Complications associated with laparoscopic sleeve gastrectomy for morbid obesity: a surgeon s guide
|
|
|
- Agatha Arnold
- 10 years ago
- Views:
Transcription
1 REVIEW REVUE Complications associated with laparoscopic sleeve gastrectomy for morbid obesity: a surgeon s guide Kourosh Sarkhosh, MD, MSc * Daniel W. Birch, MD, MSc * Arya Sharma, MD, PhD, DSc Shahzeer Karmali, BSc, MD * From the *Centre for the Advancement of Minimally Invasive Surgery (CAMIS), Royal Alexandra Hospital, and the Departments of Surgery and Medicine, University of Alberta, Edmonton, Alta. Accepted for publication Oct. 24, 2012 Correspondence to: S. Karmali CAMIS, Royal Alexandra Hospital Kingsway Edmonton AB T5H 3V9 [email protected] DOI: /cjs Obesity is a common disease affecting adults and children. The incidence of obesity in Canada is increasing. Laparoscopic sleeve gastrectomy (LSG) is a relatively new and effective procedure for weight loss. Owing to an increase in the number of bariatric surgical procedures, general surgeons should have an understanding of the complications associated with LSG and an approach for dealing with them. Early postoperative complications following LSG that need to be identified urgently include bleeding, staple line leak and development of an abscess. Delayed complications include strictures, nutritional deficiencies and gastresophageal reflux disease. We discuss the principles involved in the management of each complication. L obésité est une maladie fort répandue, tant chez les adultes que chez les enfants, et son incidence est en hausse au Canada. La gastrectomie longitudinale laparoscopique (GLL) est une intervention relativement nouvelle et efficace pour la perte de poids. Compte tenu de l augmentation du nombre d interventions chirurgicales bariatriques, les chirurgiens généralistes doivent se familiariser avec les complications associées à la GLL et avec leur prise en charge. Les complications postopératoires immédiates de la GLL qu il faut savoir reconnaître sans retard sont l hémorragie, les fuites le long de la ligne d agrafes et la formation d abcès. Parmi les complications plus tardives, mentionnons les sténoses, les carences alimentaires et le reflux gastro-œsophagien. Nous présentons les principes qui sous-tendent la prise en charge de chaque complication. Obesity is a common disease affecting more than 300 million adults worldwide. 1 It is defined as a body mass index greater than 30. In Canada, the prevalence of obesity has increased almost 3-fold in the past 2 decades. 2 Approximately 25% of the Canadian population is now classified as obese. 3 Current options for bariatric surgery are categorized by several principles. Purely restrictive procedures include laparoscopic adjustable gastric banding and sleeve gastrectomy. Roux-en-Y gastric bypass is a restrictive surgery with a minor malabsorption approach. Largely malabsorptive procedures with a restrictive component include duodenal switch and biliopancreatic diversion. Almost purely malabsorptive procedures include jejuno-ileal bypass. Laparoscopic sleeve gastrectomy (LSG), also known as longitudinal or vertical gastrectomy, is a relatively new and effective surgical option for the management of morbid obesity (Fig. 1). It was initially introduced in 1990 as an alternative to distal gastrectomy with the duodenal switch procedure to reduce the rate of complications. 4,5 Sleeve gastrectomy was first performed laparoscopically by Ren and colleagues in At the time, LSG was considered a first-stage operation in high-risk patients before biliopancreatic diversion or Roux-en-Y gastric bypass. 7 Laparoscopic sleeve gastrectomy was subsequently found to be effective as a single procedure for the treatment of morbid obes - ity. 8 Although LSG functions as a restrictive procedure, it may also cause early satiety by removing the ghrelin-producing portion of the stomach. 9 The incidence of obesity in Canada is on the rise, and more patients are undergoing bariatric surgical procedures. 10 This growth is compounded with the escalating incidence of medical tourism wherein patients are travelling abroad for surgical care, particularly bariatric surgery. 11 This inevitably translates to an 2013 Canadian Medical Association Can J Surg, Vol. 56, No. 5, October
2 REVUE increased incidence of complications associated with such procedures. It is therefore essential for all general surgeons, including those practising in smaller communities, to be aware of these potential complications and to have a basic understanding of how to manage them and when to ask for guidance from a bariatric surgeon. The purpose of this article is to shed some light on basic principles in the management of complications after LSG. We present our operative approach to LSG and review the major acute (within 2 wk of surgery) and late complications that can arise in patients following LSG (Table 1). OPERATIVE TECHNIQUE The patient is placed in a supine position with the arms spread apart. Pneumoperitoneum is achieved using a closed technique with a Veress needle placed in the left subcostal area of the abdomen. Two 10 mm ports are placed in the supraumbilical and left midabdominal areas. An additional 15 mm port is placed in the right mid - abdomen to pass the stapler. Finally, 2 additional 5 mm ports are placed in the left and right upper quadrants of the abdomen. The left lobe of the liver is retracted medially using a Nathanson retractor placed in the subxiphoid area. The stomach is