Early evaluation of an electromechanical morcellator for laparoscopic supracervical hysterectomy
|
|
|
- Russell Long
- 10 years ago
- Views:
Transcription
1 Early evaluation of an electromechanical morcellator for laparoscopic supracervical hysterectomy James F. Daniell, 1 Calvin Channell, 1 James Lindsay, 1 Stephen Staggs 1 and Traci Henry 2 1 Department of Obstetrics and Gynecology, Centennial Medical Center, Nashville, Tennessee, USA, 2 Vanderbilt University School of Nursing, Nashville, Tennessee, USA Keywords electromechanical morcellator, hysterectomy, laparoscopic, supracervical. Correspondence J. F. Daniell, 2222 State Street, Suite A, Nashville, TN 37203, USA. Accepted for publication 21 July 1998 ABSTRACT Objective To evaluate the effectiveness, safety, and cost effectiveness of electromechanical morcellation of the uterus and adnexae to enhance laparoscopic supracervical hysterectomy (LSH). Design 41 consecutive LSH procedures with and without adnectomy were reviewed. An electromechanical morcellator was used in each procedure to accomplish laparoscopic removal of the uterus and adnexae. Setting A private gynaecological practice in a full service hospital. Interventions LSH. Results The mean uterine weight was 146 g ( g). The mean operating time was 94 min ( min). The time for morcellation was available in 19 cases by reviewing videotape; the average morcellation time was 11.8 min (4 23 min). Average blood loss was 125 ml ( ml), with one case of late postoperative bleeding requiring operative intervention. The average cost for the procedure was $7998 ($6989 $11 581). All patients were discharged within 48 h of the time of admission, and 36 patients were discharged within 23 h from the time of admission. Conclusions LSH is a safe and effective method of managing patients who lack cervical pathology or pelvic relaxation. Electromechanical morcellation can enhance the performance of LSH by decreasing operating time. INTRODUCTION All variations of laparoscopic hysterectomy (LH) have been much discussed since it was first reported by Reich et al. in One particularly controversial form of LH is laparoscopic supracervical (or subtotal) hysterectomy (LSH). LSH was first described by Semm. 2 Since that report, several authors have reported their initial experience with various methods for LSH. 3 7 One recent report from Belgium has also reviewed 500 cases of LSH. 8 A recent clinical commentary by Munro discussed the pros and cons of LSH in an editorial entitled Supracervical hysterectomy: a time for reappraisal. 9 Lalonde & Daniell have recently reported on our initial experience with laparoscopic subtotal hysterectomy. 10 In this article, we report our initial experiences with an electromechanical morcellator designed for laparoscopy. We also describe and discuss in detail our other modifications of LSH; we feel that these simplify the procedure and reduce operating time and intraoperative and postoperative complications. MATERIALS AND METHODS We reviewed 41 consecutive proecedures of laparoscopic subtotal hysterectomy, performed by our group in Nashville from January 1996 through January All operations were performed by the senior author (JFD) with the assistance of one of the co-authors. The office records and hospital charts for these 41 women were reviewed to determine indications, clinical parameters, operating times, blood loss, length of 1998 Blackwell Science Ltd Gynaecological Endoscopy ,
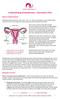
2 296 J. F. DANIELL et al. hospitalization, and complications. All patients were interviewed after at least 6 weeks following discharge from the hospital. Pathology reports were reviewed to obtain uterine weights and final pathological diagnosis. From January 1996, when we began to use the electromechanical surgical morcellator (Karl Storz Endoscopy, Culver City, California, USA), operations were monitored for both total operating times and the actual time necessary for laparoscopic morcellation and removal of the fundus of the uterus and/or adnexae. In 19 cases real-time videotapes were available for review and analysis so that exact operating and morcellation times could be obtained for accurate reporting. Findings in these 41 patients were then compared with those from 20 previous patients who had undergone LSH, carried out by JFD, without the morcellator, between January 1993 and December Patient selection All women underwent preoperative approval, through their insurance carriers, for hysterectomy and none were deemed inappropriate candidates for surgery. Postoperatively, when hospital tissue review committees reviewed the charts, no procedures were considered to be unindicated. All patients were either private patients of the authors, or had been referred to the senior author for consideration specifically for laparoscopic subtotal hysterectomy because of desire for retention of the cervix. The patients were all counselled preoperatively concerning the risks vs. benefits of subtotal hysterectomy with retention of the cervix. The option of supracervical hysterectomy was offered only to patients who had a normal cervix and no history of any abnormal cervical pathology on Papanicolaou smears. Patients with uterine descensus or cervicitis were not offered this procedure. All patients were informed of the need for and consented to lifetime follow-up Papanicolaou smears following surgery. Indications for hysterectomy included symptomatic uterine fibroids, chronic pelvic pain, chronic menometrorrhagia uncorrectable with hormonal therapy, or endometriosis. Preoperative evaluation All patients had a preoperative Papanicolaou smear within 3 months of the scheduled surgery. Patients over 35 had an endometrial biopsy and ultrasound if clinically indicated. Patients were given the opportunity to bank autologous blood prior to surgery, and were pretreated with oral iron prophylactically. Preoperative treatment with GnRH analogues, for 3 months, was given to 10 patients with fibroids and anaemia secondary to menorrhagia. Operative procedure As with our recent clinical practice, we used the most cost-effective methods for LSH whenever possible. Lateral 5-mm ports were used and reusable instruments, including all four trocars and sheaths and reusable scissors and Veress needles, were used in all cases. After general anaesthesia with endotracheal anaesthesia, a pelvic examination was performed to confirm the preoperative findings. A reusable uterine manipulator was placed, using either a polyp forceps taped to a single-toothed tenaculum or, in certain patients with a small uterus, a Hulka tenaculum was inserted. Continuous bladder drainage with a Foley catheter was used intraoperatively. A four-puncture technique was used, with a 10-mm reusable cannula infraumbilically and two lateral 5-mm cannulas laterally in each lower quadrant. These were placed under direct visualization and were placed lateral to the rectus muscle and up out of the pelvis well above the inferior epigastric vessels. This gave a good angle of attack into the pelvis and reduced the risk of bothersome bleeding from the abdominal wall puncture. Another 5-mm reusable cannula was placed suprapubically in the midline approximately 3 cm above the pubic symphysis. A video camera was attached with two videos being made, one edited tape for the patient and one real-time copy of the procedure with sound, which could be reviewed later to monitor the exact time of surgery and morcellation with the electromechanical morcellator. After initial laparoscopic inspection of the pelvis and entire abdomen and an intraoperative phone consultation with the family, the procedure was then commenced. For tissue separation, bipolar coagulation was applied at 50 W with 5-mm instruments. Initially a 5-mm disposable Maryland dissector (Everest Medical, Minneapolis, Minnesota, USA) was used for coagulation and dissection during the LSH with 5-mm reusable scissors for transection. For the last 20 cases, a 5-mm combined coagulating and transecting bipolar forceps (Everest Medical) was used (Fig. 1). With traction and countertraction for adequate exposure, the bipolar coagulating device was used to coagulate and then transect the Gynaecological Endoscopy , Blackwell Science Ltd
3 EARLY EVALUATION OF AN ELECTROMECHANICAL MORCELLATOR 297 Figure 1 Both the pistol grip handle and the distal grasping and cutting tip of the 5-mm bipolar coagulating and cutting multipurpose handle are illustrated here. Application of finger pressure compresses the jaws of the forceps and the thumb is used to advance the cutting blade when indicated. round ligaments, and also the infundibulopelvic (IP) ligaments when the adnexae were being removed. When the adnexae were being retained, the same techniques were used to coagulate and transect the round ligaments, proximal fallopian tubes, and ovarian ligaments. Once the upper portions of the fundus had been separated from its lateral attachments, the anterior cervical uterine junction was identified. We did not dissect the bladder peritoneum off of the anterior portion of the cervix, but merely coagulated the serosa transversely with bipolar coagulation forceps just above the level of the vesicouterine fold. In addition, the main branches of the uterine artery and the ureters were not dissected unless adnexal adhesions required this for adequate exposure and to facilitate removal of the adnexae. After coagulating and transecting the upper portions of the broad ligaments, the ascending branches of the uterine vessels were identified and coagulated using the bipolar coagulating forceps and then cut. At all times, care was taken to identify the main branch of the uterine artery and to be aware that the ureter passes under this visibly pulsing structure. As bipolar coagulation was being used, we