The aging process is associated with sarcopenia (loss of
|
|
|
- Horace Pope
- 10 years ago
- Views:
Transcription
1 The Healthcare Costs of Sarcopenia in the United States Ian Janssen, PhD, w Donald S. Shepard, PhD, Peter T. Katzmarzyk, PhD, wz and Ronenn Roubenoff, MD, MHS OBJECTIVES: To estimate the healthcare costs of sarcopenia in the United States and to examine the effect that a reduced sarcopenia prevalence would have on healthcare expenditures. DESIGN: Cross-sectional surveys. SETTING: Nationally representative surveys using data from the U.S. Census, Third National Health and Nutrition Examination Survey, and National Medical Care and Utilization Expenditure Survey. PARTICIPANTS: Representative samples of U.S. adults aged 60 and older. MEASUREMENTS: The healthcare costs of sarcopenia were estimated based on the effect of sarcopenia on increasing physical disability risk in older persons. In the first step, the healthcare cost of disability in older Americans was estimated from national surveys. In the second step, the proportion of the disability cost due to sarcopenia (population-attributable risk) was calculated to determine the healthcare costs of sarcopenia. These calculations relied upon previously published relative risk values for disability in sarcopenic individuals and sarcopenia prevalence rates in the older population. RESULTS: The estimated direct healthcare cost attributable to sarcopenia in the United States in 2000 was $18.5 billion ($10.8 billion in men, $7.7 billion in women), which represented about 1.5% of total healthcare expenditures for that year. A sensitivity analysis indicated that the costs could be as low as $11.8 billion and as high as $26.2 billion. The excess healthcare expenditures were $860 for every From the Nutrition, Exercise Physiology, and Sarcopenia Laboratory, Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University, Boston, Massachusetts; w Department of Community Health and Epidemiology and z School of Physical and Health Education, Queen s University, Kingston, Ontario, Canada; Schneider Institute for Health Policy, Heller School for Social Policy and Management, Brandeis University, Waltham, Massachusetts. Research supported by the U.S. Department of Agriculture under Agreement and Contract 53-K06-1. I. Dr. Janssen is supported by a Canadian Institutes of Health Research Postdoctoral Fellowship. Any opinions or recommendations expressed in this publication are those of the authors and do not necessarily reflect the view of the U.S. Department of Agriculture. Address correspondence to Ian Janssen, PhD, Department of Community Health and Epidemiology, Abramsky Hall, Queen s University, Kingston, Ontario, Canada, K7L 3N6. [email protected] sarcopenic man and $933 for every sarcopenic woman. A 10% reduction in sarcopenia prevalence would result in savings of $1.1 billion (dollars adjusted to 2000 rate) per year in U.S. healthcare costs. CONCLUSION: Sarcopenia imposes a significant but modifiable economic burden on government-reimbursed healthcare services in the United States. Because the number of older Americans is increasing, the economic costs of sarcopenia will escalate unless effective public health campaigns aimed at reducing the occurrence of sarcopenia are implemented. J Am Geriatr Soc 52:80 85, Key words: skeletal muscle; sarcopenia; disability; healthcare costs The aging process is associated with sarcopenia (loss of skeletal muscle mass) 1 3 and an increase in the prevalence of physical disability. 4 Sarcopenia 5 8 and disability 9 11 are highly prevalent in older Americans. Recent estimates indicate that approximately 45% of the older U.S. population is sarcopenic 7 and that approximately 20% of the older U.S. population is functionally disabled. 10 Not surprisingly, sarcopenia is related to physical disability in older men and women. 5 8 At the individual level, disability leads to reduced quality of life; at the societal level, it leads to an increase in healthcare expenditures. In older persons, physical disability is associated with an increased risk of nursing home placement, 12 home healthcare 13 and hospital 14 use, and healthcare expenditures. 4,15 Given the high prevalence of sarcopenia and disability in older persons, the strong effect sarcopenia has on disability, and the increased healthcare expenditures in disabled persons, the economic burden of sarcopenia is presumed to be great. Nevertheless, even though the economic costs of illnesses play an important role in health policy, 16 there is a worldwide absence of reports that seek to quantify the effect of sarcopenia on the use of health services. Thus, the primary objective of this study was to estimate the healthcare costs of sarcopenia in the United States. Because sarcopenia is a potentially avoidable and reversible condition, a secondary objective was to examine the effect that reduced sarcopenia prevalence would have on healthcare expenditures. JAGS 52:80 85, 2004 r 2004 by the American Geriatrics Society /04/$15.00
2 JAGS JANUARY 2004 VOL. 52, NO. 1 ECONOMIC COST OF SARCOPENIA 81 METHODS The only condition that is known to be related to sarcopenia and that is associated with significant healthcare costs is physical disability (e.g., requiring help with personal care needs, such as bathing and dressing, or requiring help with routine needs, such as performing household chores and getting around). Thus, the healthcare costs associated with sarcopenia were estimated based on the effect of sarcopenia on increasing the risk of physical disability in older persons. To estimate the proportion of senescencerelated disability that could theoretically be prevented in the United States if sarcopenia were eliminated, populationattributable risk (PAR) was calculated. PAR is an estimate of the effects of an individual risk factor on a given disease or conditionfthe proportion of the disease or condition due to the risk factor in question. The PAR for disability was calculated as ðpðrr 1ÞÞ=ð1 þ PðRR 1ÞÞ where P is the prevalence of sarcopenia in the population and RR is the relative risk of disability in a sarcopenic individual. The prevalence of sarcopenia in the United States and the RR of disability in sarcopenic individuals has previously been calculated using data from the Third National Health and Nutrition Examination Survey (NHANES III). 7 NHANES III is a nationally representative cross-sectional survey that was conducted from 1988 through According to the results from NHANES III, the prevalence of older (Z60) men at increased risk for disability because of moderate (skeletal muscle index (SMI) kg/m 2 ) and severe (SMI r8.74kg/m 2 ) sarcopenia are 53.1% and 11.2%, respectively (Table 1). The corresponding RRs for disability in men with moderate and severe sarcopenia are 3.48 and 4.60, respectively. The prevalences of older women at increased risk for disability in NHANES III because of moderate (SMI kg/ m 2 ) and severe (SMI r5.74 kg/m 2 ) sarcopenia are 21.9% and 9.4%, respectively. The corresponding RRs for disability in women with moderate and severe sarcopenia are 1.46 and 3.15, respectively. 7 Within each sex, the PAR was calculated separately for moderate and severe sarcopenia, and the total PAR was determined by adding the PAR for the two levels of sarcopenia. 18 Economic Costs of Sarcopenia To estimate the economic burden of disability in older Americans, data from two national surveys, NHANES III 17 and the National Medical Care Utilization and Expenditures Survey (NMCUES) were used. 19 One study 4 previously calculated medical expenditures according to disability classification in older adults (Z65) using the NMCUES data set. Using the NHANES III data set, it was determined that the prevalence of disability in older adults is 17.2%, 17 which is similar to the disability prevalence rates (B20%) for older Americans that was recently published. 10 The definition of physical disability was slightly different in the NMCUES and NHANES III studies. In the NMCUES survey, disability was defined as the number of chronic conditions limiting work or keeping house, 4 whereas in the NHANES III survey, disability was defined as requiring help with personal care (eating, bathing, dressing) or routine needs (performing household chores, doing necessary business, shopping). 17 The RR for disability in sarcopenic individuals and prevalences of sarcopenia (see previous paragraph and Table 1) were calculated based on the NHANES III definition of disability. Because information from the NHANES III and NMCUES surveys had to be combined to estimate the cost of disability in older Americans, a consistent score for disability in the two studies was determined. First, temporal changes in the prevalence of disability from when NMCUES was conducted (1980) to when NHANES III was conducted ( ) were adjusted for. To do so, data from a study 11 that reported a 12.6% reduction in the prevalence of age-related disability (activities and instrumental activities of daily living) in the United States over a similar time frame ( ) were used. It was then determined that a disability prevalence of 19.4% (17.2% adjusted to 1980 value) in the older adults in NHANES III corresponded to a disability score (number of chronic conditions) of 1.57 or greater in the older adults in NMCUES. This was determined by regressing the disability score against the number of subjects with each disability score in NMCUES. Taking into consideration the distribution of subjects along the disability spectrum in the NMCUES survey, it was determined that the average disabled person in NHANES III would have a disability Table 1. Summary of Results Group Muscle Mass Range, kg/m 2 Prevalence in Population, % Relative Risk Disability Population Attributable Risk for Disability, % Cost, billion $ Older men Normal muscle Z F F Moderate sarcopenia Severe sarcopenia r Older women Normal muscle Z F F Moderate sarcopenia Severe sarcopenia r [prevalence (RR 1)]/[11prevalence (RR 1)].
