Position Statement of the National Lymphedema Network
|
|
|
- Bertram Kelley
- 10 years ago
- Views:
Transcription
1 Position Statement of the National Lymphedema Network By: NLN Medical Advisory Committee Revised May 2012 TOPIC: Lymphedema Risk Reduction Practices Lymphedema is the accumulation of protein-rich fluid in tissues with inadequate lymphatic drainage. It is not known why some people with the same risk factors develop lymphedema and others do not. An underlying predisposition to developing lymphedema may be a contributing factor. 1, 2, 3 Scientific evidence is lacking regarding risk reduction practices 4, 5, how to reduce the risk of developing lymphedema, or how to minimize flares of lymphedema. Many recommendations for risk reduction are common sense approaches based on the body s anatomy and physiology. Because of individual variations in anatomy and because lymphedema may be caused by many different factors, each person with lymphedema or at risk for lymphedema needs to have their risk-reduction practices individualized. What works for one person may not work for another. Based on practical experience, there are some reasonable actions and precautions to be taken for individuals with or at risk for lymphedema. Lymphedema is a progressive condition without a cure; caution should be exercised to reduce the risk of developing or exacerbating lymphedema. This position paper provides information to assist the person with or at risk for lymphedema to make the best possible and most informed choices about risk-reduction practices. If you are not clear about your own risks, meet with a treatment provider who is knowledgeable about lymphedema to discuss your personal strategies for risk reduction. This paper differentiates people with a confirmed diagnosis of lymphedema 6 from people at risk of lymphedema. People at risk of lymphedema are individuals who have not yet displayed the signs and symptoms of lymphedema but have a known insufficiency of their lymphatic system. This includes people who have undergone removal of lymph nodes or radiation therapy, which increases the risk for developing lymphedema. At-risk individuals have altered lymphatic function that may impede the body s ability to take up excess fluids in the tissues. People with a confirmed diagnosis of lymphedema should consider the following actions and precautions: 1. Medical check-ups: Have regular follow-ups by professionals with training in lymphedema. The follow-up schedule should be based on your individual situation and determined by your lymphedema care provider. 2. Reporting changes: Report to your health care provider any change in your lymphedema, such as increase in size, change in sensation, color, temperature, or skin condition. If your weight or size of lymphedema body part changes, seek assistance from a lymphedema professional to determine if a new course of therapy or new garment is needed. 3. Body weight: Obesity is known to be a major risk factor for lymphedema 7, 8, 9. A person with lymphedema should maintain a normal body weight and seek professional help to lose weight if your weight is above standard recommended guidelines. In one study, lymphedema treatment was more effective if combined with weight loss. 10 People who do not know their recommended weight for age and height should seek information from a health care provider.
2 Page 2 of 8 4. Exercise: Follow recommendations on exercise for lymphedema 11, as specific forms of exercise have been shown to benefit lymphedema. 12 Incorrect or unsafe exercise may exacerbate lymphedema Compression garments: If you wear compression garments for control of lymphedema, follow the manufacturer s care recommendations. Replace the garment as recommended. Wear your usual compression garments for air travel, exercise, and exertion. 11, Infections (cellulitis): Treat all episodes of cellulitis (infection in subcutaneous tissue) as an urgent medical situation. Know the signs and symptoms of cellulitis skin infection in an area of impaired lymph drainage (signs may include redness, warmth, pain, fever, and feeling of overall illness or flu-like symptoms). 14 Cellulitis episodes may lead to worsening lymphedema. 15 If you have more than three episodes of cellulitis in a year, 14, 16 discuss with a health care provider whether your situation warrants using suppressive antibiotics. 7. Skin care: Maintain skin in good condition 17 with proper hygiene. Regularly use a moisturizer to avoid skin cracking. If you wear garments, ask your fitter or the manufacturer for information on whether you can use lotion with your garments and what type of lotion is best. Some lotions affect the fibers of compression garments. 8. Trauma: Avoid trauma to the affected area. 15 Trauma includes any situation that might typically cause swelling in a person without lymphedema, but may lead to prolonged swelling in the area of impaired lymphatic drainage. a. Protect against falls, fractures, and serious burns. 18, 19 If any of these occur, perform first aid or seek emergency care as appropriate. After the emergency is controlled, if there is prolonged edema, contact a lymphedema provider. b. If required to have venipuncture, inform the phlebotomist of your lymphedema, and use a non-lymphedema limb, if possible. 20 If not possible, inform the phlebotomist of your lymphedema condition and ask for the most experienced phlebotomist. Do not allow multiple or traumatic searches for veins, which can increase tissue edema. If a traumatic venipuncture occurs on a lymphedema extremity, immediately wash the area, apply a cold pack, then elevate until edema subsides. If it does not subside in 24 hours, contact your lymphedema provider. c. For scratches, punctures, breaks in the skin of the lymphedema part, wash with soap and water, pat dry, then apply a topical antibacterial. d. Wear non-constricting protective gear over the affected part when doing an activity that could lead to puncture or trauma, e.g., shoes and socks, protective gloves or sleeves when gardening or working with animals that scratch or bite. Ask your lymphedema provider for specifics for your lymphedema. e. Nail care may need to be done by professionals, especially toenails. For leg lymphedema, toenails may need to be trimmed by a podiatrist. Fungal infections should be treated and foot hygiene maintained. For arm lymphedema, good hand hygiene and softening the cuticles with proper cuticle moisturizer is recommended. Be careful with manicures; use clean instruments and avoid cutting cuticles. 9. Constriction: Avoid excessive or prolonged constriction of the affected part. Excessive constriction refers to tightening or squeezing in a manner that restricts lymph flow through that area or causes tissue trauma. Examples of excessive constriction include improperly fitting compression garments and clothing (tight sleeves on a lymphedema arm, tight stockings on a lymphedema leg, tight bra, or excessive pressure from an underwire on chest or breast lymphedema). Clothing and garments should be supportive and have smooth compression. Blood pressure cuffs used improperly or with extreme pressure may excessively constrict tissues (see controversies below).
