List of diagnostic flowcharts
|
|
|
- Edward Andrews
- 8 years ago
- Views:
Transcription
1
2 List of diagnostic flowcharts Chapter 3 Visual loss Transient visual loss 43 Sudden or rapidly progressive visual loss 46 Gradual visual loss 61 Chapter 4 The red eye One red eye, decreased vision 83 One red eye, normal vision 91 Two red eyes, normal vision 92 Chapter 5 Eye trauma Eye trauma 108 Chapter 6 Turned eye/double vision Turned eye in children 132 Double vision in adults 139 Chapter 7 Abnormal appearance of the eye or eyelids EYE Spot on the eye surface 154 Unequal pupils 157 White pupil and/or no red reflex 163 Nystagmus (continually moving eyes) 165 Proptosis (eye(s) pushed forwards) 167 Abnormal optic disc on ophthalmoscopy 168 EYELIDS Eyelid lump 179 Abnormal eyelid position 183 Red swollen eyelids on one side 188 Skin rash around the eye 191
3 EYE ESSENTIALS FOR EVERY DOCTOR
4
5 EYE ESSENTIALS FOR EVERY DOCTOR Anthony Pane MBBS (Hons) MMedSc FRANZCO Consultant Ophthalmic Surgeon Queensland Eye Institute Brisbane, Australia Peter Simcock MB ChB DO FRCP MRCP FRCOphth Consultant Ophthalmic Surgeon West of England Eye Unit Royal Devon and Exeter Hospital Exeter, UK Edinburgh London New York Oxford Philadelphia St Louis Sydney Toronto 2005
6 Churchill Livingstone is an imprint of Elsevier Elsevier Australia. ACN (a division of Reed International Books Australia Pty Ltd) Tower 1, 475 Victoria Avenue, Chatswood, NSW 2067 This edition 2013 Elsevier Australia UK ISBN This publication is copyright. Except as expressly provided in the Copyright Act 1968 and the Copyright Amendment (Digital Agenda) Act 2000, no part of this publication may be reproduced, stored in any retrieval system or transmitted by any means (including electronic, mechanical, microcopying, photocopying, recording or otherwise) without prior written permission from the publisher. Every attempt has been made to trace and acknowledge copyright, but in some cases this may not have been possible. The publisher apologises for any accidental infringement and would welcome any information to redress the situation. This publication has been carefully reviewed and checked to ensure that the content is as accurate and current as possible at time of publication. We would recommend, however, that the reader verify any procedures, treatments, drug dosages or legal content described in this book. Neither the author, the contributors, nor the publisher assume any liability for injury and/or damage to persons or property arising from any error in or omission from this publication. National Library of Australia Cataloguing-in-Publication Data Author: Pane, Anthony. Title: Eye essentials for every doctor / Anthony Pane, Peter Simcock. ISBN: (pbk.) Subjects: Eye--Examination. Eye--Diseases--Diagnosis. Other Authors: Simcock, Peter. Dewey Number: Commissioning Editor: Michael Parkinson Project Development Manager: Hannah Kenner Project Manager: Nancy Arnott Design Direction: George Ajayi Cover design: Avril Makula Cover photograph copyright Tatiana Makotra Illustration Manager: Bruce Hogarth Illustrators: Jane Fallow and Antbits Printer: Griffin Press
7 CONTENTS v Contents List of diagnostic flowcharts Acknowledgements Introduction How to use this book Inside front cover vi vii ix 1. Staying out of trouble with eyes 1 2. How to examine an eye patient Visual loss The red eye Eye trauma Turned eye/double vision Abnormal appearance of the eye or eyelids Watery, itchy or gritty eyes Other eye symptoms Who needs screening for eye disease? Basic eye procedures 225 Further reading 230 Index 231
8 vi Acknowledgements We would like to thank the following people for their contribution to the book: Jason Smith, Sue Masel, Matt Masel and Lawrie Hirst for their careful proof reading and excellent suggestions; at Elsevier, Michael Parkinson for picking up the book and Hannah Kenner for her energy and professionalism in its production; and my wife Kath for her endless patience, support and encouragement. Anthony Pane My parents Mae and Reg and my wife Sarah for their support and Ray MacLeod, Medical photographer, West of England Eye Unit, for his hard work in helping with the photographs Peter Simcock
9 vii Introduction As a medical student, hospital doctor or general practitioner you can t be expected to know everything. Ophthalmology is only one of many specialties, each with its own list of rare and unpleasant diseases you are sternly told you can t afford to miss! You usually have minimal examination time and little or no equipment. Despite this, many of your patients have eye complaints and rely on you for appropriate management. What do you do? This book is a symptom-based guide to ophthalmology for the non-ophthalmologist. Many eye books list disease by anatomical site, but patients don t present saying I have a disease of my optic nerve. Instead, they walk into your office and complain of blurred vision. Each of the main chapters in this book concentrates on a different presenting symptom, and contains: An overview of the problem. Critical points highlighting important management issues. Diagnostic flowcharts. An approach to use for the patient sitting before you, including questions to ask and signs to look for. A brief discussion of the symptoms, signs and management of the relevant common eye diseases. Some chapters include special features: Chapter 1 Staying out of trouble with eyes contains practical guidelines to help you avoid serious mistakes in your everyday practice. Chapter 2 How to examine an eye patient outlines a time-efficient way to assess eye patients. Chapter 10 Who needs screening for eye disease? a guide to which of your patients require regular eye screening. Chapter 11 Basic eye procedures details common practical eye procedures.
10 viii INTRODUCTION Ophthalmic diagnosis is often difficult, even with the luxury of time and the appropriate technology. However, even a brief history and examination with basic equipment can be enough to identify the general nature of most eye diseases. We hope this book helps.
11 ix How to use this book Medical students: read the chapters in order. General practitioners: If you re already good at eye examination: skip Chapter 2. Short of time? Read Chapters 1 and 10 then have a look at the overview, flowcharts and photographs in the other chapters. Keep the book handy for quick reference in the clinic. Emergency department doctors: If you re already good at eye examination: skip Chapter 2. Short of time? Chapters 1, 3, 4, 5 and 11 are particularly important for you. Please note: There are thousands of eye diseases, about which millions of pages have been written. A brief book such as this relies on massive over-simplification and there are many rare eye diseases not discussed here at all. Writing for such a wide audience means starting from the basics ; we acknowledge that many readers will already be highly knowledgeable about some of the areas covered (more advanced texts are suggested in the Further Reading). This book is not intended to be a substitute for thorough clinical training. The best way to learn ophthalmic diagnosis and management is by sitting in clinics with an experienced ophthalmologist. In this book, ophthalmic referral or ophthalmic assessment means referral to an ophthalmologist (eye surgeon) or ophthalmic emergency department. Often, real life cases aren t as clear-cut as on the printed page; if in doubt, refer.
12
13 CHAPTER TURNED EYE/DOUBLE VISION 6 CHAPTER CONTENTS TURNED EYE IN CHILDREN 130 OVERVIEW 130 Critical points: turned eye in children 130 Squint terminology 131 Ophthalmic management 131 Diagnostic flowchart 6.1: turned eye in children 132 Approach to a child with a turned eye 133 IDIOPATHIC CHILDHOOD DEVIATIONS 136 Idiopathic esotropia 136 Idiopathic intermittent exotropia 137 Idiopathic vertical deviations 137 OTHER CAUSES OF CHILDHOOD STRABISMUS 137 DOUBLE VISION IN ADULTS 138 OVERVIEW 138 Critical points: double vision in adults 138 Diagnostic flowchart 6.2: double vision in adults 139 Ophthalmic management 140 Approach to an adult with double vision 140 BRAIN DISEASES 142 NERVE DISEASES 142 Third nerve palsy 142 Fourth nerve palsy 145 Sixth nerve palsy
14 CHAPTER CONTENTS 129 CHAPTER CONTENTS cont d EYE MUSCLE DISEASES 147 Myasthenia gravis 147 Thyroid eye disease 147 ORBIT DISEASES 149 BLIND EYE 149
15 130 TURNED EYE IN CHILDREN TURNED EYE IN CHILDREN OVERVIEW A 6-month old child brought to you with an inward-turned eye most likely has idiopathic infantile ( congenital ) esotropia. There is a small chance, however, that the child actually has a brain tumour that has caused a sixth nerve palsy, or that the eye has turned because it is blind from a malignant intraocular retinoblastoma. Hence every child with a turned eye (strabismus or squint ) requires prompt ophthalmic referral. The second important reason for early referral of childhood squints is that if an eye is turned for even a few weeks early in life, or a few months in later childhood, the visual area of the developing brain develops fewer connections with the turned eye than with the straight eye. This results in amblyopia (often called lazy eye ). In amblyopia, the eyeball itself is normal; it is the connections in the visual cortex that are poorly formed. Amblyopia can cause permanent blindness of the turned eye if it is not detected and treated early. Unlike adults with new-onset squint, children with early-onset squints who are old enough to talk do not complain of double vision: this is because the young brain learns to ignore the turned eye. Turned eye in children Critical points A child of any age with strabismus ( turned eye ) has a sight- or life-threatening condition until proven otherwise and needs prompt referral. Childhood tumours of the brain and eye often present with a turned eye. Never observe a child with strabismus it is very rare for a child to grow out of it. Delay in ophthalmic referral can result in permanent visual loss from amblyopia ( lazy eye ).