3 82 JANSSEN ET AL. JANUARY 2004 VOL. 52, NO. 1 JAGS score of 1.67 in NMCUES. By regressing the disability score against healthcare expenditures, it was calculated that the theoretical excess medical expenditures (e.g., medical expenditures above that of a person with no disabling conditions) for an older person in NMCUES with a disability score of 1.67 was $6,395 per year. This value, which was calculated based on data obtained for individuals aged 65 and older, was adjusted to represent all individuals aged 60 and older, based on the percentage (25.4%) of the American population aged 60 and older who fit within the 60 to 64 age bracket in and the medical costs associated with disability in persons aged 60 to 64. The medical expenditures associated with a disability score of 1.67 for persons aged 60 to 64 in the NMCUES survey was determined by regressing age (Z45) against healthcare expenditures. Based on this information, the excess healthcare expenditure in the average disabled American aged 60 and older was estimated at $6,212 per year. All 1980 values have been converted to 2000 values using the medical component of the consumer price index. 21 The value of $6,212 per year is comparable with that previously published in another study. 15 In a sample of 843 older (Z72) adults from Connecticut, that study determined that disabled individuals accounted for $6,628 more per year (adjusted to 2000 dollars) in healthcare spending than nondisabled individuals. The number of older Americans with disability was multiplied by $6,212 to estimate the yearly healthcare cost of disability in older Americans. Using the NHANES III data set, it was determined that 10.4% of older (Z60) men and 18.1% of older women are disabled. 17 In 2000, there were 19,546,252 American men and 26,250,948 American women aged 60 and older. 20 Taken together, these results indicate that 2,032,810 older American men and 4,751,422 older American women were disabled in Thus, given that each individual with disability had an excess healthcare expenditure of $6,212/y, the estimated healthcare costs associated with disability in 2000 were $12.6 billion in older men and $29.5 billion in older women. The healthcare cost of sarcopenia was subsequently determined within each sex by multiplying the PAR by the economic cost of disability. To determine the influence of variations in the PAR and disability costs on the sarcopenia healthcare costs, a twoway sensitivity analysis similar to that previously used was performed to determine the healthcare costs of obesity 22 and physical inactivity. 23 PAR and disability healthcare cost were simultaneous varied by 720%. Savings from Reduction in Sarcopenia Because it would be unrealistic to expect an individual with severe sarcopenia to move all the way to the normal muscle category, the 10% reduced sarcopenia prevalence rates were calculated based on the assumption that those moving out of the severe sarcopenia category moved into the moderate sarcopenia category and not into the normal muscle category. Healthcare savings associated with a 10% reduction or improvement in the prevalence of sarcopenia were estimated by recalculating the PARs, assuming the prevalence of severe sarcopenia in older men to be 10.1% (11.2% 1.12%), the prevalence of moderate sarcopenia in older men to be 48.9% (53.1% 5.31% 11.12%), the prevalence of severe sarcopenia in older women to be 8.5% (9.4% 0.94%), and the prevalence of moderate sarcopenia in older women to be 20.6% (21.9% 2.19% 10.94%). The savings were then calculated by taking the difference between the costs derived using the actual and theoretical (e.g., 10% reduced) sarcopenia prevalence rates. RESULTS The PAR for disability in older men due to sarcopenia (moderate1severe) was 85.6% (Table 1). The PAR for disability due to sarcopenia (moderate1severe) in older women was 26.0%. This suggests that, if sarcopenia were completely eliminated, 85.6% of the disability cases in older men and 26.0% of the disability cases in older women would be eliminated. The estimated direct healthcare cost attributable to sarcopenia in the United States in 2000 was $18.5 billion ($10.8 billion in men, $7.7 billion in women). The sensitivity analysis indicated that the healthcare costs attributable to sarcopenia might be as low as $11.8 billion and as high as $26.2 billion. The distribution of the healthcare costs by degree of sarcopenia (moderate or severe) and sex are shown in Table 1. The excess healthcare expenditures were $860 for every sarcopenic man and $933 for every sarcopenic woman. Because the national healthcare expenditure for 2000 was $1,299 billion, 24 sarcopenia represented about 1.5% of total healthcare expenditures in the United States. Recalculating the healthcare costs with a 10% reduction in the prevalence of sarcopenia yielded a cost of $17.4 billion. Thus, a 10% reduction in sarcopenia prevalence would result in savings of $1.1 billion (2000 dollars) per year in U.S. healthcare costs. Almost half (46.6%) of this savings would occur if 10% of the population with severe sarcopenia moved into the moderate sarcopenia category; the remaining 54.4% of the savings would occur if 10% of the population with moderate sarcopenia moved into the normal muscle category. DISCUSSION The economic burden of sarcopenia in the United States was estimated using prevalence-based cost-of-illness methods and data from national surveys. The results indicate that $18.5 billion ($10.8 billion in men, $7.7 billion in women), or about 1.5% of total direct healthcare costs in the United States in 2000, were attributable to sarcopenia. Reducing the prevalence of sarcopenia by 10% would result in savings of $1.1 billion per year in U.S. healthcare costs. These findings confirm that sarcopenia is a significant public health problem, and one that imposes a significant burden on the U.S. economy. In a public health context, the finding that sarcopenia accounted for $18.5 billion in direct healthcare costs in 2000 is important. To put this in perspective, it has been estimated that the yearly economic costs of osteoporotic fractures in the United States is $16.3 billion (adjusted to 2000 dollars). 25 Given the extent of the economic burden imposed by osteoporosis, it is not surprising that there are
4 JAGS JANUARY 2004 VOL. 52, NO. 1 ECONOMIC COST OF SARCOPENIA 83 numerous public health campaigns aimed at reducing the occurrence of this disease. However, although sarcopenia accounts for a similar percentage of healthcare costs as osteoporosis, no public health campaigns are directly aimed at reducing the prevalence of sarcopenia. These estimates suggest that, if the prevalence of moderate and severe sarcopenia were reduced by 10%, it would result in savings of $1.1 billion per year in U.S. healthcare costs. Thus, even a modest reduction in the prevalence of sarcopenia in older persons would bring about marked healthcare savings when compiled over a number of years. These costs reflect the loss of skeletal muscle mass that occurs with advancing age and could theoretically be avoided if individuals maintained a healthy skeletal muscle mass throughout the lifespan. The authors recommend that older men strive to maintain a skeletal muscle mass relative to body height above kg/m 2 and that older women strive to maintain a skeletal muscle mass relative to body height above 6.75 kg/m 2. Muscle values below these cutpoints are associated with increased risk of disability. 7 An initial treatment that may reduce the normal progression of sarcopenia in older persons is to ensure that they are eating enough protein. Approximately 35% of the older population eats less than the current recommended dietary intake (RDI) for protein (0.8 g of protein kg 1 day 1 ), and about 15% eat less than 75% of this amount. 26 One study reported that eating about half of the RDI for protein over a 9-week period led to significant reductions in lean body mass in elderly women, whereas elderly women who consumed the RDI for protein maintained lean body mass. 27 However, it is not known whether modest reductions in dietary protein (e.g., 10 15% below RDI) contribute to sarcopenia or whether increasing protein intake levels to 100% of the RDI would result in an increase in muscle mass in sarcopenic individuals. Physical activity also holds great promise as a strategy for preventing and treating sarcopenia. Physically active older persons, particularly those who perform regular resistance exercise, have larger muscles than their sedentary counterparts. 