3 Page 3 of Heat and cold: Avoid exposure to extreme heat or cold 15 to the extent that tissue injury could occur such as burn or frostbite (see controversies below). 11. Surgery: If you need to have surgery on an area with lymphedema, inform your surgeon of your lymphedema condition. You may wish to meet with a lymphedema provider prior to your surgery to have a post-operative lymphedema care plan in case the lymphedema worsens after surgery. If lymphedema does not worsen after surgery, resume your prior care of lymphedema. 12. Stasis: People with leg lymphedema should avoid conditions which cause stasis. Stasis refers to sitting or standing for a long period of time without moving, changing position, or elevating the legs. In a survey study of 89 women with confirmed lymphedema after gynecologic cancer, 46 percent identified prolonged sitting in one position or standing as a major factor exacerbating lymphedema. 15 Many people who do not have lymphedema experience swelling in the legs with conditions of stasis. It is a theoretical greater risk for people who have impaired lymphatic drainage that may not be able to remove excess accumulated fluid in the legs due to prolonged sitting and standing. Moving, changing position, and exercising periodically throughout the day are recommended for people with leg lymphedema. 13. Varicose veins: People with leg lymphedema who also have varicose veins need to check with a health care provider to determine if varicose vein treatment is recommended. For some individuals with lymphedema, treating varicose veins can reduce the lymphatic load of fluid in the tissues and improve the lymphedema management. 14. Air Travel: Air travel is associated with a risk of venous thromboembolism (blood clot in the veins, or VTE) on long flights for people with and without lymphedema. 13 The risk of VTE from long-haul air travel is believed to be caused by low cabin pressure combined with lowered oxygen levels, dehydration, and lack of movement. It is unclear whether people with lymphedema have more risk of VTE than the general population (see controversies below). In one study of 89 gynecologic cancer survivors, stasis and air travel were associated with flares of leg lymphedema. 15 It is recommended for people with lymphedema to wear their usual compression garments for air travel. It is equally as important to move around, exercise the affected body part, and maintain good hydration during air travel. People at-risk for developing lymphedema should consider the following actions and precautions: 1. Medical check-ups: Medical check-ups or screening for lymphedema is recommended. 21 Individuals at risk for breast cancer-related lymphedema should follow the recommendations outlined in the National Lymphedema Network s Position Paper on Screening and Measurement for Early Detection of Breast Cancer Related LE (BCRL). 21 In other at-risk individuals, a follow-up schedule should be based on your individual situation and determined by your lymphedema care provider. 2. Reporting changes: Report to your health care provider any change in your at-risk body part, such as increase in size, change in sensation, color, temperature, or skin condition. Diagnosing and treating the onset of lymphedema at the earliest possible time improves outcomes Body weight: Obesity is known to be a major risk factor for lymphedema 7, 8, 9. A person at risk for lymphedema should maintain a normal body weight and seek professional help to lose weight if their weight is above standard recommended guidelines. People who do not know their recommended weight for age and height should seek information from a health care provider. 4. Exercise: Follow recommendations on exercise for lymphedema, 11 as specific forms of exercise may reduce the risk of developing lymphedema. 12 Incorrect or unsafe exercise may increase the risk of lymphedema. 11
4 Page 4 of 8 5. Compression garments: Consider the pros and cons of wearing compression garments during air travel before making a decision (see controversies below). Wearing compression garments during exercise is probably unnecessary unless you have noticed that swelling occurs during exercise, if exercise is more intense than usual, or in cases of significant over-activity. 22 There is no clear guidance on this area of risk reduction; discuss your concerns with a lymphedema provider. 6. Infections (cellulitis): Treat all episodes of cellulitis (infection in subcutaneous tissue) in the at-risk body part as an urgent medical situation. Know the signs and symptoms of cellulitis skin infection in an area of impaired lymph drainage (signs may include redness, warmth, pain, fever, and feeling of overall illness or flu-like symptoms). 14 Cellulitis episodes in the at-risk body part may lead to the onset of lymphedema Skin care: Maintain skin in good condition 17 with proper hygiene and regularly use a moisturizer to avoid skin cracking. 8. Trauma: Avoid trauma to the at-risk area. 15 Trauma includes any situation that might typically cause swelling in a person without lymphedema, but may lead to prolonged swelling in the area of impaired lymphatic drainage. a. Protect against falls, fractures, and serious burns. If any of these occur, perform first aid or seek emergency care as appropriate. After the emergency is controlled, if there is prolonged edema, contact a lymphedema provider. b. If required to have venipuncture, inform the phlebotomist of your lymphedema risk and use a not-at-risk limb if possible. 20 If not possible, inform the phlebotomist of your lymphedema risk condition and ask for the most experienced phlebotomist. Do not allow multiple or traumatic searches for veins, which can increase tissue edema. If a traumatic venipuncture on an at-risk lymphedema extremity occurs, immediately wash the area, apply a cold pack, and then elevate until edema subsides. If it does not subside in 24 hours, contact your lymphedema provider. c. For scratches, punctures, breaks in the skin of the at-risk body part, wash with soap and water, pat dry, then apply a topical antibacterial. d. Wear non-constricting protective gear over the a- risk body part when doing an activity that could lead to puncture or trauma, e.g., shoes and socks, protective gloves or sleeves when gardening or working with animals that scratch or bite. Ask your lymphedema provider for specifics for your lymphedema. e. Consider having nail care done by professionals, especially toenails. For people with risk of leg lymphedema, toenails may need to be trimmed by a podiatrist. Fungal infections should be treated and foot hygiene maintained. For people at-risk for arm lymphedema, good hand hygiene and softening the cuticles with proper cuticle moisturizer is recommended. Be careful with manicures; use clean instruments and avoid cutting cuticles. 9. Constriction: Avoid excessive or prolonged constriction of the at-risk body part. Excessive constriction refers to tightening or squeezing in a manner that restricts lymph flow through that area or causes tissue trauma. Examples of excessive constriction include improperly fitting compression garments and clothing (tight sleeves on a lymphedema arm, tight stockings on a lymphedema leg, tight bra, or excessive pressure from an underwire on chest or breast lymphedema). Clothing and garments should be supportive and have smooth compression. Blood pressure cuffs used improperly or with extreme pressure may excessively constrict tissues (see controversies below). 10. Heat and cold: Avoid exposure to extreme heat or cold 15 to the extent that tissue injury could occur, such as burn or frostbite (see controversies below).