decompressed at the beginning of the operation by placing an orogastric tube. The surgeon stands to the patient s right with the first assistant standing to the patient s left. The angle of His is taken down bluntly using the Goldfinger dissector (Ethicon Endo-Surgery), exposing the left crus of the diaphragm. Dissection is started about 6 cm proximal to the pylorus by taking down the gastrocolic ligament using the Harmonic Scalpel (Ethicon Endo- Surgery). Dissection is carried out proximally toward the short gastric vessels. This releases attachments to the greater curvature of the stomach and gastric fundus. The orogastric tube is then removed and replaced by a 50-French bougie placed in the stomach by the anesthesiologist and guided laparoscopically to sit in the lesser curvature of the stomach just distal to the pylorus. A 60 mm Endo GIA tri-stapler is then used to divide the stomach. We use 2 black cartridges initially to divide the distal stomach, starting 6 cm proximal to the pylorus. Next, mm purple cartridges are used to complete the division of the remainder of the stomach. The specimen is then taken out of the abdominal cavity through the 15 mm port. The bougie is then removed, and intraoperative gastroscopy is performed with air insufflation and methylene blue to rule out any leaks. We routinely close our 15 mm port fascia under direct vision before exsufflation of the abdomen. Patients receive nothing by mouth after surgery. On postoperative day 1, an upper gastrointestinal study is done using gastrografin to rule out staple line leakage (Fig. 2). A clear fluids diet is subsequently initiated. ACUTE COMPLICATIONS Hemorrhage Fig. 1. Sleeve gastrectomy. The risk of postoperative bleeding has been reported to be between 1% and 6% after LSG. 4,12 The source of bleeding can be intra- or extraluminal. Intraluminal bleeding from the staple line usually presents with an upper gastrointes - tinal bleed. Common symptoms include hematemesis or melena stools. Diagnosis and management of intraluminal bleeding follows the common algorithm taken for an Table 1. Complications associated with laparoscopic sleeve gastrectomy Complication Chronicity Diagnosis Management Hemorrhage Acute Physical findings, serial CBC Transfusion with or without laparoscopy/laparotomy Leak Acute/chronic Physical findings, UGI series Drainage (infrared laparoscopy), antibiotics with or without stenting and/or repair Abscess Chronic CT scan, ultrasound Drainage, antibiotics Stricture Chronic Endoscopy, UGI series Endoscopy (dilatation), surgery (seroyotomy) Nutrient deficiency Chronic Physical findings, blood work Nutritional supplements GERD Chronic History, endoscopy Treatment with proton pump inhibitor CBC = complete blood count; CT = computed tomography; GERD = gastroesophageal reflux disease; UGI = upper gastrointestinal. 348 J can chir, Vol. 56, N o 5, octobre 2013
3 REVIEW upper gastrointestinal bleed. This includes establishment of large bore intravenous lines for fluid resuscitation, administration of packed red blood cells if necessary, accurate measurement of urine output with insertion of a Foley catheter and an urgent gastroscopy to diagnose and control the source of bleeding. Extraluminal bleeding usually presents with a serial drop in serum hemoglobin levels or signs of tachycardia or hypotension. Common sources for extraluminal bleeding include the gastric staple line, spleen, liver or abdominal wall at the sites of trocar entry. We suggest a second-look laparoscopy in any patient who presents with extraluminal bleeding with a sustained heart rate greater than 120 beats per minute and a drop in hemoglobin of more than 10 g/l postoperatively. Urgent laparoscopy facilitates a diagnosis and allows evacuation of the clot as well as surgical control of the source of bleeding. Many times the actual source cannot be identified, but we believe that evacuation of the hematoma and placement of a closed suction drain often serves as a helpful adjunct to patient resuscitation. A number of buttressing materials are commercially available to attempt to reduce the rate of bleeding from the staple line. These include glycolide trimethylene carbonate copolymer (Gore Seamguard; W.L. Gore and Associates), bovine pericardium strips (Synovis Surgical Innovations) or porcine small intestinal submucosa (Surgisis Biodesign, Cook Medical). Whether the use of buttressing material reduces the rate of bleeding remains controversial. In a recent prospective randomized trial, Dapri and colleagues 13 compared the rate of staple line bleeding after LSG using 3 different techniques: stapling the stomach with no re - inforcement, or reinforcement with either suturing or buttressing with Gore Seamguard. These investigators observed a significantly lower rate of bleeding with the use of buttressing material. There was no difference in the incidence of a leak. Albanopoulos and colleagues, 14 however, did not observe a significant difference in their rate of postoperative bleeding between patients with staple line suturing or buttressing with Gore Seamgard after LSG. These investigators had a 6% and 0% complication rate (bleeding and leak) in their suturing and Seamgard arms, respectively, but this did not reach significance. Therefore at our institution we do not routinely use any reinforcement materials (sutures or buttresses) for LSG. Staple line leak Gastric leak is one of the most serious and dreaded complications of LSG (Fig. 3). It occurs in up to 5% of patients following LSG. 8,12 Several classifications exist Large leak Gastric sleeve Gastric sleeve Fig. 2. Radiograph showing a normal image of the stomach after laparoscopic sleeve gastrectomy. Fig. 3. Radiograph showing a leak following laparoscopic sleeve gastrectomy. Can J Surg, Vol. 56, No. 5, October
