Intraocular gas in vitreoretinal surgery
|
|
|
- Chester Maxwell
- 10 years ago
- Views:
Transcription
1 REVIEW ARTICLE Intraocular gas in vitreoretinal surgery Shaheeda Mohamed, FRCS, Timothy Y. Y. Lai, MD, FRCS Department of Ophthalmology & Visual Sciences, The Chinese University of Hong Kong, Hong Kong. Correspondence and reprint requests: Dr. Timothy Y. Y. Lai, Department of Ophthalmology and Visual Sciences, The Chinese University of Hong Kong, Hong Kong Eye Hospital, 147K Argyle Street, Hong Kong. Abstract Advances in surgical techniques, instrumentation, and vitreous substitutes over the past few decades have greatly improved the anatomical and functional success of vitreoretinal surgery. Intraocular gases are the most common type of tamponade used in vitreoretinal surgery and they are indispensable for that purpose. A thorough understanding of the properties, indications, and potential complications of intraocular gases is therefore essential to optimizing the outcomes. This article reviews the properties, indications, and complications associated with commonly used intraocular gases in vitreoretinal surgery. Key words: Fluorocarbons; Gases; Vitreous body; Vitrectomy Introduction Vitreous substitutes as surgical adjuncts were described as early as 1911, when Ohm 1 injected air into the vitreous cavity to treat retinal detachment. In 1938, Rosengren 2 further built on this concept with the technique of internal gas tamponade. Modern vitrectomy techniques introduced by Machemer et al 3 in the 1970s accelerated the use of vitreous substitutes for intraoperative and postoperative vitreous replacement. Advances in surgical techniques, instrumentation, and vitreous substitutes over the past few decades have greatly improved the anatomical and functional success rates of vitreoretinal surgery. The three most common types of substitutes in use today are intraocular gas, silicone oil, and perfluorocarbon liquid. This article reviews the properties, indications, and complications associated with commonly used intraocular gases in vitreoretinal surgery. Intraocular gases and kinetics The high surface tension between gas and fluid enables formation of an effective seal around a retinal break, thus allowing the retinal pigment epithelium (RPE) to absorb any remaining subretinal fluid to facilitate reattachment of the retina. 4 Compared to silicone oil and perfluorocarbon liquids, gases provide the highest surface tension. Because the specific gravity of any gas is lower than that of water, the intraocular gas bubble has buoyancy that keeps the retina against the RPE, and this effect is greatest at the apex of the bubble. 5 Buoyancy forces can be directed by careful positioning of the patient s head so that retinal break is placed at the apex of the bubble, until such time as chorioretinal adhesions created by laser photocoagulation or cryotherapy can be established. In cases of giant retinal tear, the buoyancy force of intraocular gases may also be used to unroll the edges of a giant retinal tear. Increasingly however, this role has been supplanted by the introduction of perfluorocarbon liquids. Four different intraocular gases are commonly used in vitreoretinal surgery: air, sulfur hexafluoride (SF 6 ), perfluoroethane (C 2 F 6 ) and perfluoropropane (C 3 F 8 ). In the vitreous cavity, these gases are colorless, odorless and inert. When injected into the vitreous cavity, air does not expand, whereas pure SF 6, C 2 F 6 and C 3 F 8 gases do. When gas enters the vitreous cavity, three phases can be distinguished: expansion, equilibrium and dissolution (Figure 1). The initial expansion is a result of the absorption into the bubble of nitrogen, oxygen and carbon dioxide from the surrounding tissue fluid. The most rapid rate of expansion occurs within the first 6 to 8 hours after gas injection. During the equilibrium phase, the partial pressures in the 2 compartments equilibrate as diffusion of nitrogen into the bubble is balanced by the diffusion of gas into the surrounding fluid. Finally, during dissolution, there 8
2 Figure 1. Phases of intraocular gas kinetics inside the vitreous cavity. is a net exit of gases as they are ultimately absorbed into the bloodstream. Absorption of intraocular gas bubbles is described reasonably accurately by first-order kinetics, which predict that a constant percentage of the volume of the intraocular gas gets absorbed over a given period of time. 6-8 Intraocular gas bubble dynamics depend on several factors, including initial gas concentration and volume, lens status and a history of prior vitrectomy. The physical properties and gas dynamics are summarised in Table 1. A pure SF 6 bubble expands to about double the volume injected within 24 to 48 hours, and exerts an effect for 1 to 2 weeks. A pure C 3 F 8 bubble expands to about 4 times of its original volume within 72 to 96 hours and persists in the vitreous cavity for 6 to 8 weeks. The maximum effective duration of the tamponade is approximately equal to 3 half-lives. 9 Intraocular gases can be used in office or in operative settings. Following vitrectomy for retinal detachment, most vitreoretinal surgeons use a non-expansile gas fill that allows placement of a large gas bubble to tamponade a large area of the retina. In contrast, pneumatic retinopexy involves the injection of a small, usually pure, expansile intraocular gas bubble in a non-vitrectomized eye; the objective being to provide focal tamponade over a retinal break. Intraocular gas may also be used as an adjunct in scleral buckling procedures, and are known as pneumatic buckles. Superior tears with retinal detachment without proliferative vitreoretinopathy (PVR) can be treated with air or short-acting gases such as SF 6. A longer-acting gas such as C 3 F 8 can be used for retinal detachment with inferior tears, giant retinal tears, or more complex rhegmatogenous and tractional retinal detachment cases result in PVR, except when silicone oil is preferred. Techniques of fluid-air exchange and intraocular gas injection Following vitrectomy, intraocular gases are usually injected via the pars plana infusion line after any fluid (e.g. balanced salt solution) in the vitreous cavity is replaced by air. This fluid-air exchange may be performed by passive or active aspiration under direct visualization. With passive aspiration, a silicone tip or flute needle is used and the force of air entering the vitreous cavity through the infusion cannula causes the vitreous fluid to egress through the lumen of the aspiration needle, which is vented to the atmosphere. Fluidair exchange with active aspiration into the vitrectomy cassette is more rapid but may result in hypotony if the aspiration of fluid is faster than the inflow of air. Subretinal fluid in eyes with a retinal detachment is usually removed during the surgery via the retinal break or a drainage retinotomy. The introduction of perfluorocarbon liquids in vitreoretinal surgery has further enhanced surgical techniques. 10 Perfluorocarbon liquids have a higher specific density than water, allowing displacement of subretinal fluid anteriorly via the retinal break and flattening of the retina. Their low viscosity permits easy injection and withdrawal through instruments. Perflurocarbon liquids are also optically clear, and tamponade using perfluorocarbon liquids can facilitate application of endolasers, especially for more posterior Table 1. Physical properties/dynamics of commonly used vitreoretinal surgery gases. Gas Molecular weight Maximal expansion Duration Non-expansile Expansivity (times) (hours) concentration Air 29 N/A 5-7 days N/A 0 SF weeks 20% 2 C 2F weeks 16% 3.3 C 3F weeks 12% 4 Abbreviations: SF6 = sulfur hexafluoride; C2F6 = perfluoroethane; C3F8 = perfluoropropane; N/A = not available. 9
3 are described in detail below. Pneumatic retinopexy in retinal detachment Pneumatic retinopexy is primarily indicated for uncomplicated retinal detachment with retinal breaks involving the superior 8 clock hours of the fundus. The multicenter pneumatic retinopexy trial and other studies have shown that despite lower single-operation success rates (about 74%) with pneumatic retinopexy, the final surgical success rate (about 96%) is comparable with that of scleral buckling procedures. 