were aware that temperatures above 50 centigrade could be reached as far as 1 cm lateral to the edge of any bipolar coagulating device. Thus, we always carefully monitored placement of the tips of the instruments before applying the bipolar energy. We used an amp meter at all times to note when tissue desiccation was completed and when it was thus safe to cut tissue. By using the 5-mm bipolar coagulating multifunction device, we eliminated the problems of cutting with scissors past the tip of the coagulated zone, since the cutting blade could not pass beyond the area of coagulation. Once the ascending branches of the uterine vessels had been coagulated close to the isthmus of the uterus, the uterus would become discoloured from reduced blood supply. Dilute pitressin (20 units diluted in 50 ml of saline) was then injected via a long spinal needle, placed directly through the lower abdominal wall into the anterior uterine fundus to reduce cervical small vessel bleeding with separation of the uterus. This was done with the approval and vigilance of the anesthesiologist because of the potential for bradycardia or hypertension with systemic absorption. Whenever possible, the posterior peritoneum over the back of the lower uterine isthmus was coagulated with the bipolar forceps to mark the intended area for transection of the low posterior fundus. At this point, the lateral third of the isthmus just above the cervical uterine junction was transected using a 50-W cutting current with reusable 5-mm unipolar scissors, incorporating active electrode monitoring via an integrated electrode (Electroscope, Boulder, Colorado, USA) to reduce the potential for accidental electrosurgical injuries, such as capacitive coupling 1998 Blackwell Science Ltd Gynaecological Endoscopy ,
4 298 J. F. DANIELL et al. Figure 2 The Steiner laparoscopic morcellator system consists of a reusable 12-mm sheath and handle and motor-driven rotating power cord. The 10-mm sharp cylinder blade rotates rapidly when the foot control to the power source, seen here, is activated. After transection of both lateral thirds of the isthmus, the uterine manipulating device was removed, but the tenaculum was maintained on the cervix for downward traction. Then with traction and countertraction, the isthmus of the uterus was transected just above the level of the cervical junction, trying to maintain a transverse plane whenever possible. Once the body of the uterus was cut away from the cervix, the cervical stump was coagulated with the bipolar forceps for haemostasis. The endocervical canal was then coagulated by placing the blunt 5-mm coagulating forceps into the cervical canal, making certain the jaws of the forceps were open, and then applying bipolar energy and slowly rotating the forceps so that the entire cervical canal could be thermally coagulated from above with electrosurgery. This was done in the hope of destroying all the endocervical tissue that might lead to later bothersome persistent vaginal spotting. In the past, we have used various methods for transecting the fundus from the cervix, including a bipolar needle, a harmonic scalpel blade, laser energy, blunt scissors, a 5-mm knife, and unipolar electrosurgical energy with scissors. We found that the 5-mm shielded reusable scissors with unipolar current (50 W, cutting blend 1) gave us the most rapid effective transection of the dense cervical tissue. Care was taken to stay just above the level of the cervix when cutting with the scissors, so as not to remove the lateral cervical stroma containing the uterine vessels. Careful coagulation of the exposed ascending branches of the uterine vessels in each lateral cervix was then performed, and any small oozing vessels from the cervical body were coagulated with the bipolar coagulating forceps. At this point, the lower 5-mm suprapubic site was converted to a 12-mm reusable sheath through which the electromechanical morcellator was introduced (Fig. 2). The electromechanical morcellator allows a rapidly circulating sharp 10-mm cylinder to be used for tissue coring with a foot control switch. Through this instrument, the uterus and adnexae were grabbed with a 10-mm claw grasper. The tip of the rotating electromechanical morcellator was always kept close to the trocar sheath in the lower abdominal wall and not allowed to wander into the abdominal cavity. The tissue was pulled up into the jaws of the rotating sharp cylinder, but the cylinder was not pushed inwards. In this fashion, we were able to minimize the potential for intra-abdominal accidents from the sharp rotating blade of the electromechanical morcellator. The long 10-mm cores of tissue were then pulled up out through the 12-mm port and deposited into a sterile pan. When removed, the adnexae were morcellated in a similar fashion. After the larger portions of the tissue were removed, a 10-mm spoon forceps was introduced and used to pick up the small remaining pieces that may have fragmented during the manipulations. The patient was taken out of the Trendelenburg position so that any accumulated intraperitoneal fluids would pool in the lower pelvis. These fluids were aspirated and replaced with fresh heparinized Ringers (5000 units of heparin per 1 l of lactated Ringers). Approximately ml of fluid containing 2 ml of polymixin, bacitracin, and neomycin was instilled to remain intraperitoneally. Nu-Knit (Johnson & Johnson Medical, Arlington, Texas, USA) was then introduced into the abdomen with the spoon forceps through the Gynaecological Endoscopy , Blackwell Science Ltd
5 EARLY EVALUATION OF AN ELECTROMECHANICAL MORCELLATOR 299 lower 12-mm trocar sheath and placed over the cervical stump. This piece of double-thickness Surgicel is designed specifically for laparoscopic application as a haemostatic agent to augment early postoperative haemostasis. The pneumoperitoneum was evacuated from the abdomen and the laparoscope was then used to inspect all the pedicles, with reduced intraperitoneal CO 2 pressure. At this point, the lower 12-mm trocar was removed and a reusable Carter Thompson fascial closure device (Inlet Medical, Eden Prairie, Minnesota, USA) was used to close the lower 12-mm peritoneum and fascia opening with an absorbable suture. The two lateral 5-mm ports were then removed and the puncture wounds inspected for any bleeding. Finally, the umbilical 10-mm reusable sheath was removed and all four skin incisions closed with subcuticular sutures. Postoperatively, the patients were seen 4 6 h after surgery, at which time the catheter was removed. After ambulating, voiding and tolerating oral fluids, patients were discharged in the care of family members. Follow up All patients were seen 2 and 6 weeks postoperatively and closely questioned concerning their recovery. They were encouraged to resume their regular activities in 2 weeks, but to avoid intercourse for 1 week following surgery. Patients who had undergone oöphorectomy, with no contraindications to oestrogen replacement therapy, were started on oestrogen the day after surgery to help them avoid early postoperative oestrogen deficiency symptoms. All patients were again counselled that they must have annual follow-up Pap smears, as well as their routine scheduled gynaecological exams. RESULTS Clinical indications for hysterectomy in this series are shown in Table 1. The age range of the patients was years, with the mean age being 43. Only three Table 1 Indications for laparoscopic supracervical hysterectomy (LSH) in 41 patients; final pathological iagnosis Indication Fibroids 23 Endometriosis 5 Bleeding 5 Chronic pelvic pain 3 Adenomyosis 5 Total 41 n patients were under 35 and the youngest patient had severe endometriosis and bilateral endometriomas. Of the women in this series, 19 were nulliparous, 14 had undergone a previous Caesarean section, but only eight had experienced a vaginal delivery. Uterine weights ranged from 48 to 569 g, with a mean weight of 146 g. The 48-g uterus was from an 80-lb woman with adenomyosis. Evaluation of length of hospital stay revealed a mean of 1.04 days. A total of 37 patients were discharged within 23 h, and the other four stayed 48 h. The actual time of the operation was calculated from placement of the first trocar until the closure of the 12-mm fascial suture, and recorded in each case. The mean operating time was 94 min, with the minimum time being 60 min and the maximum time 225 min. The prolonged operative time for one patient reflected an extremely difficult operation. This patient had a 5-cm broad ligament fibroid and extensive adhesions from two previous open myomectomies, which required significant dissection before the LSH could begin. In addition, the morcellator stopped working because of technical error in its assembly, and the most of the morcellation was done using more tedious slower methods. Average blood loss was estimated as 125 ml with a maximum blood loss of 600 ml, and minimum loss of 20 ml. No patients received any blood transfusions in this series. Table 2 summarizes these outcome variables and compares them with our similar findings in our initial report on LSH from Representative mean hospital costs were calculated, excluding surgical, anaesthesiology, and pathology fees, and before managed care discounts were included. The mean actual cost for these procedures was $7998 with a minimum of $6989 and a maximum charge of $ As expected, this Table 2 Comparison of study variable outcomes Variable 1994 LSH 1996 LSH Number of cases Average operating time, h:min 1:46 1:30 Average estimated blood loss, ml Average hospital stay, days Number of complications 2 1 Mean hospital costs* $7501 $6719 *Not including pathology, anaesthesia, managed care discounts or surgeons fees. Inflation-corrected cost estimate; actual calculated cost was $ Blackwell Science Ltd Gynaecological Endoscopy ,