16 OVERVIEW 131 SQUINT TERMINOLOGY There are many terms related to squint. A few of the basic ones are: Terms for normal eye movements: adduction: eye looking in towards the nose abduction: eye looking out towards the ear elevation: eye looking up depression: eye looking down. Horizontal squints: eye turned in: esotropia eye turned out: exotropia both of these can be constant or intermittent; they can always affect one eye or alternate between the two eyes. Vertical squints: one eye higher: hypertropia one eye lower: hypotropia. OPHTHALMIC MANAGEMENT The basic management of childhood squint by ophthalmologists is step-wise: 1. Exclude a serious underlying cause. 2. Correct refractive error, if present, with glasses. 3. If one eye is persistently turned and has poor vision from amblyopia, patch the straight eye to force the turned eye to form normal connections with the brain s visual cortex and reverse amblyopia. Patching might be needed part-time for months or years, and requires close ophthalmic supervision. 4. Once maximum visual improvement in the amblyopic eye has been attained, perform squint surgery to align the eyes. Patching might need to continue after surgery.
17 132 TURNED EYE IN CHILDREN DIAGNOSTIC FLOWCHART 6.1: TURNED EYE IN CHILDREN Eye deviation with the patient looking straight ahead? Eye turned in (esotropia) Eye turned out (exotropia) Vertical (eye turned up or down) Oblique (both horizontal and vertical) Idiopathic infantile esotropia or accommodative esotropia Sixth nerve palsy (partial or complete) Idiopathic intermittent extropia Partial third nerve palsy Idiopathic vertical deviations Fourth nerve palsy Partial third nerve palsy Partial third nerve palsy Multiple nerve palsies Combined idiopathic deviations Plus all of these deviations can also be caused by: blindness of one or both eyes extraocular muscle disease orbital disease, including tumours brain disease Examination 'clues' to the cause: restriction of eye movements in any direction (both eyes don't move fully in all directions): brain, nerve, muscle or orbit disease is possible. Restriction of movement can be very subtle and difficult to detect (e.g. in fourth nerve palsy or partial third or sixth nerve palsies) enlarged pupil that reacts poorly to light: suspect third nerve palsy ptosis (drooping upper lid): suspect third nerve palsy or muscle disease proptosis (eyeball pushed forwards): orbital inflammation or tumour red eye: orbital inflammation or tumour head tilted towards one shoulder: suspect fourth nerve palsy other neurologic signs: brain or nerve disease
18 OVERVIEW 133 APPROACH TO A CHILD WITH A TURNED EYE ASK How and when was the problem noticed? Which eye turns? Is the turn constant or intermittent? Do the parents think the child can see? (as appropriate for age) most children can: keep eye contact with their parent at age 6 weeks show interest in bright objects at 2 3 months fix and follow objects with their eyes at 3 4 months. LOOK FOR 1. Can the child see, and can they see equally out of both eyes? 2. If there is an eye turn (squint, strabismus), what direction is the deviation? 3. Does each eye move fully in all directions? 4. Is there anything wrong with the eyes apart from the squint (e.g. cataract, retinal tumour, optic nerve disease)? 5. Is there anything wrong with the child apart from the squint (e.g. developmental delay, neurological or metabolic disease)? CAN THE CHILD SEE WITH BOTH EYES OPEN? Observe the child while you re talking to the parents. 3 4 months or older: can the child fix and follow a toy? will the child pick up small sweets or toys? Older children: can the child identify small pictures or read the visual acuity chart? DO THE TWO EYES SEE EQUALLY WELL? Try to repeat the above tests with one eye covered at a time (this is often difficult). Does the child object equally to covering each eye? (he or she won t mind having a blind eye covered as much as a good eye). EYE ALIGNMENT LOOKING STRAIGHT AHEAD Observation. with the child looking at you or a torch, does one eye seem to be turned? In which direction? LOOK FOR ASK
19 134 TURNED EYE IN CHILDREN LOOK FOR Fig. 6.1 The cover test. Cover test (this can be difficult in young children) (Fig. 6.1): with the child looking straight ahead at an interesting target, cover the right eye (you can use your hand, a piece of cardboard, etc.) look at the left eye the whole time if the left eye moves when you cover the right eye, the left eye is the turned eye if it moves out, it was turned in (esotropia) if it moves in, it was turned out (exotropia) if it moves down, it was turned up (hypertropia) and so on uncover the right eye now cover the left eye look at the right eye the whole time if the right eye moves when you cover the left eye, the right eye is the turned eye. EYE MOVEMENTS (3 4 MONTHS OR OLDER) With both eyes open, have the child track a slow-moving toy from side to side and up and down. Try to repeat this one eye at a time, with the other eye covered with the parent s hand or a patch. Does each eye move fully in all directions? RED REFLEX If the red reflex is absent on one or both sides, cataract, retinoblastoma tumour or other serious disease could be present and requires urgent referral.
20 OVERVIEW 135 RELATIVE AFFERENT PUPILLARY DEFECT (RAPD) See p. 25 for details of how to test for this. The presence of a relative afferent pupillary defect is indicative of serious retinal or optic nerve disease. OPHTHALMOSCOPY Try to see the optic discs: are they normal? Is there swelling? This is often difficult in young children. In general, don t use dilating eye drops for children; special concentrations of drops will be used by the ophthalmologist if necessary.
21 136 TURNED EYE IN CHILDREN IDIOPATHIC CHILDHOOD DEVIATIONS These are a collection of common childhood strabismus syndromes of unknown cause, which usually occur in otherwise healthy children. A child presenting with any of these syndromes requires semiurgent ophthalmic referral. They are diagnoses of exclusion, after underlying eye, nerve and brain disease have been looked for and ruled out (this can usually be done clinically by an experienced ophthalmologist, but sometimes other tests are necessary). IDIOPATHIC ESOTROPIA (ONE EYE IS TURNED IN) Idiopathic infantile esotropia ( congenital esotropia) (Fig. 6.2): first noticed by parents before 6 months of age usually there is no significant refractive error correction with surgery. Accommodative esotropia: onset usually 2 4 years of age hypermetropic ( long-sighted ) refractive error prescription of glasses may partly or completely correct the squint. Diseases that can mimic idiopathic esotropia: partial or complete unilateral or bilateral sixth nerve palsy blind eye brain disease. Fig. 6.2 Idiopathic infantile esotropia.
22 IDIOPATHIC CHILDHOOD DEVIATIONS 137 Fig. 6.3 Idiopathic childhood exotropia. IDIOPATHIC INTERMITTENT EXOTROPIA (ONE EYE IS TURNED OUT) (Fig. 6.3) Onset as an intermittent deviation after 2 years of age. Correction with surgery if it becomes frequent or constant. Diseases that can mimic intermittent exotropia: partial third nerve palsy (limited adduction of one eye) blind eye brain disease. IDIOPATHIC VERTICAL DEVIATIONS These include dissociated vertical deviation and Brown s syndrome (please see one of the texts in Further reading for details). Diseases that can mimic idiopathic vertical deviations: partial third nerve palsy, fourth nerve palsy blind eye brain disease. OTHER CAUSES OF CHILDHOOD STRABISMUS Blind eyes in children tend to turn (often resulting in an esotropia or exotropia). Any of the causes of adult strabismus can also occur in children, for example: brain tumours can present with any type of squint orbital tumours can present with a squint infectious or inflammatory disease can result in third, fourth or sixth nerve palsies. Children can be born with a congenital palsy of the fourth nerve this often presents as a head tilt (the child does this to compensate for the visual tilt produced by the palsy).
23 138 DOUBLE VISION IN ADULTS DOUBLE VISION IN ADULTS OVERVIEW Adults with a turned eye will present to you complaining of double vision (diplopia seeing two images of everything). The only exceptions to this occur if there is poor vision in one eye, if the squint has been present since childhood or in complete third nerve palsy in which a complete ptosis occludes the eye. Most adults with double vision have significant eye muscle, nerve or brain pathology. Examples include thyroid eye disease, myasthenia gravis, palsies of the ocular motor nerves and complex eye movement problems from brainstem disease. Third, fourth or sixth cranial nerve palsies are often ischaemic in the elderly (due to diabetes, hypertension or temporal arteritis), but cannot be assumed to be so without a careful work-up. In particular, partial or complete third nerve palsy in an adult is often due to an expanding cerebral arterial aneurysm, which could rupture and kill the patient unless diagnosed and operated on immediately. Every adult with new-onset double vision requires urgent ophthalmic referral. Adults (and children over the age of 9) do not develop amblyopia ( lazy eye ) if one eye is constantly turned. However, constant double vision can be very annoying, makes driving illegal and often interferes with the patient s life. Double vision in adults Critical points New-onset double vision in a patient of any age is a lifethreatening cerebral aneurysm until proven otherwise all require urgent (same-day) ophthalmic referral. Never prescribe spectacle prism for double vision of unknown cause unless the patient has been assessed by an ophthalmologist. Brain tumours are a common cause of gradualonset diplopia. If a patient over 50 has transient or persisting double vision, ask about symptoms of temporal arteritis (see p. 216).