5 Page 5 of Surgery: If you need to have surgery on an area at risk for lymphedema, inform your surgeon of your risk for lymphedema. Ask your surgeon how long swelling is usually present after your type of surgery. You may wish to meet with a lymphedema provider prior to your surgery to have a post-operative lymphedema care plan in case of prolonged or excessive post-operative swelling. After surgery, if you experience prolonged or excessive swelling, notify your surgeon and request a referral to a lymphedema provider. 12. Stasis: People at risk for leg lymphedema should avoid conditions which cause stasis. Stasis refers to sitting or standing for a long period of time without moving, changing position, or elevating the legs. It is unknown if stasis can precipitate the onset of lymphedema in the at-risk leg. Many people who do not have lymphedema experience swelling in the legs with conditions of stasis. Sitting or standing for too long an interval could theoretically increase the risk for lymphedema in people who have impaired lymphatic drainage. This is because an impaired lymphatic system may not be able to remove excess fluid in the legs that accumulates during these long periods of sitting or standing. Moving, changing position, and exercising periodically throughout the day are recommended for people at risk for lymphedema of the leg. In a survey study of 89 women with confirmed lymphedema after gynecologic cancer, 46 percent identified prolonged sitting in one position or standing as a major factor exacerbating lymphedema Varicose Veins: For individuals at risk for leg lymphedema, varicose veins and postural swelling can be managed by wearing support stockings. If edema worsens, contact your health care provider. 14. Air Travel: Air travel is associated with a risk of venous thromboembolism (blood clot in veins, or VTE) on long flights for people with and without lymphedema. 13 The risk of VTE from long-haul air travel is believed to be caused by low cabin pressure combined with lowered oxygen levels, dehydration, and lack of movement. 13 It is not known whether people at risk for lymphedema have more risk of VTE than the general population. The risk of precipitating the onset of lymphedema during air travel for people with lymphedema is unclear (see controversies below). It is recommended that people with lymphedema review the pros and cons of wearing prophylactic compression during air travel (detailed in the controversies section of this paper) and make an informed personal decision. Regardless of the use of prophylactic compression, it is important to move around, exercise the at-risk body part, and maintain good hydration during air travel. 13 Controversies regarding risk reduction practices: 1. Air travel: There is little evidence that lymphedema is caused or worsened by air travel. There is a theoretical risk of swelling in the at-risk area on an airplane because of reduced cabin pressure. Stasis, or lack of movement, can cause swelling or venous blood clots during air travel for people with or without lymphedema. 13 There are isolated case reports of people with or at risk for lymphedema who have developed swelling after air travel. 23, 15 One study showed that physically fit women at risk for breast cancer-related lymphedema had no increase in swelling from air travel. 24 Another study showed that prophylactic compression had the potential to make swelling worse. 25 The NLN cannot specifically recommend or not recommend compression garments for prophylaxis in at-risk people who have not yet developed lymphedema. People at risk for lymphedema who decide to wear prophylactic compression on airplanes should work with an experienced garment fitter and should not self-purchase a garment. The person who chooses to wear prophylactic compression on an airplane should wear the garment several times prior to air travel to make sure the garment fits well and has no areas of constriction. If, while wearing a garment on an airplane, the swelling increases or the garment constricts, remove it immediately. It is recommended that people with a confirmed diagnosis of lymphedema wear properly fitting compression garments for air travel. 2. Blood pressure cuffs: Studies have not determined the actual risk of having BP taken on the at-risk arm. Some feel that an isolated, low-pressure, and brief BP assessment is unlikely to cause or worsen lymphedema. Some authors have claimed that because compression is used for lymphedema treatment, BP cuffs and air compression devices are safe. 5, 26 This is an erroneous conclusion due to the following
6 Page 6 of 8 considerations: a. Pneumatic compression devices used for lymphedema treatment are sequential, gradient compression; b. BP cuffs and tourniquets are high pressure focal compression that can lead to excessive constriction if not properly used; c. User-error with high-pressure BP machines repetitively cycling is quite different from a hand BP device pumped up to just a little higher than the usual upper level BP. Because lymphedema is a serious and progressive condition, if possible, use an uninvolved or not-at-risk extremity when taking blood pressure. In doctors offices or hospitals, where machine BPs are regularly taken, the patient can request a hand BP measurement and have the medical provider only pump the cuff to just a little above the usual BP, thereby avoiding repetitive pumping or painful squeezing. 3. Mammograms: There is no evidence that mammograms cause or worsen breast lymphedema. If you have concerns about breast tenderness, swelling, or soreness after a mammogram on a breast with or at risk for lymphedema, discuss the issue with your radiology technician or health care provider. 4. Razors: There is no evidence that shaving with a clean razor on clean skin causes or increases lymphedema. However, a common sense approach is as follows: when shaving an area with no feeling or that you cannot see, be very cautious and watch what you are doing directly or in a mirror. Do not shave dry skin or use rusty razors that can cause trauma to skin. Do not shave areas of severe lymphedema that have large skin folds, wounds, or deep creases. 5. Heat and cold: There is conflicting evidence on the risk of excessive heat or cold and lymphedema. Based on one survey study of gynecologic cancer survivors, legs may be more at risk than arms with exposure to heat. 15 Individuals should use common sense, proceed very cautiously when using heat or cold therapy, and limit the length of exposure until you know the response of your at-risk body part. Monitor closely the effect of any change in environmental condition on your at-risk body part, and stop if there is increased swelling from exposure to extreme heat or cold. There is a theoretical risk of worsening the lymphedema if the heat or cold is extreme or long enough to cause tissue damage. There is a theoretical risk of immersion moist heat (sauna, hot tub) when done to the point of raising body temperature. Topical heat may or may not have a positive or negative effect on lymphedema. 27,28,29 6. Hospitals, doctor s offices and medical facilities: Medical facilities should have a written policy regarding the at-risk limb. Since many patients have varying levels of risk for lymphedema that cannot easily be determined, the facility should make a reasonable attempt to protect any limb the patient identifies as being at risk for lymphedema. Some medical professionals are unfamiliar with lymphedema and might not take reasonable precautions unless there is a policy. The ability of phlebotomists and professionals using tourniquets or BP machines varies. It is reasonable for an individual with or at risk of lymphedema to have his or her concern properly addressed by health care professionals and facilities. In a medical emergency or when there is no uninvolved limb, health care facilities should address the medical priority, but take reasonable precaution with venipuncture and BP limb constriction to an area of impaired lymphatic drainage. If swelling occurs in an area of impaired lymphatic drainage after a procedure, the provider should give care instructions to the patient. References 1. Stanton AW, Mellor RH, Cook GJ, et al. Impairment of lymph drainage in subfascial compartment of forearm in breast cancer related lymphedema. Lymphat Res Biol. 2003;1(2): Finegold DN, Schacht V, Kimak MA, et al. HGF and MET mutations in primary and secondary lymphedema. Lymphat Res Biol. 2008;6(2): Newman B, Lose F, Kedda MA, et al. Possible genetic predisposition to lymphedema after breast cancer. Lymphat Res Bio. 2012;10(1):2-13.
