Lumbar Canal Stenosis - A Study of Spinous Process Osteotomy in Posterior Decompression
|
|
|
- Brendan Bond
- 8 years ago
- Views:
Transcription
1 Original Research Lumbar Canal Stenosis - A Study of Spinous Process Osteotomy in Posterior Decompression Manish Dwivedi 1,*, Vikas Sawla 2, Atul Varshney 3, Apoorv Acharya 4 1,2 Assistant Professor, 3 Professor, Dept. of Orthopaedics, People s College of Medical Sciences & Research, Bhopal 4 Consultant Spine Surgeon, Ahmedabad, Gujarat *Corresponding Author: ortho.md12@gmail.com ABSTRACT Study Design: Prospective Background: Lumbar canal stenosis (LCS) remains one of the most frequently encountered, clinically important degenerative spinal disorders in the ageing population. Diagnosing it clinicallyis made more difficult due tocoexisting degeneration of the spine, hip or knee joint or diseased vessels and nerves of lower limbs or due to de-conditioning of spinal musculature and ligaments. Purpose of the study: The purpose of our study was to assess the results of spinous process osteotomy & laminotomy in cases of lumbar canal stenosis. Material and Methods: It was prospective study with 25 confirmed cases of lumbar canal stenosis adhering to inclusion criteria and stable spine. Patients were assessed pre-operative and post- operative using LINS Functional Ability Criteria, VAS scale for back pain and leg pain, JOAS score and Satisfactory Recovery Rate- Hirabayashi Method( Based on Pre-op and Post-op JOAS scores) with an average follow-up of 1 year. Results: There were 25 patients, 12 (48%) males and 13 (52%) females. Mean age of group was ± 7.52.There were14 (56%) patients with two level involvement followed by 6 (24%) patients with three level involvement and 5 (20%) patients with single level involvement. In single level involvement maximum number was of L4-L5.All 25 (100%) patients presented with Claudication and radiculopathy; 9 (36%) had unilateral radiculopathy while 16 (64%) had bilateral radiculopathy.10(40%) patients had motor weakness and sensory involvement.1(4%) patient presented with cauda equina syndrome with associated sphincter involvement.all patients were treated with Spinous process osteotomy and fenestration and foraminotomy. In addition to that, discectomy was done in 14 (56%) patients while laminotomy was required in 3 (12%) patients Functional assessment as per LINS criteriashowed that satisfactory results (Percentage of patients in Excellent and Good Class) were achieved in 90% of the patients.there were significant improvement in back pain (60%) and excellent improvement in leg pain (76%) in terms of VAS. Improvement in JOAS score was also excellent (72%).according to Hirabayashi method, 12 (48%) patients had Excellent results (JOAS recovery rate >70%); and 10 (40%) patients had Good results (JOAS recovery rate between 45% and 70%). Conclusion: The Spinous Process Osteotomy (SPO) technique is one of the surgeries associated with minimal muscle injury, effective andfaster long lasting decompression, and satisfactory neurological and functional outcomes with acceptable low risk of complication highly safe for all concerned and maintenance of spinal stability by utilizing standard outcome measures with logical expectation to maintain excellent to good results at long term follow up. Keywords: Lumbar Canal Stenosis, Spinous Process Osteotomy, SPO, JAOS score, LINS criteria, Hirabayashi Method Quick Response Code: Access this article online Website: DOI: / INTRODUCTION Surgery for lumbar spinal stenosis (LSS) is the most common surgical procedure involving the adult lumbar spine. 1 Degenerative spinal stenosis is a progressive disorder that involves the entire spinal motion segment as described by Kirkaldy-Willis. 2,3 Lumbar spinal stenosis is one manifestation of the general process of spinal degeneration that occurs with aging, and often becomes symptomatic in the fifth and sixth decades of life. Unfortunately, lumbar spinal stenosis continues to be misunderstood and under-diagnosed, and many patients are never offered effective treatment for their symptoms. The symptoms of lumbar stenosis are of two types, one due to central canal narrowing causing Neurogenic Claudication (unilateral/bilateral) and other due to narrowing of the vertebral foramen causing Radicular symptoms. Patient can present with one of them or both of them. Although the diagnosis can be strongly suspected from the history and physical findings alone in many cases, noncontrast stress MRI now provides a confirmation in many cases, and now routine myelography is no longer necessary. For patients who are persistently symptomatic despite adequate conservative care, surgery can offer a highly rewarding and effective for improvement in quality of life. Indian Journal of Orthopaedics Surgery 2015;1(3):
