Dent a ; Hans Pancherz, DDS, Odont Dr, FCDSHK (Hon) b
Original Article Efficiency of Three Mandibular Anchorage Forms in Herbst Treatment: A Cephalometric Investigation Dominique Weschler, DDS, Dr Med Dent a ; Hans Pancherz, DDS, Odont Dr, FCDSHK (Hon) b
General Explanation of the Straight Wire Appliance in the Treatment of Young People and Adults Publication for the Journal du Dentiste in Belgium
 General Explanation of the Straight Wire Appliance in the Treatment of Young People and Adults Publication for the Journal du Dentiste in Belgium Today, our dental patients are asking us to provide them,
General Explanation of the Straight Wire Appliance in the Treatment of Young People and Adults Publication for the Journal du Dentiste in Belgium Today, our dental patients are asking us to provide them,
Dr. Little received his doctorate degree in dentistry from UT Health at San Antonio Dental
 Implant Solutions for the Implant Patient: Diagnosis and Treatment Planning for Predictable Results David Little, DDS 6961 U.S. Highway 87 East San Antonio, TX 78263 Phone: (210)648-4411 Fax: (210) 648-6498
Implant Solutions for the Implant Patient: Diagnosis and Treatment Planning for Predictable Results David Little, DDS 6961 U.S. Highway 87 East San Antonio, TX 78263 Phone: (210)648-4411 Fax: (210) 648-6498
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation
 Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
Unless a prosthetic replacement is inserted soon
 2013 JCO, Inc. May not be distributed without permission. www.jco-online.com Preprosthetic Molar Uprighting Using Skeletal nchorage MNUEL NIENKEMPER, DDS, MSC LEXNDER PULS, DDS JÖRN LUDWIG, DMD, MSD ENEDICT
2013 JCO, Inc. May not be distributed without permission. www.jco-online.com Preprosthetic Molar Uprighting Using Skeletal nchorage MNUEL NIENKEMPER, DDS, MSC LEXNDER PULS, DDS JÖRN LUDWIG, DMD, MSD ENEDICT
Maxillary canine palatal impaction occurs in 1
 ORIGINAL ARTICLE Prediction of maxillary canine impaction using sectors and angular measurement John H. Warford Jr, DDS, a,b Ram K. Grandhi, BDS, Dip Perio, Cert Ortho, MS, b and Daniel E. Tira, PhD c
ORIGINAL ARTICLE Prediction of maxillary canine impaction using sectors and angular measurement John H. Warford Jr, DDS, a,b Ram K. Grandhi, BDS, Dip Perio, Cert Ortho, MS, b and Daniel E. Tira, PhD c
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Accuracy of space analysis with emodels and plaster models
 ORIGINAL ARTICLE Accuracy of space analysis with emodels and plaster models S. Russell Mullen, a Chris A. Martin, b Peter Ngan, c and Marcia Gladwin d Leesburg, Va, and Morgantown, WVa Introduction: The
ORIGINAL ARTICLE Accuracy of space analysis with emodels and plaster models S. Russell Mullen, a Chris A. Martin, b Peter Ngan, c and Marcia Gladwin d Leesburg, Va, and Morgantown, WVa Introduction: The
Introduction to Dental Anatomy
 Introduction to Dental Anatomy Vickie P. Overman, RDH, MEd Continuing Education Units: N/A This continuing education course is intended for dental students and dental hygiene students. Maintaining the
Introduction to Dental Anatomy Vickie P. Overman, RDH, MEd Continuing Education Units: N/A This continuing education course is intended for dental students and dental hygiene students. Maintaining the
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
Modern Tooth Replacement Strategies & Digital Workflow
 Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
SURGICAL ORTHODONTICS: LITERATURE REVIEW AND CASE REPORT
 Orthodontics Piyush Heda, Babita Raghuwanshi, Amit Prakash, Kishore Sonawane SURGICAL ORTHODONTICS: LITERATURE REVIEW AND CASE REPORT Piyush HEDA 1, Babita RAGHUWANSHI 2, Amit PRAKASH 3, Kishore SONAWANE
Orthodontics Piyush Heda, Babita Raghuwanshi, Amit Prakash, Kishore Sonawane SURGICAL ORTHODONTICS: LITERATURE REVIEW AND CASE REPORT Piyush HEDA 1, Babita RAGHUWANSHI 2, Amit PRAKASH 3, Kishore SONAWANE
Expansion screws. Standard expansion screws. Expansion screw Mini. Expansion screw Mini