7 Page 7 of 8 4. Kilbreath SL, Breast cancer. In Lee B-B, Bergan J, Rockson, SG, eds. Lymphedema: A precise compendium of theory and practice. London, UK: Springer. 2011: Cemal Y, Pusic A, Mehrara BJ. Preventative Measures for Lymphedema: Separating Fact From Fiction. J Am Coll Surg. 2011;213(4): National Lymphedema Network. Position Paper on Diagnosis and Treatment of Lymphedema. Updated Feb Werner RS, McCormick B, Petrek J, et al. Arm edema in conservatively managed breast cancer: obesity is a major predictive factor. Radiology. 1991;180(1): Helyer L, Varnic M, Le LW, Leonq W, McCready D. Obesity is a risk factor for developing post operative lymphedema in breast cancer patients. Breast J. 2010;16(1): Ridner SH, Dietrich MS, Stewart BR, Armer JM. Body mass index and breast cancer-related lymphedema. Support Care Cancer. 2011;19(6): Shaw C, Mortimer P, Judd PA. A randomized controlled trial of weight reduction as a treatment for breast cancer related lymphedema. Cancer. 2007;110(8): National Lymphedema Network. Position Paper on Exercise. pdfdocs/ nlnexercise.pdf. Updated Apr Schmitz KH, Ahmed RL, Troxel A, et al. Weight lifting in women with breast-cancer-related lymphedema. N Engl JM. 2009;361(7): Gavish I, Brenner B. Air travel and the risk of thromboembolism. Intern Emerg Med. 2011;6(2): Feldman J. The Challenge of Infection in Lymphedema. Lymphlink. National Lymphedema Network (3). 15. Ryan M, Stainton MC, Jaconelli C, Watts S, MacKenzie P, Mansberg T. The experience of lower limb lymphedema for women after treatment for gynecologic cancer. Onc Nurs Forum. 2003;30(3): Vignes S, Dupuy A. Recurrance of lymphoedema-associated cellulitis (erysipelas) under prophylactic antibiotherapy: a retrospective cohort study. J Eur Acad Dermatol Venereol. 2006;20(7): Mortimer PS. Swollen lower limb-2: lymphoedema. BMJ. 2000;320(7248): Hettrick H, Nof L, Ward S, Ecthernach J. Incidence and prevalence of lymphedema in patients following burn injury: a five-year retrospective and three-month prospective study. Lymphat Res Biol. 2004;2(1): Maheshwari M, Khandelwal S, Maheshwari S. Elephantiasis nostras: complications of third degree acid burn. J Assoc of Physicians of India. 2006;54: Cole T. Risks and benefits of needle use in patients after axillary surgery. Br JNurs. 2006;15(18): National Lymphedema Network. Position Paper on Screening and Measurement for Breast- Cancer- Related Lymphedema (BCRL). nlnbcrl.pdf. Updated Feb Schmitz KH, Ahmed RL, Troxel AB, et al. Weight lifting for women at risk for breast cancer-related lymphedema: a randomized trial. JAMA. 2010;304(24):
8 Page 8 of Ward LC, Battersby KJ, Kilbreath SL. Airplane travel and lymphedema: a case study. Lymphology. 2009;42(3): Kilbreath SL, Ward LC, Lane K, et al. Effect of air travel on lymphedema risk in women with history of breast cancer. Breast Cancer Res Treat. 2010;120(3): Graham PH. Compression prophylaxis may increase the potential for flight-associated lymphoedema after breast cancer treatment. Breast. 2002;11(1): Greene AK, Borud L, Slavin SA. Blood pressure monitoring and venipuncture in the lymphedematous extremity. (letter to the editor) Plast Reconstruc Surg. 2005;116(7): Zhang TS, Huang WY, Han LY, Liu WY. Heat and bandage treatment for chronic lymphedema of extremities. Report of 1045 patients. Chin Med J (Engl). 1984;97(8): Chang TS, Han LY, Gan JL, Huang WY. Microwave: an alternative to electric heating in the treatment of peripheral edema. Lymphology. 1989;22(1): Liu NF, Olszewski. The influence of local hyperthermia on lymphedema and lymphedematous skin of the human leg. Lymphology. 1993;26(1): National Lymphedema Network (NLN). Permission to duplicate this handout as-is, in its entirety, for educational purposes only, not for sale. All other rights reserved. For reprint permission, please contact the NLN office at or [email protected].