28,29 Furthermore, it is well documented that strength training can increase muscle mass and strength in previously sedentary elderly men and women, independent of disease status and functional ability For example, a group of researchers 31 observed a 9% increase in muscle size after only 8 weeks of resistance training in the frail elderly. Because the age-related reduction in skeletal muscle begins in the fifth decade of life, 2,3 persons older than this should be encouraged to perform resistance exercise to help alleviate the normal reduction in muscle mass that occurs with advancing age. The American College of Sports Medicine recommends that older adults perform one to three sets of 10 to 15 repetitions for each of the major muscle groups (B8 exercises) three times per week. 32 This can be accomplished in anywhere from 1 to 3 hours per week. Although the cost-effectiveness of resistance exercise as a treatment for sarcopenia is unclear, the hypertrophic effects of resistance training occur quickly, and most exercise interventions are relatively inexpensive. Lifestyle exercise programs (home-based exercise and lifestyle counseling) cost about $200 per person per year, not including the cost of exercise equipment, and structured exercise programs (gym-based exercise and exercise counseling) cost about $600 per person per year. 34 By comparison, the analysis in this study revealed that sarcopenic individuals incurred about an extra $900 per year in healthcare expenditures. Thus, at the individual level, the healthcare costs of sarcopenia are greater than those of exercise participation, but additional research is needed to determine the cost-effectiveness of exercise interventions. A complete cost-benefit analyses would require valuing all economic inputs and outcomes to determine whether a net benefit of exercise is realized. Other inputs would include, for example, personal time and expenses (e.g., purchasing athletic clothing). Other outcomes would include, for example, the influence that exercise has on decreasing the healthcare costs of other diseases including cardiovascular disease, type II diabetes mellitus, osteoporosis, and cancer. 23,35 From a population perspective, it would take a considerable amount of time from the point at which money was invested in sarcopenia prevention and treatment to the point at which significant healthcare savings would be recognized. This lag can be explained by the fact that few older Americans perform resistance exercise on a regular basis (e.g., once per week or more). 17,36 Thus, campaigns aimed at increasing the public s awareness of incorporating resistance training as part of a well-rounded physical activity program would have to be developed and implemented before healthcare savings would occur. In addition, the feasibility of alternative programs such as dietary interventions and community-based exercise programs should be explored. The low-resistance training participation rates suggest that current resistance training practices (e.g., home-based and gym-based programs) are not effective in older persons. It is important to note that not everyone with sarcopenia is physically disabled, but depending on sex and the degree of sarcopenia (moderate or severe), the risk of disability is 1.5 to 4.6 times higher in older persons with sarcopenia than in older persons with normal muscle. 7 Furthermore, the findings of this study indicate that the proportion of disability (PAR) due to sarcopenia was 85.6% in older men and 26.0% in older women. There are two possible explanations for why sarcopenia had a greater effect on disability in men than women. The first is that the prevalence of sarcopenia is greater in men than women (64.2% vs 31.3%). 7 The second is that the other factors that contribute to disability (e.g., chronic disease) have a greater effect in women than men, consistent with the knowledge that the prevalence of disability is higher in women. 6,9,10,11 The healthcare cost estimates only took into consideration the direct costs of sarcopenia, including hospital, outpatient, and home healthcare expenditures. No attempt was made to include the indirect costs of sarcopenia such as lost productivity. Furthermore, in addition to disability, sarcopenia may also have an effect on osteoporosis, 37 obesity, 38 and type II diabetes mellitus 39,40 and their associated healthcare costs. However, a lack of epidemiological studies documenting a relationship between sarcopenia and these diseases caused us to choose a more conservative approach for the current analysis. Finally, in
5 84 JANSSEN ET AL. JANUARY 2004 VOL. 52, NO. 1 JAGS addition to economic costs, it is reasonable to assume that sarcopenic individuals have worse quality of life than do nonsarcopenic older persons and that sarcopenic individuals and their families and friends encounter additional psychosocial problems. The major limitation of this study was that the RRs for sarcopenia that were used to determine the PARs for disability were derived from cross-sectional analysis. The authors are unaware of prospective findings demonstrating a cause-and-effect relationship between sarcopenia and disability. However, muscular strength, which is in large measure determined by muscle mass, 41 is predictive of disability in longitudinal studies. 42,43 Thus, a causal relationship between sarcopenia and disability seems likely. Nonetheless, it is also probable that chronic disease of old age may lead to disability, which in turn would contribute to muscle wasting. A second limitation of the analysis was that the stage of disability for each subject was not taken into consideration. Although there is no commonly accepted system for grading disability, healthcare costs increase with greater degrees of disability. 4 It was also not possible to examine the effect of age on the relationship between disability and healthcare costs. It is possible that the cost of disability is higher in the oldest old (e.g., Z85) than in the young old (e.g., 60 70). However, to complete such an analysis would require estimates of the incidence of sarcopenia and disability and information on the costs of disability at each age for each sex. Another limitation was that the disability costs were derived from the NMCUES survey, which was conducted in The 1980 amounts were inflated to 2000 values using the medical component of the consumer price index, and it was therefore assumed that the relative contribution of disability to health expenditures did not change dramatically between 1980 and In summary, it has been demonstrated that sarcopenia imposes a significant economic burden on governmentreimbursed healthcare services in the United States. Because the number of older Americans is increasing, the economic costs of sarcopenia will escalate unless effective public health campaigns aimed at reducing the occurrence of sarcopenia are implemented. These are important observations given that economic costs of illnesses play an important role in health policy decision-making. 16 REFERENCES 1. Frontera WR, Hughes VA, Fielding RA et al. Aging of skeletal muscle: A 12-yr longitudinal study. J Appl Physiol 2000;88: Janssen I, Heymsfield SB, Wang ZM et al. Skeletal muscle mass and distribution in 468 men and women aged y. J Appl Physiol 2000;89: Kehayias JJ, Fiatarone MA, Zhuang H et al. Total body potassium and body fat: Relevance to aging. Am J Clin Nutr 1997;66: Rice DP, LaPlante MP. Medical expenditures for disability and disabling comorbidity. Am J Public Health 1992;82: Baumgartner RN, Koehler KM, Gallagher D et al. Epidemiology of sarcopenia among the elderly in New Mexico. Am J Epidemiol 1998;147: Janssen I, Heymsfield SB, Ross R. Low relative skeletal muscle mass (sarcopenia) in older persons is associated with functional impairment and physical disability. J Am Geriatr Soc 2002;50: Janssen I, Baumgartner RN, Ross R et al. Skeletal muscle cutpoints associated with elevated disability risk in older men and women. Am J Epidemiol in press. 