6 300 J. F. DANIELL et al. Figure 3 Graphical representation of uterine weight, total operating time and morcellation time. The morcellation times were obtained by review of videotapes of the surgical procedure and were available for only 19 of the cases. highest charge occurred in the patient with 225 min of operative time. On review of videotapes for this study, only 19 patients had actual real-time video coverage of the full morcellation procedure. By viewing the real-time videotapes of these operations, it was possible to determine the actual time necessary to perform tissue removal with the electromechanical morcellator. Times for morcellation ranged from 4.2 min up to 23 min in this group of 19 patients, with a mean time of min. Figure 3 illustrates this graphically, comparing uterine weights to morcellation times for 19 of 41 patients, and demonstrates the relationship between total operative anaesthesia time and morcellation times previously described. Complications in this study were few, and included two patients with minimal postoperative cervical bleeding which stopped spontaneously within 4 months. One other patient who had undergone bilateral adnectomy with the LSH had persistent right lower quadrant pain following surgery, and was thought to probably have postoperative adhesions. However, 7 months after the LSH, she underwent a diagnostic laparoscopy which revealed minimal postsurgical adhesions to the cervical stump and the left lower pelvic sidewall, but no adhesions in the area of her right lower quadrant pain and a normal appendix. With subsequent treatment for spastic colon syndrome, her symptoms resolved. There was one significant postoperative complication that led to follow-up operative procedures. The patient with significant postoperative complications was a 32-year-old 80-lb woman with two previous Caesarean deliveries. She had a very small uterus (48 g) and cervix with endometriosis, adenomyosis, and significant adhesions to the anterior cervix. During the LSH an upper portion of the small cervix on the left side was resected. Because of persistent mild cervical bleeding, a ball electrode was used transcervically 3 months after the LSH, to coagulate the endocervical canal. This was done under laparoscopic visualization which revealed that the remaining left lateral cervix was very small with significant postoperative thermal necrosis. At 10 days following this minor second operative procedure, the patient developed profuse cervical bleeding and underwent an emergency laparotomy with trachelectomy to remove a necrotic small residual cervix. At the emergency laparotomy done on a weekend night, the patient was noted to have a very small remaining portion of the left cervical tissue and it was theorized that the final bleeding episode occurred because of sloughing of the medial portions of the cervical branch of the uterine artery entering this area of thermal necrosis. At the 6-week follow-up examination and questioning, all sexually active patients reported satisfactory intercourse without significant dyspareunia. Since no presurgical questionnaires of sexual function were used in this study, no attempt was made to assess postoperative sexual function in this group. No patients developed any urinary tract infections or postoperative urinary dysfunction. There were no problems with trocar site haematomas, hernias, or wound healing in this series. Gynaecological Endoscopy , Blackwell Science Ltd
7 EARLY EVALUATION OF AN ELECTROMECHANICAL MORCELLATOR 301 DISCUSSION This short-term retrospective study indicates that the use of an electromechanical morcellator can enhance LSH. In the past, LSH required a colpotomy, a larger abdominal wall incision, or the use of tedious mechanical methods to morcellate the fundus. This device, first described by Steiner et al., 11 rapidly cores the uterus, removes the uterus and adnexae very rapidly, and reduces the operating times. In this study we reduced our average operating times for LSH by 16 min which in our operating room ($15/minute) results in a minimal cost savings alone of $240 per case. Actual dollar costs for LSH in this 1996 series were more than 1994 costs. However, our hospital reported to us annual inflation increases for all laparoscopic-assisted vaginal hysterectomy (LAVH) procedures of 8% per annum. Thus in 1994, dollars costs for this series of operations were calculated to be reduced by $881 per patient. This method of LSH reduces operator fatigue and avoids colpotomy or larger abdominal wall incisions, which can increase morbidity and give poor cosmetic results. Patients in this series were all appreciative of the fact that they only had two visible 5-mm trocar sites in each lateral lower quadrant. The 10-mm umbilical incision was hidden in the umbilicus since it was always made vertically deep down in the umbilicus, and the 12- mm suprapubic trocar site was always hidden in the pubic hair after full recovery from surgery. After personally viewing their videotapes, several patients commented on the fact that this actually was a sutureless hysterectomy, since the only sutures used were subcuticular sutures in the abdominal wall and the one fascial closure stitch. No intra-abdominal suturing was necessary, since bipolar coagulation was used for occluding all vascular pedicles. The electromechanical morcellator requires careful coordination between the assistant, the scrub nurse, and the surgeon. The technique that we have developed for morcellator use keeps the 12-mm sheath close to the abdominal wall and pulls the tissue up against the rotating blade, held high up in the lower abdomen just outside the tip of the 12-mm sheath. This reduces the chances for inadvertent injury from the sharp rotating blade. By bringing the morcellator in through the lower suprapubic site, we avoid introduction of large trocar sites laterally in the abdomen with the potential sequelae of bleeding, hernia defect or poor cosmetic results. When using the morcellator, it is appropriate to morcellate fibrotic tissue first while the blade is sharpest. In this fashion, dense fibroids can be morcellated before the less dense uterine and adnexal tissues are removed. One should discuss the use of this technique with hospital tissue committees and pathologists before undertaking to use the morcellator, since the pathologists need to be aware that tissue will be coming to them in long cylindrical cores and thus fragmented. For many years in our hospital we have done morcellation of fibroids using non-mechanical techniques, and have yet to encounter any problems with anatomical final pathological diagnosis. The constant fear is that one will morcellate a leiomyosarcoma and the pathologist will be unable to reconstruct the exact location and depth of penetration of the lesion. Clearly, the morcellator should only be used on masses which the operator is confident are benign. Complications in this study were limited to the cervical stump. In the past, we have used colpotomy on occasion to remove bulky uteri after LSH. With colpotomy, one introduces the potential for ascending infection, cuff cellulitis, and the postoperative time before a patient may have intercourse is prolonged because of the vaginal sutures. In this series and our previously reported series, we had no bladder or ureteral injuries. This reflects the fact that we do not dissect the bladder in any of our cases. We also do not dissect the ureter, although the ureter is identified and traced in all cases down to where it passes under the uterine artery. If the thermal effect from bipolar cautery stays above the uterine artery, one is unlikely to produce any thermal damage to the ureter that passes beneath that structure. As the bladder peritoneum is not dissected anteriorly with our technique, we make no attempts to reperitonealize the cervical stump. We have elected to place Nu-Knit over the cervical stump, which we feel reduces any early minor postoperative oozing. As mentioned above, Nu-Knit is double-thickness Surgicel, packaged specifically for laparoscopic application for haemostasis. It dissolves within 1 h into a gel similar to Surgicel. There are no studies in humans to suggest that Nu-Knit reduces postoperative adhesions, but theoretically, its haemostatic effects on the cervix should reduce postoperative bleeding and thus the potential for adhesions. We have recently had an opportunity to view the cervical stumps in three patients who had undergone laparoscopic subtotal hysterectomy prior to In all these patients, adnexal disease led to a repeat laparoscopy. In these patients, there was excellent reperitonealization over the cervix, with no adhesions present. To address the actual instance of adhesion formation after laparoscopic subtotal hysterectomy, one would 1998 Blackwell Science Ltd Gynaecological Endoscopy ,