24 OVERVIEW 139 DIAGNOSTIC FLOWCHART 6.2: DOUBLE VISION IN ADULTS Eye deviation with the patient looking straight ahead? Eye turned in (esotropia) Eye turned out (exotropia) Vertical (eye turned up or down) Oblique (both horizontal and vertical) Sixth nerve palsy (partial or complete) Partial third nerve palsy Fourth nerve palsy Partial or complete third nerve palsy Partial third nerve palsy Multiple nerve palsies Plus all of these deviations can also be caused by: myasthenia gravis thyroid eye disease orbital disease, including tumours brain disease Examination 'clues' to the cause: restriction of eye movements in any direction (both eyes don't move fully in all directions): brain, nerve, muscle or orbit disease is possible. Restriction of movement can be very subtle and difficult to detect (e.g. in fourth nerve palsy or partial third or sixth nerve palsies) enlarged pupil that reacts poorly to light: suspect third nerve palsy ptosis (drooping upper lid): suspect third nerve palsy or myasthenia gravis lid retraction (upper lid too high): thyroid eye disease proptosis (eyeball pushed forwards): thyroid eye disease, orbital inflammation or tumour red eye: active thyroid eye disease, orbital inflammation head tilted towards one shoulder: suspect fourth nerve palsy weakness of facial or body muscles: myasthenia gravis other neurologic signs: brain or nerve disease
25 140 DOUBLE VISION IN ADULTS LOOK FOR ASK OPHTHALMIC MANAGEMENT The basic management of adult squint by ophthalmologists is step-wise: 1. Exclude a serious underlying cause. 2. Treat the underlying cause if possible. 3. If no treatable cause is found (e.g. in ischaemic sixth nerve palsy), relieve the double vision while awaiting recovery by patching or prism spectacle lens. If no recovery in 6 12 months, eye muscle squint surgery may be considered. APPROACH TO AN ADULT WITH DOUBLE VISION ASK PRESENTING COMPLAINT When was the double vision first noticed? Was the onset sudden or gradual? (sudden onset is often ischaemic; gradual onset might be a tumour, although there are exceptions to this). Is it constant or does it vary depending on time of day? (if worse at night or when tired: could be myasthenia). SPECIFIC QUESTIONING Is there pain in or around the eye? Are there any neurological symptoms, e.g. headache, vertigo, limb weakness or numbness? Are there any symptoms of systemic myasthenia gravis? (e.g. drooping eyelids late in the day, limb muscle weakness, problems swallowing or breathing). If the patient is over 50, check for symptoms of temporal arteritis. (see p. 216). PREVIOUS MEDICAL HISTORY Risk factors for ischaemic nerve palsy, e.g. diabetes, hypertension, smoker? (however, this does not mean that a nerve palsy found in such a patient is ischaemic). LOOK FOR 1. Does the patient have normal vision in each eye? 2. Which eye is turned, and what direction is the turn with the patient looking straight ahead? 3. Do both eyes move fully in all directions? 4. Is there anything wrong with the eyes apart from the squint?
26 OVERVIEW Is there anything wrong with the patient apart from the squint? Ask whether the patient has any other neurological symptoms; if so, do a full neurological examination. VISUAL ACUITY VISUAL FIELDS Pituitary tumours can present with a squint (and a bitemporal hemianopia on visual field testing). ORBITAL SIGNS Proptosis (eyeball pushed forwards) in thyroid eye disease and orbital tumours. Conjunctival redness and swelling in acute thyroid eye disease or other inflammatory disease. EYELIDS Ptosis (drooping upper eyelid) can be a sign of: partial or complete third nerve palsy myasthenia gravis Horner s syndrome (mild ptosis only) orbit disease (e.g. tumour usually also with proptosis) Eyelid retraction (upper lid too high; +/ lower lid too low): common in thyroid eye disease (giving the eye(s) a staring appearance). PUPIL SIZE AND REACTION TO LIGHT AND DARK A large pupil that constricts poorly to light can be a sign of third nerve palsy. A small pupil that dilates poorly in the dark can be a sign of Horner s syndrome. RELATIVE AFFERENT PUPILLARY DEFECT (RAPD) If present, retinal or optic nerve disease is present. EYE ALIGNMENT AND MOVEMENT Assess as described for childhood squints (see p. 133). OPHTHALMOSCOPY Are the optic discs normal? Is there bilateral optic disc swelling? (could be a brain tumour). SYSTEMIC AND NEUROLOGIC EXAMINATION As needed. LOOK FOR
27 142 DOUBLE VISION IN ADULTS BRAIN DISEASES Brain tumours, multiple sclerosis (MS) and stroke are all common causes of double vision in adults. Diseases affecting the brainstem can cause several types of strabismus: for example: Internuclear ophthalmoplegia (INO): right internuclear ophthalmoplegia: when the patient tries to look left the right eye can t move all the way in to the nose (adduction deficit); the left eye moves out towards the left ear normally but oscillates horizontally (abducting nystagmus) vice versa for left internuclear ophthalmoplegia. Gaze palsies: these are limitations of voluntary eye movement to one side, e.g. neither eye may be able to look to the right. NERVE DISEASES The third, fourth and sixth cranial nerves between them supply all six extraocular muscles of each eye: Third nerve: superior rectus, inferior rectus, medial rectus and inferior oblique; plus the levator muscle (which elevates the upper lid) and the pupil constrictor muscle (which makes the pupil constrict to light). Fourth nerve: superior oblique. Sixth nerve: lateral rectus. THIRD NERVE PALSY CAUSES Compression of the third nerve by aneurysm or tumour. can occur in adults of any age an expanding posterior communicating artery aneurysm is a common cause of partial or complete third nerve palsy this can kill the patient within hours of onset of the double vision if it is not detected and treated before it ruptures (Fig. 6.4). Ischaemia of the nerve: overall the most common cause of third nerve palsy in adults. atherosclerosis, diabetes, hypertension temporal arteritis (this is a less common but more serious cause think of this in patients over age 50).
28 NERVE DISEASES 143 Fig. 6.4 Right partial third nerve palsy due to compression of the third nerve by a right posterior communicating artery aneurysm (right picture, arrow). The only abnormality on examination was decreased elevation of the right eye on looking up; other movements and the pupil were normal. Inflammation of the nerve: e.g. viral infections or post-viral autoimmune reaction. Raised intracranial pressure. Trauma. SYMPTOMS Horizontal, vertical or oblique diplopia. In some patients, drooping upper eyelid (ptosis) if complete and occluding the eye, the patient will not complain of diplopia. SIGNS A third nerve palsy can be partial (some function remains in one or more of the muscles supplied by the nerve) or complete (all function has been lost). A complete third nerve palsy is easy to diagnose. Partial third nerve palsies can mimic other types of strabismus and be difficult to diagnose. Partial third nerve palsy can show one or more of: exotropia with decreased adduction vertical deviation (hypertropia or hypotropia) decreased elevation or depression
29 144 DOUBLE VISION IN ADULTS oblique deviation a combination of exotropia and vertical deviation the upper lid may be normal or show ptosis (drooping upper lid) the pupil may be normal, slightly dilated, or very dilated (if dilated, it also reacts poorly to light). Complete third nerve palsy (Fig. 6.5) signs: complete ptosis (eyelid completely closed) eye deviated outwards (exotropia) and usually also slightly downwards (hypotropia) the eye can t move up, down or in at all the pupil may be normal, or dilated and unreactive to light Note: pupil-sparing third nerve palsies: it used to be said that if an eye with a third nerve palsy had a normal pupil (rather than a dilated pupil, i.e. that if the nerve palsy was pupil sparing ) the patient did not require neuroimaging because the cause was ischaemic and not compressive however, aneurysms and tumours can cause pupil-sparing third nerve palsies and partial progressive palsies, when the pupil is initially spared but later involved for this reason all patients with third nerve palsy should be urgently assessed by an ophthalmologist, regardless of the state of the pupil. Fig. 6.5 Left complete left third nerve palsy: complete ptosis and inability to adduct, elevate or depress the left eye. In this case the left pupil was dilated and unreactive to light.