Lymphedema: What Every Woman With Breast Cancer Should Know Hand and Arm Care After Surgery or Radiation Therapy for Breast Cancer
 Lymphedema: What Every Woman With Breast Cancer Should Know Hand and Arm Care After Surgery or Radiation Therapy for Breast Cancer What is lymphedema? Lymphedema (limf-uh-dee-muh) is a build-up of lymph
Lymphedema: What Every Woman With Breast Cancer Should Know Hand and Arm Care After Surgery or Radiation Therapy for Breast Cancer What is lymphedema? Lymphedema (limf-uh-dee-muh) is a build-up of lymph
Exercise After Breast Surgery. Post Mastectomy Therapy
 Exercise After Breast Surgery Post Mastectomy Therapy Dear Patient, Breast cancer is a journey and you have made it this far successfully. This booklet will help you continue your journey to recovery.
Exercise After Breast Surgery Post Mastectomy Therapy Dear Patient, Breast cancer is a journey and you have made it this far successfully. This booklet will help you continue your journey to recovery.
Lymphoedema following treatment for breast cancer
 MAY 2007 INFORMATION ABOUT Lymphoedema following treatment for breast cancer This information has been developed to help you understand the signs and symptoms of lymphoedema following treatment for breast
MAY 2007 INFORMATION ABOUT Lymphoedema following treatment for breast cancer This information has been developed to help you understand the signs and symptoms of lymphoedema following treatment for breast
Exercise and advice after breast cancer surgery
 Exercise and advice after breast cancer surgery Irving Building Physiotherapy All Rights Reserved 2015. Document for issue as handout. Role of the physiotherapist Exercises for the first week following
Exercise and advice after breast cancer surgery Irving Building Physiotherapy All Rights Reserved 2015. Document for issue as handout. Role of the physiotherapist Exercises for the first week following
Provided by the American Venous Forum: veinforum.org
 CHAPTER 20 LYMPHEDEMA DIAGNOSIS AND THERAPY Original authors: Audrea Cheville, Cindy Felty, Gail L. Gamble, Peter Gloviczki, Thom W. Rooke, David Strick Abstracted by Raghu Motaganahalli Introduction Lymphedema
CHAPTER 20 LYMPHEDEMA DIAGNOSIS AND THERAPY Original authors: Audrea Cheville, Cindy Felty, Gail L. Gamble, Peter Gloviczki, Thom W. Rooke, David Strick Abstracted by Raghu Motaganahalli Introduction Lymphedema
Provided by the American Venous Forum: veinforum.org
 CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
Information for patients Exercise and advice after breast cancer surgery
 Information for patients Exercise and advice after breast cancer surgery Physiotherapy Salford Royal NHS Foundation Trust Stott Lane, Salford, M6 8HD Telephone: 0161 206 5328 Page 1 of 5 Role of the physiotherapist
Information for patients Exercise and advice after breast cancer surgery Physiotherapy Salford Royal NHS Foundation Trust Stott Lane, Salford, M6 8HD Telephone: 0161 206 5328 Page 1 of 5 Role of the physiotherapist
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
Water is it good for your Lymphedema?
 Water is it good for your Lymphedema? Mrs. G's birthday is coming up and her husband decided to surprise her with a gift a pampering day in a spa. His wife was pleased, yet concerned. She did not know
Water is it good for your Lymphedema? Mrs. G's birthday is coming up and her husband decided to surprise her with a gift a pampering day in a spa. His wife was pleased, yet concerned. She did not know
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Breast Cancer Radiation Therapy: What You Need to Know
 Breast Cancer Radiation Therapy: What You Need to Know The information in this pamphlet is for patients, family members and caregivers. What is radiation treatment? Radiation treatment uses high energy
Breast Cancer Radiation Therapy: What You Need to Know The information in this pamphlet is for patients, family members and caregivers. What is radiation treatment? Radiation treatment uses high energy
Lymphedema of the Head and Neck After Surgery or Radiation
 PATIENT EDUCATION patienteducation.osumc.edu Lymphedema of the Head and Neck After Surgery or Radiation The lymph system helps to get rid of waste products from your cells and helps your body fight infection.
PATIENT EDUCATION patienteducation.osumc.edu Lymphedema of the Head and Neck After Surgery or Radiation The lymph system helps to get rid of waste products from your cells and helps your body fight infection.
What are spider veins? What is the best treatment for spider veins?
 Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
LYMPHEDEMA DIAGNOSIS AND TREATMENT COST SAVING ACT. HR 2499, 112th Congress REPRESENTATIVE LARRY KISSELL (NC-8)
 LYMPHEDEMA DIAGNOSIS AND TEATMENT COST SAVING ACT H, 11th Congress EPESENTATIVE LAY KISSELL (NC-8) ENDOSED BY: The American Cancer Society Komen Advocacy Alliance LiveSTONG Oncology Nursing Society The
LYMPHEDEMA DIAGNOSIS AND TEATMENT COST SAVING ACT H, 11th Congress EPESENTATIVE LAY KISSELL (NC-8) ENDOSED BY: The American Cancer Society Komen Advocacy Alliance LiveSTONG Oncology Nursing Society The
Community home-based prevention of disability due to lymphatic filariasis
 Community home-based prevention of disability due to lymphatic filariasis World Health Organization Geneva WHO/CDS/CPE/CEE/2003.35 Part 3 Figure 1 Wash your leg, or other part of the body affected by lymphoedema,
Community home-based prevention of disability due to lymphatic filariasis World Health Organization Geneva WHO/CDS/CPE/CEE/2003.35 Part 3 Figure 1 Wash your leg, or other part of the body affected by lymphoedema,
Treat Your Feet: Foot care for people with diabetes
 Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Wound Care on the Field. Objectives
 Wound Care on the Field Brittany Witte, PT, DPT Cook Children s Medical Center Objectives Name 3 different types of wounds commonly seen in sports and how to emergently provide care for them. Name all
Wound Care on the Field Brittany Witte, PT, DPT Cook Children s Medical Center Objectives Name 3 different types of wounds commonly seen in sports and how to emergently provide care for them. Name all
Safety FIRST: Infection Prevention Tips
 Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Helping you manage symptoms and side effects associated with metastatic breast cancer treatment
 Helping you manage symptoms and side effects associated with metastatic breast cancer treatment 2015 AstraZeneca. All rights reserved. 3156710 Last Updated 9/15 with metastatic breast cancer treatment
Helping you manage symptoms and side effects associated with metastatic breast cancer treatment 2015 AstraZeneca. All rights reserved. 3156710 Last Updated 9/15 with metastatic breast cancer treatment
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Information for Patients Receiving Radiation Therapy: Breast Cancer or Ductal Carcinoma in Situ (DCIS) of the Breast