8 302 J. F. DANIELL et al. have to perform second-look laparoscopy in every patient, and this is clearly not indicated. The main concern of traditional gynaecologists who are opposed to LSH is the potential for subsequent cervical disease that would not occur if the cervix had been removed at the primary operation. 12 Clearly, in this study and in our group of patients in our previous report from 1994, it is too soon to address the question of subsequent abnormal cervical pathology. To date, we have only had one patient who had undergone an LSH in our practice who has developed an abnormal Pap smear. A colposcopy and office biopsy revealed minimal atypia in that patient. It has been proposed by others that a prophylactic cervical conization can be performed at the time of LSH. 13 The theoretical advantages are that the squamocolumnar junction is removed, and therefore the potential for subsequent abnormal cellular changes is hopefully eliminated. In our previous experience, in two patients in whom we did prophylactic cervical conization with LSH, postoperative cervical bleeding occurred, most probably because of excess hyperaemia of the cervix from the trauma of the LSH, combined with the concomitant conization. In addition, our hospital tissue committee questioned our indications for doing conization in these two patients when there were only normal Pap smears and the final pathology report revealed normal cervical squamocolumnar epithelium. In the eyes of this committee, this was unnecessary and inappropriate surgery with unneccessary risks and costs to the patient. Thus, because of the potential complications of a prophylactic conization, combined with the fact that it is unneccessary surgery on normal tissue, we think that elective prophylactic conization with LSH should be abandoned. Instead, patients should be carefully followed after LSH with annual Pap smears and office colposcopy, biopsy and excisional procedures only when clinically indicated. Clearly, patients who are not capable of or available for careful long-term postoperative follow-up should not be given the opportunity to undergo LSH. In the past, a comprehensive review of the early literature on laparoscopic hysterectomies of all types, including LSH, concluded that the surgical complications are less with all forms of laparoscopic hysterectomy than with abdominal or vaginal hysterectomy. 14 Another review compared all LAVH types except LSH (3112 operations) to abdominal hysterectomy (1118 operations). 15 This review of 34 reports noted a higher rate of bladder and ureter injuries with LAVH vs. total abdominal hysterectomy (TAH). Hopefully our technique for LSH can reduce the risk of urinary tract injury. Recently, a countrywide study from Finland reported on over laparoscopies, including both diagnostic and operative. 16 In that nationwide report, ureteral injuries were 3 per 1000 and bladder injuries 3 per All of those injuries except two occurred after total laparoscopic hysterectomy, but none occurred after LSH. To our knowledge, there has not yet been a report of a ureteral or bladder injury following a laparoscopic subtotal hysterectomy. Obviously, this is a possibility, particularly if bipolar cautery is used too low or too lateral to the cervix. The surgeons must always be aware that lateral thermal damage can occur as much as 1 cm from the edge of the bipolar coagulation instrument. 17 Such thermal injuries usually present as a later complication after slow thermal necrosis. Laparoscopic supracervical hysterectomy is a very controversial procedure. Munro recently stated in his excellent clinical summary that as a result, supracervical hysterectomy could be postulated to be associated with fewer short and long-term complications and reduce direct costs of care. 9 We cannot draw any conclusions until prospective randomized blinded studies have been performed comparing laparoscopic subtotal hysterectomy with other forms of hysterectomy. Such studies have been performed comparing vaginal hysterectomy with laparoscopic hysterectomy, 18 and also comparing abdominal hysterectomy with laparoscopic assisted vaginal hysterectomy (LAVH). 19 In the authors opinion and that of others, 15 it would be very difficult in America to enrol patients for a randomized study of LSH vs. LAVH or TAH. Patients who are coming to physicians seeking retention of the cervix and who are candidates for having the cervix retained, are not going to volunteer for a study in which they have a 50% chance of having their cervix removed. Because of this fact, any randomized prospective studies comparing LSH to LAVH will be impossible with our patient population. Bladder function following LSH clearly needs further clinical evaluation. In the past, Kilkku 20 evaluated bladder function symptoms in a non-randomized study of 212 patients undergoing abdominal total or supracervical hysterectomy, and concluded that retaining the cervix reduced the postoperative bladder frequency symptoms. Lalos & Bjerle 21 evaluated 22 patients, equally divided between total abdominal and supracervical hysterectomy groups, comparing objective symptoms and urodynamic studies. They found no differences in either group concerning the frequency Gynaecological Endoscopy , Blackwell Science Ltd
9 EARLY EVALUATION OF AN ELECTROMECHANICAL MORCELLATOR 303 Table 3 Comparative studies of laparoscopic hysterectomy (LH) vs. laparoscopic subtotal hysterectomy (LSH) Authors Procedure n Operating time, min Blood loss, ml Hospital stay, h Lyons (1993) 4 LH LSH Richards & Simpkins (1995) 7 LH LSH Lalonde & Daniell (1996) 10 LH LSH of symptoms of incontinence or bladder dysfunction. However, this was a very small study and this subject clearly needs to be more carefully evaluated in the future. Unfortunately, since that of Masters & Johnson, no new pioneer studies on sexual response have appeared in the modern gynaecological literature. The only data available to us is now over a decade old, and concerns patients undergoing abdominal subtotal vs. total hysterectomy. 22 It is clear that this available data, which was fully reviewed by Hasson, 5 fails to demonstrate any difference in sexual function in women undergoing total vs. subtotal hysterectomy, either by the abdominal or laparoscopic approach. Problems in scientifically evaluating the complex physiology of the female sexual response will make it very difficult to construct proper investigations, particularly if prospective randomized studies are to be employed. We do, however, encourage investigators in the field of female sexual response to consider trying to design and go forward with such studies to address the very important question of the role of the cervix in sexual activity and response. Several studies have now recently appeared in the literature which clearly show that LAVH of all types reduces operative morbidity, and hastens recovery compared with abdominal hysterectomy. 23,24 No study yet has carefully evaluated the subgroup of laparoscopic hysterectomies performed by the laparoscopic subtotal approach. However, all of the initial reports of LSH compared with LAVH indicate shorter operating times for LSH, reduced blood loss, and a trend toward lower complication rates, particularly involving infectious processes from the cervical cuff and bladder or ureteral injury. Unfortunately, all of the initial studies involve single operators or groups extremely experienced in operative laparoscopy who are still constantly modifying their techniques. Table 3 lists and compares some of these initial studies. Many techniques have now been described for laparoscopic subtotal hysterectomy. We feel that as ours has evolved, it now combines safety, simplicity, reproducibility, and cost-effectiveness. We minimize our use of disposable instruments and use bipolar electrosurgery extensively to allow use of smaller trocar sites and to save money. Our technique of four punctures allows good traction and countertraction during the procedure. Our method for evacuation of smoke and irrigation throughout surgery also allows us basically to utilize a five-port technique, since the port containing the bipolar device also allows active suction and irrigation at the same time via the trocar stopcock site. Thus, we can enhance the view while constantly irrigating throughout the procedure, without wasting a port for constant placement of a suction aspiration device. In addition, the chore of suction of smoke and selected irrigation passes to the scrub nurse, thus freeing both hands of the surgeons. This enhances constant exposure by allowing use of two 5-mm graspers for traction and countertraction. We all need to be constantly aware of the costs of the items we use in surgery, and whenever safe, effective reusable equipment is available as an alternative to disposable types, we should incorporate those into our therapeutic regimen. This fact has been clearly addressed recently in an excellent editorial by Hurd & Diamond. 25 Recent studies in France, 26 Switzerland, 27 and America 28 clearly indicate that disposable laparoscopic instruments can be up to seven times more costly to patients, yet show no safety advantages. In the past, the senior author (JFD) has reported very high costs for early LAVH cases. 29 In retrospect, these high costs reflected high usage of laparoscopic stapling devices and throwaway instruments. Table 4 illustrates our old instrument preferences compared with our new replacement reusable instruments. From this list one clearly sees where much money was wasted in the past. At current costs to our hospital, over $2000 is saved per operation with our conversion to reusable instrumentation where possible. This has occurred with reduced operating times and no increase in complications Blackwell Science Ltd Gynaecological Endoscopy ,