30 NERVE DISEASES 145 MANAGEMENT Urgent ophthalmic referral for careful examination +/ further investigation (including urgent neuroimaging to detect aneurysm or tumour if required). FOURTH NERVE PALSY SYMPTOMS Vertical, oblique or tilted double vision. SIGNS Fourth nerve palsy can be very difficult to detect clinically; most non-ophthalmologists say that it looks to them that the eyes move normally. Often, the diagnosis cannot be made without careful examination (including cover test and prism measurements) by a practitioner experienced in eye-movement disorders. The patient will often have a head tilt to the side opposite the palsy. CAUSES Idiopathic congenital. Trauma (often mild closed head injury without loss of consciousness). Compression by a brain tumour. Ischaemia atherosclerosis, hypertension, diabetes or temporal arteritis. Inflammation or infection. MANAGEMENT Urgent ophthalmic referral for further examination and investigation.
31 146 DOUBLE VISION IN ADULTS Fig. 6.6 Left sixth nerve palsy. Top left: a left esotropia looking straight ahead. Bottom pictures show that all eye movements are normal except that the left eye cannot abduct when patient tries to look left. This nerve palsy was the only clinical sign of a left sphenoidal meningioma (top right MRI scan, arrows). SIXTH NERVE PALSY SYMPTOMS Horizontal diplopia. SIGNS Esotropia with limitation of abduction of the eye. CAUSES Ischaemia (diabetes, hypertension, temporal arteritis). Compression by a brain tumour (Fig. 6.6). Inflammation. Trauma. Raised intracranial pressure of any cause can cause a unilateral or bilateral sixth nerve palsy. MANAGEMENT All require urgent ophthalmic referral for further examination +/ investigation.
32 EYE MUSCLE DISEASES 147 EYE MUSCLE DISEASES There are many diseases of the extraocular muscles, the commonest of which is thyroid eye disease. Myasthenia gravis is not strictly a disease of the muscles themselves (it is a disease of the neuromuscular junction), but is included here because it causes muscle dysfunction. Both myasthenia and thyroid eye disease can mimic any pattern of strabismus. Looking at the eyelids can help: if the upper lid is retracted (too high), thyroid eye disease is likely if the upper lid is drooping (ptosis too low), myasthenia is a possibility. MYASTHENIA GRAVIS Auto-antibodies attack the neuro-muscular junction. Drooping upper eyelid/s (ptosis) and/or double vision (diplopia) can occur. Often variable, changing from day to day and during each day (worse at night or when tired). The ptosis might increase if you ask the patient to look up at the ceiling for 2 minutes. Non-ophthalmic symptoms can include: arm or leg weakness and easy fatigue problems swallowing or breathing (symptoms of severe disease can be fatal). Urgent ophthalmic referral. Managed in conjunction with a neurologist. THYROID EYE DISEASE Thyroid eye disease (Fig. 6.7) is a common complication of Graves disease (idiopathic hyperthyroidism). The eye disease seems to run a course independent to the thyroid disease, and occur before, during or after the period of hyperthyroidism. The clinical signs are due to enlargement and inflammation of the extraocular muscles and inflammation of the other orbital tissues.
33 148 DOUBLE VISION IN ADULTS Fig. 6.7 Thyroid eye disease. SYMPTOMS (Often) double vision. Visible change in eye appearance (the eyes seem more prominent due to lid retraction and proptosis). Discomfort/gritty eyes. (Rarely) blurred vision this requires urgent assessment because it could be due to: compressive optic neuropathy (the enlarged muscles compress the optic nerve at the orbital apex severe proptosis does not have to be present for this to occur) corneal exposure, if proptosis is severe. SIGNS One or more of: Any pattern of strabismus, with restriction of ocular movement in any direction (most commonly esotropia or hypotropia). Conjunctival swelling and redness. Eyelid swelling. Upper and lower eyelid retraction (gives a staring appearance). Proptosis ( bulging eye(s) eyeballs pushed forwards). Signs of complications: exposure corneal ulcer if severe proptosis decreased visual acuity, decreased colour vision and relative afferent papillary defect if compressive optic neuropathy.
34 EYE MUSCLE DISEASES 149 MANAGEMENT All patients with symptomatic thyroid eye disease need ophthalmic follow-up. Any patient with Graves disease complaining of blurred (rather than just double) vision requires urgent ophthalmic referral to exclude compressive optic neuropathy. ORBIT DISEASES Orbit tumours or inflammation of any cause can cause double vision. Proptosis (eyeball pushed forwards) is usually present but can be subtle or even absent. CAUSES Infection, e.g. orbital cellulitis (see p. 189). Non-infectious orbital inflammation. Tumours: benign or malignant, any age can mimic inflammation or infection. BLIND EYE Blind eyes can turn in adults, as well as in children. Although blind eyes in children can turn in or out, in adults they tend to turn out ( sensory exotropia ). The patient does not usually notice double vision because of the poor vision in the turned eye.
Fourth Nerve Palsy (a.k.a. Superior Oblique Palsy)
 Hypertropia Hypertropia is a type of strabismus characterized by vertical misalignment of the eyes. Among the many causes of vertical strabismus, one of the most common is a fourth nerve palsy (also known
Hypertropia Hypertropia is a type of strabismus characterized by vertical misalignment of the eyes. Among the many causes of vertical strabismus, one of the most common is a fourth nerve palsy (also known
Esotropia (Crossed Eye(s))
 Esotropia (Crossed Eye(s)) Esotropia is a type of strabismus or eye misalignment in which the eyes are "crossed," that is, while one eye looks straight ahead, the other eye is turned in toward the nose.
Esotropia (Crossed Eye(s)) Esotropia is a type of strabismus or eye misalignment in which the eyes are "crossed," that is, while one eye looks straight ahead, the other eye is turned in toward the nose.
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Cranial Nerves. Cranial Nerve 1: Olfactory Nerve. Cranial Nerve 1: Olfactory Nerve. Cranial Nerve 2: Optic Nerve. Cranial Nerve 2: Optic Nerve
 Cranial Nerves Examination of Cranial Nerves and Palsies Drs Nathan Kerr and Shenton Chew 1 Olfactory On 2 Optic Old 3 Oculomotor Olympus 4 Trochlear Towering 5 Trigeminal Top 6 Abducens A 7 Facial Finn
Cranial Nerves Examination of Cranial Nerves and Palsies Drs Nathan Kerr and Shenton Chew 1 Olfactory On 2 Optic Old 3 Oculomotor Olympus 4 Trochlear Towering 5 Trigeminal Top 6 Abducens A 7 Facial Finn
1 Always test and record vision wearing distance spectacles test each eye separately A 1mm pinhole will improve acuity in refractive errors
 Golden eye rules Examination techniques 1 Always test and record vision wearing distance spectacles test each eye separately A 1mm pinhole will improve acuity in refractive errors Snellen chart (6 metre)
Golden eye rules Examination techniques 1 Always test and record vision wearing distance spectacles test each eye separately A 1mm pinhole will improve acuity in refractive errors Snellen chart (6 metre)
Institute of Ophthalmology. Thyroid Eye Disease. aka Thyroid Associated Ophthalmopathy
 Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
THE EYES IN MARFAN SYNDROME
 THE EYES IN MARFAN SYNDROME Marfan syndrome and some related disorders can affect the eyes in many ways, causing dislocated lenses and other eye problems that can affect your sight. Except for dislocated
THE EYES IN MARFAN SYNDROME Marfan syndrome and some related disorders can affect the eyes in many ways, causing dislocated lenses and other eye problems that can affect your sight. Except for dislocated
Thyroid Eye Disease. A Patient s Guide
 Sashank Prasad, MD www.brighamandwomens.org/neuro-ophthalmology A Patient s Guide Symptoms Diagnosis Treatment Prognosis What are the symptoms of Thyroid Eye Disease? Patients with Thyroid Eye Disease
Sashank Prasad, MD www.brighamandwomens.org/neuro-ophthalmology A Patient s Guide Symptoms Diagnosis Treatment Prognosis What are the symptoms of Thyroid Eye Disease? Patients with Thyroid Eye Disease
Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY
 Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY Neuroophthalmology focuses on conditions caused by brain or systemic abnormalities that result in visual disturbances, among other symptoms.
Vision Health: Conditions, Disorders & Treatments NEUROOPTHALMOLOGY Neuroophthalmology focuses on conditions caused by brain or systemic abnormalities that result in visual disturbances, among other symptoms.
Squint Your Questions Answered Patient Information Leaflet
 Squint Your Questions Answered Patient Information Leaflet What is a Squint? A squint, or strabismus, occurs when the eyes are misaligned and are no longer working as a pair. It is common in childhood,
Squint Your Questions Answered Patient Information Leaflet What is a Squint? A squint, or strabismus, occurs when the eyes are misaligned and are no longer working as a pair. It is common in childhood,
Optic Neuritis. The optic nerve fibers are coated with myelin to help them conduct the electrical signals back to your brain.
 Optic Neuritis Your doctor thinks that you have had an episode of optic neuritis. This is the most common cause of sudden visual loss in a young patient. It is often associated with discomfort in or around
Optic Neuritis Your doctor thinks that you have had an episode of optic neuritis. This is the most common cause of sudden visual loss in a young patient. It is often associated with discomfort in or around
Anatomy: The sella is a depression in the sphenoid bone that makes up part of the skull base located behind the eye sockets.