 Information for Patients Receiving Radiation Therapy: Breast Cancer or Ductal Carcinoma in Situ (DCIS) of the Breast Why is radiation therapy used to treat breast cancer or DCIS? Breast cancer or DCIS
Information for Patients Receiving Radiation Therapy: Breast Cancer or Ductal Carcinoma in Situ (DCIS) of the Breast Why is radiation therapy used to treat breast cancer or DCIS? Breast cancer or DCIS
Graduated compression hosiery (stockings)
 What is compression hosiery? Compression hosiery are elasticated stockings which give support to your legs. In graduated compression hosiery, the pressure given by the stockings is greater at the ankle
What is compression hosiery? Compression hosiery are elasticated stockings which give support to your legs. In graduated compression hosiery, the pressure given by the stockings is greater at the ankle
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Illinois Department of Public Health STATEMENT OF DEFICIENCIES AND PLAN OF CORRECTION. Statement of LICENSURE Violations
 (X1) PROVER/SUPPLIER/CLIA ENTIFICATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) SUMMARY REGULATORY OR LSC ENTIFYING INFORMATION) PROVER'S PLAN OF CORRECTION Final Observations Statement of
(X1) PROVER/SUPPLIER/CLIA ENTIFICATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) SUMMARY REGULATORY OR LSC ENTIFYING INFORMATION) PROVER'S PLAN OF CORRECTION Final Observations Statement of
Breast Cancer. Sometimes cells keep dividing and growing without normal controls, causing an abnormal growth called a tumor.
 Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
X-Plain Varicose Veins Reference Summary
 X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
Throughout this reference summary, you will find out what massage therapy is, its benefits, risks, and what to expect during and after a massage.
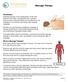 Massage Therapy Introduction Massage therapy is the manipulation of the soft tissues of the body, including the skin, tendons, muscles and connective tissue by a professional, for relaxation or to enhance
Massage Therapy Introduction Massage therapy is the manipulation of the soft tissues of the body, including the skin, tendons, muscles and connective tissue by a professional, for relaxation or to enhance
Understanding Rehabilitation and Recovery After Breast. Sharon Leslie PT, DPT Palo Alto Medical Foundation
 Understanding Rehabilitation and Recovery After Breast Surgery Sharon Leslie PT, DPT Palo Alto Medical Foundation Cancer is one of the few diseases where a patient goes in feeling reasonably well and emerges
Understanding Rehabilitation and Recovery After Breast Surgery Sharon Leslie PT, DPT Palo Alto Medical Foundation Cancer is one of the few diseases where a patient goes in feeling reasonably well and emerges
Sientra Silicone Gel Breast Implants Quick Facts About Breast Augmentation And Reconstruction
 Sientra Silicone Gel Breast Implants Quick Facts About Breast Augmentation And Reconstruction About This Brochure This brochure is intended to provide you with a high level overview of the facts about
Sientra Silicone Gel Breast Implants Quick Facts About Breast Augmentation And Reconstruction About This Brochure This brochure is intended to provide you with a high level overview of the facts about
PATIENT INFORMATION. Radiotherapy following Breast Conservation Surgery. Liverpool & Campbelltown Cancer Therapy Centres
 PATIENT INFORMATION Radiotherapy following Breast Conservation Surgery Liverpool & Campbelltown Cancer Therapy Centres 1. Introduction This booklet is to assist you with information related to the treatment
PATIENT INFORMATION Radiotherapy following Breast Conservation Surgery Liverpool & Campbelltown Cancer Therapy Centres 1. Introduction This booklet is to assist you with information related to the treatment
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Baby Your Legs! Get relief for: Heavy, tired or aching legs Swollen ankles and feet Varicose or spider veins. Managing leg health during pregnancy
 Baby Your Legs! Get relief for: Heavy, tired or aching legs Swollen ankles and feet Varicose or spider veins Managing leg health during pregnancy Common leg health problems during pregnancy Venous disorders
Baby Your Legs! Get relief for: Heavy, tired or aching legs Swollen ankles and feet Varicose or spider veins Managing leg health during pregnancy Common leg health problems during pregnancy Venous disorders
CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE
 Introduction CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE Original authors: Niren Angle, John J. Bergan, Joshua I. Greenberg, and J. Leonel Villavicencio Abstracted by Teresa L. Carman New technology has
Introduction CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE Original authors: Niren Angle, John J. Bergan, Joshua I. Greenberg, and J. Leonel Villavicencio Abstracted by Teresa L. Carman New technology has
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
VARICOSE VEINS. Information Leaflet. Your Health. Our Priority. VTE Ambulatory Clinic Stepping Hill Hospital
 VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Hemodialysis Access: What You Need to Know
 Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Lymph Node Dissection for Penile Cancer
 Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
ORTHOPAEDIC SPINE PAIN QUESTIONNAIRE
 ORTHOPAEDIC SPINE PAIN QUESTIONNAIRE NAME: DATE: ADDRESS: AGE: TELEPHONE#: RELIGION: OCCUPATION: REFERRED BY WHOM: NEAREST FRIEND/RELATIVE: TELEPHONE#: ADDRESS: PLEASE EXPLAIN WHY YOU HAVE COME TO SEE
ORTHOPAEDIC SPINE PAIN QUESTIONNAIRE NAME: DATE: ADDRESS: AGE: TELEPHONE#: RELIGION: OCCUPATION: REFERRED BY WHOM: NEAREST FRIEND/RELATIVE: TELEPHONE#: ADDRESS: PLEASE EXPLAIN WHY YOU HAVE COME TO SEE
Beaumont Hospital. Varicose Veins. and their TREATMENT. Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM
 Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Recurrent Varicose Veins
 Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED
 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED Recently, there have been a number of reports about methicillin-resistant Staph aureus (MRSA) infections
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED Recently, there have been a number of reports about methicillin-resistant Staph aureus (MRSA) infections
Vaxcel PICCs Valved and Non-Valved. A Patient s Guide
 Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Informed Consent For Laser Hair Removal
 Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
Informed Consent For Laser Hair Removal INSTRUCTIONS This informed-consent document has been prepared to help inform you about laser procedures, its risks, as well as alternative treatment(s). It is important
WHAT YOU SHOULD KNOW ABOUT. low blood counts.