4 REVUE based on the radiologic findings and time of diagnosis. 15 Based on upper gastrointestinal contrast study, gastric leak can be classified into 2 types. A type I or subclinical leak is controlled either through a surgical drain or through a fistulous tract into the abdominal or chest cavity. A type II or clinical leak is a disseminated leak with diffusion of the contrast into the abdominal or chest cavities. 16 Based on the time of diagnosis, gastric leaks are classified as early or late. An early leak is generally diagnosed within the first 3 days after surgery, whereas a delayed leak is usually diagnosed more than 8 days after surgery. 17 Gastric leaks can be diagnosed either incidentally on a routine upper gastrointestinal series performed postoperatively without any clinical signs or during exploratory laparoscopy/laparotomy performed owing to unexplained tachycardia. In a study by Kolakowski and colleagues, 18 a combination of clinical signs of fever, tachycardia and tachypnea was found to be 58.33% sensitive and 99.75% specific for detection of anastomotic leaks. Diabetes mellitus and sleep apnea were associated with a greater incidence of anastomotic leak. Therefore, we suggest an exploratory laparoscopy for diagnosis in patients who show these signs in the early postoperative period. In the presence of a leak, an abdominal washout with surgical repair of the leak (if technically feasible) and establishment of an enteral feeding route should be performed. Because the stomach is limited in size, the preferred choice for enteral feeding is typically a feeding jejunostomy. In contrast, treatment of a delayed gastric leak is more challenging surgically owing to the presence of an inflammatory reaction. In this setting, attempts to repair the leak are usually futile. Treatment options include conservative or surgical management. This depends on the patient s hemodynamic condition and on physical and radiologic findings. In the absence of hemodynamic instability and physical findings suggestive of peritonitis, conservative management may be initiated. This entails fluid resuscitation, initiation of intravenous antibiotics, nothing by mouth, percutaneous drainage of intra-abdominal collections (if drainable) and intraluminal stenting. 19 In a septic patient with radiological evidence of a leak with diffuse intra-abdominal fluid collections, surgical drainage of the fluid collection is warranted. At our institution, we have successfully managed delay - ed gastric leaks with drainage (either surgical or percutaneous), establishment of a feeding route (enteral or parenteral) and placement of gastric stents for approximately 2 4 weeks (Fig. 4). Other investigators have also used intraluminal stents for the management of gastric leaks. 20,21 Himpens and colleagues 20 reported their experience in the management of 29 patients with gastric leak after sleeve gastrectomy with stenting. These investigators left the stents in situ on average for 7 weeks. Immediate success was observed in 19 patients after placement of the first stent, whereas 5 patients required placement of a second stent. Two patients had persistent leaks requiring a surgical intervention. Abscess Intra-abdominal abscess is another possible complication after LSG. It usually presents with symptoms of abdom - inal pain, fever/chills or nausea and vomiting. If there are clinical suspicions, one should obtain a computed tomography scan of the abdomen to rule out the presence of intra-abdominal abscess. In a series of 164 patients undergoing LSG, Lalor and colleagues 22 reported 1 patient with an abscess (0.7%). Treatment includes percutaneous drain - age and antibiotics. CHRONIC COMPLICATIONS Stricture Intraluminal stent Fig. 4. Radiograph showing an intraluminal stent for the treatment of a leak following laparoscopic sleeve gastrectomy. Formation of stricture is another potential complication occurring after LSG. It could present either acutely after surgery due to tissue edema or more commonly in a delayed fashion. Presenting symptoms include food intolerance, dysphagia or nausea and vomiting. Although kinking of the stomach following LSG has been reported, 23 the most common site of stenosis is at the incisura angularis. 24 An upper gastrointestinal study or endoscopy is usually diagnostic. Treatment options depend on the time of presentation. A stricture diagnosed acutely after surgery can sometimes be treated conservatively with bowel rest (nothing by 350 J can chir, Vol. 56, N o 5, octobre 2013