 Pituitary Tumor Your doctor thinks you may have a pituitary tumor. Pituitary tumors are benign (non-cancerous) overgrowth of cells that make up the pituitary gland (the master gland that regulates other
Pituitary Tumor Your doctor thinks you may have a pituitary tumor. Pituitary tumors are benign (non-cancerous) overgrowth of cells that make up the pituitary gland (the master gland that regulates other
Eye movement problems in adults
 Eye movement problems in adults 07/12/2015 A. Dahlmann-Noor Dr med PhD FRCOphth FRCS(Ed) DipMedEd Consultant Ophthalmologist Clinical Trials Lead Paediatric Ophthalmology Horizontal misalignment (Cyclo)vertical
Eye movement problems in adults 07/12/2015 A. Dahlmann-Noor Dr med PhD FRCOphth FRCS(Ed) DipMedEd Consultant Ophthalmologist Clinical Trials Lead Paediatric Ophthalmology Horizontal misalignment (Cyclo)vertical
 THE EYES IN CHARGE: FOR THE OPHTHALMOLOGIST Roberta A. Pagon, M.D. Division of Medical Genetics, CH-25, Children's Hospital /Medical Center, Box C5371, Seattle, WA 98105-0371 bpagon@u.washington.edu (206)
THE EYES IN CHARGE: FOR THE OPHTHALMOLOGIST Roberta A. Pagon, M.D. Division of Medical Genetics, CH-25, Children's Hospital /Medical Center, Box C5371, Seattle, WA 98105-0371 bpagon@u.washington.edu (206)
Management Approach to Isolated Ocular Motor Nerve Palsies
 Management Approach to Isolated Ocular Motor Nerve Palsies Alfredo A. Sadun, MD, PhD Thornton Professor of Vision Doheny Eye Institute Departments of Ophthalmology and Neurosurgery Keck/USC School of Medicine
Management Approach to Isolated Ocular Motor Nerve Palsies Alfredo A. Sadun, MD, PhD Thornton Professor of Vision Doheny Eye Institute Departments of Ophthalmology and Neurosurgery Keck/USC School of Medicine
F r e q u e n t l y A s k e d Q u e s t i o n s
 Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Basic Cranial Nerve Examination
 Basic Cranial Nerve Examination WIPE Wash hands Introduce yourself Permission Position (Patient sitting facing you, maintain comparable eye level) Exposure (Face exposed only, i.e. remove hats etc) Identify
Basic Cranial Nerve Examination WIPE Wash hands Introduce yourself Permission Position (Patient sitting facing you, maintain comparable eye level) Exposure (Face exposed only, i.e. remove hats etc) Identify
Thyroid eye disease (TED)
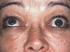 Thyroid eye disease (TED) Mr David H Verity, MD MA FRCOphth Consultant Ophthalmic Surgeon Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy This information leaflet
Thyroid eye disease (TED) Mr David H Verity, MD MA FRCOphth Consultant Ophthalmic Surgeon Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy This information leaflet
NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only)
 PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only) 1. What is the main problem that you are having? (If additional space is required, please use the back of this
PAGE 1 NEURO-OPHTHALMIC QUESTIONNAIRE NAME: AGE: DATE OF EXAM: CHART #: (Office Use Only) 1. What is the main problem that you are having? (If additional space is required, please use the back of this
Common visual symptoms and findings in MS: Clues and Identification
 Common visual symptoms and findings in MS: Clues and Identification Teresa C Frohman, PA-C, MSCS Neuro-ophthalmology Research Manager, UT Southwestern Medical Center at Dallas Professor Biomedical Engineering,
Common visual symptoms and findings in MS: Clues and Identification Teresa C Frohman, PA-C, MSCS Neuro-ophthalmology Research Manager, UT Southwestern Medical Center at Dallas Professor Biomedical Engineering,
Guideline for the Management of Acute Peripheral Facial nerve palsy. Bells Palsy in Children
 Guideline for the Management of Acute Peripheral Facial nerve palsy Definition Bells Palsy in Children Bell palsy is an acute, idiopathic unilateral lower motor neurone facial nerve palsy that is not associated
Guideline for the Management of Acute Peripheral Facial nerve palsy Definition Bells Palsy in Children Bell palsy is an acute, idiopathic unilateral lower motor neurone facial nerve palsy that is not associated
Thyroid eye disease (TED) Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy
 Thyroid eye disease (TED) Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy This information leaflet briefly covers the following issues in TED: What is TED? When
Thyroid eye disease (TED) Synonyms: Graves ophthalmopathy, thyroid ophthalmopathy, thyroid associated ophthalmopathy This information leaflet briefly covers the following issues in TED: What is TED? When
Disclosure Statement. I have no financial interest in any of material presented today
 The eyes have it PEARLS IN EVALUATION, TREATMENT, AND REFERRAL OF PEDIATRIC OCULAR CONDITIONS AND TRAUMA MICHAEL G. HUNT, MD PEDIATRIC EYE SPECIALISTS, LLP Disclosure Statement I have no financial interest
The eyes have it PEARLS IN EVALUATION, TREATMENT, AND REFERRAL OF PEDIATRIC OCULAR CONDITIONS AND TRAUMA MICHAEL G. HUNT, MD PEDIATRIC EYE SPECIALISTS, LLP Disclosure Statement I have no financial interest
Thyroid Eye Disease (TED)
 Manchester Royal Eye Hospital Thyroid Eye Disease (TED) Information For Patients 2 What is Thyroid Eye Disease (TED)? The thyroid gland is located in the neck and produces a hormone that helps regulate
Manchester Royal Eye Hospital Thyroid Eye Disease (TED) Information For Patients 2 What is Thyroid Eye Disease (TED)? The thyroid gland is located in the neck and produces a hormone that helps regulate
Exotropias: A Brief Review. Leila M. Khazaeni, MD November 2, 2008
 Exotropias: A Brief Review Leila M. Khazaeni, MD November 2, 2008 Exotropia Myths Myth #1 He/she will grow out of it FALSE 75% of XTs show progression over a 3 year period Myth #2 The only treatment choice
Exotropias: A Brief Review Leila M. Khazaeni, MD November 2, 2008 Exotropia Myths Myth #1 He/she will grow out of it FALSE 75% of XTs show progression over a 3 year period Myth #2 The only treatment choice
REPORT TO THE STATEWIDE OPHTHALMOLOGY SERVICE (SOS) OF THE GREATER METROPOLITAN CLINICAL TASKFORCE (GMCT)
 REPORT TO THE STATEWIDE OPHTHALMOLOGY SERVICE (SOS) OF THE GREATER METROPOLITAN CLINICAL TASKFORCE (GMCT) The Orthoptist and the management of visual problems in inpatients with stroke: A pilot study to
REPORT TO THE STATEWIDE OPHTHALMOLOGY SERVICE (SOS) OF THE GREATER METROPOLITAN CLINICAL TASKFORCE (GMCT) The Orthoptist and the management of visual problems in inpatients with stroke: A pilot study to
Vision and Rehabilitation After Brain Trauma Eric Singman, MD, PhD, Health.mil
 Vision and Rehabilitation After Brain Trauma Eric Singman, MD, PhD, Health.mil This article was first accessed at Brainline.org. Vision Problems After Brain Injury Visual problems following brain trauma
Vision and Rehabilitation After Brain Trauma Eric Singman, MD, PhD, Health.mil This article was first accessed at Brainline.org. Vision Problems After Brain Injury Visual problems following brain trauma
Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy
 Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy Emily S. Birkholz, MD, and Michael Wall, MD December 30, 2009 CC: 44 year old male with diplopia HPI: This 44 year old man with a history
Pseudoabducens palsy: When a VI nerve palsy is not a VI nerve palsy Emily S. Birkholz, MD, and Michael Wall, MD December 30, 2009 CC: 44 year old male with diplopia HPI: This 44 year old man with a history
Playing it safe: Hints to avoid a claim Presentation to University of Melbourne Students
 Playing it safe: Hints to avoid a claim Presentation to University of Melbourne Students Disclaimer: The information in this presentation is general information relating to legal and/or clinical issues
Playing it safe: Hints to avoid a claim Presentation to University of Melbourne Students Disclaimer: The information in this presentation is general information relating to legal and/or clinical issues
Squints (Strabismus)
 Squints (Strabismus) Squints (Strabismus) What is a squint (strabismus)? A squint or strabismus is present when the two eyes are not looking in the same direction. It may be apparent all the time or only
Squints (Strabismus) Squints (Strabismus) What is a squint (strabismus)? A squint or strabismus is present when the two eyes are not looking in the same direction. It may be apparent all the time or only
Squints and squint surgery/ophthalmology/sdhcnhsft/ 06.13/Review date 06.15. Squints and Squint Surgery
 Squints and squint surgery/ophthalmology/sdhcnhsft/ 06.13/Review date 06.15 Squints and Squint Surgery Chapter 1 Chapter 2 Chapter 3 Chapter 4 Chapter 5 Chapter 6 Squints and squint surgery Your Outpatient
Squints and squint surgery/ophthalmology/sdhcnhsft/ 06.13/Review date 06.15 Squints and Squint Surgery Chapter 1 Chapter 2 Chapter 3 Chapter 4 Chapter 5 Chapter 6 Squints and squint surgery Your Outpatient
Information for adults undergoing squint surgery