2 Lumbar canal stenosis was first described by Sachs and Frankel in However its first clinical description is attributed to Henk Verbiest a Dutch neurosurgeon (1954). Sincethen surgeons are searching for accurate method of definite diagnosis and operative treatment for the same. Various methods for operative treatment for lumbar canal stenosis have been developed and described in literature since then with varied results. These includes hemilaminectomy, standard laminectomy, wide laminectomy, laminotomy, split spinous process laminectomy, spinous process osteotomy & laminectomy and their numerous modification. Weiner 4 and other authors 5,6 have described Spinous process osteotomy with good clinical results. It gives the surgeon the possibility to work across the midline, which facilitates the approach to the lateral recesses. In spinous-process osteotomies for spinal stenosis decompression one side of the paraspinal muscle is divided and the spinous processes are cut horizontally at the junction of the lamina and spinous process. They reported its benefit of minimal muscle injury, early recovery, and minimal damage to spinal anatomy. We conducted this study with the aim to assess the results of spinous process osteotomy & laminotomy in cases of lumbar canal stenosis. MATERIAL AND METHODS It was a prospective study with 25 patients with lumbar canal stenosis, who adhered to our inclusion criteria. Evidence of lumbar canal stenosis was obtained from history, clinical examination, Lumbo sacral spine X-rays with dynamic views. It was confirmed with MRI. Inclusion Criteria: Confirmed cases of Lumbar canal stenosis not responding to conservative treatment and steroid blocks for minimum of at least 12weeks, only exception were patient with nonrecovering or deteriorating neurological symptoms. Another important criterion was claudication distance of less than 100 meters. Exclusion Criteria: Elderly patients above 70 yrs., high anaesthestic risk patients, patients with medical comorbidities like congestive heart failure, livercirrhosis, coagulopathy and diabetesmellitus. Also patients with lumbar spondylolisthesis with instability requiring additional instrumentation. Patient was assessed pre-operatively and postoperatively by using VAS Pain scale for back and leg pain, Disability (quality of life or working capacity) in terms of LINS scale, Japanese Orthopaedic Association Scale (JOAS) 7 and Satisfactory Recovery Rate- Hirabayashi Method (Based on Pre-op and Post-op JOAS scores). 8 PROCEDURE 2 Procedure was done under general Anaesthesia. Patient was put in prone position without pressure and localization of spinal levels was done according to IITV guidance. With a suitable length midline incision dorsolumbar fascia was exposed. Unilateral para-median incision in the fascia was made thus preserving the supraspinous and interspinous ligaments with subperiosteal dissection of the paraspinal muscles from the spinous process and laminae on one side only. Stripping of the multifidus muscles beyond the medial aspect of the facet joint was avoided to preserve their innervation. With a curved osteotome, each spinous process was freed from the lamina at its base. Only the levels shown to be affected on preoperative imaging were released. Freed spinous process was retracted to one side with the paraspinal muscles beneath the retractor and the other blade of the retractor beneath the multifidus muscles to expose the midline. We modified the procedure by not resecting upper and lower half of lamina but doing fenestration, foraminotomy ± laminotomy (unilateral or bilateral) depending on patient s clinical and imaging problem. Complete laminectomy was not done in any case. Intra-operatively when the discectomy was done and nerve root or dorsal root ganglion or significant root manipulation required for proper decompression then Abgel piece soaked in 40mg kanacort was put over and around it to reduce root inflammation and resulting neuritic pain during post-operative period. During closure negative suction drain was kept and spinous process was taken to its original place by suturing paraspinal muscle and fascia with supraspinous and intraspinous ligament with intermittent vicryl OS suture at all level. Water tight closure of lumbar fascia was done. POST-OPERATIVE PROTOCOL Physiotherapy in form of active back range of motion exercise, passive and active SLR exercise, back extension exercise and William s abdominal strengthening exercise to gradual gait training started suitably next post-operative day as tolerated by patient. Patients were discharged on 3rd to 5th postoperative days after favourable wound status. Patients did not need to wear a rigid lumbar brace. Patients were called in follow up on 15th day for stitch removal, 6 weeks, 3 month, 6 month and 1 year and then every 6 months. PATIENT ASSESSMENT AT FOLLOW UP Patients were evaluated preoperatively and 15th day, 6 weeks, 3 month, 6 month,1 year and then every 6 monthly postoperatively using the LINS Functional Ability Criteria, VAS scale for back pain and leg pain, JOAS score and Satisfactory Recovery Indian Journal of Orthopaedics Surgery 2015;1(3):