8. Melton LJ 3rd, Khosla S, Crowson CS et al. Epidemiology of sarcopenia. J Am Geriatr Soc 2000;48: Ostchega Y, Harris TB, Hirsch R et al. The prevalence of functional limitations and disability in older persons in the U.S. data from the National Health and Nutrition Examination Survey III. J Am Geriatr Soc 2000;48: Manton KG, Gu X. Changes in the prevalence of chronic disability in the United States black and nonblack population above age 65 from 1982 to Proc Natl Acad Sci U S A 2001;98: Manton KG, Corder L, Stallard E. Chronic disability trends in elderly United States populations, Proc Natl Acad Sci U S A 1997;94: Wolinsky FD, Callahan CM, Fitzgerald JF et al. The risk of nursing home placement and subsequent death among older adults. J Gerontol 1992;47: S173 S Branch LG, Wetle TT, Scherr PA et al. A prospective study of incident comprehensive medical home care use among the elderly. Am J Public Health 1988;78: Ferrucci L, Guralnik JM, Pahor M et al. Hospital diagnoses, Medicare charges, and nursing home admissions in the year when older persons become severely disabled. JAMA 1997;277: Fried TR, Bradley EH, Williams CS et al. Functional disability and health care expenditures for older persons. Arch Intern Med 2001;161: Rice DP, Hodgson TA, Kopstein AN. The economic costs of illness: A replication and update. Health Care Financ Rev 1985;7: U.S. Department of Health and Human Services, National Center for Health Statistics. NHANES III Reference Manuals and Reports (CD-ROM). Hyattsville, MD: Centers for Disease Control and Prevention, Powell KE, Blair SN. The public health burdens of sedentary living habits: Theoretical but realistic estimates. Med Sci Sports Exerc 1994;26: Bonham GS Procedures and Questionnaires of the National Medical Care Utilization and Expenditure Survey. Washington, DC: U.S. Government Printing Office, U.S. Census Bureau. U.S. Summary 2000FCensus 2002 Profile. Washington, DC: U.S. Census Bureau, U.S. Department of Labor, Bureau of Labor Statistics. CPI Detailed Report. Washington, DC: Labor Department, Labor Statistics Bureau, Office of Prices and Working Conditions, Birmingham CL, Muller JL, Palepu A et al. The cost of obesity in Canada. Can Med Assoc J 1999;160: Katzmarzyk PT, Gledhill N, Shephard RJ. The economic burden of physical inactivity in Canada. Can Med Assoc J 2000;163: Levit K, Smith C, Cowan C et al. Trends in U.S. health care spending, Health Aff (Millwood) 2003;22: Ray NF, Chan JK, Thamer M et al. Medical expenditures for the treatment of osteoporotic fractures in the United States in Report from the National Osteoporosis Foundation. J Bone Miner Res 1997;12: Roubenoff R, Hughes VA. Sarcopenia. Current concepts. J Gerontol A Biol Sci Med Sci 2000;55A:M716 M Castaneda C, Charnley JM, Evans WJ et al. Elderly women accommodate to a low-protein diet with losses of body cell mass, muscle function, and immune response. Am J Clin Nutr 1995;62: Melichna J, Zauner CW, Havlickova L et al. Morphologic differences in skeletal muscle with age in normally active human males and their well-trained counterparts. Hum Biol 1990;62: Klitgaard H, Mantoni M, Schiaffino S et al. Function, morphology and protein expression of ageing skeletal muscle: A cross-sectional study of elderly men with different training backgrounds. Acta Physiol Scand 1990;140: Hurley BF, Redmond RA, Pratley RE et al. Effects of strength training on muscle hypertrophy and muscle cell disruption in older men. Int J Sports Med 1995;16: Fiatarone MA, Marks EC, Ryan ND et al. High-intensity strength training in nonagenarians. JAMA 1990;263: American College of Sports Medicine Position Stand. The recommended quality and quality of exercise for developing and maintaining cardiorespiratory and muscular fitness, and flexibility in healthy adults. Med Sci Sports Exerc 1998;30: Frontera WR, Meredith CN, O Reilly KP et al. Strength conditioning in older men. Skeletal muscle hypertrophy and improved function. J Appl Physiol 1988;64: Sevick MA, Dunn AL, Morrow MS et al. Cost-effectiveness of lifestyle and structured exercise interventions in sedentary adults. Results of Project ACTIVE. Am J Prev Med 2000;19: Colditz GA. Economic costs of obesity and inactivity. Med Sci Sports Exerc 1999;31:S663 S Adams PF, Benson V. Current estimates from the National Health Interview Survey. Vital Health Stat ;October: Gillette-Guyonnet S, Nourhashemi F, Lauque S et al. Body composition and osteoporosis in elderly women. Gerontology 2000;46: Baumgartner RN. Body composition in healthy aging. Ann N Y Acad Sci 2000;904:
6 JAGS JANUARY 2004 VOL. 52, NO. 1 ECONOMIC COST OF SARCOPENIA Castaneda C, Bermudez OI, Tucker KL. Protein nutritional status and function are associated with type 2 diabetes in Hispanic elders. Am J Clin Nutr 2000;72: Gougeon R, Pencharz PB, Sigal RJ. Effect of glycemic control on the kinetics of whole-body protein metabolism in obese subjects with non-insulin-dependent diabetes mellitus during iso- and hypoenergetic feeding. Am J Clin Nutr 1997;65: Newman AB, Haggerty CL, Goodpaster B et al. Strength and muscle quality in a well-functioning cohort of older adults: The Health, Aging and Body Composition Study. J Am Geriatr Soc 2003;51: Rantanen T, Guralnik JM, Foley D et al. Midlife hand grip strength as a predictor of old age disability. JAMA 1999;281: Rantanen T, Guralnik JM, Ferrucci L et al. Coimpairments as predictors of severe walking disability in older women. J Am Geriatr Soc 2001;49:21 27.
Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides.
 Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides. Example: = Head Over Heels Take a moment Confer with your neighbour And try to solve the following word
Take a moment Confer with your neighbour And try to solve the following word picture puzzle slides. Example: = Head Over Heels Take a moment Confer with your neighbour And try to solve the following word
Your Future by Design
 Retirement Research Series Your Future by Design Health, money, retirement: The different needs of men and women This research report is one of several reports in the Your Future by Design Retirement Research
Retirement Research Series Your Future by Design Health, money, retirement: The different needs of men and women This research report is one of several reports in the Your Future by Design Retirement Research
Nutritional problems. Age-related diseases Functional impairments Drug-induced nutritional deficiencies
 Nutritional problems Age-related diseases Functional impairments Drug-induced nutritional deficiencies Protein energy Vitamins Fibre Water Malnutrition >Deficiencies Obesity Hypervitaminosis >Excesses
Nutritional problems Age-related diseases Functional impairments Drug-induced nutritional deficiencies Protein energy Vitamins Fibre Water Malnutrition >Deficiencies Obesity Hypervitaminosis >Excesses
ECONOMIC COSTS OF PHYSICAL INACTIVITY
 ECONOMIC COSTS OF PHYSICAL INACTIVITY This fact sheet highlights the prevalence and health-consequences of physical inactivity and summarises some of the key facts and figures on the economic costs of
ECONOMIC COSTS OF PHYSICAL INACTIVITY This fact sheet highlights the prevalence and health-consequences of physical inactivity and summarises some of the key facts and figures on the economic costs of
Recommendations for Prescribing Exercise to Overweight and Obese Patients
 10 Recommendations for Prescribing Exercise to Overweight and Obese Patients 10 10 Recommendations for Prescribing Exercise to Overweight and Obese Patients Effects of Exercise The increasing prevalence
10 Recommendations for Prescribing Exercise to Overweight and Obese Patients 10 10 Recommendations for Prescribing Exercise to Overweight and Obese Patients Effects of Exercise The increasing prevalence
Diabetes Prevention in Latinos
 Diabetes Prevention in Latinos Matthew O Brien, MD, MSc Assistant Professor of Medicine and Public Health Northwestern Feinberg School of Medicine Institute for Public Health and Medicine October 17, 2013
Diabetes Prevention in Latinos Matthew O Brien, MD, MSc Assistant Professor of Medicine and Public Health Northwestern Feinberg School of Medicine Institute for Public Health and Medicine October 17, 2013
Traditional View of Diabetes. Are children with type 1 diabetes obese: What can we do? 8/9/2012. Change in Traditional View of Diabetes
 Are children with type 1 diabetes obese: What can we do? Traditional View of Diabetes Type 1 Diabetes ( T1DM) Onset Juvenile Lean Type 2 Diabetes ( T2DM) Onset Adult Obese QI Project Indrajit Majumdar
Are children with type 1 diabetes obese: What can we do? Traditional View of Diabetes Type 1 Diabetes ( T1DM) Onset Juvenile Lean Type 2 Diabetes ( T2DM) Onset Adult Obese QI Project Indrajit Majumdar
GA-3 Disaster Medical Assistance Team. Physical Fitness Guide
 GA-3 Disaster Medical Assistance Team Physical Fitness Guide PURPOSE: The purpose of this Physical Fitness Guide is to provide physical fitness training information to the members of the GA-3 Disaster
GA-3 Disaster Medical Assistance Team Physical Fitness Guide PURPOSE: The purpose of this Physical Fitness Guide is to provide physical fitness training information to the members of the GA-3 Disaster
WHAT IS THE CORE RECOMMENDATION OF THE ACSM/AHA PHYSICAL ACTIVITY GUIDELINES?
 PHYSICAL ACTIVITY AND PUBLIC HEALTH GUIDELINES FREQUENTLY ASKED QUESTIONS AND FACT SHEET PHYSICAL ACTIVITY FOR THE HEALTHY ADULT WHAT IS THE CORE RECOMMENDATION OF THE ACSM/AHA PHYSICAL ACTIVITY GUIDELINES?
PHYSICAL ACTIVITY AND PUBLIC HEALTH GUIDELINES FREQUENTLY ASKED QUESTIONS AND FACT SHEET PHYSICAL ACTIVITY FOR THE HEALTHY ADULT WHAT IS THE CORE RECOMMENDATION OF THE ACSM/AHA PHYSICAL ACTIVITY GUIDELINES?