5 REVIEW mouth), rehydration with intravenous fluids and close observation. In the absence of other pathologies (e.g., abscess, leak), these strictures will spontaneously resolve with no need for further intervention. Failure of conservative management warrants endoscopic dilation. In contrast, chronic strictures usually require further intervention. These include either endoscopic or surgical treatments. Treatment options depend on the length of stenosis. Endoscopic dilatation is an invaluable tool used in this setting of a short segment stenosis. 25 Successive treatments in 4- to 6-week intervals are adequate to treat stricture and ameliorate patient symptoms. In contrast, long segment stenosis and failure of endoscopic management demands a surgical intervention. Options include laparoscopic or open seromyotomy or conversion to Roux-en-Y gastric bypass. Dapri and colleagues 26 reported their experience with laparoscopic seromyotomy in patients who had LSG. These investigators reported successful results with this treatment. Parikh and colleagues 25 reported an incidence of 3.5% of symptomatic stenosis following LSG in their series of 230 patients; 2 patients required conversion to a Roux-en-Y gastric bypass owing to failure of endoscopic management. Nutritional deficiencies Nutritional deficiencies are common after bariatric surgery. The etiology is multifactorial owing to impaired absorption and decreased oral intake. In a recent study by Gehrer and colleagues, 27 the prevalence of vitamin B12, vitamin D, folate, iron and zinc deficiency were reported to be 3%, 23%, 3%, 3% and 14%, respectively, after LSG. In general, these investigators found micronutrient deficiencies to be less prevalent after LSG than Roux-en-Y gastric bypass; however, folate deficiency was slightly more common after LSG than Roux-en-Y gastric bypass (22% v. 12%). 27 Routine blood work is therefore warranted after LSG to diagnose vitamin and mineral deficiencies. At our institution, we routinely monitor patients serum vitamin B12, vitamin D, folate, iron and calcium levels at 3, 6 and 12 months after surgery and treat them accordingly, if necessary. Gastroesophageal reflux disease Gastroesophageal reflux disease (GERD) is a condition seen commonly in the bariatric surgery population. Although some operations, such as Roux-en-Y gastric bypass, are known to be associated with a reduced incidence of reflux postoperatively, this is controversial for LSG. In a recent systematic review by Chiu and colleagues, 28 the authors found the data to be inconclusive with respect to the effect of LSG on GERD. Of the included studies, 4 showed an increased incidence of GERD postoperatively, whereas 7 showed a decrease in the incidence of GERD. Carter and colleagues 29 performed a retrospective study on patients who underwent LSG and found 47% of their patients to have persistent (> 30 d) GERD symptoms. The most common reported symptoms included heartburn (46%) and regurgitation (29%). Management of patients with persistent GERD involves treatment with proton pump inhibitors. These patients require close clinical follow-up. If their symptoms persist despite the use of proton pump inhibitors, we usually perform a gastroscopy for diagnosis. CONCLUSION Laparoscopic sleeve gastrectomy is a new and effective procedure for the surgical management of morbid obesity. Therefore, the number of patients undergoing this procedure will continue to rise. Basic understanding of common complications and available treatment options is essential for all practising general surgeons. This paper offers basic management guidelines for the treatment of complications after LSG. By early diagnosis and treatment of these complications, patient morbidity and mortality might be reduced. Competing interests: None declared for K. Sarkhosh and A. Sharma. D.W. Birch declares having received consultant and speaker fees from Johnson & Johnson, Ethicon Endo-Surgery, Covidien, Olympus, Bard and Baxter. S. Karmali declares having received speaker fees from Ethicon and Covidien. Contributors: All authors designed the study. K. Sarkhosh acquired the data, which K. Sarkhosh and A. Sharma analyzed. K. Sarkhosh and S. Karmali wrote the article, which all authors reviewed and approved for publication. References 1. Deitel M. Overweight and obesity worldwide now estimated to involve 1.7 billion people. Obes Surg 2003;13: Katzmarzyk PT, Mason C. Prevelance of class I, II and III obesity in Canada. CMAJ 2006;174: Shields M, Carroll MD, Ogden CL. Adult obesity prevalence in Canada and the United States. NCHS Data Brief 2011;56: Frezza EE. Laparoscopic vertical sleeve gastrectomy for morbid obes ity. The future procedure of choice? Surg Today 2007;37: Marceau P, Hould FS, Simard S, et al. Biliopancreatic diversion with duodenal switch. World J Surg 1998;22: Ren CJ, Patterson E, Gagner M. Early results of laparoscopic bilio - pancreatic diversion with duodenal switch: a case series of 40 con - secutive patients. Obes Surg 2000;10: Regan JP, Inabnet WB, Gagner M, et al. Early experience with twostage laparoscopic Roux-en-Y gastric bypass as an alternative in the super-super obese patient. Obes Surg 2003;13: Moon Han S, Kim WW, Oh JH. Results of laparoscopic sleeve gastrectomy (LSG) at 1 year in morbidly obese Korean patients. Obes Surg 2005;15: Gumbs AA, Gagner M, Dakin D, et al. Sleeve gastrectomy for morbid obesity. Obes Surg 2007;17: Can J Surg, Vol. 56, No. 5, October