3 Rate- Hirabayashi Method (Based on Pre-op and Post-op JOAS scores). For the purpose of checking the stability of the spine and to rule out iatrogenic RESULTS instability post-operatively, we took dynamic lateral view of lumbosacral spine in all patients at least once after 3 months. Table 1: Demographics Male Female Total No. of Patients 12 (48%) 13 (52%) 25 (100%) Age - Mean±SD ± ± ± 7.52 Pathology Level Table 2: Type and Level of Pathology Associated Spinal Pathology Degenerative LCS Stable Listhesis PIVD Stable Degenerative Scoliosis Single level L3-L4 5 (20%) L4-L5 L5-S1 6 (24%) 13 (52%) 0 (0%) 0 (0%) 4 (16%) 1 (4%) 14 (56%) Double level L3-L4,L4-L5 L4-L5,L5-S1 0 (0%) 1 (4%) 2 (8%) 2 (8%) 12 (48%) Triple Level 6 (24%) L3-L4,L4-L5,L5-S1 0 (0%) 0 (0%) 1 (4%) Total 25 (100%) 5 (20%) 14 (56%) 3 (12%) Table 3: Presenting Symptoms Symptoms No of patients Motor weakness +Associated Sensory Hypoaesthesia 10 (40%) Cauda Equina Syndrome with Sphincter involvement 1 (4%) Claudication with Unilateral radiculopathy 9 (36%) Claudication with Bilateral Radiculopathy 16 (64%) Table 4: Management Procedure SPO + Fenestration + Foraminotomy 25(100%) Additional Procedure Discectomy 14(56%) Laminotomy 3(12%) SPO Details Level of Surgery Single Level Right side 4 (16%) Left side 8 (32%) Double Level Right side 2 (8%) Left Side 9 (36%) Triple Level Right Side 0 (0%) Left side 2 (8%) Side of Decompression Unilateral Right 6 (24%) Left 8 (32%) Bilateral 11 (44%) Neurological Recovery Fully Recovered 8 (80%) Total Partially Recovered 1 (10%) 1 (10%) Same 1 (10%) Table 5: Assessment A. Functional assessment as per LINS criteria Post-op Pre-op No. of Patients Poor Fair Good Excellent Poor 13 (52%) 1 (4%) 0 (0%) 6 (24%) 6 (24%) Fair 12 (48%) 0 (0%) 0 (0%) 4 (16%) 8 (32%) Good 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Excellent 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Total 25 (100%) 1 (4%) 0 (0%) 10 (40%) 14 (56%) Indian Journal of Orthopaedics Surgery 2015;1(3):
4 B. JOAS score and VAS Criteria Pre-op Average Final Follow-up Average Improvement Back Pain VAS % Leg Pain VAS % JOAS % C. Satisfactory Recovery Rate- Hirabayashi Method (Based on JOAS Scores) Result Recovery Rate No. of patient Excellent >70% 13 (56%) Good 45-69% 10 (40%) Fair 25-44% 1 (4%) Poor <25% 1 (4%) Total 25 (100%) 1. Demographics (Table 1): There were 25 patients. Out of them there were 12 (48%) males and 13 (52%) females. Mean age of group was ± 7.52 with that of male was ± 8.27and of female was44.85 ± LCS type and Level (Table 2): There were highest number of patients 14 (56%) with two level involvement followed by 6 (24%) patients with three level involvement and 5 (20%) patients with single level involvement. In single level involvement maximum number was of L4- L5.Along with LCS there were some associated spinal pathology. 6 (24%) patients had stable listhesis and 3 (12%) patients have Stable Degenerative Scoliosis at the time of presentation. There were 14 (56%) patients had associated PID; 13 (52%) of them had PID at single level while 1 (4%) had PID at 2 levels. 3. Presenting Pathology (Table 3): All 25 (100%) patients presented with Claudication and radiculopathy; 9 (36%) had unilateral radiculopathy while 16 (64%) had bilateral radiculopathy. 10(40%) patients had motor weakness and all of them also had sensory involvement also. 1(4%) patient presented with cauda equina syndrome with associated sphincter involvement. Bilateral neurological claudication with radiculopathy was commonest presentation and cauda equina paresis with sphincter involvement was most serious presentation which needs urgent decompression. 4. Management (Table 4): All patients were treated with Spinous process osteotomy and fenestration and foraminotomy. In addition to that, discectomy was done in 14 (56%) patients while laminotomy was required in 3 (12%) patients. Paraspinal muscles on predominant side of symptoms/ neurological deficit were stripped and spinous process was retracted to opposite side.with bilateral equal symptoms, left sided approach was selected because of convenience of right handed surgeon. So, left sided approach is more common in our study. Decompression was done bilaterally in 11(44%) cases and unilaterally in 14 (56%) cases (Right-6(24%), Left 8(24%). In our study, out of 25 patients, 10 (40%) patients who initially presented with motor weakness, 8 (32%) patients showed full neurological recovery at final follow-up. 1 (4%) patient with 3 level problem has partial recovery at final follow, while 1 (4%) patient had same motor neurological status at final follow-up but show improvement in sensation with normal sphincter. 