 Information for adults undergoing squint surgery Ophthalmology Department Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information for adults undergoing squint surgery Ophthalmology Department Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
MODERN CLINICAL OPTOMETRY BILLING & CODING THE MEDICAL EYE EXAMINATION. Definitions of Eye Examinations. Federal Government Definition
 MODERN CLINICAL OPTOMETRY BILLING & CODING THE MEDICAL EYE EXAMINATION Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com Definitions of Eye Examinations Optometry
MODERN CLINICAL OPTOMETRY BILLING & CODING THE MEDICAL EYE EXAMINATION Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com Definitions of Eye Examinations Optometry
Physical and Mental Conditions Guidelines VISION CONDITIONS AND ACTIONS Page 5.4
 Physical and Mental Conditions Guidelines VISION CONDITIONS AND ACTIONS Page 5.4 AMBLYOPIA (Lazy Eye) A reduction in the acuteness of vision without apparent eye disease. This condition cannot be entirely
Physical and Mental Conditions Guidelines VISION CONDITIONS AND ACTIONS Page 5.4 AMBLYOPIA (Lazy Eye) A reduction in the acuteness of vision without apparent eye disease. This condition cannot be entirely
Doctor, I See Double : Managing Cranial Nerve Palsies
 1 Doctor, I See Double : Managing Cranial Nerve Palsies Joseph W. Sowka, OD, FAAO, Diplomate Professor of Optometry Nova Southeastern University, College of Optometry 3200 South University Drive Fort Lauderdale,
1 Doctor, I See Double : Managing Cranial Nerve Palsies Joseph W. Sowka, OD, FAAO, Diplomate Professor of Optometry Nova Southeastern University, College of Optometry 3200 South University Drive Fort Lauderdale,
ADJUSTABLE SQUINT SURGERY
 ADJUSTABLE SQUINT SURGERY Information Leaflet Your Health. Our Priority. Page 2 of 8 Introduction Adjustable squint surgery is an alternative to traditional squint surgery. It has a better success rate
ADJUSTABLE SQUINT SURGERY Information Leaflet Your Health. Our Priority. Page 2 of 8 Introduction Adjustable squint surgery is an alternative to traditional squint surgery. It has a better success rate
Ptosis. Patient Information - Adnexal
 Patient Information - Adnexal Ptosis What is ptosis? Ptosis is the medical name for the drooping of the upper eyelid, which can happen in one or both eyes. A low upper lid can interfere with vision by
Patient Information - Adnexal Ptosis What is ptosis? Ptosis is the medical name for the drooping of the upper eyelid, which can happen in one or both eyes. A low upper lid can interfere with vision by
DIPLOPIA - DON T PANIC (JUST PUT ON YOUR THINKING CAP)
 DIPLOPIA - DON T PANIC (JUST PUT ON YOUR THINKING CAP) Lisa Rovick, CO, COMT This article and accompanying quiz are worth.5 JCAHPO Group A continuing education credit. CONTINUING EDUCATION CREDITS ARE
DIPLOPIA - DON T PANIC (JUST PUT ON YOUR THINKING CAP) Lisa Rovick, CO, COMT This article and accompanying quiz are worth.5 JCAHPO Group A continuing education credit. CONTINUING EDUCATION CREDITS ARE
To: all optometrists and billing staff
 Number: Opto 27 Date: September 29, 2011 Page: 1 of 1 Subject: Schedule of Optometric Benefits amendments October 1, 2011/New explanatory code list Reference: Schedule of Optometric Benefits To: all optometrists
Number: Opto 27 Date: September 29, 2011 Page: 1 of 1 Subject: Schedule of Optometric Benefits amendments October 1, 2011/New explanatory code list Reference: Schedule of Optometric Benefits To: all optometrists
Guide to Eye Surgery and Eye-related Claims
 If you or a loved one have suffered because of a negligent error during eye treatment or surgery, you may be worried about how you will manage in the future, particularly if your eyesight has been made
If you or a loved one have suffered because of a negligent error during eye treatment or surgery, you may be worried about how you will manage in the future, particularly if your eyesight has been made
Guide to Claims against General Practitioners (GPs)
 Patients often build up a relationship of trust with their GP over a number of years. It can be devastating when a GP fails in his or her duty to a patient. Our medical negligence solicitors understand
Patients often build up a relationship of trust with their GP over a number of years. It can be devastating when a GP fails in his or her duty to a patient. Our medical negligence solicitors understand
Pediatric Eye Problems When do I refer? Hillary Onan, M.D. Eye Associates of Central Texas Dell Children s Medical Center of Central Texas
 Pediatric Eye Problems When do I refer? Hillary Onan, M.D. Eye Associates of Central Texas Dell Children s Medical Center of Central Texas Red Reflex Testing Check RR at every well child visit until child
Pediatric Eye Problems When do I refer? Hillary Onan, M.D. Eye Associates of Central Texas Dell Children s Medical Center of Central Texas Red Reflex Testing Check RR at every well child visit until child
Corporate Medical Policy Reconstructive Eyelid Surgery and Brow Lift
 Corporate Medical Policy Reconstructive Eyelid Surgery and Brow Lift File Name: Origination: Last CAP Review: Next CAP Review: Last Review: reconstructive_eyelid_surgery_and_brow_lift 1/2000 9/2015 9/2016
Corporate Medical Policy Reconstructive Eyelid Surgery and Brow Lift File Name: Origination: Last CAP Review: Next CAP Review: Last Review: reconstructive_eyelid_surgery_and_brow_lift 1/2000 9/2015 9/2016
Keeping Your Eyes Healthy after Treatment for Childhood Cancer
 Keeping Your Eyes Healthy after Treatment for Childhood Cancer High doses of radiation to the brain, eye, or eye socket (orbit) during treatment for childhood cancer can have a long-lasting affect on the
Keeping Your Eyes Healthy after Treatment for Childhood Cancer High doses of radiation to the brain, eye, or eye socket (orbit) during treatment for childhood cancer can have a long-lasting affect on the
Descemet s Stripping Endothelial Keratoplasty (DSEK)
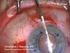 Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Understanding posterior vitreous detachment
 Understanding posterior vitreous detachment About posterior vitreous detachment Causes of PVD Symptoms and diagnosis Treatment PVD and other eye conditions Coping Useful contacts About posterior vitreous
Understanding posterior vitreous detachment About posterior vitreous detachment Causes of PVD Symptoms and diagnosis Treatment PVD and other eye conditions Coping Useful contacts About posterior vitreous
Cerebral Palsy and Visual Impairment
 CP Factsheet Cerebral Palsy and Visual Impairment Although cerebral palsy mainly causes difficulty with movement, other conditions may also occur. This is because other parts of the brain may also be affected
CP Factsheet Cerebral Palsy and Visual Impairment Although cerebral palsy mainly causes difficulty with movement, other conditions may also occur. This is because other parts of the brain may also be affected
Graduate Diploma in Optometry. Related modules Pre-requisites Satisfying requirements of second year BSc (Hons) Optometry examination board
 Posterior Eye & General Ophthalmology School and subject group Module code Module title Module type Module replaces (where appropriate) Life and Health Sciences / Optometry OP3PEG Posterior Eye & General
Posterior Eye & General Ophthalmology School and subject group Module code Module title Module type Module replaces (where appropriate) Life and Health Sciences / Optometry OP3PEG Posterior Eye & General
PUPILS AND NEAR VISION. Akilesh Gokul PhD Research Fellow Department of Ophthalmology
 PUPILS AND NEAR VISION Akilesh Gokul PhD Research Fellow Department of Ophthalmology Iris Anatomy Two muscles: Radially oriented dilator (actually a myo-epithelium) - like the spokes of a wagon wheel Sphincter/constrictor
PUPILS AND NEAR VISION Akilesh Gokul PhD Research Fellow Department of Ophthalmology Iris Anatomy Two muscles: Radially oriented dilator (actually a myo-epithelium) - like the spokes of a wagon wheel Sphincter/constrictor
Explanation of the Procedure
 Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
Squint surgery in adults
 Patient Information Strabismus service Squint surgery in adults This leaflet aims to answer some of the questions you may have about squint surgery. The leaflet does not cover everything as every patient
Patient Information Strabismus service Squint surgery in adults This leaflet aims to answer some of the questions you may have about squint surgery. The leaflet does not cover everything as every patient
IMAGE ASSISTANT: OPHTHALMOLOGY
 IMAGE ASSISTANT: OPHTHALMOLOGY Summary: The Image Assistant has been developed to provide medical doctors with a software tool to search, display, edit and use medical illustrations of their own specialty,
IMAGE ASSISTANT: OPHTHALMOLOGY Summary: The Image Assistant has been developed to provide medical doctors with a software tool to search, display, edit and use medical illustrations of their own specialty,
Thymus Cancer. This reference summary will help you better understand what thymus cancer is and what treatment options are available.
 Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
James H. Hall Eye Center
 James H. Hall Eye Center Established in 1979 Annual Activity Report September, 2010 to September, 2011 COMMUNITY CARE STATISTICS Served 2,000 patients including pre and post-operative visits Our physicians
James H. Hall Eye Center Established in 1979 Annual Activity Report September, 2010 to September, 2011 COMMUNITY CARE STATISTICS Served 2,000 patients including pre and post-operative visits Our physicians
Neuro-Ophthalmology. Bascom Palmer s clinical detectives study the links between brain and eye. The super sleuths of vision. 2Neuro-Ophthalmology
 2Neuro-Ophthalmology The super sleuths of vision Neuro-Ophthalmology Bascom Palmer s clinical detectives study the links between brain and eye When Miguel Cabrera became concerned about a drooping eyelid
2Neuro-Ophthalmology The super sleuths of vision Neuro-Ophthalmology Bascom Palmer s clinical detectives study the links between brain and eye When Miguel Cabrera became concerned about a drooping eyelid
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
PATIENT INFORMATION BOOKLET
 (060110) VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE ( BY DR. ISAAC LIPSHITZ ) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL END-STAGE AGE-RELATED MACULAR
(060110) VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE ( BY DR. ISAAC LIPSHITZ ) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL END-STAGE AGE-RELATED MACULAR
UAMS / CAVHS Adult Neurology Neuro-Ophthalmology Curriculum 6/13/08
 UAMS / CAVHS Adult Neurology Neuro-Ophthalmology Curriculum 6/13/08 Summary Description of Rotation The adult neurology neuro-ophthalmology rotation is an extremely important rotation for 1 month during
UAMS / CAVHS Adult Neurology Neuro-Ophthalmology Curriculum 6/13/08 Summary Description of Rotation The adult neurology neuro-ophthalmology rotation is an extremely important rotation for 1 month during
IntraLase and LASIK: Risks and Complications
 No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
ORANGE COUNTY EYE INSTITUTE
 ORANGE COUNTY EYE INSTITUTE *Note: It is the patient s responsibility to file insurance claims if we are not contracted with your insurance company. *Note: Be aware that most medical insurance plans do
ORANGE COUNTY EYE INSTITUTE *Note: It is the patient s responsibility to file insurance claims if we are not contracted with your insurance company. *Note: Be aware that most medical insurance plans do
Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical,
 sight see OLYMPIA EYE & LASER CENTRE Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical, At the Olympia Eye & Laser Centre, our vision is to improve
sight see OLYMPIA EYE & LASER CENTRE Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical, At the Olympia Eye & Laser Centre, our vision is to improve
Getting Ready for ICD-10. Dianna Hoskins, OCS Cincinnati Eye Institute
 Dianna Hoskins, OCS Cincinnati Eye Institute Chart Documentation: Will your documentation stand up to ICD-10? Do you always mark which eye, severity or status of the disease (chronic or acute), site, etiology
Dianna Hoskins, OCS Cincinnati Eye Institute Chart Documentation: Will your documentation stand up to ICD-10? Do you always mark which eye, severity or status of the disease (chronic or acute), site, etiology
Alexandria Fairfax Sterling Leesburg 703-931-9100 703-573-8080 703-430-4400 703-858-3170
 DIABETIC RETINOPATHY www.theeyecenter.com This pamphlet has been written to help people with diabetic retinopathy and their families and friends better understand the disease. It describes the cause, symptoms,
DIABETIC RETINOPATHY www.theeyecenter.com This pamphlet has been written to help people with diabetic retinopathy and their families and friends better understand the disease. It describes the cause, symptoms,
a guide to understanding facial palsy a publication of children s craniofacial association
 a guide to understanding facial palsy a publication of children s craniofacial association a guide to understanding facial palsy this parent s guide to facial palsy is designed to answer questions that
a guide to understanding facial palsy a publication of children s craniofacial association a guide to understanding facial palsy this parent s guide to facial palsy is designed to answer questions that
Patient Information Cataract surgery
 Patient Information Cataract surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Patient Information Cataract surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Trauma Insurance Claims Seminar Invitation
 Trauma Insurance Claims Seminar Invitation Introduction Since the development of Trauma Insurance in Australia in the 1980s, the product has evolved at a great pace. Some of the challenges faced by claims
Trauma Insurance Claims Seminar Invitation Introduction Since the development of Trauma Insurance in Australia in the 1980s, the product has evolved at a great pace. Some of the challenges faced by claims
Patient information factsheet. Cataract surgery. Consent for cataract surgery
 Patient information factsheet Cataract surgery Consent for cataract surgery This leaflet gives you information that will help you decide whether to have cataract surgery. You might want to discuss it with
Patient information factsheet Cataract surgery Consent for cataract surgery This leaflet gives you information that will help you decide whether to have cataract surgery. You might want to discuss it with
How To Treat Eye Problems With A Laser
 1550 Oak St., Suite 5 1515 Oak St., St Eugene, OR 97401 Eugene, OR 97401 (541) 687-2110 (541) 344-2010 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information is to help you make an informed
1550 Oak St., Suite 5 1515 Oak St., St Eugene, OR 97401 Eugene, OR 97401 (541) 687-2110 (541) 344-2010 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information is to help you make an informed
Facts about diabetic macular oedema
 Patient information medical retina services Facts about diabetic macular oedema What is diabetic macular oedema? Diabetic eye disease is a leading cause of blindness registration among working age adults
Patient information medical retina services Facts about diabetic macular oedema What is diabetic macular oedema? Diabetic eye disease is a leading cause of blindness registration among working age adults
MS Learn Online Feature Presentation Managing Symptoms: Vision Nancy Holland, Ed.D, RN, MSCN. Tom>> Welcome to MS Learn Online, I m Tom Kimball
 Page 1 MS Learn Online Feature Presentation Managing Symptoms: Vision Nancy Holland, Ed.D, RN, MSCN Tom>> Welcome to MS Learn Online, I m Tom Kimball Tracey>> And I m Tracey Kimball. People living with
Page 1 MS Learn Online Feature Presentation Managing Symptoms: Vision Nancy Holland, Ed.D, RN, MSCN Tom>> Welcome to MS Learn Online, I m Tom Kimball Tracey>> And I m Tracey Kimball. People living with
Marketing Samples Medical Optometry
 Marketing Samples Medical Optometry Intended Use The purpose of this marketing sample packet is to provide examples of the ways your practice can implement text for newsletters, emails or letters, on-hold
Marketing Samples Medical Optometry Intended Use The purpose of this marketing sample packet is to provide examples of the ways your practice can implement text for newsletters, emails or letters, on-hold
Eye Surgery PROCEDURAL CONSENT FORM
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v5.00-06/2011 SW9441 Facility: A. Interpreter
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v5.00-06/2011 SW9441 Facility: A. Interpreter
Tucson Eye Care, PC. Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens
 Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Squints and Squint Surgery
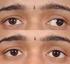 Squints and Squint Surgery Chapter 1 Chapter 2 Chapter 3 Chapter 4 Chapter 5 Chapter 6 Squints and squint surgery Your Outpatient appointments Consenting for your operation The day of your operation After
Squints and Squint Surgery Chapter 1 Chapter 2 Chapter 3 Chapter 4 Chapter 5 Chapter 6 Squints and squint surgery Your Outpatient appointments Consenting for your operation The day of your operation After
Eye Diseases. 1995-2014, The Patient Education Institute, Inc. www.x-plain.com otf30101 Last reviewed: 05/21/2014 1
 Eye Diseases Introduction Some eye problems are minor and fleeting. But some lead to a permanent loss of vision. There are many diseases that can affect the eyes. The symptoms of eye diseases vary widely,
Eye Diseases Introduction Some eye problems are minor and fleeting. But some lead to a permanent loss of vision. There are many diseases that can affect the eyes. The symptoms of eye diseases vary widely,
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK)
 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding Photorefractive Keratectomy (PRK)
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding Photorefractive Keratectomy (PRK)
Eye and Vision Care in the Patient-Centered Medical Home
 1505 Prince Street, Alexandria, VA 22314 (703) 739-9200200 FAX: (703) 739-9497494 Eye and Vision Care in the Patient-Centered Medical Home The Patient Centered Medical Home (PCMH) is an approach to providing
1505 Prince Street, Alexandria, VA 22314 (703) 739-9200200 FAX: (703) 739-9497494 Eye and Vision Care in the Patient-Centered Medical Home The Patient Centered Medical Home (PCMH) is an approach to providing
Background on Brain Injury
 CHAPTER 1 Background on Brain Injury In this chapter, you will: Read about Alberta s definition of Acquired Brain Injury and how that affects which supports you will be able to access. Learn about the
CHAPTER 1 Background on Brain Injury In this chapter, you will: Read about Alberta s definition of Acquired Brain Injury and how that affects which supports you will be able to access. Learn about the
Program Requirements for Fellowship Education in Neuro- Ophthalmology
 Program Requirements for Fellowship Education in Neuro- Ophthalmology [M] = Must have / required [S] = Should have I. Introduction A. Definition and Scope of Neuro ophthalmology Neuro ophthalmology is
Program Requirements for Fellowship Education in Neuro- Ophthalmology [M] = Must have / required [S] = Should have I. Introduction A. Definition and Scope of Neuro ophthalmology Neuro ophthalmology is
Oculopharyngeal muscular dystrophy (OPMD)
 Oculopharyngeal muscular dystrophy (OPMD) The term muscular dystrophy is used to cover a wide range of conditions which have in common progressive muscle weakness due to an inherited genetic defect (mutation).