Jill Malcolm, Karen Moir
 Evaluation of Fife- DICE: Type 2 diabetes insulin conversion Article points 1. Fife-DICE is an insulin conversion group education programme. 2. People with greater than 7.5% on maximum oral therapy are
Evaluation of Fife- DICE: Type 2 diabetes insulin conversion Article points 1. Fife-DICE is an insulin conversion group education programme. 2. People with greater than 7.5% on maximum oral therapy are
Kansas Behavioral Health Risk Bulletin
 Kansas Behavioral Health Risk Bulletin Kansas Department of Health and Environment November 7, 1995 Bureau of Chronic Disease and Health Promotion Vol. 1 No. 12 Diabetes Mellitus in Kansas Diabetes mellitus
Kansas Behavioral Health Risk Bulletin Kansas Department of Health and Environment November 7, 1995 Bureau of Chronic Disease and Health Promotion Vol. 1 No. 12 Diabetes Mellitus in Kansas Diabetes mellitus
The cost of physical inactivity
 The cost of physical inactivity October 2008 The cost of physical inactivity to the Australian economy is estimated to be $13.8 billion. It is estimated that 16,178 Australians die prematurely each year
The cost of physical inactivity October 2008 The cost of physical inactivity to the Australian economy is estimated to be $13.8 billion. It is estimated that 16,178 Australians die prematurely each year
Epidemiology of Sarcopenia among the Elderly in New Mexico
 American Journal of Epidemiology Copyright O 1998 by The Johns Hopkins University School of Hygiene and Pubflc Health All rights reserved Vol. 147, No. 8 Printed In U.SA. Epidemiology of Sarcopenia among
American Journal of Epidemiology Copyright O 1998 by The Johns Hopkins University School of Hygiene and Pubflc Health All rights reserved Vol. 147, No. 8 Printed In U.SA. Epidemiology of Sarcopenia among
A Population Based Risk Algorithm for the Development of Type 2 Diabetes: in the United States
 A Population Based Risk Algorithm for the Development of Type 2 Diabetes: Validation of the Diabetes Population Risk Tool (DPoRT) in the United States Christopher Tait PhD Student Canadian Society for
A Population Based Risk Algorithm for the Development of Type 2 Diabetes: Validation of the Diabetes Population Risk Tool (DPoRT) in the United States Christopher Tait PhD Student Canadian Society for
Nutrition for Family Living
 Susan Nitzke, Nutrition Specialist; [email protected] Sherry Tanumihardjo, Nutrition Specialist; [email protected] Amy Rettammel, Outreach Specialist; [email protected] Betsy Kelley,
Susan Nitzke, Nutrition Specialist; [email protected] Sherry Tanumihardjo, Nutrition Specialist; [email protected] Amy Rettammel, Outreach Specialist; [email protected] Betsy Kelley,
Our understanding of cancer cachexia in the past has focused on losses of
 Baracos Measurement of Lean Body Mass Using CT Scans Vickie Baracos, PhD Body Mass Index (BMI) and Weight Loss: Conventional Elements of How Cachexia and Nutritional Status Have Been Defined in Cancer
Baracos Measurement of Lean Body Mass Using CT Scans Vickie Baracos, PhD Body Mass Index (BMI) and Weight Loss: Conventional Elements of How Cachexia and Nutritional Status Have Been Defined in Cancer
Bipolar Disorder and Substance Abuse Joseph Goldberg, MD
 Diabetes and Depression in Older Adults: A Telehealth Intervention Julie E. Malphurs, PhD Asst. Professor of Psychiatry and Behavioral Science Miller School of Medicine, University of Miami Research Coordinator,
Diabetes and Depression in Older Adults: A Telehealth Intervention Julie E. Malphurs, PhD Asst. Professor of Psychiatry and Behavioral Science Miller School of Medicine, University of Miami Research Coordinator,
Upstate New York adults with diagnosed type 1 and type 2 diabetes and estimated treatment costs
 T H E F A C T S A B O U T Upstate New York adults with diagnosed type 1 and type 2 diabetes and estimated treatment costs Upstate New York Adults with diagnosed diabetes: 2003: 295,399 2008: 377,280 diagnosed
T H E F A C T S A B O U T Upstate New York adults with diagnosed type 1 and type 2 diabetes and estimated treatment costs Upstate New York Adults with diagnosed diabetes: 2003: 295,399 2008: 377,280 diagnosed
Improving Diabetes Care for All New Yorkers
 Improving Diabetes Care for All New Yorkers Lynn D. Silver, MD, MPH Assistant Commissioner Bureau of Chronic Disease Prevention and Control Diana K. Berger, MD, MSc Medical Director Diabetes Prevention
Improving Diabetes Care for All New Yorkers Lynn D. Silver, MD, MPH Assistant Commissioner Bureau of Chronic Disease Prevention and Control Diana K. Berger, MD, MSc Medical Director Diabetes Prevention
Shaping our future: a call to action to tackle the diabetes epidemic and reduce its economic impact
 Shaping our future: a call to action to tackle the diabetes epidemic and reduce its economic impact Task Force for the National Conference on Diabetes: The Task Force is comprised of Taking Control of
Shaping our future: a call to action to tackle the diabetes epidemic and reduce its economic impact Task Force for the National Conference on Diabetes: The Task Force is comprised of Taking Control of
Protein Intake in Potentially Insulin Resistant Adults: Impact on Glycemic and Lipoprotein Profiles - NPB #01-075
 Title: Protein Intake in Potentially Insulin Resistant Adults: Impact on Glycemic and Lipoprotein Profiles - NPB #01-075 Investigator: Institution: Gail Gates, PhD, RD/LD Oklahoma State University Date
Title: Protein Intake in Potentially Insulin Resistant Adults: Impact on Glycemic and Lipoprotein Profiles - NPB #01-075 Investigator: Institution: Gail Gates, PhD, RD/LD Oklahoma State University Date
How To Know Your Health
 Interpreting fitnessgram Results FITNESSGRAM uses criterion-referenced standards to evaluate fitness performance. These standards have been established to represent a level of fitness that offers some
Interpreting fitnessgram Results FITNESSGRAM uses criterion-referenced standards to evaluate fitness performance. These standards have been established to represent a level of fitness that offers some
Social Care and Obesity
 Social Care and Obesity A discussion paper Health, adult social care and ageing Introduction The number of obese people in England has been rising steadily for the best part of 20 years. Today one in four
Social Care and Obesity A discussion paper Health, adult social care and ageing Introduction The number of obese people in England has been rising steadily for the best part of 20 years. Today one in four
Grand V Challenge We must improve human health, nutrition and wellness of the U.S. population
 Grand V Challenge We must improve human health, nutrition and wellness of the U.S. population 1 Current Health Challenges Large health care costs(estimates range from $2.5 to $3 trillion in 2008 and 2009)
Grand V Challenge We must improve human health, nutrition and wellness of the U.S. population 1 Current Health Challenges Large health care costs(estimates range from $2.5 to $3 trillion in 2008 and 2009)
Trends in Bariatric Surgery for Morbid Obesity in Wisconsin
 Trends in Bariatric Surgery for Morbid Obesity in Wisconsin Jennifer L. Erickson, BA; Patrick L. Remington, MD, MPH; Paul E. Peppard, PhD ABSTRACT Background: Obesity is a national epidemic with rates
Trends in Bariatric Surgery for Morbid Obesity in Wisconsin Jennifer L. Erickson, BA; Patrick L. Remington, MD, MPH; Paul E. Peppard, PhD ABSTRACT Background: Obesity is a national epidemic with rates
http://www.cdc.gov/nchs.
 As the Nation s principal health statistics agency, the National Center for Health Statistics (NCHS) compiles statistical information to guide actions and policies to improve the health of the population.
As the Nation s principal health statistics agency, the National Center for Health Statistics (NCHS) compiles statistical information to guide actions and policies to improve the health of the population.