1 (4%) patient present with cauda equina paraparesis with bilateral motor weakness, sensory and sphincter involvement of 5 days. He recovered completely after 3 month follow up. 5. Assessment a) Functional assessment as per LINS criteria: After treatment at final follow-up; only 1 (4%) patient was in POOR Category as per LINS criteria which is due to intra-op nerve root injury during removal of adherent disc. However that patient was in POOR Category pre-op also. Out of pre-op POOR 13 (56%) patients, 6 (24%) patients become EXCELLENT and 6 (24%) GOOD at final follow up. Out of pre- op FAIR 12 (48%) patients, 8 (32%) patients become EXCELLENT and 4 (16%) patients GOOD at final follow up. Satisfactory results (Percentage of patients in Excellent and Good Class) were achieved in 90% of the patients. b) JOAS score and VAS: The study population showed significant improvement in back pain (60%) and excellent improvement in leg pain (76%) in terms of VAS. Improvement in JOAS score was also excellent (72%). c) Satisfactory Recovery Rate: Hirabayashi Method (Based on JOAS Scores) In accordance with JOAS, according to Hirabayashi method, 12 (48%) patients had Excellent results (JOAS recovery rate >70%); and 10 (40%) patients had Good results (JOAS recovery rate between 45% and 70%). Indian Journal of Orthopaedics Surgery 2015;1(3):
5 COMPLICATIONS Nerve Root Delayed Dural Puncture Injury Infection 4 (16%) 1(4%) 1(4%) 4 (16%) patients had intra-op dural puncture which was sealed with AB gel and Surgical and then checked for integrity by valsalva manoeuvre. Post op these patients were asymptomatic and they were mobilized after 5 days. Only 1(4%) patient had intra-op nerve root injury due to migrated adherent hard disc which was symptomatic pre op neurological deficit. Post op this patient slowly recovered of deteriorated neurology and sensation returned normal. However paraesthesia and minor motor deficit remain up to last follow up. 1(4%) patient had delayed wound infection which was previously operated for left sided PID L4-5; eight years back by fenestration and discectomy and now developed same level right sided PID with severe radiculopathy. He was operated by L5 spinous process osteotomy with right sided decompression. Excellent symptomatic relief was observed immediate post op and discharged on 4th post op day. After 1 month of follow up there was minor pus discharging sinus on the healed incision, on follow up contrast MRI no discitis found and decompression was satisfactory. Debridement of subcutaneous tissue and muscles done up to lamina and antibiotic given for 4 weeks according to culture sensitivity and patient recovered of problem within 4 weeks with good back range of motion without leg pain. DISCUSSION LSS is a narrowing of the spinal canal leading to compression of nervous and vascular structures. The surgical solution is to relieve this compression by performing a decompressive procedure. To achieve this goal of decompression at the disc level where the narrowing primarily takes place, most parts of the ligamentum flava and the lamina (whole or parts of it) are removed. The consequences of bone and ligament removal must be considered when performing decompression for spinal stenosis. Denervation of the paraspinal musculature occurs with wide exposures, which results in altered muscle function. This was a prospective study of effect of spinous process osteotomy in posterior decompresssion in patients with lumbar canal stenosis in 25 patients. Our study group was somewhat similar to studies of Weiner et al (46 patients) 4 and Hermansen et al. (55 patients). 9 In our study averages follow up of 1 year. Hermansen et al. had an average follow up of 21 months. 9 However Weiner et al had follow up of 5years. 4 Mean age of the study group was below 50 years with 80% of patient belonging to under 50 years age profile. Sex ratio was also almost equal. This shows that prevalence of this problem is high in middle age in our set up. Because the primary complaint often is back pain and some leg pain, pain relief after surgery may not be complete. Jönsson reported successful results after operative treatment in 62% to 67% of patients, although they noted deterioration at 5 years, with 18% requiring reoperation. 3 Most series report a 64% to 91% rate of improvement, with 42% in patients with diabetes, but most patients still have some minor complaints, usually referable to the pre-existing degenerative arthritis of the spine. Neurological findings, if present, improve inconsistently after surgery. 