11,12 Complications of this technique include subretinal passage of gas, iatrogenic retinal breaks, progression of detachment with macular involvement, and PVR. Figure 2. Fish egg bubble formation from gas injection in pneumatic retinopexy. breaks. Perfluorocarbon liquids are not intended as longterm vitreous substitutes and can be exchanged with air and gas or directly with silicone oil. When preparing the gas for injection, a sterile filter (e.g μm millipore) is recommended to prevent microbial contamination of the gas. A 50-ml syringe is flushed several times with the pure gas to avoid dilution of the desired concentration with residual air. The gas should not be left in the syringe for a prolonged period prior to injection, as diffusion will alter the effective gas concentration. For a traditional 20-gauge vitrectomy, one sclerotomy site is closed and the second site is sutured without tying the knot. The temporary closure of the second sclerotomy site involves clamping the infusion tubing to maintain the eye at a constant pressure. The gas syringe is then attached to the infusion tubing and the clamp is removed with gentle opening of the sclerotomy. Approximately 35 to 40 ml of the gas mixture is gently lavaged through the eye as air in the vitreous cavity is expelled through the open sclerotomy. The suture is then tied to close the second sclerotomy site. Finally, the infusion cannula is removed and a suture is used to close the final infusion line sclerotomy site. For a 23- or 25-gauge vitrectomy, gas can be injected via the infusion cannula while the trocars are in place. The trocars can then be removed after injection of 35 to 40 ml of the gas mixture and the integrity of the wound can be assessed. Another technique of injecting gas following vitrectomy is to close the second sclerotomy site completely, and follow-up by lavage of gas into the eye via the infusion cannula while allowing air expulsion using a 25-gauge needle inserted through the pars plana. If the eye becomes soft during closure of the third sclerotomy site, additional gas can be injected at the pars plana via a 30-gauge needle attached to a smaller 3-ml syringe containing the gas mixture. Uses of intraocular gases in vitreoretinal surgery Common uses of intraocular gases in vitreoretinal surgery The technique involves the injection of intraocular gas before or after retinopexy, which creates retinal breaks with cryotherapy or laser, and maintenance of specific head postures after surgery. Preoperative eye drops or medications can be considered to lower intraocular pressure prior to pneumatic retinopexy. The desired volume of gas (usually 0.3 to 0.5 ml) is injected rapidly into the vitreous cavity in order to minimize formation of small fish-egg bubbles (Figure 2). The intraocular pressure is monitored by digital palpation as the gas is injected into the eye. If the eye is already hypotonic after drainage of subretinal fluid, gas may be injected with a 30-gauge needle attached to a 3-ml syringe via the pars plana. If the eye is normotensive, vitreous or aqueous fluid must be removed to allow injection of more than 0.2 ml of gas, which is the maximum volume of gas that can be injected into a normotensive eye. The first method involves making a limbal anterior chamber paracentesis with a slit-knife or 30-gauge needle for aqueous drainage after gas injection. A repeat paracentesis after 5 to 10 minutes may normalize the pressure if the intraocular pressure remains elevated. The second method involves the aspiration of vitreous fluid before gas injection, using a 22- to 25-gauge needle attached to a 1- or 3-ml syringe placed via the pars plana. This method allows a larger volume of gas to be injected than the first paracentesis technique. The latter method, however, may increase the risk of retinal complications during the vitreous aspiration. 13 Intraocular gases can also be injected in association with scleral buckling procedures, especially when there is substantial residual subretinal fluid. The intraocular pressure should also be monitored for 6 hours post-injection as this is the time of maximal gas expansion. Macular hole surgery In the original description of macular hole repair by Kelly and Wendel, 14 the surgery was a 5-step procedure: posterior vitrectomy, posterior hyaloid removal, internal limiting membrane removal, intraocular gas tamponade, and 1 week of face-down posturing postoperatively. The presence of intraocular gas provides isolation or waterproofing of the macular hole from the vitreous cavity by surface-tension at the gas-liquid interface. It may also mechanically tamponade the hole and provide a template over which a nascent bridging membrane forms. The duration of gas tamponade that is required for macular hole closure has come under debate in recent years. Recent reports have shown that hole 10
4 closure can occur as early as the first postoperative day, suggesting that prolonged gas tamponade and face-down posturing may be unnecessary. Similar macular hole closure rates have been reported in studies comparing air versus 20% SF 6, and with 20% SF 6 versus 12-16% C 3 F 8. 5,15,16 Pneumatic displacement of submacular hemorrhage Submacular hemorrhage can result in sudden dramatic visual loss, and has many causes such as choroidal neovascularization, polypoidal choroidal vasculopathy, trauma and retinal artery macroaneurysm. The visual prognosis might be poor, especially if there is delayed presentation, a thick hemorrhage, foveal involvement, and an underlying choroidal neovascularization. Distinction should also be made between subretinal and sub-rpe hemorrhage as pneumatic displacement is generally not indicated for the latter, due to difficulty in displacing the hemorrhage. The technique of pneumatic displacement involves the injection of an expansile pure C 3 F 8 gas (about 0.3 ml) via the pars plana at 3.5 mm from the limbus with a 30-gauge needle, followed by strict prone positioning for 5 to 7 days. Intravitreal tissue plasminogen activator or intravitreal anti vascular endothelial growth factor (anti-vegf) agents may also be injected at the same setting using expansile gas as adjuvants Unrolling giant retinal tear A giant retinal tear may be unrolled using an intraocular gas bubble by placing the patient in a prone position and injecting gas via the infusion cannula, while removing fluid from the anterior vitreous cavity at the same time (upside down fluid-gas exchange). The gas bubble will expand in the vitreous cavity and push the retina against the underlying RPE, unrolling the edges of the giant retinal tear as the subretinal fluid moves to the anterior vitreous and is removed through an aspiration needle via the sclerotomy, which is in a dependent position. The patient is then returned to a supine position. Postoperatively, the patient should remain in a prone position to avoid slippage of the giant retinal tear edge. The use of gas to unroll the giant retinal tear is now mostly historical, since the availability of perfluorocarbon liquids has allowed a more convenient technique for unrolling the edges of a giant tear. Postoperative positioning and duration of positioning Appropriate postoperative positioning is dictated by the size of the intraocular gas bubble, the location of the retinal tear and lens status. Prone positioning in phakic patients can potentially reduce prolonged gas contact with the posterior lens surface. Pseudophakic and aphakic patients with retinal breaks in the superior periphery may avoid prolonged prone positioning because the gas bubble will provide good tamponade in the upright position. The duration of postoperative positioning is determined by the location of the retinal breaks and the absorption rate of the intraocular gas bubble. An appropriate gas concentration is chosen to provide an adequate duration of tamponade. Superior retinal breaks without a large area of retinal detachment may be treated with air. Shorter-acting gas mixtures like 5% C 3 F 8 or 20% SF 6 may be used to treat superior retinal breaks associated with retinal detachment. Inferior retinal breaks associated with retinal detachment may be treated with longer-acting 12% C 3 F 8, so that the gas bubble remains large enough for at least 10 days in order to provide adequate tamponade for this particular retinal break to close. Complex retinal detachments with PVR or giant retinal tears usually require prolonged gas tamponade with 10 to 15% C 3 F 8 gas mixtures. Contraindications for intraocular gas Postoperatively, patients with intraocular gases in situ should be advised against air travel or travelling to high altitudes, since the reduced atmospheric pressure under these conditions will lead to expansion of the intraocular gas bubble and cause considerable increase in intraocular pressure. Early manifestations include pain and decreased vision, which may be treated by prompt decent to a lower altitude. In extreme cases, the rise in intraocular pressure can result in retinal vascular occlusions and even globe explosion via surgical wounds. Experimental studies and clinical observations suggested that less than 0.6 to 1.0 ml of residual gas might be safe for air travel. 23,24 It is nevertheless advisable for the patients to avoid any air travel when there is a residual intravitreal gas bubble. Patients with intraocular gases in situ should also avoid diving. At sea level, the body is exposed to an ambient pressure of one atmosphere absolute (ATA). When diving, the absolute pressure is expressed by the formula ATA= [depth (in feet of sea water) +33]/33. Hyperbaric pressures that occur during scuba diving cause the intraocular gas bubble to decrease in size according to Boyle s law, leading to hypotony and partial globe collapse. As the eye goes from hyperbaric conditions to normal sea level, atmospheric pressure during the ascent to water surface decreases, resulting in expansion of the intraocular gas bubble and can cause a large increase in intraocular volume. Such pressureinduced changes in the volume of the gas bubble can also result in vitreous, retinal or choroidal hemorrhage. 25 Nitrous oxide anesthesia should also be avoided in patients with intraocular gas bubbles. Since nitrous oxide in the blood is highly water-soluble, it enters the intraocular gas bubble and can lead to increased intraocular pressure whenever sclerotomies are closed. Later, as the nitrous oxide in the gas bubble returns to the bloodstream, the eye becomes hypotonous. If nitrous oxide anesthesia has been commenced during eye surgery, it should be discontinued at least 30 minutes prior to the injection of intraocular gas in order to facilitate its clearance from the bloodstream and tissues. 26 Complications of intraocular gases Complications associated with the use of intraocular gas are detailed below. Elevation of intraocular pressure Elevation of intraocular pressure is one of the more 11