Nutrition Assessment. Miranda Kramer, RN, MS Nurse Practitioner/Clinical Nurse Specialist
 Nutrition Assessment Miranda Kramer, RN, MS Nurse Practitioner/Clinical Nurse Specialist General Considerations Overall caloric intake is it enough, too little or too much? What s in our calories fats,
Nutrition Assessment Miranda Kramer, RN, MS Nurse Practitioner/Clinical Nurse Specialist General Considerations Overall caloric intake is it enough, too little or too much? What s in our calories fats,
Adult Weight Management Training Summary
 Adult Weight Management Training Summary The Commission on Dietetic Registration, the credentialing agency for the Academy of Nutrition and Dietetics Marilyn Holmes, MS, RDN, LDN About This Presentation
Adult Weight Management Training Summary The Commission on Dietetic Registration, the credentialing agency for the Academy of Nutrition and Dietetics Marilyn Holmes, MS, RDN, LDN About This Presentation
Healthy Aging Lab: Current Research Abstracts
 Healthy Aging Lab: Current Research Abstracts Arsenic Exposure and Women s Health Environmental exposure to inorganic arsenic is an indisputable source of increased risk of several human cancers and chronic
Healthy Aging Lab: Current Research Abstracts Arsenic Exposure and Women s Health Environmental exposure to inorganic arsenic is an indisputable source of increased risk of several human cancers and chronic
Chapter 5 DASH Your Way to Weight Loss
 Chapter 5 DASH Your Way to Weight Loss The DASH diet makes it easy to lose weight. A healthy diet, one that is based on fruits, vegetables, and other key DASH foods, will help you have satisfying meals,
Chapter 5 DASH Your Way to Weight Loss The DASH diet makes it easy to lose weight. A healthy diet, one that is based on fruits, vegetables, and other key DASH foods, will help you have satisfying meals,
DIABETES MELLITUS. By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria
 DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
Are Men Losing Their Gonads?
 Are Men Losing Their Gonads? Andre B. Araujo, Ph.D. Director, Epidemiology New England Research Institutes Watertown, MA 02472 USA [email protected] NIA R01AG020727 Endocrine Society Annual Meeting
Are Men Losing Their Gonads? Andre B. Araujo, Ph.D. Director, Epidemiology New England Research Institutes Watertown, MA 02472 USA [email protected] NIA R01AG020727 Endocrine Society Annual Meeting
Smaller Waistlines, Sharper Minds, Stronger Bones and Healthier Hearts?
 Telephone: (212) 986-9415 Fax: (212) 697-8658 www.teausa.org 362 5th AVENUE, SUITE 801, NEW YORK, NY 10001 Smaller Waistlines, Sharper Minds, Stronger Bones and Healthier Hearts? New Findings Released
Telephone: (212) 986-9415 Fax: (212) 697-8658 www.teausa.org 362 5th AVENUE, SUITE 801, NEW YORK, NY 10001 Smaller Waistlines, Sharper Minds, Stronger Bones and Healthier Hearts? New Findings Released
Dietary treatment of cachexia challenges of nutritional research in cancer patients
 Dietary treatment of cachexia challenges of nutritional research in cancer patients Trude R. Balstad 4th International Seminar of the PRC and EAPC RN, Amsterdam 2014 Outline Cancer cachexia Dietary treatment
Dietary treatment of cachexia challenges of nutritional research in cancer patients Trude R. Balstad 4th International Seminar of the PRC and EAPC RN, Amsterdam 2014 Outline Cancer cachexia Dietary treatment
Appendix: Description of the DIETRON model
 Appendix: Description of the DIETRON model Much of the description of the DIETRON model that appears in this appendix is taken from an earlier publication outlining the development of the model (Scarborough
Appendix: Description of the DIETRON model Much of the description of the DIETRON model that appears in this appendix is taken from an earlier publication outlining the development of the model (Scarborough
Southern Grampians & Glenelg Shires COMMUNITY PROFILE
 Southern Grampians & Glenelg Shires COMMUNITY PROFILE Contents: 1. Health Status 2. Health Behaviours 3. Public Health Issues 4. References This information was last updated on 14 February 2007 1. Health
Southern Grampians & Glenelg Shires COMMUNITY PROFILE Contents: 1. Health Status 2. Health Behaviours 3. Public Health Issues 4. References This information was last updated on 14 February 2007 1. Health
16. ARTHRITIS, OSTEOPOROSIS, AND CHRONIC BACK CONDITIONS
 16. ARTHRITIS, OSTEOPOROSIS, AND CHRONIC BACK CONDITIONS Goal Reduce the impact of several major musculoskeletal conditions by reducing the occurrence, impairment, functional limitations, and limitation
16. ARTHRITIS, OSTEOPOROSIS, AND CHRONIC BACK CONDITIONS Goal Reduce the impact of several major musculoskeletal conditions by reducing the occurrence, impairment, functional limitations, and limitation
SAMA Working Paper: POPULATION AGING IN SAUDI ARABIA. February 2015. Hussain I. Abusaaq. Economic Research Department. Saudi Arabian Monetary Agency
 WP/15/2 SAMA Working Paper: POPULATION AGING IN SAUDI ARABIA February 2015 By Hussain I. Abusaaq Economic Research Department Saudi Arabian Monetary Agency Saudi Arabian Monetary Agency The views expressed
WP/15/2 SAMA Working Paper: POPULATION AGING IN SAUDI ARABIA February 2015 By Hussain I. Abusaaq Economic Research Department Saudi Arabian Monetary Agency Saudi Arabian Monetary Agency The views expressed
Prevention of and the Screening for Diabetes Part I Insulin Resistance By James L. Holly, MD Your Life Your Health The Examiner January 19, 2012
 Prevention of and the Screening for Diabetes Part I Insulin Resistance By James L. Holly, MD Your Life Your Health The Examiner January 19, 2012 In 2002, SETMA began a relationship with Joslin Diabetes
Prevention of and the Screening for Diabetes Part I Insulin Resistance By James L. Holly, MD Your Life Your Health The Examiner January 19, 2012 In 2002, SETMA began a relationship with Joslin Diabetes
Body Mass Index Measurement in Schools BMI. Executive Summary
 Body Mass Index Measurement in Schools BMI = BMI weight(kg) {height(m)} 2 Executive Summary Centers for Disease Control and Prevention National Center for Chronic Disease Prevention and Health Promotion
Body Mass Index Measurement in Schools BMI = BMI weight(kg) {height(m)} 2 Executive Summary Centers for Disease Control and Prevention National Center for Chronic Disease Prevention and Health Promotion
PEM. Criteria for sarcopenia - adopted by ESPEN/EUGMS/IAGG/IANA. muscle mass walking speed. Cachexia. Sarcopenia a novel concept for an old problem
 Sarcopenia and sarcopenic obesity one old and one new ageing problem Overlapping catabolic conditions in ill and old adults Tommy Cederholm, MD, PhD, Prof Clinical Nutrition and Metabolism, Uppsala University
Sarcopenia and sarcopenic obesity one old and one new ageing problem Overlapping catabolic conditions in ill and old adults Tommy Cederholm, MD, PhD, Prof Clinical Nutrition and Metabolism, Uppsala University
SIOG Guidelines Update 2014 Prostate Cancer. Dr Helen Boyle Centre Léon Bérard SIOG meeting 25 October 2014,Lisbon
 SIOG Guidelines Update 2014 Prostate Cancer Dr Helen Boyle Centre Léon Bérard SIOG meeting 25 October 2014,Lisbon Droz JP, Aapro M, Balducci L, Boyle H, Van den Broeck T, Cathcart P, Dickinson L, Efstathiou
SIOG Guidelines Update 2014 Prostate Cancer Dr Helen Boyle Centre Léon Bérard SIOG meeting 25 October 2014,Lisbon Droz JP, Aapro M, Balducci L, Boyle H, Van den Broeck T, Cathcart P, Dickinson L, Efstathiou
Medical Fitness. Annual Meeting December 2012. By: Deb Riggs, MEd, General Manager
 Exercise is Medicine Referral Process Utilizing an EMR Medical Fitness Association Annual Meeting December 2012 By: Deb Riggs, MEd, General Manager Faculty Disclosure Deb Riggs Deb Riggs has listed no
Exercise is Medicine Referral Process Utilizing an EMR Medical Fitness Association Annual Meeting December 2012 By: Deb Riggs, MEd, General Manager Faculty Disclosure Deb Riggs Deb Riggs has listed no
HEALTH CARE COSTS 11
 2 Health Care Costs Chronic health problems account for a substantial part of health care costs. Annually, three diseases, cardiovascular disease (including stroke), cancer, and diabetes, make up about
2 Health Care Costs Chronic health problems account for a substantial part of health care costs. Annually, three diseases, cardiovascular disease (including stroke), cancer, and diabetes, make up about
Wellness for People with MS: What do we know about Diet, Exercise and Mood And what do we still need to learn? March 2015
 Wellness for People with MS: What do we know about Diet, Exercise and Mood And what do we still need to learn? March 2015 Introduction Wellness and the strategies needed to achieve it is a high priority
Wellness for People with MS: What do we know about Diet, Exercise and Mood And what do we still need to learn? March 2015 Introduction Wellness and the strategies needed to achieve it is a high priority
Master of Science. Obesity and Weight Management
 Department of Clinical Sciences and Nutrition Master of Science in Obesity and Weight Management Dublin Part-Time Taught Modular Masters Programme Module Descriptor Outlines XN7201 The Obesity Epidemic
Department of Clinical Sciences and Nutrition Master of Science in Obesity and Weight Management Dublin Part-Time Taught Modular Masters Programme Module Descriptor Outlines XN7201 The Obesity Epidemic
TABLE OF CONTENTS. The Cost of Diabesity... 3. Employer Solutions... 4 Provide a Worksite Weight Loss Program Tailored for Diabetes...