 WHAT YOU SHOULD KNOW ABOUT low blood counts. 1 INTRODUCTION Overview It is important for you to be aware that cancer, and some treatments for cancer, may affect your blood counts. Radiation therapy and
WHAT YOU SHOULD KNOW ABOUT low blood counts. 1 INTRODUCTION Overview It is important for you to be aware that cancer, and some treatments for cancer, may affect your blood counts. Radiation therapy and
Spotlight Series: Interventional Radiology. Varicose Veins and Venous Insufficiency
 Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Varicose Vein Surgery
 Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Heat Illnesses. Common Heat Rash Sites
 Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Breast Reduction Post-Operative Instructions
 Breast Reduction Post-Operative Instructions What are my post-operative instructions? Have someone drive you home after surgery and help you at home for 1-2 days. Get plenty of rest and follow a balanced
Breast Reduction Post-Operative Instructions What are my post-operative instructions? Have someone drive you home after surgery and help you at home for 1-2 days. Get plenty of rest and follow a balanced
Care of Your Hickman Catheter
 Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
Tunneled Central Venous Catheter (CVC) Placement
 PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
How to Do Self Lymphatic Massage on your Upper Body
 How to Do Self Lymphatic Massage on your Upper Body UHN For patients who were treated for breast cancer on one side of their body. For example: Lumpectomy Mastectomy Lymph node removal from an underarm
How to Do Self Lymphatic Massage on your Upper Body UHN For patients who were treated for breast cancer on one side of their body. For example: Lumpectomy Mastectomy Lymph node removal from an underarm
ENTITLEMENT ELIGIBILITY GUIDELINES VARICOSE VEINS AND SUPERFICIAL THROMBOPHLEBITIS
 ENTITLEMENT ELIGIBILITY GUIDELINES VARICOSE VEINS AND SUPERFICIAL THROMBOPHLEBITIS 1. VARICOSE VEINS MPC 00727 ICD-9 454 DEFINITION Varicose Veins of the lower extremities are a dilatation, lengthening
ENTITLEMENT ELIGIBILITY GUIDELINES VARICOSE VEINS AND SUPERFICIAL THROMBOPHLEBITIS 1. VARICOSE VEINS MPC 00727 ICD-9 454 DEFINITION Varicose Veins of the lower extremities are a dilatation, lengthening
THERAPEUTIC USE OF HEAT AND COLD
 THERAPEUTIC USE OF HEAT AND COLD INTRODUCTION Heat and cold are simple and very effective therapeutic tools. They can be used locally or over the whole body, and the proper application of heat and cold
THERAPEUTIC USE OF HEAT AND COLD INTRODUCTION Heat and cold are simple and very effective therapeutic tools. They can be used locally or over the whole body, and the proper application of heat and cold
Image Recovery Center
 MCGLINN CANCER INSTITUTE Image Recovery Center Guide to Services www.readinghealth.org Many treatments for cancer and other illness cause temporary or permanent physical changes that, along with the diagnosis,
MCGLINN CANCER INSTITUTE Image Recovery Center Guide to Services www.readinghealth.org Many treatments for cancer and other illness cause temporary or permanent physical changes that, along with the diagnosis,
Tired legs, varicose veins
 Tired legs, varicose veins Everything you need to know What are varicose veins? Varicose veins are swollen, enlarged and twisted veins in the deep or superficial venous system of the legs, due to loss
Tired legs, varicose veins Everything you need to know What are varicose veins? Varicose veins are swollen, enlarged and twisted veins in the deep or superficial venous system of the legs, due to loss
Patella Realignment Tibial Tuberosity Transfer with Lateral Release
 Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
How does Diabetes Effect the Feet
 How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
Section 4: Your Vascular Access. What is vascular access?
 Section 4: Your Vascular Access What is vascular access? What is a fistula? Taking care of a new fistula What is a graft? Taking care of a new graft What is a hemodialysis catheter? Taking care of a hemodialysis
Section 4: Your Vascular Access What is vascular access? What is a fistula? Taking care of a new fistula What is a graft? Taking care of a new graft What is a hemodialysis catheter? Taking care of a hemodialysis
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Department of Surgery
 Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
Cellulitis. Patient Information Leaflet. Contact numbers. Out of hours contact numbers
 Contact numbers District Nurse: Intermediate Care Team: Your GP: Out of hours contact numbers District Nurse: Intermediate Care Team: Out of hours GP Service: If you would like this information in another
Contact numbers District Nurse: Intermediate Care Team: Your GP: Out of hours contact numbers District Nurse: Intermediate Care Team: Out of hours GP Service: If you would like this information in another
Protecting Myself from MRSA By Angela Ulferts RN, BSN
 Protecting Myself from MRSA By Angela Ulferts RN, BSN What is MRSA? MRSA stands for Methicillin-Resistant Staphylococcus Aureus. This is an infection that has been around for some time. But it has always
Protecting Myself from MRSA By Angela Ulferts RN, BSN What is MRSA? MRSA stands for Methicillin-Resistant Staphylococcus Aureus. This is an infection that has been around for some time. But it has always
Radiation Therapy for Breast Cancer
 Radiation Therapy for Breast Cancer www.cpmc.org/learning i learning about your health What Is? Radiation therapy is a treatment for cancer that uses high-energy x-rays to destroy cancer cells. (Radiation
Radiation Therapy for Breast Cancer www.cpmc.org/learning i learning about your health What Is? Radiation therapy is a treatment for cancer that uses high-energy x-rays to destroy cancer cells. (Radiation
Blepharoplasty - Eyelid Surgery
 Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Tibial Intramedullary Nailing
 Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
How can DIABETES affect my FEET? Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES
 THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES I. THORACIC OUTLET SYNDROME TOS is a compression of nerves or blood vessels, or both, in the thoracic outlet region, which is the space between the collarbone
THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES I. THORACIC OUTLET SYNDROME TOS is a compression of nerves or blood vessels, or both, in the thoracic outlet region, which is the space between the collarbone
Surgery for breast cancer in men
 Surgery for breast cancer in men This information is an extract from the booklet Understanding breast cancer in men. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
Surgery for breast cancer in men This information is an extract from the booklet Understanding breast cancer in men. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
Provided by the American Venous Forum: veinforum.org
 CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Venous Reflux Disease and Current Treatments VN20-87-A 01/06
 Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
The veins of the lower limbs can be subdivided into three subtypes: deep veins, superficial veins, and connecting veins (figure 1).