5 It usually develops in the first few postoperative days in a patient who is poorly compliant to prone positioning. The posterior subcapsular feathering may be reversible by diligent prone positioning, but if the patient remains noncompliant for more than a week, permanent changes such as lens vacuolation or a diffuse posterior subcapsular cataract may develop. 28 Figure 3. Postoperative lens changes with intraocular gas in situ. Figure 4. Migration of intraocular gas into the subconjunctival space. common complications in eyes with an intraocular gas bubble. Predisposing factors include pre-existing glaucoma, anterior synechiae, and impaired aqueous outflow at the drainage angle by hemorrhage, pigment, inflammation and neovascularization. 27 In the majority of eyes, the elevation in intraocular pressure is transient and can be managed with topical or systemic anti-glaucoma agents. If the gas bubble expands to such an extent that the lens-iris diaphragm shifts forward and leads to angle-closure glaucoma, gas aspiration from the vitreous cavity (via the pars plana) may be indicated. Injection of viscoelastics may help in reformation of the flat anterior chamber. Aphakic eyes may be more prone to angle closure with a very large intraocular gas bubble because the iris can easily be pushed forward. This is especially likely when the patient is lying supine. Poor compliance with prone positioning may precipitate this complication. Subsequent evaluation of the anterior chamber angle of the operated eye and the fellow eye by gonioscopy can help determine whether a peripheral laser iridotomy is indicated. Cataract Cataract may result from progressive nuclear sclerosis due to oxidative stress to the lens or trauma following vitrectomy. Prolonged contact of intraocular gas with the posterior lens surface can lead to gas-induced cataract, presenting typically as lens feathering, a manifestation of branching pattern of posterior subcapsular lens changes (Figure 3). Migration of intraocular gas bubble Migration of intraocular gas bubble into the subretinal space can rarely occur as a result of pneumatic retinopexy. This ensues if the tear is larger than the bubble, or during fluidgas exchange when there is unrelieved traction on the retina, or when the gas is injected accidentally into the subretinal space. Although the subretinal intraocular gas bubble is eventually absorbed, the retinal break may not be properly sealed by the gas bubble and thus redetachment can occur. Intraocular gas can also migrate out of the sclerotomy into the subconjunctival space if the wound integrity is not secured at the end of surgery (Figure 4). In phakic or pseudophakic patients, an intraocular gas bubble may also migrate into the anterior chamber via weakened zonules or larger posterior capsulotomy. Prolonged contact of gas with the corneal endothelium in aphakic eyes can lead to corneal decompensation. 29 These patients should be reminded to avoid sleeping in a supine position. Gas injection in eyes with an iris claw anterior chamber intraocular lens might also cause the intraocular lens to flip around its axis and intraocular lens removal or use of silicone oil might be preferable in these cases. Inadequate gas bubble size Inadequate gas bubble may ensue if the surgery is completed with a smaller-than-desired intraocular gas bubble due to removal of inadequate vitreous or subretinal fluid and exchange with air. Alternatively, intraocular gas escapes through a sclerotomy during the perioperative period could lead to loss of intravitreal gas and hypotony. Inadequate gas bubble size may also be caused by premature absorption of the gas due to errors in reconstituting the gas mixture. Other complications Other complications include iatrogenic retinal breaks and PVR, which are important causes of surgical failure after injection of intraocular gases. Visual field defects have also been reported in eyes subjected to macular hole surgery. Prolonged contact of the intraocular gas bubble with the nerve fiber layer has been postulated to have a role in causing such defects. However, other reports have associated these visual field defects with surgical trauma or the use of certain intraoperative stains, like indocyanine green. Conclusion The intraocular gas bubble is one of the most useful surgical adjuncts in vitreoretinal surgery. A thorough understanding of its properties, indications and potential complications of intraocular gases is essential to optimizing the outcomes of vitreoretinal surgery. 12
6 References 1. Olm J. Über die Behandlung der Netzhautablösung durch operative Entleerung der Subretinalen Flüssigkeit und Einspritzung von Luft in den Glaskörper. Albrecht von Graefes Arch Ophthalmol. 1911;79: Rosengren B. Results of treatment of detachment of the retina with diathermy and injection of air into the vitreous. Acta Ophthalmol. 1938;16: Machemer R, Buettner H, Norton EW, Parel JM. Vitrectomy: a pars plana approach. Trans Am Acad Ophthalmol Otolaryngol. 1971;75: de Juan E Jr, McCuen B, Tiedeman J. Intraocular tamponade and surface tension. Surv Ophthalmol. 1985;30: Gupta D. Face-down posturing after macular hole surgery: a review. Retina. 2009;29: Abrams GW, Edelhauser HF, Aaberg TM, Hamilton LH. Dynamics of intravitreal sulfur hexafluoride gas. Invest Ophthalmol. 1974;13: Lincoff A, Haft D, Liggett P, Reifer C. Intravitreal expansion of perfluorocarbon bubbles. Arch Ophthalmol. 1980;98: Lincoff H, Mardirossian J, Lincoff A, Liggett P, Iwamoto T, Jakobiec F. Intravitreal longevity of three perfluorocarbon gases. Arch Ophthalmol. 1980;98: Thompson JT. Kinetics of intraocular gases. Disappearance of air, sulfur hexafluoride, and perfluoropropane after pars plana vitrectomy. Arch Ophthalmol. 1989;107: Chang S. Low viscosity liquid fluorochemicals in vitreous surgery. Am J Ophthalmol. 1987;103: Chan CK, Lin SG, Nuthi AS, Salib DM. Pneumatic retinopexy for the repair of retinal detachments: a comprehensive review ( ). Surv Ophthalmol. 2008;53: Tornambe PE, Poliner LS, Hilton GF, Grizzard WS. Comparison of pneumatic retinopexy and scleral buckling in the management of primary rhegmatogenous retinal detachment. Am J Ophthalmol. 1999;127: Hilton GF, Das T, Majji AB, Jalali S. Pneumatic retinopexy: principles and practice. Indian J Ophthalmol. 1996;44: Kelly NE, Wendel RT. Vitreous surgery for idiopathic macular holes. Results of a pilot study. Arch Ophthalmol. 1991;109: Hasegawa Y, Hata Y, Mochizuki Y, et al. Equivalent tamponade by room air as compared with SF(6) after macular hole surgery. Graefes Arch Clin Exp Ophthalmol. 2009;247: Kim SS, Smiddy WE, Feuer WJ, Shi W. Outcomes of sulfur hexafluoride (SF6) versus perfluoropropane (C3F8) gas tamponade for macular hole surgery. Retina. 2008;28: Ohji M, Saito Y, Hayashi A, Lewis JM, Tano Y. Pneumatic displacement of subretinal hemorrhage without tissue plasminogen activator. Arch Ophthalmol. 1998;116: Daneshvar H, Kertes PJ, Leonard BC, Peyman GA. Management of submacular hemorrhage with intravitreal sulphur hexafluoride: a pilot study. Can J Ophthalmol. 1999;34: Mahesh G, Giridhar A, Saikumar SJ, Elias A. Intravitreal gas for submacular haemorrhage. Indian J Ophthalmol. 2003;51: Ogawa T, Kitaoka T, Mera A, Saitoh AK, Amemiya T. Treatment of subretinal hemorrhage in the macula: pneumatic displacement of hemorrhages. Retina. 2000;20: Gopalakrishan M, Giridhar A, Bhat S, Saikumar SJ, Elias A, N S. Pneumatic displacement of submacular hemorrhage: safety, efficacy, and patient selection. Retina. 2007;27: Chawla S, Misra V, Khemchandani M. Pneumatic displacement and intravitreal bevacizumab: a new approach for management of submacular hemorrhage in choroidal neovascular membrane. Indian J Ophthalmol. 2009;57: Mills MD, Devenyi RG, Lam WC, Berger AR, Beijer CD, Lam SR. An assessment of intraocular pressure rise in patients with gas-filled eyes during simulated air flight. Ophthalmology. 2001;108: Lincoff H, Weinberger D, Stergiu P. Air travel with intraocular gas. II. Clinical considerations. Arch Ophthalmol. 1989;107: Butler FK Jr. Diving and hyperbaric ophthalmology. Surv Ophthalmol. 1995;39: Fu AD, McDonald HR, Eliott D, et al. Complications of general anesthesia using nitrous oxide in eyes with preexisting gas bubbles. Retina. 2002;22: Gedde SJ. Management of glaucoma after retinal detachment surgery. Curr Opin Ophthalmol. 2002;13: Chang S, Lincoff HA, Coleman DJ, Fuchs W, Farber ME. Perfluorocarbon gases in vitreous surgery. Ophthalmology. 1985;92: Lee DA, Wilson MR, Yoshizumi MO, Hall M. The ocular effects of gases when injected into the anterior chamber of rabbit eyes. Arch Ophthalmol. 1991;109:
Retinal Detachments Mark E. Hammer, M.D. Ivan J. Suñer, M.D. Marc C. Peden, M.D.