3 In our study leg pain VAS was shown to have 70% relief as compared to SPO group of Weiner et al 4 (50%). In our study post-operative back pain VAS was 2.56(60 % relief) whereas post-operative leg pain VAS was 2.00 (76 % relief). It was similar to Hermansen et al 9 who reported post-operative back pain VAS as 3.96 whereas post-operative leg pain VAS was A total JOAS can range from -6 to 15, and is a good indicator of the subjective and objective function. Such assessments cover subjective symptoms (low-back pain, leg pain, and walking capacity) and clinical symptoms (straight leg raising test, and motor, sensory, and bladder functions).in our study there was 72% improvement in JAOS. In our study Recovery rate as per Hirabayashi Method was excellent in 56% and good in 36% cases making it more than 90% in terms of Satisfactory Recovery rate. It was similar to SPO group of Weiner et al. 4 (83%). When we assess our complications we found that there were 6 (24%) cases with surgical complication. It was somewhat higher than the study of Hermansen et al 9 (11%). Out of those 6 cases, 4 (16%) had dural ruptures. Weiner et al 4. Reported 4 (8%) cases who had dural rupture.hermansen 9 et al had 1(<1%) case of dural rupture. We had 1 (4%) case of infection where had Hermansen 9 et al had 1 (<1%) case of infection. When we assess our study we find one limitation in our study. We had not assessed the status of spinous process healing post operatively after osteotomy. Hermansen et al in their study reported the assessment of spinous process healing post operatively. 9 They found a radiologic union for 60 out of 135 (44%) spinous process osteotomies. They reported that complete-union group showed better clinical results and scored significantly better in the Oswestry Disability Index and EQ-5D. Indian Journal of Orthopaedics Surgery 2015;1(3):
6 However, no statistical difference was found in the pain-scores. There were no differences between the partial-union group and the no-union group. Apart from Spinous process osteotomy several surgical techniques have been adopted forpreserving paraspinal muscle function while achieving adequate decompression in lumbar spinal stenosis. Watanabe et al. improvised this technique by splitting the spinous process 10, preserving bilateral paraspinal muscle integrity and performing a complete laminectomy. Lin et al. reported a slight modification wherein they preserved the outer one third thickness of the lamina 11, bent it laterally using an osteotome along with the overlying paraspinal muscles and removed the inner two thirds thickness of the lamina. They minimised paraspinal muscle injury further by preserving their attachment to the laminar surface which was elevated in the original SPSL technique. Cho et al. used the original spinous process splitting technique 12, but restricted laminar resection to bilateral laminotomies, rather than a full laminectomy. Hatta et al. described an interlaminar technique for decompressing single level stenosis by drilling the adjacent portions of the spinous process and splitting the interspinous ligament progressively to expose the interlaminar window. 13 Banczerowski et al. used a modification of the SPSL technique for spinal tumour resection and described an archbone technique for enlarging the spinal canal diameter by placing a complimentary tricortical iliac crest graft in between the distracted ends of the split spinous processes. 14 Although spinal stability radiological and clinical appears to be unaffected in these initial preliminary results, long-term follow up is needed for confirmation. We believe this minimal muscle injury technique (which also preserves posterior spinal ligaments) can reduce back muscle atrophy and weakness and there by maintain spinal stability on longer follow up also. CONCLUSION Commonly used techniques of lumbar decompression results in extensive back musculature injury and vertebral osseous and non-osseous damage leading to significant iatrogenic instability and subsequent problem of exaggerated back pain and restenosis, whereas minimally invasive techniques like endoscopic procedure often provide inadequate visualization and/or decompression and involve costly instrumentation and time consuming. Spinous Process Osteotomy minimizes destruction to tissues not directly involved in the pathologic process, including the paraspinal musculature as well as the interspinous/supraspinous ligament complex and facets and even maintaining their stabilization properties. Thus Spinous Process Osteotomy appears to result in satisfactory spinal decompression with advantages of minimal muscle trauma and postoperative discomfort, satisfactory and fast decompression with conventional instruments, maintenance of spinal stability, earlymobilization, shortening of post op hospital stay, reduction of postoperative back pain. There is no disadvantage of this procedure except perception of new approach and initial careful orientation curve. Surgeon should perceive the method as satisfactory decompression along with combination of fenestration SOS discectomy/ laminotomy and foraminotomy. AUTHOR S CONTRIBUTION The study was designed by VS, AA. Patients screening, procedure, data collection, documentation was done by VS, AA. Literature search, study and review were done by MD. MD, AV and VS wrote the manuscript. ACKNOWLEDMENT Dr. Ashish Dwivedi s help is acknowledged for his help in statistical analysis. CONFLICT OF INTEREST: None REFERENCES 1. Ciol MA, Deyo RA, Howell E, Kreif