 VEIN DISEASE Vein disease may seem insignificant and harmless at first, but if left untreated, it can develop into a major problem. It occurs when veins have trouble transporting blood back to the heart
VEIN DISEASE Vein disease may seem insignificant and harmless at first, but if left untreated, it can develop into a major problem. It occurs when veins have trouble transporting blood back to the heart
Breast Implants: Local Complications and Adverse Outcomes
 Breast Implants: Local Complications and Adverse Outcomes This booklet highlights the most common problems associated with silicone gel-filled and saline-filled breast implants: those that occur in the
Breast Implants: Local Complications and Adverse Outcomes This booklet highlights the most common problems associated with silicone gel-filled and saline-filled breast implants: those that occur in the
Venefit treatment for varicose veins
 Oxford University Hospitals NHS Trust Venefit treatment for varicose veins Information for patients Your consultant has recommended that we treat your varicose veins with a procedure known as Venefit radio
Oxford University Hospitals NHS Trust Venefit treatment for varicose veins Information for patients Your consultant has recommended that we treat your varicose veins with a procedure known as Venefit radio
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Taking Care of Your Skin During Radiation Therapy
 Taking Care of Your Skin During Radiation Therapy Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: What a radiation skin reaction is How to
Taking Care of Your Skin During Radiation Therapy Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: What a radiation skin reaction is How to
MRSA. Living with. Acknowledgements. (Methicillin-Resistant Staphylococcus aureus)
 How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
Radical Hysterectomy and Pelvic Lymph Node Dissection
 Radical Hysterectomy and Pelvic Lymph Node Dissection Tena koutou katoa, Kia orana, Talofa lava, Malo e lelei, Fakaalofa lahi atu, Taloha Ni, Ni Sa Bula Vinaka, Greetings and Welcome to National Women's
Radical Hysterectomy and Pelvic Lymph Node Dissection Tena koutou katoa, Kia orana, Talofa lava, Malo e lelei, Fakaalofa lahi atu, Taloha Ni, Ni Sa Bula Vinaka, Greetings and Welcome to National Women's
Streptococcal Infections
 Streptococcal Infections Introduction Streptococcal, or strep, infections cause a variety of health problems. These infections can cause a mild skin infection or sore throat. But they can also cause severe,
Streptococcal Infections Introduction Streptococcal, or strep, infections cause a variety of health problems. These infections can cause a mild skin infection or sore throat. But they can also cause severe,
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Structual Fat Transfer (Fat Injection to the Breast) Musgrove Park Hospital is part of Taunton and Somerset NHS Foundation Trust. Patient Information
 Structual Fat Transfer (Fat Injection to the Breast) Musgrove Park Hospital is part of Taunton and Somerset NHS Foundation Trust Patient Information Introduction This information is for patients undergoing
Structual Fat Transfer (Fat Injection to the Breast) Musgrove Park Hospital is part of Taunton and Somerset NHS Foundation Trust Patient Information Introduction This information is for patients undergoing
Lymphedema and Early Retirement Cancer
 Early Education, Exercise and CDT Following Radiation Therapy for Breast Cancer By Linda Boyle, PT, DPT, CLT-LANA OUTLINE FOR CASE PRESENTATIONS I. Reason for presenting case Patients receiving external
Early Education, Exercise and CDT Following Radiation Therapy for Breast Cancer By Linda Boyle, PT, DPT, CLT-LANA OUTLINE FOR CASE PRESENTATIONS I. Reason for presenting case Patients receiving external
dedicated to curing BREAST CANCER
 dedicated to curing BREAST CANCER When you are diagnosed with breast cancer, you need a team of specialists who will share their knowledge of breast disease and the latest treatments available. At Cancer
dedicated to curing BREAST CANCER When you are diagnosed with breast cancer, you need a team of specialists who will share their knowledge of breast disease and the latest treatments available. At Cancer
Peripherally Inserted Central Catheter
 Peripherally Inserted Central Catheter (PICC) by Patricia Griffin Kellicker, BSN En Español (Spanish Version) Definition A peripherally inserted central catheter is a long, thin tube that is inserted through
Peripherally Inserted Central Catheter (PICC) by Patricia Griffin Kellicker, BSN En Español (Spanish Version) Definition A peripherally inserted central catheter is a long, thin tube that is inserted through
SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS)
 SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: VARICOSE VEINS - 2 PROGRAM NUMBER: 122 SUBJECT: SYMPTOMS, CAUSES, TREATMENT, PREVENTION OF VARICOSE VEINS
SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: VARICOSE VEINS - 2 PROGRAM NUMBER: 122 SUBJECT: SYMPTOMS, CAUSES, TREATMENT, PREVENTION OF VARICOSE VEINS
Renal Vascular Access Having a Fistula For Haemodialysis
 Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Exercises after breast or upper body lymph node surgery
 Exercises after breast or upper body lymph node surgery Surgery may limit the strength and movement of your arm. These exercises are helpful if you have had: breast surgery with or without lymph node removal
Exercises after breast or upper body lymph node surgery Surgery may limit the strength and movement of your arm. These exercises are helpful if you have had: breast surgery with or without lymph node removal