 Retinal Detachments Mark E. Hammer, M.D. Ivan J. Suñer, M.D. Marc C. Peden, M.D. What is a retinal detatchment? The retina is the light sensitive layer covering the inside of the back of the eye. It is
Retinal Detachments Mark E. Hammer, M.D. Ivan J. Suñer, M.D. Marc C. Peden, M.D. What is a retinal detatchment? The retina is the light sensitive layer covering the inside of the back of the eye. It is
Macular Hole. James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D.
 Macular Hole James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D. (804) 285-5300 or (804) 287-4200 www.vaeye.com Macular Hole In order to maintain
Macular Hole James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D. (804) 285-5300 or (804) 287-4200 www.vaeye.com Macular Hole In order to maintain
iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels
 iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels Normal Eye 474. Normal Eye overview 476. Cornea - overview
iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels Normal Eye 474. Normal Eye overview 476. Cornea - overview
Comparison of Silicone Oil Versus Gas Tamponade in the Treatment of Idiopathic Full-thickness Macular Hole
 Comparison of Silicone Versus Tamponade in the Treatment of Idiopathic Full-thickness Macular Hole James C. Lai, MD, 1 Sandra S. Stinnett, DrPH, 1,2 Brooks W. McCuen, II, MD 1 Purpose: To compare anatomic
Comparison of Silicone Versus Tamponade in the Treatment of Idiopathic Full-thickness Macular Hole James C. Lai, MD, 1 Sandra S. Stinnett, DrPH, 1,2 Brooks W. McCuen, II, MD 1 Purpose: To compare anatomic
Advanced Technology Expands the Role of Microincisional Vitrectomy Surgery
 Advanced Technology Expands the Role of Microincisional Vitrectomy Surgery By Manish Nagpal, MS, DO, FRCS(UK) There are several components to successful vitreoretinal surgery, and of course, surgeon skill
Advanced Technology Expands the Role of Microincisional Vitrectomy Surgery By Manish Nagpal, MS, DO, FRCS(UK) There are several components to successful vitreoretinal surgery, and of course, surgeon skill
Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling.
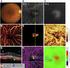 Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling. Robert Gizicki MD, Mohamed Haji, Flavio Rezende Retina Service, Hôpital Maisonneuve-Rosemont,
Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling. Robert Gizicki MD, Mohamed Haji, Flavio Rezende Retina Service, Hôpital Maisonneuve-Rosemont,
Descemet s Stripping Endothelial Keratoplasty (DSEK)
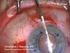 Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
COLORED PERFLUOROCARBON LIQUIDS IN VITREORETINAL SURGERY IN THE PIG EYE
 COLORED PERFLUOROCARBON LIQUIDS IN VITREORETINAL SURGERY IN THE PIG EYE Fábio Miguel Vasconcelos Trindade PhD Thesis José García-Arumí, PhD, Ophthalmologist-in-Chief of Vall D Hebron Hospital and Professor
COLORED PERFLUOROCARBON LIQUIDS IN VITREORETINAL SURGERY IN THE PIG EYE Fábio Miguel Vasconcelos Trindade PhD Thesis José García-Arumí, PhD, Ophthalmologist-in-Chief of Vall D Hebron Hospital and Professor
Retinal Detachment Information
 http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Mark D. Lomeo, M.D. Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M.
http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Mark D. Lomeo, M.D. Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M.
Retina, Cornea and Other Eye Procedures. Current Procedural Terminology 2013 American Medical Association. All Rights Reserved.
 Retina, Cornea and Other Eye Procedures Segment vs. Chamber Contains both the anterior & posterior chambers Lens focuses light onto the retina for image clarity Zonules muscles of ciliary body that shape
Retina, Cornea and Other Eye Procedures Segment vs. Chamber Contains both the anterior & posterior chambers Lens focuses light onto the retina for image clarity Zonules muscles of ciliary body that shape
Vitrectomy Eye Surgery
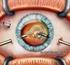 Vitrectomy Eye Surgery Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Vitreous
Vitrectomy Eye Surgery Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Vitreous
Vitrectomy surgery for macular holes. Macular hole surgery without routine membrane excision or use of adjuvants. Materials and Methods
 Macular hole surgery without routine membrane excision or use of adjuvants Eva Byhr and Bertil Lindblom Department of Ophthalmology, Sahlgren s University Hospital, Gothenburg, Sweden ABSTRACT. Purpose:
Macular hole surgery without routine membrane excision or use of adjuvants Eva Byhr and Bertil Lindblom Department of Ophthalmology, Sahlgren s University Hospital, Gothenburg, Sweden ABSTRACT. Purpose:
Perfluoron and Silicone Oil for Complex Retinal Detachments
 Perfluoron and Silicone Oil for Complex Retinal Detachments STEVEN M. COHEN, MD The development of perfluorocarbon liquids for use in vitreoretinal surgery by Stanley Chang, MD, revolutionized the treatment
Perfluoron and Silicone Oil for Complex Retinal Detachments STEVEN M. COHEN, MD The development of perfluorocarbon liquids for use in vitreoretinal surgery by Stanley Chang, MD, revolutionized the treatment
List of Abbreviations (Condition) Clinical Pearls in Vitreoretinal Surgery. List of Abbreviations (Procedure) PPV indications
 List of Abbreviations (Condition) Clinical Pearls in Vitreoretinal Surgery Mohammad Rafieetary, O.D., F.A.A.O. Charles Retina Institute Memphis, TN [email protected] EMM = Epimacular Membrane
List of Abbreviations (Condition) Clinical Pearls in Vitreoretinal Surgery Mohammad Rafieetary, O.D., F.A.A.O. Charles Retina Institute Memphis, TN [email protected] EMM = Epimacular Membrane
 Cataract Surgery in Small Eyes Richard S. Hoffman, MD Clinical Associate Professor of Ophthalmology Oregon Health & Science University No Financial Interests Anatomic Classification Short AC depth with
Cataract Surgery in Small Eyes Richard S. Hoffman, MD Clinical Associate Professor of Ophthalmology Oregon Health & Science University No Financial Interests Anatomic Classification Short AC depth with
1981-1982 Ophthalmic Consultants Northwest, Seattle, Washington Retinal and vitreous consultation and surgery
 EDUCATION Richard S. Munsen Jr., MD University of Washington Eye Institute HMC Box 359608, 325 Ninth Ave, Seattle WA 98104-2499 (206) 744-2020 for patient appointments, Fax (206) 897-4320 Academic phone
EDUCATION Richard S. Munsen Jr., MD University of Washington Eye Institute HMC Box 359608, 325 Ninth Ave, Seattle WA 98104-2499 (206) 744-2020 for patient appointments, Fax (206) 897-4320 Academic phone
Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) John D. Goosey, MD Introduction DSAEK is a corneal transplant technique where the unhealthy, diseased, posterior portion of a patient s cornea
Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) John D. Goosey, MD Introduction DSAEK is a corneal transplant technique where the unhealthy, diseased, posterior portion of a patient s cornea
Financial Disclosures. Vitreo-Retinal Surgery in Uveitis Patients. Before we start ask yourself. Vitreo-retinal Surgery in the Uveitis Patient
 Financial Disclosures Vitreo-Retinal Surgery in Uveitis Patients Advisory Board Bausch and Lomb, Eleven Research Support Bausch and Lomb, Allergan, Novartis Consultancy Bausch and Lomb Sunil K. Srivastava,
Financial Disclosures Vitreo-Retinal Surgery in Uveitis Patients Advisory Board Bausch and Lomb, Eleven Research Support Bausch and Lomb, Allergan, Novartis Consultancy Bausch and Lomb Sunil K. Srivastava,
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com
 Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY Applies to: All Ophthalmology Residents, including those in ACGME- and non-acgme-accredited specialty
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY Applies to: All Ophthalmology Residents, including those in ACGME- and non-acgme-accredited specialty
NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION
 NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION Section: E Revision History Revised 01/97; 05/03; 02/08; 04/08; 03/09; 05/09; 12/09; 01/11; 12/14 An individual is
NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION Section: E Revision History Revised 01/97; 05/03; 02/08; 04/08; 03/09; 05/09; 12/09; 01/11; 12/14 An individual is
Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy
 Medical Care for the Elderly Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy JMAJ 46(1): 27 32, 2003 Shigehiko KITANO Professor, Department of Ophthalmology, Diabetes Center,
Medical Care for the Elderly Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy JMAJ 46(1): 27 32, 2003 Shigehiko KITANO Professor, Department of Ophthalmology, Diabetes Center,
Cataract Surgery after Myopic Refractive Procedures. Ray Guard Eye Center Huang Wei-Jen, MD
 Cataract Surgery after Myopic Refractive Procedures Ray Guard Eye Center Huang Wei-Jen, MD Financial Disclosures : * No financial interest on products mentioned Cataract Surgery after Myopic Refractive
Cataract Surgery after Myopic Refractive Procedures Ray Guard Eye Center Huang Wei-Jen, MD Financial Disclosures : * No financial interest on products mentioned Cataract Surgery after Myopic Refractive
Introduction Houston Retina Associates
 1 2 Introduction This book was written by Houston Retina Associates to provide our patients with basic knowledge about retinal anatomy, an introduction to some of the diagnostic tests and treatments used
1 2 Introduction This book was written by Houston Retina Associates to provide our patients with basic knowledge about retinal anatomy, an introduction to some of the diagnostic tests and treatments used
THE EYES IN MARFAN SYNDROME
 THE EYES IN MARFAN SYNDROME Marfan syndrome and some related disorders can affect the eyes in many ways, causing dislocated lenses and other eye problems that can affect your sight. Except for dislocated
THE EYES IN MARFAN SYNDROME Marfan syndrome and some related disorders can affect the eyes in many ways, causing dislocated lenses and other eye problems that can affect your sight. Except for dislocated
EXPANDING YOUR HORIZONS
 Glaucoma Therapy EXPANDING YOUR HORIZONS Learn how to control glaucoma with SLT therapy. SLTPATIENT EDUCATION PROGRAM Glaucoma Glaucoma is a degenerative disease that if left untreated can cause permanent
Glaucoma Therapy EXPANDING YOUR HORIZONS Learn how to control glaucoma with SLT therapy. SLTPATIENT EDUCATION PROGRAM Glaucoma Glaucoma is a degenerative disease that if left untreated can cause permanent
Cataract Testing. What a Patient undergoes prior to surgery
 Cataract Testing What a Patient undergoes prior to surgery FINANCIAL DISCLOSURE I have no financial interest or relationships to disclose What do most Technicians find to be the most mundane yet very important
Cataract Testing What a Patient undergoes prior to surgery FINANCIAL DISCLOSURE I have no financial interest or relationships to disclose What do most Technicians find to be the most mundane yet very important
Three Additional Questions For WAMD Dutch Guidelines (Searches And Extractions)
 Three Additional Questions For WAMD Dutch Guidelines (Searches And Extractions) Kleijnen Systematic Reviews Ltd April 2013 Kleijnen Systematic Reviews Ltd Unit 6, Escrick Business Park Riccall Road Escrick
Three Additional Questions For WAMD Dutch Guidelines (Searches And Extractions) Kleijnen Systematic Reviews Ltd April 2013 Kleijnen Systematic Reviews Ltd Unit 6, Escrick Business Park Riccall Road Escrick
PNEUMATIC RETINOPEXY ERIC S. MANN, M.D. PH. D.
 PNEUMATIC RETINOPEXY ERIC S. MANN, M.D. PH. D. A. Retinal Detachment You have been diagnosed to have a retinal detachment which requires surgical repair. The retina is the nerve tissue membrane that lines
PNEUMATIC RETINOPEXY ERIC S. MANN, M.D. PH. D. A. Retinal Detachment You have been diagnosed to have a retinal detachment which requires surgical repair. The retina is the nerve tissue membrane that lines
PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D.
 PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D. A. INDICATIONS: Periocular steroid injection involves placement of steroid around the eye to treat intraocular inflammation or swelling of
PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D. A. INDICATIONS: Periocular steroid injection involves placement of steroid around the eye to treat intraocular inflammation or swelling of
Spontaneous and Surgical Trauma to the Eye. Richard R Dubielzig
 Spontaneous and Surgical Trauma to the Eye Richard R Dubielzig Ocular Trauma Expulsive Choroidal Hemorrhage Sudden Loss of Intraocular Pressure Early Cellular Events after Trauma Lens Epithelial Cell
Spontaneous and Surgical Trauma to the Eye Richard R Dubielzig Ocular Trauma Expulsive Choroidal Hemorrhage Sudden Loss of Intraocular Pressure Early Cellular Events after Trauma Lens Epithelial Cell
Glaucoma affects over two million Americans. Although only the minority of these
 Glaucoma surgical coding remains a challenge L. Neal Freeman, MD, MBA, CCS-P, FACS Column Editor, "coding.doc" Adapted for publication in Ophthalmology Times Glaucoma affects over two million Americans.
Glaucoma surgical coding remains a challenge L. Neal Freeman, MD, MBA, CCS-P, FACS Column Editor, "coding.doc" Adapted for publication in Ophthalmology Times Glaucoma affects over two million Americans.
Laser Procedure Note
 Laser Procedure Note Patient Name Date 1. Pre procedure diagnosis 2. Procedure and Eye Eye: 3. Pre procedure topical medications administered (and time) 4. Vital signs BP / HR Acuity OD: OS: 5. IOP: OD
Laser Procedure Note Patient Name Date 1. Pre procedure diagnosis 2. Procedure and Eye Eye: 3. Pre procedure topical medications administered (and time) 4. Vital signs BP / HR Acuity OD: OS: 5. IOP: OD
Some of the ophthalmic surgeries performed at the DMV Center.
 Some of the ophthalmic surgeries performed at the DMV Center. This document presents some types of the surgeries performed by the ophthalmology service at the DMV veterinary center as well as the equipment
Some of the ophthalmic surgeries performed at the DMV Center. This document presents some types of the surgeries performed by the ophthalmology service at the DMV veterinary center as well as the equipment
Having a vitrectomy- surgery to
 Having a vitrectomy- surgery to repair your retinal detachment If you need information on audiotape about having a vitrectomy or your hospital visit, please call 020 7188 8815. You have been given this
Having a vitrectomy- surgery to repair your retinal detachment If you need information on audiotape about having a vitrectomy or your hospital visit, please call 020 7188 8815. You have been given this
INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE DETAILED TABLE
 Proposed Disease Severity Level No apparent Mild Non- Proliferative Moderate Nonproliferative Severe Non- Proliferative Proliferative INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE
Proposed Disease Severity Level No apparent Mild Non- Proliferative Moderate Nonproliferative Severe Non- Proliferative Proliferative INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE
Tucson Eye Care, PC. Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens
 Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Complications of Strabismus Surgery
 Complications of Strabismus Surgery Tjeerd de Faber, Martha Tjon Rutger van Ruyven Alexis Damanakis Ondercorrectie Overcorrectie Wat vind je erger? 1 DELLEN Corneal dellen are small areas of thinning associated
Complications of Strabismus Surgery Tjeerd de Faber, Martha Tjon Rutger van Ruyven Alexis Damanakis Ondercorrectie Overcorrectie Wat vind je erger? 1 DELLEN Corneal dellen are small areas of thinning associated
LASER TREATMENT FOR RETINAL BREAK OR LATICE DEGENERATION ERIC MANN M.D., Ph.D.
 LASER TREATMENT FOR RETINAL BREAK OR LATICE DEGENERATION ERIC MANN M.D., Ph.D. A. INTRODUCTION Retinal break is an opening on the retina, usually located at the periphery. There may be a hole, or tear.
LASER TREATMENT FOR RETINAL BREAK OR LATICE DEGENERATION ERIC MANN M.D., Ph.D. A. INTRODUCTION Retinal break is an opening on the retina, usually located at the periphery. There may be a hole, or tear.