6 REVUE 10. Padwal RS, Lewanczuk RZ. Trends in bariatric surgery in Canada CMAJ 2005;172: Birch DW, Vu L, Karmali S, et al. Medical tourism in bariatric surgery. Am J Surg 2010;199: Melissas J, Koukouraki S, Askoxylakis J, et al. Sleeve gastrectomy: A restrictive procedure? Obes Surg 2007;17: Dapri G, Cadiere GB, Himpens J. Reinforcing the staple line during laparoscopic sleeve gastrectomy: prospective randomized clinical study comparing three different techniques. Obes Surg 2010;20: Albanopoulos K, Alevizos L, Flessas J, et al. Reinforcing the staple line during laparoscopic sleeve gastrectomy: prospective randomized clinical study comparing two different techniques. Preliminary results. Obes Surg 2012;22: Burgos AM, Braghetto I, Csendes A, et al. Gastric leak after laparoscopic sleeve gastrectomy for obesity. Obes Surg 2009;19: Csendes A, Diaz JC, Burdiles P, et al. Classification and treatment of anastomotic leakage after extended total gastrectomy in gastric carcin oma. Hepatogastroenterology 1990;37: Csendes A, Burdiles P, Burgos AM, et al. Conservative management of anastomotic leaks after 557 open gastric bypasses. Obes Surg 2005; 15: Kolakowski S, Kirkland ML, Scuricht AL. Routine postoperative upper gastrointestinal series after Roux-en-Y gastric bypass. Arch Surg 2007;142: Márquez MF, Ayza MF, Lozano RB, et al. Gastric leak after laparoscopic sleeve gastrectomy. Obes Surg 2010;20: Himpens J, Dapri G, Cadiere GB. Treatment of leaks after sleeve gastrectomy. Bariatric Times September Available: http ://bariatrictimes.com/treatment -of-leaks -after-sleeve -gastrectomy/ (ac- cessed 2012 Oct. 29). 21. Oshiro T, Kasama K, Umezawa A, et al. Successful management of refractory staple line leakage at the esophagogastric junction after a sleeve gastrectomy using the HANAROSTENT. Obes Surg 2010; 20: Lalor PF, Tucker ON, Szomstein S, et al. Complications after laparoscopic sleeve gastrectomy. Surg Obes Relat Dis 2008;4: Uglioni B, Wolnerhanssen B, Peters T, et al. Midterm results of primary versus secondary laparoscopic sleeve gastrectomy (LSG) as an isolated operation. Obes Surg 2009;19: Cottam D, Qureshi F, Mattar S, et al. Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid obesity. Surg Endosc 2006;20: Parikh A, Alley JB, Peterson RM, et al. Management options for symptomatic stenosis after laparoscopic vertical sleeve gastrectomy in the morbidly obese. Surg Endosc 2012;26: Dapri G, Cadiere GB, Himpens J. Laparoscopic seromyotomy for long stenosis after sleeve gastrectomy with or without duodenal switch. Obes Surg 2009;19: Chiu S, Birch DW, Shi X, et al. Effect of sleeve gastrectomy on gastro - esophageal reflux disease: a systematic review. Surg Obes Relat Dis 2011;7: Gehrer S, Kern B, Peters T, et al. Fewer nutrient deficiencies after laparoscopic sleeve gastrectomy (LSG) than after laparoscopic Rouxen-Y-gastric bypass (LRYGB) a prospective study. Obes Surg 2010;20: Carter PR, LeBlanc KA, Hausmann MG, et al. Association between gastroesophageal reflux disease and laparoscopic sleeve gastrectomy. Surg Obes Relat Dis 2011;7: CJS s top viewed articles* 1. Research questions, hypotheses and objectives Farrugia et al. Can J Surg 2010;53(4): Tracheostomy: from insertion to decannulation Engels et al. Can J Surg 2009;52(5): Adhesive small bowel obstruction: epidemiology, biology and prevention Attard and MacLean Can J Surg 2007;50(4): Parmacological management of postoperative ileus Zeinali et al. Can J Surg 2009;52(2): All superior pubic ramus fractures are not created equal Steinitz et al. Can J Surg 2004;47(6): Hardware removal after tibial fracture has healed Sidky and Buckley Can J Surg 2008;51(4): Bizarre parosteal osteochondromatous proliferation (Nora lesion): a resport of 3 cases and a review of the literature Gruber et al. Can J Surg 2008;51(6): Soft-tissue nail-fold excision: a definitive treatment for ingrown toenails Chapeskie and Kovac Can J Surg 2010;53(4): Topical nifedipine with lidocaine ointment versus active control for pain after hemmorhoidectomy: results of a multicentre, prospective, randomized, double-blind study Perrotti et al. Can J Surg 2010;53(1): Complications associated with adjustable gastric banding for morbid obesity: a surgeon s guide Eid et al. Can J Surg 2011;54(1):61-6 * Based on page views on PubMed Central of research, reviews, commentaries and continuing medical education articles. Updated Sept. 12, J can chir, Vol. 56, N o 5, octobre 2013
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy
 CASE REPORT Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy Ramon Vilallonga, MD, PhD, Jacques Himpens, MD Division of Bariatric Surgery, AZ St. Blasius, Dendermonde, Belgium
CASE REPORT Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy Ramon Vilallonga, MD, PhD, Jacques Himpens, MD Division of Bariatric Surgery, AZ St. Blasius, Dendermonde, Belgium
Gastric Leak After Laparoscopic-Sleeve Gastrectomy for Obesity
 DOI 10.1007/s11695-009-9884-9 RESEARCH ARTICLE Gastric Leak After Laparoscopic-Sleeve Gastrectomy for Obesity Ana Maria Burgos & Italo Braghetto & Attila Csendes & Fernando Maluenda & Owen Korn & Julio
DOI 10.1007/s11695-009-9884-9 RESEARCH ARTICLE Gastric Leak After Laparoscopic-Sleeve Gastrectomy for Obesity Ana Maria Burgos & Italo Braghetto & Attila Csendes & Fernando Maluenda & Owen Korn & Julio
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Gastric Stenosis After Laparoscopic Sleeve Gastrectomy in Morbidly Obese Patients
 OBES SURG (2013) 23:1481 1486 DOI 10.1007/s11695-013-0963-6 REVIEW Gastric Stenosis After Laparoscopic Sleeve Gastrectomy in Morbidly Obese Patients Ana María Burgos & Attila Csendes & Italo Braghetto
OBES SURG (2013) 23:1481 1486 DOI 10.1007/s11695-013-0963-6 REVIEW Gastric Stenosis After Laparoscopic Sleeve Gastrectomy in Morbidly Obese Patients Ana María Burgos & Attila Csendes & Italo Braghetto
Laparoscopic Sleeve gastrectomy
 Restrictive procedure Laparoscopic Sleeve gastrectomy Dr. R. Peterli Professional Education 1 2 Introduction Gastric sleeve resection is the restrictive part of the biliopancreatic diversion duodenal switch,
Restrictive procedure Laparoscopic Sleeve gastrectomy Dr. R. Peterli Professional Education 1 2 Introduction Gastric sleeve resection is the restrictive part of the biliopancreatic diversion duodenal switch,