S. An assessment of surgery for spinal stenosis: time trends, geographic variations, complications, and reoperations. J Am Geriatr Soc 1996; 44: Yong-Hing K, Kirkaldy-Willis WH. Osteotomy of lumbar spinous process to increase surgical exposure. Clin Orthop Relat Res Jul-Aug;( 134): Campbell s Operative Orthopaedics,12th edition,volume 2 Pages Weiner BK, Fraser RD, Peterson M. Spinous process osteotomies to facilitate lumbar decompressive surgery. Spine (Phila Pa 1976) 1999; 24: Gunzburg R, Keller TS, Szpalski M, Vandeputte K, Spratt KF. A prospective study on CT scan outcomes after conservative decompression surgery for lumbar spinal stenosis. J Spinal Disord Tech 2003; 16: El-Abed K, Barakat M, Ainscow D. Multilevel lumbar spinal stenosis decompression: midterm outcome using a modified hinge osteotomy technique. J Spinal Disord Tech 2011; 24: Japanese Orthopaedic Association (JOA). Japanese Orthopaedic Association Assessment Criteria Guidelines Manual Pages Hirabayashi K, Miyakawa J, Satomi K. Operative result and postoperative progression of ossification among patients with ossification of cervical posterior longitudinal ligament. Spine (Phila Pa 1976) 1981; 6: Hermansen E, Moen G, Fenstad AM, Birketvedt R, Indrekvam K. Spinous process osteotomy to facilitate the access to the spinal canal when decompressing the spinal canal in patients with lumbar spinal stenosis. Asian Spine J Apr; 8(2): doi: /asj Epub 2014 Apr Watanabe K, Hosoya T, Shiraishi T, et al. Lumbar spinous process-splitting laminectomy for lumbar canal stenosis. Technical note. J Neurosurg Spine. 2005; 3(5): Indian Journal of Orthopaedics Surgery 2015;1(3):
7 11. Lin SM, Jseng SH, Yang JC, et al. Chimney sublaminal decompression for degenerative lumbar stenosis. J Neurosurg Spine. 2006; 4: Cho DY, Lin HL, Lee WY, et al. Split-spinous process laminotomy and discectomy for degenerative lumbar spinal stenosis: a preliminary report. J Neurosurg Spine. 2007; 6(3): Hatta Y, Shiraishi T, Sakamoto A, et al. Muscle preserving interlaminar decompression for the lumbar spine: a minimally invasive new procedure for lumbar spinal canal stenosis. Spine (Phila Pa 1976). 2009; 34(8):E Banczerowski P, Vajda J, Veres R. Exploration and decompression of the spinal canal using split laminotomy and its modification, the "archbone" technique. Neurosurgery. 2008; 62(Suppl 2):ONS Indian Journal of Orthopaedics Surgery 2015;1(3):
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis
 Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Surgical Technique. coflex Surgical Technique
 Surgical Technique coflex Surgical Technique Interspinous Implant Overview I. Preparation II. Microsurgical Decompression III. Implant Site Preparation IV. Implant Insertion Preparation Patient Positioning
Surgical Technique coflex Surgical Technique Interspinous Implant Overview I. Preparation II. Microsurgical Decompression III. Implant Site Preparation IV. Implant Insertion Preparation Patient Positioning
Ben Okafor FRCS FRCS.orth Consultant Orthopaedic & Spine Surgeon Whipps Cross University Hospital
 Ben Okafor FRCS FRCS.orth Consultant Orthopaedic & Spine Surgeon Whipps Cross University Hospital Classification Pathology Clinical features Imaging Treatment Options Outcomes Definition: 1. Narrowing
Ben Okafor FRCS FRCS.orth Consultant Orthopaedic & Spine Surgeon Whipps Cross University Hospital Classification Pathology Clinical features Imaging Treatment Options Outcomes Definition: 1. Narrowing
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
A review of spinal problems
 Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Diagnosis and Treatment of Lumbar Spinal Canal Stenosis
 Low Back Pains Diagnosis and Treatment of Lumbar Spinal Canal Stenosis JMAJ 46(10): 439 444, 2003 Katsuro TOMITA Department of Orthopedic Surgery, Kanazawa University Abstract: Lumbar spinal canal stenosis
Low Back Pains Diagnosis and Treatment of Lumbar Spinal Canal Stenosis JMAJ 46(10): 439 444, 2003 Katsuro TOMITA Department of Orthopedic Surgery, Kanazawa University Abstract: Lumbar spinal canal stenosis
Lumbar Spinal Stenosis
 Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
The conservative surgical treatment of lumbar spinal stenosis in the elderly
 REVIEW Robert Gunzburg Marek Szpalski The conservative surgical treatment of lumbar spinal stenosis in the elderly R. Gunzburg ( ) Department of Orthopaedics, Eeuwfeestkliniek, Harmoniestraat 68, 2018
REVIEW Robert Gunzburg Marek Szpalski The conservative surgical treatment of lumbar spinal stenosis in the elderly R. Gunzburg ( ) Department of Orthopaedics, Eeuwfeestkliniek, Harmoniestraat 68, 2018
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Surgery for cervical disc prolapse or cervical osteophyte
 Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: paul@pauldurso.com
Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: paul@pauldurso.com
Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes.
 Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis
 Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis
 Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Clinical Guideline. Low Back Pain Orthopaedics. Princess Alexandra Hospital Emergency Department. 1 Purpose. 2 Background
 Princess Alexandra Hospital Emergency Department Clinical Guideline Orthopaedics Review Officer: Katherine Isoardi Version no: 1 Approval date: 18/03/2015 Review date: 18/03/2017 Approving Officer Dr James
Princess Alexandra Hospital Emergency Department Clinical Guideline Orthopaedics Review Officer: Katherine Isoardi Version no: 1 Approval date: 18/03/2015 Review date: 18/03/2017 Approving Officer Dr James
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis:
 Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN
 Cox Technic Case Report #60 sent 5/13/08 1 UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN History, Examination & Imaging Review: A 53-year-old
Cox Technic Case Report #60 sent 5/13/08 1 UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN History, Examination & Imaging Review: A 53-year-old
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
Subject: BlueCross BlueShield of North Carolina Lumbar Spine Fusion Surgery Notification
 , 2010 Don W. Bradley, M.D. Senior Vice President, Healthcare & Chief Medical Officer Blue Cross and Blue Shield of North Carolina 5901 Chapel Hill Road Durham, NC 27707 Subject: BlueCross BlueShield of
, 2010 Don W. Bradley, M.D. Senior Vice President, Healthcare & Chief Medical Officer Blue Cross and Blue Shield of North Carolina 5901 Chapel Hill Road Durham, NC 27707 Subject: BlueCross BlueShield of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Research Article Partial Facetectomy for Lumbar Foraminal Stenosis
 Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery
 Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Lumbar spinal stenosis and its symptoms
 Lumbar Spinous Process Splitting Laminoplasty: A Novel Technique for Minimally Invasive Lumbar Decompression Yaser M. K. Baghdadi, MD; Charbel D. Moussallem, MD; Mohammed A. Shuaib, MBBS; Michelle J. Clarke,
Lumbar Spinous Process Splitting Laminoplasty: A Novel Technique for Minimally Invasive Lumbar Decompression Yaser M. K. Baghdadi, MD; Charbel D. Moussallem, MD; Mohammed A. Shuaib, MBBS; Michelle J. Clarke,
CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES
 CASE REPORT CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES Atanas Davarski 1, Ivo Kehayov 1, Tanya Kitova 2, Christo Zhelyazkov 1, Borislav Kitov
CASE REPORT CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES Atanas Davarski 1, Ivo Kehayov 1, Tanya Kitova 2, Christo Zhelyazkov 1, Borislav Kitov
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013 Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally
EXPERIMENTAL AND THERAPEUTIC MEDICINE 5: 567-571, 2013 Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING
 POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING A 47 year old white married female was seen for the chief complaint of low back and right
POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING A 47 year old white married female was seen for the chief complaint of low back and right
Hitting a Nerve: The Triggers of Sciatica. Bruce Tranmer MD FRCS FACS
 Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Study Design: Purpose: Overview of Literature: Methods: Results: Conclusions: Keywords:
 Asian Spine Journal 138 Erland Hermansen Clinical Study et al. http://dx.doi.org/10.4184/asj.2014.8.2.138 Spinous Process Osteotomy to Facilitate the Access to the Spinal Canal When Decompressing the Spinal
Asian Spine Journal 138 Erland Hermansen Clinical Study et al. http://dx.doi.org/10.4184/asj.2014.8.2.138 Spinous Process Osteotomy to Facilitate the Access to the Spinal Canal When Decompressing the Spinal
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010
 Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
SPINE SURGERY - LUMBAR DECOMPRESSION
 SPINE SURGERY - LUMBAR DECOMPRESSION Information Leaflet Your Health. Our Priority. Page 2 of 7 Introduction This booklet has been compiled by the physiotherapy department to help you understand lumbar
SPINE SURGERY - LUMBAR DECOMPRESSION Information Leaflet Your Health. Our Priority. Page 2 of 7 Introduction This booklet has been compiled by the physiotherapy department to help you understand lumbar
ISPI Newsletter Archive Lumbar Spine Surgery
 ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
Surgical Treatment for Lumbar Spinal Stenosis Dynamic Interspinous Distraction Interlaminar Stabilization Implant - Coflex
 International 31st Course For Percutaneous Endoscopic Spinal Surgery And Complementary Minimal Invasive Techniques Zurich, Switzerland January 24-25, 2013 Surgical Treatment for Lumbar Spinal Stenosis
International 31st Course For Percutaneous Endoscopic Spinal Surgery And Complementary Minimal Invasive Techniques Zurich, Switzerland January 24-25, 2013 Surgical Treatment for Lumbar Spinal Stenosis
Presenter : Dr Yashpal Singh Rathore
 Presenter : Dr Yashpal Singh Rathore 1 Narrowing of the spinal canal/lateral recess/ intervertebral foramen. Verbiest (1954) first established LCS as a clinical entity Annual incidence 5 cases / 100,000
Presenter : Dr Yashpal Singh Rathore 1 Narrowing of the spinal canal/lateral recess/ intervertebral foramen. Verbiest (1954) first established LCS as a clinical entity Annual incidence 5 cases / 100,000
https://www.laserspineinstitute.com/back_problems/foraminal_stenosis/e...