United Kingdom National Ophthalmology Database Study of Vitreoretinal Surgery: Report 1; Case mix, complications, and cataract
 (2013) 27, 644 651 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye CLINICAL STUDY United Kingdom National Ophthalmology Database Study of Vitreoretinal Surgery:
(2013) 27, 644 651 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye CLINICAL STUDY United Kingdom National Ophthalmology Database Study of Vitreoretinal Surgery:
INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY
 INTRODUCTION INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
INTRODUCTION INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
Cataracts. Cataract and Primary Eye Care Service...215-928-3041. Main Number...215-928-3000. Physician Referral...1-877-AT-WILLS 1-877-289-4557
 Main Number...215-928-3000 Physician Referral...1-877-AT-WILLS 1-877-289-4557 Emergency Service...215-503-8080 Cataract and Primary Eye Care Service...215-928-3041 Retina Service... 215-928-3300 Cataract
Main Number...215-928-3000 Physician Referral...1-877-AT-WILLS 1-877-289-4557 Emergency Service...215-503-8080 Cataract and Primary Eye Care Service...215-928-3041 Retina Service... 215-928-3300 Cataract
Nick Strouthidis MBBS MD PhD FRCS FRCOphth FRANZCO CONSULTANT OPHTHALMIC SURGEON
 TUBES/SHUNTS TUBES/SHUNTS Implantation of a glaucoma drainage device (GDD - also known as a tube or aqueous shunt) works by diverting aqueous from the front of the eye via a tube to a drainage plate stitched
TUBES/SHUNTS TUBES/SHUNTS Implantation of a glaucoma drainage device (GDD - also known as a tube or aqueous shunt) works by diverting aqueous from the front of the eye via a tube to a drainage plate stitched
INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY
 INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
Verisyse Phakic IOL. Facts You Need to Know About Implantation of the Verisyse Phakic IOL (-5 to -20 D) for the Correction of Myopia (Nearsightedness)
 Verisyse Phakic IOL Facts You Need to Know About Implantation of the Verisyse Phakic IOL (-5 to -20 D) for the Correction of Myopia (Nearsightedness) Patient Information Brochure This brochure is designed
Verisyse Phakic IOL Facts You Need to Know About Implantation of the Verisyse Phakic IOL (-5 to -20 D) for the Correction of Myopia (Nearsightedness) Patient Information Brochure This brochure is designed
EYE SURGERY Retinal Detachment
 EYE SURGERY Retinal Detachment Definition: Retinal detachment occurs when the retina becomes separated from it s underlying support tissue called the choroid, resulting in visual impairement dependaing
EYE SURGERY Retinal Detachment Definition: Retinal detachment occurs when the retina becomes separated from it s underlying support tissue called the choroid, resulting in visual impairement dependaing
AcrySof IQ Toric IOL (SN6ATT) Surgeon Keys for Success & Acknowledgement
 AcrySof IQ Toric IOL (SN6ATT) Surgeon Keys for Success & Acknowledgement Alcon Laboratories, Inc is pleased to announce the availability of the AcrySof IQ Toric intraocular lens, and delighted that you
AcrySof IQ Toric IOL (SN6ATT) Surgeon Keys for Success & Acknowledgement Alcon Laboratories, Inc is pleased to announce the availability of the AcrySof IQ Toric intraocular lens, and delighted that you
Medicare Controversies in Cataract Coding One Consultant s Opinion. Riva Lee Asbell Philadelphia, PA
 Medicare Controversies in Cataract Coding One Consultant s Opinion INTRODUCTION Riva Lee Asbell Philadelphia, PA It would seem that coding for cataract surgery is a straightforward affair not so at all.
Medicare Controversies in Cataract Coding One Consultant s Opinion INTRODUCTION Riva Lee Asbell Philadelphia, PA It would seem that coding for cataract surgery is a straightforward affair not so at all.
Oxford Eye Hospital. Vitrectomy. Information for patients
 Oxford Eye Hospital Vitrectomy Information for patients What is a Vitrectomy The vitreous humour is normally a clear, transparent jelly-like substance inside the eye. It lies behind the iris (the coloured
Oxford Eye Hospital Vitrectomy Information for patients What is a Vitrectomy The vitreous humour is normally a clear, transparent jelly-like substance inside the eye. It lies behind the iris (the coloured
SECONDARY GLAUCOMA: Pseudoexfoliation (PXF), Pigmentary Dispersion Syndrome (PDS), Neovascular (NV), Uveitic
 SECONDARY GLAUCOMA: Pseudoexfoliation (PXF), Pigmentary Dispersion Syndrome (PDS), Neovascular (NV), Uveitic Many roads can lead to glaucoma. With the exception of primary open-angle glaucoma (POAG) and
SECONDARY GLAUCOMA: Pseudoexfoliation (PXF), Pigmentary Dispersion Syndrome (PDS), Neovascular (NV), Uveitic Many roads can lead to glaucoma. With the exception of primary open-angle glaucoma (POAG) and
Neovascular glaucoma is a serious complication of systemic
 GLAUCOMA SURGERY Robert F. Haverly, MD, FACS Abstract: Neovascular glaucoma is a vision- and eye-threatening disease that carries a poor prognosis. Understanding the cause of neovascular glaucoma with
GLAUCOMA SURGERY Robert F. Haverly, MD, FACS Abstract: Neovascular glaucoma is a vision- and eye-threatening disease that carries a poor prognosis. Understanding the cause of neovascular glaucoma with
Taking Your Fundus Exam to the Next Level
 Taking Your Fundus Exam to the Next Level Dr. Kelly Thompson Cincinnati VA Medical Center Taking Your Fundus Exam to the Next Level Resident Assistants Student Subjects Fundus Biomicroscopy Indirect High
Taking Your Fundus Exam to the Next Level Dr. Kelly Thompson Cincinnati VA Medical Center Taking Your Fundus Exam to the Next Level Resident Assistants Student Subjects Fundus Biomicroscopy Indirect High
Adult and Paediatric Retina (Vitreo-Retinal Surgery, Laser and Intravitreal Injection)
 CV Name: Dr Loh Boon Kwang Specialty: General Ophthalmology and Cataract Surgery Subspecialty: Adult and Paediatric Retina (Vitreo-Retinal Surgery, Laser and Intravitreal Injection) Adult Retina Conditions
CV Name: Dr Loh Boon Kwang Specialty: General Ophthalmology and Cataract Surgery Subspecialty: Adult and Paediatric Retina (Vitreo-Retinal Surgery, Laser and Intravitreal Injection) Adult Retina Conditions
Patient Information Cataract surgery
 Patient Information Cataract surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Patient Information Cataract surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
BSM Connection elearning Course
 BSM Connection elearning Course Scope of the Eye Care Practice 2008, BSM Consulting All Rights Reserved. Table of Contents OVERVIEW...1 THREE O S IN EYE CARE...1 ROUTINE VS. MEDICAL EXAMS...2 CONTACT LENSES/GLASSES...2
BSM Connection elearning Course Scope of the Eye Care Practice 2008, BSM Consulting All Rights Reserved. Table of Contents OVERVIEW...1 THREE O S IN EYE CARE...1 ROUTINE VS. MEDICAL EXAMS...2 CONTACT LENSES/GLASSES...2
How To Improve Eye Acuity With Laser Vision Correction
 The future of cataract surgery has arrived A cataract clouding of the eye s natural lens as a result of aging or injury is the leading cause of preventable blindness worldwide. 1 Cataract surgery is one
The future of cataract surgery has arrived A cataract clouding of the eye s natural lens as a result of aging or injury is the leading cause of preventable blindness worldwide. 1 Cataract surgery is one
Patient information factsheet. Cataract surgery. Consent for cataract surgery
 Patient information factsheet Cataract surgery Consent for cataract surgery This leaflet gives you information that will help you decide whether to have cataract surgery. You might want to discuss it with
Patient information factsheet Cataract surgery Consent for cataract surgery This leaflet gives you information that will help you decide whether to have cataract surgery. You might want to discuss it with
Guide to Eye Surgery and Eye-related Claims
 If you or a loved one have suffered because of a negligent error during eye treatment or surgery, you may be worried about how you will manage in the future, particularly if your eyesight has been made
If you or a loved one have suffered because of a negligent error during eye treatment or surgery, you may be worried about how you will manage in the future, particularly if your eyesight has been made
Glenn B. Cook, M.D., Ph.D. DIPLOMATE AMERICAN BOARD OF OPHTHALMOLOGY Coronado Eye Associates
 Glenn B. Cook, M.D., Ph.D. INFORMED CONSENT FOR CATARACT OPERATION AND/OR IMPLANTATION OF INTRAOCULAR LENS INTRODUCTION: RIGHT / LEFT This information is given to you so that you can make an informed decision
Glenn B. Cook, M.D., Ph.D. INFORMED CONSENT FOR CATARACT OPERATION AND/OR IMPLANTATION OF INTRAOCULAR LENS INTRODUCTION: RIGHT / LEFT This information is given to you so that you can make an informed decision
WHAT IS A CATARACT, AND HOW IS IT TREATED?