 TH E TABLE OF CONTENTS The Cost of Diabesity... 3 Employer Solutions... 4 Provide a Worksite Weight Loss Program Tailored for Diabetes... 4 Provide Healthy Food Options at the Workplace... 4 Make it Easy
TH E TABLE OF CONTENTS The Cost of Diabesity... 3 Employer Solutions... 4 Provide a Worksite Weight Loss Program Tailored for Diabetes... 4 Provide Healthy Food Options at the Workplace... 4 Make it Easy
Preventing Pediatric Diabetes: Are Racial Disparities A Factor? A Children s Health Fund Issue Brief February 2004
 Preventing Pediatric Diabetes: Are Racial Disparities A Factor? A Children s Health Fund Issue Brief February 2004 The Children s Health Fund The Children s Health Fund (CHF), working with hospitals and
Preventing Pediatric Diabetes: Are Racial Disparities A Factor? A Children s Health Fund Issue Brief February 2004 The Children s Health Fund The Children s Health Fund (CHF), working with hospitals and
Advancing institutional dietetics and school nutrition programs in Korea
 352 Asia Pac J Clin Nutr 28;17 (S1):352-356 Review Article Advancing institutional dietetics and school nutrition programs in Korea Tong-Kyung Kwak PhD 1 and Hye-Ja Chang PhD 2 1 Yonsei University, Department
352 Asia Pac J Clin Nutr 28;17 (S1):352-356 Review Article Advancing institutional dietetics and school nutrition programs in Korea Tong-Kyung Kwak PhD 1 and Hye-Ja Chang PhD 2 1 Yonsei University, Department
Obesity and Socioeconomic Status in Children and Adolescents: United States, 2005 2008
 Obesity and Socioeconomic Status in Children and Adolescents: United States, 2005 2008 Cynthia L. Ogden, Ph.D.; Molly M. Lamb, Ph.D.; Margaret D. Carroll, M.S.P.H.; and Katherine M. Flegal, Ph.D. Key findings
Obesity and Socioeconomic Status in Children and Adolescents: United States, 2005 2008 Cynthia L. Ogden, Ph.D.; Molly M. Lamb, Ph.D.; Margaret D. Carroll, M.S.P.H.; and Katherine M. Flegal, Ph.D. Key findings
adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes
 Why Eccentrics? What is it? Eccentric adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes Eccentrics is a type of muscle contraction that occurs as the
Why Eccentrics? What is it? Eccentric adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes Eccentrics is a type of muscle contraction that occurs as the
Sedentarity and Exercise in the Canadian Population. Angelo Tremblay Division of kinesiology
 Sedentarity and Exercise in the Canadian Population Angelo Tremblay Division of kinesiology Disclosure of Potential Conflicts of Interest Évolution de la pratique d activité physique des adultes canadiens
Sedentarity and Exercise in the Canadian Population Angelo Tremblay Division of kinesiology Disclosure of Potential Conflicts of Interest Évolution de la pratique d activité physique des adultes canadiens
Epidemiology of Hypertension 陈 奕 希 3120000591 李 禾 园 3120000050 王 卓 3120000613
 Epidemiology of Hypertension 陈 奕 希 3120000591 李 禾 园 3120000050 王 卓 3120000613 1 Definition Hypertension is a chronic medical condition in which the blood pressure in the arteries is elevated. 2 Primary
Epidemiology of Hypertension 陈 奕 希 3120000591 李 禾 园 3120000050 王 卓 3120000613 1 Definition Hypertension is a chronic medical condition in which the blood pressure in the arteries is elevated. 2 Primary
Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy
 Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy Judith Long, MD,RWJCS Perelman School of Medicine Philadelphia Veteran Affairs Medical Center Background Objective Overview Methods
Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy Judith Long, MD,RWJCS Perelman School of Medicine Philadelphia Veteran Affairs Medical Center Background Objective Overview Methods
Forty to fifty million US adults do not meet recommended physical activity levels. Like
 Billing and Coding for Physical Activity Counseling Elizabeth Joy, MD, MPH, FACSM Medical Director, Outcomes Research Intermountain Healthcare Professor, Family and Preventive Medicine University of Utah
Billing and Coding for Physical Activity Counseling Elizabeth Joy, MD, MPH, FACSM Medical Director, Outcomes Research Intermountain Healthcare Professor, Family and Preventive Medicine University of Utah
Diabetes mellitus is a chronic condition that occurs as a result of problems with the production and/or action of insulin in the body.
 International Diabetes Federation Diabetes Background Information Diabetes mellitus is a chronic condition that occurs as a result of problems with the production and/or action of insulin in the body.
International Diabetes Federation Diabetes Background Information Diabetes mellitus is a chronic condition that occurs as a result of problems with the production and/or action of insulin in the body.
This is an electronic reprint of the original article. This reprint may differ from the original in pagination and typographic detail.
 This is an electronic reprint of the original article. This reprint may differ from the original in pagination and typographic detail. Author(s): Viljanen, Anne; Mikkola, Tuija; Rantakokko, Merja; Kauppinen,
This is an electronic reprint of the original article. This reprint may differ from the original in pagination and typographic detail. Author(s): Viljanen, Anne; Mikkola, Tuija; Rantakokko, Merja; Kauppinen,
Prevention Status Report 2013
 The Prevention Status Reports (PSRs) highlight for all 50 states and the District of Columbia the status of public health policies and practices designed to prevent or reduce important health problems.
The Prevention Status Reports (PSRs) highlight for all 50 states and the District of Columbia the status of public health policies and practices designed to prevent or reduce important health problems.