 Standard expansion screws Expansion screw Mini holes in body of screws for better retention in acrylic built-in stops prevent screws from coming apart Indication: for transversal expansion and distalization
Standard expansion screws Expansion screw Mini holes in body of screws for better retention in acrylic built-in stops prevent screws from coming apart Indication: for transversal expansion and distalization
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Three-Dimensional Analysis Using Finite Element Method of Anterior Teeth Inclination and Center of Resistance Location
 Three-Dimensional Analysis Using Finite Element Method of Anterior Teeth Inclination and Center of Resistance Location Allahyar GERAMY 1, Ahmad SODAGAR 1, Mehdi HASSANPOUR 1 Objective: To locate the centre
Three-Dimensional Analysis Using Finite Element Method of Anterior Teeth Inclination and Center of Resistance Location Allahyar GERAMY 1, Ahmad SODAGAR 1, Mehdi HASSANPOUR 1 Objective: To locate the centre
Objectives. Objectives. Objectives. Objectives. Describe Class II div 1
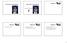 Class II div 1 Malocclusion Class II div 1 Malocclusion Objectives OR What can we do about Goofy? Objectives Describe Class II div 1 Objectives Describe Class II div 1 Describe principles of treatment
Class II div 1 Malocclusion Class II div 1 Malocclusion Objectives OR What can we do about Goofy? Objectives Describe Class II div 1 Objectives Describe Class II div 1 Describe principles of treatment
Orthodontic mini-implants, or temporary anchorage devices
 Anchors, away by John Marshall Grady, DMD, Dan E. Kastner, DMD, and Matthew C. Gornick, DMD Drs. John Marshall Grady (center), Dan E. Kastner (left), and Matthew C. Gornick (right). Drs. John Marshall
Anchors, away by John Marshall Grady, DMD, Dan E. Kastner, DMD, and Matthew C. Gornick, DMD Drs. John Marshall Grady (center), Dan E. Kastner (left), and Matthew C. Gornick (right). Drs. John Marshall
Guideline on Management of the Developing Dentition and Occlusion in Pediatric Dentistry
 Guideline on Management of the Developing Dentition and Occlusion in Pediatric Dentistry Originating Committee Clinical Affairs Committee Developing Dentition Subcommittee Review Council Council on Clinical
Guideline on Management of the Developing Dentition and Occlusion in Pediatric Dentistry Originating Committee Clinical Affairs Committee Developing Dentition Subcommittee Review Council Council on Clinical
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
There When You Need Them: 10 Principles of Successful RPD Treatment
 There When You Need Them: 10 Principles of Successful RPD Treatment Jeff Scott, DMD [email protected] 239 2 nd Ave South Suite 100 St. Petersburg, FL 33701 The West Coast District Dental
There When You Need Them: 10 Principles of Successful RPD Treatment Jeff Scott, DMD [email protected] 239 2 nd Ave South Suite 100 St. Petersburg, FL 33701 The West Coast District Dental
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Skeletal Class lll Severe Openbite Treatment Using Implant Anchorage
 Case Report Skeletal Class lll Severe Openbite Treatment Using Implant Anchorage Yuichi Sakai a ; Shingo Kuroda b ; Sakhr A. Murshid c ; Teruko Takano-Yamamoto d Abstract: A female patient with a skeletal
Case Report Skeletal Class lll Severe Openbite Treatment Using Implant Anchorage Yuichi Sakai a ; Shingo Kuroda b ; Sakhr A. Murshid c ; Teruko Takano-Yamamoto d Abstract: A female patient with a skeletal
BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT
 BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT B K Biswas 1 S Bag 2 & S Pal 3 1. Dept. of Dental Surgery, Associate Professor, KPC Medical College & Hospital, Kolkata,
BIOMECHANICAL ANALYSIS OF NORMAL AND IMPLANTED TOOTH USING BITING FORCE MEASUREMENT B K Biswas 1 S Bag 2 & S Pal 3 1. Dept. of Dental Surgery, Associate Professor, KPC Medical College & Hospital, Kolkata,
Seminar 10 expectations