 4089 TAMIAMI TRAIL NORTH SUITE A103 NAPLES, FL 34103 TELEPHONE (239) 262-2020 FAX (239) 435-1084 DOES THE PATIENT NEED OR WANT A TRANSLATOR, INTERPRETOR OR READER? YES NO TO THE PATIENT: You have the right,
4089 TAMIAMI TRAIL NORTH SUITE A103 NAPLES, FL 34103 TELEPHONE (239) 262-2020 FAX (239) 435-1084 DOES THE PATIENT NEED OR WANT A TRANSLATOR, INTERPRETOR OR READER? YES NO TO THE PATIENT: You have the right,
CONSENT FOR CATARACT SURGERY
 CONSENT FOR CATARACT SURGERY INTRODUCTION The natural crystalline lens can become cloudy due to aging, trauma, disease or medications. This condition is called a cataract. When cataracts become visually
CONSENT FOR CATARACT SURGERY INTRODUCTION The natural crystalline lens can become cloudy due to aging, trauma, disease or medications. This condition is called a cataract. When cataracts become visually
Information For Consent For Cataract Surgery
 Information For Consent For Cataract Surgery Your Ophthalmologist has diagnosed you with a visually significant cataract. The following handout will explain your condition and give you the information
Information For Consent For Cataract Surgery Your Ophthalmologist has diagnosed you with a visually significant cataract. The following handout will explain your condition and give you the information
11/11/2015. Glaucoma: Diagnosis and Treatment. Financial disclosures. Glaucoma: the problem. Joshua J. Ney, M.D. No disclosures to report
 Glaucoma: Diagnosis and Treatment Joshua J. Ney, M.D. No disclosures to report Financial disclosures Glaucoma: the problem Glaucoma is second most common cause of blindness worldwide 7 million people are
Glaucoma: Diagnosis and Treatment Joshua J. Ney, M.D. No disclosures to report Financial disclosures Glaucoma: the problem Glaucoma is second most common cause of blindness worldwide 7 million people are
Vitreomacular Traction: What s the Role of the Vitreoretinal Interface in this Disease?
 Vitreomacular Traction: What s the Role of the Vitreoretinal Interface in this Disease? Robert A. Stoltz, M.D., Ph.D. Georgia Retina, P.C. Retinal Pearls 2013 Anatomy of the Vitreous Gel Physical Properties
Vitreomacular Traction: What s the Role of the Vitreoretinal Interface in this Disease? Robert A. Stoltz, M.D., Ph.D. Georgia Retina, P.C. Retinal Pearls 2013 Anatomy of the Vitreous Gel Physical Properties
OfficeMate 11.0 Enhancements
 In this document: Eyefinity EHR Integration, 1 Patient Center, 2 Patient Demographic, 2 Rx Order Windows, 3 Products and Services, 4 For more detailed information on how to use the new features in OfficeMate
In this document: Eyefinity EHR Integration, 1 Patient Center, 2 Patient Demographic, 2 Rx Order Windows, 3 Products and Services, 4 For more detailed information on how to use the new features in OfficeMate
Involution of Threshold Retinopathy of Prematurity after Diode Laser Photocoagulation
 Involution of Threshold Retinopathy of Prematurity after Diode Laser Photocoagulation David K. Coats, MD, 1,2 Aaron M. Miller, MD, 1 Kathryn M. Brady McCreery, MD, 1 Eric R. Holz, MD, 1 Evelyn A. Paysse,
Involution of Threshold Retinopathy of Prematurity after Diode Laser Photocoagulation David K. Coats, MD, 1,2 Aaron M. Miller, MD, 1 Kathryn M. Brady McCreery, MD, 1 Eric R. Holz, MD, 1 Evelyn A. Paysse,
lenses with the vitrophage
 British Journal of Ophthalmology, 1979, 63, 771-77 Management of subluxated and dislocated lenses with the vitrophage GHOLAM A. PEYMAN, MOTILAL RAICHAND, MORTON F. GOLDBERG, AND DANIEL RITACCA From the
British Journal of Ophthalmology, 1979, 63, 771-77 Management of subluxated and dislocated lenses with the vitrophage GHOLAM A. PEYMAN, MOTILAL RAICHAND, MORTON F. GOLDBERG, AND DANIEL RITACCA From the
The Nurse/Technician Role Within the Emerging Ophthalmic Technology - OCTs/B-Scan
 The Nurse/Technician Role Within the Emerging Ophthalmic Technology - OCTs/B-Scan Margie V. Wilson, COMT Chief Clinical Supervisor UCSD Shiley Eye Center Thanks, Carol! Unfortunately. I have not financial
The Nurse/Technician Role Within the Emerging Ophthalmic Technology - OCTs/B-Scan Margie V. Wilson, COMT Chief Clinical Supervisor UCSD Shiley Eye Center Thanks, Carol! Unfortunately. I have not financial
Informed Consent for Refractive Lens Exchange (Clear Lens Replacement)
 Mark Packer, M.D. Informed Consent for Refractive Lens Exchange (Clear Lens Replacement) This surgery involves the removal of the natural lens of my eye, even though it is not a cataract. The natural lens
Mark Packer, M.D. Informed Consent for Refractive Lens Exchange (Clear Lens Replacement) This surgery involves the removal of the natural lens of my eye, even though it is not a cataract. The natural lens
Avastin (Bevacizumab) Intravitreal Injection
 Avastin (Bevacizumab) Intravitreal Injection This handout describes how Avastin may be used to treat wet age related macular degeneration (AMD) or macular edema due to retinal vascular disease such as
Avastin (Bevacizumab) Intravitreal Injection This handout describes how Avastin may be used to treat wet age related macular degeneration (AMD) or macular edema due to retinal vascular disease such as
How To Know If You Can See Without Glasses Or Contact Lense After Lasik
 The LASIK experience I WHO CAN HAVE LASIK? To be eligible for LASIK you should be at least 21 years of age, have healthy eyes and be in good general health. Your vision should not have deteriorated significantly
The LASIK experience I WHO CAN HAVE LASIK? To be eligible for LASIK you should be at least 21 years of age, have healthy eyes and be in good general health. Your vision should not have deteriorated significantly
Explanation of the Procedure
 Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
PANRETINAL PHOTOCOAGULATION (PRP) FOR RUBEOSIS AND NEOVASCULAR GLAUCOMA ERIC S. MANN M.D., Ph.D.
 PANRETINAL PHOTOCOAGULATION (PRP) FOR RUBEOSIS AND NEOVASCULAR GLAUCOMA ERIC S. MANN M.D., Ph.D. A. INTRODUCTION Rubeosis involves the growth of abnormal blood vessels on the iris (the diaphragm-like structure
PANRETINAL PHOTOCOAGULATION (PRP) FOR RUBEOSIS AND NEOVASCULAR GLAUCOMA ERIC S. MANN M.D., Ph.D. A. INTRODUCTION Rubeosis involves the growth of abnormal blood vessels on the iris (the diaphragm-like structure
CRYOTHERAPY FOR RETINAL BREAK, LATTICE DEGENERATION, OR LIMITED RETINAL DETACHMENT ERIC S. MANN M.D., Ph.D.
 CRYOTHERAPY FOR RETINAL BREAK, LATTICE DEGENERATION, OR LIMITED RETINAL DETACHMENT ERIC S. MANN M.D., Ph.D. A. INTRODUCTION: Retinal break is an opening on the retina, usually located at the periphery.
CRYOTHERAPY FOR RETINAL BREAK, LATTICE DEGENERATION, OR LIMITED RETINAL DETACHMENT ERIC S. MANN M.D., Ph.D. A. INTRODUCTION: Retinal break is an opening on the retina, usually located at the periphery.