10 304 J. F. DANIELL et al. Table 4 Comparison of 1991 instrument usage for laparoscopic-assisted vaginal hysterectomy (LAVH) to 1998 usage for LSH or LAVH; Columbia/HCA Women s Hospital, Nashville, Tennessee, USA* Laparoscopic instrumentation Old, 1991 New, 1998 Veress needle All disposable Reusable Trocars and sheath Disposable Reusable, shielded 10-mm (one) 10-mm (one) 12-mm (two) 5-mm (three) 5-mm (one) 12-mm (one) 5-mm scissors Disposable, Reusable, end point non-safety monitored safety monitored Vascular occlusion 12-mm cutter handle 5-mm bipolar coagulation/ 4 6 staple cartridges transection forcep (disposable) Hydrodissection system 5-mm disposable probe and 5 mm suction/aspiration mechanical Dorsey/ Nezhat reusable probe pump system PumpVac Plus with 10 ml vacuum syringe (disposable) Uterine manipulator Disposable systems Reusable polyp forceps or Hulka tenaculum *Estimated $2000 extra costs to patients (1998 Columbia/HCA contract purchase prices). While costs are of concern, one must always put safety first with all patient care. One example when both safety and costs are superior is the switch back to reusable 5-mm scissors. A recent study demonstrated, in a controlled animal laboratory setting, that reusable scissors with thicker insulation are safer for unipolar electrosurgical use at laparoscopy than disposable single-use thinner insulated ones. 30 Now even safer unipolar electrosurgery is possible at laparoscopy by using scissors or probes that incorporate active electrode monitoring to eliminate the rare but tragic complications from capacitive coupling. 31 We advise all careful laparoscopists using unipolar electrosurgery to incorporate this safety feature, analogous to automobile airbags, into their personal laparoscopic armamentarium. CONCLUSIONS Clearly, supracervical hysterectomy is becoming more popular, both among patients and gynaecologists in the industrialized world. We feel that with modern office screening and treatment of the cervix, that the argument for routine prophylactic removal of the cervix to eliminate the risk of cervical cancer has become archaic. Do we recommend prophylactic removal of the vagina in women undergoing hysterectomy because of the low theoretical risk of vaginal cancer? Clearly, not. Therefore, why do some physicians still insist on prophylactic removal of the cervix in women who are not at significant risk for cervical cancer and who are committed to careful lifetime follow up? Many women who in the past have undergone endometrial ablation for treatment of dysfunctional uterine bleeding still have their uterus and cervix intact, leaving them at risk for subsequent cervical (and uterine) pathologies. Obviously, no one argues with this simple operation to minimize treatment for menorrhagia. We agree with Harry Hasson, who has said the cervix is not a useless organ and should not be removed during hysterectomy without a proper indication. 5 It is time to rethink our concepts of removing the cervix and to enhance our personal skills for laparoscopic surgery. Much more clinical investigation is required to address long-term benefits of LSH. In addition, classifications of subtotal hysterectomies need to be standardized, so that people will be comparing apples to apples when reporting outcomes. Hopefully, in the near future, carefully designed prospective studies of LSH can address some of these critical areas of concern. Such scientific information will be necessary as we continue to strive to develop the most effective, safe, and cost-effective methods to manage diseases among our patients which require hysterectomy. REFERENCES 1 Reich H, DeCaprio J, McGlynn F. Laparoscopic hysterectomy. Journal of Gynecological Surgery 1989; 5: Gynaecological Endoscopy , Blackwell Science Ltd
11 EARLY EVALUATION OF AN ELECTROMECHANICAL MORCELLATOR Semm K. Hysterectomy via laparotomy or pelviscopy. A new CASH method without colpotomy. Geburtshilfe und Frauenheilkunde 1991; 51: Donnez J, Nisolle M. Laparoscopic supracervical (subtotal) hysterectomy (LASH). Journal of Gynecological Surgery 1993; 9: Lyons TL. Laparoscopic supracervical hysterectomy: a comparison of morbidity and mortality results with laparoscopically assisted vaginal hysterectomy. Journal of Reproductive Medicine 1993; 38: Hasson HM. Cervical removal at hysterectomy for benign disease, risks and benefits. Journal of Reproductive Medicine 1993; 38: Schwartz RO. Laparoscopic hysterectomy: Supracervical vs assisted vaginal. Journal of Reproductive Medicine 1994; 39: Richards SR, Simpkins S. Laparoscopic supracervical hysterectomy versus laparoscopic-assisted vaginal hysterectomy. Journal of the American Association of Gynecologic Laparoscopists 1995; 2: Donnez J, Nisolle M, Smets M, Polet R, Bassil S. Laparoscopic supracervical (subtotal) hysterectomy: a first series of 500 cases. Gynaecological Endoscopy 1997; 6: Munro MG. Supracervical hysterectomy: a time for reappraisal. Obstetrics and Gynecology 1997; 89: Lalonde CJ, Daniell JF. Early outcomes of laparoscopicassisted vaginal hysterectomy versus laparoscopic supracervical hysterectomy. Journal of the American Association of Gynecologic Laparoscopists 1996; 3: Steiner RA, Wight E, Tadir Y, Haller U. Electrical cutting device for laparoscopic removal of tissue from the abdominal cavity. Obstetrics and Gynecology 1993; 81: Pratt JH, Jefferies JA. The retained cervical stump. Obstetrics and Gynecology 1976; 48: Ewen SP, Sutton CJG. Initial experience with supracervical laparoscopic hysterectomy and removal of the cervical transformation zone. British Journal of Obstetrics and Gynaecology 1994; 101: Harris WJ, Daniell JF. Early complications of laparoscopic hysterectomy. OBGYN Surveys 1996; 51: Meikle SF, Nugent EW, Orleans M. Complications and recovery from laparoscopy-assisted vaginal hysterectomy compared with abdominal and vaginal hysterectomy. Obstetrics and Gynecology 1997; 89: Härkki-Sirén P, Kurki T. A nationwide analysis of laparoscopic complications. Obstetrics and Gynecology 1997; 89: Duffy S, Reid PC, Smith JHF, Sharp F. In vitro studies of uterine electrosurgery. Obstetrics and Gynecology 1991; 78: Summitt RL, Stovall TG, Lipscomb GH, Ling FW. Randomized comparison of laparoscopic assisted vaginal hysterectomy with standard vaginal hysterectomy in an outpatient setting. Obstetrics and Gynecology 1992; 80: Raju KS, Auld BJ. A randomised prospective study of laparoscopic vaginal hysterectomy versus abdominal hysterectomy each with bilateral salpingo-oophorectomy. British Journal of Obstetrics and Gynaecology 1991; 98: Kilkku P. Supravaginal uterine amputation versus hysterectomy with reference to subjective bladder symptoms and incontinence. Acta Obstetrica et Gynecologica Scandinavica 1985; 64: Lalos O, Bjerle P. Bladder wall mechanics and micturition before and after subtotal and total hysterectomy. European Journal of Obstetrics, Gynecology and Reproductive Biology 1986; 21: Kilkku P. Supravaginal uterine amputation vs hysterectomy: Effects on coital frequency and dyspareunia. Acta Obstetrica et Gynecologica Scandinavica 1983; 62: Ransom SB, McNeeley G, White C, Diamond MP. A cost analysis of endometrial ablation, abdominal hysterectomy, vaginal hysterectomy, and laparoscopicassisted vaginal hysterectomy in the treatment of primary menorrhagia. Journal of the American Association of Gynecologic Laparoscopists 1996; 4: Johns DA, Carrera B, Jones J, DeLeon F, Vincent R, Safely C. The medical and economic impact of laparoscopically assisted vaginal hysterectomy in a large, metropolitan, not-for-profit hospital. American Journal of Obstetrics and Gynecology 1995; 172: Hurd WW, Diamond MP. There s a hole in my bucket: the cost of disposable instruments. Fertility and Sterility 1997; 67: Chapron C, Dubuisson J. Total laparoscopic hysterectomy for benign uterine pathologies with reusable instruments: a safe, reproducible and costeffective procedure. Gynaecological Endoscopy 1996; 5: Schaer GN, Koechli OR, Haller U. Single-use versus reusable laparoscopic surgical instruments: a comparative cost analysis. American Journal of Obstetrics and Gynecology 1995; 173: Ransom SB, McNeeley SG, White C, Diamond MP. A cost-effectiveness evaluation of laparoscopic disposable versus nondisposable infraumbilical cannulas. Journal of the American Association of Gynecologic Laparoscopists 1996; 4: Daniell JF, Kurtz BR, McTavish G, et al. Laparoscopically assisted vaginal hysterectomy: the initial Nashville experience. Journal of Reproductive Medicine 1993; 38: Grosskinsky CM, Hulka JF. Unipolar electrosurgery in operative laparoscopy: capacitance as a potential source of injury. Journal of Reproductive Medicine 1995; 40: Luciano AA, Soderstrom RM, Martin DC. Essential principles of electrosurgery in operative laparoscopy. Journal of the American Association of Gynecologic Laparoscopists 1994; 1: Blackwell Science Ltd Gynaecological Endoscopy ,
Laparoscopic Assisted Vaginal Hysterectomy
 Department of Obstetrics and Gynecology, Chang Gung Memorial Hospital at ChiaYi 嘉 義 長 庚 紀 念 醫 院 婦 產 科 Clinical Guideline Laparoscopic Assisted Vaginal Hysterectomy By Dr. CJ Tseng Laparoscopic assisted
Department of Obstetrics and Gynecology, Chang Gung Memorial Hospital at ChiaYi 嘉 義 長 庚 紀 念 醫 院 婦 產 科 Clinical Guideline Laparoscopic Assisted Vaginal Hysterectomy By Dr. CJ Tseng Laparoscopic assisted
Hysterectomy. The time to take care of yourself
 Hysterectomy The time to take care of yourself The time to take care of yourself Women spend a lot of time taking care of others spouses, children, parents. We often overlook our own needs. But when our
Hysterectomy The time to take care of yourself The time to take care of yourself Women spend a lot of time taking care of others spouses, children, parents. We often overlook our own needs. But when our
Summa Health System. A Woman s Guide to Hysterectomy
 Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
About the Uterus. Hysterectomy may be done to treat conditions that affect the uterus. Some reasons a hysterectomy may be needed include:
 Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Women s Health Laparoscopy Information for patients
 Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
A Guide to Hysteroscopy. Patient Education
 A Guide to Hysteroscopy Patient Education QUESTIONS AND ANSWERS ABOUT HYSTEROSCOPY Your doctor has recommended that you have a procedure called a hysteroscopy. Naturally, you may have questions about
A Guide to Hysteroscopy Patient Education QUESTIONS AND ANSWERS ABOUT HYSTEROSCOPY Your doctor has recommended that you have a procedure called a hysteroscopy. Naturally, you may have questions about
Hysterectomy. What is a hysterectomy? Why is hysterectomy done? Are there alternatives to hysterectomy?
 ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
Treating heavy menstrual bleeding caused by fibroids or polyps
 Treating heavy menstrual bleeding caused by fibroids or polyps With today s medical advances the outlook for successful treatment of fibroids and polyps has never been better. You don t have to live with
Treating heavy menstrual bleeding caused by fibroids or polyps With today s medical advances the outlook for successful treatment of fibroids and polyps has never been better. You don t have to live with
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
How To Perform Da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Transvaginal Endoscopy TVE GYN 18 7.0 02/2015-E
 Transvaginal Endoscopy TVE GYN 18 7.0 02/2015-E TRANSVAGINAL ENDOSCOPY Leuven Institute for Fertility and Embryology Prof. Dr. S. Gordts, Dr. R. Campo, Dr. P. Puttemans, Prof. Em. Dr. I. Brosens 2 Transvaginal
Transvaginal Endoscopy TVE GYN 18 7.0 02/2015-E TRANSVAGINAL ENDOSCOPY Leuven Institute for Fertility and Embryology Prof. Dr. S. Gordts, Dr. R. Campo, Dr. P. Puttemans, Prof. Em. Dr. I. Brosens 2 Transvaginal
Physician. Patient HYSTERECTOMY HYSTERECTOMY. Treatment Options Risks and Benefits Experience and Skill
 HYSTERECTOMY Physician Treatment Options Risks and Benefits Experience and Skill Patient Personal Preferences Values and Concerns Lifestyle Choices HYSTERECTOMY Shared Decision Making A process of open
HYSTERECTOMY Physician Treatment Options Risks and Benefits Experience and Skill Patient Personal Preferences Values and Concerns Lifestyle Choices HYSTERECTOMY Shared Decision Making A process of open
Less Invasive is Best
 Less Invasive is Best June 22, 2011 By OBGYN.net Staff [1] Laparoscopic hysterectomy (LH) is an optimum approach to the second most common surgical procedure in the United States. There are close to 600,000
Less Invasive is Best June 22, 2011 By OBGYN.net Staff [1] Laparoscopic hysterectomy (LH) is an optimum approach to the second most common surgical procedure in the United States. There are close to 600,000
Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery
 Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Endometriosis Endometriosis is a condition in which the tissue that lines your uterus (the endometrium)
Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Endometriosis Endometriosis is a condition in which the tissue that lines your uterus (the endometrium)
Role of Robotic Surgery in Obese Women with Endometrial Cancer
 Role of Robotic Surgery in Obese Women with Endometrial Cancer Anil Tailor Consultant Gynaecological Oncologist Royal Surrey County Hospital Guildford, Surrey, UK St Peters Hospital Chertsey, Surrey, UK
Role of Robotic Surgery in Obese Women with Endometrial Cancer Anil Tailor Consultant Gynaecological Oncologist Royal Surrey County Hospital Guildford, Surrey, UK St Peters Hospital Chertsey, Surrey, UK
Ovarian Cystectomy / Oophorectomy
 Cystectomy and Ovarian Cysts Ovarian cysts are sacs filled with fluids or pockets located on or in an ovary. In some cases, these cysts need to be removed surgically. Types of Cysts Ovarian cysts are quite
Cystectomy and Ovarian Cysts Ovarian cysts are sacs filled with fluids or pockets located on or in an ovary. In some cases, these cysts need to be removed surgically. Types of Cysts Ovarian cysts are quite
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
No Costly Hospital Stays. No Unsightly Incisions. Far Faster, Less Painful Recovery.
 No Costly Hospital Stays. No Unsightly Incisions. Far Faster, Less Painful Recovery. No Costly Hospital Stays. No Unsightly Incisions. Far Faster, Less Painful Recovery. Welcome to the Georgia Advanced
No Costly Hospital Stays. No Unsightly Incisions. Far Faster, Less Painful Recovery. No Costly Hospital Stays. No Unsightly Incisions. Far Faster, Less Painful Recovery. Welcome to the Georgia Advanced
Laparoscopy and Hysteroscopy
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
Uterine fibroids (Leiomyoma)
 Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
Considering a Hysterectomy?
 Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Adenomyosis,
Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Adenomyosis,
Considering a Hysterectomy?
 Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Pelvic Prolapse
Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Pelvic Prolapse
Laparoscopic Hysterectomy
 Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Cervical Cancer The Importance of Cervical Screening and Vaccination
 Cervical Cancer The Importance of Cervical Screening and Vaccination Cancer Cells Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Sometimes, this
Cervical Cancer The Importance of Cervical Screening and Vaccination Cancer Cells Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Sometimes, this
Surgical techniques: robot-assisted laparoscopic hysterectomy with the da Vinci surgical system
 THE INTERNATIONAL JOURNAL OF MEDICAL ROBOTICS AND COMPUTER ASSISTED SURGERY Int J Med Robotics Comput Assist Surg 2006; 2: 305 311. Published online in Wiley InterScience (www.interscience.wiley.com)..111
THE INTERNATIONAL JOURNAL OF MEDICAL ROBOTICS AND COMPUTER ASSISTED SURGERY Int J Med Robotics Comput Assist Surg 2006; 2: 305 311. Published online in Wiley InterScience (www.interscience.wiley.com)..111
Vaginal prolapse repair surgery with mesh
 Vaginal prolapse repair surgery with mesh Your doctor has recommended a vaginal reconstructive procedure using mesh to treat your condition. The operation involves surgery to reattach the vagina to its
Vaginal prolapse repair surgery with mesh Your doctor has recommended a vaginal reconstructive procedure using mesh to treat your condition. The operation involves surgery to reattach the vagina to its
LAPAROSCOPIC OVARIAN CYSTECTOMY
 LAPAROSCOPIC OVARIAN CYSTECTOMY Information Leaflet Your Health. Our Priority. Page 2 of 5 About this information This leaflet is for you if you have a cyst on one or both ovaries and are considering surgery.
LAPAROSCOPIC OVARIAN CYSTECTOMY Information Leaflet Your Health. Our Priority. Page 2 of 5 About this information This leaflet is for you if you have a cyst on one or both ovaries and are considering surgery.
A potential treatment for your abnormal uterine bleeding
 TRUCLEAR System A potential treatment for your abnormal uterine bleeding Do You Suffer from Abnormal Uterine Bleeding? What is a Hysteroscopy? What is the TRUCLEAR Procedure? What Happens Before Your
TRUCLEAR System A potential treatment for your abnormal uterine bleeding Do You Suffer from Abnormal Uterine Bleeding? What is a Hysteroscopy? What is the TRUCLEAR Procedure? What Happens Before Your
Keyhole (Laparoscopic) Surgery
 Patient Information leaflet Keyhole (Laparoscopic) Surgery Produced by: Department of Obstetrics & Gynaecology December 2002 Reviewed April 2010 1 What is keyhole (laparoscopic) surgery? Laparoscopic surgery
Patient Information leaflet Keyhole (Laparoscopic) Surgery Produced by: Department of Obstetrics & Gynaecology December 2002 Reviewed April 2010 1 What is keyhole (laparoscopic) surgery? Laparoscopic surgery
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Uterine Fibroid Symptoms, Diagnosis and Treatment
 Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
MINIMALLY INVASIVE SURGERY FOR WOMEN Back to Life. Faster.
 MINIMALLY INVASIVE SURGERY FOR WOMEN Back to Life. Faster. Pictured above: UF gynecologists Sharon Byun, MD, Shireen Madani Sims, MD, and Michael Lukowski, MD, with the robotic surgery equipment. Make
MINIMALLY INVASIVE SURGERY FOR WOMEN Back to Life. Faster. Pictured above: UF gynecologists Sharon Byun, MD, Shireen Madani Sims, MD, and Michael Lukowski, MD, with the robotic surgery equipment. Make
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500. Endometriosis
 Endometriosis WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The lining of the uterus is called the endometrium. Sometimes, endometrial tissue grows elsewhere in the body. When this happens
Endometriosis WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The lining of the uterus is called the endometrium. Sometimes, endometrial tissue grows elsewhere in the body. When this happens
Once a woman has had a hysterectomy, she will no longer have menstrual periods and cannot have a child. She no longer needs to use contraception.
 Hysterectomy Summary Hysterectomy is the surgical removal of the womb (uterus), with or without the cervix. Hysterectomy is used to treat a number of conditions, including heavy or painful periods, fibroids
Hysterectomy Summary Hysterectomy is the surgical removal of the womb (uterus), with or without the cervix. Hysterectomy is used to treat a number of conditions, including heavy or painful periods, fibroids
NHS. Surgical repair of vaginal wall prolapse using mesh. National Institute for Health and Clinical Excellence. 1 Guidance.
 Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Why would you need a hysterectomy?
 Why would you need a hysterectomy? Removal of the uterus is performed to prevent, alleviate, or treat pain, pressure, bleeding, or cancer. Each reason is described in detail in the following pages. Benign
Why would you need a hysterectomy? Removal of the uterus is performed to prevent, alleviate, or treat pain, pressure, bleeding, or cancer. Each reason is described in detail in the following pages. Benign
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE
 Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
The percentage of women 21-64 years of age who received one or more Pap tests to screen for cervical cancer.