 Seminar 10 expectations Diagnosis 1. Explain why the transverse dimensions are so important when doing mandibular advancement surgery? How do you determine if maxillary expansion is needed to accept the
Seminar 10 expectations Diagnosis 1. Explain why the transverse dimensions are so important when doing mandibular advancement surgery? How do you determine if maxillary expansion is needed to accept the
Course Curriculum for the Master Degree in Dentistry/Orthodontics
 Jordan University of Science and Technology Faculty of Graduate Studies Course Curriculum for the Master Degree in Dentistry/Orthodontics The Master Degree in Dentistry/ Orthodontics is awarded by the
Jordan University of Science and Technology Faculty of Graduate Studies Course Curriculum for the Master Degree in Dentistry/Orthodontics The Master Degree in Dentistry/ Orthodontics is awarded by the
The distal movement of mandibular molars is
 ORIGINAL ARTICLE Distal movement of mandibular molars in adult patients with the skeletal anchorage system Junji Sugawara, DDS, PhD, a Takayoshi Daimaruya, DDS, PhD, b Mikako Umemori, DDS, PhD, b Hiroshi
ORIGINAL ARTICLE Distal movement of mandibular molars in adult patients with the skeletal anchorage system Junji Sugawara, DDS, PhD, a Takayoshi Daimaruya, DDS, PhD, b Mikako Umemori, DDS, PhD, b Hiroshi
ORTHODONTIC PROBLEMS IN PATIENTS WITH HYPODONTIA AND TAURODONTISM OF PERMANENT MOLARS
 Journal of IMAB - Annual Proceeding (Scientific Papers) 2011, vol. 17, book 2 ORTHODONTIC PROBLEMS IN PATIENTS WITH HYPODONTIA AND TAURODONTISM OF PERMANENT MOLARS Miroslava Yordanova 1, Svetlana Yordanova
Journal of IMAB - Annual Proceeding (Scientific Papers) 2011, vol. 17, book 2 ORTHODONTIC PROBLEMS IN PATIENTS WITH HYPODONTIA AND TAURODONTISM OF PERMANENT MOLARS Miroslava Yordanova 1, Svetlana Yordanova
Growth: Is it a friend or foe to orthodontic treatment?
 orthodontic waves 68 (2009) 1 5 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/odw Review Growth: Is it a friend or foe to orthodontic treatment? Peter Ngan * West Virginia
orthodontic waves 68 (2009) 1 5 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/odw Review Growth: Is it a friend or foe to orthodontic treatment? Peter Ngan * West Virginia
TADs versus traditional devices and tecniques in lower second molar uprighting procedures
 Article ID: WMC004494 ISSN 2046-1690 TADs versus traditional devices and tecniques in lower second molar uprighting procedures Peer review status: No Corresponding Author: Dr. Francesca Muggiano, Dentist,
Article ID: WMC004494 ISSN 2046-1690 TADs versus traditional devices and tecniques in lower second molar uprighting procedures Peer review status: No Corresponding Author: Dr. Francesca Muggiano, Dentist,
GUIDELINES FOR AJODO CASE REPORTS
 GUIDELINES FOR AJODO CASE REPORTS Case reports are published on a regular basis in the AJODO. Not only are these short communications interesting to the clinician in private practice, but they provide
GUIDELINES FOR AJODO CASE REPORTS Case reports are published on a regular basis in the AJODO. Not only are these short communications interesting to the clinician in private practice, but they provide
TRI Product NewsFlash. December 2015
 TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
The European Journal of Orthodontics Advance Access published January 6, 2015
 The European Journal of Orthodontics Advance Access published January 6, 2015 European Journal of Orthodontics, 2015, 1 9 doi:10.1093/ejo/cju094 Original article Comparison of short-term effects of miniimplant-supported
The European Journal of Orthodontics Advance Access published January 6, 2015 European Journal of Orthodontics, 2015, 1 9 doi:10.1093/ejo/cju094 Original article Comparison of short-term effects of miniimplant-supported
Guidelines for Referrals for Orthodontic Treatment
 Advice for General Dental Practitioners, PCTs and LHBs Guidelines for Referrals for Orthodontic Treatment This document has been produced by the British Orthodontic Society Guidelines for Referrals for