 Questions? Call toll free 1-866-249-1627 Contact us today. We're here for you seven days a week. MRI Review Consultation Live help Call 1-866-249-1627 Chat Live Home Laser Spine Institute Laser Spine Institute's
Questions? Call toll free 1-866-249-1627 Contact us today. We're here for you seven days a week. MRI Review Consultation Live help Call 1-866-249-1627 Chat Live Home Laser Spine Institute Laser Spine Institute's
Surgical Procedures of the Spine
 Surgical Procedures of the Spine Jaideep Chunduri, M.D. Orthopaedic Spine Surgeon Beacon Orthopaedics and Sports Medicine Beacon Spine Center Objectives Discuss the 4 most common procedures performed in
Surgical Procedures of the Spine Jaideep Chunduri, M.D. Orthopaedic Spine Surgeon Beacon Orthopaedics and Sports Medicine Beacon Spine Center Objectives Discuss the 4 most common procedures performed in
IMPAIRMENT RATING 5 TH EDITION MODULE II
 IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Herniated Disk in the Lower Back
 Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
MALIGNANT SPINAL CORD COMPRESSION. Kate Hamilton Head of Medical Oncology Ballarat Health Services
 MALIGNANT SPINAL CORD COMPRESSION Kate Hamilton Head of Medical Oncology Ballarat Health Services OVERVIEW Background Epidemiology Pathophysiology Diagnosis Investigation Differential Diagnosis Management
MALIGNANT SPINAL CORD COMPRESSION Kate Hamilton Head of Medical Oncology Ballarat Health Services OVERVIEW Background Epidemiology Pathophysiology Diagnosis Investigation Differential Diagnosis Management
IP'Lumbar Spinal Stenosis
 A Patient's G uide to IP'Lumbar Spinal Stenosis X*STOP Interspinous Process Decompression This patient information guide is made possible through cooperation between your physician and St. Francis Medical
A Patient's G uide to IP'Lumbar Spinal Stenosis X*STOP Interspinous Process Decompression This patient information guide is made possible through cooperation between your physician and St. Francis Medical
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Orthopaedic Approach to Back Pain. Seth Cheatham, MD
 Orthopaedic Approach to Back Pain Seth Cheatham, MD 262 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures. Focus on clinical situations where a referral to an orthopaedic surgeon
Orthopaedic Approach to Back Pain Seth Cheatham, MD 262 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures. Focus on clinical situations where a referral to an orthopaedic surgeon
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
PARADIGM SPINE. Brochure. coflex Interlaminar Stabilization
 PARADIGM SPINE Brochure Interlaminar Stabilization SPINAL STENOSIS WITH BACK PAIN THE RATIONALE FOR STABILIZATION For the treatment of spinal stenosis, surgeons have various treatment options. The continuum
PARADIGM SPINE Brochure Interlaminar Stabilization SPINAL STENOSIS WITH BACK PAIN THE RATIONALE FOR STABILIZATION For the treatment of spinal stenosis, surgeons have various treatment options. The continuum
Patient Information. Lumbar Spine Segmental Decompression. Royal Devon and Exeter NHS Foundation Trust
 Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Information on the Chiropractic Care of Lower Back Pain
 Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Case Studies Updated 10.24.11
 S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated And Fenestrated Pedicle
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
LOW BACK PAIN. common of these conditions include: muscle strain ( pulled muscle ), weak core muscles
 LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
REVIEW DECISION. Review Reference #: R0103014 Board Decision under Review: March 3, 2009
 REVIEW DECISION Re: Review Reference #: R0103014 Board Decision under Review: March 3, 2009 Date: Review Officer: Lyall Zucko The worker requests a review of the decision of WorkSafeBC (the Board) dated
REVIEW DECISION Re: Review Reference #: R0103014 Board Decision under Review: March 3, 2009 Date: Review Officer: Lyall Zucko The worker requests a review of the decision of WorkSafeBC (the Board) dated
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
SPINAL FUSION. North American Spine Society Public Education Series
 SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Image-guided Spine Procedures for Relief of Severe Lower Back Pain:
 Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults
 Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Overview Anatomy of the spinal canal What is spinal stenosis? > 1
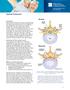 Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Spinal Decompression: Laminectomy & Laminotomy
 Spinal Decompression: Laminectomy & Laminotomy Overview Narrowing of the spinal canal, a condition called spinal stenosis can cause chronic pain, numbness, and muscle weakness in your arms or legs (Fig.
Spinal Decompression: Laminectomy & Laminotomy Overview Narrowing of the spinal canal, a condition called spinal stenosis can cause chronic pain, numbness, and muscle weakness in your arms or legs (Fig.
There are four main regions of the back; the cervical (C), thoracic (T), lumbar (L), and sacral (S) regions
 Low Back Pain Overview Low back pain is one of the most common disorders in the United States. About 80 percent of people have at least one episode of low back pain during their lifetime. Factors that
Low Back Pain Overview Low back pain is one of the most common disorders in the United States. About 80 percent of people have at least one episode of low back pain during their lifetime. Factors that
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
 Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
Lower Back Pain. Introduction. Anatomy
 Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
Surgical Guideline for Lumbar Fusion (Arthrodesis)
 I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
Balloon Kyphoplasty. Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures.
 Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