 Measure Name: Cervical Cancer Screen Owner: NCQA (CCS) Measure Code: CER Lab Data: Y Rule Description: General Criteria Summary The percentage of women 21-64 years of age who received one or more Pap tests
Measure Name: Cervical Cancer Screen Owner: NCQA (CCS) Measure Code: CER Lab Data: Y Rule Description: General Criteria Summary The percentage of women 21-64 years of age who received one or more Pap tests
FEMALE ANATOMY. the Functions of the Female Organs
 FEMALE ANATOMY the Functions of the Female Organs An educational video for every woman who is told she needs pelvic surgery, including exploratory surgery or removal of the uterus, fallopian tubes, or
FEMALE ANATOMY the Functions of the Female Organs An educational video for every woman who is told she needs pelvic surgery, including exploratory surgery or removal of the uterus, fallopian tubes, or
Abnormal Uterine Bleeding FAQ Sheet
 Abnormal Uterine Bleeding FAQ Sheet What is abnormal uterine bleeding? Under normal circumstances, a woman's uterus sheds a limited amount of blood during each menstrual period. Bleeding that occurs between
Abnormal Uterine Bleeding FAQ Sheet What is abnormal uterine bleeding? Under normal circumstances, a woman's uterus sheds a limited amount of blood during each menstrual period. Bleeding that occurs between
Hysteroscopy. What is a hysteroscopy? When is this surgery used? How do I prepare for surgery?
 What is a hysteroscopy? This is a procedure where a doctor uses a thin tube with a tiny camera to look inside the uterus. There are no incisions. Saline solution is used to expand the uterus in order to
What is a hysteroscopy? This is a procedure where a doctor uses a thin tube with a tiny camera to look inside the uterus. There are no incisions. Saline solution is used to expand the uterus in order to
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Saint Mary s Hospital. Hysterectomy. Information For Patients
 Saint Mary s Hospital Hysterectomy Information For Patients 2 Contents Welcome 4 What is a hysterectomy? 4 Why is a hysterectomy necessary? 4 How common is it? 7 Things to consider before having a hysterectomy
Saint Mary s Hospital Hysterectomy Information For Patients 2 Contents Welcome 4 What is a hysterectomy? 4 Why is a hysterectomy necessary? 4 How common is it? 7 Things to consider before having a hysterectomy
RADICAL HYSTERECTOMY IN ROBOTIC SURGERY
 RADICAL HYSTERECTOMY IN ROBOTIC SURGERY FLORENCE BOCHU CENTRE OSCAR LAMBRET LILLE PATRICIA VARUMBEKE CENTRE OSCAR LAMBRET LILLE MELANIE FLAMENT CENTRE OSCAR LAMBRET LILLE More and more centers across the
RADICAL HYSTERECTOMY IN ROBOTIC SURGERY FLORENCE BOCHU CENTRE OSCAR LAMBRET LILLE PATRICIA VARUMBEKE CENTRE OSCAR LAMBRET LILLE MELANIE FLAMENT CENTRE OSCAR LAMBRET LILLE More and more centers across the
INTERVENTIONAL PROCEDURES PROGRAMME
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radical laparoscopic hysterectomy for early stage cervical cancer Introduction This overview
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radical laparoscopic hysterectomy for early stage cervical cancer Introduction This overview
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
67273 EN V40/14 NOUVAG AG, all rights reserved Subject to change. Laparoscopic Hysterectomy Morcellator
 67273 EN V40/14 NOUVAG AG, all rights reserved Subject to change Laparoscopic Hysterectomy Morcellator Laparoscopic Hysterectomy Nowadays newly developed medical devices make hysterectomy possible by a
67273 EN V40/14 NOUVAG AG, all rights reserved Subject to change Laparoscopic Hysterectomy Morcellator Laparoscopic Hysterectomy Nowadays newly developed medical devices make hysterectomy possible by a
Surgical scissors and forceps Product List
 Surgical scissors and forceps Product List Sr. No Items Picture of Product Product specification 1 Grasping forceps-- 5 MM Grasping forceps are used to remove stones and retrieve foreign objects under
Surgical scissors and forceps Product List Sr. No Items Picture of Product Product specification 1 Grasping forceps-- 5 MM Grasping forceps are used to remove stones and retrieve foreign objects under
VAGINAL MESH FAQ. How do you decide who should get mesh as part of their repair?
 VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
Laparoscopic Hysterectomy
 Laparoscopic Hysterectomy Department of Gynaecology Patient Information What is is a a laparoscopic hysterectomy? hysterectomy? A laparoscopic hysterectomy is an operation performed under general anaesthetic
Laparoscopic Hysterectomy Department of Gynaecology Patient Information What is is a a laparoscopic hysterectomy? hysterectomy? A laparoscopic hysterectomy is an operation performed under general anaesthetic
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
2014 OB/GYN Surgery Medicare Reimbursement Coding Guide
 2014 OB/GYN Surgery Medicare Reimbursement Coding Guide Effective January 1, 2014 Medicare National Average Rates and Allowables (Not Adjusted For Geography) CPT * HCPCS Code 58150 58152 58180 58200 58210
2014 OB/GYN Surgery Medicare Reimbursement Coding Guide Effective January 1, 2014 Medicare National Average Rates and Allowables (Not Adjusted For Geography) CPT * HCPCS Code 58150 58152 58180 58200 58210
All you need to know about Endometriosis. Nordica Fertility Centre, Lagos, Asaba, Abuja
 All you need to know about Endometriosis October, 2015 About The Author Nordica Lagos Fertility Centre is one of Nigeria's leading centres for world class Assisted Reproductive Services, with comfort centres
All you need to know about Endometriosis October, 2015 About The Author Nordica Lagos Fertility Centre is one of Nigeria's leading centres for world class Assisted Reproductive Services, with comfort centres
International Journal of Case Reports in Medicine
 International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 340925, 18 minipages. DOI:10.5171/2013.340925 www.ibimapublishing.com Copyright 2013. Massinde Anthony. Distributed under
International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 340925, 18 minipages. DOI:10.5171/2013.340925 www.ibimapublishing.com Copyright 2013. Massinde Anthony. Distributed under
Frequently Asked Questions About Ovarian Cancer
 Media Contact: Gerri Gomez Howard Cell: 303-748-3933 [email protected] Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Media Contact: Gerri Gomez Howard Cell: 303-748-3933 [email protected] Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Intermediate Level Laparoscopic Surgery
 SPECIAL SKILLS TRAINING MODULE Intermediate Level Laparoscopic Surgery APRIL 00 Royal College of Obstetricians and Gynaecologists in collaboration with the British Society for Gynaecological Published
SPECIAL SKILLS TRAINING MODULE Intermediate Level Laparoscopic Surgery APRIL 00 Royal College of Obstetricians and Gynaecologists in collaboration with the British Society for Gynaecological Published
An operation for stress incontinence Tension-free Vaginal Tape (TVT)
 Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
Understanding Endometriosis - Information Pack
 What is endometriosis? Endometriosis (pronounced en- doh mee tree oh sis) is the name given to the condition where cells like the ones in the lining of the womb (uterus) are found elsewhere in the body.
What is endometriosis? Endometriosis (pronounced en- doh mee tree oh sis) is the name given to the condition where cells like the ones in the lining of the womb (uterus) are found elsewhere in the body.
Endometriosis Obstetrics & Gynaecology Women and Children s Group
 Endometriosis Obstetrics & Gynaecology Women and Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Endometriosis Obstetrics & Gynaecology Women and Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
How do I know if I need to have surgery?
 How do I know if I need to have surgery? Deciding whether or not to have surgery for your bladder, bowel and/or prolapse problems is an individual decision. The success or failure of someone else's operation
How do I know if I need to have surgery? Deciding whether or not to have surgery for your bladder, bowel and/or prolapse problems is an individual decision. The success or failure of someone else's operation
Specialists In Reproductive Medicine & Surgery, P.A.