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Dept. of Medical Imaging University of Ottawa
 ED Visits Related to Bariatric Surgery: Review of Normal Post-Surgical Anatomy as Well as Complications Dept. of Medical Imaging University of Ottawa Disclosures Background Roux-en-Y Gastric Bypass Surgery
ED Visits Related to Bariatric Surgery: Review of Normal Post-Surgical Anatomy as Well as Complications Dept. of Medical Imaging University of Ottawa Disclosures Background Roux-en-Y Gastric Bypass Surgery
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of
 Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Endoscopic therapy for obesity and complications of bariatric surgery
 Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
When, Why, and How to Revise a Failed Sleeve Gastrectomy
 When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Teresa LaMasters MD, FACS Minimally Invasive Bariatric Surgeon Iowa Health Weight Loss Specialists Throckmorton Surgical Society May 4, 2012
 Laparoscopic Sleeve Gastrectomy Teresa LaMasters MD, FACS Minimally Invasive Bariatric Surgeon Iowa Health Weight Loss Specialists Throckmorton Surgical Society May 4, 2012 Objectives Understand the anatomy
Laparoscopic Sleeve Gastrectomy Teresa LaMasters MD, FACS Minimally Invasive Bariatric Surgeon Iowa Health Weight Loss Specialists Throckmorton Surgical Society May 4, 2012 Objectives Understand the anatomy
Endoscopic Management of Strictures and Leaks. Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center
 Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
Emergencies in Post- Bariatric Surgery Patients
 Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass
 ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass Katherine Arndtz a, Helen Steed b, James Hodson
ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass Katherine Arndtz a, Helen Steed b, James Hodson
Obesity When to Recommend Surgery. Lily Chang, MD September 27, 2013
 Obesity When to Recommend Surgery Lily Chang, MD September 27, 2013 Obesity BMI >30 Trends Among U.S. Adults Source: Behavioral Risk Factor Surveillance System, CDC, 2012 Obesity Related Co-Morbidities
Obesity When to Recommend Surgery Lily Chang, MD September 27, 2013 Obesity BMI >30 Trends Among U.S. Adults Source: Behavioral Risk Factor Surveillance System, CDC, 2012 Obesity Related Co-Morbidities
Weight Loss before Hernia Repair Surgery
 Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
OG Tube/Bougie vs. Suction Calibration System for Effects on Operative Duration, Staple-line Corkscrewing, and Esophageal Perforation during LSG.
 July 14, 2015 OG Tube/Bougie vs. Suction Calibration System for Effects on Operative Duration, Staple-line Corkscrewing, and Esophageal Perforation during LSG. Michel Gagner, MD, FRCSC, FACS, FASMBS Rose
July 14, 2015 OG Tube/Bougie vs. Suction Calibration System for Effects on Operative Duration, Staple-line Corkscrewing, and Esophageal Perforation during LSG. Michel Gagner, MD, FRCSC, FACS, FASMBS Rose
Sleeve Gastrectomy. Stacy A. Brethauer, MD
 Sleeve Gastrectomy Stacy A. Brethauer, MD KEYWORDS Bariatric Sleeve gastrectomy Vertical gastrectomy HISTORY Sleeve gastrectomy (SG) was originally performed as the restrictive component of the duodenal
Sleeve Gastrectomy Stacy A. Brethauer, MD KEYWORDS Bariatric Sleeve gastrectomy Vertical gastrectomy HISTORY Sleeve gastrectomy (SG) was originally performed as the restrictive component of the duodenal
Bariatric Surgery. Overview of Procedural Options
 Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid obesity
 Surg Endosc (2005) xx: 1 6 DOI: 10.1007/s00464-005-0134-5 Ó Springer Science+Business Media, Inc. 2005 Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid
Surg Endosc (2005) xx: 1 6 DOI: 10.1007/s00464-005-0134-5 Ó Springer Science+Business Media, Inc. 2005 Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid
Emerging Concepts in Bariatric Surgery
 Emerging Concepts in Bariatric Surgery C Y N T H I A L. L O N G, M D, F A C S S I N A I H O S P I T A L O F B A L T I M O R E D E P A R T M E N T O F S U R G E R Y D I V I S I O N O F M I N I M A L L Y
Emerging Concepts in Bariatric Surgery C Y N T H I A L. L O N G, M D, F A C S S I N A I H O S P I T A L O F B A L T I M O R E D E P A R T M E N T O F S U R G E R Y D I V I S I O N O F M I N I M A L L Y
Lose the Weight, Find your Life
 Bariatric Surgery: University of Iowa Lose the Weight, Find your Life Isaac Samuel, MD, FRCS, FACS Professor of Surgery Director, Bariatric Surgery 1 Present UI Bariatric Surgeons Jessica Smith, MD Peter
Bariatric Surgery: University of Iowa Lose the Weight, Find your Life Isaac Samuel, MD, FRCS, FACS Professor of Surgery Director, Bariatric Surgery 1 Present UI Bariatric Surgeons Jessica Smith, MD Peter
Weight Loss Surgery Info for Physicians
 Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Diabetes and Weight-Loss Surgery
 WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
Types of Bariatric Procedures. Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012
 Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Roux-en-Y Gastric Bypass
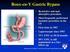 Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Technical Aspects of Bariatric Surgical Procedures. Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital
 Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
What is the Sleeve Gastrectomy?