Advice for General Dental Practitioners, PCTs and LHBs Guidelines for Referrals for Orthodontic Treatment This document has been produced by the British Orthodontic Society Guidelines for Referrals for
Wired for Learning - Orthodontic Basics
 Wired for Learning - Orthodontic Basics Lori Garland Parker, BS, MAOM, RDAEF, CDA, COA Continuing Education Units: 3 hours Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce365/ce365.aspx
Wired for Learning - Orthodontic Basics Lori Garland Parker, BS, MAOM, RDAEF, CDA, COA Continuing Education Units: 3 hours Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce365/ce365.aspx
!! # # % &! % # () +, . # / (/, 0 1 2 /+340 /)4 5 6 / //78 /+34 /) +))4 //+7)
 !! # # % &! % # () +,. # / (/, 0 1 2 /+340 /)4 5 6 / //78 /+34 /) +))4 //+7) 9 Journal of Orthodontics, Vol. 31, 2004, 3 8 CLINICAL SECTION Orthodontic palatal implants: clinical technique D. Tinsley*,
!! # # % &! % # () +,. # / (/, 0 1 2 /+340 /)4 5 6 / //78 /+34 /) +))4 //+7) 9 Journal of Orthodontics, Vol. 31, 2004, 3 8 CLINICAL SECTION Orthodontic palatal implants: clinical technique D. Tinsley*,
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
Ando A., Nakamura Y., Kanbara R., Kumano H., Miyata T., Masuda T., Ohno Y. and Tanaka Y.
 11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
Use of variable torque brackets to enhance treatment outcomes
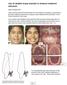 Use of variable torque brackets to enhance treatment outcomes Ralph Nicassio DDS Many clinicians performing Orthodontics for their patients are missing an opportunity to get better results because they
Use of variable torque brackets to enhance treatment outcomes Ralph Nicassio DDS Many clinicians performing Orthodontics for their patients are missing an opportunity to get better results because they
CHAPTER 10 RESTS AND PREPARATIONS. 4. Serve as a reference point for evaluating the fit of the framework to the teeth.
 CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
SCD Case Study. Treatment Considerations for Implant Rehabilitation
 SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
Group Distal Movement of Teeth Using Microscrew Implant Anchorage
 Original Article Group Distal Movement of Teeth Using Microscrew Implant Anchorage Hyo-Sang Park a ; Soo-Kyung Lee b ; Oh-Won Kwon c Abstract: The purpose of this study was to quantify the treatment effects
Original Article Group Distal Movement of Teeth Using Microscrew Implant Anchorage Hyo-Sang Park a ; Soo-Kyung Lee b ; Oh-Won Kwon c Abstract: The purpose of this study was to quantify the treatment effects
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Cross-sectional. Translate Lp3 after. Translate Lp3 after. Tipping Up3 after. ext Up2. ext Lp2. ext Lp2. Bur buc-ling with flap
 Table 2.1 Tooth movement following alveolar decortication injury is represented by 10 evidence-based, refereed, professional journal articles through to May 2013. All investigations include measurements
Table 2.1 Tooth movement following alveolar decortication injury is represented by 10 evidence-based, refereed, professional journal articles through to May 2013. All investigations include measurements
Healing Abutment Selection. Perio Implant Part I. Implant Surface Characteristics. Single Tooth Restorations. Credit and Thanks for Lecture Material
 Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Specific dimensional relationships must exist between
 ORIGINAL ARTICLE Intermaxillary tooth size discrepancy and mesiodistal crown dimensions for a Turkish population Tancan Uysal a and Zafer Sari b Kayseri and Konya, Turkey Introduction: The aims of this
ORIGINAL ARTICLE Intermaxillary tooth size discrepancy and mesiodistal crown dimensions for a Turkish population Tancan Uysal a and Zafer Sari b Kayseri and Konya, Turkey Introduction: The aims of this
The Current Concepts of Orthodontic Discrepancy Stability
 Open Journal of Stomatology, 2014, 4, 184-196 Published Online April 2014 in SciRes. http://www.scirp.org/journal/ojst http://dx.doi.org/10.4236/ojst.2014.44028 The Current Concepts of Orthodontic Discrepancy