 Specialists In Reproductive Medicine & Surgery, P.A. Craig R. Sweet, M.D. www.dreamababy.com [email protected] Excellence, Experience & Ethics Endometriosis Awareness Week/Month Common Questions
Specialists In Reproductive Medicine & Surgery, P.A. Craig R. Sweet, M.D. www.dreamababy.com [email protected] Excellence, Experience & Ethics Endometriosis Awareness Week/Month Common Questions
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Patient. Frequently Asked Questions. Transvaginal Surgical Mesh for Pelvic Organ Prolapse
 Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Endometriosis: An Overview
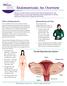 Endometriosis: An Overview www.bcwomens.ca Welcome to the BC Women s Centre for Pelvic Pain and Endometriosis. This handout will give you some basic information about endometriosis. It will also explain
Endometriosis: An Overview www.bcwomens.ca Welcome to the BC Women s Centre for Pelvic Pain and Endometriosis. This handout will give you some basic information about endometriosis. It will also explain
POST MENOPAUSAL BLEEDING CHECKLIST. Ultrasound. Information folder given to patient. Booking form faxed/emailed
 POST MENOPAUSAL BLEEDING CHECKLIST Ultrasound Information folder given to patient Booking form faxed/emailed 1 BOOKING FORM - HYSTEROSCOPY FOR POST MENOPAUSAL BLEEDING Patient s Name: Surname: DOB: / /
POST MENOPAUSAL BLEEDING CHECKLIST Ultrasound Information folder given to patient Booking form faxed/emailed 1 BOOKING FORM - HYSTEROSCOPY FOR POST MENOPAUSAL BLEEDING Patient s Name: Surname: DOB: / /
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Laparoscopic extended right hemicolectomy for transverse colon
 Laparoscopic extended right hemicolectomy for transverse colon cancer Elsa B. Valsdottir, MD Department of General Surgery University Hospital of Iceland Hringbraut 101 Reykjavik Iceland Phone +354 543
Laparoscopic extended right hemicolectomy for transverse colon cancer Elsa B. Valsdottir, MD Department of General Surgery University Hospital of Iceland Hringbraut 101 Reykjavik Iceland Phone +354 543
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE
 LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500. Ovarian Cysts
 Ovarian Cysts WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The ovaries are two small organs located on either side of a woman s uterus. An ovarian cyst is a sac or pouch filled with fluid
Ovarian Cysts WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The ovaries are two small organs located on either side of a woman s uterus. An ovarian cyst is a sac or pouch filled with fluid
Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system.
 Ovarian Cysts Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system. Most women have ovarian cysts sometime
Ovarian Cysts Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system. Most women have ovarian cysts sometime
Postoperative. Voiding Dysfunction
 Postoperative Voiding Trial Voiding Dysfunction Stephanie Pickett, MD Fellow Female Pelvic Medicine and Reconstructive Surgery Objectives Define postoperative voiding dysfunction Describe how to evaluate
Postoperative Voiding Trial Voiding Dysfunction Stephanie Pickett, MD Fellow Female Pelvic Medicine and Reconstructive Surgery Objectives Define postoperative voiding dysfunction Describe how to evaluate
SUBSEROSAL FIBROIDS TREATMENT
 INTRODUCTION Uterine fibroids, also known as leiomyomas, are the most common pelvic mass found in women. Fibroids are benign tumors that arise from the uterine muscular tissue (myometrium). They occur
INTRODUCTION Uterine fibroids, also known as leiomyomas, are the most common pelvic mass found in women. Fibroids are benign tumors that arise from the uterine muscular tissue (myometrium). They occur
PERCUTANEOUS PD CATHETER IMPLANTATION SYSTEM
 Place on Patient s Cranial Border of the Pubic Symphysis IMPLANTATION STENCIL Classic Exit Cuff Site PERCUTANEOUS PD CATHETER IMPLANTATION SYSTEM INSTRUCTIONS FOR USE VP 511 and VP-511M Implantation System
Place on Patient s Cranial Border of the Pubic Symphysis IMPLANTATION STENCIL Classic Exit Cuff Site PERCUTANEOUS PD CATHETER IMPLANTATION SYSTEM INSTRUCTIONS FOR USE VP 511 and VP-511M Implantation System
DA VINCI ROBOTIC HYSTERECTOMY
 DA VINCI ROBOTIC HYSTERECTOMY Until recently, surgery for most gynecologic conditions was performed using a large abdominal incision. This is because while conventional laparoscopic surgery is effective
DA VINCI ROBOTIC HYSTERECTOMY Until recently, surgery for most gynecologic conditions was performed using a large abdominal incision. This is because while conventional laparoscopic surgery is effective
Outpatient hysteroscopy
 Women s & Children s Outpatient hysteroscopy Information for patients Welcome to King s gynaecology service. The doctor who saw you in the outpatient clinic recently has recommended that you have a procedure
Women s & Children s Outpatient hysteroscopy Information for patients Welcome to King s gynaecology service. The doctor who saw you in the outpatient clinic recently has recommended that you have a procedure
Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON. Director of surgical department of Lefkos Stavros of Athens
 Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON Director of surgical department of Lefkos Stavros of Athens About 600,000 surgical hernia repair procedures are performed every year... Many
Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON Director of surgical department of Lefkos Stavros of Athens About 600,000 surgical hernia repair procedures are performed every year... Many
OVARIAN CYSTS. Types of Ovarian Cysts There are many types of ovarian cysts and these can be categorized into functional and nonfunctional
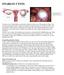 OVARIAN CYSTS Follicular Cyst Ovarian cysts are fluid-filled sacs that form within or on the ovary. The majority of these cysts are functional meaning they usually form during a normal menstrual cycle.
OVARIAN CYSTS Follicular Cyst Ovarian cysts are fluid-filled sacs that form within or on the ovary. The majority of these cysts are functional meaning they usually form during a normal menstrual cycle.
Uterine Fibroids. More than half of all women have fibroids. They are a common, benign, uterine growth.
 Uterine Fibroids More than half of all women have fibroids. They are a common, benign, uterine growth. Fibroids are not a disease. Much like the genetic blueprint that determines the color of your eyes
Uterine Fibroids More than half of all women have fibroids. They are a common, benign, uterine growth. Fibroids are not a disease. Much like the genetic blueprint that determines the color of your eyes
Birth after previous caesarean. What are my choices for birth after a caesarean delivery?
 Birth after previous caesarean Information for you Published September 2008 What are my choices for birth after a caesarean delivery? More than one in five women (20%) in the UK currently give birth by
Birth after previous caesarean Information for you Published September 2008 What are my choices for birth after a caesarean delivery? More than one in five women (20%) in the UK currently give birth by
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide
 Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Vaginal hysterectomy and vaginal repair
 Women s Service Vaginal hysterectomy and vaginal repair Information for patients Vaginal hysterectomy and vaginal repair This leaflet is for women who have been advised to have a vaginal hysterectomy.
Women s Service Vaginal hysterectomy and vaginal repair Information for patients Vaginal hysterectomy and vaginal repair This leaflet is for women who have been advised to have a vaginal hysterectomy.
In Vitro Fertilization
 Patient Education In Vitro Fertilization What to expect This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this process,
Patient Education In Vitro Fertilization What to expect This handout describes how to prepare for and what to expect when you have in vitro fertilization. It provides written information about this process,
A report of 300 cases using vacuum aspiration for the termination of pregnancy
 A report of 300 cases using vacuum aspiration for the termination of pregnancy Wu, Yuantai and Wu, Xianzhen Chinese Journal of Obstetrics and Gynaecology (1958:447-9) More than 100 years after Recamier
A report of 300 cases using vacuum aspiration for the termination of pregnancy Wu, Yuantai and Wu, Xianzhen Chinese Journal of Obstetrics and Gynaecology (1958:447-9) More than 100 years after Recamier
Ovarian cysts Diagnosis and Management
 Ovarian cysts Diagnosis and Management Mr P K Athanasias MRCOG Consultant Gynaecologist St Anthony s Hospital [email protected] Introduction ovary is an ovum-producing reproductive organ located in
Ovarian cysts Diagnosis and Management Mr P K Athanasias MRCOG Consultant Gynaecologist St Anthony s Hospital [email protected] Introduction ovary is an ovum-producing reproductive organ located in
Welcome to Cartersville Ob/Gyn Associates.
 Welcome to Cartersville Ob/Gyn Associates. We are a full-service Ob/Gyn practice, delivering women the exceptional care, medical expertise, compassion and support they deserve through every life cycle
Welcome to Cartersville Ob/Gyn Associates. We are a full-service Ob/Gyn practice, delivering women the exceptional care, medical expertise, compassion and support they deserve through every life cycle
Patient Information: Endometriosis Disease Process and Treatment
 1 William N. Burns, M. D. Associate Professor Department of Obstetrics & Gynecology Joan C. Edwards School of Medicine Marshall University Huntington, West Virginia, USA Patient Information: Endometriosis
1 William N. Burns, M. D. Associate Professor Department of Obstetrics & Gynecology Joan C. Edwards School of Medicine Marshall University Huntington, West Virginia, USA Patient Information: Endometriosis
Sterilisation for women and men: what you need to know
 Sterilisation for women and men: what you need to know Published January 2004 by the RCOG Contents Page number Key points 1 About this information 2 What are tubal occlusion and vasectomy? 2 What do I
Sterilisation for women and men: what you need to know Published January 2004 by the RCOG Contents Page number Key points 1 About this information 2 What are tubal occlusion and vasectomy? 2 What do I
Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