Principles of Sports Nutrition
 Principles of Sports Nutrition Student Education Program Course Outline CHI Sports Nutrition Education Program Course Title: Course Hours: Principles of Sports Nutrition (PSN) 24 12 weeks (12 - two hour
Principles of Sports Nutrition Student Education Program Course Outline CHI Sports Nutrition Education Program Course Title: Course Hours: Principles of Sports Nutrition (PSN) 24 12 weeks (12 - two hour
Summary Evaluation of the Medicare Lifestyle Modification Program Demonstration and the Medicare Cardiac Rehabilitation Benefit
 The Centers for Medicare & Medicaid Services' Office of Research, Development, and Information (ORDI) strives to make information available to all. Nevertheless, portions of our files including charts,
The Centers for Medicare & Medicaid Services' Office of Research, Development, and Information (ORDI) strives to make information available to all. Nevertheless, portions of our files including charts,
Against the Growing Burden of Disease. Kimberly Elmslie Director General, Centre for Chronic Disease Prevention
 Kimberly Elmslie Director General, Centre for Chronic Disease Prevention Chronic diseases are an increasing global challenge Most significant cause of death (63%) worldwide 1 Chronic diseases cause premature
Kimberly Elmslie Director General, Centre for Chronic Disease Prevention Chronic diseases are an increasing global challenge Most significant cause of death (63%) worldwide 1 Chronic diseases cause premature
DIET AND EXERCISE STRATEGIES FOR WEIGHT LOSS AND WEIGHT MAINTENANCE
 DIET AND EXERCISE STRATEGIES FOR WEIGHT LOSS AND WEIGHT MAINTENANCE 40 yo woman, BMI 36. Motivated to begin diet therapy. Which of the following is contraindicated: Robert B. Baron MD MS Professor and
DIET AND EXERCISE STRATEGIES FOR WEIGHT LOSS AND WEIGHT MAINTENANCE 40 yo woman, BMI 36. Motivated to begin diet therapy. Which of the following is contraindicated: Robert B. Baron MD MS Professor and
Educational Attainment of Veterans: 2000 to 2009
 Educational Attainment of Veterans: to 9 January 11 NCVAS National Center for Veterans Analysis and Statistics Data Source and Methods Data for this analysis come from years of the Current Population Survey
Educational Attainment of Veterans: to 9 January 11 NCVAS National Center for Veterans Analysis and Statistics Data Source and Methods Data for this analysis come from years of the Current Population Survey
The benefits of prevention: healthy eating and active living
 The benefits of prevention: healthy eating and active living A Summary of Findings By increasing the proportion of the NSW population who are a healthy weight by 2018 (so that one in two adults are of
The benefits of prevention: healthy eating and active living A Summary of Findings By increasing the proportion of the NSW population who are a healthy weight by 2018 (so that one in two adults are of
Does referral from an emergency department to an. alcohol treatment center reduce subsequent. emergency room visits in patients with alcohol
 Does referral from an emergency department to an alcohol treatment center reduce subsequent emergency room visits in patients with alcohol intoxication? Robert Sapien, MD Department of Emergency Medicine
Does referral from an emergency department to an alcohol treatment center reduce subsequent emergency room visits in patients with alcohol intoxication? Robert Sapien, MD Department of Emergency Medicine
Facts about Diabetes in Massachusetts
 Facts about Diabetes in Massachusetts Diabetes is a disease in which the body does not produce or properly use insulin (a hormone used to convert sugar, starches, and other food into the energy needed
Facts about Diabetes in Massachusetts Diabetes is a disease in which the body does not produce or properly use insulin (a hormone used to convert sugar, starches, and other food into the energy needed
The Effects of Participation in Marching Band on Physical Activity and Physical Fitness in College Aged Men and Women
 University of Rhode Island DigitalCommons@URI Senior Honors Projects Honors Program at the University of Rhode Island 2013 The Effects of Participation in Marching Band on Physical Activity and Physical
University of Rhode Island DigitalCommons@URI Senior Honors Projects Honors Program at the University of Rhode Island 2013 The Effects of Participation in Marching Band on Physical Activity and Physical
Type 1 Diabetes ( Juvenile Diabetes)
 Type 1 Diabetes W ( Juvenile Diabetes) hat is Type 1 Diabetes? Type 1 diabetes, also known as juvenile-onset diabetes, is one of the three main forms of diabetes affecting millions of people worldwide.
Type 1 Diabetes W ( Juvenile Diabetes) hat is Type 1 Diabetes? Type 1 diabetes, also known as juvenile-onset diabetes, is one of the three main forms of diabetes affecting millions of people worldwide.
The Cost of Pain and Economic Burden of Prescription Misuse, Abuse and Diversion. Angela Huskey, PharmD, CPE
 The Cost of Pain and Economic Burden of Prescription Misuse, Abuse and Diversion Angela Huskey, PharmD, CPE Case Bill is a 47 year old man with a history of low back pain and spinal stenosis Not a real
The Cost of Pain and Economic Burden of Prescription Misuse, Abuse and Diversion Angela Huskey, PharmD, CPE Case Bill is a 47 year old man with a history of low back pain and spinal stenosis Not a real
Benefits of a Working Relationship Between Medical and Allied Health Practitioners and Personal Fitness Trainers
 Benefits of a Working Relationship Between Medical and Allied Health Practitioners and Personal Fitness Trainers Introduction The health benefits of physical activity have been documented in numerous scientific
Benefits of a Working Relationship Between Medical and Allied Health Practitioners and Personal Fitness Trainers Introduction The health benefits of physical activity have been documented in numerous scientific
on a daily basis. On the whole, however, those with heart disease are more limited in their activities, including work.
 Heart Disease A disabling yet preventable condition Number 3 January 2 NATIONAL ACADEMY ON AN AGING SOCIETY Almost 18 million people 7 percent of all Americans have heart disease. More than half of the
Heart Disease A disabling yet preventable condition Number 3 January 2 NATIONAL ACADEMY ON AN AGING SOCIETY Almost 18 million people 7 percent of all Americans have heart disease. More than half of the
The affordability of healthy eating for low-income households
 Policy Briefing October 2009 The affordability of healthy eating for low-income households Introduction Healthy Food for All is an all-island multiagency initiative which seeks to combat food poverty by
Policy Briefing October 2009 The affordability of healthy eating for low-income households Introduction Healthy Food for All is an all-island multiagency initiative which seeks to combat food poverty by
Coronary Heart Disease (CHD) Brief
 Coronary Heart Disease (CHD) Brief What is Coronary Heart Disease? Coronary Heart Disease (CHD), also called coronary artery disease 1, is the most common heart condition in the United States. It occurs
Coronary Heart Disease (CHD) Brief What is Coronary Heart Disease? Coronary Heart Disease (CHD), also called coronary artery disease 1, is the most common heart condition in the United States. It occurs
Trends in Bariatric Surgery for Morbid Obesity. in Wisconsin
 Trends in Bariatric Surgery for Morbid Obesity in Wisconsin Jennifer L. Erickson, B.A. Patrick L. Remington, M.D., M.P.H. Paul E. Peppard, PhD A Working Paper of the Wisconsin Public Health and Health
Trends in Bariatric Surgery for Morbid Obesity in Wisconsin Jennifer L. Erickson, B.A. Patrick L. Remington, M.D., M.P.H. Paul E. Peppard, PhD A Working Paper of the Wisconsin Public Health and Health
Fast Facts on Osteoporosis
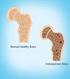 Fast Facts on Osteoporosis Definition Prevalence Osteoporosis, or porous bone, is a disease characterized by low bone mass and structural deterioration of bone tissue, leading to bone fragility and an
Fast Facts on Osteoporosis Definition Prevalence Osteoporosis, or porous bone, is a disease characterized by low bone mass and structural deterioration of bone tissue, leading to bone fragility and an
Osteoporosis has been identified by the US Surgeon General
 New Guidelines for the Prevention and Treatment of Osteoporosis E. Michael Lewiecki, MD, and Nelson B. Watts, MD Abstract: The World Health Organization Fracture Risk Assessment Tool (FRAX ) and the National
New Guidelines for the Prevention and Treatment of Osteoporosis E. Michael Lewiecki, MD, and Nelson B. Watts, MD Abstract: The World Health Organization Fracture Risk Assessment Tool (FRAX ) and the National
Adult Physical Activity
 NOO data factsheet Adult Physical Activity November 2012 Key points According to the Health Survey for England (self-reported data), 39% of men and 29% of women met the government s physical activity recommendations
NOO data factsheet Adult Physical Activity November 2012 Key points According to the Health Survey for England (self-reported data), 39% of men and 29% of women met the government s physical activity recommendations
Osteoporosis/Bone Health in Adults as a National Public Health Priority
 Position Statement Osteoporosis/Bone Health in Adults as a National Public Health Priority This Position Statement was developed as an educational tool based on the opinion of the authors. It is not a
Position Statement Osteoporosis/Bone Health in Adults as a National Public Health Priority This Position Statement was developed as an educational tool based on the opinion of the authors. It is not a
Include Dietitian Services in Extended Health Care Plan
 Include Dietitian Services in Extended Health Care Plan It s cost-effective JUNE 2015 The Problem Your employees extended health care plan does not appear to include dietitian services as an option despite
Include Dietitian Services in Extended Health Care Plan It s cost-effective JUNE 2015 The Problem Your employees extended health care plan does not appear to include dietitian services as an option despite
Objectives. What is undernutrition? What is undernutrition? What does undernutrition look like?
 Objectives Basics Jean-Pierre Habicht, MD, PhD Professor Division of Nutritional Sciences Cornell University Types and causes Determinants Consequences Global occurrence and progress Way forward What is
Objectives Basics Jean-Pierre Habicht, MD, PhD Professor Division of Nutritional Sciences Cornell University Types and causes Determinants Consequences Global occurrence and progress Way forward What is