Oculopharyngeal muscular dystrophy (OPMD) The term muscular dystrophy is used to cover a wide range of conditions which have in common progressive muscle weakness due to an inherited genetic defect (mutation).
Information for patients attending appointments at King s College Hospital only
 Ambulatory Care & Local Networks Laser iridotomy Information for patients attending appointments at King s College Hospital only This leaflet answers some of the questions you may have about having laser
Ambulatory Care & Local Networks Laser iridotomy Information for patients attending appointments at King s College Hospital only This leaflet answers some of the questions you may have about having laser
www.australiandoctor.com.au COMPLETE HOW TO TREAT QUIZZES ONLINE (www.australiandoctor.com.au/cpd) to earn CPD or PDP points.
 HowtoTreat PULL-OUT SECTION www.australiandoctor.com.au COMPLETE HOW TO TREAT QUIZZES ONLINE (www.australiandoctor.com.au/cpd) to earn CPD or PDP points. inside Childhood Assessing the child with possible
HowtoTreat PULL-OUT SECTION www.australiandoctor.com.au COMPLETE HOW TO TREAT QUIZZES ONLINE (www.australiandoctor.com.au/cpd) to earn CPD or PDP points. inside Childhood Assessing the child with possible
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Complications of Strabismus Surgery
 Complications of Strabismus Surgery Tjeerd de Faber, Martha Tjon Rutger van Ruyven Alexis Damanakis Ondercorrectie Overcorrectie Wat vind je erger? 1 DELLEN Corneal dellen are small areas of thinning associated
Complications of Strabismus Surgery Tjeerd de Faber, Martha Tjon Rutger van Ruyven Alexis Damanakis Ondercorrectie Overcorrectie Wat vind je erger? 1 DELLEN Corneal dellen are small areas of thinning associated
About MS. An introduction to. An introduction to multiple sclerosis for people who have recently been diagnosed. What is MS? Is it common?
 An introduction to multiple sclerosis for people who have recently been diagnosed When you have just been diagnosed with multiple sclerosis, you will probably have many questions about the condition and
An introduction to multiple sclerosis for people who have recently been diagnosed When you have just been diagnosed with multiple sclerosis, you will probably have many questions about the condition and
Eye Associates Custom LASIK With IntraLASIK Correction Of Nearsightedness, Farsightedness, and Astigmatism Using IntraLase TM Technology
 Eye Associates Custom LASIK With IntraLASIK Correction Of Nearsightedness, Farsightedness, and Astigmatism Using IntraLase TM Technology INDICATIONS AND PROCEDURE This information is being provided to
Eye Associates Custom LASIK With IntraLASIK Correction Of Nearsightedness, Farsightedness, and Astigmatism Using IntraLase TM Technology INDICATIONS AND PROCEDURE This information is being provided to
Cataracts. Cataract and Primary Eye Care Service...215-928-3041. Main Number...215-928-3000. Physician Referral...1-877-AT-WILLS 1-877-289-4557
 Main Number...215-928-3000 Physician Referral...1-877-AT-WILLS 1-877-289-4557 Emergency Service...215-503-8080 Cataract and Primary Eye Care Service...215-928-3041 Retina Service... 215-928-3300 Cataract
Main Number...215-928-3000 Physician Referral...1-877-AT-WILLS 1-877-289-4557 Emergency Service...215-503-8080 Cataract and Primary Eye Care Service...215-928-3041 Retina Service... 215-928-3300 Cataract
Cataract and Cataract Surgery
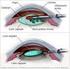 What is a cataract? A cataract is a cloudy area in the lens of your eye. The lens is located just behind the iris (coloured part of the eye). The lens helps to focus light entering the eye to give a clear
What is a cataract? A cataract is a cloudy area in the lens of your eye. The lens is located just behind the iris (coloured part of the eye). The lens helps to focus light entering the eye to give a clear
sound or ringing in the ears.
 (Idiopathic Intracranial Hypertension) Sashank Prasad, MD www.brighamandwomens.org/neuro-ophthalmology A Patient s Guide Symptoms Diagnosis Treatment Prognosis Symptoms The symptoms of include: Headaches
(Idiopathic Intracranial Hypertension) Sashank Prasad, MD www.brighamandwomens.org/neuro-ophthalmology A Patient s Guide Symptoms Diagnosis Treatment Prognosis Symptoms The symptoms of include: Headaches
Paediatric Bell s Palsy Paediatric Update November 2014
 Paediatric Bell s Palsy Paediatric Update November 2014 Richard Webster, Paediatric Neurologist Children s Hospital at Westmead Typical history Unilateral LMN facial weakness Acute onset over a day or
Paediatric Bell s Palsy Paediatric Update November 2014 Richard Webster, Paediatric Neurologist Children s Hospital at Westmead Typical history Unilateral LMN facial weakness Acute onset over a day or
Outcome of Surgery for Bilateral Third Nerve Palsy
 CLINICAL INVESTIGATIONS Outcome of Surgery for Bilateral Third Nerve Palsy Kazuhiro Aoki, Tatsushi Sakaue, Nobue Kubota and Toshio Maruo Department of Ophthalmology, Teikyo University School of Medicine,
CLINICAL INVESTIGATIONS Outcome of Surgery for Bilateral Third Nerve Palsy Kazuhiro Aoki, Tatsushi Sakaue, Nobue Kubota and Toshio Maruo Department of Ophthalmology, Teikyo University School of Medicine,
There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition?
 There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition? Dry eye can be a temporary or chronic condition and occurs when the eye does not produce tears properly,
There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition? Dry eye can be a temporary or chronic condition and occurs when the eye does not produce tears properly,
VISION REHABILITATION QUESTIONNAIRE
 VISION REHABILITATION QUESTIONNAIRE Please fill out this questionnaire carefully. Please return it to our office 1 week prior to your appointment. THANK YOU. Appointment: Day Date Time Patient s Name:
VISION REHABILITATION QUESTIONNAIRE Please fill out this questionnaire carefully. Please return it to our office 1 week prior to your appointment. THANK YOU. Appointment: Day Date Time Patient s Name:
(Please fill this out to the best of your ability) Baker Eye Institute Conway, Arkansas 501-329-3937 NAME: Today s Date:
 Page 1 of 5 (Please fill this out to the best of your ability) Baker Eye Institute Conway, Arkansas 501-329-3937 NAME: Age: What is the main reason for today s visit? Today s Date: Who referred you to
Page 1 of 5 (Please fill this out to the best of your ability) Baker Eye Institute Conway, Arkansas 501-329-3937 NAME: Age: What is the main reason for today s visit? Today s Date: Who referred you to
CONSENT FORM. Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
Blepharoplasty - Eyelid Surgery
 Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
EYE AND VISION ASSESSMENT IN PRIMARY HEALTH CARE
 EYE AND VISION ASSESSMENT IN PRIMARY HEALTH CARE Primary Health Care (PHC) professionals in Aboriginal and Torres Strait Islander health services perform basic eye and vision checks as part of routine
EYE AND VISION ASSESSMENT IN PRIMARY HEALTH CARE Primary Health Care (PHC) professionals in Aboriginal and Torres Strait Islander health services perform basic eye and vision checks as part of routine
Ptosis. Ptosis and Pupils. Ptosis. Palpebral fissure. Blepharospasm. Blepharospasm or ptosis? Bilateral, longstanding, familial: Palpebral fissure
 Ptosis and Pupils Ptosis Jack CF Chong, MS, MD 99/03/06 Ptosis Bilateral, longstanding, familial: CPEO (chronic progressive external ophthalmoplegia) D/D: Acute, recent, unilateral Palpebral fissure Palpebral
Ptosis and Pupils Ptosis Jack CF Chong, MS, MD 99/03/06 Ptosis Bilateral, longstanding, familial: CPEO (chronic progressive external ophthalmoplegia) D/D: Acute, recent, unilateral Palpebral fissure Palpebral

![Bell s Palsy ]]> <![CDATA[Bell's Palsy]]> Bell s Palsy ]]> <![CDATA[Bell's Palsy]]>](/thumbs/27/10105461.jpg)