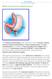 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
Laparoscopic Sleeve Gastrectomy with an Extensive Posterior Mobilization: Technique and Preliminary Results
 DOI 10.1007/s11695-011-0488-9 NEW CONCEPTS Laparoscopic Sleeve Gastrectomy with an Extensive Posterior Mobilization: Technique and Preliminary Results Ralph P. M. Gadiot & Lacer Ulas Biter & Hans J. F.
DOI 10.1007/s11695-011-0488-9 NEW CONCEPTS Laparoscopic Sleeve Gastrectomy with an Extensive Posterior Mobilization: Technique and Preliminary Results Ralph P. M. Gadiot & Lacer Ulas Biter & Hans J. F.
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Informed Consent for Laparoscopic Roux en Y Gastric Bypass. Patient Name
 Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Successful Management of Refractory Staple Line Leakage at the Esophagogastric Junction After a Sleeve Gastrectomy Using the HANAROSTENT
 DOI 10.1007/s11695-009-9976-6 CASE REPORT Successful Management of Refractory Staple Line Leakage at the Esophagogastric Junction After a Sleeve Gastrectomy Using the HANAROSTENT Takashi Oshiro & Kazunori
DOI 10.1007/s11695-009-9976-6 CASE REPORT Successful Management of Refractory Staple Line Leakage at the Esophagogastric Junction After a Sleeve Gastrectomy Using the HANAROSTENT Takashi Oshiro & Kazunori
Treatment for severe GERD after Sleeve Gastrectomy: conversion to gastric bypass or endoluminal radiofrequency. Alfonso Torquati, MD, MSCI, FACS
 Treatment for severe GERD after Sleeve Gastrectomy: conversion to gastric bypass or endoluminal radiofrequency. Alfonso Torquati, MD, MSCI, FACS Associate Professor and Chief Division of Metabolic and
Treatment for severe GERD after Sleeve Gastrectomy: conversion to gastric bypass or endoluminal radiofrequency. Alfonso Torquati, MD, MSCI, FACS Associate Professor and Chief Division of Metabolic and
Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it
 CENTER OF EXCELLENCE FOR THE STUDY AND OBESITY TREATMENT Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it Concepts and Results in a series of 11-years experience with 2,200 patients Miguel-A.
CENTER OF EXCELLENCE FOR THE STUDY AND OBESITY TREATMENT Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it Concepts and Results in a series of 11-years experience with 2,200 patients Miguel-A.
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
UW MEDICINE PATIENT EDUCATION. Weight Loss Surgery. What is bariatric surgery?
 UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy
 Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY
 INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. 201-795-8175 CarePointHealth.
 www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
If you are morbidly obese, you should remember these important points:
 What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Laparoscopic Gastric Bypass
 Restrictive and Malabsorbative procedure Laparoscopic Gastric Bypass Dr. H. Lönroth Professional Education 1 2 Introduction Gastric bypass as a therapy for morbid obesity was first published by Mason and
Restrictive and Malabsorbative procedure Laparoscopic Gastric Bypass Dr. H. Lönroth Professional Education 1 2 Introduction Gastric bypass as a therapy for morbid obesity was first published by Mason and
Bariatric Weight Loss Surgery
 BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Gastric Sleeve Surgery
 Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS
 GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures
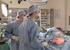 Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures Table 1: Surgeon Billing for Laparoscopic Adjustable Gastric Band Procedures 2012 Medicare Payment 2 43770
Surgeon and Radiological Services Billing for Laparoscopic Adjustable Gastric Band Procedures Table 1: Surgeon Billing for Laparoscopic Adjustable Gastric Band Procedures 2012 Medicare Payment 2 43770
Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery
 Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Obesity Obesity is defined as having a body mass index (BMI) of 30 or greater. Obesity is a serious medical
Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Obesity Obesity is defined as having a body mass index (BMI) of 30 or greater. Obesity is a serious medical
Outcomes and options in the management of leak and gastric fistula after sleeve gastrectomy.