Open Journal of Stomatology, 2014, 4, 184-196 Published Online April 2014 in SciRes. http://www.scirp.org/journal/ojst http://dx.doi.org/10.4236/ojst.2014.44028 The Current Concepts of Orthodontic Discrepancy
1 The Single Tooth Implant. The Ultimate Aesthetic Challenge
 1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
Microimplant Anchorage in Orthodontics
 Microimplant Anchorage in Orthodontics *Hee-Moon Kyung, **Bong-Gyu chang,*** Seong-Min Bae *Professor, ** Post-graduate student, *** Clinical Associate Professor Department of Orthodontics Dental School,
Microimplant Anchorage in Orthodontics *Hee-Moon Kyung, **Bong-Gyu chang,*** Seong-Min Bae *Professor, ** Post-graduate student, *** Clinical Associate Professor Department of Orthodontics Dental School,
Treatment planning for the class 0, 1A, 1B dental arches
 Treatment planning for the class 0, 1A, 1B dental arches Dr.. Peter Hermann Dr Reminder: Torquing movement on tooth supported denture : no movement Class 1 movement in one direction (depression) Class
Treatment planning for the class 0, 1A, 1B dental arches Dr.. Peter Hermann Dr Reminder: Torquing movement on tooth supported denture : no movement Class 1 movement in one direction (depression) Class
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning. Orthodontics and Implantology
 ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
Human, Male, White. Bone Clones Osteological Evaluation Report. Product Number: 1 intact mandible. General observations:
 Human, Male, White Product Number: Specimen Evaluated: Skeletal Inventory: BC-107 Bone Clones replica 1 intact cranium 1 intact mandible General observations: In general, the molding process has preserved
Human, Male, White Product Number: Specimen Evaluated: Skeletal Inventory: BC-107 Bone Clones replica 1 intact cranium 1 intact mandible General observations: In general, the molding process has preserved
Anatomic Anomalies. Anomalies. Anomalies. Anomalies. Supernumerary Teeth. Supernumerary Teeth. Steven R. Singer, DDS 212.305.5674 srs2@columbia.
 Anatomic Anomalies Steven R. Singer, DDS 212.305.5674 [email protected] Anomalies! Anomalies are variations in the:! Size! Morphology! Number! Eruption of the teeth Anomalies Anomalies There are two categories:!
Anatomic Anomalies Steven R. Singer, DDS 212.305.5674 [email protected] Anomalies! Anomalies are variations in the:! Size! Morphology! Number! Eruption of the teeth Anomalies Anomalies There are two categories:!
Luigi Vito Stefanelli,D.Eng.,DDS
 LYON, 27-28/09/2013 Luigi Vito Stefanelli,D.Eng.,DDS Assistant Researcher, Department of Oral Sciences, Sapienza University of Rome, Italy, School of Dentistry. Private practitioner dental office Stasi
LYON, 27-28/09/2013 Luigi Vito Stefanelli,D.Eng.,DDS Assistant Researcher, Department of Oral Sciences, Sapienza University of Rome, Italy, School of Dentistry. Private practitioner dental office Stasi
Implants in Orthodontics - A Litterature Rewiev
 Implants in Orthodontics - A Litterature Rewiev Thorir Schiöth University of Berne, Switzerland School of Dental Medicine Department of Orthodontics Implants in Orthodontics Published reports with specific
Implants in Orthodontics - A Litterature Rewiev Thorir Schiöth University of Berne, Switzerland School of Dental Medicine Department of Orthodontics Implants in Orthodontics Published reports with specific
Prosthetic treatment planning on the basis of scientific evidence.
 Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
The Third-Order Angle and the Maxillary Incisor s Inclination to the NA Line
 Original Article The Third-Order Angle and the Maxillary Incisor s Inclination to the NA Line Michael Knösel a ; Dietmar Kubein-Meesenburg b ; Reza Sadat-Khonsari c ABSTRACT Objective: To evaluate the
Original Article The Third-Order Angle and the Maxillary Incisor s Inclination to the NA Line Michael Knösel a ; Dietmar Kubein-Meesenburg b ; Reza Sadat-Khonsari c ABSTRACT Objective: To evaluate the