BRANCH RETINAL VEIN OCCLUSION (BRVO) AND LASER TREATMENT
 INTRODUCTION: BRANCH RETINAL VEIN OCCLUSION (BRVO) AND LASER TREATMENT Branch Retinal Vein Occlusion (BRVO) involves the obstruction of a major venous blood vessel which prevents adequate drainage of blood
INTRODUCTION: BRANCH RETINAL VEIN OCCLUSION (BRVO) AND LASER TREATMENT Branch Retinal Vein Occlusion (BRVO) involves the obstruction of a major venous blood vessel which prevents adequate drainage of blood
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
EUROPEAN JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.ejpmr.com
 ejpmr, 2015,2(3), 436-440 EUROPEAN JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.ejpmr.com Tumram et al. SJIF Impact Factor 2.026 Research Article ISSN 3294-3211 EJPMR CLINICAL OUTCOME OF TORIC IOL
ejpmr, 2015,2(3), 436-440 EUROPEAN JOURNAL OF PHARMACEUTICAL AND MEDICAL RESEARCH www.ejpmr.com Tumram et al. SJIF Impact Factor 2.026 Research Article ISSN 3294-3211 EJPMR CLINICAL OUTCOME OF TORIC IOL
Overview of Refractive Surgery
 Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH)
 Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH) Competencies addressed: PC = Patient care MK = Medical knowledge Pr = Professionalism PBLI = Practice-based
Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH) Competencies addressed: PC = Patient care MK = Medical knowledge Pr = Professionalism PBLI = Practice-based
CONSENT FORM. Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
Providing Optimal Optics For Your Astigmatic Cataract Patients. While the cornea remains relatively stable and prolate throughout life
 Providing Optimal Optics For Your Astigmatic Cataract Patients David I. Geffen, OD, FAAO Why keep the crystalline lens? While the cornea remains relatively stable and prolate throughout life Unless we
Providing Optimal Optics For Your Astigmatic Cataract Patients David I. Geffen, OD, FAAO Why keep the crystalline lens? While the cornea remains relatively stable and prolate throughout life Unless we
Corporate Medical Policy
 Corporate Medical Policy Intravitreal Implant File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intravitreal_implant 11/2010 6/2015 6/2016 6/2015 Description of Procedure or Service
Corporate Medical Policy Intravitreal Implant File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intravitreal_implant 11/2010 6/2015 6/2016 6/2015 Description of Procedure or Service
Post LASIK Ectasia. Examination: Gina M. Rogers, MD and Kenneth M. Goins, MD
 Post LASIK Ectasia Gina M. Rogers, MD and Kenneth M. Goins, MD October 6, 2012 Chief Complaint: Decreasing vision after laser- assisted in- situ keratomileusis (LASIK) History of Present Illness: This
Post LASIK Ectasia Gina M. Rogers, MD and Kenneth M. Goins, MD October 6, 2012 Chief Complaint: Decreasing vision after laser- assisted in- situ keratomileusis (LASIK) History of Present Illness: This
Cataracts & Cataract surgery
 Cataracts & Cataract surgery Normal Vision What is a cataract? Light passes through the cornea-the curved, clear front surface of the eye. It then passes through the pupil and the lens. The curved surface
Cataracts & Cataract surgery Normal Vision What is a cataract? Light passes through the cornea-the curved, clear front surface of the eye. It then passes through the pupil and the lens. The curved surface
EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE?
 24. Glaucoma: Imaging EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE? Chief Author: Dr. Amit porwal 1 Co-Authors: Dr. Kavita Porwal 2, Dr. Puja Rai 1 1. Choithram Netralaya,
24. Glaucoma: Imaging EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE? Chief Author: Dr. Amit porwal 1 Co-Authors: Dr. Kavita Porwal 2, Dr. Puja Rai 1 1. Choithram Netralaya,
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
BACKGROUND INFORMATION AND INFORMED CONSENT FOR CATARACT SURGERY AND IMPLANTATION OF AN INTRAOCULAR LENS
 OMNI EYE SPECIALISTS A Madison Street Company Proudly Owned by Employees Specializing in Medical and Surgical Care of the Eye 55 Madison St, Suite 355 Denver CO 80206 303-377-2020 800-GO-2-OMNI www.omnieye.com
OMNI EYE SPECIALISTS A Madison Street Company Proudly Owned by Employees Specializing in Medical and Surgical Care of the Eye 55 Madison St, Suite 355 Denver CO 80206 303-377-2020 800-GO-2-OMNI www.omnieye.com
Descemet s stripping with endothelial keratoplasty in 200 eyes
 J CATARACT REFRACT SURG - VOL 32, MARCH 2006 Descemet s stripping with endothelial keratoplasty in 200 eyes Early challenges and techniques to enhance donor adherence Francis W. Price Jr, MD, Marianne
J CATARACT REFRACT SURG - VOL 32, MARCH 2006 Descemet s stripping with endothelial keratoplasty in 200 eyes Early challenges and techniques to enhance donor adherence Francis W. Price Jr, MD, Marianne
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment
 Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
This newest generation laser offers specific technological features and treatment options designed to substantially improve the retina laser therapy:
 1 The latest generation of Quantel Medical Multispot Laser (Supra Scan 577) offers new technological features and treatment methods for improving retina laser therapy. Q uantel Medical Lasers give excellent
1 The latest generation of Quantel Medical Multispot Laser (Supra Scan 577) offers new technological features and treatment methods for improving retina laser therapy. Q uantel Medical Lasers give excellent
RAPID CLINICAL REPORT
 RAPID CLINICAL REPORT ADVERSE EFFECTS ASSOCIATED WITH THE ABSENCE OF HYALURONIDASE IN ANESTHESIA FOR CATARACT SURGERY Background: Issued February 13, 2001 Hyaluronidase (Wydase ) is a medical preparation
RAPID CLINICAL REPORT ADVERSE EFFECTS ASSOCIATED WITH THE ABSENCE OF HYALURONIDASE IN ANESTHESIA FOR CATARACT SURGERY Background: Issued February 13, 2001 Hyaluronidase (Wydase ) is a medical preparation
An Informational Guide to CENTRAL RETINAL VEIN OCCLUSION
 Science of CRVO www.scienceofcrvo.org An Informational Guide to CENTRAL RETINAL VEIN OCCLUSION This brochure will guide you in understanding CRVO and the treatment options available to prevent vision loss.
Science of CRVO www.scienceofcrvo.org An Informational Guide to CENTRAL RETINAL VEIN OCCLUSION This brochure will guide you in understanding CRVO and the treatment options available to prevent vision loss.
Surgeon Presentation
 Surgeon Presentation Outline Future of Myopic Refractive Surgery Phakic IOLs: Evolution & Technology The Verisyse Anterior Chamber, Iris-Fixated Phakic IOL Product features Clinical data Patient selection,
Surgeon Presentation Outline Future of Myopic Refractive Surgery Phakic IOLs: Evolution & Technology The Verisyse Anterior Chamber, Iris-Fixated Phakic IOL Product features Clinical data Patient selection,
Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report
 Case Reports in Ophthalmological Medicine Volume 2011, Article ID 796463, 4 pages doi:10.1155/2011/796463 Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report Ming Chen
Case Reports in Ophthalmological Medicine Volume 2011, Article ID 796463, 4 pages doi:10.1155/2011/796463 Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report Ming Chen
Principles of Diagnosis MEDICAL DECISION-MAKING IN OPTOMETRIC PRACTICE. Medical Decision-Making. Medical Decision-Making.
 MEDICAL DECISION-MAKING IN OPTOMETRIC PRACTICE Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 [email protected] Principles of Diagnosis The study of the art and science of
MEDICAL DECISION-MAKING IN OPTOMETRIC PRACTICE Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 [email protected] Principles of Diagnosis The study of the art and science of
Getting Ready for ICD-10. Dianna Hoskins, OCS Cincinnati Eye Institute
 Dianna Hoskins, OCS Cincinnati Eye Institute Chart Documentation: Will your documentation stand up to ICD-10? Do you always mark which eye, severity or status of the disease (chronic or acute), site, etiology
Dianna Hoskins, OCS Cincinnati Eye Institute Chart Documentation: Will your documentation stand up to ICD-10? Do you always mark which eye, severity or status of the disease (chronic or acute), site, etiology