 Outcomes and options in the management of leak and gastric fistula after sleeve gastrectomy. 1 Mercy Bariatrics, Perth Australia Leon Cohen 1 Leak and gastric fistula after sleeve gastrectomy remains one
Outcomes and options in the management of leak and gastric fistula after sleeve gastrectomy. 1 Mercy Bariatrics, Perth Australia Leon Cohen 1 Leak and gastric fistula after sleeve gastrectomy remains one
Bariatric i Surgery: Optimalizing Outcome Results. Dr. B. Dillemans AZ Sint-Jan AV Brugge-Oostende BARIATRIC SURGERY
 Bariatric i Surgery: Optimalizing i Outcome Results Dr. B. Dillemans AZ Sint-Jan AV Brugge-Oostende THE OBESE PATIENT : A CHALLENGE FOR ANAESTHESIA, Ostend,14/11/09 BARIATRIC SURGERY 50 s : First Reported
Bariatric i Surgery: Optimalizing i Outcome Results Dr. B. Dillemans AZ Sint-Jan AV Brugge-Oostende THE OBESE PATIENT : A CHALLENGE FOR ANAESTHESIA, Ostend,14/11/09 BARIATRIC SURGERY 50 s : First Reported
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
GP Guidance: Management of nutrition following bariatric surgery
 GP Guidance: Management of nutrition following bariatric surgery Introduction Patients who are morbidly obese will have struggled with their weight for many years before going forward for bariatric surgery.
GP Guidance: Management of nutrition following bariatric surgery Introduction Patients who are morbidly obese will have struggled with their weight for many years before going forward for bariatric surgery.
Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Weight Loss Program for Teens
 Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
MEDICAL COVERAGE POLICY. SERVICE: Bariatric (Weight Loss) Surgery Policy Number: 053 Effective Date: 5/27/2014 Last Review: 4/24/2014
 Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
WEIGHT LOSS SURGERY. Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010
 WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
Roux-en-y gastric bypass - clinical perspectives
 Roux-en-y gastric bypass - clinical perspectives Tom Mala Consultant surgeon Department of Gastroenterologic Surgery Oslo University Hospital Bariatric surgery weight loss Sjøstrøm L, JAMA 2012 Five-year
Roux-en-y gastric bypass - clinical perspectives Tom Mala Consultant surgeon Department of Gastroenterologic Surgery Oslo University Hospital Bariatric surgery weight loss Sjøstrøm L, JAMA 2012 Five-year
5/9/2012. What is Morbid Obesity? Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person)
 Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person) 1990 1998 The Bariatric and Metabolic Center of Colorado Bariatric Surgery: Options, Care
Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person) 1990 1998 The Bariatric and Metabolic Center of Colorado Bariatric Surgery: Options, Care
BARIATRIC SURGERY. Personalized Weight Loss Program
 BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
Gastric Imbrication: The Future or Fantasy?
 Opinions General Surgery News. Issue: July 2011 Volume 38:7 Gastric Imbrication: The Future or Fantasy? Expert Panel Meets To Discuss Major Questions About New Procedure for Weight Loss by Daniel Cottam,
Opinions General Surgery News. Issue: July 2011 Volume 38:7 Gastric Imbrication: The Future or Fantasy? Expert Panel Meets To Discuss Major Questions About New Procedure for Weight Loss by Daniel Cottam,
Removal of Peri-Gastric Fat Prevents Acute Obstruction after Lap-Band Surgery
 Obesity Surgery, 14, 224-229 Removal of Peri-Gastric Fat Prevents Acute Obstruction after Lap-Band Surgery Roy Shen, MD; Christine J. Ren, MD Department of Surgery, NYU School of Delivered Medicine, by
Obesity Surgery, 14, 224-229 Removal of Peri-Gastric Fat Prevents Acute Obstruction after Lap-Band Surgery Roy Shen, MD; Christine J. Ren, MD Department of Surgery, NYU School of Delivered Medicine, by
Gastric Surgery for Clinically Severe (Morbid) Obesity
 Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
Laparoscopic Revisional Gastric Bypass after open bariatric surgeries. Haider Alshurafa 1
 Laparoscopic Revisional Gastric Bypass after open bariatric surgeries 1 Surgery Department, Riyadh Military Hospital, Riyadh, Saudi Arabia Haider Alshurafa 1 Objective: To confirm the feasibility of the
Laparoscopic Revisional Gastric Bypass after open bariatric surgeries 1 Surgery Department, Riyadh Military Hospital, Riyadh, Saudi Arabia Haider Alshurafa 1 Objective: To confirm the feasibility of the
Early jejunojejunostomy obstruction after laparoscopic gastric bypass: case series and treatment algorithm
 Surgery for Obesity and Related Diseases 5 (2009) 203 207 Original article Early jejunojejunostomy obstruction after laparoscopic gastric bypass: case series and treatment algorithm Catherine E. Lewis,
Surgery for Obesity and Related Diseases 5 (2009) 203 207 Original article Early jejunojejunostomy obstruction after laparoscopic gastric bypass: case series and treatment algorithm Catherine E